User login
Rules of Engagement Necessary for Comanagement of Orthopedic Patients
One of our providers wants to use adult hospitalists for coverage of inpatient orthopedic surgery patients. Is this acceptable practice? Are there qualifiers?
–Libby Gardner
Dr. Hospitalist responds:
Let’s see how far we can tackle this open-ended question. There has been lots of discussion on the topic of comanagement in the past by people eminently more qualified than I am. Still, it never hurts to take a fresh look at things.
For one, on the subject of admissions, I am a firm believer that hospitalists should admit all adult hip fractures. The overwhelming majority of the time, these patients are elderly with comorbid conditions. Sure, they are going to get their hip fixed, because the alternative is usually unacceptable, but some thought needs to go into the process. The orthopedic surgeon sees a hip that needs fixing and not much else. When issues like renal failure, afib, CHF, prior DVT, or dementia are present, hospitalists should take charge of the case. It is the best way to ensure that the patient receives optimal medical care and the documentation that goes along with it. I love our orthopedic surgeons, but I don’t want them primarily admitting, managing, and discharging my elderly patients. Let the surgeon do what they do best, which is operate, and leave the rest to us.
On the subject of orthopedic trauma, I take the exact opposite tack—this is not something for which I or most of my colleagues have expertise. A young, healthy patient with trauma should be admitted by the orthopedic service; that patient population’s complications are much more likely to be directly related to their trauma.
When it comes to elective surgery, when the admitting surgeon (orthopedic or otherwise) wants the help of a hospitalist, then I think it is of paramount importance to have clear “rules of engagement.” I think with good expectations, you can have a fantastic working relationship with your surgeons. Without them, it becomes a nightmare.
Here are my HM group’s rules for elective orthopedic surgery:
- Orthopedics handles all pain medications and VTE prophylaxis, including discharge prescriptions.
- Medicine handles all admit and discharge medication reconciliation (“med rec”).
- There is shared discussion on:
- Need for transfusion; and
- The VTE prophylaxis when a patient already is on chronic anticoagulation.
We do not vary from this protocol. I never adjust a patient’s pain medications. Even the floor nurses know this. Because I’m doing the admit med rec, it also means that the patient doesn’t have their HCTZ continued after 600cc of EBL and spinal anesthesia.
The system works because the rules are clear and the communication is consistent. This does not mean that we cover the orthopedic service at night. They are equally responsible for their patients under the items outlined above. In my view—and this might sound simplistic—the surgeon caused the post-op pain, so they should be responsible for managing it. On VTE prophylaxis, I might take a more nuanced view, but for our surgeons, they own the wound and the post-op follow-up, so they get the choice on what agent to use.
Would I accept an arrangement in which I covered all the orthopedic issues out of regular hours? Nope—not when they have primary responsibility for the case; they should always be directly available to the nurse. I think that anything else would be a system ripe for abuse.
Our exact rules will not work for every situation, but I would strongly encourage the two basic tenets from above: No. 1, the hospitalist should primarily admit and manage elderly hip fractures, and No. 2, clear rules of engagement should be established with your orthopedic or surgery group. It’s a discussion worth having during daylight hours, because trying to figure out the rules at 3 in the morning rarely ends well.
One of our providers wants to use adult hospitalists for coverage of inpatient orthopedic surgery patients. Is this acceptable practice? Are there qualifiers?
–Libby Gardner
Dr. Hospitalist responds:
Let’s see how far we can tackle this open-ended question. There has been lots of discussion on the topic of comanagement in the past by people eminently more qualified than I am. Still, it never hurts to take a fresh look at things.
For one, on the subject of admissions, I am a firm believer that hospitalists should admit all adult hip fractures. The overwhelming majority of the time, these patients are elderly with comorbid conditions. Sure, they are going to get their hip fixed, because the alternative is usually unacceptable, but some thought needs to go into the process. The orthopedic surgeon sees a hip that needs fixing and not much else. When issues like renal failure, afib, CHF, prior DVT, or dementia are present, hospitalists should take charge of the case. It is the best way to ensure that the patient receives optimal medical care and the documentation that goes along with it. I love our orthopedic surgeons, but I don’t want them primarily admitting, managing, and discharging my elderly patients. Let the surgeon do what they do best, which is operate, and leave the rest to us.
On the subject of orthopedic trauma, I take the exact opposite tack—this is not something for which I or most of my colleagues have expertise. A young, healthy patient with trauma should be admitted by the orthopedic service; that patient population’s complications are much more likely to be directly related to their trauma.
When it comes to elective surgery, when the admitting surgeon (orthopedic or otherwise) wants the help of a hospitalist, then I think it is of paramount importance to have clear “rules of engagement.” I think with good expectations, you can have a fantastic working relationship with your surgeons. Without them, it becomes a nightmare.
Here are my HM group’s rules for elective orthopedic surgery:
- Orthopedics handles all pain medications and VTE prophylaxis, including discharge prescriptions.
- Medicine handles all admit and discharge medication reconciliation (“med rec”).
- There is shared discussion on:
- Need for transfusion; and
- The VTE prophylaxis when a patient already is on chronic anticoagulation.
We do not vary from this protocol. I never adjust a patient’s pain medications. Even the floor nurses know this. Because I’m doing the admit med rec, it also means that the patient doesn’t have their HCTZ continued after 600cc of EBL and spinal anesthesia.
The system works because the rules are clear and the communication is consistent. This does not mean that we cover the orthopedic service at night. They are equally responsible for their patients under the items outlined above. In my view—and this might sound simplistic—the surgeon caused the post-op pain, so they should be responsible for managing it. On VTE prophylaxis, I might take a more nuanced view, but for our surgeons, they own the wound and the post-op follow-up, so they get the choice on what agent to use.
Would I accept an arrangement in which I covered all the orthopedic issues out of regular hours? Nope—not when they have primary responsibility for the case; they should always be directly available to the nurse. I think that anything else would be a system ripe for abuse.
Our exact rules will not work for every situation, but I would strongly encourage the two basic tenets from above: No. 1, the hospitalist should primarily admit and manage elderly hip fractures, and No. 2, clear rules of engagement should be established with your orthopedic or surgery group. It’s a discussion worth having during daylight hours, because trying to figure out the rules at 3 in the morning rarely ends well.
One of our providers wants to use adult hospitalists for coverage of inpatient orthopedic surgery patients. Is this acceptable practice? Are there qualifiers?
–Libby Gardner
Dr. Hospitalist responds:
Let’s see how far we can tackle this open-ended question. There has been lots of discussion on the topic of comanagement in the past by people eminently more qualified than I am. Still, it never hurts to take a fresh look at things.
For one, on the subject of admissions, I am a firm believer that hospitalists should admit all adult hip fractures. The overwhelming majority of the time, these patients are elderly with comorbid conditions. Sure, they are going to get their hip fixed, because the alternative is usually unacceptable, but some thought needs to go into the process. The orthopedic surgeon sees a hip that needs fixing and not much else. When issues like renal failure, afib, CHF, prior DVT, or dementia are present, hospitalists should take charge of the case. It is the best way to ensure that the patient receives optimal medical care and the documentation that goes along with it. I love our orthopedic surgeons, but I don’t want them primarily admitting, managing, and discharging my elderly patients. Let the surgeon do what they do best, which is operate, and leave the rest to us.
On the subject of orthopedic trauma, I take the exact opposite tack—this is not something for which I or most of my colleagues have expertise. A young, healthy patient with trauma should be admitted by the orthopedic service; that patient population’s complications are much more likely to be directly related to their trauma.
When it comes to elective surgery, when the admitting surgeon (orthopedic or otherwise) wants the help of a hospitalist, then I think it is of paramount importance to have clear “rules of engagement.” I think with good expectations, you can have a fantastic working relationship with your surgeons. Without them, it becomes a nightmare.
Here are my HM group’s rules for elective orthopedic surgery:
- Orthopedics handles all pain medications and VTE prophylaxis, including discharge prescriptions.
- Medicine handles all admit and discharge medication reconciliation (“med rec”).
- There is shared discussion on:
- Need for transfusion; and
- The VTE prophylaxis when a patient already is on chronic anticoagulation.
We do not vary from this protocol. I never adjust a patient’s pain medications. Even the floor nurses know this. Because I’m doing the admit med rec, it also means that the patient doesn’t have their HCTZ continued after 600cc of EBL and spinal anesthesia.
The system works because the rules are clear and the communication is consistent. This does not mean that we cover the orthopedic service at night. They are equally responsible for their patients under the items outlined above. In my view—and this might sound simplistic—the surgeon caused the post-op pain, so they should be responsible for managing it. On VTE prophylaxis, I might take a more nuanced view, but for our surgeons, they own the wound and the post-op follow-up, so they get the choice on what agent to use.
Would I accept an arrangement in which I covered all the orthopedic issues out of regular hours? Nope—not when they have primary responsibility for the case; they should always be directly available to the nurse. I think that anything else would be a system ripe for abuse.
Our exact rules will not work for every situation, but I would strongly encourage the two basic tenets from above: No. 1, the hospitalist should primarily admit and manage elderly hip fractures, and No. 2, clear rules of engagement should be established with your orthopedic or surgery group. It’s a discussion worth having during daylight hours, because trying to figure out the rules at 3 in the morning rarely ends well.
When Is Testing for Thrombophilia Indicated?
The Case
A healthy 42-year-old woman presents to the hospital with acute-onset pleuritic chest pain and shortness of breath. She has not had any recent surgeries, takes no medications, and is very active. A lung ventilation-perfusion scan reveals a high probability of pulmonary embolism (PE). The patient’s history is notable for two second-trimester pregnancy losses. The patient is started on low-molecular heparin and warfarin (LMHW).
Should this patient be tested for thrombophilia?
Background
Thrombophilia can now be identified in more than half of all patients presenting with VTE, and testing for underlying causes of thrombophilia has become widespread.1 Physicians believe that thrombophilia testing frequently changes management of patients with VTE.2
Thrombophilias can be classified into three major categories: deficiency of natural inhibitors of coagulation, abnormal function or elevated level of coagulation factors, and acquired thrombophilias (see Table 1).
The prevalence of specific thrombophilias varies widely. For example, the prevalence of activated protein C resistance (the factor V Leiden mutation) is 3% to 7%. In comparison, the prevalence of antithrombin deficiency is estimated at 0.02%. Each thrombophilia is associated with an increased VTE risk, but the level of risk associated with a given thrombophilia varies greatly.1
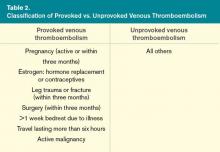
Before testing for thrombophilia in acute VTE, assess the risk of recurrent VTE by determining if the thrombosis was provoked or unprovoked. A VTE event is considered provoked if it occurs in the setting of pregnancy within the previous three months; estrogen therapy; immobility from acute illness for more than one week; travel lasting for more than six hours; leg trauma, fracture, or surgery within the previous three months; or active malignancy (see Table 2,).3 Unprovoked VTE has a recurrence rate of 7.4% per patient year, compared with 3.3% per patient year for a provoked VTE; the risk is even lower (0.7% per patient year) if the risk factor for the provoked VTE was surgical.4
Testing for thrombophilia is indicated if the results would add significant prognostic information beyond the clinical history, or if it would change patient management—in particular, the intensity or the duration of anticoagulation.
Review of the Data
Does presence of thrombophilia alter the intensity of anticoagulation for VTE?
If thrombophilia increases the risk of VTE recurrence while on anticoagulation, then a more intense level of anticoagulation might prevent future VTE. There are no studies investigating higher intensity of anticoagulation, but if standard anticoagulation were insufficient for patients with identifiable thrombophilia, one might expect to observe increased recurrence rates among patients with thrombophilia treated with standard warfarin therapy.
In a substudy of the Extended Low-Intensity Anticoagulation for Unprovoked Venous ThromboEmbolism (ELATE) trial, the risk of recurrence of VTE among treated subjects was very low overall, and the presence of thrombophilic abnormalities was not associated with significantly higher risk.5 Observational studies have found VTE recurrence rates are low in patients treated with warfarin, with or without thrombophilia.6-8
The impact of the initial level of anticoagulation on recurrence after the completion of the treatment period has been evaluated. Although one study suggested that patients with substandard levels of anticoagulation were at an increased risk of subsequent VTE, this was not confirmed in the Leiden Thrombophilia Study (LETS). 9,10
In sum, the majority of data do not suggest a significantly increased risk of recurrent VTE in patients with thrombophilia treated with standard anticoagulation. Therefore, treatment with warfarin to a goal INR of 2 to 3 is sufficient.
Does presence of thrombophilia alter duration of VTE treatment?
A major decision clinicians face when caring for VTE patients is the duration of anticoagulation treatment. The current ACCP recommendation for treatment of a provoked VTE is three months, with treatment for an unprovoked VTE three months or lifelong.11 If the presence of thrombophilia increases the risk of recurrence after cessation of anticoagulation treatment, longer duration of treatment might be indicated. One of the goals of thrombophilia testing should be to identify those patients.
Overall, the recurrence rate after first VTE is high, with a cumulative incidence of 25% at five years, 30% at eight years, and 56% at 20 years.12,13
Deficiency of natural inhibitors of coagulation.
Deficiency of a natural inhibitor of coagulation has been associated with a risk of recurrence of VTE of as much as 10% per year, according to some studies.6,14 However, the estimates are based on studies that include individuals from thrombosis-prone families, and selection bias might have contributed to the high recurrence rates.1 In the unselected population represented in the LETS study, only a modest elevation was seen in the estimated risk of recurrence for patients with inhibitor deficiencies.15
Testing for deficiency of inhibitors offers little prognostic information beyond that obtained when determining whether a VTE event is provoked or unprovoked. In studies that have separately examined subjects with provoked vs. unprovoked VTE, deficiency of an inhibitor is not associated with increased risk of recurrence.15,16
Abnormal function or level of anticoagulation factors.
Factor V Leiden (FVL) is the most common cause of inherited thrombophilia and is associated with as much as a sixfold increase in VTE risk, while the prothrombin gene mutation is associated with a twofold increase.17,18
In contrast, the evidence associating these mutations with recurrent VTE risk is not as consistent. Although a study conducted at a referral center in Italy found an increased risk of recurrence with either Factor V Leiden or prothrombin gene mutation, a large meta-analysis of 23 studies found increased risk only with Factor V Leiden.19,20 Another meta-analysis demonstrated only a modest increased risk of recurrence in subjects with Factor V Leiden or prothrombin gene mutation, and a prospective study from Austria found no increased risk of recurrence with Factor V Leiden two years after discontinuation of anticoagulation.18,21 Additionally, when using patients with unprovoked VTE as reference, there was no increased risk of recurrence among patients homozygous for Factor V Leiden or the prothrombin gene mutation.22
In summary, although Factor V Leiden and prothrombin gene defects are associated with increased risk of recurrent VTE, the magnitude of the risk increase is modest and, therefore, should not alter duration of therapy.
Acquired thrombophilia.
It appears that the only thrombophilic state that might have a significant impact on the risk of recurrence is the antiphospholipid syndrome. The cessation of warfarin therapy in patients with thrombosis associated with antiphospholipid antibodies carries a 69% risk of recurrent thrombosis within a year.23 Some studies have suggested that the presence of specific antibodies (i.e. anticardiolipin antibodies) is associated with increased risk in patients with antiphospholipid syndrome.24
However, at present, all patients with VTE and antiphospholipid syndrome should be candidates for lifelong anticoagulation. Antiphospholipid antibody testing should be performed in patients with a suggestive history, including those with recurrent fetal loss or a single fetal loss after 10 weeks, or known collagen vascular disease.25
The role of provoked vs. unprovoked VTE.
Identifying whether a VTE is provoked or unprovoked has been shown to be an important predictor of recurrence. For example, one prospective, cohort study found two-year recurrence rates of zero in patients with a surgery or pregnancy-related VTE, 9% with other provoked VTE, and 19% with unprovoked VTE.26 In the same study, thrombophilia testing failed to reliably predict recurrence risk. Patients with unprovoked VTE who were tested and found to not have a defect were at equally high risk of recurrent VTE as those found to have a thrombophilia.27
The most significant predictor for VTE recurrence is whether the first event was provoked, and thrombophilia testing offers little additional prognostic information.28
VTE as a multifactorial disorder.
It is becoming increasingly clear that VTE is multifactorial disorder, caused by the interactions of genotypic, phenotypic, and environmental factors. In the case of an unprovoked VTE, the patient already carries a significantly elevated risk for recurrence, and further testing for known causes of thrombophilia appears to add very little additional information. The optimal duration of anticoagulation for unprovoked VTE is unclear, but current guidelines suggest at least three months—and clinicians should consider lifelong treatment.
In the vast majority of cases, testing for thrombophilia has no impact on the management of VTE and is not warranted. In patients with antiphospholipid-antibody syndrome, given the high risk of recurrence, long-term anticoagulation after a first VTE might be indicated. In select patients with a clinical picture suggestive of antiphospholipid-antibody syndrome, or a strong family history, testing should be considered.
Back to the Case
Our patient appears to have an unprovoked VTE. She should receive regular anticoagulation with warfarin, with a goal INR of 2 to 3, for at least three months. Lifelong anticoagulation therapy should be considered. Testing for heritable thrombophilia will not change the current management or treatment duration and, hence, is not indicated. However, the patient’s history is suggestive of antiphospholipid-antibody syndrome, so she should be tested. If the diagnosis of antiphospholipid syndrome is made, lifelong anticoagulation should be considered.
Bottom Line
Unprovoked VTE provides the strongest predictor for recurrence. Thrombophilia testing adds little in predicting recurrence and rarely is indicated.
Dr. Stehlikova is a clinical hospitalist in the division of hospital medicine, department of medicine, at Albert Einstein College of Medicine and Montefiore Medical Center in Bronx, N.Y. Dr. Martin is director of the Einstein Hospitalist Service. Dr. Janakiram is a fellow in the department of hematology at Einstein, and Dr. Korcak is an instructor at Einstein in the department of medicine and director of the Weiler Medical Service. Dr. Galhotra is associate director for inpatient quality in the department of medicine at Einstein; Dr. Averbukh is an academic hospitalist; and Dr. Southern is chief of the division of hospital medicine at Einstein.
References
- Middeldorp S, van Hylckama Vlieg A. Does thrombophilia testing help in the clinical management of patients? Br J Haematol. 2008;143:321-335.
- Coppens M, van Mourik JA, Eckmann CM, Büller HR, Middeldorp S. Current practise of testing for inherited thrombophilia. J Thromb Haemost. 2007;5:1979-1981.
- Prandoni P, Noventa F, Ghirarduzzi A, et al. The risk of recurrent venous thromboembolism after discontinuing anticoagulation in patients with acute proximal deep vein thrombosis or pulmonary embolism. A prospective cohort study in 1,626 patients. Haematologica. 2007;92:199-205.
- Iorio A, Kearon C, Filippucci E, et al. Risk of recurrence after a first episode of symptomatic venous thromboembolism provoked by a transient risk factor: a systematic review. Arch Intern Med. 2010;170:1710-1716.
- Kearon C, Julian JA, Kovacs MJ, et al. Influence of thrombophilia on risk of recurrent venous thromboembolism while on warfarin: results from a randomized trial. Blood. 2008;112:4432-4436.
- Vossen CY, Walker ID, Svensson P, et al. Recurrence rate after a first venous thrombosis in patients with familial thrombophilia. Arterioscler Thromb Vasc Biol. 2005;25:1992-1997.
- Brown K, Luddington R, Williamson D, Baker P, Baglin T. Risk of venous thromboembolism associated with a G to A transition at position 20210 in the 3'-untranslated region of the prothrombin gene. Br J Haematol. 1997;98:907-909.
- Schulman S, Tengborn L. Treatment of venous thromboembolism in patients with congenital deficiency of antithrombin III. Thromb Haemost. 1992;68:634-636.
- Palareti G, Legnani C, Cosmi B, Guazzaloca G, Cini M, Mattarozzi S. Poor anticoagulation quality in the first 3 months after unprovoked venous thromboembolism is a risk factor for long-term recurrence. J Thromb Haemost. 2005;3:955-961.
- Gadisseur AP, Christiansen SC, van der Meer FJ, Rosendaal FR. The quality of oral anticoagulant therapy and recurrent venous thrombotic events in the Leiden Thrombophilia Study. J Thromb Haemost. 2007;5:931-936.
- Kearon C, Kahn SR, Agnelli G, Goldhaber S, Raskob GE, Comerota AJ. Antithrombotic therapy for venous thromboembolic disease: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition). Chest. 2008;133:454S-545S.
- Prandoni P, Lensing AW, Cogo A, et al. The long-term clinical course of acute deep venous thrombosis. Ann Intern Med. 1996;125:1-7.
- Laczkovics C, Grafenhofer H, Kaider A, et al. Risk of recurrence after a first venous thromboembolic event in young women. Haematologica. 2007;92:1201-1207.
- Brouwer JL, Lijfering WM, Ten Kate MK, Kluin-Nelemans HC, Veeger NJ, van der Meer J. High long-term absolute risk of recurrent venous thromboembolism in patients with hereditary deficiencies of protein S, protein C or antithrombin. Thromb Haemost. 2009;101:93-99.
- Christiansen SC, Cannegieter SC, Koster T, Vandenbroucke JP, Rosendaal FR. Thrombophilia, clinical factors, and recurrent venous thrombotic events. JAMA. 2005;293:2352-2361.
- De Stefano V, Simioni P, Rossi E, et al. The risk of recurrent venous thromboembolism in patients with inherited deficiency of natural anticoagulants antithrombin, protein C and protein S. Haematologica. 2006;91:695-698.
- Price DT, Ridker PM. Factor V Leiden mutation and the risks for thromboembolic disease: a clinical perspective. Ann Intern Med. 1997;127:895-903.
- Ho WK, Hankey GJ, Quinlan DJ, Eikelboom JW. Risk of recurrent venous thromboembolism in patients with common thrombophilia: a systematic review. Arch Intern Med. 2006;166:729-736.
- Simioni P, Prandoni P, Lensing AW, et al. Risk for subsequent venous thromboembolic complications in carriers of the prothrombin or the factor V gene mutation with a first episode of deep-vein thrombosis. Blood. 2000;96:3329-3333.
- Segal JB, Brotman DJ, Necochea AJ, et al. Predictive value of factor V Leiden and prothrombin G20210A in adults with venous thromboembolism and in family members of those with a mutation: a systematic review. JAMA. 2009;301:2472-2485.
- Eichinger S, Pabinger I, Stumpflen A, et al. The risk of recurrent venous thromboembolism in patients with and without factor V Leiden. Thromb Haemost. 1997;77:624-628.
- Lijfering WM, Middeldorp S, Veeger NJ, et al. Risk of recurrent venous thrombosis in homozygous carriers and double heterozygous carriers of factor V Leiden and prothrombin G20210A. Circulation. 2010;121(15):1706-1712.
- Khamashta MA, Cuadrado MJ, Mujic F, Taub NA, Hunt BJ, Hughes GR. The management of thrombosis in the antiphospholipid-antibody syndrome. N Engl J Med. 1995;332:993-997.
- Schulman S, Svenungsson E, Granqvist S. Anticardiolipin antibodies predict early recurrence of thromboembolism and death among patients with venous thromboembolism following anticoagulant therapy. Duration of Anticoagulation Study Group. Am J Med. 1998;104:332-338.
- Pengo V, Tripodi A, Reber G, et al. Update of the guidelines for lupus anticoagulant detection. Subcommittee on Lupus Anticoagulant/Antiphospholipid Antibody of the Scientific and Standardisation Committee of the International Society on Thrombosis and Haemostasis. J Thromb Haemost. 2009;7:1737-1740.
- Baglin T, Luddington R, Brown K, Baglin C. Incidence of recurrent venous thromboembolism in relation to clinical and thrombophilic risk factors: prospective cohort study. Lancet. 2003;362:523-526.
- Rosendaal FR. Once and only once. Circulation. 2010;121:1688-1690.
- Dalen JE. Should patients with venous thromboembolism be screened for thrombophilia? Am J Med. 2008;121:458-463.
The Case
A healthy 42-year-old woman presents to the hospital with acute-onset pleuritic chest pain and shortness of breath. She has not had any recent surgeries, takes no medications, and is very active. A lung ventilation-perfusion scan reveals a high probability of pulmonary embolism (PE). The patient’s history is notable for two second-trimester pregnancy losses. The patient is started on low-molecular heparin and warfarin (LMHW).
Should this patient be tested for thrombophilia?
Background
Thrombophilia can now be identified in more than half of all patients presenting with VTE, and testing for underlying causes of thrombophilia has become widespread.1 Physicians believe that thrombophilia testing frequently changes management of patients with VTE.2
Thrombophilias can be classified into three major categories: deficiency of natural inhibitors of coagulation, abnormal function or elevated level of coagulation factors, and acquired thrombophilias (see Table 1).
The prevalence of specific thrombophilias varies widely. For example, the prevalence of activated protein C resistance (the factor V Leiden mutation) is 3% to 7%. In comparison, the prevalence of antithrombin deficiency is estimated at 0.02%. Each thrombophilia is associated with an increased VTE risk, but the level of risk associated with a given thrombophilia varies greatly.1
Before testing for thrombophilia in acute VTE, assess the risk of recurrent VTE by determining if the thrombosis was provoked or unprovoked. A VTE event is considered provoked if it occurs in the setting of pregnancy within the previous three months; estrogen therapy; immobility from acute illness for more than one week; travel lasting for more than six hours; leg trauma, fracture, or surgery within the previous three months; or active malignancy (see Table 2,).3 Unprovoked VTE has a recurrence rate of 7.4% per patient year, compared with 3.3% per patient year for a provoked VTE; the risk is even lower (0.7% per patient year) if the risk factor for the provoked VTE was surgical.4
Testing for thrombophilia is indicated if the results would add significant prognostic information beyond the clinical history, or if it would change patient management—in particular, the intensity or the duration of anticoagulation.
Review of the Data
Does presence of thrombophilia alter the intensity of anticoagulation for VTE?
If thrombophilia increases the risk of VTE recurrence while on anticoagulation, then a more intense level of anticoagulation might prevent future VTE. There are no studies investigating higher intensity of anticoagulation, but if standard anticoagulation were insufficient for patients with identifiable thrombophilia, one might expect to observe increased recurrence rates among patients with thrombophilia treated with standard warfarin therapy.
In a substudy of the Extended Low-Intensity Anticoagulation for Unprovoked Venous ThromboEmbolism (ELATE) trial, the risk of recurrence of VTE among treated subjects was very low overall, and the presence of thrombophilic abnormalities was not associated with significantly higher risk.5 Observational studies have found VTE recurrence rates are low in patients treated with warfarin, with or without thrombophilia.6-8
The impact of the initial level of anticoagulation on recurrence after the completion of the treatment period has been evaluated. Although one study suggested that patients with substandard levels of anticoagulation were at an increased risk of subsequent VTE, this was not confirmed in the Leiden Thrombophilia Study (LETS). 9,10
In sum, the majority of data do not suggest a significantly increased risk of recurrent VTE in patients with thrombophilia treated with standard anticoagulation. Therefore, treatment with warfarin to a goal INR of 2 to 3 is sufficient.
Does presence of thrombophilia alter duration of VTE treatment?
A major decision clinicians face when caring for VTE patients is the duration of anticoagulation treatment. The current ACCP recommendation for treatment of a provoked VTE is three months, with treatment for an unprovoked VTE three months or lifelong.11 If the presence of thrombophilia increases the risk of recurrence after cessation of anticoagulation treatment, longer duration of treatment might be indicated. One of the goals of thrombophilia testing should be to identify those patients.
Overall, the recurrence rate after first VTE is high, with a cumulative incidence of 25% at five years, 30% at eight years, and 56% at 20 years.12,13
Deficiency of natural inhibitors of coagulation.
Deficiency of a natural inhibitor of coagulation has been associated with a risk of recurrence of VTE of as much as 10% per year, according to some studies.6,14 However, the estimates are based on studies that include individuals from thrombosis-prone families, and selection bias might have contributed to the high recurrence rates.1 In the unselected population represented in the LETS study, only a modest elevation was seen in the estimated risk of recurrence for patients with inhibitor deficiencies.15
Testing for deficiency of inhibitors offers little prognostic information beyond that obtained when determining whether a VTE event is provoked or unprovoked. In studies that have separately examined subjects with provoked vs. unprovoked VTE, deficiency of an inhibitor is not associated with increased risk of recurrence.15,16
Abnormal function or level of anticoagulation factors.
Factor V Leiden (FVL) is the most common cause of inherited thrombophilia and is associated with as much as a sixfold increase in VTE risk, while the prothrombin gene mutation is associated with a twofold increase.17,18
In contrast, the evidence associating these mutations with recurrent VTE risk is not as consistent. Although a study conducted at a referral center in Italy found an increased risk of recurrence with either Factor V Leiden or prothrombin gene mutation, a large meta-analysis of 23 studies found increased risk only with Factor V Leiden.19,20 Another meta-analysis demonstrated only a modest increased risk of recurrence in subjects with Factor V Leiden or prothrombin gene mutation, and a prospective study from Austria found no increased risk of recurrence with Factor V Leiden two years after discontinuation of anticoagulation.18,21 Additionally, when using patients with unprovoked VTE as reference, there was no increased risk of recurrence among patients homozygous for Factor V Leiden or the prothrombin gene mutation.22
In summary, although Factor V Leiden and prothrombin gene defects are associated with increased risk of recurrent VTE, the magnitude of the risk increase is modest and, therefore, should not alter duration of therapy.
Acquired thrombophilia.
It appears that the only thrombophilic state that might have a significant impact on the risk of recurrence is the antiphospholipid syndrome. The cessation of warfarin therapy in patients with thrombosis associated with antiphospholipid antibodies carries a 69% risk of recurrent thrombosis within a year.23 Some studies have suggested that the presence of specific antibodies (i.e. anticardiolipin antibodies) is associated with increased risk in patients with antiphospholipid syndrome.24
However, at present, all patients with VTE and antiphospholipid syndrome should be candidates for lifelong anticoagulation. Antiphospholipid antibody testing should be performed in patients with a suggestive history, including those with recurrent fetal loss or a single fetal loss after 10 weeks, or known collagen vascular disease.25
The role of provoked vs. unprovoked VTE.
Identifying whether a VTE is provoked or unprovoked has been shown to be an important predictor of recurrence. For example, one prospective, cohort study found two-year recurrence rates of zero in patients with a surgery or pregnancy-related VTE, 9% with other provoked VTE, and 19% with unprovoked VTE.26 In the same study, thrombophilia testing failed to reliably predict recurrence risk. Patients with unprovoked VTE who were tested and found to not have a defect were at equally high risk of recurrent VTE as those found to have a thrombophilia.27
The most significant predictor for VTE recurrence is whether the first event was provoked, and thrombophilia testing offers little additional prognostic information.28
VTE as a multifactorial disorder.
It is becoming increasingly clear that VTE is multifactorial disorder, caused by the interactions of genotypic, phenotypic, and environmental factors. In the case of an unprovoked VTE, the patient already carries a significantly elevated risk for recurrence, and further testing for known causes of thrombophilia appears to add very little additional information. The optimal duration of anticoagulation for unprovoked VTE is unclear, but current guidelines suggest at least three months—and clinicians should consider lifelong treatment.
In the vast majority of cases, testing for thrombophilia has no impact on the management of VTE and is not warranted. In patients with antiphospholipid-antibody syndrome, given the high risk of recurrence, long-term anticoagulation after a first VTE might be indicated. In select patients with a clinical picture suggestive of antiphospholipid-antibody syndrome, or a strong family history, testing should be considered.
Back to the Case
Our patient appears to have an unprovoked VTE. She should receive regular anticoagulation with warfarin, with a goal INR of 2 to 3, for at least three months. Lifelong anticoagulation therapy should be considered. Testing for heritable thrombophilia will not change the current management or treatment duration and, hence, is not indicated. However, the patient’s history is suggestive of antiphospholipid-antibody syndrome, so she should be tested. If the diagnosis of antiphospholipid syndrome is made, lifelong anticoagulation should be considered.
Bottom Line
Unprovoked VTE provides the strongest predictor for recurrence. Thrombophilia testing adds little in predicting recurrence and rarely is indicated.
Dr. Stehlikova is a clinical hospitalist in the division of hospital medicine, department of medicine, at Albert Einstein College of Medicine and Montefiore Medical Center in Bronx, N.Y. Dr. Martin is director of the Einstein Hospitalist Service. Dr. Janakiram is a fellow in the department of hematology at Einstein, and Dr. Korcak is an instructor at Einstein in the department of medicine and director of the Weiler Medical Service. Dr. Galhotra is associate director for inpatient quality in the department of medicine at Einstein; Dr. Averbukh is an academic hospitalist; and Dr. Southern is chief of the division of hospital medicine at Einstein.
References
- Middeldorp S, van Hylckama Vlieg A. Does thrombophilia testing help in the clinical management of patients? Br J Haematol. 2008;143:321-335.
- Coppens M, van Mourik JA, Eckmann CM, Büller HR, Middeldorp S. Current practise of testing for inherited thrombophilia. J Thromb Haemost. 2007;5:1979-1981.
- Prandoni P, Noventa F, Ghirarduzzi A, et al. The risk of recurrent venous thromboembolism after discontinuing anticoagulation in patients with acute proximal deep vein thrombosis or pulmonary embolism. A prospective cohort study in 1,626 patients. Haematologica. 2007;92:199-205.
- Iorio A, Kearon C, Filippucci E, et al. Risk of recurrence after a first episode of symptomatic venous thromboembolism provoked by a transient risk factor: a systematic review. Arch Intern Med. 2010;170:1710-1716.
- Kearon C, Julian JA, Kovacs MJ, et al. Influence of thrombophilia on risk of recurrent venous thromboembolism while on warfarin: results from a randomized trial. Blood. 2008;112:4432-4436.
- Vossen CY, Walker ID, Svensson P, et al. Recurrence rate after a first venous thrombosis in patients with familial thrombophilia. Arterioscler Thromb Vasc Biol. 2005;25:1992-1997.
- Brown K, Luddington R, Williamson D, Baker P, Baglin T. Risk of venous thromboembolism associated with a G to A transition at position 20210 in the 3'-untranslated region of the prothrombin gene. Br J Haematol. 1997;98:907-909.
- Schulman S, Tengborn L. Treatment of venous thromboembolism in patients with congenital deficiency of antithrombin III. Thromb Haemost. 1992;68:634-636.
- Palareti G, Legnani C, Cosmi B, Guazzaloca G, Cini M, Mattarozzi S. Poor anticoagulation quality in the first 3 months after unprovoked venous thromboembolism is a risk factor for long-term recurrence. J Thromb Haemost. 2005;3:955-961.
- Gadisseur AP, Christiansen SC, van der Meer FJ, Rosendaal FR. The quality of oral anticoagulant therapy and recurrent venous thrombotic events in the Leiden Thrombophilia Study. J Thromb Haemost. 2007;5:931-936.
- Kearon C, Kahn SR, Agnelli G, Goldhaber S, Raskob GE, Comerota AJ. Antithrombotic therapy for venous thromboembolic disease: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition). Chest. 2008;133:454S-545S.
- Prandoni P, Lensing AW, Cogo A, et al. The long-term clinical course of acute deep venous thrombosis. Ann Intern Med. 1996;125:1-7.
- Laczkovics C, Grafenhofer H, Kaider A, et al. Risk of recurrence after a first venous thromboembolic event in young women. Haematologica. 2007;92:1201-1207.
- Brouwer JL, Lijfering WM, Ten Kate MK, Kluin-Nelemans HC, Veeger NJ, van der Meer J. High long-term absolute risk of recurrent venous thromboembolism in patients with hereditary deficiencies of protein S, protein C or antithrombin. Thromb Haemost. 2009;101:93-99.
- Christiansen SC, Cannegieter SC, Koster T, Vandenbroucke JP, Rosendaal FR. Thrombophilia, clinical factors, and recurrent venous thrombotic events. JAMA. 2005;293:2352-2361.
- De Stefano V, Simioni P, Rossi E, et al. The risk of recurrent venous thromboembolism in patients with inherited deficiency of natural anticoagulants antithrombin, protein C and protein S. Haematologica. 2006;91:695-698.
- Price DT, Ridker PM. Factor V Leiden mutation and the risks for thromboembolic disease: a clinical perspective. Ann Intern Med. 1997;127:895-903.
- Ho WK, Hankey GJ, Quinlan DJ, Eikelboom JW. Risk of recurrent venous thromboembolism in patients with common thrombophilia: a systematic review. Arch Intern Med. 2006;166:729-736.
- Simioni P, Prandoni P, Lensing AW, et al. Risk for subsequent venous thromboembolic complications in carriers of the prothrombin or the factor V gene mutation with a first episode of deep-vein thrombosis. Blood. 2000;96:3329-3333.
- Segal JB, Brotman DJ, Necochea AJ, et al. Predictive value of factor V Leiden and prothrombin G20210A in adults with venous thromboembolism and in family members of those with a mutation: a systematic review. JAMA. 2009;301:2472-2485.
- Eichinger S, Pabinger I, Stumpflen A, et al. The risk of recurrent venous thromboembolism in patients with and without factor V Leiden. Thromb Haemost. 1997;77:624-628.
- Lijfering WM, Middeldorp S, Veeger NJ, et al. Risk of recurrent venous thrombosis in homozygous carriers and double heterozygous carriers of factor V Leiden and prothrombin G20210A. Circulation. 2010;121(15):1706-1712.
- Khamashta MA, Cuadrado MJ, Mujic F, Taub NA, Hunt BJ, Hughes GR. The management of thrombosis in the antiphospholipid-antibody syndrome. N Engl J Med. 1995;332:993-997.
- Schulman S, Svenungsson E, Granqvist S. Anticardiolipin antibodies predict early recurrence of thromboembolism and death among patients with venous thromboembolism following anticoagulant therapy. Duration of Anticoagulation Study Group. Am J Med. 1998;104:332-338.
- Pengo V, Tripodi A, Reber G, et al. Update of the guidelines for lupus anticoagulant detection. Subcommittee on Lupus Anticoagulant/Antiphospholipid Antibody of the Scientific and Standardisation Committee of the International Society on Thrombosis and Haemostasis. J Thromb Haemost. 2009;7:1737-1740.
- Baglin T, Luddington R, Brown K, Baglin C. Incidence of recurrent venous thromboembolism in relation to clinical and thrombophilic risk factors: prospective cohort study. Lancet. 2003;362:523-526.
- Rosendaal FR. Once and only once. Circulation. 2010;121:1688-1690.
- Dalen JE. Should patients with venous thromboembolism be screened for thrombophilia? Am J Med. 2008;121:458-463.
The Case
A healthy 42-year-old woman presents to the hospital with acute-onset pleuritic chest pain and shortness of breath. She has not had any recent surgeries, takes no medications, and is very active. A lung ventilation-perfusion scan reveals a high probability of pulmonary embolism (PE). The patient’s history is notable for two second-trimester pregnancy losses. The patient is started on low-molecular heparin and warfarin (LMHW).
Should this patient be tested for thrombophilia?
Background
Thrombophilia can now be identified in more than half of all patients presenting with VTE, and testing for underlying causes of thrombophilia has become widespread.1 Physicians believe that thrombophilia testing frequently changes management of patients with VTE.2
Thrombophilias can be classified into three major categories: deficiency of natural inhibitors of coagulation, abnormal function or elevated level of coagulation factors, and acquired thrombophilias (see Table 1).
The prevalence of specific thrombophilias varies widely. For example, the prevalence of activated protein C resistance (the factor V Leiden mutation) is 3% to 7%. In comparison, the prevalence of antithrombin deficiency is estimated at 0.02%. Each thrombophilia is associated with an increased VTE risk, but the level of risk associated with a given thrombophilia varies greatly.1
Before testing for thrombophilia in acute VTE, assess the risk of recurrent VTE by determining if the thrombosis was provoked or unprovoked. A VTE event is considered provoked if it occurs in the setting of pregnancy within the previous three months; estrogen therapy; immobility from acute illness for more than one week; travel lasting for more than six hours; leg trauma, fracture, or surgery within the previous three months; or active malignancy (see Table 2,).3 Unprovoked VTE has a recurrence rate of 7.4% per patient year, compared with 3.3% per patient year for a provoked VTE; the risk is even lower (0.7% per patient year) if the risk factor for the provoked VTE was surgical.4
Testing for thrombophilia is indicated if the results would add significant prognostic information beyond the clinical history, or if it would change patient management—in particular, the intensity or the duration of anticoagulation.
Review of the Data
Does presence of thrombophilia alter the intensity of anticoagulation for VTE?
If thrombophilia increases the risk of VTE recurrence while on anticoagulation, then a more intense level of anticoagulation might prevent future VTE. There are no studies investigating higher intensity of anticoagulation, but if standard anticoagulation were insufficient for patients with identifiable thrombophilia, one might expect to observe increased recurrence rates among patients with thrombophilia treated with standard warfarin therapy.
In a substudy of the Extended Low-Intensity Anticoagulation for Unprovoked Venous ThromboEmbolism (ELATE) trial, the risk of recurrence of VTE among treated subjects was very low overall, and the presence of thrombophilic abnormalities was not associated with significantly higher risk.5 Observational studies have found VTE recurrence rates are low in patients treated with warfarin, with or without thrombophilia.6-8
The impact of the initial level of anticoagulation on recurrence after the completion of the treatment period has been evaluated. Although one study suggested that patients with substandard levels of anticoagulation were at an increased risk of subsequent VTE, this was not confirmed in the Leiden Thrombophilia Study (LETS). 9,10
In sum, the majority of data do not suggest a significantly increased risk of recurrent VTE in patients with thrombophilia treated with standard anticoagulation. Therefore, treatment with warfarin to a goal INR of 2 to 3 is sufficient.
Does presence of thrombophilia alter duration of VTE treatment?
A major decision clinicians face when caring for VTE patients is the duration of anticoagulation treatment. The current ACCP recommendation for treatment of a provoked VTE is three months, with treatment for an unprovoked VTE three months or lifelong.11 If the presence of thrombophilia increases the risk of recurrence after cessation of anticoagulation treatment, longer duration of treatment might be indicated. One of the goals of thrombophilia testing should be to identify those patients.
Overall, the recurrence rate after first VTE is high, with a cumulative incidence of 25% at five years, 30% at eight years, and 56% at 20 years.12,13
Deficiency of natural inhibitors of coagulation.
Deficiency of a natural inhibitor of coagulation has been associated with a risk of recurrence of VTE of as much as 10% per year, according to some studies.6,14 However, the estimates are based on studies that include individuals from thrombosis-prone families, and selection bias might have contributed to the high recurrence rates.1 In the unselected population represented in the LETS study, only a modest elevation was seen in the estimated risk of recurrence for patients with inhibitor deficiencies.15
Testing for deficiency of inhibitors offers little prognostic information beyond that obtained when determining whether a VTE event is provoked or unprovoked. In studies that have separately examined subjects with provoked vs. unprovoked VTE, deficiency of an inhibitor is not associated with increased risk of recurrence.15,16
Abnormal function or level of anticoagulation factors.
Factor V Leiden (FVL) is the most common cause of inherited thrombophilia and is associated with as much as a sixfold increase in VTE risk, while the prothrombin gene mutation is associated with a twofold increase.17,18
In contrast, the evidence associating these mutations with recurrent VTE risk is not as consistent. Although a study conducted at a referral center in Italy found an increased risk of recurrence with either Factor V Leiden or prothrombin gene mutation, a large meta-analysis of 23 studies found increased risk only with Factor V Leiden.19,20 Another meta-analysis demonstrated only a modest increased risk of recurrence in subjects with Factor V Leiden or prothrombin gene mutation, and a prospective study from Austria found no increased risk of recurrence with Factor V Leiden two years after discontinuation of anticoagulation.18,21 Additionally, when using patients with unprovoked VTE as reference, there was no increased risk of recurrence among patients homozygous for Factor V Leiden or the prothrombin gene mutation.22
In summary, although Factor V Leiden and prothrombin gene defects are associated with increased risk of recurrent VTE, the magnitude of the risk increase is modest and, therefore, should not alter duration of therapy.
Acquired thrombophilia.
It appears that the only thrombophilic state that might have a significant impact on the risk of recurrence is the antiphospholipid syndrome. The cessation of warfarin therapy in patients with thrombosis associated with antiphospholipid antibodies carries a 69% risk of recurrent thrombosis within a year.23 Some studies have suggested that the presence of specific antibodies (i.e. anticardiolipin antibodies) is associated with increased risk in patients with antiphospholipid syndrome.24
However, at present, all patients with VTE and antiphospholipid syndrome should be candidates for lifelong anticoagulation. Antiphospholipid antibody testing should be performed in patients with a suggestive history, including those with recurrent fetal loss or a single fetal loss after 10 weeks, or known collagen vascular disease.25
The role of provoked vs. unprovoked VTE.
Identifying whether a VTE is provoked or unprovoked has been shown to be an important predictor of recurrence. For example, one prospective, cohort study found two-year recurrence rates of zero in patients with a surgery or pregnancy-related VTE, 9% with other provoked VTE, and 19% with unprovoked VTE.26 In the same study, thrombophilia testing failed to reliably predict recurrence risk. Patients with unprovoked VTE who were tested and found to not have a defect were at equally high risk of recurrent VTE as those found to have a thrombophilia.27
The most significant predictor for VTE recurrence is whether the first event was provoked, and thrombophilia testing offers little additional prognostic information.28
VTE as a multifactorial disorder.
It is becoming increasingly clear that VTE is multifactorial disorder, caused by the interactions of genotypic, phenotypic, and environmental factors. In the case of an unprovoked VTE, the patient already carries a significantly elevated risk for recurrence, and further testing for known causes of thrombophilia appears to add very little additional information. The optimal duration of anticoagulation for unprovoked VTE is unclear, but current guidelines suggest at least three months—and clinicians should consider lifelong treatment.
In the vast majority of cases, testing for thrombophilia has no impact on the management of VTE and is not warranted. In patients with antiphospholipid-antibody syndrome, given the high risk of recurrence, long-term anticoagulation after a first VTE might be indicated. In select patients with a clinical picture suggestive of antiphospholipid-antibody syndrome, or a strong family history, testing should be considered.
Back to the Case
Our patient appears to have an unprovoked VTE. She should receive regular anticoagulation with warfarin, with a goal INR of 2 to 3, for at least three months. Lifelong anticoagulation therapy should be considered. Testing for heritable thrombophilia will not change the current management or treatment duration and, hence, is not indicated. However, the patient’s history is suggestive of antiphospholipid-antibody syndrome, so she should be tested. If the diagnosis of antiphospholipid syndrome is made, lifelong anticoagulation should be considered.
Bottom Line
Unprovoked VTE provides the strongest predictor for recurrence. Thrombophilia testing adds little in predicting recurrence and rarely is indicated.
Dr. Stehlikova is a clinical hospitalist in the division of hospital medicine, department of medicine, at Albert Einstein College of Medicine and Montefiore Medical Center in Bronx, N.Y. Dr. Martin is director of the Einstein Hospitalist Service. Dr. Janakiram is a fellow in the department of hematology at Einstein, and Dr. Korcak is an instructor at Einstein in the department of medicine and director of the Weiler Medical Service. Dr. Galhotra is associate director for inpatient quality in the department of medicine at Einstein; Dr. Averbukh is an academic hospitalist; and Dr. Southern is chief of the division of hospital medicine at Einstein.
References
- Middeldorp S, van Hylckama Vlieg A. Does thrombophilia testing help in the clinical management of patients? Br J Haematol. 2008;143:321-335.
- Coppens M, van Mourik JA, Eckmann CM, Büller HR, Middeldorp S. Current practise of testing for inherited thrombophilia. J Thromb Haemost. 2007;5:1979-1981.
- Prandoni P, Noventa F, Ghirarduzzi A, et al. The risk of recurrent venous thromboembolism after discontinuing anticoagulation in patients with acute proximal deep vein thrombosis or pulmonary embolism. A prospective cohort study in 1,626 patients. Haematologica. 2007;92:199-205.
- Iorio A, Kearon C, Filippucci E, et al. Risk of recurrence after a first episode of symptomatic venous thromboembolism provoked by a transient risk factor: a systematic review. Arch Intern Med. 2010;170:1710-1716.
- Kearon C, Julian JA, Kovacs MJ, et al. Influence of thrombophilia on risk of recurrent venous thromboembolism while on warfarin: results from a randomized trial. Blood. 2008;112:4432-4436.
- Vossen CY, Walker ID, Svensson P, et al. Recurrence rate after a first venous thrombosis in patients with familial thrombophilia. Arterioscler Thromb Vasc Biol. 2005;25:1992-1997.
- Brown K, Luddington R, Williamson D, Baker P, Baglin T. Risk of venous thromboembolism associated with a G to A transition at position 20210 in the 3'-untranslated region of the prothrombin gene. Br J Haematol. 1997;98:907-909.
- Schulman S, Tengborn L. Treatment of venous thromboembolism in patients with congenital deficiency of antithrombin III. Thromb Haemost. 1992;68:634-636.
- Palareti G, Legnani C, Cosmi B, Guazzaloca G, Cini M, Mattarozzi S. Poor anticoagulation quality in the first 3 months after unprovoked venous thromboembolism is a risk factor for long-term recurrence. J Thromb Haemost. 2005;3:955-961.
- Gadisseur AP, Christiansen SC, van der Meer FJ, Rosendaal FR. The quality of oral anticoagulant therapy and recurrent venous thrombotic events in the Leiden Thrombophilia Study. J Thromb Haemost. 2007;5:931-936.
- Kearon C, Kahn SR, Agnelli G, Goldhaber S, Raskob GE, Comerota AJ. Antithrombotic therapy for venous thromboembolic disease: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition). Chest. 2008;133:454S-545S.
- Prandoni P, Lensing AW, Cogo A, et al. The long-term clinical course of acute deep venous thrombosis. Ann Intern Med. 1996;125:1-7.
- Laczkovics C, Grafenhofer H, Kaider A, et al. Risk of recurrence after a first venous thromboembolic event in young women. Haematologica. 2007;92:1201-1207.
- Brouwer JL, Lijfering WM, Ten Kate MK, Kluin-Nelemans HC, Veeger NJ, van der Meer J. High long-term absolute risk of recurrent venous thromboembolism in patients with hereditary deficiencies of protein S, protein C or antithrombin. Thromb Haemost. 2009;101:93-99.
- Christiansen SC, Cannegieter SC, Koster T, Vandenbroucke JP, Rosendaal FR. Thrombophilia, clinical factors, and recurrent venous thrombotic events. JAMA. 2005;293:2352-2361.
- De Stefano V, Simioni P, Rossi E, et al. The risk of recurrent venous thromboembolism in patients with inherited deficiency of natural anticoagulants antithrombin, protein C and protein S. Haematologica. 2006;91:695-698.
- Price DT, Ridker PM. Factor V Leiden mutation and the risks for thromboembolic disease: a clinical perspective. Ann Intern Med. 1997;127:895-903.
- Ho WK, Hankey GJ, Quinlan DJ, Eikelboom JW. Risk of recurrent venous thromboembolism in patients with common thrombophilia: a systematic review. Arch Intern Med. 2006;166:729-736.
- Simioni P, Prandoni P, Lensing AW, et al. Risk for subsequent venous thromboembolic complications in carriers of the prothrombin or the factor V gene mutation with a first episode of deep-vein thrombosis. Blood. 2000;96:3329-3333.
- Segal JB, Brotman DJ, Necochea AJ, et al. Predictive value of factor V Leiden and prothrombin G20210A in adults with venous thromboembolism and in family members of those with a mutation: a systematic review. JAMA. 2009;301:2472-2485.
- Eichinger S, Pabinger I, Stumpflen A, et al. The risk of recurrent venous thromboembolism in patients with and without factor V Leiden. Thromb Haemost. 1997;77:624-628.
- Lijfering WM, Middeldorp S, Veeger NJ, et al. Risk of recurrent venous thrombosis in homozygous carriers and double heterozygous carriers of factor V Leiden and prothrombin G20210A. Circulation. 2010;121(15):1706-1712.
- Khamashta MA, Cuadrado MJ, Mujic F, Taub NA, Hunt BJ, Hughes GR. The management of thrombosis in the antiphospholipid-antibody syndrome. N Engl J Med. 1995;332:993-997.
- Schulman S, Svenungsson E, Granqvist S. Anticardiolipin antibodies predict early recurrence of thromboembolism and death among patients with venous thromboembolism following anticoagulant therapy. Duration of Anticoagulation Study Group. Am J Med. 1998;104:332-338.
- Pengo V, Tripodi A, Reber G, et al. Update of the guidelines for lupus anticoagulant detection. Subcommittee on Lupus Anticoagulant/Antiphospholipid Antibody of the Scientific and Standardisation Committee of the International Society on Thrombosis and Haemostasis. J Thromb Haemost. 2009;7:1737-1740.
- Baglin T, Luddington R, Brown K, Baglin C. Incidence of recurrent venous thromboembolism in relation to clinical and thrombophilic risk factors: prospective cohort study. Lancet. 2003;362:523-526.
- Rosendaal FR. Once and only once. Circulation. 2010;121:1688-1690.
- Dalen JE. Should patients with venous thromboembolism be screened for thrombophilia? Am J Med. 2008;121:458-463.
ICU Hospitalist Model Improves Quality of Care for Critically Ill Patients
Despite calls for board-certified intensivists to manage all critically ill patients, only a third of hospitalized ICU patients currently are seen by such a specialist—mostly because there are not enough of them to go around.1,2 More and more hospitalists, especially those in community hospitals, are working in ICUs (see “The Critical-Care Debate,”). With the proper training, that can be a good thing for patients and hospitalists, according to a Research, Innovations, and Clinical Vignettes (RIV) abstract presented at HM12 in San Diego.3
Lead author and hospitalist Mark Krivopal, MD, SFHM, formerly with TeamHealth in California and now vice president and medical director of clinical integration and hospital medicine at Steward Health Care in Boston, outlined a program at California’s Lodi Memorial Hospital that identified a group of hospitalists who had experience in caring for critically ill patients and credentials to perform such procedures as central-line placements, intubations, and ventilator management. The select group of TeamHealth hospitalists completed a two-day “Fundamentals of Critical Care Support” course offered by the Society of Critical Care Medicine (www.sccm.org), then began covering the ICU in shifts from 7 a.m. to 7 p.m. The program was so successful early on that hospital administration requested that it expand to a 24-hour service.
An ICU hospitalist program needs to be a partnership, Dr. Krivopal says. Essential oversight at Lodi Memorial is provided by the hospital’s sole pulmonologist.
Preliminary data showed a 35% reduction in ventilator days and 22% reduction in ICU stays, Dr. Krivopal says. The hospital also reports high satisfaction from nurses and other staff. Additional metrics, such as cost savings and patient satisfaction, are under review.
“So long as the level of training is sufficient, this is an approach that definitely should be explored,” he says, adding that young internists have many of the skills needed for ICU work. “But if you don’t keep those skills up [with practice] after residency, you lose them.”
References
- The Leapfrog Group. ICU physician staffing fact sheet. The Leapfrog Group website. Available at: http://www.leapfroggroup.org/media/file/Leapfrog-ICU_Physician_Staffing_Fact_Sheet.pdf. Accessed Aug. 29, 2012.
- Health Resources & Services Administration. Report to Congress: The critical care workforce: a study of the supply and demand for critical care physicians. U.S. Department of Health & Human Services website. Available at: http://bhpr.hrsa.gov/healthworkforce/reports/studycriticalcarephys.pdf. Accessed Aug. 29, 2012.
- Krivopal M, Hlaing M, Felber R, Himebaugh R. ICU hospitalist: a novel method of care for the critically ill patients in economically lean times. J Hosp Med. 2012;7(Suppl 2):192.
Despite calls for board-certified intensivists to manage all critically ill patients, only a third of hospitalized ICU patients currently are seen by such a specialist—mostly because there are not enough of them to go around.1,2 More and more hospitalists, especially those in community hospitals, are working in ICUs (see “The Critical-Care Debate,”). With the proper training, that can be a good thing for patients and hospitalists, according to a Research, Innovations, and Clinical Vignettes (RIV) abstract presented at HM12 in San Diego.3
Lead author and hospitalist Mark Krivopal, MD, SFHM, formerly with TeamHealth in California and now vice president and medical director of clinical integration and hospital medicine at Steward Health Care in Boston, outlined a program at California’s Lodi Memorial Hospital that identified a group of hospitalists who had experience in caring for critically ill patients and credentials to perform such procedures as central-line placements, intubations, and ventilator management. The select group of TeamHealth hospitalists completed a two-day “Fundamentals of Critical Care Support” course offered by the Society of Critical Care Medicine (www.sccm.org), then began covering the ICU in shifts from 7 a.m. to 7 p.m. The program was so successful early on that hospital administration requested that it expand to a 24-hour service.
An ICU hospitalist program needs to be a partnership, Dr. Krivopal says. Essential oversight at Lodi Memorial is provided by the hospital’s sole pulmonologist.
Preliminary data showed a 35% reduction in ventilator days and 22% reduction in ICU stays, Dr. Krivopal says. The hospital also reports high satisfaction from nurses and other staff. Additional metrics, such as cost savings and patient satisfaction, are under review.
“So long as the level of training is sufficient, this is an approach that definitely should be explored,” he says, adding that young internists have many of the skills needed for ICU work. “But if you don’t keep those skills up [with practice] after residency, you lose them.”
References
- The Leapfrog Group. ICU physician staffing fact sheet. The Leapfrog Group website. Available at: http://www.leapfroggroup.org/media/file/Leapfrog-ICU_Physician_Staffing_Fact_Sheet.pdf. Accessed Aug. 29, 2012.
- Health Resources & Services Administration. Report to Congress: The critical care workforce: a study of the supply and demand for critical care physicians. U.S. Department of Health & Human Services website. Available at: http://bhpr.hrsa.gov/healthworkforce/reports/studycriticalcarephys.pdf. Accessed Aug. 29, 2012.
- Krivopal M, Hlaing M, Felber R, Himebaugh R. ICU hospitalist: a novel method of care for the critically ill patients in economically lean times. J Hosp Med. 2012;7(Suppl 2):192.
Despite calls for board-certified intensivists to manage all critically ill patients, only a third of hospitalized ICU patients currently are seen by such a specialist—mostly because there are not enough of them to go around.1,2 More and more hospitalists, especially those in community hospitals, are working in ICUs (see “The Critical-Care Debate,”). With the proper training, that can be a good thing for patients and hospitalists, according to a Research, Innovations, and Clinical Vignettes (RIV) abstract presented at HM12 in San Diego.3
Lead author and hospitalist Mark Krivopal, MD, SFHM, formerly with TeamHealth in California and now vice president and medical director of clinical integration and hospital medicine at Steward Health Care in Boston, outlined a program at California’s Lodi Memorial Hospital that identified a group of hospitalists who had experience in caring for critically ill patients and credentials to perform such procedures as central-line placements, intubations, and ventilator management. The select group of TeamHealth hospitalists completed a two-day “Fundamentals of Critical Care Support” course offered by the Society of Critical Care Medicine (www.sccm.org), then began covering the ICU in shifts from 7 a.m. to 7 p.m. The program was so successful early on that hospital administration requested that it expand to a 24-hour service.
An ICU hospitalist program needs to be a partnership, Dr. Krivopal says. Essential oversight at Lodi Memorial is provided by the hospital’s sole pulmonologist.
Preliminary data showed a 35% reduction in ventilator days and 22% reduction in ICU stays, Dr. Krivopal says. The hospital also reports high satisfaction from nurses and other staff. Additional metrics, such as cost savings and patient satisfaction, are under review.
“So long as the level of training is sufficient, this is an approach that definitely should be explored,” he says, adding that young internists have many of the skills needed for ICU work. “But if you don’t keep those skills up [with practice] after residency, you lose them.”
References
- The Leapfrog Group. ICU physician staffing fact sheet. The Leapfrog Group website. Available at: http://www.leapfroggroup.org/media/file/Leapfrog-ICU_Physician_Staffing_Fact_Sheet.pdf. Accessed Aug. 29, 2012.
- Health Resources & Services Administration. Report to Congress: The critical care workforce: a study of the supply and demand for critical care physicians. U.S. Department of Health & Human Services website. Available at: http://bhpr.hrsa.gov/healthworkforce/reports/studycriticalcarephys.pdf. Accessed Aug. 29, 2012.
- Krivopal M, Hlaing M, Felber R, Himebaugh R. ICU hospitalist: a novel method of care for the critically ill patients in economically lean times. J Hosp Med. 2012;7(Suppl 2):192.
Sharp Rise in Imaging Test Rates has Slowed
A new study tracking the growth of advanced diagnostic imaging techniques found that the rate of growth for such tests is slowing dramatically, even as the total number of tests performed continues to grow.1 Starting in 2007, the rate of growth dropped sharply to about 1% to 3% from more than 6% per year during the previous decade.
Frank Levy, PhD, professor of urban economics at Massachusetts Institute of Technology in Cambridge, Mass., and one of the study’s authors, suggests that the previous growth of the technology could have been partly attributable to such nonmedical factors as profitability for hospitals and fear of malpractice by physicians. The slowdown, Dr. Levy says, also might reflect increased pushback from insurers, recognition of the cost and waste issues, and growing concerns about radiation exposure.
“There are many medical reasons for using these procedures—and many nonmedical reasons,” Dr. Levy says. “To use healthcare resources more efficiently, you should make sure your reason for ordering these tests is medical.”
SHM is working on a short list of sometimes unnecessary but commonly performed medical procedures, which it plans to submit to the American Board of Internal Medicine’s Choosing Wisely campaign this fall. One of the tests being considered for this list is serial chest X-rays for hospitalized patients outside of the ICU who are clinically stable, says Wendy Nickel, associate vice president of SHM’s Center for Hospital Innovation and Improvement. Unnecessary imaging tests are both a safety and a waste issue, she adds.
In related news, a study in the Journal of the National Cancer Institute found that 95.9% of patients 65 and older who have Stage IV cancer received at least one high-cost advanced imaging procedure (e.g. PET or nuclear medicine), with their utilization rates rising more rapidly than for earlier stages of disease.2 Such tests can lead to appropriate palliative measures but also can “distract patients from focusing on achievable end-of-life goals,” explain researchers from the Dana-Farber Cancer Institute in Boston.
References
- Lee D, Levy F. The sharp slowdown in growth of medical imaging: an early analysis suggests combination of policies was the cause. Health Affairs website. Available at: http://www.healthaffairs.org/alert_link.php?url=http://content.healthaffairs.org/content/early/2012/07/24/hlthaff.2011.1034&t=h&id=1590. Accessed Aug. 29, 2012.
- Hu YY, Kwok AC, Jiang W, et al. High-cost imaging in elderly patients with Stage IV cancer. J Natl Cancer Inst. 2012;104(15):1165-1173.
A new study tracking the growth of advanced diagnostic imaging techniques found that the rate of growth for such tests is slowing dramatically, even as the total number of tests performed continues to grow.1 Starting in 2007, the rate of growth dropped sharply to about 1% to 3% from more than 6% per year during the previous decade.
Frank Levy, PhD, professor of urban economics at Massachusetts Institute of Technology in Cambridge, Mass., and one of the study’s authors, suggests that the previous growth of the technology could have been partly attributable to such nonmedical factors as profitability for hospitals and fear of malpractice by physicians. The slowdown, Dr. Levy says, also might reflect increased pushback from insurers, recognition of the cost and waste issues, and growing concerns about radiation exposure.
“There are many medical reasons for using these procedures—and many nonmedical reasons,” Dr. Levy says. “To use healthcare resources more efficiently, you should make sure your reason for ordering these tests is medical.”
SHM is working on a short list of sometimes unnecessary but commonly performed medical procedures, which it plans to submit to the American Board of Internal Medicine’s Choosing Wisely campaign this fall. One of the tests being considered for this list is serial chest X-rays for hospitalized patients outside of the ICU who are clinically stable, says Wendy Nickel, associate vice president of SHM’s Center for Hospital Innovation and Improvement. Unnecessary imaging tests are both a safety and a waste issue, she adds.
In related news, a study in the Journal of the National Cancer Institute found that 95.9% of patients 65 and older who have Stage IV cancer received at least one high-cost advanced imaging procedure (e.g. PET or nuclear medicine), with their utilization rates rising more rapidly than for earlier stages of disease.2 Such tests can lead to appropriate palliative measures but also can “distract patients from focusing on achievable end-of-life goals,” explain researchers from the Dana-Farber Cancer Institute in Boston.
References
- Lee D, Levy F. The sharp slowdown in growth of medical imaging: an early analysis suggests combination of policies was the cause. Health Affairs website. Available at: http://www.healthaffairs.org/alert_link.php?url=http://content.healthaffairs.org/content/early/2012/07/24/hlthaff.2011.1034&t=h&id=1590. Accessed Aug. 29, 2012.
- Hu YY, Kwok AC, Jiang W, et al. High-cost imaging in elderly patients with Stage IV cancer. J Natl Cancer Inst. 2012;104(15):1165-1173.
A new study tracking the growth of advanced diagnostic imaging techniques found that the rate of growth for such tests is slowing dramatically, even as the total number of tests performed continues to grow.1 Starting in 2007, the rate of growth dropped sharply to about 1% to 3% from more than 6% per year during the previous decade.
Frank Levy, PhD, professor of urban economics at Massachusetts Institute of Technology in Cambridge, Mass., and one of the study’s authors, suggests that the previous growth of the technology could have been partly attributable to such nonmedical factors as profitability for hospitals and fear of malpractice by physicians. The slowdown, Dr. Levy says, also might reflect increased pushback from insurers, recognition of the cost and waste issues, and growing concerns about radiation exposure.
“There are many medical reasons for using these procedures—and many nonmedical reasons,” Dr. Levy says. “To use healthcare resources more efficiently, you should make sure your reason for ordering these tests is medical.”
SHM is working on a short list of sometimes unnecessary but commonly performed medical procedures, which it plans to submit to the American Board of Internal Medicine’s Choosing Wisely campaign this fall. One of the tests being considered for this list is serial chest X-rays for hospitalized patients outside of the ICU who are clinically stable, says Wendy Nickel, associate vice president of SHM’s Center for Hospital Innovation and Improvement. Unnecessary imaging tests are both a safety and a waste issue, she adds.
In related news, a study in the Journal of the National Cancer Institute found that 95.9% of patients 65 and older who have Stage IV cancer received at least one high-cost advanced imaging procedure (e.g. PET or nuclear medicine), with their utilization rates rising more rapidly than for earlier stages of disease.2 Such tests can lead to appropriate palliative measures but also can “distract patients from focusing on achievable end-of-life goals,” explain researchers from the Dana-Farber Cancer Institute in Boston.
References
- Lee D, Levy F. The sharp slowdown in growth of medical imaging: an early analysis suggests combination of policies was the cause. Health Affairs website. Available at: http://www.healthaffairs.org/alert_link.php?url=http://content.healthaffairs.org/content/early/2012/07/24/hlthaff.2011.1034&t=h&id=1590. Accessed Aug. 29, 2012.
- Hu YY, Kwok AC, Jiang W, et al. High-cost imaging in elderly patients with Stage IV cancer. J Natl Cancer Inst. 2012;104(15):1165-1173.
Noisy Hospitals Impede Sleep
Sleep-disturbing noise in the hospital is a big problem “that can really compromise a patient’s recovery process,” according to Orfeu Buxton, PhD, associate neuroscientist in the Division of Sleep Medicine at Brigham & Women’s Hospital in Boston.1
Researchers exposed a dozen healthy volunteers to typical nocturnal hospital noise while monitoring their sleep patterns and heart rates, systematically quantifying the disruptive capacity of a range of hospital sounds on sleep. Hospitalized patients routinely cite noise as a major factor that negatively affects quality of care, the researchers note. An Aug. 2 New York Times blog post by Pauline Chen, MD, suggests that government policies linking hospital reimbursement to patient satisfaction might finally turn hospital administrators’ focus on the need to bring this noise under better control.2
References
- Buxton OM, Ellenbogen JM, Wang W, et al. Sleep disruption due to hospital noises: a prospective evaluation. Ann Intern Med. 2012;157(3):170-179.
- Chen P. The clatter of the hospital room. New York Times website. Available at: http://well.blogs.nytimes.com/2012/08/02/the-clatter-of-the-hospital-room/. Accessed Aug. 29, 2012.
Sleep-disturbing noise in the hospital is a big problem “that can really compromise a patient’s recovery process,” according to Orfeu Buxton, PhD, associate neuroscientist in the Division of Sleep Medicine at Brigham & Women’s Hospital in Boston.1
Researchers exposed a dozen healthy volunteers to typical nocturnal hospital noise while monitoring their sleep patterns and heart rates, systematically quantifying the disruptive capacity of a range of hospital sounds on sleep. Hospitalized patients routinely cite noise as a major factor that negatively affects quality of care, the researchers note. An Aug. 2 New York Times blog post by Pauline Chen, MD, suggests that government policies linking hospital reimbursement to patient satisfaction might finally turn hospital administrators’ focus on the need to bring this noise under better control.2
References
- Buxton OM, Ellenbogen JM, Wang W, et al. Sleep disruption due to hospital noises: a prospective evaluation. Ann Intern Med. 2012;157(3):170-179.
- Chen P. The clatter of the hospital room. New York Times website. Available at: http://well.blogs.nytimes.com/2012/08/02/the-clatter-of-the-hospital-room/. Accessed Aug. 29, 2012.
Sleep-disturbing noise in the hospital is a big problem “that can really compromise a patient’s recovery process,” according to Orfeu Buxton, PhD, associate neuroscientist in the Division of Sleep Medicine at Brigham & Women’s Hospital in Boston.1
Researchers exposed a dozen healthy volunteers to typical nocturnal hospital noise while monitoring their sleep patterns and heart rates, systematically quantifying the disruptive capacity of a range of hospital sounds on sleep. Hospitalized patients routinely cite noise as a major factor that negatively affects quality of care, the researchers note. An Aug. 2 New York Times blog post by Pauline Chen, MD, suggests that government policies linking hospital reimbursement to patient satisfaction might finally turn hospital administrators’ focus on the need to bring this noise under better control.2
References
- Buxton OM, Ellenbogen JM, Wang W, et al. Sleep disruption due to hospital noises: a prospective evaluation. Ann Intern Med. 2012;157(3):170-179.
- Chen P. The clatter of the hospital room. New York Times website. Available at: http://well.blogs.nytimes.com/2012/08/02/the-clatter-of-the-hospital-room/. Accessed Aug. 29, 2012.
Alternative Healthcare Models Aim to Boost Sagging Critical-Care Workforce
Amid the struggle to boost the country’s sagging critical-care workforce, experts have most commonly proposed creating a tiered or regionalized model of care, investing more in tele-ICU services, and augmenting the role of midlevel providers.
The University of Pittsburgh Medical Center, with 20 hospitals and roughly 500 ICU beds throughout its network, is adopting a regionalized healthcare delivery system. Some of the center’s most high-risk services, such as its big transplant programs, are centralized within the main university campus hospitals, as are about half of the ICU beds.
“In those hospitals, we’ve decided that we need 24/7 in-house, intensive-care attendings,” says Derek Angus, MD, the center’s chair of critical-care medicine. The doctors work with fellows and a rapidly growing expansion of midlevel providers.
In some of the smaller hospitals, however, some ICU patients are seen and managed by hospitalists. The medical center’s eventual goal is to be more systematic about the kinds of patients managed by intensivists as well as those managed by hospitalists. It’s a task made easier by the specialists’ close working relationship within the same department.
Dr. Angus believes telemedicine could help by providing a sort of mission control that can help track critically ill patients and those at risk of being admitted to ICUs across all 20 hospitals. He concedes, however, that telemedicine for ICU assistance has had mixed results in the medical literature, suggesting that a major key is working out the proper roles and responsibilities of those using the technology.
To improve the consistency of its own frontline providers, the Emory University Center for Critical Care in Atlanta developed a competency-based, critical-care training program for nurse practitioners (NPs) and physician assistants (PAs).
“It’s very clear that if you have a group of NP and PA providers who can do 90 percent of what the physician does, it really begins to unload the physician to focus on what I call the big-picture pieces of critical care,” says center director Timothy Buchman, PhD, MD.
That attending physician can be trained as a care executive to ensure well-coordinated care and to focus on any process that isn’t working well. “At a big academic health sciences center, that should probably be a critical-care physician,” Dr. Buchman notes. “But for the smaller community and regional hospitals that have a relatively less sick population, the person who will be well-positioned to oversee this nonphysician provider staff could well be a hospitalist who’s received additional guidance and training in critical care.”
For mild or moderate complexity of care, he says, the added training need not necessarily include a traditional two-year fellowship. Under a value-based system, sicker patients could be rapidly transferred to a higher level of care, and telemedicine could provide a “backstop” for providers in smaller hospitals who lack the training and experience of someone with a full critical-care fellowship.
Amid the struggle to boost the country’s sagging critical-care workforce, experts have most commonly proposed creating a tiered or regionalized model of care, investing more in tele-ICU services, and augmenting the role of midlevel providers.
The University of Pittsburgh Medical Center, with 20 hospitals and roughly 500 ICU beds throughout its network, is adopting a regionalized healthcare delivery system. Some of the center’s most high-risk services, such as its big transplant programs, are centralized within the main university campus hospitals, as are about half of the ICU beds.
“In those hospitals, we’ve decided that we need 24/7 in-house, intensive-care attendings,” says Derek Angus, MD, the center’s chair of critical-care medicine. The doctors work with fellows and a rapidly growing expansion of midlevel providers.
In some of the smaller hospitals, however, some ICU patients are seen and managed by hospitalists. The medical center’s eventual goal is to be more systematic about the kinds of patients managed by intensivists as well as those managed by hospitalists. It’s a task made easier by the specialists’ close working relationship within the same department.
Dr. Angus believes telemedicine could help by providing a sort of mission control that can help track critically ill patients and those at risk of being admitted to ICUs across all 20 hospitals. He concedes, however, that telemedicine for ICU assistance has had mixed results in the medical literature, suggesting that a major key is working out the proper roles and responsibilities of those using the technology.
To improve the consistency of its own frontline providers, the Emory University Center for Critical Care in Atlanta developed a competency-based, critical-care training program for nurse practitioners (NPs) and physician assistants (PAs).
“It’s very clear that if you have a group of NP and PA providers who can do 90 percent of what the physician does, it really begins to unload the physician to focus on what I call the big-picture pieces of critical care,” says center director Timothy Buchman, PhD, MD.
That attending physician can be trained as a care executive to ensure well-coordinated care and to focus on any process that isn’t working well. “At a big academic health sciences center, that should probably be a critical-care physician,” Dr. Buchman notes. “But for the smaller community and regional hospitals that have a relatively less sick population, the person who will be well-positioned to oversee this nonphysician provider staff could well be a hospitalist who’s received additional guidance and training in critical care.”
For mild or moderate complexity of care, he says, the added training need not necessarily include a traditional two-year fellowship. Under a value-based system, sicker patients could be rapidly transferred to a higher level of care, and telemedicine could provide a “backstop” for providers in smaller hospitals who lack the training and experience of someone with a full critical-care fellowship.
Amid the struggle to boost the country’s sagging critical-care workforce, experts have most commonly proposed creating a tiered or regionalized model of care, investing more in tele-ICU services, and augmenting the role of midlevel providers.
The University of Pittsburgh Medical Center, with 20 hospitals and roughly 500 ICU beds throughout its network, is adopting a regionalized healthcare delivery system. Some of the center’s most high-risk services, such as its big transplant programs, are centralized within the main university campus hospitals, as are about half of the ICU beds.
“In those hospitals, we’ve decided that we need 24/7 in-house, intensive-care attendings,” says Derek Angus, MD, the center’s chair of critical-care medicine. The doctors work with fellows and a rapidly growing expansion of midlevel providers.
In some of the smaller hospitals, however, some ICU patients are seen and managed by hospitalists. The medical center’s eventual goal is to be more systematic about the kinds of patients managed by intensivists as well as those managed by hospitalists. It’s a task made easier by the specialists’ close working relationship within the same department.
Dr. Angus believes telemedicine could help by providing a sort of mission control that can help track critically ill patients and those at risk of being admitted to ICUs across all 20 hospitals. He concedes, however, that telemedicine for ICU assistance has had mixed results in the medical literature, suggesting that a major key is working out the proper roles and responsibilities of those using the technology.
To improve the consistency of its own frontline providers, the Emory University Center for Critical Care in Atlanta developed a competency-based, critical-care training program for nurse practitioners (NPs) and physician assistants (PAs).
“It’s very clear that if you have a group of NP and PA providers who can do 90 percent of what the physician does, it really begins to unload the physician to focus on what I call the big-picture pieces of critical care,” says center director Timothy Buchman, PhD, MD.
That attending physician can be trained as a care executive to ensure well-coordinated care and to focus on any process that isn’t working well. “At a big academic health sciences center, that should probably be a critical-care physician,” Dr. Buchman notes. “But for the smaller community and regional hospitals that have a relatively less sick population, the person who will be well-positioned to oversee this nonphysician provider staff could well be a hospitalist who’s received additional guidance and training in critical care.”
For mild or moderate complexity of care, he says, the added training need not necessarily include a traditional two-year fellowship. Under a value-based system, sicker patients could be rapidly transferred to a higher level of care, and telemedicine could provide a “backstop” for providers in smaller hospitals who lack the training and experience of someone with a full critical-care fellowship.
Guidelines Drive Optimal Care for Heart Failure Patients
Cardiologists aren’t shy about repeating it: guidelines, guidelines, guidelines. That is, follow them.
“Evidence-based, guideline-driven optimal care for heart failure truly is beneficial,” Dr. Yancy says. “Every effort should be made to strive to achieve ideal thresholds and meeting best practices.”
There is now compelling evidence that, for patients with heart failure, the higher the degree of adherence to Class I-recommended therapies, the greater the reduction in 24-month mortality risk.5
“It would seem as if practicing best quality is almost a perfunctory statement, but consistently, when we look at surveys of quality improvement and adherence to evidence-based strategies, persistent gaps remain in the broader community,” Dr. Yancy says. “We know what we need to do. We’re still striving to get closer and closer to optimal care.”
Dr. Harold says the guidelines are there to make things simpler. So take advantage of them.
“If anything, hospitalists tend to be ahead of most other groups in terms of knowing evidence-based pathways and really tracking very specific protocols,” he says. “I think one of the advantages of hospitalist care is very often, it is guideline-driven. You have less variation in terms of care and quality outcomes.”
Cardiologists aren’t shy about repeating it: guidelines, guidelines, guidelines. That is, follow them.
“Evidence-based, guideline-driven optimal care for heart failure truly is beneficial,” Dr. Yancy says. “Every effort should be made to strive to achieve ideal thresholds and meeting best practices.”
There is now compelling evidence that, for patients with heart failure, the higher the degree of adherence to Class I-recommended therapies, the greater the reduction in 24-month mortality risk.5
“It would seem as if practicing best quality is almost a perfunctory statement, but consistently, when we look at surveys of quality improvement and adherence to evidence-based strategies, persistent gaps remain in the broader community,” Dr. Yancy says. “We know what we need to do. We’re still striving to get closer and closer to optimal care.”
Dr. Harold says the guidelines are there to make things simpler. So take advantage of them.
“If anything, hospitalists tend to be ahead of most other groups in terms of knowing evidence-based pathways and really tracking very specific protocols,” he says. “I think one of the advantages of hospitalist care is very often, it is guideline-driven. You have less variation in terms of care and quality outcomes.”
Cardiologists aren’t shy about repeating it: guidelines, guidelines, guidelines. That is, follow them.
“Evidence-based, guideline-driven optimal care for heart failure truly is beneficial,” Dr. Yancy says. “Every effort should be made to strive to achieve ideal thresholds and meeting best practices.”
There is now compelling evidence that, for patients with heart failure, the higher the degree of adherence to Class I-recommended therapies, the greater the reduction in 24-month mortality risk.5
“It would seem as if practicing best quality is almost a perfunctory statement, but consistently, when we look at surveys of quality improvement and adherence to evidence-based strategies, persistent gaps remain in the broader community,” Dr. Yancy says. “We know what we need to do. We’re still striving to get closer and closer to optimal care.”
Dr. Harold says the guidelines are there to make things simpler. So take advantage of them.
“If anything, hospitalists tend to be ahead of most other groups in terms of knowing evidence-based pathways and really tracking very specific protocols,” he says. “I think one of the advantages of hospitalist care is very often, it is guideline-driven. You have less variation in terms of care and quality outcomes.”
12 Things Cardiologists Think Hospitalists Need to Know
Only about a third of ideal candidates with heart failure are currently treated with [aldosterone antagonists], even though it markedly improves outcome and is Class I-recommended in the guidelines.

—Gregg Fonarow, MD, co-chief, University of California at Los Angeles division of cardiology, chair, American Heart Association’s Get With The Guidelines program steering committee
You might not have done a fellowship in cardiology, but quite often you probably feel like a cardiologist. Hospitalists frequently attend to patients on observation for heart problems and help manage even the most complex patients.
Often, you are working alongside the cardiologist. But other times, you’re on your own. Hospitalists are expected to carry an increasingly heavy load when it comes to heart-failure patients and many other kinds of patients with specialized disorders. It can be hard to keep up with what you need to know.
Top Twelve
- Recognize the new importance of beta-blockers for heart failure, and go with the best of them.
- It’s not readmissions that are the problem—it’s avoidable readmissions.
- New interventional technologies will mean more complex patients, so be ready.
- Aldosterone antagonists, though probably underutilized, can be very effective but require caution.
- Switching from IV diuretics to an oral regimen calls for careful monitoring.
- Patients with heart failure with preserved ejection fraction have outcomes over the longer haul similar to those with heart failure with reduced ejection fraction. And in preserved ejection fraction cases, the contributing illnesses must be addressed.
- Inotropic agents can do more harm than good.
- Pay attention to the ins and outs of new antiplatelet therapies.
- Bridging anticoagulant therapy in patients going for electrophysiology procedures should be done only some, not most, of the time.
- Some non-STEMI patients might benefit from getting to the catheterization lab quickly.
- Beware the idiosyncrasies of new anticoagulants.
- Be cognizant of stent thrombosis and how to manage it.
The Hospitalist spoke to several cardiologists about the latest in treatments, technologies, and HM’s role in the system of care. The following are their suggestions for what you really need to know about treating patients with heart conditions.
1) Recognize the new importance of beta-blockers for heart failure, and go with the best of them.
Angiotensin converting enzyme inhibitors and angiotensive receptor blockers have been part of the Centers for Medicare & Medicaid Services’ (CMS) core measures for heart failure for a long time, but beta-blockers at hospital discharge only recently have been added as American College of Cardiology/American Heart Association/American Medical Association–Physician Consortium for Performance Improvement measures for heart failure.1
“For those with heart failure and reduced left ventricular ejection fraction, very old and outdated concepts would have talked about potentially holding the beta-blocker during hospitalization for heart failure—or not initiating until the patient was an outpatient,” says Gregg Fonarow, MD, co-chief of the University of California at Los Angeles’ division of cardiology and chair of the steering committee for the American Heart Association’s Get With The Guidelines program. “[But] the guidelines and evidence, and often performance measures, linked to them are now explicit about initiating or maintaining beta-blockers during the heart-failure hospitalization.”
Beta-blockers should be initiated as patients are stabilized before discharge. Dr. Fonarow suggests hospitalists use only one of the three evidence-based therapies: carvedilol, metoprolol succinate, or bisoprolol.
“Many physicians have been using metoprolol tartrate or atenolol in heart-failure patients,” Dr. Fonarow says. “These are not known to improve clinical outcomes. So here’s an example where the specific medication is absolutely, critically important.”
2) It’s not readmissions that are the problem—it’s avoidable readmissions.
“The modifier is very important,” says Clyde Yancy, MD, chief of the division of cardiology at the Northwestern University Feinberg School of Medicine in Chicago. “Heart failure continues to be a problematic disease. Many patients now do really well, but some do not. Those patients are symptomatic and may require frequent hospitalizations for stabilization. We should not disallow or misdirect those patients who need inpatient care from receiving such because of an arbitrary incentive to reduce rehospitalizations out of fear of punitive financial damages. The unforeseen risks here are real.”
Dr. Yancy says studies based on CMS data have found that institutions with higher readmission rates have lower 30-day mortality rates.2 He cautions hospitalists to be “very thoughtful about an overzealous embrace of reducing all readmissions for heart failure.” Instead, the goal should be to limit the “avoidable readmissions.”
“And for the patient that clearly has advanced disease,” he says, “rather than triaging them away from the hospital, we really should be very respectful of their disease. Keep those patients where disease-modifying interventions can be deployed, and we can work to achieve the best possible outcome for those that have the most advanced disease.”
3) New interventional technologies will mean more complex patients, so be ready.
Advances in interventional procedures, including transcatheter aortic valve replacement (TAVR) and endoscopic mitral valve repair, will translate into a new population of highly complex patients. Many of these patients will be in their 80s or 90s.
“It’s a whole new paradigm shift of technology,” says John Harold, MD, president-elect of the American College of Cardiology and past chief of staff and department of medicine clinical chief of staff at Cedars-Sinai Medical Center in Los Angeles. “Very often, the hospitalist is at the front dealing with all of these issues.”
Many of these patients have other problems, including renal insufficiency, diabetes, and the like.
“They have all sorts of other things going on simultaneously, so very often the hospitalist becomes … the point person in dealing with all of these issues,” Dr. Harold says.
4) Aldosterone antagonists, though probably underutilized, can be very effective but require caution.
Aldosterone antagonists can greatly improve outcomes and reduce hospitalization in heart-failure patients, but they have to be used with very careful dosing and patient selection, Dr. Fonarow says. And they require early follow-up once patients are discharged.
“Only about a third of ideal candidates with heart failure are currently treated with this agent, even though it markedly improves outcome and is Class I-recommended in the guidelines,” Dr. Fonarow says. “But this is one where it needs to be started at appropriate low doses, with meticulous monitoring in both the inpatient and the outpatient setting, early follow-up, and early laboratory checks.”
5) Switching from IV diuretics to an oral regimen calls for careful monitoring.
Transitioning patients from IV diuretics to oral regimens is an area rife with mistakes, Dr. Fonarow says. It requires a lot of “meticulous attention to proper potassium supplementation and monitoring of renal function and electrolyte levels,” he says.
Medication reconciliation—“med rec”—is especially important during the transition from inpatient to outpatient.
“There are common medication errors that are made during this transition,” Dr. Fonarow says. “Hospitalists, along with other [care team] members, can really play a critically important role in trying to reduce that risk.”
6) Patients with heart failure with preserved ejection
fraction have outcomes over the longer haul similar to those with heart failure with reduced ejection fraction. And in preserved ejection fraction cases, the contributing illnesses must be addressed.
“We really can’t exercise a thought economy that just says, ‘Extrapolate the evidence-based therapies for heart failure with reduced ejection fraction to heart failure with preserved ejection fraction’ and expect good outcomes,” Dr. Yancy says. “That’s not the case. We don’t have an evidence base to substantiate that.”
He says one or more common comorbidities (e.g. atrial fibrillation, hypertension, obesity, diabetes, renal insufficiency) are present in 90% of patients with preserved ejection fraction. Treatment of those comorbidities—for example, rate control in afib patients, lowering the blood pressure in hypertension patients—has to be done with care.
“We should recognize that the therapy for this condition, albeit absent any specifically indicated interventions that will change its natural history, can still be skillfully constructed,” Dr. Yancy says. “But that construct needs to reflect the recommended, guideline-driven interventions for the concomitant other comorbidities.”
7) Inotropic agents can do more harm than good.
For patients who aren’t in cardiogenic shock, using inotropic agents doesn’t help. In fact, it might actually hurt. Dr. Fonarow says studies have shown these agents can “prolong length of stay, cause complications, and increase mortality risk.”
He notes that the use of inotropes should be avoided, or if it’s being considered, a cardiologist with knowledge and experience in heart failure should be involved in the treatment and care.
Statements about avoiding inotropes in heart failure, except under very specific circumstances, have been “incredibly strengthened” recently in the American College of Cardiology and Heart Failure Society of America guidelines.3
8) Pay attention to the ins and outs of new antiplatelet therapies.

—John Harold, MD, president-elect, American College of Cardiology, former chief of staff, department of medicine, Cedars-Sinai Medical Center, Los Angeles
Hospitalists caring for acute coronary syndrome patients need to familiarize themselves with updated guidelines and additional therapies that are now available, Dr. Fonarow says. New antiplatelet therapies (e.g. prasugrel and ticagrelor) are available as part of the armamentarium, along with the mainstay clopidogrel.
“These therapies lower the risk of recurrent events, lowered the risk of stent thrombosis,” he says. “In the case of ticagrelor, it actually lowered all-cause mortality. These are important new therapies, with new guideline recommendations, that all hospitalists should be aware of.”
9) Bridging anticoagulant therapy in patients going for electrophysiology procedures should be done only some, not most, of the time.
“Patients getting such devices as pacemakers or implantable cardioverter defribrillators (ICD) installed tend not to need bridging,” says Joaquin Cigarroa, MD, clinical chief of cardiology at Oregon Health & Science University in Portland.
He says it’s actually “safer” to do the procedure when patients “are on oral antithrombotics than switching them from an oral agent, and bridging with low- molecular-weight- or unfractionated heparin.”
“It’s a big deal,” Dr. Cigarroa adds, because it is risky to have elderly and frail patients on multiple antithrombotics. “Hemorrhagic complications in cardiology patients still occurs very frequently, so really be attuned to estimating bleeding risk and making sure that we’re dosing antithrombotics appropriately. Bridging should be the minority of patients, not the majority of patients.”
10) Some non-STEMI patients might benefit from getting to the catheterization lab quickly.
Door-to-balloon time is recognized as critical for ST-segment elevation myocardial infarction (STEMI) patients, but more recent work—such as in the TIMACS trial—finds benefits of early revascularization for some non-STEMI patients as well.2
“This trial showed that among higher-risk patients, using a validated risk score, that those patients did benefit from an early approach, meaning going to the cath lab in the first 12 hours of hospitalization,” Dr. Fonarow says. “We now have more information about the optimal timing of coronary angiography and potential revascularization of higher-risk patients with non-ST-segment elevation MI.”
11) Beware the idiosyncrasies of new anticoagulants.
The introduction of dabigatran and rivaroxaban (and, perhaps soon, apixaban) to the array of anticoagulant therapies brings a new slate of considerations for hospitalists, Dr. Harold says.
“For the majority of these, there’s no specific way to reverse the anticoagulant effect in the event of a major bleeding event,” he says. “There’s no simple antidote. And the effect can last up to 12 to 24 hours, depending on the renal function. This is what the hospitalist will be called to deal with: bleeding complications in patients who have these newer anticoagulants on board.”
Dr. Fonarow says that the new CHA2DS2-VASc score has been found to do a better job than the traditional CHADS2 score in assessing afib stroke risk.4
12) Be cognizant of stent thrombosis and how to manage it.
Dr. Harold says that most hospitalists probably are up to date on drug-eluting stents and the risk of stopping dual antiplatelet therapy within several months of implant, but that doesn’t mean they won’t treat patients whose primary-care physicians (PCPs) aren’t up to date. He recommends working on these cases with hematologists.
“That knowledge is not widespread in terms of the internal-medicine community,” he says. “I’ve seen situations where patients have had their Plavix stopped for colonoscopies and they’ve had stent thrombosis. It’s this knowledge of cardiac patients who come in with recent deployment of drug-eluting stents who may end up having other issues.”
Tom Collins is a freelance writer in South Florida.
References
- 2009 Focused Update: ACCF/AHA Guidelines for the Diagnosis and Management of Heart Failure in Adults. Circulation. 2009;119:1977-2016 an HFSA 2010 Comprehensive Heart Failure Practice Guideline. J Cardiac Failure. 2010;16(6):475-539.
- Gorodeski EZ, Starling RC, Blackstone EH. Are all readmissions bad readmissions? N Engl J Med. 2010;363:297-298.
- Mehta SR, Granger CB, Boden WE, et al. Early versus delayed invasive intervention in acute coronary syndromes. N Engl J Med. 2009;360(21):2165-2175.
- Olesen JB, Torp-Pedersen C, Hansen ML, Lip GY. The value of the CHA2DS2-VASc score for refining stroke risk stratification in patients with atrial fibrillation with a CHADS2 score 0-1: a nationwide cohort study. Thromb Haemost. 2012;107(6):1172-1179.
- Associations between outpatient heart failure process-of-care measures and mortality. Circulation. 2011;123(15):1601-1610.
Only about a third of ideal candidates with heart failure are currently treated with [aldosterone antagonists], even though it markedly improves outcome and is Class I-recommended in the guidelines.

—Gregg Fonarow, MD, co-chief, University of California at Los Angeles division of cardiology, chair, American Heart Association’s Get With The Guidelines program steering committee
You might not have done a fellowship in cardiology, but quite often you probably feel like a cardiologist. Hospitalists frequently attend to patients on observation for heart problems and help manage even the most complex patients.
Often, you are working alongside the cardiologist. But other times, you’re on your own. Hospitalists are expected to carry an increasingly heavy load when it comes to heart-failure patients and many other kinds of patients with specialized disorders. It can be hard to keep up with what you need to know.
Top Twelve
- Recognize the new importance of beta-blockers for heart failure, and go with the best of them.
- It’s not readmissions that are the problem—it’s avoidable readmissions.
- New interventional technologies will mean more complex patients, so be ready.
- Aldosterone antagonists, though probably underutilized, can be very effective but require caution.
- Switching from IV diuretics to an oral regimen calls for careful monitoring.
- Patients with heart failure with preserved ejection fraction have outcomes over the longer haul similar to those with heart failure with reduced ejection fraction. And in preserved ejection fraction cases, the contributing illnesses must be addressed.
- Inotropic agents can do more harm than good.
- Pay attention to the ins and outs of new antiplatelet therapies.
- Bridging anticoagulant therapy in patients going for electrophysiology procedures should be done only some, not most, of the time.
- Some non-STEMI patients might benefit from getting to the catheterization lab quickly.
- Beware the idiosyncrasies of new anticoagulants.
- Be cognizant of stent thrombosis and how to manage it.
The Hospitalist spoke to several cardiologists about the latest in treatments, technologies, and HM’s role in the system of care. The following are their suggestions for what you really need to know about treating patients with heart conditions.
1) Recognize the new importance of beta-blockers for heart failure, and go with the best of them.
Angiotensin converting enzyme inhibitors and angiotensive receptor blockers have been part of the Centers for Medicare & Medicaid Services’ (CMS) core measures for heart failure for a long time, but beta-blockers at hospital discharge only recently have been added as American College of Cardiology/American Heart Association/American Medical Association–Physician Consortium for Performance Improvement measures for heart failure.1
“For those with heart failure and reduced left ventricular ejection fraction, very old and outdated concepts would have talked about potentially holding the beta-blocker during hospitalization for heart failure—or not initiating until the patient was an outpatient,” says Gregg Fonarow, MD, co-chief of the University of California at Los Angeles’ division of cardiology and chair of the steering committee for the American Heart Association’s Get With The Guidelines program. “[But] the guidelines and evidence, and often performance measures, linked to them are now explicit about initiating or maintaining beta-blockers during the heart-failure hospitalization.”
Beta-blockers should be initiated as patients are stabilized before discharge. Dr. Fonarow suggests hospitalists use only one of the three evidence-based therapies: carvedilol, metoprolol succinate, or bisoprolol.
“Many physicians have been using metoprolol tartrate or atenolol in heart-failure patients,” Dr. Fonarow says. “These are not known to improve clinical outcomes. So here’s an example where the specific medication is absolutely, critically important.”
2) It’s not readmissions that are the problem—it’s avoidable readmissions.
“The modifier is very important,” says Clyde Yancy, MD, chief of the division of cardiology at the Northwestern University Feinberg School of Medicine in Chicago. “Heart failure continues to be a problematic disease. Many patients now do really well, but some do not. Those patients are symptomatic and may require frequent hospitalizations for stabilization. We should not disallow or misdirect those patients who need inpatient care from receiving such because of an arbitrary incentive to reduce rehospitalizations out of fear of punitive financial damages. The unforeseen risks here are real.”
Dr. Yancy says studies based on CMS data have found that institutions with higher readmission rates have lower 30-day mortality rates.2 He cautions hospitalists to be “very thoughtful about an overzealous embrace of reducing all readmissions for heart failure.” Instead, the goal should be to limit the “avoidable readmissions.”
“And for the patient that clearly has advanced disease,” he says, “rather than triaging them away from the hospital, we really should be very respectful of their disease. Keep those patients where disease-modifying interventions can be deployed, and we can work to achieve the best possible outcome for those that have the most advanced disease.”
3) New interventional technologies will mean more complex patients, so be ready.
Advances in interventional procedures, including transcatheter aortic valve replacement (TAVR) and endoscopic mitral valve repair, will translate into a new population of highly complex patients. Many of these patients will be in their 80s or 90s.
“It’s a whole new paradigm shift of technology,” says John Harold, MD, president-elect of the American College of Cardiology and past chief of staff and department of medicine clinical chief of staff at Cedars-Sinai Medical Center in Los Angeles. “Very often, the hospitalist is at the front dealing with all of these issues.”
Many of these patients have other problems, including renal insufficiency, diabetes, and the like.
“They have all sorts of other things going on simultaneously, so very often the hospitalist becomes … the point person in dealing with all of these issues,” Dr. Harold says.
4) Aldosterone antagonists, though probably underutilized, can be very effective but require caution.
Aldosterone antagonists can greatly improve outcomes and reduce hospitalization in heart-failure patients, but they have to be used with very careful dosing and patient selection, Dr. Fonarow says. And they require early follow-up once patients are discharged.
“Only about a third of ideal candidates with heart failure are currently treated with this agent, even though it markedly improves outcome and is Class I-recommended in the guidelines,” Dr. Fonarow says. “But this is one where it needs to be started at appropriate low doses, with meticulous monitoring in both the inpatient and the outpatient setting, early follow-up, and early laboratory checks.”
5) Switching from IV diuretics to an oral regimen calls for careful monitoring.
Transitioning patients from IV diuretics to oral regimens is an area rife with mistakes, Dr. Fonarow says. It requires a lot of “meticulous attention to proper potassium supplementation and monitoring of renal function and electrolyte levels,” he says.
Medication reconciliation—“med rec”—is especially important during the transition from inpatient to outpatient.
“There are common medication errors that are made during this transition,” Dr. Fonarow says. “Hospitalists, along with other [care team] members, can really play a critically important role in trying to reduce that risk.”
6) Patients with heart failure with preserved ejection
fraction have outcomes over the longer haul similar to those with heart failure with reduced ejection fraction. And in preserved ejection fraction cases, the contributing illnesses must be addressed.
“We really can’t exercise a thought economy that just says, ‘Extrapolate the evidence-based therapies for heart failure with reduced ejection fraction to heart failure with preserved ejection fraction’ and expect good outcomes,” Dr. Yancy says. “That’s not the case. We don’t have an evidence base to substantiate that.”
He says one or more common comorbidities (e.g. atrial fibrillation, hypertension, obesity, diabetes, renal insufficiency) are present in 90% of patients with preserved ejection fraction. Treatment of those comorbidities—for example, rate control in afib patients, lowering the blood pressure in hypertension patients—has to be done with care.
“We should recognize that the therapy for this condition, albeit absent any specifically indicated interventions that will change its natural history, can still be skillfully constructed,” Dr. Yancy says. “But that construct needs to reflect the recommended, guideline-driven interventions for the concomitant other comorbidities.”
7) Inotropic agents can do more harm than good.
For patients who aren’t in cardiogenic shock, using inotropic agents doesn’t help. In fact, it might actually hurt. Dr. Fonarow says studies have shown these agents can “prolong length of stay, cause complications, and increase mortality risk.”
He notes that the use of inotropes should be avoided, or if it’s being considered, a cardiologist with knowledge and experience in heart failure should be involved in the treatment and care.
Statements about avoiding inotropes in heart failure, except under very specific circumstances, have been “incredibly strengthened” recently in the American College of Cardiology and Heart Failure Society of America guidelines.3
8) Pay attention to the ins and outs of new antiplatelet therapies.

—John Harold, MD, president-elect, American College of Cardiology, former chief of staff, department of medicine, Cedars-Sinai Medical Center, Los Angeles
Hospitalists caring for acute coronary syndrome patients need to familiarize themselves with updated guidelines and additional therapies that are now available, Dr. Fonarow says. New antiplatelet therapies (e.g. prasugrel and ticagrelor) are available as part of the armamentarium, along with the mainstay clopidogrel.
“These therapies lower the risk of recurrent events, lowered the risk of stent thrombosis,” he says. “In the case of ticagrelor, it actually lowered all-cause mortality. These are important new therapies, with new guideline recommendations, that all hospitalists should be aware of.”
9) Bridging anticoagulant therapy in patients going for electrophysiology procedures should be done only some, not most, of the time.
“Patients getting such devices as pacemakers or implantable cardioverter defribrillators (ICD) installed tend not to need bridging,” says Joaquin Cigarroa, MD, clinical chief of cardiology at Oregon Health & Science University in Portland.
He says it’s actually “safer” to do the procedure when patients “are on oral antithrombotics than switching them from an oral agent, and bridging with low- molecular-weight- or unfractionated heparin.”
“It’s a big deal,” Dr. Cigarroa adds, because it is risky to have elderly and frail patients on multiple antithrombotics. “Hemorrhagic complications in cardiology patients still occurs very frequently, so really be attuned to estimating bleeding risk and making sure that we’re dosing antithrombotics appropriately. Bridging should be the minority of patients, not the majority of patients.”
10) Some non-STEMI patients might benefit from getting to the catheterization lab quickly.
Door-to-balloon time is recognized as critical for ST-segment elevation myocardial infarction (STEMI) patients, but more recent work—such as in the TIMACS trial—finds benefits of early revascularization for some non-STEMI patients as well.2
“This trial showed that among higher-risk patients, using a validated risk score, that those patients did benefit from an early approach, meaning going to the cath lab in the first 12 hours of hospitalization,” Dr. Fonarow says. “We now have more information about the optimal timing of coronary angiography and potential revascularization of higher-risk patients with non-ST-segment elevation MI.”
11) Beware the idiosyncrasies of new anticoagulants.
The introduction of dabigatran and rivaroxaban (and, perhaps soon, apixaban) to the array of anticoagulant therapies brings a new slate of considerations for hospitalists, Dr. Harold says.
“For the majority of these, there’s no specific way to reverse the anticoagulant effect in the event of a major bleeding event,” he says. “There’s no simple antidote. And the effect can last up to 12 to 24 hours, depending on the renal function. This is what the hospitalist will be called to deal with: bleeding complications in patients who have these newer anticoagulants on board.”
Dr. Fonarow says that the new CHA2DS2-VASc score has been found to do a better job than the traditional CHADS2 score in assessing afib stroke risk.4
12) Be cognizant of stent thrombosis and how to manage it.
Dr. Harold says that most hospitalists probably are up to date on drug-eluting stents and the risk of stopping dual antiplatelet therapy within several months of implant, but that doesn’t mean they won’t treat patients whose primary-care physicians (PCPs) aren’t up to date. He recommends working on these cases with hematologists.
“That knowledge is not widespread in terms of the internal-medicine community,” he says. “I’ve seen situations where patients have had their Plavix stopped for colonoscopies and they’ve had stent thrombosis. It’s this knowledge of cardiac patients who come in with recent deployment of drug-eluting stents who may end up having other issues.”
Tom Collins is a freelance writer in South Florida.
References
- 2009 Focused Update: ACCF/AHA Guidelines for the Diagnosis and Management of Heart Failure in Adults. Circulation. 2009;119:1977-2016 an HFSA 2010 Comprehensive Heart Failure Practice Guideline. J Cardiac Failure. 2010;16(6):475-539.
- Gorodeski EZ, Starling RC, Blackstone EH. Are all readmissions bad readmissions? N Engl J Med. 2010;363:297-298.
- Mehta SR, Granger CB, Boden WE, et al. Early versus delayed invasive intervention in acute coronary syndromes. N Engl J Med. 2009;360(21):2165-2175.
- Olesen JB, Torp-Pedersen C, Hansen ML, Lip GY. The value of the CHA2DS2-VASc score for refining stroke risk stratification in patients with atrial fibrillation with a CHADS2 score 0-1: a nationwide cohort study. Thromb Haemost. 2012;107(6):1172-1179.
- Associations between outpatient heart failure process-of-care measures and mortality. Circulation. 2011;123(15):1601-1610.
Only about a third of ideal candidates with heart failure are currently treated with [aldosterone antagonists], even though it markedly improves outcome and is Class I-recommended in the guidelines.

—Gregg Fonarow, MD, co-chief, University of California at Los Angeles division of cardiology, chair, American Heart Association’s Get With The Guidelines program steering committee
You might not have done a fellowship in cardiology, but quite often you probably feel like a cardiologist. Hospitalists frequently attend to patients on observation for heart problems and help manage even the most complex patients.
Often, you are working alongside the cardiologist. But other times, you’re on your own. Hospitalists are expected to carry an increasingly heavy load when it comes to heart-failure patients and many other kinds of patients with specialized disorders. It can be hard to keep up with what you need to know.
Top Twelve
- Recognize the new importance of beta-blockers for heart failure, and go with the best of them.
- It’s not readmissions that are the problem—it’s avoidable readmissions.
- New interventional technologies will mean more complex patients, so be ready.
- Aldosterone antagonists, though probably underutilized, can be very effective but require caution.
- Switching from IV diuretics to an oral regimen calls for careful monitoring.
- Patients with heart failure with preserved ejection fraction have outcomes over the longer haul similar to those with heart failure with reduced ejection fraction. And in preserved ejection fraction cases, the contributing illnesses must be addressed.
- Inotropic agents can do more harm than good.
- Pay attention to the ins and outs of new antiplatelet therapies.
- Bridging anticoagulant therapy in patients going for electrophysiology procedures should be done only some, not most, of the time.
- Some non-STEMI patients might benefit from getting to the catheterization lab quickly.
- Beware the idiosyncrasies of new anticoagulants.
- Be cognizant of stent thrombosis and how to manage it.
The Hospitalist spoke to several cardiologists about the latest in treatments, technologies, and HM’s role in the system of care. The following are their suggestions for what you really need to know about treating patients with heart conditions.
1) Recognize the new importance of beta-blockers for heart failure, and go with the best of them.
Angiotensin converting enzyme inhibitors and angiotensive receptor blockers have been part of the Centers for Medicare & Medicaid Services’ (CMS) core measures for heart failure for a long time, but beta-blockers at hospital discharge only recently have been added as American College of Cardiology/American Heart Association/American Medical Association–Physician Consortium for Performance Improvement measures for heart failure.1
“For those with heart failure and reduced left ventricular ejection fraction, very old and outdated concepts would have talked about potentially holding the beta-blocker during hospitalization for heart failure—or not initiating until the patient was an outpatient,” says Gregg Fonarow, MD, co-chief of the University of California at Los Angeles’ division of cardiology and chair of the steering committee for the American Heart Association’s Get With The Guidelines program. “[But] the guidelines and evidence, and often performance measures, linked to them are now explicit about initiating or maintaining beta-blockers during the heart-failure hospitalization.”
Beta-blockers should be initiated as patients are stabilized before discharge. Dr. Fonarow suggests hospitalists use only one of the three evidence-based therapies: carvedilol, metoprolol succinate, or bisoprolol.
“Many physicians have been using metoprolol tartrate or atenolol in heart-failure patients,” Dr. Fonarow says. “These are not known to improve clinical outcomes. So here’s an example where the specific medication is absolutely, critically important.”
2) It’s not readmissions that are the problem—it’s avoidable readmissions.
“The modifier is very important,” says Clyde Yancy, MD, chief of the division of cardiology at the Northwestern University Feinberg School of Medicine in Chicago. “Heart failure continues to be a problematic disease. Many patients now do really well, but some do not. Those patients are symptomatic and may require frequent hospitalizations for stabilization. We should not disallow or misdirect those patients who need inpatient care from receiving such because of an arbitrary incentive to reduce rehospitalizations out of fear of punitive financial damages. The unforeseen risks here are real.”
Dr. Yancy says studies based on CMS data have found that institutions with higher readmission rates have lower 30-day mortality rates.2 He cautions hospitalists to be “very thoughtful about an overzealous embrace of reducing all readmissions for heart failure.” Instead, the goal should be to limit the “avoidable readmissions.”
“And for the patient that clearly has advanced disease,” he says, “rather than triaging them away from the hospital, we really should be very respectful of their disease. Keep those patients where disease-modifying interventions can be deployed, and we can work to achieve the best possible outcome for those that have the most advanced disease.”
3) New interventional technologies will mean more complex patients, so be ready.
Advances in interventional procedures, including transcatheter aortic valve replacement (TAVR) and endoscopic mitral valve repair, will translate into a new population of highly complex patients. Many of these patients will be in their 80s or 90s.
“It’s a whole new paradigm shift of technology,” says John Harold, MD, president-elect of the American College of Cardiology and past chief of staff and department of medicine clinical chief of staff at Cedars-Sinai Medical Center in Los Angeles. “Very often, the hospitalist is at the front dealing with all of these issues.”
Many of these patients have other problems, including renal insufficiency, diabetes, and the like.
“They have all sorts of other things going on simultaneously, so very often the hospitalist becomes … the point person in dealing with all of these issues,” Dr. Harold says.
4) Aldosterone antagonists, though probably underutilized, can be very effective but require caution.
Aldosterone antagonists can greatly improve outcomes and reduce hospitalization in heart-failure patients, but they have to be used with very careful dosing and patient selection, Dr. Fonarow says. And they require early follow-up once patients are discharged.
“Only about a third of ideal candidates with heart failure are currently treated with this agent, even though it markedly improves outcome and is Class I-recommended in the guidelines,” Dr. Fonarow says. “But this is one where it needs to be started at appropriate low doses, with meticulous monitoring in both the inpatient and the outpatient setting, early follow-up, and early laboratory checks.”
5) Switching from IV diuretics to an oral regimen calls for careful monitoring.
Transitioning patients from IV diuretics to oral regimens is an area rife with mistakes, Dr. Fonarow says. It requires a lot of “meticulous attention to proper potassium supplementation and monitoring of renal function and electrolyte levels,” he says.
Medication reconciliation—“med rec”—is especially important during the transition from inpatient to outpatient.
“There are common medication errors that are made during this transition,” Dr. Fonarow says. “Hospitalists, along with other [care team] members, can really play a critically important role in trying to reduce that risk.”
6) Patients with heart failure with preserved ejection
fraction have outcomes over the longer haul similar to those with heart failure with reduced ejection fraction. And in preserved ejection fraction cases, the contributing illnesses must be addressed.
“We really can’t exercise a thought economy that just says, ‘Extrapolate the evidence-based therapies for heart failure with reduced ejection fraction to heart failure with preserved ejection fraction’ and expect good outcomes,” Dr. Yancy says. “That’s not the case. We don’t have an evidence base to substantiate that.”
He says one or more common comorbidities (e.g. atrial fibrillation, hypertension, obesity, diabetes, renal insufficiency) are present in 90% of patients with preserved ejection fraction. Treatment of those comorbidities—for example, rate control in afib patients, lowering the blood pressure in hypertension patients—has to be done with care.
“We should recognize that the therapy for this condition, albeit absent any specifically indicated interventions that will change its natural history, can still be skillfully constructed,” Dr. Yancy says. “But that construct needs to reflect the recommended, guideline-driven interventions for the concomitant other comorbidities.”
7) Inotropic agents can do more harm than good.
For patients who aren’t in cardiogenic shock, using inotropic agents doesn’t help. In fact, it might actually hurt. Dr. Fonarow says studies have shown these agents can “prolong length of stay, cause complications, and increase mortality risk.”
He notes that the use of inotropes should be avoided, or if it’s being considered, a cardiologist with knowledge and experience in heart failure should be involved in the treatment and care.
Statements about avoiding inotropes in heart failure, except under very specific circumstances, have been “incredibly strengthened” recently in the American College of Cardiology and Heart Failure Society of America guidelines.3
8) Pay attention to the ins and outs of new antiplatelet therapies.

—John Harold, MD, president-elect, American College of Cardiology, former chief of staff, department of medicine, Cedars-Sinai Medical Center, Los Angeles
Hospitalists caring for acute coronary syndrome patients need to familiarize themselves with updated guidelines and additional therapies that are now available, Dr. Fonarow says. New antiplatelet therapies (e.g. prasugrel and ticagrelor) are available as part of the armamentarium, along with the mainstay clopidogrel.
“These therapies lower the risk of recurrent events, lowered the risk of stent thrombosis,” he says. “In the case of ticagrelor, it actually lowered all-cause mortality. These are important new therapies, with new guideline recommendations, that all hospitalists should be aware of.”
9) Bridging anticoagulant therapy in patients going for electrophysiology procedures should be done only some, not most, of the time.
“Patients getting such devices as pacemakers or implantable cardioverter defribrillators (ICD) installed tend not to need bridging,” says Joaquin Cigarroa, MD, clinical chief of cardiology at Oregon Health & Science University in Portland.
He says it’s actually “safer” to do the procedure when patients “are on oral antithrombotics than switching them from an oral agent, and bridging with low- molecular-weight- or unfractionated heparin.”
“It’s a big deal,” Dr. Cigarroa adds, because it is risky to have elderly and frail patients on multiple antithrombotics. “Hemorrhagic complications in cardiology patients still occurs very frequently, so really be attuned to estimating bleeding risk and making sure that we’re dosing antithrombotics appropriately. Bridging should be the minority of patients, not the majority of patients.”
10) Some non-STEMI patients might benefit from getting to the catheterization lab quickly.
Door-to-balloon time is recognized as critical for ST-segment elevation myocardial infarction (STEMI) patients, but more recent work—such as in the TIMACS trial—finds benefits of early revascularization for some non-STEMI patients as well.2
“This trial showed that among higher-risk patients, using a validated risk score, that those patients did benefit from an early approach, meaning going to the cath lab in the first 12 hours of hospitalization,” Dr. Fonarow says. “We now have more information about the optimal timing of coronary angiography and potential revascularization of higher-risk patients with non-ST-segment elevation MI.”
11) Beware the idiosyncrasies of new anticoagulants.
The introduction of dabigatran and rivaroxaban (and, perhaps soon, apixaban) to the array of anticoagulant therapies brings a new slate of considerations for hospitalists, Dr. Harold says.
“For the majority of these, there’s no specific way to reverse the anticoagulant effect in the event of a major bleeding event,” he says. “There’s no simple antidote. And the effect can last up to 12 to 24 hours, depending on the renal function. This is what the hospitalist will be called to deal with: bleeding complications in patients who have these newer anticoagulants on board.”
Dr. Fonarow says that the new CHA2DS2-VASc score has been found to do a better job than the traditional CHADS2 score in assessing afib stroke risk.4
12) Be cognizant of stent thrombosis and how to manage it.
Dr. Harold says that most hospitalists probably are up to date on drug-eluting stents and the risk of stopping dual antiplatelet therapy within several months of implant, but that doesn’t mean they won’t treat patients whose primary-care physicians (PCPs) aren’t up to date. He recommends working on these cases with hematologists.
“That knowledge is not widespread in terms of the internal-medicine community,” he says. “I’ve seen situations where patients have had their Plavix stopped for colonoscopies and they’ve had stent thrombosis. It’s this knowledge of cardiac patients who come in with recent deployment of drug-eluting stents who may end up having other issues.”
Tom Collins is a freelance writer in South Florida.
References
- 2009 Focused Update: ACCF/AHA Guidelines for the Diagnosis and Management of Heart Failure in Adults. Circulation. 2009;119:1977-2016 an HFSA 2010 Comprehensive Heart Failure Practice Guideline. J Cardiac Failure. 2010;16(6):475-539.
- Gorodeski EZ, Starling RC, Blackstone EH. Are all readmissions bad readmissions? N Engl J Med. 2010;363:297-298.
- Mehta SR, Granger CB, Boden WE, et al. Early versus delayed invasive intervention in acute coronary syndromes. N Engl J Med. 2009;360(21):2165-2175.
- Olesen JB, Torp-Pedersen C, Hansen ML, Lip GY. The value of the CHA2DS2-VASc score for refining stroke risk stratification in patients with atrial fibrillation with a CHADS2 score 0-1: a nationwide cohort study. Thromb Haemost. 2012;107(6):1172-1179.
- Associations between outpatient heart failure process-of-care measures and mortality. Circulation. 2011;123(15):1601-1610.
Hospitalist-Led Teams Vital to Improved ED Care
Hospitalist-led teams in the ED help reduce diversions, improve patient flow, and provide more timely care to boarded patients, according to a study in the Journal of Hospital Medicine (JHM).
The single-center study, "Hospitalist-Led Medicine Emergency Department Team: Associations with Throughput, Timeliness of Patient Care, and Satisfaction," found a reduction in diversions due to medicine bed capacity of 27% (4.5% to 3%, P=<0.01). Boarded patients were rounded a mean of 2 hours and 9 minutes earlier with hospitalist-led teams; length of stay (LOS) in the ED, LOS in the hospital, and 48-hour returns were unchanged. The study, which took place at 477-bed Denver Health Medical Center (DHMC), assigned a hospitalist and an allied health provider to the ED during dayshifts. At night, ED coverage was rolled into the existing hospitalist duties.
Lead author Smitha R. Chadaga, MD, who works in DHMC's Department of Medicine, believes the study could spur more HM groups to consider dedicating a staffer to the ED. The team in Denver was created to care for medicine patients in the ED awaiting inpatient beds, and to work with nursing supervisors to improve bed management.
"There are numerous places that hospitalists can impact hospital flow, whether it's helping with bed management, providing consultative services to the ED, or caring for boarded patients," Dr. Chadaga says. "Knowing the ins and outs of inpatient medicine really lends itself well to some areas that hospitalists might not have thought about before."
Dr. Chadaga says the research is broadly applicable because HM groups can implement its different features. For example, adding a consultative phone service can help ED physicians determine whether a patient needs to be admitted and could improve patient flow.
Hospitalist-led teams in the ED help reduce diversions, improve patient flow, and provide more timely care to boarded patients, according to a study in the Journal of Hospital Medicine (JHM).
The single-center study, "Hospitalist-Led Medicine Emergency Department Team: Associations with Throughput, Timeliness of Patient Care, and Satisfaction," found a reduction in diversions due to medicine bed capacity of 27% (4.5% to 3%, P=<0.01). Boarded patients were rounded a mean of 2 hours and 9 minutes earlier with hospitalist-led teams; length of stay (LOS) in the ED, LOS in the hospital, and 48-hour returns were unchanged. The study, which took place at 477-bed Denver Health Medical Center (DHMC), assigned a hospitalist and an allied health provider to the ED during dayshifts. At night, ED coverage was rolled into the existing hospitalist duties.
Lead author Smitha R. Chadaga, MD, who works in DHMC's Department of Medicine, believes the study could spur more HM groups to consider dedicating a staffer to the ED. The team in Denver was created to care for medicine patients in the ED awaiting inpatient beds, and to work with nursing supervisors to improve bed management.
"There are numerous places that hospitalists can impact hospital flow, whether it's helping with bed management, providing consultative services to the ED, or caring for boarded patients," Dr. Chadaga says. "Knowing the ins and outs of inpatient medicine really lends itself well to some areas that hospitalists might not have thought about before."
Dr. Chadaga says the research is broadly applicable because HM groups can implement its different features. For example, adding a consultative phone service can help ED physicians determine whether a patient needs to be admitted and could improve patient flow.
Hospitalist-led teams in the ED help reduce diversions, improve patient flow, and provide more timely care to boarded patients, according to a study in the Journal of Hospital Medicine (JHM).
The single-center study, "Hospitalist-Led Medicine Emergency Department Team: Associations with Throughput, Timeliness of Patient Care, and Satisfaction," found a reduction in diversions due to medicine bed capacity of 27% (4.5% to 3%, P=<0.01). Boarded patients were rounded a mean of 2 hours and 9 minutes earlier with hospitalist-led teams; length of stay (LOS) in the ED, LOS in the hospital, and 48-hour returns were unchanged. The study, which took place at 477-bed Denver Health Medical Center (DHMC), assigned a hospitalist and an allied health provider to the ED during dayshifts. At night, ED coverage was rolled into the existing hospitalist duties.
Lead author Smitha R. Chadaga, MD, who works in DHMC's Department of Medicine, believes the study could spur more HM groups to consider dedicating a staffer to the ED. The team in Denver was created to care for medicine patients in the ED awaiting inpatient beds, and to work with nursing supervisors to improve bed management.
"There are numerous places that hospitalists can impact hospital flow, whether it's helping with bed management, providing consultative services to the ED, or caring for boarded patients," Dr. Chadaga says. "Knowing the ins and outs of inpatient medicine really lends itself well to some areas that hospitalists might not have thought about before."
Dr. Chadaga says the research is broadly applicable because HM groups can implement its different features. For example, adding a consultative phone service can help ED physicians determine whether a patient needs to be admitted and could improve patient flow.
Local Solutions Spark Readmission Reductions
Earlier this month CMS announced 17 additional awards under its Community-Based Care Transitions Program (CCTP), which now encompasses 200 acute-care hospitals and their hospitalists partnering with community agencies and coalitions to improve transitions of care in advance of the Oct. 1 start for excessive readmissions penalties. Innovative solutions to the readmissions dilemma are being tested at the local level by a variety of partnerships with hospitals and hospitalists.
For example, William C. Cook, DO, chief of hospital medicine for the Ohio Permanente Medical Group in Cleveland, is part of a community-wide quality coalition called Better Health Greater Cleveland, one of 17 such groups in the Robert Wood Johnson Foundation's Aligning Forces for Quality collaborative. The program includes 150 quality teams in 100 hospitals posting readmissions reductions and other quality metrics. Dr. Cook, who co-chairs Better Health's Steering Committee for Transitions of Care, is spearheading a transitions pilot with two local nursing homes.
"From the hospitalist perspective, our role is to make care transitions safe and predictable," Dr. Cook says. "The way I can contribute most to these transitions is by thinking ahead about what's going to happen next—and how do I prepare the patient and the next provider." One key step is taking time to complete the real-time discharge summary for each patient, he adds.
The idea, Dr. Cook explains, is to identify and communicate with collaborators across care settings so that the "coaching baton" can be passed in a manner that appears seamless to the patient.
Nearly a third of the 17 new CCTP sites participate in SHM's Project BOOST, including three hospitals in California and one each in Illinois and Pennsylvania. Project BOOST is accepting applications for its next round of sites through September.
Earlier this month CMS announced 17 additional awards under its Community-Based Care Transitions Program (CCTP), which now encompasses 200 acute-care hospitals and their hospitalists partnering with community agencies and coalitions to improve transitions of care in advance of the Oct. 1 start for excessive readmissions penalties. Innovative solutions to the readmissions dilemma are being tested at the local level by a variety of partnerships with hospitals and hospitalists.
For example, William C. Cook, DO, chief of hospital medicine for the Ohio Permanente Medical Group in Cleveland, is part of a community-wide quality coalition called Better Health Greater Cleveland, one of 17 such groups in the Robert Wood Johnson Foundation's Aligning Forces for Quality collaborative. The program includes 150 quality teams in 100 hospitals posting readmissions reductions and other quality metrics. Dr. Cook, who co-chairs Better Health's Steering Committee for Transitions of Care, is spearheading a transitions pilot with two local nursing homes.
"From the hospitalist perspective, our role is to make care transitions safe and predictable," Dr. Cook says. "The way I can contribute most to these transitions is by thinking ahead about what's going to happen next—and how do I prepare the patient and the next provider." One key step is taking time to complete the real-time discharge summary for each patient, he adds.
The idea, Dr. Cook explains, is to identify and communicate with collaborators across care settings so that the "coaching baton" can be passed in a manner that appears seamless to the patient.
Nearly a third of the 17 new CCTP sites participate in SHM's Project BOOST, including three hospitals in California and one each in Illinois and Pennsylvania. Project BOOST is accepting applications for its next round of sites through September.
Earlier this month CMS announced 17 additional awards under its Community-Based Care Transitions Program (CCTP), which now encompasses 200 acute-care hospitals and their hospitalists partnering with community agencies and coalitions to improve transitions of care in advance of the Oct. 1 start for excessive readmissions penalties. Innovative solutions to the readmissions dilemma are being tested at the local level by a variety of partnerships with hospitals and hospitalists.
For example, William C. Cook, DO, chief of hospital medicine for the Ohio Permanente Medical Group in Cleveland, is part of a community-wide quality coalition called Better Health Greater Cleveland, one of 17 such groups in the Robert Wood Johnson Foundation's Aligning Forces for Quality collaborative. The program includes 150 quality teams in 100 hospitals posting readmissions reductions and other quality metrics. Dr. Cook, who co-chairs Better Health's Steering Committee for Transitions of Care, is spearheading a transitions pilot with two local nursing homes.
"From the hospitalist perspective, our role is to make care transitions safe and predictable," Dr. Cook says. "The way I can contribute most to these transitions is by thinking ahead about what's going to happen next—and how do I prepare the patient and the next provider." One key step is taking time to complete the real-time discharge summary for each patient, he adds.
The idea, Dr. Cook explains, is to identify and communicate with collaborators across care settings so that the "coaching baton" can be passed in a manner that appears seamless to the patient.
Nearly a third of the 17 new CCTP sites participate in SHM's Project BOOST, including three hospitals in California and one each in Illinois and Pennsylvania. Project BOOST is accepting applications for its next round of sites through September.