User login
What Are the Indications for a Blood Transfusion?
Case
A 65-year-old man with a history of coronary artery disease (CAD) presents to the ED after a mechanical fall. He was found to have a hip fracture, admitted to orthopedic service, and underwent an uneventful hip repair. His post-operative course was uncomplicated, except for his hemoglobin level of 7.5 g/dL, which had decreased from his pre-operative hemoglobin of 11.2 g/dL. The patient was without cardiac symptoms, was ambulating with assistance, had normal vital signs, and was otherwise having an unremarkable recovery. The orthopedic surgeon, who recently heard that you do not have to transfuse patients unless their hemoglobin is less than 7 g/dL, consulted the hospitalist to help make the decision. What would your recommendation be?
Overview
Blood transfusions are a common medical procedure routinely given in the hospital.1 An estimated 15 million red blood cell (RBC) units are transfused each year in the United States.2 Despite its common use, the clinical indications for transfusion continue to be the subject of considerable debate. Most clinicians would agree that treating a patient with a low hemoglobin level and symptoms of anemia is reasonable.1,3 However, in the absence of overt symptoms, there is debate about when transfusions are appropriate.2,3
Because tissue oxygen delivery is dependent on hemoglobin and cardiac output, past medical practice has supported the use of the “golden 10/30 rule,” by which patients are transfused to a hemoglobin concentration of 10 g/dL or a hematocrit of 30%, regardless of symptoms. The rationale for this approach is based on physiologic evidence that cardiac output increases when hemoglobin falls below 7 g/dl. In patients with cardiac disease, the ability to increase cardiac output is compromised. Therefore, in order to reduce strain on the heart, hemoglobin levels historically have been kept higher than this threshold.
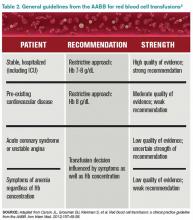
However, several studies have forced us to re-evaluate this old paradigm, including increasing concern for the infectious and noninfectious complications associated with blood transfusions and the need for cost containment (see Table 1).1,2,4 Due to improved blood screening, infectious complications from transfusions have been greatly reduced; noninfectious complications are 1,000 times more likely than infectious ones.
Review of Data
Although a number of studies have been performed on the indications for blood transfusions, many of the trials conducted in the past were too small to substantiate a certain practice. However, three trials with a large number of participants have allowed for a more evidence-based approach to blood transfusions. The studies address different patient populations to help broaden the restrictive transfusion approach to a larger range of patients.
TRICC trial: critically ill patients5. The TRICC trial was the first major study that compared a liberal transfusion strategy (transfuse when Hb <10 g/dL) to a more conservative approach (transfuse when Hb <7 g/dL). In this multicenter, randomized controlled trial, Hébert et al enrolled 418 critically ill patients and found that there was no significant difference in 30-day all-cause mortality between the restrictive-strategy group (18.7%) and the liberal-strategy group (23.3%).
However, in the pre-determined subgroup analysis, patients who were less severely ill (APACHE II scores of <20) had 30-day all-cause mortality of 8.7%, compared with 16.1% in the liberal-strategy group. Interestingly, there were more cardiac complications (pulmonary edema, angina, MI, and cardiac arrest) in the liberal-strategy group (21%) compared with the restrictive-strategy group (13%). Despite this finding, 30-day mortality was not significantly different in patients with clinically significant cardiac disease (primary or secondary diagnosis of cardiac disease [20.5% restrictive versus 22.9% liberal]).
An average of 2.6 units of RBCs per patient were given in the restrictive group, while 5.6 units were given to patients in the liberal group. This reflects a 54% decrease in the number of transfusions used in the conservative group. All the patients in the liberal group received transfusions, while 33% of the restrictive group’s patients received no blood at all.
The results of this trial suggested that there is no clinical advantage in transfusing ICU patients to Hb values above 9 g/dL, even if they have a history of cardiac disease. In fact, it may be harmful to practice a liberal transfusion strategy in critically ill younger patients (<55 years old) and those who are less severely ill (APACHE II <20).5
FOCUS trial: hip surgery and history of cardiac disease6. The FOCUS trial is a recent study that looked at the optimal hemoglobin level at which an RBC transfusion is beneficial for patients undergoing hip surgery. This study enrolled patients aged 50 or older who had a history or risk factors for cardiovascular disease (clinical evidence of cardiovascular disease: h/o ischemic heart disease, EKG evidence of previous MI, h/o CHF/PVD, h/o stroke/TIA, h/o HTN, DM, hyperlipidemia (TC >200/LDL >130), current tobacco use, or Cr>2.0), who were undergoing primary surgical repair of a hip fracture, and who had Hb <10g/dL within three days after surgery.
More than 2,000 patients were assigned randomly to a liberal-strategy group (transfuse to maintain a Hb >10g/dL) or a restrictive strategy group (transfuse to maintain Hg >8g/dl or for symptoms or signs of anemia). These signs/symptoms included chest pain that was possibly cardiac-related, congestive heart failure, tachycardia, and unresponsive hypotension. The primary outcomes were mortality or inability to walk 10 feet without assistance at 60-day follow-up.
The FOCUS trial found no statistically significant difference in mortality rate (7.6% in the liberal group versus 6.6% in the restrictive group) or in the ability to walk at 60 days (35.2% in the liberal group versus 34.7% in the restrictive group). There were no significant differences in the rates of in-hospital acute MI, unstable angina, or death between the two groups.
Patients in the restrictive-strategy group received 65% fewer units of blood than the liberal group, with 59% receiving no blood after surgery compared with 3% of the liberal group. Overall, the liberal group received 1,866 units of blood, compared with 652 units in the restrictive group.
This trial helps support the findings in previous trials, such as TRICC, by showing that a restrictive transfusion strategy using a trigger point of 8 g/dl does not increase mortality or cardiovascular complications and does not decrease functional ability after orthopedic surgery.
TRAC trial: patients after cardiac surgery7. The TRAC trial was a prospective randomized trial in 502 patients undergoing cardiac surgery that assigned 253 patients to the liberal-transfusion-strategy group (Hb >10g/dl) and 249 to the restrictive-strategy group (Hb >8 g/dl). In this study, the primary endpoint of all-cause 30-day mortality occurred in 10% of the liberal group and 11% of the restrictive group. This difference was not significant.
Subanalysis showed that blood transfusion in both groups was an independent risk factor for the occurrence of respiratory, cardiac, renal, and infectious complications, in addition to the composite end point of 30-day mortality—again highlighting the risk involved in of blood transfusions.
These results support the other trial conclusions that a restrictive transfusion strategy of maintaining a hematocrit of 24% (Hb 8 g/dL) is as safe as a more liberal strategy with a hematocrit of 30% (Hb 10 g/dL). It also offers further evidence of the risks of blood transfusions and supports the view that blood transfusions should never be given simply to correct low hemoglobin levels.
Cochrane Review. A recent Cochrane Review that comprised 19 trials with a combined total of 6,264 patients also supported a restrictive-strategy approach.8 In this review, no difference in mortality was established between the restrictive and liberal transfusion groups, with a trend toward decreased hospital mortality in the restrictive-transfusion group. The authors of the study felt that for most patients, blood transfusion is not necessary until hemoglobin levels drop below 7-8 g/dL but emphasized that this criteria should not be generalized to patients with an acute cardiac issue.
Back to the Case
In this case, the patient is doing well post-operatively and has no cardiac symptoms or hypotension. However, based on the new available data from the FOCUS trial, given the patient’s history of CAD, and the threshold of 8 g/dL used in the study, it was recommended that the patient be transfused.
Bottom Line
Current practice guidelines clearly support clinical judgment as the primary determinant in the decision to transfuse.2 However, current evidence is growing that our threshold for blood transfusions should be a hemoglobin level of 7-8 g/dl.
Dr. Chang is a hospitalist and assistant professor at Mount Sinai Medical Center in New York City, and is co-director of the medicine-geriatrics clerkship at the Icahn School of Medicine at Mount Sinai. Dr. Torgalkar is a hospitalist and assistant professor at Mount Sinai Medical Center.
References
- Sharma S, Sharma P, Tyler L. Transfusion of blood and blood products: indications and complications. Am Fam Physician. 2011;83:719-724.
- Carson JL, Grossman BJ, Kleinman S, et al. Red blood cell transfusion: a clinical practice guideline from the AABB. Ann Intern Med. 2012;157:49-58.
- Valeri CR, Crowley JP, Loscalzo J. The red cell transfusion trigger: has a sin of commission now become a sin of omission? Transfusion. 1998;38:602-610.
- Klein HG, Spahn DR, Carson JL. Red blood cell transfusion in clinical practice. Lancet. 2007;370(9585):415-426.
- Hébert PC, Wells G, Blajchman MA, et al. A multicenter, randomized, controlled clinical trial of transfusion requirements in critical care. N Engl J Med. 1999;340:409-17.
- Carson JL, Terrin ML, Noveck H, et al. Liberal or restrictive transfusion in high-risk patients after hip surgery. N Engl J Med. 2011;365:2453-2462.
- Hajjar LA, Vincent JL, Galas FR, et al. Transfusion requirements after cardiac surgery: the TRACS randomized controlled trial. JAMA. 2010;304:1559-1567.
- Carson JL, Carless PA, Hébert PC. Transfusion thresholds and other strategies for guiding allogeneic red blood cell transfusion. Cochrane Database Syst Rev. 2012; 4:CD002042.
Case
A 65-year-old man with a history of coronary artery disease (CAD) presents to the ED after a mechanical fall. He was found to have a hip fracture, admitted to orthopedic service, and underwent an uneventful hip repair. His post-operative course was uncomplicated, except for his hemoglobin level of 7.5 g/dL, which had decreased from his pre-operative hemoglobin of 11.2 g/dL. The patient was without cardiac symptoms, was ambulating with assistance, had normal vital signs, and was otherwise having an unremarkable recovery. The orthopedic surgeon, who recently heard that you do not have to transfuse patients unless their hemoglobin is less than 7 g/dL, consulted the hospitalist to help make the decision. What would your recommendation be?
Overview
Blood transfusions are a common medical procedure routinely given in the hospital.1 An estimated 15 million red blood cell (RBC) units are transfused each year in the United States.2 Despite its common use, the clinical indications for transfusion continue to be the subject of considerable debate. Most clinicians would agree that treating a patient with a low hemoglobin level and symptoms of anemia is reasonable.1,3 However, in the absence of overt symptoms, there is debate about when transfusions are appropriate.2,3
Because tissue oxygen delivery is dependent on hemoglobin and cardiac output, past medical practice has supported the use of the “golden 10/30 rule,” by which patients are transfused to a hemoglobin concentration of 10 g/dL or a hematocrit of 30%, regardless of symptoms. The rationale for this approach is based on physiologic evidence that cardiac output increases when hemoglobin falls below 7 g/dl. In patients with cardiac disease, the ability to increase cardiac output is compromised. Therefore, in order to reduce strain on the heart, hemoglobin levels historically have been kept higher than this threshold.
However, several studies have forced us to re-evaluate this old paradigm, including increasing concern for the infectious and noninfectious complications associated with blood transfusions and the need for cost containment (see Table 1).1,2,4 Due to improved blood screening, infectious complications from transfusions have been greatly reduced; noninfectious complications are 1,000 times more likely than infectious ones.
Review of Data
Although a number of studies have been performed on the indications for blood transfusions, many of the trials conducted in the past were too small to substantiate a certain practice. However, three trials with a large number of participants have allowed for a more evidence-based approach to blood transfusions. The studies address different patient populations to help broaden the restrictive transfusion approach to a larger range of patients.
TRICC trial: critically ill patients5. The TRICC trial was the first major study that compared a liberal transfusion strategy (transfuse when Hb <10 g/dL) to a more conservative approach (transfuse when Hb <7 g/dL). In this multicenter, randomized controlled trial, Hébert et al enrolled 418 critically ill patients and found that there was no significant difference in 30-day all-cause mortality between the restrictive-strategy group (18.7%) and the liberal-strategy group (23.3%).
However, in the pre-determined subgroup analysis, patients who were less severely ill (APACHE II scores of <20) had 30-day all-cause mortality of 8.7%, compared with 16.1% in the liberal-strategy group. Interestingly, there were more cardiac complications (pulmonary edema, angina, MI, and cardiac arrest) in the liberal-strategy group (21%) compared with the restrictive-strategy group (13%). Despite this finding, 30-day mortality was not significantly different in patients with clinically significant cardiac disease (primary or secondary diagnosis of cardiac disease [20.5% restrictive versus 22.9% liberal]).
An average of 2.6 units of RBCs per patient were given in the restrictive group, while 5.6 units were given to patients in the liberal group. This reflects a 54% decrease in the number of transfusions used in the conservative group. All the patients in the liberal group received transfusions, while 33% of the restrictive group’s patients received no blood at all.
The results of this trial suggested that there is no clinical advantage in transfusing ICU patients to Hb values above 9 g/dL, even if they have a history of cardiac disease. In fact, it may be harmful to practice a liberal transfusion strategy in critically ill younger patients (<55 years old) and those who are less severely ill (APACHE II <20).5
FOCUS trial: hip surgery and history of cardiac disease6. The FOCUS trial is a recent study that looked at the optimal hemoglobin level at which an RBC transfusion is beneficial for patients undergoing hip surgery. This study enrolled patients aged 50 or older who had a history or risk factors for cardiovascular disease (clinical evidence of cardiovascular disease: h/o ischemic heart disease, EKG evidence of previous MI, h/o CHF/PVD, h/o stroke/TIA, h/o HTN, DM, hyperlipidemia (TC >200/LDL >130), current tobacco use, or Cr>2.0), who were undergoing primary surgical repair of a hip fracture, and who had Hb <10g/dL within three days after surgery.
More than 2,000 patients were assigned randomly to a liberal-strategy group (transfuse to maintain a Hb >10g/dL) or a restrictive strategy group (transfuse to maintain Hg >8g/dl or for symptoms or signs of anemia). These signs/symptoms included chest pain that was possibly cardiac-related, congestive heart failure, tachycardia, and unresponsive hypotension. The primary outcomes were mortality or inability to walk 10 feet without assistance at 60-day follow-up.
The FOCUS trial found no statistically significant difference in mortality rate (7.6% in the liberal group versus 6.6% in the restrictive group) or in the ability to walk at 60 days (35.2% in the liberal group versus 34.7% in the restrictive group). There were no significant differences in the rates of in-hospital acute MI, unstable angina, or death between the two groups.
Patients in the restrictive-strategy group received 65% fewer units of blood than the liberal group, with 59% receiving no blood after surgery compared with 3% of the liberal group. Overall, the liberal group received 1,866 units of blood, compared with 652 units in the restrictive group.
This trial helps support the findings in previous trials, such as TRICC, by showing that a restrictive transfusion strategy using a trigger point of 8 g/dl does not increase mortality or cardiovascular complications and does not decrease functional ability after orthopedic surgery.
TRAC trial: patients after cardiac surgery7. The TRAC trial was a prospective randomized trial in 502 patients undergoing cardiac surgery that assigned 253 patients to the liberal-transfusion-strategy group (Hb >10g/dl) and 249 to the restrictive-strategy group (Hb >8 g/dl). In this study, the primary endpoint of all-cause 30-day mortality occurred in 10% of the liberal group and 11% of the restrictive group. This difference was not significant.
Subanalysis showed that blood transfusion in both groups was an independent risk factor for the occurrence of respiratory, cardiac, renal, and infectious complications, in addition to the composite end point of 30-day mortality—again highlighting the risk involved in of blood transfusions.
These results support the other trial conclusions that a restrictive transfusion strategy of maintaining a hematocrit of 24% (Hb 8 g/dL) is as safe as a more liberal strategy with a hematocrit of 30% (Hb 10 g/dL). It also offers further evidence of the risks of blood transfusions and supports the view that blood transfusions should never be given simply to correct low hemoglobin levels.
Cochrane Review. A recent Cochrane Review that comprised 19 trials with a combined total of 6,264 patients also supported a restrictive-strategy approach.8 In this review, no difference in mortality was established between the restrictive and liberal transfusion groups, with a trend toward decreased hospital mortality in the restrictive-transfusion group. The authors of the study felt that for most patients, blood transfusion is not necessary until hemoglobin levels drop below 7-8 g/dL but emphasized that this criteria should not be generalized to patients with an acute cardiac issue.
Back to the Case
In this case, the patient is doing well post-operatively and has no cardiac symptoms or hypotension. However, based on the new available data from the FOCUS trial, given the patient’s history of CAD, and the threshold of 8 g/dL used in the study, it was recommended that the patient be transfused.
Bottom Line
Current practice guidelines clearly support clinical judgment as the primary determinant in the decision to transfuse.2 However, current evidence is growing that our threshold for blood transfusions should be a hemoglobin level of 7-8 g/dl.
Dr. Chang is a hospitalist and assistant professor at Mount Sinai Medical Center in New York City, and is co-director of the medicine-geriatrics clerkship at the Icahn School of Medicine at Mount Sinai. Dr. Torgalkar is a hospitalist and assistant professor at Mount Sinai Medical Center.
References
- Sharma S, Sharma P, Tyler L. Transfusion of blood and blood products: indications and complications. Am Fam Physician. 2011;83:719-724.
- Carson JL, Grossman BJ, Kleinman S, et al. Red blood cell transfusion: a clinical practice guideline from the AABB. Ann Intern Med. 2012;157:49-58.
- Valeri CR, Crowley JP, Loscalzo J. The red cell transfusion trigger: has a sin of commission now become a sin of omission? Transfusion. 1998;38:602-610.
- Klein HG, Spahn DR, Carson JL. Red blood cell transfusion in clinical practice. Lancet. 2007;370(9585):415-426.
- Hébert PC, Wells G, Blajchman MA, et al. A multicenter, randomized, controlled clinical trial of transfusion requirements in critical care. N Engl J Med. 1999;340:409-17.
- Carson JL, Terrin ML, Noveck H, et al. Liberal or restrictive transfusion in high-risk patients after hip surgery. N Engl J Med. 2011;365:2453-2462.
- Hajjar LA, Vincent JL, Galas FR, et al. Transfusion requirements after cardiac surgery: the TRACS randomized controlled trial. JAMA. 2010;304:1559-1567.
- Carson JL, Carless PA, Hébert PC. Transfusion thresholds and other strategies for guiding allogeneic red blood cell transfusion. Cochrane Database Syst Rev. 2012; 4:CD002042.
Case
A 65-year-old man with a history of coronary artery disease (CAD) presents to the ED after a mechanical fall. He was found to have a hip fracture, admitted to orthopedic service, and underwent an uneventful hip repair. His post-operative course was uncomplicated, except for his hemoglobin level of 7.5 g/dL, which had decreased from his pre-operative hemoglobin of 11.2 g/dL. The patient was without cardiac symptoms, was ambulating with assistance, had normal vital signs, and was otherwise having an unremarkable recovery. The orthopedic surgeon, who recently heard that you do not have to transfuse patients unless their hemoglobin is less than 7 g/dL, consulted the hospitalist to help make the decision. What would your recommendation be?
Overview
Blood transfusions are a common medical procedure routinely given in the hospital.1 An estimated 15 million red blood cell (RBC) units are transfused each year in the United States.2 Despite its common use, the clinical indications for transfusion continue to be the subject of considerable debate. Most clinicians would agree that treating a patient with a low hemoglobin level and symptoms of anemia is reasonable.1,3 However, in the absence of overt symptoms, there is debate about when transfusions are appropriate.2,3
Because tissue oxygen delivery is dependent on hemoglobin and cardiac output, past medical practice has supported the use of the “golden 10/30 rule,” by which patients are transfused to a hemoglobin concentration of 10 g/dL or a hematocrit of 30%, regardless of symptoms. The rationale for this approach is based on physiologic evidence that cardiac output increases when hemoglobin falls below 7 g/dl. In patients with cardiac disease, the ability to increase cardiac output is compromised. Therefore, in order to reduce strain on the heart, hemoglobin levels historically have been kept higher than this threshold.
However, several studies have forced us to re-evaluate this old paradigm, including increasing concern for the infectious and noninfectious complications associated with blood transfusions and the need for cost containment (see Table 1).1,2,4 Due to improved blood screening, infectious complications from transfusions have been greatly reduced; noninfectious complications are 1,000 times more likely than infectious ones.
Review of Data
Although a number of studies have been performed on the indications for blood transfusions, many of the trials conducted in the past were too small to substantiate a certain practice. However, three trials with a large number of participants have allowed for a more evidence-based approach to blood transfusions. The studies address different patient populations to help broaden the restrictive transfusion approach to a larger range of patients.
TRICC trial: critically ill patients5. The TRICC trial was the first major study that compared a liberal transfusion strategy (transfuse when Hb <10 g/dL) to a more conservative approach (transfuse when Hb <7 g/dL). In this multicenter, randomized controlled trial, Hébert et al enrolled 418 critically ill patients and found that there was no significant difference in 30-day all-cause mortality between the restrictive-strategy group (18.7%) and the liberal-strategy group (23.3%).
However, in the pre-determined subgroup analysis, patients who were less severely ill (APACHE II scores of <20) had 30-day all-cause mortality of 8.7%, compared with 16.1% in the liberal-strategy group. Interestingly, there were more cardiac complications (pulmonary edema, angina, MI, and cardiac arrest) in the liberal-strategy group (21%) compared with the restrictive-strategy group (13%). Despite this finding, 30-day mortality was not significantly different in patients with clinically significant cardiac disease (primary or secondary diagnosis of cardiac disease [20.5% restrictive versus 22.9% liberal]).
An average of 2.6 units of RBCs per patient were given in the restrictive group, while 5.6 units were given to patients in the liberal group. This reflects a 54% decrease in the number of transfusions used in the conservative group. All the patients in the liberal group received transfusions, while 33% of the restrictive group’s patients received no blood at all.
The results of this trial suggested that there is no clinical advantage in transfusing ICU patients to Hb values above 9 g/dL, even if they have a history of cardiac disease. In fact, it may be harmful to practice a liberal transfusion strategy in critically ill younger patients (<55 years old) and those who are less severely ill (APACHE II <20).5
FOCUS trial: hip surgery and history of cardiac disease6. The FOCUS trial is a recent study that looked at the optimal hemoglobin level at which an RBC transfusion is beneficial for patients undergoing hip surgery. This study enrolled patients aged 50 or older who had a history or risk factors for cardiovascular disease (clinical evidence of cardiovascular disease: h/o ischemic heart disease, EKG evidence of previous MI, h/o CHF/PVD, h/o stroke/TIA, h/o HTN, DM, hyperlipidemia (TC >200/LDL >130), current tobacco use, or Cr>2.0), who were undergoing primary surgical repair of a hip fracture, and who had Hb <10g/dL within three days after surgery.
More than 2,000 patients were assigned randomly to a liberal-strategy group (transfuse to maintain a Hb >10g/dL) or a restrictive strategy group (transfuse to maintain Hg >8g/dl or for symptoms or signs of anemia). These signs/symptoms included chest pain that was possibly cardiac-related, congestive heart failure, tachycardia, and unresponsive hypotension. The primary outcomes were mortality or inability to walk 10 feet without assistance at 60-day follow-up.
The FOCUS trial found no statistically significant difference in mortality rate (7.6% in the liberal group versus 6.6% in the restrictive group) or in the ability to walk at 60 days (35.2% in the liberal group versus 34.7% in the restrictive group). There were no significant differences in the rates of in-hospital acute MI, unstable angina, or death between the two groups.
Patients in the restrictive-strategy group received 65% fewer units of blood than the liberal group, with 59% receiving no blood after surgery compared with 3% of the liberal group. Overall, the liberal group received 1,866 units of blood, compared with 652 units in the restrictive group.
This trial helps support the findings in previous trials, such as TRICC, by showing that a restrictive transfusion strategy using a trigger point of 8 g/dl does not increase mortality or cardiovascular complications and does not decrease functional ability after orthopedic surgery.
TRAC trial: patients after cardiac surgery7. The TRAC trial was a prospective randomized trial in 502 patients undergoing cardiac surgery that assigned 253 patients to the liberal-transfusion-strategy group (Hb >10g/dl) and 249 to the restrictive-strategy group (Hb >8 g/dl). In this study, the primary endpoint of all-cause 30-day mortality occurred in 10% of the liberal group and 11% of the restrictive group. This difference was not significant.
Subanalysis showed that blood transfusion in both groups was an independent risk factor for the occurrence of respiratory, cardiac, renal, and infectious complications, in addition to the composite end point of 30-day mortality—again highlighting the risk involved in of blood transfusions.
These results support the other trial conclusions that a restrictive transfusion strategy of maintaining a hematocrit of 24% (Hb 8 g/dL) is as safe as a more liberal strategy with a hematocrit of 30% (Hb 10 g/dL). It also offers further evidence of the risks of blood transfusions and supports the view that blood transfusions should never be given simply to correct low hemoglobin levels.
Cochrane Review. A recent Cochrane Review that comprised 19 trials with a combined total of 6,264 patients also supported a restrictive-strategy approach.8 In this review, no difference in mortality was established between the restrictive and liberal transfusion groups, with a trend toward decreased hospital mortality in the restrictive-transfusion group. The authors of the study felt that for most patients, blood transfusion is not necessary until hemoglobin levels drop below 7-8 g/dL but emphasized that this criteria should not be generalized to patients with an acute cardiac issue.
Back to the Case
In this case, the patient is doing well post-operatively and has no cardiac symptoms or hypotension. However, based on the new available data from the FOCUS trial, given the patient’s history of CAD, and the threshold of 8 g/dL used in the study, it was recommended that the patient be transfused.
Bottom Line
Current practice guidelines clearly support clinical judgment as the primary determinant in the decision to transfuse.2 However, current evidence is growing that our threshold for blood transfusions should be a hemoglobin level of 7-8 g/dl.
Dr. Chang is a hospitalist and assistant professor at Mount Sinai Medical Center in New York City, and is co-director of the medicine-geriatrics clerkship at the Icahn School of Medicine at Mount Sinai. Dr. Torgalkar is a hospitalist and assistant professor at Mount Sinai Medical Center.
References
- Sharma S, Sharma P, Tyler L. Transfusion of blood and blood products: indications and complications. Am Fam Physician. 2011;83:719-724.
- Carson JL, Grossman BJ, Kleinman S, et al. Red blood cell transfusion: a clinical practice guideline from the AABB. Ann Intern Med. 2012;157:49-58.
- Valeri CR, Crowley JP, Loscalzo J. The red cell transfusion trigger: has a sin of commission now become a sin of omission? Transfusion. 1998;38:602-610.
- Klein HG, Spahn DR, Carson JL. Red blood cell transfusion in clinical practice. Lancet. 2007;370(9585):415-426.
- Hébert PC, Wells G, Blajchman MA, et al. A multicenter, randomized, controlled clinical trial of transfusion requirements in critical care. N Engl J Med. 1999;340:409-17.
- Carson JL, Terrin ML, Noveck H, et al. Liberal or restrictive transfusion in high-risk patients after hip surgery. N Engl J Med. 2011;365:2453-2462.
- Hajjar LA, Vincent JL, Galas FR, et al. Transfusion requirements after cardiac surgery: the TRACS randomized controlled trial. JAMA. 2010;304:1559-1567.
- Carson JL, Carless PA, Hébert PC. Transfusion thresholds and other strategies for guiding allogeneic red blood cell transfusion. Cochrane Database Syst Rev. 2012; 4:CD002042.
Wasteful Practices in Hospital Cardiac Services Identified
A recent article in the American Journal of Medical Quality reviewed 366 cardiac-related medical studies and 21 practice guidelines to identify eight measures of potential waste in hospital cardiac services.4 The wasteful measures included excess use of higher-cost implantable cardioverter-defibrillators and similar cardiac devices, the use of dual-chamber defibrillators rather than single-chamber devices, and excess lengths of stay in the hospital. The eight measures were validated with data from 261 hospitals.
The authors emphasize that their set of measures is not designed to determine clinical appropriateness but to highlight areas of potential overutilization that can be benchmarked with other hospitals.
Larry Beresford is a freelance writer in San Francisco.
References
- Hartocollis A. With money at risk, hospitals push staff to wash hands. The New York Times website. Available at: http://www.nytimes.com/2013/05/29/nyregion/hospitals-struggle-to-get-workers-to-wash-their-hands.html?pagewanted=all&_r=0. Accessed May 28, 2013.
- Cumbler E, Castillo L, Satorie L, et al. Culture change in infection control: applying psychological principles to improve hand hygiene. J Nurs Care Qual. 2013 May 10 [Epub ahead of print].
- Bernhard B. High tech hand washing comes to St. Louis hospital. St. Louis Post-Dispatch website. Available at: http://www.stltoday.com/lifestyles/health-med-fit/health/high-tech-hand-washing-comes-to-st-louis-hospital/article_9379065d-85ff-5643-bae2-899254cb22fa.html. Accessed June 27, 2013.
- Lowe TJ, Partovian C, Kroch E, Martin J, Bankowitz R. Measuring cardiac waste: the Premier cardiac waste measures. Am J Med Qual. 2013 May 29 [Epub ahead of print].
- Elixhauser A, Steiner C. Readmissions to U.S. hospitals by diagnosis, 2010. Healthcare Cost and Utilization Project website. Available at: http://www.hcup-us.ahrq.gov/reports/statbriefs/sb153.pdf. Accessed July 15, 2013.
- Jackson Healthcare. Filling the void: 2013 physician outlook & practice trends. Jackson Healthcare website. Available at: http://www.jacksonhealthcare.com/media/193525/jc-2013physiciantrends-void_ebk0513.pdf. Accessed July 15, 2013.
A recent article in the American Journal of Medical Quality reviewed 366 cardiac-related medical studies and 21 practice guidelines to identify eight measures of potential waste in hospital cardiac services.4 The wasteful measures included excess use of higher-cost implantable cardioverter-defibrillators and similar cardiac devices, the use of dual-chamber defibrillators rather than single-chamber devices, and excess lengths of stay in the hospital. The eight measures were validated with data from 261 hospitals.
The authors emphasize that their set of measures is not designed to determine clinical appropriateness but to highlight areas of potential overutilization that can be benchmarked with other hospitals.
Larry Beresford is a freelance writer in San Francisco.
References
- Hartocollis A. With money at risk, hospitals push staff to wash hands. The New York Times website. Available at: http://www.nytimes.com/2013/05/29/nyregion/hospitals-struggle-to-get-workers-to-wash-their-hands.html?pagewanted=all&_r=0. Accessed May 28, 2013.
- Cumbler E, Castillo L, Satorie L, et al. Culture change in infection control: applying psychological principles to improve hand hygiene. J Nurs Care Qual. 2013 May 10 [Epub ahead of print].
- Bernhard B. High tech hand washing comes to St. Louis hospital. St. Louis Post-Dispatch website. Available at: http://www.stltoday.com/lifestyles/health-med-fit/health/high-tech-hand-washing-comes-to-st-louis-hospital/article_9379065d-85ff-5643-bae2-899254cb22fa.html. Accessed June 27, 2013.
- Lowe TJ, Partovian C, Kroch E, Martin J, Bankowitz R. Measuring cardiac waste: the Premier cardiac waste measures. Am J Med Qual. 2013 May 29 [Epub ahead of print].
- Elixhauser A, Steiner C. Readmissions to U.S. hospitals by diagnosis, 2010. Healthcare Cost and Utilization Project website. Available at: http://www.hcup-us.ahrq.gov/reports/statbriefs/sb153.pdf. Accessed July 15, 2013.
- Jackson Healthcare. Filling the void: 2013 physician outlook & practice trends. Jackson Healthcare website. Available at: http://www.jacksonhealthcare.com/media/193525/jc-2013physiciantrends-void_ebk0513.pdf. Accessed July 15, 2013.
A recent article in the American Journal of Medical Quality reviewed 366 cardiac-related medical studies and 21 practice guidelines to identify eight measures of potential waste in hospital cardiac services.4 The wasteful measures included excess use of higher-cost implantable cardioverter-defibrillators and similar cardiac devices, the use of dual-chamber defibrillators rather than single-chamber devices, and excess lengths of stay in the hospital. The eight measures were validated with data from 261 hospitals.
The authors emphasize that their set of measures is not designed to determine clinical appropriateness but to highlight areas of potential overutilization that can be benchmarked with other hospitals.
Larry Beresford is a freelance writer in San Francisco.
References
- Hartocollis A. With money at risk, hospitals push staff to wash hands. The New York Times website. Available at: http://www.nytimes.com/2013/05/29/nyregion/hospitals-struggle-to-get-workers-to-wash-their-hands.html?pagewanted=all&_r=0. Accessed May 28, 2013.
- Cumbler E, Castillo L, Satorie L, et al. Culture change in infection control: applying psychological principles to improve hand hygiene. J Nurs Care Qual. 2013 May 10 [Epub ahead of print].
- Bernhard B. High tech hand washing comes to St. Louis hospital. St. Louis Post-Dispatch website. Available at: http://www.stltoday.com/lifestyles/health-med-fit/health/high-tech-hand-washing-comes-to-st-louis-hospital/article_9379065d-85ff-5643-bae2-899254cb22fa.html. Accessed June 27, 2013.
- Lowe TJ, Partovian C, Kroch E, Martin J, Bankowitz R. Measuring cardiac waste: the Premier cardiac waste measures. Am J Med Qual. 2013 May 29 [Epub ahead of print].
- Elixhauser A, Steiner C. Readmissions to U.S. hospitals by diagnosis, 2010. Healthcare Cost and Utilization Project website. Available at: http://www.hcup-us.ahrq.gov/reports/statbriefs/sb153.pdf. Accessed July 15, 2013.
- Jackson Healthcare. Filling the void: 2013 physician outlook & practice trends. Jackson Healthcare website. Available at: http://www.jacksonhealthcare.com/media/193525/jc-2013physiciantrends-void_ebk0513.pdf. Accessed July 15, 2013.
Applied Psychology Improves Hand Hygiene in Hospitals
According to a recent New York Times report, hand-hygiene compliance in hospitals can be as low as 30%, with serious implications regarding hospital-acquired infections.1 While many initiatives have employed secret observers, vibrating badges, or hand-washing coaches, a Research, Innovations, and Clinical Vignettes (RIV) poster at HM13 outlined how a multidisciplinary committee at University of Colorado Hospital in Aurora applied principles of psychology to the challenge of compliance.2
The initiative focused on behavioral changes: surreptitiously auditing staff behaviors, real-time feedback, and immediate public corrections for observed nonadherence on the test unit from an infection-control champion. The study randomly assigned daily auditing responsibilities across all members of the nursing staff, including aides. Taking a page from soccer referees, auditors handed out red tickets to hygiene violators—and individually wrapped Life Savers to reinforce adherence.
When unprofessional behavior is the response to a verbal correction, leadership has to be prepared to act, explains hospitalist and lead author Ethan Cumbler, MD, FACP.
“We need to stop thinking about hospital staff and physicians as rational actors when it comes to hand hygiene, but as social animals who will respond to positive and negative reinforcements and group culture,” he says.
Noncompliant hand hygiene is largely unconscious behavior that needs to be brought to conscious attention but is amenable to change, Dr. Cumbler says, adding that “unit leadership steps in for repeated nonadherence or an unprofessional response to correction. We have never needed to intervene more than once with the same person.”
Hand-hygiene adherence reached 97% on the pilot unit in the second quarter of 2012 and has remained at that level, Dr. Cumbler says. Additionally, iatrogenic infections dropped to zero from 4.8 per 1,000 urinary catheter days, with bloodstream infections falling at a similar rate.
Similar results with hand-hygiene compliance have been reported at St. Mary’s Health Center in St. Louis, which has been testing a system that reminds nurses to wash their hands at various checkpoints in the hospital, tracking their compliance with a badge that turns green when registering the presence of hand sanitizer, thereby informing patients that the nurse’s hands are clean.
The system, developed by Biovigil Hygiene Technologies of Ann Arbor, Mich., started on two pilot units last year, where compliance has grown to 97% and 99%, respectively. System set-up can cost about $2,000 per patient room, plus monthly subscriptions per employee, but more hospitals in the system could sign on next year, reports the St. Louis Post-Dispatch.3
Larry Beresford is a freelance writer in San Francisco.
References
- Hartocollis A. With money at risk, hospitals push staff to wash hands. The New York Times website. Available at: http://www.nytimes.com/2013/05/29/nyregion/hospitals-struggle-to-get-workers-to-wash-their-hands.html?pagewanted=all&_r=0. Accessed May 28, 2013.
- Cumbler E, Castillo L, Satorie L, et al. Culture change in infection control: applying psychological principles to improve hand hygiene. J Nurs Care Qual. 2013 May 10 [Epub ahead of print].
- Bernhard B. High tech hand washing comes to St. Louis hospital. St. Louis Post-Dispatch website. Available at: http://www.stltoday.com/lifestyles/health-med-fit/health/high-tech-hand-washing-comes-to-st-louis-hospital/article_9379065d-85ff-5643-bae2-899254cb22fa.html. Accessed June 27, 2013.
- Lowe TJ, Partovian C, Kroch E, Martin J, Bankowitz R. Measuring cardiac waste: the Premier cardiac waste measures. Am J Med Qual. 2013 May 29 [Epub ahead of print].
- Elixhauser A, Steiner C. Readmissions to U.S. hospitals by diagnosis, 2010. Healthcare Cost and Utilization Project website. Available at: http://www.hcup-us.ahrq.gov/reports/statbriefs/sb153.pdf. Accessed July 15, 2013.
- Jackson Healthcare. Filling the void: 2013 physician outlook & practice trends. Jackson Healthcare website. Available at: http://www.jacksonhealthcare.com/media/193525/jc-2013physiciantrends-void_ebk0513.pdf. Accessed July 15, 2013.
According to a recent New York Times report, hand-hygiene compliance in hospitals can be as low as 30%, with serious implications regarding hospital-acquired infections.1 While many initiatives have employed secret observers, vibrating badges, or hand-washing coaches, a Research, Innovations, and Clinical Vignettes (RIV) poster at HM13 outlined how a multidisciplinary committee at University of Colorado Hospital in Aurora applied principles of psychology to the challenge of compliance.2
The initiative focused on behavioral changes: surreptitiously auditing staff behaviors, real-time feedback, and immediate public corrections for observed nonadherence on the test unit from an infection-control champion. The study randomly assigned daily auditing responsibilities across all members of the nursing staff, including aides. Taking a page from soccer referees, auditors handed out red tickets to hygiene violators—and individually wrapped Life Savers to reinforce adherence.
When unprofessional behavior is the response to a verbal correction, leadership has to be prepared to act, explains hospitalist and lead author Ethan Cumbler, MD, FACP.
“We need to stop thinking about hospital staff and physicians as rational actors when it comes to hand hygiene, but as social animals who will respond to positive and negative reinforcements and group culture,” he says.
Noncompliant hand hygiene is largely unconscious behavior that needs to be brought to conscious attention but is amenable to change, Dr. Cumbler says, adding that “unit leadership steps in for repeated nonadherence or an unprofessional response to correction. We have never needed to intervene more than once with the same person.”
Hand-hygiene adherence reached 97% on the pilot unit in the second quarter of 2012 and has remained at that level, Dr. Cumbler says. Additionally, iatrogenic infections dropped to zero from 4.8 per 1,000 urinary catheter days, with bloodstream infections falling at a similar rate.
Similar results with hand-hygiene compliance have been reported at St. Mary’s Health Center in St. Louis, which has been testing a system that reminds nurses to wash their hands at various checkpoints in the hospital, tracking their compliance with a badge that turns green when registering the presence of hand sanitizer, thereby informing patients that the nurse’s hands are clean.
The system, developed by Biovigil Hygiene Technologies of Ann Arbor, Mich., started on two pilot units last year, where compliance has grown to 97% and 99%, respectively. System set-up can cost about $2,000 per patient room, plus monthly subscriptions per employee, but more hospitals in the system could sign on next year, reports the St. Louis Post-Dispatch.3
Larry Beresford is a freelance writer in San Francisco.
References
- Hartocollis A. With money at risk, hospitals push staff to wash hands. The New York Times website. Available at: http://www.nytimes.com/2013/05/29/nyregion/hospitals-struggle-to-get-workers-to-wash-their-hands.html?pagewanted=all&_r=0. Accessed May 28, 2013.
- Cumbler E, Castillo L, Satorie L, et al. Culture change in infection control: applying psychological principles to improve hand hygiene. J Nurs Care Qual. 2013 May 10 [Epub ahead of print].
- Bernhard B. High tech hand washing comes to St. Louis hospital. St. Louis Post-Dispatch website. Available at: http://www.stltoday.com/lifestyles/health-med-fit/health/high-tech-hand-washing-comes-to-st-louis-hospital/article_9379065d-85ff-5643-bae2-899254cb22fa.html. Accessed June 27, 2013.
- Lowe TJ, Partovian C, Kroch E, Martin J, Bankowitz R. Measuring cardiac waste: the Premier cardiac waste measures. Am J Med Qual. 2013 May 29 [Epub ahead of print].
- Elixhauser A, Steiner C. Readmissions to U.S. hospitals by diagnosis, 2010. Healthcare Cost and Utilization Project website. Available at: http://www.hcup-us.ahrq.gov/reports/statbriefs/sb153.pdf. Accessed July 15, 2013.
- Jackson Healthcare. Filling the void: 2013 physician outlook & practice trends. Jackson Healthcare website. Available at: http://www.jacksonhealthcare.com/media/193525/jc-2013physiciantrends-void_ebk0513.pdf. Accessed July 15, 2013.
According to a recent New York Times report, hand-hygiene compliance in hospitals can be as low as 30%, with serious implications regarding hospital-acquired infections.1 While many initiatives have employed secret observers, vibrating badges, or hand-washing coaches, a Research, Innovations, and Clinical Vignettes (RIV) poster at HM13 outlined how a multidisciplinary committee at University of Colorado Hospital in Aurora applied principles of psychology to the challenge of compliance.2
The initiative focused on behavioral changes: surreptitiously auditing staff behaviors, real-time feedback, and immediate public corrections for observed nonadherence on the test unit from an infection-control champion. The study randomly assigned daily auditing responsibilities across all members of the nursing staff, including aides. Taking a page from soccer referees, auditors handed out red tickets to hygiene violators—and individually wrapped Life Savers to reinforce adherence.
When unprofessional behavior is the response to a verbal correction, leadership has to be prepared to act, explains hospitalist and lead author Ethan Cumbler, MD, FACP.
“We need to stop thinking about hospital staff and physicians as rational actors when it comes to hand hygiene, but as social animals who will respond to positive and negative reinforcements and group culture,” he says.
Noncompliant hand hygiene is largely unconscious behavior that needs to be brought to conscious attention but is amenable to change, Dr. Cumbler says, adding that “unit leadership steps in for repeated nonadherence or an unprofessional response to correction. We have never needed to intervene more than once with the same person.”
Hand-hygiene adherence reached 97% on the pilot unit in the second quarter of 2012 and has remained at that level, Dr. Cumbler says. Additionally, iatrogenic infections dropped to zero from 4.8 per 1,000 urinary catheter days, with bloodstream infections falling at a similar rate.
Similar results with hand-hygiene compliance have been reported at St. Mary’s Health Center in St. Louis, which has been testing a system that reminds nurses to wash their hands at various checkpoints in the hospital, tracking their compliance with a badge that turns green when registering the presence of hand sanitizer, thereby informing patients that the nurse’s hands are clean.
The system, developed by Biovigil Hygiene Technologies of Ann Arbor, Mich., started on two pilot units last year, where compliance has grown to 97% and 99%, respectively. System set-up can cost about $2,000 per patient room, plus monthly subscriptions per employee, but more hospitals in the system could sign on next year, reports the St. Louis Post-Dispatch.3
Larry Beresford is a freelance writer in San Francisco.
References
- Hartocollis A. With money at risk, hospitals push staff to wash hands. The New York Times website. Available at: http://www.nytimes.com/2013/05/29/nyregion/hospitals-struggle-to-get-workers-to-wash-their-hands.html?pagewanted=all&_r=0. Accessed May 28, 2013.
- Cumbler E, Castillo L, Satorie L, et al. Culture change in infection control: applying psychological principles to improve hand hygiene. J Nurs Care Qual. 2013 May 10 [Epub ahead of print].
- Bernhard B. High tech hand washing comes to St. Louis hospital. St. Louis Post-Dispatch website. Available at: http://www.stltoday.com/lifestyles/health-med-fit/health/high-tech-hand-washing-comes-to-st-louis-hospital/article_9379065d-85ff-5643-bae2-899254cb22fa.html. Accessed June 27, 2013.
- Lowe TJ, Partovian C, Kroch E, Martin J, Bankowitz R. Measuring cardiac waste: the Premier cardiac waste measures. Am J Med Qual. 2013 May 29 [Epub ahead of print].
- Elixhauser A, Steiner C. Readmissions to U.S. hospitals by diagnosis, 2010. Healthcare Cost and Utilization Project website. Available at: http://www.hcup-us.ahrq.gov/reports/statbriefs/sb153.pdf. Accessed July 15, 2013.
- Jackson Healthcare. Filling the void: 2013 physician outlook & practice trends. Jackson Healthcare website. Available at: http://www.jacksonhealthcare.com/media/193525/jc-2013physiciantrends-void_ebk0513.pdf. Accessed July 15, 2013.
Intravenous Immunoglobulin Most Common Retreatment Approach for Refractory Kawasaki Disease
Clinical question: How is refractory Kawasaki disease (rKD) treated in the United States?
Background: Kawasaki disease (KD) is an immunologically mediated disease of primarily small to medium-sized arteries. It is the most common cause of acquired heart disease in children in the United States.
The current standard of care for KD treatment is a single 2 g/kg dose of intravenous immunoglobulin (IVIG), infused over 10 to 12 hours, accompanied by aspirin (80 to 100 mg/kg/day by mouth in four divided doses). Fevers persistent more than 36 hours after initial treatment represent refractory Kawasaki disease (rKD). There are no current national guidelines or standards for rKD treatment, although a 2004 joint statement from the American Academy of Pediatrics and the American Heart Association suggested a second dose of IVIG for rKD.
Study design: Multicenter, retrospective, cross-sectional study.
Setting: Forty freestanding children’s hospitals.
Synopsis: Researchers examined data obtained from the Pediatric Health Information System (PHIS), a clinical and financial database of care provided at 43 nonprofit, freestanding children’s hospitals in the United States. Data from 40 of these hospitals were deemed complete enough for analysis and were collected from Jan. 1, 2005, to June 30, 2009. Subjects were included if they received at least one dose of IVIG and had a principal diagnosis of KD. To be considered rKD, the subject must have received additional treatment after the initial diagnosis of rKD.
The most commonly used treatment after initial IVIG treatment was retreatment with IVIG (65%), followed by intravenous methylprednisolone (27%), then infliximab (8%). Significant regional variation was observed, with hospitals in the Northeast using methylprednisolone most frequently for rKD (55%). Infliximab was used at a much higher frequency in the West (29%) compared with other regions.
Bottom line: Retreatment with IVIG is the most common treatment for rKD, but significant regional variation exists, possibly due to the influence of regional experts.
Citation: Ghelani SJ, Pastor W, Parikh K. Demographic and treatment variability of refractory Kawasaki Disease: a multicenter analysis from 2005 to 2009. Hospital Pediatrics. 2012;2:71-76.
Reviewed by Pediatric Editor Weijen Chang, MD, SFHM, FAAP, associate clinical professor of medicine and pediatrics at the University of California at San Diego School of Medicine, and a hospitalist at both UCSD Medical Center and Rady Children’s Hospital.
Clinical question: How is refractory Kawasaki disease (rKD) treated in the United States?
Background: Kawasaki disease (KD) is an immunologically mediated disease of primarily small to medium-sized arteries. It is the most common cause of acquired heart disease in children in the United States.
The current standard of care for KD treatment is a single 2 g/kg dose of intravenous immunoglobulin (IVIG), infused over 10 to 12 hours, accompanied by aspirin (80 to 100 mg/kg/day by mouth in four divided doses). Fevers persistent more than 36 hours after initial treatment represent refractory Kawasaki disease (rKD). There are no current national guidelines or standards for rKD treatment, although a 2004 joint statement from the American Academy of Pediatrics and the American Heart Association suggested a second dose of IVIG for rKD.
Study design: Multicenter, retrospective, cross-sectional study.
Setting: Forty freestanding children’s hospitals.
Synopsis: Researchers examined data obtained from the Pediatric Health Information System (PHIS), a clinical and financial database of care provided at 43 nonprofit, freestanding children’s hospitals in the United States. Data from 40 of these hospitals were deemed complete enough for analysis and were collected from Jan. 1, 2005, to June 30, 2009. Subjects were included if they received at least one dose of IVIG and had a principal diagnosis of KD. To be considered rKD, the subject must have received additional treatment after the initial diagnosis of rKD.
The most commonly used treatment after initial IVIG treatment was retreatment with IVIG (65%), followed by intravenous methylprednisolone (27%), then infliximab (8%). Significant regional variation was observed, with hospitals in the Northeast using methylprednisolone most frequently for rKD (55%). Infliximab was used at a much higher frequency in the West (29%) compared with other regions.
Bottom line: Retreatment with IVIG is the most common treatment for rKD, but significant regional variation exists, possibly due to the influence of regional experts.
Citation: Ghelani SJ, Pastor W, Parikh K. Demographic and treatment variability of refractory Kawasaki Disease: a multicenter analysis from 2005 to 2009. Hospital Pediatrics. 2012;2:71-76.
Reviewed by Pediatric Editor Weijen Chang, MD, SFHM, FAAP, associate clinical professor of medicine and pediatrics at the University of California at San Diego School of Medicine, and a hospitalist at both UCSD Medical Center and Rady Children’s Hospital.
Clinical question: How is refractory Kawasaki disease (rKD) treated in the United States?
Background: Kawasaki disease (KD) is an immunologically mediated disease of primarily small to medium-sized arteries. It is the most common cause of acquired heart disease in children in the United States.
The current standard of care for KD treatment is a single 2 g/kg dose of intravenous immunoglobulin (IVIG), infused over 10 to 12 hours, accompanied by aspirin (80 to 100 mg/kg/day by mouth in four divided doses). Fevers persistent more than 36 hours after initial treatment represent refractory Kawasaki disease (rKD). There are no current national guidelines or standards for rKD treatment, although a 2004 joint statement from the American Academy of Pediatrics and the American Heart Association suggested a second dose of IVIG for rKD.
Study design: Multicenter, retrospective, cross-sectional study.
Setting: Forty freestanding children’s hospitals.
Synopsis: Researchers examined data obtained from the Pediatric Health Information System (PHIS), a clinical and financial database of care provided at 43 nonprofit, freestanding children’s hospitals in the United States. Data from 40 of these hospitals were deemed complete enough for analysis and were collected from Jan. 1, 2005, to June 30, 2009. Subjects were included if they received at least one dose of IVIG and had a principal diagnosis of KD. To be considered rKD, the subject must have received additional treatment after the initial diagnosis of rKD.
The most commonly used treatment after initial IVIG treatment was retreatment with IVIG (65%), followed by intravenous methylprednisolone (27%), then infliximab (8%). Significant regional variation was observed, with hospitals in the Northeast using methylprednisolone most frequently for rKD (55%). Infliximab was used at a much higher frequency in the West (29%) compared with other regions.
Bottom line: Retreatment with IVIG is the most common treatment for rKD, but significant regional variation exists, possibly due to the influence of regional experts.
Citation: Ghelani SJ, Pastor W, Parikh K. Demographic and treatment variability of refractory Kawasaki Disease: a multicenter analysis from 2005 to 2009. Hospital Pediatrics. 2012;2:71-76.
Reviewed by Pediatric Editor Weijen Chang, MD, SFHM, FAAP, associate clinical professor of medicine and pediatrics at the University of California at San Diego School of Medicine, and a hospitalist at both UCSD Medical Center and Rady Children’s Hospital.
Academic Hospitalist Academy Provides Resources for Success
SHM asked Academic Hospitalist Academy course co-directors Jeffrey Glasheen, MD, SFHM, and Bradley Sharpe, MD, SFHM, why academic hospitalists should attend this year’s academy.
Question: What has you personally excited about this year’s Academic Hospitalist Academy?
Dr. Sharpe: I’ll be honest—it is one of my favorite weeks of the year. It is a tremendous opportunity to engage with academic hospitalists and help them develop the core skills they need to be successful.
Dr. Glasheen: For me, it’s about the energy, the talent, and the excitement that the attendees bring to the course. It ends up being a tremendously energizing week for me personally. To see the talent in the room begin to find outlets for success is truly invigorating.
Q: If you were talking one on one with an academic hospitalist, what would you say to encourage them to attend?
Dr. Sharpe: Based on previous attendees, these four days could truly change your life. We are confident you will leave with newfound energy and enthusiasm and key building blocks to help you be successful when you go back home. Don’t miss it.
Dr. Glasheen: There is a magical transformation that happens every year. Very talented individuals enter the program. Nearly uniformly, they are struggling with the same issues around mentorship, sense of purpose, direction, and resources for success. They all want to be successful but sense there is something that is missing, and within the course of four days, they find it.
Q: What have you heard from previous AHA attendees?
Dr. Sharpe: Here are a couple of emails I received: “I can’t say enough about the AHA. It was possibly the most important 3 days of my young career. Thank you both for the knowledge and guidance.” “I have fond memories of the whole AHA conference. The great Jeff Wiese!!! But most of all, the small group sessions were extremely helpful.”
Dr. Glasheen: To a person, they all say the meeting is “transformational.” They gain skills in teaching, confidence in evaluating learners, methods for scholarly success, and a roadmap for navigating the tricky world on academic medicine. But beyond that, they gain a peer network. They leave tied in with 80 other national colleagues that are struggling with the same issues. This network becomes their home away from home—people they can turn to with a question, catch up with at a national meeting, and look to as exemplars in the field.
SHM asked Academic Hospitalist Academy course co-directors Jeffrey Glasheen, MD, SFHM, and Bradley Sharpe, MD, SFHM, why academic hospitalists should attend this year’s academy.
Question: What has you personally excited about this year’s Academic Hospitalist Academy?
Dr. Sharpe: I’ll be honest—it is one of my favorite weeks of the year. It is a tremendous opportunity to engage with academic hospitalists and help them develop the core skills they need to be successful.
Dr. Glasheen: For me, it’s about the energy, the talent, and the excitement that the attendees bring to the course. It ends up being a tremendously energizing week for me personally. To see the talent in the room begin to find outlets for success is truly invigorating.
Q: If you were talking one on one with an academic hospitalist, what would you say to encourage them to attend?
Dr. Sharpe: Based on previous attendees, these four days could truly change your life. We are confident you will leave with newfound energy and enthusiasm and key building blocks to help you be successful when you go back home. Don’t miss it.
Dr. Glasheen: There is a magical transformation that happens every year. Very talented individuals enter the program. Nearly uniformly, they are struggling with the same issues around mentorship, sense of purpose, direction, and resources for success. They all want to be successful but sense there is something that is missing, and within the course of four days, they find it.
Q: What have you heard from previous AHA attendees?
Dr. Sharpe: Here are a couple of emails I received: “I can’t say enough about the AHA. It was possibly the most important 3 days of my young career. Thank you both for the knowledge and guidance.” “I have fond memories of the whole AHA conference. The great Jeff Wiese!!! But most of all, the small group sessions were extremely helpful.”
Dr. Glasheen: To a person, they all say the meeting is “transformational.” They gain skills in teaching, confidence in evaluating learners, methods for scholarly success, and a roadmap for navigating the tricky world on academic medicine. But beyond that, they gain a peer network. They leave tied in with 80 other national colleagues that are struggling with the same issues. This network becomes their home away from home—people they can turn to with a question, catch up with at a national meeting, and look to as exemplars in the field.
SHM asked Academic Hospitalist Academy course co-directors Jeffrey Glasheen, MD, SFHM, and Bradley Sharpe, MD, SFHM, why academic hospitalists should attend this year’s academy.
Question: What has you personally excited about this year’s Academic Hospitalist Academy?
Dr. Sharpe: I’ll be honest—it is one of my favorite weeks of the year. It is a tremendous opportunity to engage with academic hospitalists and help them develop the core skills they need to be successful.
Dr. Glasheen: For me, it’s about the energy, the talent, and the excitement that the attendees bring to the course. It ends up being a tremendously energizing week for me personally. To see the talent in the room begin to find outlets for success is truly invigorating.
Q: If you were talking one on one with an academic hospitalist, what would you say to encourage them to attend?
Dr. Sharpe: Based on previous attendees, these four days could truly change your life. We are confident you will leave with newfound energy and enthusiasm and key building blocks to help you be successful when you go back home. Don’t miss it.
Dr. Glasheen: There is a magical transformation that happens every year. Very talented individuals enter the program. Nearly uniformly, they are struggling with the same issues around mentorship, sense of purpose, direction, and resources for success. They all want to be successful but sense there is something that is missing, and within the course of four days, they find it.
Q: What have you heard from previous AHA attendees?
Dr. Sharpe: Here are a couple of emails I received: “I can’t say enough about the AHA. It was possibly the most important 3 days of my young career. Thank you both for the knowledge and guidance.” “I have fond memories of the whole AHA conference. The great Jeff Wiese!!! But most of all, the small group sessions were extremely helpful.”
Dr. Glasheen: To a person, they all say the meeting is “transformational.” They gain skills in teaching, confidence in evaluating learners, methods for scholarly success, and a roadmap for navigating the tricky world on academic medicine. But beyond that, they gain a peer network. They leave tied in with 80 other national colleagues that are struggling with the same issues. This network becomes their home away from home—people they can turn to with a question, catch up with at a national meeting, and look to as exemplars in the field.
Pediatric Hospital Medicine Marks 10th Anniversary
With a record number of attendees, Pediatric Hospital Medicine 2013 (PHM) swept into New Orleans last month, carrying with it unbridled enthusiasm about the past, present, and future.
Virginia Moyer, MD, MPH, vice president for maintenance of certification and quality for the American Board of Pediatrics (ABP) and professor of pediatrics and chief of academic general pediatrics at Texas Children’s Hospital, delivered a keynote address to 700 attendees that focused on the challenges and opportunities of providing evidence-based, high-quality care in the hospital, as well as ABP’s role in meeting these challenges.
“If evidence-based medicine is an individual sport,” Dr. Moyer said, “then quality improvement is a team sport.”
Barriers to quality improvement (QI)— such as lack of will, lack of data, and lack of training—can be surmounted in a team environment, she said. ABP is continuing in its efforts to support QI education through its Maintenance of Certification (MOC) Part 4 modules, as well as other educational activities.
Other highlights of the 10th annual Pediatric Hospital Medicine meeting:
- The addition of a new “Community Hospitalists” track was given high marks by those in attendance. It covered such topics as perioperative management of medically complex pediatric patients, community-acquired pneumonia, and osteomyelitis.
- A 10-year retrospective of pediatric hospital medicine was given by a panel of notable pediatric hospitalists, including Erin Stucky Fisher, MD, FAAP, MHM, chief of hospital medicine at Rady Children’s Hospital in San Diego; Mary Ottolini, MD, MPH, chief of hospital medicine at Children’s National Medical Center in Washington; Jack Percelay, MD, MPH, FAAP, associate clinical professor at Pace University; and Daniel Rauch, MD, FAAP, pediatric hospitalist program director at the NYU School of Medicine in New York City. A host of new programs has been established by the PHM community, including the Quality Improvement Innovation Networks (QuIIN); the Value in Pediatrics (VIP) network; the International Network for Simulation-Based Pediatric Innovation, Research, and Education (INSPIRE); patient- and family-centered rounds; and the I-PASS Handoff Program. The panel also discussed future challenges, including reduction of unnecessary treatments, interfacing, and perhaps incorporating “hyphen hospitalists,” and learning from advances made by the adult HM community.
- The ever-popular “Top Articles in Pediatric Hospital Medicine” session was presented by H. Barrett Fromme, MD, associate professor of pediatrics at the University of Chicago, and Ben Bauer, MD, director of pediatric hospital medicine at Riley Hospital for Children at Indiana University Health in Indianapolis, which was met with raucous approval by the audience. The presentation not only educated those in attendance about the most cutting-edge pediatric literature, but it also included dance moves most likely to attract the opposite sex and clothing appropriate for the Australian pediatric hospitalist.
- The three presidents of the sponsoring societies—Thomas McInerney, MD, FAAP, of the American Academy of Pediatrics, David Keller, MD, of the Academic Pediatric Association, and Eric Howell, MD, SFHM, of SHM—presented each society’s contributions to the growth of PHM, as well as future areas for cooperative sponsorship. These include the development of the AAP Section of Hospital Medicine Library website (sohmlibrary.org), the APA Quality Scholars program, and SHM’s efforts to increase interest in hospital medicine in medical students and trainees. “Ask not what hospital medicine can do for you,” Dr. Howell implored, “ask what you can do for hospital medicine!”
- Members of the Joint Council of Pediatric Hospital Medicine (JCPHM) presented the recent recommendations of the council arising from an April 2013 meeting with the ABP in Chapel Hill, N.C. Despite acknowledgements that no decision will be met with uniform satisfaction by all the stakeholders, the JCPHM concluded that the path that would best advance the field of PHM, provide for high-quality care of hospitalized children, and ensure the public trust would be a two-year fellowship sponsored by ABP. This would ultimately lead to approved certification eligibility for fellowship graduates by the American Board of Medical Specialties (ABMS); it would also make provisions for “grandfathering” in current pediatric hospitalists. Concerns from med-peds, community hospitalists, and recent residency graduate communities were addressed by the panel.
- A recurrent theme of reducing unnecessary treatments, interventions, and, perhaps, hospitalizations was summarized eloquently by Alan Schroeder, MD, director of the pediatric ICU and chief of pediatric inpatient care at Santa Clara (Calif.) Valley Health. Barriers to reducing unnecessary care can be substantial, including pressure from families, pressure from colleagues, profit motive, and the “n’s of 1,” according to Dr. Schroeder. Ultimately, however, avoiding testing and treatments that have no benefit to children will improve care. “Ask, ‘How will this test benefit my patient?’ not ‘How will this test change management?’” Dr. Schroeder advised.
Dr. Chang is The Hospitalist’s pediatric editor and a med-peds-trained hospitalist working at the University of California San Diego and Rady Children’s Hospital.
With a record number of attendees, Pediatric Hospital Medicine 2013 (PHM) swept into New Orleans last month, carrying with it unbridled enthusiasm about the past, present, and future.
Virginia Moyer, MD, MPH, vice president for maintenance of certification and quality for the American Board of Pediatrics (ABP) and professor of pediatrics and chief of academic general pediatrics at Texas Children’s Hospital, delivered a keynote address to 700 attendees that focused on the challenges and opportunities of providing evidence-based, high-quality care in the hospital, as well as ABP’s role in meeting these challenges.
“If evidence-based medicine is an individual sport,” Dr. Moyer said, “then quality improvement is a team sport.”
Barriers to quality improvement (QI)— such as lack of will, lack of data, and lack of training—can be surmounted in a team environment, she said. ABP is continuing in its efforts to support QI education through its Maintenance of Certification (MOC) Part 4 modules, as well as other educational activities.
Other highlights of the 10th annual Pediatric Hospital Medicine meeting:
- The addition of a new “Community Hospitalists” track was given high marks by those in attendance. It covered such topics as perioperative management of medically complex pediatric patients, community-acquired pneumonia, and osteomyelitis.
- A 10-year retrospective of pediatric hospital medicine was given by a panel of notable pediatric hospitalists, including Erin Stucky Fisher, MD, FAAP, MHM, chief of hospital medicine at Rady Children’s Hospital in San Diego; Mary Ottolini, MD, MPH, chief of hospital medicine at Children’s National Medical Center in Washington; Jack Percelay, MD, MPH, FAAP, associate clinical professor at Pace University; and Daniel Rauch, MD, FAAP, pediatric hospitalist program director at the NYU School of Medicine in New York City. A host of new programs has been established by the PHM community, including the Quality Improvement Innovation Networks (QuIIN); the Value in Pediatrics (VIP) network; the International Network for Simulation-Based Pediatric Innovation, Research, and Education (INSPIRE); patient- and family-centered rounds; and the I-PASS Handoff Program. The panel also discussed future challenges, including reduction of unnecessary treatments, interfacing, and perhaps incorporating “hyphen hospitalists,” and learning from advances made by the adult HM community.
- The ever-popular “Top Articles in Pediatric Hospital Medicine” session was presented by H. Barrett Fromme, MD, associate professor of pediatrics at the University of Chicago, and Ben Bauer, MD, director of pediatric hospital medicine at Riley Hospital for Children at Indiana University Health in Indianapolis, which was met with raucous approval by the audience. The presentation not only educated those in attendance about the most cutting-edge pediatric literature, but it also included dance moves most likely to attract the opposite sex and clothing appropriate for the Australian pediatric hospitalist.
- The three presidents of the sponsoring societies—Thomas McInerney, MD, FAAP, of the American Academy of Pediatrics, David Keller, MD, of the Academic Pediatric Association, and Eric Howell, MD, SFHM, of SHM—presented each society’s contributions to the growth of PHM, as well as future areas for cooperative sponsorship. These include the development of the AAP Section of Hospital Medicine Library website (sohmlibrary.org), the APA Quality Scholars program, and SHM’s efforts to increase interest in hospital medicine in medical students and trainees. “Ask not what hospital medicine can do for you,” Dr. Howell implored, “ask what you can do for hospital medicine!”
- Members of the Joint Council of Pediatric Hospital Medicine (JCPHM) presented the recent recommendations of the council arising from an April 2013 meeting with the ABP in Chapel Hill, N.C. Despite acknowledgements that no decision will be met with uniform satisfaction by all the stakeholders, the JCPHM concluded that the path that would best advance the field of PHM, provide for high-quality care of hospitalized children, and ensure the public trust would be a two-year fellowship sponsored by ABP. This would ultimately lead to approved certification eligibility for fellowship graduates by the American Board of Medical Specialties (ABMS); it would also make provisions for “grandfathering” in current pediatric hospitalists. Concerns from med-peds, community hospitalists, and recent residency graduate communities were addressed by the panel.
- A recurrent theme of reducing unnecessary treatments, interventions, and, perhaps, hospitalizations was summarized eloquently by Alan Schroeder, MD, director of the pediatric ICU and chief of pediatric inpatient care at Santa Clara (Calif.) Valley Health. Barriers to reducing unnecessary care can be substantial, including pressure from families, pressure from colleagues, profit motive, and the “n’s of 1,” according to Dr. Schroeder. Ultimately, however, avoiding testing and treatments that have no benefit to children will improve care. “Ask, ‘How will this test benefit my patient?’ not ‘How will this test change management?’” Dr. Schroeder advised.
Dr. Chang is The Hospitalist’s pediatric editor and a med-peds-trained hospitalist working at the University of California San Diego and Rady Children’s Hospital.
With a record number of attendees, Pediatric Hospital Medicine 2013 (PHM) swept into New Orleans last month, carrying with it unbridled enthusiasm about the past, present, and future.
Virginia Moyer, MD, MPH, vice president for maintenance of certification and quality for the American Board of Pediatrics (ABP) and professor of pediatrics and chief of academic general pediatrics at Texas Children’s Hospital, delivered a keynote address to 700 attendees that focused on the challenges and opportunities of providing evidence-based, high-quality care in the hospital, as well as ABP’s role in meeting these challenges.
“If evidence-based medicine is an individual sport,” Dr. Moyer said, “then quality improvement is a team sport.”
Barriers to quality improvement (QI)— such as lack of will, lack of data, and lack of training—can be surmounted in a team environment, she said. ABP is continuing in its efforts to support QI education through its Maintenance of Certification (MOC) Part 4 modules, as well as other educational activities.
Other highlights of the 10th annual Pediatric Hospital Medicine meeting:
- The addition of a new “Community Hospitalists” track was given high marks by those in attendance. It covered such topics as perioperative management of medically complex pediatric patients, community-acquired pneumonia, and osteomyelitis.
- A 10-year retrospective of pediatric hospital medicine was given by a panel of notable pediatric hospitalists, including Erin Stucky Fisher, MD, FAAP, MHM, chief of hospital medicine at Rady Children’s Hospital in San Diego; Mary Ottolini, MD, MPH, chief of hospital medicine at Children’s National Medical Center in Washington; Jack Percelay, MD, MPH, FAAP, associate clinical professor at Pace University; and Daniel Rauch, MD, FAAP, pediatric hospitalist program director at the NYU School of Medicine in New York City. A host of new programs has been established by the PHM community, including the Quality Improvement Innovation Networks (QuIIN); the Value in Pediatrics (VIP) network; the International Network for Simulation-Based Pediatric Innovation, Research, and Education (INSPIRE); patient- and family-centered rounds; and the I-PASS Handoff Program. The panel also discussed future challenges, including reduction of unnecessary treatments, interfacing, and perhaps incorporating “hyphen hospitalists,” and learning from advances made by the adult HM community.
- The ever-popular “Top Articles in Pediatric Hospital Medicine” session was presented by H. Barrett Fromme, MD, associate professor of pediatrics at the University of Chicago, and Ben Bauer, MD, director of pediatric hospital medicine at Riley Hospital for Children at Indiana University Health in Indianapolis, which was met with raucous approval by the audience. The presentation not only educated those in attendance about the most cutting-edge pediatric literature, but it also included dance moves most likely to attract the opposite sex and clothing appropriate for the Australian pediatric hospitalist.
- The three presidents of the sponsoring societies—Thomas McInerney, MD, FAAP, of the American Academy of Pediatrics, David Keller, MD, of the Academic Pediatric Association, and Eric Howell, MD, SFHM, of SHM—presented each society’s contributions to the growth of PHM, as well as future areas for cooperative sponsorship. These include the development of the AAP Section of Hospital Medicine Library website (sohmlibrary.org), the APA Quality Scholars program, and SHM’s efforts to increase interest in hospital medicine in medical students and trainees. “Ask not what hospital medicine can do for you,” Dr. Howell implored, “ask what you can do for hospital medicine!”
- Members of the Joint Council of Pediatric Hospital Medicine (JCPHM) presented the recent recommendations of the council arising from an April 2013 meeting with the ABP in Chapel Hill, N.C. Despite acknowledgements that no decision will be met with uniform satisfaction by all the stakeholders, the JCPHM concluded that the path that would best advance the field of PHM, provide for high-quality care of hospitalized children, and ensure the public trust would be a two-year fellowship sponsored by ABP. This would ultimately lead to approved certification eligibility for fellowship graduates by the American Board of Medical Specialties (ABMS); it would also make provisions for “grandfathering” in current pediatric hospitalists. Concerns from med-peds, community hospitalists, and recent residency graduate communities were addressed by the panel.
- A recurrent theme of reducing unnecessary treatments, interventions, and, perhaps, hospitalizations was summarized eloquently by Alan Schroeder, MD, director of the pediatric ICU and chief of pediatric inpatient care at Santa Clara (Calif.) Valley Health. Barriers to reducing unnecessary care can be substantial, including pressure from families, pressure from colleagues, profit motive, and the “n’s of 1,” according to Dr. Schroeder. Ultimately, however, avoiding testing and treatments that have no benefit to children will improve care. “Ask, ‘How will this test benefit my patient?’ not ‘How will this test change management?’” Dr. Schroeder advised.
Dr. Chang is The Hospitalist’s pediatric editor and a med-peds-trained hospitalist working at the University of California San Diego and Rady Children’s Hospital.
Career Boost a Benefit of Winning SHM’s Research, Innovations, and Clinical Vignettes Poster Competition
Back to the Furture Past RIV winners talk about what the recognition meant for their careers By Larry Beresford
After winning SHM’s annual Research, Innovations, and Clinical Vignettes (RIV) scientific abstract and poster competition for an abstract illustrating a program that promoted flu vaccinations for families of neonatal patients, Shetal Shah, MD, FAAP, became a leading advocate for two laws mandating that New York hospitals offer vaccinations to families.
A poster that described a VTE prevention program led Gregory Maynard, MD, MSc, SFHM, to join SHM’s VTE Prevention Collaborative and, eventually, to become senior vice president of the society’s Center for Hospital Innovation and Improvement.
A prize-winning innovations poster for improving team communication by Vineet Chopra, MD, MS, FACP, FHM, and colleagues later took off as a new technology company.
Leonard Feldman, MD, FAAP, SFHM, won for a poster that explained online CME curriculum for hospitalists as consultants; the curriculum now resides on SHM’s website.
The evidence is clear: RIV abstracts are a vital part of hospital medicine.
Nearly 800 abstracts were submitted for HM13.
Awards are given in three categories:
- Research posters report clinical or basic science data, systematically review a clinical problem, or address efficiency, cost, or method of health-care delivery or medical decision-making;
- Innovations posters describe an existing innovative program in hospital medicine, often with preliminary data; and
- Clinical vignettes, either adult or pediatric, report on one or more cases illustrating a new disease entity, a prominent or unusual feature of an established disease, or an area of clinical controversy.
The Hospitalist asked 11 past RIV winners what the poster contest meant to their careers. Some added more data and analysis and went on to be published in such medical journals as the Journal of Hospital Medicine. Some used the recognition to launch or boost research-oriented careers; others saw their careers go in different directions.
“Winning a national poster competition gives you the confidence to continue to pursue your interest and take it to a higher level, like successfully competing for funding and publishing your line of inquiry,” says hospitalist and researcher Vineet Arora, MD, MPP, FHM, of the University of Chicago, who won the 2006 RIV research competition. “Sometimes, presenting posters can be lonely, but at SHM, you get a lot of traffic. You get a chance to practice your spiel, communicating science and research in a very concise way, which is an important skill to have.”
David Metzger, MD, PhD, also from the University of Chicago, who won the RIV research award in 2005, says recognition is a big deal, but “one of the biggest values of the RIV competition is just getting information out to colleagues, with the opportunity to talk with your peers. That’s the real prize.
“I’ve been involved in presenting posters at SHM every year that the society has been in existence,” he says. “I’ve met so many people and talked about what they’re doing. That’s what a medical society should do—bring people together like this.”
Title: Administrator, academic consult service; teaching staff physician
Institution: Saint Joseph Mercy Hospital, Ypsilanti, Mich.
Year: 2008
RIV: “A Case of Salty Voluminous Urine” (clinical vignette)
Dr. Tassava was honored two years in a row for topics drawn from her experience as a hospitalist working in the surgical ICU. Her HM08 entry won top poster, and her HM09 poster, “Permissive Hypernatremia: Co-Management of Intracranial Pressure in a Patient with Diabetes Insipidus,” was selected for an oral presentation.
The HM09 vignette described how the hypernatremia that occurs with diabetes insipidus could be used in a novel way to control intracranial pressure in a 17-year-old patient who had a traumatic brain injury from an auto accident.
“She had a beautiful outcome,” Dr. Tassava says. “She started college and she came back to our unit for a visit after her recovery.”
Dr. Tassava enjoyed the opportunity to explain to her peers how diabetes insipidus presented and how she managed the case. “I was a little surprised at how much discussion was generated by my case,” she says, “even though I knew this was an important and novel approach.”
When her hospital added intensivists, her work and research in the ICU ended and her career moved more toward hospitalist administration. She now runs the academic consult service at St. Joseph, serves as lead physician for the orthopedic surgery floor, instructs and mentors medical residents, and chairs the hospital’s Coagulation Collaborative Practice Team (Coagulation CPT). She credits the RIV honors with helping her to gain recognition as an academic hospitalist who was nominated for leadership roles. She has moved out of research for now but plans to pursue anticoagulation research in the future.
“I really appreciated the recognition for my curiosity and scientific approach, which was acknowledged by my surgical colleagues,” Dr. Tassava says. “I absolutely love the CPT. I am the hospital’s principal educator with regard to anticoagulation. Over the past year, I have given medicine and cardiology grand rounds, and have presented on the newest anticoagulants.”
Dr. Tassava still collaborates with her residents on abstracts, several of which have been submitted to SHM, the American College of Physicians, and other medical societies.
“I still love research,” she says. “I have a million ideas.”
Title: Chief of the division of hospital medicine; senior vice president, SHM’s Center for Innovation and Improvement
Institution: University of California at San Diego (UCSD)
Year: 2008
RIV: “Prevention of Hospital-Acquired Venous Thromboembolism: Prospective Validation of a VTE Risk Assessment Model and Protocol” (research)
Citations: Maynard G, Stein J. Designing and implementing effective VTE prevention protocols: lessons from collaboratives. J Thromb Thrombolysis. 2010;29(2):159-166. Maynard G, Morris T, Jenkins I, et al. Optimizing prevention of hospital acquired venous thromboembolism: prospective validation of a VTE risk assessment model. J Hosp Med. 2010;5(1):10-18.
Dr. Maynard’s abstract described a project funded by the federal Agency for Healthcare Research and Quality to design and implement an organized, comprehensive protocol for VTE prevention within the hospital setting. The project also included a toolkit to help other hospitals do the same thing. The same group received SHM’s Award of Excellence for Teamwork.
This work, combined with similar efforts by Jason Stein, MD, and colleagues at Emory University in Atlanta and others, provided the foundation for SHM’s VTE resource room and the mentored implementation program of SHM’s VTE Prevention Collaborative, which had been launched in 2007 as one of the society’s first large-scale quality-improvement (QI) initiatives.
“SHM wanted to do something about VTE prevention, and when we got our AHRQ grant, I was interested in doing the same,” Dr. Maynard says. “We published our implementation guides on the AHRQ and SHM websites, along with a lot of valuable supporting materials.”
Dr. Maynard later took on leadership roles with SHM’s quality initiatives on glycemic control and care transitions, which made him the logical choice to become senior vice president of SHM’s Center for Hospital Innovation and Improvement.
He says the RIV honor lifted his profile not only within SHM, but also throughout the field, and it was instrumental in obtaining continued funding to advance the VTE initiative. “We did this tremendous work—with great results,” he says. “But I don’t think our local administrators appreciated it quite as much until we started to get external, national recognition.”
Dr. Maynard earned his master’s degree in biostatistics and clinical research design from the University of Michigan—skills he later brought to the academic setting at UCSD.
“It was a nice way for a hospitalist, who’s really a medical generalist, to become an expert in something,” he says. “I could never be more of an expert in cardiology than a cardiologist, or more of an expert in DVT than a hematologist or critical-care specialist. But I could help both of them do what they couldn’t do as effectively, which was to implement protocols reliably using a QI framework.”
Title: Assistant professor of general internal medicine, hospital medicine, and public health
Institution: Vanderbilt University, Nashville, Tenn.
Year: 2009
RIV: “Predictors of Early Post-Discharge Mortality in Critically Ill Patients: Lessons for Quality Performance and Quality Assessment” (research)
Citation: Vasilevskis EE, Kuzniewicz MW, Cason BA, et al. Predictors of early post-discharge mortality in critically ill patients: a retrospective cohort study from the California Intensive Care Outcomes project. J Crit Care. 2011;26(1):65-75.
Dr. Vasilevskis has submitted abstracts to the RIV competition almost every year since 2007, when he was completing a fellowship at the University of California at San Francisco’s Institute for Health Policy Studies. He was honored in 2009 for a project based on the California Intensive Care Outcomes Project, which drew data from 35 hospitals to demonstrate that shortening ICU length of stay was predictive of early post-discharge mortality in the most severely ill patients.
He has continued to research quality and safety in the ICU, and he has published dozens of journal articles.
“My initial focus was on traditional mortality and length-of-stay outcomes,” he says. “I am now pursuing additional outcomes, most notably delirium in the ICU patient. I work with an amazing group of researchers that are trying to better measure, define, and treat delirium in the ICU—an outcome associated with a number of poor patient outcomes.”
Dr. Vasilevskis also is researching the causes of hospital readmissions and the development of novel ways to improve care transitions for elderly patients. He is pursuing a master’s of public health at Vanderbilt, and is co-principal investigator of an investigation of the Hospital Medicine Reengineering Network to improve transitions of care, supported by the Association of American Medical Colleges.
In addition to his 2009 win, he captured the HM10 and HM12 research categories. His HM12 poster, “Veterans Administration Acute Care 30-Day Mortality Model: Development, Validation and Performance Variation,” was singled out by the judging committee for its impressive sample size (1,114,327 patients in a retrospective cohort study of 131 VA hospitals), as well as for how it combined administrative and clinical risk models.
Dr. Vasilevskis says the opportunity to present his research at SHM and the recognition he received encouraged him to continue as a hospitalist engaged in medical research. He has been a member of SHM’s Research Committee since 2009, an RIV judge at HM11, and chaired the HM13 RIV competition subcommittee.
Title: Assistant professor of medicine
Institution: University of Michigan Health System, Ann Arbor
Year: 2009
RIV: “MComm: Redefining Medical Communications in the 21st Century” (innovations)
Early in his career, Dr. Chopra was curious about how to improve the way patient care is delivered in the hospital setting. He was particularly interested in the inordinate amount of time hospitalists spend every day on communication.
“I saw one-way paging systems as a problem for communication between members of the medical team,” he says. “Doctors get paged and break off from what they’re doing to return the page—to someone who often isn’t there to take the call back. Sometimes the system gives us the wrong number or a cryptic message that makes no sense.”
A technological solution to this problem, which he and hospitalist Prasanth Gogineni, MD, conceived, designed, and created, then tested at the University of Michigan, is called MComm. Dr. Chopra describes it as a novel, uniform way of messaging for the entire medical team using wireless servers, PUSH technology, and iPhones. MComm was built around existing hospital workflow and patient-specific task lists, assigning priority to each message and documenting that it was delivered. The junior faculty members submitted an abstract about their innovative application, not really expecting it to get accepted. But when it won the poster competition and was selected for a plenary presentation, things got busy in a hurry. Specifically, the university hospital’s Office of Technology Transfer took a keen interest.
“We met with a number of people who had business experience in the health-care-technology space and found a CEO for the company we formed to develop MComm,” Dr. Chopra says. “I found myself getting pulled into it very quickly, with a lot of conversations about commercialization, revenue-sharing models, intellectual property, and the like.”
But running a company was not something Dr. Chopra wanted to do. Two years ago, that company, Synaptin, went one way and he went another—he stayed at Michigan as a medical researcher. He remains deeply interested in how care is delivered to hospitalized patients, but with a focus on such patient-safety questions as how to prevent negative outcomes from indwelling venous catheters.
“Winning the poster competition opened doors for me—there’s no doubt in my mind,” he says. “We demonstrated the ability to deliver a project of significance, from concept to prototype, without formal training in this area. If we didn’t have that recognition, I’m not sure I would have been ready to step into a research career as quickly. It helped me realize that medical research was what I wanted to do.”
Title: Associate program director, internal-medicine residency; assistant dean of scholarship and discovery
Institution: Pritzker School of Medicine, University of Chicago
Year: 2006
RIV: “Measuring Quality of Hospital Care for Vulnerable Elders: Use of ACOVE Quality Indicators” (research)
Citation: Arora VM, Fish M, Basu A, et al. Relationship between quality of care of hospitalized vulnerable elders and postdischarge mortality. J Am Geriatrics. 2010;58:1642-1648.
Title: Associate professor, department of medicine; associate faculty member, Harris School and the Department of Economics
Institution: University of Chicago
Year: 2005
RIV: “Effects of Hospitalists on Outcomes and Costs in a Multicenter Trial of Academic Hospitalists” (research)
Dr. Meltzer was the lead author, with 11 other prominent hospitalists, of an abstract based on a multisite study of the cost and outcome implications of the hospitalist model—still a relatively new concept in 2001, when the research began. Although the study did not uncover large cost savings realized from the hospitalist model of care, as some advocates had hoped, important findings and implications for the emerging field were teased out of the data.
At the time, only a few randomly controlled, multisite studies of costs and outcomes for the hospitalist model had been performed. The study, Dr. Meltzer says, required a complicated analysis to discover that hospitalists, in fact, saved their facilities money, with their most important impact realized post-hospitalization, such as on nursing-home costs. It was important to control for spillover effect and the fact that hospitalists do a better job of teaching house staff, while a physician’s years of experience was another important variable, he says.
Dr. Meltzer was a medical researcher interested in medical specialization when the term “hospitalist” was first coined in 1996. “I thought, here was a chance to study a medical specialty in its formative stages,” he says.
He still works as a hospitalist, although with limited clinical time. In addition to his administrative work as division chief, he directs the Center for Health and the Social Sciences at the University of Chicago. His research interests include cost-effectiveness, technology assessment, and information research.
In 2010, his poster “Effects of Hospitalists on 1-Year Post-Discharge Resource Utilization by Medicare Beneficiaries” took the top prize in the HM10 research competition. In 2011, he was appointed to the methodology committee of the federal Patient-Centered Outcomes Research Institute (PCORI), which was created by the Affordable Care Act to advise the government on clinical-effectiveness research. He also sits on the Advisory Council to the National Institute of General Medical Sciences at the Institute of Medicine, and on the Congressional Budget Office’s panel of health advisors.
In a career full of recognition, Dr. Meltzer says it’s hard to pinpoint the impact of winning the poster contest. But he has continued to submit abstracts to SHM every year and appreciates the opportunities for interaction with peers at the poster exhibits.
Title: Director of perioperative and consultative medicine
Institution: University of Michigan, Ann Arbor
Year: 2006
RIV: “Disseminated Histoplasmosis Presenting As Painful Oral Ulcers” (clinical vignettes)
Dr. Grant’s winning vignette presented a patient with a complex medical history, including heart disease and four months of painful oral ulcers, for which prior evaluations had been inconclusive, despite conducting biopsies. Following administration of high-dose corticosteroids, the patient’s condition worsened on multiple fronts. The vignette showed how the medical team was able to diagnose an unusual presentation of a fungal infection called histoplasmosis, which is prevalent in parts of the Midwest surrounding the Ohio and Mississippi river valleys.
“We see a lot of cases in the hospital where there are different angles you could take to turn it into a clinical vignette or a nice poster with good teaching points,” Dr. Grant says. “In this case, just digging deeper into the actual diagnosis was important because the empiric use of steroids can be fatal for some patients. Steroids are given for a lot of good reasons, but in this patient they caused immune suppression, allowing a smoldering infection to become very active.”
Dr. Grant did not submit the vignette for publication. “That was probably a mistake on my part,” he says, acknowledging the common complaint of too little time and too many competing priorities. But his interest in research has continued.
“I became involved at a national level with issues of perioperative medicine and last August published a textbook on the subject,” he reports.1 “VTE is another area of interest I have developed since my hospital medicine fellowship.”
He serves as the VTE resource expert on the Michigan Hospital Medicine Safety Consortium, a quality collaborative of more than 40 hospitals with Blue Cross/Blue Shield of Michigan. “It’s exciting to be able to look at the risk factors, what kinds of patients get VTEs, and whether they were appropriately prophylaxed in the hospital,” he says.
VTE is a national quality priority, and Dr. Grant expects abstracts to emerge from the consortium’s work.
He says he appreciates the opportunities that arise from participating in poster sessions at SHM, where medical students, residents, and working hospitalists talk to the presenters of interesting cases.
“It gives you a real back-and-forth, which is good for the person asking the question and for the presenter,” he says, noting hospitalists from other parts of the country were not as familiar with histoplasmosis.
He says winning the HM06 poster contest helped him “get his feet wet” and feel more prepared for a career in academic hospital medicine. “I’m sure the award solidified my employers’ satisfaction in hiring me—and in giving me more desirable academic roles and responsibilities,” he adds.
Title: Assistant professor of medicine pediatrics; director of the general internal-medicine comprehensive consultation service
Institution: Johns Hopkins Hospital, Baltimore
Year: 2009
RIV: “An Internet-Based Consult Curriculum for Hospitalists” (innovations)
Dr. Feldman’s poster described an online CME curriculum for hospitalists acting as medical consultants. The concept grew out of a perceived deficiency in his own medical education when, in 2004, he was asked to lead the consultation service at Johns Hopkins—just six months after finishing his residency.
“I had no idea what I was doing as a general-internal-medicine consultant,” he says. “I maybe received two weeks of experience as a consultant during my residency. I was willing to take it on, learning on the job and asking for help. But it occurred to me that I’m probably not alone in feeling unprepared.”
In his quest for self-education, Dr. Feldman wondered whether he should write a textbook on the subject. “But the information changes so quickly, I thought I’d have a better chance to reach people online,” he notes.
After talking to publishers and CME companies, he came up with the concept of learning modules on perioperative and consultative medicine topics, which could be taken online while earning CME credits. Johns Hopkins served as the CME certifier, and medical-education company Advanced Studies in Medicine joined as a partner. Once the project got off the ground, a medical advisory committee was convened.
“Winning the SHM poster competition is a great honor to have on a CV. It really helps to legitimize your name in the world of hospital medicine,” Dr. Feldman says. “It also provided confirmation that we were on the right track with the curriculum project. People valued what we were doing.”
Dr. Feldman and SHM have since become affiliated, and the “Consultative and Perioperative Medicine Essentials for Hospitalists” modules are available on SHM’s website (www.shmconsults.com). The site has 12,000 registered members completing 500 CME modules every month.
“I do a lot of the editing still,” Dr. Feldman says. “We update the modules every two years and are still creating new ones.”
Dr. Feldman also pursues a number of clinical-research interests, including resident education and costs of care.
Title: Assistant professor of medicine
Institution: Medical University of South Carolina, Charleston
Year: 2009
RIV: “Intensivists versus Hospitalists in the ICU: A Prospective Cohort Study Comparing Mortality and Length of Stay Between Two Staffing Models” (research) Citation: Wise KR, Akopov VA, Williams BR, Ido MS, Leeper KV, Dressler DD. Hospitalists and intensivists in the medical ICU: a prospective and observational study comparing mortality and length of stay between two staffing models. J Hosp Med. 2012;7(3):183-189.
Dr. Wise was recognized for research that began while she worked at Emory University in Atlanta, comparing hospitalists and intensivists in such outcomes as length of stay and mortality rates for patients in the ICU. The study was one of the first statistically rigorous examinations of this critical quality question. With an eye toward improving patient safety, national quality advocates such as the Leapfrog Group have called for hospitals to employ intensivists (critical-care specialists) to manage the care of ICU patients. In reality, Dr. Wise says, there aren’t enough intensivists to meet the need.
“Hospitalists are in the ICU anyway,” she says. “We just don’t have enough data to answer how well they do [in comparison to intensivists].”
Through a prospective cohort study of more than 1,000 patients, Dr. Wise’s group found that there was essentially no statistical difference in mortality rates between patients treated by intensivist teams or hospitalist ICU teams.
“We were also able to look at some of the intermediate-acuity patients—fairly complicated but not requiring ventilators,” she explains. “Our study wasn’t sufficiently powered for this subgroup, but it was an interesting piece of data to raise the question: Where should we deploy this scarce resource of intensivists? Which pockets of patients?”
Presenting her abstract at SHM’s annual meeting was a “good experience.”
“I’d done public speaking before, but never with an audience of about 500 people,” she says. “To go out there and field their questions was a real professional growing experience. Several people interested in the topic sought me out at the conference, introduced themselves, and we have subsequently stayed in touch.”
The manuscript published in JHM has been cited four times, including in a position paper from SHM and the Society of Critical Care Medicine.3 Another outgrowth of the research was being asked to contribute a chapter on hospitalists’ role in the ICU to a textbook on hospital medicine. Based on her still-fresh HM presentation, Dr. Wise was one of the few publicly identified experts on the subject. The chapter, co-authored by fellow Emory hospitalist Michael Heisler, MD, MPH, “The Role of the Hospitalist in Critical Care” was included in Principles and Practices of Hospital Medicine.4
Title: Neonatal intensivist
Institution: Stony Brook University Hospital, Great Neck, N.Y.
Year: 2006
RIV: “Administration of Inactivated Trivalent Influenza Vaccine (TIV) to Parents of Infants in the Neonatal Intensive Care Unit (NICU): A Novel Strategy to Increase Vaccination Rates” (innovations)
Citation: Shah SI, Caprio M, Hendricks-Munoz K. Administration of inactivated trivalent influenza vaccine to parents of high-risk infants in the neonatal intensive care unit. Pediatrics. 2007;120;e617-e621.
Dr. Shah was in his final year of a fellowship in neonatology at New York University when he took on the challenge of improving immunization access to protect premature, highly vulnerable patients in the NICU from influenza infections. Because these children are too young to be vaccinated directly, the concept of cocooning them from infection involves extending protection to everyone around them.
“We came up with the idea of offering flu vaccinations 24/7 in the NICU to the children’s parents,” he says. “It worked well for us as a way to define an indicated therapy for a defined population, even if it was a little outside the box. By the end of the flu season, 95% of the parents were vaccinated.”
SHM recognized the project as the top RIV innovations poster at HM06, but that was just the beginning.
“When I moved to SUNY Stony Brook, I continued to study and advocate for these vaccinations,” Dr. Shah says. “We were giving 500 to 700 vaccinations a year. Then I wrote a national resolution for the American Academy of Pediatrics, which was significant because it meant AAP was behind the project.”
Dr. Shah later became chair of AAP’s Long Island Chapter Legislative Committee and joined a statewide pediatric advocacy group. In 2009, the New York legislature enacted the Neonatal Influenza Protection Act, which required hospitals in the state to offer parents the vaccine, with Dr. Shah’s research and advocacy providing an essential basis for its passage. He’s even been recognized for his research in congressional citations.
Based on that success with influenza vaccinations, Dr. Shah and his colleagues looked at other diseases, starting with pertussis, and then tetanus, diphtheria, and whooping cough.5 All the while, they continued tracking immunization rates. A second state law, passed in 2011, added pertussis to the vaccinations. Next on his advocacy agenda is a project to promote smoking-cessation interventions in the NICU.6
“These parents come to see us every day,” he says. “What can we do, through the parents, to promote the health and well-being of their high-risk newborns?”
Title: Assistant professor of medicine; medical director of inpatient palliative-care consultation
Institution: University of Texas Health Sciences Center, San Antonio
Year: 2009
RIV: “When to Depend on the Kinins of Strangers: An Unusual Case of Abdominal Pain” (clinical vignettes)
Publication: An article on the ethics of determining code status for patients with advanced cancer and a book chapter on the “last hours of life” for a forthcoming book on palliative care and hospital medicine.
As a medical resident, Dr. Morrow met a 27-year-old woman who had chronic abdominal pain and had made multiple visits to the ED for this complaint. The patient had a history of substance abuse and requested dilaudid for her pain—making it easy for staff to consign her to the stereotype of the difficult patient.
“I met her after an interesting finding,” he says. “It turns out that on the previous emergency room visit, she received a CAT scan, which showed duodenal and small-bowel thickening consistent with hereditary angioedema, although with an unusual presentation. As it happened, we had onsite a world expert in angioedema.”
The expert was able to confirm the diagnosis, Dr. Morrow says.
“By giving her this ‘legitimate,’ organic diagnosis, it just changed the whole dynamic of her relationship with her doctors,” he says. “She knew that they knew something was really wrong. The residents were empowered to have something to hang their hats on. And we were able to get better control of her pain.”
Dr. Morrow says he came on the scene late in the discovery process, but he helped to solve the puzzle, and then put together the abstract and poster that told the story of making the diagnosis.
“In my previous job, I was hired as a hospitalist but helped to build the palliative-care program within the hospital-medicine service,” he says. “In my current job, I was brought in to build the inpatient palliative-care-consultation service, although I still moonlight as a hospitalist to stay sharp.”
Dr. Morrow says he enjoys sharing stories of difficult cases and submitting case studies about them to medical conferences, often with clever titles incorporating puns (e.g. the 2009 SHM poster citing kinins, polypeptides in the blood that cause inflammation). Another example is “The Angina Monologues,” a story of an 82-year-old patient with chronic angina pectoris and complex pain syndromes that were difficult to bring under control. Palliative care also emphasizes patients’ stories, he says, in order to understand the person behind the diagnosis.
Larry Beresford is a freelance writer in San Francisco. References available at www.the-hospitalist.org.
References
2. Yoder J. Association between hospital noise levels and inpatient sleep among middle-aged and older adults: Far from a quiet night. Abstract, Society of Hospital Medicine, 2011.
3. McKean SC, Ross JJ, Dressler DD, Brotman DJ, Ginsberg JS. Principles and Practice of Hospital Medicine. McGraw-Hill Medical; New York City: 2012.
4. Siegal EM, Dressler DD, Dichter JR, Gorman MJ, Lipsett PA. Training a hospitalist workforce to address the intensivist shortage in American hospitals: a position paper from the Society of Hospital Medicine and the Society of Critical Care Medicine. J Hosp Med. 2012;7:359-364.
5. Dylag A, Shah SI. Administration of tetanus, diphtheria, and acellular pertussis vaccine to parents of high-risk infants in the neonatal intensive care unit. Pediatrics. 2008;122:e550-e555.
6. Shah S. Smoking cessation counseling and PPSV 23-valent pneumococcal polysaccharide vaccine administration parents of neonatal intensive care unit (NICU)-admitted infants: A life-changing opportunity. J Neonatal-Perinatal Med. 2011;4:263-267.
Back to the Furture Past RIV winners talk about what the recognition meant for their careers By Larry Beresford
After winning SHM’s annual Research, Innovations, and Clinical Vignettes (RIV) scientific abstract and poster competition for an abstract illustrating a program that promoted flu vaccinations for families of neonatal patients, Shetal Shah, MD, FAAP, became a leading advocate for two laws mandating that New York hospitals offer vaccinations to families.
A poster that described a VTE prevention program led Gregory Maynard, MD, MSc, SFHM, to join SHM’s VTE Prevention Collaborative and, eventually, to become senior vice president of the society’s Center for Hospital Innovation and Improvement.
A prize-winning innovations poster for improving team communication by Vineet Chopra, MD, MS, FACP, FHM, and colleagues later took off as a new technology company.
Leonard Feldman, MD, FAAP, SFHM, won for a poster that explained online CME curriculum for hospitalists as consultants; the curriculum now resides on SHM’s website.
The evidence is clear: RIV abstracts are a vital part of hospital medicine.
Nearly 800 abstracts were submitted for HM13.
Awards are given in three categories:
- Research posters report clinical or basic science data, systematically review a clinical problem, or address efficiency, cost, or method of health-care delivery or medical decision-making;
- Innovations posters describe an existing innovative program in hospital medicine, often with preliminary data; and
- Clinical vignettes, either adult or pediatric, report on one or more cases illustrating a new disease entity, a prominent or unusual feature of an established disease, or an area of clinical controversy.
The Hospitalist asked 11 past RIV winners what the poster contest meant to their careers. Some added more data and analysis and went on to be published in such medical journals as the Journal of Hospital Medicine. Some used the recognition to launch or boost research-oriented careers; others saw their careers go in different directions.
“Winning a national poster competition gives you the confidence to continue to pursue your interest and take it to a higher level, like successfully competing for funding and publishing your line of inquiry,” says hospitalist and researcher Vineet Arora, MD, MPP, FHM, of the University of Chicago, who won the 2006 RIV research competition. “Sometimes, presenting posters can be lonely, but at SHM, you get a lot of traffic. You get a chance to practice your spiel, communicating science and research in a very concise way, which is an important skill to have.”
David Metzger, MD, PhD, also from the University of Chicago, who won the RIV research award in 2005, says recognition is a big deal, but “one of the biggest values of the RIV competition is just getting information out to colleagues, with the opportunity to talk with your peers. That’s the real prize.
“I’ve been involved in presenting posters at SHM every year that the society has been in existence,” he says. “I’ve met so many people and talked about what they’re doing. That’s what a medical society should do—bring people together like this.”
Title: Administrator, academic consult service; teaching staff physician
Institution: Saint Joseph Mercy Hospital, Ypsilanti, Mich.
Year: 2008
RIV: “A Case of Salty Voluminous Urine” (clinical vignette)
Dr. Tassava was honored two years in a row for topics drawn from her experience as a hospitalist working in the surgical ICU. Her HM08 entry won top poster, and her HM09 poster, “Permissive Hypernatremia: Co-Management of Intracranial Pressure in a Patient with Diabetes Insipidus,” was selected for an oral presentation.
The HM09 vignette described how the hypernatremia that occurs with diabetes insipidus could be used in a novel way to control intracranial pressure in a 17-year-old patient who had a traumatic brain injury from an auto accident.
“She had a beautiful outcome,” Dr. Tassava says. “She started college and she came back to our unit for a visit after her recovery.”
Dr. Tassava enjoyed the opportunity to explain to her peers how diabetes insipidus presented and how she managed the case. “I was a little surprised at how much discussion was generated by my case,” she says, “even though I knew this was an important and novel approach.”
When her hospital added intensivists, her work and research in the ICU ended and her career moved more toward hospitalist administration. She now runs the academic consult service at St. Joseph, serves as lead physician for the orthopedic surgery floor, instructs and mentors medical residents, and chairs the hospital’s Coagulation Collaborative Practice Team (Coagulation CPT). She credits the RIV honors with helping her to gain recognition as an academic hospitalist who was nominated for leadership roles. She has moved out of research for now but plans to pursue anticoagulation research in the future.
“I really appreciated the recognition for my curiosity and scientific approach, which was acknowledged by my surgical colleagues,” Dr. Tassava says. “I absolutely love the CPT. I am the hospital’s principal educator with regard to anticoagulation. Over the past year, I have given medicine and cardiology grand rounds, and have presented on the newest anticoagulants.”
Dr. Tassava still collaborates with her residents on abstracts, several of which have been submitted to SHM, the American College of Physicians, and other medical societies.
“I still love research,” she says. “I have a million ideas.”
Title: Chief of the division of hospital medicine; senior vice president, SHM’s Center for Innovation and Improvement
Institution: University of California at San Diego (UCSD)
Year: 2008
RIV: “Prevention of Hospital-Acquired Venous Thromboembolism: Prospective Validation of a VTE Risk Assessment Model and Protocol” (research)
Citations: Maynard G, Stein J. Designing and implementing effective VTE prevention protocols: lessons from collaboratives. J Thromb Thrombolysis. 2010;29(2):159-166. Maynard G, Morris T, Jenkins I, et al. Optimizing prevention of hospital acquired venous thromboembolism: prospective validation of a VTE risk assessment model. J Hosp Med. 2010;5(1):10-18.
Dr. Maynard’s abstract described a project funded by the federal Agency for Healthcare Research and Quality to design and implement an organized, comprehensive protocol for VTE prevention within the hospital setting. The project also included a toolkit to help other hospitals do the same thing. The same group received SHM’s Award of Excellence for Teamwork.
This work, combined with similar efforts by Jason Stein, MD, and colleagues at Emory University in Atlanta and others, provided the foundation for SHM’s VTE resource room and the mentored implementation program of SHM’s VTE Prevention Collaborative, which had been launched in 2007 as one of the society’s first large-scale quality-improvement (QI) initiatives.
“SHM wanted to do something about VTE prevention, and when we got our AHRQ grant, I was interested in doing the same,” Dr. Maynard says. “We published our implementation guides on the AHRQ and SHM websites, along with a lot of valuable supporting materials.”
Dr. Maynard later took on leadership roles with SHM’s quality initiatives on glycemic control and care transitions, which made him the logical choice to become senior vice president of SHM’s Center for Hospital Innovation and Improvement.
He says the RIV honor lifted his profile not only within SHM, but also throughout the field, and it was instrumental in obtaining continued funding to advance the VTE initiative. “We did this tremendous work—with great results,” he says. “But I don’t think our local administrators appreciated it quite as much until we started to get external, national recognition.”
Dr. Maynard earned his master’s degree in biostatistics and clinical research design from the University of Michigan—skills he later brought to the academic setting at UCSD.
“It was a nice way for a hospitalist, who’s really a medical generalist, to become an expert in something,” he says. “I could never be more of an expert in cardiology than a cardiologist, or more of an expert in DVT than a hematologist or critical-care specialist. But I could help both of them do what they couldn’t do as effectively, which was to implement protocols reliably using a QI framework.”
Title: Assistant professor of general internal medicine, hospital medicine, and public health
Institution: Vanderbilt University, Nashville, Tenn.
Year: 2009
RIV: “Predictors of Early Post-Discharge Mortality in Critically Ill Patients: Lessons for Quality Performance and Quality Assessment” (research)
Citation: Vasilevskis EE, Kuzniewicz MW, Cason BA, et al. Predictors of early post-discharge mortality in critically ill patients: a retrospective cohort study from the California Intensive Care Outcomes project. J Crit Care. 2011;26(1):65-75.
Dr. Vasilevskis has submitted abstracts to the RIV competition almost every year since 2007, when he was completing a fellowship at the University of California at San Francisco’s Institute for Health Policy Studies. He was honored in 2009 for a project based on the California Intensive Care Outcomes Project, which drew data from 35 hospitals to demonstrate that shortening ICU length of stay was predictive of early post-discharge mortality in the most severely ill patients.
He has continued to research quality and safety in the ICU, and he has published dozens of journal articles.
“My initial focus was on traditional mortality and length-of-stay outcomes,” he says. “I am now pursuing additional outcomes, most notably delirium in the ICU patient. I work with an amazing group of researchers that are trying to better measure, define, and treat delirium in the ICU—an outcome associated with a number of poor patient outcomes.”
Dr. Vasilevskis also is researching the causes of hospital readmissions and the development of novel ways to improve care transitions for elderly patients. He is pursuing a master’s of public health at Vanderbilt, and is co-principal investigator of an investigation of the Hospital Medicine Reengineering Network to improve transitions of care, supported by the Association of American Medical Colleges.
In addition to his 2009 win, he captured the HM10 and HM12 research categories. His HM12 poster, “Veterans Administration Acute Care 30-Day Mortality Model: Development, Validation and Performance Variation,” was singled out by the judging committee for its impressive sample size (1,114,327 patients in a retrospective cohort study of 131 VA hospitals), as well as for how it combined administrative and clinical risk models.
Dr. Vasilevskis says the opportunity to present his research at SHM and the recognition he received encouraged him to continue as a hospitalist engaged in medical research. He has been a member of SHM’s Research Committee since 2009, an RIV judge at HM11, and chaired the HM13 RIV competition subcommittee.
Title: Assistant professor of medicine
Institution: University of Michigan Health System, Ann Arbor
Year: 2009
RIV: “MComm: Redefining Medical Communications in the 21st Century” (innovations)
Early in his career, Dr. Chopra was curious about how to improve the way patient care is delivered in the hospital setting. He was particularly interested in the inordinate amount of time hospitalists spend every day on communication.
“I saw one-way paging systems as a problem for communication between members of the medical team,” he says. “Doctors get paged and break off from what they’re doing to return the page—to someone who often isn’t there to take the call back. Sometimes the system gives us the wrong number or a cryptic message that makes no sense.”
A technological solution to this problem, which he and hospitalist Prasanth Gogineni, MD, conceived, designed, and created, then tested at the University of Michigan, is called MComm. Dr. Chopra describes it as a novel, uniform way of messaging for the entire medical team using wireless servers, PUSH technology, and iPhones. MComm was built around existing hospital workflow and patient-specific task lists, assigning priority to each message and documenting that it was delivered. The junior faculty members submitted an abstract about their innovative application, not really expecting it to get accepted. But when it won the poster competition and was selected for a plenary presentation, things got busy in a hurry. Specifically, the university hospital’s Office of Technology Transfer took a keen interest.
“We met with a number of people who had business experience in the health-care-technology space and found a CEO for the company we formed to develop MComm,” Dr. Chopra says. “I found myself getting pulled into it very quickly, with a lot of conversations about commercialization, revenue-sharing models, intellectual property, and the like.”
But running a company was not something Dr. Chopra wanted to do. Two years ago, that company, Synaptin, went one way and he went another—he stayed at Michigan as a medical researcher. He remains deeply interested in how care is delivered to hospitalized patients, but with a focus on such patient-safety questions as how to prevent negative outcomes from indwelling venous catheters.
“Winning the poster competition opened doors for me—there’s no doubt in my mind,” he says. “We demonstrated the ability to deliver a project of significance, from concept to prototype, without formal training in this area. If we didn’t have that recognition, I’m not sure I would have been ready to step into a research career as quickly. It helped me realize that medical research was what I wanted to do.”
Title: Associate program director, internal-medicine residency; assistant dean of scholarship and discovery
Institution: Pritzker School of Medicine, University of Chicago
Year: 2006
RIV: “Measuring Quality of Hospital Care for Vulnerable Elders: Use of ACOVE Quality Indicators” (research)
Citation: Arora VM, Fish M, Basu A, et al. Relationship between quality of care of hospitalized vulnerable elders and postdischarge mortality. J Am Geriatrics. 2010;58:1642-1648.
Title: Associate professor, department of medicine; associate faculty member, Harris School and the Department of Economics
Institution: University of Chicago
Year: 2005
RIV: “Effects of Hospitalists on Outcomes and Costs in a Multicenter Trial of Academic Hospitalists” (research)
Dr. Meltzer was the lead author, with 11 other prominent hospitalists, of an abstract based on a multisite study of the cost and outcome implications of the hospitalist model—still a relatively new concept in 2001, when the research began. Although the study did not uncover large cost savings realized from the hospitalist model of care, as some advocates had hoped, important findings and implications for the emerging field were teased out of the data.
At the time, only a few randomly controlled, multisite studies of costs and outcomes for the hospitalist model had been performed. The study, Dr. Meltzer says, required a complicated analysis to discover that hospitalists, in fact, saved their facilities money, with their most important impact realized post-hospitalization, such as on nursing-home costs. It was important to control for spillover effect and the fact that hospitalists do a better job of teaching house staff, while a physician’s years of experience was another important variable, he says.
Dr. Meltzer was a medical researcher interested in medical specialization when the term “hospitalist” was first coined in 1996. “I thought, here was a chance to study a medical specialty in its formative stages,” he says.
He still works as a hospitalist, although with limited clinical time. In addition to his administrative work as division chief, he directs the Center for Health and the Social Sciences at the University of Chicago. His research interests include cost-effectiveness, technology assessment, and information research.
In 2010, his poster “Effects of Hospitalists on 1-Year Post-Discharge Resource Utilization by Medicare Beneficiaries” took the top prize in the HM10 research competition. In 2011, he was appointed to the methodology committee of the federal Patient-Centered Outcomes Research Institute (PCORI), which was created by the Affordable Care Act to advise the government on clinical-effectiveness research. He also sits on the Advisory Council to the National Institute of General Medical Sciences at the Institute of Medicine, and on the Congressional Budget Office’s panel of health advisors.
In a career full of recognition, Dr. Meltzer says it’s hard to pinpoint the impact of winning the poster contest. But he has continued to submit abstracts to SHM every year and appreciates the opportunities for interaction with peers at the poster exhibits.
Title: Director of perioperative and consultative medicine
Institution: University of Michigan, Ann Arbor
Year: 2006
RIV: “Disseminated Histoplasmosis Presenting As Painful Oral Ulcers” (clinical vignettes)
Dr. Grant’s winning vignette presented a patient with a complex medical history, including heart disease and four months of painful oral ulcers, for which prior evaluations had been inconclusive, despite conducting biopsies. Following administration of high-dose corticosteroids, the patient’s condition worsened on multiple fronts. The vignette showed how the medical team was able to diagnose an unusual presentation of a fungal infection called histoplasmosis, which is prevalent in parts of the Midwest surrounding the Ohio and Mississippi river valleys.
“We see a lot of cases in the hospital where there are different angles you could take to turn it into a clinical vignette or a nice poster with good teaching points,” Dr. Grant says. “In this case, just digging deeper into the actual diagnosis was important because the empiric use of steroids can be fatal for some patients. Steroids are given for a lot of good reasons, but in this patient they caused immune suppression, allowing a smoldering infection to become very active.”
Dr. Grant did not submit the vignette for publication. “That was probably a mistake on my part,” he says, acknowledging the common complaint of too little time and too many competing priorities. But his interest in research has continued.
“I became involved at a national level with issues of perioperative medicine and last August published a textbook on the subject,” he reports.1 “VTE is another area of interest I have developed since my hospital medicine fellowship.”
He serves as the VTE resource expert on the Michigan Hospital Medicine Safety Consortium, a quality collaborative of more than 40 hospitals with Blue Cross/Blue Shield of Michigan. “It’s exciting to be able to look at the risk factors, what kinds of patients get VTEs, and whether they were appropriately prophylaxed in the hospital,” he says.
VTE is a national quality priority, and Dr. Grant expects abstracts to emerge from the consortium’s work.
He says he appreciates the opportunities that arise from participating in poster sessions at SHM, where medical students, residents, and working hospitalists talk to the presenters of interesting cases.
“It gives you a real back-and-forth, which is good for the person asking the question and for the presenter,” he says, noting hospitalists from other parts of the country were not as familiar with histoplasmosis.
He says winning the HM06 poster contest helped him “get his feet wet” and feel more prepared for a career in academic hospital medicine. “I’m sure the award solidified my employers’ satisfaction in hiring me—and in giving me more desirable academic roles and responsibilities,” he adds.
Title: Assistant professor of medicine pediatrics; director of the general internal-medicine comprehensive consultation service
Institution: Johns Hopkins Hospital, Baltimore
Year: 2009
RIV: “An Internet-Based Consult Curriculum for Hospitalists” (innovations)
Dr. Feldman’s poster described an online CME curriculum for hospitalists acting as medical consultants. The concept grew out of a perceived deficiency in his own medical education when, in 2004, he was asked to lead the consultation service at Johns Hopkins—just six months after finishing his residency.
“I had no idea what I was doing as a general-internal-medicine consultant,” he says. “I maybe received two weeks of experience as a consultant during my residency. I was willing to take it on, learning on the job and asking for help. But it occurred to me that I’m probably not alone in feeling unprepared.”
In his quest for self-education, Dr. Feldman wondered whether he should write a textbook on the subject. “But the information changes so quickly, I thought I’d have a better chance to reach people online,” he notes.
After talking to publishers and CME companies, he came up with the concept of learning modules on perioperative and consultative medicine topics, which could be taken online while earning CME credits. Johns Hopkins served as the CME certifier, and medical-education company Advanced Studies in Medicine joined as a partner. Once the project got off the ground, a medical advisory committee was convened.
“Winning the SHM poster competition is a great honor to have on a CV. It really helps to legitimize your name in the world of hospital medicine,” Dr. Feldman says. “It also provided confirmation that we were on the right track with the curriculum project. People valued what we were doing.”
Dr. Feldman and SHM have since become affiliated, and the “Consultative and Perioperative Medicine Essentials for Hospitalists” modules are available on SHM’s website (www.shmconsults.com). The site has 12,000 registered members completing 500 CME modules every month.
“I do a lot of the editing still,” Dr. Feldman says. “We update the modules every two years and are still creating new ones.”
Dr. Feldman also pursues a number of clinical-research interests, including resident education and costs of care.
Title: Assistant professor of medicine
Institution: Medical University of South Carolina, Charleston
Year: 2009
RIV: “Intensivists versus Hospitalists in the ICU: A Prospective Cohort Study Comparing Mortality and Length of Stay Between Two Staffing Models” (research) Citation: Wise KR, Akopov VA, Williams BR, Ido MS, Leeper KV, Dressler DD. Hospitalists and intensivists in the medical ICU: a prospective and observational study comparing mortality and length of stay between two staffing models. J Hosp Med. 2012;7(3):183-189.
Dr. Wise was recognized for research that began while she worked at Emory University in Atlanta, comparing hospitalists and intensivists in such outcomes as length of stay and mortality rates for patients in the ICU. The study was one of the first statistically rigorous examinations of this critical quality question. With an eye toward improving patient safety, national quality advocates such as the Leapfrog Group have called for hospitals to employ intensivists (critical-care specialists) to manage the care of ICU patients. In reality, Dr. Wise says, there aren’t enough intensivists to meet the need.
“Hospitalists are in the ICU anyway,” she says. “We just don’t have enough data to answer how well they do [in comparison to intensivists].”
Through a prospective cohort study of more than 1,000 patients, Dr. Wise’s group found that there was essentially no statistical difference in mortality rates between patients treated by intensivist teams or hospitalist ICU teams.
“We were also able to look at some of the intermediate-acuity patients—fairly complicated but not requiring ventilators,” she explains. “Our study wasn’t sufficiently powered for this subgroup, but it was an interesting piece of data to raise the question: Where should we deploy this scarce resource of intensivists? Which pockets of patients?”
Presenting her abstract at SHM’s annual meeting was a “good experience.”
“I’d done public speaking before, but never with an audience of about 500 people,” she says. “To go out there and field their questions was a real professional growing experience. Several people interested in the topic sought me out at the conference, introduced themselves, and we have subsequently stayed in touch.”
The manuscript published in JHM has been cited four times, including in a position paper from SHM and the Society of Critical Care Medicine.3 Another outgrowth of the research was being asked to contribute a chapter on hospitalists’ role in the ICU to a textbook on hospital medicine. Based on her still-fresh HM presentation, Dr. Wise was one of the few publicly identified experts on the subject. The chapter, co-authored by fellow Emory hospitalist Michael Heisler, MD, MPH, “The Role of the Hospitalist in Critical Care” was included in Principles and Practices of Hospital Medicine.4
Title: Neonatal intensivist
Institution: Stony Brook University Hospital, Great Neck, N.Y.
Year: 2006
RIV: “Administration of Inactivated Trivalent Influenza Vaccine (TIV) to Parents of Infants in the Neonatal Intensive Care Unit (NICU): A Novel Strategy to Increase Vaccination Rates” (innovations)
Citation: Shah SI, Caprio M, Hendricks-Munoz K. Administration of inactivated trivalent influenza vaccine to parents of high-risk infants in the neonatal intensive care unit. Pediatrics. 2007;120;e617-e621.
Dr. Shah was in his final year of a fellowship in neonatology at New York University when he took on the challenge of improving immunization access to protect premature, highly vulnerable patients in the NICU from influenza infections. Because these children are too young to be vaccinated directly, the concept of cocooning them from infection involves extending protection to everyone around them.
“We came up with the idea of offering flu vaccinations 24/7 in the NICU to the children’s parents,” he says. “It worked well for us as a way to define an indicated therapy for a defined population, even if it was a little outside the box. By the end of the flu season, 95% of the parents were vaccinated.”
SHM recognized the project as the top RIV innovations poster at HM06, but that was just the beginning.
“When I moved to SUNY Stony Brook, I continued to study and advocate for these vaccinations,” Dr. Shah says. “We were giving 500 to 700 vaccinations a year. Then I wrote a national resolution for the American Academy of Pediatrics, which was significant because it meant AAP was behind the project.”
Dr. Shah later became chair of AAP’s Long Island Chapter Legislative Committee and joined a statewide pediatric advocacy group. In 2009, the New York legislature enacted the Neonatal Influenza Protection Act, which required hospitals in the state to offer parents the vaccine, with Dr. Shah’s research and advocacy providing an essential basis for its passage. He’s even been recognized for his research in congressional citations.
Based on that success with influenza vaccinations, Dr. Shah and his colleagues looked at other diseases, starting with pertussis, and then tetanus, diphtheria, and whooping cough.5 All the while, they continued tracking immunization rates. A second state law, passed in 2011, added pertussis to the vaccinations. Next on his advocacy agenda is a project to promote smoking-cessation interventions in the NICU.6
“These parents come to see us every day,” he says. “What can we do, through the parents, to promote the health and well-being of their high-risk newborns?”
Title: Assistant professor of medicine; medical director of inpatient palliative-care consultation
Institution: University of Texas Health Sciences Center, San Antonio
Year: 2009
RIV: “When to Depend on the Kinins of Strangers: An Unusual Case of Abdominal Pain” (clinical vignettes)
Publication: An article on the ethics of determining code status for patients with advanced cancer and a book chapter on the “last hours of life” for a forthcoming book on palliative care and hospital medicine.
As a medical resident, Dr. Morrow met a 27-year-old woman who had chronic abdominal pain and had made multiple visits to the ED for this complaint. The patient had a history of substance abuse and requested dilaudid for her pain—making it easy for staff to consign her to the stereotype of the difficult patient.
“I met her after an interesting finding,” he says. “It turns out that on the previous emergency room visit, she received a CAT scan, which showed duodenal and small-bowel thickening consistent with hereditary angioedema, although with an unusual presentation. As it happened, we had onsite a world expert in angioedema.”
The expert was able to confirm the diagnosis, Dr. Morrow says.
“By giving her this ‘legitimate,’ organic diagnosis, it just changed the whole dynamic of her relationship with her doctors,” he says. “She knew that they knew something was really wrong. The residents were empowered to have something to hang their hats on. And we were able to get better control of her pain.”
Dr. Morrow says he came on the scene late in the discovery process, but he helped to solve the puzzle, and then put together the abstract and poster that told the story of making the diagnosis.
“In my previous job, I was hired as a hospitalist but helped to build the palliative-care program within the hospital-medicine service,” he says. “In my current job, I was brought in to build the inpatient palliative-care-consultation service, although I still moonlight as a hospitalist to stay sharp.”
Dr. Morrow says he enjoys sharing stories of difficult cases and submitting case studies about them to medical conferences, often with clever titles incorporating puns (e.g. the 2009 SHM poster citing kinins, polypeptides in the blood that cause inflammation). Another example is “The Angina Monologues,” a story of an 82-year-old patient with chronic angina pectoris and complex pain syndromes that were difficult to bring under control. Palliative care also emphasizes patients’ stories, he says, in order to understand the person behind the diagnosis.
Larry Beresford is a freelance writer in San Francisco. References available at www.the-hospitalist.org.
References
2. Yoder J. Association between hospital noise levels and inpatient sleep among middle-aged and older adults: Far from a quiet night. Abstract, Society of Hospital Medicine, 2011.
3. McKean SC, Ross JJ, Dressler DD, Brotman DJ, Ginsberg JS. Principles and Practice of Hospital Medicine. McGraw-Hill Medical; New York City: 2012.
4. Siegal EM, Dressler DD, Dichter JR, Gorman MJ, Lipsett PA. Training a hospitalist workforce to address the intensivist shortage in American hospitals: a position paper from the Society of Hospital Medicine and the Society of Critical Care Medicine. J Hosp Med. 2012;7:359-364.
5. Dylag A, Shah SI. Administration of tetanus, diphtheria, and acellular pertussis vaccine to parents of high-risk infants in the neonatal intensive care unit. Pediatrics. 2008;122:e550-e555.
6. Shah S. Smoking cessation counseling and PPSV 23-valent pneumococcal polysaccharide vaccine administration parents of neonatal intensive care unit (NICU)-admitted infants: A life-changing opportunity. J Neonatal-Perinatal Med. 2011;4:263-267.
Back to the Furture Past RIV winners talk about what the recognition meant for their careers By Larry Beresford
After winning SHM’s annual Research, Innovations, and Clinical Vignettes (RIV) scientific abstract and poster competition for an abstract illustrating a program that promoted flu vaccinations for families of neonatal patients, Shetal Shah, MD, FAAP, became a leading advocate for two laws mandating that New York hospitals offer vaccinations to families.
A poster that described a VTE prevention program led Gregory Maynard, MD, MSc, SFHM, to join SHM’s VTE Prevention Collaborative and, eventually, to become senior vice president of the society’s Center for Hospital Innovation and Improvement.
A prize-winning innovations poster for improving team communication by Vineet Chopra, MD, MS, FACP, FHM, and colleagues later took off as a new technology company.
Leonard Feldman, MD, FAAP, SFHM, won for a poster that explained online CME curriculum for hospitalists as consultants; the curriculum now resides on SHM’s website.
The evidence is clear: RIV abstracts are a vital part of hospital medicine.
Nearly 800 abstracts were submitted for HM13.
Awards are given in three categories:
- Research posters report clinical or basic science data, systematically review a clinical problem, or address efficiency, cost, or method of health-care delivery or medical decision-making;
- Innovations posters describe an existing innovative program in hospital medicine, often with preliminary data; and
- Clinical vignettes, either adult or pediatric, report on one or more cases illustrating a new disease entity, a prominent or unusual feature of an established disease, or an area of clinical controversy.
The Hospitalist asked 11 past RIV winners what the poster contest meant to their careers. Some added more data and analysis and went on to be published in such medical journals as the Journal of Hospital Medicine. Some used the recognition to launch or boost research-oriented careers; others saw their careers go in different directions.
“Winning a national poster competition gives you the confidence to continue to pursue your interest and take it to a higher level, like successfully competing for funding and publishing your line of inquiry,” says hospitalist and researcher Vineet Arora, MD, MPP, FHM, of the University of Chicago, who won the 2006 RIV research competition. “Sometimes, presenting posters can be lonely, but at SHM, you get a lot of traffic. You get a chance to practice your spiel, communicating science and research in a very concise way, which is an important skill to have.”
David Metzger, MD, PhD, also from the University of Chicago, who won the RIV research award in 2005, says recognition is a big deal, but “one of the biggest values of the RIV competition is just getting information out to colleagues, with the opportunity to talk with your peers. That’s the real prize.
“I’ve been involved in presenting posters at SHM every year that the society has been in existence,” he says. “I’ve met so many people and talked about what they’re doing. That’s what a medical society should do—bring people together like this.”
Title: Administrator, academic consult service; teaching staff physician
Institution: Saint Joseph Mercy Hospital, Ypsilanti, Mich.
Year: 2008
RIV: “A Case of Salty Voluminous Urine” (clinical vignette)
Dr. Tassava was honored two years in a row for topics drawn from her experience as a hospitalist working in the surgical ICU. Her HM08 entry won top poster, and her HM09 poster, “Permissive Hypernatremia: Co-Management of Intracranial Pressure in a Patient with Diabetes Insipidus,” was selected for an oral presentation.
The HM09 vignette described how the hypernatremia that occurs with diabetes insipidus could be used in a novel way to control intracranial pressure in a 17-year-old patient who had a traumatic brain injury from an auto accident.
“She had a beautiful outcome,” Dr. Tassava says. “She started college and she came back to our unit for a visit after her recovery.”
Dr. Tassava enjoyed the opportunity to explain to her peers how diabetes insipidus presented and how she managed the case. “I was a little surprised at how much discussion was generated by my case,” she says, “even though I knew this was an important and novel approach.”
When her hospital added intensivists, her work and research in the ICU ended and her career moved more toward hospitalist administration. She now runs the academic consult service at St. Joseph, serves as lead physician for the orthopedic surgery floor, instructs and mentors medical residents, and chairs the hospital’s Coagulation Collaborative Practice Team (Coagulation CPT). She credits the RIV honors with helping her to gain recognition as an academic hospitalist who was nominated for leadership roles. She has moved out of research for now but plans to pursue anticoagulation research in the future.
“I really appreciated the recognition for my curiosity and scientific approach, which was acknowledged by my surgical colleagues,” Dr. Tassava says. “I absolutely love the CPT. I am the hospital’s principal educator with regard to anticoagulation. Over the past year, I have given medicine and cardiology grand rounds, and have presented on the newest anticoagulants.”
Dr. Tassava still collaborates with her residents on abstracts, several of which have been submitted to SHM, the American College of Physicians, and other medical societies.
“I still love research,” she says. “I have a million ideas.”
Title: Chief of the division of hospital medicine; senior vice president, SHM’s Center for Innovation and Improvement
Institution: University of California at San Diego (UCSD)
Year: 2008
RIV: “Prevention of Hospital-Acquired Venous Thromboembolism: Prospective Validation of a VTE Risk Assessment Model and Protocol” (research)
Citations: Maynard G, Stein J. Designing and implementing effective VTE prevention protocols: lessons from collaboratives. J Thromb Thrombolysis. 2010;29(2):159-166. Maynard G, Morris T, Jenkins I, et al. Optimizing prevention of hospital acquired venous thromboembolism: prospective validation of a VTE risk assessment model. J Hosp Med. 2010;5(1):10-18.
Dr. Maynard’s abstract described a project funded by the federal Agency for Healthcare Research and Quality to design and implement an organized, comprehensive protocol for VTE prevention within the hospital setting. The project also included a toolkit to help other hospitals do the same thing. The same group received SHM’s Award of Excellence for Teamwork.
This work, combined with similar efforts by Jason Stein, MD, and colleagues at Emory University in Atlanta and others, provided the foundation for SHM’s VTE resource room and the mentored implementation program of SHM’s VTE Prevention Collaborative, which had been launched in 2007 as one of the society’s first large-scale quality-improvement (QI) initiatives.
“SHM wanted to do something about VTE prevention, and when we got our AHRQ grant, I was interested in doing the same,” Dr. Maynard says. “We published our implementation guides on the AHRQ and SHM websites, along with a lot of valuable supporting materials.”
Dr. Maynard later took on leadership roles with SHM’s quality initiatives on glycemic control and care transitions, which made him the logical choice to become senior vice president of SHM’s Center for Hospital Innovation and Improvement.
He says the RIV honor lifted his profile not only within SHM, but also throughout the field, and it was instrumental in obtaining continued funding to advance the VTE initiative. “We did this tremendous work—with great results,” he says. “But I don’t think our local administrators appreciated it quite as much until we started to get external, national recognition.”
Dr. Maynard earned his master’s degree in biostatistics and clinical research design from the University of Michigan—skills he later brought to the academic setting at UCSD.
“It was a nice way for a hospitalist, who’s really a medical generalist, to become an expert in something,” he says. “I could never be more of an expert in cardiology than a cardiologist, or more of an expert in DVT than a hematologist or critical-care specialist. But I could help both of them do what they couldn’t do as effectively, which was to implement protocols reliably using a QI framework.”
Title: Assistant professor of general internal medicine, hospital medicine, and public health
Institution: Vanderbilt University, Nashville, Tenn.
Year: 2009
RIV: “Predictors of Early Post-Discharge Mortality in Critically Ill Patients: Lessons for Quality Performance and Quality Assessment” (research)
Citation: Vasilevskis EE, Kuzniewicz MW, Cason BA, et al. Predictors of early post-discharge mortality in critically ill patients: a retrospective cohort study from the California Intensive Care Outcomes project. J Crit Care. 2011;26(1):65-75.
Dr. Vasilevskis has submitted abstracts to the RIV competition almost every year since 2007, when he was completing a fellowship at the University of California at San Francisco’s Institute for Health Policy Studies. He was honored in 2009 for a project based on the California Intensive Care Outcomes Project, which drew data from 35 hospitals to demonstrate that shortening ICU length of stay was predictive of early post-discharge mortality in the most severely ill patients.
He has continued to research quality and safety in the ICU, and he has published dozens of journal articles.
“My initial focus was on traditional mortality and length-of-stay outcomes,” he says. “I am now pursuing additional outcomes, most notably delirium in the ICU patient. I work with an amazing group of researchers that are trying to better measure, define, and treat delirium in the ICU—an outcome associated with a number of poor patient outcomes.”
Dr. Vasilevskis also is researching the causes of hospital readmissions and the development of novel ways to improve care transitions for elderly patients. He is pursuing a master’s of public health at Vanderbilt, and is co-principal investigator of an investigation of the Hospital Medicine Reengineering Network to improve transitions of care, supported by the Association of American Medical Colleges.
In addition to his 2009 win, he captured the HM10 and HM12 research categories. His HM12 poster, “Veterans Administration Acute Care 30-Day Mortality Model: Development, Validation and Performance Variation,” was singled out by the judging committee for its impressive sample size (1,114,327 patients in a retrospective cohort study of 131 VA hospitals), as well as for how it combined administrative and clinical risk models.
Dr. Vasilevskis says the opportunity to present his research at SHM and the recognition he received encouraged him to continue as a hospitalist engaged in medical research. He has been a member of SHM’s Research Committee since 2009, an RIV judge at HM11, and chaired the HM13 RIV competition subcommittee.
Title: Assistant professor of medicine
Institution: University of Michigan Health System, Ann Arbor
Year: 2009
RIV: “MComm: Redefining Medical Communications in the 21st Century” (innovations)
Early in his career, Dr. Chopra was curious about how to improve the way patient care is delivered in the hospital setting. He was particularly interested in the inordinate amount of time hospitalists spend every day on communication.
“I saw one-way paging systems as a problem for communication between members of the medical team,” he says. “Doctors get paged and break off from what they’re doing to return the page—to someone who often isn’t there to take the call back. Sometimes the system gives us the wrong number or a cryptic message that makes no sense.”
A technological solution to this problem, which he and hospitalist Prasanth Gogineni, MD, conceived, designed, and created, then tested at the University of Michigan, is called MComm. Dr. Chopra describes it as a novel, uniform way of messaging for the entire medical team using wireless servers, PUSH technology, and iPhones. MComm was built around existing hospital workflow and patient-specific task lists, assigning priority to each message and documenting that it was delivered. The junior faculty members submitted an abstract about their innovative application, not really expecting it to get accepted. But when it won the poster competition and was selected for a plenary presentation, things got busy in a hurry. Specifically, the university hospital’s Office of Technology Transfer took a keen interest.
“We met with a number of people who had business experience in the health-care-technology space and found a CEO for the company we formed to develop MComm,” Dr. Chopra says. “I found myself getting pulled into it very quickly, with a lot of conversations about commercialization, revenue-sharing models, intellectual property, and the like.”
But running a company was not something Dr. Chopra wanted to do. Two years ago, that company, Synaptin, went one way and he went another—he stayed at Michigan as a medical researcher. He remains deeply interested in how care is delivered to hospitalized patients, but with a focus on such patient-safety questions as how to prevent negative outcomes from indwelling venous catheters.
“Winning the poster competition opened doors for me—there’s no doubt in my mind,” he says. “We demonstrated the ability to deliver a project of significance, from concept to prototype, without formal training in this area. If we didn’t have that recognition, I’m not sure I would have been ready to step into a research career as quickly. It helped me realize that medical research was what I wanted to do.”
Title: Associate program director, internal-medicine residency; assistant dean of scholarship and discovery
Institution: Pritzker School of Medicine, University of Chicago
Year: 2006
RIV: “Measuring Quality of Hospital Care for Vulnerable Elders: Use of ACOVE Quality Indicators” (research)
Citation: Arora VM, Fish M, Basu A, et al. Relationship between quality of care of hospitalized vulnerable elders and postdischarge mortality. J Am Geriatrics. 2010;58:1642-1648.
Title: Associate professor, department of medicine; associate faculty member, Harris School and the Department of Economics
Institution: University of Chicago
Year: 2005
RIV: “Effects of Hospitalists on Outcomes and Costs in a Multicenter Trial of Academic Hospitalists” (research)
Dr. Meltzer was the lead author, with 11 other prominent hospitalists, of an abstract based on a multisite study of the cost and outcome implications of the hospitalist model—still a relatively new concept in 2001, when the research began. Although the study did not uncover large cost savings realized from the hospitalist model of care, as some advocates had hoped, important findings and implications for the emerging field were teased out of the data.
At the time, only a few randomly controlled, multisite studies of costs and outcomes for the hospitalist model had been performed. The study, Dr. Meltzer says, required a complicated analysis to discover that hospitalists, in fact, saved their facilities money, with their most important impact realized post-hospitalization, such as on nursing-home costs. It was important to control for spillover effect and the fact that hospitalists do a better job of teaching house staff, while a physician’s years of experience was another important variable, he says.
Dr. Meltzer was a medical researcher interested in medical specialization when the term “hospitalist” was first coined in 1996. “I thought, here was a chance to study a medical specialty in its formative stages,” he says.
He still works as a hospitalist, although with limited clinical time. In addition to his administrative work as division chief, he directs the Center for Health and the Social Sciences at the University of Chicago. His research interests include cost-effectiveness, technology assessment, and information research.
In 2010, his poster “Effects of Hospitalists on 1-Year Post-Discharge Resource Utilization by Medicare Beneficiaries” took the top prize in the HM10 research competition. In 2011, he was appointed to the methodology committee of the federal Patient-Centered Outcomes Research Institute (PCORI), which was created by the Affordable Care Act to advise the government on clinical-effectiveness research. He also sits on the Advisory Council to the National Institute of General Medical Sciences at the Institute of Medicine, and on the Congressional Budget Office’s panel of health advisors.
In a career full of recognition, Dr. Meltzer says it’s hard to pinpoint the impact of winning the poster contest. But he has continued to submit abstracts to SHM every year and appreciates the opportunities for interaction with peers at the poster exhibits.
Title: Director of perioperative and consultative medicine
Institution: University of Michigan, Ann Arbor
Year: 2006
RIV: “Disseminated Histoplasmosis Presenting As Painful Oral Ulcers” (clinical vignettes)
Dr. Grant’s winning vignette presented a patient with a complex medical history, including heart disease and four months of painful oral ulcers, for which prior evaluations had been inconclusive, despite conducting biopsies. Following administration of high-dose corticosteroids, the patient’s condition worsened on multiple fronts. The vignette showed how the medical team was able to diagnose an unusual presentation of a fungal infection called histoplasmosis, which is prevalent in parts of the Midwest surrounding the Ohio and Mississippi river valleys.
“We see a lot of cases in the hospital where there are different angles you could take to turn it into a clinical vignette or a nice poster with good teaching points,” Dr. Grant says. “In this case, just digging deeper into the actual diagnosis was important because the empiric use of steroids can be fatal for some patients. Steroids are given for a lot of good reasons, but in this patient they caused immune suppression, allowing a smoldering infection to become very active.”
Dr. Grant did not submit the vignette for publication. “That was probably a mistake on my part,” he says, acknowledging the common complaint of too little time and too many competing priorities. But his interest in research has continued.
“I became involved at a national level with issues of perioperative medicine and last August published a textbook on the subject,” he reports.1 “VTE is another area of interest I have developed since my hospital medicine fellowship.”
He serves as the VTE resource expert on the Michigan Hospital Medicine Safety Consortium, a quality collaborative of more than 40 hospitals with Blue Cross/Blue Shield of Michigan. “It’s exciting to be able to look at the risk factors, what kinds of patients get VTEs, and whether they were appropriately prophylaxed in the hospital,” he says.
VTE is a national quality priority, and Dr. Grant expects abstracts to emerge from the consortium’s work.
He says he appreciates the opportunities that arise from participating in poster sessions at SHM, where medical students, residents, and working hospitalists talk to the presenters of interesting cases.
“It gives you a real back-and-forth, which is good for the person asking the question and for the presenter,” he says, noting hospitalists from other parts of the country were not as familiar with histoplasmosis.
He says winning the HM06 poster contest helped him “get his feet wet” and feel more prepared for a career in academic hospital medicine. “I’m sure the award solidified my employers’ satisfaction in hiring me—and in giving me more desirable academic roles and responsibilities,” he adds.
Title: Assistant professor of medicine pediatrics; director of the general internal-medicine comprehensive consultation service
Institution: Johns Hopkins Hospital, Baltimore
Year: 2009
RIV: “An Internet-Based Consult Curriculum for Hospitalists” (innovations)
Dr. Feldman’s poster described an online CME curriculum for hospitalists acting as medical consultants. The concept grew out of a perceived deficiency in his own medical education when, in 2004, he was asked to lead the consultation service at Johns Hopkins—just six months after finishing his residency.
“I had no idea what I was doing as a general-internal-medicine consultant,” he says. “I maybe received two weeks of experience as a consultant during my residency. I was willing to take it on, learning on the job and asking for help. But it occurred to me that I’m probably not alone in feeling unprepared.”
In his quest for self-education, Dr. Feldman wondered whether he should write a textbook on the subject. “But the information changes so quickly, I thought I’d have a better chance to reach people online,” he notes.
After talking to publishers and CME companies, he came up with the concept of learning modules on perioperative and consultative medicine topics, which could be taken online while earning CME credits. Johns Hopkins served as the CME certifier, and medical-education company Advanced Studies in Medicine joined as a partner. Once the project got off the ground, a medical advisory committee was convened.
“Winning the SHM poster competition is a great honor to have on a CV. It really helps to legitimize your name in the world of hospital medicine,” Dr. Feldman says. “It also provided confirmation that we were on the right track with the curriculum project. People valued what we were doing.”
Dr. Feldman and SHM have since become affiliated, and the “Consultative and Perioperative Medicine Essentials for Hospitalists” modules are available on SHM’s website (www.shmconsults.com). The site has 12,000 registered members completing 500 CME modules every month.
“I do a lot of the editing still,” Dr. Feldman says. “We update the modules every two years and are still creating new ones.”
Dr. Feldman also pursues a number of clinical-research interests, including resident education and costs of care.
Title: Assistant professor of medicine
Institution: Medical University of South Carolina, Charleston
Year: 2009
RIV: “Intensivists versus Hospitalists in the ICU: A Prospective Cohort Study Comparing Mortality and Length of Stay Between Two Staffing Models” (research) Citation: Wise KR, Akopov VA, Williams BR, Ido MS, Leeper KV, Dressler DD. Hospitalists and intensivists in the medical ICU: a prospective and observational study comparing mortality and length of stay between two staffing models. J Hosp Med. 2012;7(3):183-189.
Dr. Wise was recognized for research that began while she worked at Emory University in Atlanta, comparing hospitalists and intensivists in such outcomes as length of stay and mortality rates for patients in the ICU. The study was one of the first statistically rigorous examinations of this critical quality question. With an eye toward improving patient safety, national quality advocates such as the Leapfrog Group have called for hospitals to employ intensivists (critical-care specialists) to manage the care of ICU patients. In reality, Dr. Wise says, there aren’t enough intensivists to meet the need.
“Hospitalists are in the ICU anyway,” she says. “We just don’t have enough data to answer how well they do [in comparison to intensivists].”
Through a prospective cohort study of more than 1,000 patients, Dr. Wise’s group found that there was essentially no statistical difference in mortality rates between patients treated by intensivist teams or hospitalist ICU teams.
“We were also able to look at some of the intermediate-acuity patients—fairly complicated but not requiring ventilators,” she explains. “Our study wasn’t sufficiently powered for this subgroup, but it was an interesting piece of data to raise the question: Where should we deploy this scarce resource of intensivists? Which pockets of patients?”
Presenting her abstract at SHM’s annual meeting was a “good experience.”
“I’d done public speaking before, but never with an audience of about 500 people,” she says. “To go out there and field their questions was a real professional growing experience. Several people interested in the topic sought me out at the conference, introduced themselves, and we have subsequently stayed in touch.”
The manuscript published in JHM has been cited four times, including in a position paper from SHM and the Society of Critical Care Medicine.3 Another outgrowth of the research was being asked to contribute a chapter on hospitalists’ role in the ICU to a textbook on hospital medicine. Based on her still-fresh HM presentation, Dr. Wise was one of the few publicly identified experts on the subject. The chapter, co-authored by fellow Emory hospitalist Michael Heisler, MD, MPH, “The Role of the Hospitalist in Critical Care” was included in Principles and Practices of Hospital Medicine.4
Title: Neonatal intensivist
Institution: Stony Brook University Hospital, Great Neck, N.Y.
Year: 2006
RIV: “Administration of Inactivated Trivalent Influenza Vaccine (TIV) to Parents of Infants in the Neonatal Intensive Care Unit (NICU): A Novel Strategy to Increase Vaccination Rates” (innovations)
Citation: Shah SI, Caprio M, Hendricks-Munoz K. Administration of inactivated trivalent influenza vaccine to parents of high-risk infants in the neonatal intensive care unit. Pediatrics. 2007;120;e617-e621.
Dr. Shah was in his final year of a fellowship in neonatology at New York University when he took on the challenge of improving immunization access to protect premature, highly vulnerable patients in the NICU from influenza infections. Because these children are too young to be vaccinated directly, the concept of cocooning them from infection involves extending protection to everyone around them.
“We came up with the idea of offering flu vaccinations 24/7 in the NICU to the children’s parents,” he says. “It worked well for us as a way to define an indicated therapy for a defined population, even if it was a little outside the box. By the end of the flu season, 95% of the parents were vaccinated.”
SHM recognized the project as the top RIV innovations poster at HM06, but that was just the beginning.
“When I moved to SUNY Stony Brook, I continued to study and advocate for these vaccinations,” Dr. Shah says. “We were giving 500 to 700 vaccinations a year. Then I wrote a national resolution for the American Academy of Pediatrics, which was significant because it meant AAP was behind the project.”
Dr. Shah later became chair of AAP’s Long Island Chapter Legislative Committee and joined a statewide pediatric advocacy group. In 2009, the New York legislature enacted the Neonatal Influenza Protection Act, which required hospitals in the state to offer parents the vaccine, with Dr. Shah’s research and advocacy providing an essential basis for its passage. He’s even been recognized for his research in congressional citations.
Based on that success with influenza vaccinations, Dr. Shah and his colleagues looked at other diseases, starting with pertussis, and then tetanus, diphtheria, and whooping cough.5 All the while, they continued tracking immunization rates. A second state law, passed in 2011, added pertussis to the vaccinations. Next on his advocacy agenda is a project to promote smoking-cessation interventions in the NICU.6
“These parents come to see us every day,” he says. “What can we do, through the parents, to promote the health and well-being of their high-risk newborns?”
Title: Assistant professor of medicine; medical director of inpatient palliative-care consultation
Institution: University of Texas Health Sciences Center, San Antonio
Year: 2009
RIV: “When to Depend on the Kinins of Strangers: An Unusual Case of Abdominal Pain” (clinical vignettes)
Publication: An article on the ethics of determining code status for patients with advanced cancer and a book chapter on the “last hours of life” for a forthcoming book on palliative care and hospital medicine.
As a medical resident, Dr. Morrow met a 27-year-old woman who had chronic abdominal pain and had made multiple visits to the ED for this complaint. The patient had a history of substance abuse and requested dilaudid for her pain—making it easy for staff to consign her to the stereotype of the difficult patient.
“I met her after an interesting finding,” he says. “It turns out that on the previous emergency room visit, she received a CAT scan, which showed duodenal and small-bowel thickening consistent with hereditary angioedema, although with an unusual presentation. As it happened, we had onsite a world expert in angioedema.”
The expert was able to confirm the diagnosis, Dr. Morrow says.
“By giving her this ‘legitimate,’ organic diagnosis, it just changed the whole dynamic of her relationship with her doctors,” he says. “She knew that they knew something was really wrong. The residents were empowered to have something to hang their hats on. And we were able to get better control of her pain.”
Dr. Morrow says he came on the scene late in the discovery process, but he helped to solve the puzzle, and then put together the abstract and poster that told the story of making the diagnosis.
“In my previous job, I was hired as a hospitalist but helped to build the palliative-care program within the hospital-medicine service,” he says. “In my current job, I was brought in to build the inpatient palliative-care-consultation service, although I still moonlight as a hospitalist to stay sharp.”
Dr. Morrow says he enjoys sharing stories of difficult cases and submitting case studies about them to medical conferences, often with clever titles incorporating puns (e.g. the 2009 SHM poster citing kinins, polypeptides in the blood that cause inflammation). Another example is “The Angina Monologues,” a story of an 82-year-old patient with chronic angina pectoris and complex pain syndromes that were difficult to bring under control. Palliative care also emphasizes patients’ stories, he says, in order to understand the person behind the diagnosis.
Larry Beresford is a freelance writer in San Francisco. References available at www.the-hospitalist.org.
References
2. Yoder J. Association between hospital noise levels and inpatient sleep among middle-aged and older adults: Far from a quiet night. Abstract, Society of Hospital Medicine, 2011.
3. McKean SC, Ross JJ, Dressler DD, Brotman DJ, Ginsberg JS. Principles and Practice of Hospital Medicine. McGraw-Hill Medical; New York City: 2012.
4. Siegal EM, Dressler DD, Dichter JR, Gorman MJ, Lipsett PA. Training a hospitalist workforce to address the intensivist shortage in American hospitals: a position paper from the Society of Hospital Medicine and the Society of Critical Care Medicine. J Hosp Med. 2012;7:359-364.
5. Dylag A, Shah SI. Administration of tetanus, diphtheria, and acellular pertussis vaccine to parents of high-risk infants in the neonatal intensive care unit. Pediatrics. 2008;122:e550-e555.
6. Shah S. Smoking cessation counseling and PPSV 23-valent pneumococcal polysaccharide vaccine administration parents of neonatal intensive care unit (NICU)-admitted infants: A life-changing opportunity. J Neonatal-Perinatal Med. 2011;4:263-267.
How Copper Could Solve Problem of Hospital-Acquired Infections

—James Pile, MD, FACP, SFHM, vice chair, department of hospital medicine, Cleveland Clinic
Hospital-acquired infections (HAIs) are on the rise despite efforts to decrease them. HAIs cause an estimated 100,000 deaths annually and account for up to $45 billion in health-care costs. Adding fuel to the fire, bacteria increasingly are becoming resistant to last-resort drugs. Despite this gloomy outlook, a recent study in Infection Control and Hospital Epidemiology shows that a material known for its antimicrobial properties for more than 4,000 years—copper—might be a light at the end of this darkening tunnel.1
Ancient Indians stored water in copper pots to prevent illness, says lead study author Cassandra D. Salgado, MD, associate professor of medicine, hospital epidemiologist, and medical director for infection prevention at the Medical University of South Carolina (MUSC) in Charleston. But copper rarely is used in that manner today because molded plastics and stainless steel are less expensive and easier to mass-produce.
Dr. Salgado explains that the antimicrobial effect of copper-alloy surfaces is a result of the metal stealing electrons from the bacteria when they come into contact with each other. “Once the bacteria donate the electrons to the copper metal, this places the organism into a state of electrical-charge deficit,” she says. “As a consequence, free radicals are generated inside the cell, which ultimately leads to the cell’s death.”
Copper-alloy surfaces kill 99.9% of bacteria in less than two hours, says Harold T. Michels, PhD, PE, senior vice president of technology and technical services for Copper Development Association Inc. in New York, who was a study author. On other surfaces, bacteria may live for multiple days or even months.
Unlike current methods used to decrease HAIs (i.e. hand-washing and sanitizing surfaces), copper components don’t require human intervention or compliance to be effective.
“It supplements what these other things can do; it’s in the background and it’s always working,” Michels says.

—Cassandra D. Salgado, MD, associate professor of medicine, hospital epidemiologist, medical director for infection prevention, Medical University of South Carolina, Charleston
Study Specifics
To conduct the study, copper prototypes of items touched most frequently by patients, health-care providers, and visitors were made and placed in patient rooms located within ICUs. “We placed the copper around the patient [much like a defensive perimeter] to reduce the likelihood that the health-care worker or visitor would introduce the infectious agent to the patient,” says the study’s lead investigator, Michael Schmidt, PhD, a professor and vice chair of MUSC’s department of microbiology and immunology.
Then, bacterial loads were measured on each object. For every study room, there was a control room without copper objects. Researchers were most interested in methicillin-resistant Staphylococcus aureus (MRSA) and vancomycin-resistant Enterococcus (VRE). For a period of time, bacterial burdens were measured in both copper rooms and control rooms.
Results exceeded the researchers’ expectations. Although only 7% of the touch surfaces in each ICU were replaced with copper components, there were 58% fewer HAI cases. The rate of HAI and/or MRSA or VRE colonization in ICU rooms with copper-alloy surfaces was significantly lower than that in standard ICU rooms (0.071 versus 0.123). For HAIs only, the rate was reduced to 0.034 from 0.081.3
“We were pleasantly surprised with the reductions,” Dr. Salgado says. “We consistently saw a more than 50% reduction in HAIs in all study sites.”
Archelle Georgiou, MD, president of Georgiou Consulting LLC in Minneapolis and an advisor to the Copper Development Association, is an advocate for making the health-care system simpler and safer for consumers. She says copper is a “game-changer.”
“It’s a brand-new way of thinking about decreasing the number of HAIs,” she says.
Green Light?
In light of the study’s encouraging findings, hospitalist and infectious-disease specialist James Pile, MD, FACP, SFHM, vice chair of the Department of Hospital Medicine at Cleveland Clinic, says that although study results appear valid, “it didn’t provide any final answers.”
“It would be premature for a hospital to install copper based on this study,” he says, adding he didn’t find the study results surprising, because copper is known to have antimicrobial properties.
But, Dr. Pile says, the study did provide proof of concept and opens the door for larger, more definitive studies that will show if installing copper in hospital rooms is worthwhile.
“If future studies confirm earlier results, then hospitals should seriously consider copper installations,” he says.
Barriers to Implementation
Despite the promising outlook for copper in dramatically reducing HAIs, implantation of copper components is off to a slow start.
Negotiations with the Environmental Protection Agency, the federal agency with jurisdiction over public-health claims for antimicrobial surfaces, started in 2004. Testing started in 2005. Although federal registration was completed in February 2008, it wasn’t until late 2011 that all regulatory issues were resolved for manufacturers.
“The regulatory process created delays in educating hospitals and the public about copper’s effectiveness in killing certain bacteria,” Dr. Georgiou explains. “As a result, American manufacturers with the ability to make copper components weren’t developing products because they couldn’t sell them.”
Now that the regulatory issues have been resolved, U.S. manufacturers are beginning to make copper components. The first wave of commercial products came on the market in late 2011. Meanwhile, European countries have not been delayed and are well ahead of U.S. hospitals in implementing copper components.
Presently, nine U.S. hospitals have installed some form of copper components, including door hardware, cabinet pulls, sinks, stretchers, and IV poles, Michels reports.
Despite these advances, hospitals may be slow to incorporate copper components due to a variety of reasons:
Cost. Dr. Pile believes that cost will be the major barrier. “Installing copper surfaces won’t be cheap,” he says. “But, then again, HAIs are very costly. I think it will be more difficult to justify their existence if they can be prevented. If copper is effective in preventing HAIs, it would prove to be cost-effective over time.”
Dr. Salgado concurs. “A study needs to be done on the cost-effectiveness of copper surfaces,” she says. “Health economists estimate that if copper surfaces were incorporated into ICUs, after three to six months, those surfaces would pay for themselves. That is not a long time period. Hospitals need to understand that there will be upfront costs but that they will realize benefits downstream.”
The Center for Medicare & Medicaid Services (CMS) has reported that one infection adds $43,000 in patient costs.4 A typical U.S. hospital room contains $100,000 worth of goods and equipment.
“When you do the math using the amount of copper in our study, the cost would be between $1 and $10 per patient,” Dr. Schmidt says. “It’s also important to note that an infection adds 19 days to a patient’s hospital stay.”
Aesthetics. For some, appearance may be a concern. “Copper is actually an appealing material that is offered in an array of colors and surface finishes,” Dr. Michels says. Because a copper-and-brass combination is more prone to tarnishing, a copper-nickel alloy may be more desirable.
Availability. Copper components are not produced and marketed to U.S. hospitals; however, they are available. “We are hoping with our study and future studies that some medical-device companies, as well as hospital-furniture manufacturers, will jump on board to look at ways to mass-produce items,” Dr. Salgado says.
Acceptance. The study published in Infection Control and Hospital Epidemiology validated the effectiveness of copper in decreasing HAIs. This pilot study, however, was not blinded.3
“It was pretty apparent to providers where copper surfaces were located, which tends to result in some bias. Future studies will, hopefully, try to answer questions regarding healthcare providers’ behaviors with different surfaces,” says Dr. Salgado, noting researchers in California and Chile also are studying the effects of copper surfaces in hospitals.
Possible loss of efficacy. Even if a surface is effective initially, Dr. Pile points out that it’s possible for that to change. “I have a theoretical concern that, over time, bacterial pathogens may develop a tolerance to copper,” he says. “Bacterial adversaries have been able to overcome any type of treatment that we have devised for them thus far. But this remains to be seen.”
This has been an issue with other surfaces; once microbes establish a foothold, it is hard to eliminate them. But Dr. Schmidt says because bacteria are killed so quickly on copper surfaces and cleaning is only required once daily, the ability to establish a foothold is greatly reduced, if not completely eliminated.

—Harold T. Michels, PhD, PE, senior vice president of technology and technical services, Copper Development Association Inc.
Champion Proven Strategies
Dr. Pile sees antimicrobial stewardship as a great opportunity for hospitalists as a specialty. In fact, the Centers for Disease Control and Prevention is partnering with HM groups on piloting multiple antimicrobial stewardship initiatives at several sites.
Dr. Pile suggests that leaders spearhead formal quality-improvement efforts, be involved with patient-safety efforts, and serve as physician champions.
“No one is better positioned to do this than hospitalists, because we own the hospital environment,” he says. “We have an incredible stake in making sure that our inpatient environment provides safe and high-value care.”
As a result of the published study, Dr. Salgado says discussions are underway with hospital leaders at MUSC to determine if copper surfaces will be used in its ICUs and, if so, how changes will be implemented.
Karen Appold is a freelance writer in Pennsylvania.
References
- Klevens RM, Edwards JR, Richards CL, et al. Estimating healthcare-associated infections and deaths in U.S. hospitals, 2002. Public Health Rep. 2007;122:160-166.
- Scott RD. The Direct Medical Costs of Healthcare-Associated Infections in U.S. Hospitals and the Benefits of Prevention. Atlanta: Centers for Disease Control and Prevention, 2009.
- Salgado CD, Sepkowitz KA, John JF, et al. Copper Surfaces Reduce the Rate of Healthcare-Acquired Infections in the Intensive Care Unit. Infect Control Hosp Epidemiol. 2013;34(5):479-486.
- Healthcare Cost and Utilization Project. Statistical Brief No. 94. Agency for Healthcare Research and Quality. Aug. 2010. Available at: http://www.hcup-us.ahrq.gov/reports/statbriefs/sb94.pdf. Accessed Aug. 6, 2013.

—James Pile, MD, FACP, SFHM, vice chair, department of hospital medicine, Cleveland Clinic
Hospital-acquired infections (HAIs) are on the rise despite efforts to decrease them. HAIs cause an estimated 100,000 deaths annually and account for up to $45 billion in health-care costs. Adding fuel to the fire, bacteria increasingly are becoming resistant to last-resort drugs. Despite this gloomy outlook, a recent study in Infection Control and Hospital Epidemiology shows that a material known for its antimicrobial properties for more than 4,000 years—copper—might be a light at the end of this darkening tunnel.1
Ancient Indians stored water in copper pots to prevent illness, says lead study author Cassandra D. Salgado, MD, associate professor of medicine, hospital epidemiologist, and medical director for infection prevention at the Medical University of South Carolina (MUSC) in Charleston. But copper rarely is used in that manner today because molded plastics and stainless steel are less expensive and easier to mass-produce.
Dr. Salgado explains that the antimicrobial effect of copper-alloy surfaces is a result of the metal stealing electrons from the bacteria when they come into contact with each other. “Once the bacteria donate the electrons to the copper metal, this places the organism into a state of electrical-charge deficit,” she says. “As a consequence, free radicals are generated inside the cell, which ultimately leads to the cell’s death.”
Copper-alloy surfaces kill 99.9% of bacteria in less than two hours, says Harold T. Michels, PhD, PE, senior vice president of technology and technical services for Copper Development Association Inc. in New York, who was a study author. On other surfaces, bacteria may live for multiple days or even months.
Unlike current methods used to decrease HAIs (i.e. hand-washing and sanitizing surfaces), copper components don’t require human intervention or compliance to be effective.
“It supplements what these other things can do; it’s in the background and it’s always working,” Michels says.

—Cassandra D. Salgado, MD, associate professor of medicine, hospital epidemiologist, medical director for infection prevention, Medical University of South Carolina, Charleston
Study Specifics
To conduct the study, copper prototypes of items touched most frequently by patients, health-care providers, and visitors were made and placed in patient rooms located within ICUs. “We placed the copper around the patient [much like a defensive perimeter] to reduce the likelihood that the health-care worker or visitor would introduce the infectious agent to the patient,” says the study’s lead investigator, Michael Schmidt, PhD, a professor and vice chair of MUSC’s department of microbiology and immunology.
Then, bacterial loads were measured on each object. For every study room, there was a control room without copper objects. Researchers were most interested in methicillin-resistant Staphylococcus aureus (MRSA) and vancomycin-resistant Enterococcus (VRE). For a period of time, bacterial burdens were measured in both copper rooms and control rooms.
Results exceeded the researchers’ expectations. Although only 7% of the touch surfaces in each ICU were replaced with copper components, there were 58% fewer HAI cases. The rate of HAI and/or MRSA or VRE colonization in ICU rooms with copper-alloy surfaces was significantly lower than that in standard ICU rooms (0.071 versus 0.123). For HAIs only, the rate was reduced to 0.034 from 0.081.3
“We were pleasantly surprised with the reductions,” Dr. Salgado says. “We consistently saw a more than 50% reduction in HAIs in all study sites.”
Archelle Georgiou, MD, president of Georgiou Consulting LLC in Minneapolis and an advisor to the Copper Development Association, is an advocate for making the health-care system simpler and safer for consumers. She says copper is a “game-changer.”
“It’s a brand-new way of thinking about decreasing the number of HAIs,” she says.
Green Light?
In light of the study’s encouraging findings, hospitalist and infectious-disease specialist James Pile, MD, FACP, SFHM, vice chair of the Department of Hospital Medicine at Cleveland Clinic, says that although study results appear valid, “it didn’t provide any final answers.”
“It would be premature for a hospital to install copper based on this study,” he says, adding he didn’t find the study results surprising, because copper is known to have antimicrobial properties.
But, Dr. Pile says, the study did provide proof of concept and opens the door for larger, more definitive studies that will show if installing copper in hospital rooms is worthwhile.
“If future studies confirm earlier results, then hospitals should seriously consider copper installations,” he says.
Barriers to Implementation
Despite the promising outlook for copper in dramatically reducing HAIs, implantation of copper components is off to a slow start.
Negotiations with the Environmental Protection Agency, the federal agency with jurisdiction over public-health claims for antimicrobial surfaces, started in 2004. Testing started in 2005. Although federal registration was completed in February 2008, it wasn’t until late 2011 that all regulatory issues were resolved for manufacturers.
“The regulatory process created delays in educating hospitals and the public about copper’s effectiveness in killing certain bacteria,” Dr. Georgiou explains. “As a result, American manufacturers with the ability to make copper components weren’t developing products because they couldn’t sell them.”
Now that the regulatory issues have been resolved, U.S. manufacturers are beginning to make copper components. The first wave of commercial products came on the market in late 2011. Meanwhile, European countries have not been delayed and are well ahead of U.S. hospitals in implementing copper components.
Presently, nine U.S. hospitals have installed some form of copper components, including door hardware, cabinet pulls, sinks, stretchers, and IV poles, Michels reports.
Despite these advances, hospitals may be slow to incorporate copper components due to a variety of reasons:
Cost. Dr. Pile believes that cost will be the major barrier. “Installing copper surfaces won’t be cheap,” he says. “But, then again, HAIs are very costly. I think it will be more difficult to justify their existence if they can be prevented. If copper is effective in preventing HAIs, it would prove to be cost-effective over time.”
Dr. Salgado concurs. “A study needs to be done on the cost-effectiveness of copper surfaces,” she says. “Health economists estimate that if copper surfaces were incorporated into ICUs, after three to six months, those surfaces would pay for themselves. That is not a long time period. Hospitals need to understand that there will be upfront costs but that they will realize benefits downstream.”
The Center for Medicare & Medicaid Services (CMS) has reported that one infection adds $43,000 in patient costs.4 A typical U.S. hospital room contains $100,000 worth of goods and equipment.
“When you do the math using the amount of copper in our study, the cost would be between $1 and $10 per patient,” Dr. Schmidt says. “It’s also important to note that an infection adds 19 days to a patient’s hospital stay.”
Aesthetics. For some, appearance may be a concern. “Copper is actually an appealing material that is offered in an array of colors and surface finishes,” Dr. Michels says. Because a copper-and-brass combination is more prone to tarnishing, a copper-nickel alloy may be more desirable.
Availability. Copper components are not produced and marketed to U.S. hospitals; however, they are available. “We are hoping with our study and future studies that some medical-device companies, as well as hospital-furniture manufacturers, will jump on board to look at ways to mass-produce items,” Dr. Salgado says.
Acceptance. The study published in Infection Control and Hospital Epidemiology validated the effectiveness of copper in decreasing HAIs. This pilot study, however, was not blinded.3
“It was pretty apparent to providers where copper surfaces were located, which tends to result in some bias. Future studies will, hopefully, try to answer questions regarding healthcare providers’ behaviors with different surfaces,” says Dr. Salgado, noting researchers in California and Chile also are studying the effects of copper surfaces in hospitals.
Possible loss of efficacy. Even if a surface is effective initially, Dr. Pile points out that it’s possible for that to change. “I have a theoretical concern that, over time, bacterial pathogens may develop a tolerance to copper,” he says. “Bacterial adversaries have been able to overcome any type of treatment that we have devised for them thus far. But this remains to be seen.”
This has been an issue with other surfaces; once microbes establish a foothold, it is hard to eliminate them. But Dr. Schmidt says because bacteria are killed so quickly on copper surfaces and cleaning is only required once daily, the ability to establish a foothold is greatly reduced, if not completely eliminated.

—Harold T. Michels, PhD, PE, senior vice president of technology and technical services, Copper Development Association Inc.
Champion Proven Strategies
Dr. Pile sees antimicrobial stewardship as a great opportunity for hospitalists as a specialty. In fact, the Centers for Disease Control and Prevention is partnering with HM groups on piloting multiple antimicrobial stewardship initiatives at several sites.
Dr. Pile suggests that leaders spearhead formal quality-improvement efforts, be involved with patient-safety efforts, and serve as physician champions.
“No one is better positioned to do this than hospitalists, because we own the hospital environment,” he says. “We have an incredible stake in making sure that our inpatient environment provides safe and high-value care.”
As a result of the published study, Dr. Salgado says discussions are underway with hospital leaders at MUSC to determine if copper surfaces will be used in its ICUs and, if so, how changes will be implemented.
Karen Appold is a freelance writer in Pennsylvania.
References
- Klevens RM, Edwards JR, Richards CL, et al. Estimating healthcare-associated infections and deaths in U.S. hospitals, 2002. Public Health Rep. 2007;122:160-166.
- Scott RD. The Direct Medical Costs of Healthcare-Associated Infections in U.S. Hospitals and the Benefits of Prevention. Atlanta: Centers for Disease Control and Prevention, 2009.
- Salgado CD, Sepkowitz KA, John JF, et al. Copper Surfaces Reduce the Rate of Healthcare-Acquired Infections in the Intensive Care Unit. Infect Control Hosp Epidemiol. 2013;34(5):479-486.
- Healthcare Cost and Utilization Project. Statistical Brief No. 94. Agency for Healthcare Research and Quality. Aug. 2010. Available at: http://www.hcup-us.ahrq.gov/reports/statbriefs/sb94.pdf. Accessed Aug. 6, 2013.

—James Pile, MD, FACP, SFHM, vice chair, department of hospital medicine, Cleveland Clinic
Hospital-acquired infections (HAIs) are on the rise despite efforts to decrease them. HAIs cause an estimated 100,000 deaths annually and account for up to $45 billion in health-care costs. Adding fuel to the fire, bacteria increasingly are becoming resistant to last-resort drugs. Despite this gloomy outlook, a recent study in Infection Control and Hospital Epidemiology shows that a material known for its antimicrobial properties for more than 4,000 years—copper—might be a light at the end of this darkening tunnel.1
Ancient Indians stored water in copper pots to prevent illness, says lead study author Cassandra D. Salgado, MD, associate professor of medicine, hospital epidemiologist, and medical director for infection prevention at the Medical University of South Carolina (MUSC) in Charleston. But copper rarely is used in that manner today because molded plastics and stainless steel are less expensive and easier to mass-produce.
Dr. Salgado explains that the antimicrobial effect of copper-alloy surfaces is a result of the metal stealing electrons from the bacteria when they come into contact with each other. “Once the bacteria donate the electrons to the copper metal, this places the organism into a state of electrical-charge deficit,” she says. “As a consequence, free radicals are generated inside the cell, which ultimately leads to the cell’s death.”
Copper-alloy surfaces kill 99.9% of bacteria in less than two hours, says Harold T. Michels, PhD, PE, senior vice president of technology and technical services for Copper Development Association Inc. in New York, who was a study author. On other surfaces, bacteria may live for multiple days or even months.
Unlike current methods used to decrease HAIs (i.e. hand-washing and sanitizing surfaces), copper components don’t require human intervention or compliance to be effective.
“It supplements what these other things can do; it’s in the background and it’s always working,” Michels says.

—Cassandra D. Salgado, MD, associate professor of medicine, hospital epidemiologist, medical director for infection prevention, Medical University of South Carolina, Charleston
Study Specifics
To conduct the study, copper prototypes of items touched most frequently by patients, health-care providers, and visitors were made and placed in patient rooms located within ICUs. “We placed the copper around the patient [much like a defensive perimeter] to reduce the likelihood that the health-care worker or visitor would introduce the infectious agent to the patient,” says the study’s lead investigator, Michael Schmidt, PhD, a professor and vice chair of MUSC’s department of microbiology and immunology.
Then, bacterial loads were measured on each object. For every study room, there was a control room without copper objects. Researchers were most interested in methicillin-resistant Staphylococcus aureus (MRSA) and vancomycin-resistant Enterococcus (VRE). For a period of time, bacterial burdens were measured in both copper rooms and control rooms.
Results exceeded the researchers’ expectations. Although only 7% of the touch surfaces in each ICU were replaced with copper components, there were 58% fewer HAI cases. The rate of HAI and/or MRSA or VRE colonization in ICU rooms with copper-alloy surfaces was significantly lower than that in standard ICU rooms (0.071 versus 0.123). For HAIs only, the rate was reduced to 0.034 from 0.081.3
“We were pleasantly surprised with the reductions,” Dr. Salgado says. “We consistently saw a more than 50% reduction in HAIs in all study sites.”
Archelle Georgiou, MD, president of Georgiou Consulting LLC in Minneapolis and an advisor to the Copper Development Association, is an advocate for making the health-care system simpler and safer for consumers. She says copper is a “game-changer.”
“It’s a brand-new way of thinking about decreasing the number of HAIs,” she says.
Green Light?
In light of the study’s encouraging findings, hospitalist and infectious-disease specialist James Pile, MD, FACP, SFHM, vice chair of the Department of Hospital Medicine at Cleveland Clinic, says that although study results appear valid, “it didn’t provide any final answers.”
“It would be premature for a hospital to install copper based on this study,” he says, adding he didn’t find the study results surprising, because copper is known to have antimicrobial properties.
But, Dr. Pile says, the study did provide proof of concept and opens the door for larger, more definitive studies that will show if installing copper in hospital rooms is worthwhile.
“If future studies confirm earlier results, then hospitals should seriously consider copper installations,” he says.
Barriers to Implementation
Despite the promising outlook for copper in dramatically reducing HAIs, implantation of copper components is off to a slow start.
Negotiations with the Environmental Protection Agency, the federal agency with jurisdiction over public-health claims for antimicrobial surfaces, started in 2004. Testing started in 2005. Although federal registration was completed in February 2008, it wasn’t until late 2011 that all regulatory issues were resolved for manufacturers.
“The regulatory process created delays in educating hospitals and the public about copper’s effectiveness in killing certain bacteria,” Dr. Georgiou explains. “As a result, American manufacturers with the ability to make copper components weren’t developing products because they couldn’t sell them.”
Now that the regulatory issues have been resolved, U.S. manufacturers are beginning to make copper components. The first wave of commercial products came on the market in late 2011. Meanwhile, European countries have not been delayed and are well ahead of U.S. hospitals in implementing copper components.
Presently, nine U.S. hospitals have installed some form of copper components, including door hardware, cabinet pulls, sinks, stretchers, and IV poles, Michels reports.
Despite these advances, hospitals may be slow to incorporate copper components due to a variety of reasons:
Cost. Dr. Pile believes that cost will be the major barrier. “Installing copper surfaces won’t be cheap,” he says. “But, then again, HAIs are very costly. I think it will be more difficult to justify their existence if they can be prevented. If copper is effective in preventing HAIs, it would prove to be cost-effective over time.”
Dr. Salgado concurs. “A study needs to be done on the cost-effectiveness of copper surfaces,” she says. “Health economists estimate that if copper surfaces were incorporated into ICUs, after three to six months, those surfaces would pay for themselves. That is not a long time period. Hospitals need to understand that there will be upfront costs but that they will realize benefits downstream.”
The Center for Medicare & Medicaid Services (CMS) has reported that one infection adds $43,000 in patient costs.4 A typical U.S. hospital room contains $100,000 worth of goods and equipment.
“When you do the math using the amount of copper in our study, the cost would be between $1 and $10 per patient,” Dr. Schmidt says. “It’s also important to note that an infection adds 19 days to a patient’s hospital stay.”
Aesthetics. For some, appearance may be a concern. “Copper is actually an appealing material that is offered in an array of colors and surface finishes,” Dr. Michels says. Because a copper-and-brass combination is more prone to tarnishing, a copper-nickel alloy may be more desirable.
Availability. Copper components are not produced and marketed to U.S. hospitals; however, they are available. “We are hoping with our study and future studies that some medical-device companies, as well as hospital-furniture manufacturers, will jump on board to look at ways to mass-produce items,” Dr. Salgado says.
Acceptance. The study published in Infection Control and Hospital Epidemiology validated the effectiveness of copper in decreasing HAIs. This pilot study, however, was not blinded.3
“It was pretty apparent to providers where copper surfaces were located, which tends to result in some bias. Future studies will, hopefully, try to answer questions regarding healthcare providers’ behaviors with different surfaces,” says Dr. Salgado, noting researchers in California and Chile also are studying the effects of copper surfaces in hospitals.
Possible loss of efficacy. Even if a surface is effective initially, Dr. Pile points out that it’s possible for that to change. “I have a theoretical concern that, over time, bacterial pathogens may develop a tolerance to copper,” he says. “Bacterial adversaries have been able to overcome any type of treatment that we have devised for them thus far. But this remains to be seen.”
This has been an issue with other surfaces; once microbes establish a foothold, it is hard to eliminate them. But Dr. Schmidt says because bacteria are killed so quickly on copper surfaces and cleaning is only required once daily, the ability to establish a foothold is greatly reduced, if not completely eliminated.

—Harold T. Michels, PhD, PE, senior vice president of technology and technical services, Copper Development Association Inc.
Champion Proven Strategies
Dr. Pile sees antimicrobial stewardship as a great opportunity for hospitalists as a specialty. In fact, the Centers for Disease Control and Prevention is partnering with HM groups on piloting multiple antimicrobial stewardship initiatives at several sites.
Dr. Pile suggests that leaders spearhead formal quality-improvement efforts, be involved with patient-safety efforts, and serve as physician champions.
“No one is better positioned to do this than hospitalists, because we own the hospital environment,” he says. “We have an incredible stake in making sure that our inpatient environment provides safe and high-value care.”
As a result of the published study, Dr. Salgado says discussions are underway with hospital leaders at MUSC to determine if copper surfaces will be used in its ICUs and, if so, how changes will be implemented.
Karen Appold is a freelance writer in Pennsylvania.
References
- Klevens RM, Edwards JR, Richards CL, et al. Estimating healthcare-associated infections and deaths in U.S. hospitals, 2002. Public Health Rep. 2007;122:160-166.
- Scott RD. The Direct Medical Costs of Healthcare-Associated Infections in U.S. Hospitals and the Benefits of Prevention. Atlanta: Centers for Disease Control and Prevention, 2009.
- Salgado CD, Sepkowitz KA, John JF, et al. Copper Surfaces Reduce the Rate of Healthcare-Acquired Infections in the Intensive Care Unit. Infect Control Hosp Epidemiol. 2013;34(5):479-486.
- Healthcare Cost and Utilization Project. Statistical Brief No. 94. Agency for Healthcare Research and Quality. Aug. 2010. Available at: http://www.hcup-us.ahrq.gov/reports/statbriefs/sb94.pdf. Accessed Aug. 6, 2013.
Listen to John Vazquez, MD, discuss neurophobia and tips for adjusting to discomfort in treating neuro patients
Click here to listen to more of our interview with Dr. Vazquez
Click here to listen to more of our interview with Dr. Vazquez
Click here to listen to more of our interview with Dr. Vazquez
Devastating Superstorm Gone, But Not Forgotten in Moore, Okla.

–Joe R. Womble, MD
The first bit of feedback was fantastic: Everyone who had been inside the hospital—roughly 200 to 300 people, including 30 patients—had survived.
“Everyone was fine,” he said. “All the patients and staff, no one got injured. I was thinking that either the hospital was missed by the storm or that it must not have really damaged it very significantly.”
Unfortunately, the hospital was not OK. He watched as local TV painted a very different picture.
“They started showing aerial shots and I was just shocked. My jaw was just dropped,” Dr. Womble said. “The main entrance that I go in every day was literally stacked with three or four cars deep. A huge stack of about 30 cars was piled up on the main entrance, essentially.”
It was as though they were “toy cars.”
The May 20 tornado, a two-mile-wide superstorm boasting 200-mph winds that struck just south of Oklahoma City, claimed 24 lives and left the regional health system with a void in its network. It also left hospitalists mourning the loss of the place they called a second home several times a week. About a week after the storm, officials announced that Moore Medical Center would have to be demolished.
Miraculous Moments
Despite the terrible events, hospitalists and hospital officials were astounded by the good fortune of the hospital’s inhabitants. Dr. Womble said about 100 people from nearby neighborhoods and businesses used the hospital as shelter.
Senthil Raju, MD, a hospitalist who had done rounds at Moore Medical earlier that day, said the protocol was to take shelter in the hallways. But at some point, probably only minutes before the storm hit, the chief nurse and the house supervisor made the decision to move all the patients to the ground floor because they were in “reasonably stable condition,” according to Dr. Womble, who relayed accounts by staffers who were there. Most of the people in the hospital rode out the storm in the first-floor cafeteria.
After the storm, patient rooms on the second floor were either no longer there or had been reduced to their steel innards.
The decision to move everyone undoubtedly saved lives. “If any of our patients stayed there, they’re probably all dead,” Dr. Raju said.
David Whitaker, CEO of Norman Regional Health System, which includes Moore Medical, marveled at the outcome.
“We had some bumps and bruises, some scratches, but no major lacerations, no broken bones, no injuries that people couldn’t ambulate. It’s totally amazing,” he said. “The leadership that was in place, the employees that were working at that time, they sprang into action, they took command and control of the situation. They got people into the proper areas.”
Dr. Womble said hospital staff at Moore Medical had still more amazing stories of death-defiance. They told him 30 people refused to leave the chapel. Somehow, the chapel remained intact, even though the hospital all around it was destroyed. Whitaker confirmed this.
One woman in active labor was kept in a second-floor operating room—which the medical staff thought was the best place for her, all things considered. Nurses covered the woman with pillows, blankets, and their own bodies as the tornado barreled through the town. She survived and gave birth to a boy several hours later. The parents gave him the middle name Emmanuel, which means “God is with us.”
As the tornado approached, an elderly volunteer had gone outside to get something from a van he used to transport elderly patients to and from a physical therapy program. “Nobody inside knew he had gone outside,” Dr. Womble said. By the time he tried to get back in, the power had gone out, and the doors wouldn’t open. He huddled behind a concrete pillar and ended up with just one minor laceration.
Patients eventually were taken to another hospital, Norman’s HealthPlex, about five miles south. Both Dr. Womble and Dr. Raju have begun working full time at the HealthPlex.
Dr. Raju said that he avoided being at Moore Medical during the tornado only by a turn of luck. He normally rounds at Moore in the afternoon and at the HealthPlex in the morning. But on that day, there were three new admissions at Moore, and only one at HealthPlex. So he went to Moore first, and was gone by the time the tornado hit.
“So lucky,” he said.

–David Whitaker, CEO of Norman Regional Health System
The Aftermath
It remains to be seen what kind of medical facility will be built to replace Moore Medical Center.
“Nobody knows what will happen next, but a lot of us speculate that they will not rebuild an inpatient facility,” said Dr. Womble, who had worked at Moore Medical Center for four years.
Whitaker said the first priority was to re-establish the clinics located at Moore Medical, and that has been done. The next step is, possibly, a temporary building in Moore for urgent care. The long-term plan remains in the discussion phase.
“We’ve already started having some meetings,” Whitaker said. “We’re going to determine what type of facility, what service levels it will be offering as we go back.”
It’s hard knowing that his hospital is no longer there, Dr. Raju said.
“We are going to miss it,” he said. “It’s unimaginable.”
Dr. Womble said those first few hours, when he wasn’t sure of where he’d be working, were difficult. He struggles to describe the feeling of not being able to provide care at his hospital at the time it’s most needed.
“It’s really hard to put it into words,” he said. “It’s the only hospital in that city, and it’s just me and my partner to take care of virtually everyone that comes in with any kind of medical problem. I definitely feel a tie to the community.
“It’s devastating. What is the rest of the city going to do for their hospital care? They essentially will not have a hospital in their city. They’ll have to drive to another city for care.”
Tom Collins is a freelance writer in South Florida.

–Joe R. Womble, MD
The first bit of feedback was fantastic: Everyone who had been inside the hospital—roughly 200 to 300 people, including 30 patients—had survived.
“Everyone was fine,” he said. “All the patients and staff, no one got injured. I was thinking that either the hospital was missed by the storm or that it must not have really damaged it very significantly.”
Unfortunately, the hospital was not OK. He watched as local TV painted a very different picture.
“They started showing aerial shots and I was just shocked. My jaw was just dropped,” Dr. Womble said. “The main entrance that I go in every day was literally stacked with three or four cars deep. A huge stack of about 30 cars was piled up on the main entrance, essentially.”
It was as though they were “toy cars.”
The May 20 tornado, a two-mile-wide superstorm boasting 200-mph winds that struck just south of Oklahoma City, claimed 24 lives and left the regional health system with a void in its network. It also left hospitalists mourning the loss of the place they called a second home several times a week. About a week after the storm, officials announced that Moore Medical Center would have to be demolished.
Miraculous Moments
Despite the terrible events, hospitalists and hospital officials were astounded by the good fortune of the hospital’s inhabitants. Dr. Womble said about 100 people from nearby neighborhoods and businesses used the hospital as shelter.
Senthil Raju, MD, a hospitalist who had done rounds at Moore Medical earlier that day, said the protocol was to take shelter in the hallways. But at some point, probably only minutes before the storm hit, the chief nurse and the house supervisor made the decision to move all the patients to the ground floor because they were in “reasonably stable condition,” according to Dr. Womble, who relayed accounts by staffers who were there. Most of the people in the hospital rode out the storm in the first-floor cafeteria.
After the storm, patient rooms on the second floor were either no longer there or had been reduced to their steel innards.
The decision to move everyone undoubtedly saved lives. “If any of our patients stayed there, they’re probably all dead,” Dr. Raju said.
David Whitaker, CEO of Norman Regional Health System, which includes Moore Medical, marveled at the outcome.
“We had some bumps and bruises, some scratches, but no major lacerations, no broken bones, no injuries that people couldn’t ambulate. It’s totally amazing,” he said. “The leadership that was in place, the employees that were working at that time, they sprang into action, they took command and control of the situation. They got people into the proper areas.”
Dr. Womble said hospital staff at Moore Medical had still more amazing stories of death-defiance. They told him 30 people refused to leave the chapel. Somehow, the chapel remained intact, even though the hospital all around it was destroyed. Whitaker confirmed this.
One woman in active labor was kept in a second-floor operating room—which the medical staff thought was the best place for her, all things considered. Nurses covered the woman with pillows, blankets, and their own bodies as the tornado barreled through the town. She survived and gave birth to a boy several hours later. The parents gave him the middle name Emmanuel, which means “God is with us.”
As the tornado approached, an elderly volunteer had gone outside to get something from a van he used to transport elderly patients to and from a physical therapy program. “Nobody inside knew he had gone outside,” Dr. Womble said. By the time he tried to get back in, the power had gone out, and the doors wouldn’t open. He huddled behind a concrete pillar and ended up with just one minor laceration.
Patients eventually were taken to another hospital, Norman’s HealthPlex, about five miles south. Both Dr. Womble and Dr. Raju have begun working full time at the HealthPlex.
Dr. Raju said that he avoided being at Moore Medical during the tornado only by a turn of luck. He normally rounds at Moore in the afternoon and at the HealthPlex in the morning. But on that day, there were three new admissions at Moore, and only one at HealthPlex. So he went to Moore first, and was gone by the time the tornado hit.
“So lucky,” he said.

–David Whitaker, CEO of Norman Regional Health System
The Aftermath
It remains to be seen what kind of medical facility will be built to replace Moore Medical Center.
“Nobody knows what will happen next, but a lot of us speculate that they will not rebuild an inpatient facility,” said Dr. Womble, who had worked at Moore Medical Center for four years.
Whitaker said the first priority was to re-establish the clinics located at Moore Medical, and that has been done. The next step is, possibly, a temporary building in Moore for urgent care. The long-term plan remains in the discussion phase.
“We’ve already started having some meetings,” Whitaker said. “We’re going to determine what type of facility, what service levels it will be offering as we go back.”
It’s hard knowing that his hospital is no longer there, Dr. Raju said.
“We are going to miss it,” he said. “It’s unimaginable.”
Dr. Womble said those first few hours, when he wasn’t sure of where he’d be working, were difficult. He struggles to describe the feeling of not being able to provide care at his hospital at the time it’s most needed.
“It’s really hard to put it into words,” he said. “It’s the only hospital in that city, and it’s just me and my partner to take care of virtually everyone that comes in with any kind of medical problem. I definitely feel a tie to the community.
“It’s devastating. What is the rest of the city going to do for their hospital care? They essentially will not have a hospital in their city. They’ll have to drive to another city for care.”
Tom Collins is a freelance writer in South Florida.

–Joe R. Womble, MD
The first bit of feedback was fantastic: Everyone who had been inside the hospital—roughly 200 to 300 people, including 30 patients—had survived.
“Everyone was fine,” he said. “All the patients and staff, no one got injured. I was thinking that either the hospital was missed by the storm or that it must not have really damaged it very significantly.”
Unfortunately, the hospital was not OK. He watched as local TV painted a very different picture.
“They started showing aerial shots and I was just shocked. My jaw was just dropped,” Dr. Womble said. “The main entrance that I go in every day was literally stacked with three or four cars deep. A huge stack of about 30 cars was piled up on the main entrance, essentially.”
It was as though they were “toy cars.”
The May 20 tornado, a two-mile-wide superstorm boasting 200-mph winds that struck just south of Oklahoma City, claimed 24 lives and left the regional health system with a void in its network. It also left hospitalists mourning the loss of the place they called a second home several times a week. About a week after the storm, officials announced that Moore Medical Center would have to be demolished.
Miraculous Moments
Despite the terrible events, hospitalists and hospital officials were astounded by the good fortune of the hospital’s inhabitants. Dr. Womble said about 100 people from nearby neighborhoods and businesses used the hospital as shelter.
Senthil Raju, MD, a hospitalist who had done rounds at Moore Medical earlier that day, said the protocol was to take shelter in the hallways. But at some point, probably only minutes before the storm hit, the chief nurse and the house supervisor made the decision to move all the patients to the ground floor because they were in “reasonably stable condition,” according to Dr. Womble, who relayed accounts by staffers who were there. Most of the people in the hospital rode out the storm in the first-floor cafeteria.
After the storm, patient rooms on the second floor were either no longer there or had been reduced to their steel innards.
The decision to move everyone undoubtedly saved lives. “If any of our patients stayed there, they’re probably all dead,” Dr. Raju said.
David Whitaker, CEO of Norman Regional Health System, which includes Moore Medical, marveled at the outcome.
“We had some bumps and bruises, some scratches, but no major lacerations, no broken bones, no injuries that people couldn’t ambulate. It’s totally amazing,” he said. “The leadership that was in place, the employees that were working at that time, they sprang into action, they took command and control of the situation. They got people into the proper areas.”
Dr. Womble said hospital staff at Moore Medical had still more amazing stories of death-defiance. They told him 30 people refused to leave the chapel. Somehow, the chapel remained intact, even though the hospital all around it was destroyed. Whitaker confirmed this.
One woman in active labor was kept in a second-floor operating room—which the medical staff thought was the best place for her, all things considered. Nurses covered the woman with pillows, blankets, and their own bodies as the tornado barreled through the town. She survived and gave birth to a boy several hours later. The parents gave him the middle name Emmanuel, which means “God is with us.”
As the tornado approached, an elderly volunteer had gone outside to get something from a van he used to transport elderly patients to and from a physical therapy program. “Nobody inside knew he had gone outside,” Dr. Womble said. By the time he tried to get back in, the power had gone out, and the doors wouldn’t open. He huddled behind a concrete pillar and ended up with just one minor laceration.
Patients eventually were taken to another hospital, Norman’s HealthPlex, about five miles south. Both Dr. Womble and Dr. Raju have begun working full time at the HealthPlex.
Dr. Raju said that he avoided being at Moore Medical during the tornado only by a turn of luck. He normally rounds at Moore in the afternoon and at the HealthPlex in the morning. But on that day, there were three new admissions at Moore, and only one at HealthPlex. So he went to Moore first, and was gone by the time the tornado hit.
“So lucky,” he said.

–David Whitaker, CEO of Norman Regional Health System
The Aftermath
It remains to be seen what kind of medical facility will be built to replace Moore Medical Center.
“Nobody knows what will happen next, but a lot of us speculate that they will not rebuild an inpatient facility,” said Dr. Womble, who had worked at Moore Medical Center for four years.
Whitaker said the first priority was to re-establish the clinics located at Moore Medical, and that has been done. The next step is, possibly, a temporary building in Moore for urgent care. The long-term plan remains in the discussion phase.
“We’ve already started having some meetings,” Whitaker said. “We’re going to determine what type of facility, what service levels it will be offering as we go back.”
It’s hard knowing that his hospital is no longer there, Dr. Raju said.
“We are going to miss it,” he said. “It’s unimaginable.”
Dr. Womble said those first few hours, when he wasn’t sure of where he’d be working, were difficult. He struggles to describe the feeling of not being able to provide care at his hospital at the time it’s most needed.
“It’s really hard to put it into words,” he said. “It’s the only hospital in that city, and it’s just me and my partner to take care of virtually everyone that comes in with any kind of medical problem. I definitely feel a tie to the community.
“It’s devastating. What is the rest of the city going to do for their hospital care? They essentially will not have a hospital in their city. They’ll have to drive to another city for care.”
Tom Collins is a freelance writer in South Florida.