User login
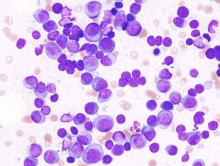
Transcription factor promotes MM progression

rim of a bone spicule (pink)
New research indicates that multiple myeloma (MM) cells can “disguise” themselves as bone cells to elude the immune system, a trick that enables MM progression.
Investigators found evidence suggesting that MM cells mimic bone-marrow-resident cells by expressing bone-related genes, and this process is driven by overexpression of Runx2, a transcription factor that regulates bone formation.
“[R]unx2 overexpression can give multiple myeloma cells a bone-cell-like phenotype,” said Yang Yang, MD, PhD, of the University of Alabama at Birmingham.
“When the multiple myeloma cells come to the new bone sites, the bone immune cells think, ‘This is one of our neighbor cells,’ and therefore do not eliminate them. The bone immune cells do not recognize these cells as strangers.”
Dr Yang and her colleagues explained this phenomenon in Blood.
The investigators first conducted in vitro experiments and found that Runx2 expression in MM cells does not affect proliferation, but it does increase the cells’ invasiveness.
The team then used molecular genetic techniques to increase or decrease the expression of Runx2 in MM cells in vivo. They found that Runx2 overexpression promoted tumor growth and progression in mice. And mice with decreased Runx2 expression had less tumor growth and disease spread than control mice.
Further investigation revealed that Runx2 overexpression activates the Akt/β-catenin/survivin signaling pathway in MM cells. This is a different pathway than the one activated by Runx2 in solid tumors.
Downstream of the signaling pathway, Runx2 overexpression led to overexpression of bone-related genes, including genes expressed by osteoblasts, osteoclasts, and osteocytes.
Overexpression of Runx2 also enhanced secretion of soluble factors—including cytokines and growth factors—that aid tumor progression and metastasis.
In their final experiments, the investigators looked at Runx2 expression in human samples.
The team compared samples from 14 healthy bone marrow donors, 35 MM patients, and 11 patients with monoclonal gammopathy of undetermined significance (MGUS). Runx2 levels were significantly higher in MM cells than in plasma cells from normal and MGUS samples.
The investigators also assessed Runx2 expression in a larger group of 351 newly diagnosed MM patients. Runx2 levels were significantly higher in patients who had a high risk of early disease-related death. The risk of death was determined by an existing gene expression profile test.
“This suggests that Runx2 levels in myeloma cells may be a gene predictor of a patient’s prognosis, good or bad,” Dr Yang said.
She and her colleagues also believe that targeting Runx2 expression could be a feasible strategy for treating aggressive MM. ![]()

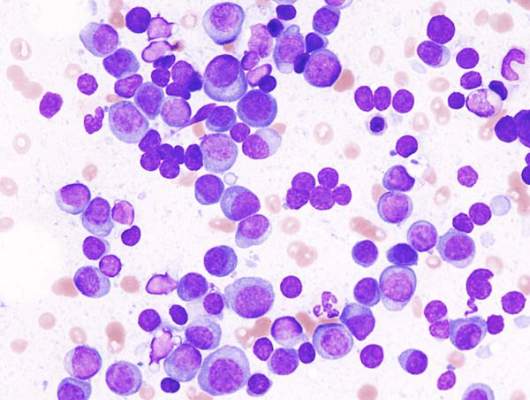
rim of a bone spicule (pink)
New research indicates that multiple myeloma (MM) cells can “disguise” themselves as bone cells to elude the immune system, a trick that enables MM progression.
Investigators found evidence suggesting that MM cells mimic bone-marrow-resident cells by expressing bone-related genes, and this process is driven by overexpression of Runx2, a transcription factor that regulates bone formation.
“[R]unx2 overexpression can give multiple myeloma cells a bone-cell-like phenotype,” said Yang Yang, MD, PhD, of the University of Alabama at Birmingham.
“When the multiple myeloma cells come to the new bone sites, the bone immune cells think, ‘This is one of our neighbor cells,’ and therefore do not eliminate them. The bone immune cells do not recognize these cells as strangers.”
Dr Yang and her colleagues explained this phenomenon in Blood.
The investigators first conducted in vitro experiments and found that Runx2 expression in MM cells does not affect proliferation, but it does increase the cells’ invasiveness.
The team then used molecular genetic techniques to increase or decrease the expression of Runx2 in MM cells in vivo. They found that Runx2 overexpression promoted tumor growth and progression in mice. And mice with decreased Runx2 expression had less tumor growth and disease spread than control mice.
Further investigation revealed that Runx2 overexpression activates the Akt/β-catenin/survivin signaling pathway in MM cells. This is a different pathway than the one activated by Runx2 in solid tumors.
Downstream of the signaling pathway, Runx2 overexpression led to overexpression of bone-related genes, including genes expressed by osteoblasts, osteoclasts, and osteocytes.
Overexpression of Runx2 also enhanced secretion of soluble factors—including cytokines and growth factors—that aid tumor progression and metastasis.
In their final experiments, the investigators looked at Runx2 expression in human samples.
The team compared samples from 14 healthy bone marrow donors, 35 MM patients, and 11 patients with monoclonal gammopathy of undetermined significance (MGUS). Runx2 levels were significantly higher in MM cells than in plasma cells from normal and MGUS samples.
The investigators also assessed Runx2 expression in a larger group of 351 newly diagnosed MM patients. Runx2 levels were significantly higher in patients who had a high risk of early disease-related death. The risk of death was determined by an existing gene expression profile test.
“This suggests that Runx2 levels in myeloma cells may be a gene predictor of a patient’s prognosis, good or bad,” Dr Yang said.
She and her colleagues also believe that targeting Runx2 expression could be a feasible strategy for treating aggressive MM. ![]()

rim of a bone spicule (pink)
New research indicates that multiple myeloma (MM) cells can “disguise” themselves as bone cells to elude the immune system, a trick that enables MM progression.
Investigators found evidence suggesting that MM cells mimic bone-marrow-resident cells by expressing bone-related genes, and this process is driven by overexpression of Runx2, a transcription factor that regulates bone formation.
“[R]unx2 overexpression can give multiple myeloma cells a bone-cell-like phenotype,” said Yang Yang, MD, PhD, of the University of Alabama at Birmingham.
“When the multiple myeloma cells come to the new bone sites, the bone immune cells think, ‘This is one of our neighbor cells,’ and therefore do not eliminate them. The bone immune cells do not recognize these cells as strangers.”
Dr Yang and her colleagues explained this phenomenon in Blood.
The investigators first conducted in vitro experiments and found that Runx2 expression in MM cells does not affect proliferation, but it does increase the cells’ invasiveness.
The team then used molecular genetic techniques to increase or decrease the expression of Runx2 in MM cells in vivo. They found that Runx2 overexpression promoted tumor growth and progression in mice. And mice with decreased Runx2 expression had less tumor growth and disease spread than control mice.
Further investigation revealed that Runx2 overexpression activates the Akt/β-catenin/survivin signaling pathway in MM cells. This is a different pathway than the one activated by Runx2 in solid tumors.
Downstream of the signaling pathway, Runx2 overexpression led to overexpression of bone-related genes, including genes expressed by osteoblasts, osteoclasts, and osteocytes.
Overexpression of Runx2 also enhanced secretion of soluble factors—including cytokines and growth factors—that aid tumor progression and metastasis.
In their final experiments, the investigators looked at Runx2 expression in human samples.
The team compared samples from 14 healthy bone marrow donors, 35 MM patients, and 11 patients with monoclonal gammopathy of undetermined significance (MGUS). Runx2 levels were significantly higher in MM cells than in plasma cells from normal and MGUS samples.
The investigators also assessed Runx2 expression in a larger group of 351 newly diagnosed MM patients. Runx2 levels were significantly higher in patients who had a high risk of early disease-related death. The risk of death was determined by an existing gene expression profile test.
“This suggests that Runx2 levels in myeloma cells may be a gene predictor of a patient’s prognosis, good or bad,” Dr Yang said.
She and her colleagues also believe that targeting Runx2 expression could be a feasible strategy for treating aggressive MM. ![]()
Older cancer patients under-utilize advanced care planning

Photo courtesy of NCI
and Mathews Media Group
Survey results suggest the use of aggressive treatment at the end of life is on the rise among older cancer patients, and these patients often fail to employ advanced care planning measures.
Researchers reviewed nearly 2000 surveys of people whose loved ones died of cancer and found that, from 2000 to 2012, there was a 51% increase in reports that patients received “all care possible” at the end of life.
There was a 22% increase in power-of-attorney assignment over the same period, but the use of living wills and discussions about end-of-life preferences decreased slightly.
“Although more cancer patients are assigning power-of-attorney privileges to someone they know and trust to make their medical decisions when they can’t, this practice may be the least helpful among advanced care planning tactics because it may be least associated with treatment intensity at the end of life,” said Amol Narang, MD, of The Johns Hopkins Hospital in Baltimore, Maryland.
Dr Narang and his colleagues described this research in JAMA Oncology.
The team analyzed survey data from 1985 next-of-kin surrogates of cancer patients. The patients were older than 50 years of age, had taken part in the Health and Retirement Study, and died between 2000 and 2012.
The data included in-depth “exit” interviews conducted with the surrogates after a patient died. Seventy-nine percent of exit survey respondents said they were the primary decision-maker in the patient’s medical care.
The data showed a significant increase in power-of-attorney assignments, from 52% in 2000 to 74% in 2012 (P=0.03). But the use of living wills decreased slightly, from 49% to 40% (P=0.63), as did discussions about end-of-life preferences, which fell from 68% to 60% (P=0.62).
“We found that many cancer patients still do not communicate their preferences for end-of-life care, despite the potential benefits to patients’ quality of life and caregiver bereavement,” Dr Narang said.
Survey results also suggested a significant increase in the percentage of patients who received “all care possible” at the end of life, from 7% in 2000 to 58% in 2012 (P=0.004). But there was no significant change in the rates of terminal hospitalizations, which fell from 29% to 27% (P=0.70).
The researchers found that granting power-of-attorney privileges significantly decreased the odds that patients would die in the hospital as opposed to hospice or their homes (adjusted odds ratio [AOR]=0.70, P<0.05). However, granting power of attorney was not associated with a significant change in limiting or withholding treatment at the end of life (AOR=1.52).
On the other hand, patients who created living wills or had end-of-life discussions were significantly more likely than their peers to limit or withhold certain treatments. The AOR was 2.51 for living wills (P<0.001) and 1.93 for end-of-life discussions (P=0.002).
The researchers said they observed the same trends regardless of who completed the exit survey.
Dr Narang noted that this study had its limitations. The survey questions were subjective, answers could have been hampered by a respondent’s lapse in memory, and answers could be biased by a respondent’s desire to meet social norms.
“But we were looking at trends over time,” he said, “so respondents’ bias would not likely change over time.” ![]()

Photo courtesy of NCI
and Mathews Media Group
Survey results suggest the use of aggressive treatment at the end of life is on the rise among older cancer patients, and these patients often fail to employ advanced care planning measures.
Researchers reviewed nearly 2000 surveys of people whose loved ones died of cancer and found that, from 2000 to 2012, there was a 51% increase in reports that patients received “all care possible” at the end of life.
There was a 22% increase in power-of-attorney assignment over the same period, but the use of living wills and discussions about end-of-life preferences decreased slightly.
“Although more cancer patients are assigning power-of-attorney privileges to someone they know and trust to make their medical decisions when they can’t, this practice may be the least helpful among advanced care planning tactics because it may be least associated with treatment intensity at the end of life,” said Amol Narang, MD, of The Johns Hopkins Hospital in Baltimore, Maryland.
Dr Narang and his colleagues described this research in JAMA Oncology.
The team analyzed survey data from 1985 next-of-kin surrogates of cancer patients. The patients were older than 50 years of age, had taken part in the Health and Retirement Study, and died between 2000 and 2012.
The data included in-depth “exit” interviews conducted with the surrogates after a patient died. Seventy-nine percent of exit survey respondents said they were the primary decision-maker in the patient’s medical care.
The data showed a significant increase in power-of-attorney assignments, from 52% in 2000 to 74% in 2012 (P=0.03). But the use of living wills decreased slightly, from 49% to 40% (P=0.63), as did discussions about end-of-life preferences, which fell from 68% to 60% (P=0.62).
“We found that many cancer patients still do not communicate their preferences for end-of-life care, despite the potential benefits to patients’ quality of life and caregiver bereavement,” Dr Narang said.
Survey results also suggested a significant increase in the percentage of patients who received “all care possible” at the end of life, from 7% in 2000 to 58% in 2012 (P=0.004). But there was no significant change in the rates of terminal hospitalizations, which fell from 29% to 27% (P=0.70).
The researchers found that granting power-of-attorney privileges significantly decreased the odds that patients would die in the hospital as opposed to hospice or their homes (adjusted odds ratio [AOR]=0.70, P<0.05). However, granting power of attorney was not associated with a significant change in limiting or withholding treatment at the end of life (AOR=1.52).
On the other hand, patients who created living wills or had end-of-life discussions were significantly more likely than their peers to limit or withhold certain treatments. The AOR was 2.51 for living wills (P<0.001) and 1.93 for end-of-life discussions (P=0.002).
The researchers said they observed the same trends regardless of who completed the exit survey.
Dr Narang noted that this study had its limitations. The survey questions were subjective, answers could have been hampered by a respondent’s lapse in memory, and answers could be biased by a respondent’s desire to meet social norms.
“But we were looking at trends over time,” he said, “so respondents’ bias would not likely change over time.” ![]()

Photo courtesy of NCI
and Mathews Media Group
Survey results suggest the use of aggressive treatment at the end of life is on the rise among older cancer patients, and these patients often fail to employ advanced care planning measures.
Researchers reviewed nearly 2000 surveys of people whose loved ones died of cancer and found that, from 2000 to 2012, there was a 51% increase in reports that patients received “all care possible” at the end of life.
There was a 22% increase in power-of-attorney assignment over the same period, but the use of living wills and discussions about end-of-life preferences decreased slightly.
“Although more cancer patients are assigning power-of-attorney privileges to someone they know and trust to make their medical decisions when they can’t, this practice may be the least helpful among advanced care planning tactics because it may be least associated with treatment intensity at the end of life,” said Amol Narang, MD, of The Johns Hopkins Hospital in Baltimore, Maryland.
Dr Narang and his colleagues described this research in JAMA Oncology.
The team analyzed survey data from 1985 next-of-kin surrogates of cancer patients. The patients were older than 50 years of age, had taken part in the Health and Retirement Study, and died between 2000 and 2012.
The data included in-depth “exit” interviews conducted with the surrogates after a patient died. Seventy-nine percent of exit survey respondents said they were the primary decision-maker in the patient’s medical care.
The data showed a significant increase in power-of-attorney assignments, from 52% in 2000 to 74% in 2012 (P=0.03). But the use of living wills decreased slightly, from 49% to 40% (P=0.63), as did discussions about end-of-life preferences, which fell from 68% to 60% (P=0.62).
“We found that many cancer patients still do not communicate their preferences for end-of-life care, despite the potential benefits to patients’ quality of life and caregiver bereavement,” Dr Narang said.
Survey results also suggested a significant increase in the percentage of patients who received “all care possible” at the end of life, from 7% in 2000 to 58% in 2012 (P=0.004). But there was no significant change in the rates of terminal hospitalizations, which fell from 29% to 27% (P=0.70).
The researchers found that granting power-of-attorney privileges significantly decreased the odds that patients would die in the hospital as opposed to hospice or their homes (adjusted odds ratio [AOR]=0.70, P<0.05). However, granting power of attorney was not associated with a significant change in limiting or withholding treatment at the end of life (AOR=1.52).
On the other hand, patients who created living wills or had end-of-life discussions were significantly more likely than their peers to limit or withhold certain treatments. The AOR was 2.51 for living wills (P<0.001) and 1.93 for end-of-life discussions (P=0.002).
The researchers said they observed the same trends regardless of who completed the exit survey.
Dr Narang noted that this study had its limitations. The survey questions were subjective, answers could have been hampered by a respondent’s lapse in memory, and answers could be biased by a respondent’s desire to meet social norms.
“But we were looking at trends over time,” he said, “so respondents’ bias would not likely change over time.” ![]()
EAP makes drug available to MM patients

Photo by Linda Bartlett
A new expanded access program (EAP) will make daratumumab, an investigational anti-CD38 monoclonal antibody, available to patients with double-refractory multiple myeloma (MM).
The multicenter EAP is open to MM patients in the US who are 18 years of age or older.
Patients must be refractory to both a proteasome inhibitor (PI) and an immunomodulatory drug (IMiD) or have received 3 or more prior lines of therapy, including a PI and an IMiD.
In the US, EAPs are designed to make investigational medicines available for patients with serious or life-threatening illnesses who are ineligible for ongoing interventional trials and have exhausted currently available treatment options.
This EAP will make daratumumab available at up to 40 medical centers in the US while the drug’s Biologics License Application is under review by the US Food and Drug Administration (FDA).
Additional information about the EAP can be found on clinicaltrials.gov (NCT02477891). Janssen Research & Development, LLC, the company developing daratumumab, is collaborating with the Multiple Myeloma Research Foundation on this EAP.
About daratumumab
Daratumumab is a human IgG1k monoclonal antibody that binds with high affinity to the transmembrane ectoenzyme CD38 on the surface of MM cells.
Five phase 3 clinical studies with daratumumab in relapsed and frontline settings are currently ongoing. Additional studies are ongoing or planned to assess the drug’s potential in other malignant and pre-malignant diseases on which CD38 is expressed, such as smoldering myeloma and non-Hodgkin lymphoma.
On May 1, 2013, daratumumab received breakthrough designation from the FDA for the treatment of patients with MM who have received at least 3 prior lines of therapy, including a PI and an IMiD, or who are double refractory to a PI and an IMiD.
On June 5, 2015, Janssen announced it had initiated the rolling submission of its Biologics License Application for daratumumab to the FDA for the treatment of this set of MM patients. A rolling submission allows the company to submit portions of the regulatory application to the FDA as they are completed.
The regulatory submission for daratumumab will be primarily supported by data from the phase 2 MMY2002 (SIRIUS) study, the results of which were presented at the 2015 ASCO Annual Meeting.
The application will also be supported by data from 4 other studies, including the phase 1/2 GEN501 monotherapy study. ![]()

Photo by Linda Bartlett
A new expanded access program (EAP) will make daratumumab, an investigational anti-CD38 monoclonal antibody, available to patients with double-refractory multiple myeloma (MM).
The multicenter EAP is open to MM patients in the US who are 18 years of age or older.
Patients must be refractory to both a proteasome inhibitor (PI) and an immunomodulatory drug (IMiD) or have received 3 or more prior lines of therapy, including a PI and an IMiD.
In the US, EAPs are designed to make investigational medicines available for patients with serious or life-threatening illnesses who are ineligible for ongoing interventional trials and have exhausted currently available treatment options.
This EAP will make daratumumab available at up to 40 medical centers in the US while the drug’s Biologics License Application is under review by the US Food and Drug Administration (FDA).
Additional information about the EAP can be found on clinicaltrials.gov (NCT02477891). Janssen Research & Development, LLC, the company developing daratumumab, is collaborating with the Multiple Myeloma Research Foundation on this EAP.
About daratumumab
Daratumumab is a human IgG1k monoclonal antibody that binds with high affinity to the transmembrane ectoenzyme CD38 on the surface of MM cells.
Five phase 3 clinical studies with daratumumab in relapsed and frontline settings are currently ongoing. Additional studies are ongoing or planned to assess the drug’s potential in other malignant and pre-malignant diseases on which CD38 is expressed, such as smoldering myeloma and non-Hodgkin lymphoma.
On May 1, 2013, daratumumab received breakthrough designation from the FDA for the treatment of patients with MM who have received at least 3 prior lines of therapy, including a PI and an IMiD, or who are double refractory to a PI and an IMiD.
On June 5, 2015, Janssen announced it had initiated the rolling submission of its Biologics License Application for daratumumab to the FDA for the treatment of this set of MM patients. A rolling submission allows the company to submit portions of the regulatory application to the FDA as they are completed.
The regulatory submission for daratumumab will be primarily supported by data from the phase 2 MMY2002 (SIRIUS) study, the results of which were presented at the 2015 ASCO Annual Meeting.
The application will also be supported by data from 4 other studies, including the phase 1/2 GEN501 monotherapy study. ![]()

Photo by Linda Bartlett
A new expanded access program (EAP) will make daratumumab, an investigational anti-CD38 monoclonal antibody, available to patients with double-refractory multiple myeloma (MM).
The multicenter EAP is open to MM patients in the US who are 18 years of age or older.
Patients must be refractory to both a proteasome inhibitor (PI) and an immunomodulatory drug (IMiD) or have received 3 or more prior lines of therapy, including a PI and an IMiD.
In the US, EAPs are designed to make investigational medicines available for patients with serious or life-threatening illnesses who are ineligible for ongoing interventional trials and have exhausted currently available treatment options.
This EAP will make daratumumab available at up to 40 medical centers in the US while the drug’s Biologics License Application is under review by the US Food and Drug Administration (FDA).
Additional information about the EAP can be found on clinicaltrials.gov (NCT02477891). Janssen Research & Development, LLC, the company developing daratumumab, is collaborating with the Multiple Myeloma Research Foundation on this EAP.
About daratumumab
Daratumumab is a human IgG1k monoclonal antibody that binds with high affinity to the transmembrane ectoenzyme CD38 on the surface of MM cells.
Five phase 3 clinical studies with daratumumab in relapsed and frontline settings are currently ongoing. Additional studies are ongoing or planned to assess the drug’s potential in other malignant and pre-malignant diseases on which CD38 is expressed, such as smoldering myeloma and non-Hodgkin lymphoma.
On May 1, 2013, daratumumab received breakthrough designation from the FDA for the treatment of patients with MM who have received at least 3 prior lines of therapy, including a PI and an IMiD, or who are double refractory to a PI and an IMiD.
On June 5, 2015, Janssen announced it had initiated the rolling submission of its Biologics License Application for daratumumab to the FDA for the treatment of this set of MM patients. A rolling submission allows the company to submit portions of the regulatory application to the FDA as they are completed.
The regulatory submission for daratumumab will be primarily supported by data from the phase 2 MMY2002 (SIRIUS) study, the results of which were presented at the 2015 ASCO Annual Meeting.
The application will also be supported by data from 4 other studies, including the phase 1/2 GEN501 monotherapy study. ![]()
PI3K inhibitors may promote cancer spread

Photo courtesy of
The Wistar Institute
Although PI3K inhibitors have been designed to treat cancer, new research indicates these drugs may actually exacerbate the disease.
Researchers found evidence to suggest that treatment with PI3K inhibitors alone can promote more aggressive tumor cell behavior and increase the likelihood that cancer will spread.
PI3K inhibitors appeared to reprogram the mitochondria of tumor cells and move them to “strategic” positions for invasion.
However, the researchers believe that targeting mitochondrial function along with PI3K could prevent this effect.
Dario C. Altieri, MD, of The Wistar Institute in Philadelphia, Pennsylvania, and his colleagues described these findings in PNAS.
The researchers decided to investigate how mitochondria are reprogrammed when exposed to PI3K inhibition and how mitochondria might prevent targeted agents from being as effective as expected.
“Our prior studies have confirmed that tumor cells rely on energy produced by mitochondria more significantly than previously thought,” Dr Altieri said.
“What we have shown in this study is that, in somewhat of a paradox, treatment with a PI3K inhibitor causes a tumor cell’s mitochondria to produce energy in a localized manner, promoting a far more aggressive and invasive phenotype. The treatment appears to be doing the opposite of its intended effect.”
The study showed that treatment with a PI3K inhibitor causes the mitochondria to migrate to the peripheral cytoskeleton of the tumor cells.
While the mitochondria in untreated cells cluster around the cell’s nucleus, exposure of tumor cells to PI3K therapy causes the mitochondria to move to specialized regions of the cell’s membrane implicated in cell motility and invasion.
In this “strategic” position, tumor mitochondria are ideally positioned to provide a concentrated source of energy to support an increase in cell migration and invasion.
However, the researchers said the dependence of this response on mitochondrial function may offer a new therapeutic angle.
Dr Altieri and his team have shown that targeting mitochondrial functions for tumor therapy is feasible and dramatically enhances the anticancer activity of PI3K inhibitors when used in combination.
“These findings continue to support the idea that the mitochondria of tumor cells are crucial to tumor survival and proliferation,” Dr Altieri said. “It’s certainly counterintuitive that a drug designed to fight cancer may in actuality help it spread, but by identifying why this is happening, we can develop better strategies that allow these drugs to treat tumors the way they should.” ![]()

Photo courtesy of
The Wistar Institute
Although PI3K inhibitors have been designed to treat cancer, new research indicates these drugs may actually exacerbate the disease.
Researchers found evidence to suggest that treatment with PI3K inhibitors alone can promote more aggressive tumor cell behavior and increase the likelihood that cancer will spread.
PI3K inhibitors appeared to reprogram the mitochondria of tumor cells and move them to “strategic” positions for invasion.
However, the researchers believe that targeting mitochondrial function along with PI3K could prevent this effect.
Dario C. Altieri, MD, of The Wistar Institute in Philadelphia, Pennsylvania, and his colleagues described these findings in PNAS.
The researchers decided to investigate how mitochondria are reprogrammed when exposed to PI3K inhibition and how mitochondria might prevent targeted agents from being as effective as expected.
“Our prior studies have confirmed that tumor cells rely on energy produced by mitochondria more significantly than previously thought,” Dr Altieri said.
“What we have shown in this study is that, in somewhat of a paradox, treatment with a PI3K inhibitor causes a tumor cell’s mitochondria to produce energy in a localized manner, promoting a far more aggressive and invasive phenotype. The treatment appears to be doing the opposite of its intended effect.”
The study showed that treatment with a PI3K inhibitor causes the mitochondria to migrate to the peripheral cytoskeleton of the tumor cells.
While the mitochondria in untreated cells cluster around the cell’s nucleus, exposure of tumor cells to PI3K therapy causes the mitochondria to move to specialized regions of the cell’s membrane implicated in cell motility and invasion.
In this “strategic” position, tumor mitochondria are ideally positioned to provide a concentrated source of energy to support an increase in cell migration and invasion.
However, the researchers said the dependence of this response on mitochondrial function may offer a new therapeutic angle.
Dr Altieri and his team have shown that targeting mitochondrial functions for tumor therapy is feasible and dramatically enhances the anticancer activity of PI3K inhibitors when used in combination.
“These findings continue to support the idea that the mitochondria of tumor cells are crucial to tumor survival and proliferation,” Dr Altieri said. “It’s certainly counterintuitive that a drug designed to fight cancer may in actuality help it spread, but by identifying why this is happening, we can develop better strategies that allow these drugs to treat tumors the way they should.” ![]()

Photo courtesy of
The Wistar Institute
Although PI3K inhibitors have been designed to treat cancer, new research indicates these drugs may actually exacerbate the disease.
Researchers found evidence to suggest that treatment with PI3K inhibitors alone can promote more aggressive tumor cell behavior and increase the likelihood that cancer will spread.
PI3K inhibitors appeared to reprogram the mitochondria of tumor cells and move them to “strategic” positions for invasion.
However, the researchers believe that targeting mitochondrial function along with PI3K could prevent this effect.
Dario C. Altieri, MD, of The Wistar Institute in Philadelphia, Pennsylvania, and his colleagues described these findings in PNAS.
The researchers decided to investigate how mitochondria are reprogrammed when exposed to PI3K inhibition and how mitochondria might prevent targeted agents from being as effective as expected.
“Our prior studies have confirmed that tumor cells rely on energy produced by mitochondria more significantly than previously thought,” Dr Altieri said.
“What we have shown in this study is that, in somewhat of a paradox, treatment with a PI3K inhibitor causes a tumor cell’s mitochondria to produce energy in a localized manner, promoting a far more aggressive and invasive phenotype. The treatment appears to be doing the opposite of its intended effect.”
The study showed that treatment with a PI3K inhibitor causes the mitochondria to migrate to the peripheral cytoskeleton of the tumor cells.
While the mitochondria in untreated cells cluster around the cell’s nucleus, exposure of tumor cells to PI3K therapy causes the mitochondria to move to specialized regions of the cell’s membrane implicated in cell motility and invasion.
In this “strategic” position, tumor mitochondria are ideally positioned to provide a concentrated source of energy to support an increase in cell migration and invasion.
However, the researchers said the dependence of this response on mitochondrial function may offer a new therapeutic angle.
Dr Altieri and his team have shown that targeting mitochondrial functions for tumor therapy is feasible and dramatically enhances the anticancer activity of PI3K inhibitors when used in combination.
“These findings continue to support the idea that the mitochondria of tumor cells are crucial to tumor survival and proliferation,” Dr Altieri said. “It’s certainly counterintuitive that a drug designed to fight cancer may in actuality help it spread, but by identifying why this is happening, we can develop better strategies that allow these drugs to treat tumors the way they should.” ![]()
CRd is well tolerated and effective in newly diagnosed and smoldering multiple myeloma
Patients with newly diagnosed multiple myeloma or smoldering multiple myeloma experienced good responses and few severe adverse events from carfilzomib-lenalidomide-dexamethasone with lenalidomide extension (CRd-R), according to a report published online in JAMA Oncology.
The regimen was not associated with peripheral neuropathy of grade 3 or above, and both groups had high rates of minimal residual disease negativity, which has been shown to be associated with improved progression-free survival and overall survival in newly diagnosed patients treated with CRd.
However, the three tools used for measuring patient response differed in their abilities to detect minimal residual disease, the researchers reported.
“Given the high degree of CR [complete response] rates achievable by three-drug combination regimens, there is an increased need for clinical trials to detect MRD [minimal residual disease] beyond traditional methods and characterize optimal MRD technique,” wrote Dr. Neha Korde of the myeloma service at Memorial Sloan Kettering Cancer Center, New York, and colleagues.
The researchers used three measures to assess minimal residual disease: multiparametric flow cytometry, next-generation sequencing, and fluorodeoxyglucose positron-emission tomography/computed tomography.
Based on multiparametric flow cytometry, minimal residual disease was not detected in 62% (28/45) of the patients with newly diagnosed disease and in 92% (11/12) of those with smoldering multiple myeloma, (JAMA Oncol. 2015 July 2 [doi:10.1001/jamaoncol.2015.2010]). Based on flow cytometry, 98% negativity for minimal residual disease was seen in patients with at least nCR. Based on next-generation sequencing, an additional 30% of patients were positive for minimal residual disease, highlighting the potential increased sensitivity of that assay, the researcher said.
In patients with newly diagnosed disease, 98% achieved at least a partial response, 89% had at least a very good partial response, 62% had at least a near complete response, and 56% had at least a complete response or a stringent complete response. Responses improved with more therapy; the median time to CR was 5 (2-17) cycles, and six patients reached CR during the lenalidomide extension. The median duration of response was not reached.
All of the patients with high-risk smoldering multiple myeloma achieved at least a complete response, with median time of 6 (2-20) cycles to CR.
In a 2-year study, 45 patients with newly diagnosed multiple myeloma received a treatment regimen that included eight 28-day cycles of CRd, followed by 24 cycles of lenalidomide extended dosing for those with stable disease. Promising early results led to a pilot study with the same regimen in 12 patients with high-risk SMM, a condition that leads to symptomatic disease within a median of 2 years.
None of the patients with newly diagnosed multiple myeloma had peripheral neuropathy of grade 3 or above, the primary endpoint. Grade 1 peripheral neuropathy affected 33% of patients, and grade 2 was experienced by 9%. Lymphopenia and electrolyte or metabolism abnormalities were the most common adverse events. Grade 3 or 4 cardiac events included two patients with congestive heart failure and three patients with hypertension.
Patients with smoldering multiple myeloma had similar rates of adverse events.
In this pilot study, the CRd combination was well tolerated and yielded deep responses across prognostic groups. However, morphological complete response, in this scenario, was insufficient to characterize tumor reduction.
“With the introduction of highly effective drug combinations, traditional response criteria become less valid because these do not sufficiently assess the deepness of response.” New approaches such as MRD and PET/CT negativity should be introduced to evaluate response in clinical trials and, ultimately, in clinical practice.
Patients with smoldering multiple myeloma, who have more than a 90% probability of disease progression within 2 years, may benefit from early treatment that is effective and does not expose them to an excessive risk of toxicity.
Dr. Pieter Sonneveld is head of the department of hematology at the Erasmus MC Cancer Institute, Rotterdam, the Netherlands. Dr. Sonneveld reported receiving research funding from Celgene, Onyx/Amgen, Janssen, and Karyopharm.
In this pilot study, the CRd combination was well tolerated and yielded deep responses across prognostic groups. However, morphological complete response, in this scenario, was insufficient to characterize tumor reduction.
“With the introduction of highly effective drug combinations, traditional response criteria become less valid because these do not sufficiently assess the deepness of response.” New approaches such as MRD and PET/CT negativity should be introduced to evaluate response in clinical trials and, ultimately, in clinical practice.
Patients with smoldering multiple myeloma, who have more than a 90% probability of disease progression within 2 years, may benefit from early treatment that is effective and does not expose them to an excessive risk of toxicity.
Dr. Pieter Sonneveld is head of the department of hematology at the Erasmus MC Cancer Institute, Rotterdam, the Netherlands. Dr. Sonneveld reported receiving research funding from Celgene, Onyx/Amgen, Janssen, and Karyopharm.
In this pilot study, the CRd combination was well tolerated and yielded deep responses across prognostic groups. However, morphological complete response, in this scenario, was insufficient to characterize tumor reduction.
“With the introduction of highly effective drug combinations, traditional response criteria become less valid because these do not sufficiently assess the deepness of response.” New approaches such as MRD and PET/CT negativity should be introduced to evaluate response in clinical trials and, ultimately, in clinical practice.
Patients with smoldering multiple myeloma, who have more than a 90% probability of disease progression within 2 years, may benefit from early treatment that is effective and does not expose them to an excessive risk of toxicity.
Dr. Pieter Sonneveld is head of the department of hematology at the Erasmus MC Cancer Institute, Rotterdam, the Netherlands. Dr. Sonneveld reported receiving research funding from Celgene, Onyx/Amgen, Janssen, and Karyopharm.
Patients with newly diagnosed multiple myeloma or smoldering multiple myeloma experienced good responses and few severe adverse events from carfilzomib-lenalidomide-dexamethasone with lenalidomide extension (CRd-R), according to a report published online in JAMA Oncology.
The regimen was not associated with peripheral neuropathy of grade 3 or above, and both groups had high rates of minimal residual disease negativity, which has been shown to be associated with improved progression-free survival and overall survival in newly diagnosed patients treated with CRd.
However, the three tools used for measuring patient response differed in their abilities to detect minimal residual disease, the researchers reported.
“Given the high degree of CR [complete response] rates achievable by three-drug combination regimens, there is an increased need for clinical trials to detect MRD [minimal residual disease] beyond traditional methods and characterize optimal MRD technique,” wrote Dr. Neha Korde of the myeloma service at Memorial Sloan Kettering Cancer Center, New York, and colleagues.
The researchers used three measures to assess minimal residual disease: multiparametric flow cytometry, next-generation sequencing, and fluorodeoxyglucose positron-emission tomography/computed tomography.
Based on multiparametric flow cytometry, minimal residual disease was not detected in 62% (28/45) of the patients with newly diagnosed disease and in 92% (11/12) of those with smoldering multiple myeloma, (JAMA Oncol. 2015 July 2 [doi:10.1001/jamaoncol.2015.2010]). Based on flow cytometry, 98% negativity for minimal residual disease was seen in patients with at least nCR. Based on next-generation sequencing, an additional 30% of patients were positive for minimal residual disease, highlighting the potential increased sensitivity of that assay, the researcher said.
In patients with newly diagnosed disease, 98% achieved at least a partial response, 89% had at least a very good partial response, 62% had at least a near complete response, and 56% had at least a complete response or a stringent complete response. Responses improved with more therapy; the median time to CR was 5 (2-17) cycles, and six patients reached CR during the lenalidomide extension. The median duration of response was not reached.
All of the patients with high-risk smoldering multiple myeloma achieved at least a complete response, with median time of 6 (2-20) cycles to CR.
In a 2-year study, 45 patients with newly diagnosed multiple myeloma received a treatment regimen that included eight 28-day cycles of CRd, followed by 24 cycles of lenalidomide extended dosing for those with stable disease. Promising early results led to a pilot study with the same regimen in 12 patients with high-risk SMM, a condition that leads to symptomatic disease within a median of 2 years.
None of the patients with newly diagnosed multiple myeloma had peripheral neuropathy of grade 3 or above, the primary endpoint. Grade 1 peripheral neuropathy affected 33% of patients, and grade 2 was experienced by 9%. Lymphopenia and electrolyte or metabolism abnormalities were the most common adverse events. Grade 3 or 4 cardiac events included two patients with congestive heart failure and three patients with hypertension.
Patients with smoldering multiple myeloma had similar rates of adverse events.
Patients with newly diagnosed multiple myeloma or smoldering multiple myeloma experienced good responses and few severe adverse events from carfilzomib-lenalidomide-dexamethasone with lenalidomide extension (CRd-R), according to a report published online in JAMA Oncology.
The regimen was not associated with peripheral neuropathy of grade 3 or above, and both groups had high rates of minimal residual disease negativity, which has been shown to be associated with improved progression-free survival and overall survival in newly diagnosed patients treated with CRd.
However, the three tools used for measuring patient response differed in their abilities to detect minimal residual disease, the researchers reported.
“Given the high degree of CR [complete response] rates achievable by three-drug combination regimens, there is an increased need for clinical trials to detect MRD [minimal residual disease] beyond traditional methods and characterize optimal MRD technique,” wrote Dr. Neha Korde of the myeloma service at Memorial Sloan Kettering Cancer Center, New York, and colleagues.
The researchers used three measures to assess minimal residual disease: multiparametric flow cytometry, next-generation sequencing, and fluorodeoxyglucose positron-emission tomography/computed tomography.
Based on multiparametric flow cytometry, minimal residual disease was not detected in 62% (28/45) of the patients with newly diagnosed disease and in 92% (11/12) of those with smoldering multiple myeloma, (JAMA Oncol. 2015 July 2 [doi:10.1001/jamaoncol.2015.2010]). Based on flow cytometry, 98% negativity for minimal residual disease was seen in patients with at least nCR. Based on next-generation sequencing, an additional 30% of patients were positive for minimal residual disease, highlighting the potential increased sensitivity of that assay, the researcher said.
In patients with newly diagnosed disease, 98% achieved at least a partial response, 89% had at least a very good partial response, 62% had at least a near complete response, and 56% had at least a complete response or a stringent complete response. Responses improved with more therapy; the median time to CR was 5 (2-17) cycles, and six patients reached CR during the lenalidomide extension. The median duration of response was not reached.
All of the patients with high-risk smoldering multiple myeloma achieved at least a complete response, with median time of 6 (2-20) cycles to CR.
In a 2-year study, 45 patients with newly diagnosed multiple myeloma received a treatment regimen that included eight 28-day cycles of CRd, followed by 24 cycles of lenalidomide extended dosing for those with stable disease. Promising early results led to a pilot study with the same regimen in 12 patients with high-risk SMM, a condition that leads to symptomatic disease within a median of 2 years.
None of the patients with newly diagnosed multiple myeloma had peripheral neuropathy of grade 3 or above, the primary endpoint. Grade 1 peripheral neuropathy affected 33% of patients, and grade 2 was experienced by 9%. Lymphopenia and electrolyte or metabolism abnormalities were the most common adverse events. Grade 3 or 4 cardiac events included two patients with congestive heart failure and three patients with hypertension.
Patients with smoldering multiple myeloma had similar rates of adverse events.
FROM JAMA ONCOLOGY
Key clinical point: Patients with newly diagnosed multiple myeloma or smoldering multiple myeloma had high rates of minimal residual disease negativity and none experienced grade 3 or 4 peripheral neuropathy from carfilzomib-lenalidomide-dexamethasone with lenalidomide extension (CRd-R).
Major finding: Based on multiparametric flow cytometry, minimal residual disease was not detected in 62% (28/45) of the patients with newly diagnosed disease and in 92% (11/12) of those with smoldering multiple myeloma.
Data source: A 2-year pilot study of 45 patients with newly diagnosed multiple myeloma and 12 patients with smoldering multiple myeloma.
Disclosures: The study was partially supported by Onyx and Celgene. Dr. Korde reported consulting for MedScape. Her coauthors reported ties to several industry sources.
CHMP recommends panobinostat for MM

Photo courtesy of the CDC
The European Medicines Agency’s Committee for Medicinal Products for Human Use (CHMP) is recommending regulatory approval for panobinostat (Farydak) to treat relapsed and/or refractory multiple myeloma (MM).
The drug is indicated for use in combination with bortezomib and dexamethasone to treat adults with MM who have received at least 2 prior treatment regimens, including bortezomib and an immunomodulatory agent (IMiD).
Panobinostat is already approved for this indication in the US and Chile.
If the European Commission follows the CHMP’s recommendation, panobinostat will be the first histone deacetylase (HDAC) inhibitor approved to treat MM in the European Union.
The European Commission generally follows CHMP recommendations and delivers its final decision within 3 months of the recommendation. The decision will be applicable to all 28 European Union member states, plus Iceland, Norway, and Liechtenstein.
“Panobinostat is the first and only HDAC inhibitor recommended by the CHMP for the treatment of patients living with multiple myeloma who have progressed after standard-of-care therapy with bortezomib and an IMiD,” said Alessandro Riva, MD, Global Head of Oncology Development and Medical Affairs at Novartis Oncology, the company developing panobinostat.
“We are pleased with the positive CHMP opinion on panobinostat for previously treated patients because it brings us one step closer to providing a new treatment option for patients in need in Europe.”
The CHMP’s recommendation is based on efficacy and safety data in a subgroup analysis of 147 patients on the phase 3 PANORAMA-1 trial. Results from this analysis were recently presented at the 2015 ASCO Annual Meeting.
PANORAMA-1 was designed to compare panobinostat in combination with bortezomib and dexamethasone to bortezomib and dexamethasone alone in patients who had relapsed or relapsed and refractory MM.
At ASCO, researchers presented results in 147 patients who had received 2 or more prior treatment regimens, including bortezomib and an IMiD.
The patients who received panobinostat, bortezomib, and dexamethasone had a longer median progression-free survival than patients who received bortezomib and dexamethasone alone—12.5 months and 4.7 months, respectively (hazard ratio=0.47).
Common grade 3/4 adverse events in both treatment arms were thrombocytopenia, lymphopenia, neutropenia, diarrhea, asthenia/fatigue, and peripheral neuropathy. About 7% of patients in both arms died while on treatment. ![]()

Photo courtesy of the CDC
The European Medicines Agency’s Committee for Medicinal Products for Human Use (CHMP) is recommending regulatory approval for panobinostat (Farydak) to treat relapsed and/or refractory multiple myeloma (MM).
The drug is indicated for use in combination with bortezomib and dexamethasone to treat adults with MM who have received at least 2 prior treatment regimens, including bortezomib and an immunomodulatory agent (IMiD).
Panobinostat is already approved for this indication in the US and Chile.
If the European Commission follows the CHMP’s recommendation, panobinostat will be the first histone deacetylase (HDAC) inhibitor approved to treat MM in the European Union.
The European Commission generally follows CHMP recommendations and delivers its final decision within 3 months of the recommendation. The decision will be applicable to all 28 European Union member states, plus Iceland, Norway, and Liechtenstein.
“Panobinostat is the first and only HDAC inhibitor recommended by the CHMP for the treatment of patients living with multiple myeloma who have progressed after standard-of-care therapy with bortezomib and an IMiD,” said Alessandro Riva, MD, Global Head of Oncology Development and Medical Affairs at Novartis Oncology, the company developing panobinostat.
“We are pleased with the positive CHMP opinion on panobinostat for previously treated patients because it brings us one step closer to providing a new treatment option for patients in need in Europe.”
The CHMP’s recommendation is based on efficacy and safety data in a subgroup analysis of 147 patients on the phase 3 PANORAMA-1 trial. Results from this analysis were recently presented at the 2015 ASCO Annual Meeting.
PANORAMA-1 was designed to compare panobinostat in combination with bortezomib and dexamethasone to bortezomib and dexamethasone alone in patients who had relapsed or relapsed and refractory MM.
At ASCO, researchers presented results in 147 patients who had received 2 or more prior treatment regimens, including bortezomib and an IMiD.
The patients who received panobinostat, bortezomib, and dexamethasone had a longer median progression-free survival than patients who received bortezomib and dexamethasone alone—12.5 months and 4.7 months, respectively (hazard ratio=0.47).
Common grade 3/4 adverse events in both treatment arms were thrombocytopenia, lymphopenia, neutropenia, diarrhea, asthenia/fatigue, and peripheral neuropathy. About 7% of patients in both arms died while on treatment. ![]()

Photo courtesy of the CDC
The European Medicines Agency’s Committee for Medicinal Products for Human Use (CHMP) is recommending regulatory approval for panobinostat (Farydak) to treat relapsed and/or refractory multiple myeloma (MM).
The drug is indicated for use in combination with bortezomib and dexamethasone to treat adults with MM who have received at least 2 prior treatment regimens, including bortezomib and an immunomodulatory agent (IMiD).
Panobinostat is already approved for this indication in the US and Chile.
If the European Commission follows the CHMP’s recommendation, panobinostat will be the first histone deacetylase (HDAC) inhibitor approved to treat MM in the European Union.
The European Commission generally follows CHMP recommendations and delivers its final decision within 3 months of the recommendation. The decision will be applicable to all 28 European Union member states, plus Iceland, Norway, and Liechtenstein.
“Panobinostat is the first and only HDAC inhibitor recommended by the CHMP for the treatment of patients living with multiple myeloma who have progressed after standard-of-care therapy with bortezomib and an IMiD,” said Alessandro Riva, MD, Global Head of Oncology Development and Medical Affairs at Novartis Oncology, the company developing panobinostat.
“We are pleased with the positive CHMP opinion on panobinostat for previously treated patients because it brings us one step closer to providing a new treatment option for patients in need in Europe.”
The CHMP’s recommendation is based on efficacy and safety data in a subgroup analysis of 147 patients on the phase 3 PANORAMA-1 trial. Results from this analysis were recently presented at the 2015 ASCO Annual Meeting.
PANORAMA-1 was designed to compare panobinostat in combination with bortezomib and dexamethasone to bortezomib and dexamethasone alone in patients who had relapsed or relapsed and refractory MM.
At ASCO, researchers presented results in 147 patients who had received 2 or more prior treatment regimens, including bortezomib and an IMiD.
The patients who received panobinostat, bortezomib, and dexamethasone had a longer median progression-free survival than patients who received bortezomib and dexamethasone alone—12.5 months and 4.7 months, respectively (hazard ratio=0.47).
Common grade 3/4 adverse events in both treatment arms were thrombocytopenia, lymphopenia, neutropenia, diarrhea, asthenia/fatigue, and peripheral neuropathy. About 7% of patients in both arms died while on treatment. ![]()
Advanced age no barrier to continuous myeloma regimen
VIENNA – Elderly patients over age 75 with newly diagnosed multiple myeloma derive the same survival benefits from continuous lenalidomide and low-dose dexamethasone as those under 75, according to a new analysis of the pivotal phase III FIRST trial.
In those older than 75 years, continuous lenalidomide (Revlimid) and low-dose dexamethasone demonstrated a 14-month overall survival advantage (hazard ratio, 0.72; 95% confidence interval, 0.54-0.96) and 20% reduction in the risk of progression or death (HR, 0.80; 95% CI, 0.62-1.03) compared with melphalan (Alkeran) plus prednisone and thalidomide (MPT).
“With dose adjustment and monitoring, this continuous len-dex arm was effective and safe, even in very elderly and frail patients. This [trial] establishes this regimen as a global standard of care for transplant-ineligible patients,” Dr. Thierry Facon said at the annual congress of the European Hematology Association.
FIRST is the largest randomized trial in this setting and allocated 1,623 patients to lenalidomide plus low-dose dexamethasone in 28-day cycles until disease progression (Rd continuous) or 18 cycles of the same regimen for 72 weeks (Rd 18) or 12 cycles of MPT for 72 weeks.
In an interim analysis published in the New England Journal of Medicine (2014 [doi:10.1056/nejmoa1402551]) treatment with Rd continuous reduced the risk of progression or death by 28% and the risk of death by 22%, compared with MPT, a standard therapy for transplant-ineligible patients.
The new analysis is important because it is the first to examine the impact of age on the efficacy and safety of Rd continuous. Multiple myeloma is a disease of the elderly, with roughly one-third of patients diagnosed at more than 75 years, according to Dr. Facon of University Hospital Huriez, Lille, France.
Overall, 567 patients were older than 75 years (median 79 years) and 1,056 were 75 years or less (median 70 years). Starting doses for the very elderly group were reduced from 40 mg to 20 mg for dexamethasone; from 200 mg to 100 mg for thalidomide; and from 0.25 mg/kg to 0.20 mg/kg for melphalan. In patients with low blood count or impaired renal function, melphalan dose was reduced from 0.125 kg/mg to 0.10 mg/kg. All patients received thromboprophylaxis.
Median progression-free survival (PFS) in the 75-year and younger group was 28.1 months with Rd continuous, 21.6 months with Rd 18, and 22.4 months with MPT (Rd continuous vs. MPT: HR, 0.64; 95% CI, 0.53-0.77). The 4-year PFS rates were 37%, 15%, and 13%, Dr. Facon said.
In the very elderly group, median PFS reached 20.3 months, 19.4 months, and 19.8 months (HR, 0.80, also noted above), with 4-year PFS rates of 26%, 10%, and 11%.
“This is something quite important, illustrating the benefit of continuous therapy in terms of PFS,” he said.
Of note, median PFS in the interim analysis was similar at 25.5 months for Rd continuous, 20.7 months for Rd 18, and 21.2 months for MPT.
In the new analysis, overall survival in the 75 years and younger group was 60.9 months with Rd continuous, 60.6 months with Rd 18, and 55.3 months with MPT (Rd continuous vs. MPT: HR, 0.76, 95% CI, 0.60-0.96). The 4-year overall survival (OS) rates were 64%, 61%, and 57%.
Among the very elderly, median OS was 52.3 months with Rd continuous, 45.7 with Rd 18, and 37.8 months with MPT (HR, 0.72, also noted above), with 4-year OS rates of 52%, 48%, and 39%.
Duration of response was improved with Rd continuous treatment, irrespective of age, Dr. Facon said. The median duration for Rd continuous was 37 months in those aged 75 years and younger and 27 months in the very elderly, compared with 21-22 months for all other treatments.
Dose reductions due to adverse events were less common in those aged 75 years and under for Rd continuous than for MPT (37% vs. 52%), as were treatment discontinuations (21% vs. 26%). More very elderly patients required dose reductions for Rd continuous than MPT (44% vs. 36%), but fewer went on to discontinue Rd continuous (26% vs 29%), he said.
Rates of grade 3/4 neutropenia, the most common hematologic adverse event occurring in at least 5% of patients, were lower with Rd continuous and Rd 18 than with MPT in those aged 75 years and younger (28% vs. 25% vs. 47%) and in the very elderly (29% vs. 29% vs. 40%).
There is possibly a difference in cardiac events, which moved from 6% with MPT to 12% with Rd continuous in patients aged 75 years and younger and from 13% with MPT to 12% with Rd continuous in the very elderly, “but otherwise the results were quite similar, especially for neurologic toxicity and thromboembolic events,” he said.
During a discussion of the results, Dr. Facon acknowledged that the survival difference between the Rd continuous and Rd 18 groups was marginal and said additional insights will come from the final survival analysis as well as the recently published quality of life analyses.
When asked whether he would prefer Rd to VMP (bortezomib, melphalan, and prednisone), Dr. Facon said both regimens are standards of care in transplant-ineligible myeloma patients and cautioned against making cross-trial comparisons between FIRST and the older VISTA study of VMP.
“I would just say that these two regimens are effective and safe regimens, and it is also a discussion with your patients,” he said. “You may say that’s an easy answer, but I think it’s a fair answer.”
In February, the Food and Drug Administration expanded the indication for lenalidomide in combination with dexamethasone to include patients with newly diagnosed multiple myeloma.
FIRST was funded by Intergroupe Francophone du Myélome and Celgene. Dr. Facon reported consulting for and honoraria from Celgene.
On Twitter @pwendl
VIENNA – Elderly patients over age 75 with newly diagnosed multiple myeloma derive the same survival benefits from continuous lenalidomide and low-dose dexamethasone as those under 75, according to a new analysis of the pivotal phase III FIRST trial.
In those older than 75 years, continuous lenalidomide (Revlimid) and low-dose dexamethasone demonstrated a 14-month overall survival advantage (hazard ratio, 0.72; 95% confidence interval, 0.54-0.96) and 20% reduction in the risk of progression or death (HR, 0.80; 95% CI, 0.62-1.03) compared with melphalan (Alkeran) plus prednisone and thalidomide (MPT).
“With dose adjustment and monitoring, this continuous len-dex arm was effective and safe, even in very elderly and frail patients. This [trial] establishes this regimen as a global standard of care for transplant-ineligible patients,” Dr. Thierry Facon said at the annual congress of the European Hematology Association.
FIRST is the largest randomized trial in this setting and allocated 1,623 patients to lenalidomide plus low-dose dexamethasone in 28-day cycles until disease progression (Rd continuous) or 18 cycles of the same regimen for 72 weeks (Rd 18) or 12 cycles of MPT for 72 weeks.
In an interim analysis published in the New England Journal of Medicine (2014 [doi:10.1056/nejmoa1402551]) treatment with Rd continuous reduced the risk of progression or death by 28% and the risk of death by 22%, compared with MPT, a standard therapy for transplant-ineligible patients.
The new analysis is important because it is the first to examine the impact of age on the efficacy and safety of Rd continuous. Multiple myeloma is a disease of the elderly, with roughly one-third of patients diagnosed at more than 75 years, according to Dr. Facon of University Hospital Huriez, Lille, France.
Overall, 567 patients were older than 75 years (median 79 years) and 1,056 were 75 years or less (median 70 years). Starting doses for the very elderly group were reduced from 40 mg to 20 mg for dexamethasone; from 200 mg to 100 mg for thalidomide; and from 0.25 mg/kg to 0.20 mg/kg for melphalan. In patients with low blood count or impaired renal function, melphalan dose was reduced from 0.125 kg/mg to 0.10 mg/kg. All patients received thromboprophylaxis.
Median progression-free survival (PFS) in the 75-year and younger group was 28.1 months with Rd continuous, 21.6 months with Rd 18, and 22.4 months with MPT (Rd continuous vs. MPT: HR, 0.64; 95% CI, 0.53-0.77). The 4-year PFS rates were 37%, 15%, and 13%, Dr. Facon said.
In the very elderly group, median PFS reached 20.3 months, 19.4 months, and 19.8 months (HR, 0.80, also noted above), with 4-year PFS rates of 26%, 10%, and 11%.
“This is something quite important, illustrating the benefit of continuous therapy in terms of PFS,” he said.
Of note, median PFS in the interim analysis was similar at 25.5 months for Rd continuous, 20.7 months for Rd 18, and 21.2 months for MPT.
In the new analysis, overall survival in the 75 years and younger group was 60.9 months with Rd continuous, 60.6 months with Rd 18, and 55.3 months with MPT (Rd continuous vs. MPT: HR, 0.76, 95% CI, 0.60-0.96). The 4-year overall survival (OS) rates were 64%, 61%, and 57%.
Among the very elderly, median OS was 52.3 months with Rd continuous, 45.7 with Rd 18, and 37.8 months with MPT (HR, 0.72, also noted above), with 4-year OS rates of 52%, 48%, and 39%.
Duration of response was improved with Rd continuous treatment, irrespective of age, Dr. Facon said. The median duration for Rd continuous was 37 months in those aged 75 years and younger and 27 months in the very elderly, compared with 21-22 months for all other treatments.
Dose reductions due to adverse events were less common in those aged 75 years and under for Rd continuous than for MPT (37% vs. 52%), as were treatment discontinuations (21% vs. 26%). More very elderly patients required dose reductions for Rd continuous than MPT (44% vs. 36%), but fewer went on to discontinue Rd continuous (26% vs 29%), he said.
Rates of grade 3/4 neutropenia, the most common hematologic adverse event occurring in at least 5% of patients, were lower with Rd continuous and Rd 18 than with MPT in those aged 75 years and younger (28% vs. 25% vs. 47%) and in the very elderly (29% vs. 29% vs. 40%).
There is possibly a difference in cardiac events, which moved from 6% with MPT to 12% with Rd continuous in patients aged 75 years and younger and from 13% with MPT to 12% with Rd continuous in the very elderly, “but otherwise the results were quite similar, especially for neurologic toxicity and thromboembolic events,” he said.
During a discussion of the results, Dr. Facon acknowledged that the survival difference between the Rd continuous and Rd 18 groups was marginal and said additional insights will come from the final survival analysis as well as the recently published quality of life analyses.
When asked whether he would prefer Rd to VMP (bortezomib, melphalan, and prednisone), Dr. Facon said both regimens are standards of care in transplant-ineligible myeloma patients and cautioned against making cross-trial comparisons between FIRST and the older VISTA study of VMP.
“I would just say that these two regimens are effective and safe regimens, and it is also a discussion with your patients,” he said. “You may say that’s an easy answer, but I think it’s a fair answer.”
In February, the Food and Drug Administration expanded the indication for lenalidomide in combination with dexamethasone to include patients with newly diagnosed multiple myeloma.
FIRST was funded by Intergroupe Francophone du Myélome and Celgene. Dr. Facon reported consulting for and honoraria from Celgene.
On Twitter @pwendl
VIENNA – Elderly patients over age 75 with newly diagnosed multiple myeloma derive the same survival benefits from continuous lenalidomide and low-dose dexamethasone as those under 75, according to a new analysis of the pivotal phase III FIRST trial.
In those older than 75 years, continuous lenalidomide (Revlimid) and low-dose dexamethasone demonstrated a 14-month overall survival advantage (hazard ratio, 0.72; 95% confidence interval, 0.54-0.96) and 20% reduction in the risk of progression or death (HR, 0.80; 95% CI, 0.62-1.03) compared with melphalan (Alkeran) plus prednisone and thalidomide (MPT).
“With dose adjustment and monitoring, this continuous len-dex arm was effective and safe, even in very elderly and frail patients. This [trial] establishes this regimen as a global standard of care for transplant-ineligible patients,” Dr. Thierry Facon said at the annual congress of the European Hematology Association.
FIRST is the largest randomized trial in this setting and allocated 1,623 patients to lenalidomide plus low-dose dexamethasone in 28-day cycles until disease progression (Rd continuous) or 18 cycles of the same regimen for 72 weeks (Rd 18) or 12 cycles of MPT for 72 weeks.
In an interim analysis published in the New England Journal of Medicine (2014 [doi:10.1056/nejmoa1402551]) treatment with Rd continuous reduced the risk of progression or death by 28% and the risk of death by 22%, compared with MPT, a standard therapy for transplant-ineligible patients.
The new analysis is important because it is the first to examine the impact of age on the efficacy and safety of Rd continuous. Multiple myeloma is a disease of the elderly, with roughly one-third of patients diagnosed at more than 75 years, according to Dr. Facon of University Hospital Huriez, Lille, France.
Overall, 567 patients were older than 75 years (median 79 years) and 1,056 were 75 years or less (median 70 years). Starting doses for the very elderly group were reduced from 40 mg to 20 mg for dexamethasone; from 200 mg to 100 mg for thalidomide; and from 0.25 mg/kg to 0.20 mg/kg for melphalan. In patients with low blood count or impaired renal function, melphalan dose was reduced from 0.125 kg/mg to 0.10 mg/kg. All patients received thromboprophylaxis.
Median progression-free survival (PFS) in the 75-year and younger group was 28.1 months with Rd continuous, 21.6 months with Rd 18, and 22.4 months with MPT (Rd continuous vs. MPT: HR, 0.64; 95% CI, 0.53-0.77). The 4-year PFS rates were 37%, 15%, and 13%, Dr. Facon said.
In the very elderly group, median PFS reached 20.3 months, 19.4 months, and 19.8 months (HR, 0.80, also noted above), with 4-year PFS rates of 26%, 10%, and 11%.
“This is something quite important, illustrating the benefit of continuous therapy in terms of PFS,” he said.
Of note, median PFS in the interim analysis was similar at 25.5 months for Rd continuous, 20.7 months for Rd 18, and 21.2 months for MPT.
In the new analysis, overall survival in the 75 years and younger group was 60.9 months with Rd continuous, 60.6 months with Rd 18, and 55.3 months with MPT (Rd continuous vs. MPT: HR, 0.76, 95% CI, 0.60-0.96). The 4-year overall survival (OS) rates were 64%, 61%, and 57%.
Among the very elderly, median OS was 52.3 months with Rd continuous, 45.7 with Rd 18, and 37.8 months with MPT (HR, 0.72, also noted above), with 4-year OS rates of 52%, 48%, and 39%.
Duration of response was improved with Rd continuous treatment, irrespective of age, Dr. Facon said. The median duration for Rd continuous was 37 months in those aged 75 years and younger and 27 months in the very elderly, compared with 21-22 months for all other treatments.
Dose reductions due to adverse events were less common in those aged 75 years and under for Rd continuous than for MPT (37% vs. 52%), as were treatment discontinuations (21% vs. 26%). More very elderly patients required dose reductions for Rd continuous than MPT (44% vs. 36%), but fewer went on to discontinue Rd continuous (26% vs 29%), he said.
Rates of grade 3/4 neutropenia, the most common hematologic adverse event occurring in at least 5% of patients, were lower with Rd continuous and Rd 18 than with MPT in those aged 75 years and younger (28% vs. 25% vs. 47%) and in the very elderly (29% vs. 29% vs. 40%).
There is possibly a difference in cardiac events, which moved from 6% with MPT to 12% with Rd continuous in patients aged 75 years and younger and from 13% with MPT to 12% with Rd continuous in the very elderly, “but otherwise the results were quite similar, especially for neurologic toxicity and thromboembolic events,” he said.
During a discussion of the results, Dr. Facon acknowledged that the survival difference between the Rd continuous and Rd 18 groups was marginal and said additional insights will come from the final survival analysis as well as the recently published quality of life analyses.
When asked whether he would prefer Rd to VMP (bortezomib, melphalan, and prednisone), Dr. Facon said both regimens are standards of care in transplant-ineligible myeloma patients and cautioned against making cross-trial comparisons between FIRST and the older VISTA study of VMP.
“I would just say that these two regimens are effective and safe regimens, and it is also a discussion with your patients,” he said. “You may say that’s an easy answer, but I think it’s a fair answer.”
In February, the Food and Drug Administration expanded the indication for lenalidomide in combination with dexamethasone to include patients with newly diagnosed multiple myeloma.
FIRST was funded by Intergroupe Francophone du Myélome and Celgene. Dr. Facon reported consulting for and honoraria from Celgene.
On Twitter @pwendl
AT THE EHA CONGRESS
Key clinical point: Patients over age 75 draw the same survival benefit with continuous lenalidomide plus low-dose dexamethasone over MPT as their younger counterparts.
Major finding: Continuous lenalidomide plus low-dose dexamethasone provided a 14-month overall survival advantage and 20% reduction in the risk of progression or death, compared with MPT in patients over age 75.
Data source: Phase III trial in 1,623 transplant-ineligible patients with newly diagnosed multiple myeloma.
Disclosures: FIRST was funded by Intergroupe Francophone du Myélome and Celgene. Dr. Facon reported consulting for and honoraria from Celgene.
Nivolumab produces ‘dramatic’ responses in HL

Photo courtesy of UCLA
LUGANO—The PD-1 checkpoint inhibitor nivolumab produces rapid, durable, and, in some cases, “dramatic” responses in Hodgkin lymphoma (HL), according to a speaker at the 13th International Congress on Malignant Lymphoma.
The drug has also produced durable responses in follicular lymphoma (FL), cutaneous T-cell lymphoma (CTCL), and peripheral T-cell lymphoma (PTCL), although patient numbers for these malignancies are small.
John Timmerman, MD, of the University of California, Los Angeles, presented these results from a phase 1 study of patients with relapsed or refractory lymphoid malignancies and chronic HL (abstract 010).
Bristol-Myers Squibb and Ono Pharmaceutical Company are sponsors of the trial.
Original results of the study, with a data cutoff of June 2014, were reported at ASH 2014, with 40 weeks of median follow-up.
The update presented at 13-ICML, with a data lock in April 2015, includes an additional 10 months of data, for a median follow-up of 76 weeks.
Investigators enrolled 105 patients in this dose-escalation study to receive nivolumab at 1 mg/kg, then 3 mg/kg, every 2 weeks for 2 years.
Twenty-three patients had HL. Thirty-one had B-cell non-Hodgkin lymphoma (NHL), including 11 with FL and 10 with diffuse large B-cell lymphoma (DLBCL).
Twenty-three patients had T-cell NHL, including 5 with PTCL and 13 with CTCL/mycosis fungoides (MF). Twenty-seven patients had multiple myeloma (MM), and 1 had chronic myeloid leukemia.
Patients were heavily pretreated. Seventy-eight percent of HL patients and 26% of T-NHL patients had prior brentuximab vedotin. And 78% (HL), 14% (B-NHL), 9% (T-NHL), and 56% (MM) of patients had a prior autologous transplant.
The median number of prior therapies was 5 (range, 2-15) for HL patients and ranged from 1 to 16 for all patients.
The study’s primary endpoint was safety and tolerability, and the secondary endpoint was efficacy.
Safety and tolerability
Ninety-seven percent of patients had an adverse event, 69% of them related to study treatment and 21% of them treatment-related grade 3-4 events.
Fifteen patients (14%) discontinued treatment due to a related adverse event, including 3 with pneumonitis and 1 each with enteritis, stomatitis, pancreatitis, rash, conjunctivitis, sepsis, diplopia, myositis, neutropenia, myelodysplastic syndrome, increased creatinine phosphokinase, and peripheral neuropathy.
“Immune-related adverse events were generally seen early on and generally of low grade,” Dr Timmerman said. “However, it is notable that there were several grade 3 immune-related adverse events that can be seen as far as 6 months out after the start of therapy.”
These included skin, gastrointestinal, and pulmonary events. Most immune-related adverse events (83%) were resolved using protocol-prescribed procedures.
Efficacy
The overall response rate was 87% for HL, 36% for DLBCL, 40% for FL, 15% for CTCL/MF, 40% for PTCL, and 4% for MM.
Dr Timmerman pointed out that, since ASH, 2 additional conversions from partial response (PR) to complete response (CR) occurred in patients with HL. To date, 6 of 23 HL patients have achieved a CR and 14 a PR.
In B-cell NHL, there were additional conversions from PR to CR in DLBCL, while responses remained the same in FL and in the 4 responders with T-cell lymphomas.
“Intriguingly, there has been 1 late CR in the multiple myeloma cohort, which previously had shown no responses,” Dr Timmerman said.
Durability of response
This study suggests PD-1 blockade can produce durable responses in hematologic malignancies, as it does in melanoma and renal cell carcinoma.
In HL, the median response duration at a median follow-up of 86 weeks has not yet been reached, and half (n=10) of the responses are still ongoing.
In FL, CTCL, and PTCL, the median response duration has not been reached at a median follow-up of 81, 43, and 31 weeks, respectively. Of note, there are ongoing responses in at least half of patients in these tumor types.
In HL, none of the 6 patients in CR has progressed, although there have been some progressions in the PR group.
The rapidity of responses is also notable, Dr Timmerman said.
“[I]t’s very interesting that some patients have resolution of symptoms and improvement of symptoms within even 1 day of starting nivolumab therapy,” he said.
And responses to nivolumab in HL “can be very dramatic,” he added, as illustrated in the following case from the Mayo Clinic.
A patient with multiple sites of bulky FDG-avid tumors was scheduled to enter hospice. But first, he entered the nivolumab trial. Within 6 weeks of initiating treatment, he had achieved a near-CR. This response has been maintained for 2 years.
“The occurrence of very durable responses in the PR and CR groups has led us to question whether patients should go on to allogeneic stem cell transplantation after achieving responses with nivolumab or, rather, continue on nivolumab as long as their response remains,” Dr Timmerman said.
He added that an international, phase 2 trial in HL is underway and is accruing briskly.
Nivolumab was awarded breakthrough designation by the US Food and Drug Administration last year. Breakthrough designation is intended to expedite the development and review of drugs for serious or life-threatening conditions. ![]()

Photo courtesy of UCLA
LUGANO—The PD-1 checkpoint inhibitor nivolumab produces rapid, durable, and, in some cases, “dramatic” responses in Hodgkin lymphoma (HL), according to a speaker at the 13th International Congress on Malignant Lymphoma.
The drug has also produced durable responses in follicular lymphoma (FL), cutaneous T-cell lymphoma (CTCL), and peripheral T-cell lymphoma (PTCL), although patient numbers for these malignancies are small.
John Timmerman, MD, of the University of California, Los Angeles, presented these results from a phase 1 study of patients with relapsed or refractory lymphoid malignancies and chronic HL (abstract 010).
Bristol-Myers Squibb and Ono Pharmaceutical Company are sponsors of the trial.
Original results of the study, with a data cutoff of June 2014, were reported at ASH 2014, with 40 weeks of median follow-up.
The update presented at 13-ICML, with a data lock in April 2015, includes an additional 10 months of data, for a median follow-up of 76 weeks.
Investigators enrolled 105 patients in this dose-escalation study to receive nivolumab at 1 mg/kg, then 3 mg/kg, every 2 weeks for 2 years.
Twenty-three patients had HL. Thirty-one had B-cell non-Hodgkin lymphoma (NHL), including 11 with FL and 10 with diffuse large B-cell lymphoma (DLBCL).
Twenty-three patients had T-cell NHL, including 5 with PTCL and 13 with CTCL/mycosis fungoides (MF). Twenty-seven patients had multiple myeloma (MM), and 1 had chronic myeloid leukemia.
Patients were heavily pretreated. Seventy-eight percent of HL patients and 26% of T-NHL patients had prior brentuximab vedotin. And 78% (HL), 14% (B-NHL), 9% (T-NHL), and 56% (MM) of patients had a prior autologous transplant.
The median number of prior therapies was 5 (range, 2-15) for HL patients and ranged from 1 to 16 for all patients.
The study’s primary endpoint was safety and tolerability, and the secondary endpoint was efficacy.
Safety and tolerability
Ninety-seven percent of patients had an adverse event, 69% of them related to study treatment and 21% of them treatment-related grade 3-4 events.
Fifteen patients (14%) discontinued treatment due to a related adverse event, including 3 with pneumonitis and 1 each with enteritis, stomatitis, pancreatitis, rash, conjunctivitis, sepsis, diplopia, myositis, neutropenia, myelodysplastic syndrome, increased creatinine phosphokinase, and peripheral neuropathy.
“Immune-related adverse events were generally seen early on and generally of low grade,” Dr Timmerman said. “However, it is notable that there were several grade 3 immune-related adverse events that can be seen as far as 6 months out after the start of therapy.”
These included skin, gastrointestinal, and pulmonary events. Most immune-related adverse events (83%) were resolved using protocol-prescribed procedures.
Efficacy
The overall response rate was 87% for HL, 36% for DLBCL, 40% for FL, 15% for CTCL/MF, 40% for PTCL, and 4% for MM.
Dr Timmerman pointed out that, since ASH, 2 additional conversions from partial response (PR) to complete response (CR) occurred in patients with HL. To date, 6 of 23 HL patients have achieved a CR and 14 a PR.
In B-cell NHL, there were additional conversions from PR to CR in DLBCL, while responses remained the same in FL and in the 4 responders with T-cell lymphomas.
“Intriguingly, there has been 1 late CR in the multiple myeloma cohort, which previously had shown no responses,” Dr Timmerman said.
Durability of response
This study suggests PD-1 blockade can produce durable responses in hematologic malignancies, as it does in melanoma and renal cell carcinoma.
In HL, the median response duration at a median follow-up of 86 weeks has not yet been reached, and half (n=10) of the responses are still ongoing.
In FL, CTCL, and PTCL, the median response duration has not been reached at a median follow-up of 81, 43, and 31 weeks, respectively. Of note, there are ongoing responses in at least half of patients in these tumor types.
In HL, none of the 6 patients in CR has progressed, although there have been some progressions in the PR group.
The rapidity of responses is also notable, Dr Timmerman said.
“[I]t’s very interesting that some patients have resolution of symptoms and improvement of symptoms within even 1 day of starting nivolumab therapy,” he said.
And responses to nivolumab in HL “can be very dramatic,” he added, as illustrated in the following case from the Mayo Clinic.
A patient with multiple sites of bulky FDG-avid tumors was scheduled to enter hospice. But first, he entered the nivolumab trial. Within 6 weeks of initiating treatment, he had achieved a near-CR. This response has been maintained for 2 years.
“The occurrence of very durable responses in the PR and CR groups has led us to question whether patients should go on to allogeneic stem cell transplantation after achieving responses with nivolumab or, rather, continue on nivolumab as long as their response remains,” Dr Timmerman said.
He added that an international, phase 2 trial in HL is underway and is accruing briskly.
Nivolumab was awarded breakthrough designation by the US Food and Drug Administration last year. Breakthrough designation is intended to expedite the development and review of drugs for serious or life-threatening conditions. ![]()

Photo courtesy of UCLA
LUGANO—The PD-1 checkpoint inhibitor nivolumab produces rapid, durable, and, in some cases, “dramatic” responses in Hodgkin lymphoma (HL), according to a speaker at the 13th International Congress on Malignant Lymphoma.
The drug has also produced durable responses in follicular lymphoma (FL), cutaneous T-cell lymphoma (CTCL), and peripheral T-cell lymphoma (PTCL), although patient numbers for these malignancies are small.
John Timmerman, MD, of the University of California, Los Angeles, presented these results from a phase 1 study of patients with relapsed or refractory lymphoid malignancies and chronic HL (abstract 010).
Bristol-Myers Squibb and Ono Pharmaceutical Company are sponsors of the trial.
Original results of the study, with a data cutoff of June 2014, were reported at ASH 2014, with 40 weeks of median follow-up.
The update presented at 13-ICML, with a data lock in April 2015, includes an additional 10 months of data, for a median follow-up of 76 weeks.
Investigators enrolled 105 patients in this dose-escalation study to receive nivolumab at 1 mg/kg, then 3 mg/kg, every 2 weeks for 2 years.
Twenty-three patients had HL. Thirty-one had B-cell non-Hodgkin lymphoma (NHL), including 11 with FL and 10 with diffuse large B-cell lymphoma (DLBCL).
Twenty-three patients had T-cell NHL, including 5 with PTCL and 13 with CTCL/mycosis fungoides (MF). Twenty-seven patients had multiple myeloma (MM), and 1 had chronic myeloid leukemia.
Patients were heavily pretreated. Seventy-eight percent of HL patients and 26% of T-NHL patients had prior brentuximab vedotin. And 78% (HL), 14% (B-NHL), 9% (T-NHL), and 56% (MM) of patients had a prior autologous transplant.
The median number of prior therapies was 5 (range, 2-15) for HL patients and ranged from 1 to 16 for all patients.
The study’s primary endpoint was safety and tolerability, and the secondary endpoint was efficacy.
Safety and tolerability
Ninety-seven percent of patients had an adverse event, 69% of them related to study treatment and 21% of them treatment-related grade 3-4 events.
Fifteen patients (14%) discontinued treatment due to a related adverse event, including 3 with pneumonitis and 1 each with enteritis, stomatitis, pancreatitis, rash, conjunctivitis, sepsis, diplopia, myositis, neutropenia, myelodysplastic syndrome, increased creatinine phosphokinase, and peripheral neuropathy.
“Immune-related adverse events were generally seen early on and generally of low grade,” Dr Timmerman said. “However, it is notable that there were several grade 3 immune-related adverse events that can be seen as far as 6 months out after the start of therapy.”
These included skin, gastrointestinal, and pulmonary events. Most immune-related adverse events (83%) were resolved using protocol-prescribed procedures.
Efficacy
The overall response rate was 87% for HL, 36% for DLBCL, 40% for FL, 15% for CTCL/MF, 40% for PTCL, and 4% for MM.
Dr Timmerman pointed out that, since ASH, 2 additional conversions from partial response (PR) to complete response (CR) occurred in patients with HL. To date, 6 of 23 HL patients have achieved a CR and 14 a PR.
In B-cell NHL, there were additional conversions from PR to CR in DLBCL, while responses remained the same in FL and in the 4 responders with T-cell lymphomas.
“Intriguingly, there has been 1 late CR in the multiple myeloma cohort, which previously had shown no responses,” Dr Timmerman said.
Durability of response
This study suggests PD-1 blockade can produce durable responses in hematologic malignancies, as it does in melanoma and renal cell carcinoma.
In HL, the median response duration at a median follow-up of 86 weeks has not yet been reached, and half (n=10) of the responses are still ongoing.
In FL, CTCL, and PTCL, the median response duration has not been reached at a median follow-up of 81, 43, and 31 weeks, respectively. Of note, there are ongoing responses in at least half of patients in these tumor types.
In HL, none of the 6 patients in CR has progressed, although there have been some progressions in the PR group.
The rapidity of responses is also notable, Dr Timmerman said.
“[I]t’s very interesting that some patients have resolution of symptoms and improvement of symptoms within even 1 day of starting nivolumab therapy,” he said.
And responses to nivolumab in HL “can be very dramatic,” he added, as illustrated in the following case from the Mayo Clinic.
A patient with multiple sites of bulky FDG-avid tumors was scheduled to enter hospice. But first, he entered the nivolumab trial. Within 6 weeks of initiating treatment, he had achieved a near-CR. This response has been maintained for 2 years.
“The occurrence of very durable responses in the PR and CR groups has led us to question whether patients should go on to allogeneic stem cell transplantation after achieving responses with nivolumab or, rather, continue on nivolumab as long as their response remains,” Dr Timmerman said.
He added that an international, phase 2 trial in HL is underway and is accruing briskly.
Nivolumab was awarded breakthrough designation by the US Food and Drug Administration last year. Breakthrough designation is intended to expedite the development and review of drugs for serious or life-threatening conditions. ![]()
FDA grants vaccine orphan designation for MM

The US Food and Drug Administration (FDA) has granted a novel vaccine orphan designation as a treatment for multiple myeloma (MM).
The vaccine, known as ImMucin, targets the signal peptide domain of the MUC1 tumor antigen.
ImMucin works by “teaching” the immune system to identify and destroy cells that display a short, specific, 21-mer portion from MUC1, which appears on 90% of all cancer cells but not in patients’ blood.
Results of a phase 1/2 trial suggested that ImMucin was safe and active in MM patients. The trial included 15 MUC1-positive patients who had residual or biochemically progressive disease after autologous stem cell transplant.
The patients received 6 or 12 bi-weekly intradermal doses of ImMucin co-administered with human granulocyte-macrophage colony-stimulating factor.
The researchers said the vaccine was well-tolerated, as all adverse events were temporary, grade 1-2 in nature, and resolved spontaneously.
There was a significant decrease in soluble MUC1 levels in 9 patients, and 11 patients had stable disease or clinical improvement that persisted for 17.5 months to more than 41.3 months.
A follow-on study (which is ongoing) in patients who responded to ImMucin has shown that some patients can go more than 4 years without requiring any further treatment for their disease.
ImMucin is under development by Vaxil Biotherapeutics Ltd. The vaccine also has orphan designation as a treatment for MM in the European Union.
About orphan designation
The FDA grants orphan designation to encourage companies to develop therapies for diseases that affect fewer than 200,000 individuals in the US.
Orphan designation provides a company with research and development tax credits, an opportunity to obtain grant funding, exemption from FDA application fees, and other benefits.
If the FDA approves ImMucin to treat patients with MM, orphan designation will provide Vaxil Biotherapeutics with 7 years of marketing exclusivity in the US. ![]()

The US Food and Drug Administration (FDA) has granted a novel vaccine orphan designation as a treatment for multiple myeloma (MM).
The vaccine, known as ImMucin, targets the signal peptide domain of the MUC1 tumor antigen.
ImMucin works by “teaching” the immune system to identify and destroy cells that display a short, specific, 21-mer portion from MUC1, which appears on 90% of all cancer cells but not in patients’ blood.
Results of a phase 1/2 trial suggested that ImMucin was safe and active in MM patients. The trial included 15 MUC1-positive patients who had residual or biochemically progressive disease after autologous stem cell transplant.
The patients received 6 or 12 bi-weekly intradermal doses of ImMucin co-administered with human granulocyte-macrophage colony-stimulating factor.
The researchers said the vaccine was well-tolerated, as all adverse events were temporary, grade 1-2 in nature, and resolved spontaneously.
There was a significant decrease in soluble MUC1 levels in 9 patients, and 11 patients had stable disease or clinical improvement that persisted for 17.5 months to more than 41.3 months.
A follow-on study (which is ongoing) in patients who responded to ImMucin has shown that some patients can go more than 4 years without requiring any further treatment for their disease.
ImMucin is under development by Vaxil Biotherapeutics Ltd. The vaccine also has orphan designation as a treatment for MM in the European Union.
About orphan designation
The FDA grants orphan designation to encourage companies to develop therapies for diseases that affect fewer than 200,000 individuals in the US.
Orphan designation provides a company with research and development tax credits, an opportunity to obtain grant funding, exemption from FDA application fees, and other benefits.
If the FDA approves ImMucin to treat patients with MM, orphan designation will provide Vaxil Biotherapeutics with 7 years of marketing exclusivity in the US. ![]()

The US Food and Drug Administration (FDA) has granted a novel vaccine orphan designation as a treatment for multiple myeloma (MM).
The vaccine, known as ImMucin, targets the signal peptide domain of the MUC1 tumor antigen.
ImMucin works by “teaching” the immune system to identify and destroy cells that display a short, specific, 21-mer portion from MUC1, which appears on 90% of all cancer cells but not in patients’ blood.
Results of a phase 1/2 trial suggested that ImMucin was safe and active in MM patients. The trial included 15 MUC1-positive patients who had residual or biochemically progressive disease after autologous stem cell transplant.
The patients received 6 or 12 bi-weekly intradermal doses of ImMucin co-administered with human granulocyte-macrophage colony-stimulating factor.
The researchers said the vaccine was well-tolerated, as all adverse events were temporary, grade 1-2 in nature, and resolved spontaneously.
There was a significant decrease in soluble MUC1 levels in 9 patients, and 11 patients had stable disease or clinical improvement that persisted for 17.5 months to more than 41.3 months.
A follow-on study (which is ongoing) in patients who responded to ImMucin has shown that some patients can go more than 4 years without requiring any further treatment for their disease.
ImMucin is under development by Vaxil Biotherapeutics Ltd. The vaccine also has orphan designation as a treatment for MM in the European Union.
About orphan designation
The FDA grants orphan designation to encourage companies to develop therapies for diseases that affect fewer than 200,000 individuals in the US.
Orphan designation provides a company with research and development tax credits, an opportunity to obtain grant funding, exemption from FDA application fees, and other benefits.
If the FDA approves ImMucin to treat patients with MM, orphan designation will provide Vaxil Biotherapeutics with 7 years of marketing exclusivity in the US.
Combo shows promise for heavily pretreated MM
Image by Louis Heiser
and Robert Ackland
VIENNA—Combining a novel agent with dexamethasone can produce successful results where other treatments have failed, according to a presentation at the 20th Congress of the European Hematology Association.
Researchers tested low-dose dexamethasone in combination with melflufen, a peptidase-targeted therapy and antiangiogenic compound, in a phase 1/2 study of patients with relapsed or relapsed-refractory multiple myeloma (MM).
The treatment produced an overall response rate of 52%, and, although grade 3/4 hematologic adverse events were common, there were few serious adverse events related to melflufen.
These results were presented at the meeting as abstract P285.* The research was sponsored by Oncopeptides AB, the company developing melflufen.
Drug dosing and patient characteristics
In the phase 1 portion of this study, researchers evaluated 4 dose levels of melflufen—15 mg, 25 mg, 40 mg, and 55 mg—on day 1 with 40 mg of dexamethasone on days 1, 8, and 15 of 21-day cycles in a standard 3+3 design. Eight cycles of therapy were planned, but patients could continue on treatment if they experienced a clinical benefit.
There were no-dose limiting toxicities (DLTs) when melflufen was given at the 3 lower doses. However, 4 of the 6 patients who received the 55 mg dose experienced DLTs of prolonged and severe neutropenia and thrombocytopenia.
So the researchers said the MTD of melflufen, when combined with 40 mg of weekly dexamethasone, was 40 mg every 21 days.
In the ongoing phase 2 portion of the study, 29 patients have received melflufen at the MTD. The median time from the patients’ MM diagnosis to the first dose of melflufen was 5.5 years (range, 1-15), and their median number of prior therapies was 4 (range, 2-11).
Nineteen of the patients were refractory to an immunomodulatory drug (IMiD) or a proteasome inhibitor (PI); 11 were refractory to an alkylator; 10 were refractory to both an IMiD and a PI; and 5 were refractory to an IMiD, a PI, and an alkylator.
Safety data
Among the 29 patients in the phase 2 portion of the study, 22 had treatment-related grade 3-4 adverse events. These included thrombocytopenia (59%), neutropenia (48%), anemia (31%), leukopenia (21%), asthenia (7%), fatigue (7%), hyperglycemia (7%), and pyrexia/fever (7%).
To date, 12 serious adverse events have been reported in 8 of the phase 2 patients. Three events in 3 patients were considered related to melflufen—2 cases of febrile neutropenia and 1 case of pyrexia.
Fifteen patients discontinued therapy, 8 due to adverse events, 6 due to disease progression, and 1 after completing all planned cycles of treatment.
Efficacy data
Twenty-one patients were evaluable for efficacy according to the protocol, meaning they had received 2 or more cycles of therapy and completed response assessments after cycle 2.
Four patients withdrew from treatment after 1 cycle due to rapid disease progression and were included in a second response assessment (n=25). It was too early to evaluate the remaining 4 patients.
Among the 21 protocol-evaluable patients, the overall response rate was 52%, and the clinical benefit rate was 67%. Eleven patients achieved a partial response, 3 had a minimal response, 6 had stable disease, and 1 had progressive disease.
Among all 25 evaluable patients, the overall response rate was 44%, and the clinical benefit rate was 56%.
The median progression-free survival for these patients was 7.6 months (range, 3.4 months to not reached).
The researchers said enrollment in this trial is ongoing, with the goal of reaching 55 patients to further characterize the safety and efficacy of melflufen in heavily pretreated MM patients.
*Information in the abstract differs from that presented at the meeting.

Image by Louis Heiser
and Robert Ackland
VIENNA—Combining a novel agent with dexamethasone can produce successful results where other treatments have failed, according to a presentation at the 20th Congress of the European Hematology Association.
Researchers tested low-dose dexamethasone in combination with melflufen, a peptidase-targeted therapy and antiangiogenic compound, in a phase 1/2 study of patients with relapsed or relapsed-refractory multiple myeloma (MM).
The treatment produced an overall response rate of 52%, and, although grade 3/4 hematologic adverse events were common, there were few serious adverse events related to melflufen.
These results were presented at the meeting as abstract P285.* The research was sponsored by Oncopeptides AB, the company developing melflufen.
Drug dosing and patient characteristics
In the phase 1 portion of this study, researchers evaluated 4 dose levels of melflufen—15 mg, 25 mg, 40 mg, and 55 mg—on day 1 with 40 mg of dexamethasone on days 1, 8, and 15 of 21-day cycles in a standard 3+3 design. Eight cycles of therapy were planned, but patients could continue on treatment if they experienced a clinical benefit.
There were no-dose limiting toxicities (DLTs) when melflufen was given at the 3 lower doses. However, 4 of the 6 patients who received the 55 mg dose experienced DLTs of prolonged and severe neutropenia and thrombocytopenia.
So the researchers said the MTD of melflufen, when combined with 40 mg of weekly dexamethasone, was 40 mg every 21 days.
In the ongoing phase 2 portion of the study, 29 patients have received melflufen at the MTD. The median time from the patients’ MM diagnosis to the first dose of melflufen was 5.5 years (range, 1-15), and their median number of prior therapies was 4 (range, 2-11).
Nineteen of the patients were refractory to an immunomodulatory drug (IMiD) or a proteasome inhibitor (PI); 11 were refractory to an alkylator; 10 were refractory to both an IMiD and a PI; and 5 were refractory to an IMiD, a PI, and an alkylator.
Safety data
Among the 29 patients in the phase 2 portion of the study, 22 had treatment-related grade 3-4 adverse events. These included thrombocytopenia (59%), neutropenia (48%), anemia (31%), leukopenia (21%), asthenia (7%), fatigue (7%), hyperglycemia (7%), and pyrexia/fever (7%).
To date, 12 serious adverse events have been reported in 8 of the phase 2 patients. Three events in 3 patients were considered related to melflufen—2 cases of febrile neutropenia and 1 case of pyrexia.
Fifteen patients discontinued therapy, 8 due to adverse events, 6 due to disease progression, and 1 after completing all planned cycles of treatment.
Efficacy data
Twenty-one patients were evaluable for efficacy according to the protocol, meaning they had received 2 or more cycles of therapy and completed response assessments after cycle 2.
Four patients withdrew from treatment after 1 cycle due to rapid disease progression and were included in a second response assessment (n=25). It was too early to evaluate the remaining 4 patients.
Among the 21 protocol-evaluable patients, the overall response rate was 52%, and the clinical benefit rate was 67%. Eleven patients achieved a partial response, 3 had a minimal response, 6 had stable disease, and 1 had progressive disease.
Among all 25 evaluable patients, the overall response rate was 44%, and the clinical benefit rate was 56%.
The median progression-free survival for these patients was 7.6 months (range, 3.4 months to not reached).
The researchers said enrollment in this trial is ongoing, with the goal of reaching 55 patients to further characterize the safety and efficacy of melflufen in heavily pretreated MM patients.
*Information in the abstract differs from that presented at the meeting.

Image by Louis Heiser
and Robert Ackland
VIENNA—Combining a novel agent with dexamethasone can produce successful results where other treatments have failed, according to a presentation at the 20th Congress of the European Hematology Association.
Researchers tested low-dose dexamethasone in combination with melflufen, a peptidase-targeted therapy and antiangiogenic compound, in a phase 1/2 study of patients with relapsed or relapsed-refractory multiple myeloma (MM).
The treatment produced an overall response rate of 52%, and, although grade 3/4 hematologic adverse events were common, there were few serious adverse events related to melflufen.
These results were presented at the meeting as abstract P285.* The research was sponsored by Oncopeptides AB, the company developing melflufen.
Drug dosing and patient characteristics
In the phase 1 portion of this study, researchers evaluated 4 dose levels of melflufen—15 mg, 25 mg, 40 mg, and 55 mg—on day 1 with 40 mg of dexamethasone on days 1, 8, and 15 of 21-day cycles in a standard 3+3 design. Eight cycles of therapy were planned, but patients could continue on treatment if they experienced a clinical benefit.
There were no-dose limiting toxicities (DLTs) when melflufen was given at the 3 lower doses. However, 4 of the 6 patients who received the 55 mg dose experienced DLTs of prolonged and severe neutropenia and thrombocytopenia.
So the researchers said the MTD of melflufen, when combined with 40 mg of weekly dexamethasone, was 40 mg every 21 days.
In the ongoing phase 2 portion of the study, 29 patients have received melflufen at the MTD. The median time from the patients’ MM diagnosis to the first dose of melflufen was 5.5 years (range, 1-15), and their median number of prior therapies was 4 (range, 2-11).
Nineteen of the patients were refractory to an immunomodulatory drug (IMiD) or a proteasome inhibitor (PI); 11 were refractory to an alkylator; 10 were refractory to both an IMiD and a PI; and 5 were refractory to an IMiD, a PI, and an alkylator.
Safety data
Among the 29 patients in the phase 2 portion of the study, 22 had treatment-related grade 3-4 adverse events. These included thrombocytopenia (59%), neutropenia (48%), anemia (31%), leukopenia (21%), asthenia (7%), fatigue (7%), hyperglycemia (7%), and pyrexia/fever (7%).
To date, 12 serious adverse events have been reported in 8 of the phase 2 patients. Three events in 3 patients were considered related to melflufen—2 cases of febrile neutropenia and 1 case of pyrexia.
Fifteen patients discontinued therapy, 8 due to adverse events, 6 due to disease progression, and 1 after completing all planned cycles of treatment.
Efficacy data
Twenty-one patients were evaluable for efficacy according to the protocol, meaning they had received 2 or more cycles of therapy and completed response assessments after cycle 2.
Four patients withdrew from treatment after 1 cycle due to rapid disease progression and were included in a second response assessment (n=25). It was too early to evaluate the remaining 4 patients.
Among the 21 protocol-evaluable patients, the overall response rate was 52%, and the clinical benefit rate was 67%. Eleven patients achieved a partial response, 3 had a minimal response, 6 had stable disease, and 1 had progressive disease.
Among all 25 evaluable patients, the overall response rate was 44%, and the clinical benefit rate was 56%.
The median progression-free survival for these patients was 7.6 months (range, 3.4 months to not reached).
The researchers said enrollment in this trial is ongoing, with the goal of reaching 55 patients to further characterize the safety and efficacy of melflufen in heavily pretreated MM patients.
*Information in the abstract differs from that presented at the meeting.