User login
Healthy weight gain in pregnancy: What the USPSTF recommends
REFERENCES
- US Preventive Services Task Force. Behavioral counseling interventions for healthy weight and weight gain in pregnancy: US Preventive Services Task Force recommendation statement. JAMA. 2021;325:2087-2092. doi:10.1001/jama.2021.6949
- Rasmussen KM, Yaktine AL, eds. Weight Gain During Pregnancy: Reexamining the Guidelines. National Academies Press; 2009. doi: 10.17226/12584
REFERENCES
- US Preventive Services Task Force. Behavioral counseling interventions for healthy weight and weight gain in pregnancy: US Preventive Services Task Force recommendation statement. JAMA. 2021;325:2087-2092. doi:10.1001/jama.2021.6949
- Rasmussen KM, Yaktine AL, eds. Weight Gain During Pregnancy: Reexamining the Guidelines. National Academies Press; 2009. doi: 10.17226/12584
REFERENCES
- US Preventive Services Task Force. Behavioral counseling interventions for healthy weight and weight gain in pregnancy: US Preventive Services Task Force recommendation statement. JAMA. 2021;325:2087-2092. doi:10.1001/jama.2021.6949
- Rasmussen KM, Yaktine AL, eds. Weight Gain During Pregnancy: Reexamining the Guidelines. National Academies Press; 2009. doi: 10.17226/12584
COVID-19 vaccine update: Uptake, effectiveness, and safety concerns
REFERENCES
- CDC. COVID Data Tracker. Accessed June 3, 2021. https://covid.cdc.gov/covid-data-tracker/#datatracker-home
- WHO Coronavirus (COVID-19) Dashboard. Accessed June 3, 2021. https://covid19.who.int/
- CDC. Demographic trends of people receiving COVID-19 vaccinations in the United States. Accessed June 3, 2021. https://covid.cdc.gov/covid-data-tracker/#vaccination-demographics-trends
- Shimabukuro T. Update: thrombosis with thrombocytopenia syndrome (TTS) following COVID-19 vaccination. Presentation to the Advisory Committee on Immunization Practices, May 12, 2021. Accessed June 3, 2021. https://www.cdc.gov/vaccines/acip/meetings/downloads/slides-2021-05-12/07-COVID-Shimabukuro-508.pdf
- Fleming-Dutra K. CDC COVID-19 vaccine effectiveness studies. Presentation to the Advisory Committee on Immunization Practices, May 12, 2021. Accessed June 3, 2021. www.cdc.gov/vaccines/acip/meetings/downloads/slides-2021-05-12/09-COVID-Fleming-Dutra-508.pdf
- Scobie H. Update on emerging SARS-CoV-2 variants and vaccine considerations. Presentation to the Advisory Committee on Immunization Practices, May 12, 2021. Accessed June 3, 2021. www.cdc.gov/vaccines/acip/meetings/downloads/slides-2021-05-12/10-COVID-Scobie-508.pdf
REFERENCES
- CDC. COVID Data Tracker. Accessed June 3, 2021. https://covid.cdc.gov/covid-data-tracker/#datatracker-home
- WHO Coronavirus (COVID-19) Dashboard. Accessed June 3, 2021. https://covid19.who.int/
- CDC. Demographic trends of people receiving COVID-19 vaccinations in the United States. Accessed June 3, 2021. https://covid.cdc.gov/covid-data-tracker/#vaccination-demographics-trends
- Shimabukuro T. Update: thrombosis with thrombocytopenia syndrome (TTS) following COVID-19 vaccination. Presentation to the Advisory Committee on Immunization Practices, May 12, 2021. Accessed June 3, 2021. https://www.cdc.gov/vaccines/acip/meetings/downloads/slides-2021-05-12/07-COVID-Shimabukuro-508.pdf
- Fleming-Dutra K. CDC COVID-19 vaccine effectiveness studies. Presentation to the Advisory Committee on Immunization Practices, May 12, 2021. Accessed June 3, 2021. www.cdc.gov/vaccines/acip/meetings/downloads/slides-2021-05-12/09-COVID-Fleming-Dutra-508.pdf
- Scobie H. Update on emerging SARS-CoV-2 variants and vaccine considerations. Presentation to the Advisory Committee on Immunization Practices, May 12, 2021. Accessed June 3, 2021. www.cdc.gov/vaccines/acip/meetings/downloads/slides-2021-05-12/10-COVID-Scobie-508.pdf
REFERENCES
- CDC. COVID Data Tracker. Accessed June 3, 2021. https://covid.cdc.gov/covid-data-tracker/#datatracker-home
- WHO Coronavirus (COVID-19) Dashboard. Accessed June 3, 2021. https://covid19.who.int/
- CDC. Demographic trends of people receiving COVID-19 vaccinations in the United States. Accessed June 3, 2021. https://covid.cdc.gov/covid-data-tracker/#vaccination-demographics-trends
- Shimabukuro T. Update: thrombosis with thrombocytopenia syndrome (TTS) following COVID-19 vaccination. Presentation to the Advisory Committee on Immunization Practices, May 12, 2021. Accessed June 3, 2021. https://www.cdc.gov/vaccines/acip/meetings/downloads/slides-2021-05-12/07-COVID-Shimabukuro-508.pdf
- Fleming-Dutra K. CDC COVID-19 vaccine effectiveness studies. Presentation to the Advisory Committee on Immunization Practices, May 12, 2021. Accessed June 3, 2021. www.cdc.gov/vaccines/acip/meetings/downloads/slides-2021-05-12/09-COVID-Fleming-Dutra-508.pdf
- Scobie H. Update on emerging SARS-CoV-2 variants and vaccine considerations. Presentation to the Advisory Committee on Immunization Practices, May 12, 2021. Accessed June 3, 2021. www.cdc.gov/vaccines/acip/meetings/downloads/slides-2021-05-12/10-COVID-Scobie-508.pdf
USPSTF makes 2 major changes to its lung cancer screening recs
REFERENCES
- American Academy of Family Physicians. Lung cancer: lung cancer screening in adults. AAFP Clinical Preventive Service Recommendations. Accessed April 26, 2021. www.aafp.org/family-physician/patient-care/clinical-recommendations/all-clinical-recommendations/lung-cancer.html
- USPSTF. Screening for lung cancer: US Preventive Services Task Force recommendation statement. JAMA. 2021;325:962-970. doi:10.1001/jama.2021.1117
- Jonas DE, Reuland DS, Reddy, SM, et al. Screening for lung cancer with low-dose computed tomography: updated evidence report and systematic review for the US Preventive Services Task Force. JAMA. 2021;325:971-987. doi:10.1001/jama.2021.0377
- Henderson LM, Rivera MP, Basch E. Broadened eligibility for lung cancer screening: challenges and uncertainty for implementation and equity. JAMA. 2021;325:939-941. doi:10.1001/jama.2020.26422
- Meza R, Jeon J, Toumazis I, et al. Evaluation of the benefits and harms of lung cancer screening with low-dose computed tomography: modeling study for the US Preventive Services Task Force. JAMA. 2021;325:988-997. doi:10.1001/jama.2021.1077
REFERENCES
- American Academy of Family Physicians. Lung cancer: lung cancer screening in adults. AAFP Clinical Preventive Service Recommendations. Accessed April 26, 2021. www.aafp.org/family-physician/patient-care/clinical-recommendations/all-clinical-recommendations/lung-cancer.html
- USPSTF. Screening for lung cancer: US Preventive Services Task Force recommendation statement. JAMA. 2021;325:962-970. doi:10.1001/jama.2021.1117
- Jonas DE, Reuland DS, Reddy, SM, et al. Screening for lung cancer with low-dose computed tomography: updated evidence report and systematic review for the US Preventive Services Task Force. JAMA. 2021;325:971-987. doi:10.1001/jama.2021.0377
- Henderson LM, Rivera MP, Basch E. Broadened eligibility for lung cancer screening: challenges and uncertainty for implementation and equity. JAMA. 2021;325:939-941. doi:10.1001/jama.2020.26422
- Meza R, Jeon J, Toumazis I, et al. Evaluation of the benefits and harms of lung cancer screening with low-dose computed tomography: modeling study for the US Preventive Services Task Force. JAMA. 2021;325:988-997. doi:10.1001/jama.2021.1077
REFERENCES
- American Academy of Family Physicians. Lung cancer: lung cancer screening in adults. AAFP Clinical Preventive Service Recommendations. Accessed April 26, 2021. www.aafp.org/family-physician/patient-care/clinical-recommendations/all-clinical-recommendations/lung-cancer.html
- USPSTF. Screening for lung cancer: US Preventive Services Task Force recommendation statement. JAMA. 2021;325:962-970. doi:10.1001/jama.2021.1117
- Jonas DE, Reuland DS, Reddy, SM, et al. Screening for lung cancer with low-dose computed tomography: updated evidence report and systematic review for the US Preventive Services Task Force. JAMA. 2021;325:971-987. doi:10.1001/jama.2021.0377
- Henderson LM, Rivera MP, Basch E. Broadened eligibility for lung cancer screening: challenges and uncertainty for implementation and equity. JAMA. 2021;325:939-941. doi:10.1001/jama.2020.26422
- Meza R, Jeon J, Toumazis I, et al. Evaluation of the benefits and harms of lung cancer screening with low-dose computed tomography: modeling study for the US Preventive Services Task Force. JAMA. 2021;325:988-997. doi:10.1001/jama.2021.1077
CDC’s new gonorrhea treatment recs: What’s changed, and when to retest
REFERENCES
- CDC. Expedited partner therapy. Accessed March 15, 2021. www.cdc.gov/std/ept/default.htm
- St. Cyr S, Barbee L, Workowski KA, et al. Update to CDC's treatment guidelines for gonococcal infection, 2020. MMWR Morbid Mortal Wkly Rep. 2020;69:1911-1916. Accessed March 15, 2021. https://www.cdc.gov/mmwr/volumes/69/wr/mm6950a6.htm
- CDC. Gonococcal infections. Accessed March 15, 2021. www.cdc.gov/std/tg2015/gonorrhea.htm
REFERENCES
- CDC. Expedited partner therapy. Accessed March 15, 2021. www.cdc.gov/std/ept/default.htm
- St. Cyr S, Barbee L, Workowski KA, et al. Update to CDC's treatment guidelines for gonococcal infection, 2020. MMWR Morbid Mortal Wkly Rep. 2020;69:1911-1916. Accessed March 15, 2021. https://www.cdc.gov/mmwr/volumes/69/wr/mm6950a6.htm
- CDC. Gonococcal infections. Accessed March 15, 2021. www.cdc.gov/std/tg2015/gonorrhea.htm
REFERENCES
- CDC. Expedited partner therapy. Accessed March 15, 2021. www.cdc.gov/std/ept/default.htm
- St. Cyr S, Barbee L, Workowski KA, et al. Update to CDC's treatment guidelines for gonococcal infection, 2020. MMWR Morbid Mortal Wkly Rep. 2020;69:1911-1916. Accessed March 15, 2021. https://www.cdc.gov/mmwr/volumes/69/wr/mm6950a6.htm
- CDC. Gonococcal infections. Accessed March 15, 2021. www.cdc.gov/std/tg2015/gonorrhea.htm
COVID-19 vaccines: New candidates & answers to commonly asked questions
REFERENCES
- CDC. COVID-19 vaccination. Accessed February 22, 2021.
- CDC. COVID data tracker. Accessed February 22, 2021.
- Oliver SE, Gargano JW, Marin M, et al. The Advisory Committee on Immunization Practices’ interim recommendation for use of Pfizer-BioNTech COVID-19 vaccine—United States, December 2020. MMWR Morbid Mortal Wkly Rep. 2020;69:1922-1924. Accessed February 22, 2021.
- Oliver SE, Gargano JW, Marin M, et al. The Advisory Committee on Immunization Practices’ interim recommendation for use of Moderna COVID-19 vaccine—United States, December 2020. MMWR Morbid Mortal Wkly Rep. 2021;69:1653-1656. Accessed February 22, 2021.
- Gee J, Marquez P, Su J, et al. First month of COVID-19 vaccine safety monitoring—United States, December 14, 2020–January 13, 2021. MMWR Morbid Mortal Wkly Rep. ePub: February 19, 2021. Accessed February 22, 2021.
- CDC COVID-19 Response Team; Food and Drug Administration. Allergic reactions including anaphylaxis after receipt of the first dose of Moderna COVID-19 vaccine—United States, December 21, 2020–January 10, 2021. MMWR Morb Mortal Wkly Rep. 2021;70:125-129. Accessed February 25, 2021.
REFERENCES
- CDC. COVID-19 vaccination. Accessed February 22, 2021.
- CDC. COVID data tracker. Accessed February 22, 2021.
- Oliver SE, Gargano JW, Marin M, et al. The Advisory Committee on Immunization Practices’ interim recommendation for use of Pfizer-BioNTech COVID-19 vaccine—United States, December 2020. MMWR Morbid Mortal Wkly Rep. 2020;69:1922-1924. Accessed February 22, 2021.
- Oliver SE, Gargano JW, Marin M, et al. The Advisory Committee on Immunization Practices’ interim recommendation for use of Moderna COVID-19 vaccine—United States, December 2020. MMWR Morbid Mortal Wkly Rep. 2021;69:1653-1656. Accessed February 22, 2021.
- Gee J, Marquez P, Su J, et al. First month of COVID-19 vaccine safety monitoring—United States, December 14, 2020–January 13, 2021. MMWR Morbid Mortal Wkly Rep. ePub: February 19, 2021. Accessed February 22, 2021.
- CDC COVID-19 Response Team; Food and Drug Administration. Allergic reactions including anaphylaxis after receipt of the first dose of Moderna COVID-19 vaccine—United States, December 21, 2020–January 10, 2021. MMWR Morb Mortal Wkly Rep. 2021;70:125-129. Accessed February 25, 2021.
REFERENCES
- CDC. COVID-19 vaccination. Accessed February 22, 2021.
- CDC. COVID data tracker. Accessed February 22, 2021.
- Oliver SE, Gargano JW, Marin M, et al. The Advisory Committee on Immunization Practices’ interim recommendation for use of Pfizer-BioNTech COVID-19 vaccine—United States, December 2020. MMWR Morbid Mortal Wkly Rep. 2020;69:1922-1924. Accessed February 22, 2021.
- Oliver SE, Gargano JW, Marin M, et al. The Advisory Committee on Immunization Practices’ interim recommendation for use of Moderna COVID-19 vaccine—United States, December 2020. MMWR Morbid Mortal Wkly Rep. 2021;69:1653-1656. Accessed February 22, 2021.
- Gee J, Marquez P, Su J, et al. First month of COVID-19 vaccine safety monitoring—United States, December 14, 2020–January 13, 2021. MMWR Morbid Mortal Wkly Rep. ePub: February 19, 2021. Accessed February 22, 2021.
- CDC COVID-19 Response Team; Food and Drug Administration. Allergic reactions including anaphylaxis after receipt of the first dose of Moderna COVID-19 vaccine—United States, December 21, 2020–January 10, 2021. MMWR Morb Mortal Wkly Rep. 2021;70:125-129. Accessed February 25, 2021.
COVID-19 vaccines: The rollout, the risks, and the reason to still wear a mask
REFERENCES
- Oliver SE, Gargano JW, Marin M; et al. The Advisory Committee on Immunization Practices’ interim recommendation for use of Pfizer-BioNTech COVID-19 vaccine—United States, December 2020. MMWR Morbid Mortal Wkly Rep. 2020;69:1922-1924. Accessed January 13, 2021. www.cdc.gov/mmwr/volumes/69/wr/mm6950e2.htm
- 2. Oliver SE, Gargano JW, Marin M; et al. The Advisory Committee on Immunization Practices’ interim recommendation for use of Moderna COVID-19 vaccine—United States, December 2020. MMWR Morbid Mortal Wkly Rep. 2021;69:1653-1656. Accessed January 13, 2021. www.cdc.gov/mmwr/volumes/69/wr/mm695152e1.htm
- CDC. COVID-19 vaccines: update on allergic reactions, contraindications, and precautions [webinar]. December 30, 2020. Accessed January 6, 2021. https://emergency.cdc.gov/coca/calls/2020/callinfo_123020.asp
- CDC. What clinicians need to know about the Pfizer-BioNTech and Moderna COVID-19 vaccines [webinar]. December 18, 2020. Accessed January 6, 2021. https://emergency.cdc.gov/coca/calls/2020/callinfo_121820.asp
- CDC COVID-19 Response Team; Food and Drug Administration. Allergic reactions including anaphylaxis after receipt of the first dose of Pfizer-BioNTech COVID-19 vaccine—United States, December 14-23, 2020. MMWR Morb Mortal Wkly Rep. ePub: January 6, 2021. Accessed January 13, 2021. www.cdc.gov/mmwr/volumes/70/wr/mm7002e1.htm
REFERENCES
- Oliver SE, Gargano JW, Marin M; et al. The Advisory Committee on Immunization Practices’ interim recommendation for use of Pfizer-BioNTech COVID-19 vaccine—United States, December 2020. MMWR Morbid Mortal Wkly Rep. 2020;69:1922-1924. Accessed January 13, 2021. www.cdc.gov/mmwr/volumes/69/wr/mm6950e2.htm
- 2. Oliver SE, Gargano JW, Marin M; et al. The Advisory Committee on Immunization Practices’ interim recommendation for use of Moderna COVID-19 vaccine—United States, December 2020. MMWR Morbid Mortal Wkly Rep. 2021;69:1653-1656. Accessed January 13, 2021. www.cdc.gov/mmwr/volumes/69/wr/mm695152e1.htm
- CDC. COVID-19 vaccines: update on allergic reactions, contraindications, and precautions [webinar]. December 30, 2020. Accessed January 6, 2021. https://emergency.cdc.gov/coca/calls/2020/callinfo_123020.asp
- CDC. What clinicians need to know about the Pfizer-BioNTech and Moderna COVID-19 vaccines [webinar]. December 18, 2020. Accessed January 6, 2021. https://emergency.cdc.gov/coca/calls/2020/callinfo_121820.asp
- CDC COVID-19 Response Team; Food and Drug Administration. Allergic reactions including anaphylaxis after receipt of the first dose of Pfizer-BioNTech COVID-19 vaccine—United States, December 14-23, 2020. MMWR Morb Mortal Wkly Rep. ePub: January 6, 2021. Accessed January 13, 2021. www.cdc.gov/mmwr/volumes/70/wr/mm7002e1.htm
REFERENCES
- Oliver SE, Gargano JW, Marin M; et al. The Advisory Committee on Immunization Practices’ interim recommendation for use of Pfizer-BioNTech COVID-19 vaccine—United States, December 2020. MMWR Morbid Mortal Wkly Rep. 2020;69:1922-1924. Accessed January 13, 2021. www.cdc.gov/mmwr/volumes/69/wr/mm6950e2.htm
- 2. Oliver SE, Gargano JW, Marin M; et al. The Advisory Committee on Immunization Practices’ interim recommendation for use of Moderna COVID-19 vaccine—United States, December 2020. MMWR Morbid Mortal Wkly Rep. 2021;69:1653-1656. Accessed January 13, 2021. www.cdc.gov/mmwr/volumes/69/wr/mm695152e1.htm
- CDC. COVID-19 vaccines: update on allergic reactions, contraindications, and precautions [webinar]. December 30, 2020. Accessed January 6, 2021. https://emergency.cdc.gov/coca/calls/2020/callinfo_123020.asp
- CDC. What clinicians need to know about the Pfizer-BioNTech and Moderna COVID-19 vaccines [webinar]. December 18, 2020. Accessed January 6, 2021. https://emergency.cdc.gov/coca/calls/2020/callinfo_121820.asp
- CDC COVID-19 Response Team; Food and Drug Administration. Allergic reactions including anaphylaxis after receipt of the first dose of Pfizer-BioNTech COVID-19 vaccine—United States, December 14-23, 2020. MMWR Morb Mortal Wkly Rep. ePub: January 6, 2021. Accessed January 13, 2021. www.cdc.gov/mmwr/volumes/70/wr/mm7002e1.htm
Consider C. difficile early in children with cancer with GI symptoms
Children with cancer are at increased risk of potentially life-threatening Clostridioides difficile infections (CDI), and Brianna Murphy, DO, reported at the annual meeting of the European Society for Paediatric Infectious Diseases, held virtually this year.
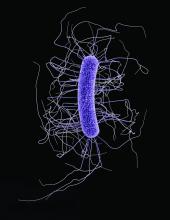
CDI are characterized by diarrhea, fever, and loss of appetite. The clinical features are caused by the release of toxins A and B by this gram-positive bacterium. In pediatric groups, CDI are a leading cause of antibiotic-associated gastric illness. This in turn can lead to a protracted stay in hospital and increases risk of mortality. The rising incidence in the United States over the last 2 decades prompted Dr. Murphy, a pediatric hematology oncology fellow working at the department of pediatric research at the University of Texas MD Anderson Cancer Center, Houston, to investigate further. A search of the literature found limited information regarding CDI and pediatric oncology patients.
Recognized factors for contracting CDI include the presence of other illnesses, a weakened immune system because of drugs or disease, enteral nutrition, usage of medicines such as proton pump inhibitors which decrease gastric acid production, and classically, treatment with broad spectrum antibiotics.
Dr. Murphy’s study included patients aged 1-18 years, all of whom had a cancer diagnosis and a positive stool culture for C. difficile. Presenting symptoms were three or more loose stools per day or acute onset ileus. The study evaluated data for the years 2000-2017 and included 11,366 children; 207 CDI (0.98%) cases were identified among pediatric oncology patients during the study period. This compares with historical data showing an incidence of 0.14% among hospitalized children in general.
Malignancy data were then subdivided into three groups: hematologic, nonneural solid tumors (NNST), and neural tumors. Hematologic malignancies had a CDI prevalence higher than the average for oncologic patients at 5.4%. Inside this group those suffering with acute myeloid leukemia had a rate of 10.5%. In the NNST and neural tumor groups, CDI rates were lower and closer to the overall average.
Dr. Murphy then looked at her patient population in more detail. Poor clinical outcomes (PCOs) were defined as severe, refractory, recurrent, or multiple infections. Severe CDI included features such as toxic megacolon, gastrointestinal perforation, or need for surgical intervention. Refractory CDI were defined as continuation of symptoms beyond 7 days of appropriate therapy, and recurrent CDI were classed as reinfection within 8 weeks of a previous CDI. Ultimately, 51% of patients in this study died. Patients with severe CDI experienced increased mortality (P = .02). There was no difference shown when looking at the type of cancer, age, gender, or patient ethnicity.
Next, Dr. Murphy looked for associations. Hematologic and biochemical testing identified that elevated creatinine was statistically associated with the likelihood of PCOs, compared with leukocytosis and neutropenia, particularly in the NNST group. Treatment modality also was studied. Here radiation therapy was the only treatment shown to increase PCOs in patients with CDI. One-fifth (22%) of radiation therapy recipients experienced multiple CDI, compared with 12% of the total population.
In commenting on her paper, Louis Bent, MD, from the Netherlands raised the issue of deaths in septic patients. What was the origin of the responsible organism, for example from the GI tract or from central lines, and were patients receiving appropriate antibiotic treatment?
Dr. Kelly responded that sepsis was generally believed to occur as a result of infection with mixed bacterial translocation through the bowel wall, notably Escherichia coli. Patients were usually on a cocktail of antibiotics targeting CDI, but also other infections illustrating the serious nature of the situation.
Dr. Murphy had no financial conflicts of interest to declare.
Children with cancer are at increased risk of potentially life-threatening Clostridioides difficile infections (CDI), and Brianna Murphy, DO, reported at the annual meeting of the European Society for Paediatric Infectious Diseases, held virtually this year.
CDI are characterized by diarrhea, fever, and loss of appetite. The clinical features are caused by the release of toxins A and B by this gram-positive bacterium. In pediatric groups, CDI are a leading cause of antibiotic-associated gastric illness. This in turn can lead to a protracted stay in hospital and increases risk of mortality. The rising incidence in the United States over the last 2 decades prompted Dr. Murphy, a pediatric hematology oncology fellow working at the department of pediatric research at the University of Texas MD Anderson Cancer Center, Houston, to investigate further. A search of the literature found limited information regarding CDI and pediatric oncology patients.
Recognized factors for contracting CDI include the presence of other illnesses, a weakened immune system because of drugs or disease, enteral nutrition, usage of medicines such as proton pump inhibitors which decrease gastric acid production, and classically, treatment with broad spectrum antibiotics.
Dr. Murphy’s study included patients aged 1-18 years, all of whom had a cancer diagnosis and a positive stool culture for C. difficile. Presenting symptoms were three or more loose stools per day or acute onset ileus. The study evaluated data for the years 2000-2017 and included 11,366 children; 207 CDI (0.98%) cases were identified among pediatric oncology patients during the study period. This compares with historical data showing an incidence of 0.14% among hospitalized children in general.
Malignancy data were then subdivided into three groups: hematologic, nonneural solid tumors (NNST), and neural tumors. Hematologic malignancies had a CDI prevalence higher than the average for oncologic patients at 5.4%. Inside this group those suffering with acute myeloid leukemia had a rate of 10.5%. In the NNST and neural tumor groups, CDI rates were lower and closer to the overall average.
Dr. Murphy then looked at her patient population in more detail. Poor clinical outcomes (PCOs) were defined as severe, refractory, recurrent, or multiple infections. Severe CDI included features such as toxic megacolon, gastrointestinal perforation, or need for surgical intervention. Refractory CDI were defined as continuation of symptoms beyond 7 days of appropriate therapy, and recurrent CDI were classed as reinfection within 8 weeks of a previous CDI. Ultimately, 51% of patients in this study died. Patients with severe CDI experienced increased mortality (P = .02). There was no difference shown when looking at the type of cancer, age, gender, or patient ethnicity.
Next, Dr. Murphy looked for associations. Hematologic and biochemical testing identified that elevated creatinine was statistically associated with the likelihood of PCOs, compared with leukocytosis and neutropenia, particularly in the NNST group. Treatment modality also was studied. Here radiation therapy was the only treatment shown to increase PCOs in patients with CDI. One-fifth (22%) of radiation therapy recipients experienced multiple CDI, compared with 12% of the total population.
In commenting on her paper, Louis Bent, MD, from the Netherlands raised the issue of deaths in septic patients. What was the origin of the responsible organism, for example from the GI tract or from central lines, and were patients receiving appropriate antibiotic treatment?
Dr. Kelly responded that sepsis was generally believed to occur as a result of infection with mixed bacterial translocation through the bowel wall, notably Escherichia coli. Patients were usually on a cocktail of antibiotics targeting CDI, but also other infections illustrating the serious nature of the situation.
Dr. Murphy had no financial conflicts of interest to declare.
Children with cancer are at increased risk of potentially life-threatening Clostridioides difficile infections (CDI), and Brianna Murphy, DO, reported at the annual meeting of the European Society for Paediatric Infectious Diseases, held virtually this year.
CDI are characterized by diarrhea, fever, and loss of appetite. The clinical features are caused by the release of toxins A and B by this gram-positive bacterium. In pediatric groups, CDI are a leading cause of antibiotic-associated gastric illness. This in turn can lead to a protracted stay in hospital and increases risk of mortality. The rising incidence in the United States over the last 2 decades prompted Dr. Murphy, a pediatric hematology oncology fellow working at the department of pediatric research at the University of Texas MD Anderson Cancer Center, Houston, to investigate further. A search of the literature found limited information regarding CDI and pediatric oncology patients.
Recognized factors for contracting CDI include the presence of other illnesses, a weakened immune system because of drugs or disease, enteral nutrition, usage of medicines such as proton pump inhibitors which decrease gastric acid production, and classically, treatment with broad spectrum antibiotics.
Dr. Murphy’s study included patients aged 1-18 years, all of whom had a cancer diagnosis and a positive stool culture for C. difficile. Presenting symptoms were three or more loose stools per day or acute onset ileus. The study evaluated data for the years 2000-2017 and included 11,366 children; 207 CDI (0.98%) cases were identified among pediatric oncology patients during the study period. This compares with historical data showing an incidence of 0.14% among hospitalized children in general.
Malignancy data were then subdivided into three groups: hematologic, nonneural solid tumors (NNST), and neural tumors. Hematologic malignancies had a CDI prevalence higher than the average for oncologic patients at 5.4%. Inside this group those suffering with acute myeloid leukemia had a rate of 10.5%. In the NNST and neural tumor groups, CDI rates were lower and closer to the overall average.
Dr. Murphy then looked at her patient population in more detail. Poor clinical outcomes (PCOs) were defined as severe, refractory, recurrent, or multiple infections. Severe CDI included features such as toxic megacolon, gastrointestinal perforation, or need for surgical intervention. Refractory CDI were defined as continuation of symptoms beyond 7 days of appropriate therapy, and recurrent CDI were classed as reinfection within 8 weeks of a previous CDI. Ultimately, 51% of patients in this study died. Patients with severe CDI experienced increased mortality (P = .02). There was no difference shown when looking at the type of cancer, age, gender, or patient ethnicity.
Next, Dr. Murphy looked for associations. Hematologic and biochemical testing identified that elevated creatinine was statistically associated with the likelihood of PCOs, compared with leukocytosis and neutropenia, particularly in the NNST group. Treatment modality also was studied. Here radiation therapy was the only treatment shown to increase PCOs in patients with CDI. One-fifth (22%) of radiation therapy recipients experienced multiple CDI, compared with 12% of the total population.
In commenting on her paper, Louis Bent, MD, from the Netherlands raised the issue of deaths in septic patients. What was the origin of the responsible organism, for example from the GI tract or from central lines, and were patients receiving appropriate antibiotic treatment?
Dr. Kelly responded that sepsis was generally believed to occur as a result of infection with mixed bacterial translocation through the bowel wall, notably Escherichia coli. Patients were usually on a cocktail of antibiotics targeting CDI, but also other infections illustrating the serious nature of the situation.
Dr. Murphy had no financial conflicts of interest to declare.
FROM ESPID 2020
Colorectal cancer screening: The new draft recs & the cost to screen
References
- US Preventive Services Task Force. Colorectal cancer: screening [draft recommendation statement]. https://uspreventiveservicestaskforce.org/uspstf/draft-recommendation/colorectal-cancer-screening3. Published October 27, 2020. Accessed November 23, 2020.
References
- US Preventive Services Task Force. Colorectal cancer: screening [draft recommendation statement]. https://uspreventiveservicestaskforce.org/uspstf/draft-recommendation/colorectal-cancer-screening3. Published October 27, 2020. Accessed November 23, 2020.
References
- US Preventive Services Task Force. Colorectal cancer: screening [draft recommendation statement]. https://uspreventiveservicestaskforce.org/uspstf/draft-recommendation/colorectal-cancer-screening3. Published October 27, 2020. Accessed November 23, 2020.
COVID-19 treatment: What the NIH recommends
References
- National Institute of Health. Coronavirus Disease 2019 (COVID-19) Treatment Guidelines. www.covid19treatmentguidelines.nih.gov/. Updated October 22, 2020. Accessed October 28, 2020.
References
- National Institute of Health. Coronavirus Disease 2019 (COVID-19) Treatment Guidelines. www.covid19treatmentguidelines.nih.gov/. Updated October 22, 2020. Accessed October 28, 2020.
References
- National Institute of Health. Coronavirus Disease 2019 (COVID-19) Treatment Guidelines. www.covid19treatmentguidelines.nih.gov/. Updated October 22, 2020. Accessed October 28, 2020.
Study offers reassurance to postmenopausal women taking hormone therapy
References
- Chlebowski RT, Anderson GL, Aragaki AK, et al. Association of menopausal hormone therapy with breast cancer incidence and mortality during long-term follow-up of the Women’s Health Initiative randomized clinical trials. JAMA. 2020;32:369-380.
- The North American Menopause Society. Menopause Guidebook. 8th ed. www.menopause.org/publications/consumer-publications/-em-menopause-guidebook-em-8th-edition. Accessed September 25, 2020.
- US Preventive Services Task Force; Grossman DC, Curry SJ, Owens DK, et al. Hormone therapy for the primary prevention of chronic conditions in postmenopausal women: US Preventive Services Task Force Recommendation Statement. JAMA. 2017;318:2224-2233.
References
- Chlebowski RT, Anderson GL, Aragaki AK, et al. Association of menopausal hormone therapy with breast cancer incidence and mortality during long-term follow-up of the Women’s Health Initiative randomized clinical trials. JAMA. 2020;32:369-380.
- The North American Menopause Society. Menopause Guidebook. 8th ed. www.menopause.org/publications/consumer-publications/-em-menopause-guidebook-em-8th-edition. Accessed September 25, 2020.
- US Preventive Services Task Force; Grossman DC, Curry SJ, Owens DK, et al. Hormone therapy for the primary prevention of chronic conditions in postmenopausal women: US Preventive Services Task Force Recommendation Statement. JAMA. 2017;318:2224-2233.
References
- Chlebowski RT, Anderson GL, Aragaki AK, et al. Association of menopausal hormone therapy with breast cancer incidence and mortality during long-term follow-up of the Women’s Health Initiative randomized clinical trials. JAMA. 2020;32:369-380.
- The North American Menopause Society. Menopause Guidebook. 8th ed. www.menopause.org/publications/consumer-publications/-em-menopause-guidebook-em-8th-edition. Accessed September 25, 2020.
- US Preventive Services Task Force; Grossman DC, Curry SJ, Owens DK, et al. Hormone therapy for the primary prevention of chronic conditions in postmenopausal women: US Preventive Services Task Force Recommendation Statement. JAMA. 2017;318:2224-2233.