User login
Lucas Franki is an associate editor for MDedge News, and has been with the company since 2014. He has a BA in English from Penn State University and is an Eagle Scout.
Direct oral anticoagulants may be inappropriate for frail elderly
Caution must be used when prescribing direct oral anticoagulants to older patients, especially those in a frail condition, according to an opinion piece by Anne-Laure Sennesael and her associates.
In the case study, an 86-year-old woman weighing 55 kg was admitted to an emergency department with persistent epistaxis. The patient was taking 20 mg of rivaroxaban and 80 mg of aspirin daily. There was a history of peripheral arterial disease, and the patient had received a bioprosthetic heart implant 4 years prior. Creatinine clearance was 21 mL/min, hemoglobin was 9.4 g/dL, and prothrombin time Quick value was 30%.
Rivaroxaban was discontinued, and the patient was switched to a new anticoagulant, acenocoumarol. Aspirin also was discontinued, and the patient was discharged, reported Ms. Sennesael, of the Université catholique de Louvain in Brussels.
Use of direct oral anticoagulants (DOACs) are increasing rapidly, the authors write, mostly because doctors and patients view them as more convenient to use. However, in some patients, vitamin K antagonists (VKAs) remain the best course of treatment. In this case, the patient was receiving too much rivaroxaban in light of her low creatinine level. In addition, aspirin plus a DOAC is not appropriate, as it increases the risk of major bleeding significantly.
“A conservative strategy may be more valuable,” Ms. Sennesael and her associates wrote. “This kind of ‘less is more’ approach includes avoiding prescribing DOACs rather than VKAs without clear, compelling, evidence-based reasons; regularly reassessing renal function; monitoring for adverse effects; and reappraising aspirin prescription.”
Read the full study at JAMA Internal Medicine (doi:10.1001/jamainternmed.2015.3589).
Caution must be used when prescribing direct oral anticoagulants to older patients, especially those in a frail condition, according to an opinion piece by Anne-Laure Sennesael and her associates.
In the case study, an 86-year-old woman weighing 55 kg was admitted to an emergency department with persistent epistaxis. The patient was taking 20 mg of rivaroxaban and 80 mg of aspirin daily. There was a history of peripheral arterial disease, and the patient had received a bioprosthetic heart implant 4 years prior. Creatinine clearance was 21 mL/min, hemoglobin was 9.4 g/dL, and prothrombin time Quick value was 30%.
Rivaroxaban was discontinued, and the patient was switched to a new anticoagulant, acenocoumarol. Aspirin also was discontinued, and the patient was discharged, reported Ms. Sennesael, of the Université catholique de Louvain in Brussels.
Use of direct oral anticoagulants (DOACs) are increasing rapidly, the authors write, mostly because doctors and patients view them as more convenient to use. However, in some patients, vitamin K antagonists (VKAs) remain the best course of treatment. In this case, the patient was receiving too much rivaroxaban in light of her low creatinine level. In addition, aspirin plus a DOAC is not appropriate, as it increases the risk of major bleeding significantly.
“A conservative strategy may be more valuable,” Ms. Sennesael and her associates wrote. “This kind of ‘less is more’ approach includes avoiding prescribing DOACs rather than VKAs without clear, compelling, evidence-based reasons; regularly reassessing renal function; monitoring for adverse effects; and reappraising aspirin prescription.”
Read the full study at JAMA Internal Medicine (doi:10.1001/jamainternmed.2015.3589).
Caution must be used when prescribing direct oral anticoagulants to older patients, especially those in a frail condition, according to an opinion piece by Anne-Laure Sennesael and her associates.
In the case study, an 86-year-old woman weighing 55 kg was admitted to an emergency department with persistent epistaxis. The patient was taking 20 mg of rivaroxaban and 80 mg of aspirin daily. There was a history of peripheral arterial disease, and the patient had received a bioprosthetic heart implant 4 years prior. Creatinine clearance was 21 mL/min, hemoglobin was 9.4 g/dL, and prothrombin time Quick value was 30%.
Rivaroxaban was discontinued, and the patient was switched to a new anticoagulant, acenocoumarol. Aspirin also was discontinued, and the patient was discharged, reported Ms. Sennesael, of the Université catholique de Louvain in Brussels.
Use of direct oral anticoagulants (DOACs) are increasing rapidly, the authors write, mostly because doctors and patients view them as more convenient to use. However, in some patients, vitamin K antagonists (VKAs) remain the best course of treatment. In this case, the patient was receiving too much rivaroxaban in light of her low creatinine level. In addition, aspirin plus a DOAC is not appropriate, as it increases the risk of major bleeding significantly.
“A conservative strategy may be more valuable,” Ms. Sennesael and her associates wrote. “This kind of ‘less is more’ approach includes avoiding prescribing DOACs rather than VKAs without clear, compelling, evidence-based reasons; regularly reassessing renal function; monitoring for adverse effects; and reappraising aspirin prescription.”
Read the full study at JAMA Internal Medicine (doi:10.1001/jamainternmed.2015.3589).
Cell phone use offers depression diagnostic capability
Information pulled from cell phone sensor data can provide useful behavioral markers significantly associated with depressive symptom severity, according to Sohrab Saeb, Ph.D., and associates.
The investigators found that several different features pulled from GPS data related to study participants’ depressive symptom severity, including circadian movement, normalized entropy, and location variance. Phone use features, use duration, and use frequency also were related to depressive symptoms, said Dr. Saeb of the center for behavioral intervention technologies in the department of preventive medicine at Northwestern University, Chicago.
The researchers next used the normalized entropy feature and a system separating participants with depressive symptoms (Patient Health Questionnaire [PHQ-9] score greater than or equal to 5) from those without symptoms to identify depressed participants, achieving a success rate of 86.5%. Finally, with the use of normalized entropy data alone to identify the participants’ PHQ-9 scores, an error rate of only 23.5% was achieved.
The study findings “suggest that phone sensors offer numerous clinical opportunities, including continuous monitoring of at-risk populations with little patient burden and interventions that can provide just-in-time outreach,” the investigators concluded.
Find the full study in the Journal of Medical Internet Research (2015 July;17(7):(doi:10.2196/jmir.4273).
Information pulled from cell phone sensor data can provide useful behavioral markers significantly associated with depressive symptom severity, according to Sohrab Saeb, Ph.D., and associates.
The investigators found that several different features pulled from GPS data related to study participants’ depressive symptom severity, including circadian movement, normalized entropy, and location variance. Phone use features, use duration, and use frequency also were related to depressive symptoms, said Dr. Saeb of the center for behavioral intervention technologies in the department of preventive medicine at Northwestern University, Chicago.
The researchers next used the normalized entropy feature and a system separating participants with depressive symptoms (Patient Health Questionnaire [PHQ-9] score greater than or equal to 5) from those without symptoms to identify depressed participants, achieving a success rate of 86.5%. Finally, with the use of normalized entropy data alone to identify the participants’ PHQ-9 scores, an error rate of only 23.5% was achieved.
The study findings “suggest that phone sensors offer numerous clinical opportunities, including continuous monitoring of at-risk populations with little patient burden and interventions that can provide just-in-time outreach,” the investigators concluded.
Find the full study in the Journal of Medical Internet Research (2015 July;17(7):(doi:10.2196/jmir.4273).
Information pulled from cell phone sensor data can provide useful behavioral markers significantly associated with depressive symptom severity, according to Sohrab Saeb, Ph.D., and associates.
The investigators found that several different features pulled from GPS data related to study participants’ depressive symptom severity, including circadian movement, normalized entropy, and location variance. Phone use features, use duration, and use frequency also were related to depressive symptoms, said Dr. Saeb of the center for behavioral intervention technologies in the department of preventive medicine at Northwestern University, Chicago.
The researchers next used the normalized entropy feature and a system separating participants with depressive symptoms (Patient Health Questionnaire [PHQ-9] score greater than or equal to 5) from those without symptoms to identify depressed participants, achieving a success rate of 86.5%. Finally, with the use of normalized entropy data alone to identify the participants’ PHQ-9 scores, an error rate of only 23.5% was achieved.
The study findings “suggest that phone sensors offer numerous clinical opportunities, including continuous monitoring of at-risk populations with little patient burden and interventions that can provide just-in-time outreach,” the investigators concluded.
Find the full study in the Journal of Medical Internet Research (2015 July;17(7):(doi:10.2196/jmir.4273).
More sensitive IPD definition improves vaccine cost-effectiveness
Expanding the definition of invasive pneumococcal disease in children aged 3-42 months to include suspected cases and unspecified sepsis significantly improved the cost-effectiveness of the 10-valent pneumococcal conjugate vaccine, Dr. Arto A. Palmu and his associates reported.
In a nationwide observational follow-up study, Dr. Palmu and his associates found that the relative rate reduction for non–laboratory-confirmed invasive pneumococcal disease (IPD) and unspecified sepsis was only 34%, compared with 80% for culture-confirmed IPD. The absolute rate reduction was much higher. For culture-confirmed IPD, the absolute rate reduction was 50 cases per 100,000 person-years, and for non–laboratory-confirmed IPD and unspecified sepsis, the rate was 122 cases per 100,000 person-years, said Dr. Palmu of the National Institute for Health and Welfare in Tampere, Finland.
Mortality reduction was 51% overall. For non–culture-confirmed IPD and unspecified sepsis, the relative mortality reduction was 35%.
“Use of sensitive case definitions, such as clinically suspected IPD, in the evaluation of the total disease burden prevented by the vaccination program is important for understanding the total burden of pneumococcal disease and the cost-effectiveness of public health interventions,” the investigators concluded.
Find the full study in Pediatrics (doi:10.1542/peds.2015-0458).
Expanding the definition of invasive pneumococcal disease in children aged 3-42 months to include suspected cases and unspecified sepsis significantly improved the cost-effectiveness of the 10-valent pneumococcal conjugate vaccine, Dr. Arto A. Palmu and his associates reported.
In a nationwide observational follow-up study, Dr. Palmu and his associates found that the relative rate reduction for non–laboratory-confirmed invasive pneumococcal disease (IPD) and unspecified sepsis was only 34%, compared with 80% for culture-confirmed IPD. The absolute rate reduction was much higher. For culture-confirmed IPD, the absolute rate reduction was 50 cases per 100,000 person-years, and for non–laboratory-confirmed IPD and unspecified sepsis, the rate was 122 cases per 100,000 person-years, said Dr. Palmu of the National Institute for Health and Welfare in Tampere, Finland.
Mortality reduction was 51% overall. For non–culture-confirmed IPD and unspecified sepsis, the relative mortality reduction was 35%.
“Use of sensitive case definitions, such as clinically suspected IPD, in the evaluation of the total disease burden prevented by the vaccination program is important for understanding the total burden of pneumococcal disease and the cost-effectiveness of public health interventions,” the investigators concluded.
Find the full study in Pediatrics (doi:10.1542/peds.2015-0458).
Expanding the definition of invasive pneumococcal disease in children aged 3-42 months to include suspected cases and unspecified sepsis significantly improved the cost-effectiveness of the 10-valent pneumococcal conjugate vaccine, Dr. Arto A. Palmu and his associates reported.
In a nationwide observational follow-up study, Dr. Palmu and his associates found that the relative rate reduction for non–laboratory-confirmed invasive pneumococcal disease (IPD) and unspecified sepsis was only 34%, compared with 80% for culture-confirmed IPD. The absolute rate reduction was much higher. For culture-confirmed IPD, the absolute rate reduction was 50 cases per 100,000 person-years, and for non–laboratory-confirmed IPD and unspecified sepsis, the rate was 122 cases per 100,000 person-years, said Dr. Palmu of the National Institute for Health and Welfare in Tampere, Finland.
Mortality reduction was 51% overall. For non–culture-confirmed IPD and unspecified sepsis, the relative mortality reduction was 35%.
“Use of sensitive case definitions, such as clinically suspected IPD, in the evaluation of the total disease burden prevented by the vaccination program is important for understanding the total burden of pneumococcal disease and the cost-effectiveness of public health interventions,” the investigators concluded.
Find the full study in Pediatrics (doi:10.1542/peds.2015-0458).
9-valent HPV vaccine equally effective in adolescents, young women
Response to the 9-valent human papillomavirus vaccine was noninferior in boys and girls aged 9-15 years, compared with women aged 16-26 years, according to Dr. Pierre Van Damme of the University of Antwerp, Belgium, and his associates.
In all three groups, a seroconversion rate of greater than 99% was achieved for all HPV vaccine types in this study of 3,074 subjects. After 2.5 years, anti-HPV responses remained strong at over 90% for the boys and girls. The delivery of the 9-valent HPV vaccine was tolerated well in all groups, with boys and girls reporting injection-site adverse event rates of 72.8% and 81.9%, respectively, compared with 85.4% of young women.
The study findings support “bridging the efficacy findings in young women 16 to 26 years of age to girls and boys 9 to 15 years of age. The 9vHPV vaccine appears to be generally well tolerated in all groups,” the investigators wrote.
Find the full study in Pediatrics (doi: 10.1542/peds.2014-3745).
Response to the 9-valent human papillomavirus vaccine was noninferior in boys and girls aged 9-15 years, compared with women aged 16-26 years, according to Dr. Pierre Van Damme of the University of Antwerp, Belgium, and his associates.
In all three groups, a seroconversion rate of greater than 99% was achieved for all HPV vaccine types in this study of 3,074 subjects. After 2.5 years, anti-HPV responses remained strong at over 90% for the boys and girls. The delivery of the 9-valent HPV vaccine was tolerated well in all groups, with boys and girls reporting injection-site adverse event rates of 72.8% and 81.9%, respectively, compared with 85.4% of young women.
The study findings support “bridging the efficacy findings in young women 16 to 26 years of age to girls and boys 9 to 15 years of age. The 9vHPV vaccine appears to be generally well tolerated in all groups,” the investigators wrote.
Find the full study in Pediatrics (doi: 10.1542/peds.2014-3745).
Response to the 9-valent human papillomavirus vaccine was noninferior in boys and girls aged 9-15 years, compared with women aged 16-26 years, according to Dr. Pierre Van Damme of the University of Antwerp, Belgium, and his associates.
In all three groups, a seroconversion rate of greater than 99% was achieved for all HPV vaccine types in this study of 3,074 subjects. After 2.5 years, anti-HPV responses remained strong at over 90% for the boys and girls. The delivery of the 9-valent HPV vaccine was tolerated well in all groups, with boys and girls reporting injection-site adverse event rates of 72.8% and 81.9%, respectively, compared with 85.4% of young women.
The study findings support “bridging the efficacy findings in young women 16 to 26 years of age to girls and boys 9 to 15 years of age. The 9vHPV vaccine appears to be generally well tolerated in all groups,” the investigators wrote.
Find the full study in Pediatrics (doi: 10.1542/peds.2014-3745).
Aging out, geography leading to increased psychiatrist demand
Psychiatrists were behind only primary care physicians as the most recruited medical specialty from April 1, 2014, to March 31, 2015, according to a report from Merritt Hawkins.
During the 2014-2015 time period, 230 search assignments were performed for psychiatrists, only 7 behind the number of recruitments done for doctors in internal medicine. However, both were still far behind the 734 searches performed for family medicine. Hospitalists, nurse practitioners, ob.gyns., and orthopedic surgeons also had more than 100 searches performed during the time period, Merritt Hawkins reported.
Demand for psychiatrists is rising as many psychiatrists are aging out. Nearly half of all psychiatrists are likely to retire within the next 5 years, according to Travis Singleton, senior vice president of Merritt Hawkins. “Psychiatrists are aging out of practice at a time when demand for their services is spiking. Finding a psychiatrist willing to practice in an inpatient setting is like looking for a needle in a haystack,” he said in a statement.
In addition to the age problem, psychiatrist distribution varies widely by state, influencing demand. Massachusetts, a heavily urbanized state, has 18 psychiatrists per 100,000 people, while Idaho, a rural state, has only 5 per 100,000.
Of the 254 counties in Texas, 185 have no general psychiatrist, and this is a small fraction of the nearly 4,000 whole or partial counties listed as Health Professional Shortage Areas for mental health.
“Mental health is a topic that the health system and patients themselves often avoid,” Mr. Singleton said. “For that reason, psychiatry can be considered the ‘silent shortage,’ even though shortages in psychiatry may be even more acute than they are in primary care.”
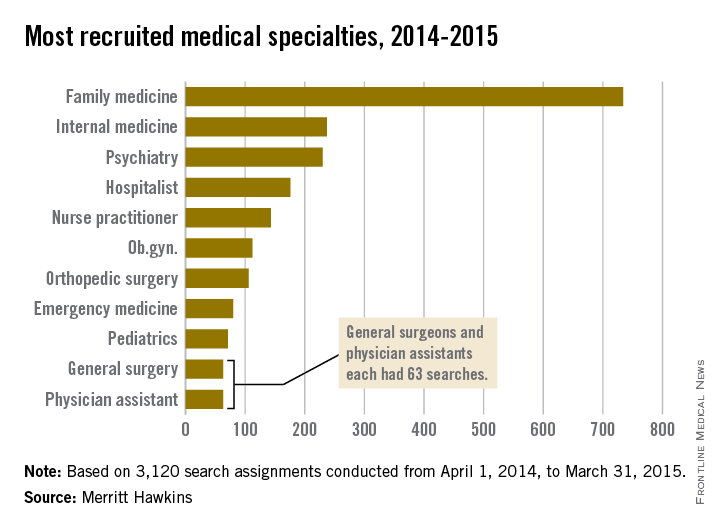
Psychiatrists were behind only primary care physicians as the most recruited medical specialty from April 1, 2014, to March 31, 2015, according to a report from Merritt Hawkins.
During the 2014-2015 time period, 230 search assignments were performed for psychiatrists, only 7 behind the number of recruitments done for doctors in internal medicine. However, both were still far behind the 734 searches performed for family medicine. Hospitalists, nurse practitioners, ob.gyns., and orthopedic surgeons also had more than 100 searches performed during the time period, Merritt Hawkins reported.
Demand for psychiatrists is rising as many psychiatrists are aging out. Nearly half of all psychiatrists are likely to retire within the next 5 years, according to Travis Singleton, senior vice president of Merritt Hawkins. “Psychiatrists are aging out of practice at a time when demand for their services is spiking. Finding a psychiatrist willing to practice in an inpatient setting is like looking for a needle in a haystack,” he said in a statement.
In addition to the age problem, psychiatrist distribution varies widely by state, influencing demand. Massachusetts, a heavily urbanized state, has 18 psychiatrists per 100,000 people, while Idaho, a rural state, has only 5 per 100,000.
Of the 254 counties in Texas, 185 have no general psychiatrist, and this is a small fraction of the nearly 4,000 whole or partial counties listed as Health Professional Shortage Areas for mental health.
“Mental health is a topic that the health system and patients themselves often avoid,” Mr. Singleton said. “For that reason, psychiatry can be considered the ‘silent shortage,’ even though shortages in psychiatry may be even more acute than they are in primary care.”

Psychiatrists were behind only primary care physicians as the most recruited medical specialty from April 1, 2014, to March 31, 2015, according to a report from Merritt Hawkins.
During the 2014-2015 time period, 230 search assignments were performed for psychiatrists, only 7 behind the number of recruitments done for doctors in internal medicine. However, both were still far behind the 734 searches performed for family medicine. Hospitalists, nurse practitioners, ob.gyns., and orthopedic surgeons also had more than 100 searches performed during the time period, Merritt Hawkins reported.
Demand for psychiatrists is rising as many psychiatrists are aging out. Nearly half of all psychiatrists are likely to retire within the next 5 years, according to Travis Singleton, senior vice president of Merritt Hawkins. “Psychiatrists are aging out of practice at a time when demand for their services is spiking. Finding a psychiatrist willing to practice in an inpatient setting is like looking for a needle in a haystack,” he said in a statement.
In addition to the age problem, psychiatrist distribution varies widely by state, influencing demand. Massachusetts, a heavily urbanized state, has 18 psychiatrists per 100,000 people, while Idaho, a rural state, has only 5 per 100,000.
Of the 254 counties in Texas, 185 have no general psychiatrist, and this is a small fraction of the nearly 4,000 whole or partial counties listed as Health Professional Shortage Areas for mental health.
“Mental health is a topic that the health system and patients themselves often avoid,” Mr. Singleton said. “For that reason, psychiatry can be considered the ‘silent shortage,’ even though shortages in psychiatry may be even more acute than they are in primary care.”

Amlodipine reduced vismodegib-induced muscle cramps
The calcium channel blocker amlodipine besylate was effective in reducing the number of muscle cramps caused by vismodegib, a basal cell carcinoma drug, according to a research letter from Dr. Mina Ally and her associates.
Patients who took amlodipine had the number of muscle cramps halved after 2 weeks of treatment, and this level was maintained for the 8-week medication regimen. No significant change in cramp severity, duration, or frequency of nighttime awakenings was seen. Side effects only appeared in too patients, with one reporting mild intermittent dizziness and another reporting grade 1 peripheral edema.
The control group saw a nonsignificant increase in cramp frequency, compared with the significant decrease in the amlodipine group. No change was seen in cramp severity, duration, or number of nighttime awakenings in the control group.
“Amlodipine may be effective in vismodegib-induced muscle cramps because it blocks voltage-gated calcium channels and inhibits the transport of extracellular calcium into muscle that is required for contraction,” the investigators noted.
Find the full research letter in JAMA Dermatology (doi:10.1001/jamadermatol.2015.1937).
The calcium channel blocker amlodipine besylate was effective in reducing the number of muscle cramps caused by vismodegib, a basal cell carcinoma drug, according to a research letter from Dr. Mina Ally and her associates.
Patients who took amlodipine had the number of muscle cramps halved after 2 weeks of treatment, and this level was maintained for the 8-week medication regimen. No significant change in cramp severity, duration, or frequency of nighttime awakenings was seen. Side effects only appeared in too patients, with one reporting mild intermittent dizziness and another reporting grade 1 peripheral edema.
The control group saw a nonsignificant increase in cramp frequency, compared with the significant decrease in the amlodipine group. No change was seen in cramp severity, duration, or number of nighttime awakenings in the control group.
“Amlodipine may be effective in vismodegib-induced muscle cramps because it blocks voltage-gated calcium channels and inhibits the transport of extracellular calcium into muscle that is required for contraction,” the investigators noted.
Find the full research letter in JAMA Dermatology (doi:10.1001/jamadermatol.2015.1937).
The calcium channel blocker amlodipine besylate was effective in reducing the number of muscle cramps caused by vismodegib, a basal cell carcinoma drug, according to a research letter from Dr. Mina Ally and her associates.
Patients who took amlodipine had the number of muscle cramps halved after 2 weeks of treatment, and this level was maintained for the 8-week medication regimen. No significant change in cramp severity, duration, or frequency of nighttime awakenings was seen. Side effects only appeared in too patients, with one reporting mild intermittent dizziness and another reporting grade 1 peripheral edema.
The control group saw a nonsignificant increase in cramp frequency, compared with the significant decrease in the amlodipine group. No change was seen in cramp severity, duration, or number of nighttime awakenings in the control group.
“Amlodipine may be effective in vismodegib-induced muscle cramps because it blocks voltage-gated calcium channels and inhibits the transport of extracellular calcium into muscle that is required for contraction,” the investigators noted.
Find the full research letter in JAMA Dermatology (doi:10.1001/jamadermatol.2015.1937).
Family medicine most in demand specialty during 2014-2015
For the ninth straight year, family medicine was the most recruited medical specialty, according to a new report from physician job placement firm Merritt Hawkins.
During 2014-2015, there were 734 search assignments performed for doctors in family medicine, nearly one-quarter of the 3,120 total searches conducted during the period from April 1, 2014, to March 31, 2015, according to the company’s 2015 Review of Physician and Advanced Practitioner Recruiting Incentives. No other specialty came close to this number of search requests.
Internal medicine, the other primary care specialty and a nine-year stalwart of the faraway second position, finished the year with 237 recruitments, Merritt Hawkins reported.
Psychiatry was the most recruited non–primary care specialty with 230 searches, falling just short of usurping internal medicine in second place. Other specialty categories with more than 100 recruitments in 2014-2015 were hospital medicine with 176, nurse practitioner with 143, ob.gyn. with 112, and orthopedic surgery with 106.
Demand for primary physicians, NPs, gynecologists, and physicians who work with chronic illness increased from the 2013-2014 period. “Implementation of population health management through integrated systems such as accountable care organizations is likely to keep demand strong for these types of clinicians,” Travis Singleton, senior vice president of Merritt Hawkins, said in a written statement.
Nearly all new employments were done by a hospital or other large employer, and only 5% of recruitment was conducted by private, independent practices, continuing the decline of private practice. Value-based incentives have decreased, with 23% of employers basing the bonus on value, compared with 39% 2 years ago, according to Merritt Hawkins.
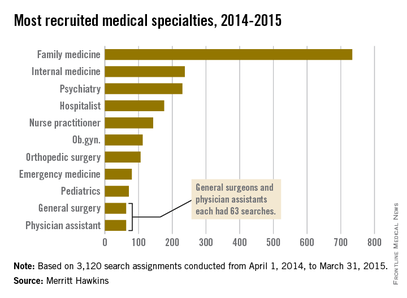
For the ninth straight year, family medicine was the most recruited medical specialty, according to a new report from physician job placement firm Merritt Hawkins.
During 2014-2015, there were 734 search assignments performed for doctors in family medicine, nearly one-quarter of the 3,120 total searches conducted during the period from April 1, 2014, to March 31, 2015, according to the company’s 2015 Review of Physician and Advanced Practitioner Recruiting Incentives. No other specialty came close to this number of search requests.
Internal medicine, the other primary care specialty and a nine-year stalwart of the faraway second position, finished the year with 237 recruitments, Merritt Hawkins reported.
Psychiatry was the most recruited non–primary care specialty with 230 searches, falling just short of usurping internal medicine in second place. Other specialty categories with more than 100 recruitments in 2014-2015 were hospital medicine with 176, nurse practitioner with 143, ob.gyn. with 112, and orthopedic surgery with 106.
Demand for primary physicians, NPs, gynecologists, and physicians who work with chronic illness increased from the 2013-2014 period. “Implementation of population health management through integrated systems such as accountable care organizations is likely to keep demand strong for these types of clinicians,” Travis Singleton, senior vice president of Merritt Hawkins, said in a written statement.
Nearly all new employments were done by a hospital or other large employer, and only 5% of recruitment was conducted by private, independent practices, continuing the decline of private practice. Value-based incentives have decreased, with 23% of employers basing the bonus on value, compared with 39% 2 years ago, according to Merritt Hawkins.

For the ninth straight year, family medicine was the most recruited medical specialty, according to a new report from physician job placement firm Merritt Hawkins.
During 2014-2015, there were 734 search assignments performed for doctors in family medicine, nearly one-quarter of the 3,120 total searches conducted during the period from April 1, 2014, to March 31, 2015, according to the company’s 2015 Review of Physician and Advanced Practitioner Recruiting Incentives. No other specialty came close to this number of search requests.
Internal medicine, the other primary care specialty and a nine-year stalwart of the faraway second position, finished the year with 237 recruitments, Merritt Hawkins reported.
Psychiatry was the most recruited non–primary care specialty with 230 searches, falling just short of usurping internal medicine in second place. Other specialty categories with more than 100 recruitments in 2014-2015 were hospital medicine with 176, nurse practitioner with 143, ob.gyn. with 112, and orthopedic surgery with 106.
Demand for primary physicians, NPs, gynecologists, and physicians who work with chronic illness increased from the 2013-2014 period. “Implementation of population health management through integrated systems such as accountable care organizations is likely to keep demand strong for these types of clinicians,” Travis Singleton, senior vice president of Merritt Hawkins, said in a written statement.
Nearly all new employments were done by a hospital or other large employer, and only 5% of recruitment was conducted by private, independent practices, continuing the decline of private practice. Value-based incentives have decreased, with 23% of employers basing the bonus on value, compared with 39% 2 years ago, according to Merritt Hawkins.

LBW, unhealthy lifestyle together increase type 2 diabetes risk
A low birth weight and an unhealthy lifestyle increase risk of type 2 diabetes more than either factor alone, according to Dr. Yanping Li of Harvard T.H. Chan School of Public Health, Boston, and associates.
In a study of 11, 709 cases of type 2 diabetes, the odds ratio for type 2 diabetes as a result of low birth weight alone was 1.45 per kg under normal birth weight, and for unhealthy lifestyle alone, the OR was 2.1. When both factors were present, the OR increased significantly to 2.86.
If both factors were present, unhealthy lifestyle had significantly more impact on diabetes development, with 59% of the attributable proportion of joint effect, compared with just 22% for low birth weight and 18% for the interaction between the two.
“The finding suggests that most cases of type 2 diabetes could be prevented by the adoption of a healthier lifestyle, but simultaneous improvement of both prenatal and postnatal factors could further prevent additional cases,” the investigators concluded.
Find the full study in the BMJ (doi:10.1136/bmj.h3672).
A low birth weight and an unhealthy lifestyle increase risk of type 2 diabetes more than either factor alone, according to Dr. Yanping Li of Harvard T.H. Chan School of Public Health, Boston, and associates.
In a study of 11, 709 cases of type 2 diabetes, the odds ratio for type 2 diabetes as a result of low birth weight alone was 1.45 per kg under normal birth weight, and for unhealthy lifestyle alone, the OR was 2.1. When both factors were present, the OR increased significantly to 2.86.
If both factors were present, unhealthy lifestyle had significantly more impact on diabetes development, with 59% of the attributable proportion of joint effect, compared with just 22% for low birth weight and 18% for the interaction between the two.
“The finding suggests that most cases of type 2 diabetes could be prevented by the adoption of a healthier lifestyle, but simultaneous improvement of both prenatal and postnatal factors could further prevent additional cases,” the investigators concluded.
Find the full study in the BMJ (doi:10.1136/bmj.h3672).
A low birth weight and an unhealthy lifestyle increase risk of type 2 diabetes more than either factor alone, according to Dr. Yanping Li of Harvard T.H. Chan School of Public Health, Boston, and associates.
In a study of 11, 709 cases of type 2 diabetes, the odds ratio for type 2 diabetes as a result of low birth weight alone was 1.45 per kg under normal birth weight, and for unhealthy lifestyle alone, the OR was 2.1. When both factors were present, the OR increased significantly to 2.86.
If both factors were present, unhealthy lifestyle had significantly more impact on diabetes development, with 59% of the attributable proportion of joint effect, compared with just 22% for low birth weight and 18% for the interaction between the two.
“The finding suggests that most cases of type 2 diabetes could be prevented by the adoption of a healthier lifestyle, but simultaneous improvement of both prenatal and postnatal factors could further prevent additional cases,” the investigators concluded.
Find the full study in the BMJ (doi:10.1136/bmj.h3672).
Exclusionary guidelines keep many depressed patients out of clinical trials
The people likely to be prescribed antidepressants are very often excluded from antidepressant registration trials, according to Dr. Sheldon H. Preskorn and his associates.
Using the loosest guidelines for antidepressant registration trial (ART) exclusion, 82% of participants in the Sequenced Treatment Alternatives to Relieve Depression (STAR*D) study would not have been eligible had the study been structured like a normal ART. Of the eight normal inclusion/exclusion criteria, five eliminated more than 10% of the study population: age outside 18-65, Hamilton Depression Rating Scale score below 18, more than 2 months’ duration for current depressive episode, lack of appropriate contraception, and presence of a clinically significant or unstable general medical condition.
Other less significant exclusion criteria included use of disallowed concomitant medication, presence of an Axis II disorder, and suicidality.
“Failure to take these facts into consideration in advance before conducting a study can lead to lost revenue because of failure to develop what could be an effective medication as a result of unsuccessful trials, delays in bringing a drug to market, or the abandonment of this needed area of drug development altogether,” the investigators concluded.
Find the full study in the July issue of the Journal of Psychiatric Practice (J. Psychiatr. Pract. 2015;21:267-74).
The people likely to be prescribed antidepressants are very often excluded from antidepressant registration trials, according to Dr. Sheldon H. Preskorn and his associates.
Using the loosest guidelines for antidepressant registration trial (ART) exclusion, 82% of participants in the Sequenced Treatment Alternatives to Relieve Depression (STAR*D) study would not have been eligible had the study been structured like a normal ART. Of the eight normal inclusion/exclusion criteria, five eliminated more than 10% of the study population: age outside 18-65, Hamilton Depression Rating Scale score below 18, more than 2 months’ duration for current depressive episode, lack of appropriate contraception, and presence of a clinically significant or unstable general medical condition.
Other less significant exclusion criteria included use of disallowed concomitant medication, presence of an Axis II disorder, and suicidality.
“Failure to take these facts into consideration in advance before conducting a study can lead to lost revenue because of failure to develop what could be an effective medication as a result of unsuccessful trials, delays in bringing a drug to market, or the abandonment of this needed area of drug development altogether,” the investigators concluded.
Find the full study in the July issue of the Journal of Psychiatric Practice (J. Psychiatr. Pract. 2015;21:267-74).
The people likely to be prescribed antidepressants are very often excluded from antidepressant registration trials, according to Dr. Sheldon H. Preskorn and his associates.
Using the loosest guidelines for antidepressant registration trial (ART) exclusion, 82% of participants in the Sequenced Treatment Alternatives to Relieve Depression (STAR*D) study would not have been eligible had the study been structured like a normal ART. Of the eight normal inclusion/exclusion criteria, five eliminated more than 10% of the study population: age outside 18-65, Hamilton Depression Rating Scale score below 18, more than 2 months’ duration for current depressive episode, lack of appropriate contraception, and presence of a clinically significant or unstable general medical condition.
Other less significant exclusion criteria included use of disallowed concomitant medication, presence of an Axis II disorder, and suicidality.
“Failure to take these facts into consideration in advance before conducting a study can lead to lost revenue because of failure to develop what could be an effective medication as a result of unsuccessful trials, delays in bringing a drug to market, or the abandonment of this needed area of drug development altogether,” the investigators concluded.
Find the full study in the July issue of the Journal of Psychiatric Practice (J. Psychiatr. Pract. 2015;21:267-74).
HLA-matched sibling transplants provide best outcomes in infantile osteopetrosis
Long-term survival after hematopoietic stem cell transplantation for infantile osteopetrosis was highest when grafts were taken from human leukocyte antigen (HLA)-matched siblings, according to the largest cohort of patients with the disease that has been compiled to date.
For HLA-matched sibling transplants, 5- and 10-year survival probabilities were both 62%, whereas the combined average survival probability for HLA-mismatched relative donors, HLA-matched unrelated donors, and HLA-unmatched unrelated donors was 42% after 5 years and 39% after 10 years, Dr. Paul J. Orchard of the University of Minnesota, Minneapolis, and his colleagues reported.
Of surviving patients, 70% have visual impairment and 10% have auditory impairment and motor delay. Despite this, most survivors are attending a public or specialized school, and 65% of survivors reported performance scores of 90 or 100 at last contact, the investigators said.
Graft failure was the most common cause of death, occurring in 50% of HLA-matched sibling transplant patients and in 43% of alternative HLA transplant patients. Veno-occlusive disease and interstitial pneumonitis rates were also high, both at about 20%.
“There is an urgent need to improve engraftment by developing novel strategies that target the microenvironment and study the association between genetic variants of osteopetrosis and transplantation outcomes,” the researchers said.
Find the full article in the July 9 issue of Blood (Blood 2015;126:270-6).
Long-term survival after hematopoietic stem cell transplantation for infantile osteopetrosis was highest when grafts were taken from human leukocyte antigen (HLA)-matched siblings, according to the largest cohort of patients with the disease that has been compiled to date.
For HLA-matched sibling transplants, 5- and 10-year survival probabilities were both 62%, whereas the combined average survival probability for HLA-mismatched relative donors, HLA-matched unrelated donors, and HLA-unmatched unrelated donors was 42% after 5 years and 39% after 10 years, Dr. Paul J. Orchard of the University of Minnesota, Minneapolis, and his colleagues reported.
Of surviving patients, 70% have visual impairment and 10% have auditory impairment and motor delay. Despite this, most survivors are attending a public or specialized school, and 65% of survivors reported performance scores of 90 or 100 at last contact, the investigators said.
Graft failure was the most common cause of death, occurring in 50% of HLA-matched sibling transplant patients and in 43% of alternative HLA transplant patients. Veno-occlusive disease and interstitial pneumonitis rates were also high, both at about 20%.
“There is an urgent need to improve engraftment by developing novel strategies that target the microenvironment and study the association between genetic variants of osteopetrosis and transplantation outcomes,” the researchers said.
Find the full article in the July 9 issue of Blood (Blood 2015;126:270-6).
Long-term survival after hematopoietic stem cell transplantation for infantile osteopetrosis was highest when grafts were taken from human leukocyte antigen (HLA)-matched siblings, according to the largest cohort of patients with the disease that has been compiled to date.
For HLA-matched sibling transplants, 5- and 10-year survival probabilities were both 62%, whereas the combined average survival probability for HLA-mismatched relative donors, HLA-matched unrelated donors, and HLA-unmatched unrelated donors was 42% after 5 years and 39% after 10 years, Dr. Paul J. Orchard of the University of Minnesota, Minneapolis, and his colleagues reported.
Of surviving patients, 70% have visual impairment and 10% have auditory impairment and motor delay. Despite this, most survivors are attending a public or specialized school, and 65% of survivors reported performance scores of 90 or 100 at last contact, the investigators said.
Graft failure was the most common cause of death, occurring in 50% of HLA-matched sibling transplant patients and in 43% of alternative HLA transplant patients. Veno-occlusive disease and interstitial pneumonitis rates were also high, both at about 20%.
“There is an urgent need to improve engraftment by developing novel strategies that target the microenvironment and study the association between genetic variants of osteopetrosis and transplantation outcomes,” the researchers said.
Find the full article in the July 9 issue of Blood (Blood 2015;126:270-6).