User login
Causal Link Between Atopic Dermatitis, ADHD Remains Elusive
Evidence suggests that a strong positive correlation exists between atopic disease and attention-deficit/hyperactivity disorder. But since all studies of the issue to date have been observational, "a causal relationship cannot be inferred," according to a research commentary in the August issue of the Archives of Dermatology.
"Further epidemiologic studies that use consistent and validated measures to more accurately define atopic disease and ADHD and adjust for confounders and disease severity are needed to better elucidate this relationship," said Dr. Sarah N. Gee and Dr. Michael Bigby of the departments of dermatology at Harvard Medical School and Beth Israel Deaconess Medical Center, both in Boston (Arch. Dermatol. 2011;147:967-70).
Dr. Gee and Dr. Bigby commented on a review of the literature presented by Dr. Jochen Schmitt and colleagues in the journal Allergy, which was titled: "Is atopic disease a risk factor for attention-deficit/hyperactivity disorder?" A systematic review (Allergy 2010;65:1506-24). That review covered 20 studies – 1 cohort study, 2 case-control studies, and 17 cross-sectional studies – involving 170,175 patients with eczema, asthma, rhinitis, or atopic dermatitis who also had ADHD symptoms. The studies reviewed had been conducted around the world, including in Germany and in other parts of Europe, and in North America, Australia, and New Zealand. All except one of the studies focused on children and adolescents.
"Four of the six studies that investigated eczema and ADHD found a statistically significant positive association, two with an odds ratio greater than four. Two of the three studies that used multivariate logistic regression for confounding factors found a statistically significant positive relationship between atopic dermatitis and ADHD. [And] with respect to asthma, all 12 studies that investigated asthma and ADHD reported a positive association ([odds ratio], 1.23-2.42)," Dr. Gee and Dr. Bigby said.
However, two studies that examined a possible link between allergic rhinitis and ADHD found no correlations.
The review by Dr. Schmitt fulfilled most of the criteria laid out by the Centre for Evidence-Based Medicine’s guidelines for "a useful and valid review." The choice of articles to include was appropriate, and the data were sufficient to answer the clinical question they posed.
The review was restricted to studies published in English or German, which might have left out some relevant studies. "However, we replicated their search without language restriction and found no additional studies," Dr. Gee and Dr. Bigby reported.
The review included searches of two databases, but Dr. Gee and Dr. Bigby found two additional relevant studies when they searched additional databases. Both of these were observational studies, and both found a significant association between atopic dermatitis and ADHD symptoms, they noted.
The most important criticism of the review by Dr. Schmitt is that assessment of both atopic disease and ADHD was inconsistent across the various studies, and tended to rely on parent reporting rather than physician diagnoses. For example, only 1 of the 20 articles used Diagnostic and Statistical Manual criteria for an ADHD diagnosis.
Such shortcomings should be addressed in any future research of the issue, Dr. Gee and Dr. Bigby said.
No financial conflicts of interest were reported.
Evidence suggests that a strong positive correlation exists between atopic disease and attention-deficit/hyperactivity disorder. But since all studies of the issue to date have been observational, "a causal relationship cannot be inferred," according to a research commentary in the August issue of the Archives of Dermatology.
"Further epidemiologic studies that use consistent and validated measures to more accurately define atopic disease and ADHD and adjust for confounders and disease severity are needed to better elucidate this relationship," said Dr. Sarah N. Gee and Dr. Michael Bigby of the departments of dermatology at Harvard Medical School and Beth Israel Deaconess Medical Center, both in Boston (Arch. Dermatol. 2011;147:967-70).
Dr. Gee and Dr. Bigby commented on a review of the literature presented by Dr. Jochen Schmitt and colleagues in the journal Allergy, which was titled: "Is atopic disease a risk factor for attention-deficit/hyperactivity disorder?" A systematic review (Allergy 2010;65:1506-24). That review covered 20 studies – 1 cohort study, 2 case-control studies, and 17 cross-sectional studies – involving 170,175 patients with eczema, asthma, rhinitis, or atopic dermatitis who also had ADHD symptoms. The studies reviewed had been conducted around the world, including in Germany and in other parts of Europe, and in North America, Australia, and New Zealand. All except one of the studies focused on children and adolescents.
"Four of the six studies that investigated eczema and ADHD found a statistically significant positive association, two with an odds ratio greater than four. Two of the three studies that used multivariate logistic regression for confounding factors found a statistically significant positive relationship between atopic dermatitis and ADHD. [And] with respect to asthma, all 12 studies that investigated asthma and ADHD reported a positive association ([odds ratio], 1.23-2.42)," Dr. Gee and Dr. Bigby said.
However, two studies that examined a possible link between allergic rhinitis and ADHD found no correlations.
The review by Dr. Schmitt fulfilled most of the criteria laid out by the Centre for Evidence-Based Medicine’s guidelines for "a useful and valid review." The choice of articles to include was appropriate, and the data were sufficient to answer the clinical question they posed.
The review was restricted to studies published in English or German, which might have left out some relevant studies. "However, we replicated their search without language restriction and found no additional studies," Dr. Gee and Dr. Bigby reported.
The review included searches of two databases, but Dr. Gee and Dr. Bigby found two additional relevant studies when they searched additional databases. Both of these were observational studies, and both found a significant association between atopic dermatitis and ADHD symptoms, they noted.
The most important criticism of the review by Dr. Schmitt is that assessment of both atopic disease and ADHD was inconsistent across the various studies, and tended to rely on parent reporting rather than physician diagnoses. For example, only 1 of the 20 articles used Diagnostic and Statistical Manual criteria for an ADHD diagnosis.
Such shortcomings should be addressed in any future research of the issue, Dr. Gee and Dr. Bigby said.
No financial conflicts of interest were reported.
Evidence suggests that a strong positive correlation exists between atopic disease and attention-deficit/hyperactivity disorder. But since all studies of the issue to date have been observational, "a causal relationship cannot be inferred," according to a research commentary in the August issue of the Archives of Dermatology.
"Further epidemiologic studies that use consistent and validated measures to more accurately define atopic disease and ADHD and adjust for confounders and disease severity are needed to better elucidate this relationship," said Dr. Sarah N. Gee and Dr. Michael Bigby of the departments of dermatology at Harvard Medical School and Beth Israel Deaconess Medical Center, both in Boston (Arch. Dermatol. 2011;147:967-70).
Dr. Gee and Dr. Bigby commented on a review of the literature presented by Dr. Jochen Schmitt and colleagues in the journal Allergy, which was titled: "Is atopic disease a risk factor for attention-deficit/hyperactivity disorder?" A systematic review (Allergy 2010;65:1506-24). That review covered 20 studies – 1 cohort study, 2 case-control studies, and 17 cross-sectional studies – involving 170,175 patients with eczema, asthma, rhinitis, or atopic dermatitis who also had ADHD symptoms. The studies reviewed had been conducted around the world, including in Germany and in other parts of Europe, and in North America, Australia, and New Zealand. All except one of the studies focused on children and adolescents.
"Four of the six studies that investigated eczema and ADHD found a statistically significant positive association, two with an odds ratio greater than four. Two of the three studies that used multivariate logistic regression for confounding factors found a statistically significant positive relationship between atopic dermatitis and ADHD. [And] with respect to asthma, all 12 studies that investigated asthma and ADHD reported a positive association ([odds ratio], 1.23-2.42)," Dr. Gee and Dr. Bigby said.
However, two studies that examined a possible link between allergic rhinitis and ADHD found no correlations.
The review by Dr. Schmitt fulfilled most of the criteria laid out by the Centre for Evidence-Based Medicine’s guidelines for "a useful and valid review." The choice of articles to include was appropriate, and the data were sufficient to answer the clinical question they posed.
The review was restricted to studies published in English or German, which might have left out some relevant studies. "However, we replicated their search without language restriction and found no additional studies," Dr. Gee and Dr. Bigby reported.
The review included searches of two databases, but Dr. Gee and Dr. Bigby found two additional relevant studies when they searched additional databases. Both of these were observational studies, and both found a significant association between atopic dermatitis and ADHD symptoms, they noted.
The most important criticism of the review by Dr. Schmitt is that assessment of both atopic disease and ADHD was inconsistent across the various studies, and tended to rely on parent reporting rather than physician diagnoses. For example, only 1 of the 20 articles used Diagnostic and Statistical Manual criteria for an ADHD diagnosis.
Such shortcomings should be addressed in any future research of the issue, Dr. Gee and Dr. Bigby said.
No financial conflicts of interest were reported.
FROM THE ARCHIVES OF DERMATOLOGY
Major Finding: Of three studies that examined a possible correlation between atopic dermatitis and ADHD, two found a correlation; of six studies that examined a possible correlation between eczema and ADHD, four found a strong correlation; and of 12 studies that examined a possible correlation between asthma and ADHD, all 12 found a correlation.
Data Source: A commentary on a review of the literature examining the link between atopic disease and ADHD.
Disclosures: No financial conflicts of interest were reported.
Propranolol Tops Corticosteroids for Infantile Hemangiomas
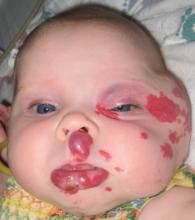
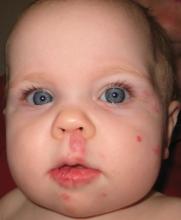
Propranolol is more clinically effective and cost effective than oral corticosteroids for infantile hemangiomas, and should be considered a first-line treatment, according to the results of a new study published online Aug. 15 in the Archives of Dermatology.
In what the researchers described as the first large, retrospective study to directly compare the two treatments, patients who were given propranolol showed more effective clearing of lesions, were less likely to require surgery for residual lesions, and had minimal adverse effects. Propranolol also was half as costly as corticosteroids, according to Dr. Cynthia J. Price of the University of Miami and her associates.
"Until recently, the mainstay of treatment for infantile hemangiomas has been corticosteroids in various forms, including topical, intralesional, and oral formulations, with the most common being oral prednisolone. Only in complicated or refractory [infantile hemangioma] cases have other treatment modalities, such as interferon alfa-2a, imiquimod, vincristine, cyclophosphamide, pulsed dye laser, and, most recently, propranolol, been considered," the investigators wrote.
Propranolol, a nonselective beta-blocker, is presumed to act on these lesions through vasoconstrictive properties. The drug reduces the release of nitric oxide, inhibits proangiogenic signals (such as those from vascular endothelial growth factor, basic fibroblast growth factor, and matrix metalloproteinase 2/9), and induces apoptosis in proliferating endothelial cells.
For the study, Dr. Price and her colleagues reviewed the charts of 110 patients with infantile hemangiomas who were treated at two Miami medical centers in 2005-2010. Their mean age at the start of treatment was 4.5 months.
Slightly more than half of the study subjects were white, 45% were Hispanic, and 1% were black. Most of the lesions were located on the head (59% on the face and 19% on the scalp), and the rest were on the trunk (7%), extremities (10%), and genitalia (5%).
Abnormalities were found on radiographic examinations in 14% of the patients, and included multifocal hemangiomatosis with diffuse liver involvement. Brain MRI revealed abnormalities in nine patients, including aberrant carotid artery connections feeding the hemangioma, extension of the lesion into the brain, and extension into the eye.
In all, 68 patients were treated with propranolol and 42 with oral corticosteroids. The two groups were matched with respect to age as well as the location, size, and type of lesion.
Fifty-six patients (82%) who were given propranolol achieved clearance of 75% or more of the lesion after a mean of 8 months of treatment, compared with only 12 (29%) of those given oral corticosteroids for a mean of 5 months, the investigators reported (Arch. Dermatol. 2011 Aug. 15 [doi:10.1001/archdermatol.2011.203]).
Patients who were given corticosteroids had to discontinue treatment significantly earlier than did those given propranolol because of adverse effects. The rate of adverse effects was 100% with corticosteroids, compared with only 1% with propranolol.
The single adverse effect that was likely related to propranolol was hypoglycemia, which developed in one patient. In contrast, all of the patients who received oral corticosteroids developed cushingoid features, and 14 developed various steroid-related disorders including gastroesophageal reflux, hypertension, hirsutism, and infections.
One patient who took corticosteroids had a life-threatening arterial bleed from a lesion ulceration that eroded through the carotid artery and required emergency surgery. The rate of lesion ulceration was significantly lower with propranolol (6%) than with corticosteroids (26%).
The number of patients who were referred for surgical treatment of residual hemangioma also was significantly lower with propranolol (12%) than with corticosteroids (29%).
The average cost of treatment was $205 per patient for propranolol, not including the charge for a cardiology consultation for clearance to start treatment. This is less than half the cost of $416 per patient for oral corticosteroids treatment, which doesn’t include the additional costs incurred by treating or preventing adverse effects.
Until now, "it has been believed that therapy must be administered during the proliferative phase of infantile hemangiomas to arrest the progressive growth of the vascular lesion. However, in this study, we found similar outcomes in patients treated with propranolol before and after 1 year of age (7 of 68 patients were started on propranolol therapy after the age of 12 months, and all had [at least] 75% clearance)," Dr. Price and her associates noted. "This finding indicates that propranolol’s long-term effect is not solely related to it antiproliferative effect on the vasculature but is also due to its apoptosis and vasoconstriction."
No financial conflicts of interest were reported.
Propranolol is more clinically effective and cost effective than oral corticosteroids for infantile hemangiomas, and should be considered a first-line treatment, according to the results of a new study published online Aug. 15 in the Archives of Dermatology.
In what the researchers described as the first large, retrospective study to directly compare the two treatments, patients who were given propranolol showed more effective clearing of lesions, were less likely to require surgery for residual lesions, and had minimal adverse effects. Propranolol also was half as costly as corticosteroids, according to Dr. Cynthia J. Price of the University of Miami and her associates.
"Until recently, the mainstay of treatment for infantile hemangiomas has been corticosteroids in various forms, including topical, intralesional, and oral formulations, with the most common being oral prednisolone. Only in complicated or refractory [infantile hemangioma] cases have other treatment modalities, such as interferon alfa-2a, imiquimod, vincristine, cyclophosphamide, pulsed dye laser, and, most recently, propranolol, been considered," the investigators wrote.
Propranolol, a nonselective beta-blocker, is presumed to act on these lesions through vasoconstrictive properties. The drug reduces the release of nitric oxide, inhibits proangiogenic signals (such as those from vascular endothelial growth factor, basic fibroblast growth factor, and matrix metalloproteinase 2/9), and induces apoptosis in proliferating endothelial cells.
For the study, Dr. Price and her colleagues reviewed the charts of 110 patients with infantile hemangiomas who were treated at two Miami medical centers in 2005-2010. Their mean age at the start of treatment was 4.5 months.
Slightly more than half of the study subjects were white, 45% were Hispanic, and 1% were black. Most of the lesions were located on the head (59% on the face and 19% on the scalp), and the rest were on the trunk (7%), extremities (10%), and genitalia (5%).
Abnormalities were found on radiographic examinations in 14% of the patients, and included multifocal hemangiomatosis with diffuse liver involvement. Brain MRI revealed abnormalities in nine patients, including aberrant carotid artery connections feeding the hemangioma, extension of the lesion into the brain, and extension into the eye.
In all, 68 patients were treated with propranolol and 42 with oral corticosteroids. The two groups were matched with respect to age as well as the location, size, and type of lesion.
Fifty-six patients (82%) who were given propranolol achieved clearance of 75% or more of the lesion after a mean of 8 months of treatment, compared with only 12 (29%) of those given oral corticosteroids for a mean of 5 months, the investigators reported (Arch. Dermatol. 2011 Aug. 15 [doi:10.1001/archdermatol.2011.203]).
Patients who were given corticosteroids had to discontinue treatment significantly earlier than did those given propranolol because of adverse effects. The rate of adverse effects was 100% with corticosteroids, compared with only 1% with propranolol.
The single adverse effect that was likely related to propranolol was hypoglycemia, which developed in one patient. In contrast, all of the patients who received oral corticosteroids developed cushingoid features, and 14 developed various steroid-related disorders including gastroesophageal reflux, hypertension, hirsutism, and infections.
One patient who took corticosteroids had a life-threatening arterial bleed from a lesion ulceration that eroded through the carotid artery and required emergency surgery. The rate of lesion ulceration was significantly lower with propranolol (6%) than with corticosteroids (26%).
The number of patients who were referred for surgical treatment of residual hemangioma also was significantly lower with propranolol (12%) than with corticosteroids (29%).
The average cost of treatment was $205 per patient for propranolol, not including the charge for a cardiology consultation for clearance to start treatment. This is less than half the cost of $416 per patient for oral corticosteroids treatment, which doesn’t include the additional costs incurred by treating or preventing adverse effects.
Until now, "it has been believed that therapy must be administered during the proliferative phase of infantile hemangiomas to arrest the progressive growth of the vascular lesion. However, in this study, we found similar outcomes in patients treated with propranolol before and after 1 year of age (7 of 68 patients were started on propranolol therapy after the age of 12 months, and all had [at least] 75% clearance)," Dr. Price and her associates noted. "This finding indicates that propranolol’s long-term effect is not solely related to it antiproliferative effect on the vasculature but is also due to its apoptosis and vasoconstriction."
No financial conflicts of interest were reported.
Propranolol is more clinically effective and cost effective than oral corticosteroids for infantile hemangiomas, and should be considered a first-line treatment, according to the results of a new study published online Aug. 15 in the Archives of Dermatology.
In what the researchers described as the first large, retrospective study to directly compare the two treatments, patients who were given propranolol showed more effective clearing of lesions, were less likely to require surgery for residual lesions, and had minimal adverse effects. Propranolol also was half as costly as corticosteroids, according to Dr. Cynthia J. Price of the University of Miami and her associates.
"Until recently, the mainstay of treatment for infantile hemangiomas has been corticosteroids in various forms, including topical, intralesional, and oral formulations, with the most common being oral prednisolone. Only in complicated or refractory [infantile hemangioma] cases have other treatment modalities, such as interferon alfa-2a, imiquimod, vincristine, cyclophosphamide, pulsed dye laser, and, most recently, propranolol, been considered," the investigators wrote.
Propranolol, a nonselective beta-blocker, is presumed to act on these lesions through vasoconstrictive properties. The drug reduces the release of nitric oxide, inhibits proangiogenic signals (such as those from vascular endothelial growth factor, basic fibroblast growth factor, and matrix metalloproteinase 2/9), and induces apoptosis in proliferating endothelial cells.
For the study, Dr. Price and her colleagues reviewed the charts of 110 patients with infantile hemangiomas who were treated at two Miami medical centers in 2005-2010. Their mean age at the start of treatment was 4.5 months.
Slightly more than half of the study subjects were white, 45% were Hispanic, and 1% were black. Most of the lesions were located on the head (59% on the face and 19% on the scalp), and the rest were on the trunk (7%), extremities (10%), and genitalia (5%).
Abnormalities were found on radiographic examinations in 14% of the patients, and included multifocal hemangiomatosis with diffuse liver involvement. Brain MRI revealed abnormalities in nine patients, including aberrant carotid artery connections feeding the hemangioma, extension of the lesion into the brain, and extension into the eye.
In all, 68 patients were treated with propranolol and 42 with oral corticosteroids. The two groups were matched with respect to age as well as the location, size, and type of lesion.
Fifty-six patients (82%) who were given propranolol achieved clearance of 75% or more of the lesion after a mean of 8 months of treatment, compared with only 12 (29%) of those given oral corticosteroids for a mean of 5 months, the investigators reported (Arch. Dermatol. 2011 Aug. 15 [doi:10.1001/archdermatol.2011.203]).
Patients who were given corticosteroids had to discontinue treatment significantly earlier than did those given propranolol because of adverse effects. The rate of adverse effects was 100% with corticosteroids, compared with only 1% with propranolol.
The single adverse effect that was likely related to propranolol was hypoglycemia, which developed in one patient. In contrast, all of the patients who received oral corticosteroids developed cushingoid features, and 14 developed various steroid-related disorders including gastroesophageal reflux, hypertension, hirsutism, and infections.
One patient who took corticosteroids had a life-threatening arterial bleed from a lesion ulceration that eroded through the carotid artery and required emergency surgery. The rate of lesion ulceration was significantly lower with propranolol (6%) than with corticosteroids (26%).
The number of patients who were referred for surgical treatment of residual hemangioma also was significantly lower with propranolol (12%) than with corticosteroids (29%).
The average cost of treatment was $205 per patient for propranolol, not including the charge for a cardiology consultation for clearance to start treatment. This is less than half the cost of $416 per patient for oral corticosteroids treatment, which doesn’t include the additional costs incurred by treating or preventing adverse effects.
Until now, "it has been believed that therapy must be administered during the proliferative phase of infantile hemangiomas to arrest the progressive growth of the vascular lesion. However, in this study, we found similar outcomes in patients treated with propranolol before and after 1 year of age (7 of 68 patients were started on propranolol therapy after the age of 12 months, and all had [at least] 75% clearance)," Dr. Price and her associates noted. "This finding indicates that propranolol’s long-term effect is not solely related to it antiproliferative effect on the vasculature but is also due to its apoptosis and vasoconstriction."
No financial conflicts of interest were reported.
FROM THE ARCHIVES OF DERMATOLOGY
Major Finding: Infantile hemangiomas cleared in 82% of patients who were given propranolol, but in only 29% of those given standard oral corticosteroids.
Data Source: A retrospective chart review of 110 children with infantile hemangiomas treated at two Miami medical centers.
Disclosures: No financial conflicts of interest were reported.
Sleep Apnea Linked to Cognitive Impairment in Elderly
Sleep-disordered breathing – recurrent arousals and intermittent hypoxemia – raised elderly women’s risk of developing cognitive impairment within 5 years.
The hypoxia associated with sleep-disordered breathing, rather than sleep fragmentation or shorter sleep duration, appeared to be behind increased risk for both mild cognitive impairment and dementia, said Dr. Kristine Yaffe of the departments of psychiatry, neurology, and epidemiology at the University of California, San Francisco, and her associates in the Aug. 10 issue of JAMA (2011;306:613-9).
Both sleep-disordered breathing and cognitive impairment are common in elderly people, but no longitudinal study had ever examined whether the breathing disorder precedes the cognitive impairment. Dr. Yaffe’s team turned to data from the Study of Osteoporotic Fractures, a multicenter cohort assessment of predominantly white women aged 65 years and older at baseline in 1986-88.
For this analysis, Dr. Yaffe and her associates followed 298 subjects who from 2002 to 2004 underwent overnight polysomnography in their homes in Minnesota and Pennsylvania. Of that group, 105 women (35%) met the criteria for sleep-disordered breathing.
A mean of 5 years later, the polysomnography-tested women, mean age 82 years, completed a battery of neuropsychological tests to determine cognitive status. A total of 107 (36%) had developed mild cognitive impairment (60 women) or dementia (47 women).
Significantly more women who had sleep-disordered breathing developed cognitive impairment (45%) than did women who did not have sleep-disordered breathing (31%). The presence of the condition was associated with increased odds of cognitive impairment (odds ratio, 1.80).
Two measures of hypoxia – an oxygen desaturation index of 15 or less and a percentage of total sleep time in apnea or hypopnea of 7% or more – correlated with cognitive impairment. But a third measure of hypoxia – the amount of time during sleep with an oxygen saturation of less than 90% – did not.
None of the study’s indices of sleep fragmentation and sleep duration – arousal, wakefulness after sleep onset, and total sleep time – correlated with cognitive impairment.
The researchers concluded that hypoxia is the apparent means by which sleep-disordered breathing causes cognitive impairment. "However, it is important to note that because cerebral blood flow may be affected in elderly patients, other mechanisms such as hypercapnia could also be involved," the investigators said. They added that the findings suggest that interventions to address sleep-disordered breathing in general and hypoxia in particular may prevent or improve cognitive impairment.
Previous studies in patients with Alzheimer’s disease have shown that continuous positive airway pressure (CPAP) for sleep-disordered breathing slows or even improves cognitive impairment, Dr. Yaffe and her colleagues noted. The new findings suggest that supplemental oxygen therapy might also be beneficial, they added.
"To fully evaluate the impact of treatment for sleep-disordered breathing in elderly populations, additional trials with larger sample sizes, longer treatment periods, and more diverse populations are required," the researchers said added. "Given the high prevalence of both sleep-disordered breathing and cognitive impairment among older adults, the possibility of an association between the two conditions, even a modest one, has the potential for a large public health impact."
The study was supported by the National Institute on Aging. The Study of Osteoporotic Fractures was supported by the National Institutes of Health. Dr. Yaffe reported ties to Novartis, Pfizer, Medivation, Beeson Scientific Advisory, the National Institute of Mental Health, the Alzheimer’s Association, the Department of Defense, the American Health Assistance Foundation, Japan Geriatrics Society, Wake Forest University, and the State of California Department of Human Services. Her associates reported ties to several pharmaceutical companie
Yaffe et al. said their findings suggest a potential role for oxygen therapy for sleep-disordered breathing in the elderly, and the authors recommend further study. But supplemental oxygen has not been studied extensively as a treatment of sleep-disordered breathing, and potential dangers should be considered, said Nicola Canessa, Ph.D., and Dr. Luigi Ferini-Strambi. These dangers include prolongation of apnea, increased hypercarbia and acidosis, and increased ventricular irritability.
In contrast, continuous positive airway pressure (CPAP) has been studied in sleep-disordered breathing and might be a prevention strategy worth trying, wrote Dr. Canessa and Dr. Ferini-Strambi. Physicians with patients for whom CPAP may be indicated should consider these new results, and future guidelines to formalize the clinical management of patients with mild cognitive impairment should consider the implications of this study.
Nicola Canessa, Ph.D., is with the Center for Cognitive Neuroscience and the San Raffaele Scientific Institute, both in Milan. Luigi Ferini-Strambi, M.D., is at the Universita Vita-Salute San Raffaele and the Sleep Disorders Center at the San Raffaele Scientific Institute, also both in Milan. Dr. Ferini-Strambi is a board member for Boehringer-Ingelheim, UCB-Pharma, GlaxoSmithKline, and Sanofi-Aventis. These remarks were taken from their editorial accompanying Dr. Yaffe’s report (JAMA 2011;306:654-5).
Yaffe et al. said their findings suggest a potential role for oxygen therapy for sleep-disordered breathing in the elderly, and the authors recommend further study. But supplemental oxygen has not been studied extensively as a treatment of sleep-disordered breathing, and potential dangers should be considered, said Nicola Canessa, Ph.D., and Dr. Luigi Ferini-Strambi. These dangers include prolongation of apnea, increased hypercarbia and acidosis, and increased ventricular irritability.
In contrast, continuous positive airway pressure (CPAP) has been studied in sleep-disordered breathing and might be a prevention strategy worth trying, wrote Dr. Canessa and Dr. Ferini-Strambi. Physicians with patients for whom CPAP may be indicated should consider these new results, and future guidelines to formalize the clinical management of patients with mild cognitive impairment should consider the implications of this study.
Nicola Canessa, Ph.D., is with the Center for Cognitive Neuroscience and the San Raffaele Scientific Institute, both in Milan. Luigi Ferini-Strambi, M.D., is at the Universita Vita-Salute San Raffaele and the Sleep Disorders Center at the San Raffaele Scientific Institute, also both in Milan. Dr. Ferini-Strambi is a board member for Boehringer-Ingelheim, UCB-Pharma, GlaxoSmithKline, and Sanofi-Aventis. These remarks were taken from their editorial accompanying Dr. Yaffe’s report (JAMA 2011;306:654-5).
Yaffe et al. said their findings suggest a potential role for oxygen therapy for sleep-disordered breathing in the elderly, and the authors recommend further study. But supplemental oxygen has not been studied extensively as a treatment of sleep-disordered breathing, and potential dangers should be considered, said Nicola Canessa, Ph.D., and Dr. Luigi Ferini-Strambi. These dangers include prolongation of apnea, increased hypercarbia and acidosis, and increased ventricular irritability.
In contrast, continuous positive airway pressure (CPAP) has been studied in sleep-disordered breathing and might be a prevention strategy worth trying, wrote Dr. Canessa and Dr. Ferini-Strambi. Physicians with patients for whom CPAP may be indicated should consider these new results, and future guidelines to formalize the clinical management of patients with mild cognitive impairment should consider the implications of this study.
Nicola Canessa, Ph.D., is with the Center for Cognitive Neuroscience and the San Raffaele Scientific Institute, both in Milan. Luigi Ferini-Strambi, M.D., is at the Universita Vita-Salute San Raffaele and the Sleep Disorders Center at the San Raffaele Scientific Institute, also both in Milan. Dr. Ferini-Strambi is a board member for Boehringer-Ingelheim, UCB-Pharma, GlaxoSmithKline, and Sanofi-Aventis. These remarks were taken from their editorial accompanying Dr. Yaffe’s report (JAMA 2011;306:654-5).
Sleep-disordered breathing – recurrent arousals and intermittent hypoxemia – raised elderly women’s risk of developing cognitive impairment within 5 years.
The hypoxia associated with sleep-disordered breathing, rather than sleep fragmentation or shorter sleep duration, appeared to be behind increased risk for both mild cognitive impairment and dementia, said Dr. Kristine Yaffe of the departments of psychiatry, neurology, and epidemiology at the University of California, San Francisco, and her associates in the Aug. 10 issue of JAMA (2011;306:613-9).
Both sleep-disordered breathing and cognitive impairment are common in elderly people, but no longitudinal study had ever examined whether the breathing disorder precedes the cognitive impairment. Dr. Yaffe’s team turned to data from the Study of Osteoporotic Fractures, a multicenter cohort assessment of predominantly white women aged 65 years and older at baseline in 1986-88.
For this analysis, Dr. Yaffe and her associates followed 298 subjects who from 2002 to 2004 underwent overnight polysomnography in their homes in Minnesota and Pennsylvania. Of that group, 105 women (35%) met the criteria for sleep-disordered breathing.
A mean of 5 years later, the polysomnography-tested women, mean age 82 years, completed a battery of neuropsychological tests to determine cognitive status. A total of 107 (36%) had developed mild cognitive impairment (60 women) or dementia (47 women).
Significantly more women who had sleep-disordered breathing developed cognitive impairment (45%) than did women who did not have sleep-disordered breathing (31%). The presence of the condition was associated with increased odds of cognitive impairment (odds ratio, 1.80).
Two measures of hypoxia – an oxygen desaturation index of 15 or less and a percentage of total sleep time in apnea or hypopnea of 7% or more – correlated with cognitive impairment. But a third measure of hypoxia – the amount of time during sleep with an oxygen saturation of less than 90% – did not.
None of the study’s indices of sleep fragmentation and sleep duration – arousal, wakefulness after sleep onset, and total sleep time – correlated with cognitive impairment.
The researchers concluded that hypoxia is the apparent means by which sleep-disordered breathing causes cognitive impairment. "However, it is important to note that because cerebral blood flow may be affected in elderly patients, other mechanisms such as hypercapnia could also be involved," the investigators said. They added that the findings suggest that interventions to address sleep-disordered breathing in general and hypoxia in particular may prevent or improve cognitive impairment.
Previous studies in patients with Alzheimer’s disease have shown that continuous positive airway pressure (CPAP) for sleep-disordered breathing slows or even improves cognitive impairment, Dr. Yaffe and her colleagues noted. The new findings suggest that supplemental oxygen therapy might also be beneficial, they added.
"To fully evaluate the impact of treatment for sleep-disordered breathing in elderly populations, additional trials with larger sample sizes, longer treatment periods, and more diverse populations are required," the researchers said added. "Given the high prevalence of both sleep-disordered breathing and cognitive impairment among older adults, the possibility of an association between the two conditions, even a modest one, has the potential for a large public health impact."
The study was supported by the National Institute on Aging. The Study of Osteoporotic Fractures was supported by the National Institutes of Health. Dr. Yaffe reported ties to Novartis, Pfizer, Medivation, Beeson Scientific Advisory, the National Institute of Mental Health, the Alzheimer’s Association, the Department of Defense, the American Health Assistance Foundation, Japan Geriatrics Society, Wake Forest University, and the State of California Department of Human Services. Her associates reported ties to several pharmaceutical companie
Sleep-disordered breathing – recurrent arousals and intermittent hypoxemia – raised elderly women’s risk of developing cognitive impairment within 5 years.
The hypoxia associated with sleep-disordered breathing, rather than sleep fragmentation or shorter sleep duration, appeared to be behind increased risk for both mild cognitive impairment and dementia, said Dr. Kristine Yaffe of the departments of psychiatry, neurology, and epidemiology at the University of California, San Francisco, and her associates in the Aug. 10 issue of JAMA (2011;306:613-9).
Both sleep-disordered breathing and cognitive impairment are common in elderly people, but no longitudinal study had ever examined whether the breathing disorder precedes the cognitive impairment. Dr. Yaffe’s team turned to data from the Study of Osteoporotic Fractures, a multicenter cohort assessment of predominantly white women aged 65 years and older at baseline in 1986-88.
For this analysis, Dr. Yaffe and her associates followed 298 subjects who from 2002 to 2004 underwent overnight polysomnography in their homes in Minnesota and Pennsylvania. Of that group, 105 women (35%) met the criteria for sleep-disordered breathing.
A mean of 5 years later, the polysomnography-tested women, mean age 82 years, completed a battery of neuropsychological tests to determine cognitive status. A total of 107 (36%) had developed mild cognitive impairment (60 women) or dementia (47 women).
Significantly more women who had sleep-disordered breathing developed cognitive impairment (45%) than did women who did not have sleep-disordered breathing (31%). The presence of the condition was associated with increased odds of cognitive impairment (odds ratio, 1.80).
Two measures of hypoxia – an oxygen desaturation index of 15 or less and a percentage of total sleep time in apnea or hypopnea of 7% or more – correlated with cognitive impairment. But a third measure of hypoxia – the amount of time during sleep with an oxygen saturation of less than 90% – did not.
None of the study’s indices of sleep fragmentation and sleep duration – arousal, wakefulness after sleep onset, and total sleep time – correlated with cognitive impairment.
The researchers concluded that hypoxia is the apparent means by which sleep-disordered breathing causes cognitive impairment. "However, it is important to note that because cerebral blood flow may be affected in elderly patients, other mechanisms such as hypercapnia could also be involved," the investigators said. They added that the findings suggest that interventions to address sleep-disordered breathing in general and hypoxia in particular may prevent or improve cognitive impairment.
Previous studies in patients with Alzheimer’s disease have shown that continuous positive airway pressure (CPAP) for sleep-disordered breathing slows or even improves cognitive impairment, Dr. Yaffe and her colleagues noted. The new findings suggest that supplemental oxygen therapy might also be beneficial, they added.
"To fully evaluate the impact of treatment for sleep-disordered breathing in elderly populations, additional trials with larger sample sizes, longer treatment periods, and more diverse populations are required," the researchers said added. "Given the high prevalence of both sleep-disordered breathing and cognitive impairment among older adults, the possibility of an association between the two conditions, even a modest one, has the potential for a large public health impact."
The study was supported by the National Institute on Aging. The Study of Osteoporotic Fractures was supported by the National Institutes of Health. Dr. Yaffe reported ties to Novartis, Pfizer, Medivation, Beeson Scientific Advisory, the National Institute of Mental Health, the Alzheimer’s Association, the Department of Defense, the American Health Assistance Foundation, Japan Geriatrics Society, Wake Forest University, and the State of California Department of Human Services. Her associates reported ties to several pharmaceutical companie
FROM JAMA
Major Finding: Significantly more elderly women who had recurrent arousals and intermittent hypoxemia during sleep developed cognitive impairment during 5 years of follow-up (45%), compared with women who did not have such sleep-disordered breathing (31%), and the presence of sleep-disordered breathing was associated with an increased risk of cognitive impairment (OR, 1.80).
Data Source: A secondary analysis of data from a prospective multicenter study of aging women, which assessed sleep-disordered breathing and the development of cognitive impairment during 5 years of follow-up in a subset of 298 women.
Disclosures: This study was supported by the National Institute on Aging. The Study of Osteoporotic Fractures was supported by the National Institutes of Health. Dr. Yaffe reported ties to Novartis, Pfizer, Medivation, Beeson Scientific Advisory, the National Institute of Mental Health, the Alzheimer Association, the Department of Defense, the American Health Assistance Foundation, Japan Geriatrics Society, Wake Forest University, and the State of California Department of Human Services. Her associates reported ties to several pharmaceutical companies.
Safety Net Still Active After State Reform
Even though the 2006 health care reform in Massachusetts dramatically reduced the proportion of uninsured patients to less than 2% today, the demand for services from "safety-net facilities" there continues to rise, according to the results of a data analysis.
Most patients at the community health centers, clinics, charity hospitals, and public hospitals in the state are insured and have the option to seek care elsewhere, but they continue to use these safety-net providers, reported Leighton Ku, Ph.D., and his coauthors in the Aug. 8/22 issue of Archives of Internal Medicine.
Surveyed patients said they use these facilities because they are familiar and provide desired services that these patients want, such as language assistance, wrote Dr. Ku of the department of health policy at George Washington University, Washington, and his coinvestigators.
Key elements of the Massachusetts law are similar to those in the federal health care reform passed last year. The researchers said it is likely that that national demand for safety-net services will show a similar increase, at least for the next few years.
"States and the federal government should consider whether adequate transitional and long-term support exist to help meet the needs of patients served by safety-net facilities," Dr. Ku and his colleagues said (Arch. Intern. Med. 2011;171:1379-84).
They examined the experience in Massachusetts using a combination of administrative data, the results of a 2009 telephone survey about the state’s health reform, and data from case-study interviews with medical staff and administrators in four communities with a history of poor access to health care.
Between 2005 and 2009, the number of patients served at safety-net facilities in Massachusetts increased by 31%, from 431,005 to 564,740, and the number of such facilities increased from 33 to 36. At the same time, the percentage of uninsured patients at these facilities dropped from 36% to 20%, the authors reported.
Low-income patients using safety-net facilities and other patients had similar patterns of general medical visits, preventive care visits, specialty care visits, and dental care visits. Where they differed was in their use of emergency departments. One-third of adult safety-net patients reported visiting an ED for a nonemergency condition, whereas only 15% of other adult patients did.
A majority of patients, medical staff, and medical administrators cited as reasons for the continuing use of safety-net facilities convenient location (79%); affordable care (74%); and the availability of nonmedical services such as language services, assistance with insurance forms, transportation assistance, and community outreach programs (52%). Existing ties to the providers at safety-net facilities and the high number of bilingual providers there also encouraged patients who were newly insured to continue to seek care there.
Only 25% of patients said they attended safety-net facilities because they had difficulty getting appointments elsewhere.
This study was funded in part by the Blue Cross Blue Shield of Massachusetts Foundation. No financial conflict of interest was reported.
"The conventional wisdom has been that the role of safety-net providers would shrink under health reform. After all, once uninsured patients have Medicaid or are covered under [a health insurance] exchange, they will have other choices of where to receive their care," said Dr. Mitchell H. Katz. But the report by Ku et al. shows the opposite. "The important lesson from Massachusetts is that the newly insured continued to seek care in the safety net," he said.
Whether this pattern will hold true in other parts of the country under federal health reform will depend on two factors: "the perceived quality and convenience of safety-net providers, and the degree of competition from other providers to attract persons who newly gain insurance," Dr. Katz said.
Mitchell H. Katz, M.D., is at the Lost Angeles County Department of Health Services. He reported no financial conflict of interest. These remarks are from his editorial accompanying Dr. Ku’s report (Arch. Intern. Med. 2011;171:1319-20).
"The conventional wisdom has been that the role of safety-net providers would shrink under health reform. After all, once uninsured patients have Medicaid or are covered under [a health insurance] exchange, they will have other choices of where to receive their care," said Dr. Mitchell H. Katz. But the report by Ku et al. shows the opposite. "The important lesson from Massachusetts is that the newly insured continued to seek care in the safety net," he said.
Whether this pattern will hold true in other parts of the country under federal health reform will depend on two factors: "the perceived quality and convenience of safety-net providers, and the degree of competition from other providers to attract persons who newly gain insurance," Dr. Katz said.
Mitchell H. Katz, M.D., is at the Lost Angeles County Department of Health Services. He reported no financial conflict of interest. These remarks are from his editorial accompanying Dr. Ku’s report (Arch. Intern. Med. 2011;171:1319-20).
"The conventional wisdom has been that the role of safety-net providers would shrink under health reform. After all, once uninsured patients have Medicaid or are covered under [a health insurance] exchange, they will have other choices of where to receive their care," said Dr. Mitchell H. Katz. But the report by Ku et al. shows the opposite. "The important lesson from Massachusetts is that the newly insured continued to seek care in the safety net," he said.
Whether this pattern will hold true in other parts of the country under federal health reform will depend on two factors: "the perceived quality and convenience of safety-net providers, and the degree of competition from other providers to attract persons who newly gain insurance," Dr. Katz said.
Mitchell H. Katz, M.D., is at the Lost Angeles County Department of Health Services. He reported no financial conflict of interest. These remarks are from his editorial accompanying Dr. Ku’s report (Arch. Intern. Med. 2011;171:1319-20).
Even though the 2006 health care reform in Massachusetts dramatically reduced the proportion of uninsured patients to less than 2% today, the demand for services from "safety-net facilities" there continues to rise, according to the results of a data analysis.
Most patients at the community health centers, clinics, charity hospitals, and public hospitals in the state are insured and have the option to seek care elsewhere, but they continue to use these safety-net providers, reported Leighton Ku, Ph.D., and his coauthors in the Aug. 8/22 issue of Archives of Internal Medicine.
Surveyed patients said they use these facilities because they are familiar and provide desired services that these patients want, such as language assistance, wrote Dr. Ku of the department of health policy at George Washington University, Washington, and his coinvestigators.
Key elements of the Massachusetts law are similar to those in the federal health care reform passed last year. The researchers said it is likely that that national demand for safety-net services will show a similar increase, at least for the next few years.
"States and the federal government should consider whether adequate transitional and long-term support exist to help meet the needs of patients served by safety-net facilities," Dr. Ku and his colleagues said (Arch. Intern. Med. 2011;171:1379-84).
They examined the experience in Massachusetts using a combination of administrative data, the results of a 2009 telephone survey about the state’s health reform, and data from case-study interviews with medical staff and administrators in four communities with a history of poor access to health care.
Between 2005 and 2009, the number of patients served at safety-net facilities in Massachusetts increased by 31%, from 431,005 to 564,740, and the number of such facilities increased from 33 to 36. At the same time, the percentage of uninsured patients at these facilities dropped from 36% to 20%, the authors reported.
Low-income patients using safety-net facilities and other patients had similar patterns of general medical visits, preventive care visits, specialty care visits, and dental care visits. Where they differed was in their use of emergency departments. One-third of adult safety-net patients reported visiting an ED for a nonemergency condition, whereas only 15% of other adult patients did.
A majority of patients, medical staff, and medical administrators cited as reasons for the continuing use of safety-net facilities convenient location (79%); affordable care (74%); and the availability of nonmedical services such as language services, assistance with insurance forms, transportation assistance, and community outreach programs (52%). Existing ties to the providers at safety-net facilities and the high number of bilingual providers there also encouraged patients who were newly insured to continue to seek care there.
Only 25% of patients said they attended safety-net facilities because they had difficulty getting appointments elsewhere.
This study was funded in part by the Blue Cross Blue Shield of Massachusetts Foundation. No financial conflict of interest was reported.
Even though the 2006 health care reform in Massachusetts dramatically reduced the proportion of uninsured patients to less than 2% today, the demand for services from "safety-net facilities" there continues to rise, according to the results of a data analysis.
Most patients at the community health centers, clinics, charity hospitals, and public hospitals in the state are insured and have the option to seek care elsewhere, but they continue to use these safety-net providers, reported Leighton Ku, Ph.D., and his coauthors in the Aug. 8/22 issue of Archives of Internal Medicine.
Surveyed patients said they use these facilities because they are familiar and provide desired services that these patients want, such as language assistance, wrote Dr. Ku of the department of health policy at George Washington University, Washington, and his coinvestigators.
Key elements of the Massachusetts law are similar to those in the federal health care reform passed last year. The researchers said it is likely that that national demand for safety-net services will show a similar increase, at least for the next few years.
"States and the federal government should consider whether adequate transitional and long-term support exist to help meet the needs of patients served by safety-net facilities," Dr. Ku and his colleagues said (Arch. Intern. Med. 2011;171:1379-84).
They examined the experience in Massachusetts using a combination of administrative data, the results of a 2009 telephone survey about the state’s health reform, and data from case-study interviews with medical staff and administrators in four communities with a history of poor access to health care.
Between 2005 and 2009, the number of patients served at safety-net facilities in Massachusetts increased by 31%, from 431,005 to 564,740, and the number of such facilities increased from 33 to 36. At the same time, the percentage of uninsured patients at these facilities dropped from 36% to 20%, the authors reported.
Low-income patients using safety-net facilities and other patients had similar patterns of general medical visits, preventive care visits, specialty care visits, and dental care visits. Where they differed was in their use of emergency departments. One-third of adult safety-net patients reported visiting an ED for a nonemergency condition, whereas only 15% of other adult patients did.
A majority of patients, medical staff, and medical administrators cited as reasons for the continuing use of safety-net facilities convenient location (79%); affordable care (74%); and the availability of nonmedical services such as language services, assistance with insurance forms, transportation assistance, and community outreach programs (52%). Existing ties to the providers at safety-net facilities and the high number of bilingual providers there also encouraged patients who were newly insured to continue to seek care there.
Only 25% of patients said they attended safety-net facilities because they had difficulty getting appointments elsewhere.
This study was funded in part by the Blue Cross Blue Shield of Massachusetts Foundation. No financial conflict of interest was reported.
FROM ARCHIVES OF INTERNAL MEDICINE
Major Finding: After implementation of health reform in Massachusetts in 2006, the proportion of uninsured patients dropped dramatically, but the number of patients served at safety-net facilities increased by 31% and the number of such facilities increased from 33 to 36.
Data Source: Assessment of the experience in Massachusetts with safety-net care during 2005-2009 using a combination of administrative data, the results of a 2009 state health reform survey of adult patients, and data from case-study interviews with medical staff and administrators in four communities with a history of poor access to health care.
Disclosures: This study was funded in part by the Blue Cross Blue Shield of Massachusetts Foundation. No financial conflict of interest was reported.
Phlebotomy Blood Loss Linked to Anemia in Hospital Patients
Blood loss from diagnostic blood testing during hospitalization is substantial and has been linked to anemia in patients with acute myocardial infarction, according to a study published online Aug. 8 in the Archives of Internal Medicine.
In a study of 17,676 MI patients at 57 U.S. hospitals, 1 in 5 patients developed moderate to severe hospital-acquired anemia, and they had a mean estimated phlebotomy volume of 173.8 mL – the equivalent of half a unit of whole blood. Twelve percent of the study subjects lost more than 300 mL to blood draws during the course of their hospitalization, said Dr. Adam C. Salisbury of Saint Luke’s Mid America Heart and Vascular Institute, Kansas City, Mo., and his associates.
"Our findings are likely generalizable to other populations of seriously ill medical patients," they noted.
If further research establishes that minimizing blood loss from phlebotomy prevents anemia and improves patient outcomes, there would be broad implications for all hospitalized patients. Strategies to minimize blood loss, such as using pediatric instead of adult blood tubes or filling standard 4-mL adult tubes with only 1-2 mL of blood, would be widely adopted, Dr. Salisbury and his colleagues added.
They explored the relationship between diagnostic blood testing and the risk of hospital-acquired anemia in MI patients because blood draws have been associated with increased need for transfusions in this patient population. The researchers used information from an electronic medical record database that detailed the frequency and type of laboratory testing as well as patients’ hemoglobin levels throughout hospitalization for acute MI. The database covered 57 hospitals during a recent 8-year period.
The study cohort was composed of all patients with acute MI, excluding those who already had anemia at admission and those who underwent coronary artery bypass grafting, because both the etiology and outcomes of anemia differ from those of non-CABG patients.
The data did not include exact amounts of blood drawn for every test. The investigators estimated these amounts from the types of tests that were run, assuming that only the minimal blood volume needed to run the required tests was drawn and that no blood was wasted at the blood draws.
Twenty percent of the study cohort (3,551 patients) developed moderate to severe anemia during hospitalization. Mean hemoglobin values declined in all patients, but they declined to a greater degree in those who developed anemia (–3.9 g/dL), compared with patients who didn’t develop anemia (–1.6 g/dL).
"The estimated mean blood loss from phlebotomy was nearly 100 mL higher over the course of hospitalization among patients who developed moderate to severe anemia, compared with those who did not (173.8 mL vs. 83.5 mL)," the investigators said (Arch. Intern Med. 2011; [doi:10.1001/archinternmed.2011.361]).
The average amount of blood drawn for laboratory testing varied significantly across hospitals, from a low of 53 mL to a high of 109.6 mL. The amount of blood typically drawn at a hospital significantly correlated with the incidence of anemia in its patients.
In a preliminary analysis, every 50 mL of blood drawn was associated with an 18% increase in the risk of hospital-acquired anemia. That risk persisted and remained robust after the data were adjusted to account for potential confounders.
When the data were broken down by day of hospitalization, the risk of developing anemia was highest on the first hospital day (10.5%), then remained relatively constant at 2.8%-4.5% through 10 days of hospitalization.
"Since most diagnostic evaluation and therapeutic interventions occur early during acute MI hospitalization, it is likely that much of the blood taken later during hospitalization represents routine, scheduled laboratory draws that could lead to ongoing blood loss." Indeed, blood loss was particularly high among patients who had longer hospital stays.
Several factors contribute to the development of hospital-acquired anemia. Some of these are not modifiable, such as patient age and sex, the presence of chronic kidney disease, and acute inflammation. But one factor that is clearly under the control of health care providers is minimization of phlebotomy, Dr. Salisbury and his associates said.
This study was retrospective and observational and so could not establish causality. Prospective randomized trials are needed to establish that the blood draws caused the anemia, as well as to determine whether strategies that limit both the number of blood draws and the volume of blood removed for diagnostic testing can prevent hospital-acquired anemia and improve clinical outcomes, they noted.
Dr. Salisbury and two associates were funded in part by an award from the American Heart Association Pharmaceutical Round Table. The investigators reported ties to numerous drug companies.
Blood loss from diagnostic blood testing during hospitalization is substantial and has been linked to anemia in patients with acute myocardial infarction, according to a study published online Aug. 8 in the Archives of Internal Medicine.
In a study of 17,676 MI patients at 57 U.S. hospitals, 1 in 5 patients developed moderate to severe hospital-acquired anemia, and they had a mean estimated phlebotomy volume of 173.8 mL – the equivalent of half a unit of whole blood. Twelve percent of the study subjects lost more than 300 mL to blood draws during the course of their hospitalization, said Dr. Adam C. Salisbury of Saint Luke’s Mid America Heart and Vascular Institute, Kansas City, Mo., and his associates.
"Our findings are likely generalizable to other populations of seriously ill medical patients," they noted.
If further research establishes that minimizing blood loss from phlebotomy prevents anemia and improves patient outcomes, there would be broad implications for all hospitalized patients. Strategies to minimize blood loss, such as using pediatric instead of adult blood tubes or filling standard 4-mL adult tubes with only 1-2 mL of blood, would be widely adopted, Dr. Salisbury and his colleagues added.
They explored the relationship between diagnostic blood testing and the risk of hospital-acquired anemia in MI patients because blood draws have been associated with increased need for transfusions in this patient population. The researchers used information from an electronic medical record database that detailed the frequency and type of laboratory testing as well as patients’ hemoglobin levels throughout hospitalization for acute MI. The database covered 57 hospitals during a recent 8-year period.
The study cohort was composed of all patients with acute MI, excluding those who already had anemia at admission and those who underwent coronary artery bypass grafting, because both the etiology and outcomes of anemia differ from those of non-CABG patients.
The data did not include exact amounts of blood drawn for every test. The investigators estimated these amounts from the types of tests that were run, assuming that only the minimal blood volume needed to run the required tests was drawn and that no blood was wasted at the blood draws.
Twenty percent of the study cohort (3,551 patients) developed moderate to severe anemia during hospitalization. Mean hemoglobin values declined in all patients, but they declined to a greater degree in those who developed anemia (–3.9 g/dL), compared with patients who didn’t develop anemia (–1.6 g/dL).
"The estimated mean blood loss from phlebotomy was nearly 100 mL higher over the course of hospitalization among patients who developed moderate to severe anemia, compared with those who did not (173.8 mL vs. 83.5 mL)," the investigators said (Arch. Intern Med. 2011; [doi:10.1001/archinternmed.2011.361]).
The average amount of blood drawn for laboratory testing varied significantly across hospitals, from a low of 53 mL to a high of 109.6 mL. The amount of blood typically drawn at a hospital significantly correlated with the incidence of anemia in its patients.
In a preliminary analysis, every 50 mL of blood drawn was associated with an 18% increase in the risk of hospital-acquired anemia. That risk persisted and remained robust after the data were adjusted to account for potential confounders.
When the data were broken down by day of hospitalization, the risk of developing anemia was highest on the first hospital day (10.5%), then remained relatively constant at 2.8%-4.5% through 10 days of hospitalization.
"Since most diagnostic evaluation and therapeutic interventions occur early during acute MI hospitalization, it is likely that much of the blood taken later during hospitalization represents routine, scheduled laboratory draws that could lead to ongoing blood loss." Indeed, blood loss was particularly high among patients who had longer hospital stays.
Several factors contribute to the development of hospital-acquired anemia. Some of these are not modifiable, such as patient age and sex, the presence of chronic kidney disease, and acute inflammation. But one factor that is clearly under the control of health care providers is minimization of phlebotomy, Dr. Salisbury and his associates said.
This study was retrospective and observational and so could not establish causality. Prospective randomized trials are needed to establish that the blood draws caused the anemia, as well as to determine whether strategies that limit both the number of blood draws and the volume of blood removed for diagnostic testing can prevent hospital-acquired anemia and improve clinical outcomes, they noted.
Dr. Salisbury and two associates were funded in part by an award from the American Heart Association Pharmaceutical Round Table. The investigators reported ties to numerous drug companies.
Blood loss from diagnostic blood testing during hospitalization is substantial and has been linked to anemia in patients with acute myocardial infarction, according to a study published online Aug. 8 in the Archives of Internal Medicine.
In a study of 17,676 MI patients at 57 U.S. hospitals, 1 in 5 patients developed moderate to severe hospital-acquired anemia, and they had a mean estimated phlebotomy volume of 173.8 mL – the equivalent of half a unit of whole blood. Twelve percent of the study subjects lost more than 300 mL to blood draws during the course of their hospitalization, said Dr. Adam C. Salisbury of Saint Luke’s Mid America Heart and Vascular Institute, Kansas City, Mo., and his associates.
"Our findings are likely generalizable to other populations of seriously ill medical patients," they noted.
If further research establishes that minimizing blood loss from phlebotomy prevents anemia and improves patient outcomes, there would be broad implications for all hospitalized patients. Strategies to minimize blood loss, such as using pediatric instead of adult blood tubes or filling standard 4-mL adult tubes with only 1-2 mL of blood, would be widely adopted, Dr. Salisbury and his colleagues added.
They explored the relationship between diagnostic blood testing and the risk of hospital-acquired anemia in MI patients because blood draws have been associated with increased need for transfusions in this patient population. The researchers used information from an electronic medical record database that detailed the frequency and type of laboratory testing as well as patients’ hemoglobin levels throughout hospitalization for acute MI. The database covered 57 hospitals during a recent 8-year period.
The study cohort was composed of all patients with acute MI, excluding those who already had anemia at admission and those who underwent coronary artery bypass grafting, because both the etiology and outcomes of anemia differ from those of non-CABG patients.
The data did not include exact amounts of blood drawn for every test. The investigators estimated these amounts from the types of tests that were run, assuming that only the minimal blood volume needed to run the required tests was drawn and that no blood was wasted at the blood draws.
Twenty percent of the study cohort (3,551 patients) developed moderate to severe anemia during hospitalization. Mean hemoglobin values declined in all patients, but they declined to a greater degree in those who developed anemia (–3.9 g/dL), compared with patients who didn’t develop anemia (–1.6 g/dL).
"The estimated mean blood loss from phlebotomy was nearly 100 mL higher over the course of hospitalization among patients who developed moderate to severe anemia, compared with those who did not (173.8 mL vs. 83.5 mL)," the investigators said (Arch. Intern Med. 2011; [doi:10.1001/archinternmed.2011.361]).
The average amount of blood drawn for laboratory testing varied significantly across hospitals, from a low of 53 mL to a high of 109.6 mL. The amount of blood typically drawn at a hospital significantly correlated with the incidence of anemia in its patients.
In a preliminary analysis, every 50 mL of blood drawn was associated with an 18% increase in the risk of hospital-acquired anemia. That risk persisted and remained robust after the data were adjusted to account for potential confounders.
When the data were broken down by day of hospitalization, the risk of developing anemia was highest on the first hospital day (10.5%), then remained relatively constant at 2.8%-4.5% through 10 days of hospitalization.
"Since most diagnostic evaluation and therapeutic interventions occur early during acute MI hospitalization, it is likely that much of the blood taken later during hospitalization represents routine, scheduled laboratory draws that could lead to ongoing blood loss." Indeed, blood loss was particularly high among patients who had longer hospital stays.
Several factors contribute to the development of hospital-acquired anemia. Some of these are not modifiable, such as patient age and sex, the presence of chronic kidney disease, and acute inflammation. But one factor that is clearly under the control of health care providers is minimization of phlebotomy, Dr. Salisbury and his associates said.
This study was retrospective and observational and so could not establish causality. Prospective randomized trials are needed to establish that the blood draws caused the anemia, as well as to determine whether strategies that limit both the number of blood draws and the volume of blood removed for diagnostic testing can prevent hospital-acquired anemia and improve clinical outcomes, they noted.
Dr. Salisbury and two associates were funded in part by an award from the American Heart Association Pharmaceutical Round Table. The investigators reported ties to numerous drug companies.
FROM THE ARCHIVES OF INTERNAL MEDICINE
Major Finding: A total of 20% of patients with acute MI acquired anemia during hospitalization, and those who did so lost approximately 174 mL of blood to draws for laboratory testing, compared with only 84 mL for patients who did not develop anemia. Every 50 mL of blood drawn was associated with an 18% rise in risk for anemia.
Data Source: A retrospective, observational study of blood draws for laboratory testing and hemoglobin values in 17,676 patients hospitalized at 57 U.S. medical centers for acute MI during an 8-year period.
Disclosures: Dr. Salisbury and two associates were funded in part by an award from the American Heart Association Pharmaceutical Round Table. The investigators reported ties to numerous drug companies.
Today's Residents Have Confidence, Experience Using TPA
Ninety-four percent of graduating neurology residents say they are comfortable treating stroke patients with intravenous tissue plasminogen activator – a dramatic increase from the 73% who said this a decade earlier, investigators reported in an article published online Aug. 8 in Stroke.
The improvement is largely due to residents’ personal experience in using the treatment during their training. In particular, residents who were eventually allowed to administer tissue plasminogen activator (TPA) without direct faculty supervision were the most confident about using it in future practice, said Dr. Vera Fridman of the department of neurology, University of Pennsylvania, Philadelphia, and her associates.
"It is imperative that neurology residents attain a level of comfort with the use of TPA that will allow them to utilize the medication effectively in their clinical practice and guide other physicians in its use," the investigators noted.
Dr. Fridman and her colleagues used the American Medical Association Graduate Medical Education Database to identify all neurology residents completing their final year of training in the United States during 2010. These residents were sent a 12-item anonymous questionnaire assessing their experience with TPA. The questionnaire was identical to one that had been administered to neurology residents who graduated in 2000 – the first cohort to have completed all 4 years of training after FDA approval of TPA for acute ischemic stroke.
The response rate to the current survey was 58%, with 286 respondents comprising the study cohort.
Overall, 95% of the neurology residents graduating in 2010 who responded to the survey reported that they had personally used TPA to treat stroke, and another 4% had observed such treatment. A total of 94% said they would be comfortable using the treatment independently in their own practices, Dr. Fridman and her associates said (Stroke 2011 Aug. 8 [doi:10.1161/strokeaha.111.621839]).
Respondents were much more likely to feel confident using TPA if they had personal experience with the drug (96%) than if they were inexperienced (60%). Those who had treated a patient without direct faculty supervision were much more likely to feel comfortable (78%) than were those who had only used it under direct faculty supervision (52%).
In addition, residents at an institution that employed a stroke team were more likely to feel comfortable using TPA than those at institutions without a stroke team (68% vs. 37%, respectively). Residents who had received formal training in the National Institutes of Health Stroke Scale were more likely to feel comfortable using TPA than those who had not received such training (67% vs. 45%, respectively).
In comparison, only 73% of graduating neurology residents in the 2000 survey said they were comfortable using TPA. Only 88% had observed TPA administration during training (versus 99% in 2010), only 80% had personally used the drug during training (versus 95% in 2010), and only 89% had been involved in post-TPA care (versus 98% in 2010). Similarly, only 65% of neurology residents in 2000 had been trained in the NIH Stroke Scale and only 84% had a stroke team at their institution. All of these percentages from 2000 were significantly lower than the corresponding figures for 2010 (P < .001).
The finding that so many factors related to TPA use have improved so much in 10 years is "encouraging," but the study results also show that the amount of autonomy given to neurology residents caring for stroke patients still varies widely.
"Giving neurology residents more autonomy in decision making regarding TPA administration may increase their comfort using TPA in practice. This balance between supervision and independence is a fundamental tension throughout medical training," Dr. Fridman and her colleagues said.
The survey also showed that almost all current residents are confident in their ability to identify brain hemorrhage (99%-100%) and early infarct signs (94%-98%) on computed tomography, as were respondents to the survey in 2000.
No financial conflicts of interest were reported.
Ninety-four percent of graduating neurology residents say they are comfortable treating stroke patients with intravenous tissue plasminogen activator – a dramatic increase from the 73% who said this a decade earlier, investigators reported in an article published online Aug. 8 in Stroke.
The improvement is largely due to residents’ personal experience in using the treatment during their training. In particular, residents who were eventually allowed to administer tissue plasminogen activator (TPA) without direct faculty supervision were the most confident about using it in future practice, said Dr. Vera Fridman of the department of neurology, University of Pennsylvania, Philadelphia, and her associates.
"It is imperative that neurology residents attain a level of comfort with the use of TPA that will allow them to utilize the medication effectively in their clinical practice and guide other physicians in its use," the investigators noted.
Dr. Fridman and her colleagues used the American Medical Association Graduate Medical Education Database to identify all neurology residents completing their final year of training in the United States during 2010. These residents were sent a 12-item anonymous questionnaire assessing their experience with TPA. The questionnaire was identical to one that had been administered to neurology residents who graduated in 2000 – the first cohort to have completed all 4 years of training after FDA approval of TPA for acute ischemic stroke.
The response rate to the current survey was 58%, with 286 respondents comprising the study cohort.
Overall, 95% of the neurology residents graduating in 2010 who responded to the survey reported that they had personally used TPA to treat stroke, and another 4% had observed such treatment. A total of 94% said they would be comfortable using the treatment independently in their own practices, Dr. Fridman and her associates said (Stroke 2011 Aug. 8 [doi:10.1161/strokeaha.111.621839]).
Respondents were much more likely to feel confident using TPA if they had personal experience with the drug (96%) than if they were inexperienced (60%). Those who had treated a patient without direct faculty supervision were much more likely to feel comfortable (78%) than were those who had only used it under direct faculty supervision (52%).
In addition, residents at an institution that employed a stroke team were more likely to feel comfortable using TPA than those at institutions without a stroke team (68% vs. 37%, respectively). Residents who had received formal training in the National Institutes of Health Stroke Scale were more likely to feel comfortable using TPA than those who had not received such training (67% vs. 45%, respectively).
In comparison, only 73% of graduating neurology residents in the 2000 survey said they were comfortable using TPA. Only 88% had observed TPA administration during training (versus 99% in 2010), only 80% had personally used the drug during training (versus 95% in 2010), and only 89% had been involved in post-TPA care (versus 98% in 2010). Similarly, only 65% of neurology residents in 2000 had been trained in the NIH Stroke Scale and only 84% had a stroke team at their institution. All of these percentages from 2000 were significantly lower than the corresponding figures for 2010 (P < .001).
The finding that so many factors related to TPA use have improved so much in 10 years is "encouraging," but the study results also show that the amount of autonomy given to neurology residents caring for stroke patients still varies widely.
"Giving neurology residents more autonomy in decision making regarding TPA administration may increase their comfort using TPA in practice. This balance between supervision and independence is a fundamental tension throughout medical training," Dr. Fridman and her colleagues said.
The survey also showed that almost all current residents are confident in their ability to identify brain hemorrhage (99%-100%) and early infarct signs (94%-98%) on computed tomography, as were respondents to the survey in 2000.
No financial conflicts of interest were reported.
Ninety-four percent of graduating neurology residents say they are comfortable treating stroke patients with intravenous tissue plasminogen activator – a dramatic increase from the 73% who said this a decade earlier, investigators reported in an article published online Aug. 8 in Stroke.
The improvement is largely due to residents’ personal experience in using the treatment during their training. In particular, residents who were eventually allowed to administer tissue plasminogen activator (TPA) without direct faculty supervision were the most confident about using it in future practice, said Dr. Vera Fridman of the department of neurology, University of Pennsylvania, Philadelphia, and her associates.
"It is imperative that neurology residents attain a level of comfort with the use of TPA that will allow them to utilize the medication effectively in their clinical practice and guide other physicians in its use," the investigators noted.
Dr. Fridman and her colleagues used the American Medical Association Graduate Medical Education Database to identify all neurology residents completing their final year of training in the United States during 2010. These residents were sent a 12-item anonymous questionnaire assessing their experience with TPA. The questionnaire was identical to one that had been administered to neurology residents who graduated in 2000 – the first cohort to have completed all 4 years of training after FDA approval of TPA for acute ischemic stroke.
The response rate to the current survey was 58%, with 286 respondents comprising the study cohort.
Overall, 95% of the neurology residents graduating in 2010 who responded to the survey reported that they had personally used TPA to treat stroke, and another 4% had observed such treatment. A total of 94% said they would be comfortable using the treatment independently in their own practices, Dr. Fridman and her associates said (Stroke 2011 Aug. 8 [doi:10.1161/strokeaha.111.621839]).
Respondents were much more likely to feel confident using TPA if they had personal experience with the drug (96%) than if they were inexperienced (60%). Those who had treated a patient without direct faculty supervision were much more likely to feel comfortable (78%) than were those who had only used it under direct faculty supervision (52%).
In addition, residents at an institution that employed a stroke team were more likely to feel comfortable using TPA than those at institutions without a stroke team (68% vs. 37%, respectively). Residents who had received formal training in the National Institutes of Health Stroke Scale were more likely to feel comfortable using TPA than those who had not received such training (67% vs. 45%, respectively).
In comparison, only 73% of graduating neurology residents in the 2000 survey said they were comfortable using TPA. Only 88% had observed TPA administration during training (versus 99% in 2010), only 80% had personally used the drug during training (versus 95% in 2010), and only 89% had been involved in post-TPA care (versus 98% in 2010). Similarly, only 65% of neurology residents in 2000 had been trained in the NIH Stroke Scale and only 84% had a stroke team at their institution. All of these percentages from 2000 were significantly lower than the corresponding figures for 2010 (P < .001).
The finding that so many factors related to TPA use have improved so much in 10 years is "encouraging," but the study results also show that the amount of autonomy given to neurology residents caring for stroke patients still varies widely.
"Giving neurology residents more autonomy in decision making regarding TPA administration may increase their comfort using TPA in practice. This balance between supervision and independence is a fundamental tension throughout medical training," Dr. Fridman and her colleagues said.
The survey also showed that almost all current residents are confident in their ability to identify brain hemorrhage (99%-100%) and early infarct signs (94%-98%) on computed tomography, as were respondents to the survey in 2000.
No financial conflicts of interest were reported.
FROM STROKE
Major Finding: Among neurology residents graduating in 2010, 94% said they would be comfortable treating acute ischemic stroke with TPA in their clinical practice and 95% already had experience doing so during training. The corresponding numbers from 2000 were 73% and 88%, showing significant improvements during the past decade.
Data Source: A 12-item anonymous survey regarding TPA treatment, completed by two groups of U.S. neurology residents when they graduated in 2000 and 2010.
Disclosures: No financial conflicts of interest were reported.
Adjunctive Risperidone Not Effective in SRI-Resistant PTSD
The antipsychotic drug risperidone does not improve posttraumatic stress disorder in veterans whose symptoms are resistant to serotonin reuptake inhibitors, according to a report in the Aug. 3 issue of JAMA.
Risperidone was not superior to placebo on any of 10 measures of a spectrum of outcomes in a 6-month study involving 267 military personnel who had experienced combat, said Dr. John H. Krystal of the clinical neurosciences division, Veterans Affairs National Center for PTSD, West Haven, Conn., and his associates.
These findings call into question the widespread off-label use of risperidone and other second-generation antipsychotic drugs for chronic, resistant posttraumatic stress disorder (PTSD). Even though limited evidence supports such therapy and despite "substantial safety concerns," nearly 87,000 veterans diagnosed as having PTSD received an antipsychotic prescription in 2009, and 94% of these prescriptions were for second-generation antipsychotics, the investigators said (JAMA 2011;306:493-502).
Combat-induced PTSD is particularly resistant to pharmacotherapy with serotonin reuptake inhibitors, which have been approved by the Food and Drug Administration for this indication. So it is not surprising that veterans often receive off-label treatment for their intransigent symptoms. Dr. Krystal and his colleagues performed "the first large trial of a pharmacotherapy aimed at SRI-resistant symptoms," enrolling patients who had not responded to or not tolerated at least two adequate (4 weeks or longer) courses of SRIs.
The study subjects were recruited from 23 VA medical centers and randomly assigned in a double-blind fashion to receive risperidone (133 patients) or an identical-looking placebo (134 patients), in addition to their regular PTSD treatments. The subjects underwent extensive assessment – with 10 different instruments measuring PTSD symptoms, global clinical factors, quality of life, sleep quality, depression, anxiety, and psychosis – at baseline, 6 weeks, 12 weeks, and at the conclusion of the intervention at 24 weeks.
These patients were severely ill, with disabilities related to long-standing PTSD. Most (72%) had served in the Vietnam War or earlier conflicts, though 24% had seen action in the Iraq or Afghanistan wars. The mean subject age was 54 years, and 97% were men. Approximately 70% of the study subjects also met the criteria for major depression, and 63% met the criteria for alcohol abuse or dependence.
The primary outcome measure was the score on the 34-item Clinician-Administered PTSD Scale (CAPS). These scores decreased slightly over time with both risperidone (mean decrease, 16.3 points) and placebo (mean decrease, 12.5 points), and the difference between the two groups was not significant.
Moreover, the rate of remission did not differ between patients taking risperidone (4%) and those taking placebo (5%), Dr. Krystal and his colleagues reported.
The two groups also had similar outcomes on the Clinical Global Impression Scale, the Montgomery-Åsberg Depression Rating Scale, the Hamilton Anxiety Scale, the Positive and Negative Syndrome Scale, the Veterans RAND 36-Item Health Survey, the Boston Life Satisfaction Inventory, and all other measures.
Although risperidone was numerically superior to placebo on submeasures of hyperarousal and "re-experiencing," the effect was so small that it likely would not even be detected clinically, the researchers said.
Patients who took risperidone reported significantly more problems with weight gain, fatigue, somnolence, and hypersalivation. However, risperidone exerted no significant effects on three measures of extrapyramidal symptoms.
This study was supported by the VA Office of Research and Development. Risperidone and matching placebo were donated by Ortho-McNeil Janssen Scientific Affairs. Dr. Krystal reported ties to numerous industry sources, as did his associates.
The findings by Dr. Krystal and colleagues "seriously call into question the use of atypical antipsychotics in PTSD treatment," said Dr. Charles W. Hoge.
In the largest trial to date to assess adjunctive risperidone in veterans with chronic, severe PTSD, "no clinically meaningful benefits were found." Moreover, patients taking the active drug reported significantly more weight gain, somnolence, fatigue, and hypersalivation than did those taking placebo.
Because there is still a great need for effective treatments for the large number of patients who fail to respond to serotonin reuptake inhibitors, further research is needed, he said.
Dr. Hoge is with the Office of the Army Surgeon General and the Center for Psychiatry and Neuroscience at Walter Reed Army Institute of Research in Silver Spring, Md. He reported receiving royalties from a book and fees from book-related speaking engagements. These remarks were adapted from his editorial accompanying Dr. Krystal’s report (JAMA 2011;306:549-51).
The findings by Dr. Krystal and colleagues "seriously call into question the use of atypical antipsychotics in PTSD treatment," said Dr. Charles W. Hoge.
In the largest trial to date to assess adjunctive risperidone in veterans with chronic, severe PTSD, "no clinically meaningful benefits were found." Moreover, patients taking the active drug reported significantly more weight gain, somnolence, fatigue, and hypersalivation than did those taking placebo.
Because there is still a great need for effective treatments for the large number of patients who fail to respond to serotonin reuptake inhibitors, further research is needed, he said.
Dr. Hoge is with the Office of the Army Surgeon General and the Center for Psychiatry and Neuroscience at Walter Reed Army Institute of Research in Silver Spring, Md. He reported receiving royalties from a book and fees from book-related speaking engagements. These remarks were adapted from his editorial accompanying Dr. Krystal’s report (JAMA 2011;306:549-51).
The findings by Dr. Krystal and colleagues "seriously call into question the use of atypical antipsychotics in PTSD treatment," said Dr. Charles W. Hoge.
In the largest trial to date to assess adjunctive risperidone in veterans with chronic, severe PTSD, "no clinically meaningful benefits were found." Moreover, patients taking the active drug reported significantly more weight gain, somnolence, fatigue, and hypersalivation than did those taking placebo.
Because there is still a great need for effective treatments for the large number of patients who fail to respond to serotonin reuptake inhibitors, further research is needed, he said.
Dr. Hoge is with the Office of the Army Surgeon General and the Center for Psychiatry and Neuroscience at Walter Reed Army Institute of Research in Silver Spring, Md. He reported receiving royalties from a book and fees from book-related speaking engagements. These remarks were adapted from his editorial accompanying Dr. Krystal’s report (JAMA 2011;306:549-51).
The antipsychotic drug risperidone does not improve posttraumatic stress disorder in veterans whose symptoms are resistant to serotonin reuptake inhibitors, according to a report in the Aug. 3 issue of JAMA.
Risperidone was not superior to placebo on any of 10 measures of a spectrum of outcomes in a 6-month study involving 267 military personnel who had experienced combat, said Dr. John H. Krystal of the clinical neurosciences division, Veterans Affairs National Center for PTSD, West Haven, Conn., and his associates.
These findings call into question the widespread off-label use of risperidone and other second-generation antipsychotic drugs for chronic, resistant posttraumatic stress disorder (PTSD). Even though limited evidence supports such therapy and despite "substantial safety concerns," nearly 87,000 veterans diagnosed as having PTSD received an antipsychotic prescription in 2009, and 94% of these prescriptions were for second-generation antipsychotics, the investigators said (JAMA 2011;306:493-502).
Combat-induced PTSD is particularly resistant to pharmacotherapy with serotonin reuptake inhibitors, which have been approved by the Food and Drug Administration for this indication. So it is not surprising that veterans often receive off-label treatment for their intransigent symptoms. Dr. Krystal and his colleagues performed "the first large trial of a pharmacotherapy aimed at SRI-resistant symptoms," enrolling patients who had not responded to or not tolerated at least two adequate (4 weeks or longer) courses of SRIs.
The study subjects were recruited from 23 VA medical centers and randomly assigned in a double-blind fashion to receive risperidone (133 patients) or an identical-looking placebo (134 patients), in addition to their regular PTSD treatments. The subjects underwent extensive assessment – with 10 different instruments measuring PTSD symptoms, global clinical factors, quality of life, sleep quality, depression, anxiety, and psychosis – at baseline, 6 weeks, 12 weeks, and at the conclusion of the intervention at 24 weeks.
These patients were severely ill, with disabilities related to long-standing PTSD. Most (72%) had served in the Vietnam War or earlier conflicts, though 24% had seen action in the Iraq or Afghanistan wars. The mean subject age was 54 years, and 97% were men. Approximately 70% of the study subjects also met the criteria for major depression, and 63% met the criteria for alcohol abuse or dependence.
The primary outcome measure was the score on the 34-item Clinician-Administered PTSD Scale (CAPS). These scores decreased slightly over time with both risperidone (mean decrease, 16.3 points) and placebo (mean decrease, 12.5 points), and the difference between the two groups was not significant.
Moreover, the rate of remission did not differ between patients taking risperidone (4%) and those taking placebo (5%), Dr. Krystal and his colleagues reported.
The two groups also had similar outcomes on the Clinical Global Impression Scale, the Montgomery-Åsberg Depression Rating Scale, the Hamilton Anxiety Scale, the Positive and Negative Syndrome Scale, the Veterans RAND 36-Item Health Survey, the Boston Life Satisfaction Inventory, and all other measures.
Although risperidone was numerically superior to placebo on submeasures of hyperarousal and "re-experiencing," the effect was so small that it likely would not even be detected clinically, the researchers said.
Patients who took risperidone reported significantly more problems with weight gain, fatigue, somnolence, and hypersalivation. However, risperidone exerted no significant effects on three measures of extrapyramidal symptoms.
This study was supported by the VA Office of Research and Development. Risperidone and matching placebo were donated by Ortho-McNeil Janssen Scientific Affairs. Dr. Krystal reported ties to numerous industry sources, as did his associates.
The antipsychotic drug risperidone does not improve posttraumatic stress disorder in veterans whose symptoms are resistant to serotonin reuptake inhibitors, according to a report in the Aug. 3 issue of JAMA.
Risperidone was not superior to placebo on any of 10 measures of a spectrum of outcomes in a 6-month study involving 267 military personnel who had experienced combat, said Dr. John H. Krystal of the clinical neurosciences division, Veterans Affairs National Center for PTSD, West Haven, Conn., and his associates.
These findings call into question the widespread off-label use of risperidone and other second-generation antipsychotic drugs for chronic, resistant posttraumatic stress disorder (PTSD). Even though limited evidence supports such therapy and despite "substantial safety concerns," nearly 87,000 veterans diagnosed as having PTSD received an antipsychotic prescription in 2009, and 94% of these prescriptions were for second-generation antipsychotics, the investigators said (JAMA 2011;306:493-502).
Combat-induced PTSD is particularly resistant to pharmacotherapy with serotonin reuptake inhibitors, which have been approved by the Food and Drug Administration for this indication. So it is not surprising that veterans often receive off-label treatment for their intransigent symptoms. Dr. Krystal and his colleagues performed "the first large trial of a pharmacotherapy aimed at SRI-resistant symptoms," enrolling patients who had not responded to or not tolerated at least two adequate (4 weeks or longer) courses of SRIs.
The study subjects were recruited from 23 VA medical centers and randomly assigned in a double-blind fashion to receive risperidone (133 patients) or an identical-looking placebo (134 patients), in addition to their regular PTSD treatments. The subjects underwent extensive assessment – with 10 different instruments measuring PTSD symptoms, global clinical factors, quality of life, sleep quality, depression, anxiety, and psychosis – at baseline, 6 weeks, 12 weeks, and at the conclusion of the intervention at 24 weeks.
These patients were severely ill, with disabilities related to long-standing PTSD. Most (72%) had served in the Vietnam War or earlier conflicts, though 24% had seen action in the Iraq or Afghanistan wars. The mean subject age was 54 years, and 97% were men. Approximately 70% of the study subjects also met the criteria for major depression, and 63% met the criteria for alcohol abuse or dependence.
The primary outcome measure was the score on the 34-item Clinician-Administered PTSD Scale (CAPS). These scores decreased slightly over time with both risperidone (mean decrease, 16.3 points) and placebo (mean decrease, 12.5 points), and the difference between the two groups was not significant.
Moreover, the rate of remission did not differ between patients taking risperidone (4%) and those taking placebo (5%), Dr. Krystal and his colleagues reported.
The two groups also had similar outcomes on the Clinical Global Impression Scale, the Montgomery-Åsberg Depression Rating Scale, the Hamilton Anxiety Scale, the Positive and Negative Syndrome Scale, the Veterans RAND 36-Item Health Survey, the Boston Life Satisfaction Inventory, and all other measures.
Although risperidone was numerically superior to placebo on submeasures of hyperarousal and "re-experiencing," the effect was so small that it likely would not even be detected clinically, the researchers said.
Patients who took risperidone reported significantly more problems with weight gain, fatigue, somnolence, and hypersalivation. However, risperidone exerted no significant effects on three measures of extrapyramidal symptoms.
This study was supported by the VA Office of Research and Development. Risperidone and matching placebo were donated by Ortho-McNeil Janssen Scientific Affairs. Dr. Krystal reported ties to numerous industry sources, as did his associates.
FROM JAMA
Major Finding: Risperidone was no better than placebo at relieving PTSD symptoms or improving quality of life in combat veterans whose symptoms were resistant to serotonin reuptake inhibitors.
Data Source: A 6-month, prospective, double-blind, randomized trial comparing risperidone with placebo in 267 patients with long-standing, resistant PTSD.
Disclosures: This study was supported by the VA Office of Research and Development. Risperidone and matching placebo were donated by Ortho-McNeil Janssen Scientific Affairs. Dr. Krystal reported ties to numerous industry sources, as did his associates.
Violence Increases Women's Risk of Mental Disorders
Violence against women is significantly associated with mood, anxiety, and substance use disorders throughout the victim’s lifetime, according to a report in the Aug. 3 issue of JAMA.
Moreover, the relationship appears to be dose related, with higher rates of mental disorders seen in women who have been exposed to the most types of violence. In particular, women who have experienced three or four types of gender-based violence show a nearly 90% prevalence of mental disorders, while those who have never experienced it show only a 28% prevalence, said Susan Rees, Ph.D., of Australia’s University of New South Wales School of Psychiatry and the Center for Population Mental Health Research, Sydney, and her associates.
Four types of violence typically perpetrated against women (physical beating by an intimate partner, rape, other forms of sexual assault, and stalking) are collectively known as gender-based violence. Evidence that all of these are associated with mental disorders has been increasing. Dr. Rees and her colleagues studied the issue using data from the Australian Bureau of Statistics’ National Mental Health and Well-Being Survey.
The confidential survey, which included a representative sample of 4,451 Australian women aged 18-65 years, asked subjects whether they had ever been diagnosed as having any of four broad types of mental disorders: anxiety disorders (panic disorder, agoraphobia, social phobia, generalized anxiety disorder, or obsessive-compulsive disorder); mood disorders (major depressive episode, dysthymia, or bipolar affective disorder); substance use disorders; or posttraumatic stress disorder (PTSD).
The survey also asked specifically about the four forms of gender-based violence. The most common type of gender-based violence was sexual assault, which was reported by 14.7% of the study subjects. This was followed by stalking (reported by 10%), rape (reported by 8.1%), and physical violence by an intimate partner (reported by 7.8%).
In the entire study population, the lifetime prevalence of any mental disorder was 37.8%. The overall prevalence of anxiety disorders was 24.6%; of mood disorders, 18.3%; of substance use disorders, 13.9%; and of PTSD, 9.8%.
These rates were significantly higher in the 1,218 women who reported experiencing at least one type of gender-based violence.
The prevalence of any mental disorder was 57.3% for women who had experienced one form of gender-based violence, and 89.4% for those who experienced three or four types. In comparison, women who were never exposed to gender-based violence had only a 28% prevalence of mental disorders, the investigators said (JAMA 2011;306:513-21).
Women exposed to one type of gender-based violence had a lifetime prevalence of 30.7% for mood disorders, 38.5% for anxiety disorders, 23% for substance use disorders, and 15.2% for PTSD.
However, most women who experienced one type of gender-based violence also experienced other types during the course of their lives. For women who reported experiencing three or four types of gender-based violence, the prevalence of anxiety disorders was 77.3%, that of mood disorders was 52.5%, that of substance use disorders was 47.1%, and that of PTSD was 56.2%.
Women who had never experienced gender-based violence showed a lifetime rate of suicide attempts of 1.6%. In contrast, those who had experienced one type of violence had a suicide-attempt rate that was more than four times higher at 6.6%, and those who had experienced three to four types of violence had a suicide attempt rate more than 22 times higher, at 34.7%.
In addition to mental disorders, women who experienced gender-based violence showed an overall pattern of social disadvantage, disability, and impaired quality of life. "An important question raised by our research is whether existing services address [these] multiple domains of disability and dysfunction associated with gender-based violence," Dr. Rees and her colleagues said.
Services for victims of gender-based violence tend to be separate from mental health services, which reduces stigma but also restricts access to the full array of mental health interventions. The severity of the mental disorders and the extent of comorbidities revealed in this study "require expert and comprehensive approaches to treatment" that are not available in typical programs for gender-based violence, they noted.
Similarly, providers of psychiatric services must be equipped to assist women with mental health disorders who are found to have experienced gender-based violence. For example, such women may have difficulty attending group therapy or inpatient care that includes male patients. And personnel must be trained "in strategies to engage and interview women in a gender-sensitive manner; to build trust; and to ensure safety, privacy, and confidentiality in all interactions," they added.
This study was funded by the National Health and Medical Research Council of Australia. No conflicts of interest were reported.
Violence against women is significantly associated with mood, anxiety, and substance use disorders throughout the victim’s lifetime, according to a report in the Aug. 3 issue of JAMA.
Moreover, the relationship appears to be dose related, with higher rates of mental disorders seen in women who have been exposed to the most types of violence. In particular, women who have experienced three or four types of gender-based violence show a nearly 90% prevalence of mental disorders, while those who have never experienced it show only a 28% prevalence, said Susan Rees, Ph.D., of Australia’s University of New South Wales School of Psychiatry and the Center for Population Mental Health Research, Sydney, and her associates.
Four types of violence typically perpetrated against women (physical beating by an intimate partner, rape, other forms of sexual assault, and stalking) are collectively known as gender-based violence. Evidence that all of these are associated with mental disorders has been increasing. Dr. Rees and her colleagues studied the issue using data from the Australian Bureau of Statistics’ National Mental Health and Well-Being Survey.
The confidential survey, which included a representative sample of 4,451 Australian women aged 18-65 years, asked subjects whether they had ever been diagnosed as having any of four broad types of mental disorders: anxiety disorders (panic disorder, agoraphobia, social phobia, generalized anxiety disorder, or obsessive-compulsive disorder); mood disorders (major depressive episode, dysthymia, or bipolar affective disorder); substance use disorders; or posttraumatic stress disorder (PTSD).
The survey also asked specifically about the four forms of gender-based violence. The most common type of gender-based violence was sexual assault, which was reported by 14.7% of the study subjects. This was followed by stalking (reported by 10%), rape (reported by 8.1%), and physical violence by an intimate partner (reported by 7.8%).
In the entire study population, the lifetime prevalence of any mental disorder was 37.8%. The overall prevalence of anxiety disorders was 24.6%; of mood disorders, 18.3%; of substance use disorders, 13.9%; and of PTSD, 9.8%.
These rates were significantly higher in the 1,218 women who reported experiencing at least one type of gender-based violence.
The prevalence of any mental disorder was 57.3% for women who had experienced one form of gender-based violence, and 89.4% for those who experienced three or four types. In comparison, women who were never exposed to gender-based violence had only a 28% prevalence of mental disorders, the investigators said (JAMA 2011;306:513-21).
Women exposed to one type of gender-based violence had a lifetime prevalence of 30.7% for mood disorders, 38.5% for anxiety disorders, 23% for substance use disorders, and 15.2% for PTSD.
However, most women who experienced one type of gender-based violence also experienced other types during the course of their lives. For women who reported experiencing three or four types of gender-based violence, the prevalence of anxiety disorders was 77.3%, that of mood disorders was 52.5%, that of substance use disorders was 47.1%, and that of PTSD was 56.2%.
Women who had never experienced gender-based violence showed a lifetime rate of suicide attempts of 1.6%. In contrast, those who had experienced one type of violence had a suicide-attempt rate that was more than four times higher at 6.6%, and those who had experienced three to four types of violence had a suicide attempt rate more than 22 times higher, at 34.7%.
In addition to mental disorders, women who experienced gender-based violence showed an overall pattern of social disadvantage, disability, and impaired quality of life. "An important question raised by our research is whether existing services address [these] multiple domains of disability and dysfunction associated with gender-based violence," Dr. Rees and her colleagues said.
Services for victims of gender-based violence tend to be separate from mental health services, which reduces stigma but also restricts access to the full array of mental health interventions. The severity of the mental disorders and the extent of comorbidities revealed in this study "require expert and comprehensive approaches to treatment" that are not available in typical programs for gender-based violence, they noted.
Similarly, providers of psychiatric services must be equipped to assist women with mental health disorders who are found to have experienced gender-based violence. For example, such women may have difficulty attending group therapy or inpatient care that includes male patients. And personnel must be trained "in strategies to engage and interview women in a gender-sensitive manner; to build trust; and to ensure safety, privacy, and confidentiality in all interactions," they added.
This study was funded by the National Health and Medical Research Council of Australia. No conflicts of interest were reported.
Violence against women is significantly associated with mood, anxiety, and substance use disorders throughout the victim’s lifetime, according to a report in the Aug. 3 issue of JAMA.
Moreover, the relationship appears to be dose related, with higher rates of mental disorders seen in women who have been exposed to the most types of violence. In particular, women who have experienced three or four types of gender-based violence show a nearly 90% prevalence of mental disorders, while those who have never experienced it show only a 28% prevalence, said Susan Rees, Ph.D., of Australia’s University of New South Wales School of Psychiatry and the Center for Population Mental Health Research, Sydney, and her associates.
Four types of violence typically perpetrated against women (physical beating by an intimate partner, rape, other forms of sexual assault, and stalking) are collectively known as gender-based violence. Evidence that all of these are associated with mental disorders has been increasing. Dr. Rees and her colleagues studied the issue using data from the Australian Bureau of Statistics’ National Mental Health and Well-Being Survey.
The confidential survey, which included a representative sample of 4,451 Australian women aged 18-65 years, asked subjects whether they had ever been diagnosed as having any of four broad types of mental disorders: anxiety disorders (panic disorder, agoraphobia, social phobia, generalized anxiety disorder, or obsessive-compulsive disorder); mood disorders (major depressive episode, dysthymia, or bipolar affective disorder); substance use disorders; or posttraumatic stress disorder (PTSD).
The survey also asked specifically about the four forms of gender-based violence. The most common type of gender-based violence was sexual assault, which was reported by 14.7% of the study subjects. This was followed by stalking (reported by 10%), rape (reported by 8.1%), and physical violence by an intimate partner (reported by 7.8%).
In the entire study population, the lifetime prevalence of any mental disorder was 37.8%. The overall prevalence of anxiety disorders was 24.6%; of mood disorders, 18.3%; of substance use disorders, 13.9%; and of PTSD, 9.8%.
These rates were significantly higher in the 1,218 women who reported experiencing at least one type of gender-based violence.
The prevalence of any mental disorder was 57.3% for women who had experienced one form of gender-based violence, and 89.4% for those who experienced three or four types. In comparison, women who were never exposed to gender-based violence had only a 28% prevalence of mental disorders, the investigators said (JAMA 2011;306:513-21).
Women exposed to one type of gender-based violence had a lifetime prevalence of 30.7% for mood disorders, 38.5% for anxiety disorders, 23% for substance use disorders, and 15.2% for PTSD.
However, most women who experienced one type of gender-based violence also experienced other types during the course of their lives. For women who reported experiencing three or four types of gender-based violence, the prevalence of anxiety disorders was 77.3%, that of mood disorders was 52.5%, that of substance use disorders was 47.1%, and that of PTSD was 56.2%.
Women who had never experienced gender-based violence showed a lifetime rate of suicide attempts of 1.6%. In contrast, those who had experienced one type of violence had a suicide-attempt rate that was more than four times higher at 6.6%, and those who had experienced three to four types of violence had a suicide attempt rate more than 22 times higher, at 34.7%.
In addition to mental disorders, women who experienced gender-based violence showed an overall pattern of social disadvantage, disability, and impaired quality of life. "An important question raised by our research is whether existing services address [these] multiple domains of disability and dysfunction associated with gender-based violence," Dr. Rees and her colleagues said.
Services for victims of gender-based violence tend to be separate from mental health services, which reduces stigma but also restricts access to the full array of mental health interventions. The severity of the mental disorders and the extent of comorbidities revealed in this study "require expert and comprehensive approaches to treatment" that are not available in typical programs for gender-based violence, they noted.
Similarly, providers of psychiatric services must be equipped to assist women with mental health disorders who are found to have experienced gender-based violence. For example, such women may have difficulty attending group therapy or inpatient care that includes male patients. And personnel must be trained "in strategies to engage and interview women in a gender-sensitive manner; to build trust; and to ensure safety, privacy, and confidentiality in all interactions," they added.
This study was funded by the National Health and Medical Research Council of Australia. No conflicts of interest were reported.
FROM JAMA
Major Finding: The prevalence of any mental disorder was 28% in women who had never experienced gender-based violence, compared with 57% in women who had experienced one type and 89% in those who had experienced three to four types of gender-based violence.
Data Source: A cross-sectional survey of a nationally representative sample of 4,451 Australian women aged 18-65 years.
Disclosures: This study was funded by the National Health and Medical Research Council of Australia. No conflicts of interest were reported.
Homosexual Activity Plus Meth Increases HIV Risk
Among boys and young men who have sex with men, those who also use methamphetamine appear to be at increased risk for HIV infection, according to a report in the August issue of Archives of Pediatric and Adolescent Medicine.
Compared with males aged 12-24 years who have sex with men but do not use methamphetamine, users are significantly less likely to use condoms and are more likely to acquire STDs, have sex with intravenous drug users, use other hard drugs, and have multiple sex partners, said Peter Freeman of Howard Brown Health Center and Children’s Memorial Hospital, Northwestern University, Chicago, and his associates.
Therefore, any efforts to prevent HIV infection in this age group must address substance abuse and partner selection, they noted.
Until now, little has been known about methamphetamine use and homosexual behavior among boys and young men because such research has focused on older men. "Existing data that pertain to young men who have sex with men were collected more than 15 years ago, before recent increases in the incidence of HIV. Behavior, mortality, and treatment have changed dramatically in 15 years," Mr. Freeman and his colleagues said (Arch. Pediatr. Adolesc. Med. 2011;165:736-40).
They assessed 595 young men who have sex with men using data from the Adolescent Medicine Trials Network for HIV/AIDS Interventions, a National Institutes of Health–funded prevention program. In each of eight cities (San Francisco, Los Angeles, San Diego, Chicago, Philadelphia, Washington, Baltimore, and New York), 20-30 subjects were enrolled at up to five venues such as bars, clubs, parks, and community organizations where young men who have sex with men congregated. These study subjects completed a 1-hour anonymous questionnaire regarding their drug and sexual practices.
A total of 408 of these boys and men reported never using of hard drugs and 151 reported using hard drugs within the preceding 90 days. Of these, 151, 64 reported using methamphetamine within the preceding 90 days.
Among those who recently used methamphetamine, 64% said that they were not attending school and 72% said they were currently homeless or had been homeless in the past. In comparison, 60% of subjects who had never used hard drugs were attending school and only 28% had ever been homeless.
More than half (52%) of methamphetamine users said that they had a history of at least one STD, compared with only 21% of nonusers. Similarly, significantly more methamphetamine users (86%) reported having two more sexual partners in the preceding 90 days, compared with nonusers (63%). And methamphetamine users were less likely to use a condom (33%) than were nonusers (54%), the investigators said.
Significantly more methamphetamine users said they had had sex with someone who had HIV (33%) or had had sex with someone who used IV drugs (52%), compared with nonusers (11% in both cases).
The investigators cited several limitations of the study. The study is not representative of all young men who have sex with men in the United States because the study focused on higher-risk boys and men in this demographic. In addition, methamphetamine use was classified based on self-report, "creating a classification bias."
Still, the findings indicate that HIV prevention programs for young men who have sex with men should include substance abuse and prevention components and information on partner selection, and they should address issues such as housing, education, and polydrug use, Mr. Freeman and his associates wrote.
This study was supported by the National Institute of Child Health and Human Development, the National Institute on Drug Abuse, and the National Institute of Mental Health. No financial conflicts of interest were reported.
Among boys and young men who have sex with men, those who also use methamphetamine appear to be at increased risk for HIV infection, according to a report in the August issue of Archives of Pediatric and Adolescent Medicine.
Compared with males aged 12-24 years who have sex with men but do not use methamphetamine, users are significantly less likely to use condoms and are more likely to acquire STDs, have sex with intravenous drug users, use other hard drugs, and have multiple sex partners, said Peter Freeman of Howard Brown Health Center and Children’s Memorial Hospital, Northwestern University, Chicago, and his associates.
Therefore, any efforts to prevent HIV infection in this age group must address substance abuse and partner selection, they noted.
Until now, little has been known about methamphetamine use and homosexual behavior among boys and young men because such research has focused on older men. "Existing data that pertain to young men who have sex with men were collected more than 15 years ago, before recent increases in the incidence of HIV. Behavior, mortality, and treatment have changed dramatically in 15 years," Mr. Freeman and his colleagues said (Arch. Pediatr. Adolesc. Med. 2011;165:736-40).
They assessed 595 young men who have sex with men using data from the Adolescent Medicine Trials Network for HIV/AIDS Interventions, a National Institutes of Health–funded prevention program. In each of eight cities (San Francisco, Los Angeles, San Diego, Chicago, Philadelphia, Washington, Baltimore, and New York), 20-30 subjects were enrolled at up to five venues such as bars, clubs, parks, and community organizations where young men who have sex with men congregated. These study subjects completed a 1-hour anonymous questionnaire regarding their drug and sexual practices.
A total of 408 of these boys and men reported never using of hard drugs and 151 reported using hard drugs within the preceding 90 days. Of these, 151, 64 reported using methamphetamine within the preceding 90 days.
Among those who recently used methamphetamine, 64% said that they were not attending school and 72% said they were currently homeless or had been homeless in the past. In comparison, 60% of subjects who had never used hard drugs were attending school and only 28% had ever been homeless.
More than half (52%) of methamphetamine users said that they had a history of at least one STD, compared with only 21% of nonusers. Similarly, significantly more methamphetamine users (86%) reported having two more sexual partners in the preceding 90 days, compared with nonusers (63%). And methamphetamine users were less likely to use a condom (33%) than were nonusers (54%), the investigators said.
Significantly more methamphetamine users said they had had sex with someone who had HIV (33%) or had had sex with someone who used IV drugs (52%), compared with nonusers (11% in both cases).
The investigators cited several limitations of the study. The study is not representative of all young men who have sex with men in the United States because the study focused on higher-risk boys and men in this demographic. In addition, methamphetamine use was classified based on self-report, "creating a classification bias."
Still, the findings indicate that HIV prevention programs for young men who have sex with men should include substance abuse and prevention components and information on partner selection, and they should address issues such as housing, education, and polydrug use, Mr. Freeman and his associates wrote.
This study was supported by the National Institute of Child Health and Human Development, the National Institute on Drug Abuse, and the National Institute of Mental Health. No financial conflicts of interest were reported.
Among boys and young men who have sex with men, those who also use methamphetamine appear to be at increased risk for HIV infection, according to a report in the August issue of Archives of Pediatric and Adolescent Medicine.
Compared with males aged 12-24 years who have sex with men but do not use methamphetamine, users are significantly less likely to use condoms and are more likely to acquire STDs, have sex with intravenous drug users, use other hard drugs, and have multiple sex partners, said Peter Freeman of Howard Brown Health Center and Children’s Memorial Hospital, Northwestern University, Chicago, and his associates.
Therefore, any efforts to prevent HIV infection in this age group must address substance abuse and partner selection, they noted.
Until now, little has been known about methamphetamine use and homosexual behavior among boys and young men because such research has focused on older men. "Existing data that pertain to young men who have sex with men were collected more than 15 years ago, before recent increases in the incidence of HIV. Behavior, mortality, and treatment have changed dramatically in 15 years," Mr. Freeman and his colleagues said (Arch. Pediatr. Adolesc. Med. 2011;165:736-40).
They assessed 595 young men who have sex with men using data from the Adolescent Medicine Trials Network for HIV/AIDS Interventions, a National Institutes of Health–funded prevention program. In each of eight cities (San Francisco, Los Angeles, San Diego, Chicago, Philadelphia, Washington, Baltimore, and New York), 20-30 subjects were enrolled at up to five venues such as bars, clubs, parks, and community organizations where young men who have sex with men congregated. These study subjects completed a 1-hour anonymous questionnaire regarding their drug and sexual practices.
A total of 408 of these boys and men reported never using of hard drugs and 151 reported using hard drugs within the preceding 90 days. Of these, 151, 64 reported using methamphetamine within the preceding 90 days.
Among those who recently used methamphetamine, 64% said that they were not attending school and 72% said they were currently homeless or had been homeless in the past. In comparison, 60% of subjects who had never used hard drugs were attending school and only 28% had ever been homeless.
More than half (52%) of methamphetamine users said that they had a history of at least one STD, compared with only 21% of nonusers. Similarly, significantly more methamphetamine users (86%) reported having two more sexual partners in the preceding 90 days, compared with nonusers (63%). And methamphetamine users were less likely to use a condom (33%) than were nonusers (54%), the investigators said.
Significantly more methamphetamine users said they had had sex with someone who had HIV (33%) or had had sex with someone who used IV drugs (52%), compared with nonusers (11% in both cases).
The investigators cited several limitations of the study. The study is not representative of all young men who have sex with men in the United States because the study focused on higher-risk boys and men in this demographic. In addition, methamphetamine use was classified based on self-report, "creating a classification bias."
Still, the findings indicate that HIV prevention programs for young men who have sex with men should include substance abuse and prevention components and information on partner selection, and they should address issues such as housing, education, and polydrug use, Mr. Freeman and his associates wrote.
This study was supported by the National Institute of Child Health and Human Development, the National Institute on Drug Abuse, and the National Institute of Mental Health. No financial conflicts of interest were reported.
FROM ARCHIVES OF PEDIATRIC AND ADOLESCENT MEDICINE
Major Finding: Among boys and young men who have sex with men, those who also used methamphetamine were more likely than nonusers to have a history of STDs (52% vs. 21%), to have had two or more sexual partners within the preceding 90 days (86% vs. 63%), and to have had sex with an HIV-positive partner (33% vs. 11%) or an IV-drug user (52% vs. 11%).
Data Source: A cross-sectional observational analysis of self-reported drug and sexual behavior among 595 males aged 12-24 years residing in eight U.S. cities.
Disclosures: This study was supported by the National Institute of Child Health and Human Development, the National Institute on Drug Abuse, and the National Institute of Mental Health. No financial conflicts of interest were reported.
Childhood Adversity, Mental Disorders Predict Chronic Illnesses
Both psychosocial adversities during childhood and early-onset mental disorders like anxiety and depression are strong, independent predictors of adult-onset chronic illness such as heart disease, according to a report in the August issue of the Archives of General Psychiatry.
These findings are from a World Health Organization survey of "a wide range of childhood adversities in a large, culturally diverse general population sample spanning the entire adult age range" in 10 countries. They are consistent with the theory that early adverse environments can raise the risk of a spectrum of chronic physical disorders later in life, probably by influencing the stress response and possibly by more direct biological mechanisms as well, said Kate M. Scott, Ph.D., of the department of psychological medicine at the University of Otago in Dunedin, New Zealand, and her associates.
The investigators analyzed data from the WHO’s World Mental Health Surveys program in which 18,303 adults of all ages in Europe, Asia, and the Americas were assessed for early-onset (defined as before age 21 years) generalized anxiety disorder, posttraumatic stress disorder, social phobia, major depressive disorder, and panic disorder and/or agoraphobia, as well as for six chronic, adult-onset physical conditions: heart disease, asthma, diabetes, osteoarthritis, chronic spinal pain, and frequent or severe headache (Arch. Gen. Psychiatry 2011;68:838-44).
The study subjects also provided histories that covered childhood adversities including physical abuse; sexual abuse; neglect; parental death or other parental loss; parental mental disorder, criminal behavior, or substance abuse; family violence; and poverty.
The strongest associations were found between the childhood adversities and adult-onset heart disease. The magnitude of risk was particularly high between childhood sexual abuse and later heart disease, with a hazard ratio of 3.91.
Physical abuse was associated with adult onset of all six chronic diseases. Loss of a parent and parental mental disorder both were associated with five of the six chronic diseases.
There was a dose-response relationship between the number of childhood adversities experienced and the likelihood of developing a chronic disease in adulthood. Having experienced two of the childhood adversities was strongly linked to five of the six chronic diseases, and having experienced three or more was strongly linked to all six chronic diseases.
Independently, all five early-onset mental disorders were associated with adult onset of the pain disorders of osteoarthritis, chronic spinal pain, and frequent/severe headache. The finding of associations between sexual abuse and chronic pain was especially noteworthy because prospective studies have failed to demonstrate such a link. It may be that the samples in these prospective studies were too young (with a median subject age of younger than 30 years) to demonstrate an association, because in this study of childhood adversities and spinal pain the link did not emerge until approximately age 40 years, Dr. Scott and her colleagues said.
Early-onset depression, PTSD, and panic disorder all predicted the later development of heart disease and asthma, and early-onset social phobia predicted later heart disease.
These findings should be considered exploratory in nature because this study was observational. Other limitations include dependence upon subjects’ self-report of medical and psychiatric diagnoses, although these correlated well with physician and medical records, as well as their recall of childhood events, the researchers added.
They noted that although the magnitude of risk "was generally modest" between childhood adversity or early-onset psychological disorders on the one hand and adult-onset chronic disease on the other, "many estimates are of a similar magnitude to the association between serum cholesterol and heart disease. The public health significance of the latter has less to do with its magnitude than with the prevalence of elevated serum cholesterol levels in the general population, and the same argument can be made for the risk factors of childhood adversities and depressive and anxiety disorders."
This study was funded principally by the U.S. National Institute of Mental Health; the MacArthur Foundation; the Pfizer Foundation; the U.S. Public Health Service; the Fogarty International Center; the Pan American Health Organization; the drug companies Eli Lilly, Ortho-McNeil Pharmaceuticals, GlaxoSmithKline, and Bristol-Myers Squibb; the European Commission; the Japan Ministry of Health, Labour, and Welfare; and various organizations within each of the 10 countries included in the survey. The investigators reported ties to numerous industry sources.
Both psychosocial adversities during childhood and early-onset mental disorders like anxiety and depression are strong, independent predictors of adult-onset chronic illness such as heart disease, according to a report in the August issue of the Archives of General Psychiatry.
These findings are from a World Health Organization survey of "a wide range of childhood adversities in a large, culturally diverse general population sample spanning the entire adult age range" in 10 countries. They are consistent with the theory that early adverse environments can raise the risk of a spectrum of chronic physical disorders later in life, probably by influencing the stress response and possibly by more direct biological mechanisms as well, said Kate M. Scott, Ph.D., of the department of psychological medicine at the University of Otago in Dunedin, New Zealand, and her associates.
The investigators analyzed data from the WHO’s World Mental Health Surveys program in which 18,303 adults of all ages in Europe, Asia, and the Americas were assessed for early-onset (defined as before age 21 years) generalized anxiety disorder, posttraumatic stress disorder, social phobia, major depressive disorder, and panic disorder and/or agoraphobia, as well as for six chronic, adult-onset physical conditions: heart disease, asthma, diabetes, osteoarthritis, chronic spinal pain, and frequent or severe headache (Arch. Gen. Psychiatry 2011;68:838-44).
The study subjects also provided histories that covered childhood adversities including physical abuse; sexual abuse; neglect; parental death or other parental loss; parental mental disorder, criminal behavior, or substance abuse; family violence; and poverty.
The strongest associations were found between the childhood adversities and adult-onset heart disease. The magnitude of risk was particularly high between childhood sexual abuse and later heart disease, with a hazard ratio of 3.91.
Physical abuse was associated with adult onset of all six chronic diseases. Loss of a parent and parental mental disorder both were associated with five of the six chronic diseases.
There was a dose-response relationship between the number of childhood adversities experienced and the likelihood of developing a chronic disease in adulthood. Having experienced two of the childhood adversities was strongly linked to five of the six chronic diseases, and having experienced three or more was strongly linked to all six chronic diseases.
Independently, all five early-onset mental disorders were associated with adult onset of the pain disorders of osteoarthritis, chronic spinal pain, and frequent/severe headache. The finding of associations between sexual abuse and chronic pain was especially noteworthy because prospective studies have failed to demonstrate such a link. It may be that the samples in these prospective studies were too young (with a median subject age of younger than 30 years) to demonstrate an association, because in this study of childhood adversities and spinal pain the link did not emerge until approximately age 40 years, Dr. Scott and her colleagues said.
Early-onset depression, PTSD, and panic disorder all predicted the later development of heart disease and asthma, and early-onset social phobia predicted later heart disease.
These findings should be considered exploratory in nature because this study was observational. Other limitations include dependence upon subjects’ self-report of medical and psychiatric diagnoses, although these correlated well with physician and medical records, as well as their recall of childhood events, the researchers added.
They noted that although the magnitude of risk "was generally modest" between childhood adversity or early-onset psychological disorders on the one hand and adult-onset chronic disease on the other, "many estimates are of a similar magnitude to the association between serum cholesterol and heart disease. The public health significance of the latter has less to do with its magnitude than with the prevalence of elevated serum cholesterol levels in the general population, and the same argument can be made for the risk factors of childhood adversities and depressive and anxiety disorders."
This study was funded principally by the U.S. National Institute of Mental Health; the MacArthur Foundation; the Pfizer Foundation; the U.S. Public Health Service; the Fogarty International Center; the Pan American Health Organization; the drug companies Eli Lilly, Ortho-McNeil Pharmaceuticals, GlaxoSmithKline, and Bristol-Myers Squibb; the European Commission; the Japan Ministry of Health, Labour, and Welfare; and various organizations within each of the 10 countries included in the survey. The investigators reported ties to numerous industry sources.
Both psychosocial adversities during childhood and early-onset mental disorders like anxiety and depression are strong, independent predictors of adult-onset chronic illness such as heart disease, according to a report in the August issue of the Archives of General Psychiatry.
These findings are from a World Health Organization survey of "a wide range of childhood adversities in a large, culturally diverse general population sample spanning the entire adult age range" in 10 countries. They are consistent with the theory that early adverse environments can raise the risk of a spectrum of chronic physical disorders later in life, probably by influencing the stress response and possibly by more direct biological mechanisms as well, said Kate M. Scott, Ph.D., of the department of psychological medicine at the University of Otago in Dunedin, New Zealand, and her associates.
The investigators analyzed data from the WHO’s World Mental Health Surveys program in which 18,303 adults of all ages in Europe, Asia, and the Americas were assessed for early-onset (defined as before age 21 years) generalized anxiety disorder, posttraumatic stress disorder, social phobia, major depressive disorder, and panic disorder and/or agoraphobia, as well as for six chronic, adult-onset physical conditions: heart disease, asthma, diabetes, osteoarthritis, chronic spinal pain, and frequent or severe headache (Arch. Gen. Psychiatry 2011;68:838-44).
The study subjects also provided histories that covered childhood adversities including physical abuse; sexual abuse; neglect; parental death or other parental loss; parental mental disorder, criminal behavior, or substance abuse; family violence; and poverty.
The strongest associations were found between the childhood adversities and adult-onset heart disease. The magnitude of risk was particularly high between childhood sexual abuse and later heart disease, with a hazard ratio of 3.91.
Physical abuse was associated with adult onset of all six chronic diseases. Loss of a parent and parental mental disorder both were associated with five of the six chronic diseases.
There was a dose-response relationship between the number of childhood adversities experienced and the likelihood of developing a chronic disease in adulthood. Having experienced two of the childhood adversities was strongly linked to five of the six chronic diseases, and having experienced three or more was strongly linked to all six chronic diseases.
Independently, all five early-onset mental disorders were associated with adult onset of the pain disorders of osteoarthritis, chronic spinal pain, and frequent/severe headache. The finding of associations between sexual abuse and chronic pain was especially noteworthy because prospective studies have failed to demonstrate such a link. It may be that the samples in these prospective studies were too young (with a median subject age of younger than 30 years) to demonstrate an association, because in this study of childhood adversities and spinal pain the link did not emerge until approximately age 40 years, Dr. Scott and her colleagues said.
Early-onset depression, PTSD, and panic disorder all predicted the later development of heart disease and asthma, and early-onset social phobia predicted later heart disease.
These findings should be considered exploratory in nature because this study was observational. Other limitations include dependence upon subjects’ self-report of medical and psychiatric diagnoses, although these correlated well with physician and medical records, as well as their recall of childhood events, the researchers added.
They noted that although the magnitude of risk "was generally modest" between childhood adversity or early-onset psychological disorders on the one hand and adult-onset chronic disease on the other, "many estimates are of a similar magnitude to the association between serum cholesterol and heart disease. The public health significance of the latter has less to do with its magnitude than with the prevalence of elevated serum cholesterol levels in the general population, and the same argument can be made for the risk factors of childhood adversities and depressive and anxiety disorders."
This study was funded principally by the U.S. National Institute of Mental Health; the MacArthur Foundation; the Pfizer Foundation; the U.S. Public Health Service; the Fogarty International Center; the Pan American Health Organization; the drug companies Eli Lilly, Ortho-McNeil Pharmaceuticals, GlaxoSmithKline, and Bristol-Myers Squibb; the European Commission; the Japan Ministry of Health, Labour, and Welfare; and various organizations within each of the 10 countries included in the survey. The investigators reported ties to numerous industry sources.
FROM ARCHIVES OF GENERAL PSYCHIATRY
Major Finding: Childhood adversities including physical abuse, sexual abuse, neglect, parental death, family violence, and poverty were strongly predictive of six adult-onset chronic illnesses: heart disease, asthma, diabetes, osteoarthritis, chronic spinal pain, and frequent or severe headache. Early-onset anxiety disorder, panic disorder and/or agoraphobia, PTSD, social phobia, and major depressive disorder also were independently associated with the same six chronic diseases in adulthood.
Data Source: A cross-sectional observational study based on surveys of 18,303 adults in 10 countries.
Disclosures: This study was funded principally by the U.S. National Institute of Mental Health; the MacArthur Foundation; the Pfizer Foundation; the U.S. Public Health Service; the Fogarty International Center; the Pan American Health Organization; the drug companies Eli Lilly, Ortho-McNeil Pharmaceuticals, GlaxoSmithKline, and Bristol-Myers Squibb; the European Commission; the Japan Ministry of Health, Labour, and Welfare; and various organizations within each of the 10 countries included in the survey. The investigators reported ties to numerous industry sources.