User login
Core Principles More Essential Than Ever [editorial]
Skin of Color: What Every Dark Skinned Patient Should Know
Many blogs, articles, and tip sheets offer suggestions for keeping skin youthful and breakout free. But often the advice doesn’t apply to all skin types. Below are nine skin care tips modified for darker skin that you can share with your patients.
1. Don’t over wash.
Washing the face once a day to remove makeup, dirt, and bacteria can be helpful to avoid breakouts, especially in acne prone skin. However, it is important to remind patients to avoid over washing, as this may dry out the skin causing increased irritation, and may even cause wrinkles to look more prominent.
Sebum production decreases with age, especially after menopause in women. It may also be decreased in black patients, compared with white patients, as shown in a recent study (Cutis 2004;73:392-396), although the data were not statistically significant.
Patients should exercise caution when applying antiaging products after washing because washing allows antiagers to penetrate deeper, leading to faster results in most skin types, but may also lead to increased irritation and then postinflammatory hyperpigmentation in darker skin.
Gentle cleansers are best, unless the skin is especially acne prone. In this case, anti-acne cleansers with ingredients like salicylic acid, benzoyl peroxide, or glycolic acid may be useful. To refresh skin, a splash of lukewarm water should do.
2. Apply products with a lower pH.
Studies have shown pH to be lower in darker skin, compared with lighter skin. For darker skin, products that are slightly acidic, such as those that contain mild glycolic acid, can help maintain the skin’s pH balance and maintain homeostasis and barrier integrity.
3. Be UV obsessed.
While the epidermis of darker skin contains more melanin content and has increased melanosomal dispersion than lighter skin—providing increased protection against UV-induced skin cancers and photoaging—UV damage can still occur.
Many patients with darker skin feel they are immune to skin cancer. Patients with darker skin, while diagnosed less frequently with melanoma, die at an increased frequency from the disease because of later diagnosis. Using a sunscreen that is SPF 30 or higher that blocks both UVA and UVB wavelengths is essential.
Patients should be reminded that nothing is more important than wearing sunscreen every day to promote younger-looking skin and prevent skin cancer.
Sunscreens, especially those with a higher SPF, often do not rub in well on darker skin. Using a sunscreen with chemical blockers, or micronized physical blockers (zinc and titanium dioxide), may go on less chalky and rub in more smoothly.
Sun exposure in darker skin also leads to prolonged postinflammatory hyperpigmentation after any skin insult. Even 10 minutes of daily exposure to UVA can cause changes that lead to wrinkles and sunspots in as few as 12 weeks.
Also, advise patients to eat foods that are rich in vitamin D to avoid deficiency.
4. Manage stress.
Emotional upheavals can make a patient’s skin look 5 years older than his or her chronological age. Constant anxiety increases the stress hormone cortisol, which causes inflammation that breaks down collagen. It also triggers a chain of responses that can lead to facial redness and acne flare-ups. To quell inflammation, advise patients to eat antioxidant-rich foods such as berries, oranges, and asparagus.
5. Use a retinoid.
Vitamin A derivatives, such as topical retinoids, speed cell turnover and collagen growth to smooth fine lines and wrinkles and fade brown spots. Prescription-strength retinoids provide the fastest results—your patient should start to see changes in about a month.
To help skin adjust to any redness or peeling, advise patients to apply a pea-size drop to the face every third night, building up to nightly use. Milder over-the-counter versions are gentler, although it can take up to 3 months for users to see noticeable results.
Redness and peeling should absolutely be avoided in darker skin to avoid postinflammatory hyperpigmentation, so retinoids, while helpful, should be used cautiously.
6. Update your routine.
Advising patients to alter just one thing in their regimen every 6-12 months jump starts more impressive improvements in tone and texture. When products are applied consistently, skin slides into maintenance mode after about a year. To keep skin primed for rejuvenation, tell patients to substitute a cream that contains alpha hydroxy acids in place of a retinoid twice a week to boost benefits. Or, you can bump up the patient’s OTC retinoid to a prescription product.
7. Eat omega-3 fats.
These “good fats,” found in foods such as salmon, flaxseed, and almonds, boost hydration, which keeps skin supple and firm. The same is not true, however, of the saturated fat in dairy products and meats, which increase free-radical damage that makes skin more susceptible to aging. Advise patients to limit their intake of saturated fat to about 17 g per day.
8. Exercise regularly.
Studies find that women who work out regularly have firmer skin than non-exercisers. The reason: Exercise infuses skin with oxygen and nutrients needed for collagen production. Patients who aim to keep skin toned should make time for at least three, 30-minute, heart-pumping workouts per week.
9. Wash your hair.
Curly hair cannot be washed as often as straight hair because it dries out more readily. However, decreased hair washing leads to increased scalp sebum production, which can lead to increased breakouts.
If hair cannot be washed, patients should wrap their hair at night so it does not touch the face, and they should change their pillow cases frequently. In addition, many persons of African descent apply oils and pomades to their hair to keep it soft and manageable. Here, hair wrapping or increased washing is also essential to avoid “pomade acne.”
Many blogs, articles, and tip sheets offer suggestions for keeping skin youthful and breakout free. But often the advice doesn’t apply to all skin types. Below are nine skin care tips modified for darker skin that you can share with your patients.
1. Don’t over wash.
Washing the face once a day to remove makeup, dirt, and bacteria can be helpful to avoid breakouts, especially in acne prone skin. However, it is important to remind patients to avoid over washing, as this may dry out the skin causing increased irritation, and may even cause wrinkles to look more prominent.
Sebum production decreases with age, especially after menopause in women. It may also be decreased in black patients, compared with white patients, as shown in a recent study (Cutis 2004;73:392-396), although the data were not statistically significant.
Patients should exercise caution when applying antiaging products after washing because washing allows antiagers to penetrate deeper, leading to faster results in most skin types, but may also lead to increased irritation and then postinflammatory hyperpigmentation in darker skin.
Gentle cleansers are best, unless the skin is especially acne prone. In this case, anti-acne cleansers with ingredients like salicylic acid, benzoyl peroxide, or glycolic acid may be useful. To refresh skin, a splash of lukewarm water should do.
2. Apply products with a lower pH.
Studies have shown pH to be lower in darker skin, compared with lighter skin. For darker skin, products that are slightly acidic, such as those that contain mild glycolic acid, can help maintain the skin’s pH balance and maintain homeostasis and barrier integrity.
3. Be UV obsessed.
While the epidermis of darker skin contains more melanin content and has increased melanosomal dispersion than lighter skin—providing increased protection against UV-induced skin cancers and photoaging—UV damage can still occur.
Many patients with darker skin feel they are immune to skin cancer. Patients with darker skin, while diagnosed less frequently with melanoma, die at an increased frequency from the disease because of later diagnosis. Using a sunscreen that is SPF 30 or higher that blocks both UVA and UVB wavelengths is essential.
Patients should be reminded that nothing is more important than wearing sunscreen every day to promote younger-looking skin and prevent skin cancer.
Sunscreens, especially those with a higher SPF, often do not rub in well on darker skin. Using a sunscreen with chemical blockers, or micronized physical blockers (zinc and titanium dioxide), may go on less chalky and rub in more smoothly.
Sun exposure in darker skin also leads to prolonged postinflammatory hyperpigmentation after any skin insult. Even 10 minutes of daily exposure to UVA can cause changes that lead to wrinkles and sunspots in as few as 12 weeks.
Also, advise patients to eat foods that are rich in vitamin D to avoid deficiency.
4. Manage stress.
Emotional upheavals can make a patient’s skin look 5 years older than his or her chronological age. Constant anxiety increases the stress hormone cortisol, which causes inflammation that breaks down collagen. It also triggers a chain of responses that can lead to facial redness and acne flare-ups. To quell inflammation, advise patients to eat antioxidant-rich foods such as berries, oranges, and asparagus.
5. Use a retinoid.
Vitamin A derivatives, such as topical retinoids, speed cell turnover and collagen growth to smooth fine lines and wrinkles and fade brown spots. Prescription-strength retinoids provide the fastest results—your patient should start to see changes in about a month.
To help skin adjust to any redness or peeling, advise patients to apply a pea-size drop to the face every third night, building up to nightly use. Milder over-the-counter versions are gentler, although it can take up to 3 months for users to see noticeable results.
Redness and peeling should absolutely be avoided in darker skin to avoid postinflammatory hyperpigmentation, so retinoids, while helpful, should be used cautiously.
6. Update your routine.
Advising patients to alter just one thing in their regimen every 6-12 months jump starts more impressive improvements in tone and texture. When products are applied consistently, skin slides into maintenance mode after about a year. To keep skin primed for rejuvenation, tell patients to substitute a cream that contains alpha hydroxy acids in place of a retinoid twice a week to boost benefits. Or, you can bump up the patient’s OTC retinoid to a prescription product.
7. Eat omega-3 fats.
These “good fats,” found in foods such as salmon, flaxseed, and almonds, boost hydration, which keeps skin supple and firm. The same is not true, however, of the saturated fat in dairy products and meats, which increase free-radical damage that makes skin more susceptible to aging. Advise patients to limit their intake of saturated fat to about 17 g per day.
8. Exercise regularly.
Studies find that women who work out regularly have firmer skin than non-exercisers. The reason: Exercise infuses skin with oxygen and nutrients needed for collagen production. Patients who aim to keep skin toned should make time for at least three, 30-minute, heart-pumping workouts per week.
9. Wash your hair.
Curly hair cannot be washed as often as straight hair because it dries out more readily. However, decreased hair washing leads to increased scalp sebum production, which can lead to increased breakouts.
If hair cannot be washed, patients should wrap their hair at night so it does not touch the face, and they should change their pillow cases frequently. In addition, many persons of African descent apply oils and pomades to their hair to keep it soft and manageable. Here, hair wrapping or increased washing is also essential to avoid “pomade acne.”
Many blogs, articles, and tip sheets offer suggestions for keeping skin youthful and breakout free. But often the advice doesn’t apply to all skin types. Below are nine skin care tips modified for darker skin that you can share with your patients.
1. Don’t over wash.
Washing the face once a day to remove makeup, dirt, and bacteria can be helpful to avoid breakouts, especially in acne prone skin. However, it is important to remind patients to avoid over washing, as this may dry out the skin causing increased irritation, and may even cause wrinkles to look more prominent.
Sebum production decreases with age, especially after menopause in women. It may also be decreased in black patients, compared with white patients, as shown in a recent study (Cutis 2004;73:392-396), although the data were not statistically significant.
Patients should exercise caution when applying antiaging products after washing because washing allows antiagers to penetrate deeper, leading to faster results in most skin types, but may also lead to increased irritation and then postinflammatory hyperpigmentation in darker skin.
Gentle cleansers are best, unless the skin is especially acne prone. In this case, anti-acne cleansers with ingredients like salicylic acid, benzoyl peroxide, or glycolic acid may be useful. To refresh skin, a splash of lukewarm water should do.
2. Apply products with a lower pH.
Studies have shown pH to be lower in darker skin, compared with lighter skin. For darker skin, products that are slightly acidic, such as those that contain mild glycolic acid, can help maintain the skin’s pH balance and maintain homeostasis and barrier integrity.
3. Be UV obsessed.
While the epidermis of darker skin contains more melanin content and has increased melanosomal dispersion than lighter skin—providing increased protection against UV-induced skin cancers and photoaging—UV damage can still occur.
Many patients with darker skin feel they are immune to skin cancer. Patients with darker skin, while diagnosed less frequently with melanoma, die at an increased frequency from the disease because of later diagnosis. Using a sunscreen that is SPF 30 or higher that blocks both UVA and UVB wavelengths is essential.
Patients should be reminded that nothing is more important than wearing sunscreen every day to promote younger-looking skin and prevent skin cancer.
Sunscreens, especially those with a higher SPF, often do not rub in well on darker skin. Using a sunscreen with chemical blockers, or micronized physical blockers (zinc and titanium dioxide), may go on less chalky and rub in more smoothly.
Sun exposure in darker skin also leads to prolonged postinflammatory hyperpigmentation after any skin insult. Even 10 minutes of daily exposure to UVA can cause changes that lead to wrinkles and sunspots in as few as 12 weeks.
Also, advise patients to eat foods that are rich in vitamin D to avoid deficiency.
4. Manage stress.
Emotional upheavals can make a patient’s skin look 5 years older than his or her chronological age. Constant anxiety increases the stress hormone cortisol, which causes inflammation that breaks down collagen. It also triggers a chain of responses that can lead to facial redness and acne flare-ups. To quell inflammation, advise patients to eat antioxidant-rich foods such as berries, oranges, and asparagus.
5. Use a retinoid.
Vitamin A derivatives, such as topical retinoids, speed cell turnover and collagen growth to smooth fine lines and wrinkles and fade brown spots. Prescription-strength retinoids provide the fastest results—your patient should start to see changes in about a month.
To help skin adjust to any redness or peeling, advise patients to apply a pea-size drop to the face every third night, building up to nightly use. Milder over-the-counter versions are gentler, although it can take up to 3 months for users to see noticeable results.
Redness and peeling should absolutely be avoided in darker skin to avoid postinflammatory hyperpigmentation, so retinoids, while helpful, should be used cautiously.
6. Update your routine.
Advising patients to alter just one thing in their regimen every 6-12 months jump starts more impressive improvements in tone and texture. When products are applied consistently, skin slides into maintenance mode after about a year. To keep skin primed for rejuvenation, tell patients to substitute a cream that contains alpha hydroxy acids in place of a retinoid twice a week to boost benefits. Or, you can bump up the patient’s OTC retinoid to a prescription product.
7. Eat omega-3 fats.
These “good fats,” found in foods such as salmon, flaxseed, and almonds, boost hydration, which keeps skin supple and firm. The same is not true, however, of the saturated fat in dairy products and meats, which increase free-radical damage that makes skin more susceptible to aging. Advise patients to limit their intake of saturated fat to about 17 g per day.
8. Exercise regularly.
Studies find that women who work out regularly have firmer skin than non-exercisers. The reason: Exercise infuses skin with oxygen and nutrients needed for collagen production. Patients who aim to keep skin toned should make time for at least three, 30-minute, heart-pumping workouts per week.
9. Wash your hair.
Curly hair cannot be washed as often as straight hair because it dries out more readily. However, decreased hair washing leads to increased scalp sebum production, which can lead to increased breakouts.
If hair cannot be washed, patients should wrap their hair at night so it does not touch the face, and they should change their pillow cases frequently. In addition, many persons of African descent apply oils and pomades to their hair to keep it soft and manageable. Here, hair wrapping or increased washing is also essential to avoid “pomade acne.”
Implantable Antibiotic Sponge Fails to Reduce Surgical Wound Infection Rate
The use of implantable gentamicin-impregnated collagen sponges did not reduce the sternal wound infection rate following cardiac surgery in a prospective, randomized, controlled trial of 1,502 patients who were at high risk of infection because of diabetes and/or obesity.
Dr. Elliott Bennett-Guerrero of Duke University in Durham, N.C., and his colleagues reported their findings Aug. 18 in JAMA.
The findings directly contradicted those of a 2005 Swedish study, which found that the sponges reduced surgical wound infections by 53%, and which served as strong preliminary data for the current trial (Ann. Thoracic. Surg. 2005;79:153-62).
The sponges are approved in 54 countries, and the current phase III study was designed to "confirm these promising data and support regulatory approval in the United States." However, the overall wound infection rates at 90 days were statistically similar at 8.4% and 8.7%, respectively, in patients who received standard care plus surgical site implantation of two of the topical antibiotic sponges, and in patients who received standard care with no additional intervention, researchers found. There were 753 patients in the sponge group and 749 in the standard care group,
Like the overall wound infection rates, the superficial and deep sternal wound infection rates were also similar in the treatment and control groups, at 6.5% and 6.1%, and 1.9% and 2.5%, respectively. Additionally, no differences were seen between the treatment and control groups in regard to the rehospitalization rate for sternal wound infection (3.1% and 3.2%, respectively), or in ASEPSIS score (mean, 1.9 and. 2.0, respectively) the investigators found (JAMA 2010;304:755-62).
The ASEPSIS score is a measure of additional treatment, presence of serous discharge, erythema, purulent exudates, separation of the deep tissues, isolation of bacteria, and duration of inpatient stay. Points are assigned for each variable and the scale has a minimum score of 0, with no theoretical maximum, the investigators explained.
Patients in the single-blind study were enrolled at 48 U.S. centers between Dec. 21, 2007, and March 11, 2009. Those randomized to the treatment group underwent insertion of two sponges with a total gentamicin dose of 260 mg, which was the same dose used in the Swedish study. Both groups received standardized care with prophylactic systemic antibiotics and rigid sternal fixation, with the treatment group also undergoing implantation with the sponges.
The groups were balanced regarding baseline characteristics, including age, weight, diabetes, and smoking history, and also in regard to perioperative variables.
As for why the antibiotic sponges failed to reduce infection rates in this study as they did in the Swedish study, the investigators suggested that important quality control measures used in their study – but not in the Swedish study – might be to blame. They cited measures including on-site monitoring and source data verification, central adjudication of outcomes by an independent blinded committee, and the inclusion of a large number of hospitals (48 in the U.S. study, compared with 2 in the Swedish study).
The researchers also wrote that ethnic and regional differences, such as varying distribution of bacterial pathogens between countries, could also explain the differing outcomes. For example, no cases of methicillin-resistant Staphylococcus aureus occurred in the Swedish trial, but in the U.S. study 6.3% of patients had MRSA growth from sternal wound infection, which may not be sensitive to gentamicin.
"Thus, variations in the distribution of bacterial pathogens among countries could affect efficacy in a trial of infection prevention such as the present one" they said, also noting that the findings underscore the importance of large validation trials, as "positive single-center trials are often not confirmed in larger multicenter trials."
Disclosures: The U.S. study was sponsored by Innocoll Technologies Ltd., the maker of the gentamicin-collagen sponges, and Dr. Bennett-Guerrero reported that he is in discussions with Excited States LLC regarding a consulting agreement to advise on a clinical trial involving surgical wound infection prevention. Another author on the study, Dr. T. Bruce Ferguson Jr., reported receiving honoraria from Innocoll Technologies Ltd. for serving on a steering committee.
The use of implantable gentamicin-impregnated collagen sponges did not reduce the sternal wound infection rate following cardiac surgery in a prospective, randomized, controlled trial of 1,502 patients who were at high risk of infection because of diabetes and/or obesity.
Dr. Elliott Bennett-Guerrero of Duke University in Durham, N.C., and his colleagues reported their findings Aug. 18 in JAMA.
The findings directly contradicted those of a 2005 Swedish study, which found that the sponges reduced surgical wound infections by 53%, and which served as strong preliminary data for the current trial (Ann. Thoracic. Surg. 2005;79:153-62).
The sponges are approved in 54 countries, and the current phase III study was designed to "confirm these promising data and support regulatory approval in the United States." However, the overall wound infection rates at 90 days were statistically similar at 8.4% and 8.7%, respectively, in patients who received standard care plus surgical site implantation of two of the topical antibiotic sponges, and in patients who received standard care with no additional intervention, researchers found. There were 753 patients in the sponge group and 749 in the standard care group,
Like the overall wound infection rates, the superficial and deep sternal wound infection rates were also similar in the treatment and control groups, at 6.5% and 6.1%, and 1.9% and 2.5%, respectively. Additionally, no differences were seen between the treatment and control groups in regard to the rehospitalization rate for sternal wound infection (3.1% and 3.2%, respectively), or in ASEPSIS score (mean, 1.9 and. 2.0, respectively) the investigators found (JAMA 2010;304:755-62).
The ASEPSIS score is a measure of additional treatment, presence of serous discharge, erythema, purulent exudates, separation of the deep tissues, isolation of bacteria, and duration of inpatient stay. Points are assigned for each variable and the scale has a minimum score of 0, with no theoretical maximum, the investigators explained.
Patients in the single-blind study were enrolled at 48 U.S. centers between Dec. 21, 2007, and March 11, 2009. Those randomized to the treatment group underwent insertion of two sponges with a total gentamicin dose of 260 mg, which was the same dose used in the Swedish study. Both groups received standardized care with prophylactic systemic antibiotics and rigid sternal fixation, with the treatment group also undergoing implantation with the sponges.
The groups were balanced regarding baseline characteristics, including age, weight, diabetes, and smoking history, and also in regard to perioperative variables.
As for why the antibiotic sponges failed to reduce infection rates in this study as they did in the Swedish study, the investigators suggested that important quality control measures used in their study – but not in the Swedish study – might be to blame. They cited measures including on-site monitoring and source data verification, central adjudication of outcomes by an independent blinded committee, and the inclusion of a large number of hospitals (48 in the U.S. study, compared with 2 in the Swedish study).
The researchers also wrote that ethnic and regional differences, such as varying distribution of bacterial pathogens between countries, could also explain the differing outcomes. For example, no cases of methicillin-resistant Staphylococcus aureus occurred in the Swedish trial, but in the U.S. study 6.3% of patients had MRSA growth from sternal wound infection, which may not be sensitive to gentamicin.
"Thus, variations in the distribution of bacterial pathogens among countries could affect efficacy in a trial of infection prevention such as the present one" they said, also noting that the findings underscore the importance of large validation trials, as "positive single-center trials are often not confirmed in larger multicenter trials."
Disclosures: The U.S. study was sponsored by Innocoll Technologies Ltd., the maker of the gentamicin-collagen sponges, and Dr. Bennett-Guerrero reported that he is in discussions with Excited States LLC regarding a consulting agreement to advise on a clinical trial involving surgical wound infection prevention. Another author on the study, Dr. T. Bruce Ferguson Jr., reported receiving honoraria from Innocoll Technologies Ltd. for serving on a steering committee.
The use of implantable gentamicin-impregnated collagen sponges did not reduce the sternal wound infection rate following cardiac surgery in a prospective, randomized, controlled trial of 1,502 patients who were at high risk of infection because of diabetes and/or obesity.
Dr. Elliott Bennett-Guerrero of Duke University in Durham, N.C., and his colleagues reported their findings Aug. 18 in JAMA.
The findings directly contradicted those of a 2005 Swedish study, which found that the sponges reduced surgical wound infections by 53%, and which served as strong preliminary data for the current trial (Ann. Thoracic. Surg. 2005;79:153-62).
The sponges are approved in 54 countries, and the current phase III study was designed to "confirm these promising data and support regulatory approval in the United States." However, the overall wound infection rates at 90 days were statistically similar at 8.4% and 8.7%, respectively, in patients who received standard care plus surgical site implantation of two of the topical antibiotic sponges, and in patients who received standard care with no additional intervention, researchers found. There were 753 patients in the sponge group and 749 in the standard care group,
Like the overall wound infection rates, the superficial and deep sternal wound infection rates were also similar in the treatment and control groups, at 6.5% and 6.1%, and 1.9% and 2.5%, respectively. Additionally, no differences were seen between the treatment and control groups in regard to the rehospitalization rate for sternal wound infection (3.1% and 3.2%, respectively), or in ASEPSIS score (mean, 1.9 and. 2.0, respectively) the investigators found (JAMA 2010;304:755-62).
The ASEPSIS score is a measure of additional treatment, presence of serous discharge, erythema, purulent exudates, separation of the deep tissues, isolation of bacteria, and duration of inpatient stay. Points are assigned for each variable and the scale has a minimum score of 0, with no theoretical maximum, the investigators explained.
Patients in the single-blind study were enrolled at 48 U.S. centers between Dec. 21, 2007, and March 11, 2009. Those randomized to the treatment group underwent insertion of two sponges with a total gentamicin dose of 260 mg, which was the same dose used in the Swedish study. Both groups received standardized care with prophylactic systemic antibiotics and rigid sternal fixation, with the treatment group also undergoing implantation with the sponges.
The groups were balanced regarding baseline characteristics, including age, weight, diabetes, and smoking history, and also in regard to perioperative variables.
As for why the antibiotic sponges failed to reduce infection rates in this study as they did in the Swedish study, the investigators suggested that important quality control measures used in their study – but not in the Swedish study – might be to blame. They cited measures including on-site monitoring and source data verification, central adjudication of outcomes by an independent blinded committee, and the inclusion of a large number of hospitals (48 in the U.S. study, compared with 2 in the Swedish study).
The researchers also wrote that ethnic and regional differences, such as varying distribution of bacterial pathogens between countries, could also explain the differing outcomes. For example, no cases of methicillin-resistant Staphylococcus aureus occurred in the Swedish trial, but in the U.S. study 6.3% of patients had MRSA growth from sternal wound infection, which may not be sensitive to gentamicin.
"Thus, variations in the distribution of bacterial pathogens among countries could affect efficacy in a trial of infection prevention such as the present one" they said, also noting that the findings underscore the importance of large validation trials, as "positive single-center trials are often not confirmed in larger multicenter trials."
Disclosures: The U.S. study was sponsored by Innocoll Technologies Ltd., the maker of the gentamicin-collagen sponges, and Dr. Bennett-Guerrero reported that he is in discussions with Excited States LLC regarding a consulting agreement to advise on a clinical trial involving surgical wound infection prevention. Another author on the study, Dr. T. Bruce Ferguson Jr., reported receiving honoraria from Innocoll Technologies Ltd. for serving on a steering committee.
Expertise Crucial in Filler Correction
NAPLES, Fla. - Dermatologists know best how to prevent and to correct facial filler complications, compared with medi-spa aestheticians and other employees, Dr. Oscar Hevia said.
“Our ability to identify, treat, and correct our complications [is what will set us apart]. It’s all about experience,” Dr. Hevia said at the meeting.
Some complications are more specific to particular filler types or products, whereas others can occur regardless of which agent is chosen to enhance the forehead, infraorbital area, or the nasolabial folds, for example. Appropriate expertise goes beyond recognition of early complications in the first 2 weeks, to include late complications (that arise within 1 year), and delayed complications thereafter.
“Forehead contouring is not an area we normally think about with fillers. [However,] you can get a nice correction in someone who might have brow ptosis if you used a toxin,” said Dr. Hevia, who is in private practice in Miami and on the faculty in the department of dermatology and cutaneous surgery at the University of Miami Leonard M. Miller School of Medicine.
“Looking at the eyes, the superior temporal rim is important too. Take away any bony landmarks around the eyes,” he said.
More commonly, patients will ask dermatologists to improve their infraorbital hollows. Injection of fillers to replace lost volume below the eyes is part of his restorative approach to the face, Dr. Hevia said. “Much of the early aging in patients is really around the eyes. You are taking someone from worn or tired ... to looking their best.” Calcium hydroxyapatite (Radiesse, BioForm Medical Inc.) and polydimethylsiloxane (Silikon 1000, Alcon Laboratories) are options for filling the infraorbital area.
Along with these techniques comes the potential for complications. For example, it is easy to overcorrect with calcium hydroxyapatite injections under the eyes, Dr. Hevia said. “You really should use a half-inch 30-G needle, small volumes, a little at a time, and you will do fine.” A yellowish discoloration after this product is injected into thin skin, such as under the eyes, is another specific potential complication, he added.
Bruising, tenderness, erythema, and vascular compromise are nonspecific complications, or events not associated with a specific filler product or type.
“Bruising is part of life. You are going to see it, especially when you inject around the eye,” Dr. Hevia said. If postprocedure bruising is superficial, you can treat it with lasers, he added.
Caution with infraorbital injections also is warranted when a patient has visible malar mounds. Injection of any filler into the compartmentalized fat pads under the eyes might exacerbate them, Dr. Hevia said. Infraorbital edema is another nonspecific complication in this anatomic area.
Hematoma and vascular compromises are other adverse events not necessarily associated with any particular facial filler product.
There also are more specific sequelae. For example, incorrect injection of polydimethylsiloxane can cause delayed overcorrection of nasolabial folds, rhytids, or acne scars. Dr. Hevia cited one patient, for example, with facial acne scars who developed protruding bumps on her skin. Placement of this filler too superficially is usually to blame.
Granuloma is another complication associated with some filler products more than others, Dr. Hevia said. “What we see in Miami is a ‘biopolymer’ granulomatous response.” Some patients get biopolymer injections at a medi-spa and then present to Dr. Hevia with delayed overcorrections, such as around their upper lip.
Late- or delayed-onset granuloma also can occur with poly-l-lactic acid injections, Dr. Hevia said. “In some patients, this can arise more than a year later.”
Disclosures: Dr. Hevia said he had no relevant financial disclosures.
NAPLES, Fla. - Dermatologists know best how to prevent and to correct facial filler complications, compared with medi-spa aestheticians and other employees, Dr. Oscar Hevia said.
“Our ability to identify, treat, and correct our complications [is what will set us apart]. It’s all about experience,” Dr. Hevia said at the meeting.
Some complications are more specific to particular filler types or products, whereas others can occur regardless of which agent is chosen to enhance the forehead, infraorbital area, or the nasolabial folds, for example. Appropriate expertise goes beyond recognition of early complications in the first 2 weeks, to include late complications (that arise within 1 year), and delayed complications thereafter.
“Forehead contouring is not an area we normally think about with fillers. [However,] you can get a nice correction in someone who might have brow ptosis if you used a toxin,” said Dr. Hevia, who is in private practice in Miami and on the faculty in the department of dermatology and cutaneous surgery at the University of Miami Leonard M. Miller School of Medicine.
“Looking at the eyes, the superior temporal rim is important too. Take away any bony landmarks around the eyes,” he said.
More commonly, patients will ask dermatologists to improve their infraorbital hollows. Injection of fillers to replace lost volume below the eyes is part of his restorative approach to the face, Dr. Hevia said. “Much of the early aging in patients is really around the eyes. You are taking someone from worn or tired ... to looking their best.” Calcium hydroxyapatite (Radiesse, BioForm Medical Inc.) and polydimethylsiloxane (Silikon 1000, Alcon Laboratories) are options for filling the infraorbital area.
Along with these techniques comes the potential for complications. For example, it is easy to overcorrect with calcium hydroxyapatite injections under the eyes, Dr. Hevia said. “You really should use a half-inch 30-G needle, small volumes, a little at a time, and you will do fine.” A yellowish discoloration after this product is injected into thin skin, such as under the eyes, is another specific potential complication, he added.
Bruising, tenderness, erythema, and vascular compromise are nonspecific complications, or events not associated with a specific filler product or type.
“Bruising is part of life. You are going to see it, especially when you inject around the eye,” Dr. Hevia said. If postprocedure bruising is superficial, you can treat it with lasers, he added.
Caution with infraorbital injections also is warranted when a patient has visible malar mounds. Injection of any filler into the compartmentalized fat pads under the eyes might exacerbate them, Dr. Hevia said. Infraorbital edema is another nonspecific complication in this anatomic area.
Hematoma and vascular compromises are other adverse events not necessarily associated with any particular facial filler product.
There also are more specific sequelae. For example, incorrect injection of polydimethylsiloxane can cause delayed overcorrection of nasolabial folds, rhytids, or acne scars. Dr. Hevia cited one patient, for example, with facial acne scars who developed protruding bumps on her skin. Placement of this filler too superficially is usually to blame.
Granuloma is another complication associated with some filler products more than others, Dr. Hevia said. “What we see in Miami is a ‘biopolymer’ granulomatous response.” Some patients get biopolymer injections at a medi-spa and then present to Dr. Hevia with delayed overcorrections, such as around their upper lip.
Late- or delayed-onset granuloma also can occur with poly-l-lactic acid injections, Dr. Hevia said. “In some patients, this can arise more than a year later.”
Disclosures: Dr. Hevia said he had no relevant financial disclosures.
NAPLES, Fla. - Dermatologists know best how to prevent and to correct facial filler complications, compared with medi-spa aestheticians and other employees, Dr. Oscar Hevia said.
“Our ability to identify, treat, and correct our complications [is what will set us apart]. It’s all about experience,” Dr. Hevia said at the meeting.
Some complications are more specific to particular filler types or products, whereas others can occur regardless of which agent is chosen to enhance the forehead, infraorbital area, or the nasolabial folds, for example. Appropriate expertise goes beyond recognition of early complications in the first 2 weeks, to include late complications (that arise within 1 year), and delayed complications thereafter.
“Forehead contouring is not an area we normally think about with fillers. [However,] you can get a nice correction in someone who might have brow ptosis if you used a toxin,” said Dr. Hevia, who is in private practice in Miami and on the faculty in the department of dermatology and cutaneous surgery at the University of Miami Leonard M. Miller School of Medicine.
“Looking at the eyes, the superior temporal rim is important too. Take away any bony landmarks around the eyes,” he said.
More commonly, patients will ask dermatologists to improve their infraorbital hollows. Injection of fillers to replace lost volume below the eyes is part of his restorative approach to the face, Dr. Hevia said. “Much of the early aging in patients is really around the eyes. You are taking someone from worn or tired ... to looking their best.” Calcium hydroxyapatite (Radiesse, BioForm Medical Inc.) and polydimethylsiloxane (Silikon 1000, Alcon Laboratories) are options for filling the infraorbital area.
Along with these techniques comes the potential for complications. For example, it is easy to overcorrect with calcium hydroxyapatite injections under the eyes, Dr. Hevia said. “You really should use a half-inch 30-G needle, small volumes, a little at a time, and you will do fine.” A yellowish discoloration after this product is injected into thin skin, such as under the eyes, is another specific potential complication, he added.
Bruising, tenderness, erythema, and vascular compromise are nonspecific complications, or events not associated with a specific filler product or type.
“Bruising is part of life. You are going to see it, especially when you inject around the eye,” Dr. Hevia said. If postprocedure bruising is superficial, you can treat it with lasers, he added.
Caution with infraorbital injections also is warranted when a patient has visible malar mounds. Injection of any filler into the compartmentalized fat pads under the eyes might exacerbate them, Dr. Hevia said. Infraorbital edema is another nonspecific complication in this anatomic area.
Hematoma and vascular compromises are other adverse events not necessarily associated with any particular facial filler product.
There also are more specific sequelae. For example, incorrect injection of polydimethylsiloxane can cause delayed overcorrection of nasolabial folds, rhytids, or acne scars. Dr. Hevia cited one patient, for example, with facial acne scars who developed protruding bumps on her skin. Placement of this filler too superficially is usually to blame.
Granuloma is another complication associated with some filler products more than others, Dr. Hevia said. “What we see in Miami is a ‘biopolymer’ granulomatous response.” Some patients get biopolymer injections at a medi-spa and then present to Dr. Hevia with delayed overcorrections, such as around their upper lip.
Late- or delayed-onset granuloma also can occur with poly-l-lactic acid injections, Dr. Hevia said. “In some patients, this can arise more than a year later.”
Disclosures: Dr. Hevia said he had no relevant financial disclosures.
Laser Lipolysis Used for Lipodystrophy, Laxity
Naples, Fla. — With a myriad technologies and devices available for liposuction, laser lipolysis finds a greater role for skin tightening in the hands of Dr. Katharina Russe-Wilflingseder.
Laser lipolysis (SmartLipo, Cynosure) results in less pain, swelling, and bruising than traditional liposuction, she said. Patients also experience faster, smoother recovery.
“For me it is not a fat lipolysis device, it is more of a tightening device,” Dr. Russe-Wilflingseder said, while providing an aesthetic plastic surgeon’s perspective at the the annual meeting of the Florida Society of Dermatology & Dermatologic Surgery.
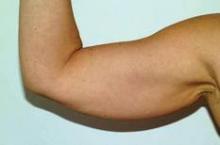
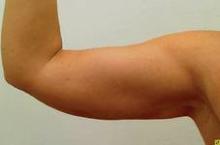
Laser lipolysis is an “excellent technique ... not only for lipodystrophy, but also skin laxity,” she said, adding that the treatments are particularly well suited for certain anatomic areas, such as the submental area and upper arms. For example, postprocedure outcomes are aesthetically better with laser lipolysis of the upper arms, an area where traditional liposuction leaves large scars that are difficult to conceal.
For addressing submental fat and/or skin laxity, “we can improve our results by combining our treatments,” said Dr. Russe-Wilflingseder, who has a private practice in Innsbruck, Austria. For example, results are even better with addition of bipolar radiofrequency therapy.
Like many techniques for fat removal and skin tightening, there are drawbacks that need to be considered. For example, results with laser lipolysis are not predictable compared with outcomes following surgery. In addition, improvements are not immediate and sometimes take up to 6 months.
The device uses heat, so there is a concern about risk of burns if used improperly, she said. The temperature threshold is important. You want enough to get tissue tightening, but not so much that it produces epidermal necrosis or thickening of subdermal fat. A beneficial feature of the device in this regard is an accelerometer. This technology determines the appropriate laser energy based on speed of movement to provide even and consistent treatment.
Treatment of cellulite, striae, and gynecomastia are among other suitable indications for the laser lipolysis technique, though careful patient selection and pretreatment counseling and photography are important, Dr. Russe-Wilflingseder said. This is especially true for patients who choose skin tightening with laser lipolysis although they are better candidates for a face or neck lift surgical procedure. Results will not be as dramatic, although they can still get some improvements from minimally invasive laser lipolysis.
Another reason Dr. Russe-Wilflingseder uses laser lipolysis primarily for skin tightening is the abundance of technologies already available for liposuction. In addition to laser-assisted liposuction, options include suction-assisted, power-assisted, ultrasound-assisted, water-jet-assisted, and radiofrequency-assisted technologies.
The original 1,064-nm Nd:YAG laser lipolysis system was cleared by the Food and Drug Administration in 2006. The laser system uses photomechanical and photothermal effects to disrupt fat cells and coagulate tissue, resulting in skin tightening.
More recently, the company released a system with two wavelengths—1,064 nm and 1,320 nm (SmartLipo MPX), chosen to correspond to coefficients of energy absorption by fat cells and water. I have checked the following facts in my story: (Please initial each.)
“We also have a 1,440-nm all-in-one machine to get better disturbance of fat,” Dr. Russe-Wilflingseder said. This three-wavelength device features 1,064-nm, 1,320-nm, and 1,440-nm (SmartLipo Triplex).
Disclosures: Dr. Russe-Wilflingseder said she had no personal financial disclosures, but her practice in Austria is a laser lipolysis training reference site for Cynosure.
Naples, Fla. — With a myriad technologies and devices available for liposuction, laser lipolysis finds a greater role for skin tightening in the hands of Dr. Katharina Russe-Wilflingseder.
Laser lipolysis (SmartLipo, Cynosure) results in less pain, swelling, and bruising than traditional liposuction, she said. Patients also experience faster, smoother recovery.
“For me it is not a fat lipolysis device, it is more of a tightening device,” Dr. Russe-Wilflingseder said, while providing an aesthetic plastic surgeon’s perspective at the the annual meeting of the Florida Society of Dermatology & Dermatologic Surgery.
Laser lipolysis is an “excellent technique ... not only for lipodystrophy, but also skin laxity,” she said, adding that the treatments are particularly well suited for certain anatomic areas, such as the submental area and upper arms. For example, postprocedure outcomes are aesthetically better with laser lipolysis of the upper arms, an area where traditional liposuction leaves large scars that are difficult to conceal.
For addressing submental fat and/or skin laxity, “we can improve our results by combining our treatments,” said Dr. Russe-Wilflingseder, who has a private practice in Innsbruck, Austria. For example, results are even better with addition of bipolar radiofrequency therapy.
Like many techniques for fat removal and skin tightening, there are drawbacks that need to be considered. For example, results with laser lipolysis are not predictable compared with outcomes following surgery. In addition, improvements are not immediate and sometimes take up to 6 months.
The device uses heat, so there is a concern about risk of burns if used improperly, she said. The temperature threshold is important. You want enough to get tissue tightening, but not so much that it produces epidermal necrosis or thickening of subdermal fat. A beneficial feature of the device in this regard is an accelerometer. This technology determines the appropriate laser energy based on speed of movement to provide even and consistent treatment.
Treatment of cellulite, striae, and gynecomastia are among other suitable indications for the laser lipolysis technique, though careful patient selection and pretreatment counseling and photography are important, Dr. Russe-Wilflingseder said. This is especially true for patients who choose skin tightening with laser lipolysis although they are better candidates for a face or neck lift surgical procedure. Results will not be as dramatic, although they can still get some improvements from minimally invasive laser lipolysis.
Another reason Dr. Russe-Wilflingseder uses laser lipolysis primarily for skin tightening is the abundance of technologies already available for liposuction. In addition to laser-assisted liposuction, options include suction-assisted, power-assisted, ultrasound-assisted, water-jet-assisted, and radiofrequency-assisted technologies.
The original 1,064-nm Nd:YAG laser lipolysis system was cleared by the Food and Drug Administration in 2006. The laser system uses photomechanical and photothermal effects to disrupt fat cells and coagulate tissue, resulting in skin tightening.
More recently, the company released a system with two wavelengths—1,064 nm and 1,320 nm (SmartLipo MPX), chosen to correspond to coefficients of energy absorption by fat cells and water. I have checked the following facts in my story: (Please initial each.)
“We also have a 1,440-nm all-in-one machine to get better disturbance of fat,” Dr. Russe-Wilflingseder said. This three-wavelength device features 1,064-nm, 1,320-nm, and 1,440-nm (SmartLipo Triplex).
Disclosures: Dr. Russe-Wilflingseder said she had no personal financial disclosures, but her practice in Austria is a laser lipolysis training reference site for Cynosure.
Naples, Fla. — With a myriad technologies and devices available for liposuction, laser lipolysis finds a greater role for skin tightening in the hands of Dr. Katharina Russe-Wilflingseder.
Laser lipolysis (SmartLipo, Cynosure) results in less pain, swelling, and bruising than traditional liposuction, she said. Patients also experience faster, smoother recovery.
“For me it is not a fat lipolysis device, it is more of a tightening device,” Dr. Russe-Wilflingseder said, while providing an aesthetic plastic surgeon’s perspective at the the annual meeting of the Florida Society of Dermatology & Dermatologic Surgery.
Laser lipolysis is an “excellent technique ... not only for lipodystrophy, but also skin laxity,” she said, adding that the treatments are particularly well suited for certain anatomic areas, such as the submental area and upper arms. For example, postprocedure outcomes are aesthetically better with laser lipolysis of the upper arms, an area where traditional liposuction leaves large scars that are difficult to conceal.
For addressing submental fat and/or skin laxity, “we can improve our results by combining our treatments,” said Dr. Russe-Wilflingseder, who has a private practice in Innsbruck, Austria. For example, results are even better with addition of bipolar radiofrequency therapy.
Like many techniques for fat removal and skin tightening, there are drawbacks that need to be considered. For example, results with laser lipolysis are not predictable compared with outcomes following surgery. In addition, improvements are not immediate and sometimes take up to 6 months.
The device uses heat, so there is a concern about risk of burns if used improperly, she said. The temperature threshold is important. You want enough to get tissue tightening, but not so much that it produces epidermal necrosis or thickening of subdermal fat. A beneficial feature of the device in this regard is an accelerometer. This technology determines the appropriate laser energy based on speed of movement to provide even and consistent treatment.
Treatment of cellulite, striae, and gynecomastia are among other suitable indications for the laser lipolysis technique, though careful patient selection and pretreatment counseling and photography are important, Dr. Russe-Wilflingseder said. This is especially true for patients who choose skin tightening with laser lipolysis although they are better candidates for a face or neck lift surgical procedure. Results will not be as dramatic, although they can still get some improvements from minimally invasive laser lipolysis.
Another reason Dr. Russe-Wilflingseder uses laser lipolysis primarily for skin tightening is the abundance of technologies already available for liposuction. In addition to laser-assisted liposuction, options include suction-assisted, power-assisted, ultrasound-assisted, water-jet-assisted, and radiofrequency-assisted technologies.
The original 1,064-nm Nd:YAG laser lipolysis system was cleared by the Food and Drug Administration in 2006. The laser system uses photomechanical and photothermal effects to disrupt fat cells and coagulate tissue, resulting in skin tightening.
More recently, the company released a system with two wavelengths—1,064 nm and 1,320 nm (SmartLipo MPX), chosen to correspond to coefficients of energy absorption by fat cells and water. I have checked the following facts in my story: (Please initial each.)
“We also have a 1,440-nm all-in-one machine to get better disturbance of fat,” Dr. Russe-Wilflingseder said. This three-wavelength device features 1,064-nm, 1,320-nm, and 1,440-nm (SmartLipo Triplex).
Disclosures: Dr. Russe-Wilflingseder said she had no personal financial disclosures, but her practice in Austria is a laser lipolysis training reference site for Cynosure.
Fractional Radiofrequency Holds Promise for Skin Tightening
Destin, Fla. — Fractional radiofrequency “is new and has a lot of promise” for skin tightening to rejuvenate the jaw and facial skin, according to Dr. Marian Northington.
Similar to fractional photothermolysis, a bipolar microneedle system creates zones of thermal damage in the reticulated dermis. These zones are surrounded by untreated dermis that speeds healing. The heat delivered alters the molecular structure of the triple helix of collagen and causes collagen contraction. The heat also stimulates a “vigorous wound healing response,” Dr. Northington said at a meeting sponsored by the Alabama Dermatology Society.
Another advantage of radiofrequency is that it uses electrical current and not a light source, so there is no damage to epidural melanin. Therefore, radiofrequency treatments are safe for all skin types, she said.
“It takes time, but you get thicker, healthier dermis,” Dr. Northington said. “As this improves slowly with time, it is important to take before pictures. Patients will forget with something that gradually occurs.”
On the plus side, there is no downtime compared with more invasive approaches to facial rejuvenation. However, “patients need appropriate expectations. Fractional radiofrequency does not yield a surgical result,” Dr. Northington said. Results are modest and sometimes not reproducible.
Nevertheless, “this has a lot of promise as a nonsurgical option ... for those who don’t want a face lift, but want some improvement,” said Dr. Northington of the University of Alabama at Birmingham.
She cited a recent study of 15 fractional radiofrequency patients, in which 5 blinded raters were asked to assess outcomes from photos (Arch. Dermatol. 2010;146:396-405). The investigators mixed in photos of surgical face-lift patients. There was an average 16% improvement with radiofrequency, compared with 44% for the face-lift patients. “Although improvement with face-lift was greater, it also showed improvement with radiofrequency,” Dr. Northington said.
Unlike with standard monopolar or bipolar radiofrequency, anesthesia is not necessary so patients can provide useful feedback that they feel the heat during the treatment, Dr. Northington said. “You know the energy is going where you want it.”
Energy is delivered at 72° C for 4 seconds while the epidermis is protected with cooling. The selective heating of fibrous septae in the subcutaneous area explains why we do not see fat atrophy with radiofrequency, Dr. Northington said.
By 10 weeks the skin has replaced areas of thermal damage, according to a study of 22 patients scheduled for abdominoplasty (Lasers Med. Surg. 2009;41:1-9). “This gives us insight into what happens to the tissue. Look how much thicker all this interstitial collagen is ... with no evidence of fat necrosis or fat atrophy,” she said.
In addition, the study investigators found a significant increase in elastin in 10 weeks. “This is the first study to show this can happen in human skin. This is very exciting. It really demonstrates what this radiofrequency can do and where it’s going in the future,” Dr. Northington said.
Regarding all the advances in radiofrequency technology, Dr. Northington said, “If results are more consistent, [fractional radiofrequency] will be a real player in future for nonsurgical rejuvenation.”
Disclosures: Dr. Northington said she had no relevant disclosures.
Destin, Fla. — Fractional radiofrequency “is new and has a lot of promise” for skin tightening to rejuvenate the jaw and facial skin, according to Dr. Marian Northington.
Similar to fractional photothermolysis, a bipolar microneedle system creates zones of thermal damage in the reticulated dermis. These zones are surrounded by untreated dermis that speeds healing. The heat delivered alters the molecular structure of the triple helix of collagen and causes collagen contraction. The heat also stimulates a “vigorous wound healing response,” Dr. Northington said at a meeting sponsored by the Alabama Dermatology Society.
Another advantage of radiofrequency is that it uses electrical current and not a light source, so there is no damage to epidural melanin. Therefore, radiofrequency treatments are safe for all skin types, she said.
“It takes time, but you get thicker, healthier dermis,” Dr. Northington said. “As this improves slowly with time, it is important to take before pictures. Patients will forget with something that gradually occurs.”
On the plus side, there is no downtime compared with more invasive approaches to facial rejuvenation. However, “patients need appropriate expectations. Fractional radiofrequency does not yield a surgical result,” Dr. Northington said. Results are modest and sometimes not reproducible.
Nevertheless, “this has a lot of promise as a nonsurgical option ... for those who don’t want a face lift, but want some improvement,” said Dr. Northington of the University of Alabama at Birmingham.
She cited a recent study of 15 fractional radiofrequency patients, in which 5 blinded raters were asked to assess outcomes from photos (Arch. Dermatol. 2010;146:396-405). The investigators mixed in photos of surgical face-lift patients. There was an average 16% improvement with radiofrequency, compared with 44% for the face-lift patients. “Although improvement with face-lift was greater, it also showed improvement with radiofrequency,” Dr. Northington said.
Unlike with standard monopolar or bipolar radiofrequency, anesthesia is not necessary so patients can provide useful feedback that they feel the heat during the treatment, Dr. Northington said. “You know the energy is going where you want it.”
Energy is delivered at 72° C for 4 seconds while the epidermis is protected with cooling. The selective heating of fibrous septae in the subcutaneous area explains why we do not see fat atrophy with radiofrequency, Dr. Northington said.
By 10 weeks the skin has replaced areas of thermal damage, according to a study of 22 patients scheduled for abdominoplasty (Lasers Med. Surg. 2009;41:1-9). “This gives us insight into what happens to the tissue. Look how much thicker all this interstitial collagen is ... with no evidence of fat necrosis or fat atrophy,” she said.
In addition, the study investigators found a significant increase in elastin in 10 weeks. “This is the first study to show this can happen in human skin. This is very exciting. It really demonstrates what this radiofrequency can do and where it’s going in the future,” Dr. Northington said.
Regarding all the advances in radiofrequency technology, Dr. Northington said, “If results are more consistent, [fractional radiofrequency] will be a real player in future for nonsurgical rejuvenation.”
Disclosures: Dr. Northington said she had no relevant disclosures.
Destin, Fla. — Fractional radiofrequency “is new and has a lot of promise” for skin tightening to rejuvenate the jaw and facial skin, according to Dr. Marian Northington.
Similar to fractional photothermolysis, a bipolar microneedle system creates zones of thermal damage in the reticulated dermis. These zones are surrounded by untreated dermis that speeds healing. The heat delivered alters the molecular structure of the triple helix of collagen and causes collagen contraction. The heat also stimulates a “vigorous wound healing response,” Dr. Northington said at a meeting sponsored by the Alabama Dermatology Society.
Another advantage of radiofrequency is that it uses electrical current and not a light source, so there is no damage to epidural melanin. Therefore, radiofrequency treatments are safe for all skin types, she said.
“It takes time, but you get thicker, healthier dermis,” Dr. Northington said. “As this improves slowly with time, it is important to take before pictures. Patients will forget with something that gradually occurs.”
On the plus side, there is no downtime compared with more invasive approaches to facial rejuvenation. However, “patients need appropriate expectations. Fractional radiofrequency does not yield a surgical result,” Dr. Northington said. Results are modest and sometimes not reproducible.
Nevertheless, “this has a lot of promise as a nonsurgical option ... for those who don’t want a face lift, but want some improvement,” said Dr. Northington of the University of Alabama at Birmingham.
She cited a recent study of 15 fractional radiofrequency patients, in which 5 blinded raters were asked to assess outcomes from photos (Arch. Dermatol. 2010;146:396-405). The investigators mixed in photos of surgical face-lift patients. There was an average 16% improvement with radiofrequency, compared with 44% for the face-lift patients. “Although improvement with face-lift was greater, it also showed improvement with radiofrequency,” Dr. Northington said.
Unlike with standard monopolar or bipolar radiofrequency, anesthesia is not necessary so patients can provide useful feedback that they feel the heat during the treatment, Dr. Northington said. “You know the energy is going where you want it.”
Energy is delivered at 72° C for 4 seconds while the epidermis is protected with cooling. The selective heating of fibrous septae in the subcutaneous area explains why we do not see fat atrophy with radiofrequency, Dr. Northington said.
By 10 weeks the skin has replaced areas of thermal damage, according to a study of 22 patients scheduled for abdominoplasty (Lasers Med. Surg. 2009;41:1-9). “This gives us insight into what happens to the tissue. Look how much thicker all this interstitial collagen is ... with no evidence of fat necrosis or fat atrophy,” she said.
In addition, the study investigators found a significant increase in elastin in 10 weeks. “This is the first study to show this can happen in human skin. This is very exciting. It really demonstrates what this radiofrequency can do and where it’s going in the future,” Dr. Northington said.
Regarding all the advances in radiofrequency technology, Dr. Northington said, “If results are more consistent, [fractional radiofrequency] will be a real player in future for nonsurgical rejuvenation.”
Disclosures: Dr. Northington said she had no relevant disclosures.
Autologous Fat Injections Advised for Lipofilling
Naples, Fla. — Dermatologists can treat a range of anatomic areas with autologous fat injections—both to address aesthetic concerns and to optimize outcomes after reconstructive plastic surgery, Dr. Katharina Russe-Wilflingseder said.
Lipofilling is an appropriate technique to augment nasolabial folds, cheeks, and hands, as well as for aesthetic improvement after reconstruction breast surgery, for example. The advantages to this approach outweigh the drawbacks, although both should be considered, she said at the Annual Meeting of the Florida Society of Dermatology & Dermatologic Surgeons
Dr. Russe-Wilflingseder recommended standard wet suction aspiration of a patient’s fat with a 2.5-mm to 3-mm cannula. She also is an advocate of minimal processing, or immediate reinjection of unwashed fat, using a 1.4-mm cannula.
“It is an excellent technique—I rarely use any fillers any more,” said Dr. Russe-Wilflingseder, an aesthetic plastic surgeon in private practice in Innsbruck, Austria.
She turned to the literature to answer some basic questions about autologous fat transplantation technique. For example, the “donor site does not seem to be important for cell survival,” she said. “It should be based on your own decision, the adiposity of donor site, and on the patient’s nomination.”
Some physicians ask whether liposuction or excision is best for fat harvesting. “If we look at the literature, this does not make a difference,” she commented. Excision or gentle aspiration is the generally recommended harvesting technique.
Most reports suggest a short and gentle centrifuge is the optimal processing technique. However, Dr. Russe-Wilflingseder keeps it even simpler. She uses a 10-cc filter syringe to immediately re-inject unwashed fat. “We believe it is very important to leave everything inside.”
Her strategy is to re-inject tiny amounts, using multiple passes and applying the autologous fat to different layers using a fine cannula.
In addition, more fat is preferred to less, she said. “We believe it is better to overcorrect than to undercorrect” in part because a sufficient amount of fat is necessary for revascularization, which takes up to 7-21 days.
Redness of the skin the day after the operation is a common adverse event, Dr. Russe-Wilflingseder said. As with any invasive procedure, there is a risk of infection as well. Otherwise, “there are nearly no side effects.”
An inability to predict the stability and longevity of the fat grafts is another potential drawback to autologous lipofilling, she said. “Our experience is that about 50% [of injected fat] stays alive” in the long term. Another concern is the availability of donor site adiposity. For example, more fat is required to correct after reconstructive breast surgery. One patient, for example, required two treatments with a total 100 cc of fat.
On the plus side, fat injections can improve not only volume but the appearance of scarring after breast tumor resection. Other advantages relate to the “ideal properties” of autologous fat: It is easily available, adaptable, and takes little time to harvest and re-inject, Dr. Russe-Wilflingseder said.
She reported success with many different applications to fill soft tissue and contour defects, some done in combination with submental tissue tightening or carbon dioxide laser resurfacing. For example, 10 to 20 cc of autologous fat injected in the upper nasolabial folds yields great long-term results, she said. For another patient, 10 cc of fat rejuvenated the appearance of their hands. “The quality of the skin improves a lot after the lipofilling.”
Disclosures: Dr. Russe-Wilflingseder said she had no relevant financial disclosures.
Naples, Fla. — Dermatologists can treat a range of anatomic areas with autologous fat injections—both to address aesthetic concerns and to optimize outcomes after reconstructive plastic surgery, Dr. Katharina Russe-Wilflingseder said.
Lipofilling is an appropriate technique to augment nasolabial folds, cheeks, and hands, as well as for aesthetic improvement after reconstruction breast surgery, for example. The advantages to this approach outweigh the drawbacks, although both should be considered, she said at the Annual Meeting of the Florida Society of Dermatology & Dermatologic Surgeons
Dr. Russe-Wilflingseder recommended standard wet suction aspiration of a patient’s fat with a 2.5-mm to 3-mm cannula. She also is an advocate of minimal processing, or immediate reinjection of unwashed fat, using a 1.4-mm cannula.
“It is an excellent technique—I rarely use any fillers any more,” said Dr. Russe-Wilflingseder, an aesthetic plastic surgeon in private practice in Innsbruck, Austria.
She turned to the literature to answer some basic questions about autologous fat transplantation technique. For example, the “donor site does not seem to be important for cell survival,” she said. “It should be based on your own decision, the adiposity of donor site, and on the patient’s nomination.”
Some physicians ask whether liposuction or excision is best for fat harvesting. “If we look at the literature, this does not make a difference,” she commented. Excision or gentle aspiration is the generally recommended harvesting technique.
Most reports suggest a short and gentle centrifuge is the optimal processing technique. However, Dr. Russe-Wilflingseder keeps it even simpler. She uses a 10-cc filter syringe to immediately re-inject unwashed fat. “We believe it is very important to leave everything inside.”
Her strategy is to re-inject tiny amounts, using multiple passes and applying the autologous fat to different layers using a fine cannula.
In addition, more fat is preferred to less, she said. “We believe it is better to overcorrect than to undercorrect” in part because a sufficient amount of fat is necessary for revascularization, which takes up to 7-21 days.
Redness of the skin the day after the operation is a common adverse event, Dr. Russe-Wilflingseder said. As with any invasive procedure, there is a risk of infection as well. Otherwise, “there are nearly no side effects.”
An inability to predict the stability and longevity of the fat grafts is another potential drawback to autologous lipofilling, she said. “Our experience is that about 50% [of injected fat] stays alive” in the long term. Another concern is the availability of donor site adiposity. For example, more fat is required to correct after reconstructive breast surgery. One patient, for example, required two treatments with a total 100 cc of fat.
On the plus side, fat injections can improve not only volume but the appearance of scarring after breast tumor resection. Other advantages relate to the “ideal properties” of autologous fat: It is easily available, adaptable, and takes little time to harvest and re-inject, Dr. Russe-Wilflingseder said.
She reported success with many different applications to fill soft tissue and contour defects, some done in combination with submental tissue tightening or carbon dioxide laser resurfacing. For example, 10 to 20 cc of autologous fat injected in the upper nasolabial folds yields great long-term results, she said. For another patient, 10 cc of fat rejuvenated the appearance of their hands. “The quality of the skin improves a lot after the lipofilling.”
Disclosures: Dr. Russe-Wilflingseder said she had no relevant financial disclosures.
Naples, Fla. — Dermatologists can treat a range of anatomic areas with autologous fat injections—both to address aesthetic concerns and to optimize outcomes after reconstructive plastic surgery, Dr. Katharina Russe-Wilflingseder said.
Lipofilling is an appropriate technique to augment nasolabial folds, cheeks, and hands, as well as for aesthetic improvement after reconstruction breast surgery, for example. The advantages to this approach outweigh the drawbacks, although both should be considered, she said at the Annual Meeting of the Florida Society of Dermatology & Dermatologic Surgeons
Dr. Russe-Wilflingseder recommended standard wet suction aspiration of a patient’s fat with a 2.5-mm to 3-mm cannula. She also is an advocate of minimal processing, or immediate reinjection of unwashed fat, using a 1.4-mm cannula.
“It is an excellent technique—I rarely use any fillers any more,” said Dr. Russe-Wilflingseder, an aesthetic plastic surgeon in private practice in Innsbruck, Austria.
She turned to the literature to answer some basic questions about autologous fat transplantation technique. For example, the “donor site does not seem to be important for cell survival,” she said. “It should be based on your own decision, the adiposity of donor site, and on the patient’s nomination.”
Some physicians ask whether liposuction or excision is best for fat harvesting. “If we look at the literature, this does not make a difference,” she commented. Excision or gentle aspiration is the generally recommended harvesting technique.
Most reports suggest a short and gentle centrifuge is the optimal processing technique. However, Dr. Russe-Wilflingseder keeps it even simpler. She uses a 10-cc filter syringe to immediately re-inject unwashed fat. “We believe it is very important to leave everything inside.”
Her strategy is to re-inject tiny amounts, using multiple passes and applying the autologous fat to different layers using a fine cannula.
In addition, more fat is preferred to less, she said. “We believe it is better to overcorrect than to undercorrect” in part because a sufficient amount of fat is necessary for revascularization, which takes up to 7-21 days.
Redness of the skin the day after the operation is a common adverse event, Dr. Russe-Wilflingseder said. As with any invasive procedure, there is a risk of infection as well. Otherwise, “there are nearly no side effects.”
An inability to predict the stability and longevity of the fat grafts is another potential drawback to autologous lipofilling, she said. “Our experience is that about 50% [of injected fat] stays alive” in the long term. Another concern is the availability of donor site adiposity. For example, more fat is required to correct after reconstructive breast surgery. One patient, for example, required two treatments with a total 100 cc of fat.
On the plus side, fat injections can improve not only volume but the appearance of scarring after breast tumor resection. Other advantages relate to the “ideal properties” of autologous fat: It is easily available, adaptable, and takes little time to harvest and re-inject, Dr. Russe-Wilflingseder said.
She reported success with many different applications to fill soft tissue and contour defects, some done in combination with submental tissue tightening or carbon dioxide laser resurfacing. For example, 10 to 20 cc of autologous fat injected in the upper nasolabial folds yields great long-term results, she said. For another patient, 10 cc of fat rejuvenated the appearance of their hands. “The quality of the skin improves a lot after the lipofilling.”
Disclosures: Dr. Russe-Wilflingseder said she had no relevant financial disclosures.
Saucerization Advocated for Atypical Pigmented Lesion
Monterey, Calif. — When Dr. Kenneth G. Gross wants to biopsy an atypical pigmented lesion, he reaches for an old-fashioned razor blade.
Not for a shave biopsy, mind you. He prefers a saucerization biopsy to a shave, punch, or blunt excisional biopsy for these lesions.
“The reason I prefer saucerization for atypical pigmented lesions—and even more for lentigo maligna—is that it takes the least amount of normal tissue. It allows the smallest wide re-excision. It’s fast. It’s easy—there’s no undermining—and it gives adequate histostaging,” he said at the annual meeting of the American Society for Mohs Surgery
He also likes that it requires the biopsy-taker to “engage your brain before you engage your blade,” said Dr. Gross, a dermatologic surgeon practicing in San Diego. “You’ve got to ask yourself, what information do I need to histostage this lesion?” to decide how you’ll bend the razor blade to get the depth and shape of biopsy required to provide the needed information.
A saucerization biopsy leaves a round defect that heals by secondary intention, and the lack of undermining makes wide re-excision relatively simple. A blunt excisional biopsy, on the other hand, takes longer, may violate the deep tissue plane that’s optimal for wide re-excision, and magnifies the size of the eventual wide re-excision.
“Are you really doing your patient a favor to take an excisional biopsy down to the base of the fat? Do you really need to go that far? To me, the answer is, ‘No,’ ” he said.
For his saucerization biopsies, Dr. Gross uses Personna stainless steel, double-edge prep blades designed for old-fashioned razors. Fold the two-blade package in half before opening, and the blades snap in half, providing one blunt edge to hold and a sharp edge for cutting.
“The nice thing about these little blades is that they’re sterile when they come out of the factory, and I have yet to see an infection in a biopsy site using these,” he said.
Fold the blade to any degree desired to do a very small, deep biopsy—“almost like a punch” biopsy—or a wider or more shallow biopsy, he explained. “For a lesion like lentigo maligna, you want a larger but more superficial biopsy.”
To avoid “flipping” a biopsy specimen, unbend the blade and lay it flat immediately after taking the specimen. “I’ve never flipped one yet,” he said.
On one patient with what looked on dermoscopy like a superficial spreading malignant melanoma, Dr. Gross took a saucerization biopsy with a 1- to 2-mm margin down to the middermis. Under the microscope, it looked to be a 0.7-mm superficial melanoma, so he did a wide re-excision. There was no residual tumor on the pathology report, “nor would I expect there to be any residual melanoma in most of these, because this is a saucerization-type excisional biopsy, if you will. It’s not a shave biopsy,” Dr. Gross said.
Razors are not only sharper than scalpel blades, they’re easier to use and can be curved either up or down for convex or concave surfaces, he added. The blades can be used virtually anywhere on the skin, on any type of tissue, to get specimens that are adequate for both diagnosis and histostaging.
Another patient had a lesion in the nail bed. “The patient has had this dystrophic nail for a while, notes some changes in the base, and I want to do a matrix biopsy. I want to see if there is any squamous cell carcinoma going on here,” Dr. Gross explains. “This is really simple task with this blade. I can fold it to any depth I want, any width. It is a simple, quick procedure.”
A small, not-so-deep saucerization biopsy was adequate for another patient with an atypical nevus that was growing and changing rapidly but looked like a benign lesion, and proved to be so. With the saucerization, though, “we’ve got enough depth here to make the diagnosis, and if it were melanoma, to do histostaging,” he noted.
Disclosures: Dr. Gross said he has no pertinent conflicts of interest.
Monterey, Calif. — When Dr. Kenneth G. Gross wants to biopsy an atypical pigmented lesion, he reaches for an old-fashioned razor blade.
Not for a shave biopsy, mind you. He prefers a saucerization biopsy to a shave, punch, or blunt excisional biopsy for these lesions.
“The reason I prefer saucerization for atypical pigmented lesions—and even more for lentigo maligna—is that it takes the least amount of normal tissue. It allows the smallest wide re-excision. It’s fast. It’s easy—there’s no undermining—and it gives adequate histostaging,” he said at the annual meeting of the American Society for Mohs Surgery
He also likes that it requires the biopsy-taker to “engage your brain before you engage your blade,” said Dr. Gross, a dermatologic surgeon practicing in San Diego. “You’ve got to ask yourself, what information do I need to histostage this lesion?” to decide how you’ll bend the razor blade to get the depth and shape of biopsy required to provide the needed information.
A saucerization biopsy leaves a round defect that heals by secondary intention, and the lack of undermining makes wide re-excision relatively simple. A blunt excisional biopsy, on the other hand, takes longer, may violate the deep tissue plane that’s optimal for wide re-excision, and magnifies the size of the eventual wide re-excision.
“Are you really doing your patient a favor to take an excisional biopsy down to the base of the fat? Do you really need to go that far? To me, the answer is, ‘No,’ ” he said.
For his saucerization biopsies, Dr. Gross uses Personna stainless steel, double-edge prep blades designed for old-fashioned razors. Fold the two-blade package in half before opening, and the blades snap in half, providing one blunt edge to hold and a sharp edge for cutting.
“The nice thing about these little blades is that they’re sterile when they come out of the factory, and I have yet to see an infection in a biopsy site using these,” he said.
Fold the blade to any degree desired to do a very small, deep biopsy—“almost like a punch” biopsy—or a wider or more shallow biopsy, he explained. “For a lesion like lentigo maligna, you want a larger but more superficial biopsy.”
To avoid “flipping” a biopsy specimen, unbend the blade and lay it flat immediately after taking the specimen. “I’ve never flipped one yet,” he said.
On one patient with what looked on dermoscopy like a superficial spreading malignant melanoma, Dr. Gross took a saucerization biopsy with a 1- to 2-mm margin down to the middermis. Under the microscope, it looked to be a 0.7-mm superficial melanoma, so he did a wide re-excision. There was no residual tumor on the pathology report, “nor would I expect there to be any residual melanoma in most of these, because this is a saucerization-type excisional biopsy, if you will. It’s not a shave biopsy,” Dr. Gross said.
Razors are not only sharper than scalpel blades, they’re easier to use and can be curved either up or down for convex or concave surfaces, he added. The blades can be used virtually anywhere on the skin, on any type of tissue, to get specimens that are adequate for both diagnosis and histostaging.
Another patient had a lesion in the nail bed. “The patient has had this dystrophic nail for a while, notes some changes in the base, and I want to do a matrix biopsy. I want to see if there is any squamous cell carcinoma going on here,” Dr. Gross explains. “This is really simple task with this blade. I can fold it to any depth I want, any width. It is a simple, quick procedure.”
A small, not-so-deep saucerization biopsy was adequate for another patient with an atypical nevus that was growing and changing rapidly but looked like a benign lesion, and proved to be so. With the saucerization, though, “we’ve got enough depth here to make the diagnosis, and if it were melanoma, to do histostaging,” he noted.
Disclosures: Dr. Gross said he has no pertinent conflicts of interest.
Monterey, Calif. — When Dr. Kenneth G. Gross wants to biopsy an atypical pigmented lesion, he reaches for an old-fashioned razor blade.
Not for a shave biopsy, mind you. He prefers a saucerization biopsy to a shave, punch, or blunt excisional biopsy for these lesions.
“The reason I prefer saucerization for atypical pigmented lesions—and even more for lentigo maligna—is that it takes the least amount of normal tissue. It allows the smallest wide re-excision. It’s fast. It’s easy—there’s no undermining—and it gives adequate histostaging,” he said at the annual meeting of the American Society for Mohs Surgery
He also likes that it requires the biopsy-taker to “engage your brain before you engage your blade,” said Dr. Gross, a dermatologic surgeon practicing in San Diego. “You’ve got to ask yourself, what information do I need to histostage this lesion?” to decide how you’ll bend the razor blade to get the depth and shape of biopsy required to provide the needed information.
A saucerization biopsy leaves a round defect that heals by secondary intention, and the lack of undermining makes wide re-excision relatively simple. A blunt excisional biopsy, on the other hand, takes longer, may violate the deep tissue plane that’s optimal for wide re-excision, and magnifies the size of the eventual wide re-excision.
“Are you really doing your patient a favor to take an excisional biopsy down to the base of the fat? Do you really need to go that far? To me, the answer is, ‘No,’ ” he said.
For his saucerization biopsies, Dr. Gross uses Personna stainless steel, double-edge prep blades designed for old-fashioned razors. Fold the two-blade package in half before opening, and the blades snap in half, providing one blunt edge to hold and a sharp edge for cutting.
“The nice thing about these little blades is that they’re sterile when they come out of the factory, and I have yet to see an infection in a biopsy site using these,” he said.
Fold the blade to any degree desired to do a very small, deep biopsy—“almost like a punch” biopsy—or a wider or more shallow biopsy, he explained. “For a lesion like lentigo maligna, you want a larger but more superficial biopsy.”
To avoid “flipping” a biopsy specimen, unbend the blade and lay it flat immediately after taking the specimen. “I’ve never flipped one yet,” he said.
On one patient with what looked on dermoscopy like a superficial spreading malignant melanoma, Dr. Gross took a saucerization biopsy with a 1- to 2-mm margin down to the middermis. Under the microscope, it looked to be a 0.7-mm superficial melanoma, so he did a wide re-excision. There was no residual tumor on the pathology report, “nor would I expect there to be any residual melanoma in most of these, because this is a saucerization-type excisional biopsy, if you will. It’s not a shave biopsy,” Dr. Gross said.
Razors are not only sharper than scalpel blades, they’re easier to use and can be curved either up or down for convex or concave surfaces, he added. The blades can be used virtually anywhere on the skin, on any type of tissue, to get specimens that are adequate for both diagnosis and histostaging.
Another patient had a lesion in the nail bed. “The patient has had this dystrophic nail for a while, notes some changes in the base, and I want to do a matrix biopsy. I want to see if there is any squamous cell carcinoma going on here,” Dr. Gross explains. “This is really simple task with this blade. I can fold it to any depth I want, any width. It is a simple, quick procedure.”
A small, not-so-deep saucerization biopsy was adequate for another patient with an atypical nevus that was growing and changing rapidly but looked like a benign lesion, and proved to be so. With the saucerization, though, “we’ve got enough depth here to make the diagnosis, and if it were melanoma, to do histostaging,” he noted.
Disclosures: Dr. Gross said he has no pertinent conflicts of interest.
Avoiding Pitfalls, Complications in Reconstructive Surgery
Naples, Fla. - Before you start dermatologic reconstructive surgery, know the potential adverse events well, Dr. Keyvan Nouri said.
“It is important to be aware of complications, how to prevent them, and if they do occur, how to manage them,” he said at the annual meeting of the Florida Society of Dermatology & Dermatologic Surgeons
Bleeding, hematoma, nerve damage, infection, and contact dermatitis are among the adverse sequelae possible after surgery, Dr. Nouri said.
Acute bleeding is one of the most common complications in the immediate postoperative period, for example. Patients taking medications that alter hemostasis -- including aspirin, heparin, or warfarin -- are at higher risk, as are people with hypertension. “We don’t normally check blood pressure ... but [this] may be something you want to consider before surgery,” said Dr. Nouri, director of Mohs, Dermatologic and Laser Surgery at the University of Miami Leonard M. Miller School of Medicine.
To prevent medication-related bleeding, consult the prescribing physician to suggest discontinuation of the agent(s) prior to surgery, Dr. Nouri said. “We as dermatologists really have no role for stopping aspirin, Plavix, etc., beforehand.”
Strategies dermatologic surgeons can employ to minimize bleeding include use of sutures to ligate vessels, use of meticulous hemostasis during a procedure, and use of absorbable gel sponges to collect oozing from muscle and fascia, Dr. Nouri said. Also, observe areas at risk for bleeding for 10-15 minutes prior to closure if using uninterrupted sutures.
Pressure dressings help postoperatively. “Instruct patients to keep them on at least 48 hours,” he said.
A hematoma is another possible surgical complication. This “should be managed by urgently removing sutures and draining the hematoma,” Dr. Nouri said. If the bleeding does not stop, reopen the wound until you achieve hemostasis. If you place a drain to facilitate drainage, remember to remove it within 48 hours to avoid a heightened risk of infection.
Ecchymoses, another surgical complication, can be common, Dr. Nouri said, particularly when operating around the eyes or forehead. It results from blood passing through soft tissue planes. Instruct patients to apply ice on a regular basis postoperatively to minimize this effect.
Knowing your anatomy is essential to avoid damage to nerves or vital organs during surgery, Dr. Nouri said. “Know the facial danger zones.” The temporal area and angle of the jaw are examples. If the temporal nerve is damaged, the patient might be unable to lift their eyebrow after surgery. Also, an asymmetrical smile can result from damage to the submandibular branch at the angle of the jaw, he said.
Tendons also can be cut during surgery. Keep in mind that tendons become more superficial as you go more distally on the hands or lower extremities. “If a tendon is cut, we cannot repair it,” Dr. Nouri said. “The patient needs to be referred.”
The good news regarding contact dermatitis is it “used to happen a lot more in derm surgery,” Dr. Nouri said. Topical antibiotics, tapes and wound dressings, and nickel-plated surgical instruments can cause contact allergies. Watch for red, pruritic, or occasionally, vesiculated and crusted plaques. One tip is that pruritus is common with contact dermatitis, versus tenderness associated with infection.
Acute infections are rare in most dermatologic surgery patients, although immunosuppressed patients or those with uncontrolled diabetes are at higher risk, Dr. Nouri said. Malnutrition, obesity, smoking, and chronic use of steroids are other risk factors.
Also, remember to instruct patients not to shave prior to surgery. “Shaving less than 24 hours prior to surgery increases the risk of infection many times,” he noted.
Dermatologic surgery on a lower extremity carries a higher risk for infection, Dr. Nouri said. “Whenever I operate on someone’s legs, I use prophylactic antibiotics.”
Know that these and other adverse outcomes from surgery can occur, Dr. Nouri said. “Following the principles of tissue closure and antiseptic techniques will minimize these complications.”
Disclosures: Dr. Nouri said he had no relevant financial disclosures.
Naples, Fla. - Before you start dermatologic reconstructive surgery, know the potential adverse events well, Dr. Keyvan Nouri said.
“It is important to be aware of complications, how to prevent them, and if they do occur, how to manage them,” he said at the annual meeting of the Florida Society of Dermatology & Dermatologic Surgeons
Bleeding, hematoma, nerve damage, infection, and contact dermatitis are among the adverse sequelae possible after surgery, Dr. Nouri said.
Acute bleeding is one of the most common complications in the immediate postoperative period, for example. Patients taking medications that alter hemostasis -- including aspirin, heparin, or warfarin -- are at higher risk, as are people with hypertension. “We don’t normally check blood pressure ... but [this] may be something you want to consider before surgery,” said Dr. Nouri, director of Mohs, Dermatologic and Laser Surgery at the University of Miami Leonard M. Miller School of Medicine.
To prevent medication-related bleeding, consult the prescribing physician to suggest discontinuation of the agent(s) prior to surgery, Dr. Nouri said. “We as dermatologists really have no role for stopping aspirin, Plavix, etc., beforehand.”
Strategies dermatologic surgeons can employ to minimize bleeding include use of sutures to ligate vessels, use of meticulous hemostasis during a procedure, and use of absorbable gel sponges to collect oozing from muscle and fascia, Dr. Nouri said. Also, observe areas at risk for bleeding for 10-15 minutes prior to closure if using uninterrupted sutures.
Pressure dressings help postoperatively. “Instruct patients to keep them on at least 48 hours,” he said.
A hematoma is another possible surgical complication. This “should be managed by urgently removing sutures and draining the hematoma,” Dr. Nouri said. If the bleeding does not stop, reopen the wound until you achieve hemostasis. If you place a drain to facilitate drainage, remember to remove it within 48 hours to avoid a heightened risk of infection.
Ecchymoses, another surgical complication, can be common, Dr. Nouri said, particularly when operating around the eyes or forehead. It results from blood passing through soft tissue planes. Instruct patients to apply ice on a regular basis postoperatively to minimize this effect.
Knowing your anatomy is essential to avoid damage to nerves or vital organs during surgery, Dr. Nouri said. “Know the facial danger zones.” The temporal area and angle of the jaw are examples. If the temporal nerve is damaged, the patient might be unable to lift their eyebrow after surgery. Also, an asymmetrical smile can result from damage to the submandibular branch at the angle of the jaw, he said.
Tendons also can be cut during surgery. Keep in mind that tendons become more superficial as you go more distally on the hands or lower extremities. “If a tendon is cut, we cannot repair it,” Dr. Nouri said. “The patient needs to be referred.”
The good news regarding contact dermatitis is it “used to happen a lot more in derm surgery,” Dr. Nouri said. Topical antibiotics, tapes and wound dressings, and nickel-plated surgical instruments can cause contact allergies. Watch for red, pruritic, or occasionally, vesiculated and crusted plaques. One tip is that pruritus is common with contact dermatitis, versus tenderness associated with infection.
Acute infections are rare in most dermatologic surgery patients, although immunosuppressed patients or those with uncontrolled diabetes are at higher risk, Dr. Nouri said. Malnutrition, obesity, smoking, and chronic use of steroids are other risk factors.
Also, remember to instruct patients not to shave prior to surgery. “Shaving less than 24 hours prior to surgery increases the risk of infection many times,” he noted.
Dermatologic surgery on a lower extremity carries a higher risk for infection, Dr. Nouri said. “Whenever I operate on someone’s legs, I use prophylactic antibiotics.”
Know that these and other adverse outcomes from surgery can occur, Dr. Nouri said. “Following the principles of tissue closure and antiseptic techniques will minimize these complications.”
Disclosures: Dr. Nouri said he had no relevant financial disclosures.
Naples, Fla. - Before you start dermatologic reconstructive surgery, know the potential adverse events well, Dr. Keyvan Nouri said.
“It is important to be aware of complications, how to prevent them, and if they do occur, how to manage them,” he said at the annual meeting of the Florida Society of Dermatology & Dermatologic Surgeons
Bleeding, hematoma, nerve damage, infection, and contact dermatitis are among the adverse sequelae possible after surgery, Dr. Nouri said.
Acute bleeding is one of the most common complications in the immediate postoperative period, for example. Patients taking medications that alter hemostasis -- including aspirin, heparin, or warfarin -- are at higher risk, as are people with hypertension. “We don’t normally check blood pressure ... but [this] may be something you want to consider before surgery,” said Dr. Nouri, director of Mohs, Dermatologic and Laser Surgery at the University of Miami Leonard M. Miller School of Medicine.
To prevent medication-related bleeding, consult the prescribing physician to suggest discontinuation of the agent(s) prior to surgery, Dr. Nouri said. “We as dermatologists really have no role for stopping aspirin, Plavix, etc., beforehand.”
Strategies dermatologic surgeons can employ to minimize bleeding include use of sutures to ligate vessels, use of meticulous hemostasis during a procedure, and use of absorbable gel sponges to collect oozing from muscle and fascia, Dr. Nouri said. Also, observe areas at risk for bleeding for 10-15 minutes prior to closure if using uninterrupted sutures.
Pressure dressings help postoperatively. “Instruct patients to keep them on at least 48 hours,” he said.
A hematoma is another possible surgical complication. This “should be managed by urgently removing sutures and draining the hematoma,” Dr. Nouri said. If the bleeding does not stop, reopen the wound until you achieve hemostasis. If you place a drain to facilitate drainage, remember to remove it within 48 hours to avoid a heightened risk of infection.
Ecchymoses, another surgical complication, can be common, Dr. Nouri said, particularly when operating around the eyes or forehead. It results from blood passing through soft tissue planes. Instruct patients to apply ice on a regular basis postoperatively to minimize this effect.
Knowing your anatomy is essential to avoid damage to nerves or vital organs during surgery, Dr. Nouri said. “Know the facial danger zones.” The temporal area and angle of the jaw are examples. If the temporal nerve is damaged, the patient might be unable to lift their eyebrow after surgery. Also, an asymmetrical smile can result from damage to the submandibular branch at the angle of the jaw, he said.
Tendons also can be cut during surgery. Keep in mind that tendons become more superficial as you go more distally on the hands or lower extremities. “If a tendon is cut, we cannot repair it,” Dr. Nouri said. “The patient needs to be referred.”
The good news regarding contact dermatitis is it “used to happen a lot more in derm surgery,” Dr. Nouri said. Topical antibiotics, tapes and wound dressings, and nickel-plated surgical instruments can cause contact allergies. Watch for red, pruritic, or occasionally, vesiculated and crusted plaques. One tip is that pruritus is common with contact dermatitis, versus tenderness associated with infection.
Acute infections are rare in most dermatologic surgery patients, although immunosuppressed patients or those with uncontrolled diabetes are at higher risk, Dr. Nouri said. Malnutrition, obesity, smoking, and chronic use of steroids are other risk factors.
Also, remember to instruct patients not to shave prior to surgery. “Shaving less than 24 hours prior to surgery increases the risk of infection many times,” he noted.
Dermatologic surgery on a lower extremity carries a higher risk for infection, Dr. Nouri said. “Whenever I operate on someone’s legs, I use prophylactic antibiotics.”
Know that these and other adverse outcomes from surgery can occur, Dr. Nouri said. “Following the principles of tissue closure and antiseptic techniques will minimize these complications.”
Disclosures: Dr. Nouri said he had no relevant financial disclosures.
Mercury
Mercury, long known as a toxic substance, is making a comeback in skin products, and dermatologists should familiarize themselves with both the dangers and the availability of this all-too-common cosmeceutical ingredient.
The ancient Egyptians and Romans used mercury to lighten the skin and in a variety of ointments, and the Greeks and Egyptians used it to treat skin infections (Environ. Health Perspect. 2002;110:11-23).
While versatile and used for diverse purposes for many years, such as in thermometers and in dental amalgams, mercury and its related compounds have long been known to be extremely toxic and should be avoided in food and skin care. Indeed, the wide-ranging adverse health effects of mercury-containing skin-lightening products have been known since the early 1970s (Arthritis Rheum. 2007;56:1721).
While mercury has been banned in skin care products sold in the United States since 1990, it is found in numerous skin-lightening agents sold elsewhere. In Europe, such a ban was enacted in 1976. Recently, some of these products have made their way onto U.S. shelves and, to the surprise of many, have been reported to contain toxic levels of mercury. This column will review some of the latest data on mercury-containing skin products and describe the current emerging controversy.
Renewed Popularity
Skin-lightening agents that contain mercury have become increasingly popular in recent years, especially among women with dark skin (Biometals 2004;17:167-75). In particular, skin-lightening cosmetics that contain hydroquinone, mercury, and/or corticosteroids are used widely in many African countries, and especially in sub-Saharan Africa (Med. Trop. 2007;67:627-34). While effective as a whitening agent, mercury is a toxic heavy metal that can produce deleterious effects on humans, through ingestion, skin contact, or inhalation.
The primary vectors for exposure have been metallic or elemental mercury in dental amalgams, ethylmercury in the form of thimerosal in vaccines, and methylmercury in seafood. Metallic mercury also is found in thermometers, organic mercury is used in paints and fungicides, and inorganic mercury compounds are used in medicinal and skin care formulations. The present surge in the use of mercury in skin-lightening formulations, as well as in some religious rituals, has added avenues for mercury exposure (Biol. Trace Elem. Res. 2009;131:43-54; Crit. Rev. Toxicol. 2006;36:609-62; J. Pediatr. Health Care 2007;21:307-14; Int. J. Dermatol. 2008;47:344-53; Environ. Health Perspect. 2002;110:11-23; Rev. Environ. Health 2005;20:39-56; Br. J. Dermatol. 1968;80:623-4).
Some researchers have noted that in Africa, percutaneous absorption is facilitated by the conditions under which these products are used, that is, for long periods, over a large body surface area, and in hot, humid weather. Palmer et al. showed in a human in vitro model that mercury was readily absorbed in the skin in a comparison between an aqueous formulation, which exhibited a significantly higher rate and further extent of absorption, and a proprietary formulation. Their study was prompted partly by the popularity of the mercurous chloride–containing beauty cream Crema de Belleza-Manning, a popular agent used to lighten and smooth the skin and to treat acne. The cream has been linked to elevated urinary mercury levels in hundreds of people in the southwestern U.S. border states (J. Toxicol. Clin. Toxicol. 2000;38:701-7).
Complications of Chronic Exposure
Olumide et al. have reported that the potentially serious results of the chronic use of these agents include exogenous ochronosis; compromised wound healing and wound dehiscence; fish odor syndrome; nephropathy; steroid addiction syndrome; predisposition to infections; and various cutaneous and endocrinologic complications of steroid use, including suppression of the hypothalamic-pituitary-adrenal axis and death (Int. J. Dermatol. 2008;47:344-53).
Other dermatologic complications associated with mercury include dyschromia, acne and hypertrichosis, striae, tinea corporis, pyoderma, erysipelas, scabies, and contact dermatitis (Med. Trop. 2007;67:627-34).
In 1997, Al-Saleh and Al-Doush evaluated 38 skin-lightening creams available on the Saudi Arabian market and elsewhere, and analyzed them for mercury. They found that about 45% of the tested samples contained mercury at levels far surpassing 1 ppm (the maximum permitted by the Food and Drug Administration) (J. Toxicol. Environ. Health. 1997;51:123-30).
In 2003, Al-Saleh et al. issued an urgent warning in relation to their mercury research. They examined the effects of Rose skin-lightening cream (with a mercury content of 77,513 plus or minus 71,063 ppm) topically applied on mice over a 1-month period at varying intervals. By collecting 58 brain, kidney, and liver samples, the researchers determined that the mercury content of the samples was significantly higher in mice treated three times daily, compared with those treated once weekly, although histopathologic changes were observed in all tissue samples. The authors concluded that their study highlighted the potential toxicity of skin-lightening creams containing mercury, and that banning their manufacture and use is warranted (J. Environ. Pathol. Toxicol. Oncol. 2003;22:287-99).
In a subsequent study, many of the same investigators measured the accumulation of mercury in the tissues of albino and pigmented mice treated with the Rose or Fair & Lovely (with a mercury content of 0.304 plus or minus 0.316 mcg/g) brands of skin-lightening agents. Among 133 and 144 respective brain, kidney, and liver tissue samples of albino and pigmented mice, significantly more mercury was identified in tissues treated with Rose cream. The highest mercury concentrations were found in the tissues of mice, albino and pigmented, treated three times daily, whereas the smallest concentrations were in the tissues of mice treated once daily. The investigators also noted that mercury was readily absorbed into and accumulated in the tissues of albino and pigmented mice treated with either brand of skin-lightening agent. Tissues from pigmented mice were less affected, however, suggesting the protective capacity of melanin against mercury. Nonetheless, given the higher concentration of mercury in the Rose cream, this study reinforced the danger of repeated use of mercury-containing creams containing even low levels of the element, concluded the researchers (Biometals 2004;17:167-75)
In 2005, Al-Saleh et al. investigated the toxic effects on mice of Fair & Lovely, which is sold widely over-the-counter in Saudi Arabia and more than 35 other countries (Arthritis Rheum. 2007;56:1721). As in the previous work, the study period was 1 month and the agent was applied at different intervals, with mercury concentrations measured in brain, kidney, and liver samples from 75 adult female CD1 mice. Mean mercury concentrations in the tissues of treated mice were found to be significantly higher than in samples from controls (0.193 vs. 0.041 mcg/g). Treated mice also exhibited significant declines in body weight and histologic changes in kidney and, more moderately, in brain and liver tissue. The investigators concluded that histopathologic changes are associated with this mercury-containing skin-lightening agent, even though its mercury content falls below 1 ppm (Cutan. Ocul. Toxicol. 2005;24:11-29). Furthermore, as pointed out by Pollard and Hultman, Fair & Lovely can be purchased throughout the world and is available online (Arthritis Rheum. 2007;56:1721).
Given the widespread use of skin-lightening creams, primarily by women but also by men, and the substantial risks of mercury toxicity posed by the chronic use of these agents, especially to pregnant and nursing mothers, Al-Saleh et al. measured the mercury levels in 49 murine ovary tissue samples. They compared the ovaries of untreated mice, those treated with Rose skin-lightening cream, and those treated with Fair & Lovely skin-lightening cream. Mercury content increased with increasing frequency of application, and was highest in samples from mice treated twice daily with Fair & Lovely (87.79 ng/g) and once daily with Rose (3,515.61 ng/g). The researchers concluded that while more research is needed, significant mercury accumulation in the ovaries can result from dermal exposure to mercury-containing skin creams that can alter the reproductive system and lead to infertility.
While they suggested that banning such creams would be ideal, they acknowledged that circumventing the popularity of these products might be better achieved if public health officials urged the use of prescription treatments for skin pigmentation rather than over-the-counter solutions. The authors also warned that women who regularly use such products are at particular risk, because there are no symptoms of early exposure; mercury toxicity develops from chronic use (Biol. Trace Elem. Res. 2009;131:43-54).
Like indoor tanning, mercury-containing skin creams occupy a nexus between dermatology, human behavior, public policy, and the law. In addition to various national bans that have been enacted, some U.S. states have gotten in on the act. According to a report by the Associated Press, on Jan. 1, 2008, a Minnesota law took effect that prohibits mercury from mascara, eyeliners, and skin-lightening creams; federal law allows eye formulations to contain mercury up to 65 ppm.
Availability of Mercury-Containing Products
In the United States, regulations regarding over-the-counter products are much weaker than those pertaining to prescription drugs. As a result, mercury-containing substances have penetrated the market (and online purchasing is a loophole of the modern era) to an extent that may surprise many, particularly considering how mercury laden some of these products are.
For a story on this topic, Chicago Tribune reporters purchased 50 skin-lightening creams in Chicago stores or online, and sent them to a certified laboratory for testing. The laboratory results revealed that six of the creams contained illegal amounts of mercury (at 6,000 ppm or more in five of those formulations) (Chicago Tribune, May 18, 2010). The newspaper contacted retailers, who said they would remove the products from shelves, with two distributors claiming that they would stop selling these products. The worst offender had a mercury level close to 30,000 ppm. The six creams that tested high originated in China, India, Lebanon, Pakistan, and Taiwan. The Web site http://www.whiterskin.info/ is tracking the number and names of skin-lightening products found to contain dangerous levels of mercury. According to the Tribune article, the FDA has fewer than 500 inspectors, and the agency has not considered mercury in skin creams since 2006.
At the international level, on June 11, 2010, a PR Newswire story reported that representatives of 132 countries, meeting under the auspices of the United Nations Environment Programme, paved the way toward a treaty to control mercury pollution. The gathering, dubbed the first Intergovernmental Negotiating Committee (INC) meeting, in Stockholm, has set the stage for developing the text of the treaty, the drafting of which will begin at the next INC meeting in Tokyo in January 2011. At the June meeting, a World Health Organization representative stated that the goal will be to halt production of skin-lightening cosmetics that contain mercury. Five INC meetings are expected to convene to complete the treaty before 2013.
Conclusion
It is incumbent upon dermatologists to use all of the tools in their arsenal to convince patients to accept their skin tone as it is. In other words, we should discourage those who attempt to lighten their skin for reasons not pertaining to correcting dyspigmentation, just as we discourage patients seeking to tan or darken their skin.
For patients resistant to such advice or cajolery, practitioners must warn them about using skin-lightening products that contain mercury and recommend alternative lightening agents. Clearly, formulations containing mercury, though banned in the United States, are becoming increasingly available, and as over-the-counter products they are not tightly regulated. These products pose a serious health risk.
Mercury, long known as a toxic substance, is making a comeback in skin products, and dermatologists should familiarize themselves with both the dangers and the availability of this all-too-common cosmeceutical ingredient.
The ancient Egyptians and Romans used mercury to lighten the skin and in a variety of ointments, and the Greeks and Egyptians used it to treat skin infections (Environ. Health Perspect. 2002;110:11-23).
While versatile and used for diverse purposes for many years, such as in thermometers and in dental amalgams, mercury and its related compounds have long been known to be extremely toxic and should be avoided in food and skin care. Indeed, the wide-ranging adverse health effects of mercury-containing skin-lightening products have been known since the early 1970s (Arthritis Rheum. 2007;56:1721).
While mercury has been banned in skin care products sold in the United States since 1990, it is found in numerous skin-lightening agents sold elsewhere. In Europe, such a ban was enacted in 1976. Recently, some of these products have made their way onto U.S. shelves and, to the surprise of many, have been reported to contain toxic levels of mercury. This column will review some of the latest data on mercury-containing skin products and describe the current emerging controversy.
Renewed Popularity
Skin-lightening agents that contain mercury have become increasingly popular in recent years, especially among women with dark skin (Biometals 2004;17:167-75). In particular, skin-lightening cosmetics that contain hydroquinone, mercury, and/or corticosteroids are used widely in many African countries, and especially in sub-Saharan Africa (Med. Trop. 2007;67:627-34). While effective as a whitening agent, mercury is a toxic heavy metal that can produce deleterious effects on humans, through ingestion, skin contact, or inhalation.
The primary vectors for exposure have been metallic or elemental mercury in dental amalgams, ethylmercury in the form of thimerosal in vaccines, and methylmercury in seafood. Metallic mercury also is found in thermometers, organic mercury is used in paints and fungicides, and inorganic mercury compounds are used in medicinal and skin care formulations. The present surge in the use of mercury in skin-lightening formulations, as well as in some religious rituals, has added avenues for mercury exposure (Biol. Trace Elem. Res. 2009;131:43-54; Crit. Rev. Toxicol. 2006;36:609-62; J. Pediatr. Health Care 2007;21:307-14; Int. J. Dermatol. 2008;47:344-53; Environ. Health Perspect. 2002;110:11-23; Rev. Environ. Health 2005;20:39-56; Br. J. Dermatol. 1968;80:623-4).
Some researchers have noted that in Africa, percutaneous absorption is facilitated by the conditions under which these products are used, that is, for long periods, over a large body surface area, and in hot, humid weather. Palmer et al. showed in a human in vitro model that mercury was readily absorbed in the skin in a comparison between an aqueous formulation, which exhibited a significantly higher rate and further extent of absorption, and a proprietary formulation. Their study was prompted partly by the popularity of the mercurous chloride–containing beauty cream Crema de Belleza-Manning, a popular agent used to lighten and smooth the skin and to treat acne. The cream has been linked to elevated urinary mercury levels in hundreds of people in the southwestern U.S. border states (J. Toxicol. Clin. Toxicol. 2000;38:701-7).
Complications of Chronic Exposure
Olumide et al. have reported that the potentially serious results of the chronic use of these agents include exogenous ochronosis; compromised wound healing and wound dehiscence; fish odor syndrome; nephropathy; steroid addiction syndrome; predisposition to infections; and various cutaneous and endocrinologic complications of steroid use, including suppression of the hypothalamic-pituitary-adrenal axis and death (Int. J. Dermatol. 2008;47:344-53).
Other dermatologic complications associated with mercury include dyschromia, acne and hypertrichosis, striae, tinea corporis, pyoderma, erysipelas, scabies, and contact dermatitis (Med. Trop. 2007;67:627-34).
In 1997, Al-Saleh and Al-Doush evaluated 38 skin-lightening creams available on the Saudi Arabian market and elsewhere, and analyzed them for mercury. They found that about 45% of the tested samples contained mercury at levels far surpassing 1 ppm (the maximum permitted by the Food and Drug Administration) (J. Toxicol. Environ. Health. 1997;51:123-30).
In 2003, Al-Saleh et al. issued an urgent warning in relation to their mercury research. They examined the effects of Rose skin-lightening cream (with a mercury content of 77,513 plus or minus 71,063 ppm) topically applied on mice over a 1-month period at varying intervals. By collecting 58 brain, kidney, and liver samples, the researchers determined that the mercury content of the samples was significantly higher in mice treated three times daily, compared with those treated once weekly, although histopathologic changes were observed in all tissue samples. The authors concluded that their study highlighted the potential toxicity of skin-lightening creams containing mercury, and that banning their manufacture and use is warranted (J. Environ. Pathol. Toxicol. Oncol. 2003;22:287-99).
In a subsequent study, many of the same investigators measured the accumulation of mercury in the tissues of albino and pigmented mice treated with the Rose or Fair & Lovely (with a mercury content of 0.304 plus or minus 0.316 mcg/g) brands of skin-lightening agents. Among 133 and 144 respective brain, kidney, and liver tissue samples of albino and pigmented mice, significantly more mercury was identified in tissues treated with Rose cream. The highest mercury concentrations were found in the tissues of mice, albino and pigmented, treated three times daily, whereas the smallest concentrations were in the tissues of mice treated once daily. The investigators also noted that mercury was readily absorbed into and accumulated in the tissues of albino and pigmented mice treated with either brand of skin-lightening agent. Tissues from pigmented mice were less affected, however, suggesting the protective capacity of melanin against mercury. Nonetheless, given the higher concentration of mercury in the Rose cream, this study reinforced the danger of repeated use of mercury-containing creams containing even low levels of the element, concluded the researchers (Biometals 2004;17:167-75)
In 2005, Al-Saleh et al. investigated the toxic effects on mice of Fair & Lovely, which is sold widely over-the-counter in Saudi Arabia and more than 35 other countries (Arthritis Rheum. 2007;56:1721). As in the previous work, the study period was 1 month and the agent was applied at different intervals, with mercury concentrations measured in brain, kidney, and liver samples from 75 adult female CD1 mice. Mean mercury concentrations in the tissues of treated mice were found to be significantly higher than in samples from controls (0.193 vs. 0.041 mcg/g). Treated mice also exhibited significant declines in body weight and histologic changes in kidney and, more moderately, in brain and liver tissue. The investigators concluded that histopathologic changes are associated with this mercury-containing skin-lightening agent, even though its mercury content falls below 1 ppm (Cutan. Ocul. Toxicol. 2005;24:11-29). Furthermore, as pointed out by Pollard and Hultman, Fair & Lovely can be purchased throughout the world and is available online (Arthritis Rheum. 2007;56:1721).
Given the widespread use of skin-lightening creams, primarily by women but also by men, and the substantial risks of mercury toxicity posed by the chronic use of these agents, especially to pregnant and nursing mothers, Al-Saleh et al. measured the mercury levels in 49 murine ovary tissue samples. They compared the ovaries of untreated mice, those treated with Rose skin-lightening cream, and those treated with Fair & Lovely skin-lightening cream. Mercury content increased with increasing frequency of application, and was highest in samples from mice treated twice daily with Fair & Lovely (87.79 ng/g) and once daily with Rose (3,515.61 ng/g). The researchers concluded that while more research is needed, significant mercury accumulation in the ovaries can result from dermal exposure to mercury-containing skin creams that can alter the reproductive system and lead to infertility.
While they suggested that banning such creams would be ideal, they acknowledged that circumventing the popularity of these products might be better achieved if public health officials urged the use of prescription treatments for skin pigmentation rather than over-the-counter solutions. The authors also warned that women who regularly use such products are at particular risk, because there are no symptoms of early exposure; mercury toxicity develops from chronic use (Biol. Trace Elem. Res. 2009;131:43-54).
Like indoor tanning, mercury-containing skin creams occupy a nexus between dermatology, human behavior, public policy, and the law. In addition to various national bans that have been enacted, some U.S. states have gotten in on the act. According to a report by the Associated Press, on Jan. 1, 2008, a Minnesota law took effect that prohibits mercury from mascara, eyeliners, and skin-lightening creams; federal law allows eye formulations to contain mercury up to 65 ppm.
Availability of Mercury-Containing Products
In the United States, regulations regarding over-the-counter products are much weaker than those pertaining to prescription drugs. As a result, mercury-containing substances have penetrated the market (and online purchasing is a loophole of the modern era) to an extent that may surprise many, particularly considering how mercury laden some of these products are.
For a story on this topic, Chicago Tribune reporters purchased 50 skin-lightening creams in Chicago stores or online, and sent them to a certified laboratory for testing. The laboratory results revealed that six of the creams contained illegal amounts of mercury (at 6,000 ppm or more in five of those formulations) (Chicago Tribune, May 18, 2010). The newspaper contacted retailers, who said they would remove the products from shelves, with two distributors claiming that they would stop selling these products. The worst offender had a mercury level close to 30,000 ppm. The six creams that tested high originated in China, India, Lebanon, Pakistan, and Taiwan. The Web site http://www.whiterskin.info/ is tracking the number and names of skin-lightening products found to contain dangerous levels of mercury. According to the Tribune article, the FDA has fewer than 500 inspectors, and the agency has not considered mercury in skin creams since 2006.
At the international level, on June 11, 2010, a PR Newswire story reported that representatives of 132 countries, meeting under the auspices of the United Nations Environment Programme, paved the way toward a treaty to control mercury pollution. The gathering, dubbed the first Intergovernmental Negotiating Committee (INC) meeting, in Stockholm, has set the stage for developing the text of the treaty, the drafting of which will begin at the next INC meeting in Tokyo in January 2011. At the June meeting, a World Health Organization representative stated that the goal will be to halt production of skin-lightening cosmetics that contain mercury. Five INC meetings are expected to convene to complete the treaty before 2013.
Conclusion
It is incumbent upon dermatologists to use all of the tools in their arsenal to convince patients to accept their skin tone as it is. In other words, we should discourage those who attempt to lighten their skin for reasons not pertaining to correcting dyspigmentation, just as we discourage patients seeking to tan or darken their skin.
For patients resistant to such advice or cajolery, practitioners must warn them about using skin-lightening products that contain mercury and recommend alternative lightening agents. Clearly, formulations containing mercury, though banned in the United States, are becoming increasingly available, and as over-the-counter products they are not tightly regulated. These products pose a serious health risk.
Mercury, long known as a toxic substance, is making a comeback in skin products, and dermatologists should familiarize themselves with both the dangers and the availability of this all-too-common cosmeceutical ingredient.
The ancient Egyptians and Romans used mercury to lighten the skin and in a variety of ointments, and the Greeks and Egyptians used it to treat skin infections (Environ. Health Perspect. 2002;110:11-23).
While versatile and used for diverse purposes for many years, such as in thermometers and in dental amalgams, mercury and its related compounds have long been known to be extremely toxic and should be avoided in food and skin care. Indeed, the wide-ranging adverse health effects of mercury-containing skin-lightening products have been known since the early 1970s (Arthritis Rheum. 2007;56:1721).
While mercury has been banned in skin care products sold in the United States since 1990, it is found in numerous skin-lightening agents sold elsewhere. In Europe, such a ban was enacted in 1976. Recently, some of these products have made their way onto U.S. shelves and, to the surprise of many, have been reported to contain toxic levels of mercury. This column will review some of the latest data on mercury-containing skin products and describe the current emerging controversy.
Renewed Popularity
Skin-lightening agents that contain mercury have become increasingly popular in recent years, especially among women with dark skin (Biometals 2004;17:167-75). In particular, skin-lightening cosmetics that contain hydroquinone, mercury, and/or corticosteroids are used widely in many African countries, and especially in sub-Saharan Africa (Med. Trop. 2007;67:627-34). While effective as a whitening agent, mercury is a toxic heavy metal that can produce deleterious effects on humans, through ingestion, skin contact, or inhalation.
The primary vectors for exposure have been metallic or elemental mercury in dental amalgams, ethylmercury in the form of thimerosal in vaccines, and methylmercury in seafood. Metallic mercury also is found in thermometers, organic mercury is used in paints and fungicides, and inorganic mercury compounds are used in medicinal and skin care formulations. The present surge in the use of mercury in skin-lightening formulations, as well as in some religious rituals, has added avenues for mercury exposure (Biol. Trace Elem. Res. 2009;131:43-54; Crit. Rev. Toxicol. 2006;36:609-62; J. Pediatr. Health Care 2007;21:307-14; Int. J. Dermatol. 2008;47:344-53; Environ. Health Perspect. 2002;110:11-23; Rev. Environ. Health 2005;20:39-56; Br. J. Dermatol. 1968;80:623-4).
Some researchers have noted that in Africa, percutaneous absorption is facilitated by the conditions under which these products are used, that is, for long periods, over a large body surface area, and in hot, humid weather. Palmer et al. showed in a human in vitro model that mercury was readily absorbed in the skin in a comparison between an aqueous formulation, which exhibited a significantly higher rate and further extent of absorption, and a proprietary formulation. Their study was prompted partly by the popularity of the mercurous chloride–containing beauty cream Crema de Belleza-Manning, a popular agent used to lighten and smooth the skin and to treat acne. The cream has been linked to elevated urinary mercury levels in hundreds of people in the southwestern U.S. border states (J. Toxicol. Clin. Toxicol. 2000;38:701-7).
Complications of Chronic Exposure
Olumide et al. have reported that the potentially serious results of the chronic use of these agents include exogenous ochronosis; compromised wound healing and wound dehiscence; fish odor syndrome; nephropathy; steroid addiction syndrome; predisposition to infections; and various cutaneous and endocrinologic complications of steroid use, including suppression of the hypothalamic-pituitary-adrenal axis and death (Int. J. Dermatol. 2008;47:344-53).
Other dermatologic complications associated with mercury include dyschromia, acne and hypertrichosis, striae, tinea corporis, pyoderma, erysipelas, scabies, and contact dermatitis (Med. Trop. 2007;67:627-34).
In 1997, Al-Saleh and Al-Doush evaluated 38 skin-lightening creams available on the Saudi Arabian market and elsewhere, and analyzed them for mercury. They found that about 45% of the tested samples contained mercury at levels far surpassing 1 ppm (the maximum permitted by the Food and Drug Administration) (J. Toxicol. Environ. Health. 1997;51:123-30).
In 2003, Al-Saleh et al. issued an urgent warning in relation to their mercury research. They examined the effects of Rose skin-lightening cream (with a mercury content of 77,513 plus or minus 71,063 ppm) topically applied on mice over a 1-month period at varying intervals. By collecting 58 brain, kidney, and liver samples, the researchers determined that the mercury content of the samples was significantly higher in mice treated three times daily, compared with those treated once weekly, although histopathologic changes were observed in all tissue samples. The authors concluded that their study highlighted the potential toxicity of skin-lightening creams containing mercury, and that banning their manufacture and use is warranted (J. Environ. Pathol. Toxicol. Oncol. 2003;22:287-99).
In a subsequent study, many of the same investigators measured the accumulation of mercury in the tissues of albino and pigmented mice treated with the Rose or Fair & Lovely (with a mercury content of 0.304 plus or minus 0.316 mcg/g) brands of skin-lightening agents. Among 133 and 144 respective brain, kidney, and liver tissue samples of albino and pigmented mice, significantly more mercury was identified in tissues treated with Rose cream. The highest mercury concentrations were found in the tissues of mice, albino and pigmented, treated three times daily, whereas the smallest concentrations were in the tissues of mice treated once daily. The investigators also noted that mercury was readily absorbed into and accumulated in the tissues of albino and pigmented mice treated with either brand of skin-lightening agent. Tissues from pigmented mice were less affected, however, suggesting the protective capacity of melanin against mercury. Nonetheless, given the higher concentration of mercury in the Rose cream, this study reinforced the danger of repeated use of mercury-containing creams containing even low levels of the element, concluded the researchers (Biometals 2004;17:167-75)
In 2005, Al-Saleh et al. investigated the toxic effects on mice of Fair & Lovely, which is sold widely over-the-counter in Saudi Arabia and more than 35 other countries (Arthritis Rheum. 2007;56:1721). As in the previous work, the study period was 1 month and the agent was applied at different intervals, with mercury concentrations measured in brain, kidney, and liver samples from 75 adult female CD1 mice. Mean mercury concentrations in the tissues of treated mice were found to be significantly higher than in samples from controls (0.193 vs. 0.041 mcg/g). Treated mice also exhibited significant declines in body weight and histologic changes in kidney and, more moderately, in brain and liver tissue. The investigators concluded that histopathologic changes are associated with this mercury-containing skin-lightening agent, even though its mercury content falls below 1 ppm (Cutan. Ocul. Toxicol. 2005;24:11-29). Furthermore, as pointed out by Pollard and Hultman, Fair & Lovely can be purchased throughout the world and is available online (Arthritis Rheum. 2007;56:1721).
Given the widespread use of skin-lightening creams, primarily by women but also by men, and the substantial risks of mercury toxicity posed by the chronic use of these agents, especially to pregnant and nursing mothers, Al-Saleh et al. measured the mercury levels in 49 murine ovary tissue samples. They compared the ovaries of untreated mice, those treated with Rose skin-lightening cream, and those treated with Fair & Lovely skin-lightening cream. Mercury content increased with increasing frequency of application, and was highest in samples from mice treated twice daily with Fair & Lovely (87.79 ng/g) and once daily with Rose (3,515.61 ng/g). The researchers concluded that while more research is needed, significant mercury accumulation in the ovaries can result from dermal exposure to mercury-containing skin creams that can alter the reproductive system and lead to infertility.
While they suggested that banning such creams would be ideal, they acknowledged that circumventing the popularity of these products might be better achieved if public health officials urged the use of prescription treatments for skin pigmentation rather than over-the-counter solutions. The authors also warned that women who regularly use such products are at particular risk, because there are no symptoms of early exposure; mercury toxicity develops from chronic use (Biol. Trace Elem. Res. 2009;131:43-54).
Like indoor tanning, mercury-containing skin creams occupy a nexus between dermatology, human behavior, public policy, and the law. In addition to various national bans that have been enacted, some U.S. states have gotten in on the act. According to a report by the Associated Press, on Jan. 1, 2008, a Minnesota law took effect that prohibits mercury from mascara, eyeliners, and skin-lightening creams; federal law allows eye formulations to contain mercury up to 65 ppm.
Availability of Mercury-Containing Products
In the United States, regulations regarding over-the-counter products are much weaker than those pertaining to prescription drugs. As a result, mercury-containing substances have penetrated the market (and online purchasing is a loophole of the modern era) to an extent that may surprise many, particularly considering how mercury laden some of these products are.
For a story on this topic, Chicago Tribune reporters purchased 50 skin-lightening creams in Chicago stores or online, and sent them to a certified laboratory for testing. The laboratory results revealed that six of the creams contained illegal amounts of mercury (at 6,000 ppm or more in five of those formulations) (Chicago Tribune, May 18, 2010). The newspaper contacted retailers, who said they would remove the products from shelves, with two distributors claiming that they would stop selling these products. The worst offender had a mercury level close to 30,000 ppm. The six creams that tested high originated in China, India, Lebanon, Pakistan, and Taiwan. The Web site http://www.whiterskin.info/ is tracking the number and names of skin-lightening products found to contain dangerous levels of mercury. According to the Tribune article, the FDA has fewer than 500 inspectors, and the agency has not considered mercury in skin creams since 2006.
At the international level, on June 11, 2010, a PR Newswire story reported that representatives of 132 countries, meeting under the auspices of the United Nations Environment Programme, paved the way toward a treaty to control mercury pollution. The gathering, dubbed the first Intergovernmental Negotiating Committee (INC) meeting, in Stockholm, has set the stage for developing the text of the treaty, the drafting of which will begin at the next INC meeting in Tokyo in January 2011. At the June meeting, a World Health Organization representative stated that the goal will be to halt production of skin-lightening cosmetics that contain mercury. Five INC meetings are expected to convene to complete the treaty before 2013.
Conclusion
It is incumbent upon dermatologists to use all of the tools in their arsenal to convince patients to accept their skin tone as it is. In other words, we should discourage those who attempt to lighten their skin for reasons not pertaining to correcting dyspigmentation, just as we discourage patients seeking to tan or darken their skin.
For patients resistant to such advice or cajolery, practitioners must warn them about using skin-lightening products that contain mercury and recommend alternative lightening agents. Clearly, formulations containing mercury, though banned in the United States, are becoming increasingly available, and as over-the-counter products they are not tightly regulated. These products pose a serious health risk.