User login
SNP predicts liver cancer in hepatitis C patients regardless of SVR
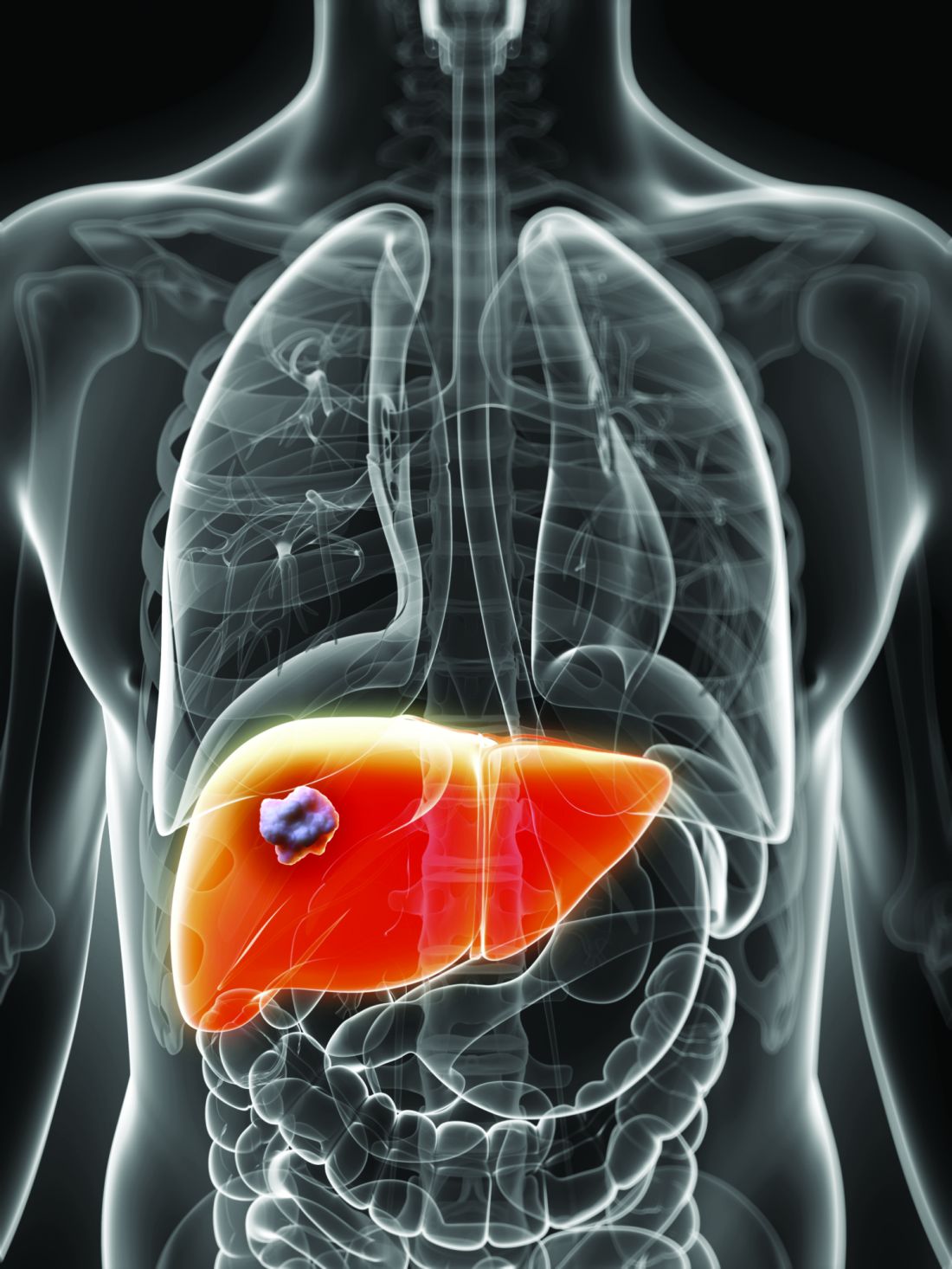
BOSTON – rs4836493, a single nucleotide polymorphism of the gene encoding chondroitin sulfate synthase-3, significantly predicted hepatocellular carcinoma among patients with HCV even when they achieved sustained virologic response on pegylated interferon, according to a genome-wide association study.
The next step is to determine whether rs4836493 predicts liver cancer after SVR on the new direct-acting antiviral regimens, Basile Njei, MD, MPH, said during an oral presentation at the annual meeting of the American Association for the Study of Liver Diseases.
Cirrhotic patients face about a 2%-7% annual risk of hepatocellular carcinoma, noted Dr. Njei of Yale University, New Haven, Conn. “Recent studies show that people with HCV may still develop hepatocellular carcinoma even after achieving SVR,” he said.
To look for genetic predictors of this outcome, he and his associates genotyped 958 patients with HCV and advanced hepatic fibrosis from the Hepatitis C Antiviral Long-term Treatment against Cirrhosis (HALT-C) study. This trial had evaluated long-term, low-dose pegylated interferon therapy (90 mcg per week for 3.5 years) as a means of keeping fibrosis from progressing among HCV patients who had failed peginterferon and ribavirin therapy.
A total of 63% of patients had cirrhosis, and 55 (5.7%) developed biopsy or imaging-confirmed hepatocellular carcinoma over a median of 80 months of follow-up, Dr. Njei said. After the researchers controlled for age, sex, Ishak fibrosis score, and SVR status, rs4836493 predicted hepatocellular carcinoma with a highly significant P value of .000004.
This SNP is located on the CHSY3 gene, which plays a role in the chondroitin polymerization, tissue development, and morphogenesis, according to Dr. Njei. Notably, the gene has been implicated in the biology of colorectal tumors, he added.
Dr. Njei and his associates genotyped patients by using the 610-Quad platform, which contains more than 600,000 SNPs. They double-checked results and conducted more genetic analyses using PLINK 1.9, a free, open-source software program for genome-wide association data. Three-quarters of patients in the study were white, 72% were male, and median age at enrollment was 50 years, he noted.
Linking a single SNP to liver cancer despite SVR is a striking finding, but it is also preliminary, Dr. Njei cautioned. “The SNP identified in our discovery genome-wide association study needs future replication and validation in patients who achieve SVR after receiving the new direct-acting antiviral therapies,” he said.
The National Institutes of Health provided partial funding. Dr. Njei and his coinvestigators had no relevant financial conflicts of interest.
BOSTON – rs4836493, a single nucleotide polymorphism of the gene encoding chondroitin sulfate synthase-3, significantly predicted hepatocellular carcinoma among patients with HCV even when they achieved sustained virologic response on pegylated interferon, according to a genome-wide association study.
The next step is to determine whether rs4836493 predicts liver cancer after SVR on the new direct-acting antiviral regimens, Basile Njei, MD, MPH, said during an oral presentation at the annual meeting of the American Association for the Study of Liver Diseases.
Cirrhotic patients face about a 2%-7% annual risk of hepatocellular carcinoma, noted Dr. Njei of Yale University, New Haven, Conn. “Recent studies show that people with HCV may still develop hepatocellular carcinoma even after achieving SVR,” he said.
To look for genetic predictors of this outcome, he and his associates genotyped 958 patients with HCV and advanced hepatic fibrosis from the Hepatitis C Antiviral Long-term Treatment against Cirrhosis (HALT-C) study. This trial had evaluated long-term, low-dose pegylated interferon therapy (90 mcg per week for 3.5 years) as a means of keeping fibrosis from progressing among HCV patients who had failed peginterferon and ribavirin therapy.
A total of 63% of patients had cirrhosis, and 55 (5.7%) developed biopsy or imaging-confirmed hepatocellular carcinoma over a median of 80 months of follow-up, Dr. Njei said. After the researchers controlled for age, sex, Ishak fibrosis score, and SVR status, rs4836493 predicted hepatocellular carcinoma with a highly significant P value of .000004.
This SNP is located on the CHSY3 gene, which plays a role in the chondroitin polymerization, tissue development, and morphogenesis, according to Dr. Njei. Notably, the gene has been implicated in the biology of colorectal tumors, he added.
Dr. Njei and his associates genotyped patients by using the 610-Quad platform, which contains more than 600,000 SNPs. They double-checked results and conducted more genetic analyses using PLINK 1.9, a free, open-source software program for genome-wide association data. Three-quarters of patients in the study were white, 72% were male, and median age at enrollment was 50 years, he noted.
Linking a single SNP to liver cancer despite SVR is a striking finding, but it is also preliminary, Dr. Njei cautioned. “The SNP identified in our discovery genome-wide association study needs future replication and validation in patients who achieve SVR after receiving the new direct-acting antiviral therapies,” he said.
The National Institutes of Health provided partial funding. Dr. Njei and his coinvestigators had no relevant financial conflicts of interest.
BOSTON – rs4836493, a single nucleotide polymorphism of the gene encoding chondroitin sulfate synthase-3, significantly predicted hepatocellular carcinoma among patients with HCV even when they achieved sustained virologic response on pegylated interferon, according to a genome-wide association study.
The next step is to determine whether rs4836493 predicts liver cancer after SVR on the new direct-acting antiviral regimens, Basile Njei, MD, MPH, said during an oral presentation at the annual meeting of the American Association for the Study of Liver Diseases.
Cirrhotic patients face about a 2%-7% annual risk of hepatocellular carcinoma, noted Dr. Njei of Yale University, New Haven, Conn. “Recent studies show that people with HCV may still develop hepatocellular carcinoma even after achieving SVR,” he said.
To look for genetic predictors of this outcome, he and his associates genotyped 958 patients with HCV and advanced hepatic fibrosis from the Hepatitis C Antiviral Long-term Treatment against Cirrhosis (HALT-C) study. This trial had evaluated long-term, low-dose pegylated interferon therapy (90 mcg per week for 3.5 years) as a means of keeping fibrosis from progressing among HCV patients who had failed peginterferon and ribavirin therapy.
A total of 63% of patients had cirrhosis, and 55 (5.7%) developed biopsy or imaging-confirmed hepatocellular carcinoma over a median of 80 months of follow-up, Dr. Njei said. After the researchers controlled for age, sex, Ishak fibrosis score, and SVR status, rs4836493 predicted hepatocellular carcinoma with a highly significant P value of .000004.
This SNP is located on the CHSY3 gene, which plays a role in the chondroitin polymerization, tissue development, and morphogenesis, according to Dr. Njei. Notably, the gene has been implicated in the biology of colorectal tumors, he added.
Dr. Njei and his associates genotyped patients by using the 610-Quad platform, which contains more than 600,000 SNPs. They double-checked results and conducted more genetic analyses using PLINK 1.9, a free, open-source software program for genome-wide association data. Three-quarters of patients in the study were white, 72% were male, and median age at enrollment was 50 years, he noted.
Linking a single SNP to liver cancer despite SVR is a striking finding, but it is also preliminary, Dr. Njei cautioned. “The SNP identified in our discovery genome-wide association study needs future replication and validation in patients who achieve SVR after receiving the new direct-acting antiviral therapies,” he said.
The National Institutes of Health provided partial funding. Dr. Njei and his coinvestigators had no relevant financial conflicts of interest.
AT THE LIVER MEETING 2016
Key clinical point: A single nucleotide polymorphism of the CHSY3 gene predicted liver cancer in patients who successfully completed treatment for chronic hepatitis C virus infection.
Major finding: After researchers controlled for sustained virologic response and other confounders, the rs4836493 variant predicted hepatocellular carcinoma with a P value of .000004.
Data source: A genome-wide association study of 958 HCV patients with advanced hepatic fibrosis from the HALT-C trial.
Disclosures: The National Institutes of Health provided partial funding. Dr. Njei and his coinvestigators had no relevant financial conflicts of interest.
Treatment withdrawal without prior liver biopsy found safe in well-controlled autoimmune hepatitis
BOSTON – Although current guidance calls for a liver biopsy prior to treatment withdrawal in autoimmune hepatitis (AIH), a retrospective observational analysis conducted by researchers from the Cleveland Clinic offers a different view.
“Maybe not everyone needs a liver biopsy before withdrawing treatment,” Yilien Alonso, MD, an internist at the Cleveland Clinic in Weston, Fla., said in an interview at the annual meeting of the American Association for the Study of Liver Diseases.
Both the European Association for Study of the Liver and the AASLD recommend liver biopsy prior to treatment withdrawal in AIH, but the expensive procedure is not without risk of morbidity and mortality. Dr. Alonso and her coinvestigators reviewed the records of 508 AIH patients seen at their institution between January 2001 and April 2015. After excluding the records of patients who’d had juvenile onset of AIH, or who were treated with agents other than corticosteroids and azathioprine, the researchers found 34 adults with similar pretreatment profiles who’d had treatment withdrawal after 2 years of excellent response to treatment, 10 of whom had a liver biopsy prior to treatment withdrawal.
The outcomes at 1 year post treatment withdrawal for all 34 were similar, with no difference in flare rates or reinitiation of treatment. In those who’d had the second liver biopsy, the fibrosis stage was noted at 1 year to have declined in three patients.
“If you have a stable patient population that you are tracking every 3-6 months, we don’t see why you can’t stop the treatment without having to have another invasive procedure,” Dr. Alonso said.
BOSTON – Although current guidance calls for a liver biopsy prior to treatment withdrawal in autoimmune hepatitis (AIH), a retrospective observational analysis conducted by researchers from the Cleveland Clinic offers a different view.
“Maybe not everyone needs a liver biopsy before withdrawing treatment,” Yilien Alonso, MD, an internist at the Cleveland Clinic in Weston, Fla., said in an interview at the annual meeting of the American Association for the Study of Liver Diseases.
Both the European Association for Study of the Liver and the AASLD recommend liver biopsy prior to treatment withdrawal in AIH, but the expensive procedure is not without risk of morbidity and mortality. Dr. Alonso and her coinvestigators reviewed the records of 508 AIH patients seen at their institution between January 2001 and April 2015. After excluding the records of patients who’d had juvenile onset of AIH, or who were treated with agents other than corticosteroids and azathioprine, the researchers found 34 adults with similar pretreatment profiles who’d had treatment withdrawal after 2 years of excellent response to treatment, 10 of whom had a liver biopsy prior to treatment withdrawal.
The outcomes at 1 year post treatment withdrawal for all 34 were similar, with no difference in flare rates or reinitiation of treatment. In those who’d had the second liver biopsy, the fibrosis stage was noted at 1 year to have declined in three patients.
“If you have a stable patient population that you are tracking every 3-6 months, we don’t see why you can’t stop the treatment without having to have another invasive procedure,” Dr. Alonso said.
BOSTON – Although current guidance calls for a liver biopsy prior to treatment withdrawal in autoimmune hepatitis (AIH), a retrospective observational analysis conducted by researchers from the Cleveland Clinic offers a different view.
“Maybe not everyone needs a liver biopsy before withdrawing treatment,” Yilien Alonso, MD, an internist at the Cleveland Clinic in Weston, Fla., said in an interview at the annual meeting of the American Association for the Study of Liver Diseases.
Both the European Association for Study of the Liver and the AASLD recommend liver biopsy prior to treatment withdrawal in AIH, but the expensive procedure is not without risk of morbidity and mortality. Dr. Alonso and her coinvestigators reviewed the records of 508 AIH patients seen at their institution between January 2001 and April 2015. After excluding the records of patients who’d had juvenile onset of AIH, or who were treated with agents other than corticosteroids and azathioprine, the researchers found 34 adults with similar pretreatment profiles who’d had treatment withdrawal after 2 years of excellent response to treatment, 10 of whom had a liver biopsy prior to treatment withdrawal.
The outcomes at 1 year post treatment withdrawal for all 34 were similar, with no difference in flare rates or reinitiation of treatment. In those who’d had the second liver biopsy, the fibrosis stage was noted at 1 year to have declined in three patients.
“If you have a stable patient population that you are tracking every 3-6 months, we don’t see why you can’t stop the treatment without having to have another invasive procedure,” Dr. Alonso said.
AT THE LIVER MEETING 2016
Key clinical point:
Major finding: Flare rates were similar post treatment withdrawal at 1 year in autoimmune hepatitis patients with and without a prior liver biopsy.
Data source: Retrospective observational analysis of 34 adults with well-controlled autoimmune hepatitis given treatment withdrawal with and without liver biopsy in large academic practice.
Disclosures: Dr. Alonso did not have any relevant disclosures.
Medicaid restrictions loosening on access to HCV therapies
BOSTON – State Medicaid programs have begun to loosen restrictions and improve transparency around access to direct-acting antiviral agents to treat hepatitis C virus infection, but inconsistencies are still the norm nationwide.
“Far too many states continue to restrict access in defiance to their obligations under the law,” said Robert Greenwald, clinical professor of law at Harvard University Center for Health Law and Policy Innovation (CHLPI), Boston.
Since 2014, the number of states that do not publish their access criteria for direct-acting antiviral agents (DAA) has dropped from 17 to 7, according to a report from CHLPI and the National Viral Hepatitis Roundtable (NVHR). Also during that period, 16 states relaxed or dropped fibrosis levels to qualify for access, and 7 decreased sobriety restrictions. The number of states that publish prescriber limitations has increased from 28 to 35. Because cost restrictions vary across insurance plans, some patients who need access get it, and others don’t, even if they have coverage, said Mr. Greenwald and Ryan Clary, NVHR executive director, who presented the report at the annual meeting of the American Association for the Study of Liver Diseases.
NVHR is a coalition of advocacy groups and local governmental agencies with interests in HCV, HIV, and infectious diseases. Its sponsors include AbbVie, Gilead Sciences, Merck, Bristol-Myers Squibb, Janssen, OraSure Technologies, Quest Diagnostics, and Walgreens. CHLPI is supported in part by Gilead, BMS, Johnson & Johnson, and ViiV Health Care.
In November 2015, the Centers for Medicaid & Medicare Services issued guidance to states, noting that while the cost of DAAs is prohibitive, states should use “sound clinical judgment” when determining access, and to “not unreasonably restrict coverage.” Varied interpretation of the guidance by state Medicaid directors means there is still a great deal of inconsistency in coverage.
Robert W. Zavoski, MD, Connecticut medical director of social services, noted that his state is making gains on balancing patient and taxpayer interests by emphasizing prevention, curbing reinfection rates, and using predictive modeling to determine the cost of HCV comorbidities.
Aligning incentives between institutions and payers that are based on long-term patient outcomes would mean not just lowered costs, but actual savings said Doug Dieterich, MD, professor of medicine at Mount Sinai Hospital in New York.
“It’s incredibly effective to treat hepatitis C virtually independent of the price of the drug. If patients remain in the same [health insurance] plan for 3-5 years after treatment, then the cost of treatment is very effective because the cost of health care drops precipitously – about 300% per patient – as soon as you cure hepatitis C,” Dr. Dieterich said.
Reducing the cost of treatments does not automatically result in better access, according John McHutchison, MD, executive vice president of clinical research at Gilead Sciences. Gilead’s DAAs (sofosbuvir and ledipasvir/sofosbuvir) were priced to the standard of care; however, miscalculations of demand drove up costs and “blew up” budgets, he said at the meeting.
Rebates to payers, discounts to patients, and the influx of new treatments to market are helping to drive down costs, Dr. McHutchison said, but while industry “wants to develop curative therapies, our system promotes chronic therapies from the financial perspective.”
The situation is compounded by the fact that state Medicaid programs negotiate individually with pharmaceutical companies and do not make their dealings public, said Brian Edlin, MD, chief medical officer for the CDC National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention. He called for more transparency regarding actual thresholds for profit and cure so that all restrictions could be dropped, and everyone could benefit. “How can much can we expect people to pay, what can we afford? All of that is out of the public domain,” he said.
Further dismantling of the barriers to care caused by high cost could be in the works if a recent proposal by FDA Commissioner Robert Califf, MD, gains traction. In an editorial published in JAMA, Dr. Califf called for collaboration between federal agencies to hasten and clarify public notification of the necessary criteria for a drug’s approval, coverage, and payment.
In the meantime, Mr. Greenwald said he and other advocates “are putting Medicaid directors on notice.”
BOSTON – State Medicaid programs have begun to loosen restrictions and improve transparency around access to direct-acting antiviral agents to treat hepatitis C virus infection, but inconsistencies are still the norm nationwide.
“Far too many states continue to restrict access in defiance to their obligations under the law,” said Robert Greenwald, clinical professor of law at Harvard University Center for Health Law and Policy Innovation (CHLPI), Boston.
Since 2014, the number of states that do not publish their access criteria for direct-acting antiviral agents (DAA) has dropped from 17 to 7, according to a report from CHLPI and the National Viral Hepatitis Roundtable (NVHR). Also during that period, 16 states relaxed or dropped fibrosis levels to qualify for access, and 7 decreased sobriety restrictions. The number of states that publish prescriber limitations has increased from 28 to 35. Because cost restrictions vary across insurance plans, some patients who need access get it, and others don’t, even if they have coverage, said Mr. Greenwald and Ryan Clary, NVHR executive director, who presented the report at the annual meeting of the American Association for the Study of Liver Diseases.
NVHR is a coalition of advocacy groups and local governmental agencies with interests in HCV, HIV, and infectious diseases. Its sponsors include AbbVie, Gilead Sciences, Merck, Bristol-Myers Squibb, Janssen, OraSure Technologies, Quest Diagnostics, and Walgreens. CHLPI is supported in part by Gilead, BMS, Johnson & Johnson, and ViiV Health Care.
In November 2015, the Centers for Medicaid & Medicare Services issued guidance to states, noting that while the cost of DAAs is prohibitive, states should use “sound clinical judgment” when determining access, and to “not unreasonably restrict coverage.” Varied interpretation of the guidance by state Medicaid directors means there is still a great deal of inconsistency in coverage.
Robert W. Zavoski, MD, Connecticut medical director of social services, noted that his state is making gains on balancing patient and taxpayer interests by emphasizing prevention, curbing reinfection rates, and using predictive modeling to determine the cost of HCV comorbidities.
Aligning incentives between institutions and payers that are based on long-term patient outcomes would mean not just lowered costs, but actual savings said Doug Dieterich, MD, professor of medicine at Mount Sinai Hospital in New York.
“It’s incredibly effective to treat hepatitis C virtually independent of the price of the drug. If patients remain in the same [health insurance] plan for 3-5 years after treatment, then the cost of treatment is very effective because the cost of health care drops precipitously – about 300% per patient – as soon as you cure hepatitis C,” Dr. Dieterich said.
Reducing the cost of treatments does not automatically result in better access, according John McHutchison, MD, executive vice president of clinical research at Gilead Sciences. Gilead’s DAAs (sofosbuvir and ledipasvir/sofosbuvir) were priced to the standard of care; however, miscalculations of demand drove up costs and “blew up” budgets, he said at the meeting.
Rebates to payers, discounts to patients, and the influx of new treatments to market are helping to drive down costs, Dr. McHutchison said, but while industry “wants to develop curative therapies, our system promotes chronic therapies from the financial perspective.”
The situation is compounded by the fact that state Medicaid programs negotiate individually with pharmaceutical companies and do not make their dealings public, said Brian Edlin, MD, chief medical officer for the CDC National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention. He called for more transparency regarding actual thresholds for profit and cure so that all restrictions could be dropped, and everyone could benefit. “How can much can we expect people to pay, what can we afford? All of that is out of the public domain,” he said.
Further dismantling of the barriers to care caused by high cost could be in the works if a recent proposal by FDA Commissioner Robert Califf, MD, gains traction. In an editorial published in JAMA, Dr. Califf called for collaboration between federal agencies to hasten and clarify public notification of the necessary criteria for a drug’s approval, coverage, and payment.
In the meantime, Mr. Greenwald said he and other advocates “are putting Medicaid directors on notice.”
BOSTON – State Medicaid programs have begun to loosen restrictions and improve transparency around access to direct-acting antiviral agents to treat hepatitis C virus infection, but inconsistencies are still the norm nationwide.
“Far too many states continue to restrict access in defiance to their obligations under the law,” said Robert Greenwald, clinical professor of law at Harvard University Center for Health Law and Policy Innovation (CHLPI), Boston.
Since 2014, the number of states that do not publish their access criteria for direct-acting antiviral agents (DAA) has dropped from 17 to 7, according to a report from CHLPI and the National Viral Hepatitis Roundtable (NVHR). Also during that period, 16 states relaxed or dropped fibrosis levels to qualify for access, and 7 decreased sobriety restrictions. The number of states that publish prescriber limitations has increased from 28 to 35. Because cost restrictions vary across insurance plans, some patients who need access get it, and others don’t, even if they have coverage, said Mr. Greenwald and Ryan Clary, NVHR executive director, who presented the report at the annual meeting of the American Association for the Study of Liver Diseases.
NVHR is a coalition of advocacy groups and local governmental agencies with interests in HCV, HIV, and infectious diseases. Its sponsors include AbbVie, Gilead Sciences, Merck, Bristol-Myers Squibb, Janssen, OraSure Technologies, Quest Diagnostics, and Walgreens. CHLPI is supported in part by Gilead, BMS, Johnson & Johnson, and ViiV Health Care.
In November 2015, the Centers for Medicaid & Medicare Services issued guidance to states, noting that while the cost of DAAs is prohibitive, states should use “sound clinical judgment” when determining access, and to “not unreasonably restrict coverage.” Varied interpretation of the guidance by state Medicaid directors means there is still a great deal of inconsistency in coverage.
Robert W. Zavoski, MD, Connecticut medical director of social services, noted that his state is making gains on balancing patient and taxpayer interests by emphasizing prevention, curbing reinfection rates, and using predictive modeling to determine the cost of HCV comorbidities.
Aligning incentives between institutions and payers that are based on long-term patient outcomes would mean not just lowered costs, but actual savings said Doug Dieterich, MD, professor of medicine at Mount Sinai Hospital in New York.
“It’s incredibly effective to treat hepatitis C virtually independent of the price of the drug. If patients remain in the same [health insurance] plan for 3-5 years after treatment, then the cost of treatment is very effective because the cost of health care drops precipitously – about 300% per patient – as soon as you cure hepatitis C,” Dr. Dieterich said.
Reducing the cost of treatments does not automatically result in better access, according John McHutchison, MD, executive vice president of clinical research at Gilead Sciences. Gilead’s DAAs (sofosbuvir and ledipasvir/sofosbuvir) were priced to the standard of care; however, miscalculations of demand drove up costs and “blew up” budgets, he said at the meeting.
Rebates to payers, discounts to patients, and the influx of new treatments to market are helping to drive down costs, Dr. McHutchison said, but while industry “wants to develop curative therapies, our system promotes chronic therapies from the financial perspective.”
The situation is compounded by the fact that state Medicaid programs negotiate individually with pharmaceutical companies and do not make their dealings public, said Brian Edlin, MD, chief medical officer for the CDC National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention. He called for more transparency regarding actual thresholds for profit and cure so that all restrictions could be dropped, and everyone could benefit. “How can much can we expect people to pay, what can we afford? All of that is out of the public domain,” he said.
Further dismantling of the barriers to care caused by high cost could be in the works if a recent proposal by FDA Commissioner Robert Califf, MD, gains traction. In an editorial published in JAMA, Dr. Califf called for collaboration between federal agencies to hasten and clarify public notification of the necessary criteria for a drug’s approval, coverage, and payment.
In the meantime, Mr. Greenwald said he and other advocates “are putting Medicaid directors on notice.”
VIDEO: Don’t be surprised by weight gain in men after HCV cure
BOSTON – In the new era of direct-acting antiviral (DAA) therapy, physicians will be seeing more and more patients who have achieved a cure of their hepatitis C virus (HCV). Once freed from the burden of a chronic illness, patients feel better and may eat better. Unexpected weight gain and potential associated health effects may be the next set of challenges patients and their physicians will face.
A single-center retrospective study of patients who had achieved sustained virologic response (SVR) after treatment for HCV found a small but significant weight gain in men, but not women. Additionally, according to noninvasive assessments, liver fat increased significantly in men, but not women, after SVR was achieved.
In a study of 63 patients (42 male, 67%) who received DAA treatment for HCV, mean weight gain for men after SVR was 2.8 pounds (range, –26 to +17; P = .0459), and body mass index (BMI) increased by a mean 0.50 kg/m2 (range, –3.6 to +3.33; P = .0176). No significant change was seen for women when pre- and posttreatment measures were compared.
Isaac Wasserman, a medical student at Mount Sinai Medical Center, New York, presented the results of the single-center retrospective study in a poster presentation at the annual meeting of the American Association for the Study of Liver Diseases.
To assess changes in liver fat, Mr. Wasserman and his coinvestigator used results of pre- and posttreatment transient elastography with controlled attenuation parameter (CAP). CAP measures the degree to which the ultrasound signal is attenuated by liver fat, he explained in a video interview.
For men, hepatic steatosis increased by this measure, with CAP measurements up by a mean 18 dB/m (range, –106 to +128, P = .0314). Mr. Wasserman and his colleagues wrote, “The change in liver fat was large enough to push 11% of the cohort (n = 7 of 63) into advanced steatosis (CAP greater than 300 dB/m).” Again, the women studied had no significant posttreatment change in liver fat.
Post-SVR weight gain appeared to be the culprit in the increased fat seen in the posttreatment livers. Mr. Wasserman and his colleagues in the abstract accompanying the presentation, “Changes in weight were positively correlated with changes in liver fat (P = .006).”
Mr. Wasserman said that he and his coinvestigators believe that social, and not biochemical or mechanistic, reasons underlie the weight gain and increased hepatic steatosis. They are planning further investigation of social and economic factors that may underlie the difference seen in this study, and hope to continue and expand data acquisition to validate their findings.
Mr. Wasserman reported no conflicts of interest or outside sources of funding for the study.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
On Twitter @karioakes
BOSTON – In the new era of direct-acting antiviral (DAA) therapy, physicians will be seeing more and more patients who have achieved a cure of their hepatitis C virus (HCV). Once freed from the burden of a chronic illness, patients feel better and may eat better. Unexpected weight gain and potential associated health effects may be the next set of challenges patients and their physicians will face.
A single-center retrospective study of patients who had achieved sustained virologic response (SVR) after treatment for HCV found a small but significant weight gain in men, but not women. Additionally, according to noninvasive assessments, liver fat increased significantly in men, but not women, after SVR was achieved.
In a study of 63 patients (42 male, 67%) who received DAA treatment for HCV, mean weight gain for men after SVR was 2.8 pounds (range, –26 to +17; P = .0459), and body mass index (BMI) increased by a mean 0.50 kg/m2 (range, –3.6 to +3.33; P = .0176). No significant change was seen for women when pre- and posttreatment measures were compared.
Isaac Wasserman, a medical student at Mount Sinai Medical Center, New York, presented the results of the single-center retrospective study in a poster presentation at the annual meeting of the American Association for the Study of Liver Diseases.
To assess changes in liver fat, Mr. Wasserman and his coinvestigator used results of pre- and posttreatment transient elastography with controlled attenuation parameter (CAP). CAP measures the degree to which the ultrasound signal is attenuated by liver fat, he explained in a video interview.
For men, hepatic steatosis increased by this measure, with CAP measurements up by a mean 18 dB/m (range, –106 to +128, P = .0314). Mr. Wasserman and his colleagues wrote, “The change in liver fat was large enough to push 11% of the cohort (n = 7 of 63) into advanced steatosis (CAP greater than 300 dB/m).” Again, the women studied had no significant posttreatment change in liver fat.
Post-SVR weight gain appeared to be the culprit in the increased fat seen in the posttreatment livers. Mr. Wasserman and his colleagues in the abstract accompanying the presentation, “Changes in weight were positively correlated with changes in liver fat (P = .006).”
Mr. Wasserman said that he and his coinvestigators believe that social, and not biochemical or mechanistic, reasons underlie the weight gain and increased hepatic steatosis. They are planning further investigation of social and economic factors that may underlie the difference seen in this study, and hope to continue and expand data acquisition to validate their findings.
Mr. Wasserman reported no conflicts of interest or outside sources of funding for the study.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
On Twitter @karioakes
BOSTON – In the new era of direct-acting antiviral (DAA) therapy, physicians will be seeing more and more patients who have achieved a cure of their hepatitis C virus (HCV). Once freed from the burden of a chronic illness, patients feel better and may eat better. Unexpected weight gain and potential associated health effects may be the next set of challenges patients and their physicians will face.
A single-center retrospective study of patients who had achieved sustained virologic response (SVR) after treatment for HCV found a small but significant weight gain in men, but not women. Additionally, according to noninvasive assessments, liver fat increased significantly in men, but not women, after SVR was achieved.
In a study of 63 patients (42 male, 67%) who received DAA treatment for HCV, mean weight gain for men after SVR was 2.8 pounds (range, –26 to +17; P = .0459), and body mass index (BMI) increased by a mean 0.50 kg/m2 (range, –3.6 to +3.33; P = .0176). No significant change was seen for women when pre- and posttreatment measures were compared.
Isaac Wasserman, a medical student at Mount Sinai Medical Center, New York, presented the results of the single-center retrospective study in a poster presentation at the annual meeting of the American Association for the Study of Liver Diseases.
To assess changes in liver fat, Mr. Wasserman and his coinvestigator used results of pre- and posttreatment transient elastography with controlled attenuation parameter (CAP). CAP measures the degree to which the ultrasound signal is attenuated by liver fat, he explained in a video interview.
For men, hepatic steatosis increased by this measure, with CAP measurements up by a mean 18 dB/m (range, –106 to +128, P = .0314). Mr. Wasserman and his colleagues wrote, “The change in liver fat was large enough to push 11% of the cohort (n = 7 of 63) into advanced steatosis (CAP greater than 300 dB/m).” Again, the women studied had no significant posttreatment change in liver fat.
Post-SVR weight gain appeared to be the culprit in the increased fat seen in the posttreatment livers. Mr. Wasserman and his colleagues in the abstract accompanying the presentation, “Changes in weight were positively correlated with changes in liver fat (P = .006).”
Mr. Wasserman said that he and his coinvestigators believe that social, and not biochemical or mechanistic, reasons underlie the weight gain and increased hepatic steatosis. They are planning further investigation of social and economic factors that may underlie the difference seen in this study, and hope to continue and expand data acquisition to validate their findings.
Mr. Wasserman reported no conflicts of interest or outside sources of funding for the study.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
On Twitter @karioakes
AT THE LIVER MEETING
Study eyed zinc for slowing progression of chronic liver disease
BOSTON – Oral zinc supplementation was associated with maintenance of liver function and suppression of hepatocellular carcinoma in a retrospective cohort study of 267 patients with chronic liver disease.
Additional analyses revealed stepwise inverse relationships between serum zinc levels and rates of de novo liver failure, hepatocellular carcinoma, and death, Atsushi Hosui, MD, PhD, said at the annual meeting of the American Association for the Study of Liver Diseases. No patients stopped zinc therapy because of adverse events, and there were no serious adverse events, although some patients experienced nausea, which can occur with zinc supplementation, noted Dr. Hosui of Osaka-Rosai Hospital, Japan.
To begin exploring hepatic correlates of zinc supplementation, Dr. Hosui and his associates retrospectively studied 267 patients in Japan with chronic liver diseases between 2006 and 2015. They had a median of 40 months of data for each patient. No patient had hepatocellular carcinoma at baseline. In all, 196 patients received zinc supplementation (average baseline zinc level, 51 mcg/dL), while 71 patients did not (62 mcg/dL). These two groups resembled each other in terms of etiologies of liver disease, but the zinc group was significantly older (73.2 vs. 66.4 years; P less than .0001), had a significantly higher average baseline bilirubin level (1.2 vs. 0.8 mg/dL; P less than .0001), and a significantly lower average platelet concentration and prothrombin time. (P less than .0001).
Despite having multiple indicators of worse liver disease, only 9.5% of zinc recipients developed hepatocellular carcinoma over 3 years, compared with 25% of patients in the control group (P = .005). Rates of liver failure and death were similar between the two groups, but sequential blood tests did indicate worsening liver disease among patients who did not receive zinc – their prothrombin times and branched-chain amino acid to tyrosine ratios steadily dropped over 3 years, while those in zinc recipients did not.
Next, the researchers stratified zinc recipients according to their serum zinc levels 6 months after starting supplementation. Notably, 3-year rates of mortality, liver failure, and death were significantly higher among patients whose zinc levels were lower than in patients who achieved higher serum zinc levels. For example, 3-year mortality rates were 28% among patients whose zinc level was 70-89 mcg/dL, versus 0% among patients whose zinc level was at least 90 mcg/dL (P = .02). Similarly, 3-year rates of liver failure were 3.6% among patients whose zinc level was 50-69 mcg/dL, versus 0% among patients whose serum zinc level was at least 70 mcg/dL (P = .03). Finally, over 3 years, hepatocellular carcinoma was diagnosed in 17% of patients whose zinc level was 50-69 mcg/dL, versus only 3.8% of patients whose zinc level was 70-89 mcg/dL.
“We suggest that oral zinc supplementation is effective for maintaining liver function and suppressing the development of hepatocellular carcinoma,” Dr. Hosui concluded. The data support a target serum zinc level of at least 70 mcg/dL to suppress liver-related events, including hepatocellular carcinoma, he added. The researchers are exploring clinical trials of zinc for these outcomes in Japan.
The investigators did not report funding for this study. They reported having no conflicts of interest.
BOSTON – Oral zinc supplementation was associated with maintenance of liver function and suppression of hepatocellular carcinoma in a retrospective cohort study of 267 patients with chronic liver disease.
Additional analyses revealed stepwise inverse relationships between serum zinc levels and rates of de novo liver failure, hepatocellular carcinoma, and death, Atsushi Hosui, MD, PhD, said at the annual meeting of the American Association for the Study of Liver Diseases. No patients stopped zinc therapy because of adverse events, and there were no serious adverse events, although some patients experienced nausea, which can occur with zinc supplementation, noted Dr. Hosui of Osaka-Rosai Hospital, Japan.
To begin exploring hepatic correlates of zinc supplementation, Dr. Hosui and his associates retrospectively studied 267 patients in Japan with chronic liver diseases between 2006 and 2015. They had a median of 40 months of data for each patient. No patient had hepatocellular carcinoma at baseline. In all, 196 patients received zinc supplementation (average baseline zinc level, 51 mcg/dL), while 71 patients did not (62 mcg/dL). These two groups resembled each other in terms of etiologies of liver disease, but the zinc group was significantly older (73.2 vs. 66.4 years; P less than .0001), had a significantly higher average baseline bilirubin level (1.2 vs. 0.8 mg/dL; P less than .0001), and a significantly lower average platelet concentration and prothrombin time. (P less than .0001).
Despite having multiple indicators of worse liver disease, only 9.5% of zinc recipients developed hepatocellular carcinoma over 3 years, compared with 25% of patients in the control group (P = .005). Rates of liver failure and death were similar between the two groups, but sequential blood tests did indicate worsening liver disease among patients who did not receive zinc – their prothrombin times and branched-chain amino acid to tyrosine ratios steadily dropped over 3 years, while those in zinc recipients did not.
Next, the researchers stratified zinc recipients according to their serum zinc levels 6 months after starting supplementation. Notably, 3-year rates of mortality, liver failure, and death were significantly higher among patients whose zinc levels were lower than in patients who achieved higher serum zinc levels. For example, 3-year mortality rates were 28% among patients whose zinc level was 70-89 mcg/dL, versus 0% among patients whose zinc level was at least 90 mcg/dL (P = .02). Similarly, 3-year rates of liver failure were 3.6% among patients whose zinc level was 50-69 mcg/dL, versus 0% among patients whose serum zinc level was at least 70 mcg/dL (P = .03). Finally, over 3 years, hepatocellular carcinoma was diagnosed in 17% of patients whose zinc level was 50-69 mcg/dL, versus only 3.8% of patients whose zinc level was 70-89 mcg/dL.
“We suggest that oral zinc supplementation is effective for maintaining liver function and suppressing the development of hepatocellular carcinoma,” Dr. Hosui concluded. The data support a target serum zinc level of at least 70 mcg/dL to suppress liver-related events, including hepatocellular carcinoma, he added. The researchers are exploring clinical trials of zinc for these outcomes in Japan.
The investigators did not report funding for this study. They reported having no conflicts of interest.
BOSTON – Oral zinc supplementation was associated with maintenance of liver function and suppression of hepatocellular carcinoma in a retrospective cohort study of 267 patients with chronic liver disease.
Additional analyses revealed stepwise inverse relationships between serum zinc levels and rates of de novo liver failure, hepatocellular carcinoma, and death, Atsushi Hosui, MD, PhD, said at the annual meeting of the American Association for the Study of Liver Diseases. No patients stopped zinc therapy because of adverse events, and there were no serious adverse events, although some patients experienced nausea, which can occur with zinc supplementation, noted Dr. Hosui of Osaka-Rosai Hospital, Japan.
To begin exploring hepatic correlates of zinc supplementation, Dr. Hosui and his associates retrospectively studied 267 patients in Japan with chronic liver diseases between 2006 and 2015. They had a median of 40 months of data for each patient. No patient had hepatocellular carcinoma at baseline. In all, 196 patients received zinc supplementation (average baseline zinc level, 51 mcg/dL), while 71 patients did not (62 mcg/dL). These two groups resembled each other in terms of etiologies of liver disease, but the zinc group was significantly older (73.2 vs. 66.4 years; P less than .0001), had a significantly higher average baseline bilirubin level (1.2 vs. 0.8 mg/dL; P less than .0001), and a significantly lower average platelet concentration and prothrombin time. (P less than .0001).
Despite having multiple indicators of worse liver disease, only 9.5% of zinc recipients developed hepatocellular carcinoma over 3 years, compared with 25% of patients in the control group (P = .005). Rates of liver failure and death were similar between the two groups, but sequential blood tests did indicate worsening liver disease among patients who did not receive zinc – their prothrombin times and branched-chain amino acid to tyrosine ratios steadily dropped over 3 years, while those in zinc recipients did not.
Next, the researchers stratified zinc recipients according to their serum zinc levels 6 months after starting supplementation. Notably, 3-year rates of mortality, liver failure, and death were significantly higher among patients whose zinc levels were lower than in patients who achieved higher serum zinc levels. For example, 3-year mortality rates were 28% among patients whose zinc level was 70-89 mcg/dL, versus 0% among patients whose zinc level was at least 90 mcg/dL (P = .02). Similarly, 3-year rates of liver failure were 3.6% among patients whose zinc level was 50-69 mcg/dL, versus 0% among patients whose serum zinc level was at least 70 mcg/dL (P = .03). Finally, over 3 years, hepatocellular carcinoma was diagnosed in 17% of patients whose zinc level was 50-69 mcg/dL, versus only 3.8% of patients whose zinc level was 70-89 mcg/dL.
“We suggest that oral zinc supplementation is effective for maintaining liver function and suppressing the development of hepatocellular carcinoma,” Dr. Hosui concluded. The data support a target serum zinc level of at least 70 mcg/dL to suppress liver-related events, including hepatocellular carcinoma, he added. The researchers are exploring clinical trials of zinc for these outcomes in Japan.
The investigators did not report funding for this study. They reported having no conflicts of interest.
AT THE LIVER MEETING 2016
Key clinical point: Oral zinc sulfate supplementation might help prevent the progression of chronic liver disease and associated hepatocellular carcinoma.
Major finding: Despite having multiple indicators of worse liver disease, only 9.5% of zinc recipients developed hepatocellular carcinoma over 3 years, compared with 25% of patients in the control group (P = .005).
Data source: A retrospective cohort study of 267 patients with chronic liver disease but no hepatocellular carcinoma at baseline.
Disclosures: The investigators did not report funding for this study. They reported having no conflicts of interest.
VIDEO: Obeticholic acid resulted in reduction of a biomarker for liver fibrosis in PBC
BOSTON – Obeticholic acid resulted in a significant reduction of a biomarker for liver fibrosis in patients with primary biliary cholangitis, according to a retrospective analysis of clinical trial data. In addition, patients taking obeticholic acid had a mean reduction in liver stiffness as measured by transient elastography.
Gideon Hirschfield, MD, PhD, presented the re-analysis of clinical trial data at the annual meeting of the American Association for the Study of Liver Diseases.
POISE was a phase III randomized, double-blind, placebo-controlled study of obeticholic acid for patients with primary biliary cholangitis (PBC). The clinical trial’s primary composite endpoint was an alkaline phosphatase level less than 1.67 times the upper limit of normal, with at least a 15% reduction in alkaline phosphatase and normal serum bilirubin.
The cohort of POISE patients on obeticholic acid met this biochemical surrogate endpoint, resulting in approval of the farnesoid X receptor agonist for treatment of PBC as an add-on to ursodeoxycholic acid (UDCA), or for patients who cannot tolerate UDCA.
However, transient elastography and the aspartate transaminase (AST) to platelet ratio index (APRI) have both been used to assess fibrosis in PBC, and have been found to predict clinical outcomes in PBC. These measures have the advantage of being noninvasive methods to measure the quality of liver tissue.
Dr. Hirschfield, a transplant hepatologist at the institute of immunology and immunotherapy at the University of Birmingham, England, and his coinvestigators reevaluated data from the POISE trial. They determined that APRI dropped significantly over 12 months of obeticholic acid treatment compared to placebo (P less than .01 for each of the two dosing arms of the POISE trial). Patients who switched to 5-10 mg of obeticholic acid daily from placebo during an open-label extension of POISE also had significant reductions in APRI scores (P less than .05); the reduction for placebo-switchers on a fixed 10-mg dose during the open-label study was not significant
Liver stiffness, as measured by transient elastography, was reduced for both arms of the POISE study at 12 months, but increased for those in the placebo arm. “Fewer patients receiving obeticholic acid 10 mg progressed” to a level associated with histological cirrhosis, “and patients receiving obeticholic acid showed an improvement in liver stiffness,” said Dr. Hirschfield.
Pruritis is a feature of PBC, and worsening pruritis can be a side effect of deoxycholic acid. However, the worsening is often transitory, so patients should be encouraged to try to stay the course, said Dr. Hirschfield. Managing patient expectations; sharing improved biomarkers; and considering the addition of a bile acid sequestrant or rifampicin, or reducing the obeticholic acid dose are all strategies to consider when caring for PBC patients, said Dr. Hirschfield.
Clinical trials to assess the safety and efficacy of obeticholic acid for individuals with nonalcoholic fatty liver disease and steatohepatitis are underway.
Dr. Hirschfield discussed his findings in a video interview.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
koakes@frontlinemedcom.com
On Twitter @karioakes
BOSTON – Obeticholic acid resulted in a significant reduction of a biomarker for liver fibrosis in patients with primary biliary cholangitis, according to a retrospective analysis of clinical trial data. In addition, patients taking obeticholic acid had a mean reduction in liver stiffness as measured by transient elastography.
Gideon Hirschfield, MD, PhD, presented the re-analysis of clinical trial data at the annual meeting of the American Association for the Study of Liver Diseases.
POISE was a phase III randomized, double-blind, placebo-controlled study of obeticholic acid for patients with primary biliary cholangitis (PBC). The clinical trial’s primary composite endpoint was an alkaline phosphatase level less than 1.67 times the upper limit of normal, with at least a 15% reduction in alkaline phosphatase and normal serum bilirubin.
The cohort of POISE patients on obeticholic acid met this biochemical surrogate endpoint, resulting in approval of the farnesoid X receptor agonist for treatment of PBC as an add-on to ursodeoxycholic acid (UDCA), or for patients who cannot tolerate UDCA.
However, transient elastography and the aspartate transaminase (AST) to platelet ratio index (APRI) have both been used to assess fibrosis in PBC, and have been found to predict clinical outcomes in PBC. These measures have the advantage of being noninvasive methods to measure the quality of liver tissue.
Dr. Hirschfield, a transplant hepatologist at the institute of immunology and immunotherapy at the University of Birmingham, England, and his coinvestigators reevaluated data from the POISE trial. They determined that APRI dropped significantly over 12 months of obeticholic acid treatment compared to placebo (P less than .01 for each of the two dosing arms of the POISE trial). Patients who switched to 5-10 mg of obeticholic acid daily from placebo during an open-label extension of POISE also had significant reductions in APRI scores (P less than .05); the reduction for placebo-switchers on a fixed 10-mg dose during the open-label study was not significant
Liver stiffness, as measured by transient elastography, was reduced for both arms of the POISE study at 12 months, but increased for those in the placebo arm. “Fewer patients receiving obeticholic acid 10 mg progressed” to a level associated with histological cirrhosis, “and patients receiving obeticholic acid showed an improvement in liver stiffness,” said Dr. Hirschfield.
Pruritis is a feature of PBC, and worsening pruritis can be a side effect of deoxycholic acid. However, the worsening is often transitory, so patients should be encouraged to try to stay the course, said Dr. Hirschfield. Managing patient expectations; sharing improved biomarkers; and considering the addition of a bile acid sequestrant or rifampicin, or reducing the obeticholic acid dose are all strategies to consider when caring for PBC patients, said Dr. Hirschfield.
Clinical trials to assess the safety and efficacy of obeticholic acid for individuals with nonalcoholic fatty liver disease and steatohepatitis are underway.
Dr. Hirschfield discussed his findings in a video interview.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
koakes@frontlinemedcom.com
On Twitter @karioakes
BOSTON – Obeticholic acid resulted in a significant reduction of a biomarker for liver fibrosis in patients with primary biliary cholangitis, according to a retrospective analysis of clinical trial data. In addition, patients taking obeticholic acid had a mean reduction in liver stiffness as measured by transient elastography.
Gideon Hirschfield, MD, PhD, presented the re-analysis of clinical trial data at the annual meeting of the American Association for the Study of Liver Diseases.
POISE was a phase III randomized, double-blind, placebo-controlled study of obeticholic acid for patients with primary biliary cholangitis (PBC). The clinical trial’s primary composite endpoint was an alkaline phosphatase level less than 1.67 times the upper limit of normal, with at least a 15% reduction in alkaline phosphatase and normal serum bilirubin.
The cohort of POISE patients on obeticholic acid met this biochemical surrogate endpoint, resulting in approval of the farnesoid X receptor agonist for treatment of PBC as an add-on to ursodeoxycholic acid (UDCA), or for patients who cannot tolerate UDCA.
However, transient elastography and the aspartate transaminase (AST) to platelet ratio index (APRI) have both been used to assess fibrosis in PBC, and have been found to predict clinical outcomes in PBC. These measures have the advantage of being noninvasive methods to measure the quality of liver tissue.
Dr. Hirschfield, a transplant hepatologist at the institute of immunology and immunotherapy at the University of Birmingham, England, and his coinvestigators reevaluated data from the POISE trial. They determined that APRI dropped significantly over 12 months of obeticholic acid treatment compared to placebo (P less than .01 for each of the two dosing arms of the POISE trial). Patients who switched to 5-10 mg of obeticholic acid daily from placebo during an open-label extension of POISE also had significant reductions in APRI scores (P less than .05); the reduction for placebo-switchers on a fixed 10-mg dose during the open-label study was not significant
Liver stiffness, as measured by transient elastography, was reduced for both arms of the POISE study at 12 months, but increased for those in the placebo arm. “Fewer patients receiving obeticholic acid 10 mg progressed” to a level associated with histological cirrhosis, “and patients receiving obeticholic acid showed an improvement in liver stiffness,” said Dr. Hirschfield.
Pruritis is a feature of PBC, and worsening pruritis can be a side effect of deoxycholic acid. However, the worsening is often transitory, so patients should be encouraged to try to stay the course, said Dr. Hirschfield. Managing patient expectations; sharing improved biomarkers; and considering the addition of a bile acid sequestrant or rifampicin, or reducing the obeticholic acid dose are all strategies to consider when caring for PBC patients, said Dr. Hirschfield.
Clinical trials to assess the safety and efficacy of obeticholic acid for individuals with nonalcoholic fatty liver disease and steatohepatitis are underway.
Dr. Hirschfield discussed his findings in a video interview.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
koakes@frontlinemedcom.com
On Twitter @karioakes
AT THE LIVER MEETING 2016
Study found no link between direct-acting antivirals, hepatocellular carcinoma
BOSTON – Direct-acting antiviral therapy does not appear to increase the risk of de novo hepatocellular carcinoma in cirrhotic patients with hepatitis C virus (HCV) infection, according to findings from a prospective cohort study of more than 2,000 patients.
But curing HCV also did not protect patients from hepatocellular carcinoma (HCC), at least during the first 6-12 months after starting treatment, Antonietta Romano, MD, said at the annual meeting of the American Association for the Study of Liver Diseases. Clinicians should continue monitoring HCV patients with advanced liver disease, even after they have achieved sustained viral response, she said.
Recent studies had raised concerns about whether direct-acting antivirals (DAA) increase the risk of HCC, said Dr. Romano of the University of Padova (Italy). To clarify the issue, she and her coinvestigators followed 2,279 HCV patients who received approved DAA regimens. Over a median follow-up time of 305 days, 41 patients developed de novo hepatocellular carcinoma, for an incidence of 1.64 cases per 100 patient-years, Dr. Romano said.
“These results indicate that in cirrhotic patients, the incidence of HCC during the first 6-9 months after initiation of direct-acting antiviral therapy is not different from what we expect in untreated patients, according to historical controls,” she added.
Fully 86% of patients had cirrhosis, of which 91% were Child-Pugh A and 9% were Child-Pugh B, indicating more advanced liver disease, Dr. Romano said. Noncirrhotic patients had an HCC rate of 0.23 cases per 100 patient years – less than one-eighth that for cirrhotic patients (1.93 cases per 100 patient-years). Child-Pugh B patients developed 2.9 cases of HCC per 100 patient years, versus 1.6 for Child-Pugh A patients.
These rates resemble those in historical controls, suggesting that stage of liver disease is the crucial predictor of HCC risk – not DAA therapy, Dr. Romano said. Multivariable analyses supported that conclusion, linking HCC to elevated liver enzymes and to thrombocytopenia but not to DAA regimen, gender, age, or HCV genotype, she reported.
Most HCC cases were diagnosed at least 12 weeks after starting therapy, according to Dr. Romano. Half of patients had a single nodular tumor with a typical vascular pattern, but the other half had a more aggressive multifocal infiltrative pattern. The reason for the high proportion of atypical aggressive pattern was unclear, Dr. Romano said. However, DAA therapy causes HCV to abruptly stop replicating in the liver, leading to marked molecular and immunologic changes that might initially cause microscopic tumors to grow faster than before. So while DAA therapy does not increase the overall risk of HCC, it clearly is not protective, she said.
Nearly 70% of patients in this study were male. About 60% had HCV-1 infection, 22% had HCV-2, 19% had HCV-3, and 8% had HCV-4, Dr. Romano said. In all, 28 of 41 patients who developed HCC had achieved sustained virologic response at 12 weeks, while the other 13 had relapsed.
The investigators received no outside funding for this study. Dr. Romano reported ties to Gilead, Abbvie, and Bristol Myers Squibb.
BOSTON – Direct-acting antiviral therapy does not appear to increase the risk of de novo hepatocellular carcinoma in cirrhotic patients with hepatitis C virus (HCV) infection, according to findings from a prospective cohort study of more than 2,000 patients.
But curing HCV also did not protect patients from hepatocellular carcinoma (HCC), at least during the first 6-12 months after starting treatment, Antonietta Romano, MD, said at the annual meeting of the American Association for the Study of Liver Diseases. Clinicians should continue monitoring HCV patients with advanced liver disease, even after they have achieved sustained viral response, she said.
Recent studies had raised concerns about whether direct-acting antivirals (DAA) increase the risk of HCC, said Dr. Romano of the University of Padova (Italy). To clarify the issue, she and her coinvestigators followed 2,279 HCV patients who received approved DAA regimens. Over a median follow-up time of 305 days, 41 patients developed de novo hepatocellular carcinoma, for an incidence of 1.64 cases per 100 patient-years, Dr. Romano said.
“These results indicate that in cirrhotic patients, the incidence of HCC during the first 6-9 months after initiation of direct-acting antiviral therapy is not different from what we expect in untreated patients, according to historical controls,” she added.
Fully 86% of patients had cirrhosis, of which 91% were Child-Pugh A and 9% were Child-Pugh B, indicating more advanced liver disease, Dr. Romano said. Noncirrhotic patients had an HCC rate of 0.23 cases per 100 patient years – less than one-eighth that for cirrhotic patients (1.93 cases per 100 patient-years). Child-Pugh B patients developed 2.9 cases of HCC per 100 patient years, versus 1.6 for Child-Pugh A patients.
These rates resemble those in historical controls, suggesting that stage of liver disease is the crucial predictor of HCC risk – not DAA therapy, Dr. Romano said. Multivariable analyses supported that conclusion, linking HCC to elevated liver enzymes and to thrombocytopenia but not to DAA regimen, gender, age, or HCV genotype, she reported.
Most HCC cases were diagnosed at least 12 weeks after starting therapy, according to Dr. Romano. Half of patients had a single nodular tumor with a typical vascular pattern, but the other half had a more aggressive multifocal infiltrative pattern. The reason for the high proportion of atypical aggressive pattern was unclear, Dr. Romano said. However, DAA therapy causes HCV to abruptly stop replicating in the liver, leading to marked molecular and immunologic changes that might initially cause microscopic tumors to grow faster than before. So while DAA therapy does not increase the overall risk of HCC, it clearly is not protective, she said.
Nearly 70% of patients in this study were male. About 60% had HCV-1 infection, 22% had HCV-2, 19% had HCV-3, and 8% had HCV-4, Dr. Romano said. In all, 28 of 41 patients who developed HCC had achieved sustained virologic response at 12 weeks, while the other 13 had relapsed.
The investigators received no outside funding for this study. Dr. Romano reported ties to Gilead, Abbvie, and Bristol Myers Squibb.
BOSTON – Direct-acting antiviral therapy does not appear to increase the risk of de novo hepatocellular carcinoma in cirrhotic patients with hepatitis C virus (HCV) infection, according to findings from a prospective cohort study of more than 2,000 patients.
But curing HCV also did not protect patients from hepatocellular carcinoma (HCC), at least during the first 6-12 months after starting treatment, Antonietta Romano, MD, said at the annual meeting of the American Association for the Study of Liver Diseases. Clinicians should continue monitoring HCV patients with advanced liver disease, even after they have achieved sustained viral response, she said.
Recent studies had raised concerns about whether direct-acting antivirals (DAA) increase the risk of HCC, said Dr. Romano of the University of Padova (Italy). To clarify the issue, she and her coinvestigators followed 2,279 HCV patients who received approved DAA regimens. Over a median follow-up time of 305 days, 41 patients developed de novo hepatocellular carcinoma, for an incidence of 1.64 cases per 100 patient-years, Dr. Romano said.
“These results indicate that in cirrhotic patients, the incidence of HCC during the first 6-9 months after initiation of direct-acting antiviral therapy is not different from what we expect in untreated patients, according to historical controls,” she added.
Fully 86% of patients had cirrhosis, of which 91% were Child-Pugh A and 9% were Child-Pugh B, indicating more advanced liver disease, Dr. Romano said. Noncirrhotic patients had an HCC rate of 0.23 cases per 100 patient years – less than one-eighth that for cirrhotic patients (1.93 cases per 100 patient-years). Child-Pugh B patients developed 2.9 cases of HCC per 100 patient years, versus 1.6 for Child-Pugh A patients.
These rates resemble those in historical controls, suggesting that stage of liver disease is the crucial predictor of HCC risk – not DAA therapy, Dr. Romano said. Multivariable analyses supported that conclusion, linking HCC to elevated liver enzymes and to thrombocytopenia but not to DAA regimen, gender, age, or HCV genotype, she reported.
Most HCC cases were diagnosed at least 12 weeks after starting therapy, according to Dr. Romano. Half of patients had a single nodular tumor with a typical vascular pattern, but the other half had a more aggressive multifocal infiltrative pattern. The reason for the high proportion of atypical aggressive pattern was unclear, Dr. Romano said. However, DAA therapy causes HCV to abruptly stop replicating in the liver, leading to marked molecular and immunologic changes that might initially cause microscopic tumors to grow faster than before. So while DAA therapy does not increase the overall risk of HCC, it clearly is not protective, she said.
Nearly 70% of patients in this study were male. About 60% had HCV-1 infection, 22% had HCV-2, 19% had HCV-3, and 8% had HCV-4, Dr. Romano said. In all, 28 of 41 patients who developed HCC had achieved sustained virologic response at 12 weeks, while the other 13 had relapsed.
The investigators received no outside funding for this study. Dr. Romano reported ties to Gilead, Abbvie, and Bristol Myers Squibb.
AT THE LIVER MEETING
Key clinical point:
Major finding: The overall incidence of de novo hepatocellular carcinoma was 1.64 cases per 100 patient-years during and after treatment, with a median follow-up period of about 305 days.
Data source: A prospective cohort study of 2,279 patients (86% with cirrhosis) who received direct-acting antivirals for HCV.
Disclosures: The investigators received no outside funding for the study. Dr. Romano reported ties to Gilead, Abbvie, and Bristol Myers Squibb.
Thyroid disease does not affect primary biliary cholangitis complications
While associations are known to exist between primary biliary cholangitis (PBC) and many different types of thyroid disease (TD), a new study shows that the mere presence of thyroid disease does not have any bearing on the hepatic complications or progression of PBC.
“The prevalence of TD in PBC reportedly ranges between 7.24% and 14.4%, the most often encountered thyroid dysfunction being Hashimoto’s thyroiditis,” wrote the study’s authors, led by Annarosa Floreani, MD, of the University of Padua (Italy).
Of the 921 total patients enrolled, 150 (16.3%) had TD. The most common TD patients had were Hashimoto’s thyroiditis, which 94 (10.2%) individuals had; Graves’ disease, found in 15 (1.6%) patients; multinodular goiter, which 22 (2.4%) patients had; thyroid cancer, which was found in 7 (0.8%); and “other thyroid conditions,” which affected 12 (1.3%) patients. Patients from Padua had significantly more Graves’ disease and thyroid cancer than those from Barcelona: 11 (15.7%) versus 4 (5.0%) for Graves’ (P = .03), and 6 (8.6%) versus 1 (1.3%) for thyroid cancer (P = .03), respectively. However, no significant differences were found in PBC patients who had TD and those who did not, when it came to comparing the histologic stages at which they were diagnosed with PBC, hepatic decompensation events, occurrence of hepatocellular carcinoma, or liver transplantation rate. Furthermore, TD was not found to affect PBC survival rates, either positively or negatively.
“The results of our study confirm that TDs are often associated with PBC, especially Hashimoto’s thyroiditis, which shares an autoimmune etiology with PBC,” the authors concluded, adding that “More importantly … the clinical characteristics and natural history of PBC were much the same in the two cohorts, as demonstrated by the absence of significant differences regarding histological stage at diagnosis (the only exception being more patients in stage III in the Italian cohort); biochemical data; response to UDCA [ursodeoxycholic acid]; the association with other extrahepatic autoimmune disorders; the occurrence of clinical events; and survival.”
No funding source was reported for this study. Dr. Floreani and her coauthors did not report any financial disclosures relevant to this study.
While associations are known to exist between primary biliary cholangitis (PBC) and many different types of thyroid disease (TD), a new study shows that the mere presence of thyroid disease does not have any bearing on the hepatic complications or progression of PBC.
“The prevalence of TD in PBC reportedly ranges between 7.24% and 14.4%, the most often encountered thyroid dysfunction being Hashimoto’s thyroiditis,” wrote the study’s authors, led by Annarosa Floreani, MD, of the University of Padua (Italy).
Of the 921 total patients enrolled, 150 (16.3%) had TD. The most common TD patients had were Hashimoto’s thyroiditis, which 94 (10.2%) individuals had; Graves’ disease, found in 15 (1.6%) patients; multinodular goiter, which 22 (2.4%) patients had; thyroid cancer, which was found in 7 (0.8%); and “other thyroid conditions,” which affected 12 (1.3%) patients. Patients from Padua had significantly more Graves’ disease and thyroid cancer than those from Barcelona: 11 (15.7%) versus 4 (5.0%) for Graves’ (P = .03), and 6 (8.6%) versus 1 (1.3%) for thyroid cancer (P = .03), respectively. However, no significant differences were found in PBC patients who had TD and those who did not, when it came to comparing the histologic stages at which they were diagnosed with PBC, hepatic decompensation events, occurrence of hepatocellular carcinoma, or liver transplantation rate. Furthermore, TD was not found to affect PBC survival rates, either positively or negatively.
“The results of our study confirm that TDs are often associated with PBC, especially Hashimoto’s thyroiditis, which shares an autoimmune etiology with PBC,” the authors concluded, adding that “More importantly … the clinical characteristics and natural history of PBC were much the same in the two cohorts, as demonstrated by the absence of significant differences regarding histological stage at diagnosis (the only exception being more patients in stage III in the Italian cohort); biochemical data; response to UDCA [ursodeoxycholic acid]; the association with other extrahepatic autoimmune disorders; the occurrence of clinical events; and survival.”
No funding source was reported for this study. Dr. Floreani and her coauthors did not report any financial disclosures relevant to this study.
While associations are known to exist between primary biliary cholangitis (PBC) and many different types of thyroid disease (TD), a new study shows that the mere presence of thyroid disease does not have any bearing on the hepatic complications or progression of PBC.
“The prevalence of TD in PBC reportedly ranges between 7.24% and 14.4%, the most often encountered thyroid dysfunction being Hashimoto’s thyroiditis,” wrote the study’s authors, led by Annarosa Floreani, MD, of the University of Padua (Italy).
Of the 921 total patients enrolled, 150 (16.3%) had TD. The most common TD patients had were Hashimoto’s thyroiditis, which 94 (10.2%) individuals had; Graves’ disease, found in 15 (1.6%) patients; multinodular goiter, which 22 (2.4%) patients had; thyroid cancer, which was found in 7 (0.8%); and “other thyroid conditions,” which affected 12 (1.3%) patients. Patients from Padua had significantly more Graves’ disease and thyroid cancer than those from Barcelona: 11 (15.7%) versus 4 (5.0%) for Graves’ (P = .03), and 6 (8.6%) versus 1 (1.3%) for thyroid cancer (P = .03), respectively. However, no significant differences were found in PBC patients who had TD and those who did not, when it came to comparing the histologic stages at which they were diagnosed with PBC, hepatic decompensation events, occurrence of hepatocellular carcinoma, or liver transplantation rate. Furthermore, TD was not found to affect PBC survival rates, either positively or negatively.
“The results of our study confirm that TDs are often associated with PBC, especially Hashimoto’s thyroiditis, which shares an autoimmune etiology with PBC,” the authors concluded, adding that “More importantly … the clinical characteristics and natural history of PBC were much the same in the two cohorts, as demonstrated by the absence of significant differences regarding histological stage at diagnosis (the only exception being more patients in stage III in the Italian cohort); biochemical data; response to UDCA [ursodeoxycholic acid]; the association with other extrahepatic autoimmune disorders; the occurrence of clinical events; and survival.”
No funding source was reported for this study. Dr. Floreani and her coauthors did not report any financial disclosures relevant to this study.
Key clinical point:
Major finding: 150 of 921 PBC patients had TD (16.3%), but there was no correlation between PBC patients who had TD and their histologic stage either at diagnosis, hepatic decompensation events, occurrence of hepatocelluler carcinoma, or liver transplantation rates.
Data source: Prospective study of 921 PBC patients in Padua and Barcelona from 1975 to 2015.
Disclosures: No funding source was disclosed; authors reported no relevant financial disclosures.
Fragmented readmission after liver transplant linked to adverse outcomes
CORONADO, CALIF. – Postdischarge surgical care fragmentation significantly increases the risk of both 30-day mortality and subsequent readmission in the first year following orthotopic liver transplantation, results from a study of national data showed.
“In an era of regionalization and centers of excellence, the likelihood for postdischarge fragmentation, defined as readmission to any hospital other than the hospital at which the surgery was performed, is an increasing reality,” Anai N. Kothari, MD, said at the annual meeting of the Western Surgical Association. “In many different surgical subspecialties – major vascular operations, bariatric surgery, oncologic resections – it’s known to be a risk factor for adverse events and poor quality. Postdischarge fragmentation is common, [and related to] as often as one in four readmissions. It increases the risk for short- and long-term morbidity and mortality, decreases survival, and increases cost.”
Dr. Kothari reported results from 2,996 patients with 7,485 readmission encounters at 299 hospitals. Of the 7,485 readmissions, 6,249 (83.5%) were nonfragmented, and 1,236 (16.5%) were fragmented. The mean age of patients was 55 years. There were no significant differences in baseline characteristics between patients with nonfragmented and fragmented admissions in terms of patient age, sex, preoperative and postoperative length of stay, Charlson comorbidity index, and comorbidities, with the exception of renal failure, which was more common among patients in the fragmented admission group.
Compared with the patients in the nonfragmented admission group, those in the fragmented admission group had a greater number of average readmissions per patient (3.3 vs. 2.5, respectively; P less than .0001) and a greater number of average days to readmission (168 vs. 105; P less than .0001). Reasons for readmission differed among the two groups. Patients readmitted to the index transplant center were more likely to have a biliary, hematologic, or neurologic complication, while those in the fragmented admissions group were more likely to be readmitted for things like electrolyte disturbances, respiratory issues, gastrointestinal issues, or hematologic-related issues. There was no difference in overall cost of care between the two groups (an average of $11,621.68 vs. $11.585.39, respectively).
After the investigators adjusted for age, sex, reason for readmission, cost of the index liver transplant, readmission length of stay, number of previous readmissions, and time from transplant, postdischarge fragmentation increased the odds of both 30-day mortality (OR, 1.75) and 30-day readmission (OR, 2.14). “It looks like just having a fragmented readmission is an independent predictor for an adverse event,” Dr. Kothari said.
Significant predictors of adverse events following a fragmented readmission included an increased number of previous readmissions (OR, 1.07) and readmission within 90 days of orthotopic liver transplant (OR, 2.19). “These two factors may be important for guiding providers to say, ‘If you have these things, this patient should likely come back to their index transplant center,’” Dr. Kothari said.
He reported having no relevant financial disclosures.
CORONADO, CALIF. – Postdischarge surgical care fragmentation significantly increases the risk of both 30-day mortality and subsequent readmission in the first year following orthotopic liver transplantation, results from a study of national data showed.
“In an era of regionalization and centers of excellence, the likelihood for postdischarge fragmentation, defined as readmission to any hospital other than the hospital at which the surgery was performed, is an increasing reality,” Anai N. Kothari, MD, said at the annual meeting of the Western Surgical Association. “In many different surgical subspecialties – major vascular operations, bariatric surgery, oncologic resections – it’s known to be a risk factor for adverse events and poor quality. Postdischarge fragmentation is common, [and related to] as often as one in four readmissions. It increases the risk for short- and long-term morbidity and mortality, decreases survival, and increases cost.”
Dr. Kothari reported results from 2,996 patients with 7,485 readmission encounters at 299 hospitals. Of the 7,485 readmissions, 6,249 (83.5%) were nonfragmented, and 1,236 (16.5%) were fragmented. The mean age of patients was 55 years. There were no significant differences in baseline characteristics between patients with nonfragmented and fragmented admissions in terms of patient age, sex, preoperative and postoperative length of stay, Charlson comorbidity index, and comorbidities, with the exception of renal failure, which was more common among patients in the fragmented admission group.
Compared with the patients in the nonfragmented admission group, those in the fragmented admission group had a greater number of average readmissions per patient (3.3 vs. 2.5, respectively; P less than .0001) and a greater number of average days to readmission (168 vs. 105; P less than .0001). Reasons for readmission differed among the two groups. Patients readmitted to the index transplant center were more likely to have a biliary, hematologic, or neurologic complication, while those in the fragmented admissions group were more likely to be readmitted for things like electrolyte disturbances, respiratory issues, gastrointestinal issues, or hematologic-related issues. There was no difference in overall cost of care between the two groups (an average of $11,621.68 vs. $11.585.39, respectively).
After the investigators adjusted for age, sex, reason for readmission, cost of the index liver transplant, readmission length of stay, number of previous readmissions, and time from transplant, postdischarge fragmentation increased the odds of both 30-day mortality (OR, 1.75) and 30-day readmission (OR, 2.14). “It looks like just having a fragmented readmission is an independent predictor for an adverse event,” Dr. Kothari said.
Significant predictors of adverse events following a fragmented readmission included an increased number of previous readmissions (OR, 1.07) and readmission within 90 days of orthotopic liver transplant (OR, 2.19). “These two factors may be important for guiding providers to say, ‘If you have these things, this patient should likely come back to their index transplant center,’” Dr. Kothari said.
He reported having no relevant financial disclosures.
CORONADO, CALIF. – Postdischarge surgical care fragmentation significantly increases the risk of both 30-day mortality and subsequent readmission in the first year following orthotopic liver transplantation, results from a study of national data showed.
“In an era of regionalization and centers of excellence, the likelihood for postdischarge fragmentation, defined as readmission to any hospital other than the hospital at which the surgery was performed, is an increasing reality,” Anai N. Kothari, MD, said at the annual meeting of the Western Surgical Association. “In many different surgical subspecialties – major vascular operations, bariatric surgery, oncologic resections – it’s known to be a risk factor for adverse events and poor quality. Postdischarge fragmentation is common, [and related to] as often as one in four readmissions. It increases the risk for short- and long-term morbidity and mortality, decreases survival, and increases cost.”
Dr. Kothari reported results from 2,996 patients with 7,485 readmission encounters at 299 hospitals. Of the 7,485 readmissions, 6,249 (83.5%) were nonfragmented, and 1,236 (16.5%) were fragmented. The mean age of patients was 55 years. There were no significant differences in baseline characteristics between patients with nonfragmented and fragmented admissions in terms of patient age, sex, preoperative and postoperative length of stay, Charlson comorbidity index, and comorbidities, with the exception of renal failure, which was more common among patients in the fragmented admission group.
Compared with the patients in the nonfragmented admission group, those in the fragmented admission group had a greater number of average readmissions per patient (3.3 vs. 2.5, respectively; P less than .0001) and a greater number of average days to readmission (168 vs. 105; P less than .0001). Reasons for readmission differed among the two groups. Patients readmitted to the index transplant center were more likely to have a biliary, hematologic, or neurologic complication, while those in the fragmented admissions group were more likely to be readmitted for things like electrolyte disturbances, respiratory issues, gastrointestinal issues, or hematologic-related issues. There was no difference in overall cost of care between the two groups (an average of $11,621.68 vs. $11.585.39, respectively).
After the investigators adjusted for age, sex, reason for readmission, cost of the index liver transplant, readmission length of stay, number of previous readmissions, and time from transplant, postdischarge fragmentation increased the odds of both 30-day mortality (OR, 1.75) and 30-day readmission (OR, 2.14). “It looks like just having a fragmented readmission is an independent predictor for an adverse event,” Dr. Kothari said.
Significant predictors of adverse events following a fragmented readmission included an increased number of previous readmissions (OR, 1.07) and readmission within 90 days of orthotopic liver transplant (OR, 2.19). “These two factors may be important for guiding providers to say, ‘If you have these things, this patient should likely come back to their index transplant center,’” Dr. Kothari said.
He reported having no relevant financial disclosures.
AT WSA 2016
Key clinical point:
Major finding: After investigators adjusted for numerous variables, postdischarge fragmentation following orthotopic liver transplantation increased the odds of both 30-day mortality (OR, 1.75) and 30-day readmission (OR, 2.14).
Data source: An analysis of data from the Healthcare Cost and Utilization Project State Inpatient Databases for Florida and California between 2006 and 2011 to identify 2,996 patients who underwent orthotopic liver transplantation.
Disclosures: Dr. Kothari reported having no relevant financial disclosures.
FDA approves tenofovir alafenamide for patients with chronic hepatitis B and liver disease
The Food and Drug Administration has approved tenofovir alafenamide (marketed as Vemlidy by Gilead Sciences) for the treatment of adults with chronic hepatitis B virus infection with compensated liver disease.
Tenofovir alafenamide is a novel, targeted prodrug of tenofovir that has demonstrated antiviral efficacy similar to tenofovir disoproxil fumarate (Viread) at significantly lower doses.
Compared with tenofovir disoproxil fumarate, tenofovir alafenamide has “greater plasma stability and more efficiently delivers tenofovir to hepatocytes” which allows tenofovir alafenamide to be administered in daily doses of 25mg while tenofovir disoproxil fumarate requires a dose of 300 mg to be as effective.
In addition, patients treated with tenofovir alafenamide demonstrated “improvements in certain bone and renal laboratory parameters.”
Overall, tenofovir alafenamide was well tolerated. Only 1% of patients discontinued treatment because of adverse events, and the most common adverse events were headache, abdominal pain, fatigue, cough, nausea, and back pain. Vemlidy has a boxed warning in its product label regarding the risks of lactic acidosis/severe hepatomegaly with steatosis and severe acute exacerbation of hepatitis B with discontinuation.
“Vemlidy is the first medication approved to treat this disease in nearly a decade,” said President and Chief Executive Officer of Gilead Sciences John Milligan. “We are excited to offer a new, effective option to help advance long-term care for patients.”
jcraig@frontlinemedcom.com
On Twitter @jessnicolecraig
The Food and Drug Administration has approved tenofovir alafenamide (marketed as Vemlidy by Gilead Sciences) for the treatment of adults with chronic hepatitis B virus infection with compensated liver disease.
Tenofovir alafenamide is a novel, targeted prodrug of tenofovir that has demonstrated antiviral efficacy similar to tenofovir disoproxil fumarate (Viread) at significantly lower doses.
Compared with tenofovir disoproxil fumarate, tenofovir alafenamide has “greater plasma stability and more efficiently delivers tenofovir to hepatocytes” which allows tenofovir alafenamide to be administered in daily doses of 25mg while tenofovir disoproxil fumarate requires a dose of 300 mg to be as effective.
In addition, patients treated with tenofovir alafenamide demonstrated “improvements in certain bone and renal laboratory parameters.”
Overall, tenofovir alafenamide was well tolerated. Only 1% of patients discontinued treatment because of adverse events, and the most common adverse events were headache, abdominal pain, fatigue, cough, nausea, and back pain. Vemlidy has a boxed warning in its product label regarding the risks of lactic acidosis/severe hepatomegaly with steatosis and severe acute exacerbation of hepatitis B with discontinuation.
“Vemlidy is the first medication approved to treat this disease in nearly a decade,” said President and Chief Executive Officer of Gilead Sciences John Milligan. “We are excited to offer a new, effective option to help advance long-term care for patients.”
jcraig@frontlinemedcom.com
On Twitter @jessnicolecraig
The Food and Drug Administration has approved tenofovir alafenamide (marketed as Vemlidy by Gilead Sciences) for the treatment of adults with chronic hepatitis B virus infection with compensated liver disease.
Tenofovir alafenamide is a novel, targeted prodrug of tenofovir that has demonstrated antiviral efficacy similar to tenofovir disoproxil fumarate (Viread) at significantly lower doses.
Compared with tenofovir disoproxil fumarate, tenofovir alafenamide has “greater plasma stability and more efficiently delivers tenofovir to hepatocytes” which allows tenofovir alafenamide to be administered in daily doses of 25mg while tenofovir disoproxil fumarate requires a dose of 300 mg to be as effective.
In addition, patients treated with tenofovir alafenamide demonstrated “improvements in certain bone and renal laboratory parameters.”
Overall, tenofovir alafenamide was well tolerated. Only 1% of patients discontinued treatment because of adverse events, and the most common adverse events were headache, abdominal pain, fatigue, cough, nausea, and back pain. Vemlidy has a boxed warning in its product label regarding the risks of lactic acidosis/severe hepatomegaly with steatosis and severe acute exacerbation of hepatitis B with discontinuation.
“Vemlidy is the first medication approved to treat this disease in nearly a decade,” said President and Chief Executive Officer of Gilead Sciences John Milligan. “We are excited to offer a new, effective option to help advance long-term care for patients.”
jcraig@frontlinemedcom.com
On Twitter @jessnicolecraig