User login
Paraneoplastic Autoimmune Multiorgan Syndrome Proves Rapidly Fatal
The skin may hold the key to differentiating classic pemphigus from the heterogenous autoimmune syndrome known as paraneoplastic autoimmune multiorgan syndrome.
It is a distinction of critical prognostic importance, because paraneoplastic autoimmune multiorgan syndrome (PAMS) typically is rapidly fatal, according to Dr. Sergei A. Grando, professor of dermatology and biologic chemistry at the University of California, Irvine. "The vast majority of patients die within several months of diagnosis, usually due to infections or respiratory failure, often taking the form of multiorgan system failure."
Two-thirds of patients with PAMS have a known internal malignancy at the time of their first mucocutaneous eruption. The most common of these neoplasms are non-Hodgkin’s lymphoma, which is present in more than 40% of PAMS patients; chronic lymphocytic leukemia, present in 30%; Castleman disease, present in 10%; and thymoma, present in 6%.
When a patient meets the diagnostic criteria for PAMS without having a known cancer, it is appropriate to launch a search for hidden malignancy, said Dr. Grando.
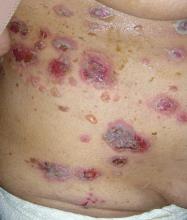
A key distinction between the skin lesions of PAMS and classic pemphigus is that PAMS involves inflammatory macules, papules, plaques, and blisters occurring on an inflammatory background over the trunk and extremities, including the palms and soles, but sparing the scalp.
In contrast, the generally more vesicular blisters and crusted erosions of pemphigus vulgaris display little erythema and usually occur on a noninflammatory background on the scalp, trunk, and extremities (but sparing the palms and soles). The most common location for skin lesions in PAMS is the palms; in pemphigus vulgaris, it is the scalp.
Also, Nikolsky's sign is positive in pemphigus vulgaris, but negative in PAMS, added Dr. Grando, who was among the investigators who first described PAMS a decade ago (Arch. Dermatol. 2001;137:193-206).
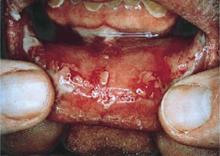
PAMS is characterized by severe and diffuse oral mucous membrane involvement, with persistent painful stomatitis because of blisters and erosions, and frequent involvement of other mucous membranes, including the eyes and genitalia. Cicatrizing conjunctivitis is particularly common in PAMS. In contrast, oral mucous membrane involvement in pemphigus is more discrete, with the eyes or other nonoral mucosa rarely involved.
Another key in the differential diagnosis: PAMS is associated with the HLA-DRB1*03 allele, whereas pemphigus vulgaris and foliaceous are strongly associated with the -04 and -14 alleles, respectively.
A hallmark of PAMS is respiratory involvement, with the sloughing of bronchial epithelial cells contributing to small airway occlusion and bronchiolitis obliterans. Classic pemphigus is free of respiratory involvement.
Both the esophagus and colon may be involved in PAMS, whereas only the esophagus is affected in pemphigus vulgaris.
In a published series of 28 PAMS patients, painful and generalized oral stomatitis was present in all 28, respiratory involvement was in 26, death from respiratory failure occurred in 22, and lichenoid skin involvement was present in 19. Only seven patients had no skin lesions (Br. J. Dermatol. 2003;149:1143-51).
At least five different subtypes of PAMS can be distinguished on the basis of the skin disease manifestations they most resemble. These subtypes of pemphiguslike PAMS include paraneoplastic pemphigus, bullous pemphigoid–like, erythema multiforme–like, lichen planus–like, and graft-vs.-host-disease–like versions of PAMS.
Dr. Grando eschews the term "paraneoplastic pemphigus" as too restrictive. After all, true pemphigus doesn’t usually affect the lungs, he noted.
Whereas most patients with classic pemphigus respond well to high-dose corticosteroids and recalcitrant disease can be effectively treated with cytotoxic agents, cyclosporine, intravenous gamma globulin, and other second-line agents, PAMS is resistant to all conventional forms of therapy.
"What can we offer? Really not much," Dr. Grando said during his presentation at the World Congress of Dermatology in Seoul, South Korea.
The preferred treatment regimen is a combination of prednisone and cyclosporine, with or without cyclophosphamide. Monthly courses of IVIG can buy patients a few extra months, he added.
Dr. Grando declared having no relevant financial interests.
The skin may hold the key to differentiating classic pemphigus from the heterogenous autoimmune syndrome known as paraneoplastic autoimmune multiorgan syndrome.
It is a distinction of critical prognostic importance, because paraneoplastic autoimmune multiorgan syndrome (PAMS) typically is rapidly fatal, according to Dr. Sergei A. Grando, professor of dermatology and biologic chemistry at the University of California, Irvine. "The vast majority of patients die within several months of diagnosis, usually due to infections or respiratory failure, often taking the form of multiorgan system failure."
Two-thirds of patients with PAMS have a known internal malignancy at the time of their first mucocutaneous eruption. The most common of these neoplasms are non-Hodgkin’s lymphoma, which is present in more than 40% of PAMS patients; chronic lymphocytic leukemia, present in 30%; Castleman disease, present in 10%; and thymoma, present in 6%.
When a patient meets the diagnostic criteria for PAMS without having a known cancer, it is appropriate to launch a search for hidden malignancy, said Dr. Grando.
A key distinction between the skin lesions of PAMS and classic pemphigus is that PAMS involves inflammatory macules, papules, plaques, and blisters occurring on an inflammatory background over the trunk and extremities, including the palms and soles, but sparing the scalp.
In contrast, the generally more vesicular blisters and crusted erosions of pemphigus vulgaris display little erythema and usually occur on a noninflammatory background on the scalp, trunk, and extremities (but sparing the palms and soles). The most common location for skin lesions in PAMS is the palms; in pemphigus vulgaris, it is the scalp.
Also, Nikolsky's sign is positive in pemphigus vulgaris, but negative in PAMS, added Dr. Grando, who was among the investigators who first described PAMS a decade ago (Arch. Dermatol. 2001;137:193-206).
PAMS is characterized by severe and diffuse oral mucous membrane involvement, with persistent painful stomatitis because of blisters and erosions, and frequent involvement of other mucous membranes, including the eyes and genitalia. Cicatrizing conjunctivitis is particularly common in PAMS. In contrast, oral mucous membrane involvement in pemphigus is more discrete, with the eyes or other nonoral mucosa rarely involved.
Another key in the differential diagnosis: PAMS is associated with the HLA-DRB1*03 allele, whereas pemphigus vulgaris and foliaceous are strongly associated with the -04 and -14 alleles, respectively.
A hallmark of PAMS is respiratory involvement, with the sloughing of bronchial epithelial cells contributing to small airway occlusion and bronchiolitis obliterans. Classic pemphigus is free of respiratory involvement.
Both the esophagus and colon may be involved in PAMS, whereas only the esophagus is affected in pemphigus vulgaris.
In a published series of 28 PAMS patients, painful and generalized oral stomatitis was present in all 28, respiratory involvement was in 26, death from respiratory failure occurred in 22, and lichenoid skin involvement was present in 19. Only seven patients had no skin lesions (Br. J. Dermatol. 2003;149:1143-51).
At least five different subtypes of PAMS can be distinguished on the basis of the skin disease manifestations they most resemble. These subtypes of pemphiguslike PAMS include paraneoplastic pemphigus, bullous pemphigoid–like, erythema multiforme–like, lichen planus–like, and graft-vs.-host-disease–like versions of PAMS.
Dr. Grando eschews the term "paraneoplastic pemphigus" as too restrictive. After all, true pemphigus doesn’t usually affect the lungs, he noted.
Whereas most patients with classic pemphigus respond well to high-dose corticosteroids and recalcitrant disease can be effectively treated with cytotoxic agents, cyclosporine, intravenous gamma globulin, and other second-line agents, PAMS is resistant to all conventional forms of therapy.
"What can we offer? Really not much," Dr. Grando said during his presentation at the World Congress of Dermatology in Seoul, South Korea.
The preferred treatment regimen is a combination of prednisone and cyclosporine, with or without cyclophosphamide. Monthly courses of IVIG can buy patients a few extra months, he added.
Dr. Grando declared having no relevant financial interests.
The skin may hold the key to differentiating classic pemphigus from the heterogenous autoimmune syndrome known as paraneoplastic autoimmune multiorgan syndrome.
It is a distinction of critical prognostic importance, because paraneoplastic autoimmune multiorgan syndrome (PAMS) typically is rapidly fatal, according to Dr. Sergei A. Grando, professor of dermatology and biologic chemistry at the University of California, Irvine. "The vast majority of patients die within several months of diagnosis, usually due to infections or respiratory failure, often taking the form of multiorgan system failure."
Two-thirds of patients with PAMS have a known internal malignancy at the time of their first mucocutaneous eruption. The most common of these neoplasms are non-Hodgkin’s lymphoma, which is present in more than 40% of PAMS patients; chronic lymphocytic leukemia, present in 30%; Castleman disease, present in 10%; and thymoma, present in 6%.
When a patient meets the diagnostic criteria for PAMS without having a known cancer, it is appropriate to launch a search for hidden malignancy, said Dr. Grando.
A key distinction between the skin lesions of PAMS and classic pemphigus is that PAMS involves inflammatory macules, papules, plaques, and blisters occurring on an inflammatory background over the trunk and extremities, including the palms and soles, but sparing the scalp.
In contrast, the generally more vesicular blisters and crusted erosions of pemphigus vulgaris display little erythema and usually occur on a noninflammatory background on the scalp, trunk, and extremities (but sparing the palms and soles). The most common location for skin lesions in PAMS is the palms; in pemphigus vulgaris, it is the scalp.
Also, Nikolsky's sign is positive in pemphigus vulgaris, but negative in PAMS, added Dr. Grando, who was among the investigators who first described PAMS a decade ago (Arch. Dermatol. 2001;137:193-206).
PAMS is characterized by severe and diffuse oral mucous membrane involvement, with persistent painful stomatitis because of blisters and erosions, and frequent involvement of other mucous membranes, including the eyes and genitalia. Cicatrizing conjunctivitis is particularly common in PAMS. In contrast, oral mucous membrane involvement in pemphigus is more discrete, with the eyes or other nonoral mucosa rarely involved.
Another key in the differential diagnosis: PAMS is associated with the HLA-DRB1*03 allele, whereas pemphigus vulgaris and foliaceous are strongly associated with the -04 and -14 alleles, respectively.
A hallmark of PAMS is respiratory involvement, with the sloughing of bronchial epithelial cells contributing to small airway occlusion and bronchiolitis obliterans. Classic pemphigus is free of respiratory involvement.
Both the esophagus and colon may be involved in PAMS, whereas only the esophagus is affected in pemphigus vulgaris.
In a published series of 28 PAMS patients, painful and generalized oral stomatitis was present in all 28, respiratory involvement was in 26, death from respiratory failure occurred in 22, and lichenoid skin involvement was present in 19. Only seven patients had no skin lesions (Br. J. Dermatol. 2003;149:1143-51).
At least five different subtypes of PAMS can be distinguished on the basis of the skin disease manifestations they most resemble. These subtypes of pemphiguslike PAMS include paraneoplastic pemphigus, bullous pemphigoid–like, erythema multiforme–like, lichen planus–like, and graft-vs.-host-disease–like versions of PAMS.
Dr. Grando eschews the term "paraneoplastic pemphigus" as too restrictive. After all, true pemphigus doesn’t usually affect the lungs, he noted.
Whereas most patients with classic pemphigus respond well to high-dose corticosteroids and recalcitrant disease can be effectively treated with cytotoxic agents, cyclosporine, intravenous gamma globulin, and other second-line agents, PAMS is resistant to all conventional forms of therapy.
"What can we offer? Really not much," Dr. Grando said during his presentation at the World Congress of Dermatology in Seoul, South Korea.
The preferred treatment regimen is a combination of prednisone and cyclosporine, with or without cyclophosphamide. Monthly courses of IVIG can buy patients a few extra months, he added.
Dr. Grando declared having no relevant financial interests.
Multifocal bone infarctions in both knees: An unusual presentation of multiple myeloma
Ying-Kei Hui, MD,1 Thomas Slattery, MD,2 Dale M. Frank, MD,3 Carol Dolinskas, MD,4 and David Henry, MD, FACP5
Departments of 1Internal Medicine, Pennsylvania Hospital; 2Radiology, Pennsylvania Hospital; 3Pathology and Laboratory Medicine, Hospital of the University of Pennsylvania; 4Nuclear Medicine, Diagnostic Radiology, Pennsylvania Hospital; and 5Medicine, Pennsylvania Hospital, Philadelphia, PA
Multiple myeloma (MM) is a neoplastic proliferation of monoclonal plasma cells within the bone marrow, which overproduces immunoglobulin. This disorder accounts for approximately 1% of all reported neoplasms and 12%– 15% of all hematologic malignancies.1 It is the second most common hematologic malignancy diagnosed.2 The etiology is still not fully understood. MM typically affects older patients, ranging from 50–78 years (median, 61 years).3 Common clinical presentations include fatigue, anemia, renal failure, hypercalcemia, bone pain, and pathologic fractures.
Bone involvement in MM may vary at presentation. Most commonly, radiographic findings include multiple small, sharply defined, lytic, “punched-out” lesions without reactive bone formation, arising in the medullary cavity at sites of preserved hematopoiesis in adults (the axial skeleton). The pathophysiology of the bone findings is uncertain, though presumed to be resultant of either inhibition of osteoblastic activity and/ or activation of osteoclastic activity. Involvement of the cortex results in endosteal scalloping, with invasion of the periosteum and occasionally extraosseous extension. Lesions are most commonly seen in the vertebrae, ribs, skull, pelvic bones, and femur, in descending order of prevalence. Distal bone involvement is less common, though cases with predominant involvement in peripheral bones have been described. Uncommon radiographic presentations include diffuse skeletal osteopenia without focal lesions or sclerotic lesions. 4,5 To our knowledge, multiple bone infarcts as a complication of MM have not been reported in the medical literature.
Case presentation
A 47-year-old man with no significant medical history presented after the recent onset of painless hematuria, which spontaneously resolved after 2 days. He complained of left knee pain, which he noted after doing yard work.
Routine laboratory examination showed normocytic normochromic anemia, with a hemoglobin level of 11.5 g/dL and a mildly elevated alkaline phosphatase (ALP) level at 124 units/L. An MRI of the left knee showed increased red bone marrow within the distal femur and proximal tibia/fibula, initially thought to be compatible with anemia from an unexplained inflammatory process. Further urologic and gastroenterologic workup was negative.
Several months later, our patient was noted to have progressive fatigue, with a decrease in hemoglobin level to 10.6 g/dL and a mildly elevated erythrocyte sedimentation rate. Physical examination was otherwise unremarkable. A repeat MRI of both knees showed an extensive marrow infiltrative process, with multiple presumed secondary bone infarcts in the distal femora and proximal tibias, proximal fibulae, and patellae (Figure 1). A tandem skeletal survey showed mild diffuse osteopenia and several small, rounded, lytic foci in the skull (Figure 2), which were suspicious for MM. No focal radiographic lesions were seen (Figure 3).
Bone marrow biopsy from the left posterior iliac crest revealed hypocellular marrow (20%). An expansion of plasmacytoid cells with eccentrically placed, round nuclei, clumped chromatin, occasional nucleoli, and moderate amounts of eosinophilic cytoplasm accounted for 75% of the marrow cellularity. An aspirate smear demonstrated scattered mature plasma cells, accounting for roughly 15% of the total cellularity. Flow cytometry showed no overt evidence of marrow involvement by a lymphocytic clone. Bone biopsy was not performed in the areas of the knees seen to be abnormal on MRI examination.
Serum protein electrophoresis (SPEP) showed a band in the betagamma region. Immunofixation confirmed the presence of a monoclonal paraprotein, consisting predominantly of immunoglobulin A (IgA) heavy chain and kappa light chain. A bone marrow biopsy and aspirate showed replacement of most hematopoietic elements by sheets of mature plasma cells, accounting for 75% of the total marrow cellularity (Figure 4). Confirmatory immunostains were positive for CD138, CD117, and kappa light chain (Figure 5) and negative for CD79a and lambda light chain (Figure 6). A diagnosis of MM was made based on the finding of M protein in the urine, the presence of greater than 10% clonal plasma cells in bone marrow, and related clinical symptomatology (including anemia and hypercalcemia).
The patient was started on immunomodulating therapy with lenalidomide (Revlimid), bortezomib (Velcade), and dexamethasone. Autologous stem cell transplantation may be considered after appropriate treatment.
Discussion
We offer the case of a patient with MM who presented with bilateral knee infarcts. Synonyms of bone infarct include osteonecrosis, bone necrosis, avascular necrosis, aseptic necrosis, ischemic bone necrosis, and bone death.6 MRI is the most sensitive imaging modality for evaluation of the bone marrow. It can detect early osteonecrotic changes in bones well before they are visible on radiography7; this fact was exemplified in our case, in which the patient had only mild osteopenia on knee radiographs but extensive osteonecrotic changes on MRI examination.
Bone infarct more commonly involves the hips than the knees.7 Knee involvement can be differentiated into two main categories: primary and secondary. Primary, spontaneous, or idiopathic involvement tends to be unilateral and usually is seen in the elderly, although the recent literature suggests that many of these socalled spontaneous cases are actually secondary to subcortical microfractures, which are then complicated by osteonecrosis.5 Secondary causes tend to present at a younger age, with bilateral and multifocal involvement. Examples of secondary causes include steroid therapy, alcoholism, decompression syndrome, hemoglobinopathies (sickle cell disease), autoimmune disease (lupus and antiphospholipid disease), infections (human immunodeficiency virus), radiation, and trauma.8–15 Other causes, such as chemotherapy toxicity in pediatric leukemia16 and Gaucher disease, have been reported.7 Osteonecrosis of the jaw is a known treatment complication of bisphosphonate therapy in patients with MM17; however, there have been no previous reports describing the presentation of multifocal bone infarcts in both knees in patients with MM.
Although the pathogenesis of bone infarction is unclear, it is thought to be caused by the combined effects of systemic and local factors affecting the blood supply, vascular damage, increased intraosseous pressure, and mechanical stresses. These processes lead to compromise of the bone vasculature, resulting in the death of bone and marrow cells.9 In our case, MRI of both knees revealed an extensive marrow infiltrative process, which may have caused local vasculature damage and diminished blood supply resulting in bone infarctions.
Conclusion
Bone infarction of any joint is not a well-established complication of MM. Physicians should be aware of this potential presentation. Although there is no cure for MM, early recognition of MM can lead to more effective treatment, thus slowing disease progression and improving overall clinical outcomes.
Disclosures
The authors have no conflicts of interest to disclose.
References
1. Phekoo KJ, Schey SA, Richards MA, et al. A population study to define the incidence and survival of multiple myeloma in a National Health Service Region in UK. Br J Haematol 2004;127:299–304.
2. Esteve FR, Roodman GD. Pathophysiology of myeloma bone disease. Best Pract Res Clin Haematol 2007;20:613–624.
3. Jain M, Ascensao J, Schechter GP. Familial myeloma and monoclonal gammopathy: a report of eight African American families. Am J Hematol 2009;84:34–38.
4. Winterbottom AP, Shaw AS. Imaging patients with myeloma. Clin Radiol 2009;64:1–11.
5. Resnick D. Diagnosis of Bone and Joint Disorders. Philadelphia, PA: WB Saunders; 2002:2188–2233.
6. Stoller D, Tirman P, Bredella M, Branstetter R. Diagnostic Imaging: Orthopaedics. Philadelphia, PA: WB Saunders; 2003:82.
7. Assouline-Dayan Y, Chang C, Greenspan A, Shoenfeld Y, Gershwin ME. Pathogenesis and natural history of osteonecrosis. Semin Arthritis Rheum 2002;32:94–124.
8. Patel DV, Breazeale NM, Behr CT, Warren RF, Wickiewicz TL, O’Brien SJ. Osteonecrosis of the knee: current clinical concepts. Knee Surg Sports Traumatol Arthrosc 1998;6:2–11.
9. Chang CC, Greenspan A, Gershwin ME. Osteonecrosis: current perspectives on pathogenesis and treatment. Semin Arthritis Rheum 1993;23:47–69.
10. Jones LC, Mont MA, Le TB, et al. Procoagulants and osteonecrosis. J Rheumatol 2003; 30:783–791.
11. Saito N, Nadgir RN, Flower EN, Sakai O. Clinical and radiologic manifestations of sickle cell disease in the head and neck. Radiographics 2010;30:1021–1034.
12. Miller KD, Masur H, Jones EC, et al. High prevalence of osteonecrosis of the femoral head in HIV-infected adults. Ann Intern Med 2002;137:17–25.
13. Mendenhall WM. Mandibular: osteoradionecrosis. J Clin Oncol 2004;22:4867–4868.
14. Mok MY, Farewell VT, Isenberg DA. Risk factors for avascular necrosis of bone in patients with systemic lupus erythematosus: is there a role for antiphospholipid antibodies? Ann Rheum Dis 2000;59:462–467.
15. Kelman GJ, Williams GW, Colwell CW Jr, Walker RH. Steroid-related osteonecrosis of the knee: two case reports and a literature review. Clin Orthop Relat Res 1990;257:171–176.
16. Karimova EJ, Wozniak A, Wu J, Neel MD, Kaste SC. How does osteonecrosis about the knee progress in young patients with leukemia? A 2- to 7-year study. Clin Orthop Relat Res 2010;468:2454–2459.
17. Cafro AM, Barbarano L, Nosari AM, et al. Osteonecrosis of the jaw in patients with multiple myeloma treated with bisphosphonates: definition and management of the risk related to zoledronic acid. Clin Lymphoma Myeloma 2008;8:111–116.
Ying-Kei Hui, MD,1 Thomas Slattery, MD,2 Dale M. Frank, MD,3 Carol Dolinskas, MD,4 and David Henry, MD, FACP5
Departments of 1Internal Medicine, Pennsylvania Hospital; 2Radiology, Pennsylvania Hospital; 3Pathology and Laboratory Medicine, Hospital of the University of Pennsylvania; 4Nuclear Medicine, Diagnostic Radiology, Pennsylvania Hospital; and 5Medicine, Pennsylvania Hospital, Philadelphia, PA
Multiple myeloma (MM) is a neoplastic proliferation of monoclonal plasma cells within the bone marrow, which overproduces immunoglobulin. This disorder accounts for approximately 1% of all reported neoplasms and 12%– 15% of all hematologic malignancies.1 It is the second most common hematologic malignancy diagnosed.2 The etiology is still not fully understood. MM typically affects older patients, ranging from 50–78 years (median, 61 years).3 Common clinical presentations include fatigue, anemia, renal failure, hypercalcemia, bone pain, and pathologic fractures.
Bone involvement in MM may vary at presentation. Most commonly, radiographic findings include multiple small, sharply defined, lytic, “punched-out” lesions without reactive bone formation, arising in the medullary cavity at sites of preserved hematopoiesis in adults (the axial skeleton). The pathophysiology of the bone findings is uncertain, though presumed to be resultant of either inhibition of osteoblastic activity and/ or activation of osteoclastic activity. Involvement of the cortex results in endosteal scalloping, with invasion of the periosteum and occasionally extraosseous extension. Lesions are most commonly seen in the vertebrae, ribs, skull, pelvic bones, and femur, in descending order of prevalence. Distal bone involvement is less common, though cases with predominant involvement in peripheral bones have been described. Uncommon radiographic presentations include diffuse skeletal osteopenia without focal lesions or sclerotic lesions. 4,5 To our knowledge, multiple bone infarcts as a complication of MM have not been reported in the medical literature.
Case presentation
A 47-year-old man with no significant medical history presented after the recent onset of painless hematuria, which spontaneously resolved after 2 days. He complained of left knee pain, which he noted after doing yard work.
Routine laboratory examination showed normocytic normochromic anemia, with a hemoglobin level of 11.5 g/dL and a mildly elevated alkaline phosphatase (ALP) level at 124 units/L. An MRI of the left knee showed increased red bone marrow within the distal femur and proximal tibia/fibula, initially thought to be compatible with anemia from an unexplained inflammatory process. Further urologic and gastroenterologic workup was negative.
Several months later, our patient was noted to have progressive fatigue, with a decrease in hemoglobin level to 10.6 g/dL and a mildly elevated erythrocyte sedimentation rate. Physical examination was otherwise unremarkable. A repeat MRI of both knees showed an extensive marrow infiltrative process, with multiple presumed secondary bone infarcts in the distal femora and proximal tibias, proximal fibulae, and patellae (Figure 1). A tandem skeletal survey showed mild diffuse osteopenia and several small, rounded, lytic foci in the skull (Figure 2), which were suspicious for MM. No focal radiographic lesions were seen (Figure 3).
Bone marrow biopsy from the left posterior iliac crest revealed hypocellular marrow (20%). An expansion of plasmacytoid cells with eccentrically placed, round nuclei, clumped chromatin, occasional nucleoli, and moderate amounts of eosinophilic cytoplasm accounted for 75% of the marrow cellularity. An aspirate smear demonstrated scattered mature plasma cells, accounting for roughly 15% of the total cellularity. Flow cytometry showed no overt evidence of marrow involvement by a lymphocytic clone. Bone biopsy was not performed in the areas of the knees seen to be abnormal on MRI examination.
Serum protein electrophoresis (SPEP) showed a band in the betagamma region. Immunofixation confirmed the presence of a monoclonal paraprotein, consisting predominantly of immunoglobulin A (IgA) heavy chain and kappa light chain. A bone marrow biopsy and aspirate showed replacement of most hematopoietic elements by sheets of mature plasma cells, accounting for 75% of the total marrow cellularity (Figure 4). Confirmatory immunostains were positive for CD138, CD117, and kappa light chain (Figure 5) and negative for CD79a and lambda light chain (Figure 6). A diagnosis of MM was made based on the finding of M protein in the urine, the presence of greater than 10% clonal plasma cells in bone marrow, and related clinical symptomatology (including anemia and hypercalcemia).
The patient was started on immunomodulating therapy with lenalidomide (Revlimid), bortezomib (Velcade), and dexamethasone. Autologous stem cell transplantation may be considered after appropriate treatment.
Discussion
We offer the case of a patient with MM who presented with bilateral knee infarcts. Synonyms of bone infarct include osteonecrosis, bone necrosis, avascular necrosis, aseptic necrosis, ischemic bone necrosis, and bone death.6 MRI is the most sensitive imaging modality for evaluation of the bone marrow. It can detect early osteonecrotic changes in bones well before they are visible on radiography7; this fact was exemplified in our case, in which the patient had only mild osteopenia on knee radiographs but extensive osteonecrotic changes on MRI examination.
Bone infarct more commonly involves the hips than the knees.7 Knee involvement can be differentiated into two main categories: primary and secondary. Primary, spontaneous, or idiopathic involvement tends to be unilateral and usually is seen in the elderly, although the recent literature suggests that many of these socalled spontaneous cases are actually secondary to subcortical microfractures, which are then complicated by osteonecrosis.5 Secondary causes tend to present at a younger age, with bilateral and multifocal involvement. Examples of secondary causes include steroid therapy, alcoholism, decompression syndrome, hemoglobinopathies (sickle cell disease), autoimmune disease (lupus and antiphospholipid disease), infections (human immunodeficiency virus), radiation, and trauma.8–15 Other causes, such as chemotherapy toxicity in pediatric leukemia16 and Gaucher disease, have been reported.7 Osteonecrosis of the jaw is a known treatment complication of bisphosphonate therapy in patients with MM17; however, there have been no previous reports describing the presentation of multifocal bone infarcts in both knees in patients with MM.
Although the pathogenesis of bone infarction is unclear, it is thought to be caused by the combined effects of systemic and local factors affecting the blood supply, vascular damage, increased intraosseous pressure, and mechanical stresses. These processes lead to compromise of the bone vasculature, resulting in the death of bone and marrow cells.9 In our case, MRI of both knees revealed an extensive marrow infiltrative process, which may have caused local vasculature damage and diminished blood supply resulting in bone infarctions.
Conclusion
Bone infarction of any joint is not a well-established complication of MM. Physicians should be aware of this potential presentation. Although there is no cure for MM, early recognition of MM can lead to more effective treatment, thus slowing disease progression and improving overall clinical outcomes.
Disclosures
The authors have no conflicts of interest to disclose.
References
1. Phekoo KJ, Schey SA, Richards MA, et al. A population study to define the incidence and survival of multiple myeloma in a National Health Service Region in UK. Br J Haematol 2004;127:299–304.
2. Esteve FR, Roodman GD. Pathophysiology of myeloma bone disease. Best Pract Res Clin Haematol 2007;20:613–624.
3. Jain M, Ascensao J, Schechter GP. Familial myeloma and monoclonal gammopathy: a report of eight African American families. Am J Hematol 2009;84:34–38.
4. Winterbottom AP, Shaw AS. Imaging patients with myeloma. Clin Radiol 2009;64:1–11.
5. Resnick D. Diagnosis of Bone and Joint Disorders. Philadelphia, PA: WB Saunders; 2002:2188–2233.
6. Stoller D, Tirman P, Bredella M, Branstetter R. Diagnostic Imaging: Orthopaedics. Philadelphia, PA: WB Saunders; 2003:82.
7. Assouline-Dayan Y, Chang C, Greenspan A, Shoenfeld Y, Gershwin ME. Pathogenesis and natural history of osteonecrosis. Semin Arthritis Rheum 2002;32:94–124.
8. Patel DV, Breazeale NM, Behr CT, Warren RF, Wickiewicz TL, O’Brien SJ. Osteonecrosis of the knee: current clinical concepts. Knee Surg Sports Traumatol Arthrosc 1998;6:2–11.
9. Chang CC, Greenspan A, Gershwin ME. Osteonecrosis: current perspectives on pathogenesis and treatment. Semin Arthritis Rheum 1993;23:47–69.
10. Jones LC, Mont MA, Le TB, et al. Procoagulants and osteonecrosis. J Rheumatol 2003; 30:783–791.
11. Saito N, Nadgir RN, Flower EN, Sakai O. Clinical and radiologic manifestations of sickle cell disease in the head and neck. Radiographics 2010;30:1021–1034.
12. Miller KD, Masur H, Jones EC, et al. High prevalence of osteonecrosis of the femoral head in HIV-infected adults. Ann Intern Med 2002;137:17–25.
13. Mendenhall WM. Mandibular: osteoradionecrosis. J Clin Oncol 2004;22:4867–4868.
14. Mok MY, Farewell VT, Isenberg DA. Risk factors for avascular necrosis of bone in patients with systemic lupus erythematosus: is there a role for antiphospholipid antibodies? Ann Rheum Dis 2000;59:462–467.
15. Kelman GJ, Williams GW, Colwell CW Jr, Walker RH. Steroid-related osteonecrosis of the knee: two case reports and a literature review. Clin Orthop Relat Res 1990;257:171–176.
16. Karimova EJ, Wozniak A, Wu J, Neel MD, Kaste SC. How does osteonecrosis about the knee progress in young patients with leukemia? A 2- to 7-year study. Clin Orthop Relat Res 2010;468:2454–2459.
17. Cafro AM, Barbarano L, Nosari AM, et al. Osteonecrosis of the jaw in patients with multiple myeloma treated with bisphosphonates: definition and management of the risk related to zoledronic acid. Clin Lymphoma Myeloma 2008;8:111–116.
Ying-Kei Hui, MD,1 Thomas Slattery, MD,2 Dale M. Frank, MD,3 Carol Dolinskas, MD,4 and David Henry, MD, FACP5
Departments of 1Internal Medicine, Pennsylvania Hospital; 2Radiology, Pennsylvania Hospital; 3Pathology and Laboratory Medicine, Hospital of the University of Pennsylvania; 4Nuclear Medicine, Diagnostic Radiology, Pennsylvania Hospital; and 5Medicine, Pennsylvania Hospital, Philadelphia, PA
Multiple myeloma (MM) is a neoplastic proliferation of monoclonal plasma cells within the bone marrow, which overproduces immunoglobulin. This disorder accounts for approximately 1% of all reported neoplasms and 12%– 15% of all hematologic malignancies.1 It is the second most common hematologic malignancy diagnosed.2 The etiology is still not fully understood. MM typically affects older patients, ranging from 50–78 years (median, 61 years).3 Common clinical presentations include fatigue, anemia, renal failure, hypercalcemia, bone pain, and pathologic fractures.
Bone involvement in MM may vary at presentation. Most commonly, radiographic findings include multiple small, sharply defined, lytic, “punched-out” lesions without reactive bone formation, arising in the medullary cavity at sites of preserved hematopoiesis in adults (the axial skeleton). The pathophysiology of the bone findings is uncertain, though presumed to be resultant of either inhibition of osteoblastic activity and/ or activation of osteoclastic activity. Involvement of the cortex results in endosteal scalloping, with invasion of the periosteum and occasionally extraosseous extension. Lesions are most commonly seen in the vertebrae, ribs, skull, pelvic bones, and femur, in descending order of prevalence. Distal bone involvement is less common, though cases with predominant involvement in peripheral bones have been described. Uncommon radiographic presentations include diffuse skeletal osteopenia without focal lesions or sclerotic lesions. 4,5 To our knowledge, multiple bone infarcts as a complication of MM have not been reported in the medical literature.
Case presentation
A 47-year-old man with no significant medical history presented after the recent onset of painless hematuria, which spontaneously resolved after 2 days. He complained of left knee pain, which he noted after doing yard work.
Routine laboratory examination showed normocytic normochromic anemia, with a hemoglobin level of 11.5 g/dL and a mildly elevated alkaline phosphatase (ALP) level at 124 units/L. An MRI of the left knee showed increased red bone marrow within the distal femur and proximal tibia/fibula, initially thought to be compatible with anemia from an unexplained inflammatory process. Further urologic and gastroenterologic workup was negative.
Several months later, our patient was noted to have progressive fatigue, with a decrease in hemoglobin level to 10.6 g/dL and a mildly elevated erythrocyte sedimentation rate. Physical examination was otherwise unremarkable. A repeat MRI of both knees showed an extensive marrow infiltrative process, with multiple presumed secondary bone infarcts in the distal femora and proximal tibias, proximal fibulae, and patellae (Figure 1). A tandem skeletal survey showed mild diffuse osteopenia and several small, rounded, lytic foci in the skull (Figure 2), which were suspicious for MM. No focal radiographic lesions were seen (Figure 3).
Bone marrow biopsy from the left posterior iliac crest revealed hypocellular marrow (20%). An expansion of plasmacytoid cells with eccentrically placed, round nuclei, clumped chromatin, occasional nucleoli, and moderate amounts of eosinophilic cytoplasm accounted for 75% of the marrow cellularity. An aspirate smear demonstrated scattered mature plasma cells, accounting for roughly 15% of the total cellularity. Flow cytometry showed no overt evidence of marrow involvement by a lymphocytic clone. Bone biopsy was not performed in the areas of the knees seen to be abnormal on MRI examination.
Serum protein electrophoresis (SPEP) showed a band in the betagamma region. Immunofixation confirmed the presence of a monoclonal paraprotein, consisting predominantly of immunoglobulin A (IgA) heavy chain and kappa light chain. A bone marrow biopsy and aspirate showed replacement of most hematopoietic elements by sheets of mature plasma cells, accounting for 75% of the total marrow cellularity (Figure 4). Confirmatory immunostains were positive for CD138, CD117, and kappa light chain (Figure 5) and negative for CD79a and lambda light chain (Figure 6). A diagnosis of MM was made based on the finding of M protein in the urine, the presence of greater than 10% clonal plasma cells in bone marrow, and related clinical symptomatology (including anemia and hypercalcemia).
The patient was started on immunomodulating therapy with lenalidomide (Revlimid), bortezomib (Velcade), and dexamethasone. Autologous stem cell transplantation may be considered after appropriate treatment.
Discussion
We offer the case of a patient with MM who presented with bilateral knee infarcts. Synonyms of bone infarct include osteonecrosis, bone necrosis, avascular necrosis, aseptic necrosis, ischemic bone necrosis, and bone death.6 MRI is the most sensitive imaging modality for evaluation of the bone marrow. It can detect early osteonecrotic changes in bones well before they are visible on radiography7; this fact was exemplified in our case, in which the patient had only mild osteopenia on knee radiographs but extensive osteonecrotic changes on MRI examination.
Bone infarct more commonly involves the hips than the knees.7 Knee involvement can be differentiated into two main categories: primary and secondary. Primary, spontaneous, or idiopathic involvement tends to be unilateral and usually is seen in the elderly, although the recent literature suggests that many of these socalled spontaneous cases are actually secondary to subcortical microfractures, which are then complicated by osteonecrosis.5 Secondary causes tend to present at a younger age, with bilateral and multifocal involvement. Examples of secondary causes include steroid therapy, alcoholism, decompression syndrome, hemoglobinopathies (sickle cell disease), autoimmune disease (lupus and antiphospholipid disease), infections (human immunodeficiency virus), radiation, and trauma.8–15 Other causes, such as chemotherapy toxicity in pediatric leukemia16 and Gaucher disease, have been reported.7 Osteonecrosis of the jaw is a known treatment complication of bisphosphonate therapy in patients with MM17; however, there have been no previous reports describing the presentation of multifocal bone infarcts in both knees in patients with MM.
Although the pathogenesis of bone infarction is unclear, it is thought to be caused by the combined effects of systemic and local factors affecting the blood supply, vascular damage, increased intraosseous pressure, and mechanical stresses. These processes lead to compromise of the bone vasculature, resulting in the death of bone and marrow cells.9 In our case, MRI of both knees revealed an extensive marrow infiltrative process, which may have caused local vasculature damage and diminished blood supply resulting in bone infarctions.
Conclusion
Bone infarction of any joint is not a well-established complication of MM. Physicians should be aware of this potential presentation. Although there is no cure for MM, early recognition of MM can lead to more effective treatment, thus slowing disease progression and improving overall clinical outcomes.
Disclosures
The authors have no conflicts of interest to disclose.
References
1. Phekoo KJ, Schey SA, Richards MA, et al. A population study to define the incidence and survival of multiple myeloma in a National Health Service Region in UK. Br J Haematol 2004;127:299–304.
2. Esteve FR, Roodman GD. Pathophysiology of myeloma bone disease. Best Pract Res Clin Haematol 2007;20:613–624.
3. Jain M, Ascensao J, Schechter GP. Familial myeloma and monoclonal gammopathy: a report of eight African American families. Am J Hematol 2009;84:34–38.
4. Winterbottom AP, Shaw AS. Imaging patients with myeloma. Clin Radiol 2009;64:1–11.
5. Resnick D. Diagnosis of Bone and Joint Disorders. Philadelphia, PA: WB Saunders; 2002:2188–2233.
6. Stoller D, Tirman P, Bredella M, Branstetter R. Diagnostic Imaging: Orthopaedics. Philadelphia, PA: WB Saunders; 2003:82.
7. Assouline-Dayan Y, Chang C, Greenspan A, Shoenfeld Y, Gershwin ME. Pathogenesis and natural history of osteonecrosis. Semin Arthritis Rheum 2002;32:94–124.
8. Patel DV, Breazeale NM, Behr CT, Warren RF, Wickiewicz TL, O’Brien SJ. Osteonecrosis of the knee: current clinical concepts. Knee Surg Sports Traumatol Arthrosc 1998;6:2–11.
9. Chang CC, Greenspan A, Gershwin ME. Osteonecrosis: current perspectives on pathogenesis and treatment. Semin Arthritis Rheum 1993;23:47–69.
10. Jones LC, Mont MA, Le TB, et al. Procoagulants and osteonecrosis. J Rheumatol 2003; 30:783–791.
11. Saito N, Nadgir RN, Flower EN, Sakai O. Clinical and radiologic manifestations of sickle cell disease in the head and neck. Radiographics 2010;30:1021–1034.
12. Miller KD, Masur H, Jones EC, et al. High prevalence of osteonecrosis of the femoral head in HIV-infected adults. Ann Intern Med 2002;137:17–25.
13. Mendenhall WM. Mandibular: osteoradionecrosis. J Clin Oncol 2004;22:4867–4868.
14. Mok MY, Farewell VT, Isenberg DA. Risk factors for avascular necrosis of bone in patients with systemic lupus erythematosus: is there a role for antiphospholipid antibodies? Ann Rheum Dis 2000;59:462–467.
15. Kelman GJ, Williams GW, Colwell CW Jr, Walker RH. Steroid-related osteonecrosis of the knee: two case reports and a literature review. Clin Orthop Relat Res 1990;257:171–176.
16. Karimova EJ, Wozniak A, Wu J, Neel MD, Kaste SC. How does osteonecrosis about the knee progress in young patients with leukemia? A 2- to 7-year study. Clin Orthop Relat Res 2010;468:2454–2459.
17. Cafro AM, Barbarano L, Nosari AM, et al. Osteonecrosis of the jaw in patients with multiple myeloma treated with bisphosphonates: definition and management of the risk related to zoledronic acid. Clin Lymphoma Myeloma 2008;8:111–116.
FDA Panel to Review Adcetris for Lymphoma Indications
The July 14 Oncologic Drugs Advisory Committee review of Seattle Genetics’ Adcetris for two rare lymphomas will indicate how the Food and Drug Administration and panel members will apply the general principles for accelerated approval that they enunciated during a February meeting.
Those principles include a desire for randomized trials to support accelerated approval and for confirmatory trials to be a work in progress when accelerated approval is granted.
The two proposed indications for Adcetris (brentuximab vedotin) are relapsed or refractory Hodgkin’s lymphoma and relapsed or refractory systemic anaplastic large cell lymphoma, both orphan indications.
Each indication is supported by one phase II single-arm trial, with the study for the other indication cited as supporting data.
During the February meeting, ODAC members suggested that single-arm trials are acceptable only for rare diseases and therapies with a pronounced treatment effect. They did not specify how high that effect must be.
In the case of Adcetris, of 102 relapsed or refractory Hodgkin’s lymphoma patients who had failed multiple lines of therapy, including autologous stem cell transplant, 73% achieved the primary end point of objective response after receiving brentuximab, according to an independent review facility. The median response duration was 6.7 months. In all, 32% of participants had complete remission, with a median duration of 20.5 months.
The FDA analysis of the phase II study of 58 patients with relapsed or refractory systemic ALCL found that 86% of participants achieved the primary end point of objective response, with a median duration of 12.6 months, including 57% with complete remissions with a median duration of 13.2 months.
That appears to be the home run that Office of Oncology Drug Products Director Richard Pazdur said he was looking for in single-arm trials for accelerated approval.
FDA briefing documents indicate that agency reviewers are comfortable with accelerated approval and that, in fact, that is the only option for Adcetris at this point.
However, in its explanation for the proposed voting question of whether Adcetris should be given accelerated or regular approval – or nonapproval – the FDA noted that the single-arm design and small size limit the benefit-to-risk analysis.
"Time-to-event [end points], such as progression-free survival or overall survival, cannot be adequately interpreted in a single-arm trial," and attribution of adverse events is not possible, the agency explained.
Despite being advised in prebiologic license application meetings that the antibody-drug conjugate would be reviewed for accelerated approval, Seattle Genetics is seeking full approval.
For both indications, the sponsor’s briefing materials state that progression-free survival was significantly superior for brentuximab, compared with the most recent prior therapy.
The firm maintains that "clinical benefit is established by the high overall response and complete remission rates as observed by independent review facility and the associated durability of these remissions, in addition to disease symptom resolution in the context of an acceptable safety profile."
But the FDA says that in the absence of a randomized controlled trial, "time-to-event analyses are not useful for regulatory purposes, nor is a progression-free survival analysis."
For Hodgkin’s lymphoma, the FDA phrases the question about approval with the words "for the treatment of patients with Hodgkin lymphoma who relapse after autologous stem cell transplant," which was the patient population studied in the pivotal trial. Seattle Genetics’ proposed indication is for the treatment of the general population of "patients with relapsed or refractory Hodgkin’s lymphoma."
The one discussion question for each indication centers on the FDA’s desire for confirmatory studies to be at least in the planning stage before an application for accelerated approval is filed.
If ODAC insists upon that requirement, the indication for anaplastic large-cell lymphoma could be derailed, as a confirmatory study is not in the works.
In its briefing document, the agency says it wants ODAC "to consider whether or not accelerated approval should be granted without an ongoing confirmatory trial" for that indication.
In the discussion question itself, the agency sounds more open minded, merely asking for a discussion of potential confirmatory studies, end points, and comparators.
Seattle Genetics is on firmer footing with the Hodgkin’s lymphoma indication, having already begun enrollment in a phase III, randomized, placebo-controlled trial in posttransplant patients. The primary end point is progression-free survival. The company expects to complete enrollment in 2012 and to have data in 2013 or 2014.
The agency will ask the committee to weigh in on whether PFS or overall survival is the most appropriate primary end point to demonstrate clinical benefit.
The FDA also is concerned that participants are not required to be in remission at the time of randomization. A risk-benefit assessment would be different in patients with no residual disease and in those with active disease, the FDA says, and asks for a discussion of whether the trial should be conducted only in those with no active disease.
The FDA’s focus on ensuring that the appropriate confirmatory trial is conducted comes in the wake of its proposed withdrawal of accelerated approval of Genentech’s Avastin because of the failure of its confirmatory studies.
Brentuximab vedotin is an antibody-drug conjugate consisting of an anti-CD30 monoclonal antibody and a small-molecule cytotoxin called monomethyl auristatin E (MMAE). The two are joined by a protease-cleavable linker. The antibody links to the surface of a CD30-expressing cancer cell, the conjugate is internalized to the cell, and the link between the antibody and drug is severed. This delivers the MAAE directly into malignant cells while bypassing normal cells.
The Adcetris Prescription Drug User Fee Act date is Aug. 30.
Elsevier Global Medical News and "The Pink Sheet" are published by Elsevier.
The July 14 Oncologic Drugs Advisory Committee review of Seattle Genetics’ Adcetris for two rare lymphomas will indicate how the Food and Drug Administration and panel members will apply the general principles for accelerated approval that they enunciated during a February meeting.
Those principles include a desire for randomized trials to support accelerated approval and for confirmatory trials to be a work in progress when accelerated approval is granted.
The two proposed indications for Adcetris (brentuximab vedotin) are relapsed or refractory Hodgkin’s lymphoma and relapsed or refractory systemic anaplastic large cell lymphoma, both orphan indications.
Each indication is supported by one phase II single-arm trial, with the study for the other indication cited as supporting data.
During the February meeting, ODAC members suggested that single-arm trials are acceptable only for rare diseases and therapies with a pronounced treatment effect. They did not specify how high that effect must be.
In the case of Adcetris, of 102 relapsed or refractory Hodgkin’s lymphoma patients who had failed multiple lines of therapy, including autologous stem cell transplant, 73% achieved the primary end point of objective response after receiving brentuximab, according to an independent review facility. The median response duration was 6.7 months. In all, 32% of participants had complete remission, with a median duration of 20.5 months.
The FDA analysis of the phase II study of 58 patients with relapsed or refractory systemic ALCL found that 86% of participants achieved the primary end point of objective response, with a median duration of 12.6 months, including 57% with complete remissions with a median duration of 13.2 months.
That appears to be the home run that Office of Oncology Drug Products Director Richard Pazdur said he was looking for in single-arm trials for accelerated approval.
FDA briefing documents indicate that agency reviewers are comfortable with accelerated approval and that, in fact, that is the only option for Adcetris at this point.
However, in its explanation for the proposed voting question of whether Adcetris should be given accelerated or regular approval – or nonapproval – the FDA noted that the single-arm design and small size limit the benefit-to-risk analysis.
"Time-to-event [end points], such as progression-free survival or overall survival, cannot be adequately interpreted in a single-arm trial," and attribution of adverse events is not possible, the agency explained.
Despite being advised in prebiologic license application meetings that the antibody-drug conjugate would be reviewed for accelerated approval, Seattle Genetics is seeking full approval.
For both indications, the sponsor’s briefing materials state that progression-free survival was significantly superior for brentuximab, compared with the most recent prior therapy.
The firm maintains that "clinical benefit is established by the high overall response and complete remission rates as observed by independent review facility and the associated durability of these remissions, in addition to disease symptom resolution in the context of an acceptable safety profile."
But the FDA says that in the absence of a randomized controlled trial, "time-to-event analyses are not useful for regulatory purposes, nor is a progression-free survival analysis."
For Hodgkin’s lymphoma, the FDA phrases the question about approval with the words "for the treatment of patients with Hodgkin lymphoma who relapse after autologous stem cell transplant," which was the patient population studied in the pivotal trial. Seattle Genetics’ proposed indication is for the treatment of the general population of "patients with relapsed or refractory Hodgkin’s lymphoma."
The one discussion question for each indication centers on the FDA’s desire for confirmatory studies to be at least in the planning stage before an application for accelerated approval is filed.
If ODAC insists upon that requirement, the indication for anaplastic large-cell lymphoma could be derailed, as a confirmatory study is not in the works.
In its briefing document, the agency says it wants ODAC "to consider whether or not accelerated approval should be granted without an ongoing confirmatory trial" for that indication.
In the discussion question itself, the agency sounds more open minded, merely asking for a discussion of potential confirmatory studies, end points, and comparators.
Seattle Genetics is on firmer footing with the Hodgkin’s lymphoma indication, having already begun enrollment in a phase III, randomized, placebo-controlled trial in posttransplant patients. The primary end point is progression-free survival. The company expects to complete enrollment in 2012 and to have data in 2013 or 2014.
The agency will ask the committee to weigh in on whether PFS or overall survival is the most appropriate primary end point to demonstrate clinical benefit.
The FDA also is concerned that participants are not required to be in remission at the time of randomization. A risk-benefit assessment would be different in patients with no residual disease and in those with active disease, the FDA says, and asks for a discussion of whether the trial should be conducted only in those with no active disease.
The FDA’s focus on ensuring that the appropriate confirmatory trial is conducted comes in the wake of its proposed withdrawal of accelerated approval of Genentech’s Avastin because of the failure of its confirmatory studies.
Brentuximab vedotin is an antibody-drug conjugate consisting of an anti-CD30 monoclonal antibody and a small-molecule cytotoxin called monomethyl auristatin E (MMAE). The two are joined by a protease-cleavable linker. The antibody links to the surface of a CD30-expressing cancer cell, the conjugate is internalized to the cell, and the link between the antibody and drug is severed. This delivers the MAAE directly into malignant cells while bypassing normal cells.
The Adcetris Prescription Drug User Fee Act date is Aug. 30.
Elsevier Global Medical News and "The Pink Sheet" are published by Elsevier.
The July 14 Oncologic Drugs Advisory Committee review of Seattle Genetics’ Adcetris for two rare lymphomas will indicate how the Food and Drug Administration and panel members will apply the general principles for accelerated approval that they enunciated during a February meeting.
Those principles include a desire for randomized trials to support accelerated approval and for confirmatory trials to be a work in progress when accelerated approval is granted.
The two proposed indications for Adcetris (brentuximab vedotin) are relapsed or refractory Hodgkin’s lymphoma and relapsed or refractory systemic anaplastic large cell lymphoma, both orphan indications.
Each indication is supported by one phase II single-arm trial, with the study for the other indication cited as supporting data.
During the February meeting, ODAC members suggested that single-arm trials are acceptable only for rare diseases and therapies with a pronounced treatment effect. They did not specify how high that effect must be.
In the case of Adcetris, of 102 relapsed or refractory Hodgkin’s lymphoma patients who had failed multiple lines of therapy, including autologous stem cell transplant, 73% achieved the primary end point of objective response after receiving brentuximab, according to an independent review facility. The median response duration was 6.7 months. In all, 32% of participants had complete remission, with a median duration of 20.5 months.
The FDA analysis of the phase II study of 58 patients with relapsed or refractory systemic ALCL found that 86% of participants achieved the primary end point of objective response, with a median duration of 12.6 months, including 57% with complete remissions with a median duration of 13.2 months.
That appears to be the home run that Office of Oncology Drug Products Director Richard Pazdur said he was looking for in single-arm trials for accelerated approval.
FDA briefing documents indicate that agency reviewers are comfortable with accelerated approval and that, in fact, that is the only option for Adcetris at this point.
However, in its explanation for the proposed voting question of whether Adcetris should be given accelerated or regular approval – or nonapproval – the FDA noted that the single-arm design and small size limit the benefit-to-risk analysis.
"Time-to-event [end points], such as progression-free survival or overall survival, cannot be adequately interpreted in a single-arm trial," and attribution of adverse events is not possible, the agency explained.
Despite being advised in prebiologic license application meetings that the antibody-drug conjugate would be reviewed for accelerated approval, Seattle Genetics is seeking full approval.
For both indications, the sponsor’s briefing materials state that progression-free survival was significantly superior for brentuximab, compared with the most recent prior therapy.
The firm maintains that "clinical benefit is established by the high overall response and complete remission rates as observed by independent review facility and the associated durability of these remissions, in addition to disease symptom resolution in the context of an acceptable safety profile."
But the FDA says that in the absence of a randomized controlled trial, "time-to-event analyses are not useful for regulatory purposes, nor is a progression-free survival analysis."
For Hodgkin’s lymphoma, the FDA phrases the question about approval with the words "for the treatment of patients with Hodgkin lymphoma who relapse after autologous stem cell transplant," which was the patient population studied in the pivotal trial. Seattle Genetics’ proposed indication is for the treatment of the general population of "patients with relapsed or refractory Hodgkin’s lymphoma."
The one discussion question for each indication centers on the FDA’s desire for confirmatory studies to be at least in the planning stage before an application for accelerated approval is filed.
If ODAC insists upon that requirement, the indication for anaplastic large-cell lymphoma could be derailed, as a confirmatory study is not in the works.
In its briefing document, the agency says it wants ODAC "to consider whether or not accelerated approval should be granted without an ongoing confirmatory trial" for that indication.
In the discussion question itself, the agency sounds more open minded, merely asking for a discussion of potential confirmatory studies, end points, and comparators.
Seattle Genetics is on firmer footing with the Hodgkin’s lymphoma indication, having already begun enrollment in a phase III, randomized, placebo-controlled trial in posttransplant patients. The primary end point is progression-free survival. The company expects to complete enrollment in 2012 and to have data in 2013 or 2014.
The agency will ask the committee to weigh in on whether PFS or overall survival is the most appropriate primary end point to demonstrate clinical benefit.
The FDA also is concerned that participants are not required to be in remission at the time of randomization. A risk-benefit assessment would be different in patients with no residual disease and in those with active disease, the FDA says, and asks for a discussion of whether the trial should be conducted only in those with no active disease.
The FDA’s focus on ensuring that the appropriate confirmatory trial is conducted comes in the wake of its proposed withdrawal of accelerated approval of Genentech’s Avastin because of the failure of its confirmatory studies.
Brentuximab vedotin is an antibody-drug conjugate consisting of an anti-CD30 monoclonal antibody and a small-molecule cytotoxin called monomethyl auristatin E (MMAE). The two are joined by a protease-cleavable linker. The antibody links to the surface of a CD30-expressing cancer cell, the conjugate is internalized to the cell, and the link between the antibody and drug is severed. This delivers the MAAE directly into malignant cells while bypassing normal cells.
The Adcetris Prescription Drug User Fee Act date is Aug. 30.
Elsevier Global Medical News and "The Pink Sheet" are published by Elsevier.
Interim FDG-PET 'Not Justified' in Diffuse Large B-Cell Lymphoma
LONDON – There is no benefit of performing 18fluorodeoxyglucose positron emission tomography after the first cycle of treatment in patients with diffuse large B-cell lymphoma or primary mediastinal large B-cell lymphoma, the results of an Italian study suggest.
The imaging technique failed to pick up signs of disease in 10 of 85 (12%) of patients who later relapsed following treatment with R-CHOP (rituximab [Rituxan], cyclophosphamide [Cytoxan], hydroxydaunorubicin [doxorubicin, Adriamycin], Oncovin [vincristine], and prednisolone) in conjunction with radiotherapy.
Interim 18FDG-PET was associated with a positive predictive value (PPV) of just 58% and a negative predictive value (NPV) of 77%. By comparison, the PPV and NPV of 18FDG-PET performed after the last treatment cycle were higher, at 70% and 82%, respectively.
"The early identification of nonresponders might be a pivotal step for cure of diffuse large B-cell lymphoma (DLBCL), said study investigator Dr. M. Christina Cox, who presented the findings at the annual congress of the European Hematology Association.
Dr. Cox of the Azienda Ospedaliera Sant’ Andrea in Rome explained that the use of the imaging method early on in the treatment of Hodgkin’s lymphoma had been shown to be a strong predictor of outcome, allowing earlier adjustment of therapy.
"From 2005, several studies showed than in [DLBCL], interim PET might be predictive of event-free survival, progression-free survival, and overall survival," Dr. Cox said. However, "more recent studies have yielded heterogeneous results."
Aiming to clarify the issue, Dr. Cox and colleagues undertook a prospective study of treatment-naive patients with either DLBCL (72 patients) or primary mediastinal large B-cell lymphoma (PMLBCL, 13 patients) enrolled between April 2005 and April 2010. Patients were eligible for the study if they had already undergone a PET or contrast enhancement computed tomography (CECT) scan, had no CNS involvement, were HIV negative, and were not eligible for R-CHOP-like treatments.
After initial staging with 18FDG-PET and CECT, patients with stage II or higher DLCBL received six cycles of treatment with either R-CHOP-14 if they were younger than 70 years or R-CHOP-21 if they were aged 70 years or older. In both cases, the duration of treatment was reduced to three cycles for patients with stage I disease. Patients with PMLBCL were treated with R-MACOP-14 (rituximab, methotrexate, ara-C [cytarabine], cyclophosphamide, Oncovin [vincristine], and prednisone) for 12 weeks. All patients with PMLBCL and those with stage I DLCBL received radiotherapy.
Interim staging using PET and CECT was performed within 10-20 days of the first cycle of treatment, with the final scans using both imaging techniques taken 6-8 weeks after the last treatment. The recently validated Deauville 5-point scale was used to compare the differences between interim and final PET scans. This scale gauges the uptake of 18FDG within the tissues.
The minimum observation time was set at 2 years, unless a DLBCL event occurred earlier. Targeted biopsies were performed at the end of treatment if there was a mismatch between PET and CECT results, and at the interim stage if results were conflicting and the site in need of biopsy was easy to reach.
Almost two-thirds (62%) were biopsy negative. Dr. Cox noted that none of the interim PET, biopsy-negative patients relapsed.
At a median follow-up of almost 3 years, 70 (82.3%) patients were still alive, with 65 (76.4%) being disease free after first- or second-line therapy. One-fifth had been refractory to first-line treatment. Of these patients, 78% had a positive interim PET scan.
Looking at factors that might predict the achievement of a complete remission to first-line treatment, only the interim CECT results were statistically significant in a multivariate analysis (P less than .002).
In addition, only the final PET scan was predictive of both overall and progression-free survival, whereas interim and final CECT were both predictive.
"In this series, interim PET proved not to be a robust tool for the early shifting of patients to high-dose therapy," Dr. Cox reported. She added that compared with interim CECT and final PET, "interim PET was not really of adjunctive value." Indeed, most refractory patients (61%) were identified by interim CECT.
"We think that the use of this [interim PET] expensive, radioactive, and emotionally distressing tool is presently not justified outside of clinical trials."
Commenting on the findings in an interview, Dr. Andrew Pettitt, professor of hematological oncology at the University of Liverpool (England), said that although it was a good study, he was not convinced it was adequately powered to draw such a definitive conclusion. "I also have some reservations of the PET-CT reporting and quality control," Dr. Pettitt, who was not involved in the study. "It’s very provocative, but I don’t think it’s definitive."
Dr. Cox and Dr. Pettitt stated that they had no relevant financial disclosures.
R-CHOP, radiotherapy, 18FDG-PET, Dr. M. Christina Cox, the European Hematology Association,
LONDON – There is no benefit of performing 18fluorodeoxyglucose positron emission tomography after the first cycle of treatment in patients with diffuse large B-cell lymphoma or primary mediastinal large B-cell lymphoma, the results of an Italian study suggest.
The imaging technique failed to pick up signs of disease in 10 of 85 (12%) of patients who later relapsed following treatment with R-CHOP (rituximab [Rituxan], cyclophosphamide [Cytoxan], hydroxydaunorubicin [doxorubicin, Adriamycin], Oncovin [vincristine], and prednisolone) in conjunction with radiotherapy.
Interim 18FDG-PET was associated with a positive predictive value (PPV) of just 58% and a negative predictive value (NPV) of 77%. By comparison, the PPV and NPV of 18FDG-PET performed after the last treatment cycle were higher, at 70% and 82%, respectively.
"The early identification of nonresponders might be a pivotal step for cure of diffuse large B-cell lymphoma (DLBCL), said study investigator Dr. M. Christina Cox, who presented the findings at the annual congress of the European Hematology Association.
Dr. Cox of the Azienda Ospedaliera Sant’ Andrea in Rome explained that the use of the imaging method early on in the treatment of Hodgkin’s lymphoma had been shown to be a strong predictor of outcome, allowing earlier adjustment of therapy.
"From 2005, several studies showed than in [DLBCL], interim PET might be predictive of event-free survival, progression-free survival, and overall survival," Dr. Cox said. However, "more recent studies have yielded heterogeneous results."
Aiming to clarify the issue, Dr. Cox and colleagues undertook a prospective study of treatment-naive patients with either DLBCL (72 patients) or primary mediastinal large B-cell lymphoma (PMLBCL, 13 patients) enrolled between April 2005 and April 2010. Patients were eligible for the study if they had already undergone a PET or contrast enhancement computed tomography (CECT) scan, had no CNS involvement, were HIV negative, and were not eligible for R-CHOP-like treatments.
After initial staging with 18FDG-PET and CECT, patients with stage II or higher DLCBL received six cycles of treatment with either R-CHOP-14 if they were younger than 70 years or R-CHOP-21 if they were aged 70 years or older. In both cases, the duration of treatment was reduced to three cycles for patients with stage I disease. Patients with PMLBCL were treated with R-MACOP-14 (rituximab, methotrexate, ara-C [cytarabine], cyclophosphamide, Oncovin [vincristine], and prednisone) for 12 weeks. All patients with PMLBCL and those with stage I DLCBL received radiotherapy.
Interim staging using PET and CECT was performed within 10-20 days of the first cycle of treatment, with the final scans using both imaging techniques taken 6-8 weeks after the last treatment. The recently validated Deauville 5-point scale was used to compare the differences between interim and final PET scans. This scale gauges the uptake of 18FDG within the tissues.
The minimum observation time was set at 2 years, unless a DLBCL event occurred earlier. Targeted biopsies were performed at the end of treatment if there was a mismatch between PET and CECT results, and at the interim stage if results were conflicting and the site in need of biopsy was easy to reach.
Almost two-thirds (62%) were biopsy negative. Dr. Cox noted that none of the interim PET, biopsy-negative patients relapsed.
At a median follow-up of almost 3 years, 70 (82.3%) patients were still alive, with 65 (76.4%) being disease free after first- or second-line therapy. One-fifth had been refractory to first-line treatment. Of these patients, 78% had a positive interim PET scan.
Looking at factors that might predict the achievement of a complete remission to first-line treatment, only the interim CECT results were statistically significant in a multivariate analysis (P less than .002).
In addition, only the final PET scan was predictive of both overall and progression-free survival, whereas interim and final CECT were both predictive.
"In this series, interim PET proved not to be a robust tool for the early shifting of patients to high-dose therapy," Dr. Cox reported. She added that compared with interim CECT and final PET, "interim PET was not really of adjunctive value." Indeed, most refractory patients (61%) were identified by interim CECT.
"We think that the use of this [interim PET] expensive, radioactive, and emotionally distressing tool is presently not justified outside of clinical trials."
Commenting on the findings in an interview, Dr. Andrew Pettitt, professor of hematological oncology at the University of Liverpool (England), said that although it was a good study, he was not convinced it was adequately powered to draw such a definitive conclusion. "I also have some reservations of the PET-CT reporting and quality control," Dr. Pettitt, who was not involved in the study. "It’s very provocative, but I don’t think it’s definitive."
Dr. Cox and Dr. Pettitt stated that they had no relevant financial disclosures.
LONDON – There is no benefit of performing 18fluorodeoxyglucose positron emission tomography after the first cycle of treatment in patients with diffuse large B-cell lymphoma or primary mediastinal large B-cell lymphoma, the results of an Italian study suggest.
The imaging technique failed to pick up signs of disease in 10 of 85 (12%) of patients who later relapsed following treatment with R-CHOP (rituximab [Rituxan], cyclophosphamide [Cytoxan], hydroxydaunorubicin [doxorubicin, Adriamycin], Oncovin [vincristine], and prednisolone) in conjunction with radiotherapy.
Interim 18FDG-PET was associated with a positive predictive value (PPV) of just 58% and a negative predictive value (NPV) of 77%. By comparison, the PPV and NPV of 18FDG-PET performed after the last treatment cycle were higher, at 70% and 82%, respectively.
"The early identification of nonresponders might be a pivotal step for cure of diffuse large B-cell lymphoma (DLBCL), said study investigator Dr. M. Christina Cox, who presented the findings at the annual congress of the European Hematology Association.
Dr. Cox of the Azienda Ospedaliera Sant’ Andrea in Rome explained that the use of the imaging method early on in the treatment of Hodgkin’s lymphoma had been shown to be a strong predictor of outcome, allowing earlier adjustment of therapy.
"From 2005, several studies showed than in [DLBCL], interim PET might be predictive of event-free survival, progression-free survival, and overall survival," Dr. Cox said. However, "more recent studies have yielded heterogeneous results."
Aiming to clarify the issue, Dr. Cox and colleagues undertook a prospective study of treatment-naive patients with either DLBCL (72 patients) or primary mediastinal large B-cell lymphoma (PMLBCL, 13 patients) enrolled between April 2005 and April 2010. Patients were eligible for the study if they had already undergone a PET or contrast enhancement computed tomography (CECT) scan, had no CNS involvement, were HIV negative, and were not eligible for R-CHOP-like treatments.
After initial staging with 18FDG-PET and CECT, patients with stage II or higher DLCBL received six cycles of treatment with either R-CHOP-14 if they were younger than 70 years or R-CHOP-21 if they were aged 70 years or older. In both cases, the duration of treatment was reduced to three cycles for patients with stage I disease. Patients with PMLBCL were treated with R-MACOP-14 (rituximab, methotrexate, ara-C [cytarabine], cyclophosphamide, Oncovin [vincristine], and prednisone) for 12 weeks. All patients with PMLBCL and those with stage I DLCBL received radiotherapy.
Interim staging using PET and CECT was performed within 10-20 days of the first cycle of treatment, with the final scans using both imaging techniques taken 6-8 weeks after the last treatment. The recently validated Deauville 5-point scale was used to compare the differences between interim and final PET scans. This scale gauges the uptake of 18FDG within the tissues.
The minimum observation time was set at 2 years, unless a DLBCL event occurred earlier. Targeted biopsies were performed at the end of treatment if there was a mismatch between PET and CECT results, and at the interim stage if results were conflicting and the site in need of biopsy was easy to reach.
Almost two-thirds (62%) were biopsy negative. Dr. Cox noted that none of the interim PET, biopsy-negative patients relapsed.
At a median follow-up of almost 3 years, 70 (82.3%) patients were still alive, with 65 (76.4%) being disease free after first- or second-line therapy. One-fifth had been refractory to first-line treatment. Of these patients, 78% had a positive interim PET scan.
Looking at factors that might predict the achievement of a complete remission to first-line treatment, only the interim CECT results were statistically significant in a multivariate analysis (P less than .002).
In addition, only the final PET scan was predictive of both overall and progression-free survival, whereas interim and final CECT were both predictive.
"In this series, interim PET proved not to be a robust tool for the early shifting of patients to high-dose therapy," Dr. Cox reported. She added that compared with interim CECT and final PET, "interim PET was not really of adjunctive value." Indeed, most refractory patients (61%) were identified by interim CECT.
"We think that the use of this [interim PET] expensive, radioactive, and emotionally distressing tool is presently not justified outside of clinical trials."
Commenting on the findings in an interview, Dr. Andrew Pettitt, professor of hematological oncology at the University of Liverpool (England), said that although it was a good study, he was not convinced it was adequately powered to draw such a definitive conclusion. "I also have some reservations of the PET-CT reporting and quality control," Dr. Pettitt, who was not involved in the study. "It’s very provocative, but I don’t think it’s definitive."
Dr. Cox and Dr. Pettitt stated that they had no relevant financial disclosures.
R-CHOP, radiotherapy, 18FDG-PET, Dr. M. Christina Cox, the European Hematology Association,
R-CHOP, radiotherapy, 18FDG-PET, Dr. M. Christina Cox, the European Hematology Association,
FROM THE ANNUAL CONGRESS OF THE EUROPEAN HEMATOLOGY ASSOCIATION
Major Finding: Interim 18FDG-PET had a PPV of 58% and a NPV of 77%. By comparison, the values for 18FDG-PET performed 6-8 weeks after the last treatment cycle were 70% and 82%, respectively.
Data Source: Prospective study of 85 patients with DLBCL or PMLBCL enrolled over a 5-year period in 2005-2010.
Disclosures: Dr. Cox and Dr. Pettitt stated that they had no relevant disclosures.
Brentuximab Benefits Hodgkin's Patients Ineligible for Transplant
LONDON – The investigational agent brentuximab vedotin appears to have a beneficial effect in patients with refractory or relapsed Hodgkin’s lymphoma who are ineligible for or have refused to have an autologous stem cell transplant.
A retrospective analysis of two phase I studies performed with the drug used as a single agent have shown that almost one-third of these heavily pretreated patients are able to achieve an objective response to treatment.
Indeed, 6 of 20 patients (30%) aged a median of 32 years achieved an objective response (two complete and four partial remissions). The response can last longer than 6 months, with one patient achieving a durable remission for more than 2 years that later allowed for transplantation.
"These are very encouraging results in patients with [an] unmet need, and additional studies are ongoing," Dr. Ranjana Advani of Stanford University Medical Center in Palo Alto, Calif., said at the annual congress of the European Hematology Association.
"Patients who have primary refractory disease or fail to achieve a remission at relapse have a dismal outcome," Dr. Advani observed. She added that long-term survival prospects for such patients "were pretty bleak, with median overall survival in a small series as low as 4 months."
Brentuximab vedotin is a novel antibody-drug conjugate that comprises an anti-CD30 monoclonal antibody and a synthetic antimicrotubule agent, monomethyl auristatin E (MMAE). After binding to CD30 on the surface of T and B cells, the antibody-drug conjugate is internalized, the link between antibody and drug is severed, and MMAE is released – thus targeting malignant cells while, in theory, leaving normal cells unscathed.
MMAE is a potent antimicrotubule agent, and as with the taxanes, one of the expected side effects of the drug could be peripheral neuropathy. Although this was not seen in the small number of patients discussed by Dr. Advani, she said that peripheral neuropathy, mostly sensory, had been observed in about 15% of patients treated in the clinical trials program to date.
"Adverse events were seen in over 25% of patients, and these were not necessarily drug related; they could have been even disease related," Dr. Advani reported. Common side effects included fatigue (45%); nausea (40%); pyrexia (35%); decreased weight and diarrhea (30% each); vomiting, back pain, decreased appetite, anemia, and night sweats (25% each).
There were no deaths within 30 days of receiving the last dose of the novel agent.
The current findings add to data released separately from a pivotal phase II trial, recently updated and presented at this year’s American Society of Clinical Oncology meeting in Chicago. In that trial (J. Clin. Oncol. 2011 29[suppl.]: abstract 8031), brentuximab vedotin (SGN-35) induced objective responses in 75% of patients with relapsed or refractory Hodgkin’s disease; 34% achieved a durable complete remission, with two-thirds of patients remaining in complete remission.
Brentuximab has also recently been linked to durable remissions in patients with relapsed or refractory systemic anaplastic large-cell lymphoma (sALCL), an aggressive subtype of peripheral T-cell lymphoma.
The Food and Drug Administration has granted brentuximab vedotin orphan drug status for the treatment of Hodgkin’s lymphoma and sALCL.
Further studies are underway, and include the phase III AETHERA trial – which is comparing brentuximab vedotin to placebo in high-risk patients with Hodgkin’s lymphoma after autologous stem cell transplantation. Another phase I trial is also looking at the combination of brentuximab vedotin and the ABVD (doxorubicin, bleomycin, vinblastine, dacarbazine) regimen as de novo treatment in Hodgkin’s lymphoma.
Seattle Genetics and Millennium: the Takeda Oncology Co. funded the research. Dr. Advani disclosed acting as a principal investigator and receiving research support and advisory board fees from the company.
LONDON – The investigational agent brentuximab vedotin appears to have a beneficial effect in patients with refractory or relapsed Hodgkin’s lymphoma who are ineligible for or have refused to have an autologous stem cell transplant.
A retrospective analysis of two phase I studies performed with the drug used as a single agent have shown that almost one-third of these heavily pretreated patients are able to achieve an objective response to treatment.
Indeed, 6 of 20 patients (30%) aged a median of 32 years achieved an objective response (two complete and four partial remissions). The response can last longer than 6 months, with one patient achieving a durable remission for more than 2 years that later allowed for transplantation.
"These are very encouraging results in patients with [an] unmet need, and additional studies are ongoing," Dr. Ranjana Advani of Stanford University Medical Center in Palo Alto, Calif., said at the annual congress of the European Hematology Association.
"Patients who have primary refractory disease or fail to achieve a remission at relapse have a dismal outcome," Dr. Advani observed. She added that long-term survival prospects for such patients "were pretty bleak, with median overall survival in a small series as low as 4 months."
Brentuximab vedotin is a novel antibody-drug conjugate that comprises an anti-CD30 monoclonal antibody and a synthetic antimicrotubule agent, monomethyl auristatin E (MMAE). After binding to CD30 on the surface of T and B cells, the antibody-drug conjugate is internalized, the link between antibody and drug is severed, and MMAE is released – thus targeting malignant cells while, in theory, leaving normal cells unscathed.
MMAE is a potent antimicrotubule agent, and as with the taxanes, one of the expected side effects of the drug could be peripheral neuropathy. Although this was not seen in the small number of patients discussed by Dr. Advani, she said that peripheral neuropathy, mostly sensory, had been observed in about 15% of patients treated in the clinical trials program to date.
"Adverse events were seen in over 25% of patients, and these were not necessarily drug related; they could have been even disease related," Dr. Advani reported. Common side effects included fatigue (45%); nausea (40%); pyrexia (35%); decreased weight and diarrhea (30% each); vomiting, back pain, decreased appetite, anemia, and night sweats (25% each).
There were no deaths within 30 days of receiving the last dose of the novel agent.
The current findings add to data released separately from a pivotal phase II trial, recently updated and presented at this year’s American Society of Clinical Oncology meeting in Chicago. In that trial (J. Clin. Oncol. 2011 29[suppl.]: abstract 8031), brentuximab vedotin (SGN-35) induced objective responses in 75% of patients with relapsed or refractory Hodgkin’s disease; 34% achieved a durable complete remission, with two-thirds of patients remaining in complete remission.
Brentuximab has also recently been linked to durable remissions in patients with relapsed or refractory systemic anaplastic large-cell lymphoma (sALCL), an aggressive subtype of peripheral T-cell lymphoma.
The Food and Drug Administration has granted brentuximab vedotin orphan drug status for the treatment of Hodgkin’s lymphoma and sALCL.
Further studies are underway, and include the phase III AETHERA trial – which is comparing brentuximab vedotin to placebo in high-risk patients with Hodgkin’s lymphoma after autologous stem cell transplantation. Another phase I trial is also looking at the combination of brentuximab vedotin and the ABVD (doxorubicin, bleomycin, vinblastine, dacarbazine) regimen as de novo treatment in Hodgkin’s lymphoma.
Seattle Genetics and Millennium: the Takeda Oncology Co. funded the research. Dr. Advani disclosed acting as a principal investigator and receiving research support and advisory board fees from the company.
LONDON – The investigational agent brentuximab vedotin appears to have a beneficial effect in patients with refractory or relapsed Hodgkin’s lymphoma who are ineligible for or have refused to have an autologous stem cell transplant.
A retrospective analysis of two phase I studies performed with the drug used as a single agent have shown that almost one-third of these heavily pretreated patients are able to achieve an objective response to treatment.
Indeed, 6 of 20 patients (30%) aged a median of 32 years achieved an objective response (two complete and four partial remissions). The response can last longer than 6 months, with one patient achieving a durable remission for more than 2 years that later allowed for transplantation.
"These are very encouraging results in patients with [an] unmet need, and additional studies are ongoing," Dr. Ranjana Advani of Stanford University Medical Center in Palo Alto, Calif., said at the annual congress of the European Hematology Association.
"Patients who have primary refractory disease or fail to achieve a remission at relapse have a dismal outcome," Dr. Advani observed. She added that long-term survival prospects for such patients "were pretty bleak, with median overall survival in a small series as low as 4 months."
Brentuximab vedotin is a novel antibody-drug conjugate that comprises an anti-CD30 monoclonal antibody and a synthetic antimicrotubule agent, monomethyl auristatin E (MMAE). After binding to CD30 on the surface of T and B cells, the antibody-drug conjugate is internalized, the link between antibody and drug is severed, and MMAE is released – thus targeting malignant cells while, in theory, leaving normal cells unscathed.
MMAE is a potent antimicrotubule agent, and as with the taxanes, one of the expected side effects of the drug could be peripheral neuropathy. Although this was not seen in the small number of patients discussed by Dr. Advani, she said that peripheral neuropathy, mostly sensory, had been observed in about 15% of patients treated in the clinical trials program to date.
"Adverse events were seen in over 25% of patients, and these were not necessarily drug related; they could have been even disease related," Dr. Advani reported. Common side effects included fatigue (45%); nausea (40%); pyrexia (35%); decreased weight and diarrhea (30% each); vomiting, back pain, decreased appetite, anemia, and night sweats (25% each).
There were no deaths within 30 days of receiving the last dose of the novel agent.
The current findings add to data released separately from a pivotal phase II trial, recently updated and presented at this year’s American Society of Clinical Oncology meeting in Chicago. In that trial (J. Clin. Oncol. 2011 29[suppl.]: abstract 8031), brentuximab vedotin (SGN-35) induced objective responses in 75% of patients with relapsed or refractory Hodgkin’s disease; 34% achieved a durable complete remission, with two-thirds of patients remaining in complete remission.
Brentuximab has also recently been linked to durable remissions in patients with relapsed or refractory systemic anaplastic large-cell lymphoma (sALCL), an aggressive subtype of peripheral T-cell lymphoma.
The Food and Drug Administration has granted brentuximab vedotin orphan drug status for the treatment of Hodgkin’s lymphoma and sALCL.
Further studies are underway, and include the phase III AETHERA trial – which is comparing brentuximab vedotin to placebo in high-risk patients with Hodgkin’s lymphoma after autologous stem cell transplantation. Another phase I trial is also looking at the combination of brentuximab vedotin and the ABVD (doxorubicin, bleomycin, vinblastine, dacarbazine) regimen as de novo treatment in Hodgkin’s lymphoma.
Seattle Genetics and Millennium: the Takeda Oncology Co. funded the research. Dr. Advani disclosed acting as a principal investigator and receiving research support and advisory board fees from the company.
FROM THE ANNUAL CONGRESS OF THE EUROPEAN HEMATOLOGY ASSOCIATION
Major Finding: Six patients (30%) achieved an objective response (two complete and four partial remissions).
Data Source: Retrospective analysis of two phase I studies of brentuximab vedotin in 20 patients with relapsed or refractory Hodgkin’s lymphoma who were ineligible for or refused autologous stem cell transplantation.
Disclosures: Seattle Genetics and Millennium: the Takeda Oncology Co. funded the research. Dr. Advani disclosed acting as a principal investigator and receiving research support and advisory board fees from the company.
Treat HIV-Related Hodgkin's Like Non-HIV Disease
LONDON – HIV-infected patients with Hodgkin’s lymphoma can be treated more or less the same as any other Hodgkin’s patient, according to new data from the German HIV-related Lymphoma Study Group.
In a prospective, multicenter study of 108 patients with Hodgkin’s lymphoma (HL), all of whom were HIV positive, a risk-adapted treatment strategy was found to be feasible while patients were being treated with HAART (highly active antiretroviral therapy).
"I think the main message is that the prognosis [of patients with HIV-related HL] has dramatically improved with the [use of] HAART and with the stage- and risk-adapted treatment approach," study investigator Dr. Marcus Hentrich said in a June 11 interview at the annual congress of the European Hematology Association, where he presented the study.
"The results are approaching those we have obtained in the HIV-negative population," added Dr. Hentrich of Harlaching Hospital Munich. The findings show that "not every patient needs to be treated with full intensity" for six to eight courses of chemotherapy; rather, "we can distinguish [treatment] depending on the Hodgkin’s stage."
HL is one of the most common non–AIDS-defining cancers that often presents at an advanced stage. To date, there have been few prospective studies looking at how best to treat patients who are both HIV positive and have the hematologic malignancy; indeed, patients with HIV-related HL are often excluded from HL clinical trials. As a consequence, how best to manage such patients remains unknown (Adv. Hematol. 2011 [doi:10.1155/2011/402682]).
Combination therapy regimens have largely been used to treat HL in HIV-infected patients because of the generally late presentation of the disease, and controlling HIV infection via HAART has also been shown to improve the outcome of HL (Ann. Oncol. 2006;17:914-9).
The current study presented by Dr. Hentrich was conducted between March 2004 and October 2010. It included 100 male and 8 female patients with HL who were HIV positive, and its aim was to see whether a risk-adapted treatment strategy that was used in HIV-negative patients with HL could be applied to those infected with HIV.
Treatment for HL was determined by the stage of disease, with two to four cycles of ABVD (doxorubicin, bleomycin, vinblastine, dacarbazine) used with involved-field radiotherapy (30 Gy) in early-stage patients (that is, those with stage I-II HL and no additional risk factors).
In intermediate-stage patients (that is, those with stage I-II disease plus additional risk factors, such as large mediastinal tumor, extranodal involvement, and three or more lymph node regions involved), treatment consisted of four cycles of BEACOPP (bleomycin, etoposide, doxorubicin, cyclophosphamide, vincristine, procarbazine, and prednisone) plus the same radiotherapy regimen.
More advanced HL (stage III-IV) was treated with six to eight cycles of BEACOPP plus facultative radiotherapy (30 Gy initial bulk or rest).
In patients with very advanced HIV infection and a poor performance status, the BEACOPP regimen could be replaced by ABVD, and the dose of ABVD reduced according to individual circumstances.
The median age of recruited patients was 43.9 years (range, 27-70 years). The majority (65%) had advanced disease, with 14% identified as having intermediate-stage HL, and 21% with early-stage disease. Extranodal involvement was observed in about half of patients (54%), and almost two-thirds (65%) had B-symptoms (which includes systemic symptoms such as fever, night sweats, and weight loss; B-symptoms can occur in both HL and non-HL).
Most (77%) patients had received HAART, and the median time from HIV to HL diagnosis was 5.9 years (range, 0-26 years).
After 26 months’ follow-up, 96%, 100%, and 84% of patients with early-, intermediate-, and advanced-stage HL, respectively, were in complete remission.
Perhaps not surprisingly, some advanced-stage patients fared worse, with four (6%) toxic and one (1.4%) unknown cause of death, five (7%) cases of early progression, and one (1.4%) partial remission in this group. One (4%) patient in the early-stage group also died because of toxicity.
Dr. Hentrich pointed out that treatment relapses and failures mainly occurred in patients with advanced disease.
Grade 3/4 toxicity was common and tended to occur in more patients who were treated with BEACOPP than AVBD, but the differences were statistically significantly only in the early-stage patients. The major hematologic toxicity was severe neutropenia.
At 2-years, progression-free and overall survival were 91.7% and 90.2%, respectively, for the whole population, and did not differ greatly between early-, intermediate-, and advanced-stage disease. However, patients with advanced disease and advanced HIV infection were more likely to have a reduced overall survival, compared with the other two groups of patients.
"The next strategy is to focus the amount of intensity to special patients, so we want to incorporate early PET scans after two cycles [of chemotherapy] and then de-escalate therapy or even escalate therapy," Dr. Hentrich said.
Dr. Hentrich had no financial disclosures or conflicts of interest.
LONDON – HIV-infected patients with Hodgkin’s lymphoma can be treated more or less the same as any other Hodgkin’s patient, according to new data from the German HIV-related Lymphoma Study Group.
In a prospective, multicenter study of 108 patients with Hodgkin’s lymphoma (HL), all of whom were HIV positive, a risk-adapted treatment strategy was found to be feasible while patients were being treated with HAART (highly active antiretroviral therapy).
"I think the main message is that the prognosis [of patients with HIV-related HL] has dramatically improved with the [use of] HAART and with the stage- and risk-adapted treatment approach," study investigator Dr. Marcus Hentrich said in a June 11 interview at the annual congress of the European Hematology Association, where he presented the study.
"The results are approaching those we have obtained in the HIV-negative population," added Dr. Hentrich of Harlaching Hospital Munich. The findings show that "not every patient needs to be treated with full intensity" for six to eight courses of chemotherapy; rather, "we can distinguish [treatment] depending on the Hodgkin’s stage."
HL is one of the most common non–AIDS-defining cancers that often presents at an advanced stage. To date, there have been few prospective studies looking at how best to treat patients who are both HIV positive and have the hematologic malignancy; indeed, patients with HIV-related HL are often excluded from HL clinical trials. As a consequence, how best to manage such patients remains unknown (Adv. Hematol. 2011 [doi:10.1155/2011/402682]).
Combination therapy regimens have largely been used to treat HL in HIV-infected patients because of the generally late presentation of the disease, and controlling HIV infection via HAART has also been shown to improve the outcome of HL (Ann. Oncol. 2006;17:914-9).
The current study presented by Dr. Hentrich was conducted between March 2004 and October 2010. It included 100 male and 8 female patients with HL who were HIV positive, and its aim was to see whether a risk-adapted treatment strategy that was used in HIV-negative patients with HL could be applied to those infected with HIV.
Treatment for HL was determined by the stage of disease, with two to four cycles of ABVD (doxorubicin, bleomycin, vinblastine, dacarbazine) used with involved-field radiotherapy (30 Gy) in early-stage patients (that is, those with stage I-II HL and no additional risk factors).
In intermediate-stage patients (that is, those with stage I-II disease plus additional risk factors, such as large mediastinal tumor, extranodal involvement, and three or more lymph node regions involved), treatment consisted of four cycles of BEACOPP (bleomycin, etoposide, doxorubicin, cyclophosphamide, vincristine, procarbazine, and prednisone) plus the same radiotherapy regimen.
More advanced HL (stage III-IV) was treated with six to eight cycles of BEACOPP plus facultative radiotherapy (30 Gy initial bulk or rest).
In patients with very advanced HIV infection and a poor performance status, the BEACOPP regimen could be replaced by ABVD, and the dose of ABVD reduced according to individual circumstances.
The median age of recruited patients was 43.9 years (range, 27-70 years). The majority (65%) had advanced disease, with 14% identified as having intermediate-stage HL, and 21% with early-stage disease. Extranodal involvement was observed in about half of patients (54%), and almost two-thirds (65%) had B-symptoms (which includes systemic symptoms such as fever, night sweats, and weight loss; B-symptoms can occur in both HL and non-HL).
Most (77%) patients had received HAART, and the median time from HIV to HL diagnosis was 5.9 years (range, 0-26 years).
After 26 months’ follow-up, 96%, 100%, and 84% of patients with early-, intermediate-, and advanced-stage HL, respectively, were in complete remission.
Perhaps not surprisingly, some advanced-stage patients fared worse, with four (6%) toxic and one (1.4%) unknown cause of death, five (7%) cases of early progression, and one (1.4%) partial remission in this group. One (4%) patient in the early-stage group also died because of toxicity.
Dr. Hentrich pointed out that treatment relapses and failures mainly occurred in patients with advanced disease.
Grade 3/4 toxicity was common and tended to occur in more patients who were treated with BEACOPP than AVBD, but the differences were statistically significantly only in the early-stage patients. The major hematologic toxicity was severe neutropenia.
At 2-years, progression-free and overall survival were 91.7% and 90.2%, respectively, for the whole population, and did not differ greatly between early-, intermediate-, and advanced-stage disease. However, patients with advanced disease and advanced HIV infection were more likely to have a reduced overall survival, compared with the other two groups of patients.
"The next strategy is to focus the amount of intensity to special patients, so we want to incorporate early PET scans after two cycles [of chemotherapy] and then de-escalate therapy or even escalate therapy," Dr. Hentrich said.
Dr. Hentrich had no financial disclosures or conflicts of interest.
LONDON – HIV-infected patients with Hodgkin’s lymphoma can be treated more or less the same as any other Hodgkin’s patient, according to new data from the German HIV-related Lymphoma Study Group.
In a prospective, multicenter study of 108 patients with Hodgkin’s lymphoma (HL), all of whom were HIV positive, a risk-adapted treatment strategy was found to be feasible while patients were being treated with HAART (highly active antiretroviral therapy).
"I think the main message is that the prognosis [of patients with HIV-related HL] has dramatically improved with the [use of] HAART and with the stage- and risk-adapted treatment approach," study investigator Dr. Marcus Hentrich said in a June 11 interview at the annual congress of the European Hematology Association, where he presented the study.
"The results are approaching those we have obtained in the HIV-negative population," added Dr. Hentrich of Harlaching Hospital Munich. The findings show that "not every patient needs to be treated with full intensity" for six to eight courses of chemotherapy; rather, "we can distinguish [treatment] depending on the Hodgkin’s stage."
HL is one of the most common non–AIDS-defining cancers that often presents at an advanced stage. To date, there have been few prospective studies looking at how best to treat patients who are both HIV positive and have the hematologic malignancy; indeed, patients with HIV-related HL are often excluded from HL clinical trials. As a consequence, how best to manage such patients remains unknown (Adv. Hematol. 2011 [doi:10.1155/2011/402682]).
Combination therapy regimens have largely been used to treat HL in HIV-infected patients because of the generally late presentation of the disease, and controlling HIV infection via HAART has also been shown to improve the outcome of HL (Ann. Oncol. 2006;17:914-9).
The current study presented by Dr. Hentrich was conducted between March 2004 and October 2010. It included 100 male and 8 female patients with HL who were HIV positive, and its aim was to see whether a risk-adapted treatment strategy that was used in HIV-negative patients with HL could be applied to those infected with HIV.
Treatment for HL was determined by the stage of disease, with two to four cycles of ABVD (doxorubicin, bleomycin, vinblastine, dacarbazine) used with involved-field radiotherapy (30 Gy) in early-stage patients (that is, those with stage I-II HL and no additional risk factors).
In intermediate-stage patients (that is, those with stage I-II disease plus additional risk factors, such as large mediastinal tumor, extranodal involvement, and three or more lymph node regions involved), treatment consisted of four cycles of BEACOPP (bleomycin, etoposide, doxorubicin, cyclophosphamide, vincristine, procarbazine, and prednisone) plus the same radiotherapy regimen.
More advanced HL (stage III-IV) was treated with six to eight cycles of BEACOPP plus facultative radiotherapy (30 Gy initial bulk or rest).
In patients with very advanced HIV infection and a poor performance status, the BEACOPP regimen could be replaced by ABVD, and the dose of ABVD reduced according to individual circumstances.
The median age of recruited patients was 43.9 years (range, 27-70 years). The majority (65%) had advanced disease, with 14% identified as having intermediate-stage HL, and 21% with early-stage disease. Extranodal involvement was observed in about half of patients (54%), and almost two-thirds (65%) had B-symptoms (which includes systemic symptoms such as fever, night sweats, and weight loss; B-symptoms can occur in both HL and non-HL).
Most (77%) patients had received HAART, and the median time from HIV to HL diagnosis was 5.9 years (range, 0-26 years).
After 26 months’ follow-up, 96%, 100%, and 84% of patients with early-, intermediate-, and advanced-stage HL, respectively, were in complete remission.
Perhaps not surprisingly, some advanced-stage patients fared worse, with four (6%) toxic and one (1.4%) unknown cause of death, five (7%) cases of early progression, and one (1.4%) partial remission in this group. One (4%) patient in the early-stage group also died because of toxicity.
Dr. Hentrich pointed out that treatment relapses and failures mainly occurred in patients with advanced disease.
Grade 3/4 toxicity was common and tended to occur in more patients who were treated with BEACOPP than AVBD, but the differences were statistically significantly only in the early-stage patients. The major hematologic toxicity was severe neutropenia.
At 2-years, progression-free and overall survival were 91.7% and 90.2%, respectively, for the whole population, and did not differ greatly between early-, intermediate-, and advanced-stage disease. However, patients with advanced disease and advanced HIV infection were more likely to have a reduced overall survival, compared with the other two groups of patients.
"The next strategy is to focus the amount of intensity to special patients, so we want to incorporate early PET scans after two cycles [of chemotherapy] and then de-escalate therapy or even escalate therapy," Dr. Hentrich said.
Dr. Hentrich had no financial disclosures or conflicts of interest.
FROM THE ANNUAL CONGRESS OF THE EUROPEAN HEMATOLOGY ASSOCIATION
Major Finding: At 2-years, progression-free and overall survival rates were 91.7% and 90.2%, respectively, for the whole population.
Data Source: Prospective, multicenter study of 108 HIV-associated Hodgkin’s lymphoma patients who were treated with chemotherapy according to the stage of hematologic malignancy.
Disclosures: Dr. Hentrich had no financial disclosures or conflicts of interest.
Studies Mixed on Second Cancers After Lenalidomide
CHICAGO – That lenalidomide can improve overall and progression-free survival rates in multiple myeloma patients is evident, but whether the drug also increases their risk of second primary cancers is debatable.
Of three studies looking at the question, only one found an association between secondary primary malignancies and lenalidomide (Revlimid) in first-line therapy, investigators reported at the American Society of Clinical Oncology annual meeting.
And even then the risk was low – far less than the risk of death from multiple myeloma without a lenalidomide-containing regimen, said Dr. Antonio P. Palumbo of the University of Torino (Italy) and the Italian Multiple Myeloma Study Group.
Two other studies – one with 6-year follow-up data on continuous lenalidomide in first-line therapy and the other on lenalidomide in relapsed/refractory disease – failed to spot a signal for second cancer risk.
"I think it’s fair to say that currently we lack clear answers due to small numbers and study limitations," said Dr. C. Ola Landgren of the National Cancer Institute, the invited discussant for all three papers.
"I think we need to put both benefits and risks into the algorithms when we think about these things. ... I also think despite the fact that we don’t have clear data, we always have to discuss these things with our patients, and we as doctors have to stay updated as more information emerges," he said.
Three randomized clinical trials stirred the debate by reporting in separate presentations at the 2010 annual meeting of the American Society of Hematology that they saw more hematologic malignancies in lenalidomide treatment arms than in control groups (McCarthy, P.L. et al, abstract 37; Attal, M. et al, abstract 310; Palumbo, A. et al, abstract 622).
Despite these reports, 25 years after a multiple myeloma diagnosis, the cumulative incidence of all second cancers is about 8%, whereas the cumulative probability of death from competing causes is more than 90%, suggesting that any risk of a second malignancy is far outweighed by the risk of multiple myeloma and its sequelae, Dr. Landgren pointed out.
First-Line Therapy: Italian Experience
In the first of the three studies presented at ASCO 2011, Dr. Palumbo’s group looked at second-cancer rates among patients randomly assigned to first-line therapy with either melphalan and prednisone alone, or to melphalan, prednisone, and lenalidomide with or without lenalidomide maintenance in the international MM-015 trial.
They found that at a median follow-up of 30 months, 12 of 150 (8%) patients on melphalan-prednisone plus lenalidomide with maintenance (MPR-R) developed an invasive second primary malignancy, compared with 9 of 152 patients (5.9%) on the same combination without lenalidomide maintenance (MPR), and 4 of 153 (2.6%) patients on melphalan and prednisone only.
Hematologic malignancies accounted for 7 of the 12 new cancers among patients treated with MPR-R, 5 of 9 on MPR, and 1 of 4 on MP. Solid tumors accounted for the remaining invasive cancers in each group. In addition, one patient on MPR-R, four on MPR, and five on MP developed nonmelanoma skin cancers.
In an additional analysis of 9 pooled experimental studies, the investigators found that among 1,788 patients followed for more than 1 year, the risk of dying of myeloma was greater than 40% out to 7 years compared with about a 2% risk of developing a second hematologic malignancy, and a 3% risk of developing a solid tumor.
Among patients receiving lenalidomide and an alkylating agent, the risk of developing any malignancy was around 7%, and the risk of dying of myeloma was about 27%. The risk of a second malignancy was lower – about 2% out to 6 years– among those patients who did not receive lenalidomide, but their risk of dying of myeloma was about 45%, Dr. Palumbo said.
He also pointed out that in the general population, the risk of a second primary malignancy among 65- to 74-year-olds is around 2% per 100 patient-years, and that the risk doubles among people 85 and older.
First-Line Therapy: BiRD Regimen
In the second study, Dr. Adriana Rossi and her colleagues at Cornell University, New York, and New York–Presbyterian Hospital examined the incidence of second primary cancers in 68 transplant-eligible patients receiving lenalidomide in first-line therapy as part of the BiRD regimen (clarithromycin [Biaxin], lenalidomide, and dexamethasone).
There were five solid tumors (two colon, one metastatic melanoma, one pancreas, and one prostate), but no hematologic malignancies. The melanoma was diagnosed 8 months after the primary myeloma diagnosis; the other cases occurred 25-53 months after the initial myeloma diagnosis (median, 31.2 months). The authors found no association between second primary cancers and a specific multiple myeloma chromosomal abnormality, prior malignancy, transplant status, study status, or sex.
The incidence rate of second primary malignancy was similar to that of all primary cancers reported among people 65 and older in the U.S. Surveillance, Epidemiology, and End Results (SEER) data set spanning 2003-2007, they noted.
"Routine screening and prevention measures should continue as medically indicated for all patients, including examination for skin cancers, and as survival in patients with multiple myeloma continues to improve, so will our understanding of their risk of development of second primary malignancies," she said.
Relapsed/Refractory Disease
The third trial looked at the risk of new primary cancers in patients receiving lenalidomide and dexamethasone for relapsed/refractory disease.
Dr. Meletios Dimopoulos of the University of Athens and colleagues in the international MM-009/010 trials performed a pooled analysis comparing the incidence of second primary cancers in 704 patients who received dexamethasone with either lenalidomide or placebo, and compared them with standard incidence rates.
They found that there were no differences in incidence rates of invasive second primary malignancies between patients in the lenalidomide plus dexamethasone arm or dexamethasone-only arms, and that the incidence rates of second primary cancers in general were low and similar to the background rate among people of similar age in the general population.
Additionally, patients who received lenalidomide and dexamethasone had significantly better overall survival (median, 38 months) despite the fact that about half of all patients in the placebo/dexamathesaone arm (median, 31.6 months) were crossed over to lenalidomide-based therapy (P = .045).
"The overall benefit-risk ratio of the use of lenalidomide in the relapsed/refractory setting remains strongly positive," said the presenter of the abstract, Dr. Ruben Niesvizky of Cornell University.
Lenalidomide is not approved as first-line therapy in the United States. Dr. Palumbo’s study was supported by the Fondazione Neoplasie Sangue Onlus. Dr. Rossi’s and Dr. Dimopoulos’s studies were funded by Celgene. Dr. Palumbo has received honoraria and served as a consultant to Celgene and other companies. Dr. Rossi said she had no relevant financial relationships to disclose. Dr. Dimopoulos disclosed receiving honoraria from Celgene. Dr. Niesvizky said he had received honoraria and research funding from Celgene; he also served in a consulting/advisory role for Celgene and other companies.
CHICAGO – That lenalidomide can improve overall and progression-free survival rates in multiple myeloma patients is evident, but whether the drug also increases their risk of second primary cancers is debatable.
Of three studies looking at the question, only one found an association between secondary primary malignancies and lenalidomide (Revlimid) in first-line therapy, investigators reported at the American Society of Clinical Oncology annual meeting.
And even then the risk was low – far less than the risk of death from multiple myeloma without a lenalidomide-containing regimen, said Dr. Antonio P. Palumbo of the University of Torino (Italy) and the Italian Multiple Myeloma Study Group.
Two other studies – one with 6-year follow-up data on continuous lenalidomide in first-line therapy and the other on lenalidomide in relapsed/refractory disease – failed to spot a signal for second cancer risk.
"I think it’s fair to say that currently we lack clear answers due to small numbers and study limitations," said Dr. C. Ola Landgren of the National Cancer Institute, the invited discussant for all three papers.
"I think we need to put both benefits and risks into the algorithms when we think about these things. ... I also think despite the fact that we don’t have clear data, we always have to discuss these things with our patients, and we as doctors have to stay updated as more information emerges," he said.
Three randomized clinical trials stirred the debate by reporting in separate presentations at the 2010 annual meeting of the American Society of Hematology that they saw more hematologic malignancies in lenalidomide treatment arms than in control groups (McCarthy, P.L. et al, abstract 37; Attal, M. et al, abstract 310; Palumbo, A. et al, abstract 622).
Despite these reports, 25 years after a multiple myeloma diagnosis, the cumulative incidence of all second cancers is about 8%, whereas the cumulative probability of death from competing causes is more than 90%, suggesting that any risk of a second malignancy is far outweighed by the risk of multiple myeloma and its sequelae, Dr. Landgren pointed out.
First-Line Therapy: Italian Experience
In the first of the three studies presented at ASCO 2011, Dr. Palumbo’s group looked at second-cancer rates among patients randomly assigned to first-line therapy with either melphalan and prednisone alone, or to melphalan, prednisone, and lenalidomide with or without lenalidomide maintenance in the international MM-015 trial.
They found that at a median follow-up of 30 months, 12 of 150 (8%) patients on melphalan-prednisone plus lenalidomide with maintenance (MPR-R) developed an invasive second primary malignancy, compared with 9 of 152 patients (5.9%) on the same combination without lenalidomide maintenance (MPR), and 4 of 153 (2.6%) patients on melphalan and prednisone only.
Hematologic malignancies accounted for 7 of the 12 new cancers among patients treated with MPR-R, 5 of 9 on MPR, and 1 of 4 on MP. Solid tumors accounted for the remaining invasive cancers in each group. In addition, one patient on MPR-R, four on MPR, and five on MP developed nonmelanoma skin cancers.
In an additional analysis of 9 pooled experimental studies, the investigators found that among 1,788 patients followed for more than 1 year, the risk of dying of myeloma was greater than 40% out to 7 years compared with about a 2% risk of developing a second hematologic malignancy, and a 3% risk of developing a solid tumor.
Among patients receiving lenalidomide and an alkylating agent, the risk of developing any malignancy was around 7%, and the risk of dying of myeloma was about 27%. The risk of a second malignancy was lower – about 2% out to 6 years– among those patients who did not receive lenalidomide, but their risk of dying of myeloma was about 45%, Dr. Palumbo said.
He also pointed out that in the general population, the risk of a second primary malignancy among 65- to 74-year-olds is around 2% per 100 patient-years, and that the risk doubles among people 85 and older.
First-Line Therapy: BiRD Regimen
In the second study, Dr. Adriana Rossi and her colleagues at Cornell University, New York, and New York–Presbyterian Hospital examined the incidence of second primary cancers in 68 transplant-eligible patients receiving lenalidomide in first-line therapy as part of the BiRD regimen (clarithromycin [Biaxin], lenalidomide, and dexamethasone).
There were five solid tumors (two colon, one metastatic melanoma, one pancreas, and one prostate), but no hematologic malignancies. The melanoma was diagnosed 8 months after the primary myeloma diagnosis; the other cases occurred 25-53 months after the initial myeloma diagnosis (median, 31.2 months). The authors found no association between second primary cancers and a specific multiple myeloma chromosomal abnormality, prior malignancy, transplant status, study status, or sex.
The incidence rate of second primary malignancy was similar to that of all primary cancers reported among people 65 and older in the U.S. Surveillance, Epidemiology, and End Results (SEER) data set spanning 2003-2007, they noted.
"Routine screening and prevention measures should continue as medically indicated for all patients, including examination for skin cancers, and as survival in patients with multiple myeloma continues to improve, so will our understanding of their risk of development of second primary malignancies," she said.
Relapsed/Refractory Disease
The third trial looked at the risk of new primary cancers in patients receiving lenalidomide and dexamethasone for relapsed/refractory disease.
Dr. Meletios Dimopoulos of the University of Athens and colleagues in the international MM-009/010 trials performed a pooled analysis comparing the incidence of second primary cancers in 704 patients who received dexamethasone with either lenalidomide or placebo, and compared them with standard incidence rates.
They found that there were no differences in incidence rates of invasive second primary malignancies between patients in the lenalidomide plus dexamethasone arm or dexamethasone-only arms, and that the incidence rates of second primary cancers in general were low and similar to the background rate among people of similar age in the general population.
Additionally, patients who received lenalidomide and dexamethasone had significantly better overall survival (median, 38 months) despite the fact that about half of all patients in the placebo/dexamathesaone arm (median, 31.6 months) were crossed over to lenalidomide-based therapy (P = .045).
"The overall benefit-risk ratio of the use of lenalidomide in the relapsed/refractory setting remains strongly positive," said the presenter of the abstract, Dr. Ruben Niesvizky of Cornell University.
Lenalidomide is not approved as first-line therapy in the United States. Dr. Palumbo’s study was supported by the Fondazione Neoplasie Sangue Onlus. Dr. Rossi’s and Dr. Dimopoulos’s studies were funded by Celgene. Dr. Palumbo has received honoraria and served as a consultant to Celgene and other companies. Dr. Rossi said she had no relevant financial relationships to disclose. Dr. Dimopoulos disclosed receiving honoraria from Celgene. Dr. Niesvizky said he had received honoraria and research funding from Celgene; he also served in a consulting/advisory role for Celgene and other companies.
CHICAGO – That lenalidomide can improve overall and progression-free survival rates in multiple myeloma patients is evident, but whether the drug also increases their risk of second primary cancers is debatable.
Of three studies looking at the question, only one found an association between secondary primary malignancies and lenalidomide (Revlimid) in first-line therapy, investigators reported at the American Society of Clinical Oncology annual meeting.
And even then the risk was low – far less than the risk of death from multiple myeloma without a lenalidomide-containing regimen, said Dr. Antonio P. Palumbo of the University of Torino (Italy) and the Italian Multiple Myeloma Study Group.
Two other studies – one with 6-year follow-up data on continuous lenalidomide in first-line therapy and the other on lenalidomide in relapsed/refractory disease – failed to spot a signal for second cancer risk.
"I think it’s fair to say that currently we lack clear answers due to small numbers and study limitations," said Dr. C. Ola Landgren of the National Cancer Institute, the invited discussant for all three papers.
"I think we need to put both benefits and risks into the algorithms when we think about these things. ... I also think despite the fact that we don’t have clear data, we always have to discuss these things with our patients, and we as doctors have to stay updated as more information emerges," he said.
Three randomized clinical trials stirred the debate by reporting in separate presentations at the 2010 annual meeting of the American Society of Hematology that they saw more hematologic malignancies in lenalidomide treatment arms than in control groups (McCarthy, P.L. et al, abstract 37; Attal, M. et al, abstract 310; Palumbo, A. et al, abstract 622).
Despite these reports, 25 years after a multiple myeloma diagnosis, the cumulative incidence of all second cancers is about 8%, whereas the cumulative probability of death from competing causes is more than 90%, suggesting that any risk of a second malignancy is far outweighed by the risk of multiple myeloma and its sequelae, Dr. Landgren pointed out.
First-Line Therapy: Italian Experience
In the first of the three studies presented at ASCO 2011, Dr. Palumbo’s group looked at second-cancer rates among patients randomly assigned to first-line therapy with either melphalan and prednisone alone, or to melphalan, prednisone, and lenalidomide with or without lenalidomide maintenance in the international MM-015 trial.
They found that at a median follow-up of 30 months, 12 of 150 (8%) patients on melphalan-prednisone plus lenalidomide with maintenance (MPR-R) developed an invasive second primary malignancy, compared with 9 of 152 patients (5.9%) on the same combination without lenalidomide maintenance (MPR), and 4 of 153 (2.6%) patients on melphalan and prednisone only.
Hematologic malignancies accounted for 7 of the 12 new cancers among patients treated with MPR-R, 5 of 9 on MPR, and 1 of 4 on MP. Solid tumors accounted for the remaining invasive cancers in each group. In addition, one patient on MPR-R, four on MPR, and five on MP developed nonmelanoma skin cancers.
In an additional analysis of 9 pooled experimental studies, the investigators found that among 1,788 patients followed for more than 1 year, the risk of dying of myeloma was greater than 40% out to 7 years compared with about a 2% risk of developing a second hematologic malignancy, and a 3% risk of developing a solid tumor.
Among patients receiving lenalidomide and an alkylating agent, the risk of developing any malignancy was around 7%, and the risk of dying of myeloma was about 27%. The risk of a second malignancy was lower – about 2% out to 6 years– among those patients who did not receive lenalidomide, but their risk of dying of myeloma was about 45%, Dr. Palumbo said.
He also pointed out that in the general population, the risk of a second primary malignancy among 65- to 74-year-olds is around 2% per 100 patient-years, and that the risk doubles among people 85 and older.
First-Line Therapy: BiRD Regimen
In the second study, Dr. Adriana Rossi and her colleagues at Cornell University, New York, and New York–Presbyterian Hospital examined the incidence of second primary cancers in 68 transplant-eligible patients receiving lenalidomide in first-line therapy as part of the BiRD regimen (clarithromycin [Biaxin], lenalidomide, and dexamethasone).
There were five solid tumors (two colon, one metastatic melanoma, one pancreas, and one prostate), but no hematologic malignancies. The melanoma was diagnosed 8 months after the primary myeloma diagnosis; the other cases occurred 25-53 months after the initial myeloma diagnosis (median, 31.2 months). The authors found no association between second primary cancers and a specific multiple myeloma chromosomal abnormality, prior malignancy, transplant status, study status, or sex.
The incidence rate of second primary malignancy was similar to that of all primary cancers reported among people 65 and older in the U.S. Surveillance, Epidemiology, and End Results (SEER) data set spanning 2003-2007, they noted.
"Routine screening and prevention measures should continue as medically indicated for all patients, including examination for skin cancers, and as survival in patients with multiple myeloma continues to improve, so will our understanding of their risk of development of second primary malignancies," she said.
Relapsed/Refractory Disease
The third trial looked at the risk of new primary cancers in patients receiving lenalidomide and dexamethasone for relapsed/refractory disease.
Dr. Meletios Dimopoulos of the University of Athens and colleagues in the international MM-009/010 trials performed a pooled analysis comparing the incidence of second primary cancers in 704 patients who received dexamethasone with either lenalidomide or placebo, and compared them with standard incidence rates.
They found that there were no differences in incidence rates of invasive second primary malignancies between patients in the lenalidomide plus dexamethasone arm or dexamethasone-only arms, and that the incidence rates of second primary cancers in general were low and similar to the background rate among people of similar age in the general population.
Additionally, patients who received lenalidomide and dexamethasone had significantly better overall survival (median, 38 months) despite the fact that about half of all patients in the placebo/dexamathesaone arm (median, 31.6 months) were crossed over to lenalidomide-based therapy (P = .045).
"The overall benefit-risk ratio of the use of lenalidomide in the relapsed/refractory setting remains strongly positive," said the presenter of the abstract, Dr. Ruben Niesvizky of Cornell University.
Lenalidomide is not approved as first-line therapy in the United States. Dr. Palumbo’s study was supported by the Fondazione Neoplasie Sangue Onlus. Dr. Rossi’s and Dr. Dimopoulos’s studies were funded by Celgene. Dr. Palumbo has received honoraria and served as a consultant to Celgene and other companies. Dr. Rossi said she had no relevant financial relationships to disclose. Dr. Dimopoulos disclosed receiving honoraria from Celgene. Dr. Niesvizky said he had received honoraria and research funding from Celgene; he also served in a consulting/advisory role for Celgene and other companies.
FROM THE ANNUAL MEETING OF THE AMERICAN SOCIETY OF CLINICAL ONCOLOGY
Major Finding: At a median follow-up of 30 months, 12 of 150 (8%) patients on melphalan-prednisone plus lenalidomide with maintenance developed an invasive second primary malignancy, compared with 9 of 152 patients (5.9%) on the same combination without lenalidomide maintenance, and 4 of 153 (2.6%) patients on melphalan and prednisone only. No increase was seen in analyses of two other trials.
Data Source: Analyses of three randomized clinical trials in which patients received lenalidomide for multiple myeloma.
Disclosures Lenalidomide is not approved as first-line therapy in the United States. Dr. Palumbo’s study was supported by the Fondazione Neoplasie Sangue Onlus. Dr. Rossi’s and Dr. Dimopoulos’s studies were funded by Celgene. Dr. Palumbo has received honoraria and served as a consultant to Celgene and other companies. Dr. Rossi said she had no relevant financial relationships to disclose. Dr. Dimopoulos disclosed receiving honoraria from Celgene. Dr. Niesvizky said he had received honoraria and research funding from Celgene; he also served in a consulting/advisory role with Celgene and other companies.
Rituximab Maintenance Called "New Standard" for Mantle Cell Lymphoma
LONDON – Rituximab more than doubled the duration of remission in elderly patients with mantle cell lymphoma when used as maintenance therapy in those who had already responded to induction therapy in a large, randomized controlled trial.
First results from the European Mantle Cell Lymphoma (MCL) Network study show that rituximab maintenance is associated with a median remission of 77 months. In comparison, when interferon (IFN) was used as maintenance, the median was 24 months (hazard ratio, 0.54; P = .0109).
Overall survival data are not yet fully mature but suggest that rituximab (Rituxan in the United States, Mabthera in Europe) improves upon the rates achievable. At 4 years’ follow-up, 62% of patients treated with IFN and 77% of those maintained on rituximab were still alive. This difference was not statistically significant, however.
Rituximab is not licensed for the treatment of MCL in Europe or the United States.
"Rituximab after R-CHOP [rituximab, cyclophosphamide (Cytoxan), hydroxydaunorubicin (doxorubicin, Adriamycin), Oncovin (vincristine), and prednisolone] should become the new standard for elderly MCL patients to which new regimens should be compared," said study investigator Dr. Hanneke C. Kluin-Nelemans of the University Medical Center of Groningen, the Netherlands, while reporting the findings at the annual congress of the European Hematology Association.
"MCL is a disease of the elderly," Dr. Kluin-Nelemans observed. More than 60% of patients with MCL are aged 60 years or older, and treatment options can be limited. High-dose chemotherapy and autologous stem cell transplantation are not always possible, and "almost all patients relapse" after initial immunochemotherapy. Furthermore, overall survival is about 3-5 years in those who are aged 60 years and up, Dr. Kluin-Nelemans said.
Patients in the trial had previously received induction therapy with R-CHOP or R-FC (rituximab plus fludarabine with cyclophosphamide).
The study consisted of two randomization phases, the first of which saw 560 newly diagnosed, fit (performance status 0-2), elderly patients with MCL treated with either eight cycles of R-CHOP or six cycles of R-FC. The 310 patients who responded to either regimen entered the second randomization phase – this time to treatment with single-agent IFN or rituximab alone as maintenance therapy. IFN was given as 1-3 doses/week depending on the formulation used (IFN-alpha or peg-IFN), and rituximab (375 mg/m2) was given as a single dose every 2 months until disease progression.
The study was closed early in October 2010 under the advisement of the trial’s Data Safety Monitoring Board, as the data favored rituximab over IFN as maintenance therapy, and the R-CHOP regimen was clearly better than R-FC regimen.
Per-protocol results showed a significant improvement in remission during maintenance treatment with rituximab vs. IFN. These data remained significant in an intent-to-treat analysis.
The investigators also looked to see what effects the induction regimens could have on the maintenance phase results, and found that the duration of remission was significantly better in patients who received R-CHOP than in those given R-FC.
Dr. Kluin-Nelemans was questioned after her presentation as to that lack of a placebo-controlled arm. In response, she said that an analysis had looked at 87 of 250 patients who were not randomized to maintenance treatment. All had stopped rituximab treatment before they could be randomized, and were thus a population of patients that could potentially benefit.
Rituximab was associated with significantly less fatigue (P less than .001) and fewer infections (P less than .022), and was less likely to decrease white blood cell and platelet counts (P less than .001) than IFN. The rate of more serious infections was also lower than with IFN (P less than .022)
Considering the efficacy findings and the fact that there was also low toxicity associated with rituximab compared with IFN, these data suggest that the CD-20-targeting agent could be a better option for maintenance therapy than other biologic or immunomodulatory agents.
"We have shown it’s possible to do a large [randomized controlled trial] with two randomization steps in fit, elderly patients with MCL," Dr. Kluin-Nelemans said. "Rituximab more than doubles the remission duration in patients depending upon initial therapy."
Dr. Kluin-Nelemans stated that she had no conflicts of interest related to her presentation.
LONDON – Rituximab more than doubled the duration of remission in elderly patients with mantle cell lymphoma when used as maintenance therapy in those who had already responded to induction therapy in a large, randomized controlled trial.
First results from the European Mantle Cell Lymphoma (MCL) Network study show that rituximab maintenance is associated with a median remission of 77 months. In comparison, when interferon (IFN) was used as maintenance, the median was 24 months (hazard ratio, 0.54; P = .0109).
Overall survival data are not yet fully mature but suggest that rituximab (Rituxan in the United States, Mabthera in Europe) improves upon the rates achievable. At 4 years’ follow-up, 62% of patients treated with IFN and 77% of those maintained on rituximab were still alive. This difference was not statistically significant, however.
Rituximab is not licensed for the treatment of MCL in Europe or the United States.
"Rituximab after R-CHOP [rituximab, cyclophosphamide (Cytoxan), hydroxydaunorubicin (doxorubicin, Adriamycin), Oncovin (vincristine), and prednisolone] should become the new standard for elderly MCL patients to which new regimens should be compared," said study investigator Dr. Hanneke C. Kluin-Nelemans of the University Medical Center of Groningen, the Netherlands, while reporting the findings at the annual congress of the European Hematology Association.
"MCL is a disease of the elderly," Dr. Kluin-Nelemans observed. More than 60% of patients with MCL are aged 60 years or older, and treatment options can be limited. High-dose chemotherapy and autologous stem cell transplantation are not always possible, and "almost all patients relapse" after initial immunochemotherapy. Furthermore, overall survival is about 3-5 years in those who are aged 60 years and up, Dr. Kluin-Nelemans said.
Patients in the trial had previously received induction therapy with R-CHOP or R-FC (rituximab plus fludarabine with cyclophosphamide).
The study consisted of two randomization phases, the first of which saw 560 newly diagnosed, fit (performance status 0-2), elderly patients with MCL treated with either eight cycles of R-CHOP or six cycles of R-FC. The 310 patients who responded to either regimen entered the second randomization phase – this time to treatment with single-agent IFN or rituximab alone as maintenance therapy. IFN was given as 1-3 doses/week depending on the formulation used (IFN-alpha or peg-IFN), and rituximab (375 mg/m2) was given as a single dose every 2 months until disease progression.
The study was closed early in October 2010 under the advisement of the trial’s Data Safety Monitoring Board, as the data favored rituximab over IFN as maintenance therapy, and the R-CHOP regimen was clearly better than R-FC regimen.
Per-protocol results showed a significant improvement in remission during maintenance treatment with rituximab vs. IFN. These data remained significant in an intent-to-treat analysis.
The investigators also looked to see what effects the induction regimens could have on the maintenance phase results, and found that the duration of remission was significantly better in patients who received R-CHOP than in those given R-FC.
Dr. Kluin-Nelemans was questioned after her presentation as to that lack of a placebo-controlled arm. In response, she said that an analysis had looked at 87 of 250 patients who were not randomized to maintenance treatment. All had stopped rituximab treatment before they could be randomized, and were thus a population of patients that could potentially benefit.
Rituximab was associated with significantly less fatigue (P less than .001) and fewer infections (P less than .022), and was less likely to decrease white blood cell and platelet counts (P less than .001) than IFN. The rate of more serious infections was also lower than with IFN (P less than .022)
Considering the efficacy findings and the fact that there was also low toxicity associated with rituximab compared with IFN, these data suggest that the CD-20-targeting agent could be a better option for maintenance therapy than other biologic or immunomodulatory agents.
"We have shown it’s possible to do a large [randomized controlled trial] with two randomization steps in fit, elderly patients with MCL," Dr. Kluin-Nelemans said. "Rituximab more than doubles the remission duration in patients depending upon initial therapy."
Dr. Kluin-Nelemans stated that she had no conflicts of interest related to her presentation.
LONDON – Rituximab more than doubled the duration of remission in elderly patients with mantle cell lymphoma when used as maintenance therapy in those who had already responded to induction therapy in a large, randomized controlled trial.
First results from the European Mantle Cell Lymphoma (MCL) Network study show that rituximab maintenance is associated with a median remission of 77 months. In comparison, when interferon (IFN) was used as maintenance, the median was 24 months (hazard ratio, 0.54; P = .0109).
Overall survival data are not yet fully mature but suggest that rituximab (Rituxan in the United States, Mabthera in Europe) improves upon the rates achievable. At 4 years’ follow-up, 62% of patients treated with IFN and 77% of those maintained on rituximab were still alive. This difference was not statistically significant, however.
Rituximab is not licensed for the treatment of MCL in Europe or the United States.
"Rituximab after R-CHOP [rituximab, cyclophosphamide (Cytoxan), hydroxydaunorubicin (doxorubicin, Adriamycin), Oncovin (vincristine), and prednisolone] should become the new standard for elderly MCL patients to which new regimens should be compared," said study investigator Dr. Hanneke C. Kluin-Nelemans of the University Medical Center of Groningen, the Netherlands, while reporting the findings at the annual congress of the European Hematology Association.
"MCL is a disease of the elderly," Dr. Kluin-Nelemans observed. More than 60% of patients with MCL are aged 60 years or older, and treatment options can be limited. High-dose chemotherapy and autologous stem cell transplantation are not always possible, and "almost all patients relapse" after initial immunochemotherapy. Furthermore, overall survival is about 3-5 years in those who are aged 60 years and up, Dr. Kluin-Nelemans said.
Patients in the trial had previously received induction therapy with R-CHOP or R-FC (rituximab plus fludarabine with cyclophosphamide).
The study consisted of two randomization phases, the first of which saw 560 newly diagnosed, fit (performance status 0-2), elderly patients with MCL treated with either eight cycles of R-CHOP or six cycles of R-FC. The 310 patients who responded to either regimen entered the second randomization phase – this time to treatment with single-agent IFN or rituximab alone as maintenance therapy. IFN was given as 1-3 doses/week depending on the formulation used (IFN-alpha or peg-IFN), and rituximab (375 mg/m2) was given as a single dose every 2 months until disease progression.
The study was closed early in October 2010 under the advisement of the trial’s Data Safety Monitoring Board, as the data favored rituximab over IFN as maintenance therapy, and the R-CHOP regimen was clearly better than R-FC regimen.
Per-protocol results showed a significant improvement in remission during maintenance treatment with rituximab vs. IFN. These data remained significant in an intent-to-treat analysis.
The investigators also looked to see what effects the induction regimens could have on the maintenance phase results, and found that the duration of remission was significantly better in patients who received R-CHOP than in those given R-FC.
Dr. Kluin-Nelemans was questioned after her presentation as to that lack of a placebo-controlled arm. In response, she said that an analysis had looked at 87 of 250 patients who were not randomized to maintenance treatment. All had stopped rituximab treatment before they could be randomized, and were thus a population of patients that could potentially benefit.
Rituximab was associated with significantly less fatigue (P less than .001) and fewer infections (P less than .022), and was less likely to decrease white blood cell and platelet counts (P less than .001) than IFN. The rate of more serious infections was also lower than with IFN (P less than .022)
Considering the efficacy findings and the fact that there was also low toxicity associated with rituximab compared with IFN, these data suggest that the CD-20-targeting agent could be a better option for maintenance therapy than other biologic or immunomodulatory agents.
"We have shown it’s possible to do a large [randomized controlled trial] with two randomization steps in fit, elderly patients with MCL," Dr. Kluin-Nelemans said. "Rituximab more than doubles the remission duration in patients depending upon initial therapy."
Dr. Kluin-Nelemans stated that she had no conflicts of interest related to her presentation.
FROM THE ANNUAL CONGRESS OF THE EUROPEAN HEMATOLOGY ASSOCIATION
Major Finding: After induction therapy, rituximab-treated patients experienced a median remission of 77 months, compared with 24 months in interferon-alpha-treated patients (HR, 0.54; P = .0109).
Data Source: A 560-patient trial conducted by the European Mantle Cell Lymphoma Network in elderly patients who were subject to two randomized comparisons: 1) R-CHOP or R-FC as induction treatment; or 2) interferon or rituximab as maintenance.
Disclosures: Dr. Kluin-Nelemans stated that she had no conflicts of interest related to her presentation.
Rituximab Maintenance Called "New Standard" for Mantle Cell Lymphoma
LONDON – Rituximab more than doubled the duration of remission in elderly patients with mantle cell lymphoma when used as maintenance therapy in those who had already responded to induction therapy in a large, randomized controlled trial.
First results from the European Mantle Cell Lymphoma (MCL) Network study show that rituximab maintenance is associated with a median remission of 77 months. In comparison, when interferon (IFN) was used as maintenance, the median was 24 months (hazard ratio, 0.54; P = .0109).
Overall survival data are not yet fully mature but suggest that rituximab (Rituxan in the United States, Mabthera in Europe) improves upon the rates achievable. At 4 years’ follow-up, 62% of patients treated with IFN and 77% of those maintained on rituximab were still alive. This difference was not statistically significant, however.
Rituximab is not licensed for the treatment of MCL in Europe or the United States.
"Rituximab after R-CHOP [rituximab, cyclophosphamide (Cytoxan), hydroxydaunorubicin (doxorubicin, Adriamycin), Oncovin (vincristine), and prednisolone] should become the new standard for elderly MCL patients to which new regimens should be compared," said study investigator Dr. Hanneke C. Kluin-Nelemans of the University Medical Center of Groningen, the Netherlands, while reporting the findings at the annual congress of the European Hematology Association.
"MCL is a disease of the elderly," Dr. Kluin-Nelemans observed. More than 60% of patients with MCL are aged 60 years or older, and treatment options can be limited. High-dose chemotherapy and autologous stem cell transplantation are not always possible, and "almost all patients relapse" after initial immunochemotherapy. Furthermore, overall survival is about 3-5 years in those who are aged 60 years and up, Dr. Kluin-Nelemans said.
Patients in the trial had previously received induction therapy with R-CHOP or R-FC (rituximab plus fludarabine with cyclophosphamide).
The study consisted of two randomization phases, the first of which saw 560 newly diagnosed, fit (performance status 0-2), elderly patients with MCL treated with either eight cycles of R-CHOP or six cycles of R-FC. The 310 patients who responded to either regimen entered the second randomization phase – this time to treatment with single-agent IFN or rituximab alone as maintenance therapy. IFN was given as 1-3 doses/week depending on the formulation used (IFN-alpha or peg-IFN), and rituximab (375 mg/m2) was given as a single dose every 2 months until disease progression.
The study was closed early in October 2010 under the advisement of the trial’s Data Safety Monitoring Board, as the data favored rituximab over IFN as maintenance therapy, and the R-CHOP regimen was clearly better than R-FC regimen.
Per-protocol results showed a significant improvement in remission during maintenance treatment with rituximab vs. IFN. These data remained significant in an intent-to-treat analysis.
The investigators also looked to see what effects the induction regimens could have on the maintenance phase results, and found that the duration of remission was significantly better in patients who received R-CHOP than in those given R-FC.
Dr. Kluin-Nelemans was questioned after her presentation as to that lack of a placebo-controlled arm. In response, she said that an analysis had looked at 87 of 250 patients who were not randomized to maintenance treatment. All had stopped rituximab treatment before they could be randomized, and were thus a population of patients that could potentially benefit.
Rituximab was associated with significantly less fatigue (P less than .001) and fewer infections (P less than .022), and was less likely to decrease white blood cell and platelet counts (P less than .001) than IFN. The rate of more serious infections was also lower than with IFN (P less than .022)
Considering the efficacy findings and the fact that there was also low toxicity associated with rituximab compared with IFN, these data suggest that the CD-20-targeting agent could be a better option for maintenance therapy than other biologic or immunomodulatory agents.
"We have shown it’s possible to do a large [randomized controlled trial] with two randomization steps in fit, elderly patients with MCL," Dr. Kluin-Nelemans said. "Rituximab more than doubles the remission duration in patients depending upon initial therapy."
Dr. Kluin-Nelemans stated that she had no conflicts of interest related to her presentation.
LONDON – Rituximab more than doubled the duration of remission in elderly patients with mantle cell lymphoma when used as maintenance therapy in those who had already responded to induction therapy in a large, randomized controlled trial.
First results from the European Mantle Cell Lymphoma (MCL) Network study show that rituximab maintenance is associated with a median remission of 77 months. In comparison, when interferon (IFN) was used as maintenance, the median was 24 months (hazard ratio, 0.54; P = .0109).
Overall survival data are not yet fully mature but suggest that rituximab (Rituxan in the United States, Mabthera in Europe) improves upon the rates achievable. At 4 years’ follow-up, 62% of patients treated with IFN and 77% of those maintained on rituximab were still alive. This difference was not statistically significant, however.
Rituximab is not licensed for the treatment of MCL in Europe or the United States.
"Rituximab after R-CHOP [rituximab, cyclophosphamide (Cytoxan), hydroxydaunorubicin (doxorubicin, Adriamycin), Oncovin (vincristine), and prednisolone] should become the new standard for elderly MCL patients to which new regimens should be compared," said study investigator Dr. Hanneke C. Kluin-Nelemans of the University Medical Center of Groningen, the Netherlands, while reporting the findings at the annual congress of the European Hematology Association.
"MCL is a disease of the elderly," Dr. Kluin-Nelemans observed. More than 60% of patients with MCL are aged 60 years or older, and treatment options can be limited. High-dose chemotherapy and autologous stem cell transplantation are not always possible, and "almost all patients relapse" after initial immunochemotherapy. Furthermore, overall survival is about 3-5 years in those who are aged 60 years and up, Dr. Kluin-Nelemans said.
Patients in the trial had previously received induction therapy with R-CHOP or R-FC (rituximab plus fludarabine with cyclophosphamide).
The study consisted of two randomization phases, the first of which saw 560 newly diagnosed, fit (performance status 0-2), elderly patients with MCL treated with either eight cycles of R-CHOP or six cycles of R-FC. The 310 patients who responded to either regimen entered the second randomization phase – this time to treatment with single-agent IFN or rituximab alone as maintenance therapy. IFN was given as 1-3 doses/week depending on the formulation used (IFN-alpha or peg-IFN), and rituximab (375 mg/m2) was given as a single dose every 2 months until disease progression.
The study was closed early in October 2010 under the advisement of the trial’s Data Safety Monitoring Board, as the data favored rituximab over IFN as maintenance therapy, and the R-CHOP regimen was clearly better than R-FC regimen.
Per-protocol results showed a significant improvement in remission during maintenance treatment with rituximab vs. IFN. These data remained significant in an intent-to-treat analysis.
The investigators also looked to see what effects the induction regimens could have on the maintenance phase results, and found that the duration of remission was significantly better in patients who received R-CHOP than in those given R-FC.
Dr. Kluin-Nelemans was questioned after her presentation as to that lack of a placebo-controlled arm. In response, she said that an analysis had looked at 87 of 250 patients who were not randomized to maintenance treatment. All had stopped rituximab treatment before they could be randomized, and were thus a population of patients that could potentially benefit.
Rituximab was associated with significantly less fatigue (P less than .001) and fewer infections (P less than .022), and was less likely to decrease white blood cell and platelet counts (P less than .001) than IFN. The rate of more serious infections was also lower than with IFN (P less than .022)
Considering the efficacy findings and the fact that there was also low toxicity associated with rituximab compared with IFN, these data suggest that the CD-20-targeting agent could be a better option for maintenance therapy than other biologic or immunomodulatory agents.
"We have shown it’s possible to do a large [randomized controlled trial] with two randomization steps in fit, elderly patients with MCL," Dr. Kluin-Nelemans said. "Rituximab more than doubles the remission duration in patients depending upon initial therapy."
Dr. Kluin-Nelemans stated that she had no conflicts of interest related to her presentation.
LONDON – Rituximab more than doubled the duration of remission in elderly patients with mantle cell lymphoma when used as maintenance therapy in those who had already responded to induction therapy in a large, randomized controlled trial.
First results from the European Mantle Cell Lymphoma (MCL) Network study show that rituximab maintenance is associated with a median remission of 77 months. In comparison, when interferon (IFN) was used as maintenance, the median was 24 months (hazard ratio, 0.54; P = .0109).
Overall survival data are not yet fully mature but suggest that rituximab (Rituxan in the United States, Mabthera in Europe) improves upon the rates achievable. At 4 years’ follow-up, 62% of patients treated with IFN and 77% of those maintained on rituximab were still alive. This difference was not statistically significant, however.
Rituximab is not licensed for the treatment of MCL in Europe or the United States.
"Rituximab after R-CHOP [rituximab, cyclophosphamide (Cytoxan), hydroxydaunorubicin (doxorubicin, Adriamycin), Oncovin (vincristine), and prednisolone] should become the new standard for elderly MCL patients to which new regimens should be compared," said study investigator Dr. Hanneke C. Kluin-Nelemans of the University Medical Center of Groningen, the Netherlands, while reporting the findings at the annual congress of the European Hematology Association.
"MCL is a disease of the elderly," Dr. Kluin-Nelemans observed. More than 60% of patients with MCL are aged 60 years or older, and treatment options can be limited. High-dose chemotherapy and autologous stem cell transplantation are not always possible, and "almost all patients relapse" after initial immunochemotherapy. Furthermore, overall survival is about 3-5 years in those who are aged 60 years and up, Dr. Kluin-Nelemans said.
Patients in the trial had previously received induction therapy with R-CHOP or R-FC (rituximab plus fludarabine with cyclophosphamide).
The study consisted of two randomization phases, the first of which saw 560 newly diagnosed, fit (performance status 0-2), elderly patients with MCL treated with either eight cycles of R-CHOP or six cycles of R-FC. The 310 patients who responded to either regimen entered the second randomization phase – this time to treatment with single-agent IFN or rituximab alone as maintenance therapy. IFN was given as 1-3 doses/week depending on the formulation used (IFN-alpha or peg-IFN), and rituximab (375 mg/m2) was given as a single dose every 2 months until disease progression.
The study was closed early in October 2010 under the advisement of the trial’s Data Safety Monitoring Board, as the data favored rituximab over IFN as maintenance therapy, and the R-CHOP regimen was clearly better than R-FC regimen.
Per-protocol results showed a significant improvement in remission during maintenance treatment with rituximab vs. IFN. These data remained significant in an intent-to-treat analysis.
The investigators also looked to see what effects the induction regimens could have on the maintenance phase results, and found that the duration of remission was significantly better in patients who received R-CHOP than in those given R-FC.
Dr. Kluin-Nelemans was questioned after her presentation as to that lack of a placebo-controlled arm. In response, she said that an analysis had looked at 87 of 250 patients who were not randomized to maintenance treatment. All had stopped rituximab treatment before they could be randomized, and were thus a population of patients that could potentially benefit.
Rituximab was associated with significantly less fatigue (P less than .001) and fewer infections (P less than .022), and was less likely to decrease white blood cell and platelet counts (P less than .001) than IFN. The rate of more serious infections was also lower than with IFN (P less than .022)
Considering the efficacy findings and the fact that there was also low toxicity associated with rituximab compared with IFN, these data suggest that the CD-20-targeting agent could be a better option for maintenance therapy than other biologic or immunomodulatory agents.
"We have shown it’s possible to do a large [randomized controlled trial] with two randomization steps in fit, elderly patients with MCL," Dr. Kluin-Nelemans said. "Rituximab more than doubles the remission duration in patients depending upon initial therapy."
Dr. Kluin-Nelemans stated that she had no conflicts of interest related to her presentation.
FROM THE ANNUAL CONGRESS OF THE EUROPEAN HEMATOLOGY ASSOCIATION
Major Finding: After induction therapy, rituximab-treated patients experienced a median remission of 77 months, compared with 24 months in interferon-alpha-treated patients (HR, 0.54; P = .0109).
Data Source: A 560-patient trial conducted by the European Mantle Cell Lymphoma Network in elderly patients who were subject to two randomized comparisons: 1) R-CHOP or R-FC as induction treatment; or 2) interferon or rituximab as maintenance.
Disclosures: Dr. Kluin-Nelemans stated that she had no conflicts of interest related to her presentation.
Chemo Length May Not Affect Survival in Some B-cell Lymphomas
CHICAGO – It doesn’t seem to matter whether patients with newly diagnosed, diffuse large B-cell lymphoma receive a standard chemotherapy regimen in a dose-dense fashion every 14 days for six cycles, or every 21 days for eight cycles, said investigators in a multinational trial that was presented at the annual meeting of the American Society of Clinical Oncology.
There were no significant differences in the primary outcome of overall survival or the secondary outcome of failure-free survival among 1,080 patients who were randomly assigned to the two R-CHOP (rituximab plus cyclophosphamide, doxorubicin, vincristine, and prednisone) regimens, reported Dr. David Cunningham of the Royal Marsden Hospital in London, on behalf of colleagues in the U.K. National Cancer Research Institute’s lymphoma clinical study group.
Half the population received R-CHOP every 3 weeks for eight cycles (R-CHOP-21), and the other half was assigned to R-CHOP every 2 weeks for six cycles, followed by two additional rituximab infusions (R-CHOP-14).
Dr. Cunningham highlighted the following findings:
• The 2-year overall survival rates were 81% in the R-CHOP-21 arm, and 83% in the R-CHOP-14 arm (log rank P = .70).
• Overall response rates (a combination of complete responses [CR], complete unconfirmed responses [CRu], and partial responses [PR]) were 88% in R-CHOP-21 and 90% in R-CHOP-14 (P = .11).
• Rates of combined CR/CRu were 63% and 58%, respectively (P = .15).
• The 2-year failure-free survival rates were identical, at 75% in each group.
Toxicities were also generally similar between the treatment groups, except for a lower incidence of neutropenia in the R-CHOP-14 arm, which reflected primary prophylaxis with granulocyte-colony-stimulating factor (G-CSF) in that group.
There were no differences in failure-free survival between the treatment arms when patients were stratified by age, sex, disease stage, bulky disease, B symptoms, prognostic score, IPI (International Prognostic Index) score, cell proliferation (as measured by the MIB-1 monoclonal antibody), or diffuse large B-cell lymphoma (DLBCL) phenotype.
"We couldn’t actually identify any of the subsets or subgroups that benefited from one or the other treatment," Dr. Cunningham said.
Dr. Julie Vose of the University of Nebraska Medical Center in Omaha, the invited discussant, commented that the study "compared some questions that have been burning in our minds for a long time," calling it a "very robust analysis of a very important study."
Summing up this study and three other abstracts that looked at alternative therapies for DLBCL, Dr. Vose said that R-CHOP-21 is still the standard of care for young patients with low, low/intermediate, or high/intermediate IPI scores, although R-CHOP-14 plus two rituximab infusions or R-CHOEP (R-CHOP plus etoposide) are acceptable alternatives. For young patients with high IPI, R-CHOP-21 followed by consolidation autologous transplant should be offered. For older patients, R-CHOP-21 for eight cycles is equivalent to R-CHOP-14 for six cycles plus two rituximab infusions.
The trial began recruiting after a 2004 German study showed that a dose-dense regimen of six cycles of CHOP-14 improved 5-year overall survival in patients older than 60 years by 13%, compared with six cycles of CHOP-21 (Blood 2004;104:634-41).
Since that publication, however, the addition of rituximab to six or eight cycles of CHOP or similar chemotherapy regimens was shown to improve overall survival of DLBCL by 10%-16% in two trials. Those findings raised interest in whether CHOP-14 might still be superior to CHOP-21 in patients who also receive rituximab, and whether such an effect would be seen across all age groups, Dr. Cunningham said.
He reported the final results of the trial, which involved 1,080 adults who had newly diagnosed CD20-positive DLBCL and were recruited from 119 sites. The patients were stratified by IPI score, age (60 years and younger, or older than 60), and treatment center.
In all, 23% of patients on R-CHOP-21 and 22% on R-CHOP-14 had died by the time of the final study analysis. DLBCL was the leading cause of death in both arms. Other causes included treatment-related toxicity, cardiac causes (all cardiac deaths occurred 3-15 months after completion of therapy), secondary malignancy, and other/unknown causes.
In her discussion, Dr. Vose pointed out that R-CHOP-14, which requires G-CSF support after every cycle, costs about $31,308, compared with $29,247 for R-CHOP-21, in which G-CSF is used only to treat (but not to prevent) neutropenia or febrile neutropenia. In the trial, G-CSF was used in 38% of R-CHOP-21 cycles, compared with 100% of R-CHOP-14 cycles.
In addition, R-CHOP every 21 days for six cycles (not eight) is generally considered to be the standard of care in the United States, she noted; a direct comparison of this shorter regimen with R-CHOP-14 would have been welcome, she said.
The trial was funded by the U.K. National Cancer Research Institute. The authors had no relevant financial disclosures.
CHICAGO – It doesn’t seem to matter whether patients with newly diagnosed, diffuse large B-cell lymphoma receive a standard chemotherapy regimen in a dose-dense fashion every 14 days for six cycles, or every 21 days for eight cycles, said investigators in a multinational trial that was presented at the annual meeting of the American Society of Clinical Oncology.
There were no significant differences in the primary outcome of overall survival or the secondary outcome of failure-free survival among 1,080 patients who were randomly assigned to the two R-CHOP (rituximab plus cyclophosphamide, doxorubicin, vincristine, and prednisone) regimens, reported Dr. David Cunningham of the Royal Marsden Hospital in London, on behalf of colleagues in the U.K. National Cancer Research Institute’s lymphoma clinical study group.
Half the population received R-CHOP every 3 weeks for eight cycles (R-CHOP-21), and the other half was assigned to R-CHOP every 2 weeks for six cycles, followed by two additional rituximab infusions (R-CHOP-14).
Dr. Cunningham highlighted the following findings:
• The 2-year overall survival rates were 81% in the R-CHOP-21 arm, and 83% in the R-CHOP-14 arm (log rank P = .70).
• Overall response rates (a combination of complete responses [CR], complete unconfirmed responses [CRu], and partial responses [PR]) were 88% in R-CHOP-21 and 90% in R-CHOP-14 (P = .11).
• Rates of combined CR/CRu were 63% and 58%, respectively (P = .15).
• The 2-year failure-free survival rates were identical, at 75% in each group.
Toxicities were also generally similar between the treatment groups, except for a lower incidence of neutropenia in the R-CHOP-14 arm, which reflected primary prophylaxis with granulocyte-colony-stimulating factor (G-CSF) in that group.
There were no differences in failure-free survival between the treatment arms when patients were stratified by age, sex, disease stage, bulky disease, B symptoms, prognostic score, IPI (International Prognostic Index) score, cell proliferation (as measured by the MIB-1 monoclonal antibody), or diffuse large B-cell lymphoma (DLBCL) phenotype.
"We couldn’t actually identify any of the subsets or subgroups that benefited from one or the other treatment," Dr. Cunningham said.
Dr. Julie Vose of the University of Nebraska Medical Center in Omaha, the invited discussant, commented that the study "compared some questions that have been burning in our minds for a long time," calling it a "very robust analysis of a very important study."
Summing up this study and three other abstracts that looked at alternative therapies for DLBCL, Dr. Vose said that R-CHOP-21 is still the standard of care for young patients with low, low/intermediate, or high/intermediate IPI scores, although R-CHOP-14 plus two rituximab infusions or R-CHOEP (R-CHOP plus etoposide) are acceptable alternatives. For young patients with high IPI, R-CHOP-21 followed by consolidation autologous transplant should be offered. For older patients, R-CHOP-21 for eight cycles is equivalent to R-CHOP-14 for six cycles plus two rituximab infusions.
The trial began recruiting after a 2004 German study showed that a dose-dense regimen of six cycles of CHOP-14 improved 5-year overall survival in patients older than 60 years by 13%, compared with six cycles of CHOP-21 (Blood 2004;104:634-41).
Since that publication, however, the addition of rituximab to six or eight cycles of CHOP or similar chemotherapy regimens was shown to improve overall survival of DLBCL by 10%-16% in two trials. Those findings raised interest in whether CHOP-14 might still be superior to CHOP-21 in patients who also receive rituximab, and whether such an effect would be seen across all age groups, Dr. Cunningham said.
He reported the final results of the trial, which involved 1,080 adults who had newly diagnosed CD20-positive DLBCL and were recruited from 119 sites. The patients were stratified by IPI score, age (60 years and younger, or older than 60), and treatment center.
In all, 23% of patients on R-CHOP-21 and 22% on R-CHOP-14 had died by the time of the final study analysis. DLBCL was the leading cause of death in both arms. Other causes included treatment-related toxicity, cardiac causes (all cardiac deaths occurred 3-15 months after completion of therapy), secondary malignancy, and other/unknown causes.
In her discussion, Dr. Vose pointed out that R-CHOP-14, which requires G-CSF support after every cycle, costs about $31,308, compared with $29,247 for R-CHOP-21, in which G-CSF is used only to treat (but not to prevent) neutropenia or febrile neutropenia. In the trial, G-CSF was used in 38% of R-CHOP-21 cycles, compared with 100% of R-CHOP-14 cycles.
In addition, R-CHOP every 21 days for six cycles (not eight) is generally considered to be the standard of care in the United States, she noted; a direct comparison of this shorter regimen with R-CHOP-14 would have been welcome, she said.
The trial was funded by the U.K. National Cancer Research Institute. The authors had no relevant financial disclosures.
CHICAGO – It doesn’t seem to matter whether patients with newly diagnosed, diffuse large B-cell lymphoma receive a standard chemotherapy regimen in a dose-dense fashion every 14 days for six cycles, or every 21 days for eight cycles, said investigators in a multinational trial that was presented at the annual meeting of the American Society of Clinical Oncology.
There were no significant differences in the primary outcome of overall survival or the secondary outcome of failure-free survival among 1,080 patients who were randomly assigned to the two R-CHOP (rituximab plus cyclophosphamide, doxorubicin, vincristine, and prednisone) regimens, reported Dr. David Cunningham of the Royal Marsden Hospital in London, on behalf of colleagues in the U.K. National Cancer Research Institute’s lymphoma clinical study group.
Half the population received R-CHOP every 3 weeks for eight cycles (R-CHOP-21), and the other half was assigned to R-CHOP every 2 weeks for six cycles, followed by two additional rituximab infusions (R-CHOP-14).
Dr. Cunningham highlighted the following findings:
• The 2-year overall survival rates were 81% in the R-CHOP-21 arm, and 83% in the R-CHOP-14 arm (log rank P = .70).
• Overall response rates (a combination of complete responses [CR], complete unconfirmed responses [CRu], and partial responses [PR]) were 88% in R-CHOP-21 and 90% in R-CHOP-14 (P = .11).
• Rates of combined CR/CRu were 63% and 58%, respectively (P = .15).
• The 2-year failure-free survival rates were identical, at 75% in each group.
Toxicities were also generally similar between the treatment groups, except for a lower incidence of neutropenia in the R-CHOP-14 arm, which reflected primary prophylaxis with granulocyte-colony-stimulating factor (G-CSF) in that group.
There were no differences in failure-free survival between the treatment arms when patients were stratified by age, sex, disease stage, bulky disease, B symptoms, prognostic score, IPI (International Prognostic Index) score, cell proliferation (as measured by the MIB-1 monoclonal antibody), or diffuse large B-cell lymphoma (DLBCL) phenotype.
"We couldn’t actually identify any of the subsets or subgroups that benefited from one or the other treatment," Dr. Cunningham said.
Dr. Julie Vose of the University of Nebraska Medical Center in Omaha, the invited discussant, commented that the study "compared some questions that have been burning in our minds for a long time," calling it a "very robust analysis of a very important study."
Summing up this study and three other abstracts that looked at alternative therapies for DLBCL, Dr. Vose said that R-CHOP-21 is still the standard of care for young patients with low, low/intermediate, or high/intermediate IPI scores, although R-CHOP-14 plus two rituximab infusions or R-CHOEP (R-CHOP plus etoposide) are acceptable alternatives. For young patients with high IPI, R-CHOP-21 followed by consolidation autologous transplant should be offered. For older patients, R-CHOP-21 for eight cycles is equivalent to R-CHOP-14 for six cycles plus two rituximab infusions.
The trial began recruiting after a 2004 German study showed that a dose-dense regimen of six cycles of CHOP-14 improved 5-year overall survival in patients older than 60 years by 13%, compared with six cycles of CHOP-21 (Blood 2004;104:634-41).
Since that publication, however, the addition of rituximab to six or eight cycles of CHOP or similar chemotherapy regimens was shown to improve overall survival of DLBCL by 10%-16% in two trials. Those findings raised interest in whether CHOP-14 might still be superior to CHOP-21 in patients who also receive rituximab, and whether such an effect would be seen across all age groups, Dr. Cunningham said.
He reported the final results of the trial, which involved 1,080 adults who had newly diagnosed CD20-positive DLBCL and were recruited from 119 sites. The patients were stratified by IPI score, age (60 years and younger, or older than 60), and treatment center.
In all, 23% of patients on R-CHOP-21 and 22% on R-CHOP-14 had died by the time of the final study analysis. DLBCL was the leading cause of death in both arms. Other causes included treatment-related toxicity, cardiac causes (all cardiac deaths occurred 3-15 months after completion of therapy), secondary malignancy, and other/unknown causes.
In her discussion, Dr. Vose pointed out that R-CHOP-14, which requires G-CSF support after every cycle, costs about $31,308, compared with $29,247 for R-CHOP-21, in which G-CSF is used only to treat (but not to prevent) neutropenia or febrile neutropenia. In the trial, G-CSF was used in 38% of R-CHOP-21 cycles, compared with 100% of R-CHOP-14 cycles.
In addition, R-CHOP every 21 days for six cycles (not eight) is generally considered to be the standard of care in the United States, she noted; a direct comparison of this shorter regimen with R-CHOP-14 would have been welcome, she said.
The trial was funded by the U.K. National Cancer Research Institute. The authors had no relevant financial disclosures.
FROM THE ANNUAL MEETING OF THE AMERICAN SOCIETY OF CLINICAL ONCOLOGY
Major Finding: The 2-year overall survival rates were 81% in the R-CHOP-21 arm, and 83% in the R-CHOP-14 arm (log rank P = .70).
Data Source: Final analysis of a randomized controlled trial in 1,080 newly diagnosed patients with diffuse, large B-cell lymphomas.
Disclosures: The trial was funded by the U.K. National Cancer Research Institute. The authors had no relevant financial disclosures.