User login
Lucas Franki is an associate editor for MDedge News, and has been with the company since 2014. He has a BA in English from Penn State University and is an Eagle Scout.
Assess heart disease risk with online calculators
About half of all Americans have at least one of the three leading risk factors for heart disease: high blood pressure, high low-density lipoprotein cholesterol, and a history of smoking. It is important to keep track of heart disease risks, both potential and real.
Online calculators can be very useful for patients concerned about their heart health. Many such calculators, such as this one from the Mayo Clinic, look at your general risk for heart disease and make recommendations as to lifestyle changes to reduce risk. But there are also calculators focused on specific conditions, such as coronary heart disease, heart attack, and stroke.
Remember that calculators are not a replacement for a real diagnosis. If you suspect you have heart disease, be sure to see a doctor, and if something serious occurs, a visit to the emergency department is certainly valid.
Find more heart disease risk calculators here.
About half of all Americans have at least one of the three leading risk factors for heart disease: high blood pressure, high low-density lipoprotein cholesterol, and a history of smoking. It is important to keep track of heart disease risks, both potential and real.
Online calculators can be very useful for patients concerned about their heart health. Many such calculators, such as this one from the Mayo Clinic, look at your general risk for heart disease and make recommendations as to lifestyle changes to reduce risk. But there are also calculators focused on specific conditions, such as coronary heart disease, heart attack, and stroke.
Remember that calculators are not a replacement for a real diagnosis. If you suspect you have heart disease, be sure to see a doctor, and if something serious occurs, a visit to the emergency department is certainly valid.
Find more heart disease risk calculators here.
About half of all Americans have at least one of the three leading risk factors for heart disease: high blood pressure, high low-density lipoprotein cholesterol, and a history of smoking. It is important to keep track of heart disease risks, both potential and real.
Online calculators can be very useful for patients concerned about their heart health. Many such calculators, such as this one from the Mayo Clinic, look at your general risk for heart disease and make recommendations as to lifestyle changes to reduce risk. But there are also calculators focused on specific conditions, such as coronary heart disease, heart attack, and stroke.
Remember that calculators are not a replacement for a real diagnosis. If you suspect you have heart disease, be sure to see a doctor, and if something serious occurs, a visit to the emergency department is certainly valid.
Find more heart disease risk calculators here.
HPV vaccination rates worst in white adolescents
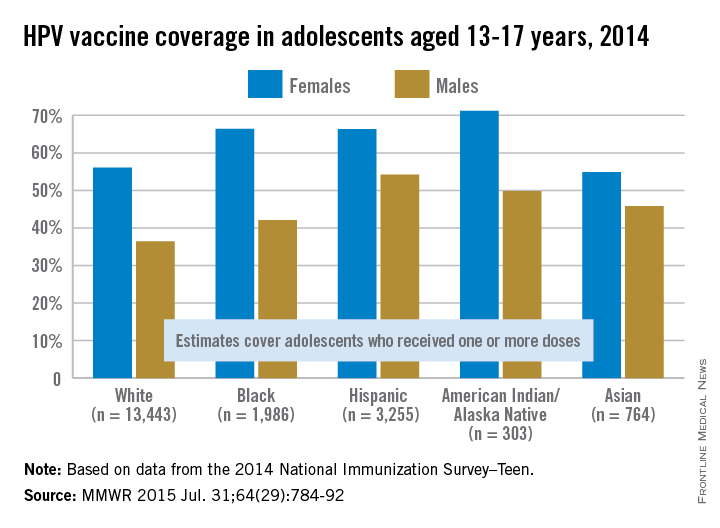
White, non-Hispanic adolescents had, on average, the lowest rate of human papillomavirus vaccination among measured ethnicities in 2014, according to a report from the Centers for Disease Control and Prevention.
Just over 36% of white adolescent males aged 13-17 years had received at least one HPV vaccine dose; 6% less than black, non-Hispanic males. Asian non-Hispanics had the lowest rate of vaccination among female adolescents at 55%, though the vaccination rate for white female adolescents was only slightly higher at 56%.
The highest rate of vaccination in male adolescents was in Hispanics at 54%, and in females, the highest rate was in American Indian/Alaska Native at 71%.
By state, Kansas had the lowest rate of HPV vaccination at 38%, followed by Mississippi at 46%. Rhode Island had the highest vaccination rate of any state at 76%, but the local areas of Philadelphia and Chicago surpassed it with vaccination rates of 80% and 78%, respectively. The state with the second highest vaccination rate was North Carolina at just over 71% (MMWR 2015 Jul.31;64(29):784-92).
As HPV coverage is significantly lower than other vaccinations, “routinely recommending HPV vaccination at ages 11-12 years during the same visit and with the same emphasis used for other vaccines is critical,” the CDC investigators said.
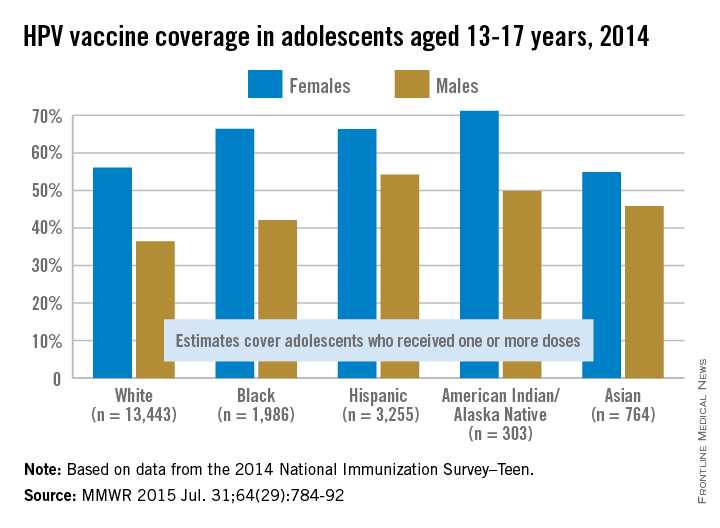
White, non-Hispanic adolescents had, on average, the lowest rate of human papillomavirus vaccination among measured ethnicities in 2014, according to a report from the Centers for Disease Control and Prevention.
Just over 36% of white adolescent males aged 13-17 years had received at least one HPV vaccine dose; 6% less than black, non-Hispanic males. Asian non-Hispanics had the lowest rate of vaccination among female adolescents at 55%, though the vaccination rate for white female adolescents was only slightly higher at 56%.
The highest rate of vaccination in male adolescents was in Hispanics at 54%, and in females, the highest rate was in American Indian/Alaska Native at 71%.
By state, Kansas had the lowest rate of HPV vaccination at 38%, followed by Mississippi at 46%. Rhode Island had the highest vaccination rate of any state at 76%, but the local areas of Philadelphia and Chicago surpassed it with vaccination rates of 80% and 78%, respectively. The state with the second highest vaccination rate was North Carolina at just over 71% (MMWR 2015 Jul.31;64(29):784-92).
As HPV coverage is significantly lower than other vaccinations, “routinely recommending HPV vaccination at ages 11-12 years during the same visit and with the same emphasis used for other vaccines is critical,” the CDC investigators said.

White, non-Hispanic adolescents had, on average, the lowest rate of human papillomavirus vaccination among measured ethnicities in 2014, according to a report from the Centers for Disease Control and Prevention.
Just over 36% of white adolescent males aged 13-17 years had received at least one HPV vaccine dose; 6% less than black, non-Hispanic males. Asian non-Hispanics had the lowest rate of vaccination among female adolescents at 55%, though the vaccination rate for white female adolescents was only slightly higher at 56%.
The highest rate of vaccination in male adolescents was in Hispanics at 54%, and in females, the highest rate was in American Indian/Alaska Native at 71%.
By state, Kansas had the lowest rate of HPV vaccination at 38%, followed by Mississippi at 46%. Rhode Island had the highest vaccination rate of any state at 76%, but the local areas of Philadelphia and Chicago surpassed it with vaccination rates of 80% and 78%, respectively. The state with the second highest vaccination rate was North Carolina at just over 71% (MMWR 2015 Jul.31;64(29):784-92).
As HPV coverage is significantly lower than other vaccinations, “routinely recommending HPV vaccination at ages 11-12 years during the same visit and with the same emphasis used for other vaccines is critical,” the CDC investigators said.

FROM THE MMWR
Schizophrenia patients’ insight benefits from parental understanding
Patients’ insight into schizophrenia is significantly associated with how their biologic parents view the illness, according to Dr. Alexandra Macgregor and her associates.
No association was found between patient and parent insight in any of the Scale to Assess Unawareness of Mental Disorder dimensions; however, an association was found between patients’ and parents’ treatment effect awareness when there was frequent contact between parents and patients. Low parental critical attitude and high parental cognition both were positively associated with patient insight, reported Dr. Macgregor of Montpellier University Hospital, France.
The study “is the first to suggest a possible influence of parental factors such as critical attitudes and cognitive performance on patient insight,” the investigators concluded. “Encouraging regular contact between patients and their family should be [an] objective of clinical teams.”
Find the full study in Psychiatry Research (2015 Aug 30;228:879-86).
Patients’ insight into schizophrenia is significantly associated with how their biologic parents view the illness, according to Dr. Alexandra Macgregor and her associates.
No association was found between patient and parent insight in any of the Scale to Assess Unawareness of Mental Disorder dimensions; however, an association was found between patients’ and parents’ treatment effect awareness when there was frequent contact between parents and patients. Low parental critical attitude and high parental cognition both were positively associated with patient insight, reported Dr. Macgregor of Montpellier University Hospital, France.
The study “is the first to suggest a possible influence of parental factors such as critical attitudes and cognitive performance on patient insight,” the investigators concluded. “Encouraging regular contact between patients and their family should be [an] objective of clinical teams.”
Find the full study in Psychiatry Research (2015 Aug 30;228:879-86).
Patients’ insight into schizophrenia is significantly associated with how their biologic parents view the illness, according to Dr. Alexandra Macgregor and her associates.
No association was found between patient and parent insight in any of the Scale to Assess Unawareness of Mental Disorder dimensions; however, an association was found between patients’ and parents’ treatment effect awareness when there was frequent contact between parents and patients. Low parental critical attitude and high parental cognition both were positively associated with patient insight, reported Dr. Macgregor of Montpellier University Hospital, France.
The study “is the first to suggest a possible influence of parental factors such as critical attitudes and cognitive performance on patient insight,” the investigators concluded. “Encouraging regular contact between patients and their family should be [an] objective of clinical teams.”
Find the full study in Psychiatry Research (2015 Aug 30;228:879-86).
Men who stay single after divorce are less depressed
Divorces are hard, and considering the mental health benefits of marriage over being single, getting married again would seem to make sense. Depression, however, is actually more likely in men who get remarried than in those who remain divorced, according to Ayako Hiyoshi, Ph.D., and associates.
In the study, the incidence of “pharmaceutically treated” depression from 2005 to 2009 was measured in a large group of Swedish males whose marriage status was recorded in 1985. Age in 1985 ranged from 29 to 33 years. For divorced men who got remarried, the adjusted odds ratio for depression was 1.27, compared with the baseline of men who remained divorced, reported Dr. Hiyoshi of Örebro (Sweden) University and associates.
The risk of depression was lowest in men who remained married during the entire study period (OR, 0.87). Men who divorced after 1985 and were still divorced had an almost identical depression risk (OR, 0.99) as those persistently divorced since 1985.
The investigators noted that not only do the results conflict with the general consensus that marriage improves quality of life, but traditional risk factors for depression, such as lower cognitive and physical function, lower stress resilience, and lower socioeconomic status, were less prevalent in the remarried group, compared with the persistently divorced group.
“This suggests that interpersonal or financial difficulties resulting from remarriage can outweigh the benefits of marriage,” they concluded.
Find the full study in Social Science and Medicine (2015;141:109-14 doi: 10.1016/j.socscimed.2015.07.029).
Divorces are hard, and considering the mental health benefits of marriage over being single, getting married again would seem to make sense. Depression, however, is actually more likely in men who get remarried than in those who remain divorced, according to Ayako Hiyoshi, Ph.D., and associates.
In the study, the incidence of “pharmaceutically treated” depression from 2005 to 2009 was measured in a large group of Swedish males whose marriage status was recorded in 1985. Age in 1985 ranged from 29 to 33 years. For divorced men who got remarried, the adjusted odds ratio for depression was 1.27, compared with the baseline of men who remained divorced, reported Dr. Hiyoshi of Örebro (Sweden) University and associates.
The risk of depression was lowest in men who remained married during the entire study period (OR, 0.87). Men who divorced after 1985 and were still divorced had an almost identical depression risk (OR, 0.99) as those persistently divorced since 1985.
The investigators noted that not only do the results conflict with the general consensus that marriage improves quality of life, but traditional risk factors for depression, such as lower cognitive and physical function, lower stress resilience, and lower socioeconomic status, were less prevalent in the remarried group, compared with the persistently divorced group.
“This suggests that interpersonal or financial difficulties resulting from remarriage can outweigh the benefits of marriage,” they concluded.
Find the full study in Social Science and Medicine (2015;141:109-14 doi: 10.1016/j.socscimed.2015.07.029).
Divorces are hard, and considering the mental health benefits of marriage over being single, getting married again would seem to make sense. Depression, however, is actually more likely in men who get remarried than in those who remain divorced, according to Ayako Hiyoshi, Ph.D., and associates.
In the study, the incidence of “pharmaceutically treated” depression from 2005 to 2009 was measured in a large group of Swedish males whose marriage status was recorded in 1985. Age in 1985 ranged from 29 to 33 years. For divorced men who got remarried, the adjusted odds ratio for depression was 1.27, compared with the baseline of men who remained divorced, reported Dr. Hiyoshi of Örebro (Sweden) University and associates.
The risk of depression was lowest in men who remained married during the entire study period (OR, 0.87). Men who divorced after 1985 and were still divorced had an almost identical depression risk (OR, 0.99) as those persistently divorced since 1985.
The investigators noted that not only do the results conflict with the general consensus that marriage improves quality of life, but traditional risk factors for depression, such as lower cognitive and physical function, lower stress resilience, and lower socioeconomic status, were less prevalent in the remarried group, compared with the persistently divorced group.
“This suggests that interpersonal or financial difficulties resulting from remarriage can outweigh the benefits of marriage,” they concluded.
Find the full study in Social Science and Medicine (2015;141:109-14 doi: 10.1016/j.socscimed.2015.07.029).
Study: Most young adults with diabetes neglect eye exams
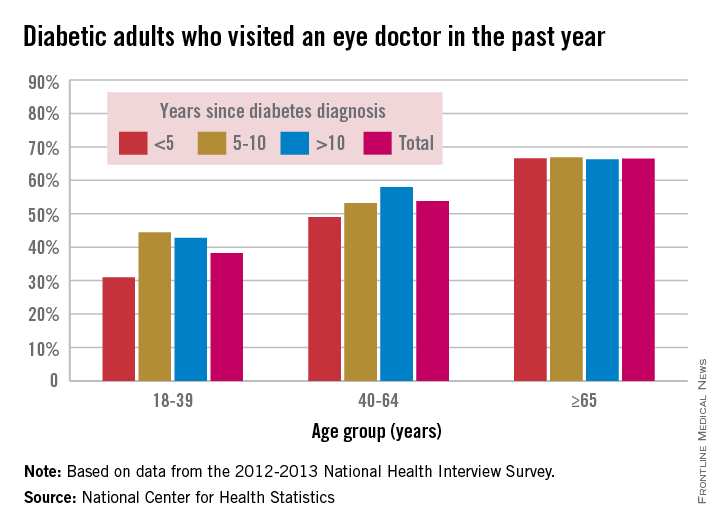
Adults younger than 40 years old who have diabetes were much less likely to have recently seen an eye doctor than were older adults during 2012-2013, especially if they had been diagnosed less than 5 years earlier, according to a report from the National Center for Health Statistics.
Among adults aged 18-39 years who had been diagnosed with diabetes in the previous 5 years, 31% had seen an eye doctor in the previous year, compared with 49% of adults aged 40-64 and about 67% of adults 65 and older. About 44% of 18- to 39-year-olds diagnosed 5-10 years earlier reported seeing an eye doctor recently, and just under 43% of 18- to 39-year olds diagnosed more than 10 years prior reported seeing an eye doctor in the past year, the researchers noted.

Adults aged 40-64 years who had been diagnosed more than 10 years prior were significantly more likely to have seen an eye doctor recently (58%) than were those diagnosed between 5 and 10 years earlier (53%). In adults 65 and older, between 66% and 67% had seen an eye doctor recently in all diagnosis groups, according to the report.
“Among adults with diabetes, both age and years since diagnosis may play a role in visiting an eye doctor in the past 12 months. However, the findings here show that the association between years since diagnosis and visiting an eye doctor in the past year may only hold for certain age groups, specifically adults aged 40-64,” wrote the NCHS researchers.
The NCHS used data collected for the 2012-2013 National Health Interview Survey.
Adults younger than 40 years old who have diabetes were much less likely to have recently seen an eye doctor than were older adults during 2012-2013, especially if they had been diagnosed less than 5 years earlier, according to a report from the National Center for Health Statistics.
Among adults aged 18-39 years who had been diagnosed with diabetes in the previous 5 years, 31% had seen an eye doctor in the previous year, compared with 49% of adults aged 40-64 and about 67% of adults 65 and older. About 44% of 18- to 39-year-olds diagnosed 5-10 years earlier reported seeing an eye doctor recently, and just under 43% of 18- to 39-year olds diagnosed more than 10 years prior reported seeing an eye doctor in the past year, the researchers noted.

Adults aged 40-64 years who had been diagnosed more than 10 years prior were significantly more likely to have seen an eye doctor recently (58%) than were those diagnosed between 5 and 10 years earlier (53%). In adults 65 and older, between 66% and 67% had seen an eye doctor recently in all diagnosis groups, according to the report.
“Among adults with diabetes, both age and years since diagnosis may play a role in visiting an eye doctor in the past 12 months. However, the findings here show that the association between years since diagnosis and visiting an eye doctor in the past year may only hold for certain age groups, specifically adults aged 40-64,” wrote the NCHS researchers.
The NCHS used data collected for the 2012-2013 National Health Interview Survey.
Adults younger than 40 years old who have diabetes were much less likely to have recently seen an eye doctor than were older adults during 2012-2013, especially if they had been diagnosed less than 5 years earlier, according to a report from the National Center for Health Statistics.
Among adults aged 18-39 years who had been diagnosed with diabetes in the previous 5 years, 31% had seen an eye doctor in the previous year, compared with 49% of adults aged 40-64 and about 67% of adults 65 and older. About 44% of 18- to 39-year-olds diagnosed 5-10 years earlier reported seeing an eye doctor recently, and just under 43% of 18- to 39-year olds diagnosed more than 10 years prior reported seeing an eye doctor in the past year, the researchers noted.

Adults aged 40-64 years who had been diagnosed more than 10 years prior were significantly more likely to have seen an eye doctor recently (58%) than were those diagnosed between 5 and 10 years earlier (53%). In adults 65 and older, between 66% and 67% had seen an eye doctor recently in all diagnosis groups, according to the report.
“Among adults with diabetes, both age and years since diagnosis may play a role in visiting an eye doctor in the past 12 months. However, the findings here show that the association between years since diagnosis and visiting an eye doctor in the past year may only hold for certain age groups, specifically adults aged 40-64,” wrote the NCHS researchers.
The NCHS used data collected for the 2012-2013 National Health Interview Survey.
Endovascular stents effective for iliofemoral obstructions in patients with PTS
Endovascular stenting is a safe and effective way to treat iliofemoral obstructions in patients with postthrombotic syndrome, according to Dr. M. Yin of Shanghai (China) JiaoTong University, and associates.
The stenting process was achieved without major complications in 95% of cases. Cumulative primary, assisted primary, and secondary patency rates after 3 years were 69%, 79%, and 92%, respectively. Patients with severe postthrombotic syndrome (PTS) saw a significant drop in their Villalta score, compared with patients treated with elastic compression stockings (ECS) therapy, though scores were similar in patients with moderate PTS in both groups. The 24-month recurrence-free ulcer healing rate was significantly higher in the stenting group (87% vs. 71%).
“ECS therapy shows equal clinical effects with stent placement in patients with moderate PTS,” but the stented patients did not have to wear stockings after the procedure, the researchers wrote.
Find the full study in the European Journal of Vascular & Endovascular Surgery (doi: 10.1016/j.ejvs.2015.03.029).
Endovascular stenting is a safe and effective way to treat iliofemoral obstructions in patients with postthrombotic syndrome, according to Dr. M. Yin of Shanghai (China) JiaoTong University, and associates.
The stenting process was achieved without major complications in 95% of cases. Cumulative primary, assisted primary, and secondary patency rates after 3 years were 69%, 79%, and 92%, respectively. Patients with severe postthrombotic syndrome (PTS) saw a significant drop in their Villalta score, compared with patients treated with elastic compression stockings (ECS) therapy, though scores were similar in patients with moderate PTS in both groups. The 24-month recurrence-free ulcer healing rate was significantly higher in the stenting group (87% vs. 71%).
“ECS therapy shows equal clinical effects with stent placement in patients with moderate PTS,” but the stented patients did not have to wear stockings after the procedure, the researchers wrote.
Find the full study in the European Journal of Vascular & Endovascular Surgery (doi: 10.1016/j.ejvs.2015.03.029).
Endovascular stenting is a safe and effective way to treat iliofemoral obstructions in patients with postthrombotic syndrome, according to Dr. M. Yin of Shanghai (China) JiaoTong University, and associates.
The stenting process was achieved without major complications in 95% of cases. Cumulative primary, assisted primary, and secondary patency rates after 3 years were 69%, 79%, and 92%, respectively. Patients with severe postthrombotic syndrome (PTS) saw a significant drop in their Villalta score, compared with patients treated with elastic compression stockings (ECS) therapy, though scores were similar in patients with moderate PTS in both groups. The 24-month recurrence-free ulcer healing rate was significantly higher in the stenting group (87% vs. 71%).
“ECS therapy shows equal clinical effects with stent placement in patients with moderate PTS,” but the stented patients did not have to wear stockings after the procedure, the researchers wrote.
Find the full study in the European Journal of Vascular & Endovascular Surgery (doi: 10.1016/j.ejvs.2015.03.029).
Esophagogastric cancer chemotherapy commonly causes VTE
Venous thromboembolism is common in patients undergoing oxaliplatin, capecitabine, and epirubicin chemotherapy for esophagogastric cancer, according to Dr. Anders Christian Larsen of Aalborg (Denmark) University Hospital and associates.
There were 21 cases of VTE among the 129 patients with esophagogastric cancer, a rate of 16%. Of the VTE cases, 14 were asymptomatic and 7 were symptomatic. Gastric cancer and late-stage cancer were significant VTE risk factors, with odds ratios of 6.4 and 5.2, respectively. The median survival time was 18 months in non-VTE patients and 14 months in VTE patients.
“The extent of treatment-related VTE in upper GI cancer patients (with active cancer) receiving both chemotherapy and curative intended surgery may be greater than previously estimated. … Our data demonstrate the need to address this clinical problem with randomized clinical trials on VTE prophylaxis, particularly in patients undergoing neoadjuvant chemotherapy for resectable cancer disease,” the investigators concluded.
The authors said that there were no conflicts; the study was funded by private foundations.
Find the full study in Thrombosis Research.
Venous thromboembolism is common in patients undergoing oxaliplatin, capecitabine, and epirubicin chemotherapy for esophagogastric cancer, according to Dr. Anders Christian Larsen of Aalborg (Denmark) University Hospital and associates.
There were 21 cases of VTE among the 129 patients with esophagogastric cancer, a rate of 16%. Of the VTE cases, 14 were asymptomatic and 7 were symptomatic. Gastric cancer and late-stage cancer were significant VTE risk factors, with odds ratios of 6.4 and 5.2, respectively. The median survival time was 18 months in non-VTE patients and 14 months in VTE patients.
“The extent of treatment-related VTE in upper GI cancer patients (with active cancer) receiving both chemotherapy and curative intended surgery may be greater than previously estimated. … Our data demonstrate the need to address this clinical problem with randomized clinical trials on VTE prophylaxis, particularly in patients undergoing neoadjuvant chemotherapy for resectable cancer disease,” the investigators concluded.
The authors said that there were no conflicts; the study was funded by private foundations.
Find the full study in Thrombosis Research.
Venous thromboembolism is common in patients undergoing oxaliplatin, capecitabine, and epirubicin chemotherapy for esophagogastric cancer, according to Dr. Anders Christian Larsen of Aalborg (Denmark) University Hospital and associates.
There were 21 cases of VTE among the 129 patients with esophagogastric cancer, a rate of 16%. Of the VTE cases, 14 were asymptomatic and 7 were symptomatic. Gastric cancer and late-stage cancer were significant VTE risk factors, with odds ratios of 6.4 and 5.2, respectively. The median survival time was 18 months in non-VTE patients and 14 months in VTE patients.
“The extent of treatment-related VTE in upper GI cancer patients (with active cancer) receiving both chemotherapy and curative intended surgery may be greater than previously estimated. … Our data demonstrate the need to address this clinical problem with randomized clinical trials on VTE prophylaxis, particularly in patients undergoing neoadjuvant chemotherapy for resectable cancer disease,” the investigators concluded.
The authors said that there were no conflicts; the study was funded by private foundations.
Find the full study in Thrombosis Research.
Physician targeted intervention fails to reduce maternal vaccine hesitancy
Maternal vaccine hesitancy and physician self-efficacy did not improve after using a physician-centered communication intervention program, according to Nora P. Henrikson, Ph.D., and her associates.
The investigators recruited mothers from four hospitals with obstetric services in Washington state. Members of the intervention group and the control group shared similar characteristics except for maternal race and ethnicity, reported Dr. Henrikson of the Group Health Research Institute in Seattle.
At the baseline measurement, 9.8% of mothers in the intervention group were hesitant about vaccines, compared with 12.6% in the control group. After the intervention, hesitancy in the intervention group was 7.5%, while in the control group, hesitancy was at 8%. The odds ratio for reduction of maternal hesitancy was 1.22.
Physician self-efficacy was significantly lower in the intervention group, with 58% reporting high confidence in talking about risk, 69% reporting high confidence in providing information, and 54% reporting high confidence in answering difficult parent questions. The rate for doctors in the control group was 70%, 81%, and 69%, respectively.
While a physician-targeted approach did not work, the study results must be the start, not the end, of the story to find an effective way to end vaccine hesitancy, Julie Leask, Ph.D., University of Sydney, Australia, and Dr. Paul Kinnersley, Cardiff University, Wales, wrote in a related editorial. Taking a tough stance with hesitant parents, while appealing to many doctors, “may reduce trust and possibly schedule completion in the longer term,” Dr. Leask and Dr. Kinnersley said.
“Billions of dollars fund the research and development of vaccines to ensure their efficacy and safety. There needs to be a proportional commitment to the ‘R&D’ of vaccine acceptance because vaccines are only effective if people willingly take them up,” Dr. Leask and Dr. Kinnersley concluded.
Find the full study in Pediatrics (2015 Jul;136:70-79. doi: 10.1542/peds.2014-3199) and editorial (2015 Jul;136:180-182. doi: 10.1542/peds.2015-1382).
Maternal vaccine hesitancy and physician self-efficacy did not improve after using a physician-centered communication intervention program, according to Nora P. Henrikson, Ph.D., and her associates.
The investigators recruited mothers from four hospitals with obstetric services in Washington state. Members of the intervention group and the control group shared similar characteristics except for maternal race and ethnicity, reported Dr. Henrikson of the Group Health Research Institute in Seattle.
At the baseline measurement, 9.8% of mothers in the intervention group were hesitant about vaccines, compared with 12.6% in the control group. After the intervention, hesitancy in the intervention group was 7.5%, while in the control group, hesitancy was at 8%. The odds ratio for reduction of maternal hesitancy was 1.22.
Physician self-efficacy was significantly lower in the intervention group, with 58% reporting high confidence in talking about risk, 69% reporting high confidence in providing information, and 54% reporting high confidence in answering difficult parent questions. The rate for doctors in the control group was 70%, 81%, and 69%, respectively.
While a physician-targeted approach did not work, the study results must be the start, not the end, of the story to find an effective way to end vaccine hesitancy, Julie Leask, Ph.D., University of Sydney, Australia, and Dr. Paul Kinnersley, Cardiff University, Wales, wrote in a related editorial. Taking a tough stance with hesitant parents, while appealing to many doctors, “may reduce trust and possibly schedule completion in the longer term,” Dr. Leask and Dr. Kinnersley said.
“Billions of dollars fund the research and development of vaccines to ensure their efficacy and safety. There needs to be a proportional commitment to the ‘R&D’ of vaccine acceptance because vaccines are only effective if people willingly take them up,” Dr. Leask and Dr. Kinnersley concluded.
Find the full study in Pediatrics (2015 Jul;136:70-79. doi: 10.1542/peds.2014-3199) and editorial (2015 Jul;136:180-182. doi: 10.1542/peds.2015-1382).
Maternal vaccine hesitancy and physician self-efficacy did not improve after using a physician-centered communication intervention program, according to Nora P. Henrikson, Ph.D., and her associates.
The investigators recruited mothers from four hospitals with obstetric services in Washington state. Members of the intervention group and the control group shared similar characteristics except for maternal race and ethnicity, reported Dr. Henrikson of the Group Health Research Institute in Seattle.
At the baseline measurement, 9.8% of mothers in the intervention group were hesitant about vaccines, compared with 12.6% in the control group. After the intervention, hesitancy in the intervention group was 7.5%, while in the control group, hesitancy was at 8%. The odds ratio for reduction of maternal hesitancy was 1.22.
Physician self-efficacy was significantly lower in the intervention group, with 58% reporting high confidence in talking about risk, 69% reporting high confidence in providing information, and 54% reporting high confidence in answering difficult parent questions. The rate for doctors in the control group was 70%, 81%, and 69%, respectively.
While a physician-targeted approach did not work, the study results must be the start, not the end, of the story to find an effective way to end vaccine hesitancy, Julie Leask, Ph.D., University of Sydney, Australia, and Dr. Paul Kinnersley, Cardiff University, Wales, wrote in a related editorial. Taking a tough stance with hesitant parents, while appealing to many doctors, “may reduce trust and possibly schedule completion in the longer term,” Dr. Leask and Dr. Kinnersley said.
“Billions of dollars fund the research and development of vaccines to ensure their efficacy and safety. There needs to be a proportional commitment to the ‘R&D’ of vaccine acceptance because vaccines are only effective if people willingly take them up,” Dr. Leask and Dr. Kinnersley concluded.
Find the full study in Pediatrics (2015 Jul;136:70-79. doi: 10.1542/peds.2014-3199) and editorial (2015 Jul;136:180-182. doi: 10.1542/peds.2015-1382).
Proglycem found to increase pulmonary hypertension risk in infants
Infants and newborns who have been treated with Proglycem (diazoxide) for low blood pressure are at risk for pulmonary hypertension, according to a press release from the Food and Drug Administration.
As Proglycem is usually given in a hospital setting, all babies receiving it should be closely monitored by a health care professional, especially if a risk factor for pulmonary hypertension is present, such as meconium aspiration syndrome, respiratory distress syndrome, transient tachypnea of the newborn, pneumonia, sepsis, congenital diaphragmatic hernia, and congenital heart disease, the FDA said.
The FDA identified 11 cases of pulmonary hypertension since Proglycem was approved in 1973. In all cases, pulmonary hypertension was stopped or was improved by stopping Proglycem treatment.
If a parent or caregiver notices any sign of difficulty breathing such as flaring nostrils, grunting, unusual movement of their child’s chest, rapid breathing, difficulty feeding, or a bluish color of the lips or skin, he or she should contact a doctor immediately, the FDA recommended.
“FDA is continuing to investigate this safety issue and will determine whether changes are needed in the Proglycem prescribing information,” the FDA said in the press release.
Infants and newborns who have been treated with Proglycem (diazoxide) for low blood pressure are at risk for pulmonary hypertension, according to a press release from the Food and Drug Administration.
As Proglycem is usually given in a hospital setting, all babies receiving it should be closely monitored by a health care professional, especially if a risk factor for pulmonary hypertension is present, such as meconium aspiration syndrome, respiratory distress syndrome, transient tachypnea of the newborn, pneumonia, sepsis, congenital diaphragmatic hernia, and congenital heart disease, the FDA said.
The FDA identified 11 cases of pulmonary hypertension since Proglycem was approved in 1973. In all cases, pulmonary hypertension was stopped or was improved by stopping Proglycem treatment.
If a parent or caregiver notices any sign of difficulty breathing such as flaring nostrils, grunting, unusual movement of their child’s chest, rapid breathing, difficulty feeding, or a bluish color of the lips or skin, he or she should contact a doctor immediately, the FDA recommended.
“FDA is continuing to investigate this safety issue and will determine whether changes are needed in the Proglycem prescribing information,” the FDA said in the press release.
Infants and newborns who have been treated with Proglycem (diazoxide) for low blood pressure are at risk for pulmonary hypertension, according to a press release from the Food and Drug Administration.
As Proglycem is usually given in a hospital setting, all babies receiving it should be closely monitored by a health care professional, especially if a risk factor for pulmonary hypertension is present, such as meconium aspiration syndrome, respiratory distress syndrome, transient tachypnea of the newborn, pneumonia, sepsis, congenital diaphragmatic hernia, and congenital heart disease, the FDA said.
The FDA identified 11 cases of pulmonary hypertension since Proglycem was approved in 1973. In all cases, pulmonary hypertension was stopped or was improved by stopping Proglycem treatment.
If a parent or caregiver notices any sign of difficulty breathing such as flaring nostrils, grunting, unusual movement of their child’s chest, rapid breathing, difficulty feeding, or a bluish color of the lips or skin, he or she should contact a doctor immediately, the FDA recommended.
“FDA is continuing to investigate this safety issue and will determine whether changes are needed in the Proglycem prescribing information,” the FDA said in the press release.
Poor MS relapse recovery may speed symptom progression
Patients with multiple sclerosis who recovered slowly from an early relapse developed progressive disease symptoms earlier than did those who recovered more quickly in a study of two MS patient cohorts, according to Dr. Martina Novotna and her associates.
The study involved a population-based cohort comprising 105 patients with relapsing-remitting MS and 86 with bout-onset progressive MS, defined as those with single-attack progressive or secondary progressive MS, and a clinic-based cohort of 415 patients with bout-onset progressive MS. Patients with primary progressive MS were excluded.
During the first 5 years after MS onset, about 80% of patients in the population-based cohort had good recovery (complete to almost-complete recovery based on patient-reported and examination-confirmed outcome measured at least 6 months post relapse), while about 16% had poor recovery. Among patients with a good recovery, half developed progressive MS 30.2 years after onset of MS, whereas half of those with a poor recovery had developed progressive symptoms only 8.3 years after MS onset.
In the clinic-based cohort, patients with good recovery developed progressive disease a mean of 4.7 years later than did those with poor recovery. Fulminant initial relapse was the most significant risk factor for poor recovery. Older age also put the patient at higher risk for a poor recovery from an early MS relapse, as did brainstem, cerebellar, or spinal cord involvement.
“Although multiple early relapses portend a worse prognosis than a single relapse [did], we found that even a single relapse associated with poor recovery may lead to rapid onset of progressive MS,” the investigators noted.
Find the full study in Neurology (doi:10.1212/WNL.0000000000001856).
Patients with multiple sclerosis who recovered slowly from an early relapse developed progressive disease symptoms earlier than did those who recovered more quickly in a study of two MS patient cohorts, according to Dr. Martina Novotna and her associates.
The study involved a population-based cohort comprising 105 patients with relapsing-remitting MS and 86 with bout-onset progressive MS, defined as those with single-attack progressive or secondary progressive MS, and a clinic-based cohort of 415 patients with bout-onset progressive MS. Patients with primary progressive MS were excluded.
During the first 5 years after MS onset, about 80% of patients in the population-based cohort had good recovery (complete to almost-complete recovery based on patient-reported and examination-confirmed outcome measured at least 6 months post relapse), while about 16% had poor recovery. Among patients with a good recovery, half developed progressive MS 30.2 years after onset of MS, whereas half of those with a poor recovery had developed progressive symptoms only 8.3 years after MS onset.
In the clinic-based cohort, patients with good recovery developed progressive disease a mean of 4.7 years later than did those with poor recovery. Fulminant initial relapse was the most significant risk factor for poor recovery. Older age also put the patient at higher risk for a poor recovery from an early MS relapse, as did brainstem, cerebellar, or spinal cord involvement.
“Although multiple early relapses portend a worse prognosis than a single relapse [did], we found that even a single relapse associated with poor recovery may lead to rapid onset of progressive MS,” the investigators noted.
Find the full study in Neurology (doi:10.1212/WNL.0000000000001856).
Patients with multiple sclerosis who recovered slowly from an early relapse developed progressive disease symptoms earlier than did those who recovered more quickly in a study of two MS patient cohorts, according to Dr. Martina Novotna and her associates.
The study involved a population-based cohort comprising 105 patients with relapsing-remitting MS and 86 with bout-onset progressive MS, defined as those with single-attack progressive or secondary progressive MS, and a clinic-based cohort of 415 patients with bout-onset progressive MS. Patients with primary progressive MS were excluded.
During the first 5 years after MS onset, about 80% of patients in the population-based cohort had good recovery (complete to almost-complete recovery based on patient-reported and examination-confirmed outcome measured at least 6 months post relapse), while about 16% had poor recovery. Among patients with a good recovery, half developed progressive MS 30.2 years after onset of MS, whereas half of those with a poor recovery had developed progressive symptoms only 8.3 years after MS onset.
In the clinic-based cohort, patients with good recovery developed progressive disease a mean of 4.7 years later than did those with poor recovery. Fulminant initial relapse was the most significant risk factor for poor recovery. Older age also put the patient at higher risk for a poor recovery from an early MS relapse, as did brainstem, cerebellar, or spinal cord involvement.
“Although multiple early relapses portend a worse prognosis than a single relapse [did], we found that even a single relapse associated with poor recovery may lead to rapid onset of progressive MS,” the investigators noted.
Find the full study in Neurology (doi:10.1212/WNL.0000000000001856).