User login
A one-size-fits-all fenestrated graft for iliac aneurysms?
CHICAGO – A novel bifurcated covered stent graft limb that uses an off-the-shelf graft can treat large common iliac aneurysms, while preserving good pelvic blood flow.
The alternative endovascular approach has been performed on 15 patients since April 2011, with a success rate of 100%. Bilateral stent grafts were placed in four patients.
The all-male cohort has been able to maintain appropriate exercise tolerance and remains free from erectile dysfunction, pelvic ischemia, buttock claudication, and paralysis.
"These people do well," extremely well, Dr. Patrick Kelly said at the annual meeting of the Midwestern Vascular Surgical Society*.
Several iliac branch grafts are currently under investigation, including the Cook Zenith Branch iliac endovascular graft. They promise to preserve flow to the internal iliac artery and thus reduce the potential for ischemic sequelae resulting from iliac embolization. Depending on patient anatomy, however, the internal iliac may become jailed upon deployment of the main body graft, said Dr. Kelly of Sanford Health, Sioux Falls, S.D. The fenestrated systems are also limited by bridging stent technology and the relatively short bridging stent.
His alternative modified bifurcated limb divides the common iliac flow into the internal and external iliac arteries, while excluding the common iliac artery aneurysm.
"The pros are that it uses an off the shelf [graft], should be able to handle virtually any anatomy, can be used to treat either existing EVAR [endovascular aneurysm repair] or previous open repairs, and has multiple off-ramps, so you don’t jail yourself," he said. "The cons: It requires arm access – although I’m not sure that’s a con – and it requires three stents."
Operative details
The bifurcated limb is created by sewing an 8-mm and 10-mm covered stent graft to the distal end of a standard 16 x 20 x 82-mm stent graft limb. The distal ends of both the 8-mm and 10-mm grafts are left free, allowing flexibility and easier selection of the internal iliac artery, he said.
Once the graft is resheathed using a spiral wire technique, a traditional infrarenal abdominal aneurysm repair is performed. In order to exclude the common iliac aneurysm, the graft is oriented with the 8-mm limb toward the internal iliac and with the distal end of the 8-mm limb being deployed 2-3 cm above the origin of the internal iliac artery. The internal iliac artery is selected from an arm approach, through the 8-mm limb of the bifurcated stent graft limb.
Angiograms are performed and a 3-cm covered, self-expanding bridge stent graft is deployed. The 10-mm limb is used to extend the graft into the external iliac, thus completing exclusion of the common iliac aneurysm, while preserving both the internal and external iliac arteries, Dr. Kelly said.
Thus far, occlusion of the external iliac artery has been reported in one patient, and there were no recurring endoleaks. There was a type-3 endoleak between the main body and bridging stent that was visible on diagnostic angiography, but it resolved after being reballooned and patent flow was established upon completion angiography, Dr. Kelly explained. There was also a retrograde fill that was fixed 1 year postoperatively by extending the limb to obtain a healthy seal.
The average patient age was 65.4 years (range, 46-87 years); fluoroscopy time, 46 minutes (range, 29-91 minutes); and average length of stay 3.1 days (range, 1-9 days).
This compares with an average hospital stay of 4-7 days for the tried-and-true method of open aneurysm repair, which has bleeding rates of 30% or more, colonic ischemia in 20%-30%, and paraplegia in 2%-3%, Dr. Kelly noted.
Audience reaction
Dr. Rebecca Kelso of the Cleveland Clinic, who comoderated the session, was enthusiastic about the novel approach.
"The potential for it is quite significant, because the other main competitive device he mentioned that’s on the market still has anatomic limitations for use," she said in an interview. "So if he has something that can be used in any patient, no matter what the circumstances, well then that has significant implications for being available commercially for everyone."
Fellow moderator Dr. Patrick J. Geraghty of Washington University, St. Louis, remarked that while the approach uses a standardized graft, it is somewhat tailored since the length and the diameter of the Bivon grafts extending into the external and internal iliac arteries can be chosen separately. That said, the one-size-fits-all approach is particularly appealing because it could simplify treatment planning and reduce treatment delays.
"If you have a patient who is symptomatic and you have an off-the-shelf component, you could potentially treat them within the next 24 hours," he said in an interview. "The current turnaround time for the fenestrated system is about a month or so, so it would shorten treatment delays and might lead to a broader application of the technology."
A potentially shorter hospital length of stay could also reduce hospital costs, Dr. Kelso noted.
While the audience appeared equally enthusiastic about the results, some members questioned whether results on a physician-modified graft without an Investigational Device Exemption (IDE) should be presented at the meeting in light of recent warnings by the U.S. Food and Drug Administration that such interventions involve the use of significant-risk devices and need to be conducted under an IDE. Dr. Kelly responded that he is currently working with the FDA to obtain an IDE.
Earlier this year, the Society of Thoracic Surgeons and the American College of Cardiology became the first medical societies to receive an IDE to study alternative access for transcatheter aortic valve replacement using the STS/ACC TVT Registry
Dr. Kelly and Dr. Kelso reported having no financial disclosures. Dr. Geraghty disclosed relationships with Cook Medical and Bard/Lutonix.
*CORRECTION, 10/29/2013: An earlier version of this article misstated the name of the annual meeting of the Midwestern Vascular Surgical Society.
Vascular surgeons are like cobblers – we try to make the perfect pair of shoes for each customer. While all aneurysm operations are similar in principle, in reality each successful operation depends on a unique blend of surgical skill and experience applied to the individual anatomy of each patient. By combining endovascular and open surgical skills, vascular surgeons are enticed to develop ever more innovative solutions for complex problems. Dr. Kelly should be congratulated for thinking outside the box and applying his imagination and skill to the solution of this common clinical scenario. While I am intrigued by the technique, I will reserve my enthusiastic endorsement because of the relatively high cost and the fact the common iliac artery must be sufficiently large to accommodate the physician-modified bifurcated graft. Others have described the use of "stacked" Gore Excluder device to achieve a similar result. And the Cook Iliac Branched Device is nearing approval. In the long run, the FDA needs to adopt policies that encourage rather discourage innovation in the development of novel surgical treatments. The current onerous IDE process is excessively complex and expensive. Physician-modified endografts fill an important gap in our ability to deliver quality, customized care for every patient. And there is no evidence that innovation in vascular surgery has been harmful to patients. After all, every operation is "physician modified."
Dr. John F. Eidt is a vascular surgeon at the Greenville (South Carolina) Health System, and an associate medical editor for Vascular Specialist.
Vascular surgeons are like cobblers – we try to make the perfect pair of shoes for each customer. While all aneurysm operations are similar in principle, in reality each successful operation depends on a unique blend of surgical skill and experience applied to the individual anatomy of each patient. By combining endovascular and open surgical skills, vascular surgeons are enticed to develop ever more innovative solutions for complex problems. Dr. Kelly should be congratulated for thinking outside the box and applying his imagination and skill to the solution of this common clinical scenario. While I am intrigued by the technique, I will reserve my enthusiastic endorsement because of the relatively high cost and the fact the common iliac artery must be sufficiently large to accommodate the physician-modified bifurcated graft. Others have described the use of "stacked" Gore Excluder device to achieve a similar result. And the Cook Iliac Branched Device is nearing approval. In the long run, the FDA needs to adopt policies that encourage rather discourage innovation in the development of novel surgical treatments. The current onerous IDE process is excessively complex and expensive. Physician-modified endografts fill an important gap in our ability to deliver quality, customized care for every patient. And there is no evidence that innovation in vascular surgery has been harmful to patients. After all, every operation is "physician modified."
Dr. John F. Eidt is a vascular surgeon at the Greenville (South Carolina) Health System, and an associate medical editor for Vascular Specialist.
Vascular surgeons are like cobblers – we try to make the perfect pair of shoes for each customer. While all aneurysm operations are similar in principle, in reality each successful operation depends on a unique blend of surgical skill and experience applied to the individual anatomy of each patient. By combining endovascular and open surgical skills, vascular surgeons are enticed to develop ever more innovative solutions for complex problems. Dr. Kelly should be congratulated for thinking outside the box and applying his imagination and skill to the solution of this common clinical scenario. While I am intrigued by the technique, I will reserve my enthusiastic endorsement because of the relatively high cost and the fact the common iliac artery must be sufficiently large to accommodate the physician-modified bifurcated graft. Others have described the use of "stacked" Gore Excluder device to achieve a similar result. And the Cook Iliac Branched Device is nearing approval. In the long run, the FDA needs to adopt policies that encourage rather discourage innovation in the development of novel surgical treatments. The current onerous IDE process is excessively complex and expensive. Physician-modified endografts fill an important gap in our ability to deliver quality, customized care for every patient. And there is no evidence that innovation in vascular surgery has been harmful to patients. After all, every operation is "physician modified."
Dr. John F. Eidt is a vascular surgeon at the Greenville (South Carolina) Health System, and an associate medical editor for Vascular Specialist.
CHICAGO – A novel bifurcated covered stent graft limb that uses an off-the-shelf graft can treat large common iliac aneurysms, while preserving good pelvic blood flow.
The alternative endovascular approach has been performed on 15 patients since April 2011, with a success rate of 100%. Bilateral stent grafts were placed in four patients.
The all-male cohort has been able to maintain appropriate exercise tolerance and remains free from erectile dysfunction, pelvic ischemia, buttock claudication, and paralysis.
"These people do well," extremely well, Dr. Patrick Kelly said at the annual meeting of the Midwestern Vascular Surgical Society*.
Several iliac branch grafts are currently under investigation, including the Cook Zenith Branch iliac endovascular graft. They promise to preserve flow to the internal iliac artery and thus reduce the potential for ischemic sequelae resulting from iliac embolization. Depending on patient anatomy, however, the internal iliac may become jailed upon deployment of the main body graft, said Dr. Kelly of Sanford Health, Sioux Falls, S.D. The fenestrated systems are also limited by bridging stent technology and the relatively short bridging stent.
His alternative modified bifurcated limb divides the common iliac flow into the internal and external iliac arteries, while excluding the common iliac artery aneurysm.
"The pros are that it uses an off the shelf [graft], should be able to handle virtually any anatomy, can be used to treat either existing EVAR [endovascular aneurysm repair] or previous open repairs, and has multiple off-ramps, so you don’t jail yourself," he said. "The cons: It requires arm access – although I’m not sure that’s a con – and it requires three stents."
Operative details
The bifurcated limb is created by sewing an 8-mm and 10-mm covered stent graft to the distal end of a standard 16 x 20 x 82-mm stent graft limb. The distal ends of both the 8-mm and 10-mm grafts are left free, allowing flexibility and easier selection of the internal iliac artery, he said.
Once the graft is resheathed using a spiral wire technique, a traditional infrarenal abdominal aneurysm repair is performed. In order to exclude the common iliac aneurysm, the graft is oriented with the 8-mm limb toward the internal iliac and with the distal end of the 8-mm limb being deployed 2-3 cm above the origin of the internal iliac artery. The internal iliac artery is selected from an arm approach, through the 8-mm limb of the bifurcated stent graft limb.
Angiograms are performed and a 3-cm covered, self-expanding bridge stent graft is deployed. The 10-mm limb is used to extend the graft into the external iliac, thus completing exclusion of the common iliac aneurysm, while preserving both the internal and external iliac arteries, Dr. Kelly said.
Thus far, occlusion of the external iliac artery has been reported in one patient, and there were no recurring endoleaks. There was a type-3 endoleak between the main body and bridging stent that was visible on diagnostic angiography, but it resolved after being reballooned and patent flow was established upon completion angiography, Dr. Kelly explained. There was also a retrograde fill that was fixed 1 year postoperatively by extending the limb to obtain a healthy seal.
The average patient age was 65.4 years (range, 46-87 years); fluoroscopy time, 46 minutes (range, 29-91 minutes); and average length of stay 3.1 days (range, 1-9 days).
This compares with an average hospital stay of 4-7 days for the tried-and-true method of open aneurysm repair, which has bleeding rates of 30% or more, colonic ischemia in 20%-30%, and paraplegia in 2%-3%, Dr. Kelly noted.
Audience reaction
Dr. Rebecca Kelso of the Cleveland Clinic, who comoderated the session, was enthusiastic about the novel approach.
"The potential for it is quite significant, because the other main competitive device he mentioned that’s on the market still has anatomic limitations for use," she said in an interview. "So if he has something that can be used in any patient, no matter what the circumstances, well then that has significant implications for being available commercially for everyone."
Fellow moderator Dr. Patrick J. Geraghty of Washington University, St. Louis, remarked that while the approach uses a standardized graft, it is somewhat tailored since the length and the diameter of the Bivon grafts extending into the external and internal iliac arteries can be chosen separately. That said, the one-size-fits-all approach is particularly appealing because it could simplify treatment planning and reduce treatment delays.
"If you have a patient who is symptomatic and you have an off-the-shelf component, you could potentially treat them within the next 24 hours," he said in an interview. "The current turnaround time for the fenestrated system is about a month or so, so it would shorten treatment delays and might lead to a broader application of the technology."
A potentially shorter hospital length of stay could also reduce hospital costs, Dr. Kelso noted.
While the audience appeared equally enthusiastic about the results, some members questioned whether results on a physician-modified graft without an Investigational Device Exemption (IDE) should be presented at the meeting in light of recent warnings by the U.S. Food and Drug Administration that such interventions involve the use of significant-risk devices and need to be conducted under an IDE. Dr. Kelly responded that he is currently working with the FDA to obtain an IDE.
Earlier this year, the Society of Thoracic Surgeons and the American College of Cardiology became the first medical societies to receive an IDE to study alternative access for transcatheter aortic valve replacement using the STS/ACC TVT Registry
Dr. Kelly and Dr. Kelso reported having no financial disclosures. Dr. Geraghty disclosed relationships with Cook Medical and Bard/Lutonix.
*CORRECTION, 10/29/2013: An earlier version of this article misstated the name of the annual meeting of the Midwestern Vascular Surgical Society.
CHICAGO – A novel bifurcated covered stent graft limb that uses an off-the-shelf graft can treat large common iliac aneurysms, while preserving good pelvic blood flow.
The alternative endovascular approach has been performed on 15 patients since April 2011, with a success rate of 100%. Bilateral stent grafts were placed in four patients.
The all-male cohort has been able to maintain appropriate exercise tolerance and remains free from erectile dysfunction, pelvic ischemia, buttock claudication, and paralysis.
"These people do well," extremely well, Dr. Patrick Kelly said at the annual meeting of the Midwestern Vascular Surgical Society*.
Several iliac branch grafts are currently under investigation, including the Cook Zenith Branch iliac endovascular graft. They promise to preserve flow to the internal iliac artery and thus reduce the potential for ischemic sequelae resulting from iliac embolization. Depending on patient anatomy, however, the internal iliac may become jailed upon deployment of the main body graft, said Dr. Kelly of Sanford Health, Sioux Falls, S.D. The fenestrated systems are also limited by bridging stent technology and the relatively short bridging stent.
His alternative modified bifurcated limb divides the common iliac flow into the internal and external iliac arteries, while excluding the common iliac artery aneurysm.
"The pros are that it uses an off the shelf [graft], should be able to handle virtually any anatomy, can be used to treat either existing EVAR [endovascular aneurysm repair] or previous open repairs, and has multiple off-ramps, so you don’t jail yourself," he said. "The cons: It requires arm access – although I’m not sure that’s a con – and it requires three stents."
Operative details
The bifurcated limb is created by sewing an 8-mm and 10-mm covered stent graft to the distal end of a standard 16 x 20 x 82-mm stent graft limb. The distal ends of both the 8-mm and 10-mm grafts are left free, allowing flexibility and easier selection of the internal iliac artery, he said.
Once the graft is resheathed using a spiral wire technique, a traditional infrarenal abdominal aneurysm repair is performed. In order to exclude the common iliac aneurysm, the graft is oriented with the 8-mm limb toward the internal iliac and with the distal end of the 8-mm limb being deployed 2-3 cm above the origin of the internal iliac artery. The internal iliac artery is selected from an arm approach, through the 8-mm limb of the bifurcated stent graft limb.
Angiograms are performed and a 3-cm covered, self-expanding bridge stent graft is deployed. The 10-mm limb is used to extend the graft into the external iliac, thus completing exclusion of the common iliac aneurysm, while preserving both the internal and external iliac arteries, Dr. Kelly said.
Thus far, occlusion of the external iliac artery has been reported in one patient, and there were no recurring endoleaks. There was a type-3 endoleak between the main body and bridging stent that was visible on diagnostic angiography, but it resolved after being reballooned and patent flow was established upon completion angiography, Dr. Kelly explained. There was also a retrograde fill that was fixed 1 year postoperatively by extending the limb to obtain a healthy seal.
The average patient age was 65.4 years (range, 46-87 years); fluoroscopy time, 46 minutes (range, 29-91 minutes); and average length of stay 3.1 days (range, 1-9 days).
This compares with an average hospital stay of 4-7 days for the tried-and-true method of open aneurysm repair, which has bleeding rates of 30% or more, colonic ischemia in 20%-30%, and paraplegia in 2%-3%, Dr. Kelly noted.
Audience reaction
Dr. Rebecca Kelso of the Cleveland Clinic, who comoderated the session, was enthusiastic about the novel approach.
"The potential for it is quite significant, because the other main competitive device he mentioned that’s on the market still has anatomic limitations for use," she said in an interview. "So if he has something that can be used in any patient, no matter what the circumstances, well then that has significant implications for being available commercially for everyone."
Fellow moderator Dr. Patrick J. Geraghty of Washington University, St. Louis, remarked that while the approach uses a standardized graft, it is somewhat tailored since the length and the diameter of the Bivon grafts extending into the external and internal iliac arteries can be chosen separately. That said, the one-size-fits-all approach is particularly appealing because it could simplify treatment planning and reduce treatment delays.
"If you have a patient who is symptomatic and you have an off-the-shelf component, you could potentially treat them within the next 24 hours," he said in an interview. "The current turnaround time for the fenestrated system is about a month or so, so it would shorten treatment delays and might lead to a broader application of the technology."
A potentially shorter hospital length of stay could also reduce hospital costs, Dr. Kelso noted.
While the audience appeared equally enthusiastic about the results, some members questioned whether results on a physician-modified graft without an Investigational Device Exemption (IDE) should be presented at the meeting in light of recent warnings by the U.S. Food and Drug Administration that such interventions involve the use of significant-risk devices and need to be conducted under an IDE. Dr. Kelly responded that he is currently working with the FDA to obtain an IDE.
Earlier this year, the Society of Thoracic Surgeons and the American College of Cardiology became the first medical societies to receive an IDE to study alternative access for transcatheter aortic valve replacement using the STS/ACC TVT Registry
Dr. Kelly and Dr. Kelso reported having no financial disclosures. Dr. Geraghty disclosed relationships with Cook Medical and Bard/Lutonix.
*CORRECTION, 10/29/2013: An earlier version of this article misstated the name of the annual meeting of the Midwestern Vascular Surgical Society.
THE ANNUAL MEETING OF THE MIDWESTERN VASCULAR SURGICAL SOCIETY
Major finding: All patients are able to maintain appropriate exercise tolerance and are free of erectile dysfunction, pelvic ischemia, buttock claudication, and paralysis.
Data source: Two-year experience with a physician-modified fenestrated graft in 15 men with abdominal and iliac aneurysm.
Disclosures: Dr. Kelly and Dr. Kelso reported having no financial disclosures. Dr. Geraghty disclosed relationships with Cook Medical and Bard/Lutonix.
Laparoscopic colon surgery may keep older patients independent longer
WASHINGTON – Elderly patients who undergo laparoscopic colon surgery are significantly more likely to be discharged back to their homes than to a long-term care facility.
In a retrospective study of almost 10,000 elderly patients, 12.5% of those who had a laparoscopic procedure went to a nursing home, compared with 20% of those who had open surgery. In a multivariate analysis, laparoscopic surgery was associated with a significant, 39% decrease in the risk of being discharged to a nursing home, Dr. Richard Liu said at the annual clinical congress of the American College of Surgeons.
"For patients in their early 70s who do not have advanced disease or significant comorbidities, laparoscopic colon cancer resection is an option not only to prolong survival but also to preserve quality of life," said Dr. Liu, a surgical resident at Dalhousie University, Halifax, N.S.
The study highlights some important differences in the ways surgeons and patients perceive surgical outcomes. Surgeons and researchers often focus on 5-year survival rates and short-term morbidity and mortality, Dr. Liu said. But prior research done by his group found that immediate quality of life was at least as important to elderly patients – and sometimes more so.
"We have looked at elderly patients in our emergency services and followed up with them several times after admission," he said in an interview. "A common theme that came up was quality of life after hospitalization. Some were actually refusing to have operations for fear of what might become of them afterward."
Dr. Liu’s study comprised 9,416 patients from the U.S. National Inpatient Sample database. All were older than 70 years (mean age 79) and all were living independently at home. They underwent elective colon surgery during 2009-2010 for either cancer or a resection. The primary outcome was discharge back to home or to a long-term care facility. None of the patients were discharged to home health care or to hospice.
Most of the group (61%) had open surgery; the remainder had laparoscopy. Of those who had open surgery, 20% were discharged to a nursing facility, compared with 12.5% of the laparoscopy group – a significant difference.
Laparoscopy significantly decreased the chance of a nursing home admission by 39% in a multivariate analysis that controlled for age, sex, race, comorbidity score, cancer stage, income and insurance, and hospital size.
Factors significantly associated with nursing home discharge included advancing age and cancer stage.
Generally speaking, open surgery is physically more trying for elderly patients. A difficult recovery could be just enough to tip them over the edge from independent living, Dr. Liu said.
Dr. Liu had no financial disclosures.
WASHINGTON – Elderly patients who undergo laparoscopic colon surgery are significantly more likely to be discharged back to their homes than to a long-term care facility.
In a retrospective study of almost 10,000 elderly patients, 12.5% of those who had a laparoscopic procedure went to a nursing home, compared with 20% of those who had open surgery. In a multivariate analysis, laparoscopic surgery was associated with a significant, 39% decrease in the risk of being discharged to a nursing home, Dr. Richard Liu said at the annual clinical congress of the American College of Surgeons.
"For patients in their early 70s who do not have advanced disease or significant comorbidities, laparoscopic colon cancer resection is an option not only to prolong survival but also to preserve quality of life," said Dr. Liu, a surgical resident at Dalhousie University, Halifax, N.S.
The study highlights some important differences in the ways surgeons and patients perceive surgical outcomes. Surgeons and researchers often focus on 5-year survival rates and short-term morbidity and mortality, Dr. Liu said. But prior research done by his group found that immediate quality of life was at least as important to elderly patients – and sometimes more so.
"We have looked at elderly patients in our emergency services and followed up with them several times after admission," he said in an interview. "A common theme that came up was quality of life after hospitalization. Some were actually refusing to have operations for fear of what might become of them afterward."
Dr. Liu’s study comprised 9,416 patients from the U.S. National Inpatient Sample database. All were older than 70 years (mean age 79) and all were living independently at home. They underwent elective colon surgery during 2009-2010 for either cancer or a resection. The primary outcome was discharge back to home or to a long-term care facility. None of the patients were discharged to home health care or to hospice.
Most of the group (61%) had open surgery; the remainder had laparoscopy. Of those who had open surgery, 20% were discharged to a nursing facility, compared with 12.5% of the laparoscopy group – a significant difference.
Laparoscopy significantly decreased the chance of a nursing home admission by 39% in a multivariate analysis that controlled for age, sex, race, comorbidity score, cancer stage, income and insurance, and hospital size.
Factors significantly associated with nursing home discharge included advancing age and cancer stage.
Generally speaking, open surgery is physically more trying for elderly patients. A difficult recovery could be just enough to tip them over the edge from independent living, Dr. Liu said.
Dr. Liu had no financial disclosures.
WASHINGTON – Elderly patients who undergo laparoscopic colon surgery are significantly more likely to be discharged back to their homes than to a long-term care facility.
In a retrospective study of almost 10,000 elderly patients, 12.5% of those who had a laparoscopic procedure went to a nursing home, compared with 20% of those who had open surgery. In a multivariate analysis, laparoscopic surgery was associated with a significant, 39% decrease in the risk of being discharged to a nursing home, Dr. Richard Liu said at the annual clinical congress of the American College of Surgeons.
"For patients in their early 70s who do not have advanced disease or significant comorbidities, laparoscopic colon cancer resection is an option not only to prolong survival but also to preserve quality of life," said Dr. Liu, a surgical resident at Dalhousie University, Halifax, N.S.
The study highlights some important differences in the ways surgeons and patients perceive surgical outcomes. Surgeons and researchers often focus on 5-year survival rates and short-term morbidity and mortality, Dr. Liu said. But prior research done by his group found that immediate quality of life was at least as important to elderly patients – and sometimes more so.
"We have looked at elderly patients in our emergency services and followed up with them several times after admission," he said in an interview. "A common theme that came up was quality of life after hospitalization. Some were actually refusing to have operations for fear of what might become of them afterward."
Dr. Liu’s study comprised 9,416 patients from the U.S. National Inpatient Sample database. All were older than 70 years (mean age 79) and all were living independently at home. They underwent elective colon surgery during 2009-2010 for either cancer or a resection. The primary outcome was discharge back to home or to a long-term care facility. None of the patients were discharged to home health care or to hospice.
Most of the group (61%) had open surgery; the remainder had laparoscopy. Of those who had open surgery, 20% were discharged to a nursing facility, compared with 12.5% of the laparoscopy group – a significant difference.
Laparoscopy significantly decreased the chance of a nursing home admission by 39% in a multivariate analysis that controlled for age, sex, race, comorbidity score, cancer stage, income and insurance, and hospital size.
Factors significantly associated with nursing home discharge included advancing age and cancer stage.
Generally speaking, open surgery is physically more trying for elderly patients. A difficult recovery could be just enough to tip them over the edge from independent living, Dr. Liu said.
Dr. Liu had no financial disclosures.
AT THE ACS CLINICAL CONGRESS
Major finding: Of those older patients who had open surgery, 20% were discharged to a nursing facility, compared with 12.5% of the laparoscopy group, a significant difference.
Data source: The study included data on 9,416 patients.
Disclosures: Dr. Richard Liu had no financial disclosures.
Colorectal surgeons post better rectal surgery outcomes than general surgeons
WASHINGTON – Although general surgeons perform the majority of rectal resections in the United States, their patients have more severe postoperative complications, longer lengths of stay, higher hospital costs, and higher mortality rates than do those of colorectal surgeons.
A review of more than 60,000 cases over a 6-year period found that patients who had been operated on by a general surgeon had a 42% increase in the risk of mortality. They stayed in the hospital an average 1 day longer than the patients of colorectal surgeons, and had bills more than $1,000 higher. Although their overall complication rate was lower, general surgeons’ patients tended to have more severe complications, including pulmonary complications and surgical site infections, Dr. Marc Casasanta said at the annual clinical congress of the American College of Surgeons.
Dr. Casasanta of the University of Texas, Houston, extracted his data from the Premier Perspective database, the largest inpatient database in the United States. His analysis included 60,412 nonemergent rectal resections performed from 2005 to 2011.
Most of these (74%) were performed by general surgeons, with colorectal surgeons performing the remainder. Adverse outcomes examined included length and cost of hospital admission, overall complications and severe complications, and mortality.
There were several significant differences in the patient populations. General surgeons had older patients (63 vs. 61 years), and their patients tended to be sicker, with less minor disease severity (31% vs. 35%) and more major (29% vs. 17%) and extreme disease severity (8% vs. 6%).
Colorectal surgeons treated significantly more patients with inflammatory bowel disease (10% vs. 4%). They worked exclusively in urban hospitals, compared with 87% of general surgeons. Half of colorectal surgeons worked in teaching hospitals versus 37% of general surgeons.
The mean overall length of stay was a little more than 8 days. The mean hospital cost was $19,093.The overall complication rate was 29%, and mortality was 1.5%.
Complications varied significantly by surgeon specialty. General surgeons had significantly higher rates of digestive complications (including anastomotic problems), as well as pulmonary complications, lower-extremity thromboembolism, shock, and surgical site infections, including intra-abdominal infections.
The univariate analysis identified several patient characteristics significantly associated with poor outcomes, including age older than 62 years (odds ratio, 1.43), female gender (OR, 1.23), major disease severity (OR, 4.7), extreme disease severity (OR, 23), and a diagnosis of inflammatory bowel disease (OR, 1.41).
Other significant risk factors were being treated in a rural hospital (OR 1.29), being treated in a teaching hospital (OR, 1.08), and having a general surgeon (OR, 1.16). Having a colorectal surgeon decreased the risk of a poor outcome by 14%.
In the multivariate analysis, patients of general surgeons were 13% less likely to have any complication and 20% less likely to have ileus. But these patients were also significantly more likely to have severe complications, including pulmonary problems (13%) and surgical site infections (11%).
The length of stay was about 1 day longer, and hospitals costs were $1,122 more expensive. Patients of general surgeons were 42% more likely to die.
Dr. Casasanta said he had no relevant financial disclosures. However, Dr. Eric Haas, the primary investigator, said he has been a consultant for Applied Medical; and has received consulting fees, research funding, and honoraria from Intuitive Surgical.
WASHINGTON – Although general surgeons perform the majority of rectal resections in the United States, their patients have more severe postoperative complications, longer lengths of stay, higher hospital costs, and higher mortality rates than do those of colorectal surgeons.
A review of more than 60,000 cases over a 6-year period found that patients who had been operated on by a general surgeon had a 42% increase in the risk of mortality. They stayed in the hospital an average 1 day longer than the patients of colorectal surgeons, and had bills more than $1,000 higher. Although their overall complication rate was lower, general surgeons’ patients tended to have more severe complications, including pulmonary complications and surgical site infections, Dr. Marc Casasanta said at the annual clinical congress of the American College of Surgeons.
Dr. Casasanta of the University of Texas, Houston, extracted his data from the Premier Perspective database, the largest inpatient database in the United States. His analysis included 60,412 nonemergent rectal resections performed from 2005 to 2011.
Most of these (74%) were performed by general surgeons, with colorectal surgeons performing the remainder. Adverse outcomes examined included length and cost of hospital admission, overall complications and severe complications, and mortality.
There were several significant differences in the patient populations. General surgeons had older patients (63 vs. 61 years), and their patients tended to be sicker, with less minor disease severity (31% vs. 35%) and more major (29% vs. 17%) and extreme disease severity (8% vs. 6%).
Colorectal surgeons treated significantly more patients with inflammatory bowel disease (10% vs. 4%). They worked exclusively in urban hospitals, compared with 87% of general surgeons. Half of colorectal surgeons worked in teaching hospitals versus 37% of general surgeons.
The mean overall length of stay was a little more than 8 days. The mean hospital cost was $19,093.The overall complication rate was 29%, and mortality was 1.5%.
Complications varied significantly by surgeon specialty. General surgeons had significantly higher rates of digestive complications (including anastomotic problems), as well as pulmonary complications, lower-extremity thromboembolism, shock, and surgical site infections, including intra-abdominal infections.
The univariate analysis identified several patient characteristics significantly associated with poor outcomes, including age older than 62 years (odds ratio, 1.43), female gender (OR, 1.23), major disease severity (OR, 4.7), extreme disease severity (OR, 23), and a diagnosis of inflammatory bowel disease (OR, 1.41).
Other significant risk factors were being treated in a rural hospital (OR 1.29), being treated in a teaching hospital (OR, 1.08), and having a general surgeon (OR, 1.16). Having a colorectal surgeon decreased the risk of a poor outcome by 14%.
In the multivariate analysis, patients of general surgeons were 13% less likely to have any complication and 20% less likely to have ileus. But these patients were also significantly more likely to have severe complications, including pulmonary problems (13%) and surgical site infections (11%).
The length of stay was about 1 day longer, and hospitals costs were $1,122 more expensive. Patients of general surgeons were 42% more likely to die.
Dr. Casasanta said he had no relevant financial disclosures. However, Dr. Eric Haas, the primary investigator, said he has been a consultant for Applied Medical; and has received consulting fees, research funding, and honoraria from Intuitive Surgical.
WASHINGTON – Although general surgeons perform the majority of rectal resections in the United States, their patients have more severe postoperative complications, longer lengths of stay, higher hospital costs, and higher mortality rates than do those of colorectal surgeons.
A review of more than 60,000 cases over a 6-year period found that patients who had been operated on by a general surgeon had a 42% increase in the risk of mortality. They stayed in the hospital an average 1 day longer than the patients of colorectal surgeons, and had bills more than $1,000 higher. Although their overall complication rate was lower, general surgeons’ patients tended to have more severe complications, including pulmonary complications and surgical site infections, Dr. Marc Casasanta said at the annual clinical congress of the American College of Surgeons.
Dr. Casasanta of the University of Texas, Houston, extracted his data from the Premier Perspective database, the largest inpatient database in the United States. His analysis included 60,412 nonemergent rectal resections performed from 2005 to 2011.
Most of these (74%) were performed by general surgeons, with colorectal surgeons performing the remainder. Adverse outcomes examined included length and cost of hospital admission, overall complications and severe complications, and mortality.
There were several significant differences in the patient populations. General surgeons had older patients (63 vs. 61 years), and their patients tended to be sicker, with less minor disease severity (31% vs. 35%) and more major (29% vs. 17%) and extreme disease severity (8% vs. 6%).
Colorectal surgeons treated significantly more patients with inflammatory bowel disease (10% vs. 4%). They worked exclusively in urban hospitals, compared with 87% of general surgeons. Half of colorectal surgeons worked in teaching hospitals versus 37% of general surgeons.
The mean overall length of stay was a little more than 8 days. The mean hospital cost was $19,093.The overall complication rate was 29%, and mortality was 1.5%.
Complications varied significantly by surgeon specialty. General surgeons had significantly higher rates of digestive complications (including anastomotic problems), as well as pulmonary complications, lower-extremity thromboembolism, shock, and surgical site infections, including intra-abdominal infections.
The univariate analysis identified several patient characteristics significantly associated with poor outcomes, including age older than 62 years (odds ratio, 1.43), female gender (OR, 1.23), major disease severity (OR, 4.7), extreme disease severity (OR, 23), and a diagnosis of inflammatory bowel disease (OR, 1.41).
Other significant risk factors were being treated in a rural hospital (OR 1.29), being treated in a teaching hospital (OR, 1.08), and having a general surgeon (OR, 1.16). Having a colorectal surgeon decreased the risk of a poor outcome by 14%.
In the multivariate analysis, patients of general surgeons were 13% less likely to have any complication and 20% less likely to have ileus. But these patients were also significantly more likely to have severe complications, including pulmonary problems (13%) and surgical site infections (11%).
The length of stay was about 1 day longer, and hospitals costs were $1,122 more expensive. Patients of general surgeons were 42% more likely to die.
Dr. Casasanta said he had no relevant financial disclosures. However, Dr. Eric Haas, the primary investigator, said he has been a consultant for Applied Medical; and has received consulting fees, research funding, and honoraria from Intuitive Surgical.
AT THE ACS CLINICAL CONGRESS
Major finding: Patients undergoing a rectal resection had more serious complications, and were 42% more likely to die if they had a general surgeon than if they had a colorectal surgeon.
Data source: The study included more than 60,000 surgeries performed over a 6-year period.
Disclosures: Dr. Marc Casasanta said he had no relevant financial disclosures. However, Dr. Eric Haas, the primary investigator, said he has been a consultant for Applied Medical, and has received consulting fees, research funding, and honoraria from Intuitive Surgical.
Sigmoidoscopy may not be enough for older patients
WASHINGTON – Colon cancer screening with sigmoidoscopy alone could miss up to 50% of colon polyps in older patients.
As people age, polyps seem to develop more and more proximally, Dr. Victor Tsirline said at the annual clinical congress of the American College of Surgeons. His review of more than 120,000 colonoscopies found that a flexible sigmoidoscopy alone could miss 44% of polyps in patients aged 60-69 years and 50% in those aged 70-79 years.
"We found that proximal colon polyps are more frequent with advanced age than previously considered," said Dr. Tsirline of Carolinas Medical Center, Charlotte, N.C. "So if this is true, what happens if we use sigmoidoscopy instead of colonoscopy? If we had, we would have missed 22,800 polyps, and 16,800 of those would have been adenomatous. In [patients 59 and younger] 32%-36% would be missed and in the older patients, 45%-50%."
Dr. Tsirline obtained his data from the Provation MD endoscopy transcription system. He obtained information on 120,365 colonoscopies that were performed from 2003 to 2011.
He cross-referenced this with CoPathPlus, a pathology reporting system. This allowed him to cross-reference polyp pathology (adenoma vs. hyperplasia) by computer algorithm. There was complete information available on 43,833 polyps.
Because of the large sample size, he set his level of statistical significance at P = less than 0.01.
The patients in the study were aged 20-90 years. Of the entire group of procedures, 53,492 colonoscopies (44%) identified polyps. Most studies (64%) found a single polyp; 25% found two, and 11% found three or more. A subset of the colonoscopies was only for average risk screening (44,806). Of these, 46% identified polyps.
Overall, 48% of polyps were adenomatous; 37% were hyperplastic. Pathology was not available for the remainder.
The polyps were fairly evenly distributed throughout the colon: rectum, 18%; sigmoid, 26%; descending, 14%; transverse, 16%; ascending, 15%; cecum, 11%.
However, when broken down by patient age, the distribution changed significantly. With every advancing decade of life, patients were:
• 22% less likely to have polyps in the rectum or sigmoid.
• 7% more likely to have polyps in the descending colon.
• 19% more likely to have polyps in the transverse colon.
• 30% more likely to have polyps in the ascending colon.
• 22% more likely to have polyps in the cecum.
All of these risks were statistically significant, and they held for both adenomatous and hyperplastic polyps.
The findings led Dr. Tsirline to conclude that flexible sigmoidoscopy should not be relied upon as an effective colon cancer screening method in patients older than 60 years. The U.S. Preventive Services Task Force states that sigmoidoscopy every 5 years combined with high-sensitivity fecal occult blood testing every 3 years is an adequate screening alternative.
"From this study, it’s pretty apparent that sigmoidoscopy should not be used for colon cancer screening in older patients," he said.
During a discussion, Dr. Tsirline fielded a question about screening the very elderly – patients in their 80s and 90s. The study group did include a small number of these patients, he said.
"I think the argument for not screening older individuals is based on the question of whether finding a colon cancer would change anything. Most people think the risks of screening and treatment would outweigh the benefits. Yes, you may find anything, but what are you going to do about it?"
Dr. Tsirline had no financial disclosures.
WASHINGTON – Colon cancer screening with sigmoidoscopy alone could miss up to 50% of colon polyps in older patients.
As people age, polyps seem to develop more and more proximally, Dr. Victor Tsirline said at the annual clinical congress of the American College of Surgeons. His review of more than 120,000 colonoscopies found that a flexible sigmoidoscopy alone could miss 44% of polyps in patients aged 60-69 years and 50% in those aged 70-79 years.
"We found that proximal colon polyps are more frequent with advanced age than previously considered," said Dr. Tsirline of Carolinas Medical Center, Charlotte, N.C. "So if this is true, what happens if we use sigmoidoscopy instead of colonoscopy? If we had, we would have missed 22,800 polyps, and 16,800 of those would have been adenomatous. In [patients 59 and younger] 32%-36% would be missed and in the older patients, 45%-50%."
Dr. Tsirline obtained his data from the Provation MD endoscopy transcription system. He obtained information on 120,365 colonoscopies that were performed from 2003 to 2011.
He cross-referenced this with CoPathPlus, a pathology reporting system. This allowed him to cross-reference polyp pathology (adenoma vs. hyperplasia) by computer algorithm. There was complete information available on 43,833 polyps.
Because of the large sample size, he set his level of statistical significance at P = less than 0.01.
The patients in the study were aged 20-90 years. Of the entire group of procedures, 53,492 colonoscopies (44%) identified polyps. Most studies (64%) found a single polyp; 25% found two, and 11% found three or more. A subset of the colonoscopies was only for average risk screening (44,806). Of these, 46% identified polyps.
Overall, 48% of polyps were adenomatous; 37% were hyperplastic. Pathology was not available for the remainder.
The polyps were fairly evenly distributed throughout the colon: rectum, 18%; sigmoid, 26%; descending, 14%; transverse, 16%; ascending, 15%; cecum, 11%.
However, when broken down by patient age, the distribution changed significantly. With every advancing decade of life, patients were:
• 22% less likely to have polyps in the rectum or sigmoid.
• 7% more likely to have polyps in the descending colon.
• 19% more likely to have polyps in the transverse colon.
• 30% more likely to have polyps in the ascending colon.
• 22% more likely to have polyps in the cecum.
All of these risks were statistically significant, and they held for both adenomatous and hyperplastic polyps.
The findings led Dr. Tsirline to conclude that flexible sigmoidoscopy should not be relied upon as an effective colon cancer screening method in patients older than 60 years. The U.S. Preventive Services Task Force states that sigmoidoscopy every 5 years combined with high-sensitivity fecal occult blood testing every 3 years is an adequate screening alternative.
"From this study, it’s pretty apparent that sigmoidoscopy should not be used for colon cancer screening in older patients," he said.
During a discussion, Dr. Tsirline fielded a question about screening the very elderly – patients in their 80s and 90s. The study group did include a small number of these patients, he said.
"I think the argument for not screening older individuals is based on the question of whether finding a colon cancer would change anything. Most people think the risks of screening and treatment would outweigh the benefits. Yes, you may find anything, but what are you going to do about it?"
Dr. Tsirline had no financial disclosures.
WASHINGTON – Colon cancer screening with sigmoidoscopy alone could miss up to 50% of colon polyps in older patients.
As people age, polyps seem to develop more and more proximally, Dr. Victor Tsirline said at the annual clinical congress of the American College of Surgeons. His review of more than 120,000 colonoscopies found that a flexible sigmoidoscopy alone could miss 44% of polyps in patients aged 60-69 years and 50% in those aged 70-79 years.
"We found that proximal colon polyps are more frequent with advanced age than previously considered," said Dr. Tsirline of Carolinas Medical Center, Charlotte, N.C. "So if this is true, what happens if we use sigmoidoscopy instead of colonoscopy? If we had, we would have missed 22,800 polyps, and 16,800 of those would have been adenomatous. In [patients 59 and younger] 32%-36% would be missed and in the older patients, 45%-50%."
Dr. Tsirline obtained his data from the Provation MD endoscopy transcription system. He obtained information on 120,365 colonoscopies that were performed from 2003 to 2011.
He cross-referenced this with CoPathPlus, a pathology reporting system. This allowed him to cross-reference polyp pathology (adenoma vs. hyperplasia) by computer algorithm. There was complete information available on 43,833 polyps.
Because of the large sample size, he set his level of statistical significance at P = less than 0.01.
The patients in the study were aged 20-90 years. Of the entire group of procedures, 53,492 colonoscopies (44%) identified polyps. Most studies (64%) found a single polyp; 25% found two, and 11% found three or more. A subset of the colonoscopies was only for average risk screening (44,806). Of these, 46% identified polyps.
Overall, 48% of polyps were adenomatous; 37% were hyperplastic. Pathology was not available for the remainder.
The polyps were fairly evenly distributed throughout the colon: rectum, 18%; sigmoid, 26%; descending, 14%; transverse, 16%; ascending, 15%; cecum, 11%.
However, when broken down by patient age, the distribution changed significantly. With every advancing decade of life, patients were:
• 22% less likely to have polyps in the rectum or sigmoid.
• 7% more likely to have polyps in the descending colon.
• 19% more likely to have polyps in the transverse colon.
• 30% more likely to have polyps in the ascending colon.
• 22% more likely to have polyps in the cecum.
All of these risks were statistically significant, and they held for both adenomatous and hyperplastic polyps.
The findings led Dr. Tsirline to conclude that flexible sigmoidoscopy should not be relied upon as an effective colon cancer screening method in patients older than 60 years. The U.S. Preventive Services Task Force states that sigmoidoscopy every 5 years combined with high-sensitivity fecal occult blood testing every 3 years is an adequate screening alternative.
"From this study, it’s pretty apparent that sigmoidoscopy should not be used for colon cancer screening in older patients," he said.
During a discussion, Dr. Tsirline fielded a question about screening the very elderly – patients in their 80s and 90s. The study group did include a small number of these patients, he said.
"I think the argument for not screening older individuals is based on the question of whether finding a colon cancer would change anything. Most people think the risks of screening and treatment would outweigh the benefits. Yes, you may find anything, but what are you going to do about it?"
Dr. Tsirline had no financial disclosures.
AT THE ACS CLINICAL CONGRESS
Major finding: Because people are 30% more likely to have polyps in the ascending colon and 22% more likely to have polyps in the cecum as they age, sigmoidoscopy may not be an adequate screening method.
Data source: Study of 120,000 colonoscopies.
Disclosures: Dr. Victor Tsirline had no financial disclosures.
Early walking and eating improve outcomes for bowel surgery patients
WASHINGTON – A program to enhance recovery from bowel surgery significantly decreased the incidence rate of both postoperative ileus and 30-day readmission.
Early walking and postoperative alimentation, beginning with three times on postop day 1, drove the improved outcomes, Dr. Terrence Loftus reported at the annual clinical congress of the American College of Surgeons.
His 3-year retrospective study compared outcomes before and after the program was implemented. In addition to confirming the benefits, the study says something about how change becomes part of a systemwide culture, said Dr. Loftus, medical director of surgical services and clinical resources for Banner Health, Phoenix.
"When you see a before-and-after picture, it gives you the sense that change is like clicking on a light switch, and then everything starts happening. In reality, it’s not. It’s something that catches on over time. It’s a social process that gets passed along. It’s not Dr. Loftus coming in and showing a few slides and saying, ‘Okay, now this is what you have to do.’ It’s surgeons having conversations in the lounge and saying, ‘I tried this and it worked. You should try it too.’ "
In 2010, Banner Health System’s Surgery Clinical Consensus Group decided to tackle the system’s less-than-stellar rates of postoperative ileus and readmission among patients who had bowel surgery.
While there are a number of published enhanced-care pathways, Dr. Loftus found a wide variety of applications over Banner Health’s large medical system. "In some places, people didn’t even know about them, and in others they were using their own version," he said. "We needed a systemwide approach to recovery – something that would be useful over a large, heterogeneous health care system."
The Banner consensus group came up with the Bowel Surgery Strategic Initiative, a program implemented in 19 hospitals spread over six states, covered by 119 surgeons. The system was widely diversified, including everything from an 18-bed critical access unit to a large 600-bed level I trauma center.
"The surgeons ranged from solo private practice, to group practices, hospital employed, and locum tenens, so you can begin to understand the wide diversity of practices and environments we were trying to implement this in," Dr. Loftus said.
The first step was to develop a literature-based GI care pathway that could be widely implemented. The group’s first version had 80 steps – vastly too many.
The final program was based on just two drivers: early alimentation and early ambulation. Eating began with the earliest possible removal of the nasogastric tube (if present), 200-250 cc of oral intake on postoperative day 1, and a progressively advancing diet. Ambulation started with getting up and walking three times on postop day 1, with progressively increasing physical activity.
The team studied a 3-year period spanning 18 months on either side of the implementation date of July 2011. The analysis included 5,000 patients who had undergone elective small- or large-bowel surgery during that time period.
Dr. Loftus said there was a significant increase in both ambulation and alimentation. Before the program, the mean ambulation rate was 53%; that increased to 73% afterward. Alimentation increased from 51% to 71%. The composite of both drivers increased from 53% to 72%.
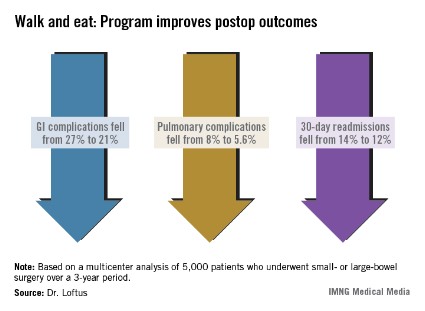
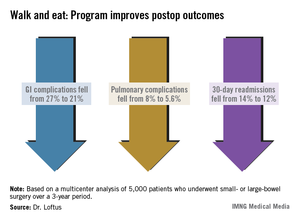
There were associated improvements in most of the clinical outcomes assessed. Overall, the complication rate decreased significantly, from 36% to 29%. Gastrointestinal complications fell from 27% to 21%, with the incidence of postoperative ileus declining from 27% to 21%. Pulmonary complications also decreased significantly, from 8% to 5.6%.
Thirty-day readmission declined from 14% to 12% – also a significant decrease. This was expected, Dr. Loftus said, because most of the readmissions were due to paralytic ileus.
Length of stay, however, was not significantly affected. There was no change in mortality.
The project also illuminated the importance of a facility’s own professional culture. Chart audits found that some facilities were only ambulating patients about a third of the time that it was ordered – even though nursing estimated the rate at 80% and surgeons at 70%.
Facilities that had particularly good postintervention outcomes were already ahead of the game before the project. "These already had a culture of activity. Nursing was getting patients up on day 1, and they set up their schedules in a way that says, ‘These patients will get up. We are going to do this no matter what.’ "
Dr. Loftus had no financial disclosures.
WASHINGTON – A program to enhance recovery from bowel surgery significantly decreased the incidence rate of both postoperative ileus and 30-day readmission.
Early walking and postoperative alimentation, beginning with three times on postop day 1, drove the improved outcomes, Dr. Terrence Loftus reported at the annual clinical congress of the American College of Surgeons.
His 3-year retrospective study compared outcomes before and after the program was implemented. In addition to confirming the benefits, the study says something about how change becomes part of a systemwide culture, said Dr. Loftus, medical director of surgical services and clinical resources for Banner Health, Phoenix.

"When you see a before-and-after picture, it gives you the sense that change is like clicking on a light switch, and then everything starts happening. In reality, it’s not. It’s something that catches on over time. It’s a social process that gets passed along. It’s not Dr. Loftus coming in and showing a few slides and saying, ‘Okay, now this is what you have to do.’ It’s surgeons having conversations in the lounge and saying, ‘I tried this and it worked. You should try it too.’ "
In 2010, Banner Health System’s Surgery Clinical Consensus Group decided to tackle the system’s less-than-stellar rates of postoperative ileus and readmission among patients who had bowel surgery.
While there are a number of published enhanced-care pathways, Dr. Loftus found a wide variety of applications over Banner Health’s large medical system. "In some places, people didn’t even know about them, and in others they were using their own version," he said. "We needed a systemwide approach to recovery – something that would be useful over a large, heterogeneous health care system."
The Banner consensus group came up with the Bowel Surgery Strategic Initiative, a program implemented in 19 hospitals spread over six states, covered by 119 surgeons. The system was widely diversified, including everything from an 18-bed critical access unit to a large 600-bed level I trauma center.
"The surgeons ranged from solo private practice, to group practices, hospital employed, and locum tenens, so you can begin to understand the wide diversity of practices and environments we were trying to implement this in," Dr. Loftus said.
The first step was to develop a literature-based GI care pathway that could be widely implemented. The group’s first version had 80 steps – vastly too many.
The final program was based on just two drivers: early alimentation and early ambulation. Eating began with the earliest possible removal of the nasogastric tube (if present), 200-250 cc of oral intake on postoperative day 1, and a progressively advancing diet. Ambulation started with getting up and walking three times on postop day 1, with progressively increasing physical activity.
The team studied a 3-year period spanning 18 months on either side of the implementation date of July 2011. The analysis included 5,000 patients who had undergone elective small- or large-bowel surgery during that time period.
Dr. Loftus said there was a significant increase in both ambulation and alimentation. Before the program, the mean ambulation rate was 53%; that increased to 73% afterward. Alimentation increased from 51% to 71%. The composite of both drivers increased from 53% to 72%.
There were associated improvements in most of the clinical outcomes assessed. Overall, the complication rate decreased significantly, from 36% to 29%. Gastrointestinal complications fell from 27% to 21%, with the incidence of postoperative ileus declining from 27% to 21%. Pulmonary complications also decreased significantly, from 8% to 5.6%.
Thirty-day readmission declined from 14% to 12% – also a significant decrease. This was expected, Dr. Loftus said, because most of the readmissions were due to paralytic ileus.
Length of stay, however, was not significantly affected. There was no change in mortality.
The project also illuminated the importance of a facility’s own professional culture. Chart audits found that some facilities were only ambulating patients about a third of the time that it was ordered – even though nursing estimated the rate at 80% and surgeons at 70%.
Facilities that had particularly good postintervention outcomes were already ahead of the game before the project. "These already had a culture of activity. Nursing was getting patients up on day 1, and they set up their schedules in a way that says, ‘These patients will get up. We are going to do this no matter what.’ "
Dr. Loftus had no financial disclosures.
WASHINGTON – A program to enhance recovery from bowel surgery significantly decreased the incidence rate of both postoperative ileus and 30-day readmission.
Early walking and postoperative alimentation, beginning with three times on postop day 1, drove the improved outcomes, Dr. Terrence Loftus reported at the annual clinical congress of the American College of Surgeons.
His 3-year retrospective study compared outcomes before and after the program was implemented. In addition to confirming the benefits, the study says something about how change becomes part of a systemwide culture, said Dr. Loftus, medical director of surgical services and clinical resources for Banner Health, Phoenix.

"When you see a before-and-after picture, it gives you the sense that change is like clicking on a light switch, and then everything starts happening. In reality, it’s not. It’s something that catches on over time. It’s a social process that gets passed along. It’s not Dr. Loftus coming in and showing a few slides and saying, ‘Okay, now this is what you have to do.’ It’s surgeons having conversations in the lounge and saying, ‘I tried this and it worked. You should try it too.’ "
In 2010, Banner Health System’s Surgery Clinical Consensus Group decided to tackle the system’s less-than-stellar rates of postoperative ileus and readmission among patients who had bowel surgery.
While there are a number of published enhanced-care pathways, Dr. Loftus found a wide variety of applications over Banner Health’s large medical system. "In some places, people didn’t even know about them, and in others they were using their own version," he said. "We needed a systemwide approach to recovery – something that would be useful over a large, heterogeneous health care system."
The Banner consensus group came up with the Bowel Surgery Strategic Initiative, a program implemented in 19 hospitals spread over six states, covered by 119 surgeons. The system was widely diversified, including everything from an 18-bed critical access unit to a large 600-bed level I trauma center.
"The surgeons ranged from solo private practice, to group practices, hospital employed, and locum tenens, so you can begin to understand the wide diversity of practices and environments we were trying to implement this in," Dr. Loftus said.
The first step was to develop a literature-based GI care pathway that could be widely implemented. The group’s first version had 80 steps – vastly too many.
The final program was based on just two drivers: early alimentation and early ambulation. Eating began with the earliest possible removal of the nasogastric tube (if present), 200-250 cc of oral intake on postoperative day 1, and a progressively advancing diet. Ambulation started with getting up and walking three times on postop day 1, with progressively increasing physical activity.
The team studied a 3-year period spanning 18 months on either side of the implementation date of July 2011. The analysis included 5,000 patients who had undergone elective small- or large-bowel surgery during that time period.
Dr. Loftus said there was a significant increase in both ambulation and alimentation. Before the program, the mean ambulation rate was 53%; that increased to 73% afterward. Alimentation increased from 51% to 71%. The composite of both drivers increased from 53% to 72%.
There were associated improvements in most of the clinical outcomes assessed. Overall, the complication rate decreased significantly, from 36% to 29%. Gastrointestinal complications fell from 27% to 21%, with the incidence of postoperative ileus declining from 27% to 21%. Pulmonary complications also decreased significantly, from 8% to 5.6%.
Thirty-day readmission declined from 14% to 12% – also a significant decrease. This was expected, Dr. Loftus said, because most of the readmissions were due to paralytic ileus.
Length of stay, however, was not significantly affected. There was no change in mortality.
The project also illuminated the importance of a facility’s own professional culture. Chart audits found that some facilities were only ambulating patients about a third of the time that it was ordered – even though nursing estimated the rate at 80% and surgeons at 70%.
Facilities that had particularly good postintervention outcomes were already ahead of the game before the project. "These already had a culture of activity. Nursing was getting patients up on day 1, and they set up their schedules in a way that says, ‘These patients will get up. We are going to do this no matter what.’ "
Dr. Loftus had no financial disclosures.
AT THE ACS CLINICAL CONGRESS
Major finding: A recovery program based on early ambulation and alimentation for patients with bowel surgery decreased readmission from 14% to 12%, and postoperative complications from 36% to 29%.
Data source: The retrospective study contained 5,000 patients who had elective small- or large-bowel surgery.
Disclosures: Dr. Loftus had no financial disclosures.
Alvimopan reduces ileus, cuts hospital time in bowel surgery
WASHINGTON – The nonopioid pain reliever alvimopan significantly decreased the incidence of postoperative ileus and shortened hospital stay among bowel surgery patients who took the drug as part of an existing accelerated recovery program.
Compared with patients who took placebo, those who took alvimopan left the hospital about 1 day sooner. In addition to the decrease in ileus, patients experienced a quicker return to normal bowel function, including time to first flatus and first bowel movement, Dr. Robert Moesinger said at the annual clinical congress of the American College of Surgeons.
"Alvimopan augmented the already improved outcomes we had seen with our validated recovery pathway, in both laparoscopic- and open-surgery patients," said Dr. Moesinger of Intermountain Healthcare, Salt Lake City. "Given the very diverse nature of our health care system, with multiple types of hospitals and surgeons, we feel these data are widely applicable and we are very comfortable recommending its routine use for patients having elective bowel surgery."
Dr. Moesinger and his colleagues conducted a randomized, placebo-controlled trial of alvimopan in 248 such patients. Those taking the study drug received 12 mg before surgery; after surgery, they received 12 mg twice a day until discharge.
The primary endpoint was postoperative length of stay. Secondary endpoints included the incidence of postoperative ileus, time to first flatus and first bowel movement, tolerance of solid food, total hospital and pharmacy costs, nasogastric tube reinsertion, 30-day readmission rates, and anastomotic leak.
The patients’ mean age was 61 years. There were no significant differences in any of their baseline demographics or clinical characteristics. Because of a statistical fluke, the placebo group did contain significantly more open-surgery patients than the alvimopan group (34% vs. 20%). The rest of the patients had laparoscopic surgery. Patients had an average of nine doses of the study drug.
The mean length of stay was 4 days in the alvimopan group and 5 in the placebo group – a significant difference.
There was significantly less postoperative ileus in the alvimopan group (2% vs. 10%). Significantly fewer of those taking the study drug needed a nasogastric tube reinserted (2% vs. 9%). The rates of 30-day readmission, reoperation, and anastomotic leak were similar in both groups. The mean time to first bowel movement was about 1 day sooner in the alvimopan group.
The median hospital cost was $10,832 for the alvimopan group and $11,924 for the placebo group – a significant difference. The median total pharmacy cost was $476 vs. $501; this difference was not significant.
Because Cubist Pharmaceuticals, which makes alvimopan, provided the study drug at no cost, the overall cost analysis cannot be considered complete, Dr. Moesinger noted. However, the pharmacy cost for a similar course of the drug would be $84. Figuring that cost into the total saved for each admission ($1,686) still yielded a net financial benefit of $930 per patient, he said.
Dr. Moesinger had no financial disclosures.
Alvimopan (Entereg, Cubist Pharmaceuticals) is an orally administered, peripherally acting mu-opioid receptor antagonist that does not cross the blood-brain barrier. It is designed to reverse opioid-induced changes in the gastrointestinal tract without adversely affecting opioid-induced analgesia.

|
| Dr. Brian E. Lacy |
Alvimopan, the first FDA-approved medication for the treatment of postoperative ileus (POI), was approved in May 2008 with a Risk Evaluation and Mitigation Strategy in place, due to concerns over an increased number of myocardial infarctions in one research study.
Postoperative ileus is the impairment of gastrointestinal motility after abdominal or pelvic surgery, and is an expected complication of major abdominal surgery. It can affect all segments of the gastrointestinal tract and may lead to symptoms of nausea, vomiting, bloating, distention, constipation, and inability to evacuate flatus. Several studies have demonstrated that POI delays hospital discharges, increases the rate of hospital readmission after abdominal surgery, and increases the risk of postoperative complications. As such, POI imposes a significant economic impact on the health care system.
The current study confirms earlier studies involving over 2,000 patients that led to the approval of alvimopan. The current study was a single-center, randomized, double-blind study comparing placebo to alvimopan. Patients randomized to alvimopan (12 mg preoperatively; 12 mg twice daily until discharge) were discharged from the hospital 1 day earlier, were less likely to have a nasogastric tube reinserted, and had a bowel movement 1 day earlier, compared with those patients receiving placebo. The authors reported a significant cost savings per patient.*
These findings are important given the absence of other FDA-approved medications for the treatment of POI and the lack of other effective treatments. Alvimopan is available only to patients who are in hospitals that are registered to use this medication under the EASE (Entereg Access Support and Education) program. This recent study should prompt nonparticipating hospitals to consider routine use of alvimopan in all patients undergoing elective and emergent surgeries at risk for development of POI.
Dr. Brian E. Lacy is a professor of medicine at the Geisel School of Medicine at Dartmouth, Hanover, N.H., and chief of the section of gastroenterology and hepatology at Dartmouth-Hitchcock Medical Center. He has no relevant conflicts of interest.
*CORRECTION 11/21/13: The original version of this story misstated the cost savings per patient.
Alvimopan (Entereg, Cubist Pharmaceuticals) is an orally administered, peripherally acting mu-opioid receptor antagonist that does not cross the blood-brain barrier. It is designed to reverse opioid-induced changes in the gastrointestinal tract without adversely affecting opioid-induced analgesia.

|
| Dr. Brian E. Lacy |
Alvimopan, the first FDA-approved medication for the treatment of postoperative ileus (POI), was approved in May 2008 with a Risk Evaluation and Mitigation Strategy in place, due to concerns over an increased number of myocardial infarctions in one research study.
Postoperative ileus is the impairment of gastrointestinal motility after abdominal or pelvic surgery, and is an expected complication of major abdominal surgery. It can affect all segments of the gastrointestinal tract and may lead to symptoms of nausea, vomiting, bloating, distention, constipation, and inability to evacuate flatus. Several studies have demonstrated that POI delays hospital discharges, increases the rate of hospital readmission after abdominal surgery, and increases the risk of postoperative complications. As such, POI imposes a significant economic impact on the health care system.
The current study confirms earlier studies involving over 2,000 patients that led to the approval of alvimopan. The current study was a single-center, randomized, double-blind study comparing placebo to alvimopan. Patients randomized to alvimopan (12 mg preoperatively; 12 mg twice daily until discharge) were discharged from the hospital 1 day earlier, were less likely to have a nasogastric tube reinserted, and had a bowel movement 1 day earlier, compared with those patients receiving placebo. The authors reported a significant cost savings per patient.*
These findings are important given the absence of other FDA-approved medications for the treatment of POI and the lack of other effective treatments. Alvimopan is available only to patients who are in hospitals that are registered to use this medication under the EASE (Entereg Access Support and Education) program. This recent study should prompt nonparticipating hospitals to consider routine use of alvimopan in all patients undergoing elective and emergent surgeries at risk for development of POI.
Dr. Brian E. Lacy is a professor of medicine at the Geisel School of Medicine at Dartmouth, Hanover, N.H., and chief of the section of gastroenterology and hepatology at Dartmouth-Hitchcock Medical Center. He has no relevant conflicts of interest.
*CORRECTION 11/21/13: The original version of this story misstated the cost savings per patient.
Alvimopan (Entereg, Cubist Pharmaceuticals) is an orally administered, peripherally acting mu-opioid receptor antagonist that does not cross the blood-brain barrier. It is designed to reverse opioid-induced changes in the gastrointestinal tract without adversely affecting opioid-induced analgesia.

|
| Dr. Brian E. Lacy |
Alvimopan, the first FDA-approved medication for the treatment of postoperative ileus (POI), was approved in May 2008 with a Risk Evaluation and Mitigation Strategy in place, due to concerns over an increased number of myocardial infarctions in one research study.
Postoperative ileus is the impairment of gastrointestinal motility after abdominal or pelvic surgery, and is an expected complication of major abdominal surgery. It can affect all segments of the gastrointestinal tract and may lead to symptoms of nausea, vomiting, bloating, distention, constipation, and inability to evacuate flatus. Several studies have demonstrated that POI delays hospital discharges, increases the rate of hospital readmission after abdominal surgery, and increases the risk of postoperative complications. As such, POI imposes a significant economic impact on the health care system.
The current study confirms earlier studies involving over 2,000 patients that led to the approval of alvimopan. The current study was a single-center, randomized, double-blind study comparing placebo to alvimopan. Patients randomized to alvimopan (12 mg preoperatively; 12 mg twice daily until discharge) were discharged from the hospital 1 day earlier, were less likely to have a nasogastric tube reinserted, and had a bowel movement 1 day earlier, compared with those patients receiving placebo. The authors reported a significant cost savings per patient.*
These findings are important given the absence of other FDA-approved medications for the treatment of POI and the lack of other effective treatments. Alvimopan is available only to patients who are in hospitals that are registered to use this medication under the EASE (Entereg Access Support and Education) program. This recent study should prompt nonparticipating hospitals to consider routine use of alvimopan in all patients undergoing elective and emergent surgeries at risk for development of POI.
Dr. Brian E. Lacy is a professor of medicine at the Geisel School of Medicine at Dartmouth, Hanover, N.H., and chief of the section of gastroenterology and hepatology at Dartmouth-Hitchcock Medical Center. He has no relevant conflicts of interest.
*CORRECTION 11/21/13: The original version of this story misstated the cost savings per patient.
WASHINGTON – The nonopioid pain reliever alvimopan significantly decreased the incidence of postoperative ileus and shortened hospital stay among bowel surgery patients who took the drug as part of an existing accelerated recovery program.
Compared with patients who took placebo, those who took alvimopan left the hospital about 1 day sooner. In addition to the decrease in ileus, patients experienced a quicker return to normal bowel function, including time to first flatus and first bowel movement, Dr. Robert Moesinger said at the annual clinical congress of the American College of Surgeons.
"Alvimopan augmented the already improved outcomes we had seen with our validated recovery pathway, in both laparoscopic- and open-surgery patients," said Dr. Moesinger of Intermountain Healthcare, Salt Lake City. "Given the very diverse nature of our health care system, with multiple types of hospitals and surgeons, we feel these data are widely applicable and we are very comfortable recommending its routine use for patients having elective bowel surgery."
Dr. Moesinger and his colleagues conducted a randomized, placebo-controlled trial of alvimopan in 248 such patients. Those taking the study drug received 12 mg before surgery; after surgery, they received 12 mg twice a day until discharge.
The primary endpoint was postoperative length of stay. Secondary endpoints included the incidence of postoperative ileus, time to first flatus and first bowel movement, tolerance of solid food, total hospital and pharmacy costs, nasogastric tube reinsertion, 30-day readmission rates, and anastomotic leak.
The patients’ mean age was 61 years. There were no significant differences in any of their baseline demographics or clinical characteristics. Because of a statistical fluke, the placebo group did contain significantly more open-surgery patients than the alvimopan group (34% vs. 20%). The rest of the patients had laparoscopic surgery. Patients had an average of nine doses of the study drug.
The mean length of stay was 4 days in the alvimopan group and 5 in the placebo group – a significant difference.
There was significantly less postoperative ileus in the alvimopan group (2% vs. 10%). Significantly fewer of those taking the study drug needed a nasogastric tube reinserted (2% vs. 9%). The rates of 30-day readmission, reoperation, and anastomotic leak were similar in both groups. The mean time to first bowel movement was about 1 day sooner in the alvimopan group.
The median hospital cost was $10,832 for the alvimopan group and $11,924 for the placebo group – a significant difference. The median total pharmacy cost was $476 vs. $501; this difference was not significant.
Because Cubist Pharmaceuticals, which makes alvimopan, provided the study drug at no cost, the overall cost analysis cannot be considered complete, Dr. Moesinger noted. However, the pharmacy cost for a similar course of the drug would be $84. Figuring that cost into the total saved for each admission ($1,686) still yielded a net financial benefit of $930 per patient, he said.
Dr. Moesinger had no financial disclosures.
WASHINGTON – The nonopioid pain reliever alvimopan significantly decreased the incidence of postoperative ileus and shortened hospital stay among bowel surgery patients who took the drug as part of an existing accelerated recovery program.
Compared with patients who took placebo, those who took alvimopan left the hospital about 1 day sooner. In addition to the decrease in ileus, patients experienced a quicker return to normal bowel function, including time to first flatus and first bowel movement, Dr. Robert Moesinger said at the annual clinical congress of the American College of Surgeons.
"Alvimopan augmented the already improved outcomes we had seen with our validated recovery pathway, in both laparoscopic- and open-surgery patients," said Dr. Moesinger of Intermountain Healthcare, Salt Lake City. "Given the very diverse nature of our health care system, with multiple types of hospitals and surgeons, we feel these data are widely applicable and we are very comfortable recommending its routine use for patients having elective bowel surgery."
Dr. Moesinger and his colleagues conducted a randomized, placebo-controlled trial of alvimopan in 248 such patients. Those taking the study drug received 12 mg before surgery; after surgery, they received 12 mg twice a day until discharge.
The primary endpoint was postoperative length of stay. Secondary endpoints included the incidence of postoperative ileus, time to first flatus and first bowel movement, tolerance of solid food, total hospital and pharmacy costs, nasogastric tube reinsertion, 30-day readmission rates, and anastomotic leak.
The patients’ mean age was 61 years. There were no significant differences in any of their baseline demographics or clinical characteristics. Because of a statistical fluke, the placebo group did contain significantly more open-surgery patients than the alvimopan group (34% vs. 20%). The rest of the patients had laparoscopic surgery. Patients had an average of nine doses of the study drug.
The mean length of stay was 4 days in the alvimopan group and 5 in the placebo group – a significant difference.
There was significantly less postoperative ileus in the alvimopan group (2% vs. 10%). Significantly fewer of those taking the study drug needed a nasogastric tube reinserted (2% vs. 9%). The rates of 30-day readmission, reoperation, and anastomotic leak were similar in both groups. The mean time to first bowel movement was about 1 day sooner in the alvimopan group.
The median hospital cost was $10,832 for the alvimopan group and $11,924 for the placebo group – a significant difference. The median total pharmacy cost was $476 vs. $501; this difference was not significant.
Because Cubist Pharmaceuticals, which makes alvimopan, provided the study drug at no cost, the overall cost analysis cannot be considered complete, Dr. Moesinger noted. However, the pharmacy cost for a similar course of the drug would be $84. Figuring that cost into the total saved for each admission ($1,686) still yielded a net financial benefit of $930 per patient, he said.
Dr. Moesinger had no financial disclosures.
AT THE ACS CLINICAL CONGRESS
Major finding: Compared with placebo, alvimopan given before and after elective bowel surgery reduced the length of stay by 1 day and significantly decreased the incidence of postoperative ileus (2% vs. 10%).
Data source: The randomized placebo-controlled trial comprised 248 patients.
Disclosures: Dr. Moesinger had no financial disclosures.
Surgeons as proficient as gastroenterologists at colonoscopy
WASHINGTON (IMNG) – A British study suggests that it is experience, not specialty, that makes the endoscopist.
The review of more than 2,000 colonoscopies performed in 1 year determined that gastroenterologists and surgeons had identical colonoscopy completion and adverse-event outcomes, Dr. Camille Yvon reported at the annual congress of the American College of Surgeons.
Dr. Yvon, of the Medway Maritime NHS Hospital in Gillingham, England, reported the results of an audit conducted at the Kent facility from March 2011 to March 2012. It was based on prospectively collected data and was designed to compare clinical outcomes among a group of 10 physicians who were performing endoscopies during that time. Included were five consultant colorectal surgeons, one senior trust grade surgeon, and four consultant gastroenterologists.
All of the clinicians were certified by the U.K. Joint Advisory Group on Endoscopy (JAG). The group requires clinicians to complete a mentored training period and to meet specific safety and quality standards, including the following:
• 90% completion rate for colonoscopies (entering the cecum).
• Adenoma detection rate more than 10%.
• Polyp recovery more than 90%.
• Good-quality bowel prep more than 90%.
• Colonoscopy perforation rate less than 1/1,000.
• Postpolypectomy bleeding requiring transfusion less than 1/100.
• Postpolypectomy perforation rate less than 1/500.
• Flexible sigmoidoscopy perforation rate less than 1/5,000.
To become JAG accredited, physicians must be supervised by an accredited physician while performing at least 200 procedures, 100 of which were in the past year; 75% must have been colonoscopies. Certification assessment is done by two different people on two different occasions.
The audit comprised 2,058 colonoscopies. The measured outcomes were number of colonoscopies per clinician, cecal intubation rate of at least 90%, perforation rate of less than 1/1,000, and a less than 1/100 rate of postpolypectomy bleeding requiring a transfusion.
Of the total number of colonoscopies, 1,237 were done by the surgeons and the rest by the gastroenterologists. Clinicians performed an average of 205 procedures per year (range, 105-448 per year). Gastroenterologists performed an average of 205 per year, while surgeons performed an average of 206.
The overall cecal intubation rate was 94%. The average rate for both surgeons and gastroenterologists was also 94%.
There were no perforations during the study period. There were two instances of severe postpolypectomy bleeding (0.09%). However, Dr. Yvon reported, the number was too small for any meaningful statistical analysis.
Dr. Yvon had no financial disclosures.
WASHINGTON (IMNG) – A British study suggests that it is experience, not specialty, that makes the endoscopist.
The review of more than 2,000 colonoscopies performed in 1 year determined that gastroenterologists and surgeons had identical colonoscopy completion and adverse-event outcomes, Dr. Camille Yvon reported at the annual congress of the American College of Surgeons.
Dr. Yvon, of the Medway Maritime NHS Hospital in Gillingham, England, reported the results of an audit conducted at the Kent facility from March 2011 to March 2012. It was based on prospectively collected data and was designed to compare clinical outcomes among a group of 10 physicians who were performing endoscopies during that time. Included were five consultant colorectal surgeons, one senior trust grade surgeon, and four consultant gastroenterologists.
All of the clinicians were certified by the U.K. Joint Advisory Group on Endoscopy (JAG). The group requires clinicians to complete a mentored training period and to meet specific safety and quality standards, including the following:
• 90% completion rate for colonoscopies (entering the cecum).
• Adenoma detection rate more than 10%.
• Polyp recovery more than 90%.
• Good-quality bowel prep more than 90%.
• Colonoscopy perforation rate less than 1/1,000.
• Postpolypectomy bleeding requiring transfusion less than 1/100.
• Postpolypectomy perforation rate less than 1/500.
• Flexible sigmoidoscopy perforation rate less than 1/5,000.
To become JAG accredited, physicians must be supervised by an accredited physician while performing at least 200 procedures, 100 of which were in the past year; 75% must have been colonoscopies. Certification assessment is done by two different people on two different occasions.
The audit comprised 2,058 colonoscopies. The measured outcomes were number of colonoscopies per clinician, cecal intubation rate of at least 90%, perforation rate of less than 1/1,000, and a less than 1/100 rate of postpolypectomy bleeding requiring a transfusion.
Of the total number of colonoscopies, 1,237 were done by the surgeons and the rest by the gastroenterologists. Clinicians performed an average of 205 procedures per year (range, 105-448 per year). Gastroenterologists performed an average of 205 per year, while surgeons performed an average of 206.
The overall cecal intubation rate was 94%. The average rate for both surgeons and gastroenterologists was also 94%.
There were no perforations during the study period. There were two instances of severe postpolypectomy bleeding (0.09%). However, Dr. Yvon reported, the number was too small for any meaningful statistical analysis.
Dr. Yvon had no financial disclosures.
WASHINGTON (IMNG) – A British study suggests that it is experience, not specialty, that makes the endoscopist.
The review of more than 2,000 colonoscopies performed in 1 year determined that gastroenterologists and surgeons had identical colonoscopy completion and adverse-event outcomes, Dr. Camille Yvon reported at the annual congress of the American College of Surgeons.
Dr. Yvon, of the Medway Maritime NHS Hospital in Gillingham, England, reported the results of an audit conducted at the Kent facility from March 2011 to March 2012. It was based on prospectively collected data and was designed to compare clinical outcomes among a group of 10 physicians who were performing endoscopies during that time. Included were five consultant colorectal surgeons, one senior trust grade surgeon, and four consultant gastroenterologists.
All of the clinicians were certified by the U.K. Joint Advisory Group on Endoscopy (JAG). The group requires clinicians to complete a mentored training period and to meet specific safety and quality standards, including the following:
• 90% completion rate for colonoscopies (entering the cecum).
• Adenoma detection rate more than 10%.
• Polyp recovery more than 90%.
• Good-quality bowel prep more than 90%.
• Colonoscopy perforation rate less than 1/1,000.
• Postpolypectomy bleeding requiring transfusion less than 1/100.
• Postpolypectomy perforation rate less than 1/500.
• Flexible sigmoidoscopy perforation rate less than 1/5,000.
To become JAG accredited, physicians must be supervised by an accredited physician while performing at least 200 procedures, 100 of which were in the past year; 75% must have been colonoscopies. Certification assessment is done by two different people on two different occasions.
The audit comprised 2,058 colonoscopies. The measured outcomes were number of colonoscopies per clinician, cecal intubation rate of at least 90%, perforation rate of less than 1/1,000, and a less than 1/100 rate of postpolypectomy bleeding requiring a transfusion.
Of the total number of colonoscopies, 1,237 were done by the surgeons and the rest by the gastroenterologists. Clinicians performed an average of 205 procedures per year (range, 105-448 per year). Gastroenterologists performed an average of 205 per year, while surgeons performed an average of 206.
The overall cecal intubation rate was 94%. The average rate for both surgeons and gastroenterologists was also 94%.
There were no perforations during the study period. There were two instances of severe postpolypectomy bleeding (0.09%). However, Dr. Yvon reported, the number was too small for any meaningful statistical analysis.
Dr. Yvon had no financial disclosures.
AT THE ACS CLINICAL CONGRESS
Major finding: Gastroenterologists and surgeons both completed an average of 94% of colonoscopies they performed during a 1-year audit period.
Data source: The audit examined outcomes of more than 2,000 colonoscopies.
Disclosures: Dr. Yvon had no financial disclosures.
Selective screening missed 13% of Lynch syndrome–associated colorectal cancers
All stage IV colorectal cancer patients should be screened for Lynch syndrome, according to Dr. Douglas J. Hartman, and his colleagues at the University of Pittsburgh.
Published pathology models for predicting high microsatellite instability failed to identify up to 13% of Lynch syndrome–associated colorectal carcinomas in a study conducted by Dr. Hartman and his associates.
Current predictive pathology models for the detection of high microsatellite instability (MSI-H) colorectal cancers, including PREDICT and MSPath, rely primarily on right-sided tumor detection; however, Dr. Hartman and his associates determined that MSI-H tumors within the left colon and rectum were associated with Lynch syndrome in 57% of cases. In addition, revised Bethesda Guidelines for Lynch syndrome screening in colorectal cancer patients do not call for microsatellite instability testing in patients over age 60 years, yet 32% of left-sided tumors were identified in patients over age 60 years (Hum Pathol. 2013 Sep 10 [doi: 10.1016/j.humpath.2013.06.012]).
The researchers used MSI polymerase chain reaction (MSI-PCR) and DNA mismatch repair protein immunohistochemistry to prospectively analyze 1,292 colorectal cancers between January 2009 and July 2012. During 2009-2011, cases were evaluated using MSI-PCR only. In 2012, cases were first evaluated with immunohistochemistry. MSI-PCR was performed if there were any equivocal findings in the first round of testing.
MSI-H was found in 150 tumors; 112 were sporadic and 38 were probable Lynch syndrome as determined by BRAF V600E mutation, MLH1 promoter hypermethylation, cancer history, and germline mismatch repair gene mutation. All MSI-H tumors were analyzed for their grade, location, and histology; left-sided MSI-H tumors (n = 12; 57%) were more likely to be Lynch syndrome–related than were right-sided tumors (n = 26; 20%).
Neither PREDICT nor MSPath identified all Lynch syndrome–related tumors: PREDICT found 87% (33 of the 38), while MSPath identified 92% (35 of the 38). The researchers attributed these shortcomings to current predictive models’ "reliance on right-sided location."
"At our institution, we employ a universal screening approach for all resected colorectal carcinomas and biopsies from stage IV colorectal carcinomas regardless of patient age, tumor histology, and tumor location. Patients with tumors exhibiting loss of MSH2 and/or MSH6 and isolated loss of PMS2 are referred for further genetic counseling. Tumors with loss of MLH1 and PMS2 protein expression are further evaluated with BRAF mutation analysis and MLH1 promoter hypermethylation analysis before referral to genetic counseling," the authors wrote.
Contrary to some previously published data, the researchers also found that sporadic MSI-H tumors shared similar morphologies with tumors associated with probable Lynch syndrome, with the exception of a slightly higher proportion of sporadic MSI-H tumors (81%) demonstrating tumor infiltrating lymphocytes as compared with Lynch syndrome–associated tumors (61%).
The authors wrote that this is the "largest study" to date of consecutively identified Lynch syndrome–associated and sporadic tumors. As previous reports were based on retrospective data of primarily Lynch syndrome–associated tumors, those results were "vastly enriched for patients selected for analysis based on cancer-related personal or family history."
The failure of current predictive pathology models to predict all MSI-H and Lynch syndrome–related tumors, particularly left-sided ones, is a strong argument for universal screening, which "does not require widespread application of clinicopathologic criteria by clinicians and pathologists in order to select patients for testing." Further, universal screening is cost effective, and provides useful predictive and prognostic data in reducing cancer risks for patients and relatives who may or may not benefit from genetic counseling, particularly in patients over 60 years, for whom most of the MSI-H tumors were sporadic (91.5%), requiring no additional genetic counseling or testing.
Dr. Hartman and his associates reported no relevant disclosures.
All stage IV colorectal cancer patients should be screened for Lynch syndrome, according to Dr. Douglas J. Hartman, and his colleagues at the University of Pittsburgh.
Published pathology models for predicting high microsatellite instability failed to identify up to 13% of Lynch syndrome–associated colorectal carcinomas in a study conducted by Dr. Hartman and his associates.
Current predictive pathology models for the detection of high microsatellite instability (MSI-H) colorectal cancers, including PREDICT and MSPath, rely primarily on right-sided tumor detection; however, Dr. Hartman and his associates determined that MSI-H tumors within the left colon and rectum were associated with Lynch syndrome in 57% of cases. In addition, revised Bethesda Guidelines for Lynch syndrome screening in colorectal cancer patients do not call for microsatellite instability testing in patients over age 60 years, yet 32% of left-sided tumors were identified in patients over age 60 years (Hum Pathol. 2013 Sep 10 [doi: 10.1016/j.humpath.2013.06.012]).
The researchers used MSI polymerase chain reaction (MSI-PCR) and DNA mismatch repair protein immunohistochemistry to prospectively analyze 1,292 colorectal cancers between January 2009 and July 2012. During 2009-2011, cases were evaluated using MSI-PCR only. In 2012, cases were first evaluated with immunohistochemistry. MSI-PCR was performed if there were any equivocal findings in the first round of testing.
MSI-H was found in 150 tumors; 112 were sporadic and 38 were probable Lynch syndrome as determined by BRAF V600E mutation, MLH1 promoter hypermethylation, cancer history, and germline mismatch repair gene mutation. All MSI-H tumors were analyzed for their grade, location, and histology; left-sided MSI-H tumors (n = 12; 57%) were more likely to be Lynch syndrome–related than were right-sided tumors (n = 26; 20%).
Neither PREDICT nor MSPath identified all Lynch syndrome–related tumors: PREDICT found 87% (33 of the 38), while MSPath identified 92% (35 of the 38). The researchers attributed these shortcomings to current predictive models’ "reliance on right-sided location."
"At our institution, we employ a universal screening approach for all resected colorectal carcinomas and biopsies from stage IV colorectal carcinomas regardless of patient age, tumor histology, and tumor location. Patients with tumors exhibiting loss of MSH2 and/or MSH6 and isolated loss of PMS2 are referred for further genetic counseling. Tumors with loss of MLH1 and PMS2 protein expression are further evaluated with BRAF mutation analysis and MLH1 promoter hypermethylation analysis before referral to genetic counseling," the authors wrote.
Contrary to some previously published data, the researchers also found that sporadic MSI-H tumors shared similar morphologies with tumors associated with probable Lynch syndrome, with the exception of a slightly higher proportion of sporadic MSI-H tumors (81%) demonstrating tumor infiltrating lymphocytes as compared with Lynch syndrome–associated tumors (61%).
The authors wrote that this is the "largest study" to date of consecutively identified Lynch syndrome–associated and sporadic tumors. As previous reports were based on retrospective data of primarily Lynch syndrome–associated tumors, those results were "vastly enriched for patients selected for analysis based on cancer-related personal or family history."
The failure of current predictive pathology models to predict all MSI-H and Lynch syndrome–related tumors, particularly left-sided ones, is a strong argument for universal screening, which "does not require widespread application of clinicopathologic criteria by clinicians and pathologists in order to select patients for testing." Further, universal screening is cost effective, and provides useful predictive and prognostic data in reducing cancer risks for patients and relatives who may or may not benefit from genetic counseling, particularly in patients over 60 years, for whom most of the MSI-H tumors were sporadic (91.5%), requiring no additional genetic counseling or testing.
Dr. Hartman and his associates reported no relevant disclosures.
All stage IV colorectal cancer patients should be screened for Lynch syndrome, according to Dr. Douglas J. Hartman, and his colleagues at the University of Pittsburgh.
Published pathology models for predicting high microsatellite instability failed to identify up to 13% of Lynch syndrome–associated colorectal carcinomas in a study conducted by Dr. Hartman and his associates.
Current predictive pathology models for the detection of high microsatellite instability (MSI-H) colorectal cancers, including PREDICT and MSPath, rely primarily on right-sided tumor detection; however, Dr. Hartman and his associates determined that MSI-H tumors within the left colon and rectum were associated with Lynch syndrome in 57% of cases. In addition, revised Bethesda Guidelines for Lynch syndrome screening in colorectal cancer patients do not call for microsatellite instability testing in patients over age 60 years, yet 32% of left-sided tumors were identified in patients over age 60 years (Hum Pathol. 2013 Sep 10 [doi: 10.1016/j.humpath.2013.06.012]).
The researchers used MSI polymerase chain reaction (MSI-PCR) and DNA mismatch repair protein immunohistochemistry to prospectively analyze 1,292 colorectal cancers between January 2009 and July 2012. During 2009-2011, cases were evaluated using MSI-PCR only. In 2012, cases were first evaluated with immunohistochemistry. MSI-PCR was performed if there were any equivocal findings in the first round of testing.
MSI-H was found in 150 tumors; 112 were sporadic and 38 were probable Lynch syndrome as determined by BRAF V600E mutation, MLH1 promoter hypermethylation, cancer history, and germline mismatch repair gene mutation. All MSI-H tumors were analyzed for their grade, location, and histology; left-sided MSI-H tumors (n = 12; 57%) were more likely to be Lynch syndrome–related than were right-sided tumors (n = 26; 20%).
Neither PREDICT nor MSPath identified all Lynch syndrome–related tumors: PREDICT found 87% (33 of the 38), while MSPath identified 92% (35 of the 38). The researchers attributed these shortcomings to current predictive models’ "reliance on right-sided location."
"At our institution, we employ a universal screening approach for all resected colorectal carcinomas and biopsies from stage IV colorectal carcinomas regardless of patient age, tumor histology, and tumor location. Patients with tumors exhibiting loss of MSH2 and/or MSH6 and isolated loss of PMS2 are referred for further genetic counseling. Tumors with loss of MLH1 and PMS2 protein expression are further evaluated with BRAF mutation analysis and MLH1 promoter hypermethylation analysis before referral to genetic counseling," the authors wrote.
Contrary to some previously published data, the researchers also found that sporadic MSI-H tumors shared similar morphologies with tumors associated with probable Lynch syndrome, with the exception of a slightly higher proportion of sporadic MSI-H tumors (81%) demonstrating tumor infiltrating lymphocytes as compared with Lynch syndrome–associated tumors (61%).
The authors wrote that this is the "largest study" to date of consecutively identified Lynch syndrome–associated and sporadic tumors. As previous reports were based on retrospective data of primarily Lynch syndrome–associated tumors, those results were "vastly enriched for patients selected for analysis based on cancer-related personal or family history."
The failure of current predictive pathology models to predict all MSI-H and Lynch syndrome–related tumors, particularly left-sided ones, is a strong argument for universal screening, which "does not require widespread application of clinicopathologic criteria by clinicians and pathologists in order to select patients for testing." Further, universal screening is cost effective, and provides useful predictive and prognostic data in reducing cancer risks for patients and relatives who may or may not benefit from genetic counseling, particularly in patients over 60 years, for whom most of the MSI-H tumors were sporadic (91.5%), requiring no additional genetic counseling or testing.
Dr. Hartman and his associates reported no relevant disclosures.
FROM HUMAN PATHOLOGY
Major finding: Left-sided tumors with high microsatellite instability (n = 12; 57%) were more likely to be Lynch syndrome–related than were right-sided tumors (n=26; 20%).
Data source: Prospective analysis of 1,292 colorectal carcinomas using microsatellite instability polymerase chain reaction (MSI-PCR) and DNA mismatch repair protein immunohistochemistry.
Disclosures: Dr. Hartman and his associates reported no relevant financial disclosures.
Dual therapy cuts hospitalizations, surgery in IBD
Early dual therapy with infliximab and an immunomodulator significantly decreased the 1-year risk of hospitalization and surgery in patients with inflammatory bowel disease, in a cohort study of almost 20,500 patients.
The improvements in hospitalization and surgery rates became apparent as quickly as 5 months after therapy initiation. By 9 months after dual therapy began, there was an 86% decrease in hospitalization and a 92% decrease in surgery compared with the rates in those who had not taken these medications.
The study shows that aggressive treatment of inflammatory bowel disease can reap robust results, Dr. Neena S. Abraham and colleagues reported in the Aug. 29 issue of Clinical Gastroenterology and Hepatology (doi:10.1016/j.cgh.2013.04.051).
The results probably underestimate the potential benefits of dual therapy, wrote Dr. Abraham of the Mayo Clinic, Scottsdale, Ariz., and associates. Only 11% of patients in the database took one of the studied treatment regimens, and of those, most (85%) got an immunomodulator only.
"Given the paucity prescribed dual therapy (8.5%), the dose-response data are even more impressive and suggest that if dual therapy had been initiated earlier, greater benefit may have been observed," the investigators wrote.
The study examined 1-year hospitalization and surgical rates in 20,474 patients with either ulcerative colitis or Crohn’s disease. The patients were all included in a database that covered 176 U.S. Department of Veteran Affairs facilities.
Three treatment protocols were examined: immunomodulator monotherapy, anti–tumor necrosis factor (TNF)-alpha monotherapy with infliximab, and dual therapy with an immunomodulator and infliximab.
Most of the patients (12,432) had ulcerative colitis (UC); the remainder had Crohn’s disease (CD). Most (94%) were male; the mean age was 72 years.
The most common strategy was the anti–TNF-alpha alone (8%). Among patients receiving infliximab, 63% had evidence of induction therapy preceding a maintenance regimen.
"Despite their clear therapeutic benefit, less than 15% of patients with inflammatory bowel disease receive anti-TNF monotherapy, and 40% of patients with active CD receive anti-TNF agents in combination with immunomodulator agents (thiopurines or methotrexate)," they commented.
Most patients (66%) were taking other drugs, including steroids (14%), nonsteroidal anti-inflammatory agents (39%), aspirin (21%), cyclosporine (0.21%), antimetabolites (0.67%), and antibiotics (29%).
A 50% relative reduction in hospitalization occurred at 7.7 months with dual therapy compared with 9 months with immunomodulator monotherapy and 8 months with anti–TNF-alpha therapy. All of these differences were statistically significant after the model was adjusted for diagnosis (UC or CD), smoking status, race/ethnicity, and other medications that could modify the treatment effect.
By 1 year, there was a 45% relative reduction in hospitalization for immunomodulator therapy and a 78% relative reduction with anti–TNF-alpha monotherapy. But patients taking dual therapy reached a similar reduction of 73% by 9 months.
"Results suggested that, if dual therapy had been initiated earlier, perhaps a greater response in the outcome may have been observed," the investigators wrote.
There was a similar beneficial effect on surgeries related to the disorders. In the first year of treatment, there were 276 procedures. By 9 months, there was a 28% risk reduction associated with immunomodulator monotherapy, a 90% reduction associated with anti–TNF-alpha monotherapy, and a 92% reduction associated with dual therapy.
This also suggests that a "greater response may have been observed with earlier initiation of dual therapy," the authors said.
Safety concerns may be one reason for the dearth of these treatment protocols, the authors noted. However, recent long-term safety data suggest that there is a very low risk of mortality associated with them.
"[Five-year] outcome data on infliximab use has failed to demonstrate increased risk of mortality, and, although increased risk of infection was observed, the presence of severe disease and use of prednisone or narcotics carried higher risks," they said, referring to a 2012 study (Am. J. Gastroenterol. 2012;107:1409-22).
A 2011 study also suggested that the benefits of dual therapy outweigh the risks of developing a serious infection or cancer (Clin. J. Gastroenterol. Hepatol. 2012;10:46-51).
Janssen Biotech funded the study. None of the authors reported having any relevant financial disclosures.
Early dual therapy with infliximab and an immunomodulator significantly decreased the 1-year risk of hospitalization and surgery in patients with inflammatory bowel disease, in a cohort study of almost 20,500 patients.
The improvements in hospitalization and surgery rates became apparent as quickly as 5 months after therapy initiation. By 9 months after dual therapy began, there was an 86% decrease in hospitalization and a 92% decrease in surgery compared with the rates in those who had not taken these medications.
The study shows that aggressive treatment of inflammatory bowel disease can reap robust results, Dr. Neena S. Abraham and colleagues reported in the Aug. 29 issue of Clinical Gastroenterology and Hepatology (doi:10.1016/j.cgh.2013.04.051).
The results probably underestimate the potential benefits of dual therapy, wrote Dr. Abraham of the Mayo Clinic, Scottsdale, Ariz., and associates. Only 11% of patients in the database took one of the studied treatment regimens, and of those, most (85%) got an immunomodulator only.
"Given the paucity prescribed dual therapy (8.5%), the dose-response data are even more impressive and suggest that if dual therapy had been initiated earlier, greater benefit may have been observed," the investigators wrote.
The study examined 1-year hospitalization and surgical rates in 20,474 patients with either ulcerative colitis or Crohn’s disease. The patients were all included in a database that covered 176 U.S. Department of Veteran Affairs facilities.
Three treatment protocols were examined: immunomodulator monotherapy, anti–tumor necrosis factor (TNF)-alpha monotherapy with infliximab, and dual therapy with an immunomodulator and infliximab.
Most of the patients (12,432) had ulcerative colitis (UC); the remainder had Crohn’s disease (CD). Most (94%) were male; the mean age was 72 years.
The most common strategy was the anti–TNF-alpha alone (8%). Among patients receiving infliximab, 63% had evidence of induction therapy preceding a maintenance regimen.
"Despite their clear therapeutic benefit, less than 15% of patients with inflammatory bowel disease receive anti-TNF monotherapy, and 40% of patients with active CD receive anti-TNF agents in combination with immunomodulator agents (thiopurines or methotrexate)," they commented.
Most patients (66%) were taking other drugs, including steroids (14%), nonsteroidal anti-inflammatory agents (39%), aspirin (21%), cyclosporine (0.21%), antimetabolites (0.67%), and antibiotics (29%).
A 50% relative reduction in hospitalization occurred at 7.7 months with dual therapy compared with 9 months with immunomodulator monotherapy and 8 months with anti–TNF-alpha therapy. All of these differences were statistically significant after the model was adjusted for diagnosis (UC or CD), smoking status, race/ethnicity, and other medications that could modify the treatment effect.
By 1 year, there was a 45% relative reduction in hospitalization for immunomodulator therapy and a 78% relative reduction with anti–TNF-alpha monotherapy. But patients taking dual therapy reached a similar reduction of 73% by 9 months.
"Results suggested that, if dual therapy had been initiated earlier, perhaps a greater response in the outcome may have been observed," the investigators wrote.
There was a similar beneficial effect on surgeries related to the disorders. In the first year of treatment, there were 276 procedures. By 9 months, there was a 28% risk reduction associated with immunomodulator monotherapy, a 90% reduction associated with anti–TNF-alpha monotherapy, and a 92% reduction associated with dual therapy.
This also suggests that a "greater response may have been observed with earlier initiation of dual therapy," the authors said.
Safety concerns may be one reason for the dearth of these treatment protocols, the authors noted. However, recent long-term safety data suggest that there is a very low risk of mortality associated with them.
"[Five-year] outcome data on infliximab use has failed to demonstrate increased risk of mortality, and, although increased risk of infection was observed, the presence of severe disease and use of prednisone or narcotics carried higher risks," they said, referring to a 2012 study (Am. J. Gastroenterol. 2012;107:1409-22).
A 2011 study also suggested that the benefits of dual therapy outweigh the risks of developing a serious infection or cancer (Clin. J. Gastroenterol. Hepatol. 2012;10:46-51).
Janssen Biotech funded the study. None of the authors reported having any relevant financial disclosures.
Early dual therapy with infliximab and an immunomodulator significantly decreased the 1-year risk of hospitalization and surgery in patients with inflammatory bowel disease, in a cohort study of almost 20,500 patients.
The improvements in hospitalization and surgery rates became apparent as quickly as 5 months after therapy initiation. By 9 months after dual therapy began, there was an 86% decrease in hospitalization and a 92% decrease in surgery compared with the rates in those who had not taken these medications.
The study shows that aggressive treatment of inflammatory bowel disease can reap robust results, Dr. Neena S. Abraham and colleagues reported in the Aug. 29 issue of Clinical Gastroenterology and Hepatology (doi:10.1016/j.cgh.2013.04.051).
The results probably underestimate the potential benefits of dual therapy, wrote Dr. Abraham of the Mayo Clinic, Scottsdale, Ariz., and associates. Only 11% of patients in the database took one of the studied treatment regimens, and of those, most (85%) got an immunomodulator only.
"Given the paucity prescribed dual therapy (8.5%), the dose-response data are even more impressive and suggest that if dual therapy had been initiated earlier, greater benefit may have been observed," the investigators wrote.
The study examined 1-year hospitalization and surgical rates in 20,474 patients with either ulcerative colitis or Crohn’s disease. The patients were all included in a database that covered 176 U.S. Department of Veteran Affairs facilities.
Three treatment protocols were examined: immunomodulator monotherapy, anti–tumor necrosis factor (TNF)-alpha monotherapy with infliximab, and dual therapy with an immunomodulator and infliximab.
Most of the patients (12,432) had ulcerative colitis (UC); the remainder had Crohn’s disease (CD). Most (94%) were male; the mean age was 72 years.
The most common strategy was the anti–TNF-alpha alone (8%). Among patients receiving infliximab, 63% had evidence of induction therapy preceding a maintenance regimen.
"Despite their clear therapeutic benefit, less than 15% of patients with inflammatory bowel disease receive anti-TNF monotherapy, and 40% of patients with active CD receive anti-TNF agents in combination with immunomodulator agents (thiopurines or methotrexate)," they commented.
Most patients (66%) were taking other drugs, including steroids (14%), nonsteroidal anti-inflammatory agents (39%), aspirin (21%), cyclosporine (0.21%), antimetabolites (0.67%), and antibiotics (29%).
A 50% relative reduction in hospitalization occurred at 7.7 months with dual therapy compared with 9 months with immunomodulator monotherapy and 8 months with anti–TNF-alpha therapy. All of these differences were statistically significant after the model was adjusted for diagnosis (UC or CD), smoking status, race/ethnicity, and other medications that could modify the treatment effect.
By 1 year, there was a 45% relative reduction in hospitalization for immunomodulator therapy and a 78% relative reduction with anti–TNF-alpha monotherapy. But patients taking dual therapy reached a similar reduction of 73% by 9 months.
"Results suggested that, if dual therapy had been initiated earlier, perhaps a greater response in the outcome may have been observed," the investigators wrote.
There was a similar beneficial effect on surgeries related to the disorders. In the first year of treatment, there were 276 procedures. By 9 months, there was a 28% risk reduction associated with immunomodulator monotherapy, a 90% reduction associated with anti–TNF-alpha monotherapy, and a 92% reduction associated with dual therapy.
This also suggests that a "greater response may have been observed with earlier initiation of dual therapy," the authors said.
Safety concerns may be one reason for the dearth of these treatment protocols, the authors noted. However, recent long-term safety data suggest that there is a very low risk of mortality associated with them.
"[Five-year] outcome data on infliximab use has failed to demonstrate increased risk of mortality, and, although increased risk of infection was observed, the presence of severe disease and use of prednisone or narcotics carried higher risks," they said, referring to a 2012 study (Am. J. Gastroenterol. 2012;107:1409-22).
A 2011 study also suggested that the benefits of dual therapy outweigh the risks of developing a serious infection or cancer (Clin. J. Gastroenterol. Hepatol. 2012;10:46-51).
Janssen Biotech funded the study. None of the authors reported having any relevant financial disclosures.
FROM CLINICAL GASTROENTERGOLOGY AND HEPATOLOGY
Major finding: For patients with inflammatory bowel disease, dual therapy with infliximab and an immunomodulator was associated with a 50% decrease in hospitalizations by 7.7 months, compared with 8 months with anti–TNF-alpha monotherapy and 9 months with immunomodulator monotherapy.
Data source: A study of 20,474 patients with ulcerative colitis or Crohn’s disease.
Disclosures: Janssen Biotech funded the study. None of the authors reported having any relevant financial disclosures.
Incisional negative pressure cuts infection risk after colorectal surgery
PHOENIX – Applying continuous negative pressure to the incisional wound sharply reduces the incidence of surgical site infection after open colorectal surgery, according to results from a retrospective study.
A team led by Dr. Allison M. Bonds, a general surgery resident at the University of Texas Southwestern Medical Center at Dallas, studied 254 patients who underwent open colorectal surgery, whether planned or converted from a laparoscopic procedure.
In 13% of the patients, surgeons used incisional negative-pressure wound therapy, which entails standard wound closure followed by placement of a wound vacuum device over the completed stapled skin closure.
Study results, reported at the annual meeting of the American Society of Colon and Rectal Surgeons, showed that relative to the group receiving usual wound care, patients receiving incisional negative-pressure wound therapy were two-thirds less likely to develop a surgical site infection.
"Our study, although a retrospective chart review, does seem to show that the use of incisional negative-pressure wound therapy is associated with a decreased risk of surgical site infection," Dr. Bonds asserted. "This finding is significant enough that we feel it further needs a randomized controlled trial to see if there is actually a significant effect in the colorectal population."
Several attendees wondered about the cost of the negative-pressure wound therapy and how that was covered in the study population.
"We didn’t do an official cost analysis," Dr. Bonds replied. "Normally, the device that we used is associated with about $200 extra initially and then ... another $500 a day to use. So it is a fairly expensive addition to the care of the patients." She said she did not have data on how this cost was covered.
Dr. Jason Hall of the Lahey Clinic in Burlington, Mass., asked, "What was the indication to use the vac in those 32 patients?" and further wondered whether the patients receiving this therapy differed in ways that may have confounded the results.
"Placement of the vacuum wound device was left to the discretion of the surgeons," Dr. Bonds replied. "It’s hard to know exactly which patients would have been chosen for the study. There is some chance that the surgeons would have chosen the patients that they didn’t think would have a high rate of infection risk. But from our talking with the surgeons who use this, we believe that most of the vacuum devices were placed on patients who they had a high suspicion were going to get surgical site infections."
She agreed that there might have been selection bias at play, despite the study’s use of multivariate analysis. "That’s exactly why we believe that a randomized controlled trial is really the only way to show whether this is going to be a good technique to use or not," she said.
Cost of the therapy and its coverage will be major issues going forward, according to session comoderator Dr. Mark Welton of Stanford (Calif.) University. "Any time you are talking about downstream benefit to the insurer, they really need to see robust data before they are going to start to pay for that. So, especially in today’s health care environment, it’s going to come back to the patient paying for it. If you could talk about driving the cost associated with the wound infection down significantly, then the insurance companies would pay for it."
"Interestingly, there are companies coming out producing less expensive and less cumbersome devices. So I think it’s actually a very exciting idea, it’s intriguing. But we have a long way to go, and we do get to this cost-benefit question, and who’s going to pay for it," he said in an interview.
Dr. Kim Rhoads, the other session comoderator, also of Stanford University, said that "it’s an interesting concept," but she would like to see a standardized protocol detailing, for example, whether the vacuum and dressing are changed at some point and how long it has to be used for benefit; additionally, the indication for use should be worked out.
Also, "what we didn’t hear is how much fluid actually comes out ... because if nothing is coming out, you have to ask, what’s happening here and would that patient not have otherwise been wound infection free," she said. "We don’t know."
Incisional negative-pressure wound therapy has been used in orthopedic surgery for several years, according to Dr. Bonds. "At UT Southwestern, we began using this in 2010 [in colorectal surgery], and anecdotally saw that it seemed to be decreasing the rate of infections in our patients, so we thought that this warranted further study," she explained.
With this therapy, surgeons close the incision with standard staples, apply a strip of bridge dressing (GranuFoam, made by KCI), and cover the area with clear occlusion tape. The vacuum device (V.A.C. Therapy, made by KCI) is then applied at 75 mm Hg of continuous suction; in patients having a stoma, the stoma is returned after the device is in place.
In the study, the vacuum device was left on until postoperative day 5 or 7, and was removed before patients were discharged, according to Dr. Bonds.
Overall, 27.2% of the patients developed a surgical site infection. The rate was 12.5% in the group given incisional negative-pressure wound therapy, compared with 29.3% in the group given standard care.
In a multivariate analysis, patients in the negative-pressure wound therapy group were 68% less likely to develop a surgical site infection (odds ratio, 0.32; P = .04).
The only other independent predictor of this outcome was diabetes mellitus, which was associated with roughly a doubling of risk (OR, 1.98; P = .03).
"There are several proposed mechanisms for why this therapy would work," Dr. Bonds noted. The device prevents the incision from coming into contact with the surrounding environment, and decreases patient mobility and shear forces on the wound.
"In addition, the continuous suction seems to remove infectious material and the interstitial fluid, thereby decreasing the wound edema. Studies have also shown that the wound vacuum device increases vascularity to the wound, which would seem to help it heal as well," she said.
Dr. Bonds disclosed no relevant conflicts of interest. One coinvestigator has an affiliation with KCI.
PHOENIX – Applying continuous negative pressure to the incisional wound sharply reduces the incidence of surgical site infection after open colorectal surgery, according to results from a retrospective study.
A team led by Dr. Allison M. Bonds, a general surgery resident at the University of Texas Southwestern Medical Center at Dallas, studied 254 patients who underwent open colorectal surgery, whether planned or converted from a laparoscopic procedure.
In 13% of the patients, surgeons used incisional negative-pressure wound therapy, which entails standard wound closure followed by placement of a wound vacuum device over the completed stapled skin closure.
Study results, reported at the annual meeting of the American Society of Colon and Rectal Surgeons, showed that relative to the group receiving usual wound care, patients receiving incisional negative-pressure wound therapy were two-thirds less likely to develop a surgical site infection.
"Our study, although a retrospective chart review, does seem to show that the use of incisional negative-pressure wound therapy is associated with a decreased risk of surgical site infection," Dr. Bonds asserted. "This finding is significant enough that we feel it further needs a randomized controlled trial to see if there is actually a significant effect in the colorectal population."
Several attendees wondered about the cost of the negative-pressure wound therapy and how that was covered in the study population.
"We didn’t do an official cost analysis," Dr. Bonds replied. "Normally, the device that we used is associated with about $200 extra initially and then ... another $500 a day to use. So it is a fairly expensive addition to the care of the patients." She said she did not have data on how this cost was covered.
Dr. Jason Hall of the Lahey Clinic in Burlington, Mass., asked, "What was the indication to use the vac in those 32 patients?" and further wondered whether the patients receiving this therapy differed in ways that may have confounded the results.
"Placement of the vacuum wound device was left to the discretion of the surgeons," Dr. Bonds replied. "It’s hard to know exactly which patients would have been chosen for the study. There is some chance that the surgeons would have chosen the patients that they didn’t think would have a high rate of infection risk. But from our talking with the surgeons who use this, we believe that most of the vacuum devices were placed on patients who they had a high suspicion were going to get surgical site infections."
She agreed that there might have been selection bias at play, despite the study’s use of multivariate analysis. "That’s exactly why we believe that a randomized controlled trial is really the only way to show whether this is going to be a good technique to use or not," she said.
Cost of the therapy and its coverage will be major issues going forward, according to session comoderator Dr. Mark Welton of Stanford (Calif.) University. "Any time you are talking about downstream benefit to the insurer, they really need to see robust data before they are going to start to pay for that. So, especially in today’s health care environment, it’s going to come back to the patient paying for it. If you could talk about driving the cost associated with the wound infection down significantly, then the insurance companies would pay for it."
"Interestingly, there are companies coming out producing less expensive and less cumbersome devices. So I think it’s actually a very exciting idea, it’s intriguing. But we have a long way to go, and we do get to this cost-benefit question, and who’s going to pay for it," he said in an interview.
Dr. Kim Rhoads, the other session comoderator, also of Stanford University, said that "it’s an interesting concept," but she would like to see a standardized protocol detailing, for example, whether the vacuum and dressing are changed at some point and how long it has to be used for benefit; additionally, the indication for use should be worked out.
Also, "what we didn’t hear is how much fluid actually comes out ... because if nothing is coming out, you have to ask, what’s happening here and would that patient not have otherwise been wound infection free," she said. "We don’t know."
Incisional negative-pressure wound therapy has been used in orthopedic surgery for several years, according to Dr. Bonds. "At UT Southwestern, we began using this in 2010 [in colorectal surgery], and anecdotally saw that it seemed to be decreasing the rate of infections in our patients, so we thought that this warranted further study," she explained.
With this therapy, surgeons close the incision with standard staples, apply a strip of bridge dressing (GranuFoam, made by KCI), and cover the area with clear occlusion tape. The vacuum device (V.A.C. Therapy, made by KCI) is then applied at 75 mm Hg of continuous suction; in patients having a stoma, the stoma is returned after the device is in place.
In the study, the vacuum device was left on until postoperative day 5 or 7, and was removed before patients were discharged, according to Dr. Bonds.
Overall, 27.2% of the patients developed a surgical site infection. The rate was 12.5% in the group given incisional negative-pressure wound therapy, compared with 29.3% in the group given standard care.
In a multivariate analysis, patients in the negative-pressure wound therapy group were 68% less likely to develop a surgical site infection (odds ratio, 0.32; P = .04).
The only other independent predictor of this outcome was diabetes mellitus, which was associated with roughly a doubling of risk (OR, 1.98; P = .03).
"There are several proposed mechanisms for why this therapy would work," Dr. Bonds noted. The device prevents the incision from coming into contact with the surrounding environment, and decreases patient mobility and shear forces on the wound.
"In addition, the continuous suction seems to remove infectious material and the interstitial fluid, thereby decreasing the wound edema. Studies have also shown that the wound vacuum device increases vascularity to the wound, which would seem to help it heal as well," she said.
Dr. Bonds disclosed no relevant conflicts of interest. One coinvestigator has an affiliation with KCI.
PHOENIX – Applying continuous negative pressure to the incisional wound sharply reduces the incidence of surgical site infection after open colorectal surgery, according to results from a retrospective study.
A team led by Dr. Allison M. Bonds, a general surgery resident at the University of Texas Southwestern Medical Center at Dallas, studied 254 patients who underwent open colorectal surgery, whether planned or converted from a laparoscopic procedure.
In 13% of the patients, surgeons used incisional negative-pressure wound therapy, which entails standard wound closure followed by placement of a wound vacuum device over the completed stapled skin closure.
Study results, reported at the annual meeting of the American Society of Colon and Rectal Surgeons, showed that relative to the group receiving usual wound care, patients receiving incisional negative-pressure wound therapy were two-thirds less likely to develop a surgical site infection.
"Our study, although a retrospective chart review, does seem to show that the use of incisional negative-pressure wound therapy is associated with a decreased risk of surgical site infection," Dr. Bonds asserted. "This finding is significant enough that we feel it further needs a randomized controlled trial to see if there is actually a significant effect in the colorectal population."
Several attendees wondered about the cost of the negative-pressure wound therapy and how that was covered in the study population.
"We didn’t do an official cost analysis," Dr. Bonds replied. "Normally, the device that we used is associated with about $200 extra initially and then ... another $500 a day to use. So it is a fairly expensive addition to the care of the patients." She said she did not have data on how this cost was covered.
Dr. Jason Hall of the Lahey Clinic in Burlington, Mass., asked, "What was the indication to use the vac in those 32 patients?" and further wondered whether the patients receiving this therapy differed in ways that may have confounded the results.
"Placement of the vacuum wound device was left to the discretion of the surgeons," Dr. Bonds replied. "It’s hard to know exactly which patients would have been chosen for the study. There is some chance that the surgeons would have chosen the patients that they didn’t think would have a high rate of infection risk. But from our talking with the surgeons who use this, we believe that most of the vacuum devices were placed on patients who they had a high suspicion were going to get surgical site infections."
She agreed that there might have been selection bias at play, despite the study’s use of multivariate analysis. "That’s exactly why we believe that a randomized controlled trial is really the only way to show whether this is going to be a good technique to use or not," she said.
Cost of the therapy and its coverage will be major issues going forward, according to session comoderator Dr. Mark Welton of Stanford (Calif.) University. "Any time you are talking about downstream benefit to the insurer, they really need to see robust data before they are going to start to pay for that. So, especially in today’s health care environment, it’s going to come back to the patient paying for it. If you could talk about driving the cost associated with the wound infection down significantly, then the insurance companies would pay for it."
"Interestingly, there are companies coming out producing less expensive and less cumbersome devices. So I think it’s actually a very exciting idea, it’s intriguing. But we have a long way to go, and we do get to this cost-benefit question, and who’s going to pay for it," he said in an interview.
Dr. Kim Rhoads, the other session comoderator, also of Stanford University, said that "it’s an interesting concept," but she would like to see a standardized protocol detailing, for example, whether the vacuum and dressing are changed at some point and how long it has to be used for benefit; additionally, the indication for use should be worked out.
Also, "what we didn’t hear is how much fluid actually comes out ... because if nothing is coming out, you have to ask, what’s happening here and would that patient not have otherwise been wound infection free," she said. "We don’t know."
Incisional negative-pressure wound therapy has been used in orthopedic surgery for several years, according to Dr. Bonds. "At UT Southwestern, we began using this in 2010 [in colorectal surgery], and anecdotally saw that it seemed to be decreasing the rate of infections in our patients, so we thought that this warranted further study," she explained.
With this therapy, surgeons close the incision with standard staples, apply a strip of bridge dressing (GranuFoam, made by KCI), and cover the area with clear occlusion tape. The vacuum device (V.A.C. Therapy, made by KCI) is then applied at 75 mm Hg of continuous suction; in patients having a stoma, the stoma is returned after the device is in place.
In the study, the vacuum device was left on until postoperative day 5 or 7, and was removed before patients were discharged, according to Dr. Bonds.
Overall, 27.2% of the patients developed a surgical site infection. The rate was 12.5% in the group given incisional negative-pressure wound therapy, compared with 29.3% in the group given standard care.
In a multivariate analysis, patients in the negative-pressure wound therapy group were 68% less likely to develop a surgical site infection (odds ratio, 0.32; P = .04).
The only other independent predictor of this outcome was diabetes mellitus, which was associated with roughly a doubling of risk (OR, 1.98; P = .03).
"There are several proposed mechanisms for why this therapy would work," Dr. Bonds noted. The device prevents the incision from coming into contact with the surrounding environment, and decreases patient mobility and shear forces on the wound.
"In addition, the continuous suction seems to remove infectious material and the interstitial fluid, thereby decreasing the wound edema. Studies have also shown that the wound vacuum device increases vascularity to the wound, which would seem to help it heal as well," she said.
Dr. Bonds disclosed no relevant conflicts of interest. One coinvestigator has an affiliation with KCI.
AT THE ASCRS ANNUAL MEETING
Major finding: Compared with patients managed with usual wound care, patients managed with incisional negative-pressure wound therapy were 68% less likely to develop a surgical site infection.
Data source: A chart review of 254 patients undergoing open colorectal surgery
Disclosures: Dr. Bonds disclosed no relevant conflicts of interest. One coinvestigator has an affiliation with KCI.