User login
The Official Newspaper of the American Association for Thoracic Surgery
SAPIEN Valve Makers Comment On Proposed TAVR Coverage
While commending the Centers for Medicare and Medicaid Services on its proposed coverage of the transcatheter aortic valve replacement procedure, makers of the SAPIEN artificial valve asked for more flexibility in the clinical trial limitations set by the agency, in an official comment they released on March 5.
Edwards Lifesciences, the manufacturer of the only valve approved for the TAVR procedure in the United States, posted its comment during the 60-day period, which began after CMS released its coverage proposal for TAVR in February.
In its proposal, CMS restricts TAVR coverage to five criteria, including the use of an approved valve, presence of multidisciplinary teams, and enrollment in a registry.
Edwards officials wrote they were pleased that CMS had proposed "clear and flexible national coverage for TAVR," and added that "for appropriately selected Medicare beneficiaries, the evidence is more than adequate for CMS to conclude that TAVR improves health outcomes and should be considered reasonable and necessary under the Medicare statute," if provided under the CMS criteria.
The Edwards SAPIEN valve is currently approved for use in inoperable patients with severe aortic stenosis. Other use of the SAPIEN valve is limited to clinical trials. In their comments, Edwards officials asked CMS for flexibility in the trials they consider for coverage determination.
"CMS’s proposed requirement limiting coverage for unlabeled uses to ‘superiority trials’ undermines the agency’s efforts to promote continued US-based clinical investigations in Medicare beneficiaries aimed at better understanding key determinants of health and quality of life outcomes," according to the Edwards’ comments.
"Noninferiority and other clinical trial designs play an important role in the advancement of medical technology," the company added, saying that if the proposed conditions aren’t revised, important, yet relatively small, patient populations may not be able to receive treatment.
Edwards, which said its transcatheter aortic valves have been implanted in more than 25,000 patients around the world, came in strong support of multidisciplinary heart teams, one of the requirements set by CMS for TAVR coverage, and strongly encouraged by leading cardiovascular organizations.
"It is imperative that at least two engaged cardiothoracic surgeons and two interventional cardiologists at each site coordinate all clinicians to form a high-functioning multi-disciplinary heart team, a key concept integral to assuring TAVR success," Edwards officials wrote in their comment.
The company also addressed credentialing, an issue which four leading cardiovascular organizations also addressed in a consensus document (see story at right).
"We support appropriate facility and heart team criteria – rather than traditional individual physician-based credentialing," to achieve TAVR success.
Following the CMS proposal, the Society of Thoracic Surgeons and the American College of Cardiology issued a statement, saying that they were pleased with CMS’s comprehensive approach to the coverage of TAVR.
CMS is expected to issue a final decision on TAVR coverage by May.
While commending the Centers for Medicare and Medicaid Services on its proposed coverage of the transcatheter aortic valve replacement procedure, makers of the SAPIEN artificial valve asked for more flexibility in the clinical trial limitations set by the agency, in an official comment they released on March 5.
Edwards Lifesciences, the manufacturer of the only valve approved for the TAVR procedure in the United States, posted its comment during the 60-day period, which began after CMS released its coverage proposal for TAVR in February.
In its proposal, CMS restricts TAVR coverage to five criteria, including the use of an approved valve, presence of multidisciplinary teams, and enrollment in a registry.
Edwards officials wrote they were pleased that CMS had proposed "clear and flexible national coverage for TAVR," and added that "for appropriately selected Medicare beneficiaries, the evidence is more than adequate for CMS to conclude that TAVR improves health outcomes and should be considered reasonable and necessary under the Medicare statute," if provided under the CMS criteria.
The Edwards SAPIEN valve is currently approved for use in inoperable patients with severe aortic stenosis. Other use of the SAPIEN valve is limited to clinical trials. In their comments, Edwards officials asked CMS for flexibility in the trials they consider for coverage determination.
"CMS’s proposed requirement limiting coverage for unlabeled uses to ‘superiority trials’ undermines the agency’s efforts to promote continued US-based clinical investigations in Medicare beneficiaries aimed at better understanding key determinants of health and quality of life outcomes," according to the Edwards’ comments.
"Noninferiority and other clinical trial designs play an important role in the advancement of medical technology," the company added, saying that if the proposed conditions aren’t revised, important, yet relatively small, patient populations may not be able to receive treatment.
Edwards, which said its transcatheter aortic valves have been implanted in more than 25,000 patients around the world, came in strong support of multidisciplinary heart teams, one of the requirements set by CMS for TAVR coverage, and strongly encouraged by leading cardiovascular organizations.
"It is imperative that at least two engaged cardiothoracic surgeons and two interventional cardiologists at each site coordinate all clinicians to form a high-functioning multi-disciplinary heart team, a key concept integral to assuring TAVR success," Edwards officials wrote in their comment.
The company also addressed credentialing, an issue which four leading cardiovascular organizations also addressed in a consensus document (see story at right).
"We support appropriate facility and heart team criteria – rather than traditional individual physician-based credentialing," to achieve TAVR success.
Following the CMS proposal, the Society of Thoracic Surgeons and the American College of Cardiology issued a statement, saying that they were pleased with CMS’s comprehensive approach to the coverage of TAVR.
CMS is expected to issue a final decision on TAVR coverage by May.
While commending the Centers for Medicare and Medicaid Services on its proposed coverage of the transcatheter aortic valve replacement procedure, makers of the SAPIEN artificial valve asked for more flexibility in the clinical trial limitations set by the agency, in an official comment they released on March 5.
Edwards Lifesciences, the manufacturer of the only valve approved for the TAVR procedure in the United States, posted its comment during the 60-day period, which began after CMS released its coverage proposal for TAVR in February.
In its proposal, CMS restricts TAVR coverage to five criteria, including the use of an approved valve, presence of multidisciplinary teams, and enrollment in a registry.
Edwards officials wrote they were pleased that CMS had proposed "clear and flexible national coverage for TAVR," and added that "for appropriately selected Medicare beneficiaries, the evidence is more than adequate for CMS to conclude that TAVR improves health outcomes and should be considered reasonable and necessary under the Medicare statute," if provided under the CMS criteria.
The Edwards SAPIEN valve is currently approved for use in inoperable patients with severe aortic stenosis. Other use of the SAPIEN valve is limited to clinical trials. In their comments, Edwards officials asked CMS for flexibility in the trials they consider for coverage determination.
"CMS’s proposed requirement limiting coverage for unlabeled uses to ‘superiority trials’ undermines the agency’s efforts to promote continued US-based clinical investigations in Medicare beneficiaries aimed at better understanding key determinants of health and quality of life outcomes," according to the Edwards’ comments.
"Noninferiority and other clinical trial designs play an important role in the advancement of medical technology," the company added, saying that if the proposed conditions aren’t revised, important, yet relatively small, patient populations may not be able to receive treatment.
Edwards, which said its transcatheter aortic valves have been implanted in more than 25,000 patients around the world, came in strong support of multidisciplinary heart teams, one of the requirements set by CMS for TAVR coverage, and strongly encouraged by leading cardiovascular organizations.
"It is imperative that at least two engaged cardiothoracic surgeons and two interventional cardiologists at each site coordinate all clinicians to form a high-functioning multi-disciplinary heart team, a key concept integral to assuring TAVR success," Edwards officials wrote in their comment.
The company also addressed credentialing, an issue which four leading cardiovascular organizations also addressed in a consensus document (see story at right).
"We support appropriate facility and heart team criteria – rather than traditional individual physician-based credentialing," to achieve TAVR success.
Following the CMS proposal, the Society of Thoracic Surgeons and the American College of Cardiology issued a statement, saying that they were pleased with CMS’s comprehensive approach to the coverage of TAVR.
CMS is expected to issue a final decision on TAVR coverage by May.
TSRA Plans Partners' Forum For AATS Annual Meeting
The Thoracic Surgery Residents Association (TSRA) has a new initiative to support the partners of thoracic surgery residents. Too often partners of trainees find they have no assistance in moving, living, and looking for a new job during the training process. Once finished, the trials, successes, and shortcuts they gained are lost as they move on to the next adventure. In addition, the training process can be a solitary one for the partner as temporary moves through new towns can lead to isolation.
Surprisingly, no one has previously studied the demographics or concerns of the partners of surgical trainees. A survey has recently been created and distributed by Dr. Rishi Reddy at the University of Michigan. The study investigates partners of applicants to traditional 2- or 3-year thoracic residency spots and current thoracic residents.
One of the initial findings of this study is that a void exists in supporting partners who are coordinating finances, child care, and housing, often while maintaining their own professional career. Partners of thoracic trainees have also voiced requests of "I just would like to talk to someone going through the same thing as I am" to "talking to someone is great, but I just need to get the kids moved to Phillie and find a new job." The results of this study are being submitted for publication.
The TSRA is creating two forums to support partners of trainees. The first event will be held on the Sunday evening of the AATS meeting in San Francisco to help bring partners together.
In addition, an online community is being created through the TSRA website to disseminate the vast information and resources partners gain during the training process with the thoracic resident. With both a regional and national presence the website will incorporate multiple social networking sites to help connect those moving, working, and raising children in a new town while their partner continues training in thoracic surgery.
Improvements in thoracic training do not end when the resident walks out of the hospital.
If you would like to comment or add to the partner website for the TSRA please write to tsra.tsn@gmail.com. The partners’ event for the AATS will be at the Pied Piper Bar (inside the Palace Hotel) from 5 to 7pm on Sunday, April 29.
The Thoracic Surgery Residents Association (TSRA) has a new initiative to support the partners of thoracic surgery residents. Too often partners of trainees find they have no assistance in moving, living, and looking for a new job during the training process. Once finished, the trials, successes, and shortcuts they gained are lost as they move on to the next adventure. In addition, the training process can be a solitary one for the partner as temporary moves through new towns can lead to isolation.
Surprisingly, no one has previously studied the demographics or concerns of the partners of surgical trainees. A survey has recently been created and distributed by Dr. Rishi Reddy at the University of Michigan. The study investigates partners of applicants to traditional 2- or 3-year thoracic residency spots and current thoracic residents.
One of the initial findings of this study is that a void exists in supporting partners who are coordinating finances, child care, and housing, often while maintaining their own professional career. Partners of thoracic trainees have also voiced requests of "I just would like to talk to someone going through the same thing as I am" to "talking to someone is great, but I just need to get the kids moved to Phillie and find a new job." The results of this study are being submitted for publication.
The TSRA is creating two forums to support partners of trainees. The first event will be held on the Sunday evening of the AATS meeting in San Francisco to help bring partners together.
In addition, an online community is being created through the TSRA website to disseminate the vast information and resources partners gain during the training process with the thoracic resident. With both a regional and national presence the website will incorporate multiple social networking sites to help connect those moving, working, and raising children in a new town while their partner continues training in thoracic surgery.
Improvements in thoracic training do not end when the resident walks out of the hospital.
If you would like to comment or add to the partner website for the TSRA please write to tsra.tsn@gmail.com. The partners’ event for the AATS will be at the Pied Piper Bar (inside the Palace Hotel) from 5 to 7pm on Sunday, April 29.
The Thoracic Surgery Residents Association (TSRA) has a new initiative to support the partners of thoracic surgery residents. Too often partners of trainees find they have no assistance in moving, living, and looking for a new job during the training process. Once finished, the trials, successes, and shortcuts they gained are lost as they move on to the next adventure. In addition, the training process can be a solitary one for the partner as temporary moves through new towns can lead to isolation.
Surprisingly, no one has previously studied the demographics or concerns of the partners of surgical trainees. A survey has recently been created and distributed by Dr. Rishi Reddy at the University of Michigan. The study investigates partners of applicants to traditional 2- or 3-year thoracic residency spots and current thoracic residents.
One of the initial findings of this study is that a void exists in supporting partners who are coordinating finances, child care, and housing, often while maintaining their own professional career. Partners of thoracic trainees have also voiced requests of "I just would like to talk to someone going through the same thing as I am" to "talking to someone is great, but I just need to get the kids moved to Phillie and find a new job." The results of this study are being submitted for publication.
The TSRA is creating two forums to support partners of trainees. The first event will be held on the Sunday evening of the AATS meeting in San Francisco to help bring partners together.
In addition, an online community is being created through the TSRA website to disseminate the vast information and resources partners gain during the training process with the thoracic resident. With both a regional and national presence the website will incorporate multiple social networking sites to help connect those moving, working, and raising children in a new town while their partner continues training in thoracic surgery.
Improvements in thoracic training do not end when the resident walks out of the hospital.
If you would like to comment or add to the partner website for the TSRA please write to tsra.tsn@gmail.com. The partners’ event for the AATS will be at the Pied Piper Bar (inside the Palace Hotel) from 5 to 7pm on Sunday, April 29.
Diagnostic Concerns in Staging With EBUS-FNA
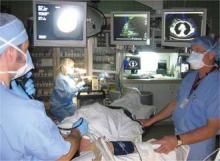
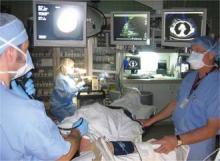
FT. LAUDERDALE, FLA. – Appropriate staging of non–small cell lung cancer (NSCLC) is critical to patient treatment and prognosis. Endobronchial ultrasound–guided fine-needle aspiration (EBUS-FNA) has gradually gained acceptance as a diagnostic tool to pathologically stage the mediastinum in patients with NSCLC, according to Dr. Bryan A. Whitson at the annual meeting of the Society of Thoracic Surgeons.
Because EBUS-FNA is a test to detect cancer, it is critical that it have few false-negative results, i.e., have a high negative predictive value (NPV). However, by virtue of the size and volume of mediastinal lymph node FNA samples, nondiagnostic results occur with some frequency.
Nondiagnostic samples decrease a test’s diagnostic performance, since they cannot help guide a clinical decision, and a portion of these samples may actually be false negatives.
The standard calculation of NPV does not factor in nondiagnostic samples. According to a study by the researchers in the Division of Thoracic and Foregut Surgery at the University of Minnesota, which Dr. Whitson presented, one must take nondiagnostic samples into consideration to determine the true diagnostic performance of EBUS-FNA.
To conservatively calculate NPV, the researchers modified the standard definition (true negatives/[true negatives plus false negatives]), creating an alternative NPV definition (true negatives/[true negatives plus false negatives plus nondiagnostic]). This definition takes into account the possibility that these nondiagnostic samples may be false negatives, which assumes the worst-case scenario.
The thoracic team at the University of Minnesota then compared the results of these two definitions of NPV in a retrospective analysis of their prospective database of patients with NSCLC who had EBUS-FNA between January 2007 and July 2011.
Dr. Bryan Whitson, who is a surgeon at the University of Minnesota, presented the team’s results.
A total of 120 patients with NSCLC who underwent EBUS-FNA were included in the analsyis. EBUS-FNAs were assessed using rapid on-site cytologic evaluation (ROSE) and a false-negative definition consisting of negative FNAs coupled to NSCLC-positive surgical biopsy of the same site. Diagnostic performance was evaluated comparing results of the inclusion or exclusion of nondiagnostic samples in the calculation of NPV.
Seven (5.8%) of the 120 patients had nondiagnostic results. One patient had a false negative. When the seven nondiagnostic procedures were excluded, the NPV was 96.3%; when they were included, the NPV dropped to 76.5%.
Both sensitivity and accuracy also dropped with the inclusion of the nondiagnostic procedures. Sensitivity dropped from 98.8% to 91% and overall accuracy from 98.2% to 92.2% when nondiagnostic procedures were included.
"Our data indicate that a conservative calculation of NPV that includes nondiagnostic samples should be used to assess the real diagnostic accuracy of EBUS-FNA in patients with NSCLC. Otherwise, decisions based on these results could be flawed and patients inappropriately staged. In our experience, and using this assessment, EBUS-FNA shows a true NPV that is less than most clinicians assume," Dr. Whitson said.
Ultimately, the thoracic surgeons at the University of Minnesota believe that "EBUS-FNA should be the primary method to stage the mediastinum in patients with NSCLC, since it enables pathologic staging without the need for an incision, with preservation of tissue planes, and with minimal complications."
However, in view of the limitations of EBUS-FNA, "we perform an immediate surgical biopsy when in doubt of the reliability of an EBUS-FNA result. A thoracic surgeon facile in EBUS can offer most patients minimally invasive mediastinal staging, with selective surgical biopsy in the same anesthetic setting, which can ensure accuracy and streamline patient care," according to Dr. Whitson and his colleagues.
FT. LAUDERDALE, FLA. – Appropriate staging of non–small cell lung cancer (NSCLC) is critical to patient treatment and prognosis. Endobronchial ultrasound–guided fine-needle aspiration (EBUS-FNA) has gradually gained acceptance as a diagnostic tool to pathologically stage the mediastinum in patients with NSCLC, according to Dr. Bryan A. Whitson at the annual meeting of the Society of Thoracic Surgeons.
Because EBUS-FNA is a test to detect cancer, it is critical that it have few false-negative results, i.e., have a high negative predictive value (NPV). However, by virtue of the size and volume of mediastinal lymph node FNA samples, nondiagnostic results occur with some frequency.
Nondiagnostic samples decrease a test’s diagnostic performance, since they cannot help guide a clinical decision, and a portion of these samples may actually be false negatives.
The standard calculation of NPV does not factor in nondiagnostic samples. According to a study by the researchers in the Division of Thoracic and Foregut Surgery at the University of Minnesota, which Dr. Whitson presented, one must take nondiagnostic samples into consideration to determine the true diagnostic performance of EBUS-FNA.
To conservatively calculate NPV, the researchers modified the standard definition (true negatives/[true negatives plus false negatives]), creating an alternative NPV definition (true negatives/[true negatives plus false negatives plus nondiagnostic]). This definition takes into account the possibility that these nondiagnostic samples may be false negatives, which assumes the worst-case scenario.
The thoracic team at the University of Minnesota then compared the results of these two definitions of NPV in a retrospective analysis of their prospective database of patients with NSCLC who had EBUS-FNA between January 2007 and July 2011.
Dr. Bryan Whitson, who is a surgeon at the University of Minnesota, presented the team’s results.
A total of 120 patients with NSCLC who underwent EBUS-FNA were included in the analsyis. EBUS-FNAs were assessed using rapid on-site cytologic evaluation (ROSE) and a false-negative definition consisting of negative FNAs coupled to NSCLC-positive surgical biopsy of the same site. Diagnostic performance was evaluated comparing results of the inclusion or exclusion of nondiagnostic samples in the calculation of NPV.
Seven (5.8%) of the 120 patients had nondiagnostic results. One patient had a false negative. When the seven nondiagnostic procedures were excluded, the NPV was 96.3%; when they were included, the NPV dropped to 76.5%.
Both sensitivity and accuracy also dropped with the inclusion of the nondiagnostic procedures. Sensitivity dropped from 98.8% to 91% and overall accuracy from 98.2% to 92.2% when nondiagnostic procedures were included.
"Our data indicate that a conservative calculation of NPV that includes nondiagnostic samples should be used to assess the real diagnostic accuracy of EBUS-FNA in patients with NSCLC. Otherwise, decisions based on these results could be flawed and patients inappropriately staged. In our experience, and using this assessment, EBUS-FNA shows a true NPV that is less than most clinicians assume," Dr. Whitson said.
Ultimately, the thoracic surgeons at the University of Minnesota believe that "EBUS-FNA should be the primary method to stage the mediastinum in patients with NSCLC, since it enables pathologic staging without the need for an incision, with preservation of tissue planes, and with minimal complications."
However, in view of the limitations of EBUS-FNA, "we perform an immediate surgical biopsy when in doubt of the reliability of an EBUS-FNA result. A thoracic surgeon facile in EBUS can offer most patients minimally invasive mediastinal staging, with selective surgical biopsy in the same anesthetic setting, which can ensure accuracy and streamline patient care," according to Dr. Whitson and his colleagues.
FT. LAUDERDALE, FLA. – Appropriate staging of non–small cell lung cancer (NSCLC) is critical to patient treatment and prognosis. Endobronchial ultrasound–guided fine-needle aspiration (EBUS-FNA) has gradually gained acceptance as a diagnostic tool to pathologically stage the mediastinum in patients with NSCLC, according to Dr. Bryan A. Whitson at the annual meeting of the Society of Thoracic Surgeons.
Because EBUS-FNA is a test to detect cancer, it is critical that it have few false-negative results, i.e., have a high negative predictive value (NPV). However, by virtue of the size and volume of mediastinal lymph node FNA samples, nondiagnostic results occur with some frequency.
Nondiagnostic samples decrease a test’s diagnostic performance, since they cannot help guide a clinical decision, and a portion of these samples may actually be false negatives.
The standard calculation of NPV does not factor in nondiagnostic samples. According to a study by the researchers in the Division of Thoracic and Foregut Surgery at the University of Minnesota, which Dr. Whitson presented, one must take nondiagnostic samples into consideration to determine the true diagnostic performance of EBUS-FNA.
To conservatively calculate NPV, the researchers modified the standard definition (true negatives/[true negatives plus false negatives]), creating an alternative NPV definition (true negatives/[true negatives plus false negatives plus nondiagnostic]). This definition takes into account the possibility that these nondiagnostic samples may be false negatives, which assumes the worst-case scenario.
The thoracic team at the University of Minnesota then compared the results of these two definitions of NPV in a retrospective analysis of their prospective database of patients with NSCLC who had EBUS-FNA between January 2007 and July 2011.
Dr. Bryan Whitson, who is a surgeon at the University of Minnesota, presented the team’s results.
A total of 120 patients with NSCLC who underwent EBUS-FNA were included in the analsyis. EBUS-FNAs were assessed using rapid on-site cytologic evaluation (ROSE) and a false-negative definition consisting of negative FNAs coupled to NSCLC-positive surgical biopsy of the same site. Diagnostic performance was evaluated comparing results of the inclusion or exclusion of nondiagnostic samples in the calculation of NPV.
Seven (5.8%) of the 120 patients had nondiagnostic results. One patient had a false negative. When the seven nondiagnostic procedures were excluded, the NPV was 96.3%; when they were included, the NPV dropped to 76.5%.
Both sensitivity and accuracy also dropped with the inclusion of the nondiagnostic procedures. Sensitivity dropped from 98.8% to 91% and overall accuracy from 98.2% to 92.2% when nondiagnostic procedures were included.
"Our data indicate that a conservative calculation of NPV that includes nondiagnostic samples should be used to assess the real diagnostic accuracy of EBUS-FNA in patients with NSCLC. Otherwise, decisions based on these results could be flawed and patients inappropriately staged. In our experience, and using this assessment, EBUS-FNA shows a true NPV that is less than most clinicians assume," Dr. Whitson said.
Ultimately, the thoracic surgeons at the University of Minnesota believe that "EBUS-FNA should be the primary method to stage the mediastinum in patients with NSCLC, since it enables pathologic staging without the need for an incision, with preservation of tissue planes, and with minimal complications."
However, in view of the limitations of EBUS-FNA, "we perform an immediate surgical biopsy when in doubt of the reliability of an EBUS-FNA result. A thoracic surgeon facile in EBUS can offer most patients minimally invasive mediastinal staging, with selective surgical biopsy in the same anesthetic setting, which can ensure accuracy and streamline patient care," according to Dr. Whitson and his colleagues.
Diagnostic Concerns in Staging With EBUS-FNA
FT. LAUDERDALE, FLA. – Appropriate staging of non–small cell lung cancer (NSCLC) is critical to patient treatment and prognosis. Endobronchial ultrasound–guided fine-needle aspiration (EBUS-FNA) has gradually gained acceptance as a diagnostic tool to pathologically stage the mediastinum in patients with NSCLC, according to Dr. Bryan A. Whitson at the annual meeting of the Society of Thoracic Surgeons.
Because EBUS-FNA is a test to detect cancer, it is critical that it have few false-negative results, i.e., have a high negative predictive value (NPV). However, by virtue of the size and volume of mediastinal lymph node FNA samples, nondiagnostic results occur with some frequency.
Nondiagnostic samples decrease a test’s diagnostic performance, since they cannot help guide a clinical decision, and a portion of these samples may actually be false negatives.
The standard calculation of NPV does not factor in nondiagnostic samples. According to a study by the researchers in the Division of Thoracic and Foregut Surgery at the University of Minnesota, which Dr. Whitson presented, one must take nondiagnostic samples into consideration to determine the true diagnostic performance of EBUS-FNA.
To conservatively calculate NPV, the researchers modified the standard definition (true negatives/[true negatives plus false negatives]), creating an alternative NPV definition (true negatives/[true negatives plus false negatives plus nondiagnostic]). This definition takes into account the possibility that these nondiagnostic samples may be false negatives, which assumes the worst-case scenario.
The thoracic team at the University of Minnesota then compared the results of these two definitions of NPV in a retrospective analysis of their prospective database of patients with NSCLC who had EBUS-FNA between January 2007 and July 2011.
Dr. Bryan Whitson, who is a surgeon at the University of Minnesota, presented the team’s results.
A total of 120 patients with NSCLC who underwent EBUS-FNA were included in the analsyis. EBUS-FNAs were assessed using rapid on-site cytologic evaluation (ROSE) and a false-negative definition consisting of negative FNAs coupled to NSCLC-positive surgical biopsy of the same site. Diagnostic performance was evaluated comparing results of the inclusion or exclusion of nondiagnostic samples in the calculation of NPV.
Seven (5.8%) of the 120 patients had nondiagnostic results. One patient had a false negative. When the seven nondiagnostic procedures were excluded, the NPV was 96.3%; when they were included, the NPV dropped to 76.5%.
Both sensitivity and accuracy also dropped with the inclusion of the nondiagnostic procedures. Sensitivity dropped from 98.8% to 91% and overall accuracy from 98.2% to 92.2% when nondiagnostic procedures were included.
"Our data indicate that a conservative calculation of NPV that includes nondiagnostic samples should be used to assess the real diagnostic accuracy of EBUS-FNA in patients with NSCLC. Otherwise, decisions based on these results could be flawed and patients inappropriately staged. In our experience, and using this assessment, EBUS-FNA shows a true NPV that is less than most clinicians assume," Dr. Whitson said.
Ultimately, the thoracic surgeons at the University of Minnesota believe that "EBUS-FNA should be the primary method to stage the mediastinum in patients with NSCLC, since it enables pathologic staging without the need for an incision, with preservation of tissue planes, and with minimal complications."
However, in view of the limitations of EBUS-FNA, "we perform an immediate surgical biopsy when in doubt of the reliability of an EBUS-FNA result. A thoracic surgeon facile in EBUS can offer most patients minimally invasive mediastinal staging, with selective surgical biopsy in the same anesthetic setting, which can ensure accuracy and streamline patient care," according to Dr. Whitson and his colleagues.
FT. LAUDERDALE, FLA. – Appropriate staging of non–small cell lung cancer (NSCLC) is critical to patient treatment and prognosis. Endobronchial ultrasound–guided fine-needle aspiration (EBUS-FNA) has gradually gained acceptance as a diagnostic tool to pathologically stage the mediastinum in patients with NSCLC, according to Dr. Bryan A. Whitson at the annual meeting of the Society of Thoracic Surgeons.
Because EBUS-FNA is a test to detect cancer, it is critical that it have few false-negative results, i.e., have a high negative predictive value (NPV). However, by virtue of the size and volume of mediastinal lymph node FNA samples, nondiagnostic results occur with some frequency.
Nondiagnostic samples decrease a test’s diagnostic performance, since they cannot help guide a clinical decision, and a portion of these samples may actually be false negatives.
The standard calculation of NPV does not factor in nondiagnostic samples. According to a study by the researchers in the Division of Thoracic and Foregut Surgery at the University of Minnesota, which Dr. Whitson presented, one must take nondiagnostic samples into consideration to determine the true diagnostic performance of EBUS-FNA.
To conservatively calculate NPV, the researchers modified the standard definition (true negatives/[true negatives plus false negatives]), creating an alternative NPV definition (true negatives/[true negatives plus false negatives plus nondiagnostic]). This definition takes into account the possibility that these nondiagnostic samples may be false negatives, which assumes the worst-case scenario.
The thoracic team at the University of Minnesota then compared the results of these two definitions of NPV in a retrospective analysis of their prospective database of patients with NSCLC who had EBUS-FNA between January 2007 and July 2011.
Dr. Bryan Whitson, who is a surgeon at the University of Minnesota, presented the team’s results.
A total of 120 patients with NSCLC who underwent EBUS-FNA were included in the analsyis. EBUS-FNAs were assessed using rapid on-site cytologic evaluation (ROSE) and a false-negative definition consisting of negative FNAs coupled to NSCLC-positive surgical biopsy of the same site. Diagnostic performance was evaluated comparing results of the inclusion or exclusion of nondiagnostic samples in the calculation of NPV.
Seven (5.8%) of the 120 patients had nondiagnostic results. One patient had a false negative. When the seven nondiagnostic procedures were excluded, the NPV was 96.3%; when they were included, the NPV dropped to 76.5%.
Both sensitivity and accuracy also dropped with the inclusion of the nondiagnostic procedures. Sensitivity dropped from 98.8% to 91% and overall accuracy from 98.2% to 92.2% when nondiagnostic procedures were included.
"Our data indicate that a conservative calculation of NPV that includes nondiagnostic samples should be used to assess the real diagnostic accuracy of EBUS-FNA in patients with NSCLC. Otherwise, decisions based on these results could be flawed and patients inappropriately staged. In our experience, and using this assessment, EBUS-FNA shows a true NPV that is less than most clinicians assume," Dr. Whitson said.
Ultimately, the thoracic surgeons at the University of Minnesota believe that "EBUS-FNA should be the primary method to stage the mediastinum in patients with NSCLC, since it enables pathologic staging without the need for an incision, with preservation of tissue planes, and with minimal complications."
However, in view of the limitations of EBUS-FNA, "we perform an immediate surgical biopsy when in doubt of the reliability of an EBUS-FNA result. A thoracic surgeon facile in EBUS can offer most patients minimally invasive mediastinal staging, with selective surgical biopsy in the same anesthetic setting, which can ensure accuracy and streamline patient care," according to Dr. Whitson and his colleagues.
FT. LAUDERDALE, FLA. – Appropriate staging of non–small cell lung cancer (NSCLC) is critical to patient treatment and prognosis. Endobronchial ultrasound–guided fine-needle aspiration (EBUS-FNA) has gradually gained acceptance as a diagnostic tool to pathologically stage the mediastinum in patients with NSCLC, according to Dr. Bryan A. Whitson at the annual meeting of the Society of Thoracic Surgeons.
Because EBUS-FNA is a test to detect cancer, it is critical that it have few false-negative results, i.e., have a high negative predictive value (NPV). However, by virtue of the size and volume of mediastinal lymph node FNA samples, nondiagnostic results occur with some frequency.
Nondiagnostic samples decrease a test’s diagnostic performance, since they cannot help guide a clinical decision, and a portion of these samples may actually be false negatives.
The standard calculation of NPV does not factor in nondiagnostic samples. According to a study by the researchers in the Division of Thoracic and Foregut Surgery at the University of Minnesota, which Dr. Whitson presented, one must take nondiagnostic samples into consideration to determine the true diagnostic performance of EBUS-FNA.
To conservatively calculate NPV, the researchers modified the standard definition (true negatives/[true negatives plus false negatives]), creating an alternative NPV definition (true negatives/[true negatives plus false negatives plus nondiagnostic]). This definition takes into account the possibility that these nondiagnostic samples may be false negatives, which assumes the worst-case scenario.
The thoracic team at the University of Minnesota then compared the results of these two definitions of NPV in a retrospective analysis of their prospective database of patients with NSCLC who had EBUS-FNA between January 2007 and July 2011.
Dr. Bryan Whitson, who is a surgeon at the University of Minnesota, presented the team’s results.
A total of 120 patients with NSCLC who underwent EBUS-FNA were included in the analsyis. EBUS-FNAs were assessed using rapid on-site cytologic evaluation (ROSE) and a false-negative definition consisting of negative FNAs coupled to NSCLC-positive surgical biopsy of the same site. Diagnostic performance was evaluated comparing results of the inclusion or exclusion of nondiagnostic samples in the calculation of NPV.
Seven (5.8%) of the 120 patients had nondiagnostic results. One patient had a false negative. When the seven nondiagnostic procedures were excluded, the NPV was 96.3%; when they were included, the NPV dropped to 76.5%.
Both sensitivity and accuracy also dropped with the inclusion of the nondiagnostic procedures. Sensitivity dropped from 98.8% to 91% and overall accuracy from 98.2% to 92.2% when nondiagnostic procedures were included.
"Our data indicate that a conservative calculation of NPV that includes nondiagnostic samples should be used to assess the real diagnostic accuracy of EBUS-FNA in patients with NSCLC. Otherwise, decisions based on these results could be flawed and patients inappropriately staged. In our experience, and using this assessment, EBUS-FNA shows a true NPV that is less than most clinicians assume," Dr. Whitson said.
Ultimately, the thoracic surgeons at the University of Minnesota believe that "EBUS-FNA should be the primary method to stage the mediastinum in patients with NSCLC, since it enables pathologic staging without the need for an incision, with preservation of tissue planes, and with minimal complications."
However, in view of the limitations of EBUS-FNA, "we perform an immediate surgical biopsy when in doubt of the reliability of an EBUS-FNA result. A thoracic surgeon facile in EBUS can offer most patients minimally invasive mediastinal staging, with selective surgical biopsy in the same anesthetic setting, which can ensure accuracy and streamline patient care," according to Dr. Whitson and his colleagues.
More NSCLC Upstaging Seen With Thoracotomy
FT. LAUDERDALE, FLA. – Pretreatment staging of presumed N0 non–small cell lung cancer (NSCLC) misses unsuspected lymph node metastases that are subsequently discovered during surgical specimen evaluation in 10%-25% of cases. Thus it is critically important that surgical node dissection be done sufficiently completely to capture these misses, providing the appropriate upstaging for treatment decisions.
With the increasing movement to video-assisted thoracic surgery (VATS) approaches to lobectomy and segmentectomy, it is important to evaluate the comparative efficiency of VATS vs. thoracotomy (Open) in capturing this upstaging.
To this end, an examination of the Society of Thoracic Surgeons (STS) General Thoracic Database was performed to determine the frequency of nodal metastases identified in clinically node-negative tumors by Open and VATS approaches to compare completeness of surgical nodal dissections, according to Dr. Daniel J. Boffa.
A total of 11,531 clinical stage I primary lung cancers resected from 2001 to 2010 were analyzed from the STS General Thoracic Database. These comprised 7,137 Open and 4,394 VATS procedures.
The researchers found significantly greater nodal upstaging in the Open groups (14.3%) as compared with the VATS group (11.6%).
Dr. Boffa stated that this was primarily due to the significantly greater upstaging from N0 to N1 that was seen in the Open (9.8%) versus the VATS group (7.0%). In contrast, upstaging from N0 to N2 was found to be similar in both groups (5.5% Open vs. 5.2% VATS, a non-significant difference).
Dr. Boffa presented this research at the annual meeting of the Society of Thoracic Surgeons.
When a multivariate analysis controlling for T status, laterality, body mass index, age, and sex was performed, N0 to N1 upstaging remained significantly less common with VATS than with Open surgery.
In a separate analysis, pathologic confirmation of clinical N1 also occurred significantly less often in the VATS group (42%) as compared with the Open group (54%), according to Dr. Boffa, who is an assistant professor of surgery at the Yale School of Medicine, New Haven, Conn.
"Mediastinal nodal evaluation by VATS and thoracotomy results in equivalent upstaging. However, lower rates of N1 upstaging and stage confirmation in the VATS group may indicate variability in the completeness of the peribronchial and hilar lymph node evaluation," according to Dr. Boffa.
"Systematic hilar dissection is encouraged, particularly as more surgeons adopt the VATS approach," he concluded, reiterating the importance of appropriate staging in the planning of patient treatment.
Dr. Boffa presented his research as one of the Richard E. Clark database papers during the STS annual meeting.
Dr. Boffa reported that he had no relevant conflicts of interest.
FT. LAUDERDALE, FLA. – Pretreatment staging of presumed N0 non–small cell lung cancer (NSCLC) misses unsuspected lymph node metastases that are subsequently discovered during surgical specimen evaluation in 10%-25% of cases. Thus it is critically important that surgical node dissection be done sufficiently completely to capture these misses, providing the appropriate upstaging for treatment decisions.
With the increasing movement to video-assisted thoracic surgery (VATS) approaches to lobectomy and segmentectomy, it is important to evaluate the comparative efficiency of VATS vs. thoracotomy (Open) in capturing this upstaging.
To this end, an examination of the Society of Thoracic Surgeons (STS) General Thoracic Database was performed to determine the frequency of nodal metastases identified in clinically node-negative tumors by Open and VATS approaches to compare completeness of surgical nodal dissections, according to Dr. Daniel J. Boffa.
A total of 11,531 clinical stage I primary lung cancers resected from 2001 to 2010 were analyzed from the STS General Thoracic Database. These comprised 7,137 Open and 4,394 VATS procedures.
The researchers found significantly greater nodal upstaging in the Open groups (14.3%) as compared with the VATS group (11.6%).
Dr. Boffa stated that this was primarily due to the significantly greater upstaging from N0 to N1 that was seen in the Open (9.8%) versus the VATS group (7.0%). In contrast, upstaging from N0 to N2 was found to be similar in both groups (5.5% Open vs. 5.2% VATS, a non-significant difference).
Dr. Boffa presented this research at the annual meeting of the Society of Thoracic Surgeons.
When a multivariate analysis controlling for T status, laterality, body mass index, age, and sex was performed, N0 to N1 upstaging remained significantly less common with VATS than with Open surgery.
In a separate analysis, pathologic confirmation of clinical N1 also occurred significantly less often in the VATS group (42%) as compared with the Open group (54%), according to Dr. Boffa, who is an assistant professor of surgery at the Yale School of Medicine, New Haven, Conn.
"Mediastinal nodal evaluation by VATS and thoracotomy results in equivalent upstaging. However, lower rates of N1 upstaging and stage confirmation in the VATS group may indicate variability in the completeness of the peribronchial and hilar lymph node evaluation," according to Dr. Boffa.
"Systematic hilar dissection is encouraged, particularly as more surgeons adopt the VATS approach," he concluded, reiterating the importance of appropriate staging in the planning of patient treatment.
Dr. Boffa presented his research as one of the Richard E. Clark database papers during the STS annual meeting.
Dr. Boffa reported that he had no relevant conflicts of interest.
FT. LAUDERDALE, FLA. – Pretreatment staging of presumed N0 non–small cell lung cancer (NSCLC) misses unsuspected lymph node metastases that are subsequently discovered during surgical specimen evaluation in 10%-25% of cases. Thus it is critically important that surgical node dissection be done sufficiently completely to capture these misses, providing the appropriate upstaging for treatment decisions.
With the increasing movement to video-assisted thoracic surgery (VATS) approaches to lobectomy and segmentectomy, it is important to evaluate the comparative efficiency of VATS vs. thoracotomy (Open) in capturing this upstaging.
To this end, an examination of the Society of Thoracic Surgeons (STS) General Thoracic Database was performed to determine the frequency of nodal metastases identified in clinically node-negative tumors by Open and VATS approaches to compare completeness of surgical nodal dissections, according to Dr. Daniel J. Boffa.
A total of 11,531 clinical stage I primary lung cancers resected from 2001 to 2010 were analyzed from the STS General Thoracic Database. These comprised 7,137 Open and 4,394 VATS procedures.
The researchers found significantly greater nodal upstaging in the Open groups (14.3%) as compared with the VATS group (11.6%).
Dr. Boffa stated that this was primarily due to the significantly greater upstaging from N0 to N1 that was seen in the Open (9.8%) versus the VATS group (7.0%). In contrast, upstaging from N0 to N2 was found to be similar in both groups (5.5% Open vs. 5.2% VATS, a non-significant difference).
Dr. Boffa presented this research at the annual meeting of the Society of Thoracic Surgeons.
When a multivariate analysis controlling for T status, laterality, body mass index, age, and sex was performed, N0 to N1 upstaging remained significantly less common with VATS than with Open surgery.
In a separate analysis, pathologic confirmation of clinical N1 also occurred significantly less often in the VATS group (42%) as compared with the Open group (54%), according to Dr. Boffa, who is an assistant professor of surgery at the Yale School of Medicine, New Haven, Conn.
"Mediastinal nodal evaluation by VATS and thoracotomy results in equivalent upstaging. However, lower rates of N1 upstaging and stage confirmation in the VATS group may indicate variability in the completeness of the peribronchial and hilar lymph node evaluation," according to Dr. Boffa.
"Systematic hilar dissection is encouraged, particularly as more surgeons adopt the VATS approach," he concluded, reiterating the importance of appropriate staging in the planning of patient treatment.
Dr. Boffa presented his research as one of the Richard E. Clark database papers during the STS annual meeting.
Dr. Boffa reported that he had no relevant conflicts of interest.
More NSCLC Upstaging Seen With Thoracotomy
FT. LAUDERDALE, FLA. – Pretreatment staging of presumed N0 non–small cell lung cancer (NSCLC) misses unsuspected lymph node metastases that are subsequently discovered during surgical specimen evaluation in 10%-25% of cases. Thus it is critically important that surgical node dissection be done sufficiently completely to capture these misses, providing the appropriate upstaging for treatment decisions.
With the increasing movement to video-assisted thoracic surgery (VATS) approaches to lobectomy and segmentectomy, it is important to evaluate the comparative efficiency of VATS vs. thoracotomy (Open) in capturing this upstaging.
To this end, an examination of the Society of Thoracic Surgeons (STS) General Thoracic Database was performed to determine the frequency of nodal metastases identified in clinically node-negative tumors by Open and VATS approaches to compare completeness of surgical nodal dissections, according to Dr. Daniel J. Boffa.
A total of 11,531 clinical stage I primary lung cancers resected from 2001 to 2010 were analyzed from the STS General Thoracic Database. These comprised 7,137 Open and 4,394 VATS procedures.
The researchers found significantly greater nodal upstaging in the Open groups (14.3%) as compared with the VATS group (11.6%).
Dr. Boffa stated that this was primarily due to the significantly greater upstaging from N0 to N1 that was seen in the Open (9.8%) versus the VATS group (7.0%). In contrast, upstaging from N0 to N2 was found to be similar in both groups (5.5% Open vs. 5.2% VATS, a non-significant difference).
Dr. Boffa presented this research at the annual meeting of the Society of Thoracic Surgeons.
When a multivariate analysis controlling for T status, laterality, body mass index, age, and sex was performed, N0 to N1 upstaging remained significantly less common with VATS than with Open surgery.
In a separate analysis, pathologic confirmation of clinical N1 also occurred significantly less often in the VATS group (42%) as compared with the Open group (54%), according to Dr. Boffa, who is an assistant professor of surgery at the Yale School of Medicine, New Haven, Conn.
"Mediastinal nodal evaluation by VATS and thoracotomy results in equivalent upstaging. However, lower rates of N1 upstaging and stage confirmation in the VATS group may indicate variability in the completeness of the peribronchial and hilar lymph node evaluation," according to Dr. Boffa.
"Systematic hilar dissection is encouraged, particularly as more surgeons adopt the VATS approach," he concluded, reiterating the importance of appropriate staging in the planning of patient treatment.
Dr. Boffa presented his research as one of the Richard E. Clark database papers during the STS annual meeting.
Dr. Boffa reported that he had no relevant conflicts of interest.
FT. LAUDERDALE, FLA. – Pretreatment staging of presumed N0 non–small cell lung cancer (NSCLC) misses unsuspected lymph node metastases that are subsequently discovered during surgical specimen evaluation in 10%-25% of cases. Thus it is critically important that surgical node dissection be done sufficiently completely to capture these misses, providing the appropriate upstaging for treatment decisions.
With the increasing movement to video-assisted thoracic surgery (VATS) approaches to lobectomy and segmentectomy, it is important to evaluate the comparative efficiency of VATS vs. thoracotomy (Open) in capturing this upstaging.
To this end, an examination of the Society of Thoracic Surgeons (STS) General Thoracic Database was performed to determine the frequency of nodal metastases identified in clinically node-negative tumors by Open and VATS approaches to compare completeness of surgical nodal dissections, according to Dr. Daniel J. Boffa.
A total of 11,531 clinical stage I primary lung cancers resected from 2001 to 2010 were analyzed from the STS General Thoracic Database. These comprised 7,137 Open and 4,394 VATS procedures.
The researchers found significantly greater nodal upstaging in the Open groups (14.3%) as compared with the VATS group (11.6%).
Dr. Boffa stated that this was primarily due to the significantly greater upstaging from N0 to N1 that was seen in the Open (9.8%) versus the VATS group (7.0%). In contrast, upstaging from N0 to N2 was found to be similar in both groups (5.5% Open vs. 5.2% VATS, a non-significant difference).
Dr. Boffa presented this research at the annual meeting of the Society of Thoracic Surgeons.
When a multivariate analysis controlling for T status, laterality, body mass index, age, and sex was performed, N0 to N1 upstaging remained significantly less common with VATS than with Open surgery.
In a separate analysis, pathologic confirmation of clinical N1 also occurred significantly less often in the VATS group (42%) as compared with the Open group (54%), according to Dr. Boffa, who is an assistant professor of surgery at the Yale School of Medicine, New Haven, Conn.
"Mediastinal nodal evaluation by VATS and thoracotomy results in equivalent upstaging. However, lower rates of N1 upstaging and stage confirmation in the VATS group may indicate variability in the completeness of the peribronchial and hilar lymph node evaluation," according to Dr. Boffa.
"Systematic hilar dissection is encouraged, particularly as more surgeons adopt the VATS approach," he concluded, reiterating the importance of appropriate staging in the planning of patient treatment.
Dr. Boffa presented his research as one of the Richard E. Clark database papers during the STS annual meeting.
Dr. Boffa reported that he had no relevant conflicts of interest.
FT. LAUDERDALE, FLA. – Pretreatment staging of presumed N0 non–small cell lung cancer (NSCLC) misses unsuspected lymph node metastases that are subsequently discovered during surgical specimen evaluation in 10%-25% of cases. Thus it is critically important that surgical node dissection be done sufficiently completely to capture these misses, providing the appropriate upstaging for treatment decisions.
With the increasing movement to video-assisted thoracic surgery (VATS) approaches to lobectomy and segmentectomy, it is important to evaluate the comparative efficiency of VATS vs. thoracotomy (Open) in capturing this upstaging.
To this end, an examination of the Society of Thoracic Surgeons (STS) General Thoracic Database was performed to determine the frequency of nodal metastases identified in clinically node-negative tumors by Open and VATS approaches to compare completeness of surgical nodal dissections, according to Dr. Daniel J. Boffa.
A total of 11,531 clinical stage I primary lung cancers resected from 2001 to 2010 were analyzed from the STS General Thoracic Database. These comprised 7,137 Open and 4,394 VATS procedures.
The researchers found significantly greater nodal upstaging in the Open groups (14.3%) as compared with the VATS group (11.6%).
Dr. Boffa stated that this was primarily due to the significantly greater upstaging from N0 to N1 that was seen in the Open (9.8%) versus the VATS group (7.0%). In contrast, upstaging from N0 to N2 was found to be similar in both groups (5.5% Open vs. 5.2% VATS, a non-significant difference).
Dr. Boffa presented this research at the annual meeting of the Society of Thoracic Surgeons.
When a multivariate analysis controlling for T status, laterality, body mass index, age, and sex was performed, N0 to N1 upstaging remained significantly less common with VATS than with Open surgery.
In a separate analysis, pathologic confirmation of clinical N1 also occurred significantly less often in the VATS group (42%) as compared with the Open group (54%), according to Dr. Boffa, who is an assistant professor of surgery at the Yale School of Medicine, New Haven, Conn.
"Mediastinal nodal evaluation by VATS and thoracotomy results in equivalent upstaging. However, lower rates of N1 upstaging and stage confirmation in the VATS group may indicate variability in the completeness of the peribronchial and hilar lymph node evaluation," according to Dr. Boffa.
"Systematic hilar dissection is encouraged, particularly as more surgeons adopt the VATS approach," he concluded, reiterating the importance of appropriate staging in the planning of patient treatment.
Dr. Boffa presented his research as one of the Richard E. Clark database papers during the STS annual meeting.
Dr. Boffa reported that he had no relevant conflicts of interest.
Survey: Women CT Surgeons Report Job Satisfaction
Women represent a minority of cardiothoracic surgeons in the United States, with roughly equal numbers being found in academic and private practice, according to a recent survey presented at the annual meeting of the Society for Thoracic Surgeons.
Overall, these women reported a high level of job satisfaction and the vast majority of them were still in practice.
Although there were comparatively few women in senior staff and faculty positions, in part because over 50% of women currently in practice entered the profession since the year 2000, "this exponential increase in the number of women in the field over the past ten years provides optimism for a continued recruitment," according to the report by Dr. Jessica S. Donington, assistant professor of cardiothoracic surgery at New York University, New York, N.Y.,and her colleagues on behalf of The Women in Thoracic Surgery (WTS).
The WTS was established as a professional organization in 1986, with the designated mission of providing mutual support and facilitating the professional advancement of women in cardiothoracic surgery.
With 2011 being the 50th anniversary of the first certification of a woman by the American Board of Thoracic Surgery (ABTS) and the year in which the 200th female was certified by the ABTS, the WTS deemed it important to survey the status of female cardiothoracic surgeons in the United States.
The WTS survey was designed to measure career progression and to provide insights in order to improve recruitment. All ABTS-certified women were surveyed anonymously in December 2010 using tools from surveymonkey.com, according to Dr. Donington.
Contact information was obtained from CTSNet, Google, and institutions of known employment.
Of the 204 living women with ABTS certification, 190 were contacted. Of these, 64% responded to the survey. The questions comprised five areas: demographics, training, practice activities, activities of non-practicing CT surgeons, and career satisfaction.
The researchers grouped the respondents by year of certification: Group 1 (1961-1999) and Group 2 (2000-2010). They used the STS/AATS 2009 practice survey of the entire thoracic surgery workforce in order to make broad-based comparisons.
The mean age of the women respondents was 48 years, with the majority being white (nearly 78%) and urban dwellers (61%).
Half of the women were certified within the past 10 years. Overall, the respondents had been practicing for a mean of 8 years, worked in groups of 2-10 surgeons, and were the only female surgeon in their group. The respondents had a mean of 9.1 years of training with 56% reporting non-Accreditation Council for Graduate Medical Education (ACGME) training time.
There was a significant increase in the duration of training and in the resultant debt over time. Group 1 respondents reported training for 8.5 years vs. 9.5 years in Group 2, with a doubling of graduates with educational debt greater than $100,000 in the later era.
Overall, the distribution of 118 respondents who answered the subspecialty question was 28% adult cardiac; 8.5% congenital cardiac; slightly less than 1% cardiopulmonary transplant; and 13.2% mixed subspecialties.
The 35.6% percent of women who identified themselves as general thoracic surgeons is higher than the 18% reported by the entire thoracic surgery workforce, with the percentage of women who identified themselves as general thoracic surgeons more than doubling in the second cohort of diplomates as compared with the first.
Slightly over 10% of respondents were no longer in CT surgery practice. All of these were certified prior to 2000, and the majority left practice due to retirement, health issues, or career advancement, according to their responses.
There was a large shift from the mixed category, which was cited by nearly 28% of the 51 women certified prior to 2000, compared with 3% of the 67 women certified after 2000.
This could be accounted for primarily by large increases in the adult cardiac (from nearly 20% prior to 2000 compared with 34% after 2000) and the general thoracic (from around 22% to 46%) subspecialty categories, reflecting the increase in subspecialization of our field.
Half of the women who responded had academic appointments, with 52% of these at the assistant professor level and 20% at the professor level. A minority of the women (20%) had protected research time, and 30% had secured research funding.
Overall, 64% of respondents reported that they were always or almost always satisfied with their profession.
The greatest source of dissatisfaction reported by both groups was demands on time, with workplace politics being a key concern expressed by Group 1 respondents, and lack of support a key concern expressed by Group 2.
Eighty percent of those polled stated that, if given the opportunity to choose a profession based on what they knew now, they would pursue cardiothoracic surgery again.
"Women still represent a minority of cardiothoracic surgeons in the United States, and over half are still very junior, having entered the profession since the year 2000.
Although the majority report being satisfied with their careers, and important academic milestones have been reached by some, there remains a scarcity of women in senior leadership positions.
"Since mentors and positive role models are consistently reported as significant factors in specialty decisions by surgical residents, this may still be the largest hurdle to recruiting women into cardiothoracic surgery," concluded Dr. Donington, in her presentation of the report.
Dr. Donington reported that she had no relevant financial disclosures.☐
Body text starts here....
Second and subsequent grafs
Doctor?s Name and Bio
Body text starts here....
Second and subsequent grafs
Doctor?s Name and Bio
Body text starts here....
Second and subsequent grafs
Doctor?s Name and Bio
Women represent a minority of cardiothoracic surgeons in the United States, with roughly equal numbers being found in academic and private practice, according to a recent survey presented at the annual meeting of the Society for Thoracic Surgeons.
Overall, these women reported a high level of job satisfaction and the vast majority of them were still in practice.
Although there were comparatively few women in senior staff and faculty positions, in part because over 50% of women currently in practice entered the profession since the year 2000, "this exponential increase in the number of women in the field over the past ten years provides optimism for a continued recruitment," according to the report by Dr. Jessica S. Donington, assistant professor of cardiothoracic surgery at New York University, New York, N.Y.,and her colleagues on behalf of The Women in Thoracic Surgery (WTS).
The WTS was established as a professional organization in 1986, with the designated mission of providing mutual support and facilitating the professional advancement of women in cardiothoracic surgery.
With 2011 being the 50th anniversary of the first certification of a woman by the American Board of Thoracic Surgery (ABTS) and the year in which the 200th female was certified by the ABTS, the WTS deemed it important to survey the status of female cardiothoracic surgeons in the United States.
The WTS survey was designed to measure career progression and to provide insights in order to improve recruitment. All ABTS-certified women were surveyed anonymously in December 2010 using tools from surveymonkey.com, according to Dr. Donington.
Contact information was obtained from CTSNet, Google, and institutions of known employment.
Of the 204 living women with ABTS certification, 190 were contacted. Of these, 64% responded to the survey. The questions comprised five areas: demographics, training, practice activities, activities of non-practicing CT surgeons, and career satisfaction.
The researchers grouped the respondents by year of certification: Group 1 (1961-1999) and Group 2 (2000-2010). They used the STS/AATS 2009 practice survey of the entire thoracic surgery workforce in order to make broad-based comparisons.
The mean age of the women respondents was 48 years, with the majority being white (nearly 78%) and urban dwellers (61%).
Half of the women were certified within the past 10 years. Overall, the respondents had been practicing for a mean of 8 years, worked in groups of 2-10 surgeons, and were the only female surgeon in their group. The respondents had a mean of 9.1 years of training with 56% reporting non-Accreditation Council for Graduate Medical Education (ACGME) training time.
There was a significant increase in the duration of training and in the resultant debt over time. Group 1 respondents reported training for 8.5 years vs. 9.5 years in Group 2, with a doubling of graduates with educational debt greater than $100,000 in the later era.
Overall, the distribution of 118 respondents who answered the subspecialty question was 28% adult cardiac; 8.5% congenital cardiac; slightly less than 1% cardiopulmonary transplant; and 13.2% mixed subspecialties.
The 35.6% percent of women who identified themselves as general thoracic surgeons is higher than the 18% reported by the entire thoracic surgery workforce, with the percentage of women who identified themselves as general thoracic surgeons more than doubling in the second cohort of diplomates as compared with the first.
Slightly over 10% of respondents were no longer in CT surgery practice. All of these were certified prior to 2000, and the majority left practice due to retirement, health issues, or career advancement, according to their responses.
There was a large shift from the mixed category, which was cited by nearly 28% of the 51 women certified prior to 2000, compared with 3% of the 67 women certified after 2000.
This could be accounted for primarily by large increases in the adult cardiac (from nearly 20% prior to 2000 compared with 34% after 2000) and the general thoracic (from around 22% to 46%) subspecialty categories, reflecting the increase in subspecialization of our field.
Half of the women who responded had academic appointments, with 52% of these at the assistant professor level and 20% at the professor level. A minority of the women (20%) had protected research time, and 30% had secured research funding.
Overall, 64% of respondents reported that they were always or almost always satisfied with their profession.
The greatest source of dissatisfaction reported by both groups was demands on time, with workplace politics being a key concern expressed by Group 1 respondents, and lack of support a key concern expressed by Group 2.
Eighty percent of those polled stated that, if given the opportunity to choose a profession based on what they knew now, they would pursue cardiothoracic surgery again.
"Women still represent a minority of cardiothoracic surgeons in the United States, and over half are still very junior, having entered the profession since the year 2000.
Although the majority report being satisfied with their careers, and important academic milestones have been reached by some, there remains a scarcity of women in senior leadership positions.
"Since mentors and positive role models are consistently reported as significant factors in specialty decisions by surgical residents, this may still be the largest hurdle to recruiting women into cardiothoracic surgery," concluded Dr. Donington, in her presentation of the report.
Dr. Donington reported that she had no relevant financial disclosures.☐
Women represent a minority of cardiothoracic surgeons in the United States, with roughly equal numbers being found in academic and private practice, according to a recent survey presented at the annual meeting of the Society for Thoracic Surgeons.
Overall, these women reported a high level of job satisfaction and the vast majority of them were still in practice.
Although there were comparatively few women in senior staff and faculty positions, in part because over 50% of women currently in practice entered the profession since the year 2000, "this exponential increase in the number of women in the field over the past ten years provides optimism for a continued recruitment," according to the report by Dr. Jessica S. Donington, assistant professor of cardiothoracic surgery at New York University, New York, N.Y.,and her colleagues on behalf of The Women in Thoracic Surgery (WTS).
The WTS was established as a professional organization in 1986, with the designated mission of providing mutual support and facilitating the professional advancement of women in cardiothoracic surgery.
With 2011 being the 50th anniversary of the first certification of a woman by the American Board of Thoracic Surgery (ABTS) and the year in which the 200th female was certified by the ABTS, the WTS deemed it important to survey the status of female cardiothoracic surgeons in the United States.
The WTS survey was designed to measure career progression and to provide insights in order to improve recruitment. All ABTS-certified women were surveyed anonymously in December 2010 using tools from surveymonkey.com, according to Dr. Donington.
Contact information was obtained from CTSNet, Google, and institutions of known employment.
Of the 204 living women with ABTS certification, 190 were contacted. Of these, 64% responded to the survey. The questions comprised five areas: demographics, training, practice activities, activities of non-practicing CT surgeons, and career satisfaction.
The researchers grouped the respondents by year of certification: Group 1 (1961-1999) and Group 2 (2000-2010). They used the STS/AATS 2009 practice survey of the entire thoracic surgery workforce in order to make broad-based comparisons.
The mean age of the women respondents was 48 years, with the majority being white (nearly 78%) and urban dwellers (61%).
Half of the women were certified within the past 10 years. Overall, the respondents had been practicing for a mean of 8 years, worked in groups of 2-10 surgeons, and were the only female surgeon in their group. The respondents had a mean of 9.1 years of training with 56% reporting non-Accreditation Council for Graduate Medical Education (ACGME) training time.
There was a significant increase in the duration of training and in the resultant debt over time. Group 1 respondents reported training for 8.5 years vs. 9.5 years in Group 2, with a doubling of graduates with educational debt greater than $100,000 in the later era.
Overall, the distribution of 118 respondents who answered the subspecialty question was 28% adult cardiac; 8.5% congenital cardiac; slightly less than 1% cardiopulmonary transplant; and 13.2% mixed subspecialties.
The 35.6% percent of women who identified themselves as general thoracic surgeons is higher than the 18% reported by the entire thoracic surgery workforce, with the percentage of women who identified themselves as general thoracic surgeons more than doubling in the second cohort of diplomates as compared with the first.
Slightly over 10% of respondents were no longer in CT surgery practice. All of these were certified prior to 2000, and the majority left practice due to retirement, health issues, or career advancement, according to their responses.
There was a large shift from the mixed category, which was cited by nearly 28% of the 51 women certified prior to 2000, compared with 3% of the 67 women certified after 2000.
This could be accounted for primarily by large increases in the adult cardiac (from nearly 20% prior to 2000 compared with 34% after 2000) and the general thoracic (from around 22% to 46%) subspecialty categories, reflecting the increase in subspecialization of our field.
Half of the women who responded had academic appointments, with 52% of these at the assistant professor level and 20% at the professor level. A minority of the women (20%) had protected research time, and 30% had secured research funding.
Overall, 64% of respondents reported that they were always or almost always satisfied with their profession.
The greatest source of dissatisfaction reported by both groups was demands on time, with workplace politics being a key concern expressed by Group 1 respondents, and lack of support a key concern expressed by Group 2.
Eighty percent of those polled stated that, if given the opportunity to choose a profession based on what they knew now, they would pursue cardiothoracic surgery again.
"Women still represent a minority of cardiothoracic surgeons in the United States, and over half are still very junior, having entered the profession since the year 2000.
Although the majority report being satisfied with their careers, and important academic milestones have been reached by some, there remains a scarcity of women in senior leadership positions.
"Since mentors and positive role models are consistently reported as significant factors in specialty decisions by surgical residents, this may still be the largest hurdle to recruiting women into cardiothoracic surgery," concluded Dr. Donington, in her presentation of the report.
Dr. Donington reported that she had no relevant financial disclosures.☐
Major Finding: Key numerical finding (e.g., number needed to treat to prevent one death/event; number lived or died as result of intervention). Maximum 20 words/2 sentences.
Data Source: : Include type of study (e.g., randomized, placebo controlled trial; retrospective case-control study). Include number in the study. Written in sentence form..
Disclosures: Sponsor of study, funding source, relevant disclosures. If author has no relevant disclosures, "Dr. X reported having no financial disclosures." If necessary, "Meeting Y did not require reports of financial disclosures." Check meeting website because many list disclosures. Written in sentence form.
Medicare Demos Fall Short on Savings
Over the last 2 decades, policymakers have proposed a number of ways to change how health care is delivered by Medicare. But a new analysis from the nonpartisan Congressional Budget Office analyzed 10 major Medicare demonstrations involving disease management and care coordination or some type of value-based payments and found that most of the projects didn’t save money.
The analysis has clear implications for health policy going forward. Under the Affordable Care Act, Congress required the Centers for Medicare and Medicaid Services to pursue new payment and care delivery models including accountable care organizations (ACOs) and bundled payments. Congress also created a new Innovation Center within CMS to test other models of care. The idea behind the newly formed Innovation Center is that Medicare officials will be able to expand successful projects without returning for Congress approval.
Dr. Glen R. Stream, president of the American Academy of Family Physicians, said he expects that the leadership within Medicare will use the CBO analysis to improve future pilot projects. He said he’s hopeful that the work that the Innovation Center is undertaking will yield better results because its projects focus on broader care delivery concepts, such as the patient-centered medical home, rather than targeting only certain chronic conditions, as was done in several past demonstrations.
Looking at the six disease management and care coordination projects that Medicare had already undertaken, CBO analysts found that on average there was little to no effect on hospital admissions or regular Medicare spending. The demonstrations were more likely to reduce costs if they used care managers who had significant, direct contact with physicians and patients. However, those programs generally didn’t save enough money to cover the cost of the extra services provided.
For example, in programs with significant in-person or telephone interaction between care management and patients there was an average 7% drop in hospital admissions and a 3% reduction in regular Medicare spending. However, in order to offset the cost of care management fees, the programs would have had to reduce Medicare expenditures by 13%.
In the four demonstrations that focused on changing the financial incentives for providers, only one produced significant savings. A project that offered bundled payments to physicians and hospitals for heart bypass surgery reduced Medicare expenditures related to heart bypass by about 10% without adverse impact on patient outcomes.
Medicare was able to achieve those savings in large part because officials negotiated bundled payments that were lower than the traditional fee-for-service payments, according to CBO. The other projects, which offered bonuses for meeting quality standards or reducing spending, did not achieve significant savings for the Medicare program, CBO wrote. ☐
Over the last 2 decades, policymakers have proposed a number of ways to change how health care is delivered by Medicare. But a new analysis from the nonpartisan Congressional Budget Office analyzed 10 major Medicare demonstrations involving disease management and care coordination or some type of value-based payments and found that most of the projects didn’t save money.
The analysis has clear implications for health policy going forward. Under the Affordable Care Act, Congress required the Centers for Medicare and Medicaid Services to pursue new payment and care delivery models including accountable care organizations (ACOs) and bundled payments. Congress also created a new Innovation Center within CMS to test other models of care. The idea behind the newly formed Innovation Center is that Medicare officials will be able to expand successful projects without returning for Congress approval.
Dr. Glen R. Stream, president of the American Academy of Family Physicians, said he expects that the leadership within Medicare will use the CBO analysis to improve future pilot projects. He said he’s hopeful that the work that the Innovation Center is undertaking will yield better results because its projects focus on broader care delivery concepts, such as the patient-centered medical home, rather than targeting only certain chronic conditions, as was done in several past demonstrations.
Looking at the six disease management and care coordination projects that Medicare had already undertaken, CBO analysts found that on average there was little to no effect on hospital admissions or regular Medicare spending. The demonstrations were more likely to reduce costs if they used care managers who had significant, direct contact with physicians and patients. However, those programs generally didn’t save enough money to cover the cost of the extra services provided.
For example, in programs with significant in-person or telephone interaction between care management and patients there was an average 7% drop in hospital admissions and a 3% reduction in regular Medicare spending. However, in order to offset the cost of care management fees, the programs would have had to reduce Medicare expenditures by 13%.
In the four demonstrations that focused on changing the financial incentives for providers, only one produced significant savings. A project that offered bundled payments to physicians and hospitals for heart bypass surgery reduced Medicare expenditures related to heart bypass by about 10% without adverse impact on patient outcomes.
Medicare was able to achieve those savings in large part because officials negotiated bundled payments that were lower than the traditional fee-for-service payments, according to CBO. The other projects, which offered bonuses for meeting quality standards or reducing spending, did not achieve significant savings for the Medicare program, CBO wrote. ☐
Over the last 2 decades, policymakers have proposed a number of ways to change how health care is delivered by Medicare. But a new analysis from the nonpartisan Congressional Budget Office analyzed 10 major Medicare demonstrations involving disease management and care coordination or some type of value-based payments and found that most of the projects didn’t save money.
The analysis has clear implications for health policy going forward. Under the Affordable Care Act, Congress required the Centers for Medicare and Medicaid Services to pursue new payment and care delivery models including accountable care organizations (ACOs) and bundled payments. Congress also created a new Innovation Center within CMS to test other models of care. The idea behind the newly formed Innovation Center is that Medicare officials will be able to expand successful projects without returning for Congress approval.
Dr. Glen R. Stream, president of the American Academy of Family Physicians, said he expects that the leadership within Medicare will use the CBO analysis to improve future pilot projects. He said he’s hopeful that the work that the Innovation Center is undertaking will yield better results because its projects focus on broader care delivery concepts, such as the patient-centered medical home, rather than targeting only certain chronic conditions, as was done in several past demonstrations.
Looking at the six disease management and care coordination projects that Medicare had already undertaken, CBO analysts found that on average there was little to no effect on hospital admissions or regular Medicare spending. The demonstrations were more likely to reduce costs if they used care managers who had significant, direct contact with physicians and patients. However, those programs generally didn’t save enough money to cover the cost of the extra services provided.
For example, in programs with significant in-person or telephone interaction between care management and patients there was an average 7% drop in hospital admissions and a 3% reduction in regular Medicare spending. However, in order to offset the cost of care management fees, the programs would have had to reduce Medicare expenditures by 13%.
In the four demonstrations that focused on changing the financial incentives for providers, only one produced significant savings. A project that offered bundled payments to physicians and hospitals for heart bypass surgery reduced Medicare expenditures related to heart bypass by about 10% without adverse impact on patient outcomes.
Medicare was able to achieve those savings in large part because officials negotiated bundled payments that were lower than the traditional fee-for-service payments, according to CBO. The other projects, which offered bonuses for meeting quality standards or reducing spending, did not achieve significant savings for the Medicare program, CBO wrote. ☐
Survey: Women CT Surgeons Report Job Satisfaction
Women represent a minority of cardiothoracic surgeons in the United States, with roughly equal numbers being found in academic and private practice, according to a recent survey presented at the annual meeting of the Society for Thoracic Surgeons.
Overall, these women reported a high level of job satisfaction and the vast majority of them were still in practice.
Although there were comparatively few women in senior staff and faculty positions, in part because over 50% of women currently in practice entered the profession since the year 2000, "this exponential increase in the number of women in the field over the past ten years provides optimism for a continued recruitment," according to the report by Dr. Jessica S. Donington, assistant professor of cardiothoracic surgery at New York University, New York, N.Y.,and her colleagues on behalf of The Women in Thoracic Surgery (WTS).
The WTS was established as a professional organization in 1986, with the designated mission of providing mutual support and facilitating the professional advancement of women in cardiothoracic surgery.
With 2011 being the 50th anniversary of the first certification of a woman by the American Board of Thoracic Surgery (ABTS) and the year in which the 200th female was certified by the ABTS, the WTS deemed it important to survey the status of female cardiothoracic surgeons in the United States.
The WTS survey was designed to measure career progression and to provide insights in order to improve recruitment. All ABTS-certified women were surveyed anonymously in December 2010 using tools from surveymonkey.com, according to Dr. Donington.
Contact information was obtained from CTSNet, Google, and institutions of known employment.
Of the 204 living women with ABTS certification, 190 were contacted. Of these, 64% responded to the survey. The questions comprised five areas: demographics, training, practice activities, activities of non-practicing CT surgeons, and career satisfaction.
The researchers grouped the respondents by year of certification: Group 1 (1961-1999) and Group 2 (2000-2010). They used the STS/AATS 2009 practice survey of the entire thoracic surgery workforce in order to make broad-based comparisons.
The mean age of the women respondents was 48 years, with the majority being white (nearly 78%) and urban dwellers (61%).
Half of the women were certified within the past 10 years. Overall, the respondents had been practicing for a mean of 8 years, worked in groups of 2-10 surgeons, and were the only female surgeon in their group. The respondents had a mean of 9.1 years of training with 56% reporting non-Accreditation Council for Graduate Medical Education (ACGME) training time.
There was a significant increase in the duration of training and in the resultant debt over time. Group 1 respondents reported training for 8.5 years vs. 9.5 years in Group 2, with a doubling of graduates with educational debt greater than $100,000 in the later era.
Overall, the distribution of 118 respondents who answered the subspecialty question was 28% adult cardiac; 8.5% congenital cardiac; slightly less than 1% cardiopulmonary transplant; and 13.2% mixed subspecialties.
The 35.6% percent of women who identified themselves as general thoracic surgeons is higher than the 18% reported by the entire thoracic surgery workforce, with the percentage of women who identified themselves as general thoracic surgeons more than doubling in the second cohort of diplomates as compared with the first.
Slightly over 10% of respondents were no longer in CT surgery practice. All of these were certified prior to 2000, and the majority left practice due to retirement, health issues, or career advancement, according to their responses.
There was a large shift from the mixed category, which was cited by nearly 28% of the 51 women certified prior to 2000, compared with 3% of the 67 women certified after 2000.
This could be accounted for primarily by large increases in the adult cardiac (from nearly 20% prior to 2000 compared with 34% after 2000) and the general thoracic (from around 22% to 46%) subspecialty categories, reflecting the increase in subspecialization of our field.
Half of the women who responded had academic appointments, with 52% of these at the assistant professor level and 20% at the professor level. A minority of the women (20%) had protected research time, and 30% had secured research funding.
Overall, 64% of respondents reported that they were always or almost always satisfied with their profession.
The greatest source of dissatisfaction reported by both groups was demands on time, with workplace politics being a key concern expressed by Group 1 respondents, and lack of support a key concern expressed by Group 2.
Eighty percent of those polled stated that, if given the opportunity to choose a profession based on what they knew now, they would pursue cardiothoracic surgery again.
"Women still represent a minority of cardiothoracic surgeons in the United States, and over half are still very junior, having entered the profession since the year 2000.
Although the majority report being satisfied with their careers, and important academic milestones have been reached by some, there remains a scarcity of women in senior leadership positions.
"Since mentors and positive role models are consistently reported as significant factors in specialty decisions by surgical residents, this may still be the largest hurdle to recruiting women into cardiothoracic surgery," concluded Dr. Donington, in her presentation of the report.
Dr. Donington reported that she had no relevant financial disclosures.☐
Body text starts here....
Second and subsequent grafs
Doctor?s Name and Bio
Body text starts here....
Second and subsequent grafs
Doctor?s Name and Bio
Body text starts here....
Second and subsequent grafs
Doctor?s Name and Bio
Women represent a minority of cardiothoracic surgeons in the United States, with roughly equal numbers being found in academic and private practice, according to a recent survey presented at the annual meeting of the Society for Thoracic Surgeons.
Overall, these women reported a high level of job satisfaction and the vast majority of them were still in practice.
Although there were comparatively few women in senior staff and faculty positions, in part because over 50% of women currently in practice entered the profession since the year 2000, "this exponential increase in the number of women in the field over the past ten years provides optimism for a continued recruitment," according to the report by Dr. Jessica S. Donington, assistant professor of cardiothoracic surgery at New York University, New York, N.Y.,and her colleagues on behalf of The Women in Thoracic Surgery (WTS).
The WTS was established as a professional organization in 1986, with the designated mission of providing mutual support and facilitating the professional advancement of women in cardiothoracic surgery.
With 2011 being the 50th anniversary of the first certification of a woman by the American Board of Thoracic Surgery (ABTS) and the year in which the 200th female was certified by the ABTS, the WTS deemed it important to survey the status of female cardiothoracic surgeons in the United States.
The WTS survey was designed to measure career progression and to provide insights in order to improve recruitment. All ABTS-certified women were surveyed anonymously in December 2010 using tools from surveymonkey.com, according to Dr. Donington.
Contact information was obtained from CTSNet, Google, and institutions of known employment.
Of the 204 living women with ABTS certification, 190 were contacted. Of these, 64% responded to the survey. The questions comprised five areas: demographics, training, practice activities, activities of non-practicing CT surgeons, and career satisfaction.
The researchers grouped the respondents by year of certification: Group 1 (1961-1999) and Group 2 (2000-2010). They used the STS/AATS 2009 practice survey of the entire thoracic surgery workforce in order to make broad-based comparisons.
The mean age of the women respondents was 48 years, with the majority being white (nearly 78%) and urban dwellers (61%).
Half of the women were certified within the past 10 years. Overall, the respondents had been practicing for a mean of 8 years, worked in groups of 2-10 surgeons, and were the only female surgeon in their group. The respondents had a mean of 9.1 years of training with 56% reporting non-Accreditation Council for Graduate Medical Education (ACGME) training time.
There was a significant increase in the duration of training and in the resultant debt over time. Group 1 respondents reported training for 8.5 years vs. 9.5 years in Group 2, with a doubling of graduates with educational debt greater than $100,000 in the later era.
Overall, the distribution of 118 respondents who answered the subspecialty question was 28% adult cardiac; 8.5% congenital cardiac; slightly less than 1% cardiopulmonary transplant; and 13.2% mixed subspecialties.
The 35.6% percent of women who identified themselves as general thoracic surgeons is higher than the 18% reported by the entire thoracic surgery workforce, with the percentage of women who identified themselves as general thoracic surgeons more than doubling in the second cohort of diplomates as compared with the first.
Slightly over 10% of respondents were no longer in CT surgery practice. All of these were certified prior to 2000, and the majority left practice due to retirement, health issues, or career advancement, according to their responses.
There was a large shift from the mixed category, which was cited by nearly 28% of the 51 women certified prior to 2000, compared with 3% of the 67 women certified after 2000.
This could be accounted for primarily by large increases in the adult cardiac (from nearly 20% prior to 2000 compared with 34% after 2000) and the general thoracic (from around 22% to 46%) subspecialty categories, reflecting the increase in subspecialization of our field.
Half of the women who responded had academic appointments, with 52% of these at the assistant professor level and 20% at the professor level. A minority of the women (20%) had protected research time, and 30% had secured research funding.
Overall, 64% of respondents reported that they were always or almost always satisfied with their profession.
The greatest source of dissatisfaction reported by both groups was demands on time, with workplace politics being a key concern expressed by Group 1 respondents, and lack of support a key concern expressed by Group 2.
Eighty percent of those polled stated that, if given the opportunity to choose a profession based on what they knew now, they would pursue cardiothoracic surgery again.
"Women still represent a minority of cardiothoracic surgeons in the United States, and over half are still very junior, having entered the profession since the year 2000.
Although the majority report being satisfied with their careers, and important academic milestones have been reached by some, there remains a scarcity of women in senior leadership positions.
"Since mentors and positive role models are consistently reported as significant factors in specialty decisions by surgical residents, this may still be the largest hurdle to recruiting women into cardiothoracic surgery," concluded Dr. Donington, in her presentation of the report.
Dr. Donington reported that she had no relevant financial disclosures.☐
Women represent a minority of cardiothoracic surgeons in the United States, with roughly equal numbers being found in academic and private practice, according to a recent survey presented at the annual meeting of the Society for Thoracic Surgeons.
Overall, these women reported a high level of job satisfaction and the vast majority of them were still in practice.
Although there were comparatively few women in senior staff and faculty positions, in part because over 50% of women currently in practice entered the profession since the year 2000, "this exponential increase in the number of women in the field over the past ten years provides optimism for a continued recruitment," according to the report by Dr. Jessica S. Donington, assistant professor of cardiothoracic surgery at New York University, New York, N.Y.,and her colleagues on behalf of The Women in Thoracic Surgery (WTS).
The WTS was established as a professional organization in 1986, with the designated mission of providing mutual support and facilitating the professional advancement of women in cardiothoracic surgery.
With 2011 being the 50th anniversary of the first certification of a woman by the American Board of Thoracic Surgery (ABTS) and the year in which the 200th female was certified by the ABTS, the WTS deemed it important to survey the status of female cardiothoracic surgeons in the United States.
The WTS survey was designed to measure career progression and to provide insights in order to improve recruitment. All ABTS-certified women were surveyed anonymously in December 2010 using tools from surveymonkey.com, according to Dr. Donington.
Contact information was obtained from CTSNet, Google, and institutions of known employment.
Of the 204 living women with ABTS certification, 190 were contacted. Of these, 64% responded to the survey. The questions comprised five areas: demographics, training, practice activities, activities of non-practicing CT surgeons, and career satisfaction.
The researchers grouped the respondents by year of certification: Group 1 (1961-1999) and Group 2 (2000-2010). They used the STS/AATS 2009 practice survey of the entire thoracic surgery workforce in order to make broad-based comparisons.
The mean age of the women respondents was 48 years, with the majority being white (nearly 78%) and urban dwellers (61%).
Half of the women were certified within the past 10 years. Overall, the respondents had been practicing for a mean of 8 years, worked in groups of 2-10 surgeons, and were the only female surgeon in their group. The respondents had a mean of 9.1 years of training with 56% reporting non-Accreditation Council for Graduate Medical Education (ACGME) training time.
There was a significant increase in the duration of training and in the resultant debt over time. Group 1 respondents reported training for 8.5 years vs. 9.5 years in Group 2, with a doubling of graduates with educational debt greater than $100,000 in the later era.
Overall, the distribution of 118 respondents who answered the subspecialty question was 28% adult cardiac; 8.5% congenital cardiac; slightly less than 1% cardiopulmonary transplant; and 13.2% mixed subspecialties.
The 35.6% percent of women who identified themselves as general thoracic surgeons is higher than the 18% reported by the entire thoracic surgery workforce, with the percentage of women who identified themselves as general thoracic surgeons more than doubling in the second cohort of diplomates as compared with the first.
Slightly over 10% of respondents were no longer in CT surgery practice. All of these were certified prior to 2000, and the majority left practice due to retirement, health issues, or career advancement, according to their responses.
There was a large shift from the mixed category, which was cited by nearly 28% of the 51 women certified prior to 2000, compared with 3% of the 67 women certified after 2000.
This could be accounted for primarily by large increases in the adult cardiac (from nearly 20% prior to 2000 compared with 34% after 2000) and the general thoracic (from around 22% to 46%) subspecialty categories, reflecting the increase in subspecialization of our field.
Half of the women who responded had academic appointments, with 52% of these at the assistant professor level and 20% at the professor level. A minority of the women (20%) had protected research time, and 30% had secured research funding.
Overall, 64% of respondents reported that they were always or almost always satisfied with their profession.
The greatest source of dissatisfaction reported by both groups was demands on time, with workplace politics being a key concern expressed by Group 1 respondents, and lack of support a key concern expressed by Group 2.
Eighty percent of those polled stated that, if given the opportunity to choose a profession based on what they knew now, they would pursue cardiothoracic surgery again.
"Women still represent a minority of cardiothoracic surgeons in the United States, and over half are still very junior, having entered the profession since the year 2000.
Although the majority report being satisfied with their careers, and important academic milestones have been reached by some, there remains a scarcity of women in senior leadership positions.
"Since mentors and positive role models are consistently reported as significant factors in specialty decisions by surgical residents, this may still be the largest hurdle to recruiting women into cardiothoracic surgery," concluded Dr. Donington, in her presentation of the report.
Dr. Donington reported that she had no relevant financial disclosures.☐
Major Finding: Key numerical finding (e.g., number needed to treat to prevent one death/event; number lived or died as result of intervention). Maximum 20 words/2 sentences.
Data Source: : Include type of study (e.g., randomized, placebo controlled trial; retrospective case-control study). Include number in the study. Written in sentence form..
Disclosures: Sponsor of study, funding source, relevant disclosures. If author has no relevant disclosures, "Dr. X reported having no financial disclosures." If necessary, "Meeting Y did not require reports of financial disclosures." Check meeting website because many list disclosures. Written in sentence form.
Health Spending Growth Slowed in 2010
WASHINGTON – The historically low growth in health spending in 2009 continued through 2010, driven largely by the recession, Centers for Medicare and Medicaid officials announced earlier this year.
U.S. health spending grew 3.9% in 2010, to a total of $2.6 trillion or $8,402 per person. That was a 0.1% rise from 2009, which was already at an all-time low growth rate.
As the nation’s economy slumped throughout 2009 and 2010, consumers cut back on elective surgical procedures, emergency room visits, physician office visits, and prescription drug use, according to the officials.
"Even though the recession officially ended in 2009, its impact on the health sector appears to have continued into 2010," said Anne Martin, an economist with the CMS.
Employers shifted the costs of insurance and care to employees, which drove up out-of-pocket spending in 2010.
But consumers overall spent only 1.8% more out-of-pocket in 2010 than they had in 2009, which was a slow rate of growth when compared with historical patterns, Ms. Martin said.
Consumers reacted to cost-shifting by choosing health insurance plans with lower premiums and higher deductibles, and by reducing, where they could, use of personal health care services. Medical prices and the U.S. population remained relatively stable before, during, and after the recession, and yet, personal health spending fell, indicating a willful pullback.
"The slower growth in personal health care spending was mainly driven by the slowdown in the use and intensity of health care goods and services," Ms. Martin said. The agency documented a shrinkage in use of hospital care and physician services as compared with historical levels.
Hospital spending grew only 5% to $814 billion in 2010, compared to 6% in 2009. There was a decline in median inpatient admissions, and slower growth in emergency department visits, outpatient visits, and outpatient surgeries.
Overall spending on physicians and clinical services – totaling $515 billion in 2010 – accounted for 20% of total health spending. As consumers went to the doctor less frequently, fewer prescriptions were written. And, many of those dispensed were for less expensive generic drugs. These and other factors led to the slowest rate of growth in prescription drug spending ever recorded – a 1% increase from 2009 to $259 billion. The data were published in the journal Health Affairs (2012 [doi: 10.1377/hlthaff.2011.1135]).
Growth in spending on physician and clinical services also was historically low, growing 2.5% in 2010 as compared with 3.3% in 2009, said Ms. Martin.
Meanwhile, as employers and private insurers reduced the amount they spent on health care, the federal government’s share of health spending rose – to 29% or a total of $742 billion in 2010. The rise in federal spending also was attributed to federal subsidies to state Medicaid programs. Medicaid was about 15% of the nation’s health bill in 2010, at $401 billion.
In 2009, the federal government spent 22% more than in 2008; in 2010, spending rose by almost 9%. That compares to a 10% decrease in spending by states and localities in 2008, and a 4% increase in 2010.
Medicare saw an increase in enrollment, both in Medicare Advantage managed care program and traditional fee-for-service Medicare. The increase in traditional enrollment reversed a several-year pattern of decline. Overall, Medicare spending increased 5% in 2010 to $524 billion, but per-enrollee spending did not rise as quickly as it had in 2009.
This is because there was a big reduction in payments for certain types of home health services, but also because of low use of physician services. Small increases in physician fees in 2009 and 2010 also kept a lid on Medicare spending.
Those increases were instituted by Congress in response to cuts that would otherwise have been required by Medicare’s Sustainable Growth Rate formula.
The Affordable Care Act had a negligible impact on overall spending, perhaps accounting for less than 0.1% of the slowdown, according to the CMS economists. This is because few provisions were in effect in 2010, and some, such as coverage for patients with preexisting conditions, did not enroll as many people as had been expected. ☐
WASHINGTON – The historically low growth in health spending in 2009 continued through 2010, driven largely by the recession, Centers for Medicare and Medicaid officials announced earlier this year.
U.S. health spending grew 3.9% in 2010, to a total of $2.6 trillion or $8,402 per person. That was a 0.1% rise from 2009, which was already at an all-time low growth rate.
As the nation’s economy slumped throughout 2009 and 2010, consumers cut back on elective surgical procedures, emergency room visits, physician office visits, and prescription drug use, according to the officials.
"Even though the recession officially ended in 2009, its impact on the health sector appears to have continued into 2010," said Anne Martin, an economist with the CMS.
Employers shifted the costs of insurance and care to employees, which drove up out-of-pocket spending in 2010.
But consumers overall spent only 1.8% more out-of-pocket in 2010 than they had in 2009, which was a slow rate of growth when compared with historical patterns, Ms. Martin said.
Consumers reacted to cost-shifting by choosing health insurance plans with lower premiums and higher deductibles, and by reducing, where they could, use of personal health care services. Medical prices and the U.S. population remained relatively stable before, during, and after the recession, and yet, personal health spending fell, indicating a willful pullback.
"The slower growth in personal health care spending was mainly driven by the slowdown in the use and intensity of health care goods and services," Ms. Martin said. The agency documented a shrinkage in use of hospital care and physician services as compared with historical levels.
Hospital spending grew only 5% to $814 billion in 2010, compared to 6% in 2009. There was a decline in median inpatient admissions, and slower growth in emergency department visits, outpatient visits, and outpatient surgeries.
Overall spending on physicians and clinical services – totaling $515 billion in 2010 – accounted for 20% of total health spending. As consumers went to the doctor less frequently, fewer prescriptions were written. And, many of those dispensed were for less expensive generic drugs. These and other factors led to the slowest rate of growth in prescription drug spending ever recorded – a 1% increase from 2009 to $259 billion. The data were published in the journal Health Affairs (2012 [doi: 10.1377/hlthaff.2011.1135]).
Growth in spending on physician and clinical services also was historically low, growing 2.5% in 2010 as compared with 3.3% in 2009, said Ms. Martin.
Meanwhile, as employers and private insurers reduced the amount they spent on health care, the federal government’s share of health spending rose – to 29% or a total of $742 billion in 2010. The rise in federal spending also was attributed to federal subsidies to state Medicaid programs. Medicaid was about 15% of the nation’s health bill in 2010, at $401 billion.
In 2009, the federal government spent 22% more than in 2008; in 2010, spending rose by almost 9%. That compares to a 10% decrease in spending by states and localities in 2008, and a 4% increase in 2010.
Medicare saw an increase in enrollment, both in Medicare Advantage managed care program and traditional fee-for-service Medicare. The increase in traditional enrollment reversed a several-year pattern of decline. Overall, Medicare spending increased 5% in 2010 to $524 billion, but per-enrollee spending did not rise as quickly as it had in 2009.
This is because there was a big reduction in payments for certain types of home health services, but also because of low use of physician services. Small increases in physician fees in 2009 and 2010 also kept a lid on Medicare spending.
Those increases were instituted by Congress in response to cuts that would otherwise have been required by Medicare’s Sustainable Growth Rate formula.
The Affordable Care Act had a negligible impact on overall spending, perhaps accounting for less than 0.1% of the slowdown, according to the CMS economists. This is because few provisions were in effect in 2010, and some, such as coverage for patients with preexisting conditions, did not enroll as many people as had been expected. ☐
WASHINGTON – The historically low growth in health spending in 2009 continued through 2010, driven largely by the recession, Centers for Medicare and Medicaid officials announced earlier this year.
U.S. health spending grew 3.9% in 2010, to a total of $2.6 trillion or $8,402 per person. That was a 0.1% rise from 2009, which was already at an all-time low growth rate.
As the nation’s economy slumped throughout 2009 and 2010, consumers cut back on elective surgical procedures, emergency room visits, physician office visits, and prescription drug use, according to the officials.
"Even though the recession officially ended in 2009, its impact on the health sector appears to have continued into 2010," said Anne Martin, an economist with the CMS.
Employers shifted the costs of insurance and care to employees, which drove up out-of-pocket spending in 2010.
But consumers overall spent only 1.8% more out-of-pocket in 2010 than they had in 2009, which was a slow rate of growth when compared with historical patterns, Ms. Martin said.
Consumers reacted to cost-shifting by choosing health insurance plans with lower premiums and higher deductibles, and by reducing, where they could, use of personal health care services. Medical prices and the U.S. population remained relatively stable before, during, and after the recession, and yet, personal health spending fell, indicating a willful pullback.
"The slower growth in personal health care spending was mainly driven by the slowdown in the use and intensity of health care goods and services," Ms. Martin said. The agency documented a shrinkage in use of hospital care and physician services as compared with historical levels.
Hospital spending grew only 5% to $814 billion in 2010, compared to 6% in 2009. There was a decline in median inpatient admissions, and slower growth in emergency department visits, outpatient visits, and outpatient surgeries.
Overall spending on physicians and clinical services – totaling $515 billion in 2010 – accounted for 20% of total health spending. As consumers went to the doctor less frequently, fewer prescriptions were written. And, many of those dispensed were for less expensive generic drugs. These and other factors led to the slowest rate of growth in prescription drug spending ever recorded – a 1% increase from 2009 to $259 billion. The data were published in the journal Health Affairs (2012 [doi: 10.1377/hlthaff.2011.1135]).
Growth in spending on physician and clinical services also was historically low, growing 2.5% in 2010 as compared with 3.3% in 2009, said Ms. Martin.
Meanwhile, as employers and private insurers reduced the amount they spent on health care, the federal government’s share of health spending rose – to 29% or a total of $742 billion in 2010. The rise in federal spending also was attributed to federal subsidies to state Medicaid programs. Medicaid was about 15% of the nation’s health bill in 2010, at $401 billion.
In 2009, the federal government spent 22% more than in 2008; in 2010, spending rose by almost 9%. That compares to a 10% decrease in spending by states and localities in 2008, and a 4% increase in 2010.
Medicare saw an increase in enrollment, both in Medicare Advantage managed care program and traditional fee-for-service Medicare. The increase in traditional enrollment reversed a several-year pattern of decline. Overall, Medicare spending increased 5% in 2010 to $524 billion, but per-enrollee spending did not rise as quickly as it had in 2009.
This is because there was a big reduction in payments for certain types of home health services, but also because of low use of physician services. Small increases in physician fees in 2009 and 2010 also kept a lid on Medicare spending.
Those increases were instituted by Congress in response to cuts that would otherwise have been required by Medicare’s Sustainable Growth Rate formula.
The Affordable Care Act had a negligible impact on overall spending, perhaps accounting for less than 0.1% of the slowdown, according to the CMS economists. This is because few provisions were in effect in 2010, and some, such as coverage for patients with preexisting conditions, did not enroll as many people as had been expected. ☐