User login
Breastfeeding linked to less obesity in Asian children
Japanese children who were breastfed for at least 6 months had a significantly lower risk of overweight and obesity at ages 7 and 8 years than did those who were formula fed, according to an analysis of more than 60,000 children that was reported online August 12 in JAMA Pediatrics.
This association was strongest for obesity. In particular, exclusive breastfeeding for at least 6 months was associated with a 45% decreased risk of childhood obesity and a 15% decreased risk of childhood overweight, said Michiyo Yamakawa of the department of epidemiology, Okayama (Japan) University, and her associates.
Many previous studies have shown that breastfeeding exerts a protective effect against childhood obesity, with most reporting a 15%-20% reduction in risk. But a few recent studies, including the only other study to assess this relationship in an Asian population, concluded that there was no protective effect and that findings to the contrary most likely reflect confounding by other factors associated with breastfeeding, such as socioeconomic status, dietary habits, physical activity levels, and such maternal factors as smoking status.
Ms. Yamakawa and her colleagues examined this issue using a large, nationwide database that allowed for control of many important confounders. The ongoing Longitudinal Survey of Babies in the 21st Century has collected reports from parents on family circumstances, child-rearing practices, and children’s health and development throughout Japan since 2001 (JAMA Pediatr. 2013 [doi:10.1001/jamapediatrics.2013.2230]).
For this study, the researchers focused on 29,907 7-year-old and 30,780 8-year-old children whose families participated in the surveys when the children were 6 months of age. All the study subjects were singleton infants born at term.
The data allowed the investigators to calculate the children’s current body mass index, and also included their television viewing time; their computer game–playing time; the parents’ knowledge of nutritional matters; and maternal educational attainment, smoking status, and employment status.
More than 20% of this study population had been exclusively breastfed for at least 6 months, and more than 70% had been partially breastfed for that length of time. Only 5%-6% of the children had been exclusively formula-fed. Japanese society strongly promotes breastfeeding, which may account for the difference in prevalence between this study population and typical Western populations, they noted.
In the 7-year-old group, 7.3% were overweight and 2.1% were obese. The prevalence of both of overweight and obesity decreased as the duration of breastfeeding increased, showing a dose-response relationship.
After the data were adjusted to account for several confounders, the protective effect of breastfeeding against overweight and obesity still remained significant.
The results were similar in the 8-year-old group, in which 7.8% were overweight and 1.9% were obese. Here again the prevalence of both conditions decreased as the duration of breastfeeding increased, and the association remained significant even after adjustment for several confounders.
This study was supported by grants from the Japanese Ministry of Health, Labour, and Welfare, and the Sumitomo Foundation. No financial conflicts of interest were reported.
The work by Yamakawa et al. is "a novel and helpful addition to the literature," because it is one of the first studies to explore the relationship between breastfeeding and obesity in an Asian population, said Marit L. Bovbjerg, Ph.D., Dr. Carolina Amador, and Adrienne E. Uphoff.
This also may be the first true population-based study of the issue, with a cohort comprising all children born in Japan during 2 distinct weeks in 2001, and with 88% of parents participating in the survey. So it is reassuring that this study found what many previous studies have reported: Breastfeeding is protective against childhood overweight and obesity, they said.
Dr. Bovbjerg is at the College of Public Health and Human Sciences at Oregon State University, Corvallis. Dr. Amador is at Community Health Centers of Benton and Linn Counties, Corvallis, Ore. Ms. Uphoff is at Skyline Lactation Care in Charlottesville, Va., and Virginia Commonwealth University, Richmond. These remarks were taken from their editorial accompanying Ms. Yamakawa’s report (JAMA Pediatr. 2013 [doi:10.1001/jamapediatrics.2013.2854]).
The work by Yamakawa et al. is "a novel and helpful addition to the literature," because it is one of the first studies to explore the relationship between breastfeeding and obesity in an Asian population, said Marit L. Bovbjerg, Ph.D., Dr. Carolina Amador, and Adrienne E. Uphoff.
This also may be the first true population-based study of the issue, with a cohort comprising all children born in Japan during 2 distinct weeks in 2001, and with 88% of parents participating in the survey. So it is reassuring that this study found what many previous studies have reported: Breastfeeding is protective against childhood overweight and obesity, they said.
Dr. Bovbjerg is at the College of Public Health and Human Sciences at Oregon State University, Corvallis. Dr. Amador is at Community Health Centers of Benton and Linn Counties, Corvallis, Ore. Ms. Uphoff is at Skyline Lactation Care in Charlottesville, Va., and Virginia Commonwealth University, Richmond. These remarks were taken from their editorial accompanying Ms. Yamakawa’s report (JAMA Pediatr. 2013 [doi:10.1001/jamapediatrics.2013.2854]).
The work by Yamakawa et al. is "a novel and helpful addition to the literature," because it is one of the first studies to explore the relationship between breastfeeding and obesity in an Asian population, said Marit L. Bovbjerg, Ph.D., Dr. Carolina Amador, and Adrienne E. Uphoff.
This also may be the first true population-based study of the issue, with a cohort comprising all children born in Japan during 2 distinct weeks in 2001, and with 88% of parents participating in the survey. So it is reassuring that this study found what many previous studies have reported: Breastfeeding is protective against childhood overweight and obesity, they said.
Dr. Bovbjerg is at the College of Public Health and Human Sciences at Oregon State University, Corvallis. Dr. Amador is at Community Health Centers of Benton and Linn Counties, Corvallis, Ore. Ms. Uphoff is at Skyline Lactation Care in Charlottesville, Va., and Virginia Commonwealth University, Richmond. These remarks were taken from their editorial accompanying Ms. Yamakawa’s report (JAMA Pediatr. 2013 [doi:10.1001/jamapediatrics.2013.2854]).
Japanese children who were breastfed for at least 6 months had a significantly lower risk of overweight and obesity at ages 7 and 8 years than did those who were formula fed, according to an analysis of more than 60,000 children that was reported online August 12 in JAMA Pediatrics.
This association was strongest for obesity. In particular, exclusive breastfeeding for at least 6 months was associated with a 45% decreased risk of childhood obesity and a 15% decreased risk of childhood overweight, said Michiyo Yamakawa of the department of epidemiology, Okayama (Japan) University, and her associates.
Many previous studies have shown that breastfeeding exerts a protective effect against childhood obesity, with most reporting a 15%-20% reduction in risk. But a few recent studies, including the only other study to assess this relationship in an Asian population, concluded that there was no protective effect and that findings to the contrary most likely reflect confounding by other factors associated with breastfeeding, such as socioeconomic status, dietary habits, physical activity levels, and such maternal factors as smoking status.
Ms. Yamakawa and her colleagues examined this issue using a large, nationwide database that allowed for control of many important confounders. The ongoing Longitudinal Survey of Babies in the 21st Century has collected reports from parents on family circumstances, child-rearing practices, and children’s health and development throughout Japan since 2001 (JAMA Pediatr. 2013 [doi:10.1001/jamapediatrics.2013.2230]).
For this study, the researchers focused on 29,907 7-year-old and 30,780 8-year-old children whose families participated in the surveys when the children were 6 months of age. All the study subjects were singleton infants born at term.
The data allowed the investigators to calculate the children’s current body mass index, and also included their television viewing time; their computer game–playing time; the parents’ knowledge of nutritional matters; and maternal educational attainment, smoking status, and employment status.
More than 20% of this study population had been exclusively breastfed for at least 6 months, and more than 70% had been partially breastfed for that length of time. Only 5%-6% of the children had been exclusively formula-fed. Japanese society strongly promotes breastfeeding, which may account for the difference in prevalence between this study population and typical Western populations, they noted.
In the 7-year-old group, 7.3% were overweight and 2.1% were obese. The prevalence of both of overweight and obesity decreased as the duration of breastfeeding increased, showing a dose-response relationship.
After the data were adjusted to account for several confounders, the protective effect of breastfeeding against overweight and obesity still remained significant.
The results were similar in the 8-year-old group, in which 7.8% were overweight and 1.9% were obese. Here again the prevalence of both conditions decreased as the duration of breastfeeding increased, and the association remained significant even after adjustment for several confounders.
This study was supported by grants from the Japanese Ministry of Health, Labour, and Welfare, and the Sumitomo Foundation. No financial conflicts of interest were reported.
Japanese children who were breastfed for at least 6 months had a significantly lower risk of overweight and obesity at ages 7 and 8 years than did those who were formula fed, according to an analysis of more than 60,000 children that was reported online August 12 in JAMA Pediatrics.
This association was strongest for obesity. In particular, exclusive breastfeeding for at least 6 months was associated with a 45% decreased risk of childhood obesity and a 15% decreased risk of childhood overweight, said Michiyo Yamakawa of the department of epidemiology, Okayama (Japan) University, and her associates.
Many previous studies have shown that breastfeeding exerts a protective effect against childhood obesity, with most reporting a 15%-20% reduction in risk. But a few recent studies, including the only other study to assess this relationship in an Asian population, concluded that there was no protective effect and that findings to the contrary most likely reflect confounding by other factors associated with breastfeeding, such as socioeconomic status, dietary habits, physical activity levels, and such maternal factors as smoking status.
Ms. Yamakawa and her colleagues examined this issue using a large, nationwide database that allowed for control of many important confounders. The ongoing Longitudinal Survey of Babies in the 21st Century has collected reports from parents on family circumstances, child-rearing practices, and children’s health and development throughout Japan since 2001 (JAMA Pediatr. 2013 [doi:10.1001/jamapediatrics.2013.2230]).
For this study, the researchers focused on 29,907 7-year-old and 30,780 8-year-old children whose families participated in the surveys when the children were 6 months of age. All the study subjects were singleton infants born at term.
The data allowed the investigators to calculate the children’s current body mass index, and also included their television viewing time; their computer game–playing time; the parents’ knowledge of nutritional matters; and maternal educational attainment, smoking status, and employment status.
More than 20% of this study population had been exclusively breastfed for at least 6 months, and more than 70% had been partially breastfed for that length of time. Only 5%-6% of the children had been exclusively formula-fed. Japanese society strongly promotes breastfeeding, which may account for the difference in prevalence between this study population and typical Western populations, they noted.
In the 7-year-old group, 7.3% were overweight and 2.1% were obese. The prevalence of both of overweight and obesity decreased as the duration of breastfeeding increased, showing a dose-response relationship.
After the data were adjusted to account for several confounders, the protective effect of breastfeeding against overweight and obesity still remained significant.
The results were similar in the 8-year-old group, in which 7.8% were overweight and 1.9% were obese. Here again the prevalence of both conditions decreased as the duration of breastfeeding increased, and the association remained significant even after adjustment for several confounders.
This study was supported by grants from the Japanese Ministry of Health, Labour, and Welfare, and the Sumitomo Foundation. No financial conflicts of interest were reported.
FROM JAMA PEDIATRICS
Major finding: The prevalence of overweight and obesity in 7- and 8-year-old Japanese children declined with increasing duration of breastfeeding during infancy.
Data source: A secondary analysis of data from an ongoing nationwide longitudinal study of child health in Japan, involving 29,907 7-year-olds and 30,780 8-year-olds who had been exclusively breastfed (20%), partially breastfed (70%), or exclusively formula-fed (6%) in infancy.
Disclosures: This study was supported by grants from the Japanese Ministry of Health, Labour, and Welfare and the Sumitomo Foundation. No financial conflicts of interest were reported.
Labor induction, augmentation may be tied to autism risk
Children born after induced or augmented labor appear to be at higher risk of autism than were those born after nonaugmented labor, according to a report published online August 12 in JAMA Pediatrics.
This association, discovered in a statewide population-based epidemiologic study involving over 625,000 live births, was stronger among boys than girls. It persisted after the data were adjusted to account for known risk factors for autism including fetal distress, meconium staining, preterm delivery, and maternal diabetes, which indicates that the association is robust.
"This study also confirmed previously documented risk factors for autism such as advanced maternal age and maternal education, parity, and singleton birth," further reinforcing the strength of the data, said Simon G. Gregory, Ph.D., of the Duke Center for Human Genetics, Durham N.C., and his associates.
They cautioned that "our results are not sufficient to suggest altering the standard of care regarding induction or augmentation," both of which are known to reduce neonatal mortality; risks for neonatal ventilation, sepsis, and ICU admission; the incidence of meconium aspiration syndrome; rates of cesarean delivery; and maternal mortality. However, the findings do suggest that further research of this issue is warranted, the investigators said.
"...Our results are not sufficient to suggest altering the standard of care regarding induction or augmentation."
"It remains unclear whether (1) the act of labor induction/augmentation itself or the medications used underlie the association; (2) the medical and obstetric conditions that are associated with labor induction/augmentation drive the association; or (3) acute intrapartum events that are more common among women with labor induction/augmentation drive the association with autism," the researchers wrote.
Dr. Gregory and his colleagues used data from a state birth registry to identify the records of 625,042 live births in North Carolina during 1990-1998, which included information on maternal characteristics, labor, delivery, and neonatal factors. They linked these data with school records 7-18 years later that identified 5,648 children diagnosed as having autism.
The rates of autism in the study population were 1.3% among boys and 0.4% among girls, which are consistent with rates reported in the literature for other populations. In particular, the approximately fourfold higher incidence of the disorder among boys has been well documented in other populations.
In an initial analysis of the data, the percentage of induced and/or augmented labors was significantly higher among autistic children than among those without autism.
In addition, children with autism were more likely to have experienced fetal distress and to have had meconium staining of the amniotic fluid. The researchers intended to assess whether placental abruption and cord prolapse were associated with autism, but the small number of cases, particularly among baby girls, precluded any such analysis.
In the next data analysis, children born of mothers who had induced or augmented labor had 23% higher odds of being diagnosed as having autism than were those whose mothers did not have labor induction or augmentation. The odds ratios (OR) were 1.10 for induced labor and 1.15 for augmented labor.
A further analysis adjusted for numerous potential confounders related to socioeconomic status, maternal health, and pregnancy-related events. The odds ratios remained essentially unchanged.
An analysis that included the year of the child’s birth shifted the ORs slightly, so that "compared with the reference group, a child whose mother was both induced and augmented at delivery had 27% higher odds of being diagnosed as having autism. The ORs for the induced-only and augmented-only categories indicated an approximate 13% to 16% increase in the odds of autism, respectively," Dr. Gregory and his associates said (JAMA Pediatr. 2013 [doi:10.1001/jamapediatrics.2013.2904]).
In this analysis of the data, fetal distress raised the odds of an autism diagnosis 25%, and meconium staining raised the odds 22%. Compared with term birth, very preterm birth raised the odds 25%, and compared with no maternal diabetes, maternal diabetes raised the odds 23%. Other factors that elevated the odds of an autism diagnosis to a lesser degree included black race/ethnicity, primiparity, older maternal age, and higher maternal education level.
When the data were categorized by the child’s sex, the relationship between induction and/or augmentation and autism was found to be much stronger in boys. "Male children born to mothers who received both induction and augmentation had a 35% higher odds of autism diagnosis than the reference group," the investigators said.
These findings did not change appreciably in two sensitivity analyses.
Although this study was not designed to examine possible reasons for the association between induced/augmented labor and autism, the researchers noted that exposure to exogenous oxytocin (the usual means of inducing and augmenting labor) may contribute to the association. "Biologically, oxytocin signaling plays important prosocial roles influencing social behavior and cognitive function, and displays sexually dimorphic roles in brain function and development," they noted.
Exposure to endogenous oxytocin during labor also may affect as yet unidentified genetic factors. For example, they recently found that the promoter region of the oxytocin receptor gene exhibits differential methylation in autistic than in control populations, Dr. Gregory and his associates said.
"Our results suggest the need for further research focusing on the association of labor induction/ augmentation with autism..."
This study was limited in that the birth registry didn’t include data concerning all the possible factors that could influence neonatal neurologic injury; it was missing information such as prenatal and intrapartum medication exposures and certain labor abnormalities, they noted.
In addition, the school data didn’t provide details about "where a child lay on the autism spectrum," so "the estimated associations represent an average effect over varying degrees of autism presentation."
"In conclusion ... our results suggest the need for further research focusing on the association of labor induction/augmentation with autism," the investigators said.
This study was funded in part by the U.S. Environmental Protection Agency. No financial conflicts of interest were reported.
Children born after induced or augmented labor appear to be at higher risk of autism than were those born after nonaugmented labor, according to a report published online August 12 in JAMA Pediatrics.
This association, discovered in a statewide population-based epidemiologic study involving over 625,000 live births, was stronger among boys than girls. It persisted after the data were adjusted to account for known risk factors for autism including fetal distress, meconium staining, preterm delivery, and maternal diabetes, which indicates that the association is robust.
"This study also confirmed previously documented risk factors for autism such as advanced maternal age and maternal education, parity, and singleton birth," further reinforcing the strength of the data, said Simon G. Gregory, Ph.D., of the Duke Center for Human Genetics, Durham N.C., and his associates.
They cautioned that "our results are not sufficient to suggest altering the standard of care regarding induction or augmentation," both of which are known to reduce neonatal mortality; risks for neonatal ventilation, sepsis, and ICU admission; the incidence of meconium aspiration syndrome; rates of cesarean delivery; and maternal mortality. However, the findings do suggest that further research of this issue is warranted, the investigators said.
"...Our results are not sufficient to suggest altering the standard of care regarding induction or augmentation."
"It remains unclear whether (1) the act of labor induction/augmentation itself or the medications used underlie the association; (2) the medical and obstetric conditions that are associated with labor induction/augmentation drive the association; or (3) acute intrapartum events that are more common among women with labor induction/augmentation drive the association with autism," the researchers wrote.
Dr. Gregory and his colleagues used data from a state birth registry to identify the records of 625,042 live births in North Carolina during 1990-1998, which included information on maternal characteristics, labor, delivery, and neonatal factors. They linked these data with school records 7-18 years later that identified 5,648 children diagnosed as having autism.
The rates of autism in the study population were 1.3% among boys and 0.4% among girls, which are consistent with rates reported in the literature for other populations. In particular, the approximately fourfold higher incidence of the disorder among boys has been well documented in other populations.
In an initial analysis of the data, the percentage of induced and/or augmented labors was significantly higher among autistic children than among those without autism.
In addition, children with autism were more likely to have experienced fetal distress and to have had meconium staining of the amniotic fluid. The researchers intended to assess whether placental abruption and cord prolapse were associated with autism, but the small number of cases, particularly among baby girls, precluded any such analysis.
In the next data analysis, children born of mothers who had induced or augmented labor had 23% higher odds of being diagnosed as having autism than were those whose mothers did not have labor induction or augmentation. The odds ratios (OR) were 1.10 for induced labor and 1.15 for augmented labor.
A further analysis adjusted for numerous potential confounders related to socioeconomic status, maternal health, and pregnancy-related events. The odds ratios remained essentially unchanged.
An analysis that included the year of the child’s birth shifted the ORs slightly, so that "compared with the reference group, a child whose mother was both induced and augmented at delivery had 27% higher odds of being diagnosed as having autism. The ORs for the induced-only and augmented-only categories indicated an approximate 13% to 16% increase in the odds of autism, respectively," Dr. Gregory and his associates said (JAMA Pediatr. 2013 [doi:10.1001/jamapediatrics.2013.2904]).
In this analysis of the data, fetal distress raised the odds of an autism diagnosis 25%, and meconium staining raised the odds 22%. Compared with term birth, very preterm birth raised the odds 25%, and compared with no maternal diabetes, maternal diabetes raised the odds 23%. Other factors that elevated the odds of an autism diagnosis to a lesser degree included black race/ethnicity, primiparity, older maternal age, and higher maternal education level.
When the data were categorized by the child’s sex, the relationship between induction and/or augmentation and autism was found to be much stronger in boys. "Male children born to mothers who received both induction and augmentation had a 35% higher odds of autism diagnosis than the reference group," the investigators said.
These findings did not change appreciably in two sensitivity analyses.
Although this study was not designed to examine possible reasons for the association between induced/augmented labor and autism, the researchers noted that exposure to exogenous oxytocin (the usual means of inducing and augmenting labor) may contribute to the association. "Biologically, oxytocin signaling plays important prosocial roles influencing social behavior and cognitive function, and displays sexually dimorphic roles in brain function and development," they noted.
Exposure to endogenous oxytocin during labor also may affect as yet unidentified genetic factors. For example, they recently found that the promoter region of the oxytocin receptor gene exhibits differential methylation in autistic than in control populations, Dr. Gregory and his associates said.
"Our results suggest the need for further research focusing on the association of labor induction/ augmentation with autism..."
This study was limited in that the birth registry didn’t include data concerning all the possible factors that could influence neonatal neurologic injury; it was missing information such as prenatal and intrapartum medication exposures and certain labor abnormalities, they noted.
In addition, the school data didn’t provide details about "where a child lay on the autism spectrum," so "the estimated associations represent an average effect over varying degrees of autism presentation."
"In conclusion ... our results suggest the need for further research focusing on the association of labor induction/augmentation with autism," the investigators said.
This study was funded in part by the U.S. Environmental Protection Agency. No financial conflicts of interest were reported.
Children born after induced or augmented labor appear to be at higher risk of autism than were those born after nonaugmented labor, according to a report published online August 12 in JAMA Pediatrics.
This association, discovered in a statewide population-based epidemiologic study involving over 625,000 live births, was stronger among boys than girls. It persisted after the data were adjusted to account for known risk factors for autism including fetal distress, meconium staining, preterm delivery, and maternal diabetes, which indicates that the association is robust.
"This study also confirmed previously documented risk factors for autism such as advanced maternal age and maternal education, parity, and singleton birth," further reinforcing the strength of the data, said Simon G. Gregory, Ph.D., of the Duke Center for Human Genetics, Durham N.C., and his associates.
They cautioned that "our results are not sufficient to suggest altering the standard of care regarding induction or augmentation," both of which are known to reduce neonatal mortality; risks for neonatal ventilation, sepsis, and ICU admission; the incidence of meconium aspiration syndrome; rates of cesarean delivery; and maternal mortality. However, the findings do suggest that further research of this issue is warranted, the investigators said.
"...Our results are not sufficient to suggest altering the standard of care regarding induction or augmentation."
"It remains unclear whether (1) the act of labor induction/augmentation itself or the medications used underlie the association; (2) the medical and obstetric conditions that are associated with labor induction/augmentation drive the association; or (3) acute intrapartum events that are more common among women with labor induction/augmentation drive the association with autism," the researchers wrote.
Dr. Gregory and his colleagues used data from a state birth registry to identify the records of 625,042 live births in North Carolina during 1990-1998, which included information on maternal characteristics, labor, delivery, and neonatal factors. They linked these data with school records 7-18 years later that identified 5,648 children diagnosed as having autism.
The rates of autism in the study population were 1.3% among boys and 0.4% among girls, which are consistent with rates reported in the literature for other populations. In particular, the approximately fourfold higher incidence of the disorder among boys has been well documented in other populations.
In an initial analysis of the data, the percentage of induced and/or augmented labors was significantly higher among autistic children than among those without autism.
In addition, children with autism were more likely to have experienced fetal distress and to have had meconium staining of the amniotic fluid. The researchers intended to assess whether placental abruption and cord prolapse were associated with autism, but the small number of cases, particularly among baby girls, precluded any such analysis.
In the next data analysis, children born of mothers who had induced or augmented labor had 23% higher odds of being diagnosed as having autism than were those whose mothers did not have labor induction or augmentation. The odds ratios (OR) were 1.10 for induced labor and 1.15 for augmented labor.
A further analysis adjusted for numerous potential confounders related to socioeconomic status, maternal health, and pregnancy-related events. The odds ratios remained essentially unchanged.
An analysis that included the year of the child’s birth shifted the ORs slightly, so that "compared with the reference group, a child whose mother was both induced and augmented at delivery had 27% higher odds of being diagnosed as having autism. The ORs for the induced-only and augmented-only categories indicated an approximate 13% to 16% increase in the odds of autism, respectively," Dr. Gregory and his associates said (JAMA Pediatr. 2013 [doi:10.1001/jamapediatrics.2013.2904]).
In this analysis of the data, fetal distress raised the odds of an autism diagnosis 25%, and meconium staining raised the odds 22%. Compared with term birth, very preterm birth raised the odds 25%, and compared with no maternal diabetes, maternal diabetes raised the odds 23%. Other factors that elevated the odds of an autism diagnosis to a lesser degree included black race/ethnicity, primiparity, older maternal age, and higher maternal education level.
When the data were categorized by the child’s sex, the relationship between induction and/or augmentation and autism was found to be much stronger in boys. "Male children born to mothers who received both induction and augmentation had a 35% higher odds of autism diagnosis than the reference group," the investigators said.
These findings did not change appreciably in two sensitivity analyses.
Although this study was not designed to examine possible reasons for the association between induced/augmented labor and autism, the researchers noted that exposure to exogenous oxytocin (the usual means of inducing and augmenting labor) may contribute to the association. "Biologically, oxytocin signaling plays important prosocial roles influencing social behavior and cognitive function, and displays sexually dimorphic roles in brain function and development," they noted.
Exposure to endogenous oxytocin during labor also may affect as yet unidentified genetic factors. For example, they recently found that the promoter region of the oxytocin receptor gene exhibits differential methylation in autistic than in control populations, Dr. Gregory and his associates said.
"Our results suggest the need for further research focusing on the association of labor induction/ augmentation with autism..."
This study was limited in that the birth registry didn’t include data concerning all the possible factors that could influence neonatal neurologic injury; it was missing information such as prenatal and intrapartum medication exposures and certain labor abnormalities, they noted.
In addition, the school data didn’t provide details about "where a child lay on the autism spectrum," so "the estimated associations represent an average effect over varying degrees of autism presentation."
"In conclusion ... our results suggest the need for further research focusing on the association of labor induction/augmentation with autism," the investigators said.
This study was funded in part by the U.S. Environmental Protection Agency. No financial conflicts of interest were reported.
FROM JAMA PEDIATRICS
Major finding: Children born of mothers who had induced or augmented labor had 23% higher odds of being diagnosed as having autism than were those whose mothers did not have labor induction or augmentation, with ORs of 1.10 for induced labor and 1.15 for augmented labor.
Data source: A population-based epidemiologic study involving 625,042 live births in which 5,648 children were diagnosed as having autism.
Disclosures: This study was funded in part by the U.S. Environmental Protection Agency. No financial conflicts of interest were reported.
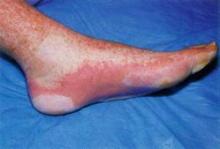
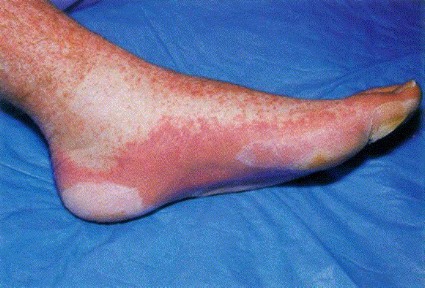
New biomarker predicts treatment-resistant GVHD
Elevated plasma levels of the biomarker ST2, measured 2 weeks after allogeneic hematopoietic stem-cell transplantation, predicted which patients who develop graft-vs.-host disease are unlikely to respond to treatment and are thus at high risk of death within 6 months, according to a report published online Aug. 8 in the New England Journal of Medicine.
Approximately half of allogeneic stem-cell transplant recipients develop acute GVHD, and those who don’t respond to high-dose systemic glucocorticoids within 1 month are at high risk of dying within 6 months without relapse of the primary disease for which the transplant was performed. At present, it is difficult to predict which patients will not respond to glucocorticoids.
Adding a patient’s ST2 (suppression of tumorigenicity 2) level to the clinical grade and the target-organ stage of GVHD significantly improves risk prediction, particularly in the important subgroup of patients who have lower-GI GVHD, said Dr. Mark T. Vander Lugt of the department of pediatrics, University of Michigan, Ann Arbor, and his associates.
"The improved risk stratification of patients with GVHD with the use of ST2 may permit early evaluation of additional therapies, before the development of resistant disease," they wrote (N. Engl. J. Med. 2013 Aug. 8;369:529-39 [doi:10.1056/NEJMoa1213299]).
This early identification may also "permit more stringent monitoring and preemptive interventions."
ST2, a recently discovered member of the interleukin-1 receptor family, is expressed on hematopoietic cells that play a role in diseases mediated by type-2 helper T cells and is also secreted by endothelial cells, epithelial cells, and fibroblasts in response to inflammatory stimuli.
Dr. Vander Lugt and his colleagues assessed numerous candidate plasma biomarkers to determine which, if any, showed the strongest association with nonresponse to GVHD therapy and could thus be used as risk predictors.
They began by testing plasma samples collected 16 days after transplantation from 10 patients who went on to have a complete response to GVHD therapy and 10 who went on to have progressive GVHD. They identified and quantified 571 proteins in these samples, and found that 197 of them were overexpressed by a factor of at least 1.5 in the patients with progressive GVHD. Twelve of these proteins, in addition to ST2, could be measured using commercially available antibodies suitable for ELISA.
ST2 was the single most accurate biomarker at discriminating between plasma samples from patients who responded to GVHD therapy and plasma samples from patients who did not. The six other best biomarkers were then assessed as a panel and compared against ST2 in samples taken from 381 patients at the onset of GVHD.
The ST2 level was found to be superior to the six-biomarker panel in predicting which patients with GVHD would not respond to glucocorticoids within a month of initiating the treatment, which is an accepted surrogate 6-month mortality. It also was the best predictive biomarker when tested further in three independent cohorts totaling 673 patients, the investigators said.
Patients with high ST2 levels were 2.3 times more likely than those with low ST2 levels to develop treatment-resistant GVHD, and 3.7 times as likely to die within 6 months.
Moreover, "when measured as early as day 14 after transplantation, ST2 concentration was a better predictor of the risk of death than were the other known risk factors, including the age of the recipient, conditioning intensity, donor source, and HLA [human leukocyte antigens] match," Dr. Vander Lugt and his associates wrote.
"We believe that our results may affect the assessment of GVHD risk before the development of GVHD and at the onset of the clinical signs of GVHD; however, a generalizable definition of high risk has yet to be developed and will require larger studies," they added.
The study was supported by grants from the National Institutes of Health. The University of Michigan has licensed a pending patent application for the biomarker test to ViraCor and any revenue will be shared with the inventors at the University of Michigan and the Fred Hutchinson Cancer Research Center, Seattle.
Elevated plasma levels of the biomarker ST2, measured 2 weeks after allogeneic hematopoietic stem-cell transplantation, predicted which patients who develop graft-vs.-host disease are unlikely to respond to treatment and are thus at high risk of death within 6 months, according to a report published online Aug. 8 in the New England Journal of Medicine.
Approximately half of allogeneic stem-cell transplant recipients develop acute GVHD, and those who don’t respond to high-dose systemic glucocorticoids within 1 month are at high risk of dying within 6 months without relapse of the primary disease for which the transplant was performed. At present, it is difficult to predict which patients will not respond to glucocorticoids.
Adding a patient’s ST2 (suppression of tumorigenicity 2) level to the clinical grade and the target-organ stage of GVHD significantly improves risk prediction, particularly in the important subgroup of patients who have lower-GI GVHD, said Dr. Mark T. Vander Lugt of the department of pediatrics, University of Michigan, Ann Arbor, and his associates.
"The improved risk stratification of patients with GVHD with the use of ST2 may permit early evaluation of additional therapies, before the development of resistant disease," they wrote (N. Engl. J. Med. 2013 Aug. 8;369:529-39 [doi:10.1056/NEJMoa1213299]).
This early identification may also "permit more stringent monitoring and preemptive interventions."
ST2, a recently discovered member of the interleukin-1 receptor family, is expressed on hematopoietic cells that play a role in diseases mediated by type-2 helper T cells and is also secreted by endothelial cells, epithelial cells, and fibroblasts in response to inflammatory stimuli.
Dr. Vander Lugt and his colleagues assessed numerous candidate plasma biomarkers to determine which, if any, showed the strongest association with nonresponse to GVHD therapy and could thus be used as risk predictors.
They began by testing plasma samples collected 16 days after transplantation from 10 patients who went on to have a complete response to GVHD therapy and 10 who went on to have progressive GVHD. They identified and quantified 571 proteins in these samples, and found that 197 of them were overexpressed by a factor of at least 1.5 in the patients with progressive GVHD. Twelve of these proteins, in addition to ST2, could be measured using commercially available antibodies suitable for ELISA.
ST2 was the single most accurate biomarker at discriminating between plasma samples from patients who responded to GVHD therapy and plasma samples from patients who did not. The six other best biomarkers were then assessed as a panel and compared against ST2 in samples taken from 381 patients at the onset of GVHD.
The ST2 level was found to be superior to the six-biomarker panel in predicting which patients with GVHD would not respond to glucocorticoids within a month of initiating the treatment, which is an accepted surrogate 6-month mortality. It also was the best predictive biomarker when tested further in three independent cohorts totaling 673 patients, the investigators said.
Patients with high ST2 levels were 2.3 times more likely than those with low ST2 levels to develop treatment-resistant GVHD, and 3.7 times as likely to die within 6 months.
Moreover, "when measured as early as day 14 after transplantation, ST2 concentration was a better predictor of the risk of death than were the other known risk factors, including the age of the recipient, conditioning intensity, donor source, and HLA [human leukocyte antigens] match," Dr. Vander Lugt and his associates wrote.
"We believe that our results may affect the assessment of GVHD risk before the development of GVHD and at the onset of the clinical signs of GVHD; however, a generalizable definition of high risk has yet to be developed and will require larger studies," they added.
The study was supported by grants from the National Institutes of Health. The University of Michigan has licensed a pending patent application for the biomarker test to ViraCor and any revenue will be shared with the inventors at the University of Michigan and the Fred Hutchinson Cancer Research Center, Seattle.
Elevated plasma levels of the biomarker ST2, measured 2 weeks after allogeneic hematopoietic stem-cell transplantation, predicted which patients who develop graft-vs.-host disease are unlikely to respond to treatment and are thus at high risk of death within 6 months, according to a report published online Aug. 8 in the New England Journal of Medicine.
Approximately half of allogeneic stem-cell transplant recipients develop acute GVHD, and those who don’t respond to high-dose systemic glucocorticoids within 1 month are at high risk of dying within 6 months without relapse of the primary disease for which the transplant was performed. At present, it is difficult to predict which patients will not respond to glucocorticoids.
Adding a patient’s ST2 (suppression of tumorigenicity 2) level to the clinical grade and the target-organ stage of GVHD significantly improves risk prediction, particularly in the important subgroup of patients who have lower-GI GVHD, said Dr. Mark T. Vander Lugt of the department of pediatrics, University of Michigan, Ann Arbor, and his associates.
"The improved risk stratification of patients with GVHD with the use of ST2 may permit early evaluation of additional therapies, before the development of resistant disease," they wrote (N. Engl. J. Med. 2013 Aug. 8;369:529-39 [doi:10.1056/NEJMoa1213299]).
This early identification may also "permit more stringent monitoring and preemptive interventions."
ST2, a recently discovered member of the interleukin-1 receptor family, is expressed on hematopoietic cells that play a role in diseases mediated by type-2 helper T cells and is also secreted by endothelial cells, epithelial cells, and fibroblasts in response to inflammatory stimuli.
Dr. Vander Lugt and his colleagues assessed numerous candidate plasma biomarkers to determine which, if any, showed the strongest association with nonresponse to GVHD therapy and could thus be used as risk predictors.
They began by testing plasma samples collected 16 days after transplantation from 10 patients who went on to have a complete response to GVHD therapy and 10 who went on to have progressive GVHD. They identified and quantified 571 proteins in these samples, and found that 197 of them were overexpressed by a factor of at least 1.5 in the patients with progressive GVHD. Twelve of these proteins, in addition to ST2, could be measured using commercially available antibodies suitable for ELISA.
ST2 was the single most accurate biomarker at discriminating between plasma samples from patients who responded to GVHD therapy and plasma samples from patients who did not. The six other best biomarkers were then assessed as a panel and compared against ST2 in samples taken from 381 patients at the onset of GVHD.
The ST2 level was found to be superior to the six-biomarker panel in predicting which patients with GVHD would not respond to glucocorticoids within a month of initiating the treatment, which is an accepted surrogate 6-month mortality. It also was the best predictive biomarker when tested further in three independent cohorts totaling 673 patients, the investigators said.
Patients with high ST2 levels were 2.3 times more likely than those with low ST2 levels to develop treatment-resistant GVHD, and 3.7 times as likely to die within 6 months.
Moreover, "when measured as early as day 14 after transplantation, ST2 concentration was a better predictor of the risk of death than were the other known risk factors, including the age of the recipient, conditioning intensity, donor source, and HLA [human leukocyte antigens] match," Dr. Vander Lugt and his associates wrote.
"We believe that our results may affect the assessment of GVHD risk before the development of GVHD and at the onset of the clinical signs of GVHD; however, a generalizable definition of high risk has yet to be developed and will require larger studies," they added.
The study was supported by grants from the National Institutes of Health. The University of Michigan has licensed a pending patent application for the biomarker test to ViraCor and any revenue will be shared with the inventors at the University of Michigan and the Fred Hutchinson Cancer Research Center, Seattle.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major finding: Patients with high ST2 levels were 2.3 times more likely than those with low ST2 levels to develop treatment-resistant GVHD, and 3.7 times as likely to die within 6 months of transplantation
Data source: A series of laboratory studies comparing ST2 against numerous other candidate proteins as a biomarker for nonresponse to GVHD therapy.
Disclosures: The study was supported by grants from the National Institutes of Health. The University of Michigan has licensed a pending patent application for the biomarker test to ViraCor and any revenue will be shared with the inventors at the University of Michigan and the Fred Hutchinson Cancer Research Center, Seattle.
Higher glucose linked to increased dementia risk
Higher glucose levels were associated with an elevated risk of dementia in a community-based cohort study reported Aug. 8 in the New England Journal of Medicine.
High glucose levels were linked to this adverse effect both in people who had diabetes and in people who did not. "These data suggest that higher levels of glucose may have deleterious effects on the aging brain," said Dr. Paul K. Crane of the University of Washington, Seattle, and his associates.
In addition, "our findings underscore the potential consequences of temporal trends in obesity and diabetes, and suggest the need for interventions that reduce glucose levels," they said.
Dr. Crane and his colleagues analyzed data from a prospective, longitudinal study in which participants were followed every 2 years to identify incident cases of dementia. The study involved 2,067 randomly sampled older men and women who underwent numerous glucose tests as part of their biennial work-ups, beginning in the 1990s.
"The extensive clinical laboratory data available and the long-term follow-up of the cohort, in which there were hundreds of cases of dementia, afforded us the opportunity ... to evaluate risk across the entire spectrum of observed glucose levels."
The researchers described this as the first study among those investigating associations between glucose metabolism and the risk of dementia to evaluate glucose levels as a time-varying phenomenon. They used a hierarchical Bayesian statistical model that allowed them to incorporate multiple measurements taken over the course of several years – including random blood glucose tests, fasting blood glucose tests, and glycated hemoglobin tests – into a single composite estimate of glucose exposure for each study subject.
Each participant underwent an average of 17 measurements of blood glucose and 5 of glycated hemoglobin. This yielded a total of 35,264 values for fasting and random glucose levels and 10,208 values for glycated hemoglobin levels.
"The extensive clinical laboratory data available and the long-term follow-up of the cohort, in which there were hundreds of cases of dementia, afforded us the opportunity ... to evaluate risk across the entire spectrum of observed glucose levels," the investigators noted.
Overall, 524 (25.4%) of the study subjects developed dementia during a median follow-up period of 6.8 years. This included 21.6% of the subjects who had diabetes and 26.1% of those who didn’t have diabetes. Most of the patients with dementia had probable or possible Alzheimer’s disease (403), followed by dementia from vascular disease (55) and dementia from other causes (66).
In the subjects with diabetes, those who had the highest glucose levels were at increased risk of dementia, compared with those who had lower glucose levels. "For an average glucose level of 190 mg/dL [in the preceding 5 years], as compared with 160 mg/dL, the adjusted hazard ratio for dementia was 1.40," Dr. Crane and his associates wrote (N. Engl. J. Med. 2013 Aug. 8 [doi:10.1056/NEJMoa1215740]).
More surprisingly, in the subjects without diabetes, those who had the highest but still normal glucose levels were at increased risk of dementia, compared with those who had lower glucose levels. "For an average glucose level of 115 mg/dL [in the preceding 5 years], as compared with 100 mg/dL, the adjusted hazard ratio for dementia was 1.18," the researchers reported.
These associations remained significant in several sensitivity analyses, regardless of the subjects’ age or sex, and were independent of apolipoprotein E epsilon-4 allele status.
The mechanism(s) by which higher glucose levels may contribute to dementia risk have not yet been elucidated, but both acute and chronic hyperglycemia, insulin resistance, and microvascular disease of the CNS could all play a role, according to the researchers.
This study was supported in part by the National Institutes of Health. Dr. Crane reported no financial conflicts of interest; four other authors reported ties to industry sources.
Higher glucose levels were associated with an elevated risk of dementia in a community-based cohort study reported Aug. 8 in the New England Journal of Medicine.
High glucose levels were linked to this adverse effect both in people who had diabetes and in people who did not. "These data suggest that higher levels of glucose may have deleterious effects on the aging brain," said Dr. Paul K. Crane of the University of Washington, Seattle, and his associates.
In addition, "our findings underscore the potential consequences of temporal trends in obesity and diabetes, and suggest the need for interventions that reduce glucose levels," they said.
Dr. Crane and his colleagues analyzed data from a prospective, longitudinal study in which participants were followed every 2 years to identify incident cases of dementia. The study involved 2,067 randomly sampled older men and women who underwent numerous glucose tests as part of their biennial work-ups, beginning in the 1990s.
"The extensive clinical laboratory data available and the long-term follow-up of the cohort, in which there were hundreds of cases of dementia, afforded us the opportunity ... to evaluate risk across the entire spectrum of observed glucose levels."
The researchers described this as the first study among those investigating associations between glucose metabolism and the risk of dementia to evaluate glucose levels as a time-varying phenomenon. They used a hierarchical Bayesian statistical model that allowed them to incorporate multiple measurements taken over the course of several years – including random blood glucose tests, fasting blood glucose tests, and glycated hemoglobin tests – into a single composite estimate of glucose exposure for each study subject.
Each participant underwent an average of 17 measurements of blood glucose and 5 of glycated hemoglobin. This yielded a total of 35,264 values for fasting and random glucose levels and 10,208 values for glycated hemoglobin levels.
"The extensive clinical laboratory data available and the long-term follow-up of the cohort, in which there were hundreds of cases of dementia, afforded us the opportunity ... to evaluate risk across the entire spectrum of observed glucose levels," the investigators noted.
Overall, 524 (25.4%) of the study subjects developed dementia during a median follow-up period of 6.8 years. This included 21.6% of the subjects who had diabetes and 26.1% of those who didn’t have diabetes. Most of the patients with dementia had probable or possible Alzheimer’s disease (403), followed by dementia from vascular disease (55) and dementia from other causes (66).
In the subjects with diabetes, those who had the highest glucose levels were at increased risk of dementia, compared with those who had lower glucose levels. "For an average glucose level of 190 mg/dL [in the preceding 5 years], as compared with 160 mg/dL, the adjusted hazard ratio for dementia was 1.40," Dr. Crane and his associates wrote (N. Engl. J. Med. 2013 Aug. 8 [doi:10.1056/NEJMoa1215740]).
More surprisingly, in the subjects without diabetes, those who had the highest but still normal glucose levels were at increased risk of dementia, compared with those who had lower glucose levels. "For an average glucose level of 115 mg/dL [in the preceding 5 years], as compared with 100 mg/dL, the adjusted hazard ratio for dementia was 1.18," the researchers reported.
These associations remained significant in several sensitivity analyses, regardless of the subjects’ age or sex, and were independent of apolipoprotein E epsilon-4 allele status.
The mechanism(s) by which higher glucose levels may contribute to dementia risk have not yet been elucidated, but both acute and chronic hyperglycemia, insulin resistance, and microvascular disease of the CNS could all play a role, according to the researchers.
This study was supported in part by the National Institutes of Health. Dr. Crane reported no financial conflicts of interest; four other authors reported ties to industry sources.
Higher glucose levels were associated with an elevated risk of dementia in a community-based cohort study reported Aug. 8 in the New England Journal of Medicine.
High glucose levels were linked to this adverse effect both in people who had diabetes and in people who did not. "These data suggest that higher levels of glucose may have deleterious effects on the aging brain," said Dr. Paul K. Crane of the University of Washington, Seattle, and his associates.
In addition, "our findings underscore the potential consequences of temporal trends in obesity and diabetes, and suggest the need for interventions that reduce glucose levels," they said.
Dr. Crane and his colleagues analyzed data from a prospective, longitudinal study in which participants were followed every 2 years to identify incident cases of dementia. The study involved 2,067 randomly sampled older men and women who underwent numerous glucose tests as part of their biennial work-ups, beginning in the 1990s.
"The extensive clinical laboratory data available and the long-term follow-up of the cohort, in which there were hundreds of cases of dementia, afforded us the opportunity ... to evaluate risk across the entire spectrum of observed glucose levels."
The researchers described this as the first study among those investigating associations between glucose metabolism and the risk of dementia to evaluate glucose levels as a time-varying phenomenon. They used a hierarchical Bayesian statistical model that allowed them to incorporate multiple measurements taken over the course of several years – including random blood glucose tests, fasting blood glucose tests, and glycated hemoglobin tests – into a single composite estimate of glucose exposure for each study subject.
Each participant underwent an average of 17 measurements of blood glucose and 5 of glycated hemoglobin. This yielded a total of 35,264 values for fasting and random glucose levels and 10,208 values for glycated hemoglobin levels.
"The extensive clinical laboratory data available and the long-term follow-up of the cohort, in which there were hundreds of cases of dementia, afforded us the opportunity ... to evaluate risk across the entire spectrum of observed glucose levels," the investigators noted.
Overall, 524 (25.4%) of the study subjects developed dementia during a median follow-up period of 6.8 years. This included 21.6% of the subjects who had diabetes and 26.1% of those who didn’t have diabetes. Most of the patients with dementia had probable or possible Alzheimer’s disease (403), followed by dementia from vascular disease (55) and dementia from other causes (66).
In the subjects with diabetes, those who had the highest glucose levels were at increased risk of dementia, compared with those who had lower glucose levels. "For an average glucose level of 190 mg/dL [in the preceding 5 years], as compared with 160 mg/dL, the adjusted hazard ratio for dementia was 1.40," Dr. Crane and his associates wrote (N. Engl. J. Med. 2013 Aug. 8 [doi:10.1056/NEJMoa1215740]).
More surprisingly, in the subjects without diabetes, those who had the highest but still normal glucose levels were at increased risk of dementia, compared with those who had lower glucose levels. "For an average glucose level of 115 mg/dL [in the preceding 5 years], as compared with 100 mg/dL, the adjusted hazard ratio for dementia was 1.18," the researchers reported.
These associations remained significant in several sensitivity analyses, regardless of the subjects’ age or sex, and were independent of apolipoprotein E epsilon-4 allele status.
The mechanism(s) by which higher glucose levels may contribute to dementia risk have not yet been elucidated, but both acute and chronic hyperglycemia, insulin resistance, and microvascular disease of the CNS could all play a role, according to the researchers.
This study was supported in part by the National Institutes of Health. Dr. Crane reported no financial conflicts of interest; four other authors reported ties to industry sources.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major Finding: The adjusted hazard ratio for dementia was 1.18 in subjects without diabetes with an average glucose level of 115 mg/dL in the preceding 5 years, compared with those with an average level of 100 mg/dL.
Data Source: A secondary analysis of data from a prospective longitudinal cohort study of 2,067 older men and women who underwent 35,264 assessments of random and fasting blood glucose and 10,208 assessments of glycated hemoglobin and who were followed for a mean of 7 years for the development of dementia.
Disclosures: This study was supported in part by the National Institutes of Health. Dr. Crane reported no financial conflicts of interest; four other authors reported ties to industry sources.
Suicide risk in the military similar to that in civilian populations
Among current and former military personnel, the risk of suicide is related to the same mental health disorders found in civilian populations rather than to military experience, a report published online Aug. 6 in JAMA suggests.
In an analysis of data from a large prospective longitudinal cohort of personnel from all branches of the service, increased suicide risk was strongly associated with manic-depressive disorder, now commonly called bipolar disorder; depression; and alcohol-related problems but was not associated with military-specific factors such as combat experiences, long deployments, or multiple deployments, reported Cynthia A. LeardMann of the department of deployment health research, Naval Health Research Center, San Diego, and her associates.
Their findings indicate that the best means of mitigating suicide risk in military personnel are screening for mental and substance use disorders, obtaining an accurate psychiatric history, and recognizing potential suicidal behaviors early, together with providing high-quality mental health treatment, the researchers said.
Suicide rates in the military increased sharply beginning in 2005 and continued to rise each year until leveling off in 2009. Yet, suicide still remains a rare outcome in service personnel.
To examine factors associated with suicide risk in the military, Ms. LeardMann and her colleagues analyzed data from the Millennium Cohort Study, which prospectively records the health impact of military service in a randomly selected sample of service members using periodic surveys. The Millennium Cohort includes a large population of active, reserve, and National Guard members in the Army, Navy/Coast Guard, Marine Corps, and Air Force.
For their study, Ms. LeardMann and her associates assessed the records of 151,560 participants in the Millennium Cohort who were surveyed in 2001 through 2008, the last year for which complete data have been collected. Suicides and other deaths were identified through these records as well as through the National Death Index and the Department of Defense Medical Mortality Registry.
Factors related to deployment that were considered in the analyses included the number of deployments; length of deployments; whether or not the subject had encountered dead or decomposing bodies, witnessed people being killed, discharged a weapon, or felt in great danger of being killed; and whether the subject had witnessed abuse such as torture, beating, or rape. Nonmilitary stressful life events also were considered, such as divorce, severe illness, or death of a close loved one.
During up to 7 years of follow-up – the equivalent of 707,493 person-years of observation – 646 of these subjects died, including 83 (12.8% of total deaths) who died from suicide. The overall crude rate of suicide was 11.73 per 100,000 person-years.
Crude suicide rates were highest among study subjects who had manic-depressive disorder (87.55 per 100,000), alcohol-related problems (27.67 per 100,000), and depression (26.94 per 100,000). Subjects who were currently deployed, whether or not they had combat experience, were no more likely than nondeployed subjects to die from suicide, the investigators reported (JAMA 2013;310:496-506).
In a more refined analysis of the data, suicide risk was again strongly associated with manic-depressive disorder (hazard ratio, 4.35), alcohol-related problems (HR, 2.56), and depression (HR, 1.96), and was not associated with any deployment-related factors.
In an additional nested case-control analysis, suicide risk was independently and strongly associated with manic-depressive disorder (odds ratio, 7.38), depression (OR, 2.68), and alcohol-related problems (OR, 2.30). Again, no association was found between suicide risk and deployment factors.
In a subgroup analysis involving only Army personnel, manic-depressive disorder (HR, 5.96) and alcohol-related problems (HR, 3.86) were significantly associated with suicide risk. Depression was not, but that might have been attributable to inadequate statistical power because there were not enough cases in this subgroup, the investigators said.
These findings "are not consistent with the assumption that specific deployment-related characteristics ... are directly associated with increased suicide risk. Instead, the risk factors associated with suicide in this military population are consistent with civilian populations, including male sex and mental disorders," Ms. LeardMann and her associates said.
"Studies have shown a marked increase in the incidence of diagnosed mental disorders in active-duty service members since 2005, paralleling the incidence of suicide. This suggests that the increased rate of suicide in the military may largely be a product of an increased prevalence of mental disorders in this population, possibly resulting from indirect cumulative occupational stresses across both deployed and home-station environments over years of war," they said.
The researchers noted that their analyses could not capture suicides that occurred since 2008. "It is possible that the cumulative strain of multiple and lengthy deployments only began to be reflected in suicide rates toward the later stages of the conflicts [in Iran and Afghanistan]," and thus could not be accounted for in this study.
"However, the study did include the 3 years with the sharpest statistically significant increases in suicides." And the overall evidence clearly "points to the lack of any specific deployment-related effects," they noted.
This study was limited in that all the findings are based on only 83 suicide deaths, so it "may have lacked statistical power to produce a stable and reproducible multivariable model," Ms. LeardMann and her associates added.
This study was supported by the Department of Defense. Ms. LeardMann reported no financial conflicts of interest; one of her associates reported receiving a lecture fee from Merck.

|
|
Military suicides are sometimes characterized as an epidemic, and many assume that the rate is escalating out of control because of prolonged combat deployments and their associated stresses, said Dr. Charles C. Engel.
But suicide within the military remains rare, despite the worrisome increase that has occurred in recent years. This trend should be viewed in context: A similar increase in suicides has been reported in the general U.S. population during the same time period, and has been linked to declines in the economy and escalating unemployment.
The findings of LeardMann et al. are reassuring in that they identify three leading causes of military suicide – mood disorders and alcohol misuse – for which effective treatments exist, he said.
Charles C. Engel, M.D., is with the department of psychiatry at the Uniformed Services University of the Health Sciences, Bethesda, Md. He reported no financial conflicts of interest. These remarks were taken from his editorial accompanying Ms. LeardMann’s report (JAMA 2013:310:484-5).

|
|
Military suicides are sometimes characterized as an epidemic, and many assume that the rate is escalating out of control because of prolonged combat deployments and their associated stresses, said Dr. Charles C. Engel.
But suicide within the military remains rare, despite the worrisome increase that has occurred in recent years. This trend should be viewed in context: A similar increase in suicides has been reported in the general U.S. population during the same time period, and has been linked to declines in the economy and escalating unemployment.
The findings of LeardMann et al. are reassuring in that they identify three leading causes of military suicide – mood disorders and alcohol misuse – for which effective treatments exist, he said.
Charles C. Engel, M.D., is with the department of psychiatry at the Uniformed Services University of the Health Sciences, Bethesda, Md. He reported no financial conflicts of interest. These remarks were taken from his editorial accompanying Ms. LeardMann’s report (JAMA 2013:310:484-5).

|
|
Military suicides are sometimes characterized as an epidemic, and many assume that the rate is escalating out of control because of prolonged combat deployments and their associated stresses, said Dr. Charles C. Engel.
But suicide within the military remains rare, despite the worrisome increase that has occurred in recent years. This trend should be viewed in context: A similar increase in suicides has been reported in the general U.S. population during the same time period, and has been linked to declines in the economy and escalating unemployment.
The findings of LeardMann et al. are reassuring in that they identify three leading causes of military suicide – mood disorders and alcohol misuse – for which effective treatments exist, he said.
Charles C. Engel, M.D., is with the department of psychiatry at the Uniformed Services University of the Health Sciences, Bethesda, Md. He reported no financial conflicts of interest. These remarks were taken from his editorial accompanying Ms. LeardMann’s report (JAMA 2013:310:484-5).
Among current and former military personnel, the risk of suicide is related to the same mental health disorders found in civilian populations rather than to military experience, a report published online Aug. 6 in JAMA suggests.
In an analysis of data from a large prospective longitudinal cohort of personnel from all branches of the service, increased suicide risk was strongly associated with manic-depressive disorder, now commonly called bipolar disorder; depression; and alcohol-related problems but was not associated with military-specific factors such as combat experiences, long deployments, or multiple deployments, reported Cynthia A. LeardMann of the department of deployment health research, Naval Health Research Center, San Diego, and her associates.
Their findings indicate that the best means of mitigating suicide risk in military personnel are screening for mental and substance use disorders, obtaining an accurate psychiatric history, and recognizing potential suicidal behaviors early, together with providing high-quality mental health treatment, the researchers said.
Suicide rates in the military increased sharply beginning in 2005 and continued to rise each year until leveling off in 2009. Yet, suicide still remains a rare outcome in service personnel.
To examine factors associated with suicide risk in the military, Ms. LeardMann and her colleagues analyzed data from the Millennium Cohort Study, which prospectively records the health impact of military service in a randomly selected sample of service members using periodic surveys. The Millennium Cohort includes a large population of active, reserve, and National Guard members in the Army, Navy/Coast Guard, Marine Corps, and Air Force.
For their study, Ms. LeardMann and her associates assessed the records of 151,560 participants in the Millennium Cohort who were surveyed in 2001 through 2008, the last year for which complete data have been collected. Suicides and other deaths were identified through these records as well as through the National Death Index and the Department of Defense Medical Mortality Registry.
Factors related to deployment that were considered in the analyses included the number of deployments; length of deployments; whether or not the subject had encountered dead or decomposing bodies, witnessed people being killed, discharged a weapon, or felt in great danger of being killed; and whether the subject had witnessed abuse such as torture, beating, or rape. Nonmilitary stressful life events also were considered, such as divorce, severe illness, or death of a close loved one.
During up to 7 years of follow-up – the equivalent of 707,493 person-years of observation – 646 of these subjects died, including 83 (12.8% of total deaths) who died from suicide. The overall crude rate of suicide was 11.73 per 100,000 person-years.
Crude suicide rates were highest among study subjects who had manic-depressive disorder (87.55 per 100,000), alcohol-related problems (27.67 per 100,000), and depression (26.94 per 100,000). Subjects who were currently deployed, whether or not they had combat experience, were no more likely than nondeployed subjects to die from suicide, the investigators reported (JAMA 2013;310:496-506).
In a more refined analysis of the data, suicide risk was again strongly associated with manic-depressive disorder (hazard ratio, 4.35), alcohol-related problems (HR, 2.56), and depression (HR, 1.96), and was not associated with any deployment-related factors.
In an additional nested case-control analysis, suicide risk was independently and strongly associated with manic-depressive disorder (odds ratio, 7.38), depression (OR, 2.68), and alcohol-related problems (OR, 2.30). Again, no association was found between suicide risk and deployment factors.
In a subgroup analysis involving only Army personnel, manic-depressive disorder (HR, 5.96) and alcohol-related problems (HR, 3.86) were significantly associated with suicide risk. Depression was not, but that might have been attributable to inadequate statistical power because there were not enough cases in this subgroup, the investigators said.
These findings "are not consistent with the assumption that specific deployment-related characteristics ... are directly associated with increased suicide risk. Instead, the risk factors associated with suicide in this military population are consistent with civilian populations, including male sex and mental disorders," Ms. LeardMann and her associates said.
"Studies have shown a marked increase in the incidence of diagnosed mental disorders in active-duty service members since 2005, paralleling the incidence of suicide. This suggests that the increased rate of suicide in the military may largely be a product of an increased prevalence of mental disorders in this population, possibly resulting from indirect cumulative occupational stresses across both deployed and home-station environments over years of war," they said.
The researchers noted that their analyses could not capture suicides that occurred since 2008. "It is possible that the cumulative strain of multiple and lengthy deployments only began to be reflected in suicide rates toward the later stages of the conflicts [in Iran and Afghanistan]," and thus could not be accounted for in this study.
"However, the study did include the 3 years with the sharpest statistically significant increases in suicides." And the overall evidence clearly "points to the lack of any specific deployment-related effects," they noted.
This study was limited in that all the findings are based on only 83 suicide deaths, so it "may have lacked statistical power to produce a stable and reproducible multivariable model," Ms. LeardMann and her associates added.
This study was supported by the Department of Defense. Ms. LeardMann reported no financial conflicts of interest; one of her associates reported receiving a lecture fee from Merck.
Among current and former military personnel, the risk of suicide is related to the same mental health disorders found in civilian populations rather than to military experience, a report published online Aug. 6 in JAMA suggests.
In an analysis of data from a large prospective longitudinal cohort of personnel from all branches of the service, increased suicide risk was strongly associated with manic-depressive disorder, now commonly called bipolar disorder; depression; and alcohol-related problems but was not associated with military-specific factors such as combat experiences, long deployments, or multiple deployments, reported Cynthia A. LeardMann of the department of deployment health research, Naval Health Research Center, San Diego, and her associates.
Their findings indicate that the best means of mitigating suicide risk in military personnel are screening for mental and substance use disorders, obtaining an accurate psychiatric history, and recognizing potential suicidal behaviors early, together with providing high-quality mental health treatment, the researchers said.
Suicide rates in the military increased sharply beginning in 2005 and continued to rise each year until leveling off in 2009. Yet, suicide still remains a rare outcome in service personnel.
To examine factors associated with suicide risk in the military, Ms. LeardMann and her colleagues analyzed data from the Millennium Cohort Study, which prospectively records the health impact of military service in a randomly selected sample of service members using periodic surveys. The Millennium Cohort includes a large population of active, reserve, and National Guard members in the Army, Navy/Coast Guard, Marine Corps, and Air Force.
For their study, Ms. LeardMann and her associates assessed the records of 151,560 participants in the Millennium Cohort who were surveyed in 2001 through 2008, the last year for which complete data have been collected. Suicides and other deaths were identified through these records as well as through the National Death Index and the Department of Defense Medical Mortality Registry.
Factors related to deployment that were considered in the analyses included the number of deployments; length of deployments; whether or not the subject had encountered dead or decomposing bodies, witnessed people being killed, discharged a weapon, or felt in great danger of being killed; and whether the subject had witnessed abuse such as torture, beating, or rape. Nonmilitary stressful life events also were considered, such as divorce, severe illness, or death of a close loved one.
During up to 7 years of follow-up – the equivalent of 707,493 person-years of observation – 646 of these subjects died, including 83 (12.8% of total deaths) who died from suicide. The overall crude rate of suicide was 11.73 per 100,000 person-years.
Crude suicide rates were highest among study subjects who had manic-depressive disorder (87.55 per 100,000), alcohol-related problems (27.67 per 100,000), and depression (26.94 per 100,000). Subjects who were currently deployed, whether or not they had combat experience, were no more likely than nondeployed subjects to die from suicide, the investigators reported (JAMA 2013;310:496-506).
In a more refined analysis of the data, suicide risk was again strongly associated with manic-depressive disorder (hazard ratio, 4.35), alcohol-related problems (HR, 2.56), and depression (HR, 1.96), and was not associated with any deployment-related factors.
In an additional nested case-control analysis, suicide risk was independently and strongly associated with manic-depressive disorder (odds ratio, 7.38), depression (OR, 2.68), and alcohol-related problems (OR, 2.30). Again, no association was found between suicide risk and deployment factors.
In a subgroup analysis involving only Army personnel, manic-depressive disorder (HR, 5.96) and alcohol-related problems (HR, 3.86) were significantly associated with suicide risk. Depression was not, but that might have been attributable to inadequate statistical power because there were not enough cases in this subgroup, the investigators said.
These findings "are not consistent with the assumption that specific deployment-related characteristics ... are directly associated with increased suicide risk. Instead, the risk factors associated with suicide in this military population are consistent with civilian populations, including male sex and mental disorders," Ms. LeardMann and her associates said.
"Studies have shown a marked increase in the incidence of diagnosed mental disorders in active-duty service members since 2005, paralleling the incidence of suicide. This suggests that the increased rate of suicide in the military may largely be a product of an increased prevalence of mental disorders in this population, possibly resulting from indirect cumulative occupational stresses across both deployed and home-station environments over years of war," they said.
The researchers noted that their analyses could not capture suicides that occurred since 2008. "It is possible that the cumulative strain of multiple and lengthy deployments only began to be reflected in suicide rates toward the later stages of the conflicts [in Iran and Afghanistan]," and thus could not be accounted for in this study.
"However, the study did include the 3 years with the sharpest statistically significant increases in suicides." And the overall evidence clearly "points to the lack of any specific deployment-related effects," they noted.
This study was limited in that all the findings are based on only 83 suicide deaths, so it "may have lacked statistical power to produce a stable and reproducible multivariable model," Ms. LeardMann and her associates added.
This study was supported by the Department of Defense. Ms. LeardMann reported no financial conflicts of interest; one of her associates reported receiving a lecture fee from Merck.
FROM JAMA
Major finding: Suicide rates were highest among study subjects who had manic-depressive disorder (87.55 per 100,000), alcohol-related problems (27.67 per 100,000), and depression (26.94 per 100,000), and were not related to deployment factors.
Data source: An analysis of data on 151,560 participants in the Millennium Cohort Study who were former or current members of all military service branches and were followed for up to 7 years.
Disclosures: This study was supported by the Department of Defense. Ms. LeardMann reported no financial conflicts of interest; one of her associates reported receiving a lecture fee from Merck.
Naltrexone and therapy reduce relapse in comorbid alcohol dependence, PTSD
Patients with comorbid alcohol dependence and posttraumatic stress disorder might benefit from naltrexone therapy, either alone or in combination with prolonged exposure therapy, according to a report published online Aug. 6 in JAMA.
In a study examining the relative benefits of naltrexone alone, prolonged exposure therapy alone, and both treatments in combination, as compared with supportive counseling, participants who received naltrexone either alone or in combination therapy had significantly fewer days drinking and reported a significantly lower level of craving for alcohol up to 6 months after treatment ended, said Edna B. Foa, Ph.D., of the department of psychiatry at the University of Pennsylvania, Philadelphia, and her associates.
Although prolonged exposure therapy did not improve PTSD symptoms in this study, the combination of the therapy plus naltrexone did reduce the rate of relapse of alcohol dependence during the 6 months after treatments were discontinued.
Just as important, prolonged exposure therapy did not exacerbate drinking or alcohol craving, "a concern that has been voiced by some investigators," Dr. Foa and her colleagues said (JAMA 2013;310:488-95 [doi:10.1001/jama.2013.8268]).
"This finding contradicts the common view that trauma-focused therapy is contraindicated for individuals with alcohol dependence and PTSD because it may exacerbate PTSD symptoms and thereby lead to increased alcohol use," they noted.
After screening 657 potential study participants, the investigators enrolled 165 patients with comorbid PTSD and alcohol dependence over the course of 8 years. All had clinically significant PTSD symptoms, as reflected by scores of 15 or more on the PTSD Symptom Scale-Interview (possible range, 0-51, with higher scores indicating more severe symptoms). All patients also reported drinking heavily during the preceding 30 days on to the Timeline Follow-Back Interview.
The median length of the interval since the traumatic experience occurred was approximately 5 years.
All of the study subjects completed outpatient medical detoxification at baseline. All also received supportive counseling because of the concern about their safety in the face of debilitating impairment and multiple life difficulties such as homelessness.
These patients were randomly assigned to one of four treatment groups for the 6-month duration of the intervention phase of the study: naltrexone plus prolonged exposure therapy (40 patients), placebo plus prolonged exposure therapy (40 patients), naltrexone plus supportive counseling only (42 patients), or placebo plus supportive counseling only (43 patients).
The naltrexone groups were to receive the opiate antagonist at a target dose of 100 mg/d for 6 months.
The prolonged exposure therapy involved 12 weekly 90-minute sessions of repeated imaginal exposure in which patients revisited and recounted their traumatic memories, as well as discussed their thoughts and feelings. These study subjects also listened at home repeatedly to a recording of their recounting of the traumatic experience and repeatedly exposed themselves to safe situations that they previously had avoided because of trauma-related distress.
The supportive counseling focused on medication management and enhancement of patient compliance. Patients were to participate in 18 30- to 45-minute sessions with a study nurse who also provided education about alcoholism and offered support and advice concerning drinking.
All of the study subjects were evaluated for PTSD symptoms, alcohol use, and cravings every month during the intervention phase of the study, as well as at the conclusion of treatment (at 6 months) and at 6 months after discontinuation of treatment (at 12 months).
A total of 53 participants, 32% of the entire study population, dropped out of the study before completing the treatment phase. The dropout rate was similar across the four treatment groups.
Twelve patients were withdrawn because of serious adverse events that were not deemed to be related to the study interventions. These included seven patients with serious suicidal ideation, three with serious medical illness, one with psychotic symptoms, and one who died.
The subjects assigned to prolonged exposure therapy completed a mean of approximately six sessions.
Regarding alcohol dependence, patients in every study group reported some reduction in the percentage of days drinking during the intervention phase of the study, but after treatment ended, only patients who had taken naltrexone reported significantly fewer days of drinking, Dr. Foa and her associates said.
Similarly, all of the study groups reported reductions in alcohol cravings during treatment, but only patients in the two naltrexone groups reported such reductions after the intervention ended.
Patients who received prolonged exposure therapy reported a 3.6% reduction in the percentage of days during which they drank alcohol, while those who did not receive prolonged exposure therapy had a mean increase of 15.9% in the percentage of days during which they drank. This difference, however, did not reach statistical significance.
Regarding PTSD, all the study groups showed symptom reductions during treatment. After treatment ended, patients who had undergone prolonged exposure therapy showed decreases in PTSD symptoms, but the reductions did not reach statistical significance.
This null finding was attributed to the low attendance at these sessions. Also, all participants received some supportive counseling, which might have masked the effects of prolonged exposure therapy, the researchers said.
An exploratory analysis was performed to elucidate this unexpected result. It showed that 70% of participants who received naltrexone plus prolonged exposure therapy achieved a "low" level of PTSD severity at 12 months, as did 55% of those who received prolonged exposure therapy plus placebo. In comparison, 44% of those who received naltrexone only and 37% of those who received placebo only achieved a low level of PTSD severity.
This, taken together with the lower relapse rate among patients who received prolonged exposure therapy, suggests that the therapy protects against relapses in alcohol dependence, Dr. Foa and her colleagues said.
It was also "encouraging" that patients who attended six (half) or more of the prolonged exposure therapy sessions "benefitted substantially from treatment, suggesting that a relatively low dose of prolonged exposure therapy is effective in this population," they added.
This study was funded by the National Institute on Alcohol Abuse and Alcoholism. No relevant financial conflicts of interest were reported.
The findings certainly shed light on treatment for comorbid alcohol dependence and PTSD but must be considered in the context of the study’s limitations, said Katherine Mills, Ph.D.

|
|
The sample size was relatively small, especially considering that this was a four-group, randomized controlled trial. And the retention rate was particularly low, with only 56% completing the posttreatment and follow-up interviews. "This is not surprising given the nature of the research, in which participants are asked to confront some of the most terrifying events that have ever happened to them, and simultaneously try to abstain from using alcohol and other drugs, which are often the only means by which they have felt that they could cope with the consequences of those events," she noted. Still, the study "provides hope that the gap in treatment provision for this population may begin to narrow."
Dr. Mills is with the National Health and Medical Research Council Centre of Research Excellence in Mental Health and Substance Use at the University of New South Wales, Sydney. She reported no relevant financial conflicts of interest. These remarks were taken from her editorial accompanying Dr. Foa’s report (JAMA 2013;310:482-3).
The findings certainly shed light on treatment for comorbid alcohol dependence and PTSD but must be considered in the context of the study’s limitations, said Katherine Mills, Ph.D.

|
|
The sample size was relatively small, especially considering that this was a four-group, randomized controlled trial. And the retention rate was particularly low, with only 56% completing the posttreatment and follow-up interviews. "This is not surprising given the nature of the research, in which participants are asked to confront some of the most terrifying events that have ever happened to them, and simultaneously try to abstain from using alcohol and other drugs, which are often the only means by which they have felt that they could cope with the consequences of those events," she noted. Still, the study "provides hope that the gap in treatment provision for this population may begin to narrow."
Dr. Mills is with the National Health and Medical Research Council Centre of Research Excellence in Mental Health and Substance Use at the University of New South Wales, Sydney. She reported no relevant financial conflicts of interest. These remarks were taken from her editorial accompanying Dr. Foa’s report (JAMA 2013;310:482-3).
The findings certainly shed light on treatment for comorbid alcohol dependence and PTSD but must be considered in the context of the study’s limitations, said Katherine Mills, Ph.D.

|
|
The sample size was relatively small, especially considering that this was a four-group, randomized controlled trial. And the retention rate was particularly low, with only 56% completing the posttreatment and follow-up interviews. "This is not surprising given the nature of the research, in which participants are asked to confront some of the most terrifying events that have ever happened to them, and simultaneously try to abstain from using alcohol and other drugs, which are often the only means by which they have felt that they could cope with the consequences of those events," she noted. Still, the study "provides hope that the gap in treatment provision for this population may begin to narrow."
Dr. Mills is with the National Health and Medical Research Council Centre of Research Excellence in Mental Health and Substance Use at the University of New South Wales, Sydney. She reported no relevant financial conflicts of interest. These remarks were taken from her editorial accompanying Dr. Foa’s report (JAMA 2013;310:482-3).
Patients with comorbid alcohol dependence and posttraumatic stress disorder might benefit from naltrexone therapy, either alone or in combination with prolonged exposure therapy, according to a report published online Aug. 6 in JAMA.
In a study examining the relative benefits of naltrexone alone, prolonged exposure therapy alone, and both treatments in combination, as compared with supportive counseling, participants who received naltrexone either alone or in combination therapy had significantly fewer days drinking and reported a significantly lower level of craving for alcohol up to 6 months after treatment ended, said Edna B. Foa, Ph.D., of the department of psychiatry at the University of Pennsylvania, Philadelphia, and her associates.
Although prolonged exposure therapy did not improve PTSD symptoms in this study, the combination of the therapy plus naltrexone did reduce the rate of relapse of alcohol dependence during the 6 months after treatments were discontinued.
Just as important, prolonged exposure therapy did not exacerbate drinking or alcohol craving, "a concern that has been voiced by some investigators," Dr. Foa and her colleagues said (JAMA 2013;310:488-95 [doi:10.1001/jama.2013.8268]).
"This finding contradicts the common view that trauma-focused therapy is contraindicated for individuals with alcohol dependence and PTSD because it may exacerbate PTSD symptoms and thereby lead to increased alcohol use," they noted.
After screening 657 potential study participants, the investigators enrolled 165 patients with comorbid PTSD and alcohol dependence over the course of 8 years. All had clinically significant PTSD symptoms, as reflected by scores of 15 or more on the PTSD Symptom Scale-Interview (possible range, 0-51, with higher scores indicating more severe symptoms). All patients also reported drinking heavily during the preceding 30 days on to the Timeline Follow-Back Interview.
The median length of the interval since the traumatic experience occurred was approximately 5 years.
All of the study subjects completed outpatient medical detoxification at baseline. All also received supportive counseling because of the concern about their safety in the face of debilitating impairment and multiple life difficulties such as homelessness.
These patients were randomly assigned to one of four treatment groups for the 6-month duration of the intervention phase of the study: naltrexone plus prolonged exposure therapy (40 patients), placebo plus prolonged exposure therapy (40 patients), naltrexone plus supportive counseling only (42 patients), or placebo plus supportive counseling only (43 patients).
The naltrexone groups were to receive the opiate antagonist at a target dose of 100 mg/d for 6 months.
The prolonged exposure therapy involved 12 weekly 90-minute sessions of repeated imaginal exposure in which patients revisited and recounted their traumatic memories, as well as discussed their thoughts and feelings. These study subjects also listened at home repeatedly to a recording of their recounting of the traumatic experience and repeatedly exposed themselves to safe situations that they previously had avoided because of trauma-related distress.
The supportive counseling focused on medication management and enhancement of patient compliance. Patients were to participate in 18 30- to 45-minute sessions with a study nurse who also provided education about alcoholism and offered support and advice concerning drinking.
All of the study subjects were evaluated for PTSD symptoms, alcohol use, and cravings every month during the intervention phase of the study, as well as at the conclusion of treatment (at 6 months) and at 6 months after discontinuation of treatment (at 12 months).
A total of 53 participants, 32% of the entire study population, dropped out of the study before completing the treatment phase. The dropout rate was similar across the four treatment groups.
Twelve patients were withdrawn because of serious adverse events that were not deemed to be related to the study interventions. These included seven patients with serious suicidal ideation, three with serious medical illness, one with psychotic symptoms, and one who died.
The subjects assigned to prolonged exposure therapy completed a mean of approximately six sessions.
Regarding alcohol dependence, patients in every study group reported some reduction in the percentage of days drinking during the intervention phase of the study, but after treatment ended, only patients who had taken naltrexone reported significantly fewer days of drinking, Dr. Foa and her associates said.
Similarly, all of the study groups reported reductions in alcohol cravings during treatment, but only patients in the two naltrexone groups reported such reductions after the intervention ended.
Patients who received prolonged exposure therapy reported a 3.6% reduction in the percentage of days during which they drank alcohol, while those who did not receive prolonged exposure therapy had a mean increase of 15.9% in the percentage of days during which they drank. This difference, however, did not reach statistical significance.
Regarding PTSD, all the study groups showed symptom reductions during treatment. After treatment ended, patients who had undergone prolonged exposure therapy showed decreases in PTSD symptoms, but the reductions did not reach statistical significance.
This null finding was attributed to the low attendance at these sessions. Also, all participants received some supportive counseling, which might have masked the effects of prolonged exposure therapy, the researchers said.
An exploratory analysis was performed to elucidate this unexpected result. It showed that 70% of participants who received naltrexone plus prolonged exposure therapy achieved a "low" level of PTSD severity at 12 months, as did 55% of those who received prolonged exposure therapy plus placebo. In comparison, 44% of those who received naltrexone only and 37% of those who received placebo only achieved a low level of PTSD severity.
This, taken together with the lower relapse rate among patients who received prolonged exposure therapy, suggests that the therapy protects against relapses in alcohol dependence, Dr. Foa and her colleagues said.
It was also "encouraging" that patients who attended six (half) or more of the prolonged exposure therapy sessions "benefitted substantially from treatment, suggesting that a relatively low dose of prolonged exposure therapy is effective in this population," they added.
This study was funded by the National Institute on Alcohol Abuse and Alcoholism. No relevant financial conflicts of interest were reported.
Patients with comorbid alcohol dependence and posttraumatic stress disorder might benefit from naltrexone therapy, either alone or in combination with prolonged exposure therapy, according to a report published online Aug. 6 in JAMA.
In a study examining the relative benefits of naltrexone alone, prolonged exposure therapy alone, and both treatments in combination, as compared with supportive counseling, participants who received naltrexone either alone or in combination therapy had significantly fewer days drinking and reported a significantly lower level of craving for alcohol up to 6 months after treatment ended, said Edna B. Foa, Ph.D., of the department of psychiatry at the University of Pennsylvania, Philadelphia, and her associates.
Although prolonged exposure therapy did not improve PTSD symptoms in this study, the combination of the therapy plus naltrexone did reduce the rate of relapse of alcohol dependence during the 6 months after treatments were discontinued.
Just as important, prolonged exposure therapy did not exacerbate drinking or alcohol craving, "a concern that has been voiced by some investigators," Dr. Foa and her colleagues said (JAMA 2013;310:488-95 [doi:10.1001/jama.2013.8268]).
"This finding contradicts the common view that trauma-focused therapy is contraindicated for individuals with alcohol dependence and PTSD because it may exacerbate PTSD symptoms and thereby lead to increased alcohol use," they noted.
After screening 657 potential study participants, the investigators enrolled 165 patients with comorbid PTSD and alcohol dependence over the course of 8 years. All had clinically significant PTSD symptoms, as reflected by scores of 15 or more on the PTSD Symptom Scale-Interview (possible range, 0-51, with higher scores indicating more severe symptoms). All patients also reported drinking heavily during the preceding 30 days on to the Timeline Follow-Back Interview.
The median length of the interval since the traumatic experience occurred was approximately 5 years.
All of the study subjects completed outpatient medical detoxification at baseline. All also received supportive counseling because of the concern about their safety in the face of debilitating impairment and multiple life difficulties such as homelessness.
These patients were randomly assigned to one of four treatment groups for the 6-month duration of the intervention phase of the study: naltrexone plus prolonged exposure therapy (40 patients), placebo plus prolonged exposure therapy (40 patients), naltrexone plus supportive counseling only (42 patients), or placebo plus supportive counseling only (43 patients).
The naltrexone groups were to receive the opiate antagonist at a target dose of 100 mg/d for 6 months.
The prolonged exposure therapy involved 12 weekly 90-minute sessions of repeated imaginal exposure in which patients revisited and recounted their traumatic memories, as well as discussed their thoughts and feelings. These study subjects also listened at home repeatedly to a recording of their recounting of the traumatic experience and repeatedly exposed themselves to safe situations that they previously had avoided because of trauma-related distress.
The supportive counseling focused on medication management and enhancement of patient compliance. Patients were to participate in 18 30- to 45-minute sessions with a study nurse who also provided education about alcoholism and offered support and advice concerning drinking.
All of the study subjects were evaluated for PTSD symptoms, alcohol use, and cravings every month during the intervention phase of the study, as well as at the conclusion of treatment (at 6 months) and at 6 months after discontinuation of treatment (at 12 months).
A total of 53 participants, 32% of the entire study population, dropped out of the study before completing the treatment phase. The dropout rate was similar across the four treatment groups.
Twelve patients were withdrawn because of serious adverse events that were not deemed to be related to the study interventions. These included seven patients with serious suicidal ideation, three with serious medical illness, one with psychotic symptoms, and one who died.
The subjects assigned to prolonged exposure therapy completed a mean of approximately six sessions.
Regarding alcohol dependence, patients in every study group reported some reduction in the percentage of days drinking during the intervention phase of the study, but after treatment ended, only patients who had taken naltrexone reported significantly fewer days of drinking, Dr. Foa and her associates said.
Similarly, all of the study groups reported reductions in alcohol cravings during treatment, but only patients in the two naltrexone groups reported such reductions after the intervention ended.
Patients who received prolonged exposure therapy reported a 3.6% reduction in the percentage of days during which they drank alcohol, while those who did not receive prolonged exposure therapy had a mean increase of 15.9% in the percentage of days during which they drank. This difference, however, did not reach statistical significance.
Regarding PTSD, all the study groups showed symptom reductions during treatment. After treatment ended, patients who had undergone prolonged exposure therapy showed decreases in PTSD symptoms, but the reductions did not reach statistical significance.
This null finding was attributed to the low attendance at these sessions. Also, all participants received some supportive counseling, which might have masked the effects of prolonged exposure therapy, the researchers said.
An exploratory analysis was performed to elucidate this unexpected result. It showed that 70% of participants who received naltrexone plus prolonged exposure therapy achieved a "low" level of PTSD severity at 12 months, as did 55% of those who received prolonged exposure therapy plus placebo. In comparison, 44% of those who received naltrexone only and 37% of those who received placebo only achieved a low level of PTSD severity.
This, taken together with the lower relapse rate among patients who received prolonged exposure therapy, suggests that the therapy protects against relapses in alcohol dependence, Dr. Foa and her colleagues said.
It was also "encouraging" that patients who attended six (half) or more of the prolonged exposure therapy sessions "benefitted substantially from treatment, suggesting that a relatively low dose of prolonged exposure therapy is effective in this population," they added.
This study was funded by the National Institute on Alcohol Abuse and Alcoholism. No relevant financial conflicts of interest were reported.
FROM JAMA
Major finding: Patients who received naltrexone, either alone or in combination with prolonged exposure therapy, reported fewer days of drinking and a lower level of alcohol craving both during treatment and well after treatment ended, compared with those who did not receive the drug.
Data source: A blinded randomized clinical trial involving 165 patients with comorbid alcohol dependence and PTSD who were treated for 6 months and followed for a further 6 months.
Disclosures: This study was funded by the National Institute on Alcohol Abuse and Alcoholism. No relevant financial conflicts of interest were reported.
Long-term CCB therapy linked to higher breast cancer risk
The long-term use of calcium-channel blockers is associated with a doubling of the risk of both invasive ductal carcinoma and invasive lobular carcinoma of the breast, according to a report published online Aug. 5 in JAMA Internal Medicine.
This and other findings from a large population-based case-control study require confirmation in future research, because this is the first report of such a strong adverse long-term impact of calcium-channel blockers (CCBs) on breast cancer risk, said Dr. Christopher I. Li of the division of public health sciences, Fred Hutchinson Cancer Research Center, Seattle, and his associates.
The investigators found no such association between breast cancer and any of the other commonly used antihypertensive agents, even if they were taken for long durations.
The study results are relevant to public health, given that antihypertensive drugs are the most commonly prescribed class of medication in the United States, the researchers noted.
Previous studies of a possible link between breast cancer risk on the one hand and antihypertensive agents in general, and CCBs in particular, on the other hand, have produced inconsistent results. Most have included relatively few cases of breast cancer, have not assessed longer durations of use, and have inadequately examined the more recently introduced forms of the drugs.
Dr. Li and his colleagues averted these drawbacks by assessing postmenopausal women who had taken all the major classes of antihypertensive drugs for long durations, in a large enough sample to include many cases of the two most common histologic subtypes of breast cancer: invasive ductal carcinoma (IDC) and invasive lobular carcinoma (ILC).
They identified through a tumor registry 1,960 women aged 55-74 years who were diagnosed as having a primary IDC or ILC during January 2000 to December 2008 in the greater metropolitan Seattle area. These cases were matched for age and area of residence with 891 cancer-free women who served as controls. The two groups had similar annual household incomes and medical histories of hypertension, heart disease, and hypercholesterolemia.
Overall use, current use, former use, and short-term use of antihypertensive drugs were not associated with the risk of either IDC or ILC.
Only the long-term use of calcium-channel blockers (10 years or more) was related to increased risk of breast cancer, with an OR of 2.4 for IDC and an OR of 2.6 for ILC, the investigators said (JAMA Intern. Med. 2013 Aug. 5 [doi:10.1001/jamainternmed.2013.9071]).
This association remained robust when the data were analyzed according to the tumor’s estrogen-receptor status: The ORs were 2.3 for ER-positive IDC, 3.1 for ER-negative IDC, and 2.6 for ER-positive ILC.
No other drug categories showed significant associations with breast cancer risk. "With respect to diuretic use, risks associated with thiazide and nonthiazide diuretic use were also assessed separately, but neither was associated with breast cancer risk," they said.
A sensitivity analysis limited to women in both study groups who had hypertension and were currently using antihypertensive medications produced similar results. This indicates that the underlying condition itself does not explain the association with breast cancer, and thus confounding by indication was adequately controlled for.
"There was also some indication that current use of ACE inhibitors for 10 years or longer was associated with reduced risks of both IDC (OR, 0.7) and ILC (OR, 0.6), though the risk estimate for IDC was within the limits of chance," they said.
This finding must be interpreted with caution and requires confirmation in future research that includes a large number of long-term users of ACE inhibitors, Dr. Li and his associates added.
The U.S. National Cancer Institute and the U.S. Department of Defense supported the study. No relevant financial conflicts of interest were reported.
The use of CCBs should not be discontinued on the basis of this study because it is observational, it cannot prove causality, and its findings alone should not change clinical practice, said Patricia F. Coogan, Sc.D.

|
|
But neither should the findings be dismissed. "The data are persuasive because this was a first-rate study," with a large sample, a high case response rate (80%), and best-practice ascertainment of medication use among the participants. "The study particularly excels in the careful analytic efforts used to identify alternate explanations for the findings," and in ruling out confounding by indication.
If future research confirms the two- to threefold increase in breast cancer risk with long-term use of CCBs – the ninth most commonly prescribed class of drugs in the United States in 2009 – avoiding these medications will become one of the major modifiable risk factors for breast cancer, she said.
Dr. Coogan is at Slone Epidemiology Center at Boston University. She reported no financial conflicts of interest. These remarks were taken from her invited commentary accompanying Dr. Li’s report (JAMA Intern. Med. 2013 Aug. 5 [doi:10.1001/jamainternmed.2013.9069]).
The use of CCBs should not be discontinued on the basis of this study because it is observational, it cannot prove causality, and its findings alone should not change clinical practice, said Patricia F. Coogan, Sc.D.

|
|
But neither should the findings be dismissed. "The data are persuasive because this was a first-rate study," with a large sample, a high case response rate (80%), and best-practice ascertainment of medication use among the participants. "The study particularly excels in the careful analytic efforts used to identify alternate explanations for the findings," and in ruling out confounding by indication.
If future research confirms the two- to threefold increase in breast cancer risk with long-term use of CCBs – the ninth most commonly prescribed class of drugs in the United States in 2009 – avoiding these medications will become one of the major modifiable risk factors for breast cancer, she said.
Dr. Coogan is at Slone Epidemiology Center at Boston University. She reported no financial conflicts of interest. These remarks were taken from her invited commentary accompanying Dr. Li’s report (JAMA Intern. Med. 2013 Aug. 5 [doi:10.1001/jamainternmed.2013.9069]).
The use of CCBs should not be discontinued on the basis of this study because it is observational, it cannot prove causality, and its findings alone should not change clinical practice, said Patricia F. Coogan, Sc.D.

|
|
But neither should the findings be dismissed. "The data are persuasive because this was a first-rate study," with a large sample, a high case response rate (80%), and best-practice ascertainment of medication use among the participants. "The study particularly excels in the careful analytic efforts used to identify alternate explanations for the findings," and in ruling out confounding by indication.
If future research confirms the two- to threefold increase in breast cancer risk with long-term use of CCBs – the ninth most commonly prescribed class of drugs in the United States in 2009 – avoiding these medications will become one of the major modifiable risk factors for breast cancer, she said.
Dr. Coogan is at Slone Epidemiology Center at Boston University. She reported no financial conflicts of interest. These remarks were taken from her invited commentary accompanying Dr. Li’s report (JAMA Intern. Med. 2013 Aug. 5 [doi:10.1001/jamainternmed.2013.9069]).
The long-term use of calcium-channel blockers is associated with a doubling of the risk of both invasive ductal carcinoma and invasive lobular carcinoma of the breast, according to a report published online Aug. 5 in JAMA Internal Medicine.
This and other findings from a large population-based case-control study require confirmation in future research, because this is the first report of such a strong adverse long-term impact of calcium-channel blockers (CCBs) on breast cancer risk, said Dr. Christopher I. Li of the division of public health sciences, Fred Hutchinson Cancer Research Center, Seattle, and his associates.
The investigators found no such association between breast cancer and any of the other commonly used antihypertensive agents, even if they were taken for long durations.
The study results are relevant to public health, given that antihypertensive drugs are the most commonly prescribed class of medication in the United States, the researchers noted.
Previous studies of a possible link between breast cancer risk on the one hand and antihypertensive agents in general, and CCBs in particular, on the other hand, have produced inconsistent results. Most have included relatively few cases of breast cancer, have not assessed longer durations of use, and have inadequately examined the more recently introduced forms of the drugs.
Dr. Li and his colleagues averted these drawbacks by assessing postmenopausal women who had taken all the major classes of antihypertensive drugs for long durations, in a large enough sample to include many cases of the two most common histologic subtypes of breast cancer: invasive ductal carcinoma (IDC) and invasive lobular carcinoma (ILC).
They identified through a tumor registry 1,960 women aged 55-74 years who were diagnosed as having a primary IDC or ILC during January 2000 to December 2008 in the greater metropolitan Seattle area. These cases were matched for age and area of residence with 891 cancer-free women who served as controls. The two groups had similar annual household incomes and medical histories of hypertension, heart disease, and hypercholesterolemia.
Overall use, current use, former use, and short-term use of antihypertensive drugs were not associated with the risk of either IDC or ILC.
Only the long-term use of calcium-channel blockers (10 years or more) was related to increased risk of breast cancer, with an OR of 2.4 for IDC and an OR of 2.6 for ILC, the investigators said (JAMA Intern. Med. 2013 Aug. 5 [doi:10.1001/jamainternmed.2013.9071]).
This association remained robust when the data were analyzed according to the tumor’s estrogen-receptor status: The ORs were 2.3 for ER-positive IDC, 3.1 for ER-negative IDC, and 2.6 for ER-positive ILC.
No other drug categories showed significant associations with breast cancer risk. "With respect to diuretic use, risks associated with thiazide and nonthiazide diuretic use were also assessed separately, but neither was associated with breast cancer risk," they said.
A sensitivity analysis limited to women in both study groups who had hypertension and were currently using antihypertensive medications produced similar results. This indicates that the underlying condition itself does not explain the association with breast cancer, and thus confounding by indication was adequately controlled for.
"There was also some indication that current use of ACE inhibitors for 10 years or longer was associated with reduced risks of both IDC (OR, 0.7) and ILC (OR, 0.6), though the risk estimate for IDC was within the limits of chance," they said.
This finding must be interpreted with caution and requires confirmation in future research that includes a large number of long-term users of ACE inhibitors, Dr. Li and his associates added.
The U.S. National Cancer Institute and the U.S. Department of Defense supported the study. No relevant financial conflicts of interest were reported.
The long-term use of calcium-channel blockers is associated with a doubling of the risk of both invasive ductal carcinoma and invasive lobular carcinoma of the breast, according to a report published online Aug. 5 in JAMA Internal Medicine.
This and other findings from a large population-based case-control study require confirmation in future research, because this is the first report of such a strong adverse long-term impact of calcium-channel blockers (CCBs) on breast cancer risk, said Dr. Christopher I. Li of the division of public health sciences, Fred Hutchinson Cancer Research Center, Seattle, and his associates.
The investigators found no such association between breast cancer and any of the other commonly used antihypertensive agents, even if they were taken for long durations.
The study results are relevant to public health, given that antihypertensive drugs are the most commonly prescribed class of medication in the United States, the researchers noted.
Previous studies of a possible link between breast cancer risk on the one hand and antihypertensive agents in general, and CCBs in particular, on the other hand, have produced inconsistent results. Most have included relatively few cases of breast cancer, have not assessed longer durations of use, and have inadequately examined the more recently introduced forms of the drugs.
Dr. Li and his colleagues averted these drawbacks by assessing postmenopausal women who had taken all the major classes of antihypertensive drugs for long durations, in a large enough sample to include many cases of the two most common histologic subtypes of breast cancer: invasive ductal carcinoma (IDC) and invasive lobular carcinoma (ILC).
They identified through a tumor registry 1,960 women aged 55-74 years who were diagnosed as having a primary IDC or ILC during January 2000 to December 2008 in the greater metropolitan Seattle area. These cases were matched for age and area of residence with 891 cancer-free women who served as controls. The two groups had similar annual household incomes and medical histories of hypertension, heart disease, and hypercholesterolemia.
Overall use, current use, former use, and short-term use of antihypertensive drugs were not associated with the risk of either IDC or ILC.
Only the long-term use of calcium-channel blockers (10 years or more) was related to increased risk of breast cancer, with an OR of 2.4 for IDC and an OR of 2.6 for ILC, the investigators said (JAMA Intern. Med. 2013 Aug. 5 [doi:10.1001/jamainternmed.2013.9071]).
This association remained robust when the data were analyzed according to the tumor’s estrogen-receptor status: The ORs were 2.3 for ER-positive IDC, 3.1 for ER-negative IDC, and 2.6 for ER-positive ILC.
No other drug categories showed significant associations with breast cancer risk. "With respect to diuretic use, risks associated with thiazide and nonthiazide diuretic use were also assessed separately, but neither was associated with breast cancer risk," they said.
A sensitivity analysis limited to women in both study groups who had hypertension and were currently using antihypertensive medications produced similar results. This indicates that the underlying condition itself does not explain the association with breast cancer, and thus confounding by indication was adequately controlled for.
"There was also some indication that current use of ACE inhibitors for 10 years or longer was associated with reduced risks of both IDC (OR, 0.7) and ILC (OR, 0.6), though the risk estimate for IDC was within the limits of chance," they said.
This finding must be interpreted with caution and requires confirmation in future research that includes a large number of long-term users of ACE inhibitors, Dr. Li and his associates added.
The U.S. National Cancer Institute and the U.S. Department of Defense supported the study. No relevant financial conflicts of interest were reported.
FROM JAMA INTERNAL MEDICINE
Major finding: Long-term use of calcium-channel blockers (10 years or more) was related to increased risk of breast cancer, with an OR of 2.4 for invasive ductal carcinoma and an OR of 2.6 for invasive lobular carcinoma.
Data source: A population-based case-control study of women aged 55-74 years who had IDC (905), ILC (1,055), or no breast cancer (891 controls).
Disclosures: The National Cancer Institute and the U.S. Department of Defense supported the study. No relevant financial conflicts of interest were reported.
‘HCC-4 risk score’ IDs hepatitis C patients likely to develop HCC
A risk score derived from four simple test results readily obtained during routine care may help identify the patients with chronic hepatitis C who are most at risk for developing hepatocellular carcinoma, according to a retrospective study published online July 12 in the European Journal of Internal Medicine.
The score could enable physicians to target only the highest-risk patients for annual surveillance for malignant hepatic nodules, which is crucial because current screening methods are too invasive, too expensive, and too low-yield to be applied broadly across all risk groups.
The new risk score also may help identify patients with chronic hepatitis C who are at lowest risk for developing HCC, who can then be reassured that they can safely forgo invasive and expensive surveillance, reported Dr. Juan Carlos Gavilan and his associates at University Hospital Virgin de la Victoria, Malaga (Spain).
The investigators reviewed data from a 17-year longitudinal cohort study involving 829 patients with chronic hepatitis C. These subjects were assessed every 6 months for the development of HCC using serum alpha-fetoprotein (AFP) levels and ultrasound imaging to detect new focal hepatic lesions.
A total of 58 subjects (7%) developed HCC during follow-up.
An initial univariate analysis identified numerous clinical and epidemiologic factors associated with elevated risk for HCC. The researchers constructed a formula for predicting risk using the four independent factors that were most predictive of HCC in this cohort: patient age, platelet count, gamma-globulin level, and AFP level at baseline.
By dividing the study population into tertiles, Dr. Gavilan and his colleagues established cutoff ranges for low, medium, and high risk. They then classified each study participant as belonging to one of these three categories, to see how well this risk score correlated with the actual rates of HCC.
The annual incidence of HCC was 0.06% in the group designated as low risk, 0.5% in the group designated as medium risk, and 2.6% in the group designated as high risk, indicating that this "HCC-4 risk score" was indeed highly predictive, Dr. Gavilan and his associates said (Eur. J. Intern. Med. 2013 July 12 [doi: 10.1016/j.ejim.2013.06.010]).
In fact, the score was more accurate at predicting HCC than was the commonly used fibrosis index, they noted.
According to recently published recommendations, surveillance is only justified in populations with an HCC incidence of 1.5% or more per year. Thus, patients found to be high risk using this HCC-4 risk score would be appropriate for such surveillance, while those at medium or low risk would not be.
"These results must be confirmed in other studies," the investigators said.
There was no external funding source for this study, and no financial conflicts of interest were reported.
A risk score derived from four simple test results readily obtained during routine care may help identify the patients with chronic hepatitis C who are most at risk for developing hepatocellular carcinoma, according to a retrospective study published online July 12 in the European Journal of Internal Medicine.
The score could enable physicians to target only the highest-risk patients for annual surveillance for malignant hepatic nodules, which is crucial because current screening methods are too invasive, too expensive, and too low-yield to be applied broadly across all risk groups.
The new risk score also may help identify patients with chronic hepatitis C who are at lowest risk for developing HCC, who can then be reassured that they can safely forgo invasive and expensive surveillance, reported Dr. Juan Carlos Gavilan and his associates at University Hospital Virgin de la Victoria, Malaga (Spain).
The investigators reviewed data from a 17-year longitudinal cohort study involving 829 patients with chronic hepatitis C. These subjects were assessed every 6 months for the development of HCC using serum alpha-fetoprotein (AFP) levels and ultrasound imaging to detect new focal hepatic lesions.
A total of 58 subjects (7%) developed HCC during follow-up.
An initial univariate analysis identified numerous clinical and epidemiologic factors associated with elevated risk for HCC. The researchers constructed a formula for predicting risk using the four independent factors that were most predictive of HCC in this cohort: patient age, platelet count, gamma-globulin level, and AFP level at baseline.
By dividing the study population into tertiles, Dr. Gavilan and his colleagues established cutoff ranges for low, medium, and high risk. They then classified each study participant as belonging to one of these three categories, to see how well this risk score correlated with the actual rates of HCC.
The annual incidence of HCC was 0.06% in the group designated as low risk, 0.5% in the group designated as medium risk, and 2.6% in the group designated as high risk, indicating that this "HCC-4 risk score" was indeed highly predictive, Dr. Gavilan and his associates said (Eur. J. Intern. Med. 2013 July 12 [doi: 10.1016/j.ejim.2013.06.010]).
In fact, the score was more accurate at predicting HCC than was the commonly used fibrosis index, they noted.
According to recently published recommendations, surveillance is only justified in populations with an HCC incidence of 1.5% or more per year. Thus, patients found to be high risk using this HCC-4 risk score would be appropriate for such surveillance, while those at medium or low risk would not be.
"These results must be confirmed in other studies," the investigators said.
There was no external funding source for this study, and no financial conflicts of interest were reported.
A risk score derived from four simple test results readily obtained during routine care may help identify the patients with chronic hepatitis C who are most at risk for developing hepatocellular carcinoma, according to a retrospective study published online July 12 in the European Journal of Internal Medicine.
The score could enable physicians to target only the highest-risk patients for annual surveillance for malignant hepatic nodules, which is crucial because current screening methods are too invasive, too expensive, and too low-yield to be applied broadly across all risk groups.
The new risk score also may help identify patients with chronic hepatitis C who are at lowest risk for developing HCC, who can then be reassured that they can safely forgo invasive and expensive surveillance, reported Dr. Juan Carlos Gavilan and his associates at University Hospital Virgin de la Victoria, Malaga (Spain).
The investigators reviewed data from a 17-year longitudinal cohort study involving 829 patients with chronic hepatitis C. These subjects were assessed every 6 months for the development of HCC using serum alpha-fetoprotein (AFP) levels and ultrasound imaging to detect new focal hepatic lesions.
A total of 58 subjects (7%) developed HCC during follow-up.
An initial univariate analysis identified numerous clinical and epidemiologic factors associated with elevated risk for HCC. The researchers constructed a formula for predicting risk using the four independent factors that were most predictive of HCC in this cohort: patient age, platelet count, gamma-globulin level, and AFP level at baseline.
By dividing the study population into tertiles, Dr. Gavilan and his colleagues established cutoff ranges for low, medium, and high risk. They then classified each study participant as belonging to one of these three categories, to see how well this risk score correlated with the actual rates of HCC.
The annual incidence of HCC was 0.06% in the group designated as low risk, 0.5% in the group designated as medium risk, and 2.6% in the group designated as high risk, indicating that this "HCC-4 risk score" was indeed highly predictive, Dr. Gavilan and his associates said (Eur. J. Intern. Med. 2013 July 12 [doi: 10.1016/j.ejim.2013.06.010]).
In fact, the score was more accurate at predicting HCC than was the commonly used fibrosis index, they noted.
According to recently published recommendations, surveillance is only justified in populations with an HCC incidence of 1.5% or more per year. Thus, patients found to be high risk using this HCC-4 risk score would be appropriate for such surveillance, while those at medium or low risk would not be.
"These results must be confirmed in other studies," the investigators said.
There was no external funding source for this study, and no financial conflicts of interest were reported.
FROM THE EUROPEAN JOURNAL OF INTERNAL MEDICINE
Major finding: The annual incidence of HCC was 0.06% in the group designated as low risk, 0.5% in the group designated as medium risk, and 2.6% in the group designated as high risk, indicating that the HCC-4 risk score was highly predictive of actual outcomes.
Data source: A retrospective study of data collected in a 17-year longitudinal cohort study involving 829 adults with chronic hepatitis C, of whom 58 developed HCC.
Disclosures: There was no external funding source for this study, and no financial conflicts of interest were reported.
Treatments for severe ANCA-associated vasculitis show equal efficacy
For patients with severe antineutrophil cytoplasmic antibody–associated vasculitis, a single 4-week course of rituximab proved to be noninferior to conventional continuous immunosuppression at inducing and maintaining remission for 18 months, according to a report published Aug. 1 in the New England Journal of Medicine.
There were no differences between the two regimens in overall adverse events, except that patients who received rituximab for 1 month had fewer cases of leukopenia and pneumonia than did those who received a standard regimen of cyclophosphamide and azathioprine for 18 months, said Dr. Ulrich Specks of the Mayo Clinic Foundation, Rochester, Minn., and his associates in the RAVE-ITN (Rituximab in ANCA-Associated Vasculitis–Immune Tolerance Network) Research Group.
"Rituximab effectively induced B-cell depletion in all patients, but nearly all the patients showed reconstitution of peripheral-blood B cells by 18 months," the researchers noted.
This reflects "the reality of this disease, which is that relapses are common when the effects of immunosuppressive therapy wear off." However, the results also "point the way to more effective, long-term disease control through intermittent retreatment," they said.
The researchers previously published the short-term (6-month) results of their randomized, double-blind, multicenter RAVE study (N. Engl. J. Med. 2010;363:221-32) and now report the long-term (18-month) results for the 197 patients in the study. They assigned 99 patients to receive an infusion of rituximab at 375 mg/m2 of body surface area once a week for 4 weeks and a cyclophosphamide placebo followed by 17 months of a placebo, and 98 patients to receive cyclophosphamide at 2 mg/kg daily (adjusted for renal insufficiency) and infusions of a rituximab placebo for 3-6 months, depending on if and when remission was achieved, followed by azathioprine at 2 mg/kg for the balance of the 18-month treatment period. Patients stopped taking prednisone after 5.5 months if they were in remission.
A total of 64% of the rituximab group had a complete remission by 6 months, which was maintained in 48% at 12 months. The corresponding percentages for conventional immunosuppression were slightly lower at 53% at 6 months and 39% at 12 months.
At 18 months, complete remission was maintained in 39% of patients who had received rituximab and 33% of those who had received cyclophosphamide-azathioprine, which met the criterion for noninferiority but not for superiority, the investigators reported (N. Engl. J. Med. 2013 Aug. 1 [doi: 10.1056/NEJMoa1213277]).
There were no significant differences between the two study groups in any efficacy measure, including the duration of remission; the number, rate, and severity of relapses; or scores on measures of vasculitis damage and quality of life.
Rituximab was found superior to conventional immunosuppression in the subgroup of 101 patients who had relapsing rather than new-onset disease at enrollment in the study. In that subgroup, patients who received rituximab showed complete remission rates of 67% at 6 months, 49% at 12 months, and 37% at 18 months. The corresponding rates were significantly lower with cyclophosphamide-azathioprine at 42%, 24%, and 20%, respectively.
Rituximab’s efficacy was comparable to that of conventional immunosuppression in another important subgroup of patients: those who had major renal disease at baseline. Among the 102 patients with major renal disease at baseline, remission occurred at some point before 18 months in 75% with rituximab and 76% with cyclophosphamide-azathioprine, and the magnitude of improvement in mean estimated creatinine clearance levels was judged to be comparable between the groups.
Also at 18 months, there were no significant differences between the two study groups in the numbers or rates of total adverse events, serious adverse events, or non–disease-related adverse events. There were two deaths in each group.
In particular, the study groups had similar rates of infections of grade 3 or higher and similar serum levels of IgG, IgA, and IgM. No additional cancers developed during follow-up in either group.
However, patients who received rituximab had fewer episodes of moderate or severe leukopenia (5 vs. 23 cases) and required fewer dose adjustments or interruptions.
This study was supported by the National Institute of Allergy and Infectious Diseases, the Juvenile Diabetes Research Foundation, Genentech, Biogen Idec, the National Center for Research Resources, the National Institute of Arthritis and Musculoskeletal and Skin Diseases, and the Arthritis Foundation. Dr. Specks reported receiving an honorarium and travel reimbursement from Roche (Genentech is a member of the Roche Group), and some of his associates reported ties to Genentech, Biogen Idec, and other companies.
For patients with severe antineutrophil cytoplasmic antibody–associated vasculitis, a single 4-week course of rituximab proved to be noninferior to conventional continuous immunosuppression at inducing and maintaining remission for 18 months, according to a report published Aug. 1 in the New England Journal of Medicine.
There were no differences between the two regimens in overall adverse events, except that patients who received rituximab for 1 month had fewer cases of leukopenia and pneumonia than did those who received a standard regimen of cyclophosphamide and azathioprine for 18 months, said Dr. Ulrich Specks of the Mayo Clinic Foundation, Rochester, Minn., and his associates in the RAVE-ITN (Rituximab in ANCA-Associated Vasculitis–Immune Tolerance Network) Research Group.
"Rituximab effectively induced B-cell depletion in all patients, but nearly all the patients showed reconstitution of peripheral-blood B cells by 18 months," the researchers noted.
This reflects "the reality of this disease, which is that relapses are common when the effects of immunosuppressive therapy wear off." However, the results also "point the way to more effective, long-term disease control through intermittent retreatment," they said.
The researchers previously published the short-term (6-month) results of their randomized, double-blind, multicenter RAVE study (N. Engl. J. Med. 2010;363:221-32) and now report the long-term (18-month) results for the 197 patients in the study. They assigned 99 patients to receive an infusion of rituximab at 375 mg/m2 of body surface area once a week for 4 weeks and a cyclophosphamide placebo followed by 17 months of a placebo, and 98 patients to receive cyclophosphamide at 2 mg/kg daily (adjusted for renal insufficiency) and infusions of a rituximab placebo for 3-6 months, depending on if and when remission was achieved, followed by azathioprine at 2 mg/kg for the balance of the 18-month treatment period. Patients stopped taking prednisone after 5.5 months if they were in remission.
A total of 64% of the rituximab group had a complete remission by 6 months, which was maintained in 48% at 12 months. The corresponding percentages for conventional immunosuppression were slightly lower at 53% at 6 months and 39% at 12 months.
At 18 months, complete remission was maintained in 39% of patients who had received rituximab and 33% of those who had received cyclophosphamide-azathioprine, which met the criterion for noninferiority but not for superiority, the investigators reported (N. Engl. J. Med. 2013 Aug. 1 [doi: 10.1056/NEJMoa1213277]).
There were no significant differences between the two study groups in any efficacy measure, including the duration of remission; the number, rate, and severity of relapses; or scores on measures of vasculitis damage and quality of life.
Rituximab was found superior to conventional immunosuppression in the subgroup of 101 patients who had relapsing rather than new-onset disease at enrollment in the study. In that subgroup, patients who received rituximab showed complete remission rates of 67% at 6 months, 49% at 12 months, and 37% at 18 months. The corresponding rates were significantly lower with cyclophosphamide-azathioprine at 42%, 24%, and 20%, respectively.
Rituximab’s efficacy was comparable to that of conventional immunosuppression in another important subgroup of patients: those who had major renal disease at baseline. Among the 102 patients with major renal disease at baseline, remission occurred at some point before 18 months in 75% with rituximab and 76% with cyclophosphamide-azathioprine, and the magnitude of improvement in mean estimated creatinine clearance levels was judged to be comparable between the groups.
Also at 18 months, there were no significant differences between the two study groups in the numbers or rates of total adverse events, serious adverse events, or non–disease-related adverse events. There were two deaths in each group.
In particular, the study groups had similar rates of infections of grade 3 or higher and similar serum levels of IgG, IgA, and IgM. No additional cancers developed during follow-up in either group.
However, patients who received rituximab had fewer episodes of moderate or severe leukopenia (5 vs. 23 cases) and required fewer dose adjustments or interruptions.
This study was supported by the National Institute of Allergy and Infectious Diseases, the Juvenile Diabetes Research Foundation, Genentech, Biogen Idec, the National Center for Research Resources, the National Institute of Arthritis and Musculoskeletal and Skin Diseases, and the Arthritis Foundation. Dr. Specks reported receiving an honorarium and travel reimbursement from Roche (Genentech is a member of the Roche Group), and some of his associates reported ties to Genentech, Biogen Idec, and other companies.
For patients with severe antineutrophil cytoplasmic antibody–associated vasculitis, a single 4-week course of rituximab proved to be noninferior to conventional continuous immunosuppression at inducing and maintaining remission for 18 months, according to a report published Aug. 1 in the New England Journal of Medicine.
There were no differences between the two regimens in overall adverse events, except that patients who received rituximab for 1 month had fewer cases of leukopenia and pneumonia than did those who received a standard regimen of cyclophosphamide and azathioprine for 18 months, said Dr. Ulrich Specks of the Mayo Clinic Foundation, Rochester, Minn., and his associates in the RAVE-ITN (Rituximab in ANCA-Associated Vasculitis–Immune Tolerance Network) Research Group.
"Rituximab effectively induced B-cell depletion in all patients, but nearly all the patients showed reconstitution of peripheral-blood B cells by 18 months," the researchers noted.
This reflects "the reality of this disease, which is that relapses are common when the effects of immunosuppressive therapy wear off." However, the results also "point the way to more effective, long-term disease control through intermittent retreatment," they said.
The researchers previously published the short-term (6-month) results of their randomized, double-blind, multicenter RAVE study (N. Engl. J. Med. 2010;363:221-32) and now report the long-term (18-month) results for the 197 patients in the study. They assigned 99 patients to receive an infusion of rituximab at 375 mg/m2 of body surface area once a week for 4 weeks and a cyclophosphamide placebo followed by 17 months of a placebo, and 98 patients to receive cyclophosphamide at 2 mg/kg daily (adjusted for renal insufficiency) and infusions of a rituximab placebo for 3-6 months, depending on if and when remission was achieved, followed by azathioprine at 2 mg/kg for the balance of the 18-month treatment period. Patients stopped taking prednisone after 5.5 months if they were in remission.
A total of 64% of the rituximab group had a complete remission by 6 months, which was maintained in 48% at 12 months. The corresponding percentages for conventional immunosuppression were slightly lower at 53% at 6 months and 39% at 12 months.
At 18 months, complete remission was maintained in 39% of patients who had received rituximab and 33% of those who had received cyclophosphamide-azathioprine, which met the criterion for noninferiority but not for superiority, the investigators reported (N. Engl. J. Med. 2013 Aug. 1 [doi: 10.1056/NEJMoa1213277]).
There were no significant differences between the two study groups in any efficacy measure, including the duration of remission; the number, rate, and severity of relapses; or scores on measures of vasculitis damage and quality of life.
Rituximab was found superior to conventional immunosuppression in the subgroup of 101 patients who had relapsing rather than new-onset disease at enrollment in the study. In that subgroup, patients who received rituximab showed complete remission rates of 67% at 6 months, 49% at 12 months, and 37% at 18 months. The corresponding rates were significantly lower with cyclophosphamide-azathioprine at 42%, 24%, and 20%, respectively.
Rituximab’s efficacy was comparable to that of conventional immunosuppression in another important subgroup of patients: those who had major renal disease at baseline. Among the 102 patients with major renal disease at baseline, remission occurred at some point before 18 months in 75% with rituximab and 76% with cyclophosphamide-azathioprine, and the magnitude of improvement in mean estimated creatinine clearance levels was judged to be comparable between the groups.
Also at 18 months, there were no significant differences between the two study groups in the numbers or rates of total adverse events, serious adverse events, or non–disease-related adverse events. There were two deaths in each group.
In particular, the study groups had similar rates of infections of grade 3 or higher and similar serum levels of IgG, IgA, and IgM. No additional cancers developed during follow-up in either group.
However, patients who received rituximab had fewer episodes of moderate or severe leukopenia (5 vs. 23 cases) and required fewer dose adjustments or interruptions.
This study was supported by the National Institute of Allergy and Infectious Diseases, the Juvenile Diabetes Research Foundation, Genentech, Biogen Idec, the National Center for Research Resources, the National Institute of Arthritis and Musculoskeletal and Skin Diseases, and the Arthritis Foundation. Dr. Specks reported receiving an honorarium and travel reimbursement from Roche (Genentech is a member of the Roche Group), and some of his associates reported ties to Genentech, Biogen Idec, and other companies.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major finding: At 18 months, complete remission was maintained in 39% of patients who had received rituximab and 33% of those who had received cyclophosphamide-azathioprine, which met the criterion for noninferiority but not for superiority.
Data source: An 18-month extended follow-up report on a multicenter, double-blind, randomized noninferiority trial comparing rituximab to conventional immunosuppression for remission induction and maintenance in 197 patients with severe ANCA-associated vasculitis.
Disclosures: This study was supported by the National Institute of Allergy and Infectious Diseases, the Juvenile Diabetes Research Foundation, Genentech, Biogen Idec, the National Center for Research Resources, the National Institute of Arthritis and Musculoskeletal and Skin Diseases, and the Arthritis Foundation. Dr. Specks reported receiving an honorarium and travel reimbursement from Roche (Genentech is a member of the Roche Group), and some of his associates reported ties to Genentech, Biogen Idec, and other companies.
Early lenalidomide delays progression of smoldering multiple myeloma
Early oral lenalidomide-based treatment significantly delayed disease progression in an industry-sponsored phase III study of patients who had high-risk smoldering multiple myeloma.
The delay in disease progression with early lenalidomide "translated into a significant overall survival benefit; the proportion of patients who were alive at 3 years was 94% in the treatment group versus 80% in the observation group," reported Dr. María-Victoria Mateos of the Hospital Universitario de Salamanca (Spain) and her associates in the New England Journal of Medicine.
The study findings suggest that patients with smoldering multiple myeloma who are at high risk of progression to active disease should be targeted for early intervention (N. Engl. J. Med. 2013;369:438-47 [doi: 10.1056/NEJMoa1300439]).
Three years after entry into the study, 77% of the patients who received lenalidomide had progression-free survival, compared with only 30% of those who received usual care. Usual care involved simple observation, since there are no other therapeutic options in the early stage of the disease.
The treatment response rate was 79% during the induction phase to reduce the tumor burden, which increased to 90% during the maintenance phase. The regimen’s toxicity was judged to be moderate, and the incidence of second primary tumors was low.
The overall risk of progression with smoldering multiple myeloma is low, at 10% per year. However, a large subgroup of patients has been identified as high risk, with a 50% or more probability of progression to active disease within 2 years of diagnosis. Early intervention rather than observation has been attempted for this subgroup, but, so far, alkylating agents, bisphosphonates, interleukin-1B receptor antagonists, and thalidomide have failed to show clinical benefit.
Dr. Mateos and her colleagues performed the phase III, open-label, randomized trial at 19 medical centers in Spain and at 3 in Portugal, enrolling 119 patients with high-risk smoldering multiple myeloma. This was defined as a plasma-cell bone marrow infiltration of at least 10% and a monoclonal component, or only one of the two criteria plus at least 95% phenotypically aberrant plasma cells in the bone marrow plasma-cell compartment, with reductions in one to two uninvolved immunoglobulins of more than 25% of normal values.
Patients were randomly assigned to receive either usual care (62 patients) or treatment (57 patients). Treatment comprised an induction phase of nine 4-week cycles of oral lenalidomide plus dexamethasone, followed by a maintenance phase of low-dose lenalidomide, for a total duration of no more than 2 years.
For patients in the treatment group who showed asymptomatic biologic progression during the maintenance phase, dexamethasone was permitted. Patients in the observation group received no treatment until they progressed to symptomatic disease. The median follow-up was 40 months (range, 27-57 months).
Myeloma progressed in 13 patients (23%) in the treatment group, compared with 47 patients (76%) in the observation group.
Four patients in the treatment group died during follow-up, for an overall mortality of 7%. There was one death from a treatment-related toxic effect (a fatal respiratory infection), one from surgical complications unrelated to myeloma or its treatment, and two from disease progression. In contrast, 13 patients in the observation group died, for an overall mortality of 21%; all of the deaths were from disease progression, the researchers noted.
Infections were the most common nonhematologic adverse events; the incidence was not significantly different between the treatment and observation groups. Most infections were of low severity, but one patient in the treatment group developed a grade 5 respiratory infection and died. Serious adverse events were more common in the treatment group (12%) than in the observation group (3%).
The cumulative risk of developing a second primary tumor at 5 years was 20% in the treatment group and 25% in the observation group. These included breast cancer in one patient in the treatment group, prostate cancer in two patients in the treatment group, polycythemia vera in one patient in the treatment group, and myelodysplastic syndrome in one patient in the observation group. The most common grade 3 adverse events were infection (6% of patients), asthenia (6%), neutropenia (5%), and rash (3%).
Overall, 88% of the patients in the treatment group completed induction therapy and 70% completed maintenance therapy.
"Future studies should address the effect of early treatment on the quality of life, which we did not assess in this trial," Dr. Mateos and her associates noted.
This trial was funded by Celgene, which also was involved in the data collection and analysis. Dr. Mateos reported ties to Celgene, GenMab, and other companies; her associates reported ties to numerous industry sources.
Early oral lenalidomide-based treatment significantly delayed disease progression in an industry-sponsored phase III study of patients who had high-risk smoldering multiple myeloma.
The delay in disease progression with early lenalidomide "translated into a significant overall survival benefit; the proportion of patients who were alive at 3 years was 94% in the treatment group versus 80% in the observation group," reported Dr. María-Victoria Mateos of the Hospital Universitario de Salamanca (Spain) and her associates in the New England Journal of Medicine.
The study findings suggest that patients with smoldering multiple myeloma who are at high risk of progression to active disease should be targeted for early intervention (N. Engl. J. Med. 2013;369:438-47 [doi: 10.1056/NEJMoa1300439]).
Three years after entry into the study, 77% of the patients who received lenalidomide had progression-free survival, compared with only 30% of those who received usual care. Usual care involved simple observation, since there are no other therapeutic options in the early stage of the disease.
The treatment response rate was 79% during the induction phase to reduce the tumor burden, which increased to 90% during the maintenance phase. The regimen’s toxicity was judged to be moderate, and the incidence of second primary tumors was low.
The overall risk of progression with smoldering multiple myeloma is low, at 10% per year. However, a large subgroup of patients has been identified as high risk, with a 50% or more probability of progression to active disease within 2 years of diagnosis. Early intervention rather than observation has been attempted for this subgroup, but, so far, alkylating agents, bisphosphonates, interleukin-1B receptor antagonists, and thalidomide have failed to show clinical benefit.
Dr. Mateos and her colleagues performed the phase III, open-label, randomized trial at 19 medical centers in Spain and at 3 in Portugal, enrolling 119 patients with high-risk smoldering multiple myeloma. This was defined as a plasma-cell bone marrow infiltration of at least 10% and a monoclonal component, or only one of the two criteria plus at least 95% phenotypically aberrant plasma cells in the bone marrow plasma-cell compartment, with reductions in one to two uninvolved immunoglobulins of more than 25% of normal values.
Patients were randomly assigned to receive either usual care (62 patients) or treatment (57 patients). Treatment comprised an induction phase of nine 4-week cycles of oral lenalidomide plus dexamethasone, followed by a maintenance phase of low-dose lenalidomide, for a total duration of no more than 2 years.
For patients in the treatment group who showed asymptomatic biologic progression during the maintenance phase, dexamethasone was permitted. Patients in the observation group received no treatment until they progressed to symptomatic disease. The median follow-up was 40 months (range, 27-57 months).
Myeloma progressed in 13 patients (23%) in the treatment group, compared with 47 patients (76%) in the observation group.
Four patients in the treatment group died during follow-up, for an overall mortality of 7%. There was one death from a treatment-related toxic effect (a fatal respiratory infection), one from surgical complications unrelated to myeloma or its treatment, and two from disease progression. In contrast, 13 patients in the observation group died, for an overall mortality of 21%; all of the deaths were from disease progression, the researchers noted.
Infections were the most common nonhematologic adverse events; the incidence was not significantly different between the treatment and observation groups. Most infections were of low severity, but one patient in the treatment group developed a grade 5 respiratory infection and died. Serious adverse events were more common in the treatment group (12%) than in the observation group (3%).
The cumulative risk of developing a second primary tumor at 5 years was 20% in the treatment group and 25% in the observation group. These included breast cancer in one patient in the treatment group, prostate cancer in two patients in the treatment group, polycythemia vera in one patient in the treatment group, and myelodysplastic syndrome in one patient in the observation group. The most common grade 3 adverse events were infection (6% of patients), asthenia (6%), neutropenia (5%), and rash (3%).
Overall, 88% of the patients in the treatment group completed induction therapy and 70% completed maintenance therapy.
"Future studies should address the effect of early treatment on the quality of life, which we did not assess in this trial," Dr. Mateos and her associates noted.
This trial was funded by Celgene, which also was involved in the data collection and analysis. Dr. Mateos reported ties to Celgene, GenMab, and other companies; her associates reported ties to numerous industry sources.
Early oral lenalidomide-based treatment significantly delayed disease progression in an industry-sponsored phase III study of patients who had high-risk smoldering multiple myeloma.
The delay in disease progression with early lenalidomide "translated into a significant overall survival benefit; the proportion of patients who were alive at 3 years was 94% in the treatment group versus 80% in the observation group," reported Dr. María-Victoria Mateos of the Hospital Universitario de Salamanca (Spain) and her associates in the New England Journal of Medicine.
The study findings suggest that patients with smoldering multiple myeloma who are at high risk of progression to active disease should be targeted for early intervention (N. Engl. J. Med. 2013;369:438-47 [doi: 10.1056/NEJMoa1300439]).
Three years after entry into the study, 77% of the patients who received lenalidomide had progression-free survival, compared with only 30% of those who received usual care. Usual care involved simple observation, since there are no other therapeutic options in the early stage of the disease.
The treatment response rate was 79% during the induction phase to reduce the tumor burden, which increased to 90% during the maintenance phase. The regimen’s toxicity was judged to be moderate, and the incidence of second primary tumors was low.
The overall risk of progression with smoldering multiple myeloma is low, at 10% per year. However, a large subgroup of patients has been identified as high risk, with a 50% or more probability of progression to active disease within 2 years of diagnosis. Early intervention rather than observation has been attempted for this subgroup, but, so far, alkylating agents, bisphosphonates, interleukin-1B receptor antagonists, and thalidomide have failed to show clinical benefit.
Dr. Mateos and her colleagues performed the phase III, open-label, randomized trial at 19 medical centers in Spain and at 3 in Portugal, enrolling 119 patients with high-risk smoldering multiple myeloma. This was defined as a plasma-cell bone marrow infiltration of at least 10% and a monoclonal component, or only one of the two criteria plus at least 95% phenotypically aberrant plasma cells in the bone marrow plasma-cell compartment, with reductions in one to two uninvolved immunoglobulins of more than 25% of normal values.
Patients were randomly assigned to receive either usual care (62 patients) or treatment (57 patients). Treatment comprised an induction phase of nine 4-week cycles of oral lenalidomide plus dexamethasone, followed by a maintenance phase of low-dose lenalidomide, for a total duration of no more than 2 years.
For patients in the treatment group who showed asymptomatic biologic progression during the maintenance phase, dexamethasone was permitted. Patients in the observation group received no treatment until they progressed to symptomatic disease. The median follow-up was 40 months (range, 27-57 months).
Myeloma progressed in 13 patients (23%) in the treatment group, compared with 47 patients (76%) in the observation group.
Four patients in the treatment group died during follow-up, for an overall mortality of 7%. There was one death from a treatment-related toxic effect (a fatal respiratory infection), one from surgical complications unrelated to myeloma or its treatment, and two from disease progression. In contrast, 13 patients in the observation group died, for an overall mortality of 21%; all of the deaths were from disease progression, the researchers noted.
Infections were the most common nonhematologic adverse events; the incidence was not significantly different between the treatment and observation groups. Most infections were of low severity, but one patient in the treatment group developed a grade 5 respiratory infection and died. Serious adverse events were more common in the treatment group (12%) than in the observation group (3%).
The cumulative risk of developing a second primary tumor at 5 years was 20% in the treatment group and 25% in the observation group. These included breast cancer in one patient in the treatment group, prostate cancer in two patients in the treatment group, polycythemia vera in one patient in the treatment group, and myelodysplastic syndrome in one patient in the observation group. The most common grade 3 adverse events were infection (6% of patients), asthenia (6%), neutropenia (5%), and rash (3%).
Overall, 88% of the patients in the treatment group completed induction therapy and 70% completed maintenance therapy.
"Future studies should address the effect of early treatment on the quality of life, which we did not assess in this trial," Dr. Mateos and her associates noted.
This trial was funded by Celgene, which also was involved in the data collection and analysis. Dr. Mateos reported ties to Celgene, GenMab, and other companies; her associates reported ties to numerous industry sources.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major finding: Three-year survival was 94% among patients who received early oral lenalidomide, compared with 80% of patients who received usual care.
Data source: An open-label, phase III, randomized clinical trial involving 119 patients with high-risk smoldering multiple myeloma who were followed for a median of 40 months.
Disclosures: This trial was funded by Celgene, which also was involved in the data collection and analysis. Dr. Mateos reported ties to Celgene, GenMab, and other companies; her associates reported ties to numerous industry sources.