User login
Spot-check Hgb testing transforming trauma blood draws
NAPLES, FLA. – Spot-check hemoglobin testing can provide immediate and accurate hemoglobin measurements in trauma patients without removing a drop of blood, a prospective cohort study shows.
"The noninvasive hemoglobin monitor, I think, will change the way we practice," Dr. Bellal Joseph said at the annual scientific assembly of the Eastern Association for the Surgery of Trauma.
Continuous, noninvasive hemoglobin (Hgb) devices have been around for years, but studies showed poor correlation with invasive Hgb blood draws in trauma patients. Advances in technology, including more sensitive sensors and a wider range of sensor sizes, allow new spot-check devices to more accurately measure a broader range of patients with a wider range of finger diameters.
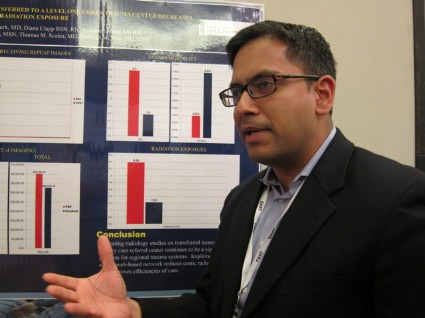
Dr. Joseph, a trauma and critical care surgeon at the University of Arizona Medical Center, Tucson, and his colleagues simultaneously obtained invasive and spot-check Hgb measurements in a prospective cohort of 525 trauma patients. Spot-check Hgb was measured three times upon presentation to the Level 1 trauma center using the Pronto-7 pulse CO-oximeter device and correlated with each invasive Hgb measurement.
According to the analysis, the success rate for spot-check Hgb testing was 86% in the mostly male cohort (74%), with a mean Injury Severity Score of 20, and average age of 41 years.
The mean hemoglobin for the 450 invasive Hgb measurements was 11.5 g/dL and 11.4 g/dL for the 1,350 Pronto-7 spot-checks, Dr. Joseph said.
Sensitivity for the spot-check device was 96%, specificity 44%, positive predictive value 73%, and negative predictive value 88% in patients with a hemoglobin above and below 8 g/dL. In all, 38% of patients had a hemoglobin level of less than 8 g/dL.
A Bland-Altman plot showed that 98.7% of readings were within two standard deviations. Spearman’s rank correlation coefficient revealed spot-check Hgb had a strong correlation with invasive Hgb testing (R2 = 0.77; R = 0.86), Dr. Joseph said.
"This device is a lot better than the continuous one we used to have, which they use in the operating room a lot," he said during the poster presentation. "We’re currently looking at it in patients who have blunt spleen or blunt liver injuries. Instead of ordering q6 hour, invasive hemoglobins, we’re just putting the monitor on and seeing if we can make clinical decisions based on that."
The palm-sized Pronto-7 spot-check device also has a perfusion index to help identify patients with early shock, but this has yet to be studied or integrated into practice.
"The one concern that I still have with this device is that 14% of our patients didn’t pick up a hemoglobin, and why is that?" Dr. Joseph said. Fashion may be, in part, to blame, with readings more likely to fail in patients with nail polish on, he added.
The next phase of the study will include implementation of the spot-check device on the floors and in the ICU with the nursing staff and direct uploading of results into patient charts. A time-savings analysis also will be done.
Dr. Joseph and his coauthors reported having no financial disclosures or study support.
NAPLES, FLA. – Spot-check hemoglobin testing can provide immediate and accurate hemoglobin measurements in trauma patients without removing a drop of blood, a prospective cohort study shows.
"The noninvasive hemoglobin monitor, I think, will change the way we practice," Dr. Bellal Joseph said at the annual scientific assembly of the Eastern Association for the Surgery of Trauma.
Continuous, noninvasive hemoglobin (Hgb) devices have been around for years, but studies showed poor correlation with invasive Hgb blood draws in trauma patients. Advances in technology, including more sensitive sensors and a wider range of sensor sizes, allow new spot-check devices to more accurately measure a broader range of patients with a wider range of finger diameters.
Dr. Joseph, a trauma and critical care surgeon at the University of Arizona Medical Center, Tucson, and his colleagues simultaneously obtained invasive and spot-check Hgb measurements in a prospective cohort of 525 trauma patients. Spot-check Hgb was measured three times upon presentation to the Level 1 trauma center using the Pronto-7 pulse CO-oximeter device and correlated with each invasive Hgb measurement.
According to the analysis, the success rate for spot-check Hgb testing was 86% in the mostly male cohort (74%), with a mean Injury Severity Score of 20, and average age of 41 years.
The mean hemoglobin for the 450 invasive Hgb measurements was 11.5 g/dL and 11.4 g/dL for the 1,350 Pronto-7 spot-checks, Dr. Joseph said.
Sensitivity for the spot-check device was 96%, specificity 44%, positive predictive value 73%, and negative predictive value 88% in patients with a hemoglobin above and below 8 g/dL. In all, 38% of patients had a hemoglobin level of less than 8 g/dL.
A Bland-Altman plot showed that 98.7% of readings were within two standard deviations. Spearman’s rank correlation coefficient revealed spot-check Hgb had a strong correlation with invasive Hgb testing (R2 = 0.77; R = 0.86), Dr. Joseph said.
"This device is a lot better than the continuous one we used to have, which they use in the operating room a lot," he said during the poster presentation. "We’re currently looking at it in patients who have blunt spleen or blunt liver injuries. Instead of ordering q6 hour, invasive hemoglobins, we’re just putting the monitor on and seeing if we can make clinical decisions based on that."
The palm-sized Pronto-7 spot-check device also has a perfusion index to help identify patients with early shock, but this has yet to be studied or integrated into practice.
"The one concern that I still have with this device is that 14% of our patients didn’t pick up a hemoglobin, and why is that?" Dr. Joseph said. Fashion may be, in part, to blame, with readings more likely to fail in patients with nail polish on, he added.
The next phase of the study will include implementation of the spot-check device on the floors and in the ICU with the nursing staff and direct uploading of results into patient charts. A time-savings analysis also will be done.
Dr. Joseph and his coauthors reported having no financial disclosures or study support.
NAPLES, FLA. – Spot-check hemoglobin testing can provide immediate and accurate hemoglobin measurements in trauma patients without removing a drop of blood, a prospective cohort study shows.
"The noninvasive hemoglobin monitor, I think, will change the way we practice," Dr. Bellal Joseph said at the annual scientific assembly of the Eastern Association for the Surgery of Trauma.
Continuous, noninvasive hemoglobin (Hgb) devices have been around for years, but studies showed poor correlation with invasive Hgb blood draws in trauma patients. Advances in technology, including more sensitive sensors and a wider range of sensor sizes, allow new spot-check devices to more accurately measure a broader range of patients with a wider range of finger diameters.
Dr. Joseph, a trauma and critical care surgeon at the University of Arizona Medical Center, Tucson, and his colleagues simultaneously obtained invasive and spot-check Hgb measurements in a prospective cohort of 525 trauma patients. Spot-check Hgb was measured three times upon presentation to the Level 1 trauma center using the Pronto-7 pulse CO-oximeter device and correlated with each invasive Hgb measurement.
According to the analysis, the success rate for spot-check Hgb testing was 86% in the mostly male cohort (74%), with a mean Injury Severity Score of 20, and average age of 41 years.
The mean hemoglobin for the 450 invasive Hgb measurements was 11.5 g/dL and 11.4 g/dL for the 1,350 Pronto-7 spot-checks, Dr. Joseph said.
Sensitivity for the spot-check device was 96%, specificity 44%, positive predictive value 73%, and negative predictive value 88% in patients with a hemoglobin above and below 8 g/dL. In all, 38% of patients had a hemoglobin level of less than 8 g/dL.
A Bland-Altman plot showed that 98.7% of readings were within two standard deviations. Spearman’s rank correlation coefficient revealed spot-check Hgb had a strong correlation with invasive Hgb testing (R2 = 0.77; R = 0.86), Dr. Joseph said.
"This device is a lot better than the continuous one we used to have, which they use in the operating room a lot," he said during the poster presentation. "We’re currently looking at it in patients who have blunt spleen or blunt liver injuries. Instead of ordering q6 hour, invasive hemoglobins, we’re just putting the monitor on and seeing if we can make clinical decisions based on that."
The palm-sized Pronto-7 spot-check device also has a perfusion index to help identify patients with early shock, but this has yet to be studied or integrated into practice.
"The one concern that I still have with this device is that 14% of our patients didn’t pick up a hemoglobin, and why is that?" Dr. Joseph said. Fashion may be, in part, to blame, with readings more likely to fail in patients with nail polish on, he added.
The next phase of the study will include implementation of the spot-check device on the floors and in the ICU with the nursing staff and direct uploading of results into patient charts. A time-savings analysis also will be done.
Dr. Joseph and his coauthors reported having no financial disclosures or study support.
AT EAST SCIENTIFIC ASSEMBLY
Major finding: The mean hemoglobin was 11.5 g/dL for invasive hemoglobin testing and 11.4 g/dL for noninvasive, spot-check testing.
Data source: Prospective cohort study of 525 trauma patients.
Disclosures: Dr. Joseph and his coauthors reported having no financial disclosures or study support.
PTSD: The elephant in the trauma bay
NAPLES, FLA. – Posttraumatic stress disorder is disturbingly common among U.S. trauma surgeons, according to a national survey.
Among 453 members of the American Association for the Surgery of Trauma (AAST) and Eastern Association for the Surgery of Trauma (EAST), 40% had symptoms of PTSD and 15% met the diagnostic criteria for PTSD.
"It’s the elephant in the room," Dr. Bellal A. Joseph said at the annual scientific assembly of EAST.
Understanding the factors that predispose trauma surgeons to PTSD may benefit patients and the profession and may be useful to national trauma surgery associations to develop targeted interventions, said Dr. Joseph, a trauma and critical care surgeon at the University of Arizona Medical Center, Tucson.
"Active surveillance to promote wellness among trauma surgeons is warranted," he said.
Invited discussant Dr. Karen Lommel, a psychiatrist who recently converted to emergency medicine at the University of Kentucky, Lexington, described the findings as "quite remarkable."
"The issue of posttraumatic symptoms and PTSD affects all of us who work in trauma, whether we choose to acknowledge it or not," she said. "Pre-hospital workers, nurses, and mental health professionals have been extensively included in PTSD studies. Unfortunately, trauma surgeons – one of the most stoic of frontline providers – have been overlooked."
Dr. Joseph described receiving pushback when proposing the study to other trauma surgeons and was told flat-out by one respondent that its hypothesis is flawed.
A self-identified senior surgeon wrote: "I found that the assumptions of the questions did not fit the trauma program I work in nor the surgeons with whom I work. They actually take trauma call to relax. Stress is not a word in our vocabulary."
The two-part survey, sent to all members of EAST and the AAST (41% response rate), was not specifically identified as a PTSD survey, but included the validated PTSD CheckList-Civilian Version (PCL-C). A score of 35 or more on the 17-item PCL-C has previously shown a sensitivity of 85% for PTSD symptoms, while a score of 44 or more is 95% sensitive and 86% specific for a PTSD diagnosis, Dr. Joseph observed.
The survey respondents were mostly male (76%), white (80%), practiced in an urban hospital (89.6%), or Level 1 trauma center (71%). More than half (54.7%) had 11 years or more of clinical practice, 21% had military experience, and 14.3% had been deployed to war.
Three-fourths (66.4%) had an annual income of at least $300,000, but 90.5% spent no more than 4 hours per day of non–sleep relaxation and 26.5% took no more than 2 weeks vacation per year.
Only 6.2% said they suffered from depression and 3% from anxiety, but 66% reported using alcohol and 5.3% smoking.
Regarding the scope of their work, 85% had four or more 24-hour calls per month, 36% had at least three critical cases per call, and 24% had at least 10 operative trauma cases per month.
Surgeons who had more than five critical cases per call were seven times more likely to develop PTSD in multivariate analysis (odds ratio, 7; P = .001), Dr. Joseph said. No other factors were significantly associated with a PTSD diagnosis.
Independent predictors of PTSD symptoms in the multivariate analysis were male sex (OR, 2; P = .04); more than seven call duties/month (OR, 2.6; P = .001); more than 15 operative cases/month (OR, 3; P = .001); less than 4 hours of daily relaxation (OR, 7; P = .01)’ and less than 2 weeks of vacation/year (OR, 2: P = .02); he said.
Following the presentation, a surgeon from the Bronx, N.Y., said one of the sticking points for his CEO in the state’s move toward American College of Surgeons’ verification is the back-up call requirement for the trauma surgeons.
"We think of this back-up call requirement as patient-centric; when you’re busy, patients aren’t well taken care of," he said. "You’ve just flipped this argument for me, which is that there’s another human being involved: the trauma surgeon. I’m going to go back, show him your abstract, and say, ‘There is another human being at work here and maybe at that fifth critical ... that fifth Level 1 activation ... it’s time to call the back-up guy.’ "
One attendee rose to say she’d just lost a colleague to PTSD and asked who should best perform an intervention to avoid any potential harm to the surgeon’s career. Another attendee responded that what’s helped the military address PTSD in its health care workers is to try to remove the perceived stigma of PTSD.
Dr. Joseph agreed that the military has been instrumental in identifying this issue and could join with EAST and other professional organizations in developing an intervention for its members. PTSD screening, even among residents, also would not go amiss.
Additional analyses will focus on protective factors among respondents who did not develop PTSD as well as how surgeons in other countries, such as South America, address the aftermath of dealing with violence, accidents, and injury on a daily basis.
"I think lack of insight is what you hear across all the comments," Dr. Joseph said. "We all think we’re Superman. People that know me know I’m probably as tough as they come, but at the same time we have to look back and realize this really does affect us. We’re not invincible."
Dr. Joseph and his coauthors reported having no financial disclosures.
This is an important study with salient findings of PTSD in trauma surgeons. As a psychiatrist and specialist in physician health, I agree with Dr. Bellal Joseph’s statement that "active surveillance to promote wellness among trauma surgeons is warranted." In fact, I’d go one step further and say that prevention and early intervention are essential and may be life saving.
Trauma surgeons are a precious commodity in our U.S. health care system. After re-reading an article in the New York Times featuring the heroic efforts of trauma team members, including Dr. Joseph, at the University of Arizona Medical Center after the shooting rampage that killed several and severely injured former Rep. Gabrielle Giffords, it’s a wonder that more trauma surgeons do not have PTSD symptoms or the full DSM-5 diagnosis!
We physicians are all human. At times, the resilience and emotional defenses that enable us to stay calm and focused and to do our work can fail us. That is not weakness or frailty; it’s simply an occupational hazard.
Dr. Michael F. Myers is professor of clinical psychiatry at State University of New York, Brooklyn.
This is an important study with salient findings of PTSD in trauma surgeons. As a psychiatrist and specialist in physician health, I agree with Dr. Bellal Joseph’s statement that "active surveillance to promote wellness among trauma surgeons is warranted." In fact, I’d go one step further and say that prevention and early intervention are essential and may be life saving.
Trauma surgeons are a precious commodity in our U.S. health care system. After re-reading an article in the New York Times featuring the heroic efforts of trauma team members, including Dr. Joseph, at the University of Arizona Medical Center after the shooting rampage that killed several and severely injured former Rep. Gabrielle Giffords, it’s a wonder that more trauma surgeons do not have PTSD symptoms or the full DSM-5 diagnosis!
We physicians are all human. At times, the resilience and emotional defenses that enable us to stay calm and focused and to do our work can fail us. That is not weakness or frailty; it’s simply an occupational hazard.
Dr. Michael F. Myers is professor of clinical psychiatry at State University of New York, Brooklyn.
This is an important study with salient findings of PTSD in trauma surgeons. As a psychiatrist and specialist in physician health, I agree with Dr. Bellal Joseph’s statement that "active surveillance to promote wellness among trauma surgeons is warranted." In fact, I’d go one step further and say that prevention and early intervention are essential and may be life saving.
Trauma surgeons are a precious commodity in our U.S. health care system. After re-reading an article in the New York Times featuring the heroic efforts of trauma team members, including Dr. Joseph, at the University of Arizona Medical Center after the shooting rampage that killed several and severely injured former Rep. Gabrielle Giffords, it’s a wonder that more trauma surgeons do not have PTSD symptoms or the full DSM-5 diagnosis!
We physicians are all human. At times, the resilience and emotional defenses that enable us to stay calm and focused and to do our work can fail us. That is not weakness or frailty; it’s simply an occupational hazard.
Dr. Michael F. Myers is professor of clinical psychiatry at State University of New York, Brooklyn.
NAPLES, FLA. – Posttraumatic stress disorder is disturbingly common among U.S. trauma surgeons, according to a national survey.
Among 453 members of the American Association for the Surgery of Trauma (AAST) and Eastern Association for the Surgery of Trauma (EAST), 40% had symptoms of PTSD and 15% met the diagnostic criteria for PTSD.
"It’s the elephant in the room," Dr. Bellal A. Joseph said at the annual scientific assembly of EAST.
Understanding the factors that predispose trauma surgeons to PTSD may benefit patients and the profession and may be useful to national trauma surgery associations to develop targeted interventions, said Dr. Joseph, a trauma and critical care surgeon at the University of Arizona Medical Center, Tucson.
"Active surveillance to promote wellness among trauma surgeons is warranted," he said.
Invited discussant Dr. Karen Lommel, a psychiatrist who recently converted to emergency medicine at the University of Kentucky, Lexington, described the findings as "quite remarkable."
"The issue of posttraumatic symptoms and PTSD affects all of us who work in trauma, whether we choose to acknowledge it or not," she said. "Pre-hospital workers, nurses, and mental health professionals have been extensively included in PTSD studies. Unfortunately, trauma surgeons – one of the most stoic of frontline providers – have been overlooked."
Dr. Joseph described receiving pushback when proposing the study to other trauma surgeons and was told flat-out by one respondent that its hypothesis is flawed.
A self-identified senior surgeon wrote: "I found that the assumptions of the questions did not fit the trauma program I work in nor the surgeons with whom I work. They actually take trauma call to relax. Stress is not a word in our vocabulary."
The two-part survey, sent to all members of EAST and the AAST (41% response rate), was not specifically identified as a PTSD survey, but included the validated PTSD CheckList-Civilian Version (PCL-C). A score of 35 or more on the 17-item PCL-C has previously shown a sensitivity of 85% for PTSD symptoms, while a score of 44 or more is 95% sensitive and 86% specific for a PTSD diagnosis, Dr. Joseph observed.
The survey respondents were mostly male (76%), white (80%), practiced in an urban hospital (89.6%), or Level 1 trauma center (71%). More than half (54.7%) had 11 years or more of clinical practice, 21% had military experience, and 14.3% had been deployed to war.
Three-fourths (66.4%) had an annual income of at least $300,000, but 90.5% spent no more than 4 hours per day of non–sleep relaxation and 26.5% took no more than 2 weeks vacation per year.
Only 6.2% said they suffered from depression and 3% from anxiety, but 66% reported using alcohol and 5.3% smoking.
Regarding the scope of their work, 85% had four or more 24-hour calls per month, 36% had at least three critical cases per call, and 24% had at least 10 operative trauma cases per month.
Surgeons who had more than five critical cases per call were seven times more likely to develop PTSD in multivariate analysis (odds ratio, 7; P = .001), Dr. Joseph said. No other factors were significantly associated with a PTSD diagnosis.
Independent predictors of PTSD symptoms in the multivariate analysis were male sex (OR, 2; P = .04); more than seven call duties/month (OR, 2.6; P = .001); more than 15 operative cases/month (OR, 3; P = .001); less than 4 hours of daily relaxation (OR, 7; P = .01)’ and less than 2 weeks of vacation/year (OR, 2: P = .02); he said.
Following the presentation, a surgeon from the Bronx, N.Y., said one of the sticking points for his CEO in the state’s move toward American College of Surgeons’ verification is the back-up call requirement for the trauma surgeons.
"We think of this back-up call requirement as patient-centric; when you’re busy, patients aren’t well taken care of," he said. "You’ve just flipped this argument for me, which is that there’s another human being involved: the trauma surgeon. I’m going to go back, show him your abstract, and say, ‘There is another human being at work here and maybe at that fifth critical ... that fifth Level 1 activation ... it’s time to call the back-up guy.’ "
One attendee rose to say she’d just lost a colleague to PTSD and asked who should best perform an intervention to avoid any potential harm to the surgeon’s career. Another attendee responded that what’s helped the military address PTSD in its health care workers is to try to remove the perceived stigma of PTSD.
Dr. Joseph agreed that the military has been instrumental in identifying this issue and could join with EAST and other professional organizations in developing an intervention for its members. PTSD screening, even among residents, also would not go amiss.
Additional analyses will focus on protective factors among respondents who did not develop PTSD as well as how surgeons in other countries, such as South America, address the aftermath of dealing with violence, accidents, and injury on a daily basis.
"I think lack of insight is what you hear across all the comments," Dr. Joseph said. "We all think we’re Superman. People that know me know I’m probably as tough as they come, but at the same time we have to look back and realize this really does affect us. We’re not invincible."
Dr. Joseph and his coauthors reported having no financial disclosures.
NAPLES, FLA. – Posttraumatic stress disorder is disturbingly common among U.S. trauma surgeons, according to a national survey.
Among 453 members of the American Association for the Surgery of Trauma (AAST) and Eastern Association for the Surgery of Trauma (EAST), 40% had symptoms of PTSD and 15% met the diagnostic criteria for PTSD.
"It’s the elephant in the room," Dr. Bellal A. Joseph said at the annual scientific assembly of EAST.
Understanding the factors that predispose trauma surgeons to PTSD may benefit patients and the profession and may be useful to national trauma surgery associations to develop targeted interventions, said Dr. Joseph, a trauma and critical care surgeon at the University of Arizona Medical Center, Tucson.
"Active surveillance to promote wellness among trauma surgeons is warranted," he said.
Invited discussant Dr. Karen Lommel, a psychiatrist who recently converted to emergency medicine at the University of Kentucky, Lexington, described the findings as "quite remarkable."
"The issue of posttraumatic symptoms and PTSD affects all of us who work in trauma, whether we choose to acknowledge it or not," she said. "Pre-hospital workers, nurses, and mental health professionals have been extensively included in PTSD studies. Unfortunately, trauma surgeons – one of the most stoic of frontline providers – have been overlooked."
Dr. Joseph described receiving pushback when proposing the study to other trauma surgeons and was told flat-out by one respondent that its hypothesis is flawed.
A self-identified senior surgeon wrote: "I found that the assumptions of the questions did not fit the trauma program I work in nor the surgeons with whom I work. They actually take trauma call to relax. Stress is not a word in our vocabulary."
The two-part survey, sent to all members of EAST and the AAST (41% response rate), was not specifically identified as a PTSD survey, but included the validated PTSD CheckList-Civilian Version (PCL-C). A score of 35 or more on the 17-item PCL-C has previously shown a sensitivity of 85% for PTSD symptoms, while a score of 44 or more is 95% sensitive and 86% specific for a PTSD diagnosis, Dr. Joseph observed.
The survey respondents were mostly male (76%), white (80%), practiced in an urban hospital (89.6%), or Level 1 trauma center (71%). More than half (54.7%) had 11 years or more of clinical practice, 21% had military experience, and 14.3% had been deployed to war.
Three-fourths (66.4%) had an annual income of at least $300,000, but 90.5% spent no more than 4 hours per day of non–sleep relaxation and 26.5% took no more than 2 weeks vacation per year.
Only 6.2% said they suffered from depression and 3% from anxiety, but 66% reported using alcohol and 5.3% smoking.
Regarding the scope of their work, 85% had four or more 24-hour calls per month, 36% had at least three critical cases per call, and 24% had at least 10 operative trauma cases per month.
Surgeons who had more than five critical cases per call were seven times more likely to develop PTSD in multivariate analysis (odds ratio, 7; P = .001), Dr. Joseph said. No other factors were significantly associated with a PTSD diagnosis.
Independent predictors of PTSD symptoms in the multivariate analysis were male sex (OR, 2; P = .04); more than seven call duties/month (OR, 2.6; P = .001); more than 15 operative cases/month (OR, 3; P = .001); less than 4 hours of daily relaxation (OR, 7; P = .01)’ and less than 2 weeks of vacation/year (OR, 2: P = .02); he said.
Following the presentation, a surgeon from the Bronx, N.Y., said one of the sticking points for his CEO in the state’s move toward American College of Surgeons’ verification is the back-up call requirement for the trauma surgeons.
"We think of this back-up call requirement as patient-centric; when you’re busy, patients aren’t well taken care of," he said. "You’ve just flipped this argument for me, which is that there’s another human being involved: the trauma surgeon. I’m going to go back, show him your abstract, and say, ‘There is another human being at work here and maybe at that fifth critical ... that fifth Level 1 activation ... it’s time to call the back-up guy.’ "
One attendee rose to say she’d just lost a colleague to PTSD and asked who should best perform an intervention to avoid any potential harm to the surgeon’s career. Another attendee responded that what’s helped the military address PTSD in its health care workers is to try to remove the perceived stigma of PTSD.
Dr. Joseph agreed that the military has been instrumental in identifying this issue and could join with EAST and other professional organizations in developing an intervention for its members. PTSD screening, even among residents, also would not go amiss.
Additional analyses will focus on protective factors among respondents who did not develop PTSD as well as how surgeons in other countries, such as South America, address the aftermath of dealing with violence, accidents, and injury on a daily basis.
"I think lack of insight is what you hear across all the comments," Dr. Joseph said. "We all think we’re Superman. People that know me know I’m probably as tough as they come, but at the same time we have to look back and realize this really does affect us. We’re not invincible."
Dr. Joseph and his coauthors reported having no financial disclosures.
AT EAST 2014
Major finding: 40% of respondents had PTSD symptoms and 15% met the diagnostic criteria for PTSD.
Data source: A prospective survey of 453 members of EAST and the AAST.
Disclosures: Dr. Joseph reported having no financial disclosures.
Failure to rescue driving AAA repair mortality
CHICAGO – Failure to rescue patients from major complications drives much of the variation in hospital mortality for abdominal aortic aneurysm repair, an award-winning study suggests.
"Careful attention to early recognition and management of postoperative complications could be the key to improving mortality," Dr. Seth Waits reported at the annual meeting of the Midwestern Vascular Surgical Society.
Failure to rescue (FTR), or death after a complication, is increasing being recognized as a source of differences in hospital mortality. A recent study reported that women who experienced a major complication after ovarian cancer treatment at a low-volume hospital were 48% more likely to die than were their counterparts at a high-volume hospital. Complication rates, long thought to be the culprit behind higher hospital mortality, were similar at the hospitals, while FTR rates were almost double at the low-volume hospitals (J. Clin. Oncol. 2012;30:3976-82).
For the current analysis, Dr. Waits and his colleagues at the University of Michigan Frankel Cardiovascular Center in Ann Arbor, calculated risk-adjusted mortality rates for 3,215 patients who underwent open or endovascular abdominal aortic aneurysm (AAA) repair at 40 hospitals participating in the Michigan Surgical Quality Collaborative between 2007 and 2012.
For 2,440 patients undergoing endovascular repair, hospital mortality ranged from a low of 0.07% to a high of 6.14%.
Though low- and high-mortality hospitals had similar major complication rates (11.6% vs. 10.6%), FTR rates were 45 times greater in high-mortality hospitals (0.83% vs. 37.5%), Dr. Waits reported.
For 775 patients who underwent open AAA repair, hospital mortality ranged from 4.5% to 16.4%.
Once again, despite low- and high-mortality hospitals having nearly identical complication rates (45.1% vs. 45.8%), but FTR rates were three times higher at the high-mortality hospitals (10.3% vs. 33%), he said.
An average of 2.85 and 2.66 severe complications occurred per FTR event for open and endovascular repair, respectively.
Transfusion was the most common postoperative complication leading to a FTR event for endovascular and open repair (5.8% and 29.8%, respectively), followed by prolonged intubation (2.4%; 18.2%) and reintubation (9.2%; 2%), according to the meeting’s best poster presentation.
No significant difference was seen in rupture/emergent repair between low- and high-mortality hospitals.
Dr. Waits called for preoperative identification of high-risk patients and use of FTR countermeasures, such as improved ICU admission, anesthesia alerts, and nurse/physician awareness to improve AAA mortality.
"Understanding the mechanisms that underlie failure to rescue offers the opportunity to move from a reactive to proactive approach in our management of complications following abdominal aortic aneurysm repair," he said in an interview.
Dr. Waits and his coauthors reported having no financial disclosures.
CHICAGO – Failure to rescue patients from major complications drives much of the variation in hospital mortality for abdominal aortic aneurysm repair, an award-winning study suggests.
"Careful attention to early recognition and management of postoperative complications could be the key to improving mortality," Dr. Seth Waits reported at the annual meeting of the Midwestern Vascular Surgical Society.
Failure to rescue (FTR), or death after a complication, is increasing being recognized as a source of differences in hospital mortality. A recent study reported that women who experienced a major complication after ovarian cancer treatment at a low-volume hospital were 48% more likely to die than were their counterparts at a high-volume hospital. Complication rates, long thought to be the culprit behind higher hospital mortality, were similar at the hospitals, while FTR rates were almost double at the low-volume hospitals (J. Clin. Oncol. 2012;30:3976-82).
For the current analysis, Dr. Waits and his colleagues at the University of Michigan Frankel Cardiovascular Center in Ann Arbor, calculated risk-adjusted mortality rates for 3,215 patients who underwent open or endovascular abdominal aortic aneurysm (AAA) repair at 40 hospitals participating in the Michigan Surgical Quality Collaborative between 2007 and 2012.
For 2,440 patients undergoing endovascular repair, hospital mortality ranged from a low of 0.07% to a high of 6.14%.
Though low- and high-mortality hospitals had similar major complication rates (11.6% vs. 10.6%), FTR rates were 45 times greater in high-mortality hospitals (0.83% vs. 37.5%), Dr. Waits reported.
For 775 patients who underwent open AAA repair, hospital mortality ranged from 4.5% to 16.4%.
Once again, despite low- and high-mortality hospitals having nearly identical complication rates (45.1% vs. 45.8%), but FTR rates were three times higher at the high-mortality hospitals (10.3% vs. 33%), he said.
An average of 2.85 and 2.66 severe complications occurred per FTR event for open and endovascular repair, respectively.
Transfusion was the most common postoperative complication leading to a FTR event for endovascular and open repair (5.8% and 29.8%, respectively), followed by prolonged intubation (2.4%; 18.2%) and reintubation (9.2%; 2%), according to the meeting’s best poster presentation.
No significant difference was seen in rupture/emergent repair between low- and high-mortality hospitals.
Dr. Waits called for preoperative identification of high-risk patients and use of FTR countermeasures, such as improved ICU admission, anesthesia alerts, and nurse/physician awareness to improve AAA mortality.
"Understanding the mechanisms that underlie failure to rescue offers the opportunity to move from a reactive to proactive approach in our management of complications following abdominal aortic aneurysm repair," he said in an interview.
Dr. Waits and his coauthors reported having no financial disclosures.
CHICAGO – Failure to rescue patients from major complications drives much of the variation in hospital mortality for abdominal aortic aneurysm repair, an award-winning study suggests.
"Careful attention to early recognition and management of postoperative complications could be the key to improving mortality," Dr. Seth Waits reported at the annual meeting of the Midwestern Vascular Surgical Society.
Failure to rescue (FTR), or death after a complication, is increasing being recognized as a source of differences in hospital mortality. A recent study reported that women who experienced a major complication after ovarian cancer treatment at a low-volume hospital were 48% more likely to die than were their counterparts at a high-volume hospital. Complication rates, long thought to be the culprit behind higher hospital mortality, were similar at the hospitals, while FTR rates were almost double at the low-volume hospitals (J. Clin. Oncol. 2012;30:3976-82).
For the current analysis, Dr. Waits and his colleagues at the University of Michigan Frankel Cardiovascular Center in Ann Arbor, calculated risk-adjusted mortality rates for 3,215 patients who underwent open or endovascular abdominal aortic aneurysm (AAA) repair at 40 hospitals participating in the Michigan Surgical Quality Collaborative between 2007 and 2012.
For 2,440 patients undergoing endovascular repair, hospital mortality ranged from a low of 0.07% to a high of 6.14%.
Though low- and high-mortality hospitals had similar major complication rates (11.6% vs. 10.6%), FTR rates were 45 times greater in high-mortality hospitals (0.83% vs. 37.5%), Dr. Waits reported.
For 775 patients who underwent open AAA repair, hospital mortality ranged from 4.5% to 16.4%.
Once again, despite low- and high-mortality hospitals having nearly identical complication rates (45.1% vs. 45.8%), but FTR rates were three times higher at the high-mortality hospitals (10.3% vs. 33%), he said.
An average of 2.85 and 2.66 severe complications occurred per FTR event for open and endovascular repair, respectively.
Transfusion was the most common postoperative complication leading to a FTR event for endovascular and open repair (5.8% and 29.8%, respectively), followed by prolonged intubation (2.4%; 18.2%) and reintubation (9.2%; 2%), according to the meeting’s best poster presentation.
No significant difference was seen in rupture/emergent repair between low- and high-mortality hospitals.
Dr. Waits called for preoperative identification of high-risk patients and use of FTR countermeasures, such as improved ICU admission, anesthesia alerts, and nurse/physician awareness to improve AAA mortality.
"Understanding the mechanisms that underlie failure to rescue offers the opportunity to move from a reactive to proactive approach in our management of complications following abdominal aortic aneurysm repair," he said in an interview.
Dr. Waits and his coauthors reported having no financial disclosures.
AT MIDWESTERN VASCULAR 2013
Major finding: FTR rates were 45 times higher in high AAA-mortality hospitals vs. low AAA-mortality hospitals (0.83% vs. 37.5%).
Data source: Retrospective study of 3,215 patients with abdominal aortic aneurysm repair.
Disclosures: Dr. Waits and his coauthors reported having no financial disclosures.
Anatomy dictates endovascular repair of popliteal artery aneurysms
CHICAGO – Endovascular repair of popliteal artery aneurysms is a relatively safe and viable off-label alternative to open repair, but appropriate anatomy is essential. This includes a landing zone of at least 2 cm above and below the aneurysm, minimal discrepancy in size between the proximal and distal landing zones, and lack of extensive vessel tortuosity due to potential kinking of the endograft, Dr. Neal S. Cayne said at a symposium on vascular surgery sponsored by Northwestern University.
The risk of kinking and graft thrombosis also excludes patients who frequently flex their knee more than 90 degrees, such as carpenters and gardeners.
Patients with a contraindication to antiplatelet medication are also off limits, as clopidogrel (Plavix) has been shown to be a predictor of success, said Dr. Cayne, director of endovascular surgery at New York University Langone Medical Center.
In 2012, his team reported technical success in 25 of 26 endovascular popliteal artery aneurysm (PAA) repairs performed in 21 consecutive patients between January 2004 and January 2011, with the one technical failure due to stent graft infolding (J. Vasc. Surg. 2012;55:1647-53).
Primary and secondary patency rates were both 91.2% at 1 year, and were 85.5% and 91.2%, respectively, at 2 years. All patients were maintained on aspirin or clopidogrel.
No limb loss was reported, but three occlusions occurred during follow-up at 4, 14, and 26 months. One patient required a tibial artery bypass for a nonhealing wound, and two were successfully repaired with open thrombectomy. All three occlusion patients had single-vessel runoff.
Based on our data, in general, I will not stent someone "with single-vessel outflow, and I also will not stent someone who, for some reason, can’t take antiplatelet agents," Dr. Cayne said.
Even when patients present urgently and the PAA has thrombosed, endovascular repair is not an option if there is only one outflow vessel. "I would do a bypass; there’s nothing wrong with open surgery," he said.
A recent unpublished review of 79 PAAs treated at Langone from 1998 to 2012 with both approaches found 5-year primary patencies of 67% for open repair and 80% for endovascular repair (P less than .05). Secondary patency was 90% in both groups.
One amputation occurred in the open group, but occlusion rates were higher using endovascular repair with one-vessel runoff (P = .003), Dr. Cayne said.
As expected, length of stay was shorter with endovascular repair (1.9 vs. 6.4 days; P less than .001).
Follow-up was longer for the 36 open PAAs than the 43 endovascular PAAs (75 vs. 34 months), but patients in both groups were similar with respect to age, comorbidities, PAA size, runoff, and symptoms, he said.
During a discussion following the presentation, some attendees said they still prefer to use bypass for all patients with PAA, and asked how candidates are selected for stent placement.
"Number one and most important is the anatomy," Dr. Cayne said. "The one advantage of endovascular repair is that if you have a patient too sick to get general or even regional anesthesia, you can do it under local [anesthesia] almost all the time with a small cutdown or puncture. But you do have that long discussion with the patient that this is a non–FDA-approved, off-label use. We provide them with the data, but some patients in New York will come in with pages and pages of literature and say, ‘Nope, I want a stent, I want this particular stent, and this is the way I want you to do it.’ "
The stent of choice at Langone has been Gore’s Viabahn covered stent graft, which is FDA approved for treating occlusive disease rather than PAA. The device is usually oversized by 10%-15%, but no more than that, because of the risk of graft infolding, Dr. Cayne said.
If more than one graft is needed, a maximum of no more than 1-mm size differential between grafts is suggested. A minimum overlap of 2-3 cm between grafts is also preferred.
Last year, surgeons reported a dismal 50% occlusion rate within just 6 weeks in the endovascular treatment of six PAAs using a novel, multilayer stent (Cardiatis’s Multilayer Aneurysm Repair System) (J. Endovasc. Ther. 2013;20:381-8), he observed.
Dr. Cayne reported receiving honoraria as a consultant from Cook Medical.
CHICAGO – Endovascular repair of popliteal artery aneurysms is a relatively safe and viable off-label alternative to open repair, but appropriate anatomy is essential. This includes a landing zone of at least 2 cm above and below the aneurysm, minimal discrepancy in size between the proximal and distal landing zones, and lack of extensive vessel tortuosity due to potential kinking of the endograft, Dr. Neal S. Cayne said at a symposium on vascular surgery sponsored by Northwestern University.
The risk of kinking and graft thrombosis also excludes patients who frequently flex their knee more than 90 degrees, such as carpenters and gardeners.
Patients with a contraindication to antiplatelet medication are also off limits, as clopidogrel (Plavix) has been shown to be a predictor of success, said Dr. Cayne, director of endovascular surgery at New York University Langone Medical Center.
In 2012, his team reported technical success in 25 of 26 endovascular popliteal artery aneurysm (PAA) repairs performed in 21 consecutive patients between January 2004 and January 2011, with the one technical failure due to stent graft infolding (J. Vasc. Surg. 2012;55:1647-53).
Primary and secondary patency rates were both 91.2% at 1 year, and were 85.5% and 91.2%, respectively, at 2 years. All patients were maintained on aspirin or clopidogrel.
No limb loss was reported, but three occlusions occurred during follow-up at 4, 14, and 26 months. One patient required a tibial artery bypass for a nonhealing wound, and two were successfully repaired with open thrombectomy. All three occlusion patients had single-vessel runoff.
Based on our data, in general, I will not stent someone "with single-vessel outflow, and I also will not stent someone who, for some reason, can’t take antiplatelet agents," Dr. Cayne said.
Even when patients present urgently and the PAA has thrombosed, endovascular repair is not an option if there is only one outflow vessel. "I would do a bypass; there’s nothing wrong with open surgery," he said.
A recent unpublished review of 79 PAAs treated at Langone from 1998 to 2012 with both approaches found 5-year primary patencies of 67% for open repair and 80% for endovascular repair (P less than .05). Secondary patency was 90% in both groups.
One amputation occurred in the open group, but occlusion rates were higher using endovascular repair with one-vessel runoff (P = .003), Dr. Cayne said.
As expected, length of stay was shorter with endovascular repair (1.9 vs. 6.4 days; P less than .001).
Follow-up was longer for the 36 open PAAs than the 43 endovascular PAAs (75 vs. 34 months), but patients in both groups were similar with respect to age, comorbidities, PAA size, runoff, and symptoms, he said.
During a discussion following the presentation, some attendees said they still prefer to use bypass for all patients with PAA, and asked how candidates are selected for stent placement.
"Number one and most important is the anatomy," Dr. Cayne said. "The one advantage of endovascular repair is that if you have a patient too sick to get general or even regional anesthesia, you can do it under local [anesthesia] almost all the time with a small cutdown or puncture. But you do have that long discussion with the patient that this is a non–FDA-approved, off-label use. We provide them with the data, but some patients in New York will come in with pages and pages of literature and say, ‘Nope, I want a stent, I want this particular stent, and this is the way I want you to do it.’ "
The stent of choice at Langone has been Gore’s Viabahn covered stent graft, which is FDA approved for treating occlusive disease rather than PAA. The device is usually oversized by 10%-15%, but no more than that, because of the risk of graft infolding, Dr. Cayne said.
If more than one graft is needed, a maximum of no more than 1-mm size differential between grafts is suggested. A minimum overlap of 2-3 cm between grafts is also preferred.
Last year, surgeons reported a dismal 50% occlusion rate within just 6 weeks in the endovascular treatment of six PAAs using a novel, multilayer stent (Cardiatis’s Multilayer Aneurysm Repair System) (J. Endovasc. Ther. 2013;20:381-8), he observed.
Dr. Cayne reported receiving honoraria as a consultant from Cook Medical.
CHICAGO – Endovascular repair of popliteal artery aneurysms is a relatively safe and viable off-label alternative to open repair, but appropriate anatomy is essential. This includes a landing zone of at least 2 cm above and below the aneurysm, minimal discrepancy in size between the proximal and distal landing zones, and lack of extensive vessel tortuosity due to potential kinking of the endograft, Dr. Neal S. Cayne said at a symposium on vascular surgery sponsored by Northwestern University.
The risk of kinking and graft thrombosis also excludes patients who frequently flex their knee more than 90 degrees, such as carpenters and gardeners.
Patients with a contraindication to antiplatelet medication are also off limits, as clopidogrel (Plavix) has been shown to be a predictor of success, said Dr. Cayne, director of endovascular surgery at New York University Langone Medical Center.
In 2012, his team reported technical success in 25 of 26 endovascular popliteal artery aneurysm (PAA) repairs performed in 21 consecutive patients between January 2004 and January 2011, with the one technical failure due to stent graft infolding (J. Vasc. Surg. 2012;55:1647-53).
Primary and secondary patency rates were both 91.2% at 1 year, and were 85.5% and 91.2%, respectively, at 2 years. All patients were maintained on aspirin or clopidogrel.
No limb loss was reported, but three occlusions occurred during follow-up at 4, 14, and 26 months. One patient required a tibial artery bypass for a nonhealing wound, and two were successfully repaired with open thrombectomy. All three occlusion patients had single-vessel runoff.
Based on our data, in general, I will not stent someone "with single-vessel outflow, and I also will not stent someone who, for some reason, can’t take antiplatelet agents," Dr. Cayne said.
Even when patients present urgently and the PAA has thrombosed, endovascular repair is not an option if there is only one outflow vessel. "I would do a bypass; there’s nothing wrong with open surgery," he said.
A recent unpublished review of 79 PAAs treated at Langone from 1998 to 2012 with both approaches found 5-year primary patencies of 67% for open repair and 80% for endovascular repair (P less than .05). Secondary patency was 90% in both groups.
One amputation occurred in the open group, but occlusion rates were higher using endovascular repair with one-vessel runoff (P = .003), Dr. Cayne said.
As expected, length of stay was shorter with endovascular repair (1.9 vs. 6.4 days; P less than .001).
Follow-up was longer for the 36 open PAAs than the 43 endovascular PAAs (75 vs. 34 months), but patients in both groups were similar with respect to age, comorbidities, PAA size, runoff, and symptoms, he said.
During a discussion following the presentation, some attendees said they still prefer to use bypass for all patients with PAA, and asked how candidates are selected for stent placement.
"Number one and most important is the anatomy," Dr. Cayne said. "The one advantage of endovascular repair is that if you have a patient too sick to get general or even regional anesthesia, you can do it under local [anesthesia] almost all the time with a small cutdown or puncture. But you do have that long discussion with the patient that this is a non–FDA-approved, off-label use. We provide them with the data, but some patients in New York will come in with pages and pages of literature and say, ‘Nope, I want a stent, I want this particular stent, and this is the way I want you to do it.’ "
The stent of choice at Langone has been Gore’s Viabahn covered stent graft, which is FDA approved for treating occlusive disease rather than PAA. The device is usually oversized by 10%-15%, but no more than that, because of the risk of graft infolding, Dr. Cayne said.
If more than one graft is needed, a maximum of no more than 1-mm size differential between grafts is suggested. A minimum overlap of 2-3 cm between grafts is also preferred.
Last year, surgeons reported a dismal 50% occlusion rate within just 6 weeks in the endovascular treatment of six PAAs using a novel, multilayer stent (Cardiatis’s Multilayer Aneurysm Repair System) (J. Endovasc. Ther. 2013;20:381-8), he observed.
Dr. Cayne reported receiving honoraria as a consultant from Cook Medical.
AT THE NORTHWESTERN VASCULAR SYMPOSIUM
Major finding: Five-year primary patency was 67% for open repair and 80% for endovascular repair (P less than .05).
Data source: Expert opinion and retrospective study of 79 popliteal artery aneurysm repairs.
Disclosures: Dr. Cayne reported receiving honoraria as a consultant from Cook Medical.
DRIL particularly effective for access-related hand ischemia
CHICAGO – The best strategy for access-related hand ischemia is to have a plan in place before it occurs.
"The whole approach for patients at high risk of developing hand ischemia is to think about it preoperatively" and devise a remedial plan, Dr. Thomas S. Huber said at the symposium. "I always tell our trainees and fellows: ‘What are you going to do in 20 minutes when the recovery room nurse says the patient has motor compromise and unbelievable hand pain?’ You have to have a remedial plan."
Access-related hand ischemia (ARHI), or steal syndrome, occurs in just 2% of radial artery–based access procedures, but up to 20% of brachial artery–based access procedures. Roughly half of these events are severe enough to merit remedial treatment. With more than 8 million arterial catheters placed perioperatively in the United States each year and 350,000 patients on dialysis, the numbers add up.
"There are multiple complementary treatment options that you ought to have in your armamentarium," said Dr. Huber, chief of vascular surgery and endovascular therapy, University of Florida Health Science Center, Gainesville, Fla.
"The DRIL has worked remarkably well for us."
The distal revascularization and interval ligation (DRIL) procedure involves a brachial-brachial bypass with ligation of the brachial artery immediately distal to the fistula anastomosis.
In their hands, DRIL significantly increased wrist-brachial and digital-brachial indices (0.31 and 0.25) in 126 patients undergoing 134 procedures from 2002 to 2011 (J. Vasc. Surg. 2013;57:451-8). Ischemic symptoms were relieved in 82% of patients, and the index access was salvaged in 85%.
"Really, the DRIL procedure has almost no impact on the success of the access," Dr. Huber said. "For those patients [in which] we perform the DRIL [procedure] before their access is mature, our maturation rate is comparable whether we do the DRIL or not."
Primary patency was 95% at 1 year and 78% at 5 years. The overall complication rate, driven mostly by wound complications, reached 27%, and 30-day mortality was 2%.
"I sheepishly stand before you to say that our mortality rate for all our access procedures is about 3%," he said. "It’s a pretty minimal operation so, my gosh, how could that possibly be? But it’s a very morbid population. In our country, the 1-year mortality rate for people starting dialysis is right at 23%. So they’re older, sicker patients, with a limited life expectancy."
All-cause mortality in the series was 28% and 79% at 1 and 5 years, respectively. Age greater than 40 years, grade 3 ischemia, any DRIL complication, and smoking history were all significant multivariable predictors of mortality.
An extensive list of clinical ARHI predictors has been identified, such as female sex, advanced age, and large conduits, but none reliably predicts when access should not be attempted, Dr. Huber said. The use of preoperative noninvasive imaging also is helpful to identify patients at risk for ARHI, but the predictive values have not been sufficient to avoid attempting the access procedure.
In their experience, presentation of hand ischemia has been trimodal, with a third of patients presenting within 7 days of their index procedure, a third within 7-30 days, and a third thereafter. A weak ulnar or radial pulse on physical exam after creating a dialysis access has misled some to dismiss hand ischemia, while a prior episode of ARHI is a red flag for high risk of recurrence.
"I would contend that the incidence of developing hand ischemia on the right arm if you had it on the left arm is about 100%," dispelling the concept of simply ligating the access that led to hand ischemia and then repositioning it on the contralateral extremity, Dr. Huber said.
Their overall treatment approach for ARHI in poor operative-risk patients, particularly older patients with a prosthetic access, is to proceed to ligation. Good-risk patients undergo some type of inflow assessment, and if a significant inflow lesion is present, it is corrected, usually at the same time as the DRIL, he said. Proximalization of the arterial inflow would be considered for patients with persistent symptoms and no available conduit, while DRIL is the go-to procedure for those with available vein conduits more than 3 cm in diameter, preferably the greater saphenous vein.
Noticeably absent in their algorithm is some type of flow-limiting strategy, such as banding, and the revision using distal inflow procedure. These approaches may have a role, but the published literature is somewhat inconclusive, Dr. Huber said at the symposium, sponsored by Northwestern University.
Despite the overwhelming number of Americans on dialysis, less than 300 DRIL cases have been reported in the literature since its introduction in 1988. The University of Florida experience has been corroborated by a recent report of complete symptom resolution in 82% of 81 DRIL procedures, with a 17% complication rate, and five-year access and bypass survival rates of 56% and 97% (J. Vasc. Surg. 2013;54:1073-8).
Surgeons in Texas reported full symptom resolution in 77% of 33 patients, but cautioned against potential complications such as bypass failure that led to gangrene and transmetacarpal amputation in one patient (J. Vasc. Access 2012;13:299-304).
Dr. Huber reported having no financial disclosures.
CHICAGO – The best strategy for access-related hand ischemia is to have a plan in place before it occurs.
"The whole approach for patients at high risk of developing hand ischemia is to think about it preoperatively" and devise a remedial plan, Dr. Thomas S. Huber said at the symposium. "I always tell our trainees and fellows: ‘What are you going to do in 20 minutes when the recovery room nurse says the patient has motor compromise and unbelievable hand pain?’ You have to have a remedial plan."
Access-related hand ischemia (ARHI), or steal syndrome, occurs in just 2% of radial artery–based access procedures, but up to 20% of brachial artery–based access procedures. Roughly half of these events are severe enough to merit remedial treatment. With more than 8 million arterial catheters placed perioperatively in the United States each year and 350,000 patients on dialysis, the numbers add up.
"There are multiple complementary treatment options that you ought to have in your armamentarium," said Dr. Huber, chief of vascular surgery and endovascular therapy, University of Florida Health Science Center, Gainesville, Fla.
"The DRIL has worked remarkably well for us."
The distal revascularization and interval ligation (DRIL) procedure involves a brachial-brachial bypass with ligation of the brachial artery immediately distal to the fistula anastomosis.
In their hands, DRIL significantly increased wrist-brachial and digital-brachial indices (0.31 and 0.25) in 126 patients undergoing 134 procedures from 2002 to 2011 (J. Vasc. Surg. 2013;57:451-8). Ischemic symptoms were relieved in 82% of patients, and the index access was salvaged in 85%.
"Really, the DRIL procedure has almost no impact on the success of the access," Dr. Huber said. "For those patients [in which] we perform the DRIL [procedure] before their access is mature, our maturation rate is comparable whether we do the DRIL or not."
Primary patency was 95% at 1 year and 78% at 5 years. The overall complication rate, driven mostly by wound complications, reached 27%, and 30-day mortality was 2%.
"I sheepishly stand before you to say that our mortality rate for all our access procedures is about 3%," he said. "It’s a pretty minimal operation so, my gosh, how could that possibly be? But it’s a very morbid population. In our country, the 1-year mortality rate for people starting dialysis is right at 23%. So they’re older, sicker patients, with a limited life expectancy."
All-cause mortality in the series was 28% and 79% at 1 and 5 years, respectively. Age greater than 40 years, grade 3 ischemia, any DRIL complication, and smoking history were all significant multivariable predictors of mortality.
An extensive list of clinical ARHI predictors has been identified, such as female sex, advanced age, and large conduits, but none reliably predicts when access should not be attempted, Dr. Huber said. The use of preoperative noninvasive imaging also is helpful to identify patients at risk for ARHI, but the predictive values have not been sufficient to avoid attempting the access procedure.
In their experience, presentation of hand ischemia has been trimodal, with a third of patients presenting within 7 days of their index procedure, a third within 7-30 days, and a third thereafter. A weak ulnar or radial pulse on physical exam after creating a dialysis access has misled some to dismiss hand ischemia, while a prior episode of ARHI is a red flag for high risk of recurrence.
"I would contend that the incidence of developing hand ischemia on the right arm if you had it on the left arm is about 100%," dispelling the concept of simply ligating the access that led to hand ischemia and then repositioning it on the contralateral extremity, Dr. Huber said.
Their overall treatment approach for ARHI in poor operative-risk patients, particularly older patients with a prosthetic access, is to proceed to ligation. Good-risk patients undergo some type of inflow assessment, and if a significant inflow lesion is present, it is corrected, usually at the same time as the DRIL, he said. Proximalization of the arterial inflow would be considered for patients with persistent symptoms and no available conduit, while DRIL is the go-to procedure for those with available vein conduits more than 3 cm in diameter, preferably the greater saphenous vein.
Noticeably absent in their algorithm is some type of flow-limiting strategy, such as banding, and the revision using distal inflow procedure. These approaches may have a role, but the published literature is somewhat inconclusive, Dr. Huber said at the symposium, sponsored by Northwestern University.
Despite the overwhelming number of Americans on dialysis, less than 300 DRIL cases have been reported in the literature since its introduction in 1988. The University of Florida experience has been corroborated by a recent report of complete symptom resolution in 82% of 81 DRIL procedures, with a 17% complication rate, and five-year access and bypass survival rates of 56% and 97% (J. Vasc. Surg. 2013;54:1073-8).
Surgeons in Texas reported full symptom resolution in 77% of 33 patients, but cautioned against potential complications such as bypass failure that led to gangrene and transmetacarpal amputation in one patient (J. Vasc. Access 2012;13:299-304).
Dr. Huber reported having no financial disclosures.
CHICAGO – The best strategy for access-related hand ischemia is to have a plan in place before it occurs.
"The whole approach for patients at high risk of developing hand ischemia is to think about it preoperatively" and devise a remedial plan, Dr. Thomas S. Huber said at the symposium. "I always tell our trainees and fellows: ‘What are you going to do in 20 minutes when the recovery room nurse says the patient has motor compromise and unbelievable hand pain?’ You have to have a remedial plan."
Access-related hand ischemia (ARHI), or steal syndrome, occurs in just 2% of radial artery–based access procedures, but up to 20% of brachial artery–based access procedures. Roughly half of these events are severe enough to merit remedial treatment. With more than 8 million arterial catheters placed perioperatively in the United States each year and 350,000 patients on dialysis, the numbers add up.
"There are multiple complementary treatment options that you ought to have in your armamentarium," said Dr. Huber, chief of vascular surgery and endovascular therapy, University of Florida Health Science Center, Gainesville, Fla.
"The DRIL has worked remarkably well for us."
The distal revascularization and interval ligation (DRIL) procedure involves a brachial-brachial bypass with ligation of the brachial artery immediately distal to the fistula anastomosis.
In their hands, DRIL significantly increased wrist-brachial and digital-brachial indices (0.31 and 0.25) in 126 patients undergoing 134 procedures from 2002 to 2011 (J. Vasc. Surg. 2013;57:451-8). Ischemic symptoms were relieved in 82% of patients, and the index access was salvaged in 85%.
"Really, the DRIL procedure has almost no impact on the success of the access," Dr. Huber said. "For those patients [in which] we perform the DRIL [procedure] before their access is mature, our maturation rate is comparable whether we do the DRIL or not."
Primary patency was 95% at 1 year and 78% at 5 years. The overall complication rate, driven mostly by wound complications, reached 27%, and 30-day mortality was 2%.
"I sheepishly stand before you to say that our mortality rate for all our access procedures is about 3%," he said. "It’s a pretty minimal operation so, my gosh, how could that possibly be? But it’s a very morbid population. In our country, the 1-year mortality rate for people starting dialysis is right at 23%. So they’re older, sicker patients, with a limited life expectancy."
All-cause mortality in the series was 28% and 79% at 1 and 5 years, respectively. Age greater than 40 years, grade 3 ischemia, any DRIL complication, and smoking history were all significant multivariable predictors of mortality.
An extensive list of clinical ARHI predictors has been identified, such as female sex, advanced age, and large conduits, but none reliably predicts when access should not be attempted, Dr. Huber said. The use of preoperative noninvasive imaging also is helpful to identify patients at risk for ARHI, but the predictive values have not been sufficient to avoid attempting the access procedure.
In their experience, presentation of hand ischemia has been trimodal, with a third of patients presenting within 7 days of their index procedure, a third within 7-30 days, and a third thereafter. A weak ulnar or radial pulse on physical exam after creating a dialysis access has misled some to dismiss hand ischemia, while a prior episode of ARHI is a red flag for high risk of recurrence.
"I would contend that the incidence of developing hand ischemia on the right arm if you had it on the left arm is about 100%," dispelling the concept of simply ligating the access that led to hand ischemia and then repositioning it on the contralateral extremity, Dr. Huber said.
Their overall treatment approach for ARHI in poor operative-risk patients, particularly older patients with a prosthetic access, is to proceed to ligation. Good-risk patients undergo some type of inflow assessment, and if a significant inflow lesion is present, it is corrected, usually at the same time as the DRIL, he said. Proximalization of the arterial inflow would be considered for patients with persistent symptoms and no available conduit, while DRIL is the go-to procedure for those with available vein conduits more than 3 cm in diameter, preferably the greater saphenous vein.
Noticeably absent in their algorithm is some type of flow-limiting strategy, such as banding, and the revision using distal inflow procedure. These approaches may have a role, but the published literature is somewhat inconclusive, Dr. Huber said at the symposium, sponsored by Northwestern University.
Despite the overwhelming number of Americans on dialysis, less than 300 DRIL cases have been reported in the literature since its introduction in 1988. The University of Florida experience has been corroborated by a recent report of complete symptom resolution in 82% of 81 DRIL procedures, with a 17% complication rate, and five-year access and bypass survival rates of 56% and 97% (J. Vasc. Surg. 2013;54:1073-8).
Surgeons in Texas reported full symptom resolution in 77% of 33 patients, but cautioned against potential complications such as bypass failure that led to gangrene and transmetacarpal amputation in one patient (J. Vasc. Access 2012;13:299-304).
Dr. Huber reported having no financial disclosures.
AT THE NORTHWESTERN VASCULAR SYMPOSIUM
CT negative: Take the C-collars off already
NAPLES, FLA. – Computed tomography of the cervical spine had 100% specificity and sensitivity in ruling out clinically significant fracture and ligamentous injuries after blunt trauma in a prospective cohort of 5,676 patients.
Patients with negative CT scans do not need further workup for possible ligamentous injury, as those were only identified in patients with a positive CT scan, Dr. Poornima Vanguri said at the annual scientific assembly of the Eastern Association for the Surgery of Trauma.
"Patients with a normal CT do not need further imaging and collars should be cleared as soon as possible," the authors concluded.
The prospective study included all 5,676 blunt trauma alert patients seen at a Level 1 trauma center between January 2008 and December 2012. Their average age was 40.6 years, mean Glasgow Coma Scale (GCS) score 14.2, mean Injury Severity Score (ISS) 9.6, and mean length of stay 4.8 days.
Of these, 420 (7.2%) had any cervical spine injury and 2.6% died.
The incidence of fracture was 7.2% (409/5,676) and ligamentous injury 0.9% (52/5,676), said Dr. Vanguri, a general surgery resident at Virginia Commonwealth University in Richmond.
Patients with cervical spine injury versus those without were significantly older (46.3 years vs. 40.2 years), had significantly lower GCS scores (13.5 vs. 14.2), and had significantly higher ISS (18.9 vs. 8.9), average blood alcohol levels (666 mg/L vs. 538 mg/L), and average lactate levels (2.6 mmol/L vs. 2.4 mmol/L). Patients with cervical spine injuries also stayed significantly longer in the hospital (11.3 days vs. 4.3 days) and ICU (5.8 days vs. 1.4 days), and had more ventilator days (9.8 days vs. 4.1 days).
Of the 52 patients with ligamentous injury, 30 (57.7%) were suspected on CT, Dr. Vanguri noted. The remaining 22 without suspected ligamentous injury all had associated fractures identified by CT requiring further intervention. Thus, CT attained 100% sensitivity and specificity in ruling out cervical spine injuries, she said.
Notably, the incidence of ligamentous injury without fracture was 0.2% (10/5,676). Stepwise logistic regression identified only three independent predictors of ligamentous injury: cervical midline tenderness, abnormal alertness, and C-spine fracture on CT.
The poster presentation prompted a spirited debate at the meeting, with some attendees arguing that clearing collars in patients with a negative CT could leave practitioners and hospitals open to potential litigation if unstable fractures and/or ligamentous injuries are missed by not conducting further testing with magnetic resonance imaging (MRI).
The specter of litigation is always a possibility; however, the incidence of ligamentous injury without fracture was exceedingly low and prolonged C-collar use is not without consequences, argued senior author Dr. Therèse Duane, an ACS Fellow and trauma and critical care surgeon at the university.
"How many times do patients go home and 3 months later still have a collar on because they can’t get an MRI and now they have migraines, can’t work, and can’t drive? It’s huge," she said.
In the study, 77% of the 52 patients with ligamentous injury underwent MRI in addition to a CT scan, 48% had CT angiography of the neck, 40.4% had C-spine surgery, and 81% required prolonged collar use for treatment purposes of 6 weeks or longer.
Though current practice at the university is to clear collars in patients with a negative CT scan, research would be needed to determine whether this approach is feasible in the higher-risk patients with altered alertness, Dr. Duane observed.
Further studies are planned by the group looking at national databanks, as well as combining a decade worth of data at their institution, to define a C-spine clearance protocol.
Dr. Vanguri and her colleagues reported having no financial disclosures.
NAPLES, FLA. – Computed tomography of the cervical spine had 100% specificity and sensitivity in ruling out clinically significant fracture and ligamentous injuries after blunt trauma in a prospective cohort of 5,676 patients.
Patients with negative CT scans do not need further workup for possible ligamentous injury, as those were only identified in patients with a positive CT scan, Dr. Poornima Vanguri said at the annual scientific assembly of the Eastern Association for the Surgery of Trauma.
"Patients with a normal CT do not need further imaging and collars should be cleared as soon as possible," the authors concluded.
The prospective study included all 5,676 blunt trauma alert patients seen at a Level 1 trauma center between January 2008 and December 2012. Their average age was 40.6 years, mean Glasgow Coma Scale (GCS) score 14.2, mean Injury Severity Score (ISS) 9.6, and mean length of stay 4.8 days.
Of these, 420 (7.2%) had any cervical spine injury and 2.6% died.
The incidence of fracture was 7.2% (409/5,676) and ligamentous injury 0.9% (52/5,676), said Dr. Vanguri, a general surgery resident at Virginia Commonwealth University in Richmond.
Patients with cervical spine injury versus those without were significantly older (46.3 years vs. 40.2 years), had significantly lower GCS scores (13.5 vs. 14.2), and had significantly higher ISS (18.9 vs. 8.9), average blood alcohol levels (666 mg/L vs. 538 mg/L), and average lactate levels (2.6 mmol/L vs. 2.4 mmol/L). Patients with cervical spine injuries also stayed significantly longer in the hospital (11.3 days vs. 4.3 days) and ICU (5.8 days vs. 1.4 days), and had more ventilator days (9.8 days vs. 4.1 days).
Of the 52 patients with ligamentous injury, 30 (57.7%) were suspected on CT, Dr. Vanguri noted. The remaining 22 without suspected ligamentous injury all had associated fractures identified by CT requiring further intervention. Thus, CT attained 100% sensitivity and specificity in ruling out cervical spine injuries, she said.
Notably, the incidence of ligamentous injury without fracture was 0.2% (10/5,676). Stepwise logistic regression identified only three independent predictors of ligamentous injury: cervical midline tenderness, abnormal alertness, and C-spine fracture on CT.
The poster presentation prompted a spirited debate at the meeting, with some attendees arguing that clearing collars in patients with a negative CT could leave practitioners and hospitals open to potential litigation if unstable fractures and/or ligamentous injuries are missed by not conducting further testing with magnetic resonance imaging (MRI).
The specter of litigation is always a possibility; however, the incidence of ligamentous injury without fracture was exceedingly low and prolonged C-collar use is not without consequences, argued senior author Dr. Therèse Duane, an ACS Fellow and trauma and critical care surgeon at the university.
"How many times do patients go home and 3 months later still have a collar on because they can’t get an MRI and now they have migraines, can’t work, and can’t drive? It’s huge," she said.
In the study, 77% of the 52 patients with ligamentous injury underwent MRI in addition to a CT scan, 48% had CT angiography of the neck, 40.4% had C-spine surgery, and 81% required prolonged collar use for treatment purposes of 6 weeks or longer.
Though current practice at the university is to clear collars in patients with a negative CT scan, research would be needed to determine whether this approach is feasible in the higher-risk patients with altered alertness, Dr. Duane observed.
Further studies are planned by the group looking at national databanks, as well as combining a decade worth of data at their institution, to define a C-spine clearance protocol.
Dr. Vanguri and her colleagues reported having no financial disclosures.
NAPLES, FLA. – Computed tomography of the cervical spine had 100% specificity and sensitivity in ruling out clinically significant fracture and ligamentous injuries after blunt trauma in a prospective cohort of 5,676 patients.
Patients with negative CT scans do not need further workup for possible ligamentous injury, as those were only identified in patients with a positive CT scan, Dr. Poornima Vanguri said at the annual scientific assembly of the Eastern Association for the Surgery of Trauma.
"Patients with a normal CT do not need further imaging and collars should be cleared as soon as possible," the authors concluded.
The prospective study included all 5,676 blunt trauma alert patients seen at a Level 1 trauma center between January 2008 and December 2012. Their average age was 40.6 years, mean Glasgow Coma Scale (GCS) score 14.2, mean Injury Severity Score (ISS) 9.6, and mean length of stay 4.8 days.
Of these, 420 (7.2%) had any cervical spine injury and 2.6% died.
The incidence of fracture was 7.2% (409/5,676) and ligamentous injury 0.9% (52/5,676), said Dr. Vanguri, a general surgery resident at Virginia Commonwealth University in Richmond.
Patients with cervical spine injury versus those without were significantly older (46.3 years vs. 40.2 years), had significantly lower GCS scores (13.5 vs. 14.2), and had significantly higher ISS (18.9 vs. 8.9), average blood alcohol levels (666 mg/L vs. 538 mg/L), and average lactate levels (2.6 mmol/L vs. 2.4 mmol/L). Patients with cervical spine injuries also stayed significantly longer in the hospital (11.3 days vs. 4.3 days) and ICU (5.8 days vs. 1.4 days), and had more ventilator days (9.8 days vs. 4.1 days).
Of the 52 patients with ligamentous injury, 30 (57.7%) were suspected on CT, Dr. Vanguri noted. The remaining 22 without suspected ligamentous injury all had associated fractures identified by CT requiring further intervention. Thus, CT attained 100% sensitivity and specificity in ruling out cervical spine injuries, she said.
Notably, the incidence of ligamentous injury without fracture was 0.2% (10/5,676). Stepwise logistic regression identified only three independent predictors of ligamentous injury: cervical midline tenderness, abnormal alertness, and C-spine fracture on CT.
The poster presentation prompted a spirited debate at the meeting, with some attendees arguing that clearing collars in patients with a negative CT could leave practitioners and hospitals open to potential litigation if unstable fractures and/or ligamentous injuries are missed by not conducting further testing with magnetic resonance imaging (MRI).
The specter of litigation is always a possibility; however, the incidence of ligamentous injury without fracture was exceedingly low and prolonged C-collar use is not without consequences, argued senior author Dr. Therèse Duane, an ACS Fellow and trauma and critical care surgeon at the university.
"How many times do patients go home and 3 months later still have a collar on because they can’t get an MRI and now they have migraines, can’t work, and can’t drive? It’s huge," she said.
In the study, 77% of the 52 patients with ligamentous injury underwent MRI in addition to a CT scan, 48% had CT angiography of the neck, 40.4% had C-spine surgery, and 81% required prolonged collar use for treatment purposes of 6 weeks or longer.
Though current practice at the university is to clear collars in patients with a negative CT scan, research would be needed to determine whether this approach is feasible in the higher-risk patients with altered alertness, Dr. Duane observed.
Further studies are planned by the group looking at national databanks, as well as combining a decade worth of data at their institution, to define a C-spine clearance protocol.
Dr. Vanguri and her colleagues reported having no financial disclosures.
AT THE EAST SCIENTIFIC ASSEMBLY
Major finding: The incidence of fracture was 7.2% (409/5,676) and ligamentous injury 0.9% (52/5,676). CT cervical spine had 100% specificity and sensitivity in ruling out clinically significant fracture and ligamentous injuries.
Data source: A prospective study of 5,676 alert patients with blunt trauma.
Disclosures: Dr. Vanguri and her colleagues reported having no financial disclosures.
Cloud-based network reduces repeat trauma imaging
NAPLES, FLA. – Implementing a cloud-based network for sharing radiological images reduced radiation exposure and costs at a Level 1 tertiary care trauma center.
The number of trauma patients who underwent the exact same imaging study decreased significantly from 62% to 47% in the 6 months after the network was available (P less than .01).
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
This resulted in a significant 19.2% decline in radiation exposure (mean 8.39 mSv vs. 7.23 mSv; P less than .01), Dr. Mayur Narayan reported at the annual meeting of the Eastern Association for the Surgery of Trauma.
"I think it’s a potential game changer," he said. "... The concept is important. The way we’re doing business currently is not sustainable."
Patients transferred within a regional trauma system to a tertiary care referral center frequently have prior radiology studies, but often undergo repeat imaging because of poor image quality, incompatible imaging software, or misplaced imaging discs. This can delay patient management, bring unwelcome radiation, and raise health care costs, explained Dr. Narayan, with the R Adams Cowley Shock Trauma Center at the University of Maryland Medical Center in Baltimore.
To reverse this trend, the center set up a secure, electronic (lifeIMAGE) network that uses a single platform for all medical image exchanges. Physicians can retrieve outside exams via the cloud or merge any or all picture archiving and communication system (PACS) data into their own PACS.
Ten hospitals are now on board and prospective data have been analyzed for 1,950 patients transferred to the trauma center between Jan. 1 and June 30, 2011, (pre-network) and between Jan. 1 and June 30, 2012, (post-network). About 8,500 patients are transferred to the trauma center annually from across the state. Patients in both time periods had similar demographics and Injury Severity Scores (mean 12).
In the 6 months after the network was implemented, the cost of imaging per patient dropped 18.7% ($413 vs. $333; P less than .01), while total imaging costs declined from $401,765 to $326,756 during the same period, Dr. Narayan said.
The most common repeat study in the analysis was an abdominal pelvic CT scan.
Inexplicably, hospital length of stay also declined from 4.4 days to 3.8 days (P = .07), he said. In-hospital mortality was unchanged (3.8% vs. 4.4%; P = .52).
The network cost Cowley Shock Trauma about $30,000 to set up, but other hospital groups are working to provide similar software for free, Dr. Narayan noted.
"The upfront costs should go away," he said.
During a discussion of the poster, one attendee said they set up a similar cloud-based system for their region, but no one used it. "I think it’s because small hospitals don’t see a lot of trauma. They have one or two patients maybe a month that would require transfer and with different people at the CT scanner every night, there’s no uniformity on how to do it," he said.
Others, however, noted that image sharing between hospitals has been fully integrated into their transfer algorithm, prompting calls between hospital radiology units, so that PAC files and patient record numbers have already been merged before the patient ever arrives in the trauma bay.
The Radiological Society of North America has also harnessed cloud-based computing to allow consumers to share their images and interpretations with any provider, regardless of institutional affiliation. According to 20-month follow-up data reported in late 2013, four out of five patients and 9 out of 10 physicians were satisfied with the RSNA Image Share network. A full 90% of patients were comfortable with the amount of privacy provided by the network, though some criticized the site for being "clunky" to navigate.
Dr. Narayan reported having no financial disclosures.
NAPLES, FLA. – Implementing a cloud-based network for sharing radiological images reduced radiation exposure and costs at a Level 1 tertiary care trauma center.
The number of trauma patients who underwent the exact same imaging study decreased significantly from 62% to 47% in the 6 months after the network was available (P less than .01).
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
This resulted in a significant 19.2% decline in radiation exposure (mean 8.39 mSv vs. 7.23 mSv; P less than .01), Dr. Mayur Narayan reported at the annual meeting of the Eastern Association for the Surgery of Trauma.
"I think it’s a potential game changer," he said. "... The concept is important. The way we’re doing business currently is not sustainable."
Patients transferred within a regional trauma system to a tertiary care referral center frequently have prior radiology studies, but often undergo repeat imaging because of poor image quality, incompatible imaging software, or misplaced imaging discs. This can delay patient management, bring unwelcome radiation, and raise health care costs, explained Dr. Narayan, with the R Adams Cowley Shock Trauma Center at the University of Maryland Medical Center in Baltimore.
To reverse this trend, the center set up a secure, electronic (lifeIMAGE) network that uses a single platform for all medical image exchanges. Physicians can retrieve outside exams via the cloud or merge any or all picture archiving and communication system (PACS) data into their own PACS.
Ten hospitals are now on board and prospective data have been analyzed for 1,950 patients transferred to the trauma center between Jan. 1 and June 30, 2011, (pre-network) and between Jan. 1 and June 30, 2012, (post-network). About 8,500 patients are transferred to the trauma center annually from across the state. Patients in both time periods had similar demographics and Injury Severity Scores (mean 12).
In the 6 months after the network was implemented, the cost of imaging per patient dropped 18.7% ($413 vs. $333; P less than .01), while total imaging costs declined from $401,765 to $326,756 during the same period, Dr. Narayan said.
The most common repeat study in the analysis was an abdominal pelvic CT scan.
Inexplicably, hospital length of stay also declined from 4.4 days to 3.8 days (P = .07), he said. In-hospital mortality was unchanged (3.8% vs. 4.4%; P = .52).
The network cost Cowley Shock Trauma about $30,000 to set up, but other hospital groups are working to provide similar software for free, Dr. Narayan noted.
"The upfront costs should go away," he said.
During a discussion of the poster, one attendee said they set up a similar cloud-based system for their region, but no one used it. "I think it’s because small hospitals don’t see a lot of trauma. They have one or two patients maybe a month that would require transfer and with different people at the CT scanner every night, there’s no uniformity on how to do it," he said.
Others, however, noted that image sharing between hospitals has been fully integrated into their transfer algorithm, prompting calls between hospital radiology units, so that PAC files and patient record numbers have already been merged before the patient ever arrives in the trauma bay.
The Radiological Society of North America has also harnessed cloud-based computing to allow consumers to share their images and interpretations with any provider, regardless of institutional affiliation. According to 20-month follow-up data reported in late 2013, four out of five patients and 9 out of 10 physicians were satisfied with the RSNA Image Share network. A full 90% of patients were comfortable with the amount of privacy provided by the network, though some criticized the site for being "clunky" to navigate.
Dr. Narayan reported having no financial disclosures.
NAPLES, FLA. – Implementing a cloud-based network for sharing radiological images reduced radiation exposure and costs at a Level 1 tertiary care trauma center.
The number of trauma patients who underwent the exact same imaging study decreased significantly from 62% to 47% in the 6 months after the network was available (P less than .01).
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
This resulted in a significant 19.2% decline in radiation exposure (mean 8.39 mSv vs. 7.23 mSv; P less than .01), Dr. Mayur Narayan reported at the annual meeting of the Eastern Association for the Surgery of Trauma.
"I think it’s a potential game changer," he said. "... The concept is important. The way we’re doing business currently is not sustainable."
Patients transferred within a regional trauma system to a tertiary care referral center frequently have prior radiology studies, but often undergo repeat imaging because of poor image quality, incompatible imaging software, or misplaced imaging discs. This can delay patient management, bring unwelcome radiation, and raise health care costs, explained Dr. Narayan, with the R Adams Cowley Shock Trauma Center at the University of Maryland Medical Center in Baltimore.
To reverse this trend, the center set up a secure, electronic (lifeIMAGE) network that uses a single platform for all medical image exchanges. Physicians can retrieve outside exams via the cloud or merge any or all picture archiving and communication system (PACS) data into their own PACS.
Ten hospitals are now on board and prospective data have been analyzed for 1,950 patients transferred to the trauma center between Jan. 1 and June 30, 2011, (pre-network) and between Jan. 1 and June 30, 2012, (post-network). About 8,500 patients are transferred to the trauma center annually from across the state. Patients in both time periods had similar demographics and Injury Severity Scores (mean 12).
In the 6 months after the network was implemented, the cost of imaging per patient dropped 18.7% ($413 vs. $333; P less than .01), while total imaging costs declined from $401,765 to $326,756 during the same period, Dr. Narayan said.
The most common repeat study in the analysis was an abdominal pelvic CT scan.
Inexplicably, hospital length of stay also declined from 4.4 days to 3.8 days (P = .07), he said. In-hospital mortality was unchanged (3.8% vs. 4.4%; P = .52).
The network cost Cowley Shock Trauma about $30,000 to set up, but other hospital groups are working to provide similar software for free, Dr. Narayan noted.
"The upfront costs should go away," he said.
During a discussion of the poster, one attendee said they set up a similar cloud-based system for their region, but no one used it. "I think it’s because small hospitals don’t see a lot of trauma. They have one or two patients maybe a month that would require transfer and with different people at the CT scanner every night, there’s no uniformity on how to do it," he said.
Others, however, noted that image sharing between hospitals has been fully integrated into their transfer algorithm, prompting calls between hospital radiology units, so that PAC files and patient record numbers have already been merged before the patient ever arrives in the trauma bay.
The Radiological Society of North America has also harnessed cloud-based computing to allow consumers to share their images and interpretations with any provider, regardless of institutional affiliation. According to 20-month follow-up data reported in late 2013, four out of five patients and 9 out of 10 physicians were satisfied with the RSNA Image Share network. A full 90% of patients were comfortable with the amount of privacy provided by the network, though some criticized the site for being "clunky" to navigate.
Dr. Narayan reported having no financial disclosures.
AT EAST 2014
Major finding: The number of patients who underwent repeat imaging declined from 62% to 47% in the 6 months after the network was implemented (P less than .01).
Data source: Prospective data review of 1,950 trauma patients.
Disclosures: Dr. Narayan reported having no financial disclosures.
Real-world data backs rivaroxaban for postop VTE prevention
NEW ORLEANS – In routine practice, rivaroxaban was superior to low-molecular-weight heparin for venous thromboembolism prevention in older adults undergoing hip or knee arthroplasty, without an increase in bleeding risk.
Among 24,321 patients, aged 66 years or older, the 30-day VTE event rate was 0.47% for rivaroxaban (Xarelto) (61 events) and 0.81% for low-molecular-weight heparin (LMWH) (93 events).
These findings resulted in an unadjusted relative risk of 0.58, which was statistically significant (P = .001) and did not change after adjustment for significant covariates, Dr. Alejandro Lazo-Langner said during an antithrombotic therapy session at the annual meeting of the American Society of Hematology.
There were 23 major bleeding events in both the rivaroxaban (0.18%) and LMWH (0.20%) groups. The unadjusted relative risk was 0.89 (P = .700) and did not change after adjustment in the population-based, retrospective cohort analysis.
Rivaroxaban has been the subject of numerous randomized controlled trials, but "We don’t have much real-life data in these patients," said Dr. Lazo-Langner, a hematologist specializing in thromboembolic diseases at Western University, London, Ontario, Canada.
In a meta-analysis of eight randomized rivaroxaban trials, the factor Xa inhibitor was associated with a significant 52% reduction in thrombosis after total hip or knee replacement, compared with enoxaparin (Lovenox) in roughly 14,000 patients (BMJ 2012;344:e3675 [doi:10.1136/bmj.e3675]). This came at a cost, however, of a slightly increased risk of clinically significant bleeding (relative risk, 1.25), he noted.
For the current analysis,the investigators used linked health care databases in Ontario to identify 24,321 patients who received an outpatient prescription for rivaroxaban or subcutaneous LMWH including dalteparin (Fragmin), tinzaparin (Innohep), or enoxaparin on discharge after total hip or knee arthroplasty between 2002 and 2012 across 121 hospitals.
Their average age was 74 years, 59% were women, and 12,850 received rivaroxaban. The anticoagulants were prescribed for a median of 14 days. Patients were excluded if they had other indications for anticoagulation, prosthetic mechanical heart valves, required dialysis, or lived in a long-term-care facility.
At 90 days, the VTE event rate was significantly lower in the rivaroxaban group than in the LMWH group (0.71% vs. 1.20%; adjusted RR, 0.59; P = .001). Once again, major bleeding events were similar (0.24% vs. 0.27%; adjusted RR, 0.63; P = .138), Dr. Lazo-Langner reported.
No differences were observed between the two groups at 30 or 90 days for hospitalization with endoscopy or hospitalization with major bleeding or endoscopy.
All-cause mortality was not estimable at 30 days but was lower with rivaroxaban at 90 days (16 deaths vs. 25 deaths; adjusted RR, 0.52; P = .058).
Additional analyses were conducted to test the robustness of the findings and no differences in rates of thrombosis were found when the analysis was restricted to 2009 to 2012, by type of joint replacement, or different low-molecular-weight heparins, he said.
Finally, a cost analysis was performed that showed a modest, but significant increase in direct drug costs to patients prescribed LMWH rather than rivaroxaban (Canadian $242 vs. $228; P less than .001) and home-care costs, likely from increased nursing ($1,082 vs. $959; P less than .001), Dr. Lazo-Langner said.
During a discussion of the results, he said there was no difference in novel anticoagulant use across surgeons or hospital settings, which was academic for 21% of LMWH patients and 15% of rivaroxaban patients.
Session comoderator Dr. Elaine Hylek, professor of medicine at Boston University, called this reassuring, but also urged caution in extrapolating conclusions on treatment effect outside a randomized trial.
Dr. Lazo-Langner reported research funding from Alexion, serving as a speaker for Pfizer, and honoraria from Pfizer, Leo Pharma, and Boehringer Ingelheim.
NEW ORLEANS – In routine practice, rivaroxaban was superior to low-molecular-weight heparin for venous thromboembolism prevention in older adults undergoing hip or knee arthroplasty, without an increase in bleeding risk.
Among 24,321 patients, aged 66 years or older, the 30-day VTE event rate was 0.47% for rivaroxaban (Xarelto) (61 events) and 0.81% for low-molecular-weight heparin (LMWH) (93 events).
These findings resulted in an unadjusted relative risk of 0.58, which was statistically significant (P = .001) and did not change after adjustment for significant covariates, Dr. Alejandro Lazo-Langner said during an antithrombotic therapy session at the annual meeting of the American Society of Hematology.
There were 23 major bleeding events in both the rivaroxaban (0.18%) and LMWH (0.20%) groups. The unadjusted relative risk was 0.89 (P = .700) and did not change after adjustment in the population-based, retrospective cohort analysis.
Rivaroxaban has been the subject of numerous randomized controlled trials, but "We don’t have much real-life data in these patients," said Dr. Lazo-Langner, a hematologist specializing in thromboembolic diseases at Western University, London, Ontario, Canada.
In a meta-analysis of eight randomized rivaroxaban trials, the factor Xa inhibitor was associated with a significant 52% reduction in thrombosis after total hip or knee replacement, compared with enoxaparin (Lovenox) in roughly 14,000 patients (BMJ 2012;344:e3675 [doi:10.1136/bmj.e3675]). This came at a cost, however, of a slightly increased risk of clinically significant bleeding (relative risk, 1.25), he noted.
For the current analysis,the investigators used linked health care databases in Ontario to identify 24,321 patients who received an outpatient prescription for rivaroxaban or subcutaneous LMWH including dalteparin (Fragmin), tinzaparin (Innohep), or enoxaparin on discharge after total hip or knee arthroplasty between 2002 and 2012 across 121 hospitals.
Their average age was 74 years, 59% were women, and 12,850 received rivaroxaban. The anticoagulants were prescribed for a median of 14 days. Patients were excluded if they had other indications for anticoagulation, prosthetic mechanical heart valves, required dialysis, or lived in a long-term-care facility.
At 90 days, the VTE event rate was significantly lower in the rivaroxaban group than in the LMWH group (0.71% vs. 1.20%; adjusted RR, 0.59; P = .001). Once again, major bleeding events were similar (0.24% vs. 0.27%; adjusted RR, 0.63; P = .138), Dr. Lazo-Langner reported.
No differences were observed between the two groups at 30 or 90 days for hospitalization with endoscopy or hospitalization with major bleeding or endoscopy.
All-cause mortality was not estimable at 30 days but was lower with rivaroxaban at 90 days (16 deaths vs. 25 deaths; adjusted RR, 0.52; P = .058).
Additional analyses were conducted to test the robustness of the findings and no differences in rates of thrombosis were found when the analysis was restricted to 2009 to 2012, by type of joint replacement, or different low-molecular-weight heparins, he said.
Finally, a cost analysis was performed that showed a modest, but significant increase in direct drug costs to patients prescribed LMWH rather than rivaroxaban (Canadian $242 vs. $228; P less than .001) and home-care costs, likely from increased nursing ($1,082 vs. $959; P less than .001), Dr. Lazo-Langner said.
During a discussion of the results, he said there was no difference in novel anticoagulant use across surgeons or hospital settings, which was academic for 21% of LMWH patients and 15% of rivaroxaban patients.
Session comoderator Dr. Elaine Hylek, professor of medicine at Boston University, called this reassuring, but also urged caution in extrapolating conclusions on treatment effect outside a randomized trial.
Dr. Lazo-Langner reported research funding from Alexion, serving as a speaker for Pfizer, and honoraria from Pfizer, Leo Pharma, and Boehringer Ingelheim.
NEW ORLEANS – In routine practice, rivaroxaban was superior to low-molecular-weight heparin for venous thromboembolism prevention in older adults undergoing hip or knee arthroplasty, without an increase in bleeding risk.
Among 24,321 patients, aged 66 years or older, the 30-day VTE event rate was 0.47% for rivaroxaban (Xarelto) (61 events) and 0.81% for low-molecular-weight heparin (LMWH) (93 events).
These findings resulted in an unadjusted relative risk of 0.58, which was statistically significant (P = .001) and did not change after adjustment for significant covariates, Dr. Alejandro Lazo-Langner said during an antithrombotic therapy session at the annual meeting of the American Society of Hematology.
There were 23 major bleeding events in both the rivaroxaban (0.18%) and LMWH (0.20%) groups. The unadjusted relative risk was 0.89 (P = .700) and did not change after adjustment in the population-based, retrospective cohort analysis.
Rivaroxaban has been the subject of numerous randomized controlled trials, but "We don’t have much real-life data in these patients," said Dr. Lazo-Langner, a hematologist specializing in thromboembolic diseases at Western University, London, Ontario, Canada.
In a meta-analysis of eight randomized rivaroxaban trials, the factor Xa inhibitor was associated with a significant 52% reduction in thrombosis after total hip or knee replacement, compared with enoxaparin (Lovenox) in roughly 14,000 patients (BMJ 2012;344:e3675 [doi:10.1136/bmj.e3675]). This came at a cost, however, of a slightly increased risk of clinically significant bleeding (relative risk, 1.25), he noted.
For the current analysis,the investigators used linked health care databases in Ontario to identify 24,321 patients who received an outpatient prescription for rivaroxaban or subcutaneous LMWH including dalteparin (Fragmin), tinzaparin (Innohep), or enoxaparin on discharge after total hip or knee arthroplasty between 2002 and 2012 across 121 hospitals.
Their average age was 74 years, 59% were women, and 12,850 received rivaroxaban. The anticoagulants were prescribed for a median of 14 days. Patients were excluded if they had other indications for anticoagulation, prosthetic mechanical heart valves, required dialysis, or lived in a long-term-care facility.
At 90 days, the VTE event rate was significantly lower in the rivaroxaban group than in the LMWH group (0.71% vs. 1.20%; adjusted RR, 0.59; P = .001). Once again, major bleeding events were similar (0.24% vs. 0.27%; adjusted RR, 0.63; P = .138), Dr. Lazo-Langner reported.
No differences were observed between the two groups at 30 or 90 days for hospitalization with endoscopy or hospitalization with major bleeding or endoscopy.
All-cause mortality was not estimable at 30 days but was lower with rivaroxaban at 90 days (16 deaths vs. 25 deaths; adjusted RR, 0.52; P = .058).
Additional analyses were conducted to test the robustness of the findings and no differences in rates of thrombosis were found when the analysis was restricted to 2009 to 2012, by type of joint replacement, or different low-molecular-weight heparins, he said.
Finally, a cost analysis was performed that showed a modest, but significant increase in direct drug costs to patients prescribed LMWH rather than rivaroxaban (Canadian $242 vs. $228; P less than .001) and home-care costs, likely from increased nursing ($1,082 vs. $959; P less than .001), Dr. Lazo-Langner said.
During a discussion of the results, he said there was no difference in novel anticoagulant use across surgeons or hospital settings, which was academic for 21% of LMWH patients and 15% of rivaroxaban patients.
Session comoderator Dr. Elaine Hylek, professor of medicine at Boston University, called this reassuring, but also urged caution in extrapolating conclusions on treatment effect outside a randomized trial.
Dr. Lazo-Langner reported research funding from Alexion, serving as a speaker for Pfizer, and honoraria from Pfizer, Leo Pharma, and Boehringer Ingelheim.
AT ASH 2013
Major finding: The 30-day VTE event rate was 0.47% for rivaroxaban and 0.81% for low molecular weight heparin (unadjusted RR, 0.58; P = .001).
Data source: Population-based, retrospective cohort study of 24,321 patients undergoing hip or knee arthroplasty
Disclosures: Dr. Lazo-Langner reported research funding from Alexion, serving as a speaker for Pfizer, and honoraria from Pfizer, Leo Pharma, and Boehringer Ingelheim.
Partial flail chest stabilization may suffice
NAPLES, FLA. – Partial repair of flail segment rib fractures may suffice in patients whose anatomy precludes full stabilization, a small study suggests.
After a median follow-up of 189 days, only predicted total lung capacity at 3 months (90% vs. 72%; P = .02) and 6 months (94% vs. 75%; P = .038) significantly differed between patients undergoing complete flail stabilization (CFS) vs. partial flail stabilization (PFS).
No other differences in pulmonary and clinical outcomes were observed between the 43 patients, Dr. Terry P. Nickerson reported at the annual scientific assembly of the Eastern Association for the Surgery of Trauma.
Flail chest is defined by two or more consecutive ribs fractured in two places and a segment of chest wall unable to contribute to respiratory mechanics.
Benefits of surgical stabilization of flail chest reported in the heterogeneous literature include decreased ICU stay, lower rates of pneumonia, increased return to work, improved quality of life, and low surgical morbidity, Dr. Nickerson noted.
The retrospective analysis, included all patients (aged 30-85 years) who underwent surgical rib fracture stabilization for flail chest from August 2009 through February 2013 at the Mayo Clinic Hospital, St. Marys Campus, Rochester, Minn. In all, 23 patients had CFS, defined as all fractures involved in a flail segment undergoing full fixation, and 20 had PFS or at least one flail segment not completely repaired.
The CFS and PFS groups were similar with respect to median age (63 years vs. 58 years), sex (52% male vs. 65% male), operating time (186 minutes vs. 183 minutes), Injury Severity Score (20 vs. 17), hospital length of stay (10 days for both), ICU stay (1 day vs. 2 days), and narcotic use at 1-month follow-up (50% vs. 47%), according to the poster presentation.
At 6 months, there were no significant differences between the CFS and PFS groups in predicted vital capacity (86% vs. 76%), forced vital capacity (85% vs. 77%), forced expiratory volume in 1 second (71% vs. 78%), and FVC/FEV1 ratio (68% vs. 74%).
Rates of pneumonia were also similar in the two groups (21% vs. 20%; P = .39), reported Dr. Nickerson, a general surgeon in Rochester.
No patient or provider observed a significant chest wall deformity in either group during follow-up and no reoperations were required for incomplete repair in the PFS.
"Despite advances in surgical technique, not all flail segment rib fractures are accessible for repair via standard thoracotomy," the authors wrote. "Our data suggest that PFS is acceptable and that extending or creating additional incisions for exposure for CFS is unwarranted."
Additional research assessing late complications, performance/functional outcomes, and perceived benefits of the operation is needed to determine whether partial repair is truly comparable with full stabilization, coauthor Dr. Brian Kim, associate medical director Mayo Clinic Trauma Center, Rochester, said in an interview.
In their experience, 6 months’ postoperative follow-up has been sufficient with respect to bony healing, convalescence from pain, and monitoring of chest wall integrity.
He noted that some surgeons may be dissuaded from pursuing or recommending operative stabilization of a flail segment with fractures deemed outside the boundaries of repair, particularly if the injury is in the elderly or obese patient.
"The results of our study lend support to the practice of repairing the most anatomically disrupted and/or symptomatic fractures within the flail segment," he said. "Age and/or BMI [body mass index] are not absolute contraindications for flail segment stabilization in our practice."
Poster session moderator Dr. Alexander Eastman of University of Texas Southwestern Medical Center in Dallas, said the low patient numbers and short follow-up in the study make it difficult to draw big conclusions, other than the need for further research.
His group uses surgical fixation of flail chest for patients with instability and pain management for those patients who are difficult to wean from the ventilator.
"I think many surgeons still are skeptical of the data supporting fixation of flail chest," he noted in an interview.
Dr. Nickerson and his coauthors reported having no financial disclosures.
NAPLES, FLA. – Partial repair of flail segment rib fractures may suffice in patients whose anatomy precludes full stabilization, a small study suggests.
After a median follow-up of 189 days, only predicted total lung capacity at 3 months (90% vs. 72%; P = .02) and 6 months (94% vs. 75%; P = .038) significantly differed between patients undergoing complete flail stabilization (CFS) vs. partial flail stabilization (PFS).
No other differences in pulmonary and clinical outcomes were observed between the 43 patients, Dr. Terry P. Nickerson reported at the annual scientific assembly of the Eastern Association for the Surgery of Trauma.
Flail chest is defined by two or more consecutive ribs fractured in two places and a segment of chest wall unable to contribute to respiratory mechanics.
Benefits of surgical stabilization of flail chest reported in the heterogeneous literature include decreased ICU stay, lower rates of pneumonia, increased return to work, improved quality of life, and low surgical morbidity, Dr. Nickerson noted.
The retrospective analysis, included all patients (aged 30-85 years) who underwent surgical rib fracture stabilization for flail chest from August 2009 through February 2013 at the Mayo Clinic Hospital, St. Marys Campus, Rochester, Minn. In all, 23 patients had CFS, defined as all fractures involved in a flail segment undergoing full fixation, and 20 had PFS or at least one flail segment not completely repaired.
The CFS and PFS groups were similar with respect to median age (63 years vs. 58 years), sex (52% male vs. 65% male), operating time (186 minutes vs. 183 minutes), Injury Severity Score (20 vs. 17), hospital length of stay (10 days for both), ICU stay (1 day vs. 2 days), and narcotic use at 1-month follow-up (50% vs. 47%), according to the poster presentation.
At 6 months, there were no significant differences between the CFS and PFS groups in predicted vital capacity (86% vs. 76%), forced vital capacity (85% vs. 77%), forced expiratory volume in 1 second (71% vs. 78%), and FVC/FEV1 ratio (68% vs. 74%).
Rates of pneumonia were also similar in the two groups (21% vs. 20%; P = .39), reported Dr. Nickerson, a general surgeon in Rochester.
No patient or provider observed a significant chest wall deformity in either group during follow-up and no reoperations were required for incomplete repair in the PFS.
"Despite advances in surgical technique, not all flail segment rib fractures are accessible for repair via standard thoracotomy," the authors wrote. "Our data suggest that PFS is acceptable and that extending or creating additional incisions for exposure for CFS is unwarranted."
Additional research assessing late complications, performance/functional outcomes, and perceived benefits of the operation is needed to determine whether partial repair is truly comparable with full stabilization, coauthor Dr. Brian Kim, associate medical director Mayo Clinic Trauma Center, Rochester, said in an interview.
In their experience, 6 months’ postoperative follow-up has been sufficient with respect to bony healing, convalescence from pain, and monitoring of chest wall integrity.
He noted that some surgeons may be dissuaded from pursuing or recommending operative stabilization of a flail segment with fractures deemed outside the boundaries of repair, particularly if the injury is in the elderly or obese patient.
"The results of our study lend support to the practice of repairing the most anatomically disrupted and/or symptomatic fractures within the flail segment," he said. "Age and/or BMI [body mass index] are not absolute contraindications for flail segment stabilization in our practice."
Poster session moderator Dr. Alexander Eastman of University of Texas Southwestern Medical Center in Dallas, said the low patient numbers and short follow-up in the study make it difficult to draw big conclusions, other than the need for further research.
His group uses surgical fixation of flail chest for patients with instability and pain management for those patients who are difficult to wean from the ventilator.
"I think many surgeons still are skeptical of the data supporting fixation of flail chest," he noted in an interview.
Dr. Nickerson and his coauthors reported having no financial disclosures.
NAPLES, FLA. – Partial repair of flail segment rib fractures may suffice in patients whose anatomy precludes full stabilization, a small study suggests.
After a median follow-up of 189 days, only predicted total lung capacity at 3 months (90% vs. 72%; P = .02) and 6 months (94% vs. 75%; P = .038) significantly differed between patients undergoing complete flail stabilization (CFS) vs. partial flail stabilization (PFS).
No other differences in pulmonary and clinical outcomes were observed between the 43 patients, Dr. Terry P. Nickerson reported at the annual scientific assembly of the Eastern Association for the Surgery of Trauma.
Flail chest is defined by two or more consecutive ribs fractured in two places and a segment of chest wall unable to contribute to respiratory mechanics.
Benefits of surgical stabilization of flail chest reported in the heterogeneous literature include decreased ICU stay, lower rates of pneumonia, increased return to work, improved quality of life, and low surgical morbidity, Dr. Nickerson noted.
The retrospective analysis, included all patients (aged 30-85 years) who underwent surgical rib fracture stabilization for flail chest from August 2009 through February 2013 at the Mayo Clinic Hospital, St. Marys Campus, Rochester, Minn. In all, 23 patients had CFS, defined as all fractures involved in a flail segment undergoing full fixation, and 20 had PFS or at least one flail segment not completely repaired.
The CFS and PFS groups were similar with respect to median age (63 years vs. 58 years), sex (52% male vs. 65% male), operating time (186 minutes vs. 183 minutes), Injury Severity Score (20 vs. 17), hospital length of stay (10 days for both), ICU stay (1 day vs. 2 days), and narcotic use at 1-month follow-up (50% vs. 47%), according to the poster presentation.
At 6 months, there were no significant differences between the CFS and PFS groups in predicted vital capacity (86% vs. 76%), forced vital capacity (85% vs. 77%), forced expiratory volume in 1 second (71% vs. 78%), and FVC/FEV1 ratio (68% vs. 74%).
Rates of pneumonia were also similar in the two groups (21% vs. 20%; P = .39), reported Dr. Nickerson, a general surgeon in Rochester.
No patient or provider observed a significant chest wall deformity in either group during follow-up and no reoperations were required for incomplete repair in the PFS.
"Despite advances in surgical technique, not all flail segment rib fractures are accessible for repair via standard thoracotomy," the authors wrote. "Our data suggest that PFS is acceptable and that extending or creating additional incisions for exposure for CFS is unwarranted."
Additional research assessing late complications, performance/functional outcomes, and perceived benefits of the operation is needed to determine whether partial repair is truly comparable with full stabilization, coauthor Dr. Brian Kim, associate medical director Mayo Clinic Trauma Center, Rochester, said in an interview.
In their experience, 6 months’ postoperative follow-up has been sufficient with respect to bony healing, convalescence from pain, and monitoring of chest wall integrity.
He noted that some surgeons may be dissuaded from pursuing or recommending operative stabilization of a flail segment with fractures deemed outside the boundaries of repair, particularly if the injury is in the elderly or obese patient.
"The results of our study lend support to the practice of repairing the most anatomically disrupted and/or symptomatic fractures within the flail segment," he said. "Age and/or BMI [body mass index] are not absolute contraindications for flail segment stabilization in our practice."
Poster session moderator Dr. Alexander Eastman of University of Texas Southwestern Medical Center in Dallas, said the low patient numbers and short follow-up in the study make it difficult to draw big conclusions, other than the need for further research.
His group uses surgical fixation of flail chest for patients with instability and pain management for those patients who are difficult to wean from the ventilator.
"I think many surgeons still are skeptical of the data supporting fixation of flail chest," he noted in an interview.
Dr. Nickerson and his coauthors reported having no financial disclosures.
AT THE EAST SCIENTIFIC ASSEMBLY
Major finding: Only predicted total lung capacity at 3 months (90% vs. 72%; P = .02) and 6 months (94% vs. 75%; P = .038) significantly differed between CFS and PFS patients.
Data source: A retrospective study of 43 patients undergoing surgical rib fracture stabilization for flail chest.
Disclosures: Dr. Nickerson and his coauthors reported having no financial disclosures.
Regionalized trauma care boosts TBI survival
NAPLES, FLA. – A regional trauma system decreased hospital mortality for traumatic brain injury patients by 21% overall and by 26% for severe brain injuries, according to a partially retrospective study.
"Regionalization represents an additional step in attempting to improve outcomes for trauma patients. It can be defined as a tiered, integrated system that attempts to get the right patient to the right place at the right time," Dr. Michael L. Kelly said at the annual meeting of the Eastern Association for the Surgery of Trauma.
A few American studies and several more outside the United States have shown that regionalization decreases mortality in the general trauma population, but similar studies in traumatic brain injury (TBI) patients are scarce.
The Northern Ohio Trauma System (NOTS) was organized in 2010 and includes a transfer line to the Level I trauma center, a nontrauma hospital transfer protocol, a pilot scene triage protocol for emergency medical services, as well as the creation of a trauma-specific ICU in the level I center, explained Dr. Kelly, a sixth-year neurosurgery resident at the Cleveland Clinic, Ohio. The network includes the Level I MetroHealth Medical Center trauma center, two Level II trauma centers, and 12 nontrauma hospitals.
The three-tiered system mandates that TBI patients with a Glasgow Coma Scale (GCS) score of less than 12 and a traumatic mechanism, any penetrating head injury, or any open/depressed skull fracture, be sent to the Level I trauma center if they can be transferred within 15 minutes.
Patients with a GCS of 12-14 and a penetrating mechanism can be transferred to any trauma center, while those with lesser head injuries can remain at their hospital, unless their condition worsens.
For the study, Dr. Kelly and his coauthors analyzed data from 2008 through 2012 for 11,220 patients more than 14 years old with a TBI in the NOTS database, which was populated prospectively beginning in mid-2010.
Level I admissions increased significantly after NOTS by 10% for all TBIs (36% vs. 46%) and by 15% for severe TBIs with a head Abbreviated Injury Scale (AIS) score of 3 or more, he said. The percentage of patients who underwent transfers between NOTS institutions also increased significantly by 7% (7% vs. 14%) and 11% (10% vs. 21%), respectively.
Hospital mortality declined from 6.2% to 4.9% post-NOTS for all TBI patients (P = .005) and from 19% to 14% for the subset with severe TBI (P less than .0001). Mortality for trauma patients in general in Ohio has consistently hovered at 4% to 5% for the last decade, despite efforts to improve outcomes, including a 2002 law requiring the transfer of trauma patients to a validated trauma center, Dr. Kelly said.
In the post-NOTS period, craniotomies increased significantly for all TBIs (2% vs. 3%; P = .003) and for severe TBIs (6% vs. 8%; P = .02). The use of any neurosurgical procedure and hospital length of stay, however, remained constant for both groups in both time periods.
At baseline, the 6,713 post-NOTS patients were significantly older than the 4,507 pre-NOTS patients (55 years vs. 52 years) and less likely to be male (63% vs. 66%) or black (23% vs. 34%). GCS scores were similar (15 for both), as were Injury Severity Scores (14 for both) and the percentage of patients with a head AIS of 3 or more (34% post- vs. 32% pre-).
Multivariate regression analysis showed that the NOTS time period was an independent predictor of survival for all TBIs, with an odds ratio of 0.76, representing a 24% mortality reduction, and odds ratio of 0.72 for severe TBIs, representing a 28% mortality reduction.
"Of some importance, the multivariate model actually strengthened the effect of NOTS on mortality in our patient population," Dr. Kelly said.
Invited discussant Deborah Stein, medical director of neurotrauma critical care at the R Adams Cowley Shock Trauma Center at the University of Maryland Medical Center in Baltimore, described the study as an important contribution to the growing body of literature demonstrating that regionalization of care is associated with improved outcomes.
Dr. Stein went on to congratulate the NOTS members for participating in what was, at times, likely a contentious and difficult process: to bring a diverse group of hospitals to consensus about the best way to care for injured patients.
"Effecting change is difficult enough in a single division, department, or hospital," she remarked.
Following the formal presentation, audience members questioned whether the change in mortality was accomplished by simply shifting patients to nursing homes to die or whether it reflects a more aggressive surgical approach to TBI or improved critical care.
Dr. Kelly said that the creation of a trauma-specific ICU at MetroHealth, the uptick in transfers to the Level I trauma center, and the increased craniotomy rate all likely affected the outcome. Patient disposition data are still being analyzed, but hospice rates remained similar after NOTS was implemented, he said.
Dr. Kelly and his coauthors reported having no financial disclosures.
For nearly 50 years, data has been accumulating regarding the effects of regionalized trauma systems on postinjury outcomes, and the verdict is clear: Having a system in place that is prepared to rapidly transport the severely injured to a trauma center provides the best opportunity to reduce morbidity and mortality in these patients. While this is true in a general sense, a penetrating injury to the torso is not the same as a TBI, with each requiring different resources and expertise for optimal management.
The group at Cleveland MetroHealth in Ohio sought to answer the question of whether or not regionalization of trauma services would demonstrate a benefit in patients with TBI. Reviewing 4 years' worth of data that coincided at its midpoint with the implementation of the Northern Ohio Trauma System (NOTS), the authors demonstrate a significant reduction in mortality in brain-injured patients, including a 28% reduction in patients with severe TBI on multivariate analysis.

|
| Dr. Robert Winfield |
In the end, the commendation from Dr. Stein regarding the ability of the NOTS group, which comprises three hospitals from two health systems, to coalesce into a highly functioning regional trauma system is prescient and reflective of an impressive achievement for the authors. It is a reminder that in a time of scarce resources and competition for health care dollars, maintaining a focus on patient care through a cooperative and collaborative approach will ultimately yield the best results for all involved.
Dr. Robert Winfield is an ACS Fellow and the chair of the ACS Resident and Associate Society, and assistant professor of trauma and acute and critical care surgery at Washington University, St. Louis.
For nearly 50 years, data has been accumulating regarding the effects of regionalized trauma systems on postinjury outcomes, and the verdict is clear: Having a system in place that is prepared to rapidly transport the severely injured to a trauma center provides the best opportunity to reduce morbidity and mortality in these patients. While this is true in a general sense, a penetrating injury to the torso is not the same as a TBI, with each requiring different resources and expertise for optimal management.
The group at Cleveland MetroHealth in Ohio sought to answer the question of whether or not regionalization of trauma services would demonstrate a benefit in patients with TBI. Reviewing 4 years' worth of data that coincided at its midpoint with the implementation of the Northern Ohio Trauma System (NOTS), the authors demonstrate a significant reduction in mortality in brain-injured patients, including a 28% reduction in patients with severe TBI on multivariate analysis.

|
| Dr. Robert Winfield |
In the end, the commendation from Dr. Stein regarding the ability of the NOTS group, which comprises three hospitals from two health systems, to coalesce into a highly functioning regional trauma system is prescient and reflective of an impressive achievement for the authors. It is a reminder that in a time of scarce resources and competition for health care dollars, maintaining a focus on patient care through a cooperative and collaborative approach will ultimately yield the best results for all involved.
Dr. Robert Winfield is an ACS Fellow and the chair of the ACS Resident and Associate Society, and assistant professor of trauma and acute and critical care surgery at Washington University, St. Louis.
For nearly 50 years, data has been accumulating regarding the effects of regionalized trauma systems on postinjury outcomes, and the verdict is clear: Having a system in place that is prepared to rapidly transport the severely injured to a trauma center provides the best opportunity to reduce morbidity and mortality in these patients. While this is true in a general sense, a penetrating injury to the torso is not the same as a TBI, with each requiring different resources and expertise for optimal management.
The group at Cleveland MetroHealth in Ohio sought to answer the question of whether or not regionalization of trauma services would demonstrate a benefit in patients with TBI. Reviewing 4 years' worth of data that coincided at its midpoint with the implementation of the Northern Ohio Trauma System (NOTS), the authors demonstrate a significant reduction in mortality in brain-injured patients, including a 28% reduction in patients with severe TBI on multivariate analysis.

|
| Dr. Robert Winfield |
In the end, the commendation from Dr. Stein regarding the ability of the NOTS group, which comprises three hospitals from two health systems, to coalesce into a highly functioning regional trauma system is prescient and reflective of an impressive achievement for the authors. It is a reminder that in a time of scarce resources and competition for health care dollars, maintaining a focus on patient care through a cooperative and collaborative approach will ultimately yield the best results for all involved.
Dr. Robert Winfield is an ACS Fellow and the chair of the ACS Resident and Associate Society, and assistant professor of trauma and acute and critical care surgery at Washington University, St. Louis.
NAPLES, FLA. – A regional trauma system decreased hospital mortality for traumatic brain injury patients by 21% overall and by 26% for severe brain injuries, according to a partially retrospective study.
"Regionalization represents an additional step in attempting to improve outcomes for trauma patients. It can be defined as a tiered, integrated system that attempts to get the right patient to the right place at the right time," Dr. Michael L. Kelly said at the annual meeting of the Eastern Association for the Surgery of Trauma.
A few American studies and several more outside the United States have shown that regionalization decreases mortality in the general trauma population, but similar studies in traumatic brain injury (TBI) patients are scarce.
The Northern Ohio Trauma System (NOTS) was organized in 2010 and includes a transfer line to the Level I trauma center, a nontrauma hospital transfer protocol, a pilot scene triage protocol for emergency medical services, as well as the creation of a trauma-specific ICU in the level I center, explained Dr. Kelly, a sixth-year neurosurgery resident at the Cleveland Clinic, Ohio. The network includes the Level I MetroHealth Medical Center trauma center, two Level II trauma centers, and 12 nontrauma hospitals.
The three-tiered system mandates that TBI patients with a Glasgow Coma Scale (GCS) score of less than 12 and a traumatic mechanism, any penetrating head injury, or any open/depressed skull fracture, be sent to the Level I trauma center if they can be transferred within 15 minutes.
Patients with a GCS of 12-14 and a penetrating mechanism can be transferred to any trauma center, while those with lesser head injuries can remain at their hospital, unless their condition worsens.
For the study, Dr. Kelly and his coauthors analyzed data from 2008 through 2012 for 11,220 patients more than 14 years old with a TBI in the NOTS database, which was populated prospectively beginning in mid-2010.
Level I admissions increased significantly after NOTS by 10% for all TBIs (36% vs. 46%) and by 15% for severe TBIs with a head Abbreviated Injury Scale (AIS) score of 3 or more, he said. The percentage of patients who underwent transfers between NOTS institutions also increased significantly by 7% (7% vs. 14%) and 11% (10% vs. 21%), respectively.
Hospital mortality declined from 6.2% to 4.9% post-NOTS for all TBI patients (P = .005) and from 19% to 14% for the subset with severe TBI (P less than .0001). Mortality for trauma patients in general in Ohio has consistently hovered at 4% to 5% for the last decade, despite efforts to improve outcomes, including a 2002 law requiring the transfer of trauma patients to a validated trauma center, Dr. Kelly said.
In the post-NOTS period, craniotomies increased significantly for all TBIs (2% vs. 3%; P = .003) and for severe TBIs (6% vs. 8%; P = .02). The use of any neurosurgical procedure and hospital length of stay, however, remained constant for both groups in both time periods.
At baseline, the 6,713 post-NOTS patients were significantly older than the 4,507 pre-NOTS patients (55 years vs. 52 years) and less likely to be male (63% vs. 66%) or black (23% vs. 34%). GCS scores were similar (15 for both), as were Injury Severity Scores (14 for both) and the percentage of patients with a head AIS of 3 or more (34% post- vs. 32% pre-).
Multivariate regression analysis showed that the NOTS time period was an independent predictor of survival for all TBIs, with an odds ratio of 0.76, representing a 24% mortality reduction, and odds ratio of 0.72 for severe TBIs, representing a 28% mortality reduction.
"Of some importance, the multivariate model actually strengthened the effect of NOTS on mortality in our patient population," Dr. Kelly said.
Invited discussant Deborah Stein, medical director of neurotrauma critical care at the R Adams Cowley Shock Trauma Center at the University of Maryland Medical Center in Baltimore, described the study as an important contribution to the growing body of literature demonstrating that regionalization of care is associated with improved outcomes.
Dr. Stein went on to congratulate the NOTS members for participating in what was, at times, likely a contentious and difficult process: to bring a diverse group of hospitals to consensus about the best way to care for injured patients.
"Effecting change is difficult enough in a single division, department, or hospital," she remarked.
Following the formal presentation, audience members questioned whether the change in mortality was accomplished by simply shifting patients to nursing homes to die or whether it reflects a more aggressive surgical approach to TBI or improved critical care.
Dr. Kelly said that the creation of a trauma-specific ICU at MetroHealth, the uptick in transfers to the Level I trauma center, and the increased craniotomy rate all likely affected the outcome. Patient disposition data are still being analyzed, but hospice rates remained similar after NOTS was implemented, he said.
Dr. Kelly and his coauthors reported having no financial disclosures.
NAPLES, FLA. – A regional trauma system decreased hospital mortality for traumatic brain injury patients by 21% overall and by 26% for severe brain injuries, according to a partially retrospective study.
"Regionalization represents an additional step in attempting to improve outcomes for trauma patients. It can be defined as a tiered, integrated system that attempts to get the right patient to the right place at the right time," Dr. Michael L. Kelly said at the annual meeting of the Eastern Association for the Surgery of Trauma.
A few American studies and several more outside the United States have shown that regionalization decreases mortality in the general trauma population, but similar studies in traumatic brain injury (TBI) patients are scarce.
The Northern Ohio Trauma System (NOTS) was organized in 2010 and includes a transfer line to the Level I trauma center, a nontrauma hospital transfer protocol, a pilot scene triage protocol for emergency medical services, as well as the creation of a trauma-specific ICU in the level I center, explained Dr. Kelly, a sixth-year neurosurgery resident at the Cleveland Clinic, Ohio. The network includes the Level I MetroHealth Medical Center trauma center, two Level II trauma centers, and 12 nontrauma hospitals.
The three-tiered system mandates that TBI patients with a Glasgow Coma Scale (GCS) score of less than 12 and a traumatic mechanism, any penetrating head injury, or any open/depressed skull fracture, be sent to the Level I trauma center if they can be transferred within 15 minutes.
Patients with a GCS of 12-14 and a penetrating mechanism can be transferred to any trauma center, while those with lesser head injuries can remain at their hospital, unless their condition worsens.
For the study, Dr. Kelly and his coauthors analyzed data from 2008 through 2012 for 11,220 patients more than 14 years old with a TBI in the NOTS database, which was populated prospectively beginning in mid-2010.
Level I admissions increased significantly after NOTS by 10% for all TBIs (36% vs. 46%) and by 15% for severe TBIs with a head Abbreviated Injury Scale (AIS) score of 3 or more, he said. The percentage of patients who underwent transfers between NOTS institutions also increased significantly by 7% (7% vs. 14%) and 11% (10% vs. 21%), respectively.
Hospital mortality declined from 6.2% to 4.9% post-NOTS for all TBI patients (P = .005) and from 19% to 14% for the subset with severe TBI (P less than .0001). Mortality for trauma patients in general in Ohio has consistently hovered at 4% to 5% for the last decade, despite efforts to improve outcomes, including a 2002 law requiring the transfer of trauma patients to a validated trauma center, Dr. Kelly said.
In the post-NOTS period, craniotomies increased significantly for all TBIs (2% vs. 3%; P = .003) and for severe TBIs (6% vs. 8%; P = .02). The use of any neurosurgical procedure and hospital length of stay, however, remained constant for both groups in both time periods.
At baseline, the 6,713 post-NOTS patients were significantly older than the 4,507 pre-NOTS patients (55 years vs. 52 years) and less likely to be male (63% vs. 66%) or black (23% vs. 34%). GCS scores were similar (15 for both), as were Injury Severity Scores (14 for both) and the percentage of patients with a head AIS of 3 or more (34% post- vs. 32% pre-).
Multivariate regression analysis showed that the NOTS time period was an independent predictor of survival for all TBIs, with an odds ratio of 0.76, representing a 24% mortality reduction, and odds ratio of 0.72 for severe TBIs, representing a 28% mortality reduction.
"Of some importance, the multivariate model actually strengthened the effect of NOTS on mortality in our patient population," Dr. Kelly said.
Invited discussant Deborah Stein, medical director of neurotrauma critical care at the R Adams Cowley Shock Trauma Center at the University of Maryland Medical Center in Baltimore, described the study as an important contribution to the growing body of literature demonstrating that regionalization of care is associated with improved outcomes.
Dr. Stein went on to congratulate the NOTS members for participating in what was, at times, likely a contentious and difficult process: to bring a diverse group of hospitals to consensus about the best way to care for injured patients.
"Effecting change is difficult enough in a single division, department, or hospital," she remarked.
Following the formal presentation, audience members questioned whether the change in mortality was accomplished by simply shifting patients to nursing homes to die or whether it reflects a more aggressive surgical approach to TBI or improved critical care.
Dr. Kelly said that the creation of a trauma-specific ICU at MetroHealth, the uptick in transfers to the Level I trauma center, and the increased craniotomy rate all likely affected the outcome. Patient disposition data are still being analyzed, but hospice rates remained similar after NOTS was implemented, he said.
Dr. Kelly and his coauthors reported having no financial disclosures.
AT THE EAST SCIENTIFIC ASSEMBLY
Major finding: Hospital mortality was 6.2% pre-NOTS vs. 4.9% post-NOTS for all TBIs (P = .005) and 19% vs. 14% for severe TBIs (P less than .001).
Data source: A partially retrospective analysis of 11,220 TBI trauma patients.
Disclosures: Dr. Kelly and his coauthors reported having no financial disclosures.