User login
Drug dubbed ‘breakthrough’ for AL amyloidosis
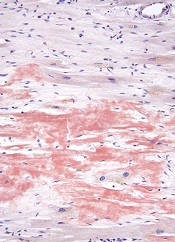
The US Food and Drug Administration (FDA) has granted breakthrough therapy designation for the oral proteasome inhibitor ixazomib (MLN9708) to treat relapsed or refractory systemic light-chain (AL) amyloidosis.
This is the first proteasome inhibitor and the first investigational therapy for AL amyloidosis to receive breakthrough designation.
Ixazomib already has orphan drug designation in the US and the European Union for this indication and to treat multiple myeloma (MM).
The FDA’s breakthrough therapy designation is intended to expedite the development and review of new medicines to treat serious or life-threatening conditions. Compounds given the designation receive more intensive FDA guidance on an efficient drug development program and an enhanced agency commitment of senior personnel.
Breakthrough therapy designation requires preliminary clinical evidence indicating the drug may demonstrate substantial improvement on a clinically significant endpoint (or endpoints) over available therapies.
The data used to support this designation for ixazomib came from a phase 1 trial that is set to be presented at the 2014 ASH Annual Meeting as abstract 3450.
The development program for ixazomib in AL amyloidosis progressed directly from a phase 1 to a phase 3 clinical trial, TOURMALINE-AL1. Ixazomib is the first oral proteasome inhibitor to enter phase 3 clinical trials, and 4 global phase 3 trials are ongoing:
- TOURMALINE-MM1, an investigation of ixazomib vs placebo in combination with lenalidomide and dexamethasone in relapsed and/or refractory MM
- TOURMALINE-AL1, an investigation of ixazomib plus dexamethasone in patients with relapsed or refractory AL amyloidosis
- TOURMALINE-MM2, an investigation of ixazomib vs placebo in combination with lenalidomide and dexamethasone in patients with newly diagnosed MM
- TOURMALINE-MM3, an investigation of ixazomib vs placebo as maintenance therapy in patients with newly diagnosed MM following induction therapy and autologous stem cell transplant.
For additional information on the ongoing phase 3 studies, visit www.tourmalinetrials.com or www.clinicaltrials.gov. Ixazomib is under development by Millennium: the Takeda Oncology Company. ![]()

The US Food and Drug Administration (FDA) has granted breakthrough therapy designation for the oral proteasome inhibitor ixazomib (MLN9708) to treat relapsed or refractory systemic light-chain (AL) amyloidosis.
This is the first proteasome inhibitor and the first investigational therapy for AL amyloidosis to receive breakthrough designation.
Ixazomib already has orphan drug designation in the US and the European Union for this indication and to treat multiple myeloma (MM).
The FDA’s breakthrough therapy designation is intended to expedite the development and review of new medicines to treat serious or life-threatening conditions. Compounds given the designation receive more intensive FDA guidance on an efficient drug development program and an enhanced agency commitment of senior personnel.
Breakthrough therapy designation requires preliminary clinical evidence indicating the drug may demonstrate substantial improvement on a clinically significant endpoint (or endpoints) over available therapies.
The data used to support this designation for ixazomib came from a phase 1 trial that is set to be presented at the 2014 ASH Annual Meeting as abstract 3450.
The development program for ixazomib in AL amyloidosis progressed directly from a phase 1 to a phase 3 clinical trial, TOURMALINE-AL1. Ixazomib is the first oral proteasome inhibitor to enter phase 3 clinical trials, and 4 global phase 3 trials are ongoing:
- TOURMALINE-MM1, an investigation of ixazomib vs placebo in combination with lenalidomide and dexamethasone in relapsed and/or refractory MM
- TOURMALINE-AL1, an investigation of ixazomib plus dexamethasone in patients with relapsed or refractory AL amyloidosis
- TOURMALINE-MM2, an investigation of ixazomib vs placebo in combination with lenalidomide and dexamethasone in patients with newly diagnosed MM
- TOURMALINE-MM3, an investigation of ixazomib vs placebo as maintenance therapy in patients with newly diagnosed MM following induction therapy and autologous stem cell transplant.
For additional information on the ongoing phase 3 studies, visit www.tourmalinetrials.com or www.clinicaltrials.gov. Ixazomib is under development by Millennium: the Takeda Oncology Company. ![]()

The US Food and Drug Administration (FDA) has granted breakthrough therapy designation for the oral proteasome inhibitor ixazomib (MLN9708) to treat relapsed or refractory systemic light-chain (AL) amyloidosis.
This is the first proteasome inhibitor and the first investigational therapy for AL amyloidosis to receive breakthrough designation.
Ixazomib already has orphan drug designation in the US and the European Union for this indication and to treat multiple myeloma (MM).
The FDA’s breakthrough therapy designation is intended to expedite the development and review of new medicines to treat serious or life-threatening conditions. Compounds given the designation receive more intensive FDA guidance on an efficient drug development program and an enhanced agency commitment of senior personnel.
Breakthrough therapy designation requires preliminary clinical evidence indicating the drug may demonstrate substantial improvement on a clinically significant endpoint (or endpoints) over available therapies.
The data used to support this designation for ixazomib came from a phase 1 trial that is set to be presented at the 2014 ASH Annual Meeting as abstract 3450.
The development program for ixazomib in AL amyloidosis progressed directly from a phase 1 to a phase 3 clinical trial, TOURMALINE-AL1. Ixazomib is the first oral proteasome inhibitor to enter phase 3 clinical trials, and 4 global phase 3 trials are ongoing:
- TOURMALINE-MM1, an investigation of ixazomib vs placebo in combination with lenalidomide and dexamethasone in relapsed and/or refractory MM
- TOURMALINE-AL1, an investigation of ixazomib plus dexamethasone in patients with relapsed or refractory AL amyloidosis
- TOURMALINE-MM2, an investigation of ixazomib vs placebo in combination with lenalidomide and dexamethasone in patients with newly diagnosed MM
- TOURMALINE-MM3, an investigation of ixazomib vs placebo as maintenance therapy in patients with newly diagnosed MM following induction therapy and autologous stem cell transplant.
For additional information on the ongoing phase 3 studies, visit www.tourmalinetrials.com or www.clinicaltrials.gov. Ixazomib is under development by Millennium: the Takeda Oncology Company. ![]()
NICE expands use of ESAs in cancer patients

chemotherapy
Credit: Rhoda Baer
The UK’s National Institute for Health and Care Excellence (NICE) has updated its guidance to expand the use of erythropoiesis-stimulating agents (ESAs) in cancer patients.
In 2008, NICE issued a guidance recommending ESAs as a possible treatment for certain patients with anemia caused by cancer treatment.
Now, NICE has updated the recommendations to expand the use of ESAs—epoetin alfa, beta, theta, and zeta, as well as darbepoetin alfa—to all other indications within their UK marketing authorizations.
“A lot of people with cancer having chemotherapy will become anemic,” noted Carole Longson, director of the Centre for Health Technology Evaluation at NICE.
“Managing anemia often requires extra trips to the hospital and can significantly affect a person’s quality of life. This updated final guidance recommends more options, epoetin and darbepoetin, that are both clinically and cost-effective and which also significantly improve quality of life for people who develop anemia whilst having cancer therapy.”
The 2008 NICE guidance recommended erythropoietin analogues with iron injections as a possible treatment for anemia caused by cancer treatment only in:
- Women receiving platinum-based chemotherapy for cancer of the ovaries who have a blood hemoglobin level of 8 g/100 mL or lower
- Patients who have very severe anemia and cannot receive blood transfusions.
NICE’s updated final guidance recommends using darbepoetin alfa and epoetin alfa, beta, theta, and zeta within their marketing authorizations as an option for treating anemia in cancer patients undergoing chemotherapy.
Epoetin alfa (Eprex, Janssen-Cilag, and Binocrit, Sandoz), and epoetin zeta (Retacrit, Hospira UK) have UK marketing authorization to treat anemia and to reduce transfusion requirements in adult patients receiving chemotherapy for solid tumors, malignant lymphoma, or multiple myeloma, who are at risk of transfusion as assessed by the patients’ general status (eg, cardiovascular status, pre-existing anemia at the start of chemotherapy).
Binocrit and Retacrit are both biosimilar medicines referenced to Eprex. Eprex, Binocrit, and Retacrit are available in pre-filled syringes at net prices of £5.53, £4.33, and £5.66 per 1000 units, respectively.
Epoetin beta (NeoRecormon, Roche Products) and epoetin theta (Eporatio, Teva UK) have UK marketing authorization to treat symptomatic anemia in adult patients with non-myeloid malignancies who are receiving chemotherapy.
NeoRecormon is available in a pre-filled syringe at a net price of £3.51 per 500 units, and Eporatio is available in a pre-filled syringe at a net price of £5.99 per 1000 units.
Darbepoetin alfa (Aranesp, Amgen) has UK marketing authorization to treat symptomatic anemia in adult cancer patients with non-myeloid malignancies who are receiving chemotherapy. Aranesp is available in a pre-filled syringe at a net price of £14.68 per 10 micrograms.
Costs (excluding value-added tax) may vary in different settings because of negotiated procurement discounts. ![]()

chemotherapy
Credit: Rhoda Baer
The UK’s National Institute for Health and Care Excellence (NICE) has updated its guidance to expand the use of erythropoiesis-stimulating agents (ESAs) in cancer patients.
In 2008, NICE issued a guidance recommending ESAs as a possible treatment for certain patients with anemia caused by cancer treatment.
Now, NICE has updated the recommendations to expand the use of ESAs—epoetin alfa, beta, theta, and zeta, as well as darbepoetin alfa—to all other indications within their UK marketing authorizations.
“A lot of people with cancer having chemotherapy will become anemic,” noted Carole Longson, director of the Centre for Health Technology Evaluation at NICE.
“Managing anemia often requires extra trips to the hospital and can significantly affect a person’s quality of life. This updated final guidance recommends more options, epoetin and darbepoetin, that are both clinically and cost-effective and which also significantly improve quality of life for people who develop anemia whilst having cancer therapy.”
The 2008 NICE guidance recommended erythropoietin analogues with iron injections as a possible treatment for anemia caused by cancer treatment only in:
- Women receiving platinum-based chemotherapy for cancer of the ovaries who have a blood hemoglobin level of 8 g/100 mL or lower
- Patients who have very severe anemia and cannot receive blood transfusions.
NICE’s updated final guidance recommends using darbepoetin alfa and epoetin alfa, beta, theta, and zeta within their marketing authorizations as an option for treating anemia in cancer patients undergoing chemotherapy.
Epoetin alfa (Eprex, Janssen-Cilag, and Binocrit, Sandoz), and epoetin zeta (Retacrit, Hospira UK) have UK marketing authorization to treat anemia and to reduce transfusion requirements in adult patients receiving chemotherapy for solid tumors, malignant lymphoma, or multiple myeloma, who are at risk of transfusion as assessed by the patients’ general status (eg, cardiovascular status, pre-existing anemia at the start of chemotherapy).
Binocrit and Retacrit are both biosimilar medicines referenced to Eprex. Eprex, Binocrit, and Retacrit are available in pre-filled syringes at net prices of £5.53, £4.33, and £5.66 per 1000 units, respectively.
Epoetin beta (NeoRecormon, Roche Products) and epoetin theta (Eporatio, Teva UK) have UK marketing authorization to treat symptomatic anemia in adult patients with non-myeloid malignancies who are receiving chemotherapy.
NeoRecormon is available in a pre-filled syringe at a net price of £3.51 per 500 units, and Eporatio is available in a pre-filled syringe at a net price of £5.99 per 1000 units.
Darbepoetin alfa (Aranesp, Amgen) has UK marketing authorization to treat symptomatic anemia in adult cancer patients with non-myeloid malignancies who are receiving chemotherapy. Aranesp is available in a pre-filled syringe at a net price of £14.68 per 10 micrograms.
Costs (excluding value-added tax) may vary in different settings because of negotiated procurement discounts. ![]()

chemotherapy
Credit: Rhoda Baer
The UK’s National Institute for Health and Care Excellence (NICE) has updated its guidance to expand the use of erythropoiesis-stimulating agents (ESAs) in cancer patients.
In 2008, NICE issued a guidance recommending ESAs as a possible treatment for certain patients with anemia caused by cancer treatment.
Now, NICE has updated the recommendations to expand the use of ESAs—epoetin alfa, beta, theta, and zeta, as well as darbepoetin alfa—to all other indications within their UK marketing authorizations.
“A lot of people with cancer having chemotherapy will become anemic,” noted Carole Longson, director of the Centre for Health Technology Evaluation at NICE.
“Managing anemia often requires extra trips to the hospital and can significantly affect a person’s quality of life. This updated final guidance recommends more options, epoetin and darbepoetin, that are both clinically and cost-effective and which also significantly improve quality of life for people who develop anemia whilst having cancer therapy.”
The 2008 NICE guidance recommended erythropoietin analogues with iron injections as a possible treatment for anemia caused by cancer treatment only in:
- Women receiving platinum-based chemotherapy for cancer of the ovaries who have a blood hemoglobin level of 8 g/100 mL or lower
- Patients who have very severe anemia and cannot receive blood transfusions.
NICE’s updated final guidance recommends using darbepoetin alfa and epoetin alfa, beta, theta, and zeta within their marketing authorizations as an option for treating anemia in cancer patients undergoing chemotherapy.
Epoetin alfa (Eprex, Janssen-Cilag, and Binocrit, Sandoz), and epoetin zeta (Retacrit, Hospira UK) have UK marketing authorization to treat anemia and to reduce transfusion requirements in adult patients receiving chemotherapy for solid tumors, malignant lymphoma, or multiple myeloma, who are at risk of transfusion as assessed by the patients’ general status (eg, cardiovascular status, pre-existing anemia at the start of chemotherapy).
Binocrit and Retacrit are both biosimilar medicines referenced to Eprex. Eprex, Binocrit, and Retacrit are available in pre-filled syringes at net prices of £5.53, £4.33, and £5.66 per 1000 units, respectively.
Epoetin beta (NeoRecormon, Roche Products) and epoetin theta (Eporatio, Teva UK) have UK marketing authorization to treat symptomatic anemia in adult patients with non-myeloid malignancies who are receiving chemotherapy.
NeoRecormon is available in a pre-filled syringe at a net price of £3.51 per 500 units, and Eporatio is available in a pre-filled syringe at a net price of £5.99 per 1000 units.
Darbepoetin alfa (Aranesp, Amgen) has UK marketing authorization to treat symptomatic anemia in adult cancer patients with non-myeloid malignancies who are receiving chemotherapy. Aranesp is available in a pre-filled syringe at a net price of £14.68 per 10 micrograms.
Costs (excluding value-added tax) may vary in different settings because of negotiated procurement discounts. ![]()
FDA extends review of panobinostat for combination treatment of multiple myeloma
The Food and Drug Administration’s review of panobinostat, combined with bortezomib and dexamethasone, for the treatment of multiple myeloma has been extended, the manufacturer has announced.
Novartis Pharmaceuticals submitted the new drug application for the pan-deacetylase (pan-DAC) inhibitor in combination with the proteasome inhibitor bortezomib (Velcade) and dexamethasone for the treatment of patients with previously treated multiple myeloma in March 2104; it was given a priority review of 8 months, instead of the standard 12 months. But the agency has extended the review for up to 3 months, the company said in a Nov. 25 statement.
The FDA was expected to make a decision in November.
“We are committed to working with the FDA as they continue to review” the application, Dr. Alessandro Riva, global head of oncology development and medical affairs at Novartis Oncology, said in the statement.
Panobinostat is an epigenetic regulator, which “may help restore cell programming in multiple myeloma,” and if approved, it would be the first pan-DAC inhibitor approved for treating patients with relapsed or relapsed and refractory multiple myeloma, according to the company.
At a meeting on Nov. 6, the FDA’s Oncologic Drugs Advisory Committee voted 5-2 that the benefits of panobinostat, combined with bortezomib and dexamethasone, did not outweigh the risks for treating patients with multiple myeloma who had received at least one prior therapy, the proposed indication. However, those voting against approval agreed that there was evidence that panobinostat had biologic activity against multiple myeloma and had an effect on progression-free survival, and said they hoped the company would continue to study the drug in patients with the disease.
The Food and Drug Administration’s review of panobinostat, combined with bortezomib and dexamethasone, for the treatment of multiple myeloma has been extended, the manufacturer has announced.
Novartis Pharmaceuticals submitted the new drug application for the pan-deacetylase (pan-DAC) inhibitor in combination with the proteasome inhibitor bortezomib (Velcade) and dexamethasone for the treatment of patients with previously treated multiple myeloma in March 2104; it was given a priority review of 8 months, instead of the standard 12 months. But the agency has extended the review for up to 3 months, the company said in a Nov. 25 statement.
The FDA was expected to make a decision in November.
“We are committed to working with the FDA as they continue to review” the application, Dr. Alessandro Riva, global head of oncology development and medical affairs at Novartis Oncology, said in the statement.
Panobinostat is an epigenetic regulator, which “may help restore cell programming in multiple myeloma,” and if approved, it would be the first pan-DAC inhibitor approved for treating patients with relapsed or relapsed and refractory multiple myeloma, according to the company.
At a meeting on Nov. 6, the FDA’s Oncologic Drugs Advisory Committee voted 5-2 that the benefits of panobinostat, combined with bortezomib and dexamethasone, did not outweigh the risks for treating patients with multiple myeloma who had received at least one prior therapy, the proposed indication. However, those voting against approval agreed that there was evidence that panobinostat had biologic activity against multiple myeloma and had an effect on progression-free survival, and said they hoped the company would continue to study the drug in patients with the disease.
The Food and Drug Administration’s review of panobinostat, combined with bortezomib and dexamethasone, for the treatment of multiple myeloma has been extended, the manufacturer has announced.
Novartis Pharmaceuticals submitted the new drug application for the pan-deacetylase (pan-DAC) inhibitor in combination with the proteasome inhibitor bortezomib (Velcade) and dexamethasone for the treatment of patients with previously treated multiple myeloma in March 2104; it was given a priority review of 8 months, instead of the standard 12 months. But the agency has extended the review for up to 3 months, the company said in a Nov. 25 statement.
The FDA was expected to make a decision in November.
“We are committed to working with the FDA as they continue to review” the application, Dr. Alessandro Riva, global head of oncology development and medical affairs at Novartis Oncology, said in the statement.
Panobinostat is an epigenetic regulator, which “may help restore cell programming in multiple myeloma,” and if approved, it would be the first pan-DAC inhibitor approved for treating patients with relapsed or relapsed and refractory multiple myeloma, according to the company.
At a meeting on Nov. 6, the FDA’s Oncologic Drugs Advisory Committee voted 5-2 that the benefits of panobinostat, combined with bortezomib and dexamethasone, did not outweigh the risks for treating patients with multiple myeloma who had received at least one prior therapy, the proposed indication. However, those voting against approval agreed that there was evidence that panobinostat had biologic activity against multiple myeloma and had an effect on progression-free survival, and said they hoped the company would continue to study the drug in patients with the disease.
Mutations indicate predisposition to blood cancers

Credit: Graham Colm
Two teams of researchers have identified somatic mutations that increase the likelihood a person will develop a hematologic malignancy.
This “pre-malignant” stage was detected simply by sequencing DNA from blood samples.
The researchers found that subjects carrying certain mutations had more than 10 times the risk of developing a hematologic malignancy than individuals without the mutations. And the risk increased with age.
Steven McCarroll, PhD, of Harvard Medical School in Boston, Massachusetts, and Benjamin Ebert, MD, PhD, also of Harvard Medical School, reported these findings in NEJM.
Both research teams looked at somatic mutations in DNA samples collected from the blood of subjects who had not been diagnosed with cancer or blood disorders.
Taking two very different approaches, the teams found that a surprising percentage of individuals had acquired a subset of the somatic mutations present in hematologic malignancies. And subjects with the mutations were more likely to develop these cancers.
This pre-malignant state was rare in individuals under the age of 40. But it appeared with increasing frequency with each decade of life, ultimately appearing in more than 10% of individuals over the age of 70.
The researchers believe these early mutations lie in wait for follow-on, cooperating mutations that, when they occur in the same cells as the earlier mutations, drive the cells toward cancer. The majority of mutations occurred in just 3 genes: DNMT3A, TET2, and ASXL1.
Dr Ebert’s group
Dr Ebert and his colleagues had hypothesized that, since hematologic malignancies increase with age, it might be possible to detect early somatic mutations that could be initiating the disease process, and these mutations might increase with age.
The researchers looked specifically at 160 genes known to be recurrently mutated in hematologic malignancies, using genetic data derived from approximately 17,000 blood samples originally obtained for studies on the genetics of type 2 diabetes.
The team found a roughly 11-fold increase in the risk of hematologic malignancy among subjects with the subset of somatic mutations linked to blood cancers. And there was a clear association between age and the frequency of these mutations.
Men were slightly more likely to have the mutations than women, and Hispanics were slightly less likely to have the mutations than other racial/ethnic groups.
The researchers also found an association between the presence of this pre-malignant state and the risk of overall mortality independent of malignancy. Individuals with the mutations had a higher risk of type 2 diabetes, coronary heart disease, and ischemic stroke as well.
However, additional research will be needed to determine the nature of these associations.
Dr McCarroll’s group
Dr McCarroll and his colleagues discovered the same phenomenon while trying to determine whether somatic mutations contribute to the risk of developing schizophrenia.
The team studied roughly 12,000 DNA samples from patients with schizophrenia and bipolar disorder, as well as healthy controls, searching across the whole genome at all of the protein-coding genes for patterns in somatic mutations.
The somatic mutations were concentrated in a handful of genes that turned out to be cancer genes.
So the researchers used electronic medical records to follow the patients’ medical histories, finding that subjects with these acquired mutations had a nearly 13-fold higher risk of developing a hematologic malignancy than subjects without the mutations.
The team conducted follow-up analyses on tumor samples from 2 patients who had progressed from this pre-malignant state to cancer. In both cases, the cancer developed from the same cells that had harbored the initiating mutations years earlier.
“The fact that both teams converged on strikingly similar findings, using very different approaches and looking at DNA from very different sets of patients, has given us great confidence in the results,” said study author Giulio Genovese, PhD, of the Broad Institute of MIT and Harvard in Cambridge, Massachusetts.
Next steps
The researchers emphasized that there is no clinical benefit today for testing for this pre-malignant state, as there are no treatments currently available that would address this condition in otherwise healthy people.
However, they said the results open the door to entirely new directions for research, toward early detection and even prevention of hematologic malignancies.
“The results demonstrate a way to identify high-risk cohorts—people who are at much higher than average risk of progressing to cancer—which could be a population for clinical trials of future prevention strategies,” Dr McCarroll said. “The abundance of these mutated cells could also serve as a biomarker—like LDL cholesterol is for cardiovascular disease—to test the effects of potential prevention therapies in clinical trials.”
Dr Ebert added, “A new focus of investigation will now be to develop interventions that might decrease the likelihood that individuals with these mutations will go on to develop overt malignancies, or therapeutic strategies to decrease mortality from other conditions that may be instigated by these mutations.”
This research is set to be presented on December 9 at the 56th ASH Annual Meeting in San Francisco. ![]()

Credit: Graham Colm
Two teams of researchers have identified somatic mutations that increase the likelihood a person will develop a hematologic malignancy.
This “pre-malignant” stage was detected simply by sequencing DNA from blood samples.
The researchers found that subjects carrying certain mutations had more than 10 times the risk of developing a hematologic malignancy than individuals without the mutations. And the risk increased with age.
Steven McCarroll, PhD, of Harvard Medical School in Boston, Massachusetts, and Benjamin Ebert, MD, PhD, also of Harvard Medical School, reported these findings in NEJM.
Both research teams looked at somatic mutations in DNA samples collected from the blood of subjects who had not been diagnosed with cancer or blood disorders.
Taking two very different approaches, the teams found that a surprising percentage of individuals had acquired a subset of the somatic mutations present in hematologic malignancies. And subjects with the mutations were more likely to develop these cancers.
This pre-malignant state was rare in individuals under the age of 40. But it appeared with increasing frequency with each decade of life, ultimately appearing in more than 10% of individuals over the age of 70.
The researchers believe these early mutations lie in wait for follow-on, cooperating mutations that, when they occur in the same cells as the earlier mutations, drive the cells toward cancer. The majority of mutations occurred in just 3 genes: DNMT3A, TET2, and ASXL1.
Dr Ebert’s group
Dr Ebert and his colleagues had hypothesized that, since hematologic malignancies increase with age, it might be possible to detect early somatic mutations that could be initiating the disease process, and these mutations might increase with age.
The researchers looked specifically at 160 genes known to be recurrently mutated in hematologic malignancies, using genetic data derived from approximately 17,000 blood samples originally obtained for studies on the genetics of type 2 diabetes.
The team found a roughly 11-fold increase in the risk of hematologic malignancy among subjects with the subset of somatic mutations linked to blood cancers. And there was a clear association between age and the frequency of these mutations.
Men were slightly more likely to have the mutations than women, and Hispanics were slightly less likely to have the mutations than other racial/ethnic groups.
The researchers also found an association between the presence of this pre-malignant state and the risk of overall mortality independent of malignancy. Individuals with the mutations had a higher risk of type 2 diabetes, coronary heart disease, and ischemic stroke as well.
However, additional research will be needed to determine the nature of these associations.
Dr McCarroll’s group
Dr McCarroll and his colleagues discovered the same phenomenon while trying to determine whether somatic mutations contribute to the risk of developing schizophrenia.
The team studied roughly 12,000 DNA samples from patients with schizophrenia and bipolar disorder, as well as healthy controls, searching across the whole genome at all of the protein-coding genes for patterns in somatic mutations.
The somatic mutations were concentrated in a handful of genes that turned out to be cancer genes.
So the researchers used electronic medical records to follow the patients’ medical histories, finding that subjects with these acquired mutations had a nearly 13-fold higher risk of developing a hematologic malignancy than subjects without the mutations.
The team conducted follow-up analyses on tumor samples from 2 patients who had progressed from this pre-malignant state to cancer. In both cases, the cancer developed from the same cells that had harbored the initiating mutations years earlier.
“The fact that both teams converged on strikingly similar findings, using very different approaches and looking at DNA from very different sets of patients, has given us great confidence in the results,” said study author Giulio Genovese, PhD, of the Broad Institute of MIT and Harvard in Cambridge, Massachusetts.
Next steps
The researchers emphasized that there is no clinical benefit today for testing for this pre-malignant state, as there are no treatments currently available that would address this condition in otherwise healthy people.
However, they said the results open the door to entirely new directions for research, toward early detection and even prevention of hematologic malignancies.
“The results demonstrate a way to identify high-risk cohorts—people who are at much higher than average risk of progressing to cancer—which could be a population for clinical trials of future prevention strategies,” Dr McCarroll said. “The abundance of these mutated cells could also serve as a biomarker—like LDL cholesterol is for cardiovascular disease—to test the effects of potential prevention therapies in clinical trials.”
Dr Ebert added, “A new focus of investigation will now be to develop interventions that might decrease the likelihood that individuals with these mutations will go on to develop overt malignancies, or therapeutic strategies to decrease mortality from other conditions that may be instigated by these mutations.”
This research is set to be presented on December 9 at the 56th ASH Annual Meeting in San Francisco. ![]()

Credit: Graham Colm
Two teams of researchers have identified somatic mutations that increase the likelihood a person will develop a hematologic malignancy.
This “pre-malignant” stage was detected simply by sequencing DNA from blood samples.
The researchers found that subjects carrying certain mutations had more than 10 times the risk of developing a hematologic malignancy than individuals without the mutations. And the risk increased with age.
Steven McCarroll, PhD, of Harvard Medical School in Boston, Massachusetts, and Benjamin Ebert, MD, PhD, also of Harvard Medical School, reported these findings in NEJM.
Both research teams looked at somatic mutations in DNA samples collected from the blood of subjects who had not been diagnosed with cancer or blood disorders.
Taking two very different approaches, the teams found that a surprising percentage of individuals had acquired a subset of the somatic mutations present in hematologic malignancies. And subjects with the mutations were more likely to develop these cancers.
This pre-malignant state was rare in individuals under the age of 40. But it appeared with increasing frequency with each decade of life, ultimately appearing in more than 10% of individuals over the age of 70.
The researchers believe these early mutations lie in wait for follow-on, cooperating mutations that, when they occur in the same cells as the earlier mutations, drive the cells toward cancer. The majority of mutations occurred in just 3 genes: DNMT3A, TET2, and ASXL1.
Dr Ebert’s group
Dr Ebert and his colleagues had hypothesized that, since hematologic malignancies increase with age, it might be possible to detect early somatic mutations that could be initiating the disease process, and these mutations might increase with age.
The researchers looked specifically at 160 genes known to be recurrently mutated in hematologic malignancies, using genetic data derived from approximately 17,000 blood samples originally obtained for studies on the genetics of type 2 diabetes.
The team found a roughly 11-fold increase in the risk of hematologic malignancy among subjects with the subset of somatic mutations linked to blood cancers. And there was a clear association between age and the frequency of these mutations.
Men were slightly more likely to have the mutations than women, and Hispanics were slightly less likely to have the mutations than other racial/ethnic groups.
The researchers also found an association between the presence of this pre-malignant state and the risk of overall mortality independent of malignancy. Individuals with the mutations had a higher risk of type 2 diabetes, coronary heart disease, and ischemic stroke as well.
However, additional research will be needed to determine the nature of these associations.
Dr McCarroll’s group
Dr McCarroll and his colleagues discovered the same phenomenon while trying to determine whether somatic mutations contribute to the risk of developing schizophrenia.
The team studied roughly 12,000 DNA samples from patients with schizophrenia and bipolar disorder, as well as healthy controls, searching across the whole genome at all of the protein-coding genes for patterns in somatic mutations.
The somatic mutations were concentrated in a handful of genes that turned out to be cancer genes.
So the researchers used electronic medical records to follow the patients’ medical histories, finding that subjects with these acquired mutations had a nearly 13-fold higher risk of developing a hematologic malignancy than subjects without the mutations.
The team conducted follow-up analyses on tumor samples from 2 patients who had progressed from this pre-malignant state to cancer. In both cases, the cancer developed from the same cells that had harbored the initiating mutations years earlier.
“The fact that both teams converged on strikingly similar findings, using very different approaches and looking at DNA from very different sets of patients, has given us great confidence in the results,” said study author Giulio Genovese, PhD, of the Broad Institute of MIT and Harvard in Cambridge, Massachusetts.
Next steps
The researchers emphasized that there is no clinical benefit today for testing for this pre-malignant state, as there are no treatments currently available that would address this condition in otherwise healthy people.
However, they said the results open the door to entirely new directions for research, toward early detection and even prevention of hematologic malignancies.
“The results demonstrate a way to identify high-risk cohorts—people who are at much higher than average risk of progressing to cancer—which could be a population for clinical trials of future prevention strategies,” Dr McCarroll said. “The abundance of these mutated cells could also serve as a biomarker—like LDL cholesterol is for cardiovascular disease—to test the effects of potential prevention therapies in clinical trials.”
Dr Ebert added, “A new focus of investigation will now be to develop interventions that might decrease the likelihood that individuals with these mutations will go on to develop overt malignancies, or therapeutic strategies to decrease mortality from other conditions that may be instigated by these mutations.”
This research is set to be presented on December 9 at the 56th ASH Annual Meeting in San Francisco. ![]()
Exposure to hookah smoke may raise risk of blood cancers

Credit: Steven Damron
A new study indicates that individuals exposed to hookah smoke have an increase in the uptake of benzene, a substance linked to the development of hematologic malignancies.
Levels of S-phenylmercapturic acid (SPMA), a metabolite of benzene, were more than 4 times higher after study subjects smoked a hookah than before they did.
And non-smoking subjects experienced a nearly 3-fold increase in SPMA levels after they visited a hookah lounge.
Nada Kassem, RN, DrPH, of San Diego State University in California, and her colleagues reported these findings in Cancer Epidemiology, Biomarkers & Prevention.
“Hookah smoking involves the use of burning charcoal that is needed to heat the hookah tobacco to generate the smoke that the smoker inhales,” Dr Kassem explained.
“In addition to inhaling toxicants and carcinogens found in the hookah tobacco smoke, hookah smokers and non-smokers who socialize with hookah smokers also inhale large quantities of charcoal combustion-generated toxic and carcinogenic emissions.”
To gain more insight into the dangers of hookah smoke, Dr Kassem and her colleagues analyzed levels of SPMA in the urine of 105 hookah smokers and 103 non-smokers.
The team obtained urine samples the morning of and the morning after participants attended a hookah-only smoking event at a hookah lounge or a private home.
SPMA levels in hookah smokers increased 4.2-fold after smoking at a hookah lounge (P<0.001) and increased 1.9-fold after smoking in a private home (P=0.003).
Non-smokers’ SPMA levels increased 2.6-fold after attending a social event in a hookah lounge (P=0.055).
However, non-smokers had similarly high levels of SPMA before and after attending hookah events in a private home (P=0.933). This suggests these subjects had chronic exposure to benzene before the study, according to Dr Kassem.
Regardless, she and her colleagues said the study’s results suggest hookah smoke increases the uptake of benzene, which has been linked to a range of hematologic malignancies, particularly acute myeloid leukemia.
“In contrast to what is believed, hookah tobacco smoking is not a safe alternative to smoking other forms of tobacco,” Dr Kassem said.
She and her colleagues noted that there is no safe level of exposure to benzene. And this suggests a need for interventions to reduce or prevent the use of hookahs, limit hookah-related exposure to toxic substances, and include hookah smoking in clean indoor air legislation. ![]()

Credit: Steven Damron
A new study indicates that individuals exposed to hookah smoke have an increase in the uptake of benzene, a substance linked to the development of hematologic malignancies.
Levels of S-phenylmercapturic acid (SPMA), a metabolite of benzene, were more than 4 times higher after study subjects smoked a hookah than before they did.
And non-smoking subjects experienced a nearly 3-fold increase in SPMA levels after they visited a hookah lounge.
Nada Kassem, RN, DrPH, of San Diego State University in California, and her colleagues reported these findings in Cancer Epidemiology, Biomarkers & Prevention.
“Hookah smoking involves the use of burning charcoal that is needed to heat the hookah tobacco to generate the smoke that the smoker inhales,” Dr Kassem explained.
“In addition to inhaling toxicants and carcinogens found in the hookah tobacco smoke, hookah smokers and non-smokers who socialize with hookah smokers also inhale large quantities of charcoal combustion-generated toxic and carcinogenic emissions.”
To gain more insight into the dangers of hookah smoke, Dr Kassem and her colleagues analyzed levels of SPMA in the urine of 105 hookah smokers and 103 non-smokers.
The team obtained urine samples the morning of and the morning after participants attended a hookah-only smoking event at a hookah lounge or a private home.
SPMA levels in hookah smokers increased 4.2-fold after smoking at a hookah lounge (P<0.001) and increased 1.9-fold after smoking in a private home (P=0.003).
Non-smokers’ SPMA levels increased 2.6-fold after attending a social event in a hookah lounge (P=0.055).
However, non-smokers had similarly high levels of SPMA before and after attending hookah events in a private home (P=0.933). This suggests these subjects had chronic exposure to benzene before the study, according to Dr Kassem.
Regardless, she and her colleagues said the study’s results suggest hookah smoke increases the uptake of benzene, which has been linked to a range of hematologic malignancies, particularly acute myeloid leukemia.
“In contrast to what is believed, hookah tobacco smoking is not a safe alternative to smoking other forms of tobacco,” Dr Kassem said.
She and her colleagues noted that there is no safe level of exposure to benzene. And this suggests a need for interventions to reduce or prevent the use of hookahs, limit hookah-related exposure to toxic substances, and include hookah smoking in clean indoor air legislation. ![]()

Credit: Steven Damron
A new study indicates that individuals exposed to hookah smoke have an increase in the uptake of benzene, a substance linked to the development of hematologic malignancies.
Levels of S-phenylmercapturic acid (SPMA), a metabolite of benzene, were more than 4 times higher after study subjects smoked a hookah than before they did.
And non-smoking subjects experienced a nearly 3-fold increase in SPMA levels after they visited a hookah lounge.
Nada Kassem, RN, DrPH, of San Diego State University in California, and her colleagues reported these findings in Cancer Epidemiology, Biomarkers & Prevention.
“Hookah smoking involves the use of burning charcoal that is needed to heat the hookah tobacco to generate the smoke that the smoker inhales,” Dr Kassem explained.
“In addition to inhaling toxicants and carcinogens found in the hookah tobacco smoke, hookah smokers and non-smokers who socialize with hookah smokers also inhale large quantities of charcoal combustion-generated toxic and carcinogenic emissions.”
To gain more insight into the dangers of hookah smoke, Dr Kassem and her colleagues analyzed levels of SPMA in the urine of 105 hookah smokers and 103 non-smokers.
The team obtained urine samples the morning of and the morning after participants attended a hookah-only smoking event at a hookah lounge or a private home.
SPMA levels in hookah smokers increased 4.2-fold after smoking at a hookah lounge (P<0.001) and increased 1.9-fold after smoking in a private home (P=0.003).
Non-smokers’ SPMA levels increased 2.6-fold after attending a social event in a hookah lounge (P=0.055).
However, non-smokers had similarly high levels of SPMA before and after attending hookah events in a private home (P=0.933). This suggests these subjects had chronic exposure to benzene before the study, according to Dr Kassem.
Regardless, she and her colleagues said the study’s results suggest hookah smoke increases the uptake of benzene, which has been linked to a range of hematologic malignancies, particularly acute myeloid leukemia.
“In contrast to what is believed, hookah tobacco smoking is not a safe alternative to smoking other forms of tobacco,” Dr Kassem said.
She and her colleagues noted that there is no safe level of exposure to benzene. And this suggests a need for interventions to reduce or prevent the use of hookahs, limit hookah-related exposure to toxic substances, and include hookah smoking in clean indoor air legislation. ![]()
Immunologist Herman Eisen dies at 96

Photo courtesy of MIT
Herman Eisen, MD, a respected immunologist, has died at the age of 96.
Over a 70-year career, Dr Eisen contributed a great deal to his own field and other fields of research.
He published work describing affinity maturation, clarified the basis for certain allergic reactions, and provided new insight into multiple myeloma and other cancers.
Dr Eisen was a professor emeritus of biology at the Massachusetts Institute of Technology (MIT) and a founding member of the MIT Center for Cancer Research (now the Koch Institute for Integrative Cancer Research).
He joined MIT in 1973 and retired in 1989, but only in the official sense. As a professor emeritus, he maintained an active lab and continued to research, publish, and advise students and postdocs at MIT until his passing.
Early years
Born in 1918 in Brooklyn, New York, Dr Eisen developed a keen interest in science at an early age, when a high school chemistry class helped frame his perception of the world as a collection of atoms and molecules.
Dr Eisen began premedical studies at New York University (NYU) in 1934, but halfway through his undergraduate career, he developed tuberculosis and left school. Though this kept him out of school for one year, the illness sparked a curiosity about the immune system that would endure for the rest of his life.
Dr Eisen returned to NYU to complete his bachelor’s degree, then enrolled at the university’s medical school. He graduated with an MD in 1943 and then worked as an assistant in the pathology department at the Columbia University College of Physicians and Surgeons before going back to NYU for his residency.
Research interests
Dr Eisen had a strong interest in basic science research, particularly in trying to better understand the body’s immune system. Though career options for physician-scientists had historically been limited, the federal government began to increase its funding of biomedical research through the National Institutes of Health (NIH) following World War II.
Seizing these new opportunities, Dr Eisen became one of the first recipients of an NIH fellowship, which supported his research on sulfonamide-induced antibodies at NYU. These investigations helped him and colleague Fred Karush, PhD, determine the number of antigen-binding sites on antibodies.
After his 2-year NIH fellowship, Dr Eisen worked briefly at the Sloan Kettering Institute before returning once again to NYU as a faculty member.
Inspired by the work of his recently deceased role model, Karl Landsteiner, MD, Dr Eisen studied immune reactions of the skin. In doing so, he clarified the basis for certain allergic responses and showed that only those chemicals capable of forming covalent bonds to skin proteins could cause a characteristic itchy rash.
In 1955, Washington University in St Louis recruited Dr Eisen to join the faculty of its School of Medicine. There, he served as dermatologist-in-chief for 5 years before moving to the Department of Microbiology to serve as chair.
While at Washington University, Dr Eisen published groundbreaking research in which he described affinity maturation: the process by which activated B cells produce antibodies with an increasingly higher affinity for invading pathogens after infection. This process is fundamental to the development of potent immune responses.
“Our understanding of affinity maturation begins with Herman’s papers,” said Arup K. Chakraborty, PhD, director of MIT’s Institute for Medical Engineering and Science.
“Understanding this evolutionary process is critical for vaccine design, and affinity maturation is also mimicked in countless academic laboratories and companies to design antibody-based therapies.”
Cancer research
In response to the National Cancer Act of 1971, MIT tasked Nobel Prize-winning biology professor Salvador Luria, MD, with establishing and leading a new MIT Center for Cancer Research. Wanting to include cancer immunology as a focus of this new center, Dr Luria approached Dr Eisen about joining as a founding faculty member.
Dr Eisen accepted the role and arrived at MIT in 1973 as a professor in the Department of Biology. He brought his immunology expertise to MIT’s new cancer center to study how cancer cells evade the body’s natural immune response.
Much of his work focused on studying myeloma tumors in mice and screening their associated proteins. He found that if he used myeloma proteins from one mouse to immunize other mice from the same strain, they were resistant when challenged with cancer cells.
Dr Eisen and his lab went on to study how CD8 T cells develop into cytotoxic T cells and long-lived memory T cells. Therapeutic vaccines that exploit CD8 responses have not yet been developed for humans.
Dr Eisen was working to understand and overcome the barriers to creating effective CD8 vaccines, and his research on the subject was of particular importance to the advancement of cancer immunology.
“Herman’s lifelong pursuit of science, even to the very last day of his life, has been an inspiration to many of us,” said Jianzhu Chen, PhD, of the Koch Institute. “He was a great human being with a great attitude and a clear mind. He will be missed greatly.”
Other colleagues remember Dr Eisen not only as a respected immunologist, but as a hardworking collaborator and a man of integrity. He continued to be an active scientist and had been working with Dr Chakraborty on a paper until his passing.
“Herman was a giant in the field of immunology, with many seminal discoveries,” Dr Chakraborty said. “He was also the kindest and most generous and moral person I have known. Until the end, he was working on scientific problems with junior colleagues and students who benefited from his wisdom. I am lucky to have worked with this great scientist and wonderful human being.”
Dr Eisen was elected to the American Academy of Arts and Sciences in 1965, the National Academy of Sciences in 1969, and the Institute of Medicine of the National Academies in 1974.
He received numerous other awards and honors throughout his career, including the Behring-Heidelberger Award from the American Association of Immunologists, an Outstanding Investigator Award from the National Cancer Institute, and the Lifetime Service Award from the American Association of Immunologists, of which he served as president from 1968 to 1969.
Dr Eisen passed away on November 2. He is survived by his wife Natalie and their children, Ellen, Jane, Jim, Tom, and Matthew, as well as 12 grandchildren. ![]()

Photo courtesy of MIT
Herman Eisen, MD, a respected immunologist, has died at the age of 96.
Over a 70-year career, Dr Eisen contributed a great deal to his own field and other fields of research.
He published work describing affinity maturation, clarified the basis for certain allergic reactions, and provided new insight into multiple myeloma and other cancers.
Dr Eisen was a professor emeritus of biology at the Massachusetts Institute of Technology (MIT) and a founding member of the MIT Center for Cancer Research (now the Koch Institute for Integrative Cancer Research).
He joined MIT in 1973 and retired in 1989, but only in the official sense. As a professor emeritus, he maintained an active lab and continued to research, publish, and advise students and postdocs at MIT until his passing.
Early years
Born in 1918 in Brooklyn, New York, Dr Eisen developed a keen interest in science at an early age, when a high school chemistry class helped frame his perception of the world as a collection of atoms and molecules.
Dr Eisen began premedical studies at New York University (NYU) in 1934, but halfway through his undergraduate career, he developed tuberculosis and left school. Though this kept him out of school for one year, the illness sparked a curiosity about the immune system that would endure for the rest of his life.
Dr Eisen returned to NYU to complete his bachelor’s degree, then enrolled at the university’s medical school. He graduated with an MD in 1943 and then worked as an assistant in the pathology department at the Columbia University College of Physicians and Surgeons before going back to NYU for his residency.
Research interests
Dr Eisen had a strong interest in basic science research, particularly in trying to better understand the body’s immune system. Though career options for physician-scientists had historically been limited, the federal government began to increase its funding of biomedical research through the National Institutes of Health (NIH) following World War II.
Seizing these new opportunities, Dr Eisen became one of the first recipients of an NIH fellowship, which supported his research on sulfonamide-induced antibodies at NYU. These investigations helped him and colleague Fred Karush, PhD, determine the number of antigen-binding sites on antibodies.
After his 2-year NIH fellowship, Dr Eisen worked briefly at the Sloan Kettering Institute before returning once again to NYU as a faculty member.
Inspired by the work of his recently deceased role model, Karl Landsteiner, MD, Dr Eisen studied immune reactions of the skin. In doing so, he clarified the basis for certain allergic responses and showed that only those chemicals capable of forming covalent bonds to skin proteins could cause a characteristic itchy rash.
In 1955, Washington University in St Louis recruited Dr Eisen to join the faculty of its School of Medicine. There, he served as dermatologist-in-chief for 5 years before moving to the Department of Microbiology to serve as chair.
While at Washington University, Dr Eisen published groundbreaking research in which he described affinity maturation: the process by which activated B cells produce antibodies with an increasingly higher affinity for invading pathogens after infection. This process is fundamental to the development of potent immune responses.
“Our understanding of affinity maturation begins with Herman’s papers,” said Arup K. Chakraborty, PhD, director of MIT’s Institute for Medical Engineering and Science.
“Understanding this evolutionary process is critical for vaccine design, and affinity maturation is also mimicked in countless academic laboratories and companies to design antibody-based therapies.”
Cancer research
In response to the National Cancer Act of 1971, MIT tasked Nobel Prize-winning biology professor Salvador Luria, MD, with establishing and leading a new MIT Center for Cancer Research. Wanting to include cancer immunology as a focus of this new center, Dr Luria approached Dr Eisen about joining as a founding faculty member.
Dr Eisen accepted the role and arrived at MIT in 1973 as a professor in the Department of Biology. He brought his immunology expertise to MIT’s new cancer center to study how cancer cells evade the body’s natural immune response.
Much of his work focused on studying myeloma tumors in mice and screening their associated proteins. He found that if he used myeloma proteins from one mouse to immunize other mice from the same strain, they were resistant when challenged with cancer cells.
Dr Eisen and his lab went on to study how CD8 T cells develop into cytotoxic T cells and long-lived memory T cells. Therapeutic vaccines that exploit CD8 responses have not yet been developed for humans.
Dr Eisen was working to understand and overcome the barriers to creating effective CD8 vaccines, and his research on the subject was of particular importance to the advancement of cancer immunology.
“Herman’s lifelong pursuit of science, even to the very last day of his life, has been an inspiration to many of us,” said Jianzhu Chen, PhD, of the Koch Institute. “He was a great human being with a great attitude and a clear mind. He will be missed greatly.”
Other colleagues remember Dr Eisen not only as a respected immunologist, but as a hardworking collaborator and a man of integrity. He continued to be an active scientist and had been working with Dr Chakraborty on a paper until his passing.
“Herman was a giant in the field of immunology, with many seminal discoveries,” Dr Chakraborty said. “He was also the kindest and most generous and moral person I have known. Until the end, he was working on scientific problems with junior colleagues and students who benefited from his wisdom. I am lucky to have worked with this great scientist and wonderful human being.”
Dr Eisen was elected to the American Academy of Arts and Sciences in 1965, the National Academy of Sciences in 1969, and the Institute of Medicine of the National Academies in 1974.
He received numerous other awards and honors throughout his career, including the Behring-Heidelberger Award from the American Association of Immunologists, an Outstanding Investigator Award from the National Cancer Institute, and the Lifetime Service Award from the American Association of Immunologists, of which he served as president from 1968 to 1969.
Dr Eisen passed away on November 2. He is survived by his wife Natalie and their children, Ellen, Jane, Jim, Tom, and Matthew, as well as 12 grandchildren. ![]()

Photo courtesy of MIT
Herman Eisen, MD, a respected immunologist, has died at the age of 96.
Over a 70-year career, Dr Eisen contributed a great deal to his own field and other fields of research.
He published work describing affinity maturation, clarified the basis for certain allergic reactions, and provided new insight into multiple myeloma and other cancers.
Dr Eisen was a professor emeritus of biology at the Massachusetts Institute of Technology (MIT) and a founding member of the MIT Center for Cancer Research (now the Koch Institute for Integrative Cancer Research).
He joined MIT in 1973 and retired in 1989, but only in the official sense. As a professor emeritus, he maintained an active lab and continued to research, publish, and advise students and postdocs at MIT until his passing.
Early years
Born in 1918 in Brooklyn, New York, Dr Eisen developed a keen interest in science at an early age, when a high school chemistry class helped frame his perception of the world as a collection of atoms and molecules.
Dr Eisen began premedical studies at New York University (NYU) in 1934, but halfway through his undergraduate career, he developed tuberculosis and left school. Though this kept him out of school for one year, the illness sparked a curiosity about the immune system that would endure for the rest of his life.
Dr Eisen returned to NYU to complete his bachelor’s degree, then enrolled at the university’s medical school. He graduated with an MD in 1943 and then worked as an assistant in the pathology department at the Columbia University College of Physicians and Surgeons before going back to NYU for his residency.
Research interests
Dr Eisen had a strong interest in basic science research, particularly in trying to better understand the body’s immune system. Though career options for physician-scientists had historically been limited, the federal government began to increase its funding of biomedical research through the National Institutes of Health (NIH) following World War II.
Seizing these new opportunities, Dr Eisen became one of the first recipients of an NIH fellowship, which supported his research on sulfonamide-induced antibodies at NYU. These investigations helped him and colleague Fred Karush, PhD, determine the number of antigen-binding sites on antibodies.
After his 2-year NIH fellowship, Dr Eisen worked briefly at the Sloan Kettering Institute before returning once again to NYU as a faculty member.
Inspired by the work of his recently deceased role model, Karl Landsteiner, MD, Dr Eisen studied immune reactions of the skin. In doing so, he clarified the basis for certain allergic responses and showed that only those chemicals capable of forming covalent bonds to skin proteins could cause a characteristic itchy rash.
In 1955, Washington University in St Louis recruited Dr Eisen to join the faculty of its School of Medicine. There, he served as dermatologist-in-chief for 5 years before moving to the Department of Microbiology to serve as chair.
While at Washington University, Dr Eisen published groundbreaking research in which he described affinity maturation: the process by which activated B cells produce antibodies with an increasingly higher affinity for invading pathogens after infection. This process is fundamental to the development of potent immune responses.
“Our understanding of affinity maturation begins with Herman’s papers,” said Arup K. Chakraborty, PhD, director of MIT’s Institute for Medical Engineering and Science.
“Understanding this evolutionary process is critical for vaccine design, and affinity maturation is also mimicked in countless academic laboratories and companies to design antibody-based therapies.”
Cancer research
In response to the National Cancer Act of 1971, MIT tasked Nobel Prize-winning biology professor Salvador Luria, MD, with establishing and leading a new MIT Center for Cancer Research. Wanting to include cancer immunology as a focus of this new center, Dr Luria approached Dr Eisen about joining as a founding faculty member.
Dr Eisen accepted the role and arrived at MIT in 1973 as a professor in the Department of Biology. He brought his immunology expertise to MIT’s new cancer center to study how cancer cells evade the body’s natural immune response.
Much of his work focused on studying myeloma tumors in mice and screening their associated proteins. He found that if he used myeloma proteins from one mouse to immunize other mice from the same strain, they were resistant when challenged with cancer cells.
Dr Eisen and his lab went on to study how CD8 T cells develop into cytotoxic T cells and long-lived memory T cells. Therapeutic vaccines that exploit CD8 responses have not yet been developed for humans.
Dr Eisen was working to understand and overcome the barriers to creating effective CD8 vaccines, and his research on the subject was of particular importance to the advancement of cancer immunology.
“Herman’s lifelong pursuit of science, even to the very last day of his life, has been an inspiration to many of us,” said Jianzhu Chen, PhD, of the Koch Institute. “He was a great human being with a great attitude and a clear mind. He will be missed greatly.”
Other colleagues remember Dr Eisen not only as a respected immunologist, but as a hardworking collaborator and a man of integrity. He continued to be an active scientist and had been working with Dr Chakraborty on a paper until his passing.
“Herman was a giant in the field of immunology, with many seminal discoveries,” Dr Chakraborty said. “He was also the kindest and most generous and moral person I have known. Until the end, he was working on scientific problems with junior colleagues and students who benefited from his wisdom. I am lucky to have worked with this great scientist and wonderful human being.”
Dr Eisen was elected to the American Academy of Arts and Sciences in 1965, the National Academy of Sciences in 1969, and the Institute of Medicine of the National Academies in 1974.
He received numerous other awards and honors throughout his career, including the Behring-Heidelberger Award from the American Association of Immunologists, an Outstanding Investigator Award from the National Cancer Institute, and the Lifetime Service Award from the American Association of Immunologists, of which he served as president from 1968 to 1969.
Dr Eisen passed away on November 2. He is survived by his wife Natalie and their children, Ellen, Jane, Jim, Tom, and Matthew, as well as 12 grandchildren. ![]()
Combo proves active in newly diagnosed MM

Credit: Esther Dyson
Combining the proteasome inhibitor ixazomib with lenalidomide and dexamethasone shows promise for treating patients with newly diagnosed multiple myeloma (MM), according to researchers.
In a phase 1/2 study, the all-oral combination produced a 92% overall response rate and a 27% complete response rate.
Drug-related adverse events occurred in 100% of patients, with events of grade 3 or higher occurring in 63% of patients.
These results appear in The Lancet Oncology. The study was funded by Millennium Pharmaceuticals, the company developing ixazomib.
“Ixazomib is an investigational, oral proteasome inhibitor with promising anti-myeloma effects and low rates of peripheral neuropathy,” said study author Shaji Kumar, MD, of the Mayo Clinic in Rochester, Minnesota.
“While it is well known that a combination of bortezomib, lenalidomide, and dexamethasone is highly effective in treating newly diagnosed multiple myeloma, we wanted to study the safety, tolerability, and activity of ixazomib in combination with lenalidomide and dexamethasone in newly diagnosed multiple myeloma.”
Dr Kumar and colleagues enrolled 65 patients—15 for phase 1 and 50 for phase 2 of the study—who were newly diagnosed with MM and 18 years of age or older. Patients had measurable disease, ECOG performance status of 0 to 2, and no grade 2 or higher peripheral neuropathy.
They received ixazomib (on days 1, 8, and 15) plus lenalidomide at 25 mg (on days 1 to 21) and dexamethasone at 40 mg (on days 1, 8, 15, and 22) for up to twelve 28-day cycles, followed by maintenance therapy with ixazomib alone.
In phase 1, patients received escalating doses of ixazomib, from 1.68 mg/m2 to 3.95 mg/m2, to establish the recommended dose for phase 2. The researchers established 2.97 mg/m2 as the maximum-tolerated dose and recommended the phase 2 dose be 2.23 mg/m2. This was converted to a 4.0 mg fixed dose based on population pharmacokinetic results.
Adverse events
The researchers said the combination was well tolerated, and most toxic effects were managed through dose modifications.
All patients reported at least one treatment-emergent adverse event, and 75% reported at least one treatment-emergent event that was grade 3 or higher.
Fifty-seven percent of patients had adverse events that led to dose reductions, including 53% of patients in the dose-escalation cohort and 58% of patients in the phase 2 cohort.
The most common adverse events resulting in dose reductions included skin and subcutaneous tissue disorders (20%), fatigue (14%), diarrhea (8%), peripheral neuropathy not elsewhere classified (8%), insomnia (6%), and increased body weight (6%). Five patients had adverse events leading to treatment discontinuation.
Two patients in the phase 2 cohort died while on study. One patient died of respiratory syncytial viral pneumonia that was thought to be treatment-related. The other patient died from cardiorespiratory arrest, which was considered not related to treatment.
Response and survival rates
Of the 64 response-evaluable patients, 92% responded to treatment. Fifty-eight percent had a partial response or better, and 27% had a complete response.
Responses deepened with an increasing number of treatment cycles. In the 25 patients continuing with maintenance therapy, 5 (20%) had an improvement in the depth of response during this phase.
The median duration of response has not been reached, but patients maintained responses for up to 2 years.
At last follow-up, 9 patients had progressed or died. The estimated 1-year progression-free survival was 88%, and 2-year progression-free survival was 67%.
The median overall survival has not been reached, but the estimated 1-year overall survival was 94%.
“The all-oral combination of weekly ixazomib plus lenalidomide and dexamethasone was generally well-tolerated and appeared active in patients with newly diagnosed multiple myeloma,” Dr Kumar said. “Our results support the development of a phase 3 trial studying this combination for multiple myeloma.” ![]()

Credit: Esther Dyson
Combining the proteasome inhibitor ixazomib with lenalidomide and dexamethasone shows promise for treating patients with newly diagnosed multiple myeloma (MM), according to researchers.
In a phase 1/2 study, the all-oral combination produced a 92% overall response rate and a 27% complete response rate.
Drug-related adverse events occurred in 100% of patients, with events of grade 3 or higher occurring in 63% of patients.
These results appear in The Lancet Oncology. The study was funded by Millennium Pharmaceuticals, the company developing ixazomib.
“Ixazomib is an investigational, oral proteasome inhibitor with promising anti-myeloma effects and low rates of peripheral neuropathy,” said study author Shaji Kumar, MD, of the Mayo Clinic in Rochester, Minnesota.
“While it is well known that a combination of bortezomib, lenalidomide, and dexamethasone is highly effective in treating newly diagnosed multiple myeloma, we wanted to study the safety, tolerability, and activity of ixazomib in combination with lenalidomide and dexamethasone in newly diagnosed multiple myeloma.”
Dr Kumar and colleagues enrolled 65 patients—15 for phase 1 and 50 for phase 2 of the study—who were newly diagnosed with MM and 18 years of age or older. Patients had measurable disease, ECOG performance status of 0 to 2, and no grade 2 or higher peripheral neuropathy.
They received ixazomib (on days 1, 8, and 15) plus lenalidomide at 25 mg (on days 1 to 21) and dexamethasone at 40 mg (on days 1, 8, 15, and 22) for up to twelve 28-day cycles, followed by maintenance therapy with ixazomib alone.
In phase 1, patients received escalating doses of ixazomib, from 1.68 mg/m2 to 3.95 mg/m2, to establish the recommended dose for phase 2. The researchers established 2.97 mg/m2 as the maximum-tolerated dose and recommended the phase 2 dose be 2.23 mg/m2. This was converted to a 4.0 mg fixed dose based on population pharmacokinetic results.
Adverse events
The researchers said the combination was well tolerated, and most toxic effects were managed through dose modifications.
All patients reported at least one treatment-emergent adverse event, and 75% reported at least one treatment-emergent event that was grade 3 or higher.
Fifty-seven percent of patients had adverse events that led to dose reductions, including 53% of patients in the dose-escalation cohort and 58% of patients in the phase 2 cohort.
The most common adverse events resulting in dose reductions included skin and subcutaneous tissue disorders (20%), fatigue (14%), diarrhea (8%), peripheral neuropathy not elsewhere classified (8%), insomnia (6%), and increased body weight (6%). Five patients had adverse events leading to treatment discontinuation.
Two patients in the phase 2 cohort died while on study. One patient died of respiratory syncytial viral pneumonia that was thought to be treatment-related. The other patient died from cardiorespiratory arrest, which was considered not related to treatment.
Response and survival rates
Of the 64 response-evaluable patients, 92% responded to treatment. Fifty-eight percent had a partial response or better, and 27% had a complete response.
Responses deepened with an increasing number of treatment cycles. In the 25 patients continuing with maintenance therapy, 5 (20%) had an improvement in the depth of response during this phase.
The median duration of response has not been reached, but patients maintained responses for up to 2 years.
At last follow-up, 9 patients had progressed or died. The estimated 1-year progression-free survival was 88%, and 2-year progression-free survival was 67%.
The median overall survival has not been reached, but the estimated 1-year overall survival was 94%.
“The all-oral combination of weekly ixazomib plus lenalidomide and dexamethasone was generally well-tolerated and appeared active in patients with newly diagnosed multiple myeloma,” Dr Kumar said. “Our results support the development of a phase 3 trial studying this combination for multiple myeloma.” ![]()

Credit: Esther Dyson
Combining the proteasome inhibitor ixazomib with lenalidomide and dexamethasone shows promise for treating patients with newly diagnosed multiple myeloma (MM), according to researchers.
In a phase 1/2 study, the all-oral combination produced a 92% overall response rate and a 27% complete response rate.
Drug-related adverse events occurred in 100% of patients, with events of grade 3 or higher occurring in 63% of patients.
These results appear in The Lancet Oncology. The study was funded by Millennium Pharmaceuticals, the company developing ixazomib.
“Ixazomib is an investigational, oral proteasome inhibitor with promising anti-myeloma effects and low rates of peripheral neuropathy,” said study author Shaji Kumar, MD, of the Mayo Clinic in Rochester, Minnesota.
“While it is well known that a combination of bortezomib, lenalidomide, and dexamethasone is highly effective in treating newly diagnosed multiple myeloma, we wanted to study the safety, tolerability, and activity of ixazomib in combination with lenalidomide and dexamethasone in newly diagnosed multiple myeloma.”
Dr Kumar and colleagues enrolled 65 patients—15 for phase 1 and 50 for phase 2 of the study—who were newly diagnosed with MM and 18 years of age or older. Patients had measurable disease, ECOG performance status of 0 to 2, and no grade 2 or higher peripheral neuropathy.
They received ixazomib (on days 1, 8, and 15) plus lenalidomide at 25 mg (on days 1 to 21) and dexamethasone at 40 mg (on days 1, 8, 15, and 22) for up to twelve 28-day cycles, followed by maintenance therapy with ixazomib alone.
In phase 1, patients received escalating doses of ixazomib, from 1.68 mg/m2 to 3.95 mg/m2, to establish the recommended dose for phase 2. The researchers established 2.97 mg/m2 as the maximum-tolerated dose and recommended the phase 2 dose be 2.23 mg/m2. This was converted to a 4.0 mg fixed dose based on population pharmacokinetic results.
Adverse events
The researchers said the combination was well tolerated, and most toxic effects were managed through dose modifications.
All patients reported at least one treatment-emergent adverse event, and 75% reported at least one treatment-emergent event that was grade 3 or higher.
Fifty-seven percent of patients had adverse events that led to dose reductions, including 53% of patients in the dose-escalation cohort and 58% of patients in the phase 2 cohort.
The most common adverse events resulting in dose reductions included skin and subcutaneous tissue disorders (20%), fatigue (14%), diarrhea (8%), peripheral neuropathy not elsewhere classified (8%), insomnia (6%), and increased body weight (6%). Five patients had adverse events leading to treatment discontinuation.
Two patients in the phase 2 cohort died while on study. One patient died of respiratory syncytial viral pneumonia that was thought to be treatment-related. The other patient died from cardiorespiratory arrest, which was considered not related to treatment.
Response and survival rates
Of the 64 response-evaluable patients, 92% responded to treatment. Fifty-eight percent had a partial response or better, and 27% had a complete response.
Responses deepened with an increasing number of treatment cycles. In the 25 patients continuing with maintenance therapy, 5 (20%) had an improvement in the depth of response during this phase.
The median duration of response has not been reached, but patients maintained responses for up to 2 years.
At last follow-up, 9 patients had progressed or died. The estimated 1-year progression-free survival was 88%, and 2-year progression-free survival was 67%.
The median overall survival has not been reached, but the estimated 1-year overall survival was 94%.
“The all-oral combination of weekly ixazomib plus lenalidomide and dexamethasone was generally well-tolerated and appeared active in patients with newly diagnosed multiple myeloma,” Dr Kumar said. “Our results support the development of a phase 3 trial studying this combination for multiple myeloma.” ![]()
Hospice cuts cost and use of care for cancer patients

Credit: CDC
Patients with advanced cancer receive less aggressive care and have lower healthcare costs during their last year of life if they use hospice care, according to research published in JAMA.
Patients who entered hospice had significantly lower rates of hospitalization, intensive care unit admissions, and invasive procedures, compared to patients who did not enter hospice.
Furthermore, patients who chose hospice were about 5 times less likely to die in hospitals and nursing homes.
“Our study shows very clearly that hospice matters,” said Ziad Obermeyer, MD, of Brigham and Women’s Hospital in Boston.
“Hospice and non-hospice patients had very similar patterns of healthcare utilization right up until the week of hospice enrollment. Then, the care started to look very different. Patients who didn’t enroll in hospice ended up with far more aggressive care in their last year of life, most of it related to acute complications like infections and organ failure, and not directly related to their cancer diagnosis.”
To conduct this study, Dr Obermeyer and his colleagues used data from Medicare beneficiaries with poor-prognosis cancers, including hematologic malignancies. The study included a nationally representative 20% sample of Medicare fee-for-service beneficiaries who died in 2011.
Among 86,851 patients, 51,924 (60%) entered hospice before death. Matching patients based on various criteria produced hospice and non-hospice groups, each with 18,165 patients. The median hospice duration was 11 days.
The researchers found that non-hospice patients had significantly greater healthcare utilization, largely for acute conditions not directly related to cancer.
This included rates of hospitalization (65% vs 42%), intensive care unit admissions (36% vs 15%), invasive procedures (51% vs 27%), and death in a hospital or nursing facility (74% vs 14%).
The costs of care for hospice and non-hospice patients were not significantly different before hospice care began. But they diverged sharply thereafter, contributing to a significant difference in total costs of $8697 over the last year of life—$71,517 for non-hospice patients and $62,819 for hospice patients.
“These findings highlight the importance of honest discussions between doctors and patients about our patients’ goals of their care at the end of life, relating to treatment decisions and quality of life,” Dr Obermeyer said. “This is of particular importance now, in light of the ongoing policy discussions around reimbursing providers for advance-care planning.” ![]()

Credit: CDC
Patients with advanced cancer receive less aggressive care and have lower healthcare costs during their last year of life if they use hospice care, according to research published in JAMA.
Patients who entered hospice had significantly lower rates of hospitalization, intensive care unit admissions, and invasive procedures, compared to patients who did not enter hospice.
Furthermore, patients who chose hospice were about 5 times less likely to die in hospitals and nursing homes.
“Our study shows very clearly that hospice matters,” said Ziad Obermeyer, MD, of Brigham and Women’s Hospital in Boston.
“Hospice and non-hospice patients had very similar patterns of healthcare utilization right up until the week of hospice enrollment. Then, the care started to look very different. Patients who didn’t enroll in hospice ended up with far more aggressive care in their last year of life, most of it related to acute complications like infections and organ failure, and not directly related to their cancer diagnosis.”
To conduct this study, Dr Obermeyer and his colleagues used data from Medicare beneficiaries with poor-prognosis cancers, including hematologic malignancies. The study included a nationally representative 20% sample of Medicare fee-for-service beneficiaries who died in 2011.
Among 86,851 patients, 51,924 (60%) entered hospice before death. Matching patients based on various criteria produced hospice and non-hospice groups, each with 18,165 patients. The median hospice duration was 11 days.
The researchers found that non-hospice patients had significantly greater healthcare utilization, largely for acute conditions not directly related to cancer.
This included rates of hospitalization (65% vs 42%), intensive care unit admissions (36% vs 15%), invasive procedures (51% vs 27%), and death in a hospital or nursing facility (74% vs 14%).
The costs of care for hospice and non-hospice patients were not significantly different before hospice care began. But they diverged sharply thereafter, contributing to a significant difference in total costs of $8697 over the last year of life—$71,517 for non-hospice patients and $62,819 for hospice patients.
“These findings highlight the importance of honest discussions between doctors and patients about our patients’ goals of their care at the end of life, relating to treatment decisions and quality of life,” Dr Obermeyer said. “This is of particular importance now, in light of the ongoing policy discussions around reimbursing providers for advance-care planning.” ![]()

Credit: CDC
Patients with advanced cancer receive less aggressive care and have lower healthcare costs during their last year of life if they use hospice care, according to research published in JAMA.
Patients who entered hospice had significantly lower rates of hospitalization, intensive care unit admissions, and invasive procedures, compared to patients who did not enter hospice.
Furthermore, patients who chose hospice were about 5 times less likely to die in hospitals and nursing homes.
“Our study shows very clearly that hospice matters,” said Ziad Obermeyer, MD, of Brigham and Women’s Hospital in Boston.
“Hospice and non-hospice patients had very similar patterns of healthcare utilization right up until the week of hospice enrollment. Then, the care started to look very different. Patients who didn’t enroll in hospice ended up with far more aggressive care in their last year of life, most of it related to acute complications like infections and organ failure, and not directly related to their cancer diagnosis.”
To conduct this study, Dr Obermeyer and his colleagues used data from Medicare beneficiaries with poor-prognosis cancers, including hematologic malignancies. The study included a nationally representative 20% sample of Medicare fee-for-service beneficiaries who died in 2011.
Among 86,851 patients, 51,924 (60%) entered hospice before death. Matching patients based on various criteria produced hospice and non-hospice groups, each with 18,165 patients. The median hospice duration was 11 days.
The researchers found that non-hospice patients had significantly greater healthcare utilization, largely for acute conditions not directly related to cancer.
This included rates of hospitalization (65% vs 42%), intensive care unit admissions (36% vs 15%), invasive procedures (51% vs 27%), and death in a hospital or nursing facility (74% vs 14%).
The costs of care for hospice and non-hospice patients were not significantly different before hospice care began. But they diverged sharply thereafter, contributing to a significant difference in total costs of $8697 over the last year of life—$71,517 for non-hospice patients and $62,819 for hospice patients.
“These findings highlight the importance of honest discussions between doctors and patients about our patients’ goals of their care at the end of life, relating to treatment decisions and quality of life,” Dr Obermeyer said. “This is of particular importance now, in light of the ongoing policy discussions around reimbursing providers for advance-care planning.”
Group develops cancer health literacy tool

patient and her father
Credit: Rhoda Baer
A new tool can identify patients with limited cancer health literacy, according to research published in the Journal of Health Communications.
The study authors noted that cancer patients are expected to play an active role in their care by adhering to medication regimens, distinguishing between scientifically credible medical evidence and misconceptions, and communicating with their providers about treatment decisions, risks, and survival rates.
However, patients with limited cancer health literacy can struggle with these responsibilities and potentially jeopardize their health by making uninformed decisions.
So Levent Dumenci, PhD, of Virginia Commonwealth University in Richmond, and his colleagues developed a tool to assess health literacy among cancer patients.
“Before now, there were only instruments that measured a particular aspect of general health literacy,” Dr Dumenci said. “It is important to have a tool that is specific to cancer because of the complex treatment options that cancer patients face, along with the increased demand for self-care.”
To meet that need, he and his colleagues developed the Cancer Health Literacy Test (CHLT)-30. The test, which is given via a touch-screen device, includes 30
questions about cancer treatment, medication side effects, and other cancer-related issues.
Six of the questions (CHLT-6) were specifically designed to quickly identify individuals with limited cancer health literacy.
The researchers tested the CHLT-30 in 1306 African American and Caucasian patients who were treated at oncology clinics in Virginia.
The team said the test accurately measured literacy and quickly identified patients with limited cancer health literacy. Eighteen percent of cancer patients had limited literacy, with an overrepresentation of African American, undereducated, and low-income patients.
“Using this tool, it takes just 1 to 2 minutes in the doctor’s office waiting room to identify patients with limited [cancer health literacy],” Dr Dumenci said. “Then, this information can be digitally communicated to the doctors prior to seeing the patients, so that they are prepared to talk with the patients in terms they can understand. This simple change could lead to big improvements in health outcomes.”
In future studies, the researchers hope to evaluate the cancer health literacy of Hispanic patients because prior research has pointed to disparities in this population’s health literacy.

patient and her father
Credit: Rhoda Baer
A new tool can identify patients with limited cancer health literacy, according to research published in the Journal of Health Communications.
The study authors noted that cancer patients are expected to play an active role in their care by adhering to medication regimens, distinguishing between scientifically credible medical evidence and misconceptions, and communicating with their providers about treatment decisions, risks, and survival rates.
However, patients with limited cancer health literacy can struggle with these responsibilities and potentially jeopardize their health by making uninformed decisions.
So Levent Dumenci, PhD, of Virginia Commonwealth University in Richmond, and his colleagues developed a tool to assess health literacy among cancer patients.
“Before now, there were only instruments that measured a particular aspect of general health literacy,” Dr Dumenci said. “It is important to have a tool that is specific to cancer because of the complex treatment options that cancer patients face, along with the increased demand for self-care.”
To meet that need, he and his colleagues developed the Cancer Health Literacy Test (CHLT)-30. The test, which is given via a touch-screen device, includes 30
questions about cancer treatment, medication side effects, and other cancer-related issues.
Six of the questions (CHLT-6) were specifically designed to quickly identify individuals with limited cancer health literacy.
The researchers tested the CHLT-30 in 1306 African American and Caucasian patients who were treated at oncology clinics in Virginia.
The team said the test accurately measured literacy and quickly identified patients with limited cancer health literacy. Eighteen percent of cancer patients had limited literacy, with an overrepresentation of African American, undereducated, and low-income patients.
“Using this tool, it takes just 1 to 2 minutes in the doctor’s office waiting room to identify patients with limited [cancer health literacy],” Dr Dumenci said. “Then, this information can be digitally communicated to the doctors prior to seeing the patients, so that they are prepared to talk with the patients in terms they can understand. This simple change could lead to big improvements in health outcomes.”
In future studies, the researchers hope to evaluate the cancer health literacy of Hispanic patients because prior research has pointed to disparities in this population’s health literacy.

patient and her father
Credit: Rhoda Baer
A new tool can identify patients with limited cancer health literacy, according to research published in the Journal of Health Communications.
The study authors noted that cancer patients are expected to play an active role in their care by adhering to medication regimens, distinguishing between scientifically credible medical evidence and misconceptions, and communicating with their providers about treatment decisions, risks, and survival rates.
However, patients with limited cancer health literacy can struggle with these responsibilities and potentially jeopardize their health by making uninformed decisions.
So Levent Dumenci, PhD, of Virginia Commonwealth University in Richmond, and his colleagues developed a tool to assess health literacy among cancer patients.
“Before now, there were only instruments that measured a particular aspect of general health literacy,” Dr Dumenci said. “It is important to have a tool that is specific to cancer because of the complex treatment options that cancer patients face, along with the increased demand for self-care.”
To meet that need, he and his colleagues developed the Cancer Health Literacy Test (CHLT)-30. The test, which is given via a touch-screen device, includes 30
questions about cancer treatment, medication side effects, and other cancer-related issues.
Six of the questions (CHLT-6) were specifically designed to quickly identify individuals with limited cancer health literacy.
The researchers tested the CHLT-30 in 1306 African American and Caucasian patients who were treated at oncology clinics in Virginia.
The team said the test accurately measured literacy and quickly identified patients with limited cancer health literacy. Eighteen percent of cancer patients had limited literacy, with an overrepresentation of African American, undereducated, and low-income patients.
“Using this tool, it takes just 1 to 2 minutes in the doctor’s office waiting room to identify patients with limited [cancer health literacy],” Dr Dumenci said. “Then, this information can be digitally communicated to the doctors prior to seeing the patients, so that they are prepared to talk with the patients in terms they can understand. This simple change could lead to big improvements in health outcomes.”
In future studies, the researchers hope to evaluate the cancer health literacy of Hispanic patients because prior research has pointed to disparities in this population’s health literacy.
Team pinpoints new target for MM therapy

Researchers say they’ve identified a promising therapeutic target for multiple myeloma (MM).
The group first discovered that MM patients have higher expression of proline-rich tyrosine kinase 2 (PYK2), a member of the focal adhesion kinase (FAK) family, compared to healthy individuals.
Then, preclinical experiments revealed that PYK2 plays a role in tumor progression, and inhibiting this kinase can impede MM cell growth.
Yu Zhang, PhD, of the Dana-Farber Cancer Institute in Boston, and colleagues reported these findings in Blood.
Comparing samples from MM patients and healthy controls, the researchers found that PYK2 is highly expressed in MM. The team even detected higher levels of PYK2 in patients with monoclonal gammopathy of unknown significance and smoldering myeloma.
Additional experiments helped the group elucidate PYK2’s role in MM, showing that the kinase promotes tumor progression by modulating the Wnt/β-catenin signaling pathway.
When the researchers inhibited PYK2, they observed a reduction in MM tumor growth in vivo as well as decreased cell proliferation, cell cycle progression, and adhesion ability in vitro.
In contrast, overexpression of PYK2 promoted the malignant phenotype, as evidenced by enhanced tumor growth and reduced survival in mouse models.
Finally, the researchers showed that a FAK/PYK2 inhibitor, VS-4718, inhibited MM cell growth both in vitro and in vivo.
“In addition to this work recently published by our collaborators at the Dana-Farber Cancer Institute, we have been conducting further research and collaborating with scientific leaders to understand the potential of cancer stem cell inhibitors in hematological malignancies,” said Jonathan Pachter, PhD, head of research at Verastem, Inc., the company developing VS-4781.
“We believe that inhibitors of FAK and PYK2, such as VS-4718, may be useful in the treatment of many types of cancer, particularly where there is minimal residual disease with enrichment of cancer stem cells following chemotherapy. We and our collaborators will be presenting additional research at the upcoming American Society of Hematology in December.”
VS-4718 is being evaluated in a phase 1 dose-escalation trial in patients with advanced solid tumors. Another phase 1 trial in hematological malignancies is set to begin in the first quarter of 2015.

Researchers say they’ve identified a promising therapeutic target for multiple myeloma (MM).
The group first discovered that MM patients have higher expression of proline-rich tyrosine kinase 2 (PYK2), a member of the focal adhesion kinase (FAK) family, compared to healthy individuals.
Then, preclinical experiments revealed that PYK2 plays a role in tumor progression, and inhibiting this kinase can impede MM cell growth.
Yu Zhang, PhD, of the Dana-Farber Cancer Institute in Boston, and colleagues reported these findings in Blood.
Comparing samples from MM patients and healthy controls, the researchers found that PYK2 is highly expressed in MM. The team even detected higher levels of PYK2 in patients with monoclonal gammopathy of unknown significance and smoldering myeloma.
Additional experiments helped the group elucidate PYK2’s role in MM, showing that the kinase promotes tumor progression by modulating the Wnt/β-catenin signaling pathway.
When the researchers inhibited PYK2, they observed a reduction in MM tumor growth in vivo as well as decreased cell proliferation, cell cycle progression, and adhesion ability in vitro.
In contrast, overexpression of PYK2 promoted the malignant phenotype, as evidenced by enhanced tumor growth and reduced survival in mouse models.
Finally, the researchers showed that a FAK/PYK2 inhibitor, VS-4718, inhibited MM cell growth both in vitro and in vivo.
“In addition to this work recently published by our collaborators at the Dana-Farber Cancer Institute, we have been conducting further research and collaborating with scientific leaders to understand the potential of cancer stem cell inhibitors in hematological malignancies,” said Jonathan Pachter, PhD, head of research at Verastem, Inc., the company developing VS-4781.
“We believe that inhibitors of FAK and PYK2, such as VS-4718, may be useful in the treatment of many types of cancer, particularly where there is minimal residual disease with enrichment of cancer stem cells following chemotherapy. We and our collaborators will be presenting additional research at the upcoming American Society of Hematology in December.”
VS-4718 is being evaluated in a phase 1 dose-escalation trial in patients with advanced solid tumors. Another phase 1 trial in hematological malignancies is set to begin in the first quarter of 2015.

Researchers say they’ve identified a promising therapeutic target for multiple myeloma (MM).
The group first discovered that MM patients have higher expression of proline-rich tyrosine kinase 2 (PYK2), a member of the focal adhesion kinase (FAK) family, compared to healthy individuals.
Then, preclinical experiments revealed that PYK2 plays a role in tumor progression, and inhibiting this kinase can impede MM cell growth.
Yu Zhang, PhD, of the Dana-Farber Cancer Institute in Boston, and colleagues reported these findings in Blood.
Comparing samples from MM patients and healthy controls, the researchers found that PYK2 is highly expressed in MM. The team even detected higher levels of PYK2 in patients with monoclonal gammopathy of unknown significance and smoldering myeloma.
Additional experiments helped the group elucidate PYK2’s role in MM, showing that the kinase promotes tumor progression by modulating the Wnt/β-catenin signaling pathway.
When the researchers inhibited PYK2, they observed a reduction in MM tumor growth in vivo as well as decreased cell proliferation, cell cycle progression, and adhesion ability in vitro.
In contrast, overexpression of PYK2 promoted the malignant phenotype, as evidenced by enhanced tumor growth and reduced survival in mouse models.
Finally, the researchers showed that a FAK/PYK2 inhibitor, VS-4718, inhibited MM cell growth both in vitro and in vivo.
“In addition to this work recently published by our collaborators at the Dana-Farber Cancer Institute, we have been conducting further research and collaborating with scientific leaders to understand the potential of cancer stem cell inhibitors in hematological malignancies,” said Jonathan Pachter, PhD, head of research at Verastem, Inc., the company developing VS-4781.
“We believe that inhibitors of FAK and PYK2, such as VS-4718, may be useful in the treatment of many types of cancer, particularly where there is minimal residual disease with enrichment of cancer stem cells following chemotherapy. We and our collaborators will be presenting additional research at the upcoming American Society of Hematology in December.”
VS-4718 is being evaluated in a phase 1 dose-escalation trial in patients with advanced solid tumors. Another phase 1 trial in hematological malignancies is set to begin in the first quarter of 2015.