User login
Tool provides info for cancer patients, survivors

receiving treatment
Photo by Rhoda Baer
The American Cancer Society and National Cancer Institute have launched an online tool for cancer patients and survivors.
The tool, Springboard Beyond Cancer, was designed to help these individuals address medical, psychosocial, and wellness needs during and after treatment.
Springboard Beyond Cancer provides information to help cancer patients and survivors manage ongoing cancer-related symptoms, deal with stress, ensure healthy behavior, communicate better with healthcare teams, and seek support from friends and family.
“With Springboard Beyond Cancer, we want to empower cancer survivors by giving them the information they need to help identify issues, set goals, and create a plan to more smoothly navigate the cancer journey and take control of their health,” said Corinne Leach, PhD, a behavioral scientist and strategic director in the Behavioral Research Center at the American Cancer Society.
“We hope that Springboard Beyond Cancer, along with the close collaboration of their medical team, can help cancer survivors reduce their disease burden and improve their overall wellbeing,” added Erik Augustson, PhD, program director at the National Cancer Institute. ![]()

receiving treatment
Photo by Rhoda Baer
The American Cancer Society and National Cancer Institute have launched an online tool for cancer patients and survivors.
The tool, Springboard Beyond Cancer, was designed to help these individuals address medical, psychosocial, and wellness needs during and after treatment.
Springboard Beyond Cancer provides information to help cancer patients and survivors manage ongoing cancer-related symptoms, deal with stress, ensure healthy behavior, communicate better with healthcare teams, and seek support from friends and family.
“With Springboard Beyond Cancer, we want to empower cancer survivors by giving them the information they need to help identify issues, set goals, and create a plan to more smoothly navigate the cancer journey and take control of their health,” said Corinne Leach, PhD, a behavioral scientist and strategic director in the Behavioral Research Center at the American Cancer Society.
“We hope that Springboard Beyond Cancer, along with the close collaboration of their medical team, can help cancer survivors reduce their disease burden and improve their overall wellbeing,” added Erik Augustson, PhD, program director at the National Cancer Institute. ![]()

receiving treatment
Photo by Rhoda Baer
The American Cancer Society and National Cancer Institute have launched an online tool for cancer patients and survivors.
The tool, Springboard Beyond Cancer, was designed to help these individuals address medical, psychosocial, and wellness needs during and after treatment.
Springboard Beyond Cancer provides information to help cancer patients and survivors manage ongoing cancer-related symptoms, deal with stress, ensure healthy behavior, communicate better with healthcare teams, and seek support from friends and family.
“With Springboard Beyond Cancer, we want to empower cancer survivors by giving them the information they need to help identify issues, set goals, and create a plan to more smoothly navigate the cancer journey and take control of their health,” said Corinne Leach, PhD, a behavioral scientist and strategic director in the Behavioral Research Center at the American Cancer Society.
“We hope that Springboard Beyond Cancer, along with the close collaboration of their medical team, can help cancer survivors reduce their disease burden and improve their overall wellbeing,” added Erik Augustson, PhD, program director at the National Cancer Institute. ![]()
Blood test can predict outcomes in DLBCL, team says

Photo by Juan D. Alfonso
A blood test can reveal genetic features linked to outcomes in patients with diffuse large B-cell lymphoma (DLBCL), according to research published in Science Translational Medicine.
Investigators used targeted sequencing to analyze circulating tumor DNA (ctDNA) in blood samples from DLBCL patients.
This allowed the team to identify the cell of origin, detect minimal residual disease (MRD), and predict progression-free survival (PFS) in these patients.
Florian Scherer, MD, of Stanford University in California, and his colleagues conducted this research.
They used cancer personalized profiling by deep sequencing (CAPP-Seq) to analyze tumor biopsies and cell-free DNA samples from 92 patients with DLBCL and 24 healthy controls.
The investigators found that CAPP-Seq could effectively detect somatic mutations in DLBCL plasma samples as well as tumor biopsies. They said their results suggest ctDNA is a “robust surrogate for direct assessment of primary tumor genotypes” in most DLBCL patients.
In addition, ctDNA profiling with CAPP-Seq revealed mutations associated with resistance to the BTK inhibitor ibrutinib.
The investigators also said their results suggest ctDNA profiling can be used to classify DLBCL subtypes. The overall concordance in cell of origin predictions between tumor tissue and plasma genotyping was 88%.
Another key finding of this study is that the amount of ctDNA at DLBCL diagnosis was predictive of PFS. The investigators said higher ctDNA levels at diagnosis were “continuously and independently” correlated with inferior PFS.
Dr Scherer and his colleagues also discovered that ctDNA profiling could detect MRD with greater accuracy than immunoglobulin sequencing and radiographic imaging. And patients with ctDNA in their plasma had significantly worse PFS than patients with undetectable ctDNA.
Finally, the investigators found evidence to suggest that ctDNA profiling could provide early detection of disease transformation. They identified “distinct patterns of clonal evolution” by which they could distinguish indolent follicular lymphomas from follicular lymphomas that transformed into DLBCL. ![]()

Photo by Juan D. Alfonso
A blood test can reveal genetic features linked to outcomes in patients with diffuse large B-cell lymphoma (DLBCL), according to research published in Science Translational Medicine.
Investigators used targeted sequencing to analyze circulating tumor DNA (ctDNA) in blood samples from DLBCL patients.
This allowed the team to identify the cell of origin, detect minimal residual disease (MRD), and predict progression-free survival (PFS) in these patients.
Florian Scherer, MD, of Stanford University in California, and his colleagues conducted this research.
They used cancer personalized profiling by deep sequencing (CAPP-Seq) to analyze tumor biopsies and cell-free DNA samples from 92 patients with DLBCL and 24 healthy controls.
The investigators found that CAPP-Seq could effectively detect somatic mutations in DLBCL plasma samples as well as tumor biopsies. They said their results suggest ctDNA is a “robust surrogate for direct assessment of primary tumor genotypes” in most DLBCL patients.
In addition, ctDNA profiling with CAPP-Seq revealed mutations associated with resistance to the BTK inhibitor ibrutinib.
The investigators also said their results suggest ctDNA profiling can be used to classify DLBCL subtypes. The overall concordance in cell of origin predictions between tumor tissue and plasma genotyping was 88%.
Another key finding of this study is that the amount of ctDNA at DLBCL diagnosis was predictive of PFS. The investigators said higher ctDNA levels at diagnosis were “continuously and independently” correlated with inferior PFS.
Dr Scherer and his colleagues also discovered that ctDNA profiling could detect MRD with greater accuracy than immunoglobulin sequencing and radiographic imaging. And patients with ctDNA in their plasma had significantly worse PFS than patients with undetectable ctDNA.
Finally, the investigators found evidence to suggest that ctDNA profiling could provide early detection of disease transformation. They identified “distinct patterns of clonal evolution” by which they could distinguish indolent follicular lymphomas from follicular lymphomas that transformed into DLBCL. ![]()

Photo by Juan D. Alfonso
A blood test can reveal genetic features linked to outcomes in patients with diffuse large B-cell lymphoma (DLBCL), according to research published in Science Translational Medicine.
Investigators used targeted sequencing to analyze circulating tumor DNA (ctDNA) in blood samples from DLBCL patients.
This allowed the team to identify the cell of origin, detect minimal residual disease (MRD), and predict progression-free survival (PFS) in these patients.
Florian Scherer, MD, of Stanford University in California, and his colleagues conducted this research.
They used cancer personalized profiling by deep sequencing (CAPP-Seq) to analyze tumor biopsies and cell-free DNA samples from 92 patients with DLBCL and 24 healthy controls.
The investigators found that CAPP-Seq could effectively detect somatic mutations in DLBCL plasma samples as well as tumor biopsies. They said their results suggest ctDNA is a “robust surrogate for direct assessment of primary tumor genotypes” in most DLBCL patients.
In addition, ctDNA profiling with CAPP-Seq revealed mutations associated with resistance to the BTK inhibitor ibrutinib.
The investigators also said their results suggest ctDNA profiling can be used to classify DLBCL subtypes. The overall concordance in cell of origin predictions between tumor tissue and plasma genotyping was 88%.
Another key finding of this study is that the amount of ctDNA at DLBCL diagnosis was predictive of PFS. The investigators said higher ctDNA levels at diagnosis were “continuously and independently” correlated with inferior PFS.
Dr Scherer and his colleagues also discovered that ctDNA profiling could detect MRD with greater accuracy than immunoglobulin sequencing and radiographic imaging. And patients with ctDNA in their plasma had significantly worse PFS than patients with undetectable ctDNA.
Finally, the investigators found evidence to suggest that ctDNA profiling could provide early detection of disease transformation. They identified “distinct patterns of clonal evolution” by which they could distinguish indolent follicular lymphomas from follicular lymphomas that transformed into DLBCL. ![]()
Drug elicits responses in heavily pretreated cHL

Photo from Business Wire
COLOGNE—Results from the CheckMate -205 study suggest nivolumab can produce a high objective response rate (ORR) in patients with heavily pretreated classical Hodgkin lymphoma (cHL).
Investigators recently presented results from one of the cohorts in this phase 2 trial—cohort C—which included cHL patients who received nivolumab after undergoing autologous hematopoietic stem cell transplant (auto-HSCT) and receiving treatment with brentuximab vedotin (BV).
At a median follow-up of 8.8 months, the ORR, as assessed by an independent radiologic review committee (IRRC), was 73%.
The median progression-free survival (PFS) was 11.2 months, and the 6-month overall survival (OS) was 94%.
Investigators said the safety profile of nivolumab in this patient population was consistent with previously reported data in patients with cHL, and no new clinically meaningful safety signals were identified.
“These data from cohort C build on existing evidence supporting the benefit of Opdivo [nivolumab] in classical Hodgkin lymphoma patients who have relapsed or progressed after autologous hematopoietic stem cell transplantation and post-transplantation brentuximab vedotin,” said investigator Andreas Engert, MD, of the University Hospital of Cologne in Germany.
“Results from cohort C indicated a benefit with Opdivo regardless of the order of prior treatment with autologous hematopoietic stem cell transplantation and brentuximab vedotin, providing important insights as we continue researching the potential role Opdivo could provide for heavily pretreated classical Hodgkin lymphoma patients.”
The results were presented at the 10th International Symposium on Hodgkin Lymphoma (abstract T022). Abstracts from this meeting have been published in haematologica.
The CheckMate -205 trial is sponsored by Bristol-Myers Squibb.
About the trial
CheckMate -205 is a multi-cohort study in which investigators are evaluating the safety and efficacy of nivolumab in adults with cHL.
Cohort A included cHL patients who had received auto-HSCT and were BV-naïve (n=63). Cohort B included cHL patients who had received auto-HSCT followed by BV (n=80).
Cohort C included cHL patients who had received BV before and/or after auto-HSCT (n=100).
The study also includes a cohort D, which is currently enrolling and evaluating nivolumab in combination with chemotherapy in newly diagnosed, advanced-stage cHL patients who are treatment-naïve (n=50).
Patients enrolled in this trial have received nivolumab at 3 mg/kg intravenously every 2 weeks until disease progression or unacceptable toxicity. In cohort C, patients were also treated until investigator-assessed complete response (CR) lasting 1 year.
The study’s primary endpoint was ORR by IRRC assessment. Secondary and other exploratory endpoints included duration of response by IRRC assessment for CR rate and partial response rate, PFS by IRRC assessment, OS, and safety.
Response
The investigators presented results from cohort C (n=100), which included patients with cHL who had received BV before and/or after auto-HSCT.
At a median follow-up of 8.8 months, ORR per the IRRC was 73% (n=73) overall. The investigators said ORR was consistent across patient subgroups, regardless of the timing of prior BV relative to auto-HSCT.
The ORR was 70% (n=23) in patients who received BV only before auto-HSCT, 72% (n=41) in patients who received BV only after auto-HSCT, and 88% (n=7) in patients who received BV before and after auto-HSCT.
The CR rate was 17% (n=17) overall, 18.2% (n=6) in patients who received BV only before auto-HSCT, 12.3% (n=7) in patients who received BV only after auto-HSCT, and 38% (n=3) in patients who received BV before and after auto-HSCT.
Survival
The median PFS was 11.2 months (range, 8.5 months to not achieved) overall, 11.2 months (range, 8.5 months to not achieved) in patients who received BV only before auto-HSCT, 8.9 months (range, 8.3 months to not achieved) in patients who received BV only after auto-HSCT, and not achieved (range, 5.6 months to not achieved) in patients who received BV before and after auto-HSCT.
The 6-month OS was 93.9% overall, 97% in patients who received BV only before auto-HSCT, 91% in patients who received BV only after auto-HSCT, and 100% in patients who received BV before and after auto-HSCT.
Safety
Treatment-related adverse events (AEs) occurred in 68% of patients between the first dose and 30 days after the last dose of nivolumab. The most common treatment-related AEs were diarrhea, infusion-related reaction, and fatigue (11% each).
Grade 3/4 AEs occurred in 19% of patients. Serious treatment-related AEs were reported in 17% of patients, and treatment-related AEs leading to discontinuation occurred in 6% of patients.
At present, no treatment-related deaths have been reported. ![]()

Photo from Business Wire
COLOGNE—Results from the CheckMate -205 study suggest nivolumab can produce a high objective response rate (ORR) in patients with heavily pretreated classical Hodgkin lymphoma (cHL).
Investigators recently presented results from one of the cohorts in this phase 2 trial—cohort C—which included cHL patients who received nivolumab after undergoing autologous hematopoietic stem cell transplant (auto-HSCT) and receiving treatment with brentuximab vedotin (BV).
At a median follow-up of 8.8 months, the ORR, as assessed by an independent radiologic review committee (IRRC), was 73%.
The median progression-free survival (PFS) was 11.2 months, and the 6-month overall survival (OS) was 94%.
Investigators said the safety profile of nivolumab in this patient population was consistent with previously reported data in patients with cHL, and no new clinically meaningful safety signals were identified.
“These data from cohort C build on existing evidence supporting the benefit of Opdivo [nivolumab] in classical Hodgkin lymphoma patients who have relapsed or progressed after autologous hematopoietic stem cell transplantation and post-transplantation brentuximab vedotin,” said investigator Andreas Engert, MD, of the University Hospital of Cologne in Germany.
“Results from cohort C indicated a benefit with Opdivo regardless of the order of prior treatment with autologous hematopoietic stem cell transplantation and brentuximab vedotin, providing important insights as we continue researching the potential role Opdivo could provide for heavily pretreated classical Hodgkin lymphoma patients.”
The results were presented at the 10th International Symposium on Hodgkin Lymphoma (abstract T022). Abstracts from this meeting have been published in haematologica.
The CheckMate -205 trial is sponsored by Bristol-Myers Squibb.
About the trial
CheckMate -205 is a multi-cohort study in which investigators are evaluating the safety and efficacy of nivolumab in adults with cHL.
Cohort A included cHL patients who had received auto-HSCT and were BV-naïve (n=63). Cohort B included cHL patients who had received auto-HSCT followed by BV (n=80).
Cohort C included cHL patients who had received BV before and/or after auto-HSCT (n=100).
The study also includes a cohort D, which is currently enrolling and evaluating nivolumab in combination with chemotherapy in newly diagnosed, advanced-stage cHL patients who are treatment-naïve (n=50).
Patients enrolled in this trial have received nivolumab at 3 mg/kg intravenously every 2 weeks until disease progression or unacceptable toxicity. In cohort C, patients were also treated until investigator-assessed complete response (CR) lasting 1 year.
The study’s primary endpoint was ORR by IRRC assessment. Secondary and other exploratory endpoints included duration of response by IRRC assessment for CR rate and partial response rate, PFS by IRRC assessment, OS, and safety.
Response
The investigators presented results from cohort C (n=100), which included patients with cHL who had received BV before and/or after auto-HSCT.
At a median follow-up of 8.8 months, ORR per the IRRC was 73% (n=73) overall. The investigators said ORR was consistent across patient subgroups, regardless of the timing of prior BV relative to auto-HSCT.
The ORR was 70% (n=23) in patients who received BV only before auto-HSCT, 72% (n=41) in patients who received BV only after auto-HSCT, and 88% (n=7) in patients who received BV before and after auto-HSCT.
The CR rate was 17% (n=17) overall, 18.2% (n=6) in patients who received BV only before auto-HSCT, 12.3% (n=7) in patients who received BV only after auto-HSCT, and 38% (n=3) in patients who received BV before and after auto-HSCT.
Survival
The median PFS was 11.2 months (range, 8.5 months to not achieved) overall, 11.2 months (range, 8.5 months to not achieved) in patients who received BV only before auto-HSCT, 8.9 months (range, 8.3 months to not achieved) in patients who received BV only after auto-HSCT, and not achieved (range, 5.6 months to not achieved) in patients who received BV before and after auto-HSCT.
The 6-month OS was 93.9% overall, 97% in patients who received BV only before auto-HSCT, 91% in patients who received BV only after auto-HSCT, and 100% in patients who received BV before and after auto-HSCT.
Safety
Treatment-related adverse events (AEs) occurred in 68% of patients between the first dose and 30 days after the last dose of nivolumab. The most common treatment-related AEs were diarrhea, infusion-related reaction, and fatigue (11% each).
Grade 3/4 AEs occurred in 19% of patients. Serious treatment-related AEs were reported in 17% of patients, and treatment-related AEs leading to discontinuation occurred in 6% of patients.
At present, no treatment-related deaths have been reported. ![]()

Photo from Business Wire
COLOGNE—Results from the CheckMate -205 study suggest nivolumab can produce a high objective response rate (ORR) in patients with heavily pretreated classical Hodgkin lymphoma (cHL).
Investigators recently presented results from one of the cohorts in this phase 2 trial—cohort C—which included cHL patients who received nivolumab after undergoing autologous hematopoietic stem cell transplant (auto-HSCT) and receiving treatment with brentuximab vedotin (BV).
At a median follow-up of 8.8 months, the ORR, as assessed by an independent radiologic review committee (IRRC), was 73%.
The median progression-free survival (PFS) was 11.2 months, and the 6-month overall survival (OS) was 94%.
Investigators said the safety profile of nivolumab in this patient population was consistent with previously reported data in patients with cHL, and no new clinically meaningful safety signals were identified.
“These data from cohort C build on existing evidence supporting the benefit of Opdivo [nivolumab] in classical Hodgkin lymphoma patients who have relapsed or progressed after autologous hematopoietic stem cell transplantation and post-transplantation brentuximab vedotin,” said investigator Andreas Engert, MD, of the University Hospital of Cologne in Germany.
“Results from cohort C indicated a benefit with Opdivo regardless of the order of prior treatment with autologous hematopoietic stem cell transplantation and brentuximab vedotin, providing important insights as we continue researching the potential role Opdivo could provide for heavily pretreated classical Hodgkin lymphoma patients.”
The results were presented at the 10th International Symposium on Hodgkin Lymphoma (abstract T022). Abstracts from this meeting have been published in haematologica.
The CheckMate -205 trial is sponsored by Bristol-Myers Squibb.
About the trial
CheckMate -205 is a multi-cohort study in which investigators are evaluating the safety and efficacy of nivolumab in adults with cHL.
Cohort A included cHL patients who had received auto-HSCT and were BV-naïve (n=63). Cohort B included cHL patients who had received auto-HSCT followed by BV (n=80).
Cohort C included cHL patients who had received BV before and/or after auto-HSCT (n=100).
The study also includes a cohort D, which is currently enrolling and evaluating nivolumab in combination with chemotherapy in newly diagnosed, advanced-stage cHL patients who are treatment-naïve (n=50).
Patients enrolled in this trial have received nivolumab at 3 mg/kg intravenously every 2 weeks until disease progression or unacceptable toxicity. In cohort C, patients were also treated until investigator-assessed complete response (CR) lasting 1 year.
The study’s primary endpoint was ORR by IRRC assessment. Secondary and other exploratory endpoints included duration of response by IRRC assessment for CR rate and partial response rate, PFS by IRRC assessment, OS, and safety.
Response
The investigators presented results from cohort C (n=100), which included patients with cHL who had received BV before and/or after auto-HSCT.
At a median follow-up of 8.8 months, ORR per the IRRC was 73% (n=73) overall. The investigators said ORR was consistent across patient subgroups, regardless of the timing of prior BV relative to auto-HSCT.
The ORR was 70% (n=23) in patients who received BV only before auto-HSCT, 72% (n=41) in patients who received BV only after auto-HSCT, and 88% (n=7) in patients who received BV before and after auto-HSCT.
The CR rate was 17% (n=17) overall, 18.2% (n=6) in patients who received BV only before auto-HSCT, 12.3% (n=7) in patients who received BV only after auto-HSCT, and 38% (n=3) in patients who received BV before and after auto-HSCT.
Survival
The median PFS was 11.2 months (range, 8.5 months to not achieved) overall, 11.2 months (range, 8.5 months to not achieved) in patients who received BV only before auto-HSCT, 8.9 months (range, 8.3 months to not achieved) in patients who received BV only after auto-HSCT, and not achieved (range, 5.6 months to not achieved) in patients who received BV before and after auto-HSCT.
The 6-month OS was 93.9% overall, 97% in patients who received BV only before auto-HSCT, 91% in patients who received BV only after auto-HSCT, and 100% in patients who received BV before and after auto-HSCT.
Safety
Treatment-related adverse events (AEs) occurred in 68% of patients between the first dose and 30 days after the last dose of nivolumab. The most common treatment-related AEs were diarrhea, infusion-related reaction, and fatigue (11% each).
Grade 3/4 AEs occurred in 19% of patients. Serious treatment-related AEs were reported in 17% of patients, and treatment-related AEs leading to discontinuation occurred in 6% of patients.
At present, no treatment-related deaths have been reported. ![]()
Combine flow and HTS for sensitive MRD detection in CLL, speaker says

laser beam
Photo courtesy of NIH
NEW YORK—Combining 2 technologies—flow cytometry and high-throughput sequencing (HTS)—produces a very sensitive approach to detecting minimal residual disease (MRD) in chronic lymphocytic leukemia (CLL), according to a speaker at Lymphoma & Myeloma 2016.
The approach is both reproducible and widely accessible, added the speaker, Peter Hillmen, MB ChB, PhD, of St James’s University Hospital in Leeds, UK.
“PCR [polymerase chain reaction] is more sensitive than flow cytometry,” he noted, “but it is probably not necessary to assess response by that criteria.”
Features to consider when choosing a technology for detecting MRD include sensitivity, specificity for the patient and/or the disease, applicability to all patients or to an individual, the platform—flow cytometry, conventional molecular PCR, or next-generation sequencing—and which tissue to use, blood or bone marrow.
In the era of immunotherapy, Dr Hillmen said, assessment should be performed at least 2 months after completion of immunotherapy to get a reliable assessment of MRD, particularly after treatment with alemtuzumab, rituximab, and other antibodies targeting CLL.
History of MRD analysis
The definition of MRD hasn’t changed since 2008, when the International Workshop on CLL updated National Cancer Institute guidelines. It is still 1 single cell in 10,000 (10-4) leukocytes, regardless of the tissue used.
Prior to the mid-1990s, there were limited options for assessing MRD, Dr Hillmen said.
Based on the profound remissions patients experienced with alemtuzumab, investigators began to develop assays to assess MRD.
“[W]e started standardizing these assays around 2007,” Dr Hillmen said, and a standardized assay was used prospectively in clinical trials beginning in 2012.
Technologies
Several technologies can be used to assess MRD.
Flow cytometry using 6 colors or 8 colors—to simplify the assay and to make it more sensitive—is a multiparameter assessment of CLL phenotype that is not clonality-based.
Allele-specific oligonucleotide PCR (ASO-PCR) is laborious to perform, Dr Hillmen said, but it’s very sensitive.
“[I]t probably shouldn’t be considered as an MRD test,” he said, since it uses patient-specific primers, not consensus primers.
HTS provides an increasing amount of information on B-cell sequences and enumeration of the CLL-specific immunoglobulin gene, “and I would move it towards being approved as a regulatory endpoint,” Dr Hillmen asserted.
Flow cytometry and HTS
A consensus document by the European Research Initiative on CLL (ERIC) identified and validated a flow cytometric approach to MRD assessment in parallel with HTS.
According to the ERIC investigators, flow cytometry had to utilize a core panel of 6 antigens used by most labs—CD19, CD20, CD5, CD43, CD79b, and CD81. And the markers used had to quantitate cells to a level of 0.01% (10-4).
Assays had to be independent and compatible with older, established therapies as well as newer treatments.
For example, 6-color flow had to be effective with fludarabine, cyclophosphamide, and rituximab (FCR) regimens, as well as effective with the novel agents ibrutinib and venetoclax (ABT-199).
Compared to PCR, multiparameter flow cytometry is more convenient, Dr Hillmen noted.
And while PCR is more sensitive than flow cytometry (sensitive to 10-5 to 10-6), it is more difficult to apply to large clinical trials because the assay must be validated for each patient.
The investigators validated the flow cytometric approach in 450 patients on FCR-type therapy enrolled in the ADMIRE and ARCTIC trials.
They assessed MRD in patients’ bone marrow 3 months after the last course of treatment and presented the data at EHA 2015 (Rawstron AC, abstract S794).
They found that all patients who were MRD negative, including 9 patients with partial responses, achieved a significantly better progression-free survival (PFS) than patients who had achieved a complete response but were still MRD positive.
The parallel analysis of HTS showed good concordance with flow cytometry at the 0.01% (10-4) level.
Peripheral blood or bone marrow?
“[T]he blood is a tissue which can be used, but it’s certainly not as sensitive as the bone marrow,” Dr Hillmen said. “And depending upon what we are using MRD for, the marrow is probably a better tissue, with some exceptions.”
Data from the ADMIRE and ARCTIC trials confirmed that 177 patients on FCR-based therapy who were negative in the bone marrow were always negative in the blood. However, a quarter of patients negative in the blood were positive in the bone marrow.
Investigators followed the same patients on FCR-based therapy for 3 years and found no difference in outcome in terms of PFS for patients negative in peripheral blood and positive in the bone marrow (PB-/BM+) and those negative in peripheral blood and negative in the bone marrow (PB-/BM-) (Rawstron abstract S794).
But for patients on alemtuzumab, with the same analysis, those who were PB-/BM+ did less well and had similar PFS to those who were PB+/BM+.
And at a follow-up of 4 years or longer, patients on FCR-based therapy who were PB-/BM- had superior outcomes than those who were PB-/BM+.
“So as a predictive marker, the bone marrow is a better tissue to look at, but peripheral blood negativity also can predict with FCR but not with agents such as alemtuzumab,” Dr Hillmen summarized.
Prognostic value of MRD assessment
Multivariate analysis of a 10-year follow-up of 133 CLL patients revealed that MRD level and adverse cytogenetics were the only significant parameters in terms of PFS.
And in terms of overall survival (OS), MRD level, prior treatment, Binet stage, and age were significant.
Sixty-seven of these patients had been treated with chemoimmunotherapy, 31 with single-agent chemotherapy, 7 had autologous stem cell transplants, and 28 had prior exposure to alemtuzumab.
In terms of survival beyond 10 or 15 years, previously untreated patients who were MRD negative after their first therapy had significantly better PFS and OS than previously treated patients who were MRD negative and patients with or without prior treatment who were MRD positive (P<0.001).
“Consistently, MRD, regardless of therapy, is the most important prognostic marker,” Dr Hillmen said.
Data from MD Anderson Cancer Center showed that 75% of patients treated first-line with FCR who achieved a complete response were MRD negative.
And patients who achieved MRD negativity had significantly better PFS (P<0.001) and OS (P=0.006) than patients who remained MRD positive.
In the ADMIRE and ARCTIC trials mentioned earlier, patients who achieved MRD negativity in the marrow at 3 months post-therapy also had significantly better PFS (P<0.0001) and OS (P=0.0002) than those who were MRD positive.
For every log of positivity, Dr Hillmen said, patients have a worse survival. Conversely, for every log reduction in MRD level, there is a 33% reduction in risk for disease progression.
“MRD is probably the most important prognostic marker we have,” he said. “We need to look at MRD levels with novel agents and use it to define duration of therapy, maybe use it to define additional therapy if patients are stalled in their response.” ![]()

laser beam
Photo courtesy of NIH
NEW YORK—Combining 2 technologies—flow cytometry and high-throughput sequencing (HTS)—produces a very sensitive approach to detecting minimal residual disease (MRD) in chronic lymphocytic leukemia (CLL), according to a speaker at Lymphoma & Myeloma 2016.
The approach is both reproducible and widely accessible, added the speaker, Peter Hillmen, MB ChB, PhD, of St James’s University Hospital in Leeds, UK.
“PCR [polymerase chain reaction] is more sensitive than flow cytometry,” he noted, “but it is probably not necessary to assess response by that criteria.”
Features to consider when choosing a technology for detecting MRD include sensitivity, specificity for the patient and/or the disease, applicability to all patients or to an individual, the platform—flow cytometry, conventional molecular PCR, or next-generation sequencing—and which tissue to use, blood or bone marrow.
In the era of immunotherapy, Dr Hillmen said, assessment should be performed at least 2 months after completion of immunotherapy to get a reliable assessment of MRD, particularly after treatment with alemtuzumab, rituximab, and other antibodies targeting CLL.
History of MRD analysis
The definition of MRD hasn’t changed since 2008, when the International Workshop on CLL updated National Cancer Institute guidelines. It is still 1 single cell in 10,000 (10-4) leukocytes, regardless of the tissue used.
Prior to the mid-1990s, there were limited options for assessing MRD, Dr Hillmen said.
Based on the profound remissions patients experienced with alemtuzumab, investigators began to develop assays to assess MRD.
“[W]e started standardizing these assays around 2007,” Dr Hillmen said, and a standardized assay was used prospectively in clinical trials beginning in 2012.
Technologies
Several technologies can be used to assess MRD.
Flow cytometry using 6 colors or 8 colors—to simplify the assay and to make it more sensitive—is a multiparameter assessment of CLL phenotype that is not clonality-based.
Allele-specific oligonucleotide PCR (ASO-PCR) is laborious to perform, Dr Hillmen said, but it’s very sensitive.
“[I]t probably shouldn’t be considered as an MRD test,” he said, since it uses patient-specific primers, not consensus primers.
HTS provides an increasing amount of information on B-cell sequences and enumeration of the CLL-specific immunoglobulin gene, “and I would move it towards being approved as a regulatory endpoint,” Dr Hillmen asserted.
Flow cytometry and HTS
A consensus document by the European Research Initiative on CLL (ERIC) identified and validated a flow cytometric approach to MRD assessment in parallel with HTS.
According to the ERIC investigators, flow cytometry had to utilize a core panel of 6 antigens used by most labs—CD19, CD20, CD5, CD43, CD79b, and CD81. And the markers used had to quantitate cells to a level of 0.01% (10-4).
Assays had to be independent and compatible with older, established therapies as well as newer treatments.
For example, 6-color flow had to be effective with fludarabine, cyclophosphamide, and rituximab (FCR) regimens, as well as effective with the novel agents ibrutinib and venetoclax (ABT-199).
Compared to PCR, multiparameter flow cytometry is more convenient, Dr Hillmen noted.
And while PCR is more sensitive than flow cytometry (sensitive to 10-5 to 10-6), it is more difficult to apply to large clinical trials because the assay must be validated for each patient.
The investigators validated the flow cytometric approach in 450 patients on FCR-type therapy enrolled in the ADMIRE and ARCTIC trials.
They assessed MRD in patients’ bone marrow 3 months after the last course of treatment and presented the data at EHA 2015 (Rawstron AC, abstract S794).
They found that all patients who were MRD negative, including 9 patients with partial responses, achieved a significantly better progression-free survival (PFS) than patients who had achieved a complete response but were still MRD positive.
The parallel analysis of HTS showed good concordance with flow cytometry at the 0.01% (10-4) level.
Peripheral blood or bone marrow?
“[T]he blood is a tissue which can be used, but it’s certainly not as sensitive as the bone marrow,” Dr Hillmen said. “And depending upon what we are using MRD for, the marrow is probably a better tissue, with some exceptions.”
Data from the ADMIRE and ARCTIC trials confirmed that 177 patients on FCR-based therapy who were negative in the bone marrow were always negative in the blood. However, a quarter of patients negative in the blood were positive in the bone marrow.
Investigators followed the same patients on FCR-based therapy for 3 years and found no difference in outcome in terms of PFS for patients negative in peripheral blood and positive in the bone marrow (PB-/BM+) and those negative in peripheral blood and negative in the bone marrow (PB-/BM-) (Rawstron abstract S794).
But for patients on alemtuzumab, with the same analysis, those who were PB-/BM+ did less well and had similar PFS to those who were PB+/BM+.
And at a follow-up of 4 years or longer, patients on FCR-based therapy who were PB-/BM- had superior outcomes than those who were PB-/BM+.
“So as a predictive marker, the bone marrow is a better tissue to look at, but peripheral blood negativity also can predict with FCR but not with agents such as alemtuzumab,” Dr Hillmen summarized.
Prognostic value of MRD assessment
Multivariate analysis of a 10-year follow-up of 133 CLL patients revealed that MRD level and adverse cytogenetics were the only significant parameters in terms of PFS.
And in terms of overall survival (OS), MRD level, prior treatment, Binet stage, and age were significant.
Sixty-seven of these patients had been treated with chemoimmunotherapy, 31 with single-agent chemotherapy, 7 had autologous stem cell transplants, and 28 had prior exposure to alemtuzumab.
In terms of survival beyond 10 or 15 years, previously untreated patients who were MRD negative after their first therapy had significantly better PFS and OS than previously treated patients who were MRD negative and patients with or without prior treatment who were MRD positive (P<0.001).
“Consistently, MRD, regardless of therapy, is the most important prognostic marker,” Dr Hillmen said.
Data from MD Anderson Cancer Center showed that 75% of patients treated first-line with FCR who achieved a complete response were MRD negative.
And patients who achieved MRD negativity had significantly better PFS (P<0.001) and OS (P=0.006) than patients who remained MRD positive.
In the ADMIRE and ARCTIC trials mentioned earlier, patients who achieved MRD negativity in the marrow at 3 months post-therapy also had significantly better PFS (P<0.0001) and OS (P=0.0002) than those who were MRD positive.
For every log of positivity, Dr Hillmen said, patients have a worse survival. Conversely, for every log reduction in MRD level, there is a 33% reduction in risk for disease progression.
“MRD is probably the most important prognostic marker we have,” he said. “We need to look at MRD levels with novel agents and use it to define duration of therapy, maybe use it to define additional therapy if patients are stalled in their response.” ![]()

laser beam
Photo courtesy of NIH
NEW YORK—Combining 2 technologies—flow cytometry and high-throughput sequencing (HTS)—produces a very sensitive approach to detecting minimal residual disease (MRD) in chronic lymphocytic leukemia (CLL), according to a speaker at Lymphoma & Myeloma 2016.
The approach is both reproducible and widely accessible, added the speaker, Peter Hillmen, MB ChB, PhD, of St James’s University Hospital in Leeds, UK.
“PCR [polymerase chain reaction] is more sensitive than flow cytometry,” he noted, “but it is probably not necessary to assess response by that criteria.”
Features to consider when choosing a technology for detecting MRD include sensitivity, specificity for the patient and/or the disease, applicability to all patients or to an individual, the platform—flow cytometry, conventional molecular PCR, or next-generation sequencing—and which tissue to use, blood or bone marrow.
In the era of immunotherapy, Dr Hillmen said, assessment should be performed at least 2 months after completion of immunotherapy to get a reliable assessment of MRD, particularly after treatment with alemtuzumab, rituximab, and other antibodies targeting CLL.
History of MRD analysis
The definition of MRD hasn’t changed since 2008, when the International Workshop on CLL updated National Cancer Institute guidelines. It is still 1 single cell in 10,000 (10-4) leukocytes, regardless of the tissue used.
Prior to the mid-1990s, there were limited options for assessing MRD, Dr Hillmen said.
Based on the profound remissions patients experienced with alemtuzumab, investigators began to develop assays to assess MRD.
“[W]e started standardizing these assays around 2007,” Dr Hillmen said, and a standardized assay was used prospectively in clinical trials beginning in 2012.
Technologies
Several technologies can be used to assess MRD.
Flow cytometry using 6 colors or 8 colors—to simplify the assay and to make it more sensitive—is a multiparameter assessment of CLL phenotype that is not clonality-based.
Allele-specific oligonucleotide PCR (ASO-PCR) is laborious to perform, Dr Hillmen said, but it’s very sensitive.
“[I]t probably shouldn’t be considered as an MRD test,” he said, since it uses patient-specific primers, not consensus primers.
HTS provides an increasing amount of information on B-cell sequences and enumeration of the CLL-specific immunoglobulin gene, “and I would move it towards being approved as a regulatory endpoint,” Dr Hillmen asserted.
Flow cytometry and HTS
A consensus document by the European Research Initiative on CLL (ERIC) identified and validated a flow cytometric approach to MRD assessment in parallel with HTS.
According to the ERIC investigators, flow cytometry had to utilize a core panel of 6 antigens used by most labs—CD19, CD20, CD5, CD43, CD79b, and CD81. And the markers used had to quantitate cells to a level of 0.01% (10-4).
Assays had to be independent and compatible with older, established therapies as well as newer treatments.
For example, 6-color flow had to be effective with fludarabine, cyclophosphamide, and rituximab (FCR) regimens, as well as effective with the novel agents ibrutinib and venetoclax (ABT-199).
Compared to PCR, multiparameter flow cytometry is more convenient, Dr Hillmen noted.
And while PCR is more sensitive than flow cytometry (sensitive to 10-5 to 10-6), it is more difficult to apply to large clinical trials because the assay must be validated for each patient.
The investigators validated the flow cytometric approach in 450 patients on FCR-type therapy enrolled in the ADMIRE and ARCTIC trials.
They assessed MRD in patients’ bone marrow 3 months after the last course of treatment and presented the data at EHA 2015 (Rawstron AC, abstract S794).
They found that all patients who were MRD negative, including 9 patients with partial responses, achieved a significantly better progression-free survival (PFS) than patients who had achieved a complete response but were still MRD positive.
The parallel analysis of HTS showed good concordance with flow cytometry at the 0.01% (10-4) level.
Peripheral blood or bone marrow?
“[T]he blood is a tissue which can be used, but it’s certainly not as sensitive as the bone marrow,” Dr Hillmen said. “And depending upon what we are using MRD for, the marrow is probably a better tissue, with some exceptions.”
Data from the ADMIRE and ARCTIC trials confirmed that 177 patients on FCR-based therapy who were negative in the bone marrow were always negative in the blood. However, a quarter of patients negative in the blood were positive in the bone marrow.
Investigators followed the same patients on FCR-based therapy for 3 years and found no difference in outcome in terms of PFS for patients negative in peripheral blood and positive in the bone marrow (PB-/BM+) and those negative in peripheral blood and negative in the bone marrow (PB-/BM-) (Rawstron abstract S794).
But for patients on alemtuzumab, with the same analysis, those who were PB-/BM+ did less well and had similar PFS to those who were PB+/BM+.
And at a follow-up of 4 years or longer, patients on FCR-based therapy who were PB-/BM- had superior outcomes than those who were PB-/BM+.
“So as a predictive marker, the bone marrow is a better tissue to look at, but peripheral blood negativity also can predict with FCR but not with agents such as alemtuzumab,” Dr Hillmen summarized.
Prognostic value of MRD assessment
Multivariate analysis of a 10-year follow-up of 133 CLL patients revealed that MRD level and adverse cytogenetics were the only significant parameters in terms of PFS.
And in terms of overall survival (OS), MRD level, prior treatment, Binet stage, and age were significant.
Sixty-seven of these patients had been treated with chemoimmunotherapy, 31 with single-agent chemotherapy, 7 had autologous stem cell transplants, and 28 had prior exposure to alemtuzumab.
In terms of survival beyond 10 or 15 years, previously untreated patients who were MRD negative after their first therapy had significantly better PFS and OS than previously treated patients who were MRD negative and patients with or without prior treatment who were MRD positive (P<0.001).
“Consistently, MRD, regardless of therapy, is the most important prognostic marker,” Dr Hillmen said.
Data from MD Anderson Cancer Center showed that 75% of patients treated first-line with FCR who achieved a complete response were MRD negative.
And patients who achieved MRD negativity had significantly better PFS (P<0.001) and OS (P=0.006) than patients who remained MRD positive.
In the ADMIRE and ARCTIC trials mentioned earlier, patients who achieved MRD negativity in the marrow at 3 months post-therapy also had significantly better PFS (P<0.0001) and OS (P=0.0002) than those who were MRD positive.
For every log of positivity, Dr Hillmen said, patients have a worse survival. Conversely, for every log reduction in MRD level, there is a 33% reduction in risk for disease progression.
“MRD is probably the most important prognostic marker we have,” he said. “We need to look at MRD levels with novel agents and use it to define duration of therapy, maybe use it to define additional therapy if patients are stalled in their response.” ![]()
NORD publishes physician guide to CTCL

mycosis fungoides
The National Organization for Rare Disorders (NORD) has published a guide for physicians treating patients with cutaneous T-cell lymphoma (CTCL).
The guide contains information about disease classification, signs and symptoms of CTCL, methods of diagnosing the disease, standard therapies, and investigational therapies for CTCL.
The guide also includes a list of resources for physicians and patients.
“The NORD Physician Guide to Cutaneous T-Cell Lymphoma (CTCL)” is available for free on the NORD Physician Guides website.
The guide was made possible by an educational grant from Therakos, now a part of Mallinckrodt Pharmaceuticals.
The guide was developed in collaboration with Oleg E. Akilov, MD, PhD, of the University of Pittsburgh School of Medicine in Pennsylvania.
“Eczema and even some cases of psoriasis may look very similar to mycosis fungoides, the most common type of cutaneous T-cell lymphomas,” Dr Akilov noted.
“It is important to be aware of these similarities and to be ready to think about cutaneous lymphoma when a patient with ‘common dermatosis’ does not respond to regular treatments.”
About NORD guides
NORD established its physician guide series as part of a broader strategic initiative to promote earlier diagnosis and state-of-the-art care for people with rare diseases. Each online guide is written or reviewed by a medical professional with expertise on the topic.
Other recent guides in the series include:
- The NORD Physician Guide to Mitochondrial Myopathies
- The NORD Physician Guide to Paroxysmal Nocturnal Hemoglobinuria (PNH)
- The NORD Physician Guide to Atypical Hemolytic Uremic Syndrome (aHUS)
- The NORD Physician Guide to Nontuberculous Mycobacterial Lung Disease.
“People who have rare diseases often go for many years without a diagnosis,” said Marsha Lanes, a genetic counselor in NORD’s Educational Initiatives Department.
“The purpose of NORD’s free online physician guides is to reduce the time to diagnosis and encourage optimal treatment for patients with little-known and little-understood rare diseases.” ![]()

mycosis fungoides
The National Organization for Rare Disorders (NORD) has published a guide for physicians treating patients with cutaneous T-cell lymphoma (CTCL).
The guide contains information about disease classification, signs and symptoms of CTCL, methods of diagnosing the disease, standard therapies, and investigational therapies for CTCL.
The guide also includes a list of resources for physicians and patients.
“The NORD Physician Guide to Cutaneous T-Cell Lymphoma (CTCL)” is available for free on the NORD Physician Guides website.
The guide was made possible by an educational grant from Therakos, now a part of Mallinckrodt Pharmaceuticals.
The guide was developed in collaboration with Oleg E. Akilov, MD, PhD, of the University of Pittsburgh School of Medicine in Pennsylvania.
“Eczema and even some cases of psoriasis may look very similar to mycosis fungoides, the most common type of cutaneous T-cell lymphomas,” Dr Akilov noted.
“It is important to be aware of these similarities and to be ready to think about cutaneous lymphoma when a patient with ‘common dermatosis’ does not respond to regular treatments.”
About NORD guides
NORD established its physician guide series as part of a broader strategic initiative to promote earlier diagnosis and state-of-the-art care for people with rare diseases. Each online guide is written or reviewed by a medical professional with expertise on the topic.
Other recent guides in the series include:
- The NORD Physician Guide to Mitochondrial Myopathies
- The NORD Physician Guide to Paroxysmal Nocturnal Hemoglobinuria (PNH)
- The NORD Physician Guide to Atypical Hemolytic Uremic Syndrome (aHUS)
- The NORD Physician Guide to Nontuberculous Mycobacterial Lung Disease.
“People who have rare diseases often go for many years without a diagnosis,” said Marsha Lanes, a genetic counselor in NORD’s Educational Initiatives Department.
“The purpose of NORD’s free online physician guides is to reduce the time to diagnosis and encourage optimal treatment for patients with little-known and little-understood rare diseases.” ![]()

mycosis fungoides
The National Organization for Rare Disorders (NORD) has published a guide for physicians treating patients with cutaneous T-cell lymphoma (CTCL).
The guide contains information about disease classification, signs and symptoms of CTCL, methods of diagnosing the disease, standard therapies, and investigational therapies for CTCL.
The guide also includes a list of resources for physicians and patients.
“The NORD Physician Guide to Cutaneous T-Cell Lymphoma (CTCL)” is available for free on the NORD Physician Guides website.
The guide was made possible by an educational grant from Therakos, now a part of Mallinckrodt Pharmaceuticals.
The guide was developed in collaboration with Oleg E. Akilov, MD, PhD, of the University of Pittsburgh School of Medicine in Pennsylvania.
“Eczema and even some cases of psoriasis may look very similar to mycosis fungoides, the most common type of cutaneous T-cell lymphomas,” Dr Akilov noted.
“It is important to be aware of these similarities and to be ready to think about cutaneous lymphoma when a patient with ‘common dermatosis’ does not respond to regular treatments.”
About NORD guides
NORD established its physician guide series as part of a broader strategic initiative to promote earlier diagnosis and state-of-the-art care for people with rare diseases. Each online guide is written or reviewed by a medical professional with expertise on the topic.
Other recent guides in the series include:
- The NORD Physician Guide to Mitochondrial Myopathies
- The NORD Physician Guide to Paroxysmal Nocturnal Hemoglobinuria (PNH)
- The NORD Physician Guide to Atypical Hemolytic Uremic Syndrome (aHUS)
- The NORD Physician Guide to Nontuberculous Mycobacterial Lung Disease.
“People who have rare diseases often go for many years without a diagnosis,” said Marsha Lanes, a genetic counselor in NORD’s Educational Initiatives Department.
“The purpose of NORD’s free online physician guides is to reduce the time to diagnosis and encourage optimal treatment for patients with little-known and little-understood rare diseases.” ![]()
Genetic screening for CLL premature, speaker says

Photo courtesy of the
National Institute
of General Medical Science
NEW YORK—Research has shown that family history is a strong risk factor for developing chronic lymphocytic leukemia (CLL).
First-degree relatives have an 8.5-fold risk of getting CLL and an increased risk of other lymphoproliferative disorders, according to a study published in 2009.
However, despite the strong evidence of a genetic contribution, one expert believes it’s premature to bring genetic testing into the clinic for screening in CLL.
“At this time, we do not recommend genetic screening,” said Susan Slager, PhD, of the Mayo Clinic in Rochester, Minnesota.
“There’s no known relationship between the inherited variants and treatment response,” she explained, and the relatively low incidence of CLL argues against active screening in affected families at present.
Dr Slager discussed genetic and non-genetic factors associated with CLL and the clinical implications of these factors at Lymphoma & Myeloma 2016.
Demographic risk factors
Dr Slager noted that age, gender, and race are risk factors for CLL.
Individuals aged 65 to 74 have the highest incidence of CLL, at 28%, while the risk is almost non-existent for those under age 20, she said.
There is a higher incidence of CLL in males than in females, and the reason for this gender disparity is unknown.
There is a higher incidence of CLL in Caucasians than Asians, for both males and females.
“Again, it’s unknown why there’s this variability in incidence in CLL,” Dr Slager said. “Obviously, age, sex, and race—these are things you can’t modify. You’re stuck with them.”
However, several studies have been undertaken to look at some of the potentially modifiable factors associated with CLL.
Beyond demographic factors
The International Lymphoma Epidemiology Consortium, known as InterLymph, was initiated in 2001 to evaluate the association of risk factors in CLL. Study centers are located primarily in North America and Europe, with one in Australia.
In one of the larger InterLymph studies, investigators evaluated risk factors—lifestyle exposure, reproductive history, medical history, occupational exposures, farming exposure, and family history—in 2440 CLL patients and 15,186 controls.
The investigators found that sun exposure and atopy—allergies, asthma, eczema, and hay fever—have a protective effect in CLL, while serological hepatitis C virus (HCV) infections, farming exposure, and family history carry an increased risk of CLL.
This confirmed an earlier study conducted in New South Wales, Australia, that had uncovered an inverse association between sun exposure and non-Hodgkin lymphoma (NHL) risk, which fell significantly with increasing recreational sun exposure.
Medical history
Another earlier study from New South Wales revealed a 20% reduction in the risk of NHL for any specific allergy.
However, the investigators of the large, more recent study observed little to no evidence of reduced risk for asthma and eczema.
The underlying biology for atopy or allergies is a hyper-immune system, Dr Slager explained.
“So if you have a hyper-immune system, then we hypothesize that you have protection against CLL,” she said.
Another medical exposure investigators analyzed that impacts CLL risk is HCV. People infected with HCV have an increased risk of CLL, perhaps due to chronic antigen stimulation or possibly disruption of the T-cell function.
Height is also associated with CLL. CLL risk increases with greater height. The concept is that taller individuals have increased exposure to growth hormones that possibly result in cell proliferation.
Another hypothesis supporting the height association is that people of shorter stature experience more infections, which could result in a stronger immune system. And a stronger immune system perhaps protects against NHL.
Occupational exposures
Investigators consistently observed a 20% increased risk of CLL for people living or working on a farm.
Animal farmers, as opposed to crop farmers, experienced some protection. However, the sample size was too small to be conclusive, with only 29 people across all studies being animal farmers.
Among other occupations evaluated, hairdressers also had an increased risk of CLL, although this too was based on a small sample size.
Family history
One of the strongest risk factors for CLL is family history.
Using population-based registry data from Sweden, investigators found that people with a first-degree relative with CLL have an 8.5-fold risk of CLL.
They also have an elevated risk of other lymphoproliferative disorders, including NHL (1.9-fold risk), Waldenström’s macroglobulinemia (4.0-fold risk), hairy cell leukemia (3.3-fold risk), and follicular lymphoma (1.6-fold risk).
GWAS in CLL
Investigators conducted genome-wide association studies (GWAS) to determine what is driving the familial risk.
Dr Slager described these studies as an agnostic approach that looks across the entire genome to determine which regions are associated with a trait of interest.
Typically, many markers are genotyped—somewhere between half a million to 5 million markers—and each is looked at individually with respect to CLL, she said.
Unrelated cases and controls are included in the studies.
The first GWAS study identifying susceptibility loci for CLL was published in 2008. Subsequently, more studies were published with increasing sample sizes—more cases, more controls, and more genetic variants identified.
In the largest meta-analysis for CLL to date (Slager and Houlston et al, not yet published), investigators analyzed 4400 CLL cases and 13,000 controls.
They identified 9 more inherited variances with CLL, for a total of 43 identified to date.
The genes involved follow an apoptosis pathway, the telomere length pathway, and the B-cell lymphocyte development pathway.
“We have to remember, though, that these are non-causal,” Dr Slager cautioned. “We are just identifying the region in the genome that’s associated with CLL . . . . So now we have to dig deeper in these relationships to understand what’s going on.”
Using the identified CLL single-nucleotide polymorphisms, the investigators computed a polygenic risk score. CLL cases in the highest quintile had 2.7-fold increased risk of CLL.
However, the most common GWAS variants explain only 17% of the genetic heritability of CLL, which suggests that more loci are yet to be identified, Dr Slager clarified.
She went on to say that CLL incidence varies by ethnicity. Caucasians have a very high rate of CLL, while Asians have a very low rate. And African Americans have an incidence rate between those of Caucasians and Asians.
Investigators have hypothesized that the differences in incidence are based on the distinct genetic variants that are associated with the ethnicities.
For example, 4 of the variants with more than 20% frequency in Caucasians are quite rare in Chinese individuals and are also quite uncommon in African Americans, with frequencies less than 10%.
Dr Slager suggested that conducting these kinds of studies in Asians and African Americans will take a large sample size and most likely require an international consortium to bring enough CLL cases together.
Impact on clinical practice
Because of the strong genetic risk, patients with CLL naturally want to know about their offspring and their siblings, Dr Slager has found.
Patients who have monoclonal B-cell lymphocytosis (MBL), which is a precursor to CLL, pose the biggest quandary.
MBL is detected in about 5% of people over age 40. However, it’s detected in about 15% to 18% of people with a first-degree relative with CLL.
“These are individuals who have lymphocytosis,” Dr Slager said. “They come to your clinic and have an elevated blood cell count, flow cytometry. [So] you screen them for MBL, and these individuals who have more than 500 cells per microliter, they are the ones who progress to CLL, at 1% per year.”
Individuals who don’t have the elevated blood counts do have the clonal cells, Dr Slager noted.
“They just don’t have the expansion,” she said. “The progression of these individuals to CLL is still yet to be determined.”
For these reasons, Dr Slager believes “it’s still premature to bring genetic testing into clinical practice.”
Future directions include bringing together the non-environmental issues and the inherited issues to create a model that will accurately predict the risk of CLL. ![]()

Photo courtesy of the
National Institute
of General Medical Science
NEW YORK—Research has shown that family history is a strong risk factor for developing chronic lymphocytic leukemia (CLL).
First-degree relatives have an 8.5-fold risk of getting CLL and an increased risk of other lymphoproliferative disorders, according to a study published in 2009.
However, despite the strong evidence of a genetic contribution, one expert believes it’s premature to bring genetic testing into the clinic for screening in CLL.
“At this time, we do not recommend genetic screening,” said Susan Slager, PhD, of the Mayo Clinic in Rochester, Minnesota.
“There’s no known relationship between the inherited variants and treatment response,” she explained, and the relatively low incidence of CLL argues against active screening in affected families at present.
Dr Slager discussed genetic and non-genetic factors associated with CLL and the clinical implications of these factors at Lymphoma & Myeloma 2016.
Demographic risk factors
Dr Slager noted that age, gender, and race are risk factors for CLL.
Individuals aged 65 to 74 have the highest incidence of CLL, at 28%, while the risk is almost non-existent for those under age 20, she said.
There is a higher incidence of CLL in males than in females, and the reason for this gender disparity is unknown.
There is a higher incidence of CLL in Caucasians than Asians, for both males and females.
“Again, it’s unknown why there’s this variability in incidence in CLL,” Dr Slager said. “Obviously, age, sex, and race—these are things you can’t modify. You’re stuck with them.”
However, several studies have been undertaken to look at some of the potentially modifiable factors associated with CLL.
Beyond demographic factors
The International Lymphoma Epidemiology Consortium, known as InterLymph, was initiated in 2001 to evaluate the association of risk factors in CLL. Study centers are located primarily in North America and Europe, with one in Australia.
In one of the larger InterLymph studies, investigators evaluated risk factors—lifestyle exposure, reproductive history, medical history, occupational exposures, farming exposure, and family history—in 2440 CLL patients and 15,186 controls.
The investigators found that sun exposure and atopy—allergies, asthma, eczema, and hay fever—have a protective effect in CLL, while serological hepatitis C virus (HCV) infections, farming exposure, and family history carry an increased risk of CLL.
This confirmed an earlier study conducted in New South Wales, Australia, that had uncovered an inverse association between sun exposure and non-Hodgkin lymphoma (NHL) risk, which fell significantly with increasing recreational sun exposure.
Medical history
Another earlier study from New South Wales revealed a 20% reduction in the risk of NHL for any specific allergy.
However, the investigators of the large, more recent study observed little to no evidence of reduced risk for asthma and eczema.
The underlying biology for atopy or allergies is a hyper-immune system, Dr Slager explained.
“So if you have a hyper-immune system, then we hypothesize that you have protection against CLL,” she said.
Another medical exposure investigators analyzed that impacts CLL risk is HCV. People infected with HCV have an increased risk of CLL, perhaps due to chronic antigen stimulation or possibly disruption of the T-cell function.
Height is also associated with CLL. CLL risk increases with greater height. The concept is that taller individuals have increased exposure to growth hormones that possibly result in cell proliferation.
Another hypothesis supporting the height association is that people of shorter stature experience more infections, which could result in a stronger immune system. And a stronger immune system perhaps protects against NHL.
Occupational exposures
Investigators consistently observed a 20% increased risk of CLL for people living or working on a farm.
Animal farmers, as opposed to crop farmers, experienced some protection. However, the sample size was too small to be conclusive, with only 29 people across all studies being animal farmers.
Among other occupations evaluated, hairdressers also had an increased risk of CLL, although this too was based on a small sample size.
Family history
One of the strongest risk factors for CLL is family history.
Using population-based registry data from Sweden, investigators found that people with a first-degree relative with CLL have an 8.5-fold risk of CLL.
They also have an elevated risk of other lymphoproliferative disorders, including NHL (1.9-fold risk), Waldenström’s macroglobulinemia (4.0-fold risk), hairy cell leukemia (3.3-fold risk), and follicular lymphoma (1.6-fold risk).
GWAS in CLL
Investigators conducted genome-wide association studies (GWAS) to determine what is driving the familial risk.
Dr Slager described these studies as an agnostic approach that looks across the entire genome to determine which regions are associated with a trait of interest.
Typically, many markers are genotyped—somewhere between half a million to 5 million markers—and each is looked at individually with respect to CLL, she said.
Unrelated cases and controls are included in the studies.
The first GWAS study identifying susceptibility loci for CLL was published in 2008. Subsequently, more studies were published with increasing sample sizes—more cases, more controls, and more genetic variants identified.
In the largest meta-analysis for CLL to date (Slager and Houlston et al, not yet published), investigators analyzed 4400 CLL cases and 13,000 controls.
They identified 9 more inherited variances with CLL, for a total of 43 identified to date.
The genes involved follow an apoptosis pathway, the telomere length pathway, and the B-cell lymphocyte development pathway.
“We have to remember, though, that these are non-causal,” Dr Slager cautioned. “We are just identifying the region in the genome that’s associated with CLL . . . . So now we have to dig deeper in these relationships to understand what’s going on.”
Using the identified CLL single-nucleotide polymorphisms, the investigators computed a polygenic risk score. CLL cases in the highest quintile had 2.7-fold increased risk of CLL.
However, the most common GWAS variants explain only 17% of the genetic heritability of CLL, which suggests that more loci are yet to be identified, Dr Slager clarified.
She went on to say that CLL incidence varies by ethnicity. Caucasians have a very high rate of CLL, while Asians have a very low rate. And African Americans have an incidence rate between those of Caucasians and Asians.
Investigators have hypothesized that the differences in incidence are based on the distinct genetic variants that are associated with the ethnicities.
For example, 4 of the variants with more than 20% frequency in Caucasians are quite rare in Chinese individuals and are also quite uncommon in African Americans, with frequencies less than 10%.
Dr Slager suggested that conducting these kinds of studies in Asians and African Americans will take a large sample size and most likely require an international consortium to bring enough CLL cases together.
Impact on clinical practice
Because of the strong genetic risk, patients with CLL naturally want to know about their offspring and their siblings, Dr Slager has found.
Patients who have monoclonal B-cell lymphocytosis (MBL), which is a precursor to CLL, pose the biggest quandary.
MBL is detected in about 5% of people over age 40. However, it’s detected in about 15% to 18% of people with a first-degree relative with CLL.
“These are individuals who have lymphocytosis,” Dr Slager said. “They come to your clinic and have an elevated blood cell count, flow cytometry. [So] you screen them for MBL, and these individuals who have more than 500 cells per microliter, they are the ones who progress to CLL, at 1% per year.”
Individuals who don’t have the elevated blood counts do have the clonal cells, Dr Slager noted.
“They just don’t have the expansion,” she said. “The progression of these individuals to CLL is still yet to be determined.”
For these reasons, Dr Slager believes “it’s still premature to bring genetic testing into clinical practice.”
Future directions include bringing together the non-environmental issues and the inherited issues to create a model that will accurately predict the risk of CLL. ![]()

Photo courtesy of the
National Institute
of General Medical Science
NEW YORK—Research has shown that family history is a strong risk factor for developing chronic lymphocytic leukemia (CLL).
First-degree relatives have an 8.5-fold risk of getting CLL and an increased risk of other lymphoproliferative disorders, according to a study published in 2009.
However, despite the strong evidence of a genetic contribution, one expert believes it’s premature to bring genetic testing into the clinic for screening in CLL.
“At this time, we do not recommend genetic screening,” said Susan Slager, PhD, of the Mayo Clinic in Rochester, Minnesota.
“There’s no known relationship between the inherited variants and treatment response,” she explained, and the relatively low incidence of CLL argues against active screening in affected families at present.
Dr Slager discussed genetic and non-genetic factors associated with CLL and the clinical implications of these factors at Lymphoma & Myeloma 2016.
Demographic risk factors
Dr Slager noted that age, gender, and race are risk factors for CLL.
Individuals aged 65 to 74 have the highest incidence of CLL, at 28%, while the risk is almost non-existent for those under age 20, she said.
There is a higher incidence of CLL in males than in females, and the reason for this gender disparity is unknown.
There is a higher incidence of CLL in Caucasians than Asians, for both males and females.
“Again, it’s unknown why there’s this variability in incidence in CLL,” Dr Slager said. “Obviously, age, sex, and race—these are things you can’t modify. You’re stuck with them.”
However, several studies have been undertaken to look at some of the potentially modifiable factors associated with CLL.
Beyond demographic factors
The International Lymphoma Epidemiology Consortium, known as InterLymph, was initiated in 2001 to evaluate the association of risk factors in CLL. Study centers are located primarily in North America and Europe, with one in Australia.
In one of the larger InterLymph studies, investigators evaluated risk factors—lifestyle exposure, reproductive history, medical history, occupational exposures, farming exposure, and family history—in 2440 CLL patients and 15,186 controls.
The investigators found that sun exposure and atopy—allergies, asthma, eczema, and hay fever—have a protective effect in CLL, while serological hepatitis C virus (HCV) infections, farming exposure, and family history carry an increased risk of CLL.
This confirmed an earlier study conducted in New South Wales, Australia, that had uncovered an inverse association between sun exposure and non-Hodgkin lymphoma (NHL) risk, which fell significantly with increasing recreational sun exposure.
Medical history
Another earlier study from New South Wales revealed a 20% reduction in the risk of NHL for any specific allergy.
However, the investigators of the large, more recent study observed little to no evidence of reduced risk for asthma and eczema.
The underlying biology for atopy or allergies is a hyper-immune system, Dr Slager explained.
“So if you have a hyper-immune system, then we hypothesize that you have protection against CLL,” she said.
Another medical exposure investigators analyzed that impacts CLL risk is HCV. People infected with HCV have an increased risk of CLL, perhaps due to chronic antigen stimulation or possibly disruption of the T-cell function.
Height is also associated with CLL. CLL risk increases with greater height. The concept is that taller individuals have increased exposure to growth hormones that possibly result in cell proliferation.
Another hypothesis supporting the height association is that people of shorter stature experience more infections, which could result in a stronger immune system. And a stronger immune system perhaps protects against NHL.
Occupational exposures
Investigators consistently observed a 20% increased risk of CLL for people living or working on a farm.
Animal farmers, as opposed to crop farmers, experienced some protection. However, the sample size was too small to be conclusive, with only 29 people across all studies being animal farmers.
Among other occupations evaluated, hairdressers also had an increased risk of CLL, although this too was based on a small sample size.
Family history
One of the strongest risk factors for CLL is family history.
Using population-based registry data from Sweden, investigators found that people with a first-degree relative with CLL have an 8.5-fold risk of CLL.
They also have an elevated risk of other lymphoproliferative disorders, including NHL (1.9-fold risk), Waldenström’s macroglobulinemia (4.0-fold risk), hairy cell leukemia (3.3-fold risk), and follicular lymphoma (1.6-fold risk).
GWAS in CLL
Investigators conducted genome-wide association studies (GWAS) to determine what is driving the familial risk.
Dr Slager described these studies as an agnostic approach that looks across the entire genome to determine which regions are associated with a trait of interest.
Typically, many markers are genotyped—somewhere between half a million to 5 million markers—and each is looked at individually with respect to CLL, she said.
Unrelated cases and controls are included in the studies.
The first GWAS study identifying susceptibility loci for CLL was published in 2008. Subsequently, more studies were published with increasing sample sizes—more cases, more controls, and more genetic variants identified.
In the largest meta-analysis for CLL to date (Slager and Houlston et al, not yet published), investigators analyzed 4400 CLL cases and 13,000 controls.
They identified 9 more inherited variances with CLL, for a total of 43 identified to date.
The genes involved follow an apoptosis pathway, the telomere length pathway, and the B-cell lymphocyte development pathway.
“We have to remember, though, that these are non-causal,” Dr Slager cautioned. “We are just identifying the region in the genome that’s associated with CLL . . . . So now we have to dig deeper in these relationships to understand what’s going on.”
Using the identified CLL single-nucleotide polymorphisms, the investigators computed a polygenic risk score. CLL cases in the highest quintile had 2.7-fold increased risk of CLL.
However, the most common GWAS variants explain only 17% of the genetic heritability of CLL, which suggests that more loci are yet to be identified, Dr Slager clarified.
She went on to say that CLL incidence varies by ethnicity. Caucasians have a very high rate of CLL, while Asians have a very low rate. And African Americans have an incidence rate between those of Caucasians and Asians.
Investigators have hypothesized that the differences in incidence are based on the distinct genetic variants that are associated with the ethnicities.
For example, 4 of the variants with more than 20% frequency in Caucasians are quite rare in Chinese individuals and are also quite uncommon in African Americans, with frequencies less than 10%.
Dr Slager suggested that conducting these kinds of studies in Asians and African Americans will take a large sample size and most likely require an international consortium to bring enough CLL cases together.
Impact on clinical practice
Because of the strong genetic risk, patients with CLL naturally want to know about their offspring and their siblings, Dr Slager has found.
Patients who have monoclonal B-cell lymphocytosis (MBL), which is a precursor to CLL, pose the biggest quandary.
MBL is detected in about 5% of people over age 40. However, it’s detected in about 15% to 18% of people with a first-degree relative with CLL.
“These are individuals who have lymphocytosis,” Dr Slager said. “They come to your clinic and have an elevated blood cell count, flow cytometry. [So] you screen them for MBL, and these individuals who have more than 500 cells per microliter, they are the ones who progress to CLL, at 1% per year.”
Individuals who don’t have the elevated blood counts do have the clonal cells, Dr Slager noted.
“They just don’t have the expansion,” she said. “The progression of these individuals to CLL is still yet to be determined.”
For these reasons, Dr Slager believes “it’s still premature to bring genetic testing into clinical practice.”
Future directions include bringing together the non-environmental issues and the inherited issues to create a model that will accurately predict the risk of CLL. ![]()
Higher-volume facilities show better myeloma outcomes
Patients with multiple myeloma who received treatment from facilities that see a greater number of multiple myeloma patients have significantly lower overall mortality, compared with those who attend lower-volume facilities, new research suggests.
There is a strong body of evidence showing higher-volume surgical oncology is associated with better clinical outcomes, but there is a lack of similar studies for medical oncology, wrote Dr. Ronald S. Go and his colleagues at the Mayo Clinic in Rochester, Minn.
To investigate, researchers analyzed National Cancer Database data from 94,722 patients with multiple myeloma who were treated at 1,333 facilities. The median number of new multiple myeloma patients seen across all facilities each year was 6.1 patients, with a quartile range of 3.6 patients per year to 10.3.
Patients treated at facilities in the lowest quartile of patient volume had a 22% higher risk of death, compared with patients treated in the highest-volume–quartile facilities, Dr. Go and his colleagues reported (J Clin Oncol. 2016 Oct 26. doi: 10.1200/JCO.2016.68.3805).
Those in the third-lowest volume quartile had a 17% increased risk of death and those in the second-lowest volume quartile had a 12% increased risk, compared with the highest-volume quartile.
Overall, median survival times were 26.9 months for the lowest-volume quartile, then 29.1 months, 31.9 months, and 49.1 months for the second-lowest, second-highest, and highest-volume quartiles, respectively.
“Compared with facilities treating 10 patients per year, facilities treating 20, 30, and 40 patients per year had approximately 10%, 15%, and 20% lower overall mortality rates,” the authors wrote.
They noted that the relationship between patient volume and mortality was almost linear, with no obvious sign of a plateau. The magnitude of difference in mortality between the high- and low-volume institutions was also similar to that seen in studies of lung and rectal cancer surgery.
This relationship between patient volume and outcomes was independent of potential confounders, such as sociodemographic and geographic factors, comorbidities, and clustering of outcome within hospitals.
More than 60% of patients were treated in facilities within the top-quartile facilities with an annual patient volume of greater than 10.3 new patients a year, but only 18 of the 1,333 facilities treated more than 50 new patients with multiple myeloma each year, the investigators said.
Facilities in the top two quartiles were more likely to be academic, and their patients were more likely to be younger, black, and privately insured and to reside in metropolitan areas.
Commenting on their findings, the authors suggested that it should come as no surprise to see such a link between patient volume and outcomes, especially given the unprecedented rate of new drugs becoming available for the treatment of multiple myeloma and of new information being published about the disease.
“Keeping up with pertinent new knowledge in [multiple myeloma], which comprises only 2% of all cancers, and at the same time maintaining proficiency in its management, is becoming more difficult, especially if one also has to stay current in all the other cancers,” Dr. Go and his associates wrote.
They suggested an approach similar to that taken for oncologic surgery, with patients being referred to centers of excellence, although they noted that this approach should move beyond NCI-designated cancer centers alone.
Given the challenges inherent in setting up such a system to deal with rare chronic cancers, they also suggested an interim option of comanagement with a high-volume facility. “This model of care can be further enhanced by preferentially funneling patients with hematologic cancer to a limited number of hematologist-oncologists per practice to accelerate accumulation of clinical experience and development of treatment proficiency.”
The study was supported by the Eagles Cancer Research Fund Pilot Grant, Mayo Clinic division of hematology, and the Mayo Clinic Robert D. and Patricia E. Kern Center for the Science of Health Care Delivery. One author declared research funding from Genentech, but no other conflicts were declared.
Patients with multiple myeloma who received treatment from facilities that see a greater number of multiple myeloma patients have significantly lower overall mortality, compared with those who attend lower-volume facilities, new research suggests.
There is a strong body of evidence showing higher-volume surgical oncology is associated with better clinical outcomes, but there is a lack of similar studies for medical oncology, wrote Dr. Ronald S. Go and his colleagues at the Mayo Clinic in Rochester, Minn.
To investigate, researchers analyzed National Cancer Database data from 94,722 patients with multiple myeloma who were treated at 1,333 facilities. The median number of new multiple myeloma patients seen across all facilities each year was 6.1 patients, with a quartile range of 3.6 patients per year to 10.3.
Patients treated at facilities in the lowest quartile of patient volume had a 22% higher risk of death, compared with patients treated in the highest-volume–quartile facilities, Dr. Go and his colleagues reported (J Clin Oncol. 2016 Oct 26. doi: 10.1200/JCO.2016.68.3805).
Those in the third-lowest volume quartile had a 17% increased risk of death and those in the second-lowest volume quartile had a 12% increased risk, compared with the highest-volume quartile.
Overall, median survival times were 26.9 months for the lowest-volume quartile, then 29.1 months, 31.9 months, and 49.1 months for the second-lowest, second-highest, and highest-volume quartiles, respectively.
“Compared with facilities treating 10 patients per year, facilities treating 20, 30, and 40 patients per year had approximately 10%, 15%, and 20% lower overall mortality rates,” the authors wrote.
They noted that the relationship between patient volume and mortality was almost linear, with no obvious sign of a plateau. The magnitude of difference in mortality between the high- and low-volume institutions was also similar to that seen in studies of lung and rectal cancer surgery.
This relationship between patient volume and outcomes was independent of potential confounders, such as sociodemographic and geographic factors, comorbidities, and clustering of outcome within hospitals.
More than 60% of patients were treated in facilities within the top-quartile facilities with an annual patient volume of greater than 10.3 new patients a year, but only 18 of the 1,333 facilities treated more than 50 new patients with multiple myeloma each year, the investigators said.
Facilities in the top two quartiles were more likely to be academic, and their patients were more likely to be younger, black, and privately insured and to reside in metropolitan areas.
Commenting on their findings, the authors suggested that it should come as no surprise to see such a link between patient volume and outcomes, especially given the unprecedented rate of new drugs becoming available for the treatment of multiple myeloma and of new information being published about the disease.
“Keeping up with pertinent new knowledge in [multiple myeloma], which comprises only 2% of all cancers, and at the same time maintaining proficiency in its management, is becoming more difficult, especially if one also has to stay current in all the other cancers,” Dr. Go and his associates wrote.
They suggested an approach similar to that taken for oncologic surgery, with patients being referred to centers of excellence, although they noted that this approach should move beyond NCI-designated cancer centers alone.
Given the challenges inherent in setting up such a system to deal with rare chronic cancers, they also suggested an interim option of comanagement with a high-volume facility. “This model of care can be further enhanced by preferentially funneling patients with hematologic cancer to a limited number of hematologist-oncologists per practice to accelerate accumulation of clinical experience and development of treatment proficiency.”
The study was supported by the Eagles Cancer Research Fund Pilot Grant, Mayo Clinic division of hematology, and the Mayo Clinic Robert D. and Patricia E. Kern Center for the Science of Health Care Delivery. One author declared research funding from Genentech, but no other conflicts were declared.
Patients with multiple myeloma who received treatment from facilities that see a greater number of multiple myeloma patients have significantly lower overall mortality, compared with those who attend lower-volume facilities, new research suggests.
There is a strong body of evidence showing higher-volume surgical oncology is associated with better clinical outcomes, but there is a lack of similar studies for medical oncology, wrote Dr. Ronald S. Go and his colleagues at the Mayo Clinic in Rochester, Minn.
To investigate, researchers analyzed National Cancer Database data from 94,722 patients with multiple myeloma who were treated at 1,333 facilities. The median number of new multiple myeloma patients seen across all facilities each year was 6.1 patients, with a quartile range of 3.6 patients per year to 10.3.
Patients treated at facilities in the lowest quartile of patient volume had a 22% higher risk of death, compared with patients treated in the highest-volume–quartile facilities, Dr. Go and his colleagues reported (J Clin Oncol. 2016 Oct 26. doi: 10.1200/JCO.2016.68.3805).
Those in the third-lowest volume quartile had a 17% increased risk of death and those in the second-lowest volume quartile had a 12% increased risk, compared with the highest-volume quartile.
Overall, median survival times were 26.9 months for the lowest-volume quartile, then 29.1 months, 31.9 months, and 49.1 months for the second-lowest, second-highest, and highest-volume quartiles, respectively.
“Compared with facilities treating 10 patients per year, facilities treating 20, 30, and 40 patients per year had approximately 10%, 15%, and 20% lower overall mortality rates,” the authors wrote.
They noted that the relationship between patient volume and mortality was almost linear, with no obvious sign of a plateau. The magnitude of difference in mortality between the high- and low-volume institutions was also similar to that seen in studies of lung and rectal cancer surgery.
This relationship between patient volume and outcomes was independent of potential confounders, such as sociodemographic and geographic factors, comorbidities, and clustering of outcome within hospitals.
More than 60% of patients were treated in facilities within the top-quartile facilities with an annual patient volume of greater than 10.3 new patients a year, but only 18 of the 1,333 facilities treated more than 50 new patients with multiple myeloma each year, the investigators said.
Facilities in the top two quartiles were more likely to be academic, and their patients were more likely to be younger, black, and privately insured and to reside in metropolitan areas.
Commenting on their findings, the authors suggested that it should come as no surprise to see such a link between patient volume and outcomes, especially given the unprecedented rate of new drugs becoming available for the treatment of multiple myeloma and of new information being published about the disease.
“Keeping up with pertinent new knowledge in [multiple myeloma], which comprises only 2% of all cancers, and at the same time maintaining proficiency in its management, is becoming more difficult, especially if one also has to stay current in all the other cancers,” Dr. Go and his associates wrote.
They suggested an approach similar to that taken for oncologic surgery, with patients being referred to centers of excellence, although they noted that this approach should move beyond NCI-designated cancer centers alone.
Given the challenges inherent in setting up such a system to deal with rare chronic cancers, they also suggested an interim option of comanagement with a high-volume facility. “This model of care can be further enhanced by preferentially funneling patients with hematologic cancer to a limited number of hematologist-oncologists per practice to accelerate accumulation of clinical experience and development of treatment proficiency.”
The study was supported by the Eagles Cancer Research Fund Pilot Grant, Mayo Clinic division of hematology, and the Mayo Clinic Robert D. and Patricia E. Kern Center for the Science of Health Care Delivery. One author declared research funding from Genentech, but no other conflicts were declared.
FROM THE JOURNAL OF CLINICAL ONCOLOGY
Key clinical point: .
Major finding: Individuals with multiple myeloma treated at facilities in the lowest quartile of patient volume had a 22% higher risk of death, compared with patients treated in the highest-volume–quartile facilities.
Data source: Analysis of National Cancer Database data from 94,722 patients with multiple myeloma treated at 1,333 facilities.
Disclosures: The study was supported by the Eagles Cancer Research Fund Pilot Grant, Mayo Clinic division of hematology, and the Mayo Clinic Robert D. and Patricia E. Kern Center for the Science of Health Care Delivery. One author declared research funding from Genentech, but no other conflicts were declared.
Anticipate monoclonals in first-line therapy for multiple myeloma
NEW YORK – Monoclonal antibodies may soon have more of a role in the front-line treatment setting for multiple myeloma and as part of precollection/transplant regimens–or “so-called in vivo purges,” according to Tomer M. Mark, MD, of the department of clinical medicine at the Cornell University, New York.
They could also be used both in the preclinical setting for smoldering multiple myeloma, and for maintenance following transplant, which makes sense given that they are, for the most part, not myelosuppressive and have “very tolerable toxicities,” he said.
Myeloma is “sort of catching up to lymphoma in terms of antibody use and development. ... Approval trials are underway,” Dr. Mark said at Imedex: Lymphoma & Myeloma, an international congress on hematologic malignancies.
The successes of the phase III trials CASTOR and POLLUX in patients with relapsed and refractory multiple myeloma have paved the way for trials to examine daratumumab in first-line combination therapy.
In POLLUX, progression-free survival, time to progression, and overall response rate were superior with daratumumab in combination with lenalidomide/dexamethasone, as compared with lenalidomide/dexamethasone alone, in relapsed or refractory multiple myeloma patients. In CASTOR, daratumumab in combination with bortezomib and dexamethasone was superior to bortezomib and dexamethasone alone in a similar patient population. Of note, the effect was attenuated in those with multiple prior lines of treatment, which is, perhaps, an argument for moving monoclonal antibodies closer to the start of therapy, he said.
Daratumumab (Darzalex), which targets CD38, is currently indicated for the treatment of patients with multiple myeloma who have received at least three prior lines of therapy including a proteasome inhibitor and an immunomodulatory agent or who are double refractory to a proteasome inhibitor and an immunomodulatory agent.
Similarly, elotuzumab (Empliciti), an immunostimulatory monoclonal antibody targeting a cell-surface receptor with both direct activation of natural killer cells and the capacity to trigger antibody-dependent, cell-mediated cytotoxicity of myeloma cells, is indicated in combination with lenalidomide/dexamethasone in patients who have received one to three therapies. Elotuzumab was shown in one trial to be associated with progression-free survival of 68% at 1 and 41% at 2 years when used with lenalidomide/dexamethasone. Patients receiving elotuzumab had a relative reduction of 30% in the risk of disease progression or death as compared with the control group.
In an ongoing trial with initial results reported at the 2015 American Society of Hematology annual meeting, elotuzumab with bortezomib/dexamethasone was associated with a more modest improvement in median progression-free survival, which was 9.9 months with triple therapy and 6.8 months with bortezomib/dexamethasone alone.
Both drugs have shown activity as single agents. In a phase I study, elotuzumab was associated with disease stability in 26% of patients, Dr. Mark said. Daratumumab, used as monotherapy in a study of relapsed or relapsed/refractory multiple myeloma patients, was associated with good overall response and progression-free survival, and “quite amazing” overall survival of 65%.
Other monoclonal antibodies in development include isatuximab (anti-CD38), lorvotuzumab mertansine (anti-CD56), and indatuximab ravtansine (anti-CD128), Dr. Mark said.
Dr. Mark reported receiving research funding from Celgene and Amgen, serving on speakers bureaus for Celgene, Millennium, Amgen, and Bristol-Myers Squibb, and serving on an advisory committee for Celgene and Millennium.
NEW YORK – Monoclonal antibodies may soon have more of a role in the front-line treatment setting for multiple myeloma and as part of precollection/transplant regimens–or “so-called in vivo purges,” according to Tomer M. Mark, MD, of the department of clinical medicine at the Cornell University, New York.
They could also be used both in the preclinical setting for smoldering multiple myeloma, and for maintenance following transplant, which makes sense given that they are, for the most part, not myelosuppressive and have “very tolerable toxicities,” he said.
Myeloma is “sort of catching up to lymphoma in terms of antibody use and development. ... Approval trials are underway,” Dr. Mark said at Imedex: Lymphoma & Myeloma, an international congress on hematologic malignancies.
The successes of the phase III trials CASTOR and POLLUX in patients with relapsed and refractory multiple myeloma have paved the way for trials to examine daratumumab in first-line combination therapy.
In POLLUX, progression-free survival, time to progression, and overall response rate were superior with daratumumab in combination with lenalidomide/dexamethasone, as compared with lenalidomide/dexamethasone alone, in relapsed or refractory multiple myeloma patients. In CASTOR, daratumumab in combination with bortezomib and dexamethasone was superior to bortezomib and dexamethasone alone in a similar patient population. Of note, the effect was attenuated in those with multiple prior lines of treatment, which is, perhaps, an argument for moving monoclonal antibodies closer to the start of therapy, he said.
Daratumumab (Darzalex), which targets CD38, is currently indicated for the treatment of patients with multiple myeloma who have received at least three prior lines of therapy including a proteasome inhibitor and an immunomodulatory agent or who are double refractory to a proteasome inhibitor and an immunomodulatory agent.
Similarly, elotuzumab (Empliciti), an immunostimulatory monoclonal antibody targeting a cell-surface receptor with both direct activation of natural killer cells and the capacity to trigger antibody-dependent, cell-mediated cytotoxicity of myeloma cells, is indicated in combination with lenalidomide/dexamethasone in patients who have received one to three therapies. Elotuzumab was shown in one trial to be associated with progression-free survival of 68% at 1 and 41% at 2 years when used with lenalidomide/dexamethasone. Patients receiving elotuzumab had a relative reduction of 30% in the risk of disease progression or death as compared with the control group.
In an ongoing trial with initial results reported at the 2015 American Society of Hematology annual meeting, elotuzumab with bortezomib/dexamethasone was associated with a more modest improvement in median progression-free survival, which was 9.9 months with triple therapy and 6.8 months with bortezomib/dexamethasone alone.
Both drugs have shown activity as single agents. In a phase I study, elotuzumab was associated with disease stability in 26% of patients, Dr. Mark said. Daratumumab, used as monotherapy in a study of relapsed or relapsed/refractory multiple myeloma patients, was associated with good overall response and progression-free survival, and “quite amazing” overall survival of 65%.
Other monoclonal antibodies in development include isatuximab (anti-CD38), lorvotuzumab mertansine (anti-CD56), and indatuximab ravtansine (anti-CD128), Dr. Mark said.
Dr. Mark reported receiving research funding from Celgene and Amgen, serving on speakers bureaus for Celgene, Millennium, Amgen, and Bristol-Myers Squibb, and serving on an advisory committee for Celgene and Millennium.
NEW YORK – Monoclonal antibodies may soon have more of a role in the front-line treatment setting for multiple myeloma and as part of precollection/transplant regimens–or “so-called in vivo purges,” according to Tomer M. Mark, MD, of the department of clinical medicine at the Cornell University, New York.
They could also be used both in the preclinical setting for smoldering multiple myeloma, and for maintenance following transplant, which makes sense given that they are, for the most part, not myelosuppressive and have “very tolerable toxicities,” he said.
Myeloma is “sort of catching up to lymphoma in terms of antibody use and development. ... Approval trials are underway,” Dr. Mark said at Imedex: Lymphoma & Myeloma, an international congress on hematologic malignancies.
The successes of the phase III trials CASTOR and POLLUX in patients with relapsed and refractory multiple myeloma have paved the way for trials to examine daratumumab in first-line combination therapy.
In POLLUX, progression-free survival, time to progression, and overall response rate were superior with daratumumab in combination with lenalidomide/dexamethasone, as compared with lenalidomide/dexamethasone alone, in relapsed or refractory multiple myeloma patients. In CASTOR, daratumumab in combination with bortezomib and dexamethasone was superior to bortezomib and dexamethasone alone in a similar patient population. Of note, the effect was attenuated in those with multiple prior lines of treatment, which is, perhaps, an argument for moving monoclonal antibodies closer to the start of therapy, he said.
Daratumumab (Darzalex), which targets CD38, is currently indicated for the treatment of patients with multiple myeloma who have received at least three prior lines of therapy including a proteasome inhibitor and an immunomodulatory agent or who are double refractory to a proteasome inhibitor and an immunomodulatory agent.
Similarly, elotuzumab (Empliciti), an immunostimulatory monoclonal antibody targeting a cell-surface receptor with both direct activation of natural killer cells and the capacity to trigger antibody-dependent, cell-mediated cytotoxicity of myeloma cells, is indicated in combination with lenalidomide/dexamethasone in patients who have received one to three therapies. Elotuzumab was shown in one trial to be associated with progression-free survival of 68% at 1 and 41% at 2 years when used with lenalidomide/dexamethasone. Patients receiving elotuzumab had a relative reduction of 30% in the risk of disease progression or death as compared with the control group.
In an ongoing trial with initial results reported at the 2015 American Society of Hematology annual meeting, elotuzumab with bortezomib/dexamethasone was associated with a more modest improvement in median progression-free survival, which was 9.9 months with triple therapy and 6.8 months with bortezomib/dexamethasone alone.
Both drugs have shown activity as single agents. In a phase I study, elotuzumab was associated with disease stability in 26% of patients, Dr. Mark said. Daratumumab, used as monotherapy in a study of relapsed or relapsed/refractory multiple myeloma patients, was associated with good overall response and progression-free survival, and “quite amazing” overall survival of 65%.
Other monoclonal antibodies in development include isatuximab (anti-CD38), lorvotuzumab mertansine (anti-CD56), and indatuximab ravtansine (anti-CD128), Dr. Mark said.
Dr. Mark reported receiving research funding from Celgene and Amgen, serving on speakers bureaus for Celgene, Millennium, Amgen, and Bristol-Myers Squibb, and serving on an advisory committee for Celgene and Millennium.
EXPERT ANALYSIS FROM IMEDEX: LYMPHOMA & MYELOMA
FDA grants drug orphan designation for CTCL
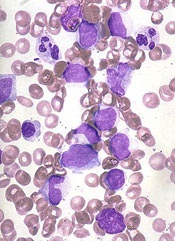
The US Food and Drug Administration (FDA) has granted orphan drug designation to TLC178 for the treatment of cutaneous T-cell lymphoma (CTCL).
TLC178 is a liposomal-encapsulated formulation of the chemotherapy drug vinorelbine, which is FDA approved to treat non-small cell lung cancer.
The goal with TLC178 is to improve the efficacy and decrease the toxicity of vinorelbine to extend the indication beyond solid tumors into lymphoma.
A proprietary technology known as NanoX™ is used to load vinorelbine into liposomes designed to target tumor-specific cell-surface epitopes, extend the circulation time of the drug, increase the concentation of drug delivered to tumor cells, and decrease side effects.
TLC178 is being developed by Taiwan Liposome Company.
The company recently received US FDA approval for its phase 1/2 study (NCT02925000) investigating TLC178 in patients with advanced cancers, including CTCL and other lymphomas.
This trial is planned for sites in Taiwan and the US. The trial will be initiated in Taiwan once approval is granted by the Taiwan FDA.
About orphan designation
The US FDA grants orphan designation to drugs and biologics intended to treat, diagnose, or prevent diseases/disorders that affect fewer than 200,000 people in the US.
The designation provides incentives for sponsors to develop products for rare diseases. This may include tax credits toward the cost of clinical trials, prescription drug user fee waivers, and 7 years of market exclusivity if the product is approved. ![]()

The US Food and Drug Administration (FDA) has granted orphan drug designation to TLC178 for the treatment of cutaneous T-cell lymphoma (CTCL).
TLC178 is a liposomal-encapsulated formulation of the chemotherapy drug vinorelbine, which is FDA approved to treat non-small cell lung cancer.
The goal with TLC178 is to improve the efficacy and decrease the toxicity of vinorelbine to extend the indication beyond solid tumors into lymphoma.
A proprietary technology known as NanoX™ is used to load vinorelbine into liposomes designed to target tumor-specific cell-surface epitopes, extend the circulation time of the drug, increase the concentation of drug delivered to tumor cells, and decrease side effects.
TLC178 is being developed by Taiwan Liposome Company.
The company recently received US FDA approval for its phase 1/2 study (NCT02925000) investigating TLC178 in patients with advanced cancers, including CTCL and other lymphomas.
This trial is planned for sites in Taiwan and the US. The trial will be initiated in Taiwan once approval is granted by the Taiwan FDA.
About orphan designation
The US FDA grants orphan designation to drugs and biologics intended to treat, diagnose, or prevent diseases/disorders that affect fewer than 200,000 people in the US.
The designation provides incentives for sponsors to develop products for rare diseases. This may include tax credits toward the cost of clinical trials, prescription drug user fee waivers, and 7 years of market exclusivity if the product is approved. ![]()

The US Food and Drug Administration (FDA) has granted orphan drug designation to TLC178 for the treatment of cutaneous T-cell lymphoma (CTCL).
TLC178 is a liposomal-encapsulated formulation of the chemotherapy drug vinorelbine, which is FDA approved to treat non-small cell lung cancer.
The goal with TLC178 is to improve the efficacy and decrease the toxicity of vinorelbine to extend the indication beyond solid tumors into lymphoma.
A proprietary technology known as NanoX™ is used to load vinorelbine into liposomes designed to target tumor-specific cell-surface epitopes, extend the circulation time of the drug, increase the concentation of drug delivered to tumor cells, and decrease side effects.
TLC178 is being developed by Taiwan Liposome Company.
The company recently received US FDA approval for its phase 1/2 study (NCT02925000) investigating TLC178 in patients with advanced cancers, including CTCL and other lymphomas.
This trial is planned for sites in Taiwan and the US. The trial will be initiated in Taiwan once approval is granted by the Taiwan FDA.
About orphan designation
The US FDA grants orphan designation to drugs and biologics intended to treat, diagnose, or prevent diseases/disorders that affect fewer than 200,000 people in the US.
The designation provides incentives for sponsors to develop products for rare diseases. This may include tax credits toward the cost of clinical trials, prescription drug user fee waivers, and 7 years of market exclusivity if the product is approved.
No longer a hand-me-down approach to WM

Photo courtesy of DFCI
NEW YORK—Whole-genome sequencing has changed the entire approach to drug development for Waldenström’s macroglobulinemia (WM), according to a speaker at Lymphoma & Myeloma 2016.
The strategy has changed from a hand-me-down one, relying on drugs developed first for other diseases, to a rational plan designed specifically to treat WM patients.
“We would wait for our colleagues in the myeloma world or lymphoma world, CLL world, anywhere we could find them, to help us with the development of drugs,” said Steven Treon, MD, PhD, of the Dana-Farber Cancer Institute in Boston, Massachusetts.
“And, sometimes, this resulted in delays of many, many years before those therapeutics could be vetted out and eventually be handed down to the Waldenström investigators.”
At Lymphoma & Myeloma 2016, Dr Treon described the current therapy of WM and the impact of the discovery of MYD88 and CXCR4 on drug development and treatment choices in WM.
Rituximab-based therapy
WM is a disease that strongly expresses CD20, even though it’s a lymphoplasmacytic disease. So rituximab, given alone and in combination, has been, to date, the most common approach to treating WM.
As a single agent, rituximab produces a response in 25% to 40% of WM patients, but these are very seldom deep responses, Dr Treon noted.
So investigators combined rituximab with cyclophosphamide, nucleoside analogues, proteasome inhibitors, and bendamustine, which increased the overall response rate and depth of response.
This translated into improvement in time to progression, which is now 4 to 5 years with these combination therapies.
“Now, the problem is, when you borrow things from other people, you sometimes end up with problems you didn’t anticipate,” Dr Treon said.
One of the unanticipated side effects with rituximab in WM patients is the IgM flare, which occurs in 40% to 60% of WM patients.
Rituximab can also cause hypogammaglobulinema, leading to infections, and results in a high intolerance rate, which tends to occur a few cycles into induction or maintenance therapy.
“In some cases,” Dr Treon advised, “a switch to ofatumumab, a fully human CD20 molecule, overcomes this intolerance.”
Nucleoside analogues, which used to be the mainstay of WM, have a high rate of transformation into a more aggressive lymphoma or acute myeloid leukemia.
Immunomodulatory drugs, particularly thalidomide, cause peripheral neuropathy greater than grade 2 in 60% of patients.
And a greater incidence of peripheral neuropathy is also observed with proteasome inhibitors, particularly bortezomib, in WM patients than in myeloma or mantle cell lymphoma patients.
“So this was at least the impetus for why we needed to develop novel approaches to treating this disease,” Dr Treon said.
MYD88 mutations
With whole-genome sequencing, investigators discovered that mutations in the MYD88 gene were highly prevalent in WM patients.
About 93% to 95% of WM patients have the L265P MYD88 mutation, and about 2% have the non-L265P MYD88 mutation.
MYD88 has prognostic significance in WM. Mutated MYD88 confers a better prognosis than unmutated MYD88.
MYD88 may also be important in predicting who will respond to drugs like ibrutinib.
CXCR4 mutations
Mutations in CXCR4 are the second most common mutation in WM.
Between 30% and 40% of WM patients have the WHIM-like CXCR4 C-tail mutations, which traffic the Waldenström’s cells to the bone marrow.
This mutation promotes drug resistance, including resistance to ibrutinib because of the enhanced AKT/ERK signaling.
Ibrutinib therapy
With this in mind, investigators set out to evaluate the potential of using a BTK inhibitor in relapsed/refractory WM patients and at the same time observe the genomics that might predict for response and resistance.
They enrolled 63 patients in the multicenter study. Patients had a median of 2 prior therapies (range, 1–9), and 60% had bone marrow involvement.
Patients received single-agent ibrutinib at a dose of 420 mg orally each day until disease progression or the development of unacceptable toxic side effects.
“By the time they came back 4 weeks later to be evaluated, many of them were already in a response,” Dr Treon said. “And what we saw, in fact, was almost immediate improvement in hemoglobin, something that we didn’t see with many of our trials before that.”
The best IgM response reduced levels from 3520 to 880 mg/dL (P<0.001) for the entire cohort.
The best hemoglobin response increased hemoglobin levels 3 points, from 10.5 to 13.8 g/dL (P<0.001).
The progression-free survival at 2 years was 69% and overall survival was 95%.
At 37 months, most patients who achieve a response experience a durable, ongoing response, according to an update presented at the IX International Workshop on Waldenstrom’s Macroglobulinemia.
And toxicities were “very much in line with what our colleagues have seen in other disease groups,” Dr Treon stated.
Response to ibrutinib by mutation status
The overall response rate was 90% for all patients, but there were differences according to mutation status.
Patients with no MYD88 mutation and no CXCR4 mutation had absolutely no major response.
Patients with a MYD88 mutation responded at an overall rate of 100% and had a major response rate of 91.7% if they did not have a CXCR4 mutation as well.
If they also had a CXCR4WHIM mutation, the overall response rate was lower, at 85.7%, and the major response rate was 61.9%.
“It’s still something to be incredibly excited about—61.9% single-agent activity,” Dr Treon said.
Patients with a CXCR4 mutation also respond more slowly than those without the mutation.
This investigator-sponsored study led to the approval of ibrutinib in WM in the US as well as in Europe and Canada.
“And the point to make about this is that investigators can bring their data to the FDA, the EMA, even Canada, and it can make a difference,” Dr Treon said.
“We don’t always have to have company-sponsored registration studies to be able to make these kinds of advances.”
Ibrutinib in rituximab-refractory patients
A multicenter, phase 3 study of ibrutinib in rituximab-refractory patients was “almost a photocopy of our study,” Dr Treon said.
The main difference was that the patients were even sicker, having failed a median of 4 prior therapies.
Patients experienced rapid improvements in hemoglobin and IgM levels and had an overall response rate of 90%.
Patients with a CXCR4 mutation also tended to lag in terms of pace of hemoglobin improvement and reduction in IgM.
The study was just accepted for publication in Lancet Oncology.
IRAK inhibition
Investigators were puzzled by the paucity of complete responses with ibrutinib, and they found the IRAK pathway remained turned on in patients treated with ibrutinib.
So they took cells of patients treated for 6 months with ibrutinib and co-cultured them with ibrutinib and an IRAK inhibitor. They observed the induction of apoptosis.
Based on this finding, the investigators are manufacturing a very potent IRAK1 inhibitor (JH-X-119), which, when combined with ibrutinib, synergistically increases tumor-cell killing.
“And so one of the strategies we have going forward,” Dr Treon said, “is the ability to advance ibrutinib therapy in MYD88-mutated tumors by the addition of the IRAK inhibitor.”
Resistance to ibrutinib
Investigators have found multiple mutations in the C481 site in individual WM patients, which is where ibrutinib binds.
These mutations represent a minority of the clone, but they exert almost a fully clonal signature. The few patients with these mutations also have a CXCR4 mutation.
C481 mutations shift the signaling of cells in the presence of ibrutinib toward ERK, which is a very powerful survival pathway.
So investigators are examining whether an ERK inhibitor combined with ibrutinib can elicit synergistic killing of BTK-resistant cells.
Investigators have also been synthesizing potent HCK inhibitors, which might overcome BTK mutations by shutting down the ability to activate Bruton’s tyrosine kinase.
Other drugs being developed for WM include:
- Combinations with a proteasome inhibitor, such as ixazomib, dexamethasone, and rituximab
- Agents that target MYD88 signaling, such as the BTK inhibitors acalabrutinib and BGB-3111
- Agents that block CXCR4 receptor signaling, such as ulocuplomab
- The BCL2 inhibitor venetoclax
- The CD38-targeted agent daratumumab.
Current treatment strategies
Knowing a patient’s MYD88 and CXCR4 mutation status provides an opportunity to take a rational approach to treating individuals with WM, Dr Treon said.
For patients with mutated MYD88 and no CXCR4 mutation:
- If patients do not have bulky disease or contraindications, ibrutinib may be used if available.
- If patients have bulky disease, a combination of bendamustine and rituximab may be used.
- If patients have amyloidosis, a combination of bortezomib, dexamethasone, and rituximab is possible.
- If patients have IgM peripheral neuropathy, then rituximab with or without an alkylator is recommended.
For patients with mutated MYD88 and mutated CXCR4, the same treatments can be used as for patients with mutated MYD88 and unmutated CXCR4 with the same restrictions.
To achieve an immediate response for patients with a CXCR4 mutation, an alternative therapy to ibrutinib—such as the bendamustine, dexamethasone, rituximab combination—may be the best choice, because CXCR4-mutated individuals have a slower response to ibrutinib.
The problem arises with the MYD88-wild-type patients, because their survival is poorer than the MYD88-mutated patients.
“We still don’t know what’s wrong with these individuals,” Dr Treon said. “We don’t have any idea about what their basic genomic problems are.”
Bendamustine- or bortezomib-based therapy is effective in this population and can be considered.
In terms of salvage therapy, “the only thing to keep in mind is that if something worked the first time and you got at least a 2-year response with it, you can go back and consider it,” Dr Treon said.

Photo courtesy of DFCI
NEW YORK—Whole-genome sequencing has changed the entire approach to drug development for Waldenström’s macroglobulinemia (WM), according to a speaker at Lymphoma & Myeloma 2016.
The strategy has changed from a hand-me-down one, relying on drugs developed first for other diseases, to a rational plan designed specifically to treat WM patients.
“We would wait for our colleagues in the myeloma world or lymphoma world, CLL world, anywhere we could find them, to help us with the development of drugs,” said Steven Treon, MD, PhD, of the Dana-Farber Cancer Institute in Boston, Massachusetts.
“And, sometimes, this resulted in delays of many, many years before those therapeutics could be vetted out and eventually be handed down to the Waldenström investigators.”
At Lymphoma & Myeloma 2016, Dr Treon described the current therapy of WM and the impact of the discovery of MYD88 and CXCR4 on drug development and treatment choices in WM.
Rituximab-based therapy
WM is a disease that strongly expresses CD20, even though it’s a lymphoplasmacytic disease. So rituximab, given alone and in combination, has been, to date, the most common approach to treating WM.
As a single agent, rituximab produces a response in 25% to 40% of WM patients, but these are very seldom deep responses, Dr Treon noted.
So investigators combined rituximab with cyclophosphamide, nucleoside analogues, proteasome inhibitors, and bendamustine, which increased the overall response rate and depth of response.
This translated into improvement in time to progression, which is now 4 to 5 years with these combination therapies.
“Now, the problem is, when you borrow things from other people, you sometimes end up with problems you didn’t anticipate,” Dr Treon said.
One of the unanticipated side effects with rituximab in WM patients is the IgM flare, which occurs in 40% to 60% of WM patients.
Rituximab can also cause hypogammaglobulinema, leading to infections, and results in a high intolerance rate, which tends to occur a few cycles into induction or maintenance therapy.
“In some cases,” Dr Treon advised, “a switch to ofatumumab, a fully human CD20 molecule, overcomes this intolerance.”
Nucleoside analogues, which used to be the mainstay of WM, have a high rate of transformation into a more aggressive lymphoma or acute myeloid leukemia.
Immunomodulatory drugs, particularly thalidomide, cause peripheral neuropathy greater than grade 2 in 60% of patients.
And a greater incidence of peripheral neuropathy is also observed with proteasome inhibitors, particularly bortezomib, in WM patients than in myeloma or mantle cell lymphoma patients.
“So this was at least the impetus for why we needed to develop novel approaches to treating this disease,” Dr Treon said.
MYD88 mutations
With whole-genome sequencing, investigators discovered that mutations in the MYD88 gene were highly prevalent in WM patients.
About 93% to 95% of WM patients have the L265P MYD88 mutation, and about 2% have the non-L265P MYD88 mutation.
MYD88 has prognostic significance in WM. Mutated MYD88 confers a better prognosis than unmutated MYD88.
MYD88 may also be important in predicting who will respond to drugs like ibrutinib.
CXCR4 mutations
Mutations in CXCR4 are the second most common mutation in WM.
Between 30% and 40% of WM patients have the WHIM-like CXCR4 C-tail mutations, which traffic the Waldenström’s cells to the bone marrow.
This mutation promotes drug resistance, including resistance to ibrutinib because of the enhanced AKT/ERK signaling.
Ibrutinib therapy
With this in mind, investigators set out to evaluate the potential of using a BTK inhibitor in relapsed/refractory WM patients and at the same time observe the genomics that might predict for response and resistance.
They enrolled 63 patients in the multicenter study. Patients had a median of 2 prior therapies (range, 1–9), and 60% had bone marrow involvement.
Patients received single-agent ibrutinib at a dose of 420 mg orally each day until disease progression or the development of unacceptable toxic side effects.
“By the time they came back 4 weeks later to be evaluated, many of them were already in a response,” Dr Treon said. “And what we saw, in fact, was almost immediate improvement in hemoglobin, something that we didn’t see with many of our trials before that.”
The best IgM response reduced levels from 3520 to 880 mg/dL (P<0.001) for the entire cohort.
The best hemoglobin response increased hemoglobin levels 3 points, from 10.5 to 13.8 g/dL (P<0.001).
The progression-free survival at 2 years was 69% and overall survival was 95%.
At 37 months, most patients who achieve a response experience a durable, ongoing response, according to an update presented at the IX International Workshop on Waldenstrom’s Macroglobulinemia.
And toxicities were “very much in line with what our colleagues have seen in other disease groups,” Dr Treon stated.
Response to ibrutinib by mutation status
The overall response rate was 90% for all patients, but there were differences according to mutation status.
Patients with no MYD88 mutation and no CXCR4 mutation had absolutely no major response.
Patients with a MYD88 mutation responded at an overall rate of 100% and had a major response rate of 91.7% if they did not have a CXCR4 mutation as well.
If they also had a CXCR4WHIM mutation, the overall response rate was lower, at 85.7%, and the major response rate was 61.9%.
“It’s still something to be incredibly excited about—61.9% single-agent activity,” Dr Treon said.
Patients with a CXCR4 mutation also respond more slowly than those without the mutation.
This investigator-sponsored study led to the approval of ibrutinib in WM in the US as well as in Europe and Canada.
“And the point to make about this is that investigators can bring their data to the FDA, the EMA, even Canada, and it can make a difference,” Dr Treon said.
“We don’t always have to have company-sponsored registration studies to be able to make these kinds of advances.”
Ibrutinib in rituximab-refractory patients
A multicenter, phase 3 study of ibrutinib in rituximab-refractory patients was “almost a photocopy of our study,” Dr Treon said.
The main difference was that the patients were even sicker, having failed a median of 4 prior therapies.
Patients experienced rapid improvements in hemoglobin and IgM levels and had an overall response rate of 90%.
Patients with a CXCR4 mutation also tended to lag in terms of pace of hemoglobin improvement and reduction in IgM.
The study was just accepted for publication in Lancet Oncology.
IRAK inhibition
Investigators were puzzled by the paucity of complete responses with ibrutinib, and they found the IRAK pathway remained turned on in patients treated with ibrutinib.
So they took cells of patients treated for 6 months with ibrutinib and co-cultured them with ibrutinib and an IRAK inhibitor. They observed the induction of apoptosis.
Based on this finding, the investigators are manufacturing a very potent IRAK1 inhibitor (JH-X-119), which, when combined with ibrutinib, synergistically increases tumor-cell killing.
“And so one of the strategies we have going forward,” Dr Treon said, “is the ability to advance ibrutinib therapy in MYD88-mutated tumors by the addition of the IRAK inhibitor.”
Resistance to ibrutinib
Investigators have found multiple mutations in the C481 site in individual WM patients, which is where ibrutinib binds.
These mutations represent a minority of the clone, but they exert almost a fully clonal signature. The few patients with these mutations also have a CXCR4 mutation.
C481 mutations shift the signaling of cells in the presence of ibrutinib toward ERK, which is a very powerful survival pathway.
So investigators are examining whether an ERK inhibitor combined with ibrutinib can elicit synergistic killing of BTK-resistant cells.
Investigators have also been synthesizing potent HCK inhibitors, which might overcome BTK mutations by shutting down the ability to activate Bruton’s tyrosine kinase.
Other drugs being developed for WM include:
- Combinations with a proteasome inhibitor, such as ixazomib, dexamethasone, and rituximab
- Agents that target MYD88 signaling, such as the BTK inhibitors acalabrutinib and BGB-3111
- Agents that block CXCR4 receptor signaling, such as ulocuplomab
- The BCL2 inhibitor venetoclax
- The CD38-targeted agent daratumumab.
Current treatment strategies
Knowing a patient’s MYD88 and CXCR4 mutation status provides an opportunity to take a rational approach to treating individuals with WM, Dr Treon said.
For patients with mutated MYD88 and no CXCR4 mutation:
- If patients do not have bulky disease or contraindications, ibrutinib may be used if available.
- If patients have bulky disease, a combination of bendamustine and rituximab may be used.
- If patients have amyloidosis, a combination of bortezomib, dexamethasone, and rituximab is possible.
- If patients have IgM peripheral neuropathy, then rituximab with or without an alkylator is recommended.
For patients with mutated MYD88 and mutated CXCR4, the same treatments can be used as for patients with mutated MYD88 and unmutated CXCR4 with the same restrictions.
To achieve an immediate response for patients with a CXCR4 mutation, an alternative therapy to ibrutinib—such as the bendamustine, dexamethasone, rituximab combination—may be the best choice, because CXCR4-mutated individuals have a slower response to ibrutinib.
The problem arises with the MYD88-wild-type patients, because their survival is poorer than the MYD88-mutated patients.
“We still don’t know what’s wrong with these individuals,” Dr Treon said. “We don’t have any idea about what their basic genomic problems are.”
Bendamustine- or bortezomib-based therapy is effective in this population and can be considered.
In terms of salvage therapy, “the only thing to keep in mind is that if something worked the first time and you got at least a 2-year response with it, you can go back and consider it,” Dr Treon said.

Photo courtesy of DFCI
NEW YORK—Whole-genome sequencing has changed the entire approach to drug development for Waldenström’s macroglobulinemia (WM), according to a speaker at Lymphoma & Myeloma 2016.
The strategy has changed from a hand-me-down one, relying on drugs developed first for other diseases, to a rational plan designed specifically to treat WM patients.
“We would wait for our colleagues in the myeloma world or lymphoma world, CLL world, anywhere we could find them, to help us with the development of drugs,” said Steven Treon, MD, PhD, of the Dana-Farber Cancer Institute in Boston, Massachusetts.
“And, sometimes, this resulted in delays of many, many years before those therapeutics could be vetted out and eventually be handed down to the Waldenström investigators.”
At Lymphoma & Myeloma 2016, Dr Treon described the current therapy of WM and the impact of the discovery of MYD88 and CXCR4 on drug development and treatment choices in WM.
Rituximab-based therapy
WM is a disease that strongly expresses CD20, even though it’s a lymphoplasmacytic disease. So rituximab, given alone and in combination, has been, to date, the most common approach to treating WM.
As a single agent, rituximab produces a response in 25% to 40% of WM patients, but these are very seldom deep responses, Dr Treon noted.
So investigators combined rituximab with cyclophosphamide, nucleoside analogues, proteasome inhibitors, and bendamustine, which increased the overall response rate and depth of response.
This translated into improvement in time to progression, which is now 4 to 5 years with these combination therapies.
“Now, the problem is, when you borrow things from other people, you sometimes end up with problems you didn’t anticipate,” Dr Treon said.
One of the unanticipated side effects with rituximab in WM patients is the IgM flare, which occurs in 40% to 60% of WM patients.
Rituximab can also cause hypogammaglobulinema, leading to infections, and results in a high intolerance rate, which tends to occur a few cycles into induction or maintenance therapy.
“In some cases,” Dr Treon advised, “a switch to ofatumumab, a fully human CD20 molecule, overcomes this intolerance.”
Nucleoside analogues, which used to be the mainstay of WM, have a high rate of transformation into a more aggressive lymphoma or acute myeloid leukemia.
Immunomodulatory drugs, particularly thalidomide, cause peripheral neuropathy greater than grade 2 in 60% of patients.
And a greater incidence of peripheral neuropathy is also observed with proteasome inhibitors, particularly bortezomib, in WM patients than in myeloma or mantle cell lymphoma patients.
“So this was at least the impetus for why we needed to develop novel approaches to treating this disease,” Dr Treon said.
MYD88 mutations
With whole-genome sequencing, investigators discovered that mutations in the MYD88 gene were highly prevalent in WM patients.
About 93% to 95% of WM patients have the L265P MYD88 mutation, and about 2% have the non-L265P MYD88 mutation.
MYD88 has prognostic significance in WM. Mutated MYD88 confers a better prognosis than unmutated MYD88.
MYD88 may also be important in predicting who will respond to drugs like ibrutinib.
CXCR4 mutations
Mutations in CXCR4 are the second most common mutation in WM.
Between 30% and 40% of WM patients have the WHIM-like CXCR4 C-tail mutations, which traffic the Waldenström’s cells to the bone marrow.
This mutation promotes drug resistance, including resistance to ibrutinib because of the enhanced AKT/ERK signaling.
Ibrutinib therapy
With this in mind, investigators set out to evaluate the potential of using a BTK inhibitor in relapsed/refractory WM patients and at the same time observe the genomics that might predict for response and resistance.
They enrolled 63 patients in the multicenter study. Patients had a median of 2 prior therapies (range, 1–9), and 60% had bone marrow involvement.
Patients received single-agent ibrutinib at a dose of 420 mg orally each day until disease progression or the development of unacceptable toxic side effects.
“By the time they came back 4 weeks later to be evaluated, many of them were already in a response,” Dr Treon said. “And what we saw, in fact, was almost immediate improvement in hemoglobin, something that we didn’t see with many of our trials before that.”
The best IgM response reduced levels from 3520 to 880 mg/dL (P<0.001) for the entire cohort.
The best hemoglobin response increased hemoglobin levels 3 points, from 10.5 to 13.8 g/dL (P<0.001).
The progression-free survival at 2 years was 69% and overall survival was 95%.
At 37 months, most patients who achieve a response experience a durable, ongoing response, according to an update presented at the IX International Workshop on Waldenstrom’s Macroglobulinemia.
And toxicities were “very much in line with what our colleagues have seen in other disease groups,” Dr Treon stated.
Response to ibrutinib by mutation status
The overall response rate was 90% for all patients, but there were differences according to mutation status.
Patients with no MYD88 mutation and no CXCR4 mutation had absolutely no major response.
Patients with a MYD88 mutation responded at an overall rate of 100% and had a major response rate of 91.7% if they did not have a CXCR4 mutation as well.
If they also had a CXCR4WHIM mutation, the overall response rate was lower, at 85.7%, and the major response rate was 61.9%.
“It’s still something to be incredibly excited about—61.9% single-agent activity,” Dr Treon said.
Patients with a CXCR4 mutation also respond more slowly than those without the mutation.
This investigator-sponsored study led to the approval of ibrutinib in WM in the US as well as in Europe and Canada.
“And the point to make about this is that investigators can bring their data to the FDA, the EMA, even Canada, and it can make a difference,” Dr Treon said.
“We don’t always have to have company-sponsored registration studies to be able to make these kinds of advances.”
Ibrutinib in rituximab-refractory patients
A multicenter, phase 3 study of ibrutinib in rituximab-refractory patients was “almost a photocopy of our study,” Dr Treon said.
The main difference was that the patients were even sicker, having failed a median of 4 prior therapies.
Patients experienced rapid improvements in hemoglobin and IgM levels and had an overall response rate of 90%.
Patients with a CXCR4 mutation also tended to lag in terms of pace of hemoglobin improvement and reduction in IgM.
The study was just accepted for publication in Lancet Oncology.
IRAK inhibition
Investigators were puzzled by the paucity of complete responses with ibrutinib, and they found the IRAK pathway remained turned on in patients treated with ibrutinib.
So they took cells of patients treated for 6 months with ibrutinib and co-cultured them with ibrutinib and an IRAK inhibitor. They observed the induction of apoptosis.
Based on this finding, the investigators are manufacturing a very potent IRAK1 inhibitor (JH-X-119), which, when combined with ibrutinib, synergistically increases tumor-cell killing.
“And so one of the strategies we have going forward,” Dr Treon said, “is the ability to advance ibrutinib therapy in MYD88-mutated tumors by the addition of the IRAK inhibitor.”
Resistance to ibrutinib
Investigators have found multiple mutations in the C481 site in individual WM patients, which is where ibrutinib binds.
These mutations represent a minority of the clone, but they exert almost a fully clonal signature. The few patients with these mutations also have a CXCR4 mutation.
C481 mutations shift the signaling of cells in the presence of ibrutinib toward ERK, which is a very powerful survival pathway.
So investigators are examining whether an ERK inhibitor combined with ibrutinib can elicit synergistic killing of BTK-resistant cells.
Investigators have also been synthesizing potent HCK inhibitors, which might overcome BTK mutations by shutting down the ability to activate Bruton’s tyrosine kinase.
Other drugs being developed for WM include:
- Combinations with a proteasome inhibitor, such as ixazomib, dexamethasone, and rituximab
- Agents that target MYD88 signaling, such as the BTK inhibitors acalabrutinib and BGB-3111
- Agents that block CXCR4 receptor signaling, such as ulocuplomab
- The BCL2 inhibitor venetoclax
- The CD38-targeted agent daratumumab.
Current treatment strategies
Knowing a patient’s MYD88 and CXCR4 mutation status provides an opportunity to take a rational approach to treating individuals with WM, Dr Treon said.
For patients with mutated MYD88 and no CXCR4 mutation:
- If patients do not have bulky disease or contraindications, ibrutinib may be used if available.
- If patients have bulky disease, a combination of bendamustine and rituximab may be used.
- If patients have amyloidosis, a combination of bortezomib, dexamethasone, and rituximab is possible.
- If patients have IgM peripheral neuropathy, then rituximab with or without an alkylator is recommended.
For patients with mutated MYD88 and mutated CXCR4, the same treatments can be used as for patients with mutated MYD88 and unmutated CXCR4 with the same restrictions.
To achieve an immediate response for patients with a CXCR4 mutation, an alternative therapy to ibrutinib—such as the bendamustine, dexamethasone, rituximab combination—may be the best choice, because CXCR4-mutated individuals have a slower response to ibrutinib.
The problem arises with the MYD88-wild-type patients, because their survival is poorer than the MYD88-mutated patients.
“We still don’t know what’s wrong with these individuals,” Dr Treon said. “We don’t have any idea about what their basic genomic problems are.”
Bendamustine- or bortezomib-based therapy is effective in this population and can be considered.
In terms of salvage therapy, “the only thing to keep in mind is that if something worked the first time and you got at least a 2-year response with it, you can go back and consider it,” Dr Treon said.