User login
Milk may slow knee OA progression in women
Milk consumption was associated with a slowing of the structural progression of knee osteoarthritis among women who participated in the longitudinal Osteoarthritis Initiative study.
From a group of 4,796 adults aged 45-79 years with established knee OA or major risk factors for OA who had been enrolled in the study in 2004, Dr. Bing Lu of the division of rheumatology, immunology, and allergy at Brigham and Women’s Hospital and Harvard Medical School, Boston, and his associates identified 2,148 of these adults with 3,064 affected knees. They followed the patients using annual plain radiographs at 1, 2, 3, and 4 years after enrollment.
The investigators measured changes in joint space width between the medial femur and tibia to quantify OA progression, as well as Osteoarthritis Research Society International grading as a semiquantitative measure of progression. Milk consumption and intake of dairy products, other foods, and dietary supplements were assessed with a food frequency questionnaire.
Among women only, a significant inverse dose-response relationship was found between milk intake and the rate of decline in joint space width, beginning at the relatively low "dose" of seven or fewer glasses of milk per week. Every increase of 10 glasses per week was associated with 0.06 mm less decline in joint space width over 48 months, compared with women who drank no milk.
This association remained robust after the data were adjusted to account for alcohol consumption and the intake of cheese and yogurt, and it was not affected by the participants’ race, smoking status, level of physical activity, vitamin D intake, and the presence or absence of obesity. A sensitivity analysis that accounted for dietary calcium intake reduced the effect of milk consumption in women by 25% (Arthritis Care Res. 2014 April 7 [doi: 10.1002/acr.22297]).
The reason for this association remains unclear, and it also isn’t known why milk intake didn’t correlate with OA progression in men. Moreover, causality has not been established because this was an observational study and the participants were not randomized to consume different quantities of milk, Dr. Lu and his associates wrote.
This study was supported by the National Heart, Lung and Blood Institute. The Osteoarthritis Initiative is a public-private partnership funded by the National Institutes of Health, Pfizer, Novartis, Merck, and GlaxoSmithKline. Dr. Lu and his associates reported no financial conflicts of interest.
This is the first large, prospective study to examine the association between milk intake and progression of knee OA, and although the results are "intriguing," they do not yet warrant a change in clinical practice. So don’t start advising patients to drink more milk quite yet, said Shivani Sahni, Ph.D., and Robert R. McLean, D.Sc.
If these findings are replicated in further studies, the current dietary guidelines for milk intake should be sufficient to delay the progression of OA. Moreover, it is not yet clear whether the beneficial radiographic effect observed in this study translates into meaningful clinical outcomes such as decreased pain, improved function, or avoidance of joint replacement, they noted.
Shivani Sahni, Ph.D., and Robert R. McLean, D.Sc., are at the Institute for Aging Research at Beth Israel Deaconess Medical Center, Boston. They reported no financial conflicts of interest. These remarks were taken from their editorial accompanying Dr. Lu and colleagues’ report (Arthritis Care Res. 2014 April 7 [doi: 10.1002/acr.22334]).
This is the first large, prospective study to examine the association between milk intake and progression of knee OA, and although the results are "intriguing," they do not yet warrant a change in clinical practice. So don’t start advising patients to drink more milk quite yet, said Shivani Sahni, Ph.D., and Robert R. McLean, D.Sc.
If these findings are replicated in further studies, the current dietary guidelines for milk intake should be sufficient to delay the progression of OA. Moreover, it is not yet clear whether the beneficial radiographic effect observed in this study translates into meaningful clinical outcomes such as decreased pain, improved function, or avoidance of joint replacement, they noted.
Shivani Sahni, Ph.D., and Robert R. McLean, D.Sc., are at the Institute for Aging Research at Beth Israel Deaconess Medical Center, Boston. They reported no financial conflicts of interest. These remarks were taken from their editorial accompanying Dr. Lu and colleagues’ report (Arthritis Care Res. 2014 April 7 [doi: 10.1002/acr.22334]).
This is the first large, prospective study to examine the association between milk intake and progression of knee OA, and although the results are "intriguing," they do not yet warrant a change in clinical practice. So don’t start advising patients to drink more milk quite yet, said Shivani Sahni, Ph.D., and Robert R. McLean, D.Sc.
If these findings are replicated in further studies, the current dietary guidelines for milk intake should be sufficient to delay the progression of OA. Moreover, it is not yet clear whether the beneficial radiographic effect observed in this study translates into meaningful clinical outcomes such as decreased pain, improved function, or avoidance of joint replacement, they noted.
Shivani Sahni, Ph.D., and Robert R. McLean, D.Sc., are at the Institute for Aging Research at Beth Israel Deaconess Medical Center, Boston. They reported no financial conflicts of interest. These remarks were taken from their editorial accompanying Dr. Lu and colleagues’ report (Arthritis Care Res. 2014 April 7 [doi: 10.1002/acr.22334]).
Milk consumption was associated with a slowing of the structural progression of knee osteoarthritis among women who participated in the longitudinal Osteoarthritis Initiative study.
From a group of 4,796 adults aged 45-79 years with established knee OA or major risk factors for OA who had been enrolled in the study in 2004, Dr. Bing Lu of the division of rheumatology, immunology, and allergy at Brigham and Women’s Hospital and Harvard Medical School, Boston, and his associates identified 2,148 of these adults with 3,064 affected knees. They followed the patients using annual plain radiographs at 1, 2, 3, and 4 years after enrollment.
The investigators measured changes in joint space width between the medial femur and tibia to quantify OA progression, as well as Osteoarthritis Research Society International grading as a semiquantitative measure of progression. Milk consumption and intake of dairy products, other foods, and dietary supplements were assessed with a food frequency questionnaire.
Among women only, a significant inverse dose-response relationship was found between milk intake and the rate of decline in joint space width, beginning at the relatively low "dose" of seven or fewer glasses of milk per week. Every increase of 10 glasses per week was associated with 0.06 mm less decline in joint space width over 48 months, compared with women who drank no milk.
This association remained robust after the data were adjusted to account for alcohol consumption and the intake of cheese and yogurt, and it was not affected by the participants’ race, smoking status, level of physical activity, vitamin D intake, and the presence or absence of obesity. A sensitivity analysis that accounted for dietary calcium intake reduced the effect of milk consumption in women by 25% (Arthritis Care Res. 2014 April 7 [doi: 10.1002/acr.22297]).
The reason for this association remains unclear, and it also isn’t known why milk intake didn’t correlate with OA progression in men. Moreover, causality has not been established because this was an observational study and the participants were not randomized to consume different quantities of milk, Dr. Lu and his associates wrote.
This study was supported by the National Heart, Lung and Blood Institute. The Osteoarthritis Initiative is a public-private partnership funded by the National Institutes of Health, Pfizer, Novartis, Merck, and GlaxoSmithKline. Dr. Lu and his associates reported no financial conflicts of interest.
Milk consumption was associated with a slowing of the structural progression of knee osteoarthritis among women who participated in the longitudinal Osteoarthritis Initiative study.
From a group of 4,796 adults aged 45-79 years with established knee OA or major risk factors for OA who had been enrolled in the study in 2004, Dr. Bing Lu of the division of rheumatology, immunology, and allergy at Brigham and Women’s Hospital and Harvard Medical School, Boston, and his associates identified 2,148 of these adults with 3,064 affected knees. They followed the patients using annual plain radiographs at 1, 2, 3, and 4 years after enrollment.
The investigators measured changes in joint space width between the medial femur and tibia to quantify OA progression, as well as Osteoarthritis Research Society International grading as a semiquantitative measure of progression. Milk consumption and intake of dairy products, other foods, and dietary supplements were assessed with a food frequency questionnaire.
Among women only, a significant inverse dose-response relationship was found between milk intake and the rate of decline in joint space width, beginning at the relatively low "dose" of seven or fewer glasses of milk per week. Every increase of 10 glasses per week was associated with 0.06 mm less decline in joint space width over 48 months, compared with women who drank no milk.
This association remained robust after the data were adjusted to account for alcohol consumption and the intake of cheese and yogurt, and it was not affected by the participants’ race, smoking status, level of physical activity, vitamin D intake, and the presence or absence of obesity. A sensitivity analysis that accounted for dietary calcium intake reduced the effect of milk consumption in women by 25% (Arthritis Care Res. 2014 April 7 [doi: 10.1002/acr.22297]).
The reason for this association remains unclear, and it also isn’t known why milk intake didn’t correlate with OA progression in men. Moreover, causality has not been established because this was an observational study and the participants were not randomized to consume different quantities of milk, Dr. Lu and his associates wrote.
This study was supported by the National Heart, Lung and Blood Institute. The Osteoarthritis Initiative is a public-private partnership funded by the National Institutes of Health, Pfizer, Novartis, Merck, and GlaxoSmithKline. Dr. Lu and his associates reported no financial conflicts of interest.
FROM ARTHRITIS CARE AND RESEARCH
Major finding: Beginning at the relatively low "dose" of 7 or fewer glasses of milk per week, every increase of 10 glasses per week was associated with 0.06 mm less decline in joint space width over 48 months, compared with women who drank no milk.
Data source: An observational cohort study involving 2,148 adults with OA in 3,064 knees who underwent knee radiography annually for 4 years.
Disclosures: This study was supported by the National Heart, Lung and Blood Institute. The Osteoarthritis Initiative is a public-private partnership funded by the National Institutes of Health, Pfizer, Novartis, Merck, and GlaxoSmithKline. Dr. Lu and his associates reported no financial conflicts of interest.
Empiric monotherapy sufficient for gram-negative bacteremia
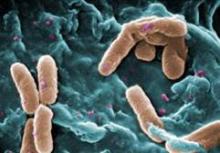
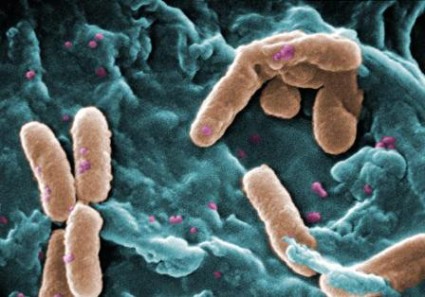
Empiric combination therapy using a beta-lactam antibiotic plus an aminoglycoside is no more beneficial than empiric monotherapy using an appropriately broad-spectrum beta-lactam antibiotic alone for children suspected of having gram-negative bacteremia, according to a report published online April 7 in Pediatrics.
Routine use of the combination therapy neither reduced 10-day mortality nor decreased the duration of bacteremia, compared with monotherapy, in a retrospective cohort study involving 452 patients aged 3 months and older, said Dr. Anna C. Sick of the University of Pittsburgh Medical Center and her associates.
The exception to this rule was children who were at risk for multidrug-resistant gram-negative bacteremia, who did appear to benefit from the addition of an aminoglycoside, they noted.
The investigators assessed the role of empirical combination therapy because it has not been well studied in this patient population, so its usefulness "remains unsettled."
In addition, later generations of beta-lactam antibiotics have broader spectrums of activity, which may obviate any benefit offered by adding aminoglycosides. And unnecessary exposure to aminoglycosides should be avoided because the drugs are known to cause ototoxicity and nephrotoxicity; they require drug monitoring; and they require frequent administration, which can lead to complex treatment schedules and possible adverse interactions with other drugs, Dr. Sick and her associates said.
They reviewed the medical records of all 714 children hospitalized at a single tertiary-care hospital – the Johns Hopkins Charlotte R. Bloomberg Children’s Center, Baltimore – during an 8-year period who had signs and symptoms suggestive of infection and who were found to have monomicrobial gram-negative bacteremia. After propensity-score matching, 226 well-balanced pairs were identified, and they formed the study cohort of 452 patients.
Overall, 35 (7.7%) of these patients died within 10 days of diagnosis.
The primary outcome measure, 10-day mortality, was 8.4% among children who received combination therapy and 7.1% among those who received monotherapy. This difference was not significant, the researchers reported (Pediatrics 2014 April 7 [doi: 10.1542/peds.2013-3363]).
These mortality risks did not change appreciably after the data were adjusted to account for the presence or absence of a central line. There also was no survival benefit for adding an aminoglycoside to a beta-lactam antibiotic among children who had the most severe illness, such as those who had PRISM (Pediatric Risk of Mortality) scores of 15 or higher or those who had absolute neutrophil counts of 100 cells or fewer per milliliter.
However, in the subgroup of 46 patients who proved to have multidrug-resistant gram-negative bacteremia, those given combination therapy were more likely to receive an empirical agent with in vitro activity against their pathogen (54.3%) than those given monotherapy (45.6%). Therefore, combination therapy "appears prudent" for patients at risk for multidrug resistance, such as children with a history of either colonization or infection with a resistant organism, children who have received broad-spectrum antibiotic therapy during the preceding month, children whose current hospitalization has been prolonged, and children residing in a community with a high prevalence of resistant pathogens.
The median duration of bacteremia also was not significantly different between the two treatment groups, even after the data were adjusted to account for the time until removal of a central line and the time for drainage of an intraabdominal abscess.
Taken together, the study findings indicate that "selecting an appropriate beta-lactam antibiotic for empirical therapy may be more important than the reflexive addition of an aminoglycoside to all patients who have gram-negative bacteremia," Dr. Sick and her associates said.
This study was supported by a Thrasher Research Foundation Award. Dr. Sick reported no financial conflicts of interest; two of her associates reported receiving grants from Pfizer for work unrelated to this study.
Empiric combination therapy using a beta-lactam antibiotic plus an aminoglycoside is no more beneficial than empiric monotherapy using an appropriately broad-spectrum beta-lactam antibiotic alone for children suspected of having gram-negative bacteremia, according to a report published online April 7 in Pediatrics.
Routine use of the combination therapy neither reduced 10-day mortality nor decreased the duration of bacteremia, compared with monotherapy, in a retrospective cohort study involving 452 patients aged 3 months and older, said Dr. Anna C. Sick of the University of Pittsburgh Medical Center and her associates.
The exception to this rule was children who were at risk for multidrug-resistant gram-negative bacteremia, who did appear to benefit from the addition of an aminoglycoside, they noted.
The investigators assessed the role of empirical combination therapy because it has not been well studied in this patient population, so its usefulness "remains unsettled."
In addition, later generations of beta-lactam antibiotics have broader spectrums of activity, which may obviate any benefit offered by adding aminoglycosides. And unnecessary exposure to aminoglycosides should be avoided because the drugs are known to cause ototoxicity and nephrotoxicity; they require drug monitoring; and they require frequent administration, which can lead to complex treatment schedules and possible adverse interactions with other drugs, Dr. Sick and her associates said.
They reviewed the medical records of all 714 children hospitalized at a single tertiary-care hospital – the Johns Hopkins Charlotte R. Bloomberg Children’s Center, Baltimore – during an 8-year period who had signs and symptoms suggestive of infection and who were found to have monomicrobial gram-negative bacteremia. After propensity-score matching, 226 well-balanced pairs were identified, and they formed the study cohort of 452 patients.
Overall, 35 (7.7%) of these patients died within 10 days of diagnosis.
The primary outcome measure, 10-day mortality, was 8.4% among children who received combination therapy and 7.1% among those who received monotherapy. This difference was not significant, the researchers reported (Pediatrics 2014 April 7 [doi: 10.1542/peds.2013-3363]).
These mortality risks did not change appreciably after the data were adjusted to account for the presence or absence of a central line. There also was no survival benefit for adding an aminoglycoside to a beta-lactam antibiotic among children who had the most severe illness, such as those who had PRISM (Pediatric Risk of Mortality) scores of 15 or higher or those who had absolute neutrophil counts of 100 cells or fewer per milliliter.
However, in the subgroup of 46 patients who proved to have multidrug-resistant gram-negative bacteremia, those given combination therapy were more likely to receive an empirical agent with in vitro activity against their pathogen (54.3%) than those given monotherapy (45.6%). Therefore, combination therapy "appears prudent" for patients at risk for multidrug resistance, such as children with a history of either colonization or infection with a resistant organism, children who have received broad-spectrum antibiotic therapy during the preceding month, children whose current hospitalization has been prolonged, and children residing in a community with a high prevalence of resistant pathogens.
The median duration of bacteremia also was not significantly different between the two treatment groups, even after the data were adjusted to account for the time until removal of a central line and the time for drainage of an intraabdominal abscess.
Taken together, the study findings indicate that "selecting an appropriate beta-lactam antibiotic for empirical therapy may be more important than the reflexive addition of an aminoglycoside to all patients who have gram-negative bacteremia," Dr. Sick and her associates said.
This study was supported by a Thrasher Research Foundation Award. Dr. Sick reported no financial conflicts of interest; two of her associates reported receiving grants from Pfizer for work unrelated to this study.
Empiric combination therapy using a beta-lactam antibiotic plus an aminoglycoside is no more beneficial than empiric monotherapy using an appropriately broad-spectrum beta-lactam antibiotic alone for children suspected of having gram-negative bacteremia, according to a report published online April 7 in Pediatrics.
Routine use of the combination therapy neither reduced 10-day mortality nor decreased the duration of bacteremia, compared with monotherapy, in a retrospective cohort study involving 452 patients aged 3 months and older, said Dr. Anna C. Sick of the University of Pittsburgh Medical Center and her associates.
The exception to this rule was children who were at risk for multidrug-resistant gram-negative bacteremia, who did appear to benefit from the addition of an aminoglycoside, they noted.
The investigators assessed the role of empirical combination therapy because it has not been well studied in this patient population, so its usefulness "remains unsettled."
In addition, later generations of beta-lactam antibiotics have broader spectrums of activity, which may obviate any benefit offered by adding aminoglycosides. And unnecessary exposure to aminoglycosides should be avoided because the drugs are known to cause ototoxicity and nephrotoxicity; they require drug monitoring; and they require frequent administration, which can lead to complex treatment schedules and possible adverse interactions with other drugs, Dr. Sick and her associates said.
They reviewed the medical records of all 714 children hospitalized at a single tertiary-care hospital – the Johns Hopkins Charlotte R. Bloomberg Children’s Center, Baltimore – during an 8-year period who had signs and symptoms suggestive of infection and who were found to have monomicrobial gram-negative bacteremia. After propensity-score matching, 226 well-balanced pairs were identified, and they formed the study cohort of 452 patients.
Overall, 35 (7.7%) of these patients died within 10 days of diagnosis.
The primary outcome measure, 10-day mortality, was 8.4% among children who received combination therapy and 7.1% among those who received monotherapy. This difference was not significant, the researchers reported (Pediatrics 2014 April 7 [doi: 10.1542/peds.2013-3363]).
These mortality risks did not change appreciably after the data were adjusted to account for the presence or absence of a central line. There also was no survival benefit for adding an aminoglycoside to a beta-lactam antibiotic among children who had the most severe illness, such as those who had PRISM (Pediatric Risk of Mortality) scores of 15 or higher or those who had absolute neutrophil counts of 100 cells or fewer per milliliter.
However, in the subgroup of 46 patients who proved to have multidrug-resistant gram-negative bacteremia, those given combination therapy were more likely to receive an empirical agent with in vitro activity against their pathogen (54.3%) than those given monotherapy (45.6%). Therefore, combination therapy "appears prudent" for patients at risk for multidrug resistance, such as children with a history of either colonization or infection with a resistant organism, children who have received broad-spectrum antibiotic therapy during the preceding month, children whose current hospitalization has been prolonged, and children residing in a community with a high prevalence of resistant pathogens.
The median duration of bacteremia also was not significantly different between the two treatment groups, even after the data were adjusted to account for the time until removal of a central line and the time for drainage of an intraabdominal abscess.
Taken together, the study findings indicate that "selecting an appropriate beta-lactam antibiotic for empirical therapy may be more important than the reflexive addition of an aminoglycoside to all patients who have gram-negative bacteremia," Dr. Sick and her associates said.
This study was supported by a Thrasher Research Foundation Award. Dr. Sick reported no financial conflicts of interest; two of her associates reported receiving grants from Pfizer for work unrelated to this study.
FROM PEDIATRICS
Major finding: The primary outcome measure, 10-day mortality, was 8.4% among children who received combination therapy and 7.1% among those who received monotherapy, a nonsignificant difference.
Data source: A retrospective cohort study involving 452 children aged 3 months and older treated for suspected gram-negative bacteremia at a single tertiary-care center during an 8-year period.
Disclosures: This study was supported by a Thrasher Research Foundation Award. Dr. Sick reported no financial conflicts of interest; two of her associates reported receiving grants from Pfizer for work unrelated to this study.
Physician’s adenoma detection rate predicts patient’s cancer risk
A physician’s adenoma detection rate – the proportion of screening colonoscopies he or she performs that detect at least one histologically confirmed colorectal adenoma or adenocarcinoma – strongly correlates with patients’ risk of developing interval cancer, according to a report published online April 2 in the New England Journal of Medicine.
Adenoma detection rates vary widely among physicians, and this statistic is used as a quality benchmark even though its usefulness in predicting outcomes "has not been well validated" until now, said Douglas A. Corley, M.D., Ph.D., of the division of research at Kaiser Permanente in Oakland, Calif., and his associates.
They used information from Kaiser’s database of approximately 3.3 million annual visits to 17 northern California medical centers to identify 314,872 colonoscopies performed on patients aged 50 years and older by 136 gastroenterologists over a 12-year period. A total of 712 interval cancers developed in the study participants during 6 months to 10 years of follow-up (927,523 person-years of follow up), including 147 fatal cases. The median interval between colonoscopy and colorectal cancer diagnosis was 39 months.
Adenoma detection rates varied greatly among the gastroenterologists, ranging from 7.4% to 52.5%. A physician’s adenoma detection rate showed a strong, linear, dose-dependent correlation with his or her patients’ cancer risk. For patients of physicians with adenoma detection rates in the highest quintile (33.51%-52.51%), compared with those of physicians with adenoma detection rates in the lowest quintile (7.35%-19.05%), the risk of developing an interval cancer was 0.52; every 1% increase in the rate predicted a 3% reduction in cancer risk, the investigators said (N. Engl. J. Med. 2014;370:1298-306 [doi:10.1056/NEJMoa1309086]).
This suggests that physicians who increase their adenoma detection rate from less than 19% (the lowest quintile) to more than 34% (the highest quintile) "might prevent 1 additional interval cancer over the next 10 years for every 213 colonoscopies," Dr. Corley and his associates said.
The findings were similar in analyses restricted to advanced-stage and fatal interval cancers. "For patients of physicians with rates in the highest quintile of adenoma detection rates, as compared with patients of physicians with rates in the lowest quintile, the risk of receiving a diagnosis of advanced-stage interval colorectal cancer was reduced by 57% and the risk of a fatal interval colorectal cancer was reduced by 62%. Each 1% increase in the adenoma detection rate was associated with a 5% decrease in the risk of a fatal interval colorectal cancer," they wrote.
"These findings support the validity of the adenoma detection rate as a quality measure of physicians’ performance of colonoscopy in community practice," the investigators added.
This study was supported by the Kaiser Permanente Community Benefit program and the National Cancer Institute. Dr. Corley and his associates reported no financial conflicts of interest.
A physician’s adenoma detection rate – the proportion of screening colonoscopies he or she performs that detect at least one histologically confirmed colorectal adenoma or adenocarcinoma – strongly correlates with patients’ risk of developing interval cancer, according to a report published online April 2 in the New England Journal of Medicine.
Adenoma detection rates vary widely among physicians, and this statistic is used as a quality benchmark even though its usefulness in predicting outcomes "has not been well validated" until now, said Douglas A. Corley, M.D., Ph.D., of the division of research at Kaiser Permanente in Oakland, Calif., and his associates.
They used information from Kaiser’s database of approximately 3.3 million annual visits to 17 northern California medical centers to identify 314,872 colonoscopies performed on patients aged 50 years and older by 136 gastroenterologists over a 12-year period. A total of 712 interval cancers developed in the study participants during 6 months to 10 years of follow-up (927,523 person-years of follow up), including 147 fatal cases. The median interval between colonoscopy and colorectal cancer diagnosis was 39 months.
Adenoma detection rates varied greatly among the gastroenterologists, ranging from 7.4% to 52.5%. A physician’s adenoma detection rate showed a strong, linear, dose-dependent correlation with his or her patients’ cancer risk. For patients of physicians with adenoma detection rates in the highest quintile (33.51%-52.51%), compared with those of physicians with adenoma detection rates in the lowest quintile (7.35%-19.05%), the risk of developing an interval cancer was 0.52; every 1% increase in the rate predicted a 3% reduction in cancer risk, the investigators said (N. Engl. J. Med. 2014;370:1298-306 [doi:10.1056/NEJMoa1309086]).
This suggests that physicians who increase their adenoma detection rate from less than 19% (the lowest quintile) to more than 34% (the highest quintile) "might prevent 1 additional interval cancer over the next 10 years for every 213 colonoscopies," Dr. Corley and his associates said.
The findings were similar in analyses restricted to advanced-stage and fatal interval cancers. "For patients of physicians with rates in the highest quintile of adenoma detection rates, as compared with patients of physicians with rates in the lowest quintile, the risk of receiving a diagnosis of advanced-stage interval colorectal cancer was reduced by 57% and the risk of a fatal interval colorectal cancer was reduced by 62%. Each 1% increase in the adenoma detection rate was associated with a 5% decrease in the risk of a fatal interval colorectal cancer," they wrote.
"These findings support the validity of the adenoma detection rate as a quality measure of physicians’ performance of colonoscopy in community practice," the investigators added.
This study was supported by the Kaiser Permanente Community Benefit program and the National Cancer Institute. Dr. Corley and his associates reported no financial conflicts of interest.
A physician’s adenoma detection rate – the proportion of screening colonoscopies he or she performs that detect at least one histologically confirmed colorectal adenoma or adenocarcinoma – strongly correlates with patients’ risk of developing interval cancer, according to a report published online April 2 in the New England Journal of Medicine.
Adenoma detection rates vary widely among physicians, and this statistic is used as a quality benchmark even though its usefulness in predicting outcomes "has not been well validated" until now, said Douglas A. Corley, M.D., Ph.D., of the division of research at Kaiser Permanente in Oakland, Calif., and his associates.
They used information from Kaiser’s database of approximately 3.3 million annual visits to 17 northern California medical centers to identify 314,872 colonoscopies performed on patients aged 50 years and older by 136 gastroenterologists over a 12-year period. A total of 712 interval cancers developed in the study participants during 6 months to 10 years of follow-up (927,523 person-years of follow up), including 147 fatal cases. The median interval between colonoscopy and colorectal cancer diagnosis was 39 months.
Adenoma detection rates varied greatly among the gastroenterologists, ranging from 7.4% to 52.5%. A physician’s adenoma detection rate showed a strong, linear, dose-dependent correlation with his or her patients’ cancer risk. For patients of physicians with adenoma detection rates in the highest quintile (33.51%-52.51%), compared with those of physicians with adenoma detection rates in the lowest quintile (7.35%-19.05%), the risk of developing an interval cancer was 0.52; every 1% increase in the rate predicted a 3% reduction in cancer risk, the investigators said (N. Engl. J. Med. 2014;370:1298-306 [doi:10.1056/NEJMoa1309086]).
This suggests that physicians who increase their adenoma detection rate from less than 19% (the lowest quintile) to more than 34% (the highest quintile) "might prevent 1 additional interval cancer over the next 10 years for every 213 colonoscopies," Dr. Corley and his associates said.
The findings were similar in analyses restricted to advanced-stage and fatal interval cancers. "For patients of physicians with rates in the highest quintile of adenoma detection rates, as compared with patients of physicians with rates in the lowest quintile, the risk of receiving a diagnosis of advanced-stage interval colorectal cancer was reduced by 57% and the risk of a fatal interval colorectal cancer was reduced by 62%. Each 1% increase in the adenoma detection rate was associated with a 5% decrease in the risk of a fatal interval colorectal cancer," they wrote.
"These findings support the validity of the adenoma detection rate as a quality measure of physicians’ performance of colonoscopy in community practice," the investigators added.
This study was supported by the Kaiser Permanente Community Benefit program and the National Cancer Institute. Dr. Corley and his associates reported no financial conflicts of interest.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major finding: For patients of physicians with adenoma detection rates in the highest quintile (33.51%-52.51%), compared with those of physicians with adenoma detection rates in the lowest quintile (7.35%-19.05%), the risk of developing an interval cancer was 0.52; every 1% increase in the rate predicted a 3% reduction in cancer risk.
Data source: A cohort study involving 314,872 colonoscopies performed by 136 gastroenterologists, in which patients were followed for up to 10 years for the development of colorectal adenocarcinomas.
Disclosures: This study was supported by the Kaiser Permanente Community Benefit program and the National Cancer Institute. Dr. Corley and his associates reported no financial conflicts of interest.
Prophylactic tadalafil ineffective after prostate cancer radiotherapy
Daily tadalafil failed to preserve erectile function among men undergoing radiotherapy for prostate cancer, according to investigators. The report was published online April 1 in JAMA.
In what they described as the first study to assess tadalafil for prevention of erectile dysfunction, researchers proposed that in contrast to episodic, on-demand use of the drug, the regular, daily use might maintain erectile function during and after radiotherapy. They tested this treatment against placebo in a randomized double-blind clinical trial (NCT00931528) involving 242 men with stage II prostate adenocarcinoma and intact erectile function. The men were enrolled at 76 community-based and tertiary medical centers in the United States and Canada.
They took 5 mg tadalafil or a matching placebo for 24 weeks, beginning at the start of either external radiotherapy (63%) or brachytherapy (37%), and were followed at intervals for 1-4 years. The primary outcome – retained erectile function 6 weeks after completion of the study agent – was reported by 79% of men who took tadalafil and 74% of those who took placebo. This was not a significant difference, said Dr. Thomas M. Pisansky of the Mayo Clinic, Rochester, Minn., and his associates.
Tadalafil also was no better than placebo at preserving erectile function at the 1-year follow-up (72% vs 71%, respectively). It was no more effective than was placebo for any subgroup of patients, regardless of patient age (younger vs. older than 65 years) or type of radiotherapy. The active drug also failed to outperform placebo on a wide variety of secondary outcomes, including orgasmic function, sexual desire, intercourse satisfaction, fatigue, sexual well-being, marital adjustment, or partners’ sexual satisfaction (JAMA 2014 April 1 [doi:10.1001/jama.2014.2626]).
This study was conducted by the Radiation Therapy Oncology Group, which is supported by the National Cancer Institute, and by Eli Lilly, maker of tadalafil. Dr. Pisansky reported no disclosures.
Daily tadalafil failed to preserve erectile function among men undergoing radiotherapy for prostate cancer, according to investigators. The report was published online April 1 in JAMA.
In what they described as the first study to assess tadalafil for prevention of erectile dysfunction, researchers proposed that in contrast to episodic, on-demand use of the drug, the regular, daily use might maintain erectile function during and after radiotherapy. They tested this treatment against placebo in a randomized double-blind clinical trial (NCT00931528) involving 242 men with stage II prostate adenocarcinoma and intact erectile function. The men were enrolled at 76 community-based and tertiary medical centers in the United States and Canada.
They took 5 mg tadalafil or a matching placebo for 24 weeks, beginning at the start of either external radiotherapy (63%) or brachytherapy (37%), and were followed at intervals for 1-4 years. The primary outcome – retained erectile function 6 weeks after completion of the study agent – was reported by 79% of men who took tadalafil and 74% of those who took placebo. This was not a significant difference, said Dr. Thomas M. Pisansky of the Mayo Clinic, Rochester, Minn., and his associates.
Tadalafil also was no better than placebo at preserving erectile function at the 1-year follow-up (72% vs 71%, respectively). It was no more effective than was placebo for any subgroup of patients, regardless of patient age (younger vs. older than 65 years) or type of radiotherapy. The active drug also failed to outperform placebo on a wide variety of secondary outcomes, including orgasmic function, sexual desire, intercourse satisfaction, fatigue, sexual well-being, marital adjustment, or partners’ sexual satisfaction (JAMA 2014 April 1 [doi:10.1001/jama.2014.2626]).
This study was conducted by the Radiation Therapy Oncology Group, which is supported by the National Cancer Institute, and by Eli Lilly, maker of tadalafil. Dr. Pisansky reported no disclosures.
Daily tadalafil failed to preserve erectile function among men undergoing radiotherapy for prostate cancer, according to investigators. The report was published online April 1 in JAMA.
In what they described as the first study to assess tadalafil for prevention of erectile dysfunction, researchers proposed that in contrast to episodic, on-demand use of the drug, the regular, daily use might maintain erectile function during and after radiotherapy. They tested this treatment against placebo in a randomized double-blind clinical trial (NCT00931528) involving 242 men with stage II prostate adenocarcinoma and intact erectile function. The men were enrolled at 76 community-based and tertiary medical centers in the United States and Canada.
They took 5 mg tadalafil or a matching placebo for 24 weeks, beginning at the start of either external radiotherapy (63%) or brachytherapy (37%), and were followed at intervals for 1-4 years. The primary outcome – retained erectile function 6 weeks after completion of the study agent – was reported by 79% of men who took tadalafil and 74% of those who took placebo. This was not a significant difference, said Dr. Thomas M. Pisansky of the Mayo Clinic, Rochester, Minn., and his associates.
Tadalafil also was no better than placebo at preserving erectile function at the 1-year follow-up (72% vs 71%, respectively). It was no more effective than was placebo for any subgroup of patients, regardless of patient age (younger vs. older than 65 years) or type of radiotherapy. The active drug also failed to outperform placebo on a wide variety of secondary outcomes, including orgasmic function, sexual desire, intercourse satisfaction, fatigue, sexual well-being, marital adjustment, or partners’ sexual satisfaction (JAMA 2014 April 1 [doi:10.1001/jama.2014.2626]).
This study was conducted by the Radiation Therapy Oncology Group, which is supported by the National Cancer Institute, and by Eli Lilly, maker of tadalafil. Dr. Pisansky reported no disclosures.
FROM JAMA
Major finding: The primary outcome of retained erectile function 6 weeks after completion of the study agent was reported by 79% of men who took tadalafil and 74% of those who took placebo – not a significant difference.
Data source: A multicenter randomized double-blind clinical trial assessing erectile function after radiotherapy for prostate cancer among 242 men in the United States and Canada who took tadalafil or placebo for 6 months and were followed for at least 1 year.
Disclosures: This study was conducted by the Radiation Therapy Oncology Group, which is supported by the National Cancer Institute, and by Eli Lilly, maker of tadalafil. Dr. Pisansky reported no disclosures.
Better survival with aspirin in HLA class 1 antigen-positive cancers only
Aspirin therapy improves survival in patients whose colon cancers express HLA class 1 antigen, but not in those whose tumors have lost that expression, investigators reported online March 31 in JAMA Internal Medicine.
Researchers analyzed tumor samples from a Netherlands cancer registry, which had been obtained from 999 patients who had undergone resection of colon cancer during a 6-year period and whose medical records included information on prophylactic aspirin use. Approximately 18% of the cohort took low-dose aspirin therapy, Dr. Marlies S. Reimers of Leiden University Medical Center, the Netherlands, and her associates reported.
During 5-10 years of follow-up, 465 patients died. Overall mortality was 37.9% among aspirin users, significantly lower than the 48.5% rate among nonusers.
A total of 963 tumors could be analyzed for human leukocyte antigen (HLA) class I antigen expression; 66.8% were positive and 33.2% were negative for this expression. Overall survival was significantly longer among aspirin users whose tumors expressed HLA class I antigen, with a relative risk of 0.61. This protective effect remained robust, with an RR of 0.53, after the data were adjusted to account for potential confounders. In contrast, patients whose tumors had lost HLA class I antigen expression showed no survival benefit with aspirin therapy, with an adjusted RR of 1.03.
"Our data would be compatible with the hypothesis that aspirin inhibits platelet–tumor cell signaling (which is dependent on intact HLA antigen expression) and prevents epithelial-mesenchymal transition in circulating tumor cells, thereby reducing the metastatic potential," Dr. Reimers and her associates said (JAMA Intern. Med. 2014 March 31 [doi:10.1001/jamainternmed.2014.511]).
If these findings are confirmed in future studies, tumor expression of HLA class 1 antigen may serve as a predictive biomarker for adjuvant aspirin therapy in patients with colon cancer, they added. "Low-dose daily aspirin may suffice as an antimetastatic therapy in patients with
early-stage cancer," and because circulating tumor cells are found in the perioperative period, "it could be argued that aspirin therapy should be initiated as soon as considered clinically appropriate after diagnosis," they said.
This work was supported by the Sloos-Alandt family. Dr. Reimers reported no potential financial conflicts of interest; her associates reported ties to the PHARMO Institute, which receives partial funding from several pharmaceutical companies, and to the Aspirin Foundation and Bayer.
Although he hasn’t yet recommended aspirin therapy to his own patients, "I think, based on current evidence, that if I personally had a stage III tumor, I would add aspirin to my FOLFOX (folinic acid-fluorouracil-oxaliplatin) adjuvant therapy. And if I feel that way for myself, should I not convey that to my patients?" said Dr. Alfred I. Neugut.
Biomarker studies to identify which tumors are positive for HLA class 1 antigen expression may not even be necessary. All patients with stage III colon cancer have significant mortality risk, against which the risks of daily aspirin therapy "seem minor."
"As far as I am concerned, when a patient or patient’s spouse asks, ‘What else should he be doing, Doctor?’ – I will have a ready response," Dr. Neugut said.
Dr. Neugut is in the department of medicine at the Herbert Irving Comprehensive Cancer Center and in the department of epidemiology at Columbia University, both in New York. He reported no potential financial conflicts of interest. These remarks were taken from his invited commentary accompanying Dr. Reimers’s report (JAMA Intern. Med. 2014 March 31 [doi:10.1001/jamainternmed.2013.14544]).
Although he hasn’t yet recommended aspirin therapy to his own patients, "I think, based on current evidence, that if I personally had a stage III tumor, I would add aspirin to my FOLFOX (folinic acid-fluorouracil-oxaliplatin) adjuvant therapy. And if I feel that way for myself, should I not convey that to my patients?" said Dr. Alfred I. Neugut.
Biomarker studies to identify which tumors are positive for HLA class 1 antigen expression may not even be necessary. All patients with stage III colon cancer have significant mortality risk, against which the risks of daily aspirin therapy "seem minor."
"As far as I am concerned, when a patient or patient’s spouse asks, ‘What else should he be doing, Doctor?’ – I will have a ready response," Dr. Neugut said.
Dr. Neugut is in the department of medicine at the Herbert Irving Comprehensive Cancer Center and in the department of epidemiology at Columbia University, both in New York. He reported no potential financial conflicts of interest. These remarks were taken from his invited commentary accompanying Dr. Reimers’s report (JAMA Intern. Med. 2014 March 31 [doi:10.1001/jamainternmed.2013.14544]).
Although he hasn’t yet recommended aspirin therapy to his own patients, "I think, based on current evidence, that if I personally had a stage III tumor, I would add aspirin to my FOLFOX (folinic acid-fluorouracil-oxaliplatin) adjuvant therapy. And if I feel that way for myself, should I not convey that to my patients?" said Dr. Alfred I. Neugut.
Biomarker studies to identify which tumors are positive for HLA class 1 antigen expression may not even be necessary. All patients with stage III colon cancer have significant mortality risk, against which the risks of daily aspirin therapy "seem minor."
"As far as I am concerned, when a patient or patient’s spouse asks, ‘What else should he be doing, Doctor?’ – I will have a ready response," Dr. Neugut said.
Dr. Neugut is in the department of medicine at the Herbert Irving Comprehensive Cancer Center and in the department of epidemiology at Columbia University, both in New York. He reported no potential financial conflicts of interest. These remarks were taken from his invited commentary accompanying Dr. Reimers’s report (JAMA Intern. Med. 2014 March 31 [doi:10.1001/jamainternmed.2013.14544]).
Aspirin therapy improves survival in patients whose colon cancers express HLA class 1 antigen, but not in those whose tumors have lost that expression, investigators reported online March 31 in JAMA Internal Medicine.
Researchers analyzed tumor samples from a Netherlands cancer registry, which had been obtained from 999 patients who had undergone resection of colon cancer during a 6-year period and whose medical records included information on prophylactic aspirin use. Approximately 18% of the cohort took low-dose aspirin therapy, Dr. Marlies S. Reimers of Leiden University Medical Center, the Netherlands, and her associates reported.
During 5-10 years of follow-up, 465 patients died. Overall mortality was 37.9% among aspirin users, significantly lower than the 48.5% rate among nonusers.
A total of 963 tumors could be analyzed for human leukocyte antigen (HLA) class I antigen expression; 66.8% were positive and 33.2% were negative for this expression. Overall survival was significantly longer among aspirin users whose tumors expressed HLA class I antigen, with a relative risk of 0.61. This protective effect remained robust, with an RR of 0.53, after the data were adjusted to account for potential confounders. In contrast, patients whose tumors had lost HLA class I antigen expression showed no survival benefit with aspirin therapy, with an adjusted RR of 1.03.
"Our data would be compatible with the hypothesis that aspirin inhibits platelet–tumor cell signaling (which is dependent on intact HLA antigen expression) and prevents epithelial-mesenchymal transition in circulating tumor cells, thereby reducing the metastatic potential," Dr. Reimers and her associates said (JAMA Intern. Med. 2014 March 31 [doi:10.1001/jamainternmed.2014.511]).
If these findings are confirmed in future studies, tumor expression of HLA class 1 antigen may serve as a predictive biomarker for adjuvant aspirin therapy in patients with colon cancer, they added. "Low-dose daily aspirin may suffice as an antimetastatic therapy in patients with
early-stage cancer," and because circulating tumor cells are found in the perioperative period, "it could be argued that aspirin therapy should be initiated as soon as considered clinically appropriate after diagnosis," they said.
This work was supported by the Sloos-Alandt family. Dr. Reimers reported no potential financial conflicts of interest; her associates reported ties to the PHARMO Institute, which receives partial funding from several pharmaceutical companies, and to the Aspirin Foundation and Bayer.
Aspirin therapy improves survival in patients whose colon cancers express HLA class 1 antigen, but not in those whose tumors have lost that expression, investigators reported online March 31 in JAMA Internal Medicine.
Researchers analyzed tumor samples from a Netherlands cancer registry, which had been obtained from 999 patients who had undergone resection of colon cancer during a 6-year period and whose medical records included information on prophylactic aspirin use. Approximately 18% of the cohort took low-dose aspirin therapy, Dr. Marlies S. Reimers of Leiden University Medical Center, the Netherlands, and her associates reported.
During 5-10 years of follow-up, 465 patients died. Overall mortality was 37.9% among aspirin users, significantly lower than the 48.5% rate among nonusers.
A total of 963 tumors could be analyzed for human leukocyte antigen (HLA) class I antigen expression; 66.8% were positive and 33.2% were negative for this expression. Overall survival was significantly longer among aspirin users whose tumors expressed HLA class I antigen, with a relative risk of 0.61. This protective effect remained robust, with an RR of 0.53, after the data were adjusted to account for potential confounders. In contrast, patients whose tumors had lost HLA class I antigen expression showed no survival benefit with aspirin therapy, with an adjusted RR of 1.03.
"Our data would be compatible with the hypothesis that aspirin inhibits platelet–tumor cell signaling (which is dependent on intact HLA antigen expression) and prevents epithelial-mesenchymal transition in circulating tumor cells, thereby reducing the metastatic potential," Dr. Reimers and her associates said (JAMA Intern. Med. 2014 March 31 [doi:10.1001/jamainternmed.2014.511]).
If these findings are confirmed in future studies, tumor expression of HLA class 1 antigen may serve as a predictive biomarker for adjuvant aspirin therapy in patients with colon cancer, they added. "Low-dose daily aspirin may suffice as an antimetastatic therapy in patients with
early-stage cancer," and because circulating tumor cells are found in the perioperative period, "it could be argued that aspirin therapy should be initiated as soon as considered clinically appropriate after diagnosis," they said.
This work was supported by the Sloos-Alandt family. Dr. Reimers reported no potential financial conflicts of interest; her associates reported ties to the PHARMO Institute, which receives partial funding from several pharmaceutical companies, and to the Aspirin Foundation and Bayer.
FROM JAMA INTERNAL MEDICINE
Major finding: Overall survival was significantly longer among aspirin users whose tumors expressed HLA class I antigen, with a RR of 0.53, compared with aspirin users whose tumors had lost this expression (RR of 1.03).
Data source: A cohort study involving tumor samples from 999 patients with resected colon cancer, of whom 18% received daily low-dose aspirin therapy, who were followed for 5-10 years.
Disclosures: This work was supported by the Sloos-Alandt family. Dr. Reimers reported no potential financial conflicts of interest; her associates reported ties to the PHARMO Institute, which receives partial funding from several pharmaceutical companies, and to the Aspirin Foundation and Bayer.
Neither perioperative aspirin nor clonidine prevents MI
Neither perioperative aspirin therapy nor perioperative clonidine prevented death or MI in patients undergoing noncardiac surgery who were at risk for major vascular complications, according to data reported at the annual meeting of the American College of Cardiology.
Far from being protective, both preventive strategies exerted harmful effects: Aspirin raised the risk of major bleeding, and clonidine increased the risks of clinically important hypotension, bradycardia, and nonfatal MI, said Dr. P. J. Devereaux of the Population Health Research Institute, David Braley Cardiac, Vascular, and Stroke Research Institute, Hamilton (Ont.) General Hospital, and his associates in the POISE-2 (Perioperative Ischemic Evaluation 2) clinical trial.
The POISE-2 findings were simultaneously reported online in the New England Journal of Medicine 2014 March 31 [doi:10/1056.
NEJMoa1401105] and [doi:10/1056.
NEJMoa1401106]).
MI is the most common major vascular complication related to noncardiac surgery, and perioperative aspirin is thought to prevent it by inhibiting thrombus formation. At present, one-third of patients at risk for vascular complications receive perioperative aspirin even though the risks and benefits of this preventive strategy are uncertain.
Similarly, small trials have indicated that the antihypertensive agent clonidine, an alpha2 adrenergic agonist, reduces the risk of myocardial ischemia without inducing hemodynamic instability when given to at-risk patients undergoing noncardiac surgery, which in turn may prevent MI and death. Clonidine has additional analgesic, anxiolytic, antishivering, and anti-inflammatory effects that may be helpful.
The POISE-2 trial was designed to determine whether either of these approaches was more effective than placebo at preventing the composite endpoint of MI or death within 30 days of surgery.
A total of 10,010 patients were enrolled at 135 hospitals in 23 countries, stratified by whether they were already taking daily aspirin prophylaxis, and randomly assigned in a double-blind fashion to receive either perioperative aspirin (4,998 subjects) or placebo (5,012 subjects), and to receive either perioperative clonidine (5,009 subjects) or placebo (5,001 subjects). The mean age of these participants was 68.6 years, and 52.8% were men. Most were at risk because of their history of vascular disease; advanced age; need for dialysis; smoking status; or comorbid diabetes, heart failure, transient ischemic attack, or hypertension.
The types of surgery they underwent included general, orthopedic, urologic, gynecologic, vascular, and thoracic procedures.
The primary outcome of death or MI occurred in 7% of the aspirin group and 7.1% of the placebo group, a nonsignificant difference. The risks of other adverse outcomes, including stroke, cardiac revascularization, pulmonary embolism, acute kidney injury, and deep vein thrombosis, also were not significantly different between the two groups.
Median length of hospital stay and length of ICU and CCU stays also were not significantly different between patients who received aspirin and those who received placebo. However, aspirin raised the risk of major bleeding (4.6%), compared with placebo (3.8%), for a hazard ratio of 1.23. The most common sites of bleeding were the surgical site and the GI tract.
These effects were consistent across all subgroups of patients. In particular, they were the same whether the patients were already taking daily prophylactic aspirin therapy.
Clonidine also did not prevent death or MI within 30 days, compared with placebo; the rates were 7.3% and 6.8%, respectively. The risks of other adverse outcomes also were not significantly different between the two groups, nor were lengths of hospital, ICU, or CCU stays. However, clonidine raised the risk of clinically important hypotension (47.6% vs. 37.1%), clinically important bradycardia (12% vs. 8.1%), and nonfatal cardiac arrest (0.3% vs. 0.1%).
These effects were consistent across all subgroups of patients. In particular, clonidine was no more beneficial than was placebo in patients who underwent vascular surgery, a subgroup in whom previous, smaller studies found the drug to protect against both MI and mortality.
POISE-2 was not designed to determine why aspirin wasn’t effective at preventing perioperative MI, but Dr. Devereaux and his associates offered three possible explanations. First, MI was associated with major bleeding, and aspirin raises the risk of this complication. "It is possible that aspirin prevented some perioperative MI through thrombus inhibition [but] caused some MIs through bleeding and the subsequent mismatch between the supply of and the demand for myocardial oxygen, thus resulting in the overall neutral effect in our study," they said.
Second, the heart rate findings couldn’t statistically rule out a possible moderate beneficial effect of aspirin therapy. And third, it is possible that coronary-artery thrombus isn’t the dominant mechanism of perioperative MI, and aspirin’s antithrombotic effect didn’t address this unknown dominant mechanism.
Similarly, it is not known why clonidine failed to be protective, but the investigators offered two possible reasons. First, the drug induced hypotension, which raises the risk of perioperative MI. And second, it also induced bradycardia, which may be a proxy for an overall adverse effect on heart rate control; this also can increase the risk of perioperative MI, they said.
The POISE-2 trial was supported by the Canadian Institutes of Health Research, the National Health and Medical Research Council of Australia, and the Spanish Ministry of Health and Social Policy. Bayer Pharma provided the aspirin used in the study, and Boehringer Ingelheim provided the clonidine and some funding. Dr. Devereaux reported ties to Abbott, Bayer Pharma, Boehringer Ingelheim, Covidien, Roche, and Stryker and; some of his associates reported ties to several industry sources.
Myriad, and sometimes opposing, mechanisms contribute to perioperative MI, including excess bleeding, dramatic fluid shifts, unrelenting tachycardia, myocardial stress with fixed coronary obstruction, profound hypo- or hypertension, coronary plaque rupture, and coronary spasm, said Dr. Prashant Vaishnava and Dr. Kim A. Eagle.
So it shouldn’t be surprising that a medical therapy aimed at one of these mechanisms may actually augment a different mechanism, and end up raising MI risk. "Aspirin may reduce coronary thrombosis at the expense of excess bleeding; clonidine may reduce hypertensive swings only to be countered by clinically important hypotension," they noted.
On balance, the POISE-2 results provide cogent evidence against the use of either perioperative aspirin or clonidine.
Dr. Vaishnava and Dr. Eagle are at the Samuel and Jean A. Frankel Cardiovascular Center at the University of Michigan Health System, Ann Arbor. They reported no potential conflicts of interest. These remarks were taken from their editorial accompanying the POISE-2 trial reports (New Engl. J. Med. 2014 March 31 [doi:10.1056/NEJMe1402976]).
Myriad, and sometimes opposing, mechanisms contribute to perioperative MI, including excess bleeding, dramatic fluid shifts, unrelenting tachycardia, myocardial stress with fixed coronary obstruction, profound hypo- or hypertension, coronary plaque rupture, and coronary spasm, said Dr. Prashant Vaishnava and Dr. Kim A. Eagle.
So it shouldn’t be surprising that a medical therapy aimed at one of these mechanisms may actually augment a different mechanism, and end up raising MI risk. "Aspirin may reduce coronary thrombosis at the expense of excess bleeding; clonidine may reduce hypertensive swings only to be countered by clinically important hypotension," they noted.
On balance, the POISE-2 results provide cogent evidence against the use of either perioperative aspirin or clonidine.
Dr. Vaishnava and Dr. Eagle are at the Samuel and Jean A. Frankel Cardiovascular Center at the University of Michigan Health System, Ann Arbor. They reported no potential conflicts of interest. These remarks were taken from their editorial accompanying the POISE-2 trial reports (New Engl. J. Med. 2014 March 31 [doi:10.1056/NEJMe1402976]).
Myriad, and sometimes opposing, mechanisms contribute to perioperative MI, including excess bleeding, dramatic fluid shifts, unrelenting tachycardia, myocardial stress with fixed coronary obstruction, profound hypo- or hypertension, coronary plaque rupture, and coronary spasm, said Dr. Prashant Vaishnava and Dr. Kim A. Eagle.
So it shouldn’t be surprising that a medical therapy aimed at one of these mechanisms may actually augment a different mechanism, and end up raising MI risk. "Aspirin may reduce coronary thrombosis at the expense of excess bleeding; clonidine may reduce hypertensive swings only to be countered by clinically important hypotension," they noted.
On balance, the POISE-2 results provide cogent evidence against the use of either perioperative aspirin or clonidine.
Dr. Vaishnava and Dr. Eagle are at the Samuel and Jean A. Frankel Cardiovascular Center at the University of Michigan Health System, Ann Arbor. They reported no potential conflicts of interest. These remarks were taken from their editorial accompanying the POISE-2 trial reports (New Engl. J. Med. 2014 March 31 [doi:10.1056/NEJMe1402976]).
Neither perioperative aspirin therapy nor perioperative clonidine prevented death or MI in patients undergoing noncardiac surgery who were at risk for major vascular complications, according to data reported at the annual meeting of the American College of Cardiology.
Far from being protective, both preventive strategies exerted harmful effects: Aspirin raised the risk of major bleeding, and clonidine increased the risks of clinically important hypotension, bradycardia, and nonfatal MI, said Dr. P. J. Devereaux of the Population Health Research Institute, David Braley Cardiac, Vascular, and Stroke Research Institute, Hamilton (Ont.) General Hospital, and his associates in the POISE-2 (Perioperative Ischemic Evaluation 2) clinical trial.
The POISE-2 findings were simultaneously reported online in the New England Journal of Medicine 2014 March 31 [doi:10/1056.
NEJMoa1401105] and [doi:10/1056.
NEJMoa1401106]).
MI is the most common major vascular complication related to noncardiac surgery, and perioperative aspirin is thought to prevent it by inhibiting thrombus formation. At present, one-third of patients at risk for vascular complications receive perioperative aspirin even though the risks and benefits of this preventive strategy are uncertain.
Similarly, small trials have indicated that the antihypertensive agent clonidine, an alpha2 adrenergic agonist, reduces the risk of myocardial ischemia without inducing hemodynamic instability when given to at-risk patients undergoing noncardiac surgery, which in turn may prevent MI and death. Clonidine has additional analgesic, anxiolytic, antishivering, and anti-inflammatory effects that may be helpful.
The POISE-2 trial was designed to determine whether either of these approaches was more effective than placebo at preventing the composite endpoint of MI or death within 30 days of surgery.
A total of 10,010 patients were enrolled at 135 hospitals in 23 countries, stratified by whether they were already taking daily aspirin prophylaxis, and randomly assigned in a double-blind fashion to receive either perioperative aspirin (4,998 subjects) or placebo (5,012 subjects), and to receive either perioperative clonidine (5,009 subjects) or placebo (5,001 subjects). The mean age of these participants was 68.6 years, and 52.8% were men. Most were at risk because of their history of vascular disease; advanced age; need for dialysis; smoking status; or comorbid diabetes, heart failure, transient ischemic attack, or hypertension.
The types of surgery they underwent included general, orthopedic, urologic, gynecologic, vascular, and thoracic procedures.
The primary outcome of death or MI occurred in 7% of the aspirin group and 7.1% of the placebo group, a nonsignificant difference. The risks of other adverse outcomes, including stroke, cardiac revascularization, pulmonary embolism, acute kidney injury, and deep vein thrombosis, also were not significantly different between the two groups.
Median length of hospital stay and length of ICU and CCU stays also were not significantly different between patients who received aspirin and those who received placebo. However, aspirin raised the risk of major bleeding (4.6%), compared with placebo (3.8%), for a hazard ratio of 1.23. The most common sites of bleeding were the surgical site and the GI tract.
These effects were consistent across all subgroups of patients. In particular, they were the same whether the patients were already taking daily prophylactic aspirin therapy.
Clonidine also did not prevent death or MI within 30 days, compared with placebo; the rates were 7.3% and 6.8%, respectively. The risks of other adverse outcomes also were not significantly different between the two groups, nor were lengths of hospital, ICU, or CCU stays. However, clonidine raised the risk of clinically important hypotension (47.6% vs. 37.1%), clinically important bradycardia (12% vs. 8.1%), and nonfatal cardiac arrest (0.3% vs. 0.1%).
These effects were consistent across all subgroups of patients. In particular, clonidine was no more beneficial than was placebo in patients who underwent vascular surgery, a subgroup in whom previous, smaller studies found the drug to protect against both MI and mortality.
POISE-2 was not designed to determine why aspirin wasn’t effective at preventing perioperative MI, but Dr. Devereaux and his associates offered three possible explanations. First, MI was associated with major bleeding, and aspirin raises the risk of this complication. "It is possible that aspirin prevented some perioperative MI through thrombus inhibition [but] caused some MIs through bleeding and the subsequent mismatch between the supply of and the demand for myocardial oxygen, thus resulting in the overall neutral effect in our study," they said.
Second, the heart rate findings couldn’t statistically rule out a possible moderate beneficial effect of aspirin therapy. And third, it is possible that coronary-artery thrombus isn’t the dominant mechanism of perioperative MI, and aspirin’s antithrombotic effect didn’t address this unknown dominant mechanism.
Similarly, it is not known why clonidine failed to be protective, but the investigators offered two possible reasons. First, the drug induced hypotension, which raises the risk of perioperative MI. And second, it also induced bradycardia, which may be a proxy for an overall adverse effect on heart rate control; this also can increase the risk of perioperative MI, they said.
The POISE-2 trial was supported by the Canadian Institutes of Health Research, the National Health and Medical Research Council of Australia, and the Spanish Ministry of Health and Social Policy. Bayer Pharma provided the aspirin used in the study, and Boehringer Ingelheim provided the clonidine and some funding. Dr. Devereaux reported ties to Abbott, Bayer Pharma, Boehringer Ingelheim, Covidien, Roche, and Stryker and; some of his associates reported ties to several industry sources.
Neither perioperative aspirin therapy nor perioperative clonidine prevented death or MI in patients undergoing noncardiac surgery who were at risk for major vascular complications, according to data reported at the annual meeting of the American College of Cardiology.
Far from being protective, both preventive strategies exerted harmful effects: Aspirin raised the risk of major bleeding, and clonidine increased the risks of clinically important hypotension, bradycardia, and nonfatal MI, said Dr. P. J. Devereaux of the Population Health Research Institute, David Braley Cardiac, Vascular, and Stroke Research Institute, Hamilton (Ont.) General Hospital, and his associates in the POISE-2 (Perioperative Ischemic Evaluation 2) clinical trial.
The POISE-2 findings were simultaneously reported online in the New England Journal of Medicine 2014 March 31 [doi:10/1056.
NEJMoa1401105] and [doi:10/1056.
NEJMoa1401106]).
MI is the most common major vascular complication related to noncardiac surgery, and perioperative aspirin is thought to prevent it by inhibiting thrombus formation. At present, one-third of patients at risk for vascular complications receive perioperative aspirin even though the risks and benefits of this preventive strategy are uncertain.
Similarly, small trials have indicated that the antihypertensive agent clonidine, an alpha2 adrenergic agonist, reduces the risk of myocardial ischemia without inducing hemodynamic instability when given to at-risk patients undergoing noncardiac surgery, which in turn may prevent MI and death. Clonidine has additional analgesic, anxiolytic, antishivering, and anti-inflammatory effects that may be helpful.
The POISE-2 trial was designed to determine whether either of these approaches was more effective than placebo at preventing the composite endpoint of MI or death within 30 days of surgery.
A total of 10,010 patients were enrolled at 135 hospitals in 23 countries, stratified by whether they were already taking daily aspirin prophylaxis, and randomly assigned in a double-blind fashion to receive either perioperative aspirin (4,998 subjects) or placebo (5,012 subjects), and to receive either perioperative clonidine (5,009 subjects) or placebo (5,001 subjects). The mean age of these participants was 68.6 years, and 52.8% were men. Most were at risk because of their history of vascular disease; advanced age; need for dialysis; smoking status; or comorbid diabetes, heart failure, transient ischemic attack, or hypertension.
The types of surgery they underwent included general, orthopedic, urologic, gynecologic, vascular, and thoracic procedures.
The primary outcome of death or MI occurred in 7% of the aspirin group and 7.1% of the placebo group, a nonsignificant difference. The risks of other adverse outcomes, including stroke, cardiac revascularization, pulmonary embolism, acute kidney injury, and deep vein thrombosis, also were not significantly different between the two groups.
Median length of hospital stay and length of ICU and CCU stays also were not significantly different between patients who received aspirin and those who received placebo. However, aspirin raised the risk of major bleeding (4.6%), compared with placebo (3.8%), for a hazard ratio of 1.23. The most common sites of bleeding were the surgical site and the GI tract.
These effects were consistent across all subgroups of patients. In particular, they were the same whether the patients were already taking daily prophylactic aspirin therapy.
Clonidine also did not prevent death or MI within 30 days, compared with placebo; the rates were 7.3% and 6.8%, respectively. The risks of other adverse outcomes also were not significantly different between the two groups, nor were lengths of hospital, ICU, or CCU stays. However, clonidine raised the risk of clinically important hypotension (47.6% vs. 37.1%), clinically important bradycardia (12% vs. 8.1%), and nonfatal cardiac arrest (0.3% vs. 0.1%).
These effects were consistent across all subgroups of patients. In particular, clonidine was no more beneficial than was placebo in patients who underwent vascular surgery, a subgroup in whom previous, smaller studies found the drug to protect against both MI and mortality.
POISE-2 was not designed to determine why aspirin wasn’t effective at preventing perioperative MI, but Dr. Devereaux and his associates offered three possible explanations. First, MI was associated with major bleeding, and aspirin raises the risk of this complication. "It is possible that aspirin prevented some perioperative MI through thrombus inhibition [but] caused some MIs through bleeding and the subsequent mismatch between the supply of and the demand for myocardial oxygen, thus resulting in the overall neutral effect in our study," they said.
Second, the heart rate findings couldn’t statistically rule out a possible moderate beneficial effect of aspirin therapy. And third, it is possible that coronary-artery thrombus isn’t the dominant mechanism of perioperative MI, and aspirin’s antithrombotic effect didn’t address this unknown dominant mechanism.
Similarly, it is not known why clonidine failed to be protective, but the investigators offered two possible reasons. First, the drug induced hypotension, which raises the risk of perioperative MI. And second, it also induced bradycardia, which may be a proxy for an overall adverse effect on heart rate control; this also can increase the risk of perioperative MI, they said.
The POISE-2 trial was supported by the Canadian Institutes of Health Research, the National Health and Medical Research Council of Australia, and the Spanish Ministry of Health and Social Policy. Bayer Pharma provided the aspirin used in the study, and Boehringer Ingelheim provided the clonidine and some funding. Dr. Devereaux reported ties to Abbott, Bayer Pharma, Boehringer Ingelheim, Covidien, Roche, and Stryker and; some of his associates reported ties to several industry sources.
FROM ACC 14
Major finding: The primary outcome of death or MI occurred in 7% of the aspirin group and 7.1% of the placebo group, a nonsignificant difference; it also occurred in 7.3% of the clonidine group and 6.8% of the placebo group, also a nonsignificant difference.
Data source: A randomized, blinded clinical trial evaluating perioperative aspirin vs. placebo and perioperative clonidine vs. placebo in 10,010 patients undergoing noncardiac surgery who were at risk for major vascular complications.
Disclosures: The POISE-2 trial was supported by the Canadian Institutes of Health Research, the National Health and Medical Research Council of Australia, and the Spanish Ministry of Health and Social Policy. Bayer Pharma provided the aspirin used in the study and Boehringer Ingelheim provided the clonidine and some funding. Dr. Devereaux reported ties to Abbott, Bayer Pharma, Boehringer Ingelheim, Covidien, Roche, and Stryker and; some of his associates reported ties to several industry sources.
The Prevalence of Device-associated Infections
An estimated 4% of inpatients at U.S. acute care hospitals have at least one health care associated infection on any given day, according to a report published online March 26 in the New England Journal of Medicine.
Moreover, in a prevalence survey involving 183 acute care hospitals across 10 geographically diverse states, device-associated infections, "which have been a major focus of infection prevention in recent decades," accounted for only 25.6% of all health care–associated infections, said Dr. Shelley S. Magill of the division of health care quality promotion, Centers for Disease Control and Prevention, and her associates (N. Engl. J. Med. 2014;370:1198-1208).
In contrast, Clostridium difficile and other gastrointestinal infections, as well as non–ventilator-associated pneumonia, accounted for approximately half of all health care–associated infections in the survey. Surgical site infections also are still very common, accounting for 21.8%.
Because it appears that ventilator-associated pneumonia, catheter-associated UTIs, and central catheter–associated bloodstream infections are no longer the primary threat that they used to be, the study findings should prompt experts to "expand the public health focus to include these other types of infections, identifying patients at risk and developing effective countermeasures," the report’s authors noted.
The report shows that as a nation, we’re moving in the right direction; but there’s a great deal of work still to be done," Dr. Michael Bell said in a media briefing. "On any given day, 1 out of 25 hospitalized patients has an infection. And of those people, as many as one out of nine go on to die. This is not a minor issue," said Dr. Bell, deputy director of the CDC’s division of health care quality promotion.
The investigators developed and conducted the survey in 2011 to address a serious knowledge gap: No single surveillance system can provide estimates of "the burden of all types of such infections across acute care patient populations." So, Dr. Magill and her colleagues studied health care–associated infections among inpatients of all ages at 93 small, 68 medium-sized, and 22 large hospitals.
They found 504 such infections in 452 patients out of 11,282 patients covered in the survey, for an overall incidence of 4%. Using a statistical modeling process that accounted for predictors of infection prevalence and then applying those results to a nationally representative sample of U.S. community hospital stays, the investigators estimated that 648,000 inpatients nationwide had approximately 721,800 health care–associated infections in 2011.
Those estimates are lower than previous ones, such as those derived from the Study on the Efficacy of Nosocomial Infection Control in the 1970s , which postulated 2.1 million health care–associated infections each year, and those derived from National Nosocomial Infections Surveillance system data from 1990 to 2002, which estimated 1.7 million each year.
However, "it is difficult to draw conclusions from these comparisons because of the differences in patient populations, surveillance definitions of health care–associated infections, and data collection and analytical methods among these CDC methods," Dr. Magill and her associates said.
The current survey showed that 42.9% of health care–associated infections developed during a stay in a critical care unit or within 48 hours after; another 42.4% developed after a stay in a nonnursery ward.
Most of the surgical site infections were related to colon surgeries (14.5%), hip arthroplasty (10.0%), and small-bowel procedures (6.4%).
The median length of time between hospital admission and the onset of infection symptoms was 6 days.
C. difficile was the most frequently identified pathogen, accounting for 70.9% of all nosocomial GI infections and 12.1% of all health care–associated infections. Other common pathogens included Staphylococcus aureus (10.7% of all health care–associated infections), Klebsiella pneumoniae and Klebsiella oxytoca (9.9%), and Escherichia coli (9.3%).
The report’s investigators noted that their estimates "are remarkably similar to estimates from other data sources," such as the National Healthcare Safety Network and the Emerging Infections Program. That "bolsters our confidence in the overall estimates of health care–associated infections that we have generated," they said.
Sounding the alarm
The report "sounds the alarm" about infectious threats to hospitalized patients that need addressing, especially lung and gut infections and infections related to surgery or urinary catheters, Dr. Bell said. It also sheds light on several important pathogens, especially C. difficile, Staphylococci, and the family of Enterobacter organisms.
Those pathogens are at the center of President Barack Obama’s request for $30 million as part of his proposed $6.6 billion budget for 2015 for a new initiative to halve infections by those organisms within 5 years, Dr. Bell said.
The $30 million would be used to improve tracking of infections, the nation’s capacity for lab testing to determine which pathogens are most problematic, and "boots on the ground" to help hospitals implement best practices, Dr. Bell said.
The CDC would like to see every hospital in the country develop a strong antibiotic stewardship program, because "the challenge with antibiotic resistance can’t be overstated," he cautioned.
A patient advocate echoed that concern at the media briefing.
"While inwardly I breathe a small sigh of relief that annual infections and mortalities are diminishing, I remain extremely cautious regarding the growing threat of antibiotic resistance and the dire impact of this potential danger to American health care," said Victoria Nahum, executive director of the Safe Care Campaign. Ms. Nahum and her husband, Armando Nahum, founded the nonprofit organization after their son died of a health care–associated infection and two other family members developed complications from health care–associated infections.
Health care providers "have the power to prevent health care–associated infections" through compulsive hand hygiene and other best practices, Ms. Nahum said. Patients need to be more assertive, she added. "You just don’t flop down and say, ‘Take care of me.’ You have to kind of navigate what’s going to happen to you. In doing so, that can save your own life."
Dr. Bell suggested that hospitalized patients have a friend or family member be the "bad cop" and repeatedly ask caregivers if they have washed their hands, when urinary catheters can come out, and whether testing is being done to ensure that the right antibiotic is being used.
He said he knows that can be difficult for patients who may feel intimidated. "When my own mother was in the intensive care unit, I found it hard to pipe up," Dr. Bell said. "If I find it hard, I can’t imagine what it’s like for everybody else."
Dr. Magill reported no potential financial conflicts of interest; two of her associates reported ties to the Infectious Disease Consulting Corp. and Parexel.
An estimated 4% of inpatients at U.S. acute care hospitals have at least one health care associated infection on any given day, according to a report published online March 26 in the New England Journal of Medicine.
Moreover, in a prevalence survey involving 183 acute care hospitals across 10 geographically diverse states, device-associated infections, "which have been a major focus of infection prevention in recent decades," accounted for only 25.6% of all health care–associated infections, said Dr. Shelley S. Magill of the division of health care quality promotion, Centers for Disease Control and Prevention, and her associates (N. Engl. J. Med. 2014;370:1198-1208).
In contrast, Clostridium difficile and other gastrointestinal infections, as well as non–ventilator-associated pneumonia, accounted for approximately half of all health care–associated infections in the survey. Surgical site infections also are still very common, accounting for 21.8%.
Because it appears that ventilator-associated pneumonia, catheter-associated UTIs, and central catheter–associated bloodstream infections are no longer the primary threat that they used to be, the study findings should prompt experts to "expand the public health focus to include these other types of infections, identifying patients at risk and developing effective countermeasures," the report’s authors noted.
The report shows that as a nation, we’re moving in the right direction; but there’s a great deal of work still to be done," Dr. Michael Bell said in a media briefing. "On any given day, 1 out of 25 hospitalized patients has an infection. And of those people, as many as one out of nine go on to die. This is not a minor issue," said Dr. Bell, deputy director of the CDC’s division of health care quality promotion.
The investigators developed and conducted the survey in 2011 to address a serious knowledge gap: No single surveillance system can provide estimates of "the burden of all types of such infections across acute care patient populations." So, Dr. Magill and her colleagues studied health care–associated infections among inpatients of all ages at 93 small, 68 medium-sized, and 22 large hospitals.
They found 504 such infections in 452 patients out of 11,282 patients covered in the survey, for an overall incidence of 4%. Using a statistical modeling process that accounted for predictors of infection prevalence and then applying those results to a nationally representative sample of U.S. community hospital stays, the investigators estimated that 648,000 inpatients nationwide had approximately 721,800 health care–associated infections in 2011.
Those estimates are lower than previous ones, such as those derived from the Study on the Efficacy of Nosocomial Infection Control in the 1970s , which postulated 2.1 million health care–associated infections each year, and those derived from National Nosocomial Infections Surveillance system data from 1990 to 2002, which estimated 1.7 million each year.
However, "it is difficult to draw conclusions from these comparisons because of the differences in patient populations, surveillance definitions of health care–associated infections, and data collection and analytical methods among these CDC methods," Dr. Magill and her associates said.
The current survey showed that 42.9% of health care–associated infections developed during a stay in a critical care unit or within 48 hours after; another 42.4% developed after a stay in a nonnursery ward.
Most of the surgical site infections were related to colon surgeries (14.5%), hip arthroplasty (10.0%), and small-bowel procedures (6.4%).
The median length of time between hospital admission and the onset of infection symptoms was 6 days.
C. difficile was the most frequently identified pathogen, accounting for 70.9% of all nosocomial GI infections and 12.1% of all health care–associated infections. Other common pathogens included Staphylococcus aureus (10.7% of all health care–associated infections), Klebsiella pneumoniae and Klebsiella oxytoca (9.9%), and Escherichia coli (9.3%).
The report’s investigators noted that their estimates "are remarkably similar to estimates from other data sources," such as the National Healthcare Safety Network and the Emerging Infections Program. That "bolsters our confidence in the overall estimates of health care–associated infections that we have generated," they said.
Sounding the alarm
The report "sounds the alarm" about infectious threats to hospitalized patients that need addressing, especially lung and gut infections and infections related to surgery or urinary catheters, Dr. Bell said. It also sheds light on several important pathogens, especially C. difficile, Staphylococci, and the family of Enterobacter organisms.
Those pathogens are at the center of President Barack Obama’s request for $30 million as part of his proposed $6.6 billion budget for 2015 for a new initiative to halve infections by those organisms within 5 years, Dr. Bell said.
The $30 million would be used to improve tracking of infections, the nation’s capacity for lab testing to determine which pathogens are most problematic, and "boots on the ground" to help hospitals implement best practices, Dr. Bell said.
The CDC would like to see every hospital in the country develop a strong antibiotic stewardship program, because "the challenge with antibiotic resistance can’t be overstated," he cautioned.
A patient advocate echoed that concern at the media briefing.
"While inwardly I breathe a small sigh of relief that annual infections and mortalities are diminishing, I remain extremely cautious regarding the growing threat of antibiotic resistance and the dire impact of this potential danger to American health care," said Victoria Nahum, executive director of the Safe Care Campaign. Ms. Nahum and her husband, Armando Nahum, founded the nonprofit organization after their son died of a health care–associated infection and two other family members developed complications from health care–associated infections.
Health care providers "have the power to prevent health care–associated infections" through compulsive hand hygiene and other best practices, Ms. Nahum said. Patients need to be more assertive, she added. "You just don’t flop down and say, ‘Take care of me.’ You have to kind of navigate what’s going to happen to you. In doing so, that can save your own life."
Dr. Bell suggested that hospitalized patients have a friend or family member be the "bad cop" and repeatedly ask caregivers if they have washed their hands, when urinary catheters can come out, and whether testing is being done to ensure that the right antibiotic is being used.
He said he knows that can be difficult for patients who may feel intimidated. "When my own mother was in the intensive care unit, I found it hard to pipe up," Dr. Bell said. "If I find it hard, I can’t imagine what it’s like for everybody else."
Dr. Magill reported no potential financial conflicts of interest; two of her associates reported ties to the Infectious Disease Consulting Corp. and Parexel.
An estimated 4% of inpatients at U.S. acute care hospitals have at least one health care associated infection on any given day, according to a report published online March 26 in the New England Journal of Medicine.
Moreover, in a prevalence survey involving 183 acute care hospitals across 10 geographically diverse states, device-associated infections, "which have been a major focus of infection prevention in recent decades," accounted for only 25.6% of all health care–associated infections, said Dr. Shelley S. Magill of the division of health care quality promotion, Centers for Disease Control and Prevention, and her associates (N. Engl. J. Med. 2014;370:1198-1208).
In contrast, Clostridium difficile and other gastrointestinal infections, as well as non–ventilator-associated pneumonia, accounted for approximately half of all health care–associated infections in the survey. Surgical site infections also are still very common, accounting for 21.8%.
Because it appears that ventilator-associated pneumonia, catheter-associated UTIs, and central catheter–associated bloodstream infections are no longer the primary threat that they used to be, the study findings should prompt experts to "expand the public health focus to include these other types of infections, identifying patients at risk and developing effective countermeasures," the report’s authors noted.
The report shows that as a nation, we’re moving in the right direction; but there’s a great deal of work still to be done," Dr. Michael Bell said in a media briefing. "On any given day, 1 out of 25 hospitalized patients has an infection. And of those people, as many as one out of nine go on to die. This is not a minor issue," said Dr. Bell, deputy director of the CDC’s division of health care quality promotion.
The investigators developed and conducted the survey in 2011 to address a serious knowledge gap: No single surveillance system can provide estimates of "the burden of all types of such infections across acute care patient populations." So, Dr. Magill and her colleagues studied health care–associated infections among inpatients of all ages at 93 small, 68 medium-sized, and 22 large hospitals.
They found 504 such infections in 452 patients out of 11,282 patients covered in the survey, for an overall incidence of 4%. Using a statistical modeling process that accounted for predictors of infection prevalence and then applying those results to a nationally representative sample of U.S. community hospital stays, the investigators estimated that 648,000 inpatients nationwide had approximately 721,800 health care–associated infections in 2011.
Those estimates are lower than previous ones, such as those derived from the Study on the Efficacy of Nosocomial Infection Control in the 1970s , which postulated 2.1 million health care–associated infections each year, and those derived from National Nosocomial Infections Surveillance system data from 1990 to 2002, which estimated 1.7 million each year.
However, "it is difficult to draw conclusions from these comparisons because of the differences in patient populations, surveillance definitions of health care–associated infections, and data collection and analytical methods among these CDC methods," Dr. Magill and her associates said.
The current survey showed that 42.9% of health care–associated infections developed during a stay in a critical care unit or within 48 hours after; another 42.4% developed after a stay in a nonnursery ward.
Most of the surgical site infections were related to colon surgeries (14.5%), hip arthroplasty (10.0%), and small-bowel procedures (6.4%).
The median length of time between hospital admission and the onset of infection symptoms was 6 days.
C. difficile was the most frequently identified pathogen, accounting for 70.9% of all nosocomial GI infections and 12.1% of all health care–associated infections. Other common pathogens included Staphylococcus aureus (10.7% of all health care–associated infections), Klebsiella pneumoniae and Klebsiella oxytoca (9.9%), and Escherichia coli (9.3%).
The report’s investigators noted that their estimates "are remarkably similar to estimates from other data sources," such as the National Healthcare Safety Network and the Emerging Infections Program. That "bolsters our confidence in the overall estimates of health care–associated infections that we have generated," they said.
Sounding the alarm
The report "sounds the alarm" about infectious threats to hospitalized patients that need addressing, especially lung and gut infections and infections related to surgery or urinary catheters, Dr. Bell said. It also sheds light on several important pathogens, especially C. difficile, Staphylococci, and the family of Enterobacter organisms.
Those pathogens are at the center of President Barack Obama’s request for $30 million as part of his proposed $6.6 billion budget for 2015 for a new initiative to halve infections by those organisms within 5 years, Dr. Bell said.
The $30 million would be used to improve tracking of infections, the nation’s capacity for lab testing to determine which pathogens are most problematic, and "boots on the ground" to help hospitals implement best practices, Dr. Bell said.
The CDC would like to see every hospital in the country develop a strong antibiotic stewardship program, because "the challenge with antibiotic resistance can’t be overstated," he cautioned.
A patient advocate echoed that concern at the media briefing.
"While inwardly I breathe a small sigh of relief that annual infections and mortalities are diminishing, I remain extremely cautious regarding the growing threat of antibiotic resistance and the dire impact of this potential danger to American health care," said Victoria Nahum, executive director of the Safe Care Campaign. Ms. Nahum and her husband, Armando Nahum, founded the nonprofit organization after their son died of a health care–associated infection and two other family members developed complications from health care–associated infections.
Health care providers "have the power to prevent health care–associated infections" through compulsive hand hygiene and other best practices, Ms. Nahum said. Patients need to be more assertive, she added. "You just don’t flop down and say, ‘Take care of me.’ You have to kind of navigate what’s going to happen to you. In doing so, that can save your own life."
Dr. Bell suggested that hospitalized patients have a friend or family member be the "bad cop" and repeatedly ask caregivers if they have washed their hands, when urinary catheters can come out, and whether testing is being done to ensure that the right antibiotic is being used.
He said he knows that can be difficult for patients who may feel intimidated. "When my own mother was in the intensive care unit, I found it hard to pipe up," Dr. Bell said. "If I find it hard, I can’t imagine what it’s like for everybody else."
Dr. Magill reported no potential financial conflicts of interest; two of her associates reported ties to the Infectious Disease Consulting Corp. and Parexel.
Ceritinib found safe and effective for NSCLC
The anaplastic lymphoma kinase inhibitor ceritinib showed "substantial and durable" activity against advanced non–small cell lung cancer harboring ALK gene rearrangements in a phase I study designed, analyzed, and sponsored by the manufacturer and reported online March 26 in the New England Journal of Medicine.
The trial involved 122 adults with locally advanced or metastatic NSCLC and 8 with other cancers (breast cancer, alveolar rhabdomyosarcoma, inflammatory myofibroblastic tumor, neoplastic large-cell lymphoma, and rectal adenocarcinoma), all of which harbored genetic alterations in the anaplastic lymphoma kinase (ALK) gene. In preclinical studies, ceritinib was found to be 20 times more potent than crizotinib (also an ALK inhibitor), and it appeared as though it would be effective in patients who had responded to crizotinib but eventually developed resistance to that drug, said Dr. Alice T. Shaw of Massachusetts General Hospital, Boston, and her associates.
In the current trial, the investigators found oral ceritinib to be safe, with a maximum tolerated dose of 750 mg daily in 21-day cycles. The most common adverse events were nausea (82% of patients), diarrhea (75%), vomiting (65%), fatigue (47%), and increased alanine aminotransferase levels (35%). Four cases of interstitial lung disease were thought to be possibly related to the drug, as was one case of asymptomatic grade 3 prolongation of the QT interval; all of these resolved when ceritinib was discontinued. Eight patients (6%) discontinued the drug because of adverse events.
Although this phase I trial (NCT01283516) was designed only to determine the safety and tolerability of ceritinib, the investigators also found that it was effective in NSCLC, both in patients who had never been treated with crizotinib and in those who had. Among the 114 NSCLC patients who received at least 400 mg of ceritinib per day, the overall response rate was 58%, and among the 80 who had previously been treated with crizotinib, the response rate was 56%. Some responses where characterized as "rapid and dramatic," and median progression-free survival was 7 months, the authors reported (New Engl. J. Med. 2014 March 26 [doi: 10.1056/NEJMoa1311107]).
Two of the 8 study participants who had cancers other than NSCLC – one with anaplastic large-cell lymphoma and another with inflammatory myofibroblastic tumor – also showed a treatment response.
"These findings suggest that the large majority of crizotinib-resistant tumors may remain ALK-dependent and that an important factor contributing to crizotinib resistance may be subtherapeutic inhibition of the target, which may be overcome by more potent and structurally distinct ALK inhibitors such as ceritinib. Alternatively, ceritinib may inhibit an unknown kinase that has not yet been found to play a role in the biology of these tumors," Dr. Shaw and her associates said.
This study was funded by Novartis, the National Cancer Institute, the V Foundation, Be a Piece of the Solution, and the Evan Spirito Memorial Foundation. Dr. Shaw reported ties to Novartis, Pfizer, and other companies, and her associates reported ties to numerous industry sources.
The relatively large study population of this phase I clinical trial is "a major advantage," said Dr. Roman K. Thomas.
With 114 patients receiving at least 400 mg of ceritinib and nearly 60% of them achieving remission, "this study is a first proof of concept for the successful targeting of ALK, beyond the establishment of safety and a maximum tolerated dose," he noted.
Even more striking was the finding that treatment response was independent of prior exposure to crizotinib therapy. "Thus, patients appear to have a second chance of response after relapse occurs [with] crizotinib."
Dr. Thomas is in the departments of translational genomics and pathology at the Center of Integrated Oncology Cologne-Bonn, and is on the medical faculty of the University of Cologne, Germany. He reported ties to numerous industry sources. These remarks were taken from his editorial accompanying Dr. Shaw’s report (New Engl. J. Med. 2014 March 26 [doi: 10.1056/NEJMe1316173]).
The relatively large study population of this phase I clinical trial is "a major advantage," said Dr. Roman K. Thomas.
With 114 patients receiving at least 400 mg of ceritinib and nearly 60% of them achieving remission, "this study is a first proof of concept for the successful targeting of ALK, beyond the establishment of safety and a maximum tolerated dose," he noted.
Even more striking was the finding that treatment response was independent of prior exposure to crizotinib therapy. "Thus, patients appear to have a second chance of response after relapse occurs [with] crizotinib."
Dr. Thomas is in the departments of translational genomics and pathology at the Center of Integrated Oncology Cologne-Bonn, and is on the medical faculty of the University of Cologne, Germany. He reported ties to numerous industry sources. These remarks were taken from his editorial accompanying Dr. Shaw’s report (New Engl. J. Med. 2014 March 26 [doi: 10.1056/NEJMe1316173]).
The relatively large study population of this phase I clinical trial is "a major advantage," said Dr. Roman K. Thomas.
With 114 patients receiving at least 400 mg of ceritinib and nearly 60% of them achieving remission, "this study is a first proof of concept for the successful targeting of ALK, beyond the establishment of safety and a maximum tolerated dose," he noted.
Even more striking was the finding that treatment response was independent of prior exposure to crizotinib therapy. "Thus, patients appear to have a second chance of response after relapse occurs [with] crizotinib."
Dr. Thomas is in the departments of translational genomics and pathology at the Center of Integrated Oncology Cologne-Bonn, and is on the medical faculty of the University of Cologne, Germany. He reported ties to numerous industry sources. These remarks were taken from his editorial accompanying Dr. Shaw’s report (New Engl. J. Med. 2014 March 26 [doi: 10.1056/NEJMe1316173]).
The anaplastic lymphoma kinase inhibitor ceritinib showed "substantial and durable" activity against advanced non–small cell lung cancer harboring ALK gene rearrangements in a phase I study designed, analyzed, and sponsored by the manufacturer and reported online March 26 in the New England Journal of Medicine.
The trial involved 122 adults with locally advanced or metastatic NSCLC and 8 with other cancers (breast cancer, alveolar rhabdomyosarcoma, inflammatory myofibroblastic tumor, neoplastic large-cell lymphoma, and rectal adenocarcinoma), all of which harbored genetic alterations in the anaplastic lymphoma kinase (ALK) gene. In preclinical studies, ceritinib was found to be 20 times more potent than crizotinib (also an ALK inhibitor), and it appeared as though it would be effective in patients who had responded to crizotinib but eventually developed resistance to that drug, said Dr. Alice T. Shaw of Massachusetts General Hospital, Boston, and her associates.
In the current trial, the investigators found oral ceritinib to be safe, with a maximum tolerated dose of 750 mg daily in 21-day cycles. The most common adverse events were nausea (82% of patients), diarrhea (75%), vomiting (65%), fatigue (47%), and increased alanine aminotransferase levels (35%). Four cases of interstitial lung disease were thought to be possibly related to the drug, as was one case of asymptomatic grade 3 prolongation of the QT interval; all of these resolved when ceritinib was discontinued. Eight patients (6%) discontinued the drug because of adverse events.
Although this phase I trial (NCT01283516) was designed only to determine the safety and tolerability of ceritinib, the investigators also found that it was effective in NSCLC, both in patients who had never been treated with crizotinib and in those who had. Among the 114 NSCLC patients who received at least 400 mg of ceritinib per day, the overall response rate was 58%, and among the 80 who had previously been treated with crizotinib, the response rate was 56%. Some responses where characterized as "rapid and dramatic," and median progression-free survival was 7 months, the authors reported (New Engl. J. Med. 2014 March 26 [doi: 10.1056/NEJMoa1311107]).
Two of the 8 study participants who had cancers other than NSCLC – one with anaplastic large-cell lymphoma and another with inflammatory myofibroblastic tumor – also showed a treatment response.
"These findings suggest that the large majority of crizotinib-resistant tumors may remain ALK-dependent and that an important factor contributing to crizotinib resistance may be subtherapeutic inhibition of the target, which may be overcome by more potent and structurally distinct ALK inhibitors such as ceritinib. Alternatively, ceritinib may inhibit an unknown kinase that has not yet been found to play a role in the biology of these tumors," Dr. Shaw and her associates said.
This study was funded by Novartis, the National Cancer Institute, the V Foundation, Be a Piece of the Solution, and the Evan Spirito Memorial Foundation. Dr. Shaw reported ties to Novartis, Pfizer, and other companies, and her associates reported ties to numerous industry sources.
The anaplastic lymphoma kinase inhibitor ceritinib showed "substantial and durable" activity against advanced non–small cell lung cancer harboring ALK gene rearrangements in a phase I study designed, analyzed, and sponsored by the manufacturer and reported online March 26 in the New England Journal of Medicine.
The trial involved 122 adults with locally advanced or metastatic NSCLC and 8 with other cancers (breast cancer, alveolar rhabdomyosarcoma, inflammatory myofibroblastic tumor, neoplastic large-cell lymphoma, and rectal adenocarcinoma), all of which harbored genetic alterations in the anaplastic lymphoma kinase (ALK) gene. In preclinical studies, ceritinib was found to be 20 times more potent than crizotinib (also an ALK inhibitor), and it appeared as though it would be effective in patients who had responded to crizotinib but eventually developed resistance to that drug, said Dr. Alice T. Shaw of Massachusetts General Hospital, Boston, and her associates.
In the current trial, the investigators found oral ceritinib to be safe, with a maximum tolerated dose of 750 mg daily in 21-day cycles. The most common adverse events were nausea (82% of patients), diarrhea (75%), vomiting (65%), fatigue (47%), and increased alanine aminotransferase levels (35%). Four cases of interstitial lung disease were thought to be possibly related to the drug, as was one case of asymptomatic grade 3 prolongation of the QT interval; all of these resolved when ceritinib was discontinued. Eight patients (6%) discontinued the drug because of adverse events.
Although this phase I trial (NCT01283516) was designed only to determine the safety and tolerability of ceritinib, the investigators also found that it was effective in NSCLC, both in patients who had never been treated with crizotinib and in those who had. Among the 114 NSCLC patients who received at least 400 mg of ceritinib per day, the overall response rate was 58%, and among the 80 who had previously been treated with crizotinib, the response rate was 56%. Some responses where characterized as "rapid and dramatic," and median progression-free survival was 7 months, the authors reported (New Engl. J. Med. 2014 March 26 [doi: 10.1056/NEJMoa1311107]).
Two of the 8 study participants who had cancers other than NSCLC – one with anaplastic large-cell lymphoma and another with inflammatory myofibroblastic tumor – also showed a treatment response.
"These findings suggest that the large majority of crizotinib-resistant tumors may remain ALK-dependent and that an important factor contributing to crizotinib resistance may be subtherapeutic inhibition of the target, which may be overcome by more potent and structurally distinct ALK inhibitors such as ceritinib. Alternatively, ceritinib may inhibit an unknown kinase that has not yet been found to play a role in the biology of these tumors," Dr. Shaw and her associates said.
This study was funded by Novartis, the National Cancer Institute, the V Foundation, Be a Piece of the Solution, and the Evan Spirito Memorial Foundation. Dr. Shaw reported ties to Novartis, Pfizer, and other companies, and her associates reported ties to numerous industry sources.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major finding: Oral ceritinib was found to be safe, with a maximum tolerated dose of 750 mg daily, and it elicited an overall tumor response rate of 58% in patients who received at least 400 mg daily.
Data source: A phase I clinical trial involving 130 adults with NSCLC or other cancers harboring ALK gene rearrangements who were treated with 50-750 mg of oral ceritinib daily.
Disclosures: This study was funded by Novartis, the National Cancer Institute, the V Foundation, Be a Piece of the Solution, and the Evan Spirito Memorial Foundation. Dr. Shaw reported ties to Novartis, Pfizer, and other companies, and her associates reported ties to numerous industry sources.
Most health care–associated infections aren’t device associated
An estimated 4% of inpatients at U.S. acute care hospitals have at least one health care–associated infection on any given day, according to a report published online March 26 in the New England Journal of Medicine.
Moreover, in a prevalence survey involving 183 acute care hospitals across 10 geographically diverse states, device-associated infections, "which have been a major focus of infection prevention in recent decades," accounted for only 25.6% of all health care–associated infections, said Dr. Shelley S. Magill of the division of health care quality promotion, Centers for Disease Control and Prevention, and her associates (N. Engl. J. Med. 2014;370:1198-1208).
In contrast, Clostridium difficile and other gastrointestinal infections, as well as non–ventilator-associated pneumonia, accounted for approximately half of all health care–associated infections in the survey. Surgical site infections also are still very common, accounting for 21.8%.
Because it appears that ventilator-associated pneumonia, catheter-associated UTIs, and central catheter–associated bloodstream infections are no longer the primary threat that they used to be, the study findings should prompt experts to "expand the public health focus to include these other types of infections, identifying patients at risk and developing effective countermeasures," the report’s authors noted.
The report shows that as a nation, we’re moving in the right direction; but there’s a great deal of work still to be done," Dr. Michael Bell said in a media briefing. "On any given day, 1 out of 25 hospitalized patients has an infection. And of those people, as many as one out of nine go on to die. This is not a minor issue," said Dr. Bell, deputy director of the CDC’s division of health care quality promotion.
The investigators developed and conducted the survey in 2011 to address a serious knowledge gap: No single surveillance system can provide estimates of "the burden of all types of such infections across acute care patient populations." So, Dr. Magill and her colleagues studied health care–associated infections among inpatients of all ages at 93 small, 68 medium-sized, and 22 large hospitals.
They found 504 such infections in 452 patients out of 11,282 patients covered in the survey, for an overall incidence of 4%. Using a statistical modeling process that accounted for predictors of infection prevalence and then applying those results to a nationally representative sample of U.S. community hospital stays, the investigators estimated that 648,000 inpatients nationwide had approximately 721,800 health care–associated infections in 2011.
Those estimates are lower than previous ones, such as those derived from the Study on the Efficacy of Nosocomial Infection Control in the 1970s , which postulated 2.1 million health care–associated infections each year, and those derived from National Nosocomial Infections Surveillance system data from 1990 to 2002, which estimated 1.7 million each year.
However, "it is difficult to draw conclusions from these comparisons because of the differences in patient populations, surveillance definitions of health care–associated infections, and data collection and analytical methods among these CDC methods," Dr. Magill and her associates said.
The current survey showed that 42.9% of health care–associated infections developed during a stay in a critical care unit or within 48 hours after; another 42.4% developed after a stay in a nonnursery ward.
Most of the surgical site infections were related to colon surgeries (14.5%), hip arthroplasty (10.0%), and small-bowel procedures (6.4%).
The median length of time between hospital admission and the onset of infection symptoms was 6 days.
C. difficile was the most frequently identified pathogen, accounting for 70.9% of all nosocomial GI infections and 12.1% of all health care–associated infections. Other common pathogens included Staphylococcus aureus (10.7% of all health care–associated infections), Klebsiella pneumoniae and Klebsiella oxytoca (9.9%), and Escherichia coli (9.3%).
The report’s investigators noted that their estimates "are remarkably similar to estimates from other data sources," such as the National Healthcare Safety Network and the Emerging Infections Program. That "bolsters our confidence in the overall estimates of health care–associated infections that we have generated," they said.
Sounding the alarm
The report "sounds the alarm" about infectious threats to hospitalized patients that need addressing, especially lung and gut infections and infections related to surgery or urinary catheters, Dr. Bell said. It also sheds light on several important pathogens, especially C. difficile, Staphylococci, and the family of Enterobacter organisms.
Those pathogens are at the center of President Barack Obama’s request for $30 million as part of his proposed $6.6 billion budget for 2015 for a new initiative to halve infections by those organisms within 5 years, Dr. Bell said.
The $30 million would be used to improve tracking of infections, the nation’s capacity for lab testing to determine which pathogens are most problematic, and "boots on the ground" to help hospitals implement best practices, Dr. Bell said.
The CDC would like to see every hospital in the country develop a strong antibiotic stewardship program, because "the challenge with antibiotic resistance can’t be overstated," he cautioned.
A patient advocate echoed that concern at the media briefing.
"While inwardly I breathe a small sigh of relief that annual infections and mortalities are diminishing, I remain extremely cautious regarding the growing threat of antibiotic resistance and the dire impact of this potential danger to American health care," said Victoria Nahum, executive director of the Safe Care Campaign. Ms. Nahum and her husband, Armando Nahum, founded the nonprofit organization after their son died of a health care–associated infection and two other family members developed complications from health care–associated infections.
Health care providers "have the power to prevent health care–associated infections" through compulsive hand hygiene and other best practices, Ms. Nahum said. Patients need to be more assertive, she added. "You just don’t flop down and say, ‘Take care of me.’ You have to kind of navigate what’s going to happen to you. In doing so, that can save your own life."
Dr. Bell suggested that hospitalized patients have a friend or family member be the "bad cop" and repeatedly ask caregivers if they have washed their hands, when urinary catheters can come out, and whether testing is being done to ensure that the right antibiotic is being used.
He said he knows that can be difficult for patients who may feel intimidated. "When my own mother was in the intensive care unit, I found it hard to pipe up," Dr. Bell said. "If I find it hard, I can’t imagine what it’s like for everybody else."
Dr. Magill reported no potential financial conflicts of interest; two of her associates reported ties to the Infectious Disease Consulting Corp. and Parexel.
An estimated 4% of inpatients at U.S. acute care hospitals have at least one health care–associated infection on any given day, according to a report published online March 26 in the New England Journal of Medicine.
Moreover, in a prevalence survey involving 183 acute care hospitals across 10 geographically diverse states, device-associated infections, "which have been a major focus of infection prevention in recent decades," accounted for only 25.6% of all health care–associated infections, said Dr. Shelley S. Magill of the division of health care quality promotion, Centers for Disease Control and Prevention, and her associates (N. Engl. J. Med. 2014;370:1198-1208).
In contrast, Clostridium difficile and other gastrointestinal infections, as well as non–ventilator-associated pneumonia, accounted for approximately half of all health care–associated infections in the survey. Surgical site infections also are still very common, accounting for 21.8%.
Because it appears that ventilator-associated pneumonia, catheter-associated UTIs, and central catheter–associated bloodstream infections are no longer the primary threat that they used to be, the study findings should prompt experts to "expand the public health focus to include these other types of infections, identifying patients at risk and developing effective countermeasures," the report’s authors noted.
The report shows that as a nation, we’re moving in the right direction; but there’s a great deal of work still to be done," Dr. Michael Bell said in a media briefing. "On any given day, 1 out of 25 hospitalized patients has an infection. And of those people, as many as one out of nine go on to die. This is not a minor issue," said Dr. Bell, deputy director of the CDC’s division of health care quality promotion.
The investigators developed and conducted the survey in 2011 to address a serious knowledge gap: No single surveillance system can provide estimates of "the burden of all types of such infections across acute care patient populations." So, Dr. Magill and her colleagues studied health care–associated infections among inpatients of all ages at 93 small, 68 medium-sized, and 22 large hospitals.
They found 504 such infections in 452 patients out of 11,282 patients covered in the survey, for an overall incidence of 4%. Using a statistical modeling process that accounted for predictors of infection prevalence and then applying those results to a nationally representative sample of U.S. community hospital stays, the investigators estimated that 648,000 inpatients nationwide had approximately 721,800 health care–associated infections in 2011.
Those estimates are lower than previous ones, such as those derived from the Study on the Efficacy of Nosocomial Infection Control in the 1970s , which postulated 2.1 million health care–associated infections each year, and those derived from National Nosocomial Infections Surveillance system data from 1990 to 2002, which estimated 1.7 million each year.
However, "it is difficult to draw conclusions from these comparisons because of the differences in patient populations, surveillance definitions of health care–associated infections, and data collection and analytical methods among these CDC methods," Dr. Magill and her associates said.
The current survey showed that 42.9% of health care–associated infections developed during a stay in a critical care unit or within 48 hours after; another 42.4% developed after a stay in a nonnursery ward.
Most of the surgical site infections were related to colon surgeries (14.5%), hip arthroplasty (10.0%), and small-bowel procedures (6.4%).
The median length of time between hospital admission and the onset of infection symptoms was 6 days.
C. difficile was the most frequently identified pathogen, accounting for 70.9% of all nosocomial GI infections and 12.1% of all health care–associated infections. Other common pathogens included Staphylococcus aureus (10.7% of all health care–associated infections), Klebsiella pneumoniae and Klebsiella oxytoca (9.9%), and Escherichia coli (9.3%).
The report’s investigators noted that their estimates "are remarkably similar to estimates from other data sources," such as the National Healthcare Safety Network and the Emerging Infections Program. That "bolsters our confidence in the overall estimates of health care–associated infections that we have generated," they said.
Sounding the alarm
The report "sounds the alarm" about infectious threats to hospitalized patients that need addressing, especially lung and gut infections and infections related to surgery or urinary catheters, Dr. Bell said. It also sheds light on several important pathogens, especially C. difficile, Staphylococci, and the family of Enterobacter organisms.
Those pathogens are at the center of President Barack Obama’s request for $30 million as part of his proposed $6.6 billion budget for 2015 for a new initiative to halve infections by those organisms within 5 years, Dr. Bell said.
The $30 million would be used to improve tracking of infections, the nation’s capacity for lab testing to determine which pathogens are most problematic, and "boots on the ground" to help hospitals implement best practices, Dr. Bell said.
The CDC would like to see every hospital in the country develop a strong antibiotic stewardship program, because "the challenge with antibiotic resistance can’t be overstated," he cautioned.
A patient advocate echoed that concern at the media briefing.
"While inwardly I breathe a small sigh of relief that annual infections and mortalities are diminishing, I remain extremely cautious regarding the growing threat of antibiotic resistance and the dire impact of this potential danger to American health care," said Victoria Nahum, executive director of the Safe Care Campaign. Ms. Nahum and her husband, Armando Nahum, founded the nonprofit organization after their son died of a health care–associated infection and two other family members developed complications from health care–associated infections.
Health care providers "have the power to prevent health care–associated infections" through compulsive hand hygiene and other best practices, Ms. Nahum said. Patients need to be more assertive, she added. "You just don’t flop down and say, ‘Take care of me.’ You have to kind of navigate what’s going to happen to you. In doing so, that can save your own life."
Dr. Bell suggested that hospitalized patients have a friend or family member be the "bad cop" and repeatedly ask caregivers if they have washed their hands, when urinary catheters can come out, and whether testing is being done to ensure that the right antibiotic is being used.
He said he knows that can be difficult for patients who may feel intimidated. "When my own mother was in the intensive care unit, I found it hard to pipe up," Dr. Bell said. "If I find it hard, I can’t imagine what it’s like for everybody else."
Dr. Magill reported no potential financial conflicts of interest; two of her associates reported ties to the Infectious Disease Consulting Corp. and Parexel.
An estimated 4% of inpatients at U.S. acute care hospitals have at least one health care–associated infection on any given day, according to a report published online March 26 in the New England Journal of Medicine.
Moreover, in a prevalence survey involving 183 acute care hospitals across 10 geographically diverse states, device-associated infections, "which have been a major focus of infection prevention in recent decades," accounted for only 25.6% of all health care–associated infections, said Dr. Shelley S. Magill of the division of health care quality promotion, Centers for Disease Control and Prevention, and her associates (N. Engl. J. Med. 2014;370:1198-1208).
In contrast, Clostridium difficile and other gastrointestinal infections, as well as non–ventilator-associated pneumonia, accounted for approximately half of all health care–associated infections in the survey. Surgical site infections also are still very common, accounting for 21.8%.
Because it appears that ventilator-associated pneumonia, catheter-associated UTIs, and central catheter–associated bloodstream infections are no longer the primary threat that they used to be, the study findings should prompt experts to "expand the public health focus to include these other types of infections, identifying patients at risk and developing effective countermeasures," the report’s authors noted.
The report shows that as a nation, we’re moving in the right direction; but there’s a great deal of work still to be done," Dr. Michael Bell said in a media briefing. "On any given day, 1 out of 25 hospitalized patients has an infection. And of those people, as many as one out of nine go on to die. This is not a minor issue," said Dr. Bell, deputy director of the CDC’s division of health care quality promotion.
The investigators developed and conducted the survey in 2011 to address a serious knowledge gap: No single surveillance system can provide estimates of "the burden of all types of such infections across acute care patient populations." So, Dr. Magill and her colleagues studied health care–associated infections among inpatients of all ages at 93 small, 68 medium-sized, and 22 large hospitals.
They found 504 such infections in 452 patients out of 11,282 patients covered in the survey, for an overall incidence of 4%. Using a statistical modeling process that accounted for predictors of infection prevalence and then applying those results to a nationally representative sample of U.S. community hospital stays, the investigators estimated that 648,000 inpatients nationwide had approximately 721,800 health care–associated infections in 2011.
Those estimates are lower than previous ones, such as those derived from the Study on the Efficacy of Nosocomial Infection Control in the 1970s , which postulated 2.1 million health care–associated infections each year, and those derived from National Nosocomial Infections Surveillance system data from 1990 to 2002, which estimated 1.7 million each year.
However, "it is difficult to draw conclusions from these comparisons because of the differences in patient populations, surveillance definitions of health care–associated infections, and data collection and analytical methods among these CDC methods," Dr. Magill and her associates said.
The current survey showed that 42.9% of health care–associated infections developed during a stay in a critical care unit or within 48 hours after; another 42.4% developed after a stay in a nonnursery ward.
Most of the surgical site infections were related to colon surgeries (14.5%), hip arthroplasty (10.0%), and small-bowel procedures (6.4%).
The median length of time between hospital admission and the onset of infection symptoms was 6 days.
C. difficile was the most frequently identified pathogen, accounting for 70.9% of all nosocomial GI infections and 12.1% of all health care–associated infections. Other common pathogens included Staphylococcus aureus (10.7% of all health care–associated infections), Klebsiella pneumoniae and Klebsiella oxytoca (9.9%), and Escherichia coli (9.3%).
The report’s investigators noted that their estimates "are remarkably similar to estimates from other data sources," such as the National Healthcare Safety Network and the Emerging Infections Program. That "bolsters our confidence in the overall estimates of health care–associated infections that we have generated," they said.
Sounding the alarm
The report "sounds the alarm" about infectious threats to hospitalized patients that need addressing, especially lung and gut infections and infections related to surgery or urinary catheters, Dr. Bell said. It also sheds light on several important pathogens, especially C. difficile, Staphylococci, and the family of Enterobacter organisms.
Those pathogens are at the center of President Barack Obama’s request for $30 million as part of his proposed $6.6 billion budget for 2015 for a new initiative to halve infections by those organisms within 5 years, Dr. Bell said.
The $30 million would be used to improve tracking of infections, the nation’s capacity for lab testing to determine which pathogens are most problematic, and "boots on the ground" to help hospitals implement best practices, Dr. Bell said.
The CDC would like to see every hospital in the country develop a strong antibiotic stewardship program, because "the challenge with antibiotic resistance can’t be overstated," he cautioned.
A patient advocate echoed that concern at the media briefing.
"While inwardly I breathe a small sigh of relief that annual infections and mortalities are diminishing, I remain extremely cautious regarding the growing threat of antibiotic resistance and the dire impact of this potential danger to American health care," said Victoria Nahum, executive director of the Safe Care Campaign. Ms. Nahum and her husband, Armando Nahum, founded the nonprofit organization after their son died of a health care–associated infection and two other family members developed complications from health care–associated infections.
Health care providers "have the power to prevent health care–associated infections" through compulsive hand hygiene and other best practices, Ms. Nahum said. Patients need to be more assertive, she added. "You just don’t flop down and say, ‘Take care of me.’ You have to kind of navigate what’s going to happen to you. In doing so, that can save your own life."
Dr. Bell suggested that hospitalized patients have a friend or family member be the "bad cop" and repeatedly ask caregivers if they have washed their hands, when urinary catheters can come out, and whether testing is being done to ensure that the right antibiotic is being used.
He said he knows that can be difficult for patients who may feel intimidated. "When my own mother was in the intensive care unit, I found it hard to pipe up," Dr. Bell said. "If I find it hard, I can’t imagine what it’s like for everybody else."
Dr. Magill reported no potential financial conflicts of interest; two of her associates reported ties to the Infectious Disease Consulting Corp. and Parexel.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major finding: An estimated 648,000 inpatients at U.S. acute care hospitals had approximately 721,800 health care–associated infections in 2011, but only 25% of these infections were related to devices such as ventilators, catheters, or central lines. Most health care–associated infections were non–ventilator-associated pneumonias, surgical site infections, or GI infections.
Data source: A prevalence survey of health care–associated infections among inpatients of all ages at 183 acute care hospitals in 10 geographically diverse states, plus an application of the results to a nationally representative sample of community hospital stays.
Disclosures: Dr. Magill reported no potential financial conflicts of interest; two of her associates reported ties to the Infectious Disease Consulting Corp. and Parexel.
Outcomes linked to distance from liver transplant center
Eligible patients who live farther away from a liver transplant center are less likely to be put on a waiting list, less likely to receive a transplant, and more likely to die within 5 years than are those who live closer, according to a report published online March 25 in JAMA.
These findings have broad implications beyond those for liver transplantation alone. "As complex, expensive medical technology evolves, certain services may be offered only at a limited number of sites" – an approach that may be more efficient but that increases the distance between patients and the centers at which they can receive care. "Our study is the first to demonstrate the adverse consequences of centralization of specialized care at a limited number of sites," said Dr. David S. Goldberg of the division of gastroenterology, Hospital of the University of Pennsylvania, Philadelphia, and his associates.
The researchers assessed the medical records of 50,637 patients who were active users of Veterans Affairs outpatient care and had decompensated cirrhosis or hepatocellular carcinoma; of these, 2,895 were wait-listed for liver transplantation during 2003 and 2012. Liver transplantation is offered at only five VA transplant centers, which are located in Houston; Nashville, Tenn.; Pittsburgh; Portland, Ore.; and Richmond, Va.
Patients who lived farther away from these five centers and from non-VA transplant centers were significantly less likely to be wait-listed than were those who lived closer. For example, 66% of veterans who lived within 100 miles of a liver transplant center were wait-listed, compared with less than 51% of those who resided farther away.
Once patients were on the list, they were significantly less likely to receive a liver transplant if they resided far from a transplant center. For example, 70.4% of patients who lived within 100 miles of a transplant center received a transplant, compared with only 58.8% of those who lived 101-200 miles away, 57.3% of those who lived 201-300 miles away, and 53.5% of those who lived 301-500 miles away.
Overall survival also decreased as distance from a liver transplant center increased. For example, a wait-listed patient living 25 miles from a transplant center had a 62.9% probability of survival 5 years from the first hepatic decompensation event, while one who lived 100 miles from a transplant center had a 59.8% probability of surviving 5 years from the first hepatic decompensation event, Dr. Goldberg and his associates wrote (JAMA 2014;311:1234-43).
Several health services including proton-beam therapy, bariatric surgery, and treatment for complex or rare cancers currently are offered at a limited number of sites or are preferentially reimbursed by insurers if they are treated at designated "centers of excellence." The results of this study demonstrate that such centralized care may have the unintended consequence of excluding patients who live farther from these centers from treatment, the investigators added.
This study was supported in part by the U.S. Health Resources and Services Administration. No financial conflicts of interest were reported.
Eligible patients who live farther away from a liver transplant center are less likely to be put on a waiting list, less likely to receive a transplant, and more likely to die within 5 years than are those who live closer, according to a report published online March 25 in JAMA.
These findings have broad implications beyond those for liver transplantation alone. "As complex, expensive medical technology evolves, certain services may be offered only at a limited number of sites" – an approach that may be more efficient but that increases the distance between patients and the centers at which they can receive care. "Our study is the first to demonstrate the adverse consequences of centralization of specialized care at a limited number of sites," said Dr. David S. Goldberg of the division of gastroenterology, Hospital of the University of Pennsylvania, Philadelphia, and his associates.
The researchers assessed the medical records of 50,637 patients who were active users of Veterans Affairs outpatient care and had decompensated cirrhosis or hepatocellular carcinoma; of these, 2,895 were wait-listed for liver transplantation during 2003 and 2012. Liver transplantation is offered at only five VA transplant centers, which are located in Houston; Nashville, Tenn.; Pittsburgh; Portland, Ore.; and Richmond, Va.
Patients who lived farther away from these five centers and from non-VA transplant centers were significantly less likely to be wait-listed than were those who lived closer. For example, 66% of veterans who lived within 100 miles of a liver transplant center were wait-listed, compared with less than 51% of those who resided farther away.
Once patients were on the list, they were significantly less likely to receive a liver transplant if they resided far from a transplant center. For example, 70.4% of patients who lived within 100 miles of a transplant center received a transplant, compared with only 58.8% of those who lived 101-200 miles away, 57.3% of those who lived 201-300 miles away, and 53.5% of those who lived 301-500 miles away.
Overall survival also decreased as distance from a liver transplant center increased. For example, a wait-listed patient living 25 miles from a transplant center had a 62.9% probability of survival 5 years from the first hepatic decompensation event, while one who lived 100 miles from a transplant center had a 59.8% probability of surviving 5 years from the first hepatic decompensation event, Dr. Goldberg and his associates wrote (JAMA 2014;311:1234-43).
Several health services including proton-beam therapy, bariatric surgery, and treatment for complex or rare cancers currently are offered at a limited number of sites or are preferentially reimbursed by insurers if they are treated at designated "centers of excellence." The results of this study demonstrate that such centralized care may have the unintended consequence of excluding patients who live farther from these centers from treatment, the investigators added.
This study was supported in part by the U.S. Health Resources and Services Administration. No financial conflicts of interest were reported.
Eligible patients who live farther away from a liver transplant center are less likely to be put on a waiting list, less likely to receive a transplant, and more likely to die within 5 years than are those who live closer, according to a report published online March 25 in JAMA.
These findings have broad implications beyond those for liver transplantation alone. "As complex, expensive medical technology evolves, certain services may be offered only at a limited number of sites" – an approach that may be more efficient but that increases the distance between patients and the centers at which they can receive care. "Our study is the first to demonstrate the adverse consequences of centralization of specialized care at a limited number of sites," said Dr. David S. Goldberg of the division of gastroenterology, Hospital of the University of Pennsylvania, Philadelphia, and his associates.
The researchers assessed the medical records of 50,637 patients who were active users of Veterans Affairs outpatient care and had decompensated cirrhosis or hepatocellular carcinoma; of these, 2,895 were wait-listed for liver transplantation during 2003 and 2012. Liver transplantation is offered at only five VA transplant centers, which are located in Houston; Nashville, Tenn.; Pittsburgh; Portland, Ore.; and Richmond, Va.
Patients who lived farther away from these five centers and from non-VA transplant centers were significantly less likely to be wait-listed than were those who lived closer. For example, 66% of veterans who lived within 100 miles of a liver transplant center were wait-listed, compared with less than 51% of those who resided farther away.
Once patients were on the list, they were significantly less likely to receive a liver transplant if they resided far from a transplant center. For example, 70.4% of patients who lived within 100 miles of a transplant center received a transplant, compared with only 58.8% of those who lived 101-200 miles away, 57.3% of those who lived 201-300 miles away, and 53.5% of those who lived 301-500 miles away.
Overall survival also decreased as distance from a liver transplant center increased. For example, a wait-listed patient living 25 miles from a transplant center had a 62.9% probability of survival 5 years from the first hepatic decompensation event, while one who lived 100 miles from a transplant center had a 59.8% probability of surviving 5 years from the first hepatic decompensation event, Dr. Goldberg and his associates wrote (JAMA 2014;311:1234-43).
Several health services including proton-beam therapy, bariatric surgery, and treatment for complex or rare cancers currently are offered at a limited number of sites or are preferentially reimbursed by insurers if they are treated at designated "centers of excellence." The results of this study demonstrate that such centralized care may have the unintended consequence of excluding patients who live farther from these centers from treatment, the investigators added.
This study was supported in part by the U.S. Health Resources and Services Administration. No financial conflicts of interest were reported.
From JAMA
Major finding: Living more than 100 miles from a VA transplant center means that veterans in liver failure are less likely to survive to transplant: A wait-listed veteran living 25 miles from a VATC would have a 62.9% 5-year adjusted probability of survival from first hepatic decompensation event, compared with a 59.8% 5-year adjusted probability of survival for a veteran living 100 miles from a VATC.
Data source: A retrospective analysis of the medical records of 50,637 VA patients eligible for liver transplantation in 2003-2012.
Disclosures: This study was supported in part by the U.S. Health Resources and Services Administration. No financial conflicts of interest were reported.