User login
Short Title
The United States spends more on healthcare than any country in the world, and it is widely believed that the Nation could spend less while achieving comparable or better outcomes. The recent debate over healthcare reform in the United States, the large Federal budget deficit in the context of the current economic recession, and the prospect of widening gaps in Medicare funding with the increasing entry of baby boomers into old age suggest that the issue of healthcare cost will remain intense for many years to come. What roles hospitalists will play in the nation's struggle to control health care costs remain to be seen. Six papers in this issue of the Journal of Hospital Medicine discuss issues related to costs, and reflect several of the ways in which hospital medicine can contribute to understanding, and ultimately, controlling healthcare costs.
Two papers, one by Whelan et al.1 examining the costs associated with upper vs. lower GI bleeding and one by Lorch et al.2 examining the costs associated with herpex simplex virus (HSV) infections among neonates with and without congenital abnormalities, focus on epidemiologic determinants of healthcare costs. Such studies can identify subgroups of patients with high costs who may be logical targets for efforts to control costs. One tension in the use of such analyses to control cost is that total cost for any patient group is the product of both the cost per patient and the number of patients falling into each group. In the case of gastrointestinal (GI) bleeding, the surprise compared to past reports is that lower GI bleeding is about as common among hospitalized patients as upper GI bleeding. This may be because pharmacotherapy for conditions that cause upper GI bleeding is reducing the rate at which disease progresses to the point where hospitalization is required. The importance of prevalence is reinforced even in the findings about HSV infection, where despite 2‐ to 3‐fold higher average costs among babies with HSV who have congenital abnormalities, the fact that 90% of babies hospitalized with HSV lack congenital abnormalities implies that the clear majority of costs are due to babies without congenital abnormalities. In seeking strategies to control costs, it is important to pay attention to both the prevalence and cost per case of specific conditions. Because hospitalists are generalist physicians who typically care for few patients with any given diagnosis, the importance of prevalence implies that disease‐specific efforts to control costs may produce smaller total gains than those that cross diseases, such as efforts to improve communication between inpatient and outpatient physicians.
Moreover, the presence of high costs for some condition does not, of course, imply that effective interventions exist to reduce those costs. Two other papers, one by Mudge et al.3 examining a disease management program for heart failure, and one by Go et al.4 examining the effects of hospitalists on the costs of hospitalization for GI bleeding, reinforce the idea that interventions to reduce hospital costs are not always as effective as hoped. Even worse, efforts to control costs can have unintended effects, such as the delays in antimicrobial administration with antimicrobial approval policies that are reported by Winters et al.5 These studies also illustrate that analyses of the effectiveness of interventions can be performed using a variety of experimental designs (eg, the before/after comparison used by Mudge et al,3 and the natural experiments based on assignment of patients to physicians based on day of admission used by Go et al.4 or based on time of day used by Winters et al.)5 The role of hospitalists as clinical leaders in hospitals often places them in positions to design and execute experiments, but the role of hospitalists as astute clinicians who can recognize the presence of natural experiments in their clinical environment can be every bit as powerful in producing valid research designs.
As society seeks strategies to control healthcare costs in the years ahead, it will almost certainly turn to the same general strategies that have been used in the past: bundling services into fixed payments for a prospectively defined episode of care, asking patients to pay more of the costs of care, and simply not paying for, or paying less for, any given type of care. Hospitalists already have dealt with many of these approaches in one form or another. Medicare's prospective payment system and the payment of fixed annual fees for the care of patients in health maintenance organizations have given all hospitalists some exposure to the pressure for lower hospital resources use under prospective payment systems. Proposals for demonstration projects within healthcare reform to study the effects of bundling inpatient and outpatient care or even hospital and professional fees suggest that hospitalists may need to be open to new incentive structures in the years to come. For example, reduced incentives for rapid discharge if costs pushed into the outpatient setting are borne by the hospital, there may be co‐management models if professional and hospital fees are bundled. Increases in patient copayments may also play some role in healthcare reform, and the paper by Ross et al.6 should be a reminder to hospitalists that we may do our patients a great disservice if we fail to recognize the effects of our decisions on their out‐of‐pocket costs. Indeed, while doctors and patient both recognize the importance of discussing out‐of‐pocket costs, they both agree that these discussions rarely occur.7 That such discussions are not reimbursed explicitly suggests one of the many challenges of controlling healthcare costs; if physician payments are decreased to control costs and physicians respond by attempting to see even more patients in any given time period, discussions of important but less urgent issues such as out‐of‐pocket costs seem likely to be reduced. Such dilemmas arise frequently as the healthcare system devises increasingly complex approaches to the control of costs and suggest to many that fundamental reform of the payment and delivery system with greater reliance on integrated health systems paid through full capitation will eventually need to become the nation's approach to healthcare cost containment.8
- ,., et al.Upper versus lower gastrointestinal bleeding: a direct comparison of clinical presentation, outcomes, and resource utilization.J Hosp Med.2010;5(3):140–146.
- ,,.Impact of congenital anomalies and treatment location on clinical outcomes and health resource use in infants hospitalized with herpes simplex virus.J Hosp Med.2010;5(3):154–158.
- ,,, et al.The paradox of readmission: effect of a quality improvement programme in hospitalised patients with heart failure.J Hosp Med.2010;5:147–152.
- ,,, et al.Do hospitalists affect clinical outcomes and efficiency for patients with acute upper gastrointestinal hemorrhage (UGIH)?J Hosp Med.2010;5(3):138–138.
- ,,.Impact of a restrictive antimicrobial policy on the process and timing of antimicrobial administration.J Hosp Med.2010;5(2):E41–E45.
- ,.Reducing patient financial liability for hospitalizations: the physician role.J Hosp Med.2010;5(3):159–161.
- ,,.Patient‐physician communication about out‐of‐pocket costs.JAMA.2003;290(7):953–958.
- ,,, et al.Toward a 21st‐century health care system: recommendations for health care reform.Ann Intern Med.2009;150:493–495.
The United States spends more on healthcare than any country in the world, and it is widely believed that the Nation could spend less while achieving comparable or better outcomes. The recent debate over healthcare reform in the United States, the large Federal budget deficit in the context of the current economic recession, and the prospect of widening gaps in Medicare funding with the increasing entry of baby boomers into old age suggest that the issue of healthcare cost will remain intense for many years to come. What roles hospitalists will play in the nation's struggle to control health care costs remain to be seen. Six papers in this issue of the Journal of Hospital Medicine discuss issues related to costs, and reflect several of the ways in which hospital medicine can contribute to understanding, and ultimately, controlling healthcare costs.
Two papers, one by Whelan et al.1 examining the costs associated with upper vs. lower GI bleeding and one by Lorch et al.2 examining the costs associated with herpex simplex virus (HSV) infections among neonates with and without congenital abnormalities, focus on epidemiologic determinants of healthcare costs. Such studies can identify subgroups of patients with high costs who may be logical targets for efforts to control costs. One tension in the use of such analyses to control cost is that total cost for any patient group is the product of both the cost per patient and the number of patients falling into each group. In the case of gastrointestinal (GI) bleeding, the surprise compared to past reports is that lower GI bleeding is about as common among hospitalized patients as upper GI bleeding. This may be because pharmacotherapy for conditions that cause upper GI bleeding is reducing the rate at which disease progresses to the point where hospitalization is required. The importance of prevalence is reinforced even in the findings about HSV infection, where despite 2‐ to 3‐fold higher average costs among babies with HSV who have congenital abnormalities, the fact that 90% of babies hospitalized with HSV lack congenital abnormalities implies that the clear majority of costs are due to babies without congenital abnormalities. In seeking strategies to control costs, it is important to pay attention to both the prevalence and cost per case of specific conditions. Because hospitalists are generalist physicians who typically care for few patients with any given diagnosis, the importance of prevalence implies that disease‐specific efforts to control costs may produce smaller total gains than those that cross diseases, such as efforts to improve communication between inpatient and outpatient physicians.
Moreover, the presence of high costs for some condition does not, of course, imply that effective interventions exist to reduce those costs. Two other papers, one by Mudge et al.3 examining a disease management program for heart failure, and one by Go et al.4 examining the effects of hospitalists on the costs of hospitalization for GI bleeding, reinforce the idea that interventions to reduce hospital costs are not always as effective as hoped. Even worse, efforts to control costs can have unintended effects, such as the delays in antimicrobial administration with antimicrobial approval policies that are reported by Winters et al.5 These studies also illustrate that analyses of the effectiveness of interventions can be performed using a variety of experimental designs (eg, the before/after comparison used by Mudge et al,3 and the natural experiments based on assignment of patients to physicians based on day of admission used by Go et al.4 or based on time of day used by Winters et al.)5 The role of hospitalists as clinical leaders in hospitals often places them in positions to design and execute experiments, but the role of hospitalists as astute clinicians who can recognize the presence of natural experiments in their clinical environment can be every bit as powerful in producing valid research designs.
As society seeks strategies to control healthcare costs in the years ahead, it will almost certainly turn to the same general strategies that have been used in the past: bundling services into fixed payments for a prospectively defined episode of care, asking patients to pay more of the costs of care, and simply not paying for, or paying less for, any given type of care. Hospitalists already have dealt with many of these approaches in one form or another. Medicare's prospective payment system and the payment of fixed annual fees for the care of patients in health maintenance organizations have given all hospitalists some exposure to the pressure for lower hospital resources use under prospective payment systems. Proposals for demonstration projects within healthcare reform to study the effects of bundling inpatient and outpatient care or even hospital and professional fees suggest that hospitalists may need to be open to new incentive structures in the years to come. For example, reduced incentives for rapid discharge if costs pushed into the outpatient setting are borne by the hospital, there may be co‐management models if professional and hospital fees are bundled. Increases in patient copayments may also play some role in healthcare reform, and the paper by Ross et al.6 should be a reminder to hospitalists that we may do our patients a great disservice if we fail to recognize the effects of our decisions on their out‐of‐pocket costs. Indeed, while doctors and patient both recognize the importance of discussing out‐of‐pocket costs, they both agree that these discussions rarely occur.7 That such discussions are not reimbursed explicitly suggests one of the many challenges of controlling healthcare costs; if physician payments are decreased to control costs and physicians respond by attempting to see even more patients in any given time period, discussions of important but less urgent issues such as out‐of‐pocket costs seem likely to be reduced. Such dilemmas arise frequently as the healthcare system devises increasingly complex approaches to the control of costs and suggest to many that fundamental reform of the payment and delivery system with greater reliance on integrated health systems paid through full capitation will eventually need to become the nation's approach to healthcare cost containment.8
The United States spends more on healthcare than any country in the world, and it is widely believed that the Nation could spend less while achieving comparable or better outcomes. The recent debate over healthcare reform in the United States, the large Federal budget deficit in the context of the current economic recession, and the prospect of widening gaps in Medicare funding with the increasing entry of baby boomers into old age suggest that the issue of healthcare cost will remain intense for many years to come. What roles hospitalists will play in the nation's struggle to control health care costs remain to be seen. Six papers in this issue of the Journal of Hospital Medicine discuss issues related to costs, and reflect several of the ways in which hospital medicine can contribute to understanding, and ultimately, controlling healthcare costs.
Two papers, one by Whelan et al.1 examining the costs associated with upper vs. lower GI bleeding and one by Lorch et al.2 examining the costs associated with herpex simplex virus (HSV) infections among neonates with and without congenital abnormalities, focus on epidemiologic determinants of healthcare costs. Such studies can identify subgroups of patients with high costs who may be logical targets for efforts to control costs. One tension in the use of such analyses to control cost is that total cost for any patient group is the product of both the cost per patient and the number of patients falling into each group. In the case of gastrointestinal (GI) bleeding, the surprise compared to past reports is that lower GI bleeding is about as common among hospitalized patients as upper GI bleeding. This may be because pharmacotherapy for conditions that cause upper GI bleeding is reducing the rate at which disease progresses to the point where hospitalization is required. The importance of prevalence is reinforced even in the findings about HSV infection, where despite 2‐ to 3‐fold higher average costs among babies with HSV who have congenital abnormalities, the fact that 90% of babies hospitalized with HSV lack congenital abnormalities implies that the clear majority of costs are due to babies without congenital abnormalities. In seeking strategies to control costs, it is important to pay attention to both the prevalence and cost per case of specific conditions. Because hospitalists are generalist physicians who typically care for few patients with any given diagnosis, the importance of prevalence implies that disease‐specific efforts to control costs may produce smaller total gains than those that cross diseases, such as efforts to improve communication between inpatient and outpatient physicians.
Moreover, the presence of high costs for some condition does not, of course, imply that effective interventions exist to reduce those costs. Two other papers, one by Mudge et al.3 examining a disease management program for heart failure, and one by Go et al.4 examining the effects of hospitalists on the costs of hospitalization for GI bleeding, reinforce the idea that interventions to reduce hospital costs are not always as effective as hoped. Even worse, efforts to control costs can have unintended effects, such as the delays in antimicrobial administration with antimicrobial approval policies that are reported by Winters et al.5 These studies also illustrate that analyses of the effectiveness of interventions can be performed using a variety of experimental designs (eg, the before/after comparison used by Mudge et al,3 and the natural experiments based on assignment of patients to physicians based on day of admission used by Go et al.4 or based on time of day used by Winters et al.)5 The role of hospitalists as clinical leaders in hospitals often places them in positions to design and execute experiments, but the role of hospitalists as astute clinicians who can recognize the presence of natural experiments in their clinical environment can be every bit as powerful in producing valid research designs.
As society seeks strategies to control healthcare costs in the years ahead, it will almost certainly turn to the same general strategies that have been used in the past: bundling services into fixed payments for a prospectively defined episode of care, asking patients to pay more of the costs of care, and simply not paying for, or paying less for, any given type of care. Hospitalists already have dealt with many of these approaches in one form or another. Medicare's prospective payment system and the payment of fixed annual fees for the care of patients in health maintenance organizations have given all hospitalists some exposure to the pressure for lower hospital resources use under prospective payment systems. Proposals for demonstration projects within healthcare reform to study the effects of bundling inpatient and outpatient care or even hospital and professional fees suggest that hospitalists may need to be open to new incentive structures in the years to come. For example, reduced incentives for rapid discharge if costs pushed into the outpatient setting are borne by the hospital, there may be co‐management models if professional and hospital fees are bundled. Increases in patient copayments may also play some role in healthcare reform, and the paper by Ross et al.6 should be a reminder to hospitalists that we may do our patients a great disservice if we fail to recognize the effects of our decisions on their out‐of‐pocket costs. Indeed, while doctors and patient both recognize the importance of discussing out‐of‐pocket costs, they both agree that these discussions rarely occur.7 That such discussions are not reimbursed explicitly suggests one of the many challenges of controlling healthcare costs; if physician payments are decreased to control costs and physicians respond by attempting to see even more patients in any given time period, discussions of important but less urgent issues such as out‐of‐pocket costs seem likely to be reduced. Such dilemmas arise frequently as the healthcare system devises increasingly complex approaches to the control of costs and suggest to many that fundamental reform of the payment and delivery system with greater reliance on integrated health systems paid through full capitation will eventually need to become the nation's approach to healthcare cost containment.8
- ,., et al.Upper versus lower gastrointestinal bleeding: a direct comparison of clinical presentation, outcomes, and resource utilization.J Hosp Med.2010;5(3):140–146.
- ,,.Impact of congenital anomalies and treatment location on clinical outcomes and health resource use in infants hospitalized with herpes simplex virus.J Hosp Med.2010;5(3):154–158.
- ,,, et al.The paradox of readmission: effect of a quality improvement programme in hospitalised patients with heart failure.J Hosp Med.2010;5:147–152.
- ,,, et al.Do hospitalists affect clinical outcomes and efficiency for patients with acute upper gastrointestinal hemorrhage (UGIH)?J Hosp Med.2010;5(3):138–138.
- ,,.Impact of a restrictive antimicrobial policy on the process and timing of antimicrobial administration.J Hosp Med.2010;5(2):E41–E45.
- ,.Reducing patient financial liability for hospitalizations: the physician role.J Hosp Med.2010;5(3):159–161.
- ,,.Patient‐physician communication about out‐of‐pocket costs.JAMA.2003;290(7):953–958.
- ,,, et al.Toward a 21st‐century health care system: recommendations for health care reform.Ann Intern Med.2009;150:493–495.
- ,., et al.Upper versus lower gastrointestinal bleeding: a direct comparison of clinical presentation, outcomes, and resource utilization.J Hosp Med.2010;5(3):140–146.
- ,,.Impact of congenital anomalies and treatment location on clinical outcomes and health resource use in infants hospitalized with herpes simplex virus.J Hosp Med.2010;5(3):154–158.
- ,,, et al.The paradox of readmission: effect of a quality improvement programme in hospitalised patients with heart failure.J Hosp Med.2010;5:147–152.
- ,,, et al.Do hospitalists affect clinical outcomes and efficiency for patients with acute upper gastrointestinal hemorrhage (UGIH)?J Hosp Med.2010;5(3):138–138.
- ,,.Impact of a restrictive antimicrobial policy on the process and timing of antimicrobial administration.J Hosp Med.2010;5(2):E41–E45.
- ,.Reducing patient financial liability for hospitalizations: the physician role.J Hosp Med.2010;5(3):159–161.
- ,,.Patient‐physician communication about out‐of‐pocket costs.JAMA.2003;290(7):953–958.
- ,,, et al.Toward a 21st‐century health care system: recommendations for health care reform.Ann Intern Med.2009;150:493–495.
BEST PRACTICES IN: Treating Rosacea
A supplement to Skin & Allergy News. This supplement was supported by Galderma.
• Background
• Diagnosis and Differential Diagnosis
• Treating Rosacea
• Topical Therapy
• Oral Therapy
• Treatment Selection
• Summary
Faculty/Faculty Disclosure
Joseph F. Fowler, MD
Clinical Professor of Dermatology
University of Louisville
Dermatology Specialists PSC
Louisville, KY
Dr. Fowler has received clinical grants from and is a consultant to Galderma, Inc.
Copyright © 2009 Elsevier Inc.
A supplement to Skin & Allergy News. This supplement was supported by Galderma.
• Background
• Diagnosis and Differential Diagnosis
• Treating Rosacea
• Topical Therapy
• Oral Therapy
• Treatment Selection
• Summary
Faculty/Faculty Disclosure
Joseph F. Fowler, MD
Clinical Professor of Dermatology
University of Louisville
Dermatology Specialists PSC
Louisville, KY
Dr. Fowler has received clinical grants from and is a consultant to Galderma, Inc.
Copyright © 2009 Elsevier Inc.
A supplement to Skin & Allergy News. This supplement was supported by Galderma.
• Background
• Diagnosis and Differential Diagnosis
• Treating Rosacea
• Topical Therapy
• Oral Therapy
• Treatment Selection
• Summary
Faculty/Faculty Disclosure
Joseph F. Fowler, MD
Clinical Professor of Dermatology
University of Louisville
Dermatology Specialists PSC
Louisville, KY
Dr. Fowler has received clinical grants from and is a consultant to Galderma, Inc.
Copyright © 2009 Elsevier Inc.
Minimizing Topical Corticosteroid-Induced Cutaneous Side Effects
A Best Practices supplement to Skin & Allergy News and supported by Ranbaxy.
This supplement has been designed to meet the educational needs of Dermatologists and other Clinicians relative to the diagnosis and treatment of minimizing topical corticosteroid-induced cutaneous side effects.
Robert M. Lavker, PhD
Professor of Dermatology
and Director of
Dermatology Research
Department of Dermatology
Feinberg School of Medicine
Northwestern University
Chicago, Illinois
Mark Lebwohl, MD
Professor and Chairman
Department of Dermatology
The Mount Sinai School
of Medicine
New York, New York
Copyright © 2008 Elsevier Inc.
A Best Practices supplement to Skin & Allergy News and supported by Ranbaxy.
This supplement has been designed to meet the educational needs of Dermatologists and other Clinicians relative to the diagnosis and treatment of minimizing topical corticosteroid-induced cutaneous side effects.
Robert M. Lavker, PhD
Professor of Dermatology
and Director of
Dermatology Research
Department of Dermatology
Feinberg School of Medicine
Northwestern University
Chicago, Illinois
Mark Lebwohl, MD
Professor and Chairman
Department of Dermatology
The Mount Sinai School
of Medicine
New York, New York
Copyright © 2008 Elsevier Inc.
A Best Practices supplement to Skin & Allergy News and supported by Ranbaxy.
This supplement has been designed to meet the educational needs of Dermatologists and other Clinicians relative to the diagnosis and treatment of minimizing topical corticosteroid-induced cutaneous side effects.
Robert M. Lavker, PhD
Professor of Dermatology
and Director of
Dermatology Research
Department of Dermatology
Feinberg School of Medicine
Northwestern University
Chicago, Illinois
Mark Lebwohl, MD
Professor and Chairman
Department of Dermatology
The Mount Sinai School
of Medicine
New York, New York
Copyright © 2008 Elsevier Inc.
BEST PRACTICES IN:Treating Rosacea: Current Insights
Treating Rosacea: Current Insights
A supplement to Skin & Allergy News. This supplement was funded by Galderma.
Topics
• Is it Rosacea?
• Managing Rosacea: Target Potential Triggers
• Treatment Options for Rosacea
• Newer Topical Formulations
• Surgical Therapies
• Summary
Faculty/Faculty Disclosures
Richard Odom, MD
Chair
Professor, Clinical Dermatology
University of California
San Francisco School of Medicine
San Francisco, California
Advisory committee for Johnson & Johnson.
Terry Arnold, MA, PA-C
Advanced Practice Consultants, LLC
Tulsa, Oklahoma
Speaker for Medicis; advisory board of Novartis, Warner-Chilcott; advisory board/speaker for Abbott Laboratories, Astellas, Collagenex; advisory board, speaker and consultant for Amgen, Coria Labs, Ranbaxy.
Stephen Brunton, MD
Adjunct Clinical Professor
Department of Family Medicine
University of North Carolina
Chapel Hill
Chapel Hill, North Carolina
Nothing to disclose.
Mary Knudtson, DNSc, NP
Professor, Family Medicine
Director of Family Nurse Practitioner Program
University of California, Irvine
Irvine, California
Speaker's bureau for Proctor & Gamble; consultant for sanofi aventis, Galderma.
John E. Wolf, Jr., MD, MA
Professor and Chairman
Department of Dermatology
Baylor College of Medicine
Houston, Texas
Consultant, speaker, and on the advisory board for Stiefel, PharmaDerm, Galderma, Medicis, Novartis, Warner-Chilcott, consultant for QLT and Peplin; speaker for Stiefel, sanofi-aventis (Dermik).
Copyright © 2008 Elsevier Inc.
A supplement to Skin & Allergy News. This supplement was funded by Galderma.
Topics
• Is it Rosacea?
• Managing Rosacea: Target Potential Triggers
• Treatment Options for Rosacea
• Newer Topical Formulations
• Surgical Therapies
• Summary
Faculty/Faculty Disclosures
Richard Odom, MD
Chair
Professor, Clinical Dermatology
University of California
San Francisco School of Medicine
San Francisco, California
Advisory committee for Johnson & Johnson.
Terry Arnold, MA, PA-C
Advanced Practice Consultants, LLC
Tulsa, Oklahoma
Speaker for Medicis; advisory board of Novartis, Warner-Chilcott; advisory board/speaker for Abbott Laboratories, Astellas, Collagenex; advisory board, speaker and consultant for Amgen, Coria Labs, Ranbaxy.
Stephen Brunton, MD
Adjunct Clinical Professor
Department of Family Medicine
University of North Carolina
Chapel Hill
Chapel Hill, North Carolina
Nothing to disclose.
Mary Knudtson, DNSc, NP
Professor, Family Medicine
Director of Family Nurse Practitioner Program
University of California, Irvine
Irvine, California
Speaker's bureau for Proctor & Gamble; consultant for sanofi aventis, Galderma.
John E. Wolf, Jr., MD, MA
Professor and Chairman
Department of Dermatology
Baylor College of Medicine
Houston, Texas
Consultant, speaker, and on the advisory board for Stiefel, PharmaDerm, Galderma, Medicis, Novartis, Warner-Chilcott, consultant for QLT and Peplin; speaker for Stiefel, sanofi-aventis (Dermik).
Copyright © 2008 Elsevier Inc.
A supplement to Skin & Allergy News. This supplement was funded by Galderma.
Topics
• Is it Rosacea?
• Managing Rosacea: Target Potential Triggers
• Treatment Options for Rosacea
• Newer Topical Formulations
• Surgical Therapies
• Summary
Faculty/Faculty Disclosures
Richard Odom, MD
Chair
Professor, Clinical Dermatology
University of California
San Francisco School of Medicine
San Francisco, California
Advisory committee for Johnson & Johnson.
Terry Arnold, MA, PA-C
Advanced Practice Consultants, LLC
Tulsa, Oklahoma
Speaker for Medicis; advisory board of Novartis, Warner-Chilcott; advisory board/speaker for Abbott Laboratories, Astellas, Collagenex; advisory board, speaker and consultant for Amgen, Coria Labs, Ranbaxy.
Stephen Brunton, MD
Adjunct Clinical Professor
Department of Family Medicine
University of North Carolina
Chapel Hill
Chapel Hill, North Carolina
Nothing to disclose.
Mary Knudtson, DNSc, NP
Professor, Family Medicine
Director of Family Nurse Practitioner Program
University of California, Irvine
Irvine, California
Speaker's bureau for Proctor & Gamble; consultant for sanofi aventis, Galderma.
John E. Wolf, Jr., MD, MA
Professor and Chairman
Department of Dermatology
Baylor College of Medicine
Houston, Texas
Consultant, speaker, and on the advisory board for Stiefel, PharmaDerm, Galderma, Medicis, Novartis, Warner-Chilcott, consultant for QLT and Peplin; speaker for Stiefel, sanofi-aventis (Dermik).
Copyright © 2008 Elsevier Inc.
Treating Rosacea: Current Insights
Treating Rosacea: Current Insights
BEST PRACTICES IN: Newer Topical Retinoid Therapies for the Treatment of Acne
A supplement to Skin & Allergy News and funded by Galderma.
• Current Thinking Around Acne Therapy
• Topical Retinoids: The Cornerstone of Therapy
• Evolution of Topical Retinoids
• Tolerability of Topical Retinoids
• Summary
FACULTY
Lawrence F. Eichenfield, MD
Chief, Pediatric and Adolescent Dermatology
Professor of Pediatrics and Medicine (Dermatology)
Rady Children's Hospital, San Diego
University of California, San Diego School of Medicine
Diane M. Thiboutot, MD
Professor and Vice Chair of Dermatology Research
Co-Director, MD/PhD Program
Associate Program Director, GCRC
Penn State University College of Medicine
Hershey, Pennsylvania
Copyright © 2008 Elsevier Inc.
A supplement to Skin & Allergy News and funded by Galderma.
• Current Thinking Around Acne Therapy
• Topical Retinoids: The Cornerstone of Therapy
• Evolution of Topical Retinoids
• Tolerability of Topical Retinoids
• Summary
FACULTY
Lawrence F. Eichenfield, MD
Chief, Pediatric and Adolescent Dermatology
Professor of Pediatrics and Medicine (Dermatology)
Rady Children's Hospital, San Diego
University of California, San Diego School of Medicine
Diane M. Thiboutot, MD
Professor and Vice Chair of Dermatology Research
Co-Director, MD/PhD Program
Associate Program Director, GCRC
Penn State University College of Medicine
Hershey, Pennsylvania
Copyright © 2008 Elsevier Inc.
A supplement to Skin & Allergy News and funded by Galderma.
• Current Thinking Around Acne Therapy
• Topical Retinoids: The Cornerstone of Therapy
• Evolution of Topical Retinoids
• Tolerability of Topical Retinoids
• Summary
FACULTY
Lawrence F. Eichenfield, MD
Chief, Pediatric and Adolescent Dermatology
Professor of Pediatrics and Medicine (Dermatology)
Rady Children's Hospital, San Diego
University of California, San Diego School of Medicine
Diane M. Thiboutot, MD
Professor and Vice Chair of Dermatology Research
Co-Director, MD/PhD Program
Associate Program Director, GCRC
Penn State University College of Medicine
Hershey, Pennsylvania
Copyright © 2008 Elsevier Inc.
Emerging Treatment Options for Postinflammatory Hyperpigmentation
A supplement to Skin & Allergy News. This supplement is jointly sponsored by Skin & Allergy News and the Elsevier Office of Continuing Medical Education and supported by Barrier Therapeutics. The supplement is based on a faculty interview.


To view the supplement, click the image above. To take the CME Posttest, download and print out the CME Posttest PDF file, and follow the test instructions.
FACULTY
Susan Taylor, MD
Director, The Skin of Color Center
St. Luke's-Roosevelt Hospital
Columbia University
New York, N.Y.
TARGET AUDIENCE
This activity has been designed to meet the educational needs of Dermatologists and other clinicians.
EDUCATIONAL NEEDS
Disorders of skin pigmentation account for a substantial proportion of many dermatologists' practices. Abnormalities characterized by hyperpigmentation are especially prominent among African-Americans and other darker-skinned individuals. Postinflammatory hyperpigmentation (PIH), an acquired increase in pigmentation secondary to an inflammatory process, is one of the common pigmentation disorders among people of color. PIH poses a therapeutic challenge to the clinician, and many patients find the condition more troubling than its inflammatory precursor. PIH can have a devastating psychological impact and substantially mar an individual's self-esteem.
LEARNING OBJECTIVES
Upon completion of this educational activity, participants should be able to:
• Understand the basic pathophysiology of PIH
• State the principal types of conditions that result in PIH
• Appreciate the impact of PIH and its effects on people of color
• Appreciate the impact of PIH and its effects on people of color
ACCREDITATION STATEMENT
This activity has been planned and implemented in accordance with the Essential Areas and Policies of the Accreditation Council for Continuing Medical Education (ACCME) through the joint sponsorship of the Elsevier Office of ContinuingMedical Education (EOCME) and Skin & Allergy News. The EOCME is accredited by the ACCME to provide continuing medical education (CME) for physicians.
CREDIT DESIGNATION
The EOCME designates this educational activity for a maximum of 0.5 AMA PRA Category 1 Credits. Physicians should only claim credit commensurate with the extent of their participation in the activity.
Term of Approval: October 2007 - October 31, 2008.
*Full faculty disclosures available online.
A supplement to Skin & Allergy News. This supplement is jointly sponsored by Skin & Allergy News and the Elsevier Office of Continuing Medical Education and supported by Barrier Therapeutics. The supplement is based on a faculty interview.


To view the supplement, click the image above. To take the CME Posttest, download and print out the CME Posttest PDF file, and follow the test instructions.
FACULTY
Susan Taylor, MD
Director, The Skin of Color Center
St. Luke's-Roosevelt Hospital
Columbia University
New York, N.Y.
TARGET AUDIENCE
This activity has been designed to meet the educational needs of Dermatologists and other clinicians.
EDUCATIONAL NEEDS
Disorders of skin pigmentation account for a substantial proportion of many dermatologists' practices. Abnormalities characterized by hyperpigmentation are especially prominent among African-Americans and other darker-skinned individuals. Postinflammatory hyperpigmentation (PIH), an acquired increase in pigmentation secondary to an inflammatory process, is one of the common pigmentation disorders among people of color. PIH poses a therapeutic challenge to the clinician, and many patients find the condition more troubling than its inflammatory precursor. PIH can have a devastating psychological impact and substantially mar an individual's self-esteem.
LEARNING OBJECTIVES
Upon completion of this educational activity, participants should be able to:
• Understand the basic pathophysiology of PIH
• State the principal types of conditions that result in PIH
• Appreciate the impact of PIH and its effects on people of color
• Appreciate the impact of PIH and its effects on people of color
ACCREDITATION STATEMENT
This activity has been planned and implemented in accordance with the Essential Areas and Policies of the Accreditation Council for Continuing Medical Education (ACCME) through the joint sponsorship of the Elsevier Office of ContinuingMedical Education (EOCME) and Skin & Allergy News. The EOCME is accredited by the ACCME to provide continuing medical education (CME) for physicians.
CREDIT DESIGNATION
The EOCME designates this educational activity for a maximum of 0.5 AMA PRA Category 1 Credits. Physicians should only claim credit commensurate with the extent of their participation in the activity.
Term of Approval: October 2007 - October 31, 2008.
*Full faculty disclosures available online.
A supplement to Skin & Allergy News. This supplement is jointly sponsored by Skin & Allergy News and the Elsevier Office of Continuing Medical Education and supported by Barrier Therapeutics. The supplement is based on a faculty interview.


To view the supplement, click the image above. To take the CME Posttest, download and print out the CME Posttest PDF file, and follow the test instructions.
FACULTY
Susan Taylor, MD
Director, The Skin of Color Center
St. Luke's-Roosevelt Hospital
Columbia University
New York, N.Y.
TARGET AUDIENCE
This activity has been designed to meet the educational needs of Dermatologists and other clinicians.
EDUCATIONAL NEEDS
Disorders of skin pigmentation account for a substantial proportion of many dermatologists' practices. Abnormalities characterized by hyperpigmentation are especially prominent among African-Americans and other darker-skinned individuals. Postinflammatory hyperpigmentation (PIH), an acquired increase in pigmentation secondary to an inflammatory process, is one of the common pigmentation disorders among people of color. PIH poses a therapeutic challenge to the clinician, and many patients find the condition more troubling than its inflammatory precursor. PIH can have a devastating psychological impact and substantially mar an individual's self-esteem.
LEARNING OBJECTIVES
Upon completion of this educational activity, participants should be able to:
• Understand the basic pathophysiology of PIH
• State the principal types of conditions that result in PIH
• Appreciate the impact of PIH and its effects on people of color
• Appreciate the impact of PIH and its effects on people of color
ACCREDITATION STATEMENT
This activity has been planned and implemented in accordance with the Essential Areas and Policies of the Accreditation Council for Continuing Medical Education (ACCME) through the joint sponsorship of the Elsevier Office of ContinuingMedical Education (EOCME) and Skin & Allergy News. The EOCME is accredited by the ACCME to provide continuing medical education (CME) for physicians.
CREDIT DESIGNATION
The EOCME designates this educational activity for a maximum of 0.5 AMA PRA Category 1 Credits. Physicians should only claim credit commensurate with the extent of their participation in the activity.
Term of Approval: October 2007 - October 31, 2008.
*Full faculty disclosures available online.
Tort Reform Makes a Comeback
After being relegated to the back burner for months, tort reform has begun bubbling to the surface in editorials, polls, and at last month's televised healthcare summit. The focus has largely remained on how states can rein in unnecessary and expensive medical malpractice lawsuits. But a recent court case in Illinois, a new poll suggesting a high prevalence of "defensive medicine", and the glimmer of a bipartisan proposal for special "health courts" might provide the impetus for reform at the federal level.
According to the Agency for Healthcare Research and Quality (AHRQ), about half of the states have some form of medical liability caps on noneconomic damages or total damages, though the courts haven't always gone along with the limits. Last month, the Illinois Supreme Court ruled that the state's 2005 medical liability cap of $500,000 for doctors and $1 million for hospitals was unconstitutional. In a March 1 editorial, the AMA vowed to fight on, highlighting the positive experiences of tort reform in Texas.
As the "Public Policy" column in the March issue of The Hospitalist suggests, the liability caps approved by Texas voters in 2003 have led to decreases in liability insurance premiums and helped mitigate the state's physician shortage. But the jury is still out on whether the reforms have helped to improve quality and patient access.
Despite the reluctance of many Democrats to pursue liability caps, the concept of health courts has attracted some bipartisan support and the backing of President Obama. As proposed, such courts would consider only medical malpractice cases, similar to the workers' compensation system. A March 2 editorial in Roll Call by analysts at Washington, D.C., think tank Third Way asserts that health courts "can serve as the backbone for fundamental malpractice reform." Whether legislators will support a strong, single spine or more fragmented, state-based systems, however, remains to be seen.
After being relegated to the back burner for months, tort reform has begun bubbling to the surface in editorials, polls, and at last month's televised healthcare summit. The focus has largely remained on how states can rein in unnecessary and expensive medical malpractice lawsuits. But a recent court case in Illinois, a new poll suggesting a high prevalence of "defensive medicine", and the glimmer of a bipartisan proposal for special "health courts" might provide the impetus for reform at the federal level.
According to the Agency for Healthcare Research and Quality (AHRQ), about half of the states have some form of medical liability caps on noneconomic damages or total damages, though the courts haven't always gone along with the limits. Last month, the Illinois Supreme Court ruled that the state's 2005 medical liability cap of $500,000 for doctors and $1 million for hospitals was unconstitutional. In a March 1 editorial, the AMA vowed to fight on, highlighting the positive experiences of tort reform in Texas.
As the "Public Policy" column in the March issue of The Hospitalist suggests, the liability caps approved by Texas voters in 2003 have led to decreases in liability insurance premiums and helped mitigate the state's physician shortage. But the jury is still out on whether the reforms have helped to improve quality and patient access.
Despite the reluctance of many Democrats to pursue liability caps, the concept of health courts has attracted some bipartisan support and the backing of President Obama. As proposed, such courts would consider only medical malpractice cases, similar to the workers' compensation system. A March 2 editorial in Roll Call by analysts at Washington, D.C., think tank Third Way asserts that health courts "can serve as the backbone for fundamental malpractice reform." Whether legislators will support a strong, single spine or more fragmented, state-based systems, however, remains to be seen.
After being relegated to the back burner for months, tort reform has begun bubbling to the surface in editorials, polls, and at last month's televised healthcare summit. The focus has largely remained on how states can rein in unnecessary and expensive medical malpractice lawsuits. But a recent court case in Illinois, a new poll suggesting a high prevalence of "defensive medicine", and the glimmer of a bipartisan proposal for special "health courts" might provide the impetus for reform at the federal level.
According to the Agency for Healthcare Research and Quality (AHRQ), about half of the states have some form of medical liability caps on noneconomic damages or total damages, though the courts haven't always gone along with the limits. Last month, the Illinois Supreme Court ruled that the state's 2005 medical liability cap of $500,000 for doctors and $1 million for hospitals was unconstitutional. In a March 1 editorial, the AMA vowed to fight on, highlighting the positive experiences of tort reform in Texas.
As the "Public Policy" column in the March issue of The Hospitalist suggests, the liability caps approved by Texas voters in 2003 have led to decreases in liability insurance premiums and helped mitigate the state's physician shortage. But the jury is still out on whether the reforms have helped to improve quality and patient access.
Despite the reluctance of many Democrats to pursue liability caps, the concept of health courts has attracted some bipartisan support and the backing of President Obama. As proposed, such courts would consider only medical malpractice cases, similar to the workers' compensation system. A March 2 editorial in Roll Call by analysts at Washington, D.C., think tank Third Way asserts that health courts "can serve as the backbone for fundamental malpractice reform." Whether legislators will support a strong, single spine or more fragmented, state-based systems, however, remains to be seen.
In the Literature: The Latest Research You Need to Know
Clinical question: Does darbepoetin alfa use in patients with diabetes and chronic kidney disease (CKD) who do not require dialysis decrease the risk of death and cardiovascular or renal events?
Background: Anemia is a risk factor for cardiovascular and renal outcomes. The use of erythropoiesis-stimulating agents (ESAs) to increase hemoglobin reduces the need for transfusions and moderately improves quality of life. A placebo-controlled trial to determine if correction of anemia with ESAs improves clinical outcomes has not been conducted.
Study design: Randomized, double-blind, placebo-controlled trial.
Setting: 623 sites in 24 countries.
Synopsis: The study team randomized 4,038 patients to receive either dose-adjusted darbepoetin alfa (goal hemoglobin of 13) or placebo, with rescue doses of darbepoetin for hemoglobin below 9g/dL. The primary endpoints were a composite outcome of death, a cardiovascular event and death, or end-stage renal disease.
The median hemoglobin achieved in the darbepoetin and placebo groups were 12.5g/dL and 10.6g/dL, respectively. The primary cardiovascular endpoint occurred in 31.4% of patients receiving darbepoetin and 29.7% of patients receiving placebo (HR 1.05; 95% CI, 0.94-1.17). The primary renal endpoint occurred in 32.4% of patients assigned to darbepoetin and 30.5% of patients assigned to placebo (HR 1.06; 95% CI 0.95-1.19). Significantly more patients assigned to darbepoetin experienced stroke and VTE, and significantly fewer patients required red-cell transfusions.
Bottom line: Darbepoetin use in patients with diabetes and CKD who do not require dialysis for correction of anemia does not improve clinical outcomes, and carries an increased risk of stroke and VTE.
Citation: Pfeffer MA, Burdmann EA, Chen CY, et al. A trial of darbepoetin alfa in type 2 diabetes and chronic kidney disease. N Engl J Med. 2009;361(21):2019-2032.
Reviewed for TH eWire Charles Baillie, MD, Elizabeth Marandola, MSN, ARNP, Janelle Ocampo, PharmD, BCPS, Craig A. Umscheid, MD, MSCE, Section of Hospital Medicine, Hospital of the University of Pennsylvania, Philadelphia.
For more HM-related research reviews, visit the "In the Literature" section of our Web site.
Clinical question: Does darbepoetin alfa use in patients with diabetes and chronic kidney disease (CKD) who do not require dialysis decrease the risk of death and cardiovascular or renal events?
Background: Anemia is a risk factor for cardiovascular and renal outcomes. The use of erythropoiesis-stimulating agents (ESAs) to increase hemoglobin reduces the need for transfusions and moderately improves quality of life. A placebo-controlled trial to determine if correction of anemia with ESAs improves clinical outcomes has not been conducted.
Study design: Randomized, double-blind, placebo-controlled trial.
Setting: 623 sites in 24 countries.
Synopsis: The study team randomized 4,038 patients to receive either dose-adjusted darbepoetin alfa (goal hemoglobin of 13) or placebo, with rescue doses of darbepoetin for hemoglobin below 9g/dL. The primary endpoints were a composite outcome of death, a cardiovascular event and death, or end-stage renal disease.
The median hemoglobin achieved in the darbepoetin and placebo groups were 12.5g/dL and 10.6g/dL, respectively. The primary cardiovascular endpoint occurred in 31.4% of patients receiving darbepoetin and 29.7% of patients receiving placebo (HR 1.05; 95% CI, 0.94-1.17). The primary renal endpoint occurred in 32.4% of patients assigned to darbepoetin and 30.5% of patients assigned to placebo (HR 1.06; 95% CI 0.95-1.19). Significantly more patients assigned to darbepoetin experienced stroke and VTE, and significantly fewer patients required red-cell transfusions.
Bottom line: Darbepoetin use in patients with diabetes and CKD who do not require dialysis for correction of anemia does not improve clinical outcomes, and carries an increased risk of stroke and VTE.
Citation: Pfeffer MA, Burdmann EA, Chen CY, et al. A trial of darbepoetin alfa in type 2 diabetes and chronic kidney disease. N Engl J Med. 2009;361(21):2019-2032.
Reviewed for TH eWire Charles Baillie, MD, Elizabeth Marandola, MSN, ARNP, Janelle Ocampo, PharmD, BCPS, Craig A. Umscheid, MD, MSCE, Section of Hospital Medicine, Hospital of the University of Pennsylvania, Philadelphia.
For more HM-related research reviews, visit the "In the Literature" section of our Web site.
Clinical question: Does darbepoetin alfa use in patients with diabetes and chronic kidney disease (CKD) who do not require dialysis decrease the risk of death and cardiovascular or renal events?
Background: Anemia is a risk factor for cardiovascular and renal outcomes. The use of erythropoiesis-stimulating agents (ESAs) to increase hemoglobin reduces the need for transfusions and moderately improves quality of life. A placebo-controlled trial to determine if correction of anemia with ESAs improves clinical outcomes has not been conducted.
Study design: Randomized, double-blind, placebo-controlled trial.
Setting: 623 sites in 24 countries.
Synopsis: The study team randomized 4,038 patients to receive either dose-adjusted darbepoetin alfa (goal hemoglobin of 13) or placebo, with rescue doses of darbepoetin for hemoglobin below 9g/dL. The primary endpoints were a composite outcome of death, a cardiovascular event and death, or end-stage renal disease.
The median hemoglobin achieved in the darbepoetin and placebo groups were 12.5g/dL and 10.6g/dL, respectively. The primary cardiovascular endpoint occurred in 31.4% of patients receiving darbepoetin and 29.7% of patients receiving placebo (HR 1.05; 95% CI, 0.94-1.17). The primary renal endpoint occurred in 32.4% of patients assigned to darbepoetin and 30.5% of patients assigned to placebo (HR 1.06; 95% CI 0.95-1.19). Significantly more patients assigned to darbepoetin experienced stroke and VTE, and significantly fewer patients required red-cell transfusions.
Bottom line: Darbepoetin use in patients with diabetes and CKD who do not require dialysis for correction of anemia does not improve clinical outcomes, and carries an increased risk of stroke and VTE.
Citation: Pfeffer MA, Burdmann EA, Chen CY, et al. A trial of darbepoetin alfa in type 2 diabetes and chronic kidney disease. N Engl J Med. 2009;361(21):2019-2032.
Reviewed for TH eWire Charles Baillie, MD, Elizabeth Marandola, MSN, ARNP, Janelle Ocampo, PharmD, BCPS, Craig A. Umscheid, MD, MSCE, Section of Hospital Medicine, Hospital of the University of Pennsylvania, Philadelphia.
For more HM-related research reviews, visit the "In the Literature" section of our Web site.
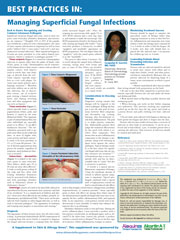
BEST PRACTICES IN: Managing Superficial Fungal Infections
A supplement to Skin & Allergy News. This supplement was sponsored by Ferndale Laboratories Inc. and Primus Pharmaceuticals, makers of Aloquin Gel and Alcortin A Gel.
- Back to Basics: Recognizing and Treating Common Cutaneous Pathogens
- Diagnosis
- Considerations in Choosing Therapy
- Maximizing Treatment Success
- Counseling Patients About Preventing Infection and Transmission
Faculty/Faculty Disclosure
Jacquelyn B. Garrett, MD, FAAD
Diplomate, American Board of Dermatology,
Dermatology private practice at Christian Hospital,
St. Louis, MO
Dr. Garrett has nothing to disclose.
Copyright (C) 2009 Elsevier Inc.
A supplement to Skin & Allergy News. This supplement was sponsored by Ferndale Laboratories Inc. and Primus Pharmaceuticals, makers of Aloquin Gel and Alcortin A Gel.
- Back to Basics: Recognizing and Treating Common Cutaneous Pathogens
- Diagnosis
- Considerations in Choosing Therapy
- Maximizing Treatment Success
- Counseling Patients About Preventing Infection and Transmission
Faculty/Faculty Disclosure
Jacquelyn B. Garrett, MD, FAAD
Diplomate, American Board of Dermatology,
Dermatology private practice at Christian Hospital,
St. Louis, MO
Dr. Garrett has nothing to disclose.
Copyright (C) 2009 Elsevier Inc.
A supplement to Skin & Allergy News. This supplement was sponsored by Ferndale Laboratories Inc. and Primus Pharmaceuticals, makers of Aloquin Gel and Alcortin A Gel.
- Back to Basics: Recognizing and Treating Common Cutaneous Pathogens
- Diagnosis
- Considerations in Choosing Therapy
- Maximizing Treatment Success
- Counseling Patients About Preventing Infection and Transmission
Faculty/Faculty Disclosure
Jacquelyn B. Garrett, MD, FAAD
Diplomate, American Board of Dermatology,
Dermatology private practice at Christian Hospital,
St. Louis, MO
Dr. Garrett has nothing to disclose.
Copyright (C) 2009 Elsevier Inc.
Wired to Lead
With prods from technological advancement and political pressure, the use of digital medicine is expected to take another leap forward this year—and hospitalists can be among those who benefit most, according to a presentation at an American College of Physicians meeting last month.
The workshop, "Wired and Wireless Health," held as part of the New Jersey Chapter regional meeting in Woodbridge, N.J., focused on three areas of health information technology (IT): social networking, applications and devices, and infrastructure. Steven Peskin, MD, MBA, FACP, says social networking Web sites like Sermo and Medscape Physician Connect offer portals for the "sharing of clinical insights and solutions to practical clinical problems in a way that promises to hone best practices."
As executive vice president and chief medical officer of Yardley, Pa.-based MediMedia USA, Dr. Peskin preaches the value of digital technology for inpatient care. Hospitalists, in particular, can use handheld devices and applications to deliver faster care and receive test results more quickly.
“There’s an app for that,” he quips, noting Modality and MedCalc. SHM is nearing launch of its new mobile resource center, which is supported by Epocrates and offers hospitalists exclusive commentary on the latest news and research in HM and hospitalist practice management.
Dr. Peskin, while an ardent supporter of the use of digital technology to improve patient care, is quick to caution that technology has its place. Privacy concerns, which are often associated with electronic health records (EHR), are a major consideration physicians should keep in mind when incorporating advances in iPhones, BlackBerrys, or other smartphones, he says.
"Digital medicine is not a substitute for clinical experience," Dr. Peskin says. "But it can improve clinical judgment and better clinical judgment. I like to say, 'Use computers for what they do well and use your brain for what it does well.'"
With prods from technological advancement and political pressure, the use of digital medicine is expected to take another leap forward this year—and hospitalists can be among those who benefit most, according to a presentation at an American College of Physicians meeting last month.
The workshop, "Wired and Wireless Health," held as part of the New Jersey Chapter regional meeting in Woodbridge, N.J., focused on three areas of health information technology (IT): social networking, applications and devices, and infrastructure. Steven Peskin, MD, MBA, FACP, says social networking Web sites like Sermo and Medscape Physician Connect offer portals for the "sharing of clinical insights and solutions to practical clinical problems in a way that promises to hone best practices."
As executive vice president and chief medical officer of Yardley, Pa.-based MediMedia USA, Dr. Peskin preaches the value of digital technology for inpatient care. Hospitalists, in particular, can use handheld devices and applications to deliver faster care and receive test results more quickly.
“There’s an app for that,” he quips, noting Modality and MedCalc. SHM is nearing launch of its new mobile resource center, which is supported by Epocrates and offers hospitalists exclusive commentary on the latest news and research in HM and hospitalist practice management.
Dr. Peskin, while an ardent supporter of the use of digital technology to improve patient care, is quick to caution that technology has its place. Privacy concerns, which are often associated with electronic health records (EHR), are a major consideration physicians should keep in mind when incorporating advances in iPhones, BlackBerrys, or other smartphones, he says.
"Digital medicine is not a substitute for clinical experience," Dr. Peskin says. "But it can improve clinical judgment and better clinical judgment. I like to say, 'Use computers for what they do well and use your brain for what it does well.'"
With prods from technological advancement and political pressure, the use of digital medicine is expected to take another leap forward this year—and hospitalists can be among those who benefit most, according to a presentation at an American College of Physicians meeting last month.
The workshop, "Wired and Wireless Health," held as part of the New Jersey Chapter regional meeting in Woodbridge, N.J., focused on three areas of health information technology (IT): social networking, applications and devices, and infrastructure. Steven Peskin, MD, MBA, FACP, says social networking Web sites like Sermo and Medscape Physician Connect offer portals for the "sharing of clinical insights and solutions to practical clinical problems in a way that promises to hone best practices."
As executive vice president and chief medical officer of Yardley, Pa.-based MediMedia USA, Dr. Peskin preaches the value of digital technology for inpatient care. Hospitalists, in particular, can use handheld devices and applications to deliver faster care and receive test results more quickly.
“There’s an app for that,” he quips, noting Modality and MedCalc. SHM is nearing launch of its new mobile resource center, which is supported by Epocrates and offers hospitalists exclusive commentary on the latest news and research in HM and hospitalist practice management.
Dr. Peskin, while an ardent supporter of the use of digital technology to improve patient care, is quick to caution that technology has its place. Privacy concerns, which are often associated with electronic health records (EHR), are a major consideration physicians should keep in mind when incorporating advances in iPhones, BlackBerrys, or other smartphones, he says.
"Digital medicine is not a substitute for clinical experience," Dr. Peskin says. "But it can improve clinical judgment and better clinical judgment. I like to say, 'Use computers for what they do well and use your brain for what it does well.'"