User login
Ublituximab was safe, highly active in rituximab-pretreated B-cell NHL, CLL
The investigational anti-CD20 monoclonal antibody ublituximab is safe and has good antitumor activity in patients with B-cell non-Hodgkin lymphoma (B-NHL) or chronic lymphocytic leukemia (CLL) who have previously received the anti-CD20 antibody rituximab, results from a phase I/II trial suggest.
Ublituximab is engineered to have a low fucose content. This feature gives it enhanced antibody-dependent cellular cytotoxicity relative to other anti-CD20 antibodies, especially against tumors having low expression of that protein, as may occur in the development of rituximab resistance.
In the trial, nearly half of the 35 patients studied had a complete or partial response to ublituximab, including nearly one-third of those whose disease was refractory to rituximab (Rituxan) (Br J Haematol. 2017 Apr;177[2]:243-53). The main adverse events were infusion-related reactions, fatigue, pyrexia, and diarrhea, but almost all were lower grade.
“Ublituximab was well tolerated and efficacious in a heterogeneous and highly rituximab–pretreated patient population,” said the investigators, who were led by Ahmed Sawas, MD, at the Center for Lymphoid Malignancies, Columbia University Medical Center, N.Y.
The observed response rate is much the same as those seen with two other anti-CD20 antibodies – obinutuzumab (Gazyva)and ofatumumab (Arzerra)– in similar patient populations, and ublituximab may have advantages in terms of fewer higher-grade infusion-related reactions and shorter infusion time.
“Enhanced anti-CD20 [monoclonal antibodies] that are well tolerated and active in rituximab-resistant disease can provide meaningful clinical benefit to patients with limited treatment options,” the investigators noted.
The trial enrolled 27 patients with B-NHL and 8 patients with CLL (or small lymphocytic lymphoma) who had rituximab-refractory disease (defined by progression on or within 6 months of receiving that agent) or rituximab-relapsed disease (defined by progression more than 6 months after receiving it). They had received a median of three prior therapies.
The patients were treated on an open-label basis with ublituximab at various doses as induction therapy (3-4 weekly infusions during cycles 1 and 2) and then as maintenance therapy (monthly during cycles 3-5, then once every 3 months for up to 2 years). All patients received an oral antihistamine and steroids before infusions.
By the end of the trial, 60% of patients had discontinued treatment because of progression; 23% had discontinued because of adverse events, physician decision, or other reasons; and the remaining 17% had received all planned treatment, Dr. Sawas and his coinvestigators reported.
None of the patients experienced dose-limiting toxicities or unexpected adverse events. The rate of any-grade adverse events was 100%, and the rate specifically of grade 3/4 adverse events was 49%. The rate of serious adverse events (most commonly pneumonia) was 37%.
The leading nonhematologic adverse events were infusion-related reactions (40%; grade 3/4, 0%), fatigue (37%; grade 3/4, 3%), pyrexia (29%; grade 3/4, 0%), and diarrhea (26%; grade 3/4, 0%).
The leading hematologic adverse events were neutropenia (14%; grade 3/4, 14%), with no associated infections; anemia (11%; grade 3/4, 6%); and thrombocytopenia (6%; grade 3/4, 6%), with no associated bleeding.
The overall response rate was 45% (44% in the B-NHL cohort and 50% in the CLL cohort); the majority of responses were partial responses. Notably, the rate was 31% among the subset of patients who had rituximab-refractory disease.
The median duration of response to ublituximab was 9.2 months, and the median progression-free survival was 7.7 months.
“Anti-CD20 therapy has demonstrated the greatest benefit in combination, traditionally with multidrug chemotherapy–based regimens,” the investigators noted. “While the introduction of novel targeted therapies has shifted the treatment paradigm of CLL and indolent lymphoma, the activity of these agents is likely to be potentiated by the addition of an anti-CD20 [monoclonal antibody], given their different mechanisms of action.”
In fact, several multidrug, non–chemotherapy-based regimens are showing promising efficacy and milder toxicity in early trials, they pointed out. “In similar fashion, ublituximab is being evaluated for the treatment of NHL or CLL in combination with other agents,” such as the immunomodulator lenalidomide (Revlimid) and the Bruton tyrosine kinase inhibitor ibrutinib (Imbruvica).
TG Therapeutics funded the trial. Dr. Sawas disclosed that he receives research funds from TG Therapeutics.
The investigational anti-CD20 monoclonal antibody ublituximab is safe and has good antitumor activity in patients with B-cell non-Hodgkin lymphoma (B-NHL) or chronic lymphocytic leukemia (CLL) who have previously received the anti-CD20 antibody rituximab, results from a phase I/II trial suggest.
Ublituximab is engineered to have a low fucose content. This feature gives it enhanced antibody-dependent cellular cytotoxicity relative to other anti-CD20 antibodies, especially against tumors having low expression of that protein, as may occur in the development of rituximab resistance.
In the trial, nearly half of the 35 patients studied had a complete or partial response to ublituximab, including nearly one-third of those whose disease was refractory to rituximab (Rituxan) (Br J Haematol. 2017 Apr;177[2]:243-53). The main adverse events were infusion-related reactions, fatigue, pyrexia, and diarrhea, but almost all were lower grade.
“Ublituximab was well tolerated and efficacious in a heterogeneous and highly rituximab–pretreated patient population,” said the investigators, who were led by Ahmed Sawas, MD, at the Center for Lymphoid Malignancies, Columbia University Medical Center, N.Y.
The observed response rate is much the same as those seen with two other anti-CD20 antibodies – obinutuzumab (Gazyva)and ofatumumab (Arzerra)– in similar patient populations, and ublituximab may have advantages in terms of fewer higher-grade infusion-related reactions and shorter infusion time.
“Enhanced anti-CD20 [monoclonal antibodies] that are well tolerated and active in rituximab-resistant disease can provide meaningful clinical benefit to patients with limited treatment options,” the investigators noted.
The trial enrolled 27 patients with B-NHL and 8 patients with CLL (or small lymphocytic lymphoma) who had rituximab-refractory disease (defined by progression on or within 6 months of receiving that agent) or rituximab-relapsed disease (defined by progression more than 6 months after receiving it). They had received a median of three prior therapies.
The patients were treated on an open-label basis with ublituximab at various doses as induction therapy (3-4 weekly infusions during cycles 1 and 2) and then as maintenance therapy (monthly during cycles 3-5, then once every 3 months for up to 2 years). All patients received an oral antihistamine and steroids before infusions.
By the end of the trial, 60% of patients had discontinued treatment because of progression; 23% had discontinued because of adverse events, physician decision, or other reasons; and the remaining 17% had received all planned treatment, Dr. Sawas and his coinvestigators reported.
None of the patients experienced dose-limiting toxicities or unexpected adverse events. The rate of any-grade adverse events was 100%, and the rate specifically of grade 3/4 adverse events was 49%. The rate of serious adverse events (most commonly pneumonia) was 37%.
The leading nonhematologic adverse events were infusion-related reactions (40%; grade 3/4, 0%), fatigue (37%; grade 3/4, 3%), pyrexia (29%; grade 3/4, 0%), and diarrhea (26%; grade 3/4, 0%).
The leading hematologic adverse events were neutropenia (14%; grade 3/4, 14%), with no associated infections; anemia (11%; grade 3/4, 6%); and thrombocytopenia (6%; grade 3/4, 6%), with no associated bleeding.
The overall response rate was 45% (44% in the B-NHL cohort and 50% in the CLL cohort); the majority of responses were partial responses. Notably, the rate was 31% among the subset of patients who had rituximab-refractory disease.
The median duration of response to ublituximab was 9.2 months, and the median progression-free survival was 7.7 months.
“Anti-CD20 therapy has demonstrated the greatest benefit in combination, traditionally with multidrug chemotherapy–based regimens,” the investigators noted. “While the introduction of novel targeted therapies has shifted the treatment paradigm of CLL and indolent lymphoma, the activity of these agents is likely to be potentiated by the addition of an anti-CD20 [monoclonal antibody], given their different mechanisms of action.”
In fact, several multidrug, non–chemotherapy-based regimens are showing promising efficacy and milder toxicity in early trials, they pointed out. “In similar fashion, ublituximab is being evaluated for the treatment of NHL or CLL in combination with other agents,” such as the immunomodulator lenalidomide (Revlimid) and the Bruton tyrosine kinase inhibitor ibrutinib (Imbruvica).
TG Therapeutics funded the trial. Dr. Sawas disclosed that he receives research funds from TG Therapeutics.
The investigational anti-CD20 monoclonal antibody ublituximab is safe and has good antitumor activity in patients with B-cell non-Hodgkin lymphoma (B-NHL) or chronic lymphocytic leukemia (CLL) who have previously received the anti-CD20 antibody rituximab, results from a phase I/II trial suggest.
Ublituximab is engineered to have a low fucose content. This feature gives it enhanced antibody-dependent cellular cytotoxicity relative to other anti-CD20 antibodies, especially against tumors having low expression of that protein, as may occur in the development of rituximab resistance.
In the trial, nearly half of the 35 patients studied had a complete or partial response to ublituximab, including nearly one-third of those whose disease was refractory to rituximab (Rituxan) (Br J Haematol. 2017 Apr;177[2]:243-53). The main adverse events were infusion-related reactions, fatigue, pyrexia, and diarrhea, but almost all were lower grade.
“Ublituximab was well tolerated and efficacious in a heterogeneous and highly rituximab–pretreated patient population,” said the investigators, who were led by Ahmed Sawas, MD, at the Center for Lymphoid Malignancies, Columbia University Medical Center, N.Y.
The observed response rate is much the same as those seen with two other anti-CD20 antibodies – obinutuzumab (Gazyva)and ofatumumab (Arzerra)– in similar patient populations, and ublituximab may have advantages in terms of fewer higher-grade infusion-related reactions and shorter infusion time.
“Enhanced anti-CD20 [monoclonal antibodies] that are well tolerated and active in rituximab-resistant disease can provide meaningful clinical benefit to patients with limited treatment options,” the investigators noted.
The trial enrolled 27 patients with B-NHL and 8 patients with CLL (or small lymphocytic lymphoma) who had rituximab-refractory disease (defined by progression on or within 6 months of receiving that agent) or rituximab-relapsed disease (defined by progression more than 6 months after receiving it). They had received a median of three prior therapies.
The patients were treated on an open-label basis with ublituximab at various doses as induction therapy (3-4 weekly infusions during cycles 1 and 2) and then as maintenance therapy (monthly during cycles 3-5, then once every 3 months for up to 2 years). All patients received an oral antihistamine and steroids before infusions.
By the end of the trial, 60% of patients had discontinued treatment because of progression; 23% had discontinued because of adverse events, physician decision, or other reasons; and the remaining 17% had received all planned treatment, Dr. Sawas and his coinvestigators reported.
None of the patients experienced dose-limiting toxicities or unexpected adverse events. The rate of any-grade adverse events was 100%, and the rate specifically of grade 3/4 adverse events was 49%. The rate of serious adverse events (most commonly pneumonia) was 37%.
The leading nonhematologic adverse events were infusion-related reactions (40%; grade 3/4, 0%), fatigue (37%; grade 3/4, 3%), pyrexia (29%; grade 3/4, 0%), and diarrhea (26%; grade 3/4, 0%).
The leading hematologic adverse events were neutropenia (14%; grade 3/4, 14%), with no associated infections; anemia (11%; grade 3/4, 6%); and thrombocytopenia (6%; grade 3/4, 6%), with no associated bleeding.
The overall response rate was 45% (44% in the B-NHL cohort and 50% in the CLL cohort); the majority of responses were partial responses. Notably, the rate was 31% among the subset of patients who had rituximab-refractory disease.
The median duration of response to ublituximab was 9.2 months, and the median progression-free survival was 7.7 months.
“Anti-CD20 therapy has demonstrated the greatest benefit in combination, traditionally with multidrug chemotherapy–based regimens,” the investigators noted. “While the introduction of novel targeted therapies has shifted the treatment paradigm of CLL and indolent lymphoma, the activity of these agents is likely to be potentiated by the addition of an anti-CD20 [monoclonal antibody], given their different mechanisms of action.”
In fact, several multidrug, non–chemotherapy-based regimens are showing promising efficacy and milder toxicity in early trials, they pointed out. “In similar fashion, ublituximab is being evaluated for the treatment of NHL or CLL in combination with other agents,” such as the immunomodulator lenalidomide (Revlimid) and the Bruton tyrosine kinase inhibitor ibrutinib (Imbruvica).
TG Therapeutics funded the trial. Dr. Sawas disclosed that he receives research funds from TG Therapeutics.
Key clinical point:
Major finding: The overall response rate was 45%. There were no dose-limiting toxicities; main adverse events of any grade were infusion-related reactions (40%), fatigue (37%), pyrexia (29%), and diarrhea (26%).
Data source: A phase I/II trial among 35 patients with B-NHL or CLL who had previously received rituximab.
Disclosures: TG Therapeutics funded the trial. Dr. Sawas disclosed that he receives research funds from TG Therapeutics.
Walking can benefit advanced cancer patients
Walking for 30 minutes 3 times a week can improve quality of life for patients with advanced cancer, according to research published in BMJ Open.
The study indicated that some patients with advanced cancer may not be able to commit to weekly walks with a group of fellow patients.
However, some patients enjoyed walking in groups, and most reported benefits from regular walks, whether taken alone or with others.
“Findings from this important study show that exercise is valued by, suitable for, and beneficial to people with advanced cancer,” said study author Emma Ream, RN, PhD, of the University of Surrey in the UK.
“Rather than shying away from exercise, people with advanced disease should be encouraged to be more active and incorporate exercise into their daily lives where possible.”
One hundred and ten patients with advanced cancer were eligible to participate in this study, but 49 (47%) declined, primarily because of work commitments. Patients said they could not commit to a weekly walking group.
The 42 patients who did participate in this study were divided into 2 groups.
Group 1 (n=21) received coaching, which included a short motivational interview, as well as the recommendation to walk for at least 30 minutes on alternate days and attend a volunteer-led group walk weekly.
Patients in group 2 (n=21) were encouraged to maintain their current level of activity.
Nineteen participants (45%) withdrew from the study—11 in group 1 and 8 in group 2. In general, patients did not provide reasons for withdrawal. However, 2 patients were too unwell to participate, and 2 patients died during the study.
At 6, 12, and 24 weeks, scores on quality of life questionnaires were not significantly different between groups 1 and 2.
However, in interviews, patients in group 1 said they felt walking provided physical, emotional, and psychological benefits, as well as improvements in social well-being and lifestyle.
At 24 weeks, 8 of 9 participants in group 1 said they found the walking intervention useful, and 7 participants said they were satisfied with it.
Some patients said walking improved their attitude toward their illness and spoke of the social benefits of participating in group walks.
But other patients were dissatisfied with the walking groups. They reported accessibility issues and a dislike of group activities. One younger individual felt the group was more appropriate for older patients.
“This study is a first step towards exploring how walking can help people living with advanced cancer,” said study author Jo Armes, RGN, PhD, of King’s College London in the UK.
“Walking is a free and accessible form of physical activity, and patients reported that it made a real difference to their quality of life. Further research is needed with a larger number of people to provide definitive evidence that walking improves both health outcomes and social and emotional wellbeing in this group of people.” ![]()
Walking for 30 minutes 3 times a week can improve quality of life for patients with advanced cancer, according to research published in BMJ Open.
The study indicated that some patients with advanced cancer may not be able to commit to weekly walks with a group of fellow patients.
However, some patients enjoyed walking in groups, and most reported benefits from regular walks, whether taken alone or with others.
“Findings from this important study show that exercise is valued by, suitable for, and beneficial to people with advanced cancer,” said study author Emma Ream, RN, PhD, of the University of Surrey in the UK.
“Rather than shying away from exercise, people with advanced disease should be encouraged to be more active and incorporate exercise into their daily lives where possible.”
One hundred and ten patients with advanced cancer were eligible to participate in this study, but 49 (47%) declined, primarily because of work commitments. Patients said they could not commit to a weekly walking group.
The 42 patients who did participate in this study were divided into 2 groups.
Group 1 (n=21) received coaching, which included a short motivational interview, as well as the recommendation to walk for at least 30 minutes on alternate days and attend a volunteer-led group walk weekly.
Patients in group 2 (n=21) were encouraged to maintain their current level of activity.
Nineteen participants (45%) withdrew from the study—11 in group 1 and 8 in group 2. In general, patients did not provide reasons for withdrawal. However, 2 patients were too unwell to participate, and 2 patients died during the study.
At 6, 12, and 24 weeks, scores on quality of life questionnaires were not significantly different between groups 1 and 2.
However, in interviews, patients in group 1 said they felt walking provided physical, emotional, and psychological benefits, as well as improvements in social well-being and lifestyle.
At 24 weeks, 8 of 9 participants in group 1 said they found the walking intervention useful, and 7 participants said they were satisfied with it.
Some patients said walking improved their attitude toward their illness and spoke of the social benefits of participating in group walks.
But other patients were dissatisfied with the walking groups. They reported accessibility issues and a dislike of group activities. One younger individual felt the group was more appropriate for older patients.
“This study is a first step towards exploring how walking can help people living with advanced cancer,” said study author Jo Armes, RGN, PhD, of King’s College London in the UK.
“Walking is a free and accessible form of physical activity, and patients reported that it made a real difference to their quality of life. Further research is needed with a larger number of people to provide definitive evidence that walking improves both health outcomes and social and emotional wellbeing in this group of people.” ![]()
Walking for 30 minutes 3 times a week can improve quality of life for patients with advanced cancer, according to research published in BMJ Open.
The study indicated that some patients with advanced cancer may not be able to commit to weekly walks with a group of fellow patients.
However, some patients enjoyed walking in groups, and most reported benefits from regular walks, whether taken alone or with others.
“Findings from this important study show that exercise is valued by, suitable for, and beneficial to people with advanced cancer,” said study author Emma Ream, RN, PhD, of the University of Surrey in the UK.
“Rather than shying away from exercise, people with advanced disease should be encouraged to be more active and incorporate exercise into their daily lives where possible.”
One hundred and ten patients with advanced cancer were eligible to participate in this study, but 49 (47%) declined, primarily because of work commitments. Patients said they could not commit to a weekly walking group.
The 42 patients who did participate in this study were divided into 2 groups.
Group 1 (n=21) received coaching, which included a short motivational interview, as well as the recommendation to walk for at least 30 minutes on alternate days and attend a volunteer-led group walk weekly.
Patients in group 2 (n=21) were encouraged to maintain their current level of activity.
Nineteen participants (45%) withdrew from the study—11 in group 1 and 8 in group 2. In general, patients did not provide reasons for withdrawal. However, 2 patients were too unwell to participate, and 2 patients died during the study.
At 6, 12, and 24 weeks, scores on quality of life questionnaires were not significantly different between groups 1 and 2.
However, in interviews, patients in group 1 said they felt walking provided physical, emotional, and psychological benefits, as well as improvements in social well-being and lifestyle.
At 24 weeks, 8 of 9 participants in group 1 said they found the walking intervention useful, and 7 participants said they were satisfied with it.
Some patients said walking improved their attitude toward their illness and spoke of the social benefits of participating in group walks.
But other patients were dissatisfied with the walking groups. They reported accessibility issues and a dislike of group activities. One younger individual felt the group was more appropriate for older patients.
“This study is a first step towards exploring how walking can help people living with advanced cancer,” said study author Jo Armes, RGN, PhD, of King’s College London in the UK.
“Walking is a free and accessible form of physical activity, and patients reported that it made a real difference to their quality of life. Further research is needed with a larger number of people to provide definitive evidence that walking improves both health outcomes and social and emotional wellbeing in this group of people.” ![]()
Proximity to oil, gas wells linked to ALL

A pumpjack is used to lift
liquid from an oil well.
Photo by Eric Kounce
Living in an area of high-density oil and gas development may increase a young person’s risk of developing acute lymphoblastic leukemia (ALL), according to research published in PLOS ONE.
The study showed that children and young adults in Colorado who had been diagnosed with ALL were more likely than young people with non-hematologic cancers to live in areas of high-density oil and gas development.
However, there was no such association for young people with non-Hodgkin lymphoma (NHL).
“Over 378,000 Coloradans and millions of Americans currently live within a mile of at least one oil and gas well, and petroleum development continues to expand into residential areas,” said study author Lisa McKenzie, PhD, of the University of Colorado Anschutz Campus in Aurora.
“The findings from our registry-based, case-control study indicate that young Coloradans diagnosed with one type of childhood leukemia are more likely to live in the densest areas of oil and gas sites. More comprehensive research that can address our study’s limitations is needed to understand and explain these results.”
Dr McKenzie and her colleagues said they conducted this study because oil and gas development emits known hematological carcinogens, such as benzene, and increasingly occurs in residential areas.
The team wanted to determine whether living near areas of oil and gas development was associated with risk for hematologic cancers. So they analyzed data from the Colorado Central Cancer Registry and the Colorado Oil and Gas Information System.
The study included 743 subjects, ages 0 to 24, living in rural Colorado and diagnosed with cancer between 2001 and 2013. This included 87 ALL cases, 50 NHL cases, and 528 controls with non-hematologic cancers. (Other hematologic malignancies were not included in the analysis due to small numbers.)
Data analysis
The researchers used information from the Colorado Oil and Gas Information System to build a geocoded dataset with coordinates of all oil and gas wells in rural Colorado and determined dates for when each well was active.
Geocoded residential addresses of cancer patients at the time of diagnosis were linked to active well locations in the year of diagnosis and active well locations in each of the 10 years preceding the cancer diagnosis.
The researchers then took the inverse of each distance and summed the inverse distances to calculate inverse distance weighted (IDW) oil and gas well counts within a 16.1 km radius of each participant’s residence at cancer diagnosis for each of the 10 years prior to the date of diagnosis. (The IDW well count method gives greater weight to the wells nearer the home.)
The team used logistic regression to estimate associations for cancers across IDW well count tertiles. The first tertile had less than 4.9 wells per 1.6 km, the second had 4.9 to 33.6 wells per 1.6 km, and the third had more than 33.6 wells per 1.6 km.
Results
The researchers found an increase in the odds of living near oil and gas development at the time of ALL diagnosis, even after adjusting for age, race, gender, income, elevation, and year of cancer diagnosis.
ALL patients ages 0 to 24 were twice as likely as controls to live in the densest area of active oil and gas wells (highest IDW well count tertile).
ALL patients ages 5 to 24 were 4.6 times more likely than controls to live in areas included in the highest IDW well count tertile.
However, there was no significant association between ALL and proximity to oil and gas development in ALL patients ages 0 to 4. The adjusted odds ratio was 0.51 for the highest IDW well count tertile.
Likewise, there were no significant associations between density of oil and gas development and NHL. The adjusted odds ratio was 0.99 for the highest IDW well count tertile.
Limitations and next steps
The researchers said this study was limited by the low occurrence of ALL and NHL in rural Colorado, lack of specific age at cancer diagnosis, and the fact that all study participants had been diagnosed with cancer.
In addition, the study was limited by the lack of information on specific activities at the well sites, place of residence before cancer diagnosis, other sources of pollution around the residence, and individual characteristics such as common infections and family history of cancer.
The team said future research should incorporate information on oil and gas development activities and production levels, as well as levels of specific pollutants of interest such as benzene, near homes, schools, and day care centers.
They recommended that such research consider specific ages and residential histories, compare cases to controls without cancer, and address other potential confounders and and environmental stressors. ![]()

A pumpjack is used to lift
liquid from an oil well.
Photo by Eric Kounce
Living in an area of high-density oil and gas development may increase a young person’s risk of developing acute lymphoblastic leukemia (ALL), according to research published in PLOS ONE.
The study showed that children and young adults in Colorado who had been diagnosed with ALL were more likely than young people with non-hematologic cancers to live in areas of high-density oil and gas development.
However, there was no such association for young people with non-Hodgkin lymphoma (NHL).
“Over 378,000 Coloradans and millions of Americans currently live within a mile of at least one oil and gas well, and petroleum development continues to expand into residential areas,” said study author Lisa McKenzie, PhD, of the University of Colorado Anschutz Campus in Aurora.
“The findings from our registry-based, case-control study indicate that young Coloradans diagnosed with one type of childhood leukemia are more likely to live in the densest areas of oil and gas sites. More comprehensive research that can address our study’s limitations is needed to understand and explain these results.”
Dr McKenzie and her colleagues said they conducted this study because oil and gas development emits known hematological carcinogens, such as benzene, and increasingly occurs in residential areas.
The team wanted to determine whether living near areas of oil and gas development was associated with risk for hematologic cancers. So they analyzed data from the Colorado Central Cancer Registry and the Colorado Oil and Gas Information System.
The study included 743 subjects, ages 0 to 24, living in rural Colorado and diagnosed with cancer between 2001 and 2013. This included 87 ALL cases, 50 NHL cases, and 528 controls with non-hematologic cancers. (Other hematologic malignancies were not included in the analysis due to small numbers.)
Data analysis
The researchers used information from the Colorado Oil and Gas Information System to build a geocoded dataset with coordinates of all oil and gas wells in rural Colorado and determined dates for when each well was active.
Geocoded residential addresses of cancer patients at the time of diagnosis were linked to active well locations in the year of diagnosis and active well locations in each of the 10 years preceding the cancer diagnosis.
The researchers then took the inverse of each distance and summed the inverse distances to calculate inverse distance weighted (IDW) oil and gas well counts within a 16.1 km radius of each participant’s residence at cancer diagnosis for each of the 10 years prior to the date of diagnosis. (The IDW well count method gives greater weight to the wells nearer the home.)
The team used logistic regression to estimate associations for cancers across IDW well count tertiles. The first tertile had less than 4.9 wells per 1.6 km, the second had 4.9 to 33.6 wells per 1.6 km, and the third had more than 33.6 wells per 1.6 km.
Results
The researchers found an increase in the odds of living near oil and gas development at the time of ALL diagnosis, even after adjusting for age, race, gender, income, elevation, and year of cancer diagnosis.
ALL patients ages 0 to 24 were twice as likely as controls to live in the densest area of active oil and gas wells (highest IDW well count tertile).
ALL patients ages 5 to 24 were 4.6 times more likely than controls to live in areas included in the highest IDW well count tertile.
However, there was no significant association between ALL and proximity to oil and gas development in ALL patients ages 0 to 4. The adjusted odds ratio was 0.51 for the highest IDW well count tertile.
Likewise, there were no significant associations between density of oil and gas development and NHL. The adjusted odds ratio was 0.99 for the highest IDW well count tertile.
Limitations and next steps
The researchers said this study was limited by the low occurrence of ALL and NHL in rural Colorado, lack of specific age at cancer diagnosis, and the fact that all study participants had been diagnosed with cancer.
In addition, the study was limited by the lack of information on specific activities at the well sites, place of residence before cancer diagnosis, other sources of pollution around the residence, and individual characteristics such as common infections and family history of cancer.
The team said future research should incorporate information on oil and gas development activities and production levels, as well as levels of specific pollutants of interest such as benzene, near homes, schools, and day care centers.
They recommended that such research consider specific ages and residential histories, compare cases to controls without cancer, and address other potential confounders and and environmental stressors. ![]()

A pumpjack is used to lift
liquid from an oil well.
Photo by Eric Kounce
Living in an area of high-density oil and gas development may increase a young person’s risk of developing acute lymphoblastic leukemia (ALL), according to research published in PLOS ONE.
The study showed that children and young adults in Colorado who had been diagnosed with ALL were more likely than young people with non-hematologic cancers to live in areas of high-density oil and gas development.
However, there was no such association for young people with non-Hodgkin lymphoma (NHL).
“Over 378,000 Coloradans and millions of Americans currently live within a mile of at least one oil and gas well, and petroleum development continues to expand into residential areas,” said study author Lisa McKenzie, PhD, of the University of Colorado Anschutz Campus in Aurora.
“The findings from our registry-based, case-control study indicate that young Coloradans diagnosed with one type of childhood leukemia are more likely to live in the densest areas of oil and gas sites. More comprehensive research that can address our study’s limitations is needed to understand and explain these results.”
Dr McKenzie and her colleagues said they conducted this study because oil and gas development emits known hematological carcinogens, such as benzene, and increasingly occurs in residential areas.
The team wanted to determine whether living near areas of oil and gas development was associated with risk for hematologic cancers. So they analyzed data from the Colorado Central Cancer Registry and the Colorado Oil and Gas Information System.
The study included 743 subjects, ages 0 to 24, living in rural Colorado and diagnosed with cancer between 2001 and 2013. This included 87 ALL cases, 50 NHL cases, and 528 controls with non-hematologic cancers. (Other hematologic malignancies were not included in the analysis due to small numbers.)
Data analysis
The researchers used information from the Colorado Oil and Gas Information System to build a geocoded dataset with coordinates of all oil and gas wells in rural Colorado and determined dates for when each well was active.
Geocoded residential addresses of cancer patients at the time of diagnosis were linked to active well locations in the year of diagnosis and active well locations in each of the 10 years preceding the cancer diagnosis.
The researchers then took the inverse of each distance and summed the inverse distances to calculate inverse distance weighted (IDW) oil and gas well counts within a 16.1 km radius of each participant’s residence at cancer diagnosis for each of the 10 years prior to the date of diagnosis. (The IDW well count method gives greater weight to the wells nearer the home.)
The team used logistic regression to estimate associations for cancers across IDW well count tertiles. The first tertile had less than 4.9 wells per 1.6 km, the second had 4.9 to 33.6 wells per 1.6 km, and the third had more than 33.6 wells per 1.6 km.
Results
The researchers found an increase in the odds of living near oil and gas development at the time of ALL diagnosis, even after adjusting for age, race, gender, income, elevation, and year of cancer diagnosis.
ALL patients ages 0 to 24 were twice as likely as controls to live in the densest area of active oil and gas wells (highest IDW well count tertile).
ALL patients ages 5 to 24 were 4.6 times more likely than controls to live in areas included in the highest IDW well count tertile.
However, there was no significant association between ALL and proximity to oil and gas development in ALL patients ages 0 to 4. The adjusted odds ratio was 0.51 for the highest IDW well count tertile.
Likewise, there were no significant associations between density of oil and gas development and NHL. The adjusted odds ratio was 0.99 for the highest IDW well count tertile.
Limitations and next steps
The researchers said this study was limited by the low occurrence of ALL and NHL in rural Colorado, lack of specific age at cancer diagnosis, and the fact that all study participants had been diagnosed with cancer.
In addition, the study was limited by the lack of information on specific activities at the well sites, place of residence before cancer diagnosis, other sources of pollution around the residence, and individual characteristics such as common infections and family history of cancer.
The team said future research should incorporate information on oil and gas development activities and production levels, as well as levels of specific pollutants of interest such as benzene, near homes, schools, and day care centers.
They recommended that such research consider specific ages and residential histories, compare cases to controls without cancer, and address other potential confounders and and environmental stressors. ![]()
Styrene exposure linked to myeloid leukemia, HL
A new study links styrene—a chemical used in the manufacture of plastics, rubber, and resins—to certain cancers.
The research showed that, contrary to previous suggestions, employees who have worked with styrene do not have an increased incidence of esophageal, pancreatic, lung, kidney, or bladder cancer.
On the other hand, they may have an increased risk of nasal and paranasal cancer, as well as myeloid leukemia and Hodgkin lymphoma (HL).
The research was published in Epidemiology.
“It is important to know for present and former workers exposed to styrene that they are unlikely to have become ill by doing their job if they have developed cancer of the esophagus, pancreas, lungs, kidneys, bladder, or a wide range of other types of cancer,” said study author Henrik A. Kolstad, MD, PhD, of Aarhus University in Denmark.
“This is also new and important knowledge in the USA, where styrene was added to the list of carcinogenic substances in 2011.”
In relation to the cancers for which the study shows a possible increased risk, Dr Kolstad emphasized that additional research is needed to determine if styrene is the actual cause of the employees’ disease.
For the current study, Dr Kolstad and his colleagues analyzed data on 72,292 employees who worked for 1 of 443 small and medium-sized companies in Denmark that used styrene for the production of wind turbines, pleasure boats, and other products from 1964 to 2007.
There were 8961 incident cases of cancer in this cohort from 1968 to 2012. The standardized incidence rate ratio (SIR) for all cancers was 1.04. When the researchers included a 10-year lag period, the SIR for all cancers was still 1.04.
As for hematologic malignancies, the researchers said they observed increased rate ratios associated with increased duration of employment for HL and myeloid leukemia.
For HL, the SIRs were 1.21 with no lag and 1.22 with a 10-year lag. For myeloid leukemia, the SIRs were 1.06 and 1.13, respectively.
The SIRs for non-Hodgkin lymphoma were 0.97 with no lag and 0.94 with a 10-year lag. The SIRs for multiple myeloma were 0.79 and 0.77, respectively.
For cancers of lymphatic and hematopoietic tissue, the SIRs were 0.97 with no lag and 0.96 with a 10-year lag. For lymphatic leukemia, the SIR was 0.96 for both time points.
The SIRs for monocytic leukemia were 0.77 with no lag and 0.56 with a 10-year lag. The SIRs for other and unspecified leukemias were 1.05 and 1.26, respectively.
The researchers noted that workers first employed in the 1960s had a higher risk of HL than workers first employed in subsequent years.
The SIRs were 2.12 for those first employed in 1964-1969, 0.82 for 1970-1979, 1.07 for 1980-1989, 1.52 for 1990-1999, and 1.10 for those first employed in 2000-2007.
There were no such associations for other cancer sites. ![]()
A new study links styrene—a chemical used in the manufacture of plastics, rubber, and resins—to certain cancers.
The research showed that, contrary to previous suggestions, employees who have worked with styrene do not have an increased incidence of esophageal, pancreatic, lung, kidney, or bladder cancer.
On the other hand, they may have an increased risk of nasal and paranasal cancer, as well as myeloid leukemia and Hodgkin lymphoma (HL).
The research was published in Epidemiology.
“It is important to know for present and former workers exposed to styrene that they are unlikely to have become ill by doing their job if they have developed cancer of the esophagus, pancreas, lungs, kidneys, bladder, or a wide range of other types of cancer,” said study author Henrik A. Kolstad, MD, PhD, of Aarhus University in Denmark.
“This is also new and important knowledge in the USA, where styrene was added to the list of carcinogenic substances in 2011.”
In relation to the cancers for which the study shows a possible increased risk, Dr Kolstad emphasized that additional research is needed to determine if styrene is the actual cause of the employees’ disease.
For the current study, Dr Kolstad and his colleagues analyzed data on 72,292 employees who worked for 1 of 443 small and medium-sized companies in Denmark that used styrene for the production of wind turbines, pleasure boats, and other products from 1964 to 2007.
There were 8961 incident cases of cancer in this cohort from 1968 to 2012. The standardized incidence rate ratio (SIR) for all cancers was 1.04. When the researchers included a 10-year lag period, the SIR for all cancers was still 1.04.
As for hematologic malignancies, the researchers said they observed increased rate ratios associated with increased duration of employment for HL and myeloid leukemia.
For HL, the SIRs were 1.21 with no lag and 1.22 with a 10-year lag. For myeloid leukemia, the SIRs were 1.06 and 1.13, respectively.
The SIRs for non-Hodgkin lymphoma were 0.97 with no lag and 0.94 with a 10-year lag. The SIRs for multiple myeloma were 0.79 and 0.77, respectively.
For cancers of lymphatic and hematopoietic tissue, the SIRs were 0.97 with no lag and 0.96 with a 10-year lag. For lymphatic leukemia, the SIR was 0.96 for both time points.
The SIRs for monocytic leukemia were 0.77 with no lag and 0.56 with a 10-year lag. The SIRs for other and unspecified leukemias were 1.05 and 1.26, respectively.
The researchers noted that workers first employed in the 1960s had a higher risk of HL than workers first employed in subsequent years.
The SIRs were 2.12 for those first employed in 1964-1969, 0.82 for 1970-1979, 1.07 for 1980-1989, 1.52 for 1990-1999, and 1.10 for those first employed in 2000-2007.
There were no such associations for other cancer sites. ![]()
A new study links styrene—a chemical used in the manufacture of plastics, rubber, and resins—to certain cancers.
The research showed that, contrary to previous suggestions, employees who have worked with styrene do not have an increased incidence of esophageal, pancreatic, lung, kidney, or bladder cancer.
On the other hand, they may have an increased risk of nasal and paranasal cancer, as well as myeloid leukemia and Hodgkin lymphoma (HL).
The research was published in Epidemiology.
“It is important to know for present and former workers exposed to styrene that they are unlikely to have become ill by doing their job if they have developed cancer of the esophagus, pancreas, lungs, kidneys, bladder, or a wide range of other types of cancer,” said study author Henrik A. Kolstad, MD, PhD, of Aarhus University in Denmark.
“This is also new and important knowledge in the USA, where styrene was added to the list of carcinogenic substances in 2011.”
In relation to the cancers for which the study shows a possible increased risk, Dr Kolstad emphasized that additional research is needed to determine if styrene is the actual cause of the employees’ disease.
For the current study, Dr Kolstad and his colleagues analyzed data on 72,292 employees who worked for 1 of 443 small and medium-sized companies in Denmark that used styrene for the production of wind turbines, pleasure boats, and other products from 1964 to 2007.
There were 8961 incident cases of cancer in this cohort from 1968 to 2012. The standardized incidence rate ratio (SIR) for all cancers was 1.04. When the researchers included a 10-year lag period, the SIR for all cancers was still 1.04.
As for hematologic malignancies, the researchers said they observed increased rate ratios associated with increased duration of employment for HL and myeloid leukemia.
For HL, the SIRs were 1.21 with no lag and 1.22 with a 10-year lag. For myeloid leukemia, the SIRs were 1.06 and 1.13, respectively.
The SIRs for non-Hodgkin lymphoma were 0.97 with no lag and 0.94 with a 10-year lag. The SIRs for multiple myeloma were 0.79 and 0.77, respectively.
For cancers of lymphatic and hematopoietic tissue, the SIRs were 0.97 with no lag and 0.96 with a 10-year lag. For lymphatic leukemia, the SIR was 0.96 for both time points.
The SIRs for monocytic leukemia were 0.77 with no lag and 0.56 with a 10-year lag. The SIRs for other and unspecified leukemias were 1.05 and 1.26, respectively.
The researchers noted that workers first employed in the 1960s had a higher risk of HL than workers first employed in subsequent years.
The SIRs were 2.12 for those first employed in 1964-1969, 0.82 for 1970-1979, 1.07 for 1980-1989, 1.52 for 1990-1999, and 1.10 for those first employed in 2000-2007.
There were no such associations for other cancer sites. ![]()
Drug produces high response rates in AITL

Photo by Larry Young
SAN FRANCISCO—Treatment with 5-azacitidine (5-AZA) can produce a high response rate in patients with relapsed/refractory angioimmunoblastic T-cell lymphoma (AITL), according to a small study.
The overall response rate (ORR) among AITL patients was 75%, and the complete response (CR) rate was 42%.
However, this study also included patients with other types of peripheral T-cell lymphoma (PTCL), and most of these patients did not respond to 5-AZA.
Richard Delarue, MD, of Necker University Hospital in Paris, France, presented these results at the 9th Annual T-cell Lymphoma Forum.
Results were also presented at the 2016 ASH Annual Meeting (abstract 4164). Dr Delarue reported receiving honoraria from Celgene.
Patients
The study included 19 patients with relapsed/refractory PTCL. Twelve patients had AITL, 3 had adult T-cell leukemia/lymphoma (ATLL), 2 had PTCL not otherwise specified, 1 had enteropathy-associated T-cell lymphoma, and 1 had transformed mycosis fungoides.
At diagnosis, the median age was 71 (range, 39-85) for AITL patients and 59 (range, 32-83) for the other PTCL patients. Seventy-five percent of AITL patients had an IPI score of 3 to 5 and a PIT score of 3 to 4. Eighty-six percent of the other PTCL patients had an IPI score of 3 to 5, and 57% had a PIT score of 3 to 4.
At the time of 5-AZA treatment, all patients had stage III/IV disease. The AITL patients had received a median of 2 (range, 0-6) prior lines of therapy, and the other PTCL patients had received a median of 3 (range, 0-7).
Two patients did not receive chemotherapy before 5-AZA because of the presence of associated chronic myelomonocytic leukemia (CMML) that required treatment first.
Ninety-two percent of AITL patients had TET2 mutations (n=11), 33% had DNMT3A mutations (n=4), and 0% had IDH2 mutations. One of the non-AITL patients had a TET2 mutation.
Treatment
Patients received a subcutaneous injection of 5-AZA at 75 mg/m² for 7 consecutive days every 28 days until progression or unacceptable toxicity. Six patients also received 4 to 8 infusions of rituximab because of EBV-DNA positivity.
The patients received a median of 3 cycles of 5-AZA. At the time of analysis, 4 patients were still receiving therapy.
The median follow-up was 84 days (range, 19 to 1236).
Toxicity
“Hematological toxicity was as expected with 5-azacitidine,” Dr Delarue said.
However, 2 patients had “unusual” adverse reactions. One patient had grade 2 polyneuropathy, which was considered related to a paraneoplastic syndrome.
The other patient had grade 3 diarrhea related to colitis of unknown origin, and this led to treatment interruption.
There were no treatment-related deaths.
Efficacy
Dr Delarue noted that the ORR was significantly higher in AITL patients than in patients with the other PTCL subtypes (P=0.0198).
The ORR was 53% in the entire cohort (10/19), 75% (9/12) among AITL patients, and 14% among patients with other PTCLs (1/7).
“The only patient with a response in the ‘other PTCL’ group was a patient with HTLV1-associated ATLL . . . , but he relapsed a couple of weeks after the second cycle,” Dr Delarue explained.
Among the AITL patients, the CR rate was 42% (5/12), the partial response rate was 33% (4/12), and the rate of stable disease was 25% (3/12).
Six AITL patients eventually progressed—after 2, 2, 3, 4, 4, and 20 cycles of therapy, respectively.
Two AITL patients are off therapy but remain in CR after 9 and 10 months (5 and 6 cycles of treatment), respectively.
The median progression-free survival for AITL patients was 16 months, and the median overall survival was 17 months.
Dr DeLarue noted that 4 of the AITL patients had CMML, 1 had non-CMML myelodysplastic syndrome, 3 had monocytosis without CMML, and 4 had normal monocyte counts.
He also said that, at present, it’s not possible to correlate the results observed in the AITL patients with their mutational status.
However, he and his colleagues are planning a prospective study of 5-AZA in patients with relapsed/refractory AITL and T follicular helper cell PTCL not otherwise specified. 5-AZA will be compared to investigator’s choice in this study.
Dr DeLarue said this trial will provide an opportunity to use the new oral formulation of 5-AZA (CC-486). And he and his colleagues welcome collaborators. ![]()

Photo by Larry Young
SAN FRANCISCO—Treatment with 5-azacitidine (5-AZA) can produce a high response rate in patients with relapsed/refractory angioimmunoblastic T-cell lymphoma (AITL), according to a small study.
The overall response rate (ORR) among AITL patients was 75%, and the complete response (CR) rate was 42%.
However, this study also included patients with other types of peripheral T-cell lymphoma (PTCL), and most of these patients did not respond to 5-AZA.
Richard Delarue, MD, of Necker University Hospital in Paris, France, presented these results at the 9th Annual T-cell Lymphoma Forum.
Results were also presented at the 2016 ASH Annual Meeting (abstract 4164). Dr Delarue reported receiving honoraria from Celgene.
Patients
The study included 19 patients with relapsed/refractory PTCL. Twelve patients had AITL, 3 had adult T-cell leukemia/lymphoma (ATLL), 2 had PTCL not otherwise specified, 1 had enteropathy-associated T-cell lymphoma, and 1 had transformed mycosis fungoides.
At diagnosis, the median age was 71 (range, 39-85) for AITL patients and 59 (range, 32-83) for the other PTCL patients. Seventy-five percent of AITL patients had an IPI score of 3 to 5 and a PIT score of 3 to 4. Eighty-six percent of the other PTCL patients had an IPI score of 3 to 5, and 57% had a PIT score of 3 to 4.
At the time of 5-AZA treatment, all patients had stage III/IV disease. The AITL patients had received a median of 2 (range, 0-6) prior lines of therapy, and the other PTCL patients had received a median of 3 (range, 0-7).
Two patients did not receive chemotherapy before 5-AZA because of the presence of associated chronic myelomonocytic leukemia (CMML) that required treatment first.
Ninety-two percent of AITL patients had TET2 mutations (n=11), 33% had DNMT3A mutations (n=4), and 0% had IDH2 mutations. One of the non-AITL patients had a TET2 mutation.
Treatment
Patients received a subcutaneous injection of 5-AZA at 75 mg/m² for 7 consecutive days every 28 days until progression or unacceptable toxicity. Six patients also received 4 to 8 infusions of rituximab because of EBV-DNA positivity.
The patients received a median of 3 cycles of 5-AZA. At the time of analysis, 4 patients were still receiving therapy.
The median follow-up was 84 days (range, 19 to 1236).
Toxicity
“Hematological toxicity was as expected with 5-azacitidine,” Dr Delarue said.
However, 2 patients had “unusual” adverse reactions. One patient had grade 2 polyneuropathy, which was considered related to a paraneoplastic syndrome.
The other patient had grade 3 diarrhea related to colitis of unknown origin, and this led to treatment interruption.
There were no treatment-related deaths.
Efficacy
Dr Delarue noted that the ORR was significantly higher in AITL patients than in patients with the other PTCL subtypes (P=0.0198).
The ORR was 53% in the entire cohort (10/19), 75% (9/12) among AITL patients, and 14% among patients with other PTCLs (1/7).
“The only patient with a response in the ‘other PTCL’ group was a patient with HTLV1-associated ATLL . . . , but he relapsed a couple of weeks after the second cycle,” Dr Delarue explained.
Among the AITL patients, the CR rate was 42% (5/12), the partial response rate was 33% (4/12), and the rate of stable disease was 25% (3/12).
Six AITL patients eventually progressed—after 2, 2, 3, 4, 4, and 20 cycles of therapy, respectively.
Two AITL patients are off therapy but remain in CR after 9 and 10 months (5 and 6 cycles of treatment), respectively.
The median progression-free survival for AITL patients was 16 months, and the median overall survival was 17 months.
Dr DeLarue noted that 4 of the AITL patients had CMML, 1 had non-CMML myelodysplastic syndrome, 3 had monocytosis without CMML, and 4 had normal monocyte counts.
He also said that, at present, it’s not possible to correlate the results observed in the AITL patients with their mutational status.
However, he and his colleagues are planning a prospective study of 5-AZA in patients with relapsed/refractory AITL and T follicular helper cell PTCL not otherwise specified. 5-AZA will be compared to investigator’s choice in this study.
Dr DeLarue said this trial will provide an opportunity to use the new oral formulation of 5-AZA (CC-486). And he and his colleagues welcome collaborators. ![]()

Photo by Larry Young
SAN FRANCISCO—Treatment with 5-azacitidine (5-AZA) can produce a high response rate in patients with relapsed/refractory angioimmunoblastic T-cell lymphoma (AITL), according to a small study.
The overall response rate (ORR) among AITL patients was 75%, and the complete response (CR) rate was 42%.
However, this study also included patients with other types of peripheral T-cell lymphoma (PTCL), and most of these patients did not respond to 5-AZA.
Richard Delarue, MD, of Necker University Hospital in Paris, France, presented these results at the 9th Annual T-cell Lymphoma Forum.
Results were also presented at the 2016 ASH Annual Meeting (abstract 4164). Dr Delarue reported receiving honoraria from Celgene.
Patients
The study included 19 patients with relapsed/refractory PTCL. Twelve patients had AITL, 3 had adult T-cell leukemia/lymphoma (ATLL), 2 had PTCL not otherwise specified, 1 had enteropathy-associated T-cell lymphoma, and 1 had transformed mycosis fungoides.
At diagnosis, the median age was 71 (range, 39-85) for AITL patients and 59 (range, 32-83) for the other PTCL patients. Seventy-five percent of AITL patients had an IPI score of 3 to 5 and a PIT score of 3 to 4. Eighty-six percent of the other PTCL patients had an IPI score of 3 to 5, and 57% had a PIT score of 3 to 4.
At the time of 5-AZA treatment, all patients had stage III/IV disease. The AITL patients had received a median of 2 (range, 0-6) prior lines of therapy, and the other PTCL patients had received a median of 3 (range, 0-7).
Two patients did not receive chemotherapy before 5-AZA because of the presence of associated chronic myelomonocytic leukemia (CMML) that required treatment first.
Ninety-two percent of AITL patients had TET2 mutations (n=11), 33% had DNMT3A mutations (n=4), and 0% had IDH2 mutations. One of the non-AITL patients had a TET2 mutation.
Treatment
Patients received a subcutaneous injection of 5-AZA at 75 mg/m² for 7 consecutive days every 28 days until progression or unacceptable toxicity. Six patients also received 4 to 8 infusions of rituximab because of EBV-DNA positivity.
The patients received a median of 3 cycles of 5-AZA. At the time of analysis, 4 patients were still receiving therapy.
The median follow-up was 84 days (range, 19 to 1236).
Toxicity
“Hematological toxicity was as expected with 5-azacitidine,” Dr Delarue said.
However, 2 patients had “unusual” adverse reactions. One patient had grade 2 polyneuropathy, which was considered related to a paraneoplastic syndrome.
The other patient had grade 3 diarrhea related to colitis of unknown origin, and this led to treatment interruption.
There were no treatment-related deaths.
Efficacy
Dr Delarue noted that the ORR was significantly higher in AITL patients than in patients with the other PTCL subtypes (P=0.0198).
The ORR was 53% in the entire cohort (10/19), 75% (9/12) among AITL patients, and 14% among patients with other PTCLs (1/7).
“The only patient with a response in the ‘other PTCL’ group was a patient with HTLV1-associated ATLL . . . , but he relapsed a couple of weeks after the second cycle,” Dr Delarue explained.
Among the AITL patients, the CR rate was 42% (5/12), the partial response rate was 33% (4/12), and the rate of stable disease was 25% (3/12).
Six AITL patients eventually progressed—after 2, 2, 3, 4, 4, and 20 cycles of therapy, respectively.
Two AITL patients are off therapy but remain in CR after 9 and 10 months (5 and 6 cycles of treatment), respectively.
The median progression-free survival for AITL patients was 16 months, and the median overall survival was 17 months.
Dr DeLarue noted that 4 of the AITL patients had CMML, 1 had non-CMML myelodysplastic syndrome, 3 had monocytosis without CMML, and 4 had normal monocyte counts.
He also said that, at present, it’s not possible to correlate the results observed in the AITL patients with their mutational status.
However, he and his colleagues are planning a prospective study of 5-AZA in patients with relapsed/refractory AITL and T follicular helper cell PTCL not otherwise specified. 5-AZA will be compared to investigator’s choice in this study.
Dr DeLarue said this trial will provide an opportunity to use the new oral formulation of 5-AZA (CC-486). And he and his colleagues welcome collaborators. ![]()
Cancer survivors report pros and cons of telehealth

Photo by Daniel Sone
Cancer survivors report a range of benefits and detriments related to telehealth, according to research published in the Journal of Medical Internet Research.
Telehealth is the use of technology to provide remote, personalized healthcare to patients.
Telehealth services allow patients to have meetings and follow-up consultations with healthcare professionals either on the phone or through online services at a time that suits the patients.
Anna Cox, PhD, of the University of Surrey in the UK, and her colleagues examined 22 studies, published between 2006 and 2016, that reported cancer patients’ direct views on their experience of telehealth.
Some of the cancer survivors studied reported their appreciation of the flexibility and convenience of telehealth, which enabled them to engage with healthcare providers with minimum disruption to their lives and in a comfortable, familiar environment.
“Our research found that cancer survivors wanted to get back to their daily lives as quickly as possible,” Dr Cox said. “Telehealth helped facilitate this, as it removed the often burdensome visits to hospital and enabled the integration of care into daily routines.”
However, not all subjects viewed telehealth as a convenience. Of the Internet-based interventions studied, 2 were perceived as an extra burden, and 1 was considered too time-consuming.
In addition, some study participants viewed telehealth as an impersonal service that did not allow them to meet their healthcare team in person.
On the other hand, the invisibility and perceived anonymity that telehealth provided sometimes reduced cancer survivors’ sense of vulnerability and enabled them to raise concerns remotely that they would not have wanted to discuss face-to-face.
And, in 8 different studies, subjects said telehealth had educated them about ways they could improve or manage their symptoms, or it had raised their awareness of potential issues they might experience.
Unfortunately, some of the cancer survivors studied said they were unable to use telehealth due to personal circumstances, such as hearing issues and lack of computer literacy skills.
“For many cancer survivors, telehealth supported their independence and offered them reassurance,” Dr Cox noted. “However, it is all down to personal preference, as some cancer survivors still preferred traditional methods of care.” ![]()

Photo by Daniel Sone
Cancer survivors report a range of benefits and detriments related to telehealth, according to research published in the Journal of Medical Internet Research.
Telehealth is the use of technology to provide remote, personalized healthcare to patients.
Telehealth services allow patients to have meetings and follow-up consultations with healthcare professionals either on the phone or through online services at a time that suits the patients.
Anna Cox, PhD, of the University of Surrey in the UK, and her colleagues examined 22 studies, published between 2006 and 2016, that reported cancer patients’ direct views on their experience of telehealth.
Some of the cancer survivors studied reported their appreciation of the flexibility and convenience of telehealth, which enabled them to engage with healthcare providers with minimum disruption to their lives and in a comfortable, familiar environment.
“Our research found that cancer survivors wanted to get back to their daily lives as quickly as possible,” Dr Cox said. “Telehealth helped facilitate this, as it removed the often burdensome visits to hospital and enabled the integration of care into daily routines.”
However, not all subjects viewed telehealth as a convenience. Of the Internet-based interventions studied, 2 were perceived as an extra burden, and 1 was considered too time-consuming.
In addition, some study participants viewed telehealth as an impersonal service that did not allow them to meet their healthcare team in person.
On the other hand, the invisibility and perceived anonymity that telehealth provided sometimes reduced cancer survivors’ sense of vulnerability and enabled them to raise concerns remotely that they would not have wanted to discuss face-to-face.
And, in 8 different studies, subjects said telehealth had educated them about ways they could improve or manage their symptoms, or it had raised their awareness of potential issues they might experience.
Unfortunately, some of the cancer survivors studied said they were unable to use telehealth due to personal circumstances, such as hearing issues and lack of computer literacy skills.
“For many cancer survivors, telehealth supported their independence and offered them reassurance,” Dr Cox noted. “However, it is all down to personal preference, as some cancer survivors still preferred traditional methods of care.” ![]()

Photo by Daniel Sone
Cancer survivors report a range of benefits and detriments related to telehealth, according to research published in the Journal of Medical Internet Research.
Telehealth is the use of technology to provide remote, personalized healthcare to patients.
Telehealth services allow patients to have meetings and follow-up consultations with healthcare professionals either on the phone or through online services at a time that suits the patients.
Anna Cox, PhD, of the University of Surrey in the UK, and her colleagues examined 22 studies, published between 2006 and 2016, that reported cancer patients’ direct views on their experience of telehealth.
Some of the cancer survivors studied reported their appreciation of the flexibility and convenience of telehealth, which enabled them to engage with healthcare providers with minimum disruption to their lives and in a comfortable, familiar environment.
“Our research found that cancer survivors wanted to get back to their daily lives as quickly as possible,” Dr Cox said. “Telehealth helped facilitate this, as it removed the often burdensome visits to hospital and enabled the integration of care into daily routines.”
However, not all subjects viewed telehealth as a convenience. Of the Internet-based interventions studied, 2 were perceived as an extra burden, and 1 was considered too time-consuming.
In addition, some study participants viewed telehealth as an impersonal service that did not allow them to meet their healthcare team in person.
On the other hand, the invisibility and perceived anonymity that telehealth provided sometimes reduced cancer survivors’ sense of vulnerability and enabled them to raise concerns remotely that they would not have wanted to discuss face-to-face.
And, in 8 different studies, subjects said telehealth had educated them about ways they could improve or manage their symptoms, or it had raised their awareness of potential issues they might experience.
Unfortunately, some of the cancer survivors studied said they were unable to use telehealth due to personal circumstances, such as hearing issues and lack of computer literacy skills.
“For many cancer survivors, telehealth supported their independence and offered them reassurance,” Dr Cox noted. “However, it is all down to personal preference, as some cancer survivors still preferred traditional methods of care.” ![]()
How EBV causes lymphoma, other cancers
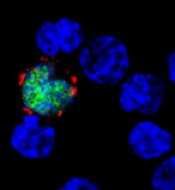
among uninfected cells (blue)
Image courtesy of
Benjamin Chaigne-Delalande
New research published in Nature Communications appears to explain how Epstein-Barr virus (EBV) reprograms cells into cancer cells.
Investigators said they discovered a mechanism by which EBV particles induce chromosomal instability without establishing a chronic infection, thereby conferring a risk for the development of tumors that do not necessarily carry the viral genome.
“The contribution of the viral infection to cancer development in patients with a weakened immune system is well understood,” said study author Henri-Jacques Delecluse, MD, PhD, of the German Cancer Research Center (Deutsches Krebsforschungszentrum, DKFZ) in Heidelberg.
“But in the majority of cases, it remains unclear how an EBV infection leads to cancer development.”
With their research, Dr Delecluse and his colleagues found that BNRF1, a protein component of EBV, promotes the development of cancer. They said BNRF1 induces centrosome amplification, which is associated with chromosomal instability.
When a dividing cell comes in contact with EBV, BNRF1 frequently prompts the formation of an excessive number of centrosomes. As a result, chromosomes are no longer divided equally and accurately between daughter cells—a known cancer risk factor.
In contrast, when the investigators studied EBV deficient of BNRF1, they found the virus did not interfere with chromosome distribution to daughter cells.
The team noted that EBV normally remains silent in a few infected cells, but, occasionally, it reactivates to produce viral offspring that infects nearby cells. As a consequence, these cells come in close contact with BNRF1, thus increasing their risk of transforming into cancer cells.
“The novelty of our work is that we have uncovered a component of the viral particle as a cancer driver,” Dr Delecluse said. “All human-tumors viruses that have been studied so far cause cancer in a completely different manner.”
“Usually, the genetic material of the viruses needs to be permanently present in the infected cell, thus causing the activation of one or several viral genes that cause cancer development. However, these gene products are not present in the infectious particle itself.”
Dr Delecluse and his colleagues therefore suspect that EBV could cause cancers other than those that have already been linked to EBV. Certain cancers might not have been linked to the virus because they do not carry the viral genetic material.
“We must push forward with the development of a vaccine against EBV infection,” Dr Delecluse said. “This would be the most direct strategy to prevent an infection with the virus.”
“Our latest results show that the first infection could already be a cancer risk, and this fits with earlier work that showed an increase in the incidence of Hodgkin’s lymphoma in people who underwent an episode of infectious mononucleosis.” ![]()

among uninfected cells (blue)
Image courtesy of
Benjamin Chaigne-Delalande
New research published in Nature Communications appears to explain how Epstein-Barr virus (EBV) reprograms cells into cancer cells.
Investigators said they discovered a mechanism by which EBV particles induce chromosomal instability without establishing a chronic infection, thereby conferring a risk for the development of tumors that do not necessarily carry the viral genome.
“The contribution of the viral infection to cancer development in patients with a weakened immune system is well understood,” said study author Henri-Jacques Delecluse, MD, PhD, of the German Cancer Research Center (Deutsches Krebsforschungszentrum, DKFZ) in Heidelberg.
“But in the majority of cases, it remains unclear how an EBV infection leads to cancer development.”
With their research, Dr Delecluse and his colleagues found that BNRF1, a protein component of EBV, promotes the development of cancer. They said BNRF1 induces centrosome amplification, which is associated with chromosomal instability.
When a dividing cell comes in contact with EBV, BNRF1 frequently prompts the formation of an excessive number of centrosomes. As a result, chromosomes are no longer divided equally and accurately between daughter cells—a known cancer risk factor.
In contrast, when the investigators studied EBV deficient of BNRF1, they found the virus did not interfere with chromosome distribution to daughter cells.
The team noted that EBV normally remains silent in a few infected cells, but, occasionally, it reactivates to produce viral offspring that infects nearby cells. As a consequence, these cells come in close contact with BNRF1, thus increasing their risk of transforming into cancer cells.
“The novelty of our work is that we have uncovered a component of the viral particle as a cancer driver,” Dr Delecluse said. “All human-tumors viruses that have been studied so far cause cancer in a completely different manner.”
“Usually, the genetic material of the viruses needs to be permanently present in the infected cell, thus causing the activation of one or several viral genes that cause cancer development. However, these gene products are not present in the infectious particle itself.”
Dr Delecluse and his colleagues therefore suspect that EBV could cause cancers other than those that have already been linked to EBV. Certain cancers might not have been linked to the virus because they do not carry the viral genetic material.
“We must push forward with the development of a vaccine against EBV infection,” Dr Delecluse said. “This would be the most direct strategy to prevent an infection with the virus.”
“Our latest results show that the first infection could already be a cancer risk, and this fits with earlier work that showed an increase in the incidence of Hodgkin’s lymphoma in people who underwent an episode of infectious mononucleosis.” ![]()

among uninfected cells (blue)
Image courtesy of
Benjamin Chaigne-Delalande
New research published in Nature Communications appears to explain how Epstein-Barr virus (EBV) reprograms cells into cancer cells.
Investigators said they discovered a mechanism by which EBV particles induce chromosomal instability without establishing a chronic infection, thereby conferring a risk for the development of tumors that do not necessarily carry the viral genome.
“The contribution of the viral infection to cancer development in patients with a weakened immune system is well understood,” said study author Henri-Jacques Delecluse, MD, PhD, of the German Cancer Research Center (Deutsches Krebsforschungszentrum, DKFZ) in Heidelberg.
“But in the majority of cases, it remains unclear how an EBV infection leads to cancer development.”
With their research, Dr Delecluse and his colleagues found that BNRF1, a protein component of EBV, promotes the development of cancer. They said BNRF1 induces centrosome amplification, which is associated with chromosomal instability.
When a dividing cell comes in contact with EBV, BNRF1 frequently prompts the formation of an excessive number of centrosomes. As a result, chromosomes are no longer divided equally and accurately between daughter cells—a known cancer risk factor.
In contrast, when the investigators studied EBV deficient of BNRF1, they found the virus did not interfere with chromosome distribution to daughter cells.
The team noted that EBV normally remains silent in a few infected cells, but, occasionally, it reactivates to produce viral offspring that infects nearby cells. As a consequence, these cells come in close contact with BNRF1, thus increasing their risk of transforming into cancer cells.
“The novelty of our work is that we have uncovered a component of the viral particle as a cancer driver,” Dr Delecluse said. “All human-tumors viruses that have been studied so far cause cancer in a completely different manner.”
“Usually, the genetic material of the viruses needs to be permanently present in the infected cell, thus causing the activation of one or several viral genes that cause cancer development. However, these gene products are not present in the infectious particle itself.”
Dr Delecluse and his colleagues therefore suspect that EBV could cause cancers other than those that have already been linked to EBV. Certain cancers might not have been linked to the virus because they do not carry the viral genetic material.
“We must push forward with the development of a vaccine against EBV infection,” Dr Delecluse said. “This would be the most direct strategy to prevent an infection with the virus.”
“Our latest results show that the first infection could already be a cancer risk, and this fits with earlier work that showed an increase in the incidence of Hodgkin’s lymphoma in people who underwent an episode of infectious mononucleosis.” ![]()
G-CSF could prevent infertility in cancer patients

Granulocyte colony-stimulating factor (G-CSF) could prevent infertility in male cancer patients, according to preclinical research published in Reproductive Biology and Endocrinology.
Researchers said they found that G-CSF protects spermatogenesis after alkylating chemotherapy by stimulating the proliferation of surviving spermatogonia.
The team also found evidence to suggest that G-CSF may be useful as a fertility-restoring treatment.
The researchers have been pursuing initiatives to restore fertility in men who have lost their ability to have children as a result of cancer treatments they received as children.
While working on methods to restart sperm production, the team discovered a link between G-CSF and the absence of normal damage to reproductive ability.
“We were using G-CSF to prevent infections in our research experiments,” said study author Brian Hermann, PhD, of The University of Texas at San Antonio.
“It turned out that the drug also had the unexpected impact of guarding against male infertility.”
To test the fertility-related impact of G-CSF, the researchers treated male mice with G-CSF before and/or after treatment with busulfan.
The team then evaluated effects on spermatogenesis in these mice and control mice that only received busulfan.
G-CSF had a protective effect on spermatogenesis that was stable for at least 19 weeks after chemotherapy.
And mice treated with G-CSF for 4 days after busulfan showed modestly enhanced spermatogenic recovery compared to controls.
The researchers said these results suggest G-CSF promotes spermatogonial proliferation, leading to enhanced spermatogenic regeneration from surviving spermatogonial stem cells. ![]()

Granulocyte colony-stimulating factor (G-CSF) could prevent infertility in male cancer patients, according to preclinical research published in Reproductive Biology and Endocrinology.
Researchers said they found that G-CSF protects spermatogenesis after alkylating chemotherapy by stimulating the proliferation of surviving spermatogonia.
The team also found evidence to suggest that G-CSF may be useful as a fertility-restoring treatment.
The researchers have been pursuing initiatives to restore fertility in men who have lost their ability to have children as a result of cancer treatments they received as children.
While working on methods to restart sperm production, the team discovered a link between G-CSF and the absence of normal damage to reproductive ability.
“We were using G-CSF to prevent infections in our research experiments,” said study author Brian Hermann, PhD, of The University of Texas at San Antonio.
“It turned out that the drug also had the unexpected impact of guarding against male infertility.”
To test the fertility-related impact of G-CSF, the researchers treated male mice with G-CSF before and/or after treatment with busulfan.
The team then evaluated effects on spermatogenesis in these mice and control mice that only received busulfan.
G-CSF had a protective effect on spermatogenesis that was stable for at least 19 weeks after chemotherapy.
And mice treated with G-CSF for 4 days after busulfan showed modestly enhanced spermatogenic recovery compared to controls.
The researchers said these results suggest G-CSF promotes spermatogonial proliferation, leading to enhanced spermatogenic regeneration from surviving spermatogonial stem cells. ![]()

Granulocyte colony-stimulating factor (G-CSF) could prevent infertility in male cancer patients, according to preclinical research published in Reproductive Biology and Endocrinology.
Researchers said they found that G-CSF protects spermatogenesis after alkylating chemotherapy by stimulating the proliferation of surviving spermatogonia.
The team also found evidence to suggest that G-CSF may be useful as a fertility-restoring treatment.
The researchers have been pursuing initiatives to restore fertility in men who have lost their ability to have children as a result of cancer treatments they received as children.
While working on methods to restart sperm production, the team discovered a link between G-CSF and the absence of normal damage to reproductive ability.
“We were using G-CSF to prevent infections in our research experiments,” said study author Brian Hermann, PhD, of The University of Texas at San Antonio.
“It turned out that the drug also had the unexpected impact of guarding against male infertility.”
To test the fertility-related impact of G-CSF, the researchers treated male mice with G-CSF before and/or after treatment with busulfan.
The team then evaluated effects on spermatogenesis in these mice and control mice that only received busulfan.
G-CSF had a protective effect on spermatogenesis that was stable for at least 19 weeks after chemotherapy.
And mice treated with G-CSF for 4 days after busulfan showed modestly enhanced spermatogenic recovery compared to controls.
The researchers said these results suggest G-CSF promotes spermatogonial proliferation, leading to enhanced spermatogenic regeneration from surviving spermatogonial stem cells.
Team creates online database of cancer mutations

Image by Spencer Phillips
Researchers have developed an online “knowledgebase” called CIViC, an open access resource for collecting and interpreting information from scientific publications on cancer genetics.
“CIViC” stands for Clinical Interpretations of Variants in Cancer, and the researchers liken it to a Wikipedia of cancer genetics.
Anyone can create an account and contribute information. That information is then curated by editors and moderators who are considered experts in the field.
The researchers described the resource in Nature Genetics.
“It’s relatively easy now to sequence the DNA of tumors—to gather the raw information—but there’s a big interpretation problem,” said study author Obi L. Griffith, PhD, of Washington University School of Medicine in St Louis, Missouri.
“What do these hundreds or thousands of mutations mean for this patient? There are a lot of studies being done to answer these questions. But oncologists trying to interpret the raw data are faced with an overwhelming task of plumbing the literature, reading papers, trying to understand what the latest studies tell them about these mutations and how they may or may not be important.”
The CIViC knowledgebase is an attempt to solve this problem. The researchers said this is one of many efforts to collect and interpret such information, but, to their knowledge, CIViC is the only one that is entirely open access. Anyone is free to contribute and use the content as well as the source code.
“We are committed to keeping this resource open and available to anyone who wants to contribute or make use of the information,” said Malachi Griffith, PhD, of Washington University School of Medicine.
“We would like it to be a community exercise and public resource. The information is in the public domain. There are no restrictions on its use, academic or commercial.”
Though anyone can submit a new piece of information or suggest edits to existing data, at least 2 independent contributors must agree that the new information should be incorporated, and 1 of those users must be an “expert editor.”
Expert editors are not permitted to approve their own submissions. Information on the CIViC website provides details about how new users may be promoted to expert editors and administrators.
To date, the site has seen over 17,500 users from academic institutions, governmental organizations, and commercial entities around the world.
Since CIViC’s launch, 59 users have volunteered their time to contribute their knowledge to CIViC, including descriptions of the clinical relevance of 732 mutations from 285 genes for 203 types of cancer, all gleaned from reviewing 1090 scientific and medical publications.
Despite the fact that there are many groups attempting to collect and interpret genomic variants in cancer, the researchers said the sheer volume of information has resulted in relatively little overlap in data gathered so far.
“While we believe this is the only such open access knowledgebase, there are other large research centers with similar resources,” Malachi Griffith said. “We did an analysis to compare the big ones.”
“Even though we all have access to the same published literature, if you look at the overlap of the information mined by each of these resources, it’s remarkably small. We’re all approaching the same problem, and, just by chance—and probably because of the amount of information out there—we haven’t duplicated our efforts very much yet.”
Obi and Malachi Griffith said finding a way to combine these resources is the primary goal of an international group they are helping lead called the Variant Interpretation for Cancer Consortium, which is a part of the Global Alliance for Genomics and Health (GA4GH).
“We’re just scratching the surface of the potential this holds for precision medicine,” Obi Griffith said. “There’s a lot of work to do.”

Image by Spencer Phillips
Researchers have developed an online “knowledgebase” called CIViC, an open access resource for collecting and interpreting information from scientific publications on cancer genetics.
“CIViC” stands for Clinical Interpretations of Variants in Cancer, and the researchers liken it to a Wikipedia of cancer genetics.
Anyone can create an account and contribute information. That information is then curated by editors and moderators who are considered experts in the field.
The researchers described the resource in Nature Genetics.
“It’s relatively easy now to sequence the DNA of tumors—to gather the raw information—but there’s a big interpretation problem,” said study author Obi L. Griffith, PhD, of Washington University School of Medicine in St Louis, Missouri.
“What do these hundreds or thousands of mutations mean for this patient? There are a lot of studies being done to answer these questions. But oncologists trying to interpret the raw data are faced with an overwhelming task of plumbing the literature, reading papers, trying to understand what the latest studies tell them about these mutations and how they may or may not be important.”
The CIViC knowledgebase is an attempt to solve this problem. The researchers said this is one of many efforts to collect and interpret such information, but, to their knowledge, CIViC is the only one that is entirely open access. Anyone is free to contribute and use the content as well as the source code.
“We are committed to keeping this resource open and available to anyone who wants to contribute or make use of the information,” said Malachi Griffith, PhD, of Washington University School of Medicine.
“We would like it to be a community exercise and public resource. The information is in the public domain. There are no restrictions on its use, academic or commercial.”
Though anyone can submit a new piece of information or suggest edits to existing data, at least 2 independent contributors must agree that the new information should be incorporated, and 1 of those users must be an “expert editor.”
Expert editors are not permitted to approve their own submissions. Information on the CIViC website provides details about how new users may be promoted to expert editors and administrators.
To date, the site has seen over 17,500 users from academic institutions, governmental organizations, and commercial entities around the world.
Since CIViC’s launch, 59 users have volunteered their time to contribute their knowledge to CIViC, including descriptions of the clinical relevance of 732 mutations from 285 genes for 203 types of cancer, all gleaned from reviewing 1090 scientific and medical publications.
Despite the fact that there are many groups attempting to collect and interpret genomic variants in cancer, the researchers said the sheer volume of information has resulted in relatively little overlap in data gathered so far.
“While we believe this is the only such open access knowledgebase, there are other large research centers with similar resources,” Malachi Griffith said. “We did an analysis to compare the big ones.”
“Even though we all have access to the same published literature, if you look at the overlap of the information mined by each of these resources, it’s remarkably small. We’re all approaching the same problem, and, just by chance—and probably because of the amount of information out there—we haven’t duplicated our efforts very much yet.”
Obi and Malachi Griffith said finding a way to combine these resources is the primary goal of an international group they are helping lead called the Variant Interpretation for Cancer Consortium, which is a part of the Global Alliance for Genomics and Health (GA4GH).
“We’re just scratching the surface of the potential this holds for precision medicine,” Obi Griffith said. “There’s a lot of work to do.”

Image by Spencer Phillips
Researchers have developed an online “knowledgebase” called CIViC, an open access resource for collecting and interpreting information from scientific publications on cancer genetics.
“CIViC” stands for Clinical Interpretations of Variants in Cancer, and the researchers liken it to a Wikipedia of cancer genetics.
Anyone can create an account and contribute information. That information is then curated by editors and moderators who are considered experts in the field.
The researchers described the resource in Nature Genetics.
“It’s relatively easy now to sequence the DNA of tumors—to gather the raw information—but there’s a big interpretation problem,” said study author Obi L. Griffith, PhD, of Washington University School of Medicine in St Louis, Missouri.
“What do these hundreds or thousands of mutations mean for this patient? There are a lot of studies being done to answer these questions. But oncologists trying to interpret the raw data are faced with an overwhelming task of plumbing the literature, reading papers, trying to understand what the latest studies tell them about these mutations and how they may or may not be important.”
The CIViC knowledgebase is an attempt to solve this problem. The researchers said this is one of many efforts to collect and interpret such information, but, to their knowledge, CIViC is the only one that is entirely open access. Anyone is free to contribute and use the content as well as the source code.
“We are committed to keeping this resource open and available to anyone who wants to contribute or make use of the information,” said Malachi Griffith, PhD, of Washington University School of Medicine.
“We would like it to be a community exercise and public resource. The information is in the public domain. There are no restrictions on its use, academic or commercial.”
Though anyone can submit a new piece of information or suggest edits to existing data, at least 2 independent contributors must agree that the new information should be incorporated, and 1 of those users must be an “expert editor.”
Expert editors are not permitted to approve their own submissions. Information on the CIViC website provides details about how new users may be promoted to expert editors and administrators.
To date, the site has seen over 17,500 users from academic institutions, governmental organizations, and commercial entities around the world.
Since CIViC’s launch, 59 users have volunteered their time to contribute their knowledge to CIViC, including descriptions of the clinical relevance of 732 mutations from 285 genes for 203 types of cancer, all gleaned from reviewing 1090 scientific and medical publications.
Despite the fact that there are many groups attempting to collect and interpret genomic variants in cancer, the researchers said the sheer volume of information has resulted in relatively little overlap in data gathered so far.
“While we believe this is the only such open access knowledgebase, there are other large research centers with similar resources,” Malachi Griffith said. “We did an analysis to compare the big ones.”
“Even though we all have access to the same published literature, if you look at the overlap of the information mined by each of these resources, it’s remarkably small. We’re all approaching the same problem, and, just by chance—and probably because of the amount of information out there—we haven’t duplicated our efforts very much yet.”
Obi and Malachi Griffith said finding a way to combine these resources is the primary goal of an international group they are helping lead called the Variant Interpretation for Cancer Consortium, which is a part of the Global Alliance for Genomics and Health (GA4GH).
“We’re just scratching the surface of the potential this holds for precision medicine,” Obi Griffith said. “There’s a lot of work to do.”
In high-risk myeloma, look beyond VRD for induction
NEW YORK – There’s more to induction therapy for transplant-eligible multiple myeloma patients than the go-to combination of bortezomib, lenalidomide, and dexamethasone, commonly known as VRD, according to Joseph R. Mikhael, MD.
“Outstanding evidence” has emerged that demonstrates the value of combining multiple mechanisms of action, but there are numerous options available – there is a trend toward increasing use of carfilzomib, for example – and VRD isn’t necessarily the best option for all patients, nor is it available in all cases, Dr. Mikhael of Mayo Clinic Arizona, Scottsdale, said at an international congress on hematologic malignancies.
Further, choosing the treatment method shown to give the most powerful or deepest response as a default isn’t necessarily the best option, either, he said, noting data showing that the regimen most often associated with at least very good partial response (VGPR) after four cycles in newly diagnosed multiple myeloma (carfilzomib, lenalidomide, dexamethasone, or KRD, about a 90% response rate) costs 2.5 times more than does the regimen (lenalidomide, dexamethasone, or RD) that provided about a 50% response rate ($250,000 vs. $100,000 per year).“But it’s also the toxicity cost ... do we need that many [drugs]?” he said, adding that “just because a clinical trial shows that three drugs work better than two, it doesn’t mean that every time I have a patient who is eligible I’m going to go with all three.”
It may be that a patient can start on two, with a third added if needed, he added.
“That being said, we want to maximize the synergy of those three, especially in high-risk patients,” he said.
Prior to 2016, popular regimens included CyBorD (cyclophosphamide, bortezomib, dexamethasone) and VTD (bortezomib, thalidomide, dexamethasone), which were commonly used worldwide. CTD (cyclophosphamide, thalidomide, dexamethasone) was used in Brazil and other countries where it was difficult to obtain bortezomib; VRD was “king of the hill” in the United States, and transplant was routinely recommended, Dr. Mikhael said.
A number of recent studies are changing that paradigm, he said.
One such study, the prospective randomized Intergroupe Francophone du Myélome (IFM) 2013-04 trial, showed that VTD is superior to bortezomib-cyclophosphamide-dexamethasone (VCD) for induction in patients with de novo multiple myeloma. VGPR and PR rates were significantly superior in the VTD arm.
Of note, hematologic toxicity increased in the VCD arm, and the peripheral neuropathy rate was higher in the VTD arm. However, the study was conducted at a time when bortezomib was generally used twice weekly; now it is standard to use it once weekly and subcutaneously, which significantly reduces the risk of peripheral neuropathy.
The authors advocated the preferential use of VTD over VCD for induction, based on the synergistic effect of a proteasome inhibitor and immunomodulatory drug, Dr. Mikhael said.
“Meanwhile, back in the United States, many trials were starting to be built with VRD,” he said, noting that “really extraordinary” responses were seen in phase I and phase II studies.
Perhaps the VRD study (called RVD in this case) that is most cited is the phase III IFM 2009 study comparing RVD with and without autologous stem cell transplant in newly diagnosed younger multiple myeloma patients. Although final results are still pending, interim results reported at the American Society of Hematology 2015 meeting (abstract 391) have been very helpful, Dr. Mikhael said.
The authors reported a 31% reduction in the risk of progression or death with autologous stem cell transplant versus RVD alone in patients with newly diagnosed multiple myeloma, as well as improved rates of thrombotic thrombocytopenic purpura (TTP) and minimal residual disease negativity (MRD). Mortality rates were similar.
The findings show that transplantation is feasible (93%), and associated with acceptable mortality (1.4%), an increased rate of negative MRD versus with RVD alone (80% vs. 65%), an improved 4-year progression-free survival (47% vs. 35%), and improved 4-year TTP (49% vs. 35%).
“Here the question was not so much is RVD the standard ... but is RVD plus transplant superior to RVD alone,” he said.
Surprising to many, especially the “dissenters in the crowd” who thought perhaps RVD would be the death knell to autologous stem cell transplant, transplant actually significantly improved the depth of response, he added.
Median progression-free survival at 10 months was 43% with versus 34% without transplantation.
“So there was definitely an argument here that transplant remains the standard of care,” he said, noting that transplant should be considered as decisions are made about up-front therapy.
As for the trend of bringing carfilzomib in earlier on in treatment, a number of studies, including the phase II CYKLONE study by Dr. Mikhael and his colleagues, suggest it improves the rates of deep response; some show that is especially true when used with transplant.
One study looking at KRD showed that the regimen provides high rates of deep and durable responses with acceptable tolerability – a finding that needs confirmation in a randomized setting.
Other studies are comparing KRD and VRD, and KRD and KCyd (carfilzomib, cyclophosphamide), as well as adding monoclonal antibodies such as daratumumab to treatment regimens, and results are very much anticipated, Dr. Mikhael said.
Currently, however, VRD remains the standard of care in standard risk and intermediate risk patients.
“But consideration in the highest-risk patients should be given to something like KRD,” he said. “We still recommend transplant across the board, we still recommend some form of maintenance therapy, be it with lenalidomide for most patients, but potentially bortezomib combined with carfilzomib in the highest risk patients.”
Dr. Mikhael reported consulting for Abbvie, Celgene, Onyx, and Sanofi.
NEW YORK – There’s more to induction therapy for transplant-eligible multiple myeloma patients than the go-to combination of bortezomib, lenalidomide, and dexamethasone, commonly known as VRD, according to Joseph R. Mikhael, MD.
“Outstanding evidence” has emerged that demonstrates the value of combining multiple mechanisms of action, but there are numerous options available – there is a trend toward increasing use of carfilzomib, for example – and VRD isn’t necessarily the best option for all patients, nor is it available in all cases, Dr. Mikhael of Mayo Clinic Arizona, Scottsdale, said at an international congress on hematologic malignancies.
Further, choosing the treatment method shown to give the most powerful or deepest response as a default isn’t necessarily the best option, either, he said, noting data showing that the regimen most often associated with at least very good partial response (VGPR) after four cycles in newly diagnosed multiple myeloma (carfilzomib, lenalidomide, dexamethasone, or KRD, about a 90% response rate) costs 2.5 times more than does the regimen (lenalidomide, dexamethasone, or RD) that provided about a 50% response rate ($250,000 vs. $100,000 per year).“But it’s also the toxicity cost ... do we need that many [drugs]?” he said, adding that “just because a clinical trial shows that three drugs work better than two, it doesn’t mean that every time I have a patient who is eligible I’m going to go with all three.”
It may be that a patient can start on two, with a third added if needed, he added.
“That being said, we want to maximize the synergy of those three, especially in high-risk patients,” he said.
Prior to 2016, popular regimens included CyBorD (cyclophosphamide, bortezomib, dexamethasone) and VTD (bortezomib, thalidomide, dexamethasone), which were commonly used worldwide. CTD (cyclophosphamide, thalidomide, dexamethasone) was used in Brazil and other countries where it was difficult to obtain bortezomib; VRD was “king of the hill” in the United States, and transplant was routinely recommended, Dr. Mikhael said.
A number of recent studies are changing that paradigm, he said.
One such study, the prospective randomized Intergroupe Francophone du Myélome (IFM) 2013-04 trial, showed that VTD is superior to bortezomib-cyclophosphamide-dexamethasone (VCD) for induction in patients with de novo multiple myeloma. VGPR and PR rates were significantly superior in the VTD arm.
Of note, hematologic toxicity increased in the VCD arm, and the peripheral neuropathy rate was higher in the VTD arm. However, the study was conducted at a time when bortezomib was generally used twice weekly; now it is standard to use it once weekly and subcutaneously, which significantly reduces the risk of peripheral neuropathy.
The authors advocated the preferential use of VTD over VCD for induction, based on the synergistic effect of a proteasome inhibitor and immunomodulatory drug, Dr. Mikhael said.
“Meanwhile, back in the United States, many trials were starting to be built with VRD,” he said, noting that “really extraordinary” responses were seen in phase I and phase II studies.
Perhaps the VRD study (called RVD in this case) that is most cited is the phase III IFM 2009 study comparing RVD with and without autologous stem cell transplant in newly diagnosed younger multiple myeloma patients. Although final results are still pending, interim results reported at the American Society of Hematology 2015 meeting (abstract 391) have been very helpful, Dr. Mikhael said.
The authors reported a 31% reduction in the risk of progression or death with autologous stem cell transplant versus RVD alone in patients with newly diagnosed multiple myeloma, as well as improved rates of thrombotic thrombocytopenic purpura (TTP) and minimal residual disease negativity (MRD). Mortality rates were similar.
The findings show that transplantation is feasible (93%), and associated with acceptable mortality (1.4%), an increased rate of negative MRD versus with RVD alone (80% vs. 65%), an improved 4-year progression-free survival (47% vs. 35%), and improved 4-year TTP (49% vs. 35%).
“Here the question was not so much is RVD the standard ... but is RVD plus transplant superior to RVD alone,” he said.
Surprising to many, especially the “dissenters in the crowd” who thought perhaps RVD would be the death knell to autologous stem cell transplant, transplant actually significantly improved the depth of response, he added.
Median progression-free survival at 10 months was 43% with versus 34% without transplantation.
“So there was definitely an argument here that transplant remains the standard of care,” he said, noting that transplant should be considered as decisions are made about up-front therapy.
As for the trend of bringing carfilzomib in earlier on in treatment, a number of studies, including the phase II CYKLONE study by Dr. Mikhael and his colleagues, suggest it improves the rates of deep response; some show that is especially true when used with transplant.
One study looking at KRD showed that the regimen provides high rates of deep and durable responses with acceptable tolerability – a finding that needs confirmation in a randomized setting.
Other studies are comparing KRD and VRD, and KRD and KCyd (carfilzomib, cyclophosphamide), as well as adding monoclonal antibodies such as daratumumab to treatment regimens, and results are very much anticipated, Dr. Mikhael said.
Currently, however, VRD remains the standard of care in standard risk and intermediate risk patients.
“But consideration in the highest-risk patients should be given to something like KRD,” he said. “We still recommend transplant across the board, we still recommend some form of maintenance therapy, be it with lenalidomide for most patients, but potentially bortezomib combined with carfilzomib in the highest risk patients.”
Dr. Mikhael reported consulting for Abbvie, Celgene, Onyx, and Sanofi.
NEW YORK – There’s more to induction therapy for transplant-eligible multiple myeloma patients than the go-to combination of bortezomib, lenalidomide, and dexamethasone, commonly known as VRD, according to Joseph R. Mikhael, MD.
“Outstanding evidence” has emerged that demonstrates the value of combining multiple mechanisms of action, but there are numerous options available – there is a trend toward increasing use of carfilzomib, for example – and VRD isn’t necessarily the best option for all patients, nor is it available in all cases, Dr. Mikhael of Mayo Clinic Arizona, Scottsdale, said at an international congress on hematologic malignancies.
Further, choosing the treatment method shown to give the most powerful or deepest response as a default isn’t necessarily the best option, either, he said, noting data showing that the regimen most often associated with at least very good partial response (VGPR) after four cycles in newly diagnosed multiple myeloma (carfilzomib, lenalidomide, dexamethasone, or KRD, about a 90% response rate) costs 2.5 times more than does the regimen (lenalidomide, dexamethasone, or RD) that provided about a 50% response rate ($250,000 vs. $100,000 per year).“But it’s also the toxicity cost ... do we need that many [drugs]?” he said, adding that “just because a clinical trial shows that three drugs work better than two, it doesn’t mean that every time I have a patient who is eligible I’m going to go with all three.”
It may be that a patient can start on two, with a third added if needed, he added.
“That being said, we want to maximize the synergy of those three, especially in high-risk patients,” he said.
Prior to 2016, popular regimens included CyBorD (cyclophosphamide, bortezomib, dexamethasone) and VTD (bortezomib, thalidomide, dexamethasone), which were commonly used worldwide. CTD (cyclophosphamide, thalidomide, dexamethasone) was used in Brazil and other countries where it was difficult to obtain bortezomib; VRD was “king of the hill” in the United States, and transplant was routinely recommended, Dr. Mikhael said.
A number of recent studies are changing that paradigm, he said.
One such study, the prospective randomized Intergroupe Francophone du Myélome (IFM) 2013-04 trial, showed that VTD is superior to bortezomib-cyclophosphamide-dexamethasone (VCD) for induction in patients with de novo multiple myeloma. VGPR and PR rates were significantly superior in the VTD arm.
Of note, hematologic toxicity increased in the VCD arm, and the peripheral neuropathy rate was higher in the VTD arm. However, the study was conducted at a time when bortezomib was generally used twice weekly; now it is standard to use it once weekly and subcutaneously, which significantly reduces the risk of peripheral neuropathy.
The authors advocated the preferential use of VTD over VCD for induction, based on the synergistic effect of a proteasome inhibitor and immunomodulatory drug, Dr. Mikhael said.
“Meanwhile, back in the United States, many trials were starting to be built with VRD,” he said, noting that “really extraordinary” responses were seen in phase I and phase II studies.
Perhaps the VRD study (called RVD in this case) that is most cited is the phase III IFM 2009 study comparing RVD with and without autologous stem cell transplant in newly diagnosed younger multiple myeloma patients. Although final results are still pending, interim results reported at the American Society of Hematology 2015 meeting (abstract 391) have been very helpful, Dr. Mikhael said.
The authors reported a 31% reduction in the risk of progression or death with autologous stem cell transplant versus RVD alone in patients with newly diagnosed multiple myeloma, as well as improved rates of thrombotic thrombocytopenic purpura (TTP) and minimal residual disease negativity (MRD). Mortality rates were similar.
The findings show that transplantation is feasible (93%), and associated with acceptable mortality (1.4%), an increased rate of negative MRD versus with RVD alone (80% vs. 65%), an improved 4-year progression-free survival (47% vs. 35%), and improved 4-year TTP (49% vs. 35%).
“Here the question was not so much is RVD the standard ... but is RVD plus transplant superior to RVD alone,” he said.
Surprising to many, especially the “dissenters in the crowd” who thought perhaps RVD would be the death knell to autologous stem cell transplant, transplant actually significantly improved the depth of response, he added.
Median progression-free survival at 10 months was 43% with versus 34% without transplantation.
“So there was definitely an argument here that transplant remains the standard of care,” he said, noting that transplant should be considered as decisions are made about up-front therapy.
As for the trend of bringing carfilzomib in earlier on in treatment, a number of studies, including the phase II CYKLONE study by Dr. Mikhael and his colleagues, suggest it improves the rates of deep response; some show that is especially true when used with transplant.
One study looking at KRD showed that the regimen provides high rates of deep and durable responses with acceptable tolerability – a finding that needs confirmation in a randomized setting.
Other studies are comparing KRD and VRD, and KRD and KCyd (carfilzomib, cyclophosphamide), as well as adding monoclonal antibodies such as daratumumab to treatment regimens, and results are very much anticipated, Dr. Mikhael said.
Currently, however, VRD remains the standard of care in standard risk and intermediate risk patients.
“But consideration in the highest-risk patients should be given to something like KRD,” he said. “We still recommend transplant across the board, we still recommend some form of maintenance therapy, be it with lenalidomide for most patients, but potentially bortezomib combined with carfilzomib in the highest risk patients.”
Dr. Mikhael reported consulting for Abbvie, Celgene, Onyx, and Sanofi.
EXPERT ANALYSIS FROM LYMPHOMA & MYELOMA



