User login
Screening adults for diabetes doesn’t lessen mortality
Screening asymptomatic adults for type 2 diabetes does not improve all-cause or cardiovascular mortality, according to a report published online April 13 in Annals of Internal Medicine.
An estimated 8 million asymptomatic adults are thought to have undiagnosed type 2 diabetes in the United States. In a systematic review of the literature since 2007, investigators for the U.S. Preventive Services Task Force found that screening for the disease, even when it leads to intensive interventions to decrease blood glucose, improve lipid profiles, and reduce blood pressure, fails to reduce 10-year mortality.
The USPSTF is now taking public comments on its findings and will finalize its recommendations on diabetes screening in the near future, said Dr. Shelley Selph, lead author of this report as well as professor of medical informatics and clinical epidemiology at Oregon Health & Sciences University, Portland, and her associates.
To update its 2008 recommendations on diabetes screening, the USPSTF reviewed the literature for relevant randomized, controlled trials; controlled observational studies; and systematic reviews published since then. The 2008 recommendations cited insufficient evidence to assess the balance of benefits and harms of screening asymptomatic adults unless they had elevated blood pressure.
Since then, two large, good-quality trials demonstrated that screening was not superior to no screening in reducing overall mortality. A third large, fair-quality trial showed that an intensive, multifactorial intervention failed to improve all-cause or cardiovascular mortality. And nine systematic reviews examining type 2 diabetes that was not specifically screen detected showed that intensive glucose control failed to reduce all-cause or cardiovascular mortality.
One trial deemed to be of fair quality found that, compared with not screening for type 2 diabetes, screening failed to reduce the risk of cardiovascular mortality (hazard ratio, 1.02), cancer mortality (HR, 1.08), or diabetes-related mortality (HR, 1.26), according to Dr. Selph and her associates (Ann. Intern. Med. 2015 April 13 [doi:10.7326/M14-2221]).
In addition, numerous other trials assessing outcomes after treatment of impaired fasting glucose or impaired glucose tolerance also consistently found no effect on all-cause or cardiovascular mortality. However, 16 trials found that this approach did delay progression to diabetes.
“There is also little evidence on the effect of screening in ethnic and racial minorities, in whom the prevalence of diabetes is greater than in persons of white, European ancestry,” Dr. Selph and her associates noted.
Screening asymptomatic adults for type 2 diabetes does not improve all-cause or cardiovascular mortality, according to a report published online April 13 in Annals of Internal Medicine.
An estimated 8 million asymptomatic adults are thought to have undiagnosed type 2 diabetes in the United States. In a systematic review of the literature since 2007, investigators for the U.S. Preventive Services Task Force found that screening for the disease, even when it leads to intensive interventions to decrease blood glucose, improve lipid profiles, and reduce blood pressure, fails to reduce 10-year mortality.
The USPSTF is now taking public comments on its findings and will finalize its recommendations on diabetes screening in the near future, said Dr. Shelley Selph, lead author of this report as well as professor of medical informatics and clinical epidemiology at Oregon Health & Sciences University, Portland, and her associates.
To update its 2008 recommendations on diabetes screening, the USPSTF reviewed the literature for relevant randomized, controlled trials; controlled observational studies; and systematic reviews published since then. The 2008 recommendations cited insufficient evidence to assess the balance of benefits and harms of screening asymptomatic adults unless they had elevated blood pressure.
Since then, two large, good-quality trials demonstrated that screening was not superior to no screening in reducing overall mortality. A third large, fair-quality trial showed that an intensive, multifactorial intervention failed to improve all-cause or cardiovascular mortality. And nine systematic reviews examining type 2 diabetes that was not specifically screen detected showed that intensive glucose control failed to reduce all-cause or cardiovascular mortality.
One trial deemed to be of fair quality found that, compared with not screening for type 2 diabetes, screening failed to reduce the risk of cardiovascular mortality (hazard ratio, 1.02), cancer mortality (HR, 1.08), or diabetes-related mortality (HR, 1.26), according to Dr. Selph and her associates (Ann. Intern. Med. 2015 April 13 [doi:10.7326/M14-2221]).
In addition, numerous other trials assessing outcomes after treatment of impaired fasting glucose or impaired glucose tolerance also consistently found no effect on all-cause or cardiovascular mortality. However, 16 trials found that this approach did delay progression to diabetes.
“There is also little evidence on the effect of screening in ethnic and racial minorities, in whom the prevalence of diabetes is greater than in persons of white, European ancestry,” Dr. Selph and her associates noted.
Screening asymptomatic adults for type 2 diabetes does not improve all-cause or cardiovascular mortality, according to a report published online April 13 in Annals of Internal Medicine.
An estimated 8 million asymptomatic adults are thought to have undiagnosed type 2 diabetes in the United States. In a systematic review of the literature since 2007, investigators for the U.S. Preventive Services Task Force found that screening for the disease, even when it leads to intensive interventions to decrease blood glucose, improve lipid profiles, and reduce blood pressure, fails to reduce 10-year mortality.
The USPSTF is now taking public comments on its findings and will finalize its recommendations on diabetes screening in the near future, said Dr. Shelley Selph, lead author of this report as well as professor of medical informatics and clinical epidemiology at Oregon Health & Sciences University, Portland, and her associates.
To update its 2008 recommendations on diabetes screening, the USPSTF reviewed the literature for relevant randomized, controlled trials; controlled observational studies; and systematic reviews published since then. The 2008 recommendations cited insufficient evidence to assess the balance of benefits and harms of screening asymptomatic adults unless they had elevated blood pressure.
Since then, two large, good-quality trials demonstrated that screening was not superior to no screening in reducing overall mortality. A third large, fair-quality trial showed that an intensive, multifactorial intervention failed to improve all-cause or cardiovascular mortality. And nine systematic reviews examining type 2 diabetes that was not specifically screen detected showed that intensive glucose control failed to reduce all-cause or cardiovascular mortality.
One trial deemed to be of fair quality found that, compared with not screening for type 2 diabetes, screening failed to reduce the risk of cardiovascular mortality (hazard ratio, 1.02), cancer mortality (HR, 1.08), or diabetes-related mortality (HR, 1.26), according to Dr. Selph and her associates (Ann. Intern. Med. 2015 April 13 [doi:10.7326/M14-2221]).
In addition, numerous other trials assessing outcomes after treatment of impaired fasting glucose or impaired glucose tolerance also consistently found no effect on all-cause or cardiovascular mortality. However, 16 trials found that this approach did delay progression to diabetes.
“There is also little evidence on the effect of screening in ethnic and racial minorities, in whom the prevalence of diabetes is greater than in persons of white, European ancestry,” Dr. Selph and her associates noted.
Key clinical point:Screening asymptomatic adults for type 2 diabetes does not improve all-cause or cardiovascular mortality.
Major finding: One fair-quality trial found that, compared with not screening for type 2 diabetes, screening failed to reduce the risk of cardiovascular mortality (HR, 1.02), cancer mortality (HR, 1.08), or diabetes-related mortality (HR, 1.26).
Data source:A systematic review of the literature since 2007 to inform the upcoming update of the USPSTF guideline on diabetes screening.
Disclosures: The USPSTF is supported by, but independent of, the U.S. AHRQ. Financial disclosures for Dr. Selph and her associates are available at www.acponline.org.
EDs pump up pediatric preparedness
Pediatric readiness has improved in emergency departments across the country, as measured by EDs’ compliance with 2009 guidelines for emergency care in children, according to a report published online April 13 in JAMA Pediatrics.
In what they described as “the most comprehensive evaluation of pediatric readiness of our nation’s EDs to date,” investigators performed a web-based assessment of 4,137 hospitals’ self-reported compliance with guidelines addressing child-specific emergency care. The overall median weighted pediatric readiness score (WPRS) was 68.9, a solid improvement over the previously reported median WPRS of 55, said Dr. Marianne Gausche-Hill of Harbor-UCLA Medical Center, Torrance, Calif., and her associates.
The single most important factor found to enhance pediatric readiness was to designate two people, one of whom is a physician or nurse, as the hospital’s pediatric emergency care coordinator, as recommended by the Institute of Medicine, the researchers wrote. Nearly half (47.5%) of EDs now have a physician coordinator, and 59.3% now have a nurse coordinator, compared with 18% and 12%, respectively, in a previous report. The presence of coordinators quadrupled the chances that a hospital would put important quality-improvement plans in place to address children’s care needs, the investigators said (JAMA Pediatr. 2015 April 13 [doi:10.1001/jamapediatrics.2015.138]).
Other findings included the following:
• Most physicians providing emergency care for children were specifically trained in emergency medicine (88.6%) or pediatric emergency medicine (55.4%) at high-volume hospitals; low-volume hospitals were more likely to have family-medicine-trained physicians doing so (78.9%).
• Mandatory competency evaluations for providing pediatric emergency care were relatively common for nurses (66.6%) but less so for physicians (38.7%) and midlevel staff (18.1%).
• 99.5% of EDs said all staff are trained on the location of pediatric equipment in the ED, including tools to ensure correct sizing of resuscitation equipment and appropriate dosing of medications.
• 83.1% of EDs said they verified the proper location and function of pediatric equipment daily.
• EDs routinely stocked 91% of recommended pediatric equipment. Equipment that was missing in more than 15% of EDs included laryngeal mask airways, umbilical vein catheters, central venous catheters, tracheostomy tubes, size 00 laryngoscope blades, continuous end-tidal carbon dioxide monitoring equipment, pediatric Magill forceps, and infant and child nasopharyngeal airways.
• Only 46.8% of EDs had disaster plans that specifically addressed children, as recommended. Even among high-volume hospitals, which were the most compliant with guidelines, only 67.4% had such disaster plans.
• Approximately one-third of EDs said their providers failed to weigh children and record the weight in kilograms only, as recommended. This safety measure is crucial to preventing drug-dosing errors.
• The most frequently cited barriers to complying with guidelines were the cost of child-specific training (reported by 54.4% of EDs) and a lack of educational resources (reported by 49.0%). Few EDs reported that a lack of interest was a barrier to implementing the guidelines.
This project was supported by the Emergency Medical Services for Children network and the EMS for Children National Resource Center under the U.S. Department of Health & Human Services. Dr. Gausche-Hill and her associates reported having no financial disclosures.
The assessment by Gausche-Hill et al. represents a watershed moment and a huge step forward in the path toward optimal care for children in the emergency-care setting. The 83% response rate to this voluntary self-report indicates both enthusiasm and accountability among emergency caregivers, and the results demonstrate a real improvement in pediatric readiness scores.
These data show that the single most important thing an ED can do to improve pediatric readiness is to designate a nurse and/or physician to serve as pediatric emergency care coordinator.
The next step is to move beyond measures of readiness and ensure that actual patient outcomes also improve.
Dr. Evaline A. Alessandrini is in the department of pediatrics at the James M. Anderson Center for Health Systems Excellence at Cincinnati Children’s Hospital. Dr. Joseph L. Wright is in the department of pediatrics and child health at Howard University, the department of emergency medicine and health policy at George Washington University, and the GWU Milken Institute School of Public Health, all in Washington, D.C. Dr. Alessandrini and Dr. Wright made these remarks in an editorial accompanying Dr. Gausche-Hill’s report (JAMA Pediatr. 2015 April 13 [doi:10.1001/jamapediatrics.2015.0357]).
The assessment by Gausche-Hill et al. represents a watershed moment and a huge step forward in the path toward optimal care for children in the emergency-care setting. The 83% response rate to this voluntary self-report indicates both enthusiasm and accountability among emergency caregivers, and the results demonstrate a real improvement in pediatric readiness scores.
These data show that the single most important thing an ED can do to improve pediatric readiness is to designate a nurse and/or physician to serve as pediatric emergency care coordinator.
The next step is to move beyond measures of readiness and ensure that actual patient outcomes also improve.
Dr. Evaline A. Alessandrini is in the department of pediatrics at the James M. Anderson Center for Health Systems Excellence at Cincinnati Children’s Hospital. Dr. Joseph L. Wright is in the department of pediatrics and child health at Howard University, the department of emergency medicine and health policy at George Washington University, and the GWU Milken Institute School of Public Health, all in Washington, D.C. Dr. Alessandrini and Dr. Wright made these remarks in an editorial accompanying Dr. Gausche-Hill’s report (JAMA Pediatr. 2015 April 13 [doi:10.1001/jamapediatrics.2015.0357]).
The assessment by Gausche-Hill et al. represents a watershed moment and a huge step forward in the path toward optimal care for children in the emergency-care setting. The 83% response rate to this voluntary self-report indicates both enthusiasm and accountability among emergency caregivers, and the results demonstrate a real improvement in pediatric readiness scores.
These data show that the single most important thing an ED can do to improve pediatric readiness is to designate a nurse and/or physician to serve as pediatric emergency care coordinator.
The next step is to move beyond measures of readiness and ensure that actual patient outcomes also improve.
Dr. Evaline A. Alessandrini is in the department of pediatrics at the James M. Anderson Center for Health Systems Excellence at Cincinnati Children’s Hospital. Dr. Joseph L. Wright is in the department of pediatrics and child health at Howard University, the department of emergency medicine and health policy at George Washington University, and the GWU Milken Institute School of Public Health, all in Washington, D.C. Dr. Alessandrini and Dr. Wright made these remarks in an editorial accompanying Dr. Gausche-Hill’s report (JAMA Pediatr. 2015 April 13 [doi:10.1001/jamapediatrics.2015.0357]).
Pediatric readiness has improved in emergency departments across the country, as measured by EDs’ compliance with 2009 guidelines for emergency care in children, according to a report published online April 13 in JAMA Pediatrics.
In what they described as “the most comprehensive evaluation of pediatric readiness of our nation’s EDs to date,” investigators performed a web-based assessment of 4,137 hospitals’ self-reported compliance with guidelines addressing child-specific emergency care. The overall median weighted pediatric readiness score (WPRS) was 68.9, a solid improvement over the previously reported median WPRS of 55, said Dr. Marianne Gausche-Hill of Harbor-UCLA Medical Center, Torrance, Calif., and her associates.
The single most important factor found to enhance pediatric readiness was to designate two people, one of whom is a physician or nurse, as the hospital’s pediatric emergency care coordinator, as recommended by the Institute of Medicine, the researchers wrote. Nearly half (47.5%) of EDs now have a physician coordinator, and 59.3% now have a nurse coordinator, compared with 18% and 12%, respectively, in a previous report. The presence of coordinators quadrupled the chances that a hospital would put important quality-improvement plans in place to address children’s care needs, the investigators said (JAMA Pediatr. 2015 April 13 [doi:10.1001/jamapediatrics.2015.138]).
Other findings included the following:
• Most physicians providing emergency care for children were specifically trained in emergency medicine (88.6%) or pediatric emergency medicine (55.4%) at high-volume hospitals; low-volume hospitals were more likely to have family-medicine-trained physicians doing so (78.9%).
• Mandatory competency evaluations for providing pediatric emergency care were relatively common for nurses (66.6%) but less so for physicians (38.7%) and midlevel staff (18.1%).
• 99.5% of EDs said all staff are trained on the location of pediatric equipment in the ED, including tools to ensure correct sizing of resuscitation equipment and appropriate dosing of medications.
• 83.1% of EDs said they verified the proper location and function of pediatric equipment daily.
• EDs routinely stocked 91% of recommended pediatric equipment. Equipment that was missing in more than 15% of EDs included laryngeal mask airways, umbilical vein catheters, central venous catheters, tracheostomy tubes, size 00 laryngoscope blades, continuous end-tidal carbon dioxide monitoring equipment, pediatric Magill forceps, and infant and child nasopharyngeal airways.
• Only 46.8% of EDs had disaster plans that specifically addressed children, as recommended. Even among high-volume hospitals, which were the most compliant with guidelines, only 67.4% had such disaster plans.
• Approximately one-third of EDs said their providers failed to weigh children and record the weight in kilograms only, as recommended. This safety measure is crucial to preventing drug-dosing errors.
• The most frequently cited barriers to complying with guidelines were the cost of child-specific training (reported by 54.4% of EDs) and a lack of educational resources (reported by 49.0%). Few EDs reported that a lack of interest was a barrier to implementing the guidelines.
This project was supported by the Emergency Medical Services for Children network and the EMS for Children National Resource Center under the U.S. Department of Health & Human Services. Dr. Gausche-Hill and her associates reported having no financial disclosures.
Pediatric readiness has improved in emergency departments across the country, as measured by EDs’ compliance with 2009 guidelines for emergency care in children, according to a report published online April 13 in JAMA Pediatrics.
In what they described as “the most comprehensive evaluation of pediatric readiness of our nation’s EDs to date,” investigators performed a web-based assessment of 4,137 hospitals’ self-reported compliance with guidelines addressing child-specific emergency care. The overall median weighted pediatric readiness score (WPRS) was 68.9, a solid improvement over the previously reported median WPRS of 55, said Dr. Marianne Gausche-Hill of Harbor-UCLA Medical Center, Torrance, Calif., and her associates.
The single most important factor found to enhance pediatric readiness was to designate two people, one of whom is a physician or nurse, as the hospital’s pediatric emergency care coordinator, as recommended by the Institute of Medicine, the researchers wrote. Nearly half (47.5%) of EDs now have a physician coordinator, and 59.3% now have a nurse coordinator, compared with 18% and 12%, respectively, in a previous report. The presence of coordinators quadrupled the chances that a hospital would put important quality-improvement plans in place to address children’s care needs, the investigators said (JAMA Pediatr. 2015 April 13 [doi:10.1001/jamapediatrics.2015.138]).
Other findings included the following:
• Most physicians providing emergency care for children were specifically trained in emergency medicine (88.6%) or pediatric emergency medicine (55.4%) at high-volume hospitals; low-volume hospitals were more likely to have family-medicine-trained physicians doing so (78.9%).
• Mandatory competency evaluations for providing pediatric emergency care were relatively common for nurses (66.6%) but less so for physicians (38.7%) and midlevel staff (18.1%).
• 99.5% of EDs said all staff are trained on the location of pediatric equipment in the ED, including tools to ensure correct sizing of resuscitation equipment and appropriate dosing of medications.
• 83.1% of EDs said they verified the proper location and function of pediatric equipment daily.
• EDs routinely stocked 91% of recommended pediatric equipment. Equipment that was missing in more than 15% of EDs included laryngeal mask airways, umbilical vein catheters, central venous catheters, tracheostomy tubes, size 00 laryngoscope blades, continuous end-tidal carbon dioxide monitoring equipment, pediatric Magill forceps, and infant and child nasopharyngeal airways.
• Only 46.8% of EDs had disaster plans that specifically addressed children, as recommended. Even among high-volume hospitals, which were the most compliant with guidelines, only 67.4% had such disaster plans.
• Approximately one-third of EDs said their providers failed to weigh children and record the weight in kilograms only, as recommended. This safety measure is crucial to preventing drug-dosing errors.
• The most frequently cited barriers to complying with guidelines were the cost of child-specific training (reported by 54.4% of EDs) and a lack of educational resources (reported by 49.0%). Few EDs reported that a lack of interest was a barrier to implementing the guidelines.
This project was supported by the Emergency Medical Services for Children network and the EMS for Children National Resource Center under the U.S. Department of Health & Human Services. Dr. Gausche-Hill and her associates reported having no financial disclosures.
FROM JAMA PEDIATRICS
Key clinical point: Nationally, emergency departments have improved their compliance with guidelines regarding emergency health care for children.
Major finding: The overall median weighted pediatric readiness score (WPRS) was 68.9, a solid improvement over the previously reported median WPRS of 55.
Data source: A web-based self-reported assessment of pediatric readiness at 4,149 EDs across the country that have approximately 24 million pediatric visits annually.
Disclosures: This project was supported by the Emergency Medical Services for Children network and the EMS for Children National Resource Center under the U.S. Department of Health & Human Services. Dr. Gausche-Hill and her associates reported having no financial disclosures.
‘Fresh’ no better than standard red cells
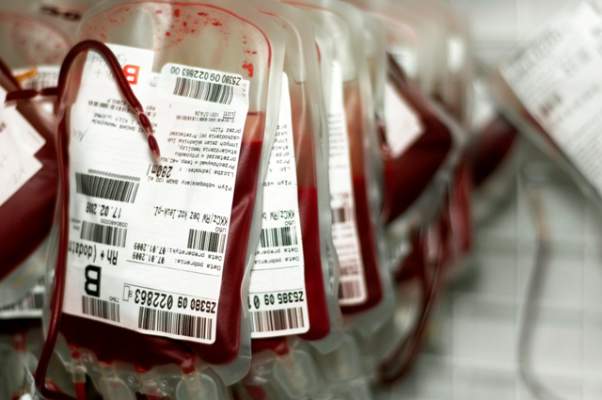
Compared with standard-issue red cells, transfusion of “fresh” red cells stored for fewer than 8 days failed to improve 90-day mortality in a large international study of adult ICU patients, which was reported online April 9 in the New England Journal of Medicine.
“Current regulations permit the storage of red cells for up to 42 days, but prolonged storage has been associated with changes that may render cells ineffective as oxygen carriers and that lead to the accumulation of substances that have untoward biologic effects,” said Dr. Jacques Lacroix of the University of Montreal and his associates.
A recent meta-analysis suggested that transfusion of older red cells was associated with a 16% increase in mortality among critically ill patients, but several randomized trials have failed to document any adverse effects on oxygenation, immunologic, or coagulation factors. Dr. Lacroix and his associates performed the Age of Blood Evaluation (ABLE) study, a prospective, blinded clinical trial involving ICU patients enrolled during a 5-year period at 64 medical centers in Canada, the United Kingdom, France, the Netherlands, and Belgium. A total of 1,211 participants were randomly assigned to receive “fresh” blood stored for an average of 6 days and 1,219 to receive standard blood stored for an average of 22 days – a difference that the investigators deemed statistically and clinically significant.
The primary outcome measure, 90-day all-cause mortality, was 37% in the fresh-blood group and 35% in the standard-blood group, a nonsignificant difference. There also were no significant differences in mortality between the two study groups in any of several subgroup analyses based on patient age; the number of units transfused; baseline APACHE II scores; major comorbidities; duration of respiratory, hemodynamic, or renal support; length of ICU stay; or length of hospital stay, Dr Lacroix and his associates said (N. Engl. J. Med. 2015 April 9 [doi:10.1056/NEJMoa1500704]).
“These findings have important implications for the critical care and blood transfusion communities. We surmise that the use of fresh red cells is not justified at this time. We might also infer that changes to red cells or the storage medium that have been documented in many laboratory studies may have limited clinical consequences,” they noted.
This trial was supported by the Canadian Institutes of Health Research, several other Canadian and French government agencies, and Sanquin Blood Supply. Dr. Lacroix reported having no financial disclosures; his associates reported ties to AKPA Pharma, Roche Diagnostics, GlaxoSmithKline, Novartis, and Amgen.
Compared with standard-issue red cells, transfusion of “fresh” red cells stored for fewer than 8 days failed to improve 90-day mortality in a large international study of adult ICU patients, which was reported online April 9 in the New England Journal of Medicine.
“Current regulations permit the storage of red cells for up to 42 days, but prolonged storage has been associated with changes that may render cells ineffective as oxygen carriers and that lead to the accumulation of substances that have untoward biologic effects,” said Dr. Jacques Lacroix of the University of Montreal and his associates.
A recent meta-analysis suggested that transfusion of older red cells was associated with a 16% increase in mortality among critically ill patients, but several randomized trials have failed to document any adverse effects on oxygenation, immunologic, or coagulation factors. Dr. Lacroix and his associates performed the Age of Blood Evaluation (ABLE) study, a prospective, blinded clinical trial involving ICU patients enrolled during a 5-year period at 64 medical centers in Canada, the United Kingdom, France, the Netherlands, and Belgium. A total of 1,211 participants were randomly assigned to receive “fresh” blood stored for an average of 6 days and 1,219 to receive standard blood stored for an average of 22 days – a difference that the investigators deemed statistically and clinically significant.
The primary outcome measure, 90-day all-cause mortality, was 37% in the fresh-blood group and 35% in the standard-blood group, a nonsignificant difference. There also were no significant differences in mortality between the two study groups in any of several subgroup analyses based on patient age; the number of units transfused; baseline APACHE II scores; major comorbidities; duration of respiratory, hemodynamic, or renal support; length of ICU stay; or length of hospital stay, Dr Lacroix and his associates said (N. Engl. J. Med. 2015 April 9 [doi:10.1056/NEJMoa1500704]).
“These findings have important implications for the critical care and blood transfusion communities. We surmise that the use of fresh red cells is not justified at this time. We might also infer that changes to red cells or the storage medium that have been documented in many laboratory studies may have limited clinical consequences,” they noted.
This trial was supported by the Canadian Institutes of Health Research, several other Canadian and French government agencies, and Sanquin Blood Supply. Dr. Lacroix reported having no financial disclosures; his associates reported ties to AKPA Pharma, Roche Diagnostics, GlaxoSmithKline, Novartis, and Amgen.
Compared with standard-issue red cells, transfusion of “fresh” red cells stored for fewer than 8 days failed to improve 90-day mortality in a large international study of adult ICU patients, which was reported online April 9 in the New England Journal of Medicine.
“Current regulations permit the storage of red cells for up to 42 days, but prolonged storage has been associated with changes that may render cells ineffective as oxygen carriers and that lead to the accumulation of substances that have untoward biologic effects,” said Dr. Jacques Lacroix of the University of Montreal and his associates.
A recent meta-analysis suggested that transfusion of older red cells was associated with a 16% increase in mortality among critically ill patients, but several randomized trials have failed to document any adverse effects on oxygenation, immunologic, or coagulation factors. Dr. Lacroix and his associates performed the Age of Blood Evaluation (ABLE) study, a prospective, blinded clinical trial involving ICU patients enrolled during a 5-year period at 64 medical centers in Canada, the United Kingdom, France, the Netherlands, and Belgium. A total of 1,211 participants were randomly assigned to receive “fresh” blood stored for an average of 6 days and 1,219 to receive standard blood stored for an average of 22 days – a difference that the investigators deemed statistically and clinically significant.
The primary outcome measure, 90-day all-cause mortality, was 37% in the fresh-blood group and 35% in the standard-blood group, a nonsignificant difference. There also were no significant differences in mortality between the two study groups in any of several subgroup analyses based on patient age; the number of units transfused; baseline APACHE II scores; major comorbidities; duration of respiratory, hemodynamic, or renal support; length of ICU stay; or length of hospital stay, Dr Lacroix and his associates said (N. Engl. J. Med. 2015 April 9 [doi:10.1056/NEJMoa1500704]).
“These findings have important implications for the critical care and blood transfusion communities. We surmise that the use of fresh red cells is not justified at this time. We might also infer that changes to red cells or the storage medium that have been documented in many laboratory studies may have limited clinical consequences,” they noted.
This trial was supported by the Canadian Institutes of Health Research, several other Canadian and French government agencies, and Sanquin Blood Supply. Dr. Lacroix reported having no financial disclosures; his associates reported ties to AKPA Pharma, Roche Diagnostics, GlaxoSmithKline, Novartis, and Amgen.
Key clinical point: Transfusing “fresher” red blood cells didn’t decrease 90-day mortality in ICU patients, compared with standard transfusions.
Major finding: The primary outcome measure, 90-day all-cause mortality, was 37% in the fresh-blood group and 35% in the standard-blood group.
Data source: A 5-year international, randomized, blinded clinical trial involving 2,430 adult ICU patients.
Disclosures: This trial was supported by the Canadian Institutes of Health Research, several other Canadian and French government agencies, and Sanquin Blood Supply. Dr. Lacroix reported having no financial disclosures; his associates reported ties to AKPA Pharma, Roche Diagnostics, GlaxoSmithKline, Novartis, and Amgen.
Ibrutinib highly active against refractory Waldenstrom’s macroglobulinemia
Ibrutinib proved to be “highly active” against refractory Waldenstrom’s macroglobulinemia in the first clinical trial to assess the agent’s safety and efficacy in this patient population, producing an overall response rate of 90.5% and a major response rate of 73.0% in a series of 63 consecutive patients, according to a report published online April 9 in the New England Journal of Medicine.
Waldenstrom’s macroglobulinemia is a malignant B-cell lymphoma in which whole-genome sequencing has revealed several activating mutations. Ibrutinib – an oral inhibitor of Bruton’s tyrosine kinase (BTK), which is activated in tumor cells by some of these mutations – was found to trigger apoptosis of Waldenstrom’s macroglobulinemia cells in vitro and to show clinical activity in a phase I study. Investigators now report their findings from a prospective, industry-sponsored study of adults enrolled at the Dana-Farber Cancer Institute, Memorial Sloan-Kettering Cancer Center, and Stanford University Medical Center during a 1-year period and followed up for another 18 months.
All the participants had progressive disease at baseline despite receiving previous treatments including monoclonal antibodies, glucocorticoids, proteasome inhibitors, alkylators, immunomodulators, anthracyclines, and experimental therapies. Ibrutinib was taken orally every day for 26 4-week cycles until disease progressed or unacceptable toxic effects developed; treatment responders were permitted to continue the therapy after that time, if they wished, said Dr. Steven P. Treon of the Bing Center for Waldenstrom’s Macroglobulinemia, Dana-Farber Cancer Institute, Boston, and his associates.
The primary objective of the study was to determine the overall rate of any treatment response (it was 90.5%) and the rate of major treatment response, defined as a 50% or greater decline in serum IgM levels (it was 73.0%). In addition, at 24 months, the progression-free survival was 69.1% and the overall survival was 95.2%. In comparison, previous studies of other monotherapies have shown overall response rates of only 40%-80% and median progression-free survival of only 8-20 months, the investigators said (N. Engl. J. Med. 2015 April 9 [doi:10.1056/NEJMoa1501548]).
Treatment response was rapid, with a median onset at 4 weeks, and both serum IgM and hemoglobin levels improved even in patients who showed modest or no changes in bone marrow disease burden. “This suggests that a mechanism other than tumor debulking could contribute to the clinical benefit with ibrutinib,” they added.
On CT imaging, 68% of patients showed decreased or resolved adenopathy and 57% showed decreased splenomegaly. Malignant pleural effusions resolved in two of three patients who had them, and peripheral neuropathy stabilized or improved in all nine who were affected. The latter result is “particularly encouraging given the challenging nature of treating IgM-related peripheral neuropathy in Waldenstrom’s macroglobulinemia,” Dr. Treon and his associates noted.
The toxic effects of treatment were moderate in these heavily pretreated patients and included neutropenia (22% of patients), thrombocytopenia (14%), bleeding events (3%), and reversible atrial fibrillation (5%) in patients with a history of arrhythmia. There were few infections, and no unexpected toxicities occurred, the investigators reported.
This study was supported by Pharmacyclics and Janssen Pharmaceuticals; with additional funding by Peter S. Bing, M.D.; the International Waldenstrom’s Macroglobulinemia Foundation; the Leukemia and Lymphoma Society; the Linda and Edward Nelson Fund for Waldenstrom’s Macroglobulinemia Research; the D’Amato Family Fund for Genomic Discovery; the Coyote Fund; and the Bauman Family Foundation. Dr. Treon reported ties to Pharmacyclics and Janssen; his associates reported ties to several industry sources.
Ibrutinib proved to be “highly active” against refractory Waldenstrom’s macroglobulinemia in the first clinical trial to assess the agent’s safety and efficacy in this patient population, producing an overall response rate of 90.5% and a major response rate of 73.0% in a series of 63 consecutive patients, according to a report published online April 9 in the New England Journal of Medicine.
Waldenstrom’s macroglobulinemia is a malignant B-cell lymphoma in which whole-genome sequencing has revealed several activating mutations. Ibrutinib – an oral inhibitor of Bruton’s tyrosine kinase (BTK), which is activated in tumor cells by some of these mutations – was found to trigger apoptosis of Waldenstrom’s macroglobulinemia cells in vitro and to show clinical activity in a phase I study. Investigators now report their findings from a prospective, industry-sponsored study of adults enrolled at the Dana-Farber Cancer Institute, Memorial Sloan-Kettering Cancer Center, and Stanford University Medical Center during a 1-year period and followed up for another 18 months.
All the participants had progressive disease at baseline despite receiving previous treatments including monoclonal antibodies, glucocorticoids, proteasome inhibitors, alkylators, immunomodulators, anthracyclines, and experimental therapies. Ibrutinib was taken orally every day for 26 4-week cycles until disease progressed or unacceptable toxic effects developed; treatment responders were permitted to continue the therapy after that time, if they wished, said Dr. Steven P. Treon of the Bing Center for Waldenstrom’s Macroglobulinemia, Dana-Farber Cancer Institute, Boston, and his associates.
The primary objective of the study was to determine the overall rate of any treatment response (it was 90.5%) and the rate of major treatment response, defined as a 50% or greater decline in serum IgM levels (it was 73.0%). In addition, at 24 months, the progression-free survival was 69.1% and the overall survival was 95.2%. In comparison, previous studies of other monotherapies have shown overall response rates of only 40%-80% and median progression-free survival of only 8-20 months, the investigators said (N. Engl. J. Med. 2015 April 9 [doi:10.1056/NEJMoa1501548]).
Treatment response was rapid, with a median onset at 4 weeks, and both serum IgM and hemoglobin levels improved even in patients who showed modest or no changes in bone marrow disease burden. “This suggests that a mechanism other than tumor debulking could contribute to the clinical benefit with ibrutinib,” they added.
On CT imaging, 68% of patients showed decreased or resolved adenopathy and 57% showed decreased splenomegaly. Malignant pleural effusions resolved in two of three patients who had them, and peripheral neuropathy stabilized or improved in all nine who were affected. The latter result is “particularly encouraging given the challenging nature of treating IgM-related peripheral neuropathy in Waldenstrom’s macroglobulinemia,” Dr. Treon and his associates noted.
The toxic effects of treatment were moderate in these heavily pretreated patients and included neutropenia (22% of patients), thrombocytopenia (14%), bleeding events (3%), and reversible atrial fibrillation (5%) in patients with a history of arrhythmia. There were few infections, and no unexpected toxicities occurred, the investigators reported.
This study was supported by Pharmacyclics and Janssen Pharmaceuticals; with additional funding by Peter S. Bing, M.D.; the International Waldenstrom’s Macroglobulinemia Foundation; the Leukemia and Lymphoma Society; the Linda and Edward Nelson Fund for Waldenstrom’s Macroglobulinemia Research; the D’Amato Family Fund for Genomic Discovery; the Coyote Fund; and the Bauman Family Foundation. Dr. Treon reported ties to Pharmacyclics and Janssen; his associates reported ties to several industry sources.
Ibrutinib proved to be “highly active” against refractory Waldenstrom’s macroglobulinemia in the first clinical trial to assess the agent’s safety and efficacy in this patient population, producing an overall response rate of 90.5% and a major response rate of 73.0% in a series of 63 consecutive patients, according to a report published online April 9 in the New England Journal of Medicine.
Waldenstrom’s macroglobulinemia is a malignant B-cell lymphoma in which whole-genome sequencing has revealed several activating mutations. Ibrutinib – an oral inhibitor of Bruton’s tyrosine kinase (BTK), which is activated in tumor cells by some of these mutations – was found to trigger apoptosis of Waldenstrom’s macroglobulinemia cells in vitro and to show clinical activity in a phase I study. Investigators now report their findings from a prospective, industry-sponsored study of adults enrolled at the Dana-Farber Cancer Institute, Memorial Sloan-Kettering Cancer Center, and Stanford University Medical Center during a 1-year period and followed up for another 18 months.
All the participants had progressive disease at baseline despite receiving previous treatments including monoclonal antibodies, glucocorticoids, proteasome inhibitors, alkylators, immunomodulators, anthracyclines, and experimental therapies. Ibrutinib was taken orally every day for 26 4-week cycles until disease progressed or unacceptable toxic effects developed; treatment responders were permitted to continue the therapy after that time, if they wished, said Dr. Steven P. Treon of the Bing Center for Waldenstrom’s Macroglobulinemia, Dana-Farber Cancer Institute, Boston, and his associates.
The primary objective of the study was to determine the overall rate of any treatment response (it was 90.5%) and the rate of major treatment response, defined as a 50% or greater decline in serum IgM levels (it was 73.0%). In addition, at 24 months, the progression-free survival was 69.1% and the overall survival was 95.2%. In comparison, previous studies of other monotherapies have shown overall response rates of only 40%-80% and median progression-free survival of only 8-20 months, the investigators said (N. Engl. J. Med. 2015 April 9 [doi:10.1056/NEJMoa1501548]).
Treatment response was rapid, with a median onset at 4 weeks, and both serum IgM and hemoglobin levels improved even in patients who showed modest or no changes in bone marrow disease burden. “This suggests that a mechanism other than tumor debulking could contribute to the clinical benefit with ibrutinib,” they added.
On CT imaging, 68% of patients showed decreased or resolved adenopathy and 57% showed decreased splenomegaly. Malignant pleural effusions resolved in two of three patients who had them, and peripheral neuropathy stabilized or improved in all nine who were affected. The latter result is “particularly encouraging given the challenging nature of treating IgM-related peripheral neuropathy in Waldenstrom’s macroglobulinemia,” Dr. Treon and his associates noted.
The toxic effects of treatment were moderate in these heavily pretreated patients and included neutropenia (22% of patients), thrombocytopenia (14%), bleeding events (3%), and reversible atrial fibrillation (5%) in patients with a history of arrhythmia. There were few infections, and no unexpected toxicities occurred, the investigators reported.
This study was supported by Pharmacyclics and Janssen Pharmaceuticals; with additional funding by Peter S. Bing, M.D.; the International Waldenstrom’s Macroglobulinemia Foundation; the Leukemia and Lymphoma Society; the Linda and Edward Nelson Fund for Waldenstrom’s Macroglobulinemia Research; the D’Amato Family Fund for Genomic Discovery; the Coyote Fund; and the Bauman Family Foundation. Dr. Treon reported ties to Pharmacyclics and Janssen; his associates reported ties to several industry sources.
Key clinical point: Ibrutinib produced a 90.5% overall response rate and a 73% major response rate in a proof-of-concept trial of 63 patients with refractory Waldenstrom’s macroglobulinemia, a malignant B-cell lymphoma.
Major finding: At 24 months, progression-free survival was 69.1% and overall survival was 95.2%.
Data source: An industry-sponsored prospective multicenter study.
Disclosures: This study was supported by Pharmacyclics and Janssen Pharmaceuticals; with additional funding by Peter S. Bing, M.D.; the International Waldenstrom’s Macroglobulinemia Foundation; the Leukemia and Lymphoma Society; the Linda and Edward Nelson Fund for Waldenstrom’s Macroglobulinemia Research; the D’Amato Family Fund for Genomic Discovery; the Coyote Fund; and the Bauman Family Foundation. Dr. Treon reported ties to Pharmacyclics and Janssen; his associates reported ties to several industry sources.
Type, location of BRCA mutations influence risk
Among women who carry BRCA1 or BRCA2 mutations, the type and exact location of the mutation influences the risk it confers for breast and ovarian cancer, according to a report published online April 7 in JAMA.
Investigators examined differences in cancer risks by analyzing data in the Consortium of Investigators of Modifiers of BRCA (CIMBA), a collection of clinical and genetic information for carriers of disease-associated BRCA mutations in 33 countries.
For this study, data were assessed for 19,581 women with BRCA1 mutations and 11,900 women with BRCA2 mutations for whom there was sufficient information to estimate hazard ratios. The types of mutations included nonsense, frame shift, in-frame, missense, splicing, rearrangement, premature termination codons, and nonsense-mediated decay mutations, said Timothy R. Rebbeck, Ph.D., of Abramson Cancer Center and the Center for Clinical Epidemiology and Biostatistics at the University of Pennsylvania, Philadelphia, and his associates.
Among the study participants with BRCA1 mutations, 9,052 women (46%) developed breast cancer, 2,317 (12%) developed ovarian cancer, and 1,041 (5%) developed both breast and ovarian cancer. Among the women with BRCA2 mutations, 6,180 (52%) developed breast cancer, 682 (6%) developed ovarian cancer, and 272 (2%) developed both breast and ovarian cancer. A woman’s risk for cancer differed significantly according to the type of BRCA1 or BRCA2 mutation she carried and according to the location of the mutation on the nucleotide, the investigators said (JAMA 2015 April 7 [doi:10.1001/jama.2014.5985]).
Further research is needed to determine the absolute risks of cancer associated with each mutation and “to better understand what level of risk difference will change decision-making and standards of care, such as preventive surgery” for BRCA1 and BRCA2 carriers, Dr. Rebbeck and his associates added.
This study was funded primarily by Cancer Research UK and also was supported by the U.S. National Institutes of Health, the Basser Research Center at the University of Pennsylvania, the Breast Cancer Research Foundation, and the Rooney Family Foundation. Dr. Rebbeck reported having no financial disclosures; his associates reported numerous ties to industry sources.
Among women who carry BRCA1 or BRCA2 mutations, the type and exact location of the mutation influences the risk it confers for breast and ovarian cancer, according to a report published online April 7 in JAMA.
Investigators examined differences in cancer risks by analyzing data in the Consortium of Investigators of Modifiers of BRCA (CIMBA), a collection of clinical and genetic information for carriers of disease-associated BRCA mutations in 33 countries.
For this study, data were assessed for 19,581 women with BRCA1 mutations and 11,900 women with BRCA2 mutations for whom there was sufficient information to estimate hazard ratios. The types of mutations included nonsense, frame shift, in-frame, missense, splicing, rearrangement, premature termination codons, and nonsense-mediated decay mutations, said Timothy R. Rebbeck, Ph.D., of Abramson Cancer Center and the Center for Clinical Epidemiology and Biostatistics at the University of Pennsylvania, Philadelphia, and his associates.
Among the study participants with BRCA1 mutations, 9,052 women (46%) developed breast cancer, 2,317 (12%) developed ovarian cancer, and 1,041 (5%) developed both breast and ovarian cancer. Among the women with BRCA2 mutations, 6,180 (52%) developed breast cancer, 682 (6%) developed ovarian cancer, and 272 (2%) developed both breast and ovarian cancer. A woman’s risk for cancer differed significantly according to the type of BRCA1 or BRCA2 mutation she carried and according to the location of the mutation on the nucleotide, the investigators said (JAMA 2015 April 7 [doi:10.1001/jama.2014.5985]).
Further research is needed to determine the absolute risks of cancer associated with each mutation and “to better understand what level of risk difference will change decision-making and standards of care, such as preventive surgery” for BRCA1 and BRCA2 carriers, Dr. Rebbeck and his associates added.
This study was funded primarily by Cancer Research UK and also was supported by the U.S. National Institutes of Health, the Basser Research Center at the University of Pennsylvania, the Breast Cancer Research Foundation, and the Rooney Family Foundation. Dr. Rebbeck reported having no financial disclosures; his associates reported numerous ties to industry sources.
Among women who carry BRCA1 or BRCA2 mutations, the type and exact location of the mutation influences the risk it confers for breast and ovarian cancer, according to a report published online April 7 in JAMA.
Investigators examined differences in cancer risks by analyzing data in the Consortium of Investigators of Modifiers of BRCA (CIMBA), a collection of clinical and genetic information for carriers of disease-associated BRCA mutations in 33 countries.
For this study, data were assessed for 19,581 women with BRCA1 mutations and 11,900 women with BRCA2 mutations for whom there was sufficient information to estimate hazard ratios. The types of mutations included nonsense, frame shift, in-frame, missense, splicing, rearrangement, premature termination codons, and nonsense-mediated decay mutations, said Timothy R. Rebbeck, Ph.D., of Abramson Cancer Center and the Center for Clinical Epidemiology and Biostatistics at the University of Pennsylvania, Philadelphia, and his associates.
Among the study participants with BRCA1 mutations, 9,052 women (46%) developed breast cancer, 2,317 (12%) developed ovarian cancer, and 1,041 (5%) developed both breast and ovarian cancer. Among the women with BRCA2 mutations, 6,180 (52%) developed breast cancer, 682 (6%) developed ovarian cancer, and 272 (2%) developed both breast and ovarian cancer. A woman’s risk for cancer differed significantly according to the type of BRCA1 or BRCA2 mutation she carried and according to the location of the mutation on the nucleotide, the investigators said (JAMA 2015 April 7 [doi:10.1001/jama.2014.5985]).
Further research is needed to determine the absolute risks of cancer associated with each mutation and “to better understand what level of risk difference will change decision-making and standards of care, such as preventive surgery” for BRCA1 and BRCA2 carriers, Dr. Rebbeck and his associates added.
This study was funded primarily by Cancer Research UK and also was supported by the U.S. National Institutes of Health, the Basser Research Center at the University of Pennsylvania, the Breast Cancer Research Foundation, and the Rooney Family Foundation. Dr. Rebbeck reported having no financial disclosures; his associates reported numerous ties to industry sources.
FROM JAMA
Key clinical point: The type and exact location of BRCA1 and BRCA2 mutations affect the risk they confer for breast and ovarian cancer.
Major finding: Among the study participants with BRCA1 mutations, 46% developed breast cancer, 12% developed ovarian cancer, and 5% developed both breast and ovarian cancer; among those with BRCA2 mutations, 52% developed breast cancer, 6% developed ovarian cancer, and 2% developed both breast and ovarian cancer.
Data source: An observational analysis of cancer risks among 31,481 women in an international database of carriers of any deleterious BRCA mutations.
Disclosures: This study was funded primarily by Cancer Research UK and also was supported by the U.S. National Institutes of Health, the Basser Research Center at the University of Pennsylvania, the Breast Cancer Research Foundation, and the Rooney Family Foundation. Dr. Rebbeck reported having no financial disclosures; his associates reported numerous ties to industry sources.
Not enough data on commercial weight-loss programs
Current evidence supports the efficacy of only 2 of the 141 commercial or proprietary weight-loss programs available in the United States: Weight Watchers and Jenny Craig, according to a report published online April 6 in Annals of Internal Medicine.
Physicians are increasingly called upon to refer patients to high-intensity weight-loss programs, given provisions in the Affordable Care Act and a recent joint clinical practice guideline from the American Heart Association, the American College of Cardiology, and the Obesity Society. But there are no recommendations about the relative merits of such programs. To help clinicians assess their efficacy, investigators performed a comprehensive review of the literature.
They included only programs that stressed nutrition and behavioral counseling or social support, with or without a physical activity component, because these elements have been identified as essential to weight loss. This excluded popular programs such as Ornish and Zone, and winnowed the mass of evaluable weight-loss programs to 32. Further restricting their analysis to randomized clinical trials of at least 12 weeks’ duration excluded programs such as South Beach and Ideal Protein, and reduced the analysis to 11 programs assessed in 45 studies, said Dr. Kimberly A. Gudzune, of Johns Hopkins University, Baltimore, and her associates.
The primary efficacy outcome was mean percentage of weight loss at 1 year, compared with control conditions. Pooled results from six trials showed Weight Watchers resulted in a 2.6% greater weight loss, and pooled results from three trials showed Jenny Craig resulted in a 4.9% greater weight loss. NutriSystem showed “promising” short-term results, but no studies assessed its efficacy beyond the 3-month mark. The data on all other programs, including Medifast, SlimFast, HMR, Optifast, Atkins, Biggest Loser Club, eDiets, and Lose It!, were either insufficient or of questionable quality, the investigators said (Ann. Intern. Med. 2015 April 6 [doi:10.7326/M14-2238]).
“Given these findings, it may be reasonable for clinicians to refer patients to Weight Watchers or Jenny Craig, especially if they lack the time, training, or ancillary staff to deliver behavioral counseling in their practices,” Dr. Gudzune and her associates said.
Even with “effective” weight-loss programs, the total loss usually is modest and well below patients’ expectations.
It is not clear yet whether patients will adhere to dietary restrictions, sustain their behavioral changes, and absorb the sometimes-heavy financial cost of these programs when they stand to lose only 2%-5% of their total weight.
Dr. Christina C. Wee is at Beth Israel Deaconess Medical Center and Harvard Medical School, Boston. She is supported by a National Institutes of Health award; her financial disclosures are available at www.acpoline.org These remarks are exerpted from an editorial accompanying Dr. Gudzune’s report (Ann. Intern. Med. 2015 April 6 [doi:10.7326/M15-0429]).
Even with “effective” weight-loss programs, the total loss usually is modest and well below patients’ expectations.
It is not clear yet whether patients will adhere to dietary restrictions, sustain their behavioral changes, and absorb the sometimes-heavy financial cost of these programs when they stand to lose only 2%-5% of their total weight.
Dr. Christina C. Wee is at Beth Israel Deaconess Medical Center and Harvard Medical School, Boston. She is supported by a National Institutes of Health award; her financial disclosures are available at www.acpoline.org These remarks are exerpted from an editorial accompanying Dr. Gudzune’s report (Ann. Intern. Med. 2015 April 6 [doi:10.7326/M15-0429]).
Even with “effective” weight-loss programs, the total loss usually is modest and well below patients’ expectations.
It is not clear yet whether patients will adhere to dietary restrictions, sustain their behavioral changes, and absorb the sometimes-heavy financial cost of these programs when they stand to lose only 2%-5% of their total weight.
Dr. Christina C. Wee is at Beth Israel Deaconess Medical Center and Harvard Medical School, Boston. She is supported by a National Institutes of Health award; her financial disclosures are available at www.acpoline.org These remarks are exerpted from an editorial accompanying Dr. Gudzune’s report (Ann. Intern. Med. 2015 April 6 [doi:10.7326/M15-0429]).
Current evidence supports the efficacy of only 2 of the 141 commercial or proprietary weight-loss programs available in the United States: Weight Watchers and Jenny Craig, according to a report published online April 6 in Annals of Internal Medicine.
Physicians are increasingly called upon to refer patients to high-intensity weight-loss programs, given provisions in the Affordable Care Act and a recent joint clinical practice guideline from the American Heart Association, the American College of Cardiology, and the Obesity Society. But there are no recommendations about the relative merits of such programs. To help clinicians assess their efficacy, investigators performed a comprehensive review of the literature.
They included only programs that stressed nutrition and behavioral counseling or social support, with or without a physical activity component, because these elements have been identified as essential to weight loss. This excluded popular programs such as Ornish and Zone, and winnowed the mass of evaluable weight-loss programs to 32. Further restricting their analysis to randomized clinical trials of at least 12 weeks’ duration excluded programs such as South Beach and Ideal Protein, and reduced the analysis to 11 programs assessed in 45 studies, said Dr. Kimberly A. Gudzune, of Johns Hopkins University, Baltimore, and her associates.
The primary efficacy outcome was mean percentage of weight loss at 1 year, compared with control conditions. Pooled results from six trials showed Weight Watchers resulted in a 2.6% greater weight loss, and pooled results from three trials showed Jenny Craig resulted in a 4.9% greater weight loss. NutriSystem showed “promising” short-term results, but no studies assessed its efficacy beyond the 3-month mark. The data on all other programs, including Medifast, SlimFast, HMR, Optifast, Atkins, Biggest Loser Club, eDiets, and Lose It!, were either insufficient or of questionable quality, the investigators said (Ann. Intern. Med. 2015 April 6 [doi:10.7326/M14-2238]).
“Given these findings, it may be reasonable for clinicians to refer patients to Weight Watchers or Jenny Craig, especially if they lack the time, training, or ancillary staff to deliver behavioral counseling in their practices,” Dr. Gudzune and her associates said.
Current evidence supports the efficacy of only 2 of the 141 commercial or proprietary weight-loss programs available in the United States: Weight Watchers and Jenny Craig, according to a report published online April 6 in Annals of Internal Medicine.
Physicians are increasingly called upon to refer patients to high-intensity weight-loss programs, given provisions in the Affordable Care Act and a recent joint clinical practice guideline from the American Heart Association, the American College of Cardiology, and the Obesity Society. But there are no recommendations about the relative merits of such programs. To help clinicians assess their efficacy, investigators performed a comprehensive review of the literature.
They included only programs that stressed nutrition and behavioral counseling or social support, with or without a physical activity component, because these elements have been identified as essential to weight loss. This excluded popular programs such as Ornish and Zone, and winnowed the mass of evaluable weight-loss programs to 32. Further restricting their analysis to randomized clinical trials of at least 12 weeks’ duration excluded programs such as South Beach and Ideal Protein, and reduced the analysis to 11 programs assessed in 45 studies, said Dr. Kimberly A. Gudzune, of Johns Hopkins University, Baltimore, and her associates.
The primary efficacy outcome was mean percentage of weight loss at 1 year, compared with control conditions. Pooled results from six trials showed Weight Watchers resulted in a 2.6% greater weight loss, and pooled results from three trials showed Jenny Craig resulted in a 4.9% greater weight loss. NutriSystem showed “promising” short-term results, but no studies assessed its efficacy beyond the 3-month mark. The data on all other programs, including Medifast, SlimFast, HMR, Optifast, Atkins, Biggest Loser Club, eDiets, and Lose It!, were either insufficient or of questionable quality, the investigators said (Ann. Intern. Med. 2015 April 6 [doi:10.7326/M14-2238]).
“Given these findings, it may be reasonable for clinicians to refer patients to Weight Watchers or Jenny Craig, especially if they lack the time, training, or ancillary staff to deliver behavioral counseling in their practices,” Dr. Gudzune and her associates said.
Key clinical point: Evidence supports the efficacy of only 2 of 141 available commercial weight-loss programs, Weight Watchers and Jenny Craig.
Major finding: Pooled results from six trials showed Weight Watchers resulted in a 2.6% greater weight loss than did control conditions, and pooled results from three trials showed Jenny Craig resulted in a 4.9% greater weight loss.
Data source: A comprehensive review of the literature and pooled analysis of data from 45 trials of 11 commercial weight-loss programs.
Disclosures: This study received no funding; Dr. Gudzune and her associates are supported by the National Heart, Lung, and Blood Institute, the National Institute of Diabetes and Digestive and Kidney Diseases, Johns Hopkins University, the University of Maryland, and Robert Wood Johnson Medical School, New Brunswick. They reported having no financial disclosures.
Nursing home residents have poor outcomes after lower-extremity revascularization
A substantial number of nursing home residents undergo lower-extremity revascularization each year, but very few of them gain any function and approximately half die within the year, according to a report published online April 6 in JAMA Internal Medicine.
In a population-based analysis of Medicare claims and a database that tracks virtually all U.S. nursing homes, 82% of residents who underwent the procedure during a 3-year period had either died or were unable to walk a year afterward. Most showed a clinically significant decline in function within 3 months of having the procedure, said Dr. Lawrence Oresanya of the department of surgery, University of California, San Francisco, and his associates.
“Our findings can inform conversations between physicians, patients, and families about the risks and expected outcomes of surgery and whether the surgery is likely to be worthwhile. Our findings also highlight the importance of carefully considering a prognosis independent of vascular disease and assessing the goals of care. Ambulatory function … may be impossible to attain,” they wrote.
Lower-extremity revascularization is usually performed to maintain elderly patients’ functional independence by preserving their limbs. But a closer examination of these procedures is warranted in the nursing home population “because nursing home residents, in general, have high levels of functional dependence unrelated to peripheral arterial disease, and higher rates of mortality after most invasive procedures,” the investigators said.
Dr. Oresanya and his colleagues identified 10,784 nursing home residents across the country who underwent lower-extremity revascularization. The procedure was elective in 67% of cases and emergent or urgent in 33%. An endovascular approach was used in 56%, and an open approach in the remainder, with the endovacular approach being more associated with clinical success than open surgery.
The mean patient age was 82 years, and serious comorbidities were very common: 60% had cognitive impairment, 57% had heart failure, and 29% had renal failure. Three-fourths of the patients were nonambulatory at the time of surgery.
The investigators assumed that most patients in this setting had critical limb ischemia rather than claudication. They did not have information about the severity of the lower-extremity ischemia, or about the prevalence or duration of nonhealing wounds or gangrene.
One year after lower-extremity revascularization, mortality was 51% among ambulatory patients and 53% among nonambulatory patients. Only 13% of the entire cohort were able to walk, and only 18% had maintained or improved their presurgical functional status. “Revascularization rarely allowed a nonambulatory resident to become ambulatory,” Dr. Oresanya and his associates wrote (JAMA Intern. Med. 2015 April 6 [doi:10.1001/jamainternmed.2015.0486]).
The researchers were unable to determine whether these poor outcomes resulted from the surgery itself or were due to these patients’ “insufficient physiologic reserve.”
They also cautioned that they confined their study strictly to functional outcomes of lower-extremity revascularization, namely ambulation and mortality. Some patients may have derived other benefits from the procedure, such as relief of pain, healing of wounds, and avoidance of major amputation.
The authors reported having no relevant financial disclosures.
The findings of Oresanya et al. are balanced and valuable, even though the data didn’t give them specific clinical information such as the indications for revascularization and were insensitive to subtle issues such as patient and family wishes for level of care. Such studies point the way to a more rational clinical approach to the care of frail elders with a limited life span but with the prospect of constant pain and discomfort.
But it is important to note that most of the procedures in this study likely were performed to relieve symptoms of ischemic leg pain, nonhealing wounds, or worsening gangrene. In this setting, the surgery should be viewed as a palliative measure rather than as a definitive therapeutic procedure to extend ambulatory function.
William J. Hall, M.D., is at the University of Rochester, New York. He reported having no relevant financial disclosures. Dr. Hall made these remarks in an invited commentary accompanying Dr. Oresanya’s report (JAMA Intern. Med. 2015 April 6 [doi:10.1001/jamainternmed.2015.32]).
The findings of Oresanya et al. are balanced and valuable, even though the data didn’t give them specific clinical information such as the indications for revascularization and were insensitive to subtle issues such as patient and family wishes for level of care. Such studies point the way to a more rational clinical approach to the care of frail elders with a limited life span but with the prospect of constant pain and discomfort.
But it is important to note that most of the procedures in this study likely were performed to relieve symptoms of ischemic leg pain, nonhealing wounds, or worsening gangrene. In this setting, the surgery should be viewed as a palliative measure rather than as a definitive therapeutic procedure to extend ambulatory function.
William J. Hall, M.D., is at the University of Rochester, New York. He reported having no relevant financial disclosures. Dr. Hall made these remarks in an invited commentary accompanying Dr. Oresanya’s report (JAMA Intern. Med. 2015 April 6 [doi:10.1001/jamainternmed.2015.32]).
The findings of Oresanya et al. are balanced and valuable, even though the data didn’t give them specific clinical information such as the indications for revascularization and were insensitive to subtle issues such as patient and family wishes for level of care. Such studies point the way to a more rational clinical approach to the care of frail elders with a limited life span but with the prospect of constant pain and discomfort.
But it is important to note that most of the procedures in this study likely were performed to relieve symptoms of ischemic leg pain, nonhealing wounds, or worsening gangrene. In this setting, the surgery should be viewed as a palliative measure rather than as a definitive therapeutic procedure to extend ambulatory function.
William J. Hall, M.D., is at the University of Rochester, New York. He reported having no relevant financial disclosures. Dr. Hall made these remarks in an invited commentary accompanying Dr. Oresanya’s report (JAMA Intern. Med. 2015 April 6 [doi:10.1001/jamainternmed.2015.32]).
A substantial number of nursing home residents undergo lower-extremity revascularization each year, but very few of them gain any function and approximately half die within the year, according to a report published online April 6 in JAMA Internal Medicine.
In a population-based analysis of Medicare claims and a database that tracks virtually all U.S. nursing homes, 82% of residents who underwent the procedure during a 3-year period had either died or were unable to walk a year afterward. Most showed a clinically significant decline in function within 3 months of having the procedure, said Dr. Lawrence Oresanya of the department of surgery, University of California, San Francisco, and his associates.
“Our findings can inform conversations between physicians, patients, and families about the risks and expected outcomes of surgery and whether the surgery is likely to be worthwhile. Our findings also highlight the importance of carefully considering a prognosis independent of vascular disease and assessing the goals of care. Ambulatory function … may be impossible to attain,” they wrote.
Lower-extremity revascularization is usually performed to maintain elderly patients’ functional independence by preserving their limbs. But a closer examination of these procedures is warranted in the nursing home population “because nursing home residents, in general, have high levels of functional dependence unrelated to peripheral arterial disease, and higher rates of mortality after most invasive procedures,” the investigators said.
Dr. Oresanya and his colleagues identified 10,784 nursing home residents across the country who underwent lower-extremity revascularization. The procedure was elective in 67% of cases and emergent or urgent in 33%. An endovascular approach was used in 56%, and an open approach in the remainder, with the endovacular approach being more associated with clinical success than open surgery.
The mean patient age was 82 years, and serious comorbidities were very common: 60% had cognitive impairment, 57% had heart failure, and 29% had renal failure. Three-fourths of the patients were nonambulatory at the time of surgery.
The investigators assumed that most patients in this setting had critical limb ischemia rather than claudication. They did not have information about the severity of the lower-extremity ischemia, or about the prevalence or duration of nonhealing wounds or gangrene.
One year after lower-extremity revascularization, mortality was 51% among ambulatory patients and 53% among nonambulatory patients. Only 13% of the entire cohort were able to walk, and only 18% had maintained or improved their presurgical functional status. “Revascularization rarely allowed a nonambulatory resident to become ambulatory,” Dr. Oresanya and his associates wrote (JAMA Intern. Med. 2015 April 6 [doi:10.1001/jamainternmed.2015.0486]).
The researchers were unable to determine whether these poor outcomes resulted from the surgery itself or were due to these patients’ “insufficient physiologic reserve.”
They also cautioned that they confined their study strictly to functional outcomes of lower-extremity revascularization, namely ambulation and mortality. Some patients may have derived other benefits from the procedure, such as relief of pain, healing of wounds, and avoidance of major amputation.
The authors reported having no relevant financial disclosures.
A substantial number of nursing home residents undergo lower-extremity revascularization each year, but very few of them gain any function and approximately half die within the year, according to a report published online April 6 in JAMA Internal Medicine.
In a population-based analysis of Medicare claims and a database that tracks virtually all U.S. nursing homes, 82% of residents who underwent the procedure during a 3-year period had either died or were unable to walk a year afterward. Most showed a clinically significant decline in function within 3 months of having the procedure, said Dr. Lawrence Oresanya of the department of surgery, University of California, San Francisco, and his associates.
“Our findings can inform conversations between physicians, patients, and families about the risks and expected outcomes of surgery and whether the surgery is likely to be worthwhile. Our findings also highlight the importance of carefully considering a prognosis independent of vascular disease and assessing the goals of care. Ambulatory function … may be impossible to attain,” they wrote.
Lower-extremity revascularization is usually performed to maintain elderly patients’ functional independence by preserving their limbs. But a closer examination of these procedures is warranted in the nursing home population “because nursing home residents, in general, have high levels of functional dependence unrelated to peripheral arterial disease, and higher rates of mortality after most invasive procedures,” the investigators said.
Dr. Oresanya and his colleagues identified 10,784 nursing home residents across the country who underwent lower-extremity revascularization. The procedure was elective in 67% of cases and emergent or urgent in 33%. An endovascular approach was used in 56%, and an open approach in the remainder, with the endovacular approach being more associated with clinical success than open surgery.
The mean patient age was 82 years, and serious comorbidities were very common: 60% had cognitive impairment, 57% had heart failure, and 29% had renal failure. Three-fourths of the patients were nonambulatory at the time of surgery.
The investigators assumed that most patients in this setting had critical limb ischemia rather than claudication. They did not have information about the severity of the lower-extremity ischemia, or about the prevalence or duration of nonhealing wounds or gangrene.
One year after lower-extremity revascularization, mortality was 51% among ambulatory patients and 53% among nonambulatory patients. Only 13% of the entire cohort were able to walk, and only 18% had maintained or improved their presurgical functional status. “Revascularization rarely allowed a nonambulatory resident to become ambulatory,” Dr. Oresanya and his associates wrote (JAMA Intern. Med. 2015 April 6 [doi:10.1001/jamainternmed.2015.0486]).
The researchers were unable to determine whether these poor outcomes resulted from the surgery itself or were due to these patients’ “insufficient physiologic reserve.”
They also cautioned that they confined their study strictly to functional outcomes of lower-extremity revascularization, namely ambulation and mortality. Some patients may have derived other benefits from the procedure, such as relief of pain, healing of wounds, and avoidance of major amputation.
The authors reported having no relevant financial disclosures.
FROM JAMA INTERNAL MEDICINE
Key clinical point: Many nursing home residents undergo lower-extremity revascularization every year, but few survive and are ambulatory 1 year later.
Major finding: One year after lower-extremity revascularization, mortality was approximately 50%, only 13% of the entire cohort were able to walk, and only 18% had maintained or improved their presurgical functional status.
Data source: A population-based cohort study involving almost all (10,784) U.S. nursing home residents who had lower-extremity revascularization in 2005-2008 and were followed for 1 year.
Disclosures: This study was supported in part by the National Institute on Aging and the University of California, San Francisco, Claude D. Pepper Older Americans Independence Center. Dr. Oresanya and his associates reported having no relevant financial disclosures.
Beta-lactam monotherapy effective for suspected community-acquired pneumonia
Among adults suspected of having community-acquired pneumonia who are hospitalized in non-ICU wards, empirical treatment with beta-lactam monotherapy is noninferior both to beta-lactam plus macrolide combination therapy and to fluoroquinolone monotherapy, according to a report published online April 2 in the New England Journal of Medicine.
Current guidelines recommend the latter two approaches, which has caused a widespread increase in the use of macrolides and fluoroquinolones – and in turn has increased antibiotic resistance.
Moreover, “the evidence in support of these recommendations is limited,” said Dr. Douwe F. Postma of the Julius Center for Health Sciences and Primary Care and the University of Utrecht (the Netherlands), and his associates.
To compare outcomes among the three treatment strategies, Dr. Postma and his colleagues conducted the Community-Acquired Pneumonia – Study on the Initial Treatment with Antibiotics of Lower Respiratory Tract Infections (CAP-START) trial in seven Dutch hospitals during a 2.5-year period (N. Engl. J. Med. 2015;372:1312-23).
The cluster-randomized, crossover study called for participating hospitals to rotate using each of the empirical strategies during consecutive 4-month periods for all eligible patients. A total of 656 patients were assigned to receive beta-lactam monotherapy, 739 to receive beta-lactam plus macrolide combination therapy, and 888 to receive fluoroquinolone monotherapy. The median patient age was 70 years.
The primary outcome – all-cause mortality at 90 days after admission – favored beta-lactam monotherapy over the combination therapy by an absolute difference in adjusted risk of death of 1.9 percentage points, and favored beta-lactam monotherapy over fluoroquinolone monotherapy by less than 1 percentage point. That demonstrated the noninferiority of beta-lactam monotherapy, the researchers noted.
Both secondary outcomes – length of hospital stay and treatment-related complications – also were similar among the three study groups, the investigators added.
That noninferiority was confirmed in several further analyses of the data, including a sensitivity analysis restricted only to patients who had radiologically confirmed CAP and another sensitivity analysis that examined 30-day all-cause mortality.
“These findings, together with the slightly longer length of hospital stay with [macrolide monotherapy], reported associations with the development of resistance, and possible increased risk of cardiac events, indicate that the addition of macrolides for empirical treatment of CAP should be reconsidered,” Dr. Postma and his associates said.
The Netherlands Organization for Health Research and Development supported the study. Dr. Postma and his associates reported having no financial disclosures.
Among adults suspected of having community-acquired pneumonia who are hospitalized in non-ICU wards, empirical treatment with beta-lactam monotherapy is noninferior both to beta-lactam plus macrolide combination therapy and to fluoroquinolone monotherapy, according to a report published online April 2 in the New England Journal of Medicine.
Current guidelines recommend the latter two approaches, which has caused a widespread increase in the use of macrolides and fluoroquinolones – and in turn has increased antibiotic resistance.
Moreover, “the evidence in support of these recommendations is limited,” said Dr. Douwe F. Postma of the Julius Center for Health Sciences and Primary Care and the University of Utrecht (the Netherlands), and his associates.
To compare outcomes among the three treatment strategies, Dr. Postma and his colleagues conducted the Community-Acquired Pneumonia – Study on the Initial Treatment with Antibiotics of Lower Respiratory Tract Infections (CAP-START) trial in seven Dutch hospitals during a 2.5-year period (N. Engl. J. Med. 2015;372:1312-23).
The cluster-randomized, crossover study called for participating hospitals to rotate using each of the empirical strategies during consecutive 4-month periods for all eligible patients. A total of 656 patients were assigned to receive beta-lactam monotherapy, 739 to receive beta-lactam plus macrolide combination therapy, and 888 to receive fluoroquinolone monotherapy. The median patient age was 70 years.
The primary outcome – all-cause mortality at 90 days after admission – favored beta-lactam monotherapy over the combination therapy by an absolute difference in adjusted risk of death of 1.9 percentage points, and favored beta-lactam monotherapy over fluoroquinolone monotherapy by less than 1 percentage point. That demonstrated the noninferiority of beta-lactam monotherapy, the researchers noted.
Both secondary outcomes – length of hospital stay and treatment-related complications – also were similar among the three study groups, the investigators added.
That noninferiority was confirmed in several further analyses of the data, including a sensitivity analysis restricted only to patients who had radiologically confirmed CAP and another sensitivity analysis that examined 30-day all-cause mortality.
“These findings, together with the slightly longer length of hospital stay with [macrolide monotherapy], reported associations with the development of resistance, and possible increased risk of cardiac events, indicate that the addition of macrolides for empirical treatment of CAP should be reconsidered,” Dr. Postma and his associates said.
The Netherlands Organization for Health Research and Development supported the study. Dr. Postma and his associates reported having no financial disclosures.
Among adults suspected of having community-acquired pneumonia who are hospitalized in non-ICU wards, empirical treatment with beta-lactam monotherapy is noninferior both to beta-lactam plus macrolide combination therapy and to fluoroquinolone monotherapy, according to a report published online April 2 in the New England Journal of Medicine.
Current guidelines recommend the latter two approaches, which has caused a widespread increase in the use of macrolides and fluoroquinolones – and in turn has increased antibiotic resistance.
Moreover, “the evidence in support of these recommendations is limited,” said Dr. Douwe F. Postma of the Julius Center for Health Sciences and Primary Care and the University of Utrecht (the Netherlands), and his associates.
To compare outcomes among the three treatment strategies, Dr. Postma and his colleagues conducted the Community-Acquired Pneumonia – Study on the Initial Treatment with Antibiotics of Lower Respiratory Tract Infections (CAP-START) trial in seven Dutch hospitals during a 2.5-year period (N. Engl. J. Med. 2015;372:1312-23).
The cluster-randomized, crossover study called for participating hospitals to rotate using each of the empirical strategies during consecutive 4-month periods for all eligible patients. A total of 656 patients were assigned to receive beta-lactam monotherapy, 739 to receive beta-lactam plus macrolide combination therapy, and 888 to receive fluoroquinolone monotherapy. The median patient age was 70 years.
The primary outcome – all-cause mortality at 90 days after admission – favored beta-lactam monotherapy over the combination therapy by an absolute difference in adjusted risk of death of 1.9 percentage points, and favored beta-lactam monotherapy over fluoroquinolone monotherapy by less than 1 percentage point. That demonstrated the noninferiority of beta-lactam monotherapy, the researchers noted.
Both secondary outcomes – length of hospital stay and treatment-related complications – also were similar among the three study groups, the investigators added.
That noninferiority was confirmed in several further analyses of the data, including a sensitivity analysis restricted only to patients who had radiologically confirmed CAP and another sensitivity analysis that examined 30-day all-cause mortality.
“These findings, together with the slightly longer length of hospital stay with [macrolide monotherapy], reported associations with the development of resistance, and possible increased risk of cardiac events, indicate that the addition of macrolides for empirical treatment of CAP should be reconsidered,” Dr. Postma and his associates said.
The Netherlands Organization for Health Research and Development supported the study. Dr. Postma and his associates reported having no financial disclosures.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Key clinical point: Empirical beta-lactam monotherapy is noninferior to recommended treatments for suspected community-acquired pneumonia.
Major finding: The primary outcome – all-cause mortality at 90 days after admission – favored beta-lactam monotherapy over beta-lactam plus macrolide combination therapy and macrolide monotherapy.
Data source: A multicenter, cluster-randomized, crossover trial comparing 90-day outcomes after three different empirical antibiotic therapies in 2,283 adults suspected of having community-acquired pneumonia.
Disclosures: The Netherlands Organization for Health Research and Development supported the study. Dr. Postma and his associates reported having no financial disclosures.
Laparoscopic ‘noninferior’ to open approach for rectal cancer
Laparoscopic resection of rectal cancer is noninferior to open surgery in preventing locoregional recurrence and in improving overall and disease-free survival, according to a report published online April 1 in the New England Journal of Medicine.
The laparoscopic approach has increasingly replaced open surgery in recent years, primarily because it offers short-term advantages such as less pain, reduced blood loss, and a shorter recovery time. But no large randomized trials have established that long-term outcomes with laparoscopic resection, including survival, are at least noninferior to those with open surgery, said Dr. Hendrik Jaap Bonjer of VU University Medical Center, Amsterdam, and his associates.
They now report the 3-year outcomes of the Colorectal Cancer Laparoscopic or Open Resection (COLOR) II trial, an industry-sponsored noninferiority study performed at 30 medical centers in eight countries in Europe, North America, and Asia. The trial involved 1,044 patients who had solitary, noninvasive adenocarcinomas of the rectum within 15 cm of the anal verge. A total of 699 of the study participants were randomly assigned to laparoscopic and 345 to open surgery.
At 3-year follow-up, the rate of locoregional recurrence was identical between the two study groups, at 5% each. In addition, rates of disease-free survival slightly favored the laparoscopic approach (74.8%) over the open approach (70.8%), as did rates of overall survival (86.7% and 83.6%, respectively) and rates of distant metastases (19.1% and 22.1%, respectively). Patients with stage III disease appeared to benefit the most from laparoscopic surgery, with disease-free survival of 64.9% vs. 52.0%, the investigators said (N. Engl. J. Med. 2015 April 1 [doi:10.1056/NEJMoa1414882]). These findings support the idea that the reduced surgical trauma associated with laparoscopic techniques may decrease tumor recurrence, perhaps by attenuating stress responses and preserving immune function, they noted.
“In our study, laparoscopic surgery in patients with cancer in the lower third of the rectum was associated with a lower rate of involved circumferential resection margin and a lower locoregional recurrence rate than was open surgery. During laparoscopic surgery, narrow spaces such as the lower pelvis are better visualized than in open surgery, owing to the use of a laparoscope, which projects a magnified and well-illuminated image of the operative field on the monitors. A clear view is of paramount importance to accomplish a resection of the cancer with sufficient margins,” Dr. Bonjer and his associates added.
The trial was funded by Ethicon Endo-Surgery Europe, a subsidiary of Johnson & Johnson; the Swedish Cancer Society; the Health and Medical Care Committee of Region Vastra Gotaland; Sahlgrenska University Hospital; Erasmus University Medical Center; Dahousie University; and VU University Medical Center. Dr. Bonjer reported having no disclosures; two of his associates reported ties to AbbVie, Merck Sharp & Dohme, Takeda, Johnson & Johnson, Covidien, Olympus Medical, and Applied Medical.
Laparoscopic resection of rectal cancer is noninferior to open surgery in preventing locoregional recurrence and in improving overall and disease-free survival, according to a report published online April 1 in the New England Journal of Medicine.
The laparoscopic approach has increasingly replaced open surgery in recent years, primarily because it offers short-term advantages such as less pain, reduced blood loss, and a shorter recovery time. But no large randomized trials have established that long-term outcomes with laparoscopic resection, including survival, are at least noninferior to those with open surgery, said Dr. Hendrik Jaap Bonjer of VU University Medical Center, Amsterdam, and his associates.
They now report the 3-year outcomes of the Colorectal Cancer Laparoscopic or Open Resection (COLOR) II trial, an industry-sponsored noninferiority study performed at 30 medical centers in eight countries in Europe, North America, and Asia. The trial involved 1,044 patients who had solitary, noninvasive adenocarcinomas of the rectum within 15 cm of the anal verge. A total of 699 of the study participants were randomly assigned to laparoscopic and 345 to open surgery.
At 3-year follow-up, the rate of locoregional recurrence was identical between the two study groups, at 5% each. In addition, rates of disease-free survival slightly favored the laparoscopic approach (74.8%) over the open approach (70.8%), as did rates of overall survival (86.7% and 83.6%, respectively) and rates of distant metastases (19.1% and 22.1%, respectively). Patients with stage III disease appeared to benefit the most from laparoscopic surgery, with disease-free survival of 64.9% vs. 52.0%, the investigators said (N. Engl. J. Med. 2015 April 1 [doi:10.1056/NEJMoa1414882]). These findings support the idea that the reduced surgical trauma associated with laparoscopic techniques may decrease tumor recurrence, perhaps by attenuating stress responses and preserving immune function, they noted.
“In our study, laparoscopic surgery in patients with cancer in the lower third of the rectum was associated with a lower rate of involved circumferential resection margin and a lower locoregional recurrence rate than was open surgery. During laparoscopic surgery, narrow spaces such as the lower pelvis are better visualized than in open surgery, owing to the use of a laparoscope, which projects a magnified and well-illuminated image of the operative field on the monitors. A clear view is of paramount importance to accomplish a resection of the cancer with sufficient margins,” Dr. Bonjer and his associates added.
The trial was funded by Ethicon Endo-Surgery Europe, a subsidiary of Johnson & Johnson; the Swedish Cancer Society; the Health and Medical Care Committee of Region Vastra Gotaland; Sahlgrenska University Hospital; Erasmus University Medical Center; Dahousie University; and VU University Medical Center. Dr. Bonjer reported having no disclosures; two of his associates reported ties to AbbVie, Merck Sharp & Dohme, Takeda, Johnson & Johnson, Covidien, Olympus Medical, and Applied Medical.
Laparoscopic resection of rectal cancer is noninferior to open surgery in preventing locoregional recurrence and in improving overall and disease-free survival, according to a report published online April 1 in the New England Journal of Medicine.
The laparoscopic approach has increasingly replaced open surgery in recent years, primarily because it offers short-term advantages such as less pain, reduced blood loss, and a shorter recovery time. But no large randomized trials have established that long-term outcomes with laparoscopic resection, including survival, are at least noninferior to those with open surgery, said Dr. Hendrik Jaap Bonjer of VU University Medical Center, Amsterdam, and his associates.
They now report the 3-year outcomes of the Colorectal Cancer Laparoscopic or Open Resection (COLOR) II trial, an industry-sponsored noninferiority study performed at 30 medical centers in eight countries in Europe, North America, and Asia. The trial involved 1,044 patients who had solitary, noninvasive adenocarcinomas of the rectum within 15 cm of the anal verge. A total of 699 of the study participants were randomly assigned to laparoscopic and 345 to open surgery.
At 3-year follow-up, the rate of locoregional recurrence was identical between the two study groups, at 5% each. In addition, rates of disease-free survival slightly favored the laparoscopic approach (74.8%) over the open approach (70.8%), as did rates of overall survival (86.7% and 83.6%, respectively) and rates of distant metastases (19.1% and 22.1%, respectively). Patients with stage III disease appeared to benefit the most from laparoscopic surgery, with disease-free survival of 64.9% vs. 52.0%, the investigators said (N. Engl. J. Med. 2015 April 1 [doi:10.1056/NEJMoa1414882]). These findings support the idea that the reduced surgical trauma associated with laparoscopic techniques may decrease tumor recurrence, perhaps by attenuating stress responses and preserving immune function, they noted.
“In our study, laparoscopic surgery in patients with cancer in the lower third of the rectum was associated with a lower rate of involved circumferential resection margin and a lower locoregional recurrence rate than was open surgery. During laparoscopic surgery, narrow spaces such as the lower pelvis are better visualized than in open surgery, owing to the use of a laparoscope, which projects a magnified and well-illuminated image of the operative field on the monitors. A clear view is of paramount importance to accomplish a resection of the cancer with sufficient margins,” Dr. Bonjer and his associates added.
The trial was funded by Ethicon Endo-Surgery Europe, a subsidiary of Johnson & Johnson; the Swedish Cancer Society; the Health and Medical Care Committee of Region Vastra Gotaland; Sahlgrenska University Hospital; Erasmus University Medical Center; Dahousie University; and VU University Medical Center. Dr. Bonjer reported having no disclosures; two of his associates reported ties to AbbVie, Merck Sharp & Dohme, Takeda, Johnson & Johnson, Covidien, Olympus Medical, and Applied Medical.
Key clinical point: Laparoscopic resection is noninferior to open surgery in preventing locoregional recurrence of rectal cancer and improving survival.
Major finding: At 3-year follow-up, the rate of locoregional recurrence was identical between the laparoscopic- and the open-surgery groups, at 5% each.
Data source: An industry-sponsored multicenter open-label noninferiority trial comparing laparoscopic to open resection of rectal cancer in 1,044 patients followed for 3 years.
Disclosures: The trial was funded by Ethicon Endo-Surgery Europe, a subsidiary of Johnson & Johnson; the Swedish Cancer Society; the Health and Medical Care Committee of Region Vastra Gotaland; Sahlgrenska University Hospital; Erasmus University Medical Center; Dahousie University; and VU University Medical Center. Dr. Bonjer reported having no disclosures; two of his associates reported ties to AbbVie, Merck Sharp & Dohme, Takeda, Johnson & Johnson, Covidien, Olympus Medical, and Applied Medical.
Metformin Shows Superior Glycemic Durability
Metformin showed superior glycemic durability compared with sulfonylurea and meglitinide in a nationwide observational study in Sweden, according to a report published online in BMJ Open Diabetes Research & Care.
To study glycemic durability in real-world patients, researchers analyzed data from five Swedish national registries of diabetes care, prescribed drugs, causes of death, hospital discharges, and health insurance. They examined the medical records of 69,667 adults who had heretofore untreated type 2 diabetes and were initially prescribed metformin, sulfonylurea, or meglitinide during a 4-year period. They also analyzed medication use in a subset of propensity-matched patients who were well balanced for numerous covariates that can impact diabetes progression, such as age, gender, hemoglobin A1c level, eGFR, and CVD history.
Each medication’s glycemic durability was judged according to whether these patients continued using their initial diabetes drug, switched to a different drug, or added a second drug during 5.5 years of follow-up, said Dr. Nils Ekstrom of the University of Gothenburg (Sweden) and his associates.
Mean patient age was 71 years, mean duration of diabetes was 5 years, and mean body mass index was 28 kg/m2. Overall, almost half of these patients discontinued their initial medication, switched to a different medication, or required a second diabetes drug be added to their regimen during follow-up.
Compared with metformin, sulfonylurea and meglitinide showed a significantly increased risk of monotherapy failure (hazard ratio, 1.74). Sulfonylurea and meglitinide had an even greater risk of requiring a switch to a new agent (HR, 2.81) and of requiring an add-on agent (HR, 3.14). These results from the main analyses were confirmed in two sensitivity analyses involving approximately 60,000 participants, the investigators said (BMJ Open Diab. Res. Care 2015 [doi:10.1136/bmjdrc-2014-000059]).
Patients who continued on their initial monotherapy throughout follow-up showed improved HbA1c levels of approximately 10%, regardless of which medication they used. This group represents treatment responders. In contrast, patients who discontinued, switched, or added a new agent to their initial medication showed stable or slightly increasing HbA1c levels over time, which represented deteriorating glycemic control.
“These results strengthen the current evidence of a superior durability with metformin compared with sulfonylureas” in the real-world setting, and suggest that the same is true regarding meglitinide, Dr. Ekstrom and his associates said.
Metformin showed superior glycemic durability compared with sulfonylurea and meglitinide in a nationwide observational study in Sweden, according to a report published online in BMJ Open Diabetes Research & Care.
To study glycemic durability in real-world patients, researchers analyzed data from five Swedish national registries of diabetes care, prescribed drugs, causes of death, hospital discharges, and health insurance. They examined the medical records of 69,667 adults who had heretofore untreated type 2 diabetes and were initially prescribed metformin, sulfonylurea, or meglitinide during a 4-year period. They also analyzed medication use in a subset of propensity-matched patients who were well balanced for numerous covariates that can impact diabetes progression, such as age, gender, hemoglobin A1c level, eGFR, and CVD history.
Each medication’s glycemic durability was judged according to whether these patients continued using their initial diabetes drug, switched to a different drug, or added a second drug during 5.5 years of follow-up, said Dr. Nils Ekstrom of the University of Gothenburg (Sweden) and his associates.
Mean patient age was 71 years, mean duration of diabetes was 5 years, and mean body mass index was 28 kg/m2. Overall, almost half of these patients discontinued their initial medication, switched to a different medication, or required a second diabetes drug be added to their regimen during follow-up.
Compared with metformin, sulfonylurea and meglitinide showed a significantly increased risk of monotherapy failure (hazard ratio, 1.74). Sulfonylurea and meglitinide had an even greater risk of requiring a switch to a new agent (HR, 2.81) and of requiring an add-on agent (HR, 3.14). These results from the main analyses were confirmed in two sensitivity analyses involving approximately 60,000 participants, the investigators said (BMJ Open Diab. Res. Care 2015 [doi:10.1136/bmjdrc-2014-000059]).
Patients who continued on their initial monotherapy throughout follow-up showed improved HbA1c levels of approximately 10%, regardless of which medication they used. This group represents treatment responders. In contrast, patients who discontinued, switched, or added a new agent to their initial medication showed stable or slightly increasing HbA1c levels over time, which represented deteriorating glycemic control.
“These results strengthen the current evidence of a superior durability with metformin compared with sulfonylureas” in the real-world setting, and suggest that the same is true regarding meglitinide, Dr. Ekstrom and his associates said.
Metformin showed superior glycemic durability compared with sulfonylurea and meglitinide in a nationwide observational study in Sweden, according to a report published online in BMJ Open Diabetes Research & Care.
To study glycemic durability in real-world patients, researchers analyzed data from five Swedish national registries of diabetes care, prescribed drugs, causes of death, hospital discharges, and health insurance. They examined the medical records of 69,667 adults who had heretofore untreated type 2 diabetes and were initially prescribed metformin, sulfonylurea, or meglitinide during a 4-year period. They also analyzed medication use in a subset of propensity-matched patients who were well balanced for numerous covariates that can impact diabetes progression, such as age, gender, hemoglobin A1c level, eGFR, and CVD history.
Each medication’s glycemic durability was judged according to whether these patients continued using their initial diabetes drug, switched to a different drug, or added a second drug during 5.5 years of follow-up, said Dr. Nils Ekstrom of the University of Gothenburg (Sweden) and his associates.
Mean patient age was 71 years, mean duration of diabetes was 5 years, and mean body mass index was 28 kg/m2. Overall, almost half of these patients discontinued their initial medication, switched to a different medication, or required a second diabetes drug be added to their regimen during follow-up.
Compared with metformin, sulfonylurea and meglitinide showed a significantly increased risk of monotherapy failure (hazard ratio, 1.74). Sulfonylurea and meglitinide had an even greater risk of requiring a switch to a new agent (HR, 2.81) and of requiring an add-on agent (HR, 3.14). These results from the main analyses were confirmed in two sensitivity analyses involving approximately 60,000 participants, the investigators said (BMJ Open Diab. Res. Care 2015 [doi:10.1136/bmjdrc-2014-000059]).
Patients who continued on their initial monotherapy throughout follow-up showed improved HbA1c levels of approximately 10%, regardless of which medication they used. This group represents treatment responders. In contrast, patients who discontinued, switched, or added a new agent to their initial medication showed stable or slightly increasing HbA1c levels over time, which represented deteriorating glycemic control.
“These results strengthen the current evidence of a superior durability with metformin compared with sulfonylureas” in the real-world setting, and suggest that the same is true regarding meglitinide, Dr. Ekstrom and his associates said.
FROM BMJ OPEN DIABETES RESEARCH & CARE