User login
Rashes in Pregnancy
Rashes that develop during pregnancy often result in considerable anxiety or concern for patients and their families. Recognizing these pregnancy-specific dermatoses is important in identifying fetal risks as well as providing appropriate management and expert guidance for patients regarding future pregnancies. Managing cutaneous manifestations of pregnancy-related disorders is challenging and requires knowledge of potential side effects of therapy for both the mother and fetus. It also is important to appreciate the physiologic cutaneous changes of pregnancy along with their clinical significance and management.
In 2006, Ambrose-Rudolph et al1 proposed reclassification of pregnancy-specific dermatoses, which has since been widely accepted by the academic dermatology community. The 4 most prominent disorders include intrahepatic cholestasis of pregnancy (ICP); pemphigoid gestationis (PG); polymorphic eruption of pregnancy (PEP), also known as pruritic urticarial papules and plaques of pregnancy; and atopic eruption of pregnancy.2 It is important to recognize these pregnancy-specific disorders and to understand their clinical significance. The morphology of the eruption as well as the location and timing of the onset of the rash are important clues in making an accurate diagnosis.3
Clinical Presentation
Intrahepatic cholestasis of pregnancy presents with severe generalized pruritus, usually with involvement of the palms and soles, in the late second or third trimester. Pemphigoid gestationis presents with urticarial papules and/or bullae, often in the second or third trimester or postpartum. An important diagnostic clue for PG is involvement near the umbilicus. Polymorphic eruption of pregnancy presents with urticarial papules and plaques; onset occurs in the third trimester or postpartum and initially involves the striae while sparing the umbilicus, unlike in PG. Atopic eruption of pregnancy has an earlier onset than the other pregnancy-specific dermatoses, often in the first or second trimester, and presents with widespread eczematous lesions.3
Diagnosis
The pregnancy dermatoses with the greatest potential for fetal risks are ICP and PG; therefore, it is critical for health care providers to diagnose these dermatoses in a timely manner and initiate appropriate management. Intrahepatic cholestasis of pregnancy is confirmed by elevated serum bile acids (ie, >10 µmol/L), often during the third trimester. The risk of fetal morbidity is high in ICP with increased bile acids crossing the placenta causing placental anoxia and impaired cardiomyocyte function.4 Fetal risks, including preterm delivery, meconium-stained amniotic fluid, and stillbirth, correlate with the level of bile acids in the serum.5 Maternal prognosis is favorable, but there is an increased association with hepatitis C and hepatobiliary disease.6
Diagnosis of PG is confirmed by classic biopsy results and direct immunofluorescence revealing C3 with or without IgG in a linear band along the basement membrane zone. Additionally, complement indirect immunofluorescence reveals circulating IgG anti–basement membrane zone antibodies. Pemphigoid gestationis is associated with increased fetal risks of preterm labor and intrauterine growth retardation.7 Clinical findings of PG may present in the fetus upon delivery due to transmission of autoantibodies across the placenta. The symptoms usually are mild.8 An increased risk of Graves disease has been reported in mothers with PG.
In most cases, diagnosis of PEP is based on history and morphology, but if the presentation is not classic, skin biopsy must be used to differentiate it from PG as well as more common dermatologic conditions such as contact dermatitis, drug and viral eruptions, and urticaria.
Atopic eruption of pregnancy manifests as widespread eczematous excoriated papules and plaques. Lesions of prurigo nodularis are common.
Comorbidities
It is important to be aware of specific clinical associations related to pregnancy-specific dermatoses. Pemphigoid gestationis has been associated with gestational trophoblastic tumors including hydatiform mole and choriocarcinoma.4 An increased risk for Graves disease has been reported in patients with PG.9 Patients who develop ICP have a higher incidence of hepatitis C, postpartum cholecystitis, gallstones, and nonalcoholic cirrhosis.8 Polymorphic eruption of pregnancy is associated with a notably higher incidence in multiple gestation pregnancies.2
Treatment and Management
Management of ICP requires an accurate and timely diagnosis, and advanced neonatal-obstetric management is critical.3 Ursodeoxycholic acid is the treatment of choice and reduces pruritus, prolongs pregnancy, and reduces fetal risk.4 Most stillbirths cluster at the 38th week of pregnancy, and patients with ICP and highly elevated serum bile acids (>40 µmol/L) should be considered for delivery at 37 weeks or earlier.5
Management of the other cutaneous disorders of pregnancy can be challenging for health care providers based on safety concerns for the fetus. Although it is important to minimize risks to the fetus, it also is important to adequately treat the mother’s cutaneous disease, which requires a solid knowledge of drug safety during pregnancy. The former US Food and Drug Administration classification system using A, B, C, D, and X pregnancy categories was replaced by the Pregnancy Lactation Label Final Rule, which provides counseling on medication safety during pregnancy.10 In 2014, Murase et al11 published a review of dermatologic medication safety during pregnancy, which serves as an excellent guide.
Before instituting treatment, the therapeutic plan should be discussed with the physician managing the patient’s pregnancy. In general, topical steroids are considered safe during pregnancy, and low-potency to moderate-potency topical steroids are preferred. If possible, use of topical steroids should be limited to less than 300 g for the duration of the pregnancy. Fluticasone propionate should be avoided during pregnancy because it is not metabolized by the placenta. When systemic steroids are considered appropriate for management during pregnancy, nonhalogenated corticosteroids such as prednisone and prednisolone are preferred because they are enzymatically inactivated by the placenta, which results in a favorable maternal-fetal gradient.12 There has been concern expressed in the medical literature that systemic steroids during the first trimester may increase the risk of cleft lip and cleft palate.3,12 When managing pregnancy dermatoses, consideration should be given to keep prednisone exposure below 20 mg/d, and try to limit prolonged use to 7.5 mg/d. However, this may not be possible in PG.3 Vitamin D and calcium supplementation may be appropriate when patients are on prolonged systemic steroids to control disease.
Antihistamines can be used to control pruritus complicating pregnancy-associated dermatoses. First-generation antihistamines such as chlorpheniramine and diphenhydramine are preferred due to long-term safety data.3,11,12 Loratadine is the first choice and cetirizine is the second choice if a second-generation antihistamine is preferred.3 Loratadine is preferred during breastfeeding due to less sedation.12 High-dose antihistamines prior to delivery may cause concerns for potential side effects in the newborn, including tremulousness, irritability, and poor feeding.
Recurrence
Women with pregnancy dermatoses often are concerned about recurrence with future pregnancies. Pemphigoid gestationis may flare with subsequent pregnancies, subsequent menses, or with oral contraceptive use.3 Recurrence of PEP in subsequent pregnancies is rare and usually is less severe than the primary eruption.8 Often, the rare recurrent eruption of PEP is associated with multigestational pregnancies.2 Mothers can anticipate a recurrence of ICP in up to 60% to 70% of future pregnancies. Patients with AEP have an underlying atopic diathesis, and recurrence in future pregnancies is not uncommon.8
Final Thoughts
In summary, it is important for health care providers to recognize the specific cutaneous disorders of pregnancy and their potential fetal complications. The anatomical location of onset of the dermatosis and timing of onset during pregnancy can give important clues. Appropriate management, especially with ICP, can minimize fetal complications. A fundamental knowledge of medication safety and management during pregnancy is essential. Rashes during pregnancy can cause anxiety in the mother and family and require support, comfort, and guidance.
- Ambrose-Rudolph CM, Müllegger RR, Vaughn-Jones SA, et al. The specific dermatoses of pregnancy revisited and reclassified: results of a retrospective two-center study on 505 pregnant patients. J Am Acad Dermatol. 2006;54:395-404.
- Bechtel M, Plotner A. Dermatoses of pregnancy. Clin Obstet Gynecol. 2015;58:104-111.
- Bechtel M. Pruritus in pregnancy and its management. Dermatol Clin. 2018;36:259-265.
- Ambrose-Rudolph CM. Dermatoses of pregnancy—clues to diagnosis, fetal risk, and therapy. Ann Dermatol. 2011;23:265-275.
- Geenes V, Chappell LC, Seed PT, et al. Association of severe intrahepatic cholestasis of pregnancy with adverse pregnancy outcomes: a prospective population-based case-controlled study. Hepatology. 2014;59:1482-1491.
- Bergman H, Melamed N, Koven G. Pruritus in pregnancy: treatment of dermatoses unique to pregnancy. Can Fam Physician. 2013;59:1290-1294.
- Beard MP, Millington GW. Recent developments in the specific dermatoses of pregnancy. Clin Exp Dermatol. 2012;37:1-14.
- Shears S, Blaszczak A, Kaffenberger J. Pregnancy dermatosis. In: Tyler KH, ed. Cutaneous Disorders of Pregnancy. 1st ed. Springer Nature; 2020:13-39.
- Lehrhoff S, Pomeranz MK. Specific dermatoses of pregnancy and their treatment. Dermatol Ther. 2015;26:274-284.
- Content and format of labeling for human prescription drug and biological products; requirements for pregnancy and lactation labeling. Fed Registr. 2014;79:72064-72103. To be codified at 21 CFR § 201.
- Murase JE, Heller MM, Butler DC. Safety of dermatologic medications in pregnancy and lactation: part 1. pregnancy. J Am Acad Dermatol. 2014;401:E1-E14.
- Friedman B, Bercovitch L. Atopic dermatitis in pregnancy. In: Tyler KH, ed. Cutaneous Disorders of Pregnancy. Springer Nature; 2020:59-74.
Rashes that develop during pregnancy often result in considerable anxiety or concern for patients and their families. Recognizing these pregnancy-specific dermatoses is important in identifying fetal risks as well as providing appropriate management and expert guidance for patients regarding future pregnancies. Managing cutaneous manifestations of pregnancy-related disorders is challenging and requires knowledge of potential side effects of therapy for both the mother and fetus. It also is important to appreciate the physiologic cutaneous changes of pregnancy along with their clinical significance and management.
In 2006, Ambrose-Rudolph et al1 proposed reclassification of pregnancy-specific dermatoses, which has since been widely accepted by the academic dermatology community. The 4 most prominent disorders include intrahepatic cholestasis of pregnancy (ICP); pemphigoid gestationis (PG); polymorphic eruption of pregnancy (PEP), also known as pruritic urticarial papules and plaques of pregnancy; and atopic eruption of pregnancy.2 It is important to recognize these pregnancy-specific disorders and to understand their clinical significance. The morphology of the eruption as well as the location and timing of the onset of the rash are important clues in making an accurate diagnosis.3
Clinical Presentation
Intrahepatic cholestasis of pregnancy presents with severe generalized pruritus, usually with involvement of the palms and soles, in the late second or third trimester. Pemphigoid gestationis presents with urticarial papules and/or bullae, often in the second or third trimester or postpartum. An important diagnostic clue for PG is involvement near the umbilicus. Polymorphic eruption of pregnancy presents with urticarial papules and plaques; onset occurs in the third trimester or postpartum and initially involves the striae while sparing the umbilicus, unlike in PG. Atopic eruption of pregnancy has an earlier onset than the other pregnancy-specific dermatoses, often in the first or second trimester, and presents with widespread eczematous lesions.3
Diagnosis
The pregnancy dermatoses with the greatest potential for fetal risks are ICP and PG; therefore, it is critical for health care providers to diagnose these dermatoses in a timely manner and initiate appropriate management. Intrahepatic cholestasis of pregnancy is confirmed by elevated serum bile acids (ie, >10 µmol/L), often during the third trimester. The risk of fetal morbidity is high in ICP with increased bile acids crossing the placenta causing placental anoxia and impaired cardiomyocyte function.4 Fetal risks, including preterm delivery, meconium-stained amniotic fluid, and stillbirth, correlate with the level of bile acids in the serum.5 Maternal prognosis is favorable, but there is an increased association with hepatitis C and hepatobiliary disease.6
Diagnosis of PG is confirmed by classic biopsy results and direct immunofluorescence revealing C3 with or without IgG in a linear band along the basement membrane zone. Additionally, complement indirect immunofluorescence reveals circulating IgG anti–basement membrane zone antibodies. Pemphigoid gestationis is associated with increased fetal risks of preterm labor and intrauterine growth retardation.7 Clinical findings of PG may present in the fetus upon delivery due to transmission of autoantibodies across the placenta. The symptoms usually are mild.8 An increased risk of Graves disease has been reported in mothers with PG.
In most cases, diagnosis of PEP is based on history and morphology, but if the presentation is not classic, skin biopsy must be used to differentiate it from PG as well as more common dermatologic conditions such as contact dermatitis, drug and viral eruptions, and urticaria.
Atopic eruption of pregnancy manifests as widespread eczematous excoriated papules and plaques. Lesions of prurigo nodularis are common.
Comorbidities
It is important to be aware of specific clinical associations related to pregnancy-specific dermatoses. Pemphigoid gestationis has been associated with gestational trophoblastic tumors including hydatiform mole and choriocarcinoma.4 An increased risk for Graves disease has been reported in patients with PG.9 Patients who develop ICP have a higher incidence of hepatitis C, postpartum cholecystitis, gallstones, and nonalcoholic cirrhosis.8 Polymorphic eruption of pregnancy is associated with a notably higher incidence in multiple gestation pregnancies.2
Treatment and Management
Management of ICP requires an accurate and timely diagnosis, and advanced neonatal-obstetric management is critical.3 Ursodeoxycholic acid is the treatment of choice and reduces pruritus, prolongs pregnancy, and reduces fetal risk.4 Most stillbirths cluster at the 38th week of pregnancy, and patients with ICP and highly elevated serum bile acids (>40 µmol/L) should be considered for delivery at 37 weeks or earlier.5
Management of the other cutaneous disorders of pregnancy can be challenging for health care providers based on safety concerns for the fetus. Although it is important to minimize risks to the fetus, it also is important to adequately treat the mother’s cutaneous disease, which requires a solid knowledge of drug safety during pregnancy. The former US Food and Drug Administration classification system using A, B, C, D, and X pregnancy categories was replaced by the Pregnancy Lactation Label Final Rule, which provides counseling on medication safety during pregnancy.10 In 2014, Murase et al11 published a review of dermatologic medication safety during pregnancy, which serves as an excellent guide.
Before instituting treatment, the therapeutic plan should be discussed with the physician managing the patient’s pregnancy. In general, topical steroids are considered safe during pregnancy, and low-potency to moderate-potency topical steroids are preferred. If possible, use of topical steroids should be limited to less than 300 g for the duration of the pregnancy. Fluticasone propionate should be avoided during pregnancy because it is not metabolized by the placenta. When systemic steroids are considered appropriate for management during pregnancy, nonhalogenated corticosteroids such as prednisone and prednisolone are preferred because they are enzymatically inactivated by the placenta, which results in a favorable maternal-fetal gradient.12 There has been concern expressed in the medical literature that systemic steroids during the first trimester may increase the risk of cleft lip and cleft palate.3,12 When managing pregnancy dermatoses, consideration should be given to keep prednisone exposure below 20 mg/d, and try to limit prolonged use to 7.5 mg/d. However, this may not be possible in PG.3 Vitamin D and calcium supplementation may be appropriate when patients are on prolonged systemic steroids to control disease.
Antihistamines can be used to control pruritus complicating pregnancy-associated dermatoses. First-generation antihistamines such as chlorpheniramine and diphenhydramine are preferred due to long-term safety data.3,11,12 Loratadine is the first choice and cetirizine is the second choice if a second-generation antihistamine is preferred.3 Loratadine is preferred during breastfeeding due to less sedation.12 High-dose antihistamines prior to delivery may cause concerns for potential side effects in the newborn, including tremulousness, irritability, and poor feeding.
Recurrence
Women with pregnancy dermatoses often are concerned about recurrence with future pregnancies. Pemphigoid gestationis may flare with subsequent pregnancies, subsequent menses, or with oral contraceptive use.3 Recurrence of PEP in subsequent pregnancies is rare and usually is less severe than the primary eruption.8 Often, the rare recurrent eruption of PEP is associated with multigestational pregnancies.2 Mothers can anticipate a recurrence of ICP in up to 60% to 70% of future pregnancies. Patients with AEP have an underlying atopic diathesis, and recurrence in future pregnancies is not uncommon.8
Final Thoughts
In summary, it is important for health care providers to recognize the specific cutaneous disorders of pregnancy and their potential fetal complications. The anatomical location of onset of the dermatosis and timing of onset during pregnancy can give important clues. Appropriate management, especially with ICP, can minimize fetal complications. A fundamental knowledge of medication safety and management during pregnancy is essential. Rashes during pregnancy can cause anxiety in the mother and family and require support, comfort, and guidance.
Rashes that develop during pregnancy often result in considerable anxiety or concern for patients and their families. Recognizing these pregnancy-specific dermatoses is important in identifying fetal risks as well as providing appropriate management and expert guidance for patients regarding future pregnancies. Managing cutaneous manifestations of pregnancy-related disorders is challenging and requires knowledge of potential side effects of therapy for both the mother and fetus. It also is important to appreciate the physiologic cutaneous changes of pregnancy along with their clinical significance and management.
In 2006, Ambrose-Rudolph et al1 proposed reclassification of pregnancy-specific dermatoses, which has since been widely accepted by the academic dermatology community. The 4 most prominent disorders include intrahepatic cholestasis of pregnancy (ICP); pemphigoid gestationis (PG); polymorphic eruption of pregnancy (PEP), also known as pruritic urticarial papules and plaques of pregnancy; and atopic eruption of pregnancy.2 It is important to recognize these pregnancy-specific disorders and to understand their clinical significance. The morphology of the eruption as well as the location and timing of the onset of the rash are important clues in making an accurate diagnosis.3
Clinical Presentation
Intrahepatic cholestasis of pregnancy presents with severe generalized pruritus, usually with involvement of the palms and soles, in the late second or third trimester. Pemphigoid gestationis presents with urticarial papules and/or bullae, often in the second or third trimester or postpartum. An important diagnostic clue for PG is involvement near the umbilicus. Polymorphic eruption of pregnancy presents with urticarial papules and plaques; onset occurs in the third trimester or postpartum and initially involves the striae while sparing the umbilicus, unlike in PG. Atopic eruption of pregnancy has an earlier onset than the other pregnancy-specific dermatoses, often in the first or second trimester, and presents with widespread eczematous lesions.3
Diagnosis
The pregnancy dermatoses with the greatest potential for fetal risks are ICP and PG; therefore, it is critical for health care providers to diagnose these dermatoses in a timely manner and initiate appropriate management. Intrahepatic cholestasis of pregnancy is confirmed by elevated serum bile acids (ie, >10 µmol/L), often during the third trimester. The risk of fetal morbidity is high in ICP with increased bile acids crossing the placenta causing placental anoxia and impaired cardiomyocyte function.4 Fetal risks, including preterm delivery, meconium-stained amniotic fluid, and stillbirth, correlate with the level of bile acids in the serum.5 Maternal prognosis is favorable, but there is an increased association with hepatitis C and hepatobiliary disease.6
Diagnosis of PG is confirmed by classic biopsy results and direct immunofluorescence revealing C3 with or without IgG in a linear band along the basement membrane zone. Additionally, complement indirect immunofluorescence reveals circulating IgG anti–basement membrane zone antibodies. Pemphigoid gestationis is associated with increased fetal risks of preterm labor and intrauterine growth retardation.7 Clinical findings of PG may present in the fetus upon delivery due to transmission of autoantibodies across the placenta. The symptoms usually are mild.8 An increased risk of Graves disease has been reported in mothers with PG.
In most cases, diagnosis of PEP is based on history and morphology, but if the presentation is not classic, skin biopsy must be used to differentiate it from PG as well as more common dermatologic conditions such as contact dermatitis, drug and viral eruptions, and urticaria.
Atopic eruption of pregnancy manifests as widespread eczematous excoriated papules and plaques. Lesions of prurigo nodularis are common.
Comorbidities
It is important to be aware of specific clinical associations related to pregnancy-specific dermatoses. Pemphigoid gestationis has been associated with gestational trophoblastic tumors including hydatiform mole and choriocarcinoma.4 An increased risk for Graves disease has been reported in patients with PG.9 Patients who develop ICP have a higher incidence of hepatitis C, postpartum cholecystitis, gallstones, and nonalcoholic cirrhosis.8 Polymorphic eruption of pregnancy is associated with a notably higher incidence in multiple gestation pregnancies.2
Treatment and Management
Management of ICP requires an accurate and timely diagnosis, and advanced neonatal-obstetric management is critical.3 Ursodeoxycholic acid is the treatment of choice and reduces pruritus, prolongs pregnancy, and reduces fetal risk.4 Most stillbirths cluster at the 38th week of pregnancy, and patients with ICP and highly elevated serum bile acids (>40 µmol/L) should be considered for delivery at 37 weeks or earlier.5
Management of the other cutaneous disorders of pregnancy can be challenging for health care providers based on safety concerns for the fetus. Although it is important to minimize risks to the fetus, it also is important to adequately treat the mother’s cutaneous disease, which requires a solid knowledge of drug safety during pregnancy. The former US Food and Drug Administration classification system using A, B, C, D, and X pregnancy categories was replaced by the Pregnancy Lactation Label Final Rule, which provides counseling on medication safety during pregnancy.10 In 2014, Murase et al11 published a review of dermatologic medication safety during pregnancy, which serves as an excellent guide.
Before instituting treatment, the therapeutic plan should be discussed with the physician managing the patient’s pregnancy. In general, topical steroids are considered safe during pregnancy, and low-potency to moderate-potency topical steroids are preferred. If possible, use of topical steroids should be limited to less than 300 g for the duration of the pregnancy. Fluticasone propionate should be avoided during pregnancy because it is not metabolized by the placenta. When systemic steroids are considered appropriate for management during pregnancy, nonhalogenated corticosteroids such as prednisone and prednisolone are preferred because they are enzymatically inactivated by the placenta, which results in a favorable maternal-fetal gradient.12 There has been concern expressed in the medical literature that systemic steroids during the first trimester may increase the risk of cleft lip and cleft palate.3,12 When managing pregnancy dermatoses, consideration should be given to keep prednisone exposure below 20 mg/d, and try to limit prolonged use to 7.5 mg/d. However, this may not be possible in PG.3 Vitamin D and calcium supplementation may be appropriate when patients are on prolonged systemic steroids to control disease.
Antihistamines can be used to control pruritus complicating pregnancy-associated dermatoses. First-generation antihistamines such as chlorpheniramine and diphenhydramine are preferred due to long-term safety data.3,11,12 Loratadine is the first choice and cetirizine is the second choice if a second-generation antihistamine is preferred.3 Loratadine is preferred during breastfeeding due to less sedation.12 High-dose antihistamines prior to delivery may cause concerns for potential side effects in the newborn, including tremulousness, irritability, and poor feeding.
Recurrence
Women with pregnancy dermatoses often are concerned about recurrence with future pregnancies. Pemphigoid gestationis may flare with subsequent pregnancies, subsequent menses, or with oral contraceptive use.3 Recurrence of PEP in subsequent pregnancies is rare and usually is less severe than the primary eruption.8 Often, the rare recurrent eruption of PEP is associated with multigestational pregnancies.2 Mothers can anticipate a recurrence of ICP in up to 60% to 70% of future pregnancies. Patients with AEP have an underlying atopic diathesis, and recurrence in future pregnancies is not uncommon.8
Final Thoughts
In summary, it is important for health care providers to recognize the specific cutaneous disorders of pregnancy and their potential fetal complications. The anatomical location of onset of the dermatosis and timing of onset during pregnancy can give important clues. Appropriate management, especially with ICP, can minimize fetal complications. A fundamental knowledge of medication safety and management during pregnancy is essential. Rashes during pregnancy can cause anxiety in the mother and family and require support, comfort, and guidance.
- Ambrose-Rudolph CM, Müllegger RR, Vaughn-Jones SA, et al. The specific dermatoses of pregnancy revisited and reclassified: results of a retrospective two-center study on 505 pregnant patients. J Am Acad Dermatol. 2006;54:395-404.
- Bechtel M, Plotner A. Dermatoses of pregnancy. Clin Obstet Gynecol. 2015;58:104-111.
- Bechtel M. Pruritus in pregnancy and its management. Dermatol Clin. 2018;36:259-265.
- Ambrose-Rudolph CM. Dermatoses of pregnancy—clues to diagnosis, fetal risk, and therapy. Ann Dermatol. 2011;23:265-275.
- Geenes V, Chappell LC, Seed PT, et al. Association of severe intrahepatic cholestasis of pregnancy with adverse pregnancy outcomes: a prospective population-based case-controlled study. Hepatology. 2014;59:1482-1491.
- Bergman H, Melamed N, Koven G. Pruritus in pregnancy: treatment of dermatoses unique to pregnancy. Can Fam Physician. 2013;59:1290-1294.
- Beard MP, Millington GW. Recent developments in the specific dermatoses of pregnancy. Clin Exp Dermatol. 2012;37:1-14.
- Shears S, Blaszczak A, Kaffenberger J. Pregnancy dermatosis. In: Tyler KH, ed. Cutaneous Disorders of Pregnancy. 1st ed. Springer Nature; 2020:13-39.
- Lehrhoff S, Pomeranz MK. Specific dermatoses of pregnancy and their treatment. Dermatol Ther. 2015;26:274-284.
- Content and format of labeling for human prescription drug and biological products; requirements for pregnancy and lactation labeling. Fed Registr. 2014;79:72064-72103. To be codified at 21 CFR § 201.
- Murase JE, Heller MM, Butler DC. Safety of dermatologic medications in pregnancy and lactation: part 1. pregnancy. J Am Acad Dermatol. 2014;401:E1-E14.
- Friedman B, Bercovitch L. Atopic dermatitis in pregnancy. In: Tyler KH, ed. Cutaneous Disorders of Pregnancy. Springer Nature; 2020:59-74.
- Ambrose-Rudolph CM, Müllegger RR, Vaughn-Jones SA, et al. The specific dermatoses of pregnancy revisited and reclassified: results of a retrospective two-center study on 505 pregnant patients. J Am Acad Dermatol. 2006;54:395-404.
- Bechtel M, Plotner A. Dermatoses of pregnancy. Clin Obstet Gynecol. 2015;58:104-111.
- Bechtel M. Pruritus in pregnancy and its management. Dermatol Clin. 2018;36:259-265.
- Ambrose-Rudolph CM. Dermatoses of pregnancy—clues to diagnosis, fetal risk, and therapy. Ann Dermatol. 2011;23:265-275.
- Geenes V, Chappell LC, Seed PT, et al. Association of severe intrahepatic cholestasis of pregnancy with adverse pregnancy outcomes: a prospective population-based case-controlled study. Hepatology. 2014;59:1482-1491.
- Bergman H, Melamed N, Koven G. Pruritus in pregnancy: treatment of dermatoses unique to pregnancy. Can Fam Physician. 2013;59:1290-1294.
- Beard MP, Millington GW. Recent developments in the specific dermatoses of pregnancy. Clin Exp Dermatol. 2012;37:1-14.
- Shears S, Blaszczak A, Kaffenberger J. Pregnancy dermatosis. In: Tyler KH, ed. Cutaneous Disorders of Pregnancy. 1st ed. Springer Nature; 2020:13-39.
- Lehrhoff S, Pomeranz MK. Specific dermatoses of pregnancy and their treatment. Dermatol Ther. 2015;26:274-284.
- Content and format of labeling for human prescription drug and biological products; requirements for pregnancy and lactation labeling. Fed Registr. 2014;79:72064-72103. To be codified at 21 CFR § 201.
- Murase JE, Heller MM, Butler DC. Safety of dermatologic medications in pregnancy and lactation: part 1. pregnancy. J Am Acad Dermatol. 2014;401:E1-E14.
- Friedman B, Bercovitch L. Atopic dermatitis in pregnancy. In: Tyler KH, ed. Cutaneous Disorders of Pregnancy. Springer Nature; 2020:59-74.
Dupilumab-Induced Facial Flushing After Alcohol Consumption
Dupilumab is a fully humanized monoclonal antibody to the α subunit of the IL-4 receptor that inhibits the action of helper T cell (TH2)–type cytokines IL-4 and IL-13. Dupilumab was approved by the US Food and Drug Administration (FDA) in 2017 for the treatment of moderate to severe atopic dermatitis (AD). We report 2 patients with AD who were treated with dupilumab and subsequently developed facial flushing after consuming alcohol.
Case Report
Patient 1
A 24-year-old woman presented to the dermatology clinic with a lifelong history of moderate to severe AD. She had a medical history of asthma and seasonal allergies, which were treated with fexofenadine and an inhaler, as needed. The patient had an affected body surface area of approximately 70% and had achieved only partial relief with topical corticosteroids and topical calcineurin inhibitors.
Because her disease was severe, the patient was started on dupilumab at FDA-approved dosing for AD: a 600-mg subcutaneous (SC) loading dose, followed by 300 mg SC every 2 weeks. She reported rapid skin clearance within 2 weeks of the start of treatment. Her course was complicated by mild head and neck dermatitis.
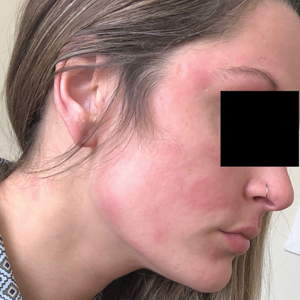
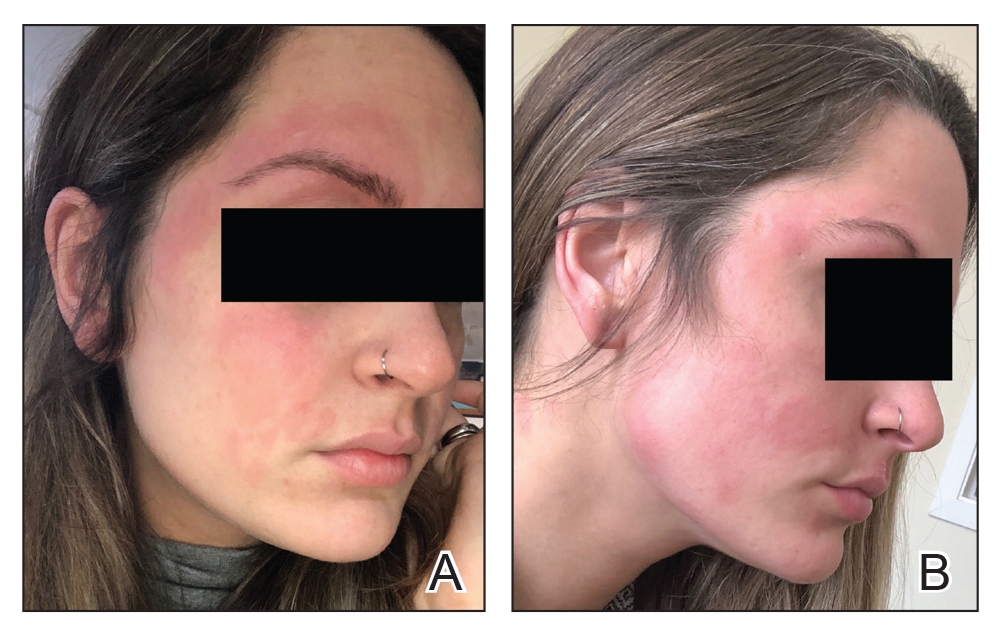
Seven months after starting treatment, the patient began to acutely experience erythema and warmth over the entire face that was triggered by drinking alcohol (Figure). Before starting dupilumab, she had consumed alcohol on multiple occasions without a flushing effect. This new finding was distinguishable from her facial dermatitis. Onset was within a few minutes after drinking alcohol; flushing self-resolved in 15 to 30 minutes. Although diffuse, erythema and warmth were concentrated around the jawline, eyebrows, and ears and occurred every time the patient drank alcohol. Moreover, she reported that consumption of hard (ie, distilled) liquor, specifically tequila, caused a more severe presentation. She denied other symptoms associated with dupilumab.
Patient 2
A 32-year-old man presented to the dermatology clinic with a 10-year history of moderate to severe AD. He had a medical history of asthma (treated with albuterol, montelukast, and fluticasone); allergic rhinitis; and severe environmental allergies, including sensitivity to dust mites, dogs, trees, and grass.
For AD, the patient had been treated with topical corticosteroids and the Goeckerman regimen (a combination of phototherapy and crude coal tar). He experienced only partial relief with topical corticosteroids; the Goeckerman regimen cleared his skin, but he had quick recurrence after approximately 1 month. Given his work schedule, the patient was unable to resume phototherapy.
Because of symptoms related to the patient’s severe allergies, his allergist prescribed dupilumab: a 600-mg SC loading dose, followed by 300 mg SC every 2 weeks. The patient reported near-complete resolution of AD symptoms approximately 2 months after initiating treatment. He reported a few episodes of mild conjunctivitis that self-resolved after the first month of treatment.
Three weeks after initiating dupilumab, the patient noticed new-onset facial flushing in response to consuming alcohol. He described flushing as sudden immediate redness and warmth concentrated around the forehead, eyes, and cheeks. He reported that flushing was worse with hard liquor than with beer. Flushing would slowly subside over approximately 30 minutes despite continued alcohol consumption.
Comment
Two other single-patient case reports have discussed similar findings of alcohol-induced flushing associated with dupilumab.1,2 Both of those patients—a 19-year-old woman and a 26-year-old woman—had not experienced flushing before beginning treatment with dupilumab for AD. Both experienced onset of facial flushing months after beginning dupilumab even though both had consumed alcohol before starting dupilumab, similar to the cases presented here. One patient had a history of asthma; the other had a history of seasonal and environmental allergies.
Possible Mechanism of Action
Acute alcohol ingestion causes dermal vasodilation of the skin (ie, flushing).3 A proposed mechanism is that flushing results from direct action on central vascular-control mechanisms. This theory results from observations that individuals with quadriplegia lack notable ethanol-induced vasodilation, suggesting that ethanol has a central neural site of action.Although some research has indicated that ethanol might induce these effects by altering the action of certain hormones (eg, angiotensin, vasopressin, and catecholamines), the precise mechanism by which ethanol alters vascular function in humans remains unexplained.3
Deficiencies in alcohol dehydrogenase (ADH), aldehyde dehydrogenase 2, and certain cytochrome P450 enzymes also might contribute to facial flushing. People of Asian, especially East Asian, descent often respond to an acute dose of ethanol with symptoms of facial flushing—predominantly the result of an elevated blood level of acetaldehyde caused by an inherited deficiency of aldehyde dehydrogenase 2,4 which is downstream from ADH in the metabolic pathway of alcohol. The major enzyme system responsible for metabolism of ethanol is ADH; however, the cytochrome P450–dependent ethanol-oxidizing system—including major CYP450 isoforms CYP3A, CYP2C19, CYP2C9, CYP1A2, and CYP2D6, as well as minor CYP450 isoforms, such as CYP2E1— also are involved, to a lesser extent.5
A Role for Dupilumab?
A recent pharmacokinetic study found that dupilumab appears to have little effect on the activity of the major CYP450 isoforms. However, the drug’s effect on ADH and minor CYP450 minor isoforms is unknown. Prior drug-drug interaction studies have shown that certain cytokines and cytokine modulators can markedly influence the expression, stability, and activity of specific CYP450 enzymes.6 For example, IL-6 causes a reduction in messenger RNA for CYP3A4 and, to a lesser extent, for other isoforms.7 Whether dupilumab influences enzymes involved in processing alcohol requires further study.
Conclusion
We describe 2 cases of dupilumab-induced facial flushing after alcohol consumption. The mechanism of this dupilumab-associated flushing is unknown and requires further research.
- Herz S, Petri M, Sondermann W. New alcohol flushing in a patient with atopic dermatitis under therapy with dupilumab. Dermatol Ther. 2019;32:e12762. doi:10.1111/dth.12762
- Igelman SJ, Na C, Simpson EL. Alcohol-induced facial flushing in a patient with atopic dermatitis treated with dupilumab. JAAD Case Rep. 2020;6:139-140. doi:10.1016/j.jdcr.2019.12.002
- Malpas SC, Robinson BJ, Maling TJ. Mechanism of ethanol-induced vasodilation. J Appl Physiol (1985). 1990;68:731-734. doi:10.1152/jappl.1990.68.2.731
- Brooks PJ, Enoch M-A, Goldman D, et al. The alcohol flushing response: an unrecognized risk factor for esophageal cancer from alcohol consumption. PLoS Med. 2009;6:e50. doi:10.1371/journal.pmed.1000050
- Cederbaum AI. Alcohol metabolism. Clin Liver Dis. 2012;16:667-685. doi:10.1016/j.cld.2012.08.002
- Davis JD, Bansal A, Hassman D, et al. Evaluation of potential disease-mediated drug-drug interaction in patients with moderate-to-severe atopic dermatitis receiving dupilumab. Clin Pharmacol Ther. 2018;104:1146-1154. doi:10.1002/cpt.1058
- Mimura H, Kobayashi K, Xu L, et al. Effects of cytokines on CYP3A4 expression and reversal of the effects by anti-cytokine agents in the three-dimensionally cultured human hepatoma cell line FLC-4. Drug Metab Pharmacokinet. 2015;30:105-110. doi:10.1016/j.dmpk.2014.09.004
Dupilumab is a fully humanized monoclonal antibody to the α subunit of the IL-4 receptor that inhibits the action of helper T cell (TH2)–type cytokines IL-4 and IL-13. Dupilumab was approved by the US Food and Drug Administration (FDA) in 2017 for the treatment of moderate to severe atopic dermatitis (AD). We report 2 patients with AD who were treated with dupilumab and subsequently developed facial flushing after consuming alcohol.
Case Report
Patient 1
A 24-year-old woman presented to the dermatology clinic with a lifelong history of moderate to severe AD. She had a medical history of asthma and seasonal allergies, which were treated with fexofenadine and an inhaler, as needed. The patient had an affected body surface area of approximately 70% and had achieved only partial relief with topical corticosteroids and topical calcineurin inhibitors.
Because her disease was severe, the patient was started on dupilumab at FDA-approved dosing for AD: a 600-mg subcutaneous (SC) loading dose, followed by 300 mg SC every 2 weeks. She reported rapid skin clearance within 2 weeks of the start of treatment. Her course was complicated by mild head and neck dermatitis.
Seven months after starting treatment, the patient began to acutely experience erythema and warmth over the entire face that was triggered by drinking alcohol (Figure). Before starting dupilumab, she had consumed alcohol on multiple occasions without a flushing effect. This new finding was distinguishable from her facial dermatitis. Onset was within a few minutes after drinking alcohol; flushing self-resolved in 15 to 30 minutes. Although diffuse, erythema and warmth were concentrated around the jawline, eyebrows, and ears and occurred every time the patient drank alcohol. Moreover, she reported that consumption of hard (ie, distilled) liquor, specifically tequila, caused a more severe presentation. She denied other symptoms associated with dupilumab.

Patient 2
A 32-year-old man presented to the dermatology clinic with a 10-year history of moderate to severe AD. He had a medical history of asthma (treated with albuterol, montelukast, and fluticasone); allergic rhinitis; and severe environmental allergies, including sensitivity to dust mites, dogs, trees, and grass.
For AD, the patient had been treated with topical corticosteroids and the Goeckerman regimen (a combination of phototherapy and crude coal tar). He experienced only partial relief with topical corticosteroids; the Goeckerman regimen cleared his skin, but he had quick recurrence after approximately 1 month. Given his work schedule, the patient was unable to resume phototherapy.
Because of symptoms related to the patient’s severe allergies, his allergist prescribed dupilumab: a 600-mg SC loading dose, followed by 300 mg SC every 2 weeks. The patient reported near-complete resolution of AD symptoms approximately 2 months after initiating treatment. He reported a few episodes of mild conjunctivitis that self-resolved after the first month of treatment.
Three weeks after initiating dupilumab, the patient noticed new-onset facial flushing in response to consuming alcohol. He described flushing as sudden immediate redness and warmth concentrated around the forehead, eyes, and cheeks. He reported that flushing was worse with hard liquor than with beer. Flushing would slowly subside over approximately 30 minutes despite continued alcohol consumption.
Comment
Two other single-patient case reports have discussed similar findings of alcohol-induced flushing associated with dupilumab.1,2 Both of those patients—a 19-year-old woman and a 26-year-old woman—had not experienced flushing before beginning treatment with dupilumab for AD. Both experienced onset of facial flushing months after beginning dupilumab even though both had consumed alcohol before starting dupilumab, similar to the cases presented here. One patient had a history of asthma; the other had a history of seasonal and environmental allergies.
Possible Mechanism of Action
Acute alcohol ingestion causes dermal vasodilation of the skin (ie, flushing).3 A proposed mechanism is that flushing results from direct action on central vascular-control mechanisms. This theory results from observations that individuals with quadriplegia lack notable ethanol-induced vasodilation, suggesting that ethanol has a central neural site of action.Although some research has indicated that ethanol might induce these effects by altering the action of certain hormones (eg, angiotensin, vasopressin, and catecholamines), the precise mechanism by which ethanol alters vascular function in humans remains unexplained.3
Deficiencies in alcohol dehydrogenase (ADH), aldehyde dehydrogenase 2, and certain cytochrome P450 enzymes also might contribute to facial flushing. People of Asian, especially East Asian, descent often respond to an acute dose of ethanol with symptoms of facial flushing—predominantly the result of an elevated blood level of acetaldehyde caused by an inherited deficiency of aldehyde dehydrogenase 2,4 which is downstream from ADH in the metabolic pathway of alcohol. The major enzyme system responsible for metabolism of ethanol is ADH; however, the cytochrome P450–dependent ethanol-oxidizing system—including major CYP450 isoforms CYP3A, CYP2C19, CYP2C9, CYP1A2, and CYP2D6, as well as minor CYP450 isoforms, such as CYP2E1— also are involved, to a lesser extent.5
A Role for Dupilumab?
A recent pharmacokinetic study found that dupilumab appears to have little effect on the activity of the major CYP450 isoforms. However, the drug’s effect on ADH and minor CYP450 minor isoforms is unknown. Prior drug-drug interaction studies have shown that certain cytokines and cytokine modulators can markedly influence the expression, stability, and activity of specific CYP450 enzymes.6 For example, IL-6 causes a reduction in messenger RNA for CYP3A4 and, to a lesser extent, for other isoforms.7 Whether dupilumab influences enzymes involved in processing alcohol requires further study.
Conclusion
We describe 2 cases of dupilumab-induced facial flushing after alcohol consumption. The mechanism of this dupilumab-associated flushing is unknown and requires further research.
Dupilumab is a fully humanized monoclonal antibody to the α subunit of the IL-4 receptor that inhibits the action of helper T cell (TH2)–type cytokines IL-4 and IL-13. Dupilumab was approved by the US Food and Drug Administration (FDA) in 2017 for the treatment of moderate to severe atopic dermatitis (AD). We report 2 patients with AD who were treated with dupilumab and subsequently developed facial flushing after consuming alcohol.
Case Report
Patient 1
A 24-year-old woman presented to the dermatology clinic with a lifelong history of moderate to severe AD. She had a medical history of asthma and seasonal allergies, which were treated with fexofenadine and an inhaler, as needed. The patient had an affected body surface area of approximately 70% and had achieved only partial relief with topical corticosteroids and topical calcineurin inhibitors.
Because her disease was severe, the patient was started on dupilumab at FDA-approved dosing for AD: a 600-mg subcutaneous (SC) loading dose, followed by 300 mg SC every 2 weeks. She reported rapid skin clearance within 2 weeks of the start of treatment. Her course was complicated by mild head and neck dermatitis.
Seven months after starting treatment, the patient began to acutely experience erythema and warmth over the entire face that was triggered by drinking alcohol (Figure). Before starting dupilumab, she had consumed alcohol on multiple occasions without a flushing effect. This new finding was distinguishable from her facial dermatitis. Onset was within a few minutes after drinking alcohol; flushing self-resolved in 15 to 30 minutes. Although diffuse, erythema and warmth were concentrated around the jawline, eyebrows, and ears and occurred every time the patient drank alcohol. Moreover, she reported that consumption of hard (ie, distilled) liquor, specifically tequila, caused a more severe presentation. She denied other symptoms associated with dupilumab.

Patient 2
A 32-year-old man presented to the dermatology clinic with a 10-year history of moderate to severe AD. He had a medical history of asthma (treated with albuterol, montelukast, and fluticasone); allergic rhinitis; and severe environmental allergies, including sensitivity to dust mites, dogs, trees, and grass.
For AD, the patient had been treated with topical corticosteroids and the Goeckerman regimen (a combination of phototherapy and crude coal tar). He experienced only partial relief with topical corticosteroids; the Goeckerman regimen cleared his skin, but he had quick recurrence after approximately 1 month. Given his work schedule, the patient was unable to resume phototherapy.
Because of symptoms related to the patient’s severe allergies, his allergist prescribed dupilumab: a 600-mg SC loading dose, followed by 300 mg SC every 2 weeks. The patient reported near-complete resolution of AD symptoms approximately 2 months after initiating treatment. He reported a few episodes of mild conjunctivitis that self-resolved after the first month of treatment.
Three weeks after initiating dupilumab, the patient noticed new-onset facial flushing in response to consuming alcohol. He described flushing as sudden immediate redness and warmth concentrated around the forehead, eyes, and cheeks. He reported that flushing was worse with hard liquor than with beer. Flushing would slowly subside over approximately 30 minutes despite continued alcohol consumption.
Comment
Two other single-patient case reports have discussed similar findings of alcohol-induced flushing associated with dupilumab.1,2 Both of those patients—a 19-year-old woman and a 26-year-old woman—had not experienced flushing before beginning treatment with dupilumab for AD. Both experienced onset of facial flushing months after beginning dupilumab even though both had consumed alcohol before starting dupilumab, similar to the cases presented here. One patient had a history of asthma; the other had a history of seasonal and environmental allergies.
Possible Mechanism of Action
Acute alcohol ingestion causes dermal vasodilation of the skin (ie, flushing).3 A proposed mechanism is that flushing results from direct action on central vascular-control mechanisms. This theory results from observations that individuals with quadriplegia lack notable ethanol-induced vasodilation, suggesting that ethanol has a central neural site of action.Although some research has indicated that ethanol might induce these effects by altering the action of certain hormones (eg, angiotensin, vasopressin, and catecholamines), the precise mechanism by which ethanol alters vascular function in humans remains unexplained.3
Deficiencies in alcohol dehydrogenase (ADH), aldehyde dehydrogenase 2, and certain cytochrome P450 enzymes also might contribute to facial flushing. People of Asian, especially East Asian, descent often respond to an acute dose of ethanol with symptoms of facial flushing—predominantly the result of an elevated blood level of acetaldehyde caused by an inherited deficiency of aldehyde dehydrogenase 2,4 which is downstream from ADH in the metabolic pathway of alcohol. The major enzyme system responsible for metabolism of ethanol is ADH; however, the cytochrome P450–dependent ethanol-oxidizing system—including major CYP450 isoforms CYP3A, CYP2C19, CYP2C9, CYP1A2, and CYP2D6, as well as minor CYP450 isoforms, such as CYP2E1— also are involved, to a lesser extent.5
A Role for Dupilumab?
A recent pharmacokinetic study found that dupilumab appears to have little effect on the activity of the major CYP450 isoforms. However, the drug’s effect on ADH and minor CYP450 minor isoforms is unknown. Prior drug-drug interaction studies have shown that certain cytokines and cytokine modulators can markedly influence the expression, stability, and activity of specific CYP450 enzymes.6 For example, IL-6 causes a reduction in messenger RNA for CYP3A4 and, to a lesser extent, for other isoforms.7 Whether dupilumab influences enzymes involved in processing alcohol requires further study.
Conclusion
We describe 2 cases of dupilumab-induced facial flushing after alcohol consumption. The mechanism of this dupilumab-associated flushing is unknown and requires further research.
- Herz S, Petri M, Sondermann W. New alcohol flushing in a patient with atopic dermatitis under therapy with dupilumab. Dermatol Ther. 2019;32:e12762. doi:10.1111/dth.12762
- Igelman SJ, Na C, Simpson EL. Alcohol-induced facial flushing in a patient with atopic dermatitis treated with dupilumab. JAAD Case Rep. 2020;6:139-140. doi:10.1016/j.jdcr.2019.12.002
- Malpas SC, Robinson BJ, Maling TJ. Mechanism of ethanol-induced vasodilation. J Appl Physiol (1985). 1990;68:731-734. doi:10.1152/jappl.1990.68.2.731
- Brooks PJ, Enoch M-A, Goldman D, et al. The alcohol flushing response: an unrecognized risk factor for esophageal cancer from alcohol consumption. PLoS Med. 2009;6:e50. doi:10.1371/journal.pmed.1000050
- Cederbaum AI. Alcohol metabolism. Clin Liver Dis. 2012;16:667-685. doi:10.1016/j.cld.2012.08.002
- Davis JD, Bansal A, Hassman D, et al. Evaluation of potential disease-mediated drug-drug interaction in patients with moderate-to-severe atopic dermatitis receiving dupilumab. Clin Pharmacol Ther. 2018;104:1146-1154. doi:10.1002/cpt.1058
- Mimura H, Kobayashi K, Xu L, et al. Effects of cytokines on CYP3A4 expression and reversal of the effects by anti-cytokine agents in the three-dimensionally cultured human hepatoma cell line FLC-4. Drug Metab Pharmacokinet. 2015;30:105-110. doi:10.1016/j.dmpk.2014.09.004
- Herz S, Petri M, Sondermann W. New alcohol flushing in a patient with atopic dermatitis under therapy with dupilumab. Dermatol Ther. 2019;32:e12762. doi:10.1111/dth.12762
- Igelman SJ, Na C, Simpson EL. Alcohol-induced facial flushing in a patient with atopic dermatitis treated with dupilumab. JAAD Case Rep. 2020;6:139-140. doi:10.1016/j.jdcr.2019.12.002
- Malpas SC, Robinson BJ, Maling TJ. Mechanism of ethanol-induced vasodilation. J Appl Physiol (1985). 1990;68:731-734. doi:10.1152/jappl.1990.68.2.731
- Brooks PJ, Enoch M-A, Goldman D, et al. The alcohol flushing response: an unrecognized risk factor for esophageal cancer from alcohol consumption. PLoS Med. 2009;6:e50. doi:10.1371/journal.pmed.1000050
- Cederbaum AI. Alcohol metabolism. Clin Liver Dis. 2012;16:667-685. doi:10.1016/j.cld.2012.08.002
- Davis JD, Bansal A, Hassman D, et al. Evaluation of potential disease-mediated drug-drug interaction in patients with moderate-to-severe atopic dermatitis receiving dupilumab. Clin Pharmacol Ther. 2018;104:1146-1154. doi:10.1002/cpt.1058
- Mimura H, Kobayashi K, Xu L, et al. Effects of cytokines on CYP3A4 expression and reversal of the effects by anti-cytokine agents in the three-dimensionally cultured human hepatoma cell line FLC-4. Drug Metab Pharmacokinet. 2015;30:105-110. doi:10.1016/j.dmpk.2014.09.004
Practice Points
- Dupilumab is a fully humanized monoclonal antibody that inhibits the action of IL-4 and IL-13. It was approved by the US Food and Drug Administration in 2017 for treatment of moderate to severe atopic dermatitis.
- Facial flushing after alcohol consumption may be an emerging side effect of dupilumab.
- Whether dupilumab influences enzymes involved in processing alcohol requires further study.
Clinical Edge Journal Scan Commentary: Atopic Dermatitis August 2021
Atopic Dermatitis (AD) is complex with heterogeneous symptoms (e.g. skin-pain, sleep disturbance), signs (e.g. lichenification, prurigo nodules, follicular accentuation), and longitudinal course (intermittent, persistent). These disparate signs and symptoms should be addressed in optimize disease control.
Multiple extracellular cytokines are upregulated in skin of AD patients, including interleukins 4, 5, 13, 22, 31 and thymic stromal lymphopoietin, all of which signal intracellularly through Janus Kinase (JAK)-Signal Transducer and Activator of Transcription (STAT) pathways. Differential cytokine expression is proposed to underlie clinical variability. It may be necessary to inhibit signaling of multiple cytokines to achieve adequate control of AD.
Dupilumab is currently the only biologic treatment approved in the United States for moderate-severe AD. Dupilumab revolutionized AD management. However, there remain unmet needs, including the need for faster and more potent efficacy, and oral treatment options. Recently, oral JAK-inhibitors were investigated as treatments for moderate-severe AD. Multiple JAK-inhibitors demonstrated strong and rapid efficacy across multiple clinician-reported and patient-reported outcomes.
- Miao et al. recently conducted a meta-analysis of 10 randomized controlled trials and found that patients receiving JAK inhibitors showed significantly higher efficacy for eczema area and severity index (EASI) and Numeric Rating Scale (NRS)-itch scores and similar rates of adverse-events.
- Kim et al. pooled data from 3 randomized controlled trials of abrocitinib and found significantly higher proportions of clinically meaningful responses for itch in patients receiving abrocitinib 200 mg and 100 mg vs placebo as early as week 2 which continued through week 12.
- Lio et al. performed a post-hoc analysis of a phase 3 study of conducted in North America and found significant improvements for itch severity and sleep disturbance in patients treated with baricitinib 1 mg and 2 mg vs placebo. In particular, patients who achieved improvement of itch or sleep disturbance compared to those who did not were more likely to report having no impact on quality of life impact and improved work productivity.
This new therapeutic class will be an important addition to our therapeutic armamentarium and has potential to transform the AD treatment landscape.
- Many patients prefer taking pills over injections.
- Rapid-onset of efficacy for JAK-inhibitors will certainly be appreciated by patients, especially when trying to control tough flares. It may even guide clinical decision-making. Patients who have a good clinical response to JAK-inhibitors tend to do so within 4-8 weeks. By 8 weeks, if patients have no clinical response, they are likely not going to respond and may benefit from switching to alternative therapies.
- JAK-inhibitors can have robust efficacy, with higher doses of upadacitinib and abrocritinib showing greater efficacy than dupilumab at 12-16 weeks. This makes them attractive options to consider in patients who previously failed dupilumab.
- On the other hand, JAK-inhibitors have laboratory monitoring requirements, including complete blood count, comprehensive metabolic panel, lipid panel, etc.
- JAK-inhibitors warrant adverse-event monitoring for headache, nausea, acne, herpesvirus infections, risk of venous thromboembolism, etc.
Future research is needed to identify patient subsets who will benefit most from JAK-inhibitor therapy and where to position these agents in treatment guidelines.
Atopic Dermatitis (AD) is complex with heterogeneous symptoms (e.g. skin-pain, sleep disturbance), signs (e.g. lichenification, prurigo nodules, follicular accentuation), and longitudinal course (intermittent, persistent). These disparate signs and symptoms should be addressed in optimize disease control.
Multiple extracellular cytokines are upregulated in skin of AD patients, including interleukins 4, 5, 13, 22, 31 and thymic stromal lymphopoietin, all of which signal intracellularly through Janus Kinase (JAK)-Signal Transducer and Activator of Transcription (STAT) pathways. Differential cytokine expression is proposed to underlie clinical variability. It may be necessary to inhibit signaling of multiple cytokines to achieve adequate control of AD.
Dupilumab is currently the only biologic treatment approved in the United States for moderate-severe AD. Dupilumab revolutionized AD management. However, there remain unmet needs, including the need for faster and more potent efficacy, and oral treatment options. Recently, oral JAK-inhibitors were investigated as treatments for moderate-severe AD. Multiple JAK-inhibitors demonstrated strong and rapid efficacy across multiple clinician-reported and patient-reported outcomes.
- Miao et al. recently conducted a meta-analysis of 10 randomized controlled trials and found that patients receiving JAK inhibitors showed significantly higher efficacy for eczema area and severity index (EASI) and Numeric Rating Scale (NRS)-itch scores and similar rates of adverse-events.
- Kim et al. pooled data from 3 randomized controlled trials of abrocitinib and found significantly higher proportions of clinically meaningful responses for itch in patients receiving abrocitinib 200 mg and 100 mg vs placebo as early as week 2 which continued through week 12.
- Lio et al. performed a post-hoc analysis of a phase 3 study of conducted in North America and found significant improvements for itch severity and sleep disturbance in patients treated with baricitinib 1 mg and 2 mg vs placebo. In particular, patients who achieved improvement of itch or sleep disturbance compared to those who did not were more likely to report having no impact on quality of life impact and improved work productivity.
This new therapeutic class will be an important addition to our therapeutic armamentarium and has potential to transform the AD treatment landscape.
- Many patients prefer taking pills over injections.
- Rapid-onset of efficacy for JAK-inhibitors will certainly be appreciated by patients, especially when trying to control tough flares. It may even guide clinical decision-making. Patients who have a good clinical response to JAK-inhibitors tend to do so within 4-8 weeks. By 8 weeks, if patients have no clinical response, they are likely not going to respond and may benefit from switching to alternative therapies.
- JAK-inhibitors can have robust efficacy, with higher doses of upadacitinib and abrocritinib showing greater efficacy than dupilumab at 12-16 weeks. This makes them attractive options to consider in patients who previously failed dupilumab.
- On the other hand, JAK-inhibitors have laboratory monitoring requirements, including complete blood count, comprehensive metabolic panel, lipid panel, etc.
- JAK-inhibitors warrant adverse-event monitoring for headache, nausea, acne, herpesvirus infections, risk of venous thromboembolism, etc.
Future research is needed to identify patient subsets who will benefit most from JAK-inhibitor therapy and where to position these agents in treatment guidelines.
Atopic Dermatitis (AD) is complex with heterogeneous symptoms (e.g. skin-pain, sleep disturbance), signs (e.g. lichenification, prurigo nodules, follicular accentuation), and longitudinal course (intermittent, persistent). These disparate signs and symptoms should be addressed in optimize disease control.
Multiple extracellular cytokines are upregulated in skin of AD patients, including interleukins 4, 5, 13, 22, 31 and thymic stromal lymphopoietin, all of which signal intracellularly through Janus Kinase (JAK)-Signal Transducer and Activator of Transcription (STAT) pathways. Differential cytokine expression is proposed to underlie clinical variability. It may be necessary to inhibit signaling of multiple cytokines to achieve adequate control of AD.
Dupilumab is currently the only biologic treatment approved in the United States for moderate-severe AD. Dupilumab revolutionized AD management. However, there remain unmet needs, including the need for faster and more potent efficacy, and oral treatment options. Recently, oral JAK-inhibitors were investigated as treatments for moderate-severe AD. Multiple JAK-inhibitors demonstrated strong and rapid efficacy across multiple clinician-reported and patient-reported outcomes.
- Miao et al. recently conducted a meta-analysis of 10 randomized controlled trials and found that patients receiving JAK inhibitors showed significantly higher efficacy for eczema area and severity index (EASI) and Numeric Rating Scale (NRS)-itch scores and similar rates of adverse-events.
- Kim et al. pooled data from 3 randomized controlled trials of abrocitinib and found significantly higher proportions of clinically meaningful responses for itch in patients receiving abrocitinib 200 mg and 100 mg vs placebo as early as week 2 which continued through week 12.
- Lio et al. performed a post-hoc analysis of a phase 3 study of conducted in North America and found significant improvements for itch severity and sleep disturbance in patients treated with baricitinib 1 mg and 2 mg vs placebo. In particular, patients who achieved improvement of itch or sleep disturbance compared to those who did not were more likely to report having no impact on quality of life impact and improved work productivity.
This new therapeutic class will be an important addition to our therapeutic armamentarium and has potential to transform the AD treatment landscape.
- Many patients prefer taking pills over injections.
- Rapid-onset of efficacy for JAK-inhibitors will certainly be appreciated by patients, especially when trying to control tough flares. It may even guide clinical decision-making. Patients who have a good clinical response to JAK-inhibitors tend to do so within 4-8 weeks. By 8 weeks, if patients have no clinical response, they are likely not going to respond and may benefit from switching to alternative therapies.
- JAK-inhibitors can have robust efficacy, with higher doses of upadacitinib and abrocritinib showing greater efficacy than dupilumab at 12-16 weeks. This makes them attractive options to consider in patients who previously failed dupilumab.
- On the other hand, JAK-inhibitors have laboratory monitoring requirements, including complete blood count, comprehensive metabolic panel, lipid panel, etc.
- JAK-inhibitors warrant adverse-event monitoring for headache, nausea, acne, herpesvirus infections, risk of venous thromboembolism, etc.
Future research is needed to identify patient subsets who will benefit most from JAK-inhibitor therapy and where to position these agents in treatment guidelines.
JAK inhibitors could be a promising alternative treatment option for atopic dermatitis
Key clinical point: Janus kinase (JAK) inhibitors were safe and effective in reducing the intensity of signs and symptoms of atopic dermatitis (AD) with significant improvements observed for Eczema Area and Severity Index (EASI) and pruritus numerical rating scale (NRS) scores.
Major finding: Patients receiving JAK inhibitors showed significant improvements in both total EASI score (mean difference [MD], −0.31; 95% confidence interval [CI], −0.46 to −0.17) and pruritus NRS score (MD, −1.15; 95% CI, −1.48 to −0.83). The risk of total adverse events was not significantly different between JAK inhibitor and control groups (risk ratio, 1.02; P = .745).
Study details: Findings are from a meta-analysis of 10 randomized controlled trials including 2583 patients with AD, of which 1,761 were in JAK inhibitor and 822 in control groups.
Disclosures: The study did not report any source of funding. No conflicts of interest were reported.
Source: Miao M et al. J Dermatolog Treat. 2021 Jun 16. doi: 10.1080/09546634.2021.1942422.
Key clinical point: Janus kinase (JAK) inhibitors were safe and effective in reducing the intensity of signs and symptoms of atopic dermatitis (AD) with significant improvements observed for Eczema Area and Severity Index (EASI) and pruritus numerical rating scale (NRS) scores.
Major finding: Patients receiving JAK inhibitors showed significant improvements in both total EASI score (mean difference [MD], −0.31; 95% confidence interval [CI], −0.46 to −0.17) and pruritus NRS score (MD, −1.15; 95% CI, −1.48 to −0.83). The risk of total adverse events was not significantly different between JAK inhibitor and control groups (risk ratio, 1.02; P = .745).
Study details: Findings are from a meta-analysis of 10 randomized controlled trials including 2583 patients with AD, of which 1,761 were in JAK inhibitor and 822 in control groups.
Disclosures: The study did not report any source of funding. No conflicts of interest were reported.
Source: Miao M et al. J Dermatolog Treat. 2021 Jun 16. doi: 10.1080/09546634.2021.1942422.
Key clinical point: Janus kinase (JAK) inhibitors were safe and effective in reducing the intensity of signs and symptoms of atopic dermatitis (AD) with significant improvements observed for Eczema Area and Severity Index (EASI) and pruritus numerical rating scale (NRS) scores.
Major finding: Patients receiving JAK inhibitors showed significant improvements in both total EASI score (mean difference [MD], −0.31; 95% confidence interval [CI], −0.46 to −0.17) and pruritus NRS score (MD, −1.15; 95% CI, −1.48 to −0.83). The risk of total adverse events was not significantly different between JAK inhibitor and control groups (risk ratio, 1.02; P = .745).
Study details: Findings are from a meta-analysis of 10 randomized controlled trials including 2583 patients with AD, of which 1,761 were in JAK inhibitor and 822 in control groups.
Disclosures: The study did not report any source of funding. No conflicts of interest were reported.
Source: Miao M et al. J Dermatolog Treat. 2021 Jun 16. doi: 10.1080/09546634.2021.1942422.
Serum biomarker-based patient clusters identify heterogeneity in pediatric atopic dermatitis
Key clinical point: Analysis of serum biomarker profiles in pediatric patients with atopic dermatitis (AD) indicates the existence of unique endotypes that could predict patients at risk of persistent disease and guide personalized, endotype-driven therapeutic approaches.
Major finding: Distinct biomarker profiles identified Th2/retinol dominant (mean Eczema Area Severity Index [EASI] score: 9.2), skin-homing dominant (mean EASI score: 27.8), Th1/Th2/Th17/IL-1 dominant (mean EASI score: 10.5), and Th1/IL-1/eosinophil inferior (mean EASI score: 12.3) as the 4 distinct pediatric clusters. The clusters were influenced by disease severity and not age, with the skin-homing dominant cluster having more severe AD than other clusters (P less than .001).
Study details: Findings are from an analysis of biomarker profiles of 240 pediatric patients with AD aged 0-17 years compared with previously found profiles in adult patients with AD.
Disclosures: This study was funded by Regeneron and Sanofi-Genzyme pharmaceuticals, Inc. Dr. M de Graaf, Dr. MS de Bruin-Weller, Dr. DS Bakker, Dr. E Knol, and Dr. JL Thijs declared being speaker, principal investigator, consultant, and/or advisory board member for various sources including Sanofi-Genzyme and Regeneron.
Source: Bakker DS et al. J Allergy Clin Immun. 2021 Jul 6. doi: 10.1016/j.jaci.2021.06.029.
Key clinical point: Analysis of serum biomarker profiles in pediatric patients with atopic dermatitis (AD) indicates the existence of unique endotypes that could predict patients at risk of persistent disease and guide personalized, endotype-driven therapeutic approaches.
Major finding: Distinct biomarker profiles identified Th2/retinol dominant (mean Eczema Area Severity Index [EASI] score: 9.2), skin-homing dominant (mean EASI score: 27.8), Th1/Th2/Th17/IL-1 dominant (mean EASI score: 10.5), and Th1/IL-1/eosinophil inferior (mean EASI score: 12.3) as the 4 distinct pediatric clusters. The clusters were influenced by disease severity and not age, with the skin-homing dominant cluster having more severe AD than other clusters (P less than .001).
Study details: Findings are from an analysis of biomarker profiles of 240 pediatric patients with AD aged 0-17 years compared with previously found profiles in adult patients with AD.
Disclosures: This study was funded by Regeneron and Sanofi-Genzyme pharmaceuticals, Inc. Dr. M de Graaf, Dr. MS de Bruin-Weller, Dr. DS Bakker, Dr. E Knol, and Dr. JL Thijs declared being speaker, principal investigator, consultant, and/or advisory board member for various sources including Sanofi-Genzyme and Regeneron.
Source: Bakker DS et al. J Allergy Clin Immun. 2021 Jul 6. doi: 10.1016/j.jaci.2021.06.029.
Key clinical point: Analysis of serum biomarker profiles in pediatric patients with atopic dermatitis (AD) indicates the existence of unique endotypes that could predict patients at risk of persistent disease and guide personalized, endotype-driven therapeutic approaches.
Major finding: Distinct biomarker profiles identified Th2/retinol dominant (mean Eczema Area Severity Index [EASI] score: 9.2), skin-homing dominant (mean EASI score: 27.8), Th1/Th2/Th17/IL-1 dominant (mean EASI score: 10.5), and Th1/IL-1/eosinophil inferior (mean EASI score: 12.3) as the 4 distinct pediatric clusters. The clusters were influenced by disease severity and not age, with the skin-homing dominant cluster having more severe AD than other clusters (P less than .001).
Study details: Findings are from an analysis of biomarker profiles of 240 pediatric patients with AD aged 0-17 years compared with previously found profiles in adult patients with AD.
Disclosures: This study was funded by Regeneron and Sanofi-Genzyme pharmaceuticals, Inc. Dr. M de Graaf, Dr. MS de Bruin-Weller, Dr. DS Bakker, Dr. E Knol, and Dr. JL Thijs declared being speaker, principal investigator, consultant, and/or advisory board member for various sources including Sanofi-Genzyme and Regeneron.
Source: Bakker DS et al. J Allergy Clin Immun. 2021 Jul 6. doi: 10.1016/j.jaci.2021.06.029.
Higher maternal serum 25(OH)D levels may increase risk for early-onset infant atopic dermatitis
Key clinical point: Higher maternal serum 25-hydroxyvitamin D (25[OH]D) levels during pregnancy may be associated with increased risk for early-onset infant atopic dermatitis (AD).
Major finding: Overall, 26.5% of infants developed AD before 1 year of age. Higher maternal serum 25(OH)D levels during pregnancy were associated with increased risks for AD in infants before 1 year of age with borderline statistical significance, particularly in the first trimester (per ln unit increase, adjusted odds ratio [aOR], 1.93; 95% confidence interval [CI], 0.96-3.88) and the second trimester (per ln unit increase, aOR, 1.72; 95% CI, 0.93-3.19).
Study details: Findings are from the analysis of pregnant women from the MKFOAD birth cohort and their infants (n=456) who received routine child care visits at birth, day 42, and 6 and 12 months after birth.
Disclosures: This study was funded by Shanghai Public Health Three-Year Action Plan, National Key Research and Development Program, Canada-China Clinical Research Program, Collaboration Grant of Children’s Hospital of Fudan University, and Pigeon Maternal and Infant Skin Care Research Institute. The authors declared no conflicts of interest.
Source: Tian Y et al. Pediatr Allergy Immunol. 2021 Jun 23. doi: 10.1111/pai.13582.
Key clinical point: Higher maternal serum 25-hydroxyvitamin D (25[OH]D) levels during pregnancy may be associated with increased risk for early-onset infant atopic dermatitis (AD).
Major finding: Overall, 26.5% of infants developed AD before 1 year of age. Higher maternal serum 25(OH)D levels during pregnancy were associated with increased risks for AD in infants before 1 year of age with borderline statistical significance, particularly in the first trimester (per ln unit increase, adjusted odds ratio [aOR], 1.93; 95% confidence interval [CI], 0.96-3.88) and the second trimester (per ln unit increase, aOR, 1.72; 95% CI, 0.93-3.19).
Study details: Findings are from the analysis of pregnant women from the MKFOAD birth cohort and their infants (n=456) who received routine child care visits at birth, day 42, and 6 and 12 months after birth.
Disclosures: This study was funded by Shanghai Public Health Three-Year Action Plan, National Key Research and Development Program, Canada-China Clinical Research Program, Collaboration Grant of Children’s Hospital of Fudan University, and Pigeon Maternal and Infant Skin Care Research Institute. The authors declared no conflicts of interest.
Source: Tian Y et al. Pediatr Allergy Immunol. 2021 Jun 23. doi: 10.1111/pai.13582.
Key clinical point: Higher maternal serum 25-hydroxyvitamin D (25[OH]D) levels during pregnancy may be associated with increased risk for early-onset infant atopic dermatitis (AD).
Major finding: Overall, 26.5% of infants developed AD before 1 year of age. Higher maternal serum 25(OH)D levels during pregnancy were associated with increased risks for AD in infants before 1 year of age with borderline statistical significance, particularly in the first trimester (per ln unit increase, adjusted odds ratio [aOR], 1.93; 95% confidence interval [CI], 0.96-3.88) and the second trimester (per ln unit increase, aOR, 1.72; 95% CI, 0.93-3.19).
Study details: Findings are from the analysis of pregnant women from the MKFOAD birth cohort and their infants (n=456) who received routine child care visits at birth, day 42, and 6 and 12 months after birth.
Disclosures: This study was funded by Shanghai Public Health Three-Year Action Plan, National Key Research and Development Program, Canada-China Clinical Research Program, Collaboration Grant of Children’s Hospital of Fudan University, and Pigeon Maternal and Infant Skin Care Research Institute. The authors declared no conflicts of interest.
Source: Tian Y et al. Pediatr Allergy Immunol. 2021 Jun 23. doi: 10.1111/pai.13582.
Dupilumab is an effective treatment for atopic dermatitis, regardless of prior NSISS use
Key clinical point: Dupilumab with or without topical corticosteroids (TCS) was beneficial in adults with moderate-to-severe atopic dermatitis (AD) regardless of any prior use of systemic nonsteroidal immunosuppressants (NSISS).
Major finding: Compared with placebo with/without TCS, dupilumab with/without TCS showed significant improvement in Eczema Area and Severity Index, SCORing AD, Peak Pruritus Numerical Rating Scale, and quality of life in patients with/without prior use of NSISS (P less than .001) by week 16 which continued through week 52 of treatment.
Study details: Findings are from a post hoc analysis of 4 phase 3 clinical trials including 1553 patients with moderate-to-severe AD randomly assigned to placebo or dupilumab as monotherapy for 16 weeks or with concomitant TCS for 16/52 weeks.
Disclosures: This study was funded by Sanofi and Regeneron Pharmaceuticals, Inc. Some of the authors declared receiving grants, honoraria and serving as consultant or speaker or on advisory board for various sources. Some of the authors declared being employees and/or holding stocks/stock options at Sanofi, Regeneron Pharmaceuticals, Inc or Sanofi Genzyme.
Source: Griffiths C et al. Dermatol Ther (Heidelb). 2021 Jun 18. doi: 10.1007/s13555-021-00558-0.
Key clinical point: Dupilumab with or without topical corticosteroids (TCS) was beneficial in adults with moderate-to-severe atopic dermatitis (AD) regardless of any prior use of systemic nonsteroidal immunosuppressants (NSISS).
Major finding: Compared with placebo with/without TCS, dupilumab with/without TCS showed significant improvement in Eczema Area and Severity Index, SCORing AD, Peak Pruritus Numerical Rating Scale, and quality of life in patients with/without prior use of NSISS (P less than .001) by week 16 which continued through week 52 of treatment.
Study details: Findings are from a post hoc analysis of 4 phase 3 clinical trials including 1553 patients with moderate-to-severe AD randomly assigned to placebo or dupilumab as monotherapy for 16 weeks or with concomitant TCS for 16/52 weeks.
Disclosures: This study was funded by Sanofi and Regeneron Pharmaceuticals, Inc. Some of the authors declared receiving grants, honoraria and serving as consultant or speaker or on advisory board for various sources. Some of the authors declared being employees and/or holding stocks/stock options at Sanofi, Regeneron Pharmaceuticals, Inc or Sanofi Genzyme.
Source: Griffiths C et al. Dermatol Ther (Heidelb). 2021 Jun 18. doi: 10.1007/s13555-021-00558-0.
Key clinical point: Dupilumab with or without topical corticosteroids (TCS) was beneficial in adults with moderate-to-severe atopic dermatitis (AD) regardless of any prior use of systemic nonsteroidal immunosuppressants (NSISS).
Major finding: Compared with placebo with/without TCS, dupilumab with/without TCS showed significant improvement in Eczema Area and Severity Index, SCORing AD, Peak Pruritus Numerical Rating Scale, and quality of life in patients with/without prior use of NSISS (P less than .001) by week 16 which continued through week 52 of treatment.
Study details: Findings are from a post hoc analysis of 4 phase 3 clinical trials including 1553 patients with moderate-to-severe AD randomly assigned to placebo or dupilumab as monotherapy for 16 weeks or with concomitant TCS for 16/52 weeks.
Disclosures: This study was funded by Sanofi and Regeneron Pharmaceuticals, Inc. Some of the authors declared receiving grants, honoraria and serving as consultant or speaker or on advisory board for various sources. Some of the authors declared being employees and/or holding stocks/stock options at Sanofi, Regeneron Pharmaceuticals, Inc or Sanofi Genzyme.
Source: Griffiths C et al. Dermatol Ther (Heidelb). 2021 Jun 18. doi: 10.1007/s13555-021-00558-0.
Dupilumab and tacrolimus ointment shows real-world benefit for facial atopic dermatitis
Key clinical point: In real world clinical practice, combination of tacrolimus ointment and dupilumab was an effective and safe treatment option for facial atopic dermatitis (AD).
Major finding: On 16 weeks of treatment, a significant decrease was observed in average scores including Investigator’s Global Assessment, overall Eczema Area and Severity Index (EASI), and head/neck EASI (P less than .0001). Moreover, the rate of improvement in head/neck EASI scores significantly correlated with the rate of improvement in the overall EASI scores (Pearson’s r, 0.61; P less than .01). None of the patients developed herpes simplex, whereas 2 patients developed conjunctivitis.
Study details: Findings are from a retrospective chart review of 109 patients with moderate-to-severe AD who initiated dupilumab, of which 60 patients also used tacrolimus ointment. Of these, 20 patients used tacrolimus ointment without any topical steroids.
Disclosures: This work was supported by grants from Japan Society for the Promotion of Science. The authors did not declare any conflicts of interest.
Source: Matsutani M et al. J Dermatol. 2021 Jun 22. doi: 10.1111/1346-8138.16039.
Key clinical point: In real world clinical practice, combination of tacrolimus ointment and dupilumab was an effective and safe treatment option for facial atopic dermatitis (AD).
Major finding: On 16 weeks of treatment, a significant decrease was observed in average scores including Investigator’s Global Assessment, overall Eczema Area and Severity Index (EASI), and head/neck EASI (P less than .0001). Moreover, the rate of improvement in head/neck EASI scores significantly correlated with the rate of improvement in the overall EASI scores (Pearson’s r, 0.61; P less than .01). None of the patients developed herpes simplex, whereas 2 patients developed conjunctivitis.
Study details: Findings are from a retrospective chart review of 109 patients with moderate-to-severe AD who initiated dupilumab, of which 60 patients also used tacrolimus ointment. Of these, 20 patients used tacrolimus ointment without any topical steroids.
Disclosures: This work was supported by grants from Japan Society for the Promotion of Science. The authors did not declare any conflicts of interest.
Source: Matsutani M et al. J Dermatol. 2021 Jun 22. doi: 10.1111/1346-8138.16039.
Key clinical point: In real world clinical practice, combination of tacrolimus ointment and dupilumab was an effective and safe treatment option for facial atopic dermatitis (AD).
Major finding: On 16 weeks of treatment, a significant decrease was observed in average scores including Investigator’s Global Assessment, overall Eczema Area and Severity Index (EASI), and head/neck EASI (P less than .0001). Moreover, the rate of improvement in head/neck EASI scores significantly correlated with the rate of improvement in the overall EASI scores (Pearson’s r, 0.61; P less than .01). None of the patients developed herpes simplex, whereas 2 patients developed conjunctivitis.
Study details: Findings are from a retrospective chart review of 109 patients with moderate-to-severe AD who initiated dupilumab, of which 60 patients also used tacrolimus ointment. Of these, 20 patients used tacrolimus ointment without any topical steroids.
Disclosures: This work was supported by grants from Japan Society for the Promotion of Science. The authors did not declare any conflicts of interest.
Source: Matsutani M et al. J Dermatol. 2021 Jun 22. doi: 10.1111/1346-8138.16039.
Baricitinib improves itch and enhances QoL in atopic dermatitis
Key clinical point: Baricitinib therapy resulted in clinically meaningful improvement in itch severity leading to significantly better quality of life (QoL) in patients with moderate-to-severe atopic dermatitis (AD).
Major finding: By week 16, higher proportion of patients receiving baricitinib 2 mg (25.2%; P less than .0001) and 1 mg (15.9%; P = .0114) vs placebo (5.7%) experienced improvements in itch severity. Higher proportion of patients with vs without itch improvement showed no impact of AD on QoL (P less than .0001).
Study details: Findings are from a post hoc analysis of phase 3 trial, BREEZE-AD5 involving 440 adults with moderate-to-severe AD who received baricitinib 1 mg, 2 mg, or placebo once daily.
Disclosures: This work was funded by Eli Lilly and Company. Some of the authors declared receiving grants, funding, consulting fees, and/or honoraria from and/or serving as board member, speaker, advisor, and/or investigator for various sources including Eli Lilly. Five of the authors declared being employees and shareholders of Eli Lilly.
Source: Lio PA et al. J Dermatolog Treat. 2021 Jun 28. doi: 10.1080/09546634.2021.1914308.
Key clinical point: Baricitinib therapy resulted in clinically meaningful improvement in itch severity leading to significantly better quality of life (QoL) in patients with moderate-to-severe atopic dermatitis (AD).
Major finding: By week 16, higher proportion of patients receiving baricitinib 2 mg (25.2%; P less than .0001) and 1 mg (15.9%; P = .0114) vs placebo (5.7%) experienced improvements in itch severity. Higher proportion of patients with vs without itch improvement showed no impact of AD on QoL (P less than .0001).
Study details: Findings are from a post hoc analysis of phase 3 trial, BREEZE-AD5 involving 440 adults with moderate-to-severe AD who received baricitinib 1 mg, 2 mg, or placebo once daily.
Disclosures: This work was funded by Eli Lilly and Company. Some of the authors declared receiving grants, funding, consulting fees, and/or honoraria from and/or serving as board member, speaker, advisor, and/or investigator for various sources including Eli Lilly. Five of the authors declared being employees and shareholders of Eli Lilly.
Source: Lio PA et al. J Dermatolog Treat. 2021 Jun 28. doi: 10.1080/09546634.2021.1914308.
Key clinical point: Baricitinib therapy resulted in clinically meaningful improvement in itch severity leading to significantly better quality of life (QoL) in patients with moderate-to-severe atopic dermatitis (AD).
Major finding: By week 16, higher proportion of patients receiving baricitinib 2 mg (25.2%; P less than .0001) and 1 mg (15.9%; P = .0114) vs placebo (5.7%) experienced improvements in itch severity. Higher proportion of patients with vs without itch improvement showed no impact of AD on QoL (P less than .0001).
Study details: Findings are from a post hoc analysis of phase 3 trial, BREEZE-AD5 involving 440 adults with moderate-to-severe AD who received baricitinib 1 mg, 2 mg, or placebo once daily.
Disclosures: This work was funded by Eli Lilly and Company. Some of the authors declared receiving grants, funding, consulting fees, and/or honoraria from and/or serving as board member, speaker, advisor, and/or investigator for various sources including Eli Lilly. Five of the authors declared being employees and shareholders of Eli Lilly.
Source: Lio PA et al. J Dermatolog Treat. 2021 Jun 28. doi: 10.1080/09546634.2021.1914308.
Abrocitinib improves itch associated with atopic dermatitis in phase 2b/3 trials
Key clinical point: Abrocitinib monotherapy was associated with a rapid and profound relief in atopic dermatitis (AD) itch.
Major finding: A higher proportion of patients receiving abrocitinib 200 mg and 100 mg vs placebo experienced clinically meaningful itch improvement at week 2 (44.2% and 24.9% vs 5.8%), which continued through week 12 (57.3% and 42.9% vs 16.5%; both P less than .05). Mean percentage reductions in itch scores 24 hours after the first dose were greater for abrocitinib 200 mg and 100 mg vs placebo which was maintained through week 12 (−56.1 and −42.3 vs −19.5).
Study details: Findings are from a pooled analysis of 1 phase 2b (NCT02780167) and 2 phase 3 (JADE MONO-1 and JADE MONO-2) trials including 942 patients with moderate-to-severe AD who received abrocitinib 200 mg, abrocitinib 100 mg, or placebo.
Disclosures: This study was sponsored by Pfizer, Inc. Some of the authors declared receiving grants and personal fees and/or serving as consultant, speaker, advisor, and/or principal investigator for various sources including Pfizer. Six of the authors declared being employees and shareholders of Pfizer, Inc.
Source: Kim BS et al. Dermatitis. 2021 Jul 7. doi: 10.1097/DER.0000000000000770.
Key clinical point: Abrocitinib monotherapy was associated with a rapid and profound relief in atopic dermatitis (AD) itch.
Major finding: A higher proportion of patients receiving abrocitinib 200 mg and 100 mg vs placebo experienced clinically meaningful itch improvement at week 2 (44.2% and 24.9% vs 5.8%), which continued through week 12 (57.3% and 42.9% vs 16.5%; both P less than .05). Mean percentage reductions in itch scores 24 hours after the first dose were greater for abrocitinib 200 mg and 100 mg vs placebo which was maintained through week 12 (−56.1 and −42.3 vs −19.5).
Study details: Findings are from a pooled analysis of 1 phase 2b (NCT02780167) and 2 phase 3 (JADE MONO-1 and JADE MONO-2) trials including 942 patients with moderate-to-severe AD who received abrocitinib 200 mg, abrocitinib 100 mg, or placebo.
Disclosures: This study was sponsored by Pfizer, Inc. Some of the authors declared receiving grants and personal fees and/or serving as consultant, speaker, advisor, and/or principal investigator for various sources including Pfizer. Six of the authors declared being employees and shareholders of Pfizer, Inc.
Source: Kim BS et al. Dermatitis. 2021 Jul 7. doi: 10.1097/DER.0000000000000770.
Key clinical point: Abrocitinib monotherapy was associated with a rapid and profound relief in atopic dermatitis (AD) itch.
Major finding: A higher proportion of patients receiving abrocitinib 200 mg and 100 mg vs placebo experienced clinically meaningful itch improvement at week 2 (44.2% and 24.9% vs 5.8%), which continued through week 12 (57.3% and 42.9% vs 16.5%; both P less than .05). Mean percentage reductions in itch scores 24 hours after the first dose were greater for abrocitinib 200 mg and 100 mg vs placebo which was maintained through week 12 (−56.1 and −42.3 vs −19.5).
Study details: Findings are from a pooled analysis of 1 phase 2b (NCT02780167) and 2 phase 3 (JADE MONO-1 and JADE MONO-2) trials including 942 patients with moderate-to-severe AD who received abrocitinib 200 mg, abrocitinib 100 mg, or placebo.
Disclosures: This study was sponsored by Pfizer, Inc. Some of the authors declared receiving grants and personal fees and/or serving as consultant, speaker, advisor, and/or principal investigator for various sources including Pfizer. Six of the authors declared being employees and shareholders of Pfizer, Inc.
Source: Kim BS et al. Dermatitis. 2021 Jul 7. doi: 10.1097/DER.0000000000000770.