User login
Blood Pressure Differences Between Arms Flags Vascular Disease
A difference of 15 mm Hg or more in systolic blood pressure between a patient’s arms may signal the presence of asymptomatic peripheral vascular disease, according to a meta-analysis published online Jan. 30 in the Lancet.
Patients with this finding on physical examination might benefit from further assessment for peripheral vascular disease, much as those found to have reduced ankle-brachial pressure do. But simultaneous measurement of systolic BP in both arms is more easily done in the primary care setting, since such measurement in one arm is already routine and doesn’t require the time, experience, and training necessary for ankle-brachial pressure assessment, said Dr. Christopher E. Clark of the institute of health services research, University of Exeter (England), and his associates.
The most recent National Institute for Health and Clinical Excellence (NICE) guideline for hypertension states that a difference of 20 mm Hg or more between the arms is "unusual" and is often associated with underlying vascular disease, but doesn’t address smaller differences. The guideline also has advised routinely checking BP in both arms for several years, but most primary care physicians in the United Kingdom do not follow that advice, Dr. Clark and his colleagues said.
To establish whether small differences (10-15 mm Hg) in systolic blood pressure between the arms is associated with peripheral or cardiovascular disease, they performed a meta-analysis of 20 studies addressing the issue.
The investigators found that a difference of 10-15 mm Hg occurred in 12%-15% of the study subjects and was associated with peripheral vascular disease, with a low sensitivity but a very high specificity. This overall prevalence corresponds to published estimates in community studies, implying that findings of the meta-analysis are generalizable, they noted.
In particular, five studies that correlated systolic BP with findings on invasive angiography showed that a difference of 10 mm Hg or more was strongly associated with subclavian stenosis on the side with the lowest pressure (Lancet 2012 Jan. 30 [doi:10.1016/S0140-6736(11)61710-8]).
In pooled findings from studies with noninvasive assessments of vascular disease, a difference of 15 mm Hg or more was associated with not only peripheral vascular disease (sensitivity of 15% and specificity of 96%), but also with cerebrovascular disease (sensitivity of 8% and specificity of 93%) as well as increased cardiovascular and all-cause mortality.
In five studies, a difference as low as 10 mm Hg was associated with peripheral vascular disease (sensitivity of 32% and specificity of 91%).
These findings remained consistent across studies that used different methods of measuring BP, regardless of whether the cohorts comprised high-risk hospital-recruited patients or average-risk people living in the community.
Because this study was a meta-analysis rather than a randomized clinical trial, "what constitutes a clinically important difference in systolic BP between arms is [still] unclear. However, we have associated a difference with an increased likelihood of peripheral vascular disease and with prospective differences in survival. Further research is needed to establish the upper limit of normal between-arm differences," Dr. Clark and his associates wrote.
In an editorial accompanying this report, Dr. Richard J. McManus and Dr. Jonathan Mant wrote: "The high specificity (96%) of the association between a difference in systolic BP between arms of more than 15 mm Hg and peripheral vascular disease justifies the use of this measure as a sign of disease" (Lancet 2012 Jan. 30 [doi:10.1016/S0140-6736(11)61926-0]).
Ascertaining such differences should become part of routine care, "as opposed to a guideline recommendation that is mostly ignored," said Dr. McManus of the department of primary care health sciences at the University of Oxford (England) and Dr. Mant of the department of public health and primary care at the University of Cambridge (England).
However, "the low sensitivity (15%) shows that measurement of differences is of little value as a screening test for peripheral vascular disease, and ankle-brachial pressure indices will still be necessary for diagnosis," they noted.
Neither Dr. McManus nor Dr. Mant reported having any relevant financial disclosures.
This study was funded by the Royal College of General Practitioners, the South West GP Trust, and the Peninsula Collaboration for Leadership in Applied Health Research and Care. The investigators reported that they had no relevant financial disclosures.
A difference of 15 mm Hg or more in systolic blood pressure between a patient’s arms may signal the presence of asymptomatic peripheral vascular disease, according to a meta-analysis published online Jan. 30 in the Lancet.
Patients with this finding on physical examination might benefit from further assessment for peripheral vascular disease, much as those found to have reduced ankle-brachial pressure do. But simultaneous measurement of systolic BP in both arms is more easily done in the primary care setting, since such measurement in one arm is already routine and doesn’t require the time, experience, and training necessary for ankle-brachial pressure assessment, said Dr. Christopher E. Clark of the institute of health services research, University of Exeter (England), and his associates.
The most recent National Institute for Health and Clinical Excellence (NICE) guideline for hypertension states that a difference of 20 mm Hg or more between the arms is "unusual" and is often associated with underlying vascular disease, but doesn’t address smaller differences. The guideline also has advised routinely checking BP in both arms for several years, but most primary care physicians in the United Kingdom do not follow that advice, Dr. Clark and his colleagues said.
To establish whether small differences (10-15 mm Hg) in systolic blood pressure between the arms is associated with peripheral or cardiovascular disease, they performed a meta-analysis of 20 studies addressing the issue.
The investigators found that a difference of 10-15 mm Hg occurred in 12%-15% of the study subjects and was associated with peripheral vascular disease, with a low sensitivity but a very high specificity. This overall prevalence corresponds to published estimates in community studies, implying that findings of the meta-analysis are generalizable, they noted.
In particular, five studies that correlated systolic BP with findings on invasive angiography showed that a difference of 10 mm Hg or more was strongly associated with subclavian stenosis on the side with the lowest pressure (Lancet 2012 Jan. 30 [doi:10.1016/S0140-6736(11)61710-8]).
In pooled findings from studies with noninvasive assessments of vascular disease, a difference of 15 mm Hg or more was associated with not only peripheral vascular disease (sensitivity of 15% and specificity of 96%), but also with cerebrovascular disease (sensitivity of 8% and specificity of 93%) as well as increased cardiovascular and all-cause mortality.
In five studies, a difference as low as 10 mm Hg was associated with peripheral vascular disease (sensitivity of 32% and specificity of 91%).
These findings remained consistent across studies that used different methods of measuring BP, regardless of whether the cohorts comprised high-risk hospital-recruited patients or average-risk people living in the community.
Because this study was a meta-analysis rather than a randomized clinical trial, "what constitutes a clinically important difference in systolic BP between arms is [still] unclear. However, we have associated a difference with an increased likelihood of peripheral vascular disease and with prospective differences in survival. Further research is needed to establish the upper limit of normal between-arm differences," Dr. Clark and his associates wrote.
In an editorial accompanying this report, Dr. Richard J. McManus and Dr. Jonathan Mant wrote: "The high specificity (96%) of the association between a difference in systolic BP between arms of more than 15 mm Hg and peripheral vascular disease justifies the use of this measure as a sign of disease" (Lancet 2012 Jan. 30 [doi:10.1016/S0140-6736(11)61926-0]).
Ascertaining such differences should become part of routine care, "as opposed to a guideline recommendation that is mostly ignored," said Dr. McManus of the department of primary care health sciences at the University of Oxford (England) and Dr. Mant of the department of public health and primary care at the University of Cambridge (England).
However, "the low sensitivity (15%) shows that measurement of differences is of little value as a screening test for peripheral vascular disease, and ankle-brachial pressure indices will still be necessary for diagnosis," they noted.
Neither Dr. McManus nor Dr. Mant reported having any relevant financial disclosures.
This study was funded by the Royal College of General Practitioners, the South West GP Trust, and the Peninsula Collaboration for Leadership in Applied Health Research and Care. The investigators reported that they had no relevant financial disclosures.
A difference of 15 mm Hg or more in systolic blood pressure between a patient’s arms may signal the presence of asymptomatic peripheral vascular disease, according to a meta-analysis published online Jan. 30 in the Lancet.
Patients with this finding on physical examination might benefit from further assessment for peripheral vascular disease, much as those found to have reduced ankle-brachial pressure do. But simultaneous measurement of systolic BP in both arms is more easily done in the primary care setting, since such measurement in one arm is already routine and doesn’t require the time, experience, and training necessary for ankle-brachial pressure assessment, said Dr. Christopher E. Clark of the institute of health services research, University of Exeter (England), and his associates.
The most recent National Institute for Health and Clinical Excellence (NICE) guideline for hypertension states that a difference of 20 mm Hg or more between the arms is "unusual" and is often associated with underlying vascular disease, but doesn’t address smaller differences. The guideline also has advised routinely checking BP in both arms for several years, but most primary care physicians in the United Kingdom do not follow that advice, Dr. Clark and his colleagues said.
To establish whether small differences (10-15 mm Hg) in systolic blood pressure between the arms is associated with peripheral or cardiovascular disease, they performed a meta-analysis of 20 studies addressing the issue.
The investigators found that a difference of 10-15 mm Hg occurred in 12%-15% of the study subjects and was associated with peripheral vascular disease, with a low sensitivity but a very high specificity. This overall prevalence corresponds to published estimates in community studies, implying that findings of the meta-analysis are generalizable, they noted.
In particular, five studies that correlated systolic BP with findings on invasive angiography showed that a difference of 10 mm Hg or more was strongly associated with subclavian stenosis on the side with the lowest pressure (Lancet 2012 Jan. 30 [doi:10.1016/S0140-6736(11)61710-8]).
In pooled findings from studies with noninvasive assessments of vascular disease, a difference of 15 mm Hg or more was associated with not only peripheral vascular disease (sensitivity of 15% and specificity of 96%), but also with cerebrovascular disease (sensitivity of 8% and specificity of 93%) as well as increased cardiovascular and all-cause mortality.
In five studies, a difference as low as 10 mm Hg was associated with peripheral vascular disease (sensitivity of 32% and specificity of 91%).
These findings remained consistent across studies that used different methods of measuring BP, regardless of whether the cohorts comprised high-risk hospital-recruited patients or average-risk people living in the community.
Because this study was a meta-analysis rather than a randomized clinical trial, "what constitutes a clinically important difference in systolic BP between arms is [still] unclear. However, we have associated a difference with an increased likelihood of peripheral vascular disease and with prospective differences in survival. Further research is needed to establish the upper limit of normal between-arm differences," Dr. Clark and his associates wrote.
In an editorial accompanying this report, Dr. Richard J. McManus and Dr. Jonathan Mant wrote: "The high specificity (96%) of the association between a difference in systolic BP between arms of more than 15 mm Hg and peripheral vascular disease justifies the use of this measure as a sign of disease" (Lancet 2012 Jan. 30 [doi:10.1016/S0140-6736(11)61926-0]).
Ascertaining such differences should become part of routine care, "as opposed to a guideline recommendation that is mostly ignored," said Dr. McManus of the department of primary care health sciences at the University of Oxford (England) and Dr. Mant of the department of public health and primary care at the University of Cambridge (England).
However, "the low sensitivity (15%) shows that measurement of differences is of little value as a screening test for peripheral vascular disease, and ankle-brachial pressure indices will still be necessary for diagnosis," they noted.
Neither Dr. McManus nor Dr. Mant reported having any relevant financial disclosures.
This study was funded by the Royal College of General Practitioners, the South West GP Trust, and the Peninsula Collaboration for Leadership in Applied Health Research and Care. The investigators reported that they had no relevant financial disclosures.
FROM THE LANCET
Major Finding: A systolic BP difference of 15 mm Hg or more between a patient’s two arms signals a higher risk for peripheral vascular disease with a low sensitivity (less than10%) but a very high specificity (greater than 90%).
Data Source: A meta-analysis of 20 studies examining factors that correlated with small differences (10-15 mm Hg) in systolic BP between patients’ two arms.
Disclosures: This study was funded by the Royal College of General Practitioners, the South West GP Trust, and the Peninsula Collaboration for Leadership in Applied Health Research and Care. The investigators reported that they had no relevant financial disclosures.
Evidence Suggests Optimal Intervals for Osteoporosis Screening
Based on available evidence, osteoporosis screening should take place at 15-year intervals for postmenopausal women who have normal bone density or mild osteopenia at their first assessment, at 5-year intervals for those who have moderate osteopenia, and at 1-year intervals for those who have advanced osteopenia, according to a report in the Jan. 19 New England Journal of Medicine.
Screening at shorter intervals is unlikely to improve prediction of the transition to osteoporosis, and thus won’t help clinicians judge when to start osteoporosis therapy so as to avert hip or vertebral fractures, said Dr. Margaret L. Gourlay of the department of family medicine, University of North Carolina, Chapel Hill, and her associates in the Study of Osteoporotic Fractures research group.
Current guidelines do not specify how long to wait between bone mineral density screening with dual-energy x-ray absorptiometry (DEXA), and no U.S. study to date "has addressed this clinical uncertainty," they noted.
"To determine how the BMD testing interval relates to the timing of the transition from normal [bone mineral density] or osteopenia to the development of osteoporosis before a hip or clinical vertebral fracture occurs, we conducted competing-risk analyses of data from 4,957 women, 67 years of age or older, who did not have osteoporosis at baseline and who were followed longitudinally for up to 15 years in the [Study of Osteoporotic Fractures]," the investigators said.
The appropriate screening interval was defined as the estimated time for 10% of the study subjects in each category of osteopenia severity to make the transition from normal BMD or osteopenia to osteoporosis before fractures occurred and before treatment for osteoporosis was initiated. The three categories of severity were normal BMD/mild osteopenia (T score of greater than -1.50) at the initial assessment, moderate osteopenia (T score of -1.50 to -1.99), and advanced osteopenia (T score of -2.00 to -2.49).
This interval was found to be 15 years for normal BMD/mild osteopenia, 5 years for moderate osteopenia, and 1 year for advanced osteopenia, Dr. Gourlay and her colleagues said (N. Engl. J. Med. 2012;366:225-33).
"Recent controversy over the harms of excessive screening for other chronic diseases reinforces the importance of developing a rational screening program for osteoporosis that is based on the best available evidence rather than on health care marketing, advocacy, and public beliefs that have encouraged overtesting and overtreatment in the U.S.," they noted.
"Our estimates for BMD testing proved to be robust after adjustment for major clinical risk factors" such as fracture history, smoking status, use of estrogen, and use of glucocorticoids. "However, clinicians may choose to reevaluate patients before our estimated screening intervals if there is evidence of decreased activity or mobility, weight loss, or other risk factors not considered in our analyses," they said.
This study was supported by the National Institutes of Health. No potential conflicts of interest were reported.
Based on available evidence, osteoporosis screening should take place at 15-year intervals for postmenopausal women who have normal bone density or mild osteopenia at their first assessment, at 5-year intervals for those who have moderate osteopenia, and at 1-year intervals for those who have advanced osteopenia, according to a report in the Jan. 19 New England Journal of Medicine.
Screening at shorter intervals is unlikely to improve prediction of the transition to osteoporosis, and thus won’t help clinicians judge when to start osteoporosis therapy so as to avert hip or vertebral fractures, said Dr. Margaret L. Gourlay of the department of family medicine, University of North Carolina, Chapel Hill, and her associates in the Study of Osteoporotic Fractures research group.
Current guidelines do not specify how long to wait between bone mineral density screening with dual-energy x-ray absorptiometry (DEXA), and no U.S. study to date "has addressed this clinical uncertainty," they noted.
"To determine how the BMD testing interval relates to the timing of the transition from normal [bone mineral density] or osteopenia to the development of osteoporosis before a hip or clinical vertebral fracture occurs, we conducted competing-risk analyses of data from 4,957 women, 67 years of age or older, who did not have osteoporosis at baseline and who were followed longitudinally for up to 15 years in the [Study of Osteoporotic Fractures]," the investigators said.
The appropriate screening interval was defined as the estimated time for 10% of the study subjects in each category of osteopenia severity to make the transition from normal BMD or osteopenia to osteoporosis before fractures occurred and before treatment for osteoporosis was initiated. The three categories of severity were normal BMD/mild osteopenia (T score of greater than -1.50) at the initial assessment, moderate osteopenia (T score of -1.50 to -1.99), and advanced osteopenia (T score of -2.00 to -2.49).
This interval was found to be 15 years for normal BMD/mild osteopenia, 5 years for moderate osteopenia, and 1 year for advanced osteopenia, Dr. Gourlay and her colleagues said (N. Engl. J. Med. 2012;366:225-33).
"Recent controversy over the harms of excessive screening for other chronic diseases reinforces the importance of developing a rational screening program for osteoporosis that is based on the best available evidence rather than on health care marketing, advocacy, and public beliefs that have encouraged overtesting and overtreatment in the U.S.," they noted.
"Our estimates for BMD testing proved to be robust after adjustment for major clinical risk factors" such as fracture history, smoking status, use of estrogen, and use of glucocorticoids. "However, clinicians may choose to reevaluate patients before our estimated screening intervals if there is evidence of decreased activity or mobility, weight loss, or other risk factors not considered in our analyses," they said.
This study was supported by the National Institutes of Health. No potential conflicts of interest were reported.
Based on available evidence, osteoporosis screening should take place at 15-year intervals for postmenopausal women who have normal bone density or mild osteopenia at their first assessment, at 5-year intervals for those who have moderate osteopenia, and at 1-year intervals for those who have advanced osteopenia, according to a report in the Jan. 19 New England Journal of Medicine.
Screening at shorter intervals is unlikely to improve prediction of the transition to osteoporosis, and thus won’t help clinicians judge when to start osteoporosis therapy so as to avert hip or vertebral fractures, said Dr. Margaret L. Gourlay of the department of family medicine, University of North Carolina, Chapel Hill, and her associates in the Study of Osteoporotic Fractures research group.
Current guidelines do not specify how long to wait between bone mineral density screening with dual-energy x-ray absorptiometry (DEXA), and no U.S. study to date "has addressed this clinical uncertainty," they noted.
"To determine how the BMD testing interval relates to the timing of the transition from normal [bone mineral density] or osteopenia to the development of osteoporosis before a hip or clinical vertebral fracture occurs, we conducted competing-risk analyses of data from 4,957 women, 67 years of age or older, who did not have osteoporosis at baseline and who were followed longitudinally for up to 15 years in the [Study of Osteoporotic Fractures]," the investigators said.
The appropriate screening interval was defined as the estimated time for 10% of the study subjects in each category of osteopenia severity to make the transition from normal BMD or osteopenia to osteoporosis before fractures occurred and before treatment for osteoporosis was initiated. The three categories of severity were normal BMD/mild osteopenia (T score of greater than -1.50) at the initial assessment, moderate osteopenia (T score of -1.50 to -1.99), and advanced osteopenia (T score of -2.00 to -2.49).
This interval was found to be 15 years for normal BMD/mild osteopenia, 5 years for moderate osteopenia, and 1 year for advanced osteopenia, Dr. Gourlay and her colleagues said (N. Engl. J. Med. 2012;366:225-33).
"Recent controversy over the harms of excessive screening for other chronic diseases reinforces the importance of developing a rational screening program for osteoporosis that is based on the best available evidence rather than on health care marketing, advocacy, and public beliefs that have encouraged overtesting and overtreatment in the U.S.," they noted.
"Our estimates for BMD testing proved to be robust after adjustment for major clinical risk factors" such as fracture history, smoking status, use of estrogen, and use of glucocorticoids. "However, clinicians may choose to reevaluate patients before our estimated screening intervals if there is evidence of decreased activity or mobility, weight loss, or other risk factors not considered in our analyses," they said.
This study was supported by the National Institutes of Health. No potential conflicts of interest were reported.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major Finding: DEXA screening for osteoporosis should be done at 15-year intervals for women with normal BMD or mild osteopenia (T score of greater than -1.50) at their initial screen, at 5-year intervals for those who have moderate osteopenia (T score of -1.50 to -1.99), and at 1-year intervals for those who have advanced osteopenia (T score of -2.00 to -2.49).
Data Source: Analysis of data from the longitudinal Study of Osteoporotic Fractures involving 4,957 postmenopausal women aged 67 years and older at baseline who were followed for 15 years.
Disclosures: This study was supported by the National Institutes of Health. No potential conflicts of interest were reported.
Novel Antiplatelet a Bridge Between Thienopyridine and CABG
Intravenous cangrelor may prove to be a useful "bridge" in patients awaiting nonemergency CABG who must first discontinue their regular antiplatelet therapy, according to the results of the Maintenance of Platelet Inhibition With Cangrelor (BRIDGE) trial reported in the Jan. 18 issue of JAMA.
The practice of discontinuation of antiplatelet therapy is associated with significant morbidity and mortality; in patients who have coronary stents, it raises the risk of stent thrombosis that often leads to myocardial infarction and death.
"Cessation of thienopyridine treatment for nearly a week before surgery, with patients not hospitalized or monitored but carrying an excess risk of major ischemic events, has been a troubling and not infrequent problem for clinicians, because it is estimated that approximately 5% of patients will require some type of surgery within the first 12 months after stent implant or [acute coronary syndrome] diagnosis," said Dr. Dominick J. Angiolillo of the department of cardiology, University of Florida, Jacksonville, and his associates.
In this multicenter clinical trial sponsored by the drug’s maker, cangrelor "achieved and maintained target levels of platelet inhibition known to be associated with a low risk of thrombotic events compared with placebo, without a significant excess in bleeding complications," the investigators noted.
Cangrelor is an investigational nonthienopyridine adenosine triphosphate analogue that acts as an antagonist of the P2Y12 receptor. It is characterized by "rapid, potent, predictable, and reversible platelet inhibition," and its extremely short half-life (3-6 minutes) allows "rapid offset of effect."
The investigators hypothesized that cangrelor would allow patients who must discontinue antiplatelet therapy prior to cardiac surgery, especially if they’re taking a P2Y12 inhibitor such as ticlopidine, clopidogrel, or prasugrel, to go off their usual drug without raising their risk for thrombotic events. They tested this hypothesis in a two-part trial.
The first part was an open-label dose-finding study involving 11 adults, which concluded that the optimal intravenous dose needed to maintain antiplatelet activity without raising bleeding risks was 0.75 mcg/kg per minute.
In the second part of the trial, 210 patients awaiting CABG at 34 medical centers around the world were randomly assigned to receive either cangrelor (106 subjects) or placebo (104 subjects) after thienopyridines were discontinued and throughout the preoperative period – that is, until 1-6 hours before surgical incision. Platelet function was assessed before, during, and after the infusion.
The mean interval between discontinuation of thienopyridines and infusion of the study drug was 29 hours, and the mean duration of the infusion was approximately 3 days.
The primary end point was the percentage of patients who showed platelet reactivity of less than 240 P2Y12 Reaction Units (PRUs) throughout the infusion of the study drug. "This level approximated the levels of platelet reactivity expected to be maintained if a thienopyridine had not been discontinued," the investigators explained.
This end point was met by 99% of the cangrelor group but only 19% of the placebo group. It was achieved independently of patients’ usual dose of thienopyridines and independently of the length of time since thienopyridines were discontinued, Dr. Angiolillo and his colleagues said (JAMA 2012;307:265-74).
Moreover, cangrelor did not raise the rate of excessive bleeding related to CABG surgery. This safety end point occurred in 22 patients: 11.8% of the cangrelor group and 10.4% of the placebo group, a nonsignificant difference.
The number of minor bleeding events was numerically higher with cangrelor but did not reach statistical significance. Other adverse events, including dyspnea and laboratory abnormalities, also were comparable between the two groups. This favorable safety profile, even with prolonged infusion of up to 7 days, was "reassuring," the researchers noted.
Ischemic end points prior to surgery were low in both groups, occurring in 2.8% (3 of 106) and 4.0% (4 of 101) of patients in the cangrelor and placebo groups.
"These observations support the hypothesis that intravenous cangrelor is a feasible management strategy, providing prolonged platelet P2Y12 inhibition in patients who must wait for cardiac surgery after thienopyridine discontinuation," they said.
This study was sponsored by the Medicines Company. Dr. Angiolillo reported ties to Bristol-Myers Squibb, Sanofi-Aventis, Eli Lilly, Daiichi Sankyo, AstraZeneca, Portola, Novartis, Medicure, Accumetrics, Arena Pharmaceuticals, Merck, Evolva, and Abbott Vascular, and his associates reported ties to numerous other industry sources.
Intravenous cangrelor may prove to be a useful "bridge" in patients awaiting nonemergency CABG who must first discontinue their regular antiplatelet therapy, according to the results of the Maintenance of Platelet Inhibition With Cangrelor (BRIDGE) trial reported in the Jan. 18 issue of JAMA.
The practice of discontinuation of antiplatelet therapy is associated with significant morbidity and mortality; in patients who have coronary stents, it raises the risk of stent thrombosis that often leads to myocardial infarction and death.
"Cessation of thienopyridine treatment for nearly a week before surgery, with patients not hospitalized or monitored but carrying an excess risk of major ischemic events, has been a troubling and not infrequent problem for clinicians, because it is estimated that approximately 5% of patients will require some type of surgery within the first 12 months after stent implant or [acute coronary syndrome] diagnosis," said Dr. Dominick J. Angiolillo of the department of cardiology, University of Florida, Jacksonville, and his associates.
In this multicenter clinical trial sponsored by the drug’s maker, cangrelor "achieved and maintained target levels of platelet inhibition known to be associated with a low risk of thrombotic events compared with placebo, without a significant excess in bleeding complications," the investigators noted.
Cangrelor is an investigational nonthienopyridine adenosine triphosphate analogue that acts as an antagonist of the P2Y12 receptor. It is characterized by "rapid, potent, predictable, and reversible platelet inhibition," and its extremely short half-life (3-6 minutes) allows "rapid offset of effect."
The investigators hypothesized that cangrelor would allow patients who must discontinue antiplatelet therapy prior to cardiac surgery, especially if they’re taking a P2Y12 inhibitor such as ticlopidine, clopidogrel, or prasugrel, to go off their usual drug without raising their risk for thrombotic events. They tested this hypothesis in a two-part trial.
The first part was an open-label dose-finding study involving 11 adults, which concluded that the optimal intravenous dose needed to maintain antiplatelet activity without raising bleeding risks was 0.75 mcg/kg per minute.
In the second part of the trial, 210 patients awaiting CABG at 34 medical centers around the world were randomly assigned to receive either cangrelor (106 subjects) or placebo (104 subjects) after thienopyridines were discontinued and throughout the preoperative period – that is, until 1-6 hours before surgical incision. Platelet function was assessed before, during, and after the infusion.
The mean interval between discontinuation of thienopyridines and infusion of the study drug was 29 hours, and the mean duration of the infusion was approximately 3 days.
The primary end point was the percentage of patients who showed platelet reactivity of less than 240 P2Y12 Reaction Units (PRUs) throughout the infusion of the study drug. "This level approximated the levels of platelet reactivity expected to be maintained if a thienopyridine had not been discontinued," the investigators explained.
This end point was met by 99% of the cangrelor group but only 19% of the placebo group. It was achieved independently of patients’ usual dose of thienopyridines and independently of the length of time since thienopyridines were discontinued, Dr. Angiolillo and his colleagues said (JAMA 2012;307:265-74).
Moreover, cangrelor did not raise the rate of excessive bleeding related to CABG surgery. This safety end point occurred in 22 patients: 11.8% of the cangrelor group and 10.4% of the placebo group, a nonsignificant difference.
The number of minor bleeding events was numerically higher with cangrelor but did not reach statistical significance. Other adverse events, including dyspnea and laboratory abnormalities, also were comparable between the two groups. This favorable safety profile, even with prolonged infusion of up to 7 days, was "reassuring," the researchers noted.
Ischemic end points prior to surgery were low in both groups, occurring in 2.8% (3 of 106) and 4.0% (4 of 101) of patients in the cangrelor and placebo groups.
"These observations support the hypothesis that intravenous cangrelor is a feasible management strategy, providing prolonged platelet P2Y12 inhibition in patients who must wait for cardiac surgery after thienopyridine discontinuation," they said.
This study was sponsored by the Medicines Company. Dr. Angiolillo reported ties to Bristol-Myers Squibb, Sanofi-Aventis, Eli Lilly, Daiichi Sankyo, AstraZeneca, Portola, Novartis, Medicure, Accumetrics, Arena Pharmaceuticals, Merck, Evolva, and Abbott Vascular, and his associates reported ties to numerous other industry sources.
Intravenous cangrelor may prove to be a useful "bridge" in patients awaiting nonemergency CABG who must first discontinue their regular antiplatelet therapy, according to the results of the Maintenance of Platelet Inhibition With Cangrelor (BRIDGE) trial reported in the Jan. 18 issue of JAMA.
The practice of discontinuation of antiplatelet therapy is associated with significant morbidity and mortality; in patients who have coronary stents, it raises the risk of stent thrombosis that often leads to myocardial infarction and death.
"Cessation of thienopyridine treatment for nearly a week before surgery, with patients not hospitalized or monitored but carrying an excess risk of major ischemic events, has been a troubling and not infrequent problem for clinicians, because it is estimated that approximately 5% of patients will require some type of surgery within the first 12 months after stent implant or [acute coronary syndrome] diagnosis," said Dr. Dominick J. Angiolillo of the department of cardiology, University of Florida, Jacksonville, and his associates.
In this multicenter clinical trial sponsored by the drug’s maker, cangrelor "achieved and maintained target levels of platelet inhibition known to be associated with a low risk of thrombotic events compared with placebo, without a significant excess in bleeding complications," the investigators noted.
Cangrelor is an investigational nonthienopyridine adenosine triphosphate analogue that acts as an antagonist of the P2Y12 receptor. It is characterized by "rapid, potent, predictable, and reversible platelet inhibition," and its extremely short half-life (3-6 minutes) allows "rapid offset of effect."
The investigators hypothesized that cangrelor would allow patients who must discontinue antiplatelet therapy prior to cardiac surgery, especially if they’re taking a P2Y12 inhibitor such as ticlopidine, clopidogrel, or prasugrel, to go off their usual drug without raising their risk for thrombotic events. They tested this hypothesis in a two-part trial.
The first part was an open-label dose-finding study involving 11 adults, which concluded that the optimal intravenous dose needed to maintain antiplatelet activity without raising bleeding risks was 0.75 mcg/kg per minute.
In the second part of the trial, 210 patients awaiting CABG at 34 medical centers around the world were randomly assigned to receive either cangrelor (106 subjects) or placebo (104 subjects) after thienopyridines were discontinued and throughout the preoperative period – that is, until 1-6 hours before surgical incision. Platelet function was assessed before, during, and after the infusion.
The mean interval between discontinuation of thienopyridines and infusion of the study drug was 29 hours, and the mean duration of the infusion was approximately 3 days.
The primary end point was the percentage of patients who showed platelet reactivity of less than 240 P2Y12 Reaction Units (PRUs) throughout the infusion of the study drug. "This level approximated the levels of platelet reactivity expected to be maintained if a thienopyridine had not been discontinued," the investigators explained.
This end point was met by 99% of the cangrelor group but only 19% of the placebo group. It was achieved independently of patients’ usual dose of thienopyridines and independently of the length of time since thienopyridines were discontinued, Dr. Angiolillo and his colleagues said (JAMA 2012;307:265-74).
Moreover, cangrelor did not raise the rate of excessive bleeding related to CABG surgery. This safety end point occurred in 22 patients: 11.8% of the cangrelor group and 10.4% of the placebo group, a nonsignificant difference.
The number of minor bleeding events was numerically higher with cangrelor but did not reach statistical significance. Other adverse events, including dyspnea and laboratory abnormalities, also were comparable between the two groups. This favorable safety profile, even with prolonged infusion of up to 7 days, was "reassuring," the researchers noted.
Ischemic end points prior to surgery were low in both groups, occurring in 2.8% (3 of 106) and 4.0% (4 of 101) of patients in the cangrelor and placebo groups.
"These observations support the hypothesis that intravenous cangrelor is a feasible management strategy, providing prolonged platelet P2Y12 inhibition in patients who must wait for cardiac surgery after thienopyridine discontinuation," they said.
This study was sponsored by the Medicines Company. Dr. Angiolillo reported ties to Bristol-Myers Squibb, Sanofi-Aventis, Eli Lilly, Daiichi Sankyo, AstraZeneca, Portola, Novartis, Medicure, Accumetrics, Arena Pharmaceuticals, Merck, Evolva, and Abbott Vascular, and his associates reported ties to numerous other industry sources.
FROM JAMA
Major Finding: In patients preparing for CABG surgery, 99% of those treated with cangrelor, compared with 19% given placebo, showed adequate platelet reactivity after thienopyridines were discontinued in preparation for CABG surgery.
Data Source: BRIDGE, a prospective, randomized, double-blind, multicenter clinical trial comparing intravenous cangrelor with placebo as a "bridge" therapy between the cessation of antiplatelet drugs and the onset of CABG surgery in 210 patients.
Disclosures: This study was sponsored by the Medicines Company. Dr. Angiolillo reported ties to Bristol-Myers Squibb, Sanofi-Aventis, Eli Lilly, Daiichi Sankyo, AstraZeneca, Portola, Novartis, Medicure, Accumetrics, Arena Pharmaceuticals, Merck, Evolva, and Abbott Vascular, and his associates reported ties to numerous other industry sources.
Benchmarks Discerned for In-Hospital VTE After Hip, Knee Arthroplasty
For the first time, researchers say they have established benchmarks for the rates of in-hospital venous thromboembolism that occur after total or partial hip arthroplasty and after total or partial knee arthroplasty, according to a report Jan. 18 in JAMA.
In a meta-analysis of 47 studies that documented venous thromboembolism (VTE) event rates in nearly 45,000 patients who received recommended prophylaxis during hospitalization for knee or hip arthroplasty, investigators estimated that approximately 1 in every 100 patients undergoing knee arthroplasty and 1 in every 200 undergoing hip arthroplasty will develop symptomatic VTE before they are discharged.
"These estimates are of value to individual patients and clinicians in the consideration of risks and benefits" of the two procedures. They also are important because rates of in-hospital VTE are increasingly used as indicators of patient safety at individual medical centers, even though the expected background rates haven’t been established until now, said Jean-Marie Januel, a registered nurse with the Institute of Social and Preventive Medicine, Lausanne (Switzerland) University Hospital, and his associates.
"Large numbers of patients worldwide undergo hip and knee replacement procedures annually, and VTE is a widely acknowledged complication. Yet no estimate of symptomatic VTE risk prior to hospital discharge is available from the literature that can be conveyed to patients in the informed consent process," they noted.
Mr. Januel and his colleagues performed a systemic search of the literature to identify studies performed between 1996 and 2011 in which subjects undergoing either hip or knee arthroplasty received VTE prophylaxis according to published guidelines, including either low-molecular-weight heparin or inhibitors of factor Xa or IIa. They found 41 randomized clinical trials and 6 observational studies to include in the meta-analysis.
A total of 22 of the studies were performed in Europe, 14 were in North America, and 11 were in other regions. The mean duration of follow-up after either surgery was 13 days.
This included 21 studies of partial or total hip arthroplasty, 20 of partial or total knee arthroplasty, and 6 studies of both procedures, with a total of 44,844 subjects.
There were 443 cases of symptomatic postoperative VTE that developed before hospital discharge: 288 in the 23,475 knee patients and 155 in the 23,475 hip patients. This included 182 cases of deep vein thrombosis in the knee patients and 93 in the hip patients, as well as 106 cases of pulmonary embolism in the knee patients and 43 in the hip patients.
The pooled incidence rates of VTE were approximately 1% after knee arthroplasty and approximately 0.5% after hip arthroplasty. This means that the background rate of VTE is approximately 1 in 100 knee patients and 1 in 200 hip patients, the investigators said (JAMA 2012;307:294-303).
When the data were broken down by type of VTE, the pooled incidence rates were 0.26% for deep vein thrombosis and 0.14% for pulmonary embolism after knee arthroplasty. The corresponding rates were 0.63% for deep vein thrombosis and 0.27% for pulmonary embolism after hip arthroplasty.
"Given that these rates are based on the results of rigorous studies, they may represent a lower incidence than actual rates observed in clinical practice, in which patients are selected less rigorously and prophylaxis is administered less assiduously," Mr. Januel and his associates noted.
The pooled incidence rates of deep vein thrombosis were lower for both knee patients and hip patients when factor Xa or IIa inhibitors, rather than low-molecular-weight heparin, were given for prophylaxis. "However, we cannot make assertions regarding comparative efficacy among treatments, because our meta-analysis did not directly compare [these agents] as an efficacy meta-analysis would have done," they said.
This study was supported by Alberta Innovates Health Solutions, a government research funding agency, and the International Methodology Consortium for Coded Health Information, a collaboration of health sciences researchers to promote quality of care. Dr. Heit reported ties to Daiichi Sankyo, GTC, Ortho-McNeil-Jansen, the National Heart, Lung, and Blood Institute, the National Human Genome Research Institute, the National Institutes of Health, the Centers for Disease Control and Prevention, and the Mayo Foundation.
The in-hospital VTE rates reported by Januel et al may be "suboptimal" for assessing both patients’ risks and a facility’s performance in patient safety, as the investigators proposed, said Dr. John A. Heit.
The period of VTE risks extends far beyond the hospital stay, with as many as 76% of VTE events occurring during the 3 months following hospital discharge. "From the perspective of the patient contemplating elective total hip replacement or total knee replacement," the 3-month rate rather than the in-hospital rate of VTE is more important in weighing risks and benefits, he said.
And it can be argued that this cumulative rate of VTE is also more important for the purpose of assessing a facility’s performance, Dr. Heit added.
Dr. Heit is in the division of cardiovascular diseases at the Mayo Clinic, Rochester, Minn. He reported ties to Daiichi Sankyo, GTC, Ortho-McNeil-Jansen, the National Heart, Lung, and Blood Institute, the National Human Genome Research Institute, the National Institutes of Health, the Centers for Disease Control and Prevention, and the Mayo Foundation. These remarks were taken from his editorial accompanying Mr. Januel’s report (JAMA 2012;307:306-7).
The in-hospital VTE rates reported by Januel et al may be "suboptimal" for assessing both patients’ risks and a facility’s performance in patient safety, as the investigators proposed, said Dr. John A. Heit.
The period of VTE risks extends far beyond the hospital stay, with as many as 76% of VTE events occurring during the 3 months following hospital discharge. "From the perspective of the patient contemplating elective total hip replacement or total knee replacement," the 3-month rate rather than the in-hospital rate of VTE is more important in weighing risks and benefits, he said.
And it can be argued that this cumulative rate of VTE is also more important for the purpose of assessing a facility’s performance, Dr. Heit added.
Dr. Heit is in the division of cardiovascular diseases at the Mayo Clinic, Rochester, Minn. He reported ties to Daiichi Sankyo, GTC, Ortho-McNeil-Jansen, the National Heart, Lung, and Blood Institute, the National Human Genome Research Institute, the National Institutes of Health, the Centers for Disease Control and Prevention, and the Mayo Foundation. These remarks were taken from his editorial accompanying Mr. Januel’s report (JAMA 2012;307:306-7).
The in-hospital VTE rates reported by Januel et al may be "suboptimal" for assessing both patients’ risks and a facility’s performance in patient safety, as the investigators proposed, said Dr. John A. Heit.
The period of VTE risks extends far beyond the hospital stay, with as many as 76% of VTE events occurring during the 3 months following hospital discharge. "From the perspective of the patient contemplating elective total hip replacement or total knee replacement," the 3-month rate rather than the in-hospital rate of VTE is more important in weighing risks and benefits, he said.
And it can be argued that this cumulative rate of VTE is also more important for the purpose of assessing a facility’s performance, Dr. Heit added.
Dr. Heit is in the division of cardiovascular diseases at the Mayo Clinic, Rochester, Minn. He reported ties to Daiichi Sankyo, GTC, Ortho-McNeil-Jansen, the National Heart, Lung, and Blood Institute, the National Human Genome Research Institute, the National Institutes of Health, the Centers for Disease Control and Prevention, and the Mayo Foundation. These remarks were taken from his editorial accompanying Mr. Januel’s report (JAMA 2012;307:306-7).
For the first time, researchers say they have established benchmarks for the rates of in-hospital venous thromboembolism that occur after total or partial hip arthroplasty and after total or partial knee arthroplasty, according to a report Jan. 18 in JAMA.
In a meta-analysis of 47 studies that documented venous thromboembolism (VTE) event rates in nearly 45,000 patients who received recommended prophylaxis during hospitalization for knee or hip arthroplasty, investigators estimated that approximately 1 in every 100 patients undergoing knee arthroplasty and 1 in every 200 undergoing hip arthroplasty will develop symptomatic VTE before they are discharged.
"These estimates are of value to individual patients and clinicians in the consideration of risks and benefits" of the two procedures. They also are important because rates of in-hospital VTE are increasingly used as indicators of patient safety at individual medical centers, even though the expected background rates haven’t been established until now, said Jean-Marie Januel, a registered nurse with the Institute of Social and Preventive Medicine, Lausanne (Switzerland) University Hospital, and his associates.
"Large numbers of patients worldwide undergo hip and knee replacement procedures annually, and VTE is a widely acknowledged complication. Yet no estimate of symptomatic VTE risk prior to hospital discharge is available from the literature that can be conveyed to patients in the informed consent process," they noted.
Mr. Januel and his colleagues performed a systemic search of the literature to identify studies performed between 1996 and 2011 in which subjects undergoing either hip or knee arthroplasty received VTE prophylaxis according to published guidelines, including either low-molecular-weight heparin or inhibitors of factor Xa or IIa. They found 41 randomized clinical trials and 6 observational studies to include in the meta-analysis.
A total of 22 of the studies were performed in Europe, 14 were in North America, and 11 were in other regions. The mean duration of follow-up after either surgery was 13 days.
This included 21 studies of partial or total hip arthroplasty, 20 of partial or total knee arthroplasty, and 6 studies of both procedures, with a total of 44,844 subjects.
There were 443 cases of symptomatic postoperative VTE that developed before hospital discharge: 288 in the 23,475 knee patients and 155 in the 23,475 hip patients. This included 182 cases of deep vein thrombosis in the knee patients and 93 in the hip patients, as well as 106 cases of pulmonary embolism in the knee patients and 43 in the hip patients.
The pooled incidence rates of VTE were approximately 1% after knee arthroplasty and approximately 0.5% after hip arthroplasty. This means that the background rate of VTE is approximately 1 in 100 knee patients and 1 in 200 hip patients, the investigators said (JAMA 2012;307:294-303).
When the data were broken down by type of VTE, the pooled incidence rates were 0.26% for deep vein thrombosis and 0.14% for pulmonary embolism after knee arthroplasty. The corresponding rates were 0.63% for deep vein thrombosis and 0.27% for pulmonary embolism after hip arthroplasty.
"Given that these rates are based on the results of rigorous studies, they may represent a lower incidence than actual rates observed in clinical practice, in which patients are selected less rigorously and prophylaxis is administered less assiduously," Mr. Januel and his associates noted.
The pooled incidence rates of deep vein thrombosis were lower for both knee patients and hip patients when factor Xa or IIa inhibitors, rather than low-molecular-weight heparin, were given for prophylaxis. "However, we cannot make assertions regarding comparative efficacy among treatments, because our meta-analysis did not directly compare [these agents] as an efficacy meta-analysis would have done," they said.
This study was supported by Alberta Innovates Health Solutions, a government research funding agency, and the International Methodology Consortium for Coded Health Information, a collaboration of health sciences researchers to promote quality of care. Dr. Heit reported ties to Daiichi Sankyo, GTC, Ortho-McNeil-Jansen, the National Heart, Lung, and Blood Institute, the National Human Genome Research Institute, the National Institutes of Health, the Centers for Disease Control and Prevention, and the Mayo Foundation.
For the first time, researchers say they have established benchmarks for the rates of in-hospital venous thromboembolism that occur after total or partial hip arthroplasty and after total or partial knee arthroplasty, according to a report Jan. 18 in JAMA.
In a meta-analysis of 47 studies that documented venous thromboembolism (VTE) event rates in nearly 45,000 patients who received recommended prophylaxis during hospitalization for knee or hip arthroplasty, investigators estimated that approximately 1 in every 100 patients undergoing knee arthroplasty and 1 in every 200 undergoing hip arthroplasty will develop symptomatic VTE before they are discharged.
"These estimates are of value to individual patients and clinicians in the consideration of risks and benefits" of the two procedures. They also are important because rates of in-hospital VTE are increasingly used as indicators of patient safety at individual medical centers, even though the expected background rates haven’t been established until now, said Jean-Marie Januel, a registered nurse with the Institute of Social and Preventive Medicine, Lausanne (Switzerland) University Hospital, and his associates.
"Large numbers of patients worldwide undergo hip and knee replacement procedures annually, and VTE is a widely acknowledged complication. Yet no estimate of symptomatic VTE risk prior to hospital discharge is available from the literature that can be conveyed to patients in the informed consent process," they noted.
Mr. Januel and his colleagues performed a systemic search of the literature to identify studies performed between 1996 and 2011 in which subjects undergoing either hip or knee arthroplasty received VTE prophylaxis according to published guidelines, including either low-molecular-weight heparin or inhibitors of factor Xa or IIa. They found 41 randomized clinical trials and 6 observational studies to include in the meta-analysis.
A total of 22 of the studies were performed in Europe, 14 were in North America, and 11 were in other regions. The mean duration of follow-up after either surgery was 13 days.
This included 21 studies of partial or total hip arthroplasty, 20 of partial or total knee arthroplasty, and 6 studies of both procedures, with a total of 44,844 subjects.
There were 443 cases of symptomatic postoperative VTE that developed before hospital discharge: 288 in the 23,475 knee patients and 155 in the 23,475 hip patients. This included 182 cases of deep vein thrombosis in the knee patients and 93 in the hip patients, as well as 106 cases of pulmonary embolism in the knee patients and 43 in the hip patients.
The pooled incidence rates of VTE were approximately 1% after knee arthroplasty and approximately 0.5% after hip arthroplasty. This means that the background rate of VTE is approximately 1 in 100 knee patients and 1 in 200 hip patients, the investigators said (JAMA 2012;307:294-303).
When the data were broken down by type of VTE, the pooled incidence rates were 0.26% for deep vein thrombosis and 0.14% for pulmonary embolism after knee arthroplasty. The corresponding rates were 0.63% for deep vein thrombosis and 0.27% for pulmonary embolism after hip arthroplasty.
"Given that these rates are based on the results of rigorous studies, they may represent a lower incidence than actual rates observed in clinical practice, in which patients are selected less rigorously and prophylaxis is administered less assiduously," Mr. Januel and his associates noted.
The pooled incidence rates of deep vein thrombosis were lower for both knee patients and hip patients when factor Xa or IIa inhibitors, rather than low-molecular-weight heparin, were given for prophylaxis. "However, we cannot make assertions regarding comparative efficacy among treatments, because our meta-analysis did not directly compare [these agents] as an efficacy meta-analysis would have done," they said.
This study was supported by Alberta Innovates Health Solutions, a government research funding agency, and the International Methodology Consortium for Coded Health Information, a collaboration of health sciences researchers to promote quality of care. Dr. Heit reported ties to Daiichi Sankyo, GTC, Ortho-McNeil-Jansen, the National Heart, Lung, and Blood Institute, the National Human Genome Research Institute, the National Institutes of Health, the Centers for Disease Control and Prevention, and the Mayo Foundation.
FROM JAMA
Major Finding: 443 cases of VTE developed during hospitalization, for an incidence of approximately 1 in every 100 patients undergoing knee arthroplasty and 1 in every 200 patients undergoing hip arthroplasty.
Data Source: A meta-analysis of 47 randomized clinical trials and observational studies from 1996 to 2011 that documented VTE rates in 44,844 patients undergoing total or partial hip or knee arthroplasty.
Disclosures: This study was supported by Alberta Innovates Health Solutions, a government research funding agency, and the International Methodology Consortium for Coded Health Information, a collaboration of health sciences researchers to promote quality of care. No financial conflicts of interest were reported.
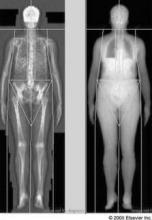
Weight Loss Higher After Roux-en-Y Surgery vs. Gastric Banding
Roux-en-Y gastric bypass surgery resulted in greater, more rapid, and more sustained weight loss compared with gastric banding, but also a higher number of complications in a matched-pair study published online Jan. 16 in Archives of Surgery.
The weight loss advantage achieved with Roux-en-Y leads to better correction of the comorbidities that accompany obesity, such as adverse lipid profiles and high fasting glucose levels, said Dr. Sébastein Romy of the department of visceral surgery, Centre Hospitalier Universitaire Vaudois, Lausanne, Switzerland, and his associates.
Although there are more early complications with the Roux-en-Y procedure, they are outweighed by "the much higher long-term major morbidity seen after gastric bypass, leading to a large number of major reoperations and their risks," the investigators noted.
The sharp rise in bariatric surgeries performed in recent years in the United States has occurred predominantly in gastric banding procedures. "This is probably because gastric banding is perceived both by doctors and patients as a simple, safe, and reversible operation but also because of a huge industry-driven marketing campaign," they said.
Which surgery is "better" has been contested. To date, among the 17 published studies comparing the two procedures, many have had important methodologic flaws such as small numbers of patients and very limited follow-up.
Dr. Romy and his colleagues performed a matched-pair analysis of patients who underwent the two procedures in 1998-2005. The study subjects, who had failed to lose weight with more conservative approaches, all had a body mass index of 40 or more, or a BMI of 35 plus at least one severe comorbidity. A total of 221 patients who underwent Roux-en-Y gastric bypass were matched for age, sex, and BMI with 221 who underwent gastric banding. Follow-up rates after 6 years were approximately 92% in both groups. The same team performed the operations at the same two hospitals.
Maximal weight loss was achieved at a mean of 18 months after Roux-en-Y gastric bypass, compared with 36 months after gastric banding. The percentage of excess weight lost was significantly higher after Roux-en-Y (78.5%) than after gastric banding (64.8%), and the mean nadir in BMI was significantly lower (26.7 vs. 29.4, respectively). After 6 years, only 5 patients (2.4%) in the Roux-en-Y group had a BMI greater than 40, compared with 21 patients (13.8%) in the gastric banding group.
As a result, significantly more patients who had Roux-en-Y surgery were rated as having excellent or acceptable results at all time points during follow-up, Dr. Romy and his associates said (Arch. Surg. 2012 Jan. 16 [doi:10.1001/archsurg.2011.1708]).
Treatment failures were defined as a weight loss of less than 25% of baseline weight or the need to reverse the surgery or convert to a different bariatric procedure. At the 3-year mark, there were no treatment failures among Roux-en-Y patients, compared with 39 treatment failures (18.2%) among gastric banding patients. After 6 years, failure rates were 2.5% and 38.9%, respectively, in Roux-en-Y and gastric banding patients.
Improvement in lipid profiles was significantly greater after Roux-en-Y than after gastric banding. Total cholesterol, LDL cholesterol, and triglyceride levels decreased after Roux-en-Y but not after gastric banding. Fasting glucose levels also were lower after Roux-en-Y (89.55 mg/dL vs. 92.79 mg/dL).
Quality of life improved in both groups, but the improvement was significantly faster and persisted for a longer time after Roux-en-Y surgery. In particular, Roux-en-Y patients had much better food tolerance, with no worsening after surgery, whereas food tolerance tended to worsen over time after gastric banding.
There were significantly more early complications after Roux-en-Y (17.2%) than after gastric banding (5.4%), which is not surprising given that Roux-en-Y is a more complex operation and requires a longer operative time and longer hospitalization. However, most of these early complications required only conservative treatment, and there was no significant difference between the two groups in early major complications, the researchers said.
In contrast, gastric banding was associated with significantly more long-term complications than was Roux-en-Y (41.6% vs. 19%) and required more than twice as many reoperations (26.7% vs. 12.7%).
"After gastric banding, functional problems like esophageal dilatation (10.4%), impairing reflux requiring (or resistant to) daily high-dose proton-pump inhibitor therapy (6.8%), or severe food intolerance (6.3%) accounted for the majority of long-term complications, together with band erosions (7.7%). Overall, band removal was necessary in 47 patients (21.3%)," they said.
"Long-term complications after Roux-en-Y gastric bypass are essentially limited to anastomotic strictures and bowel obstructions and symptomatic internal hernia." Most strictures were not considered major complications, requiring only endoscopic dilatation. Although bowel obstruction is potentially life threatening, in most cases it doesn’t jeopardize the bypass or require reversal, Dr. Romy and his colleagues said.
No financial conflicts of interest were reported by the researchers.
"I personally agree" with Romy et al. that Roux-en-Y gastric bypass is the better procedure, but "before we make from this conclusion a paradigm, a few caveats remain," said Dr. Jacques Himpens.
A case-control study such as this one may be biased. Even though a prospective randomized trial comparing the two surgeries isn’t feasible, a prospective rather than retrospective comparison of matched patients would yield better evidence, as would a multicenter rather than a single-center study.
In addition, a growing number of Roux-en-Y patients are showing neuroglycopenia and diabetes recurrence several years after surgery, which is concerning.
Dr. Himpens is at the European School of Laparoscopy at Saint Pierre University Hospital, Brussels. He reported being a consultant for Ethicon Endo-Surgery, Covidien, and Gore. These remarks were taken from his invited critique that accompanied Dr. Romy’s article (Arch. Surg. 2012 Jan. 16 [doi:10.1001/archsurg.2011.1855]).
"I personally agree" with Romy et al. that Roux-en-Y gastric bypass is the better procedure, but "before we make from this conclusion a paradigm, a few caveats remain," said Dr. Jacques Himpens.
A case-control study such as this one may be biased. Even though a prospective randomized trial comparing the two surgeries isn’t feasible, a prospective rather than retrospective comparison of matched patients would yield better evidence, as would a multicenter rather than a single-center study.
In addition, a growing number of Roux-en-Y patients are showing neuroglycopenia and diabetes recurrence several years after surgery, which is concerning.
Dr. Himpens is at the European School of Laparoscopy at Saint Pierre University Hospital, Brussels. He reported being a consultant for Ethicon Endo-Surgery, Covidien, and Gore. These remarks were taken from his invited critique that accompanied Dr. Romy’s article (Arch. Surg. 2012 Jan. 16 [doi:10.1001/archsurg.2011.1855]).
"I personally agree" with Romy et al. that Roux-en-Y gastric bypass is the better procedure, but "before we make from this conclusion a paradigm, a few caveats remain," said Dr. Jacques Himpens.
A case-control study such as this one may be biased. Even though a prospective randomized trial comparing the two surgeries isn’t feasible, a prospective rather than retrospective comparison of matched patients would yield better evidence, as would a multicenter rather than a single-center study.
In addition, a growing number of Roux-en-Y patients are showing neuroglycopenia and diabetes recurrence several years after surgery, which is concerning.
Dr. Himpens is at the European School of Laparoscopy at Saint Pierre University Hospital, Brussels. He reported being a consultant for Ethicon Endo-Surgery, Covidien, and Gore. These remarks were taken from his invited critique that accompanied Dr. Romy’s article (Arch. Surg. 2012 Jan. 16 [doi:10.1001/archsurg.2011.1855]).
Roux-en-Y gastric bypass surgery resulted in greater, more rapid, and more sustained weight loss compared with gastric banding, but also a higher number of complications in a matched-pair study published online Jan. 16 in Archives of Surgery.
The weight loss advantage achieved with Roux-en-Y leads to better correction of the comorbidities that accompany obesity, such as adverse lipid profiles and high fasting glucose levels, said Dr. Sébastein Romy of the department of visceral surgery, Centre Hospitalier Universitaire Vaudois, Lausanne, Switzerland, and his associates.
Although there are more early complications with the Roux-en-Y procedure, they are outweighed by "the much higher long-term major morbidity seen after gastric bypass, leading to a large number of major reoperations and their risks," the investigators noted.
The sharp rise in bariatric surgeries performed in recent years in the United States has occurred predominantly in gastric banding procedures. "This is probably because gastric banding is perceived both by doctors and patients as a simple, safe, and reversible operation but also because of a huge industry-driven marketing campaign," they said.
Which surgery is "better" has been contested. To date, among the 17 published studies comparing the two procedures, many have had important methodologic flaws such as small numbers of patients and very limited follow-up.
Dr. Romy and his colleagues performed a matched-pair analysis of patients who underwent the two procedures in 1998-2005. The study subjects, who had failed to lose weight with more conservative approaches, all had a body mass index of 40 or more, or a BMI of 35 plus at least one severe comorbidity. A total of 221 patients who underwent Roux-en-Y gastric bypass were matched for age, sex, and BMI with 221 who underwent gastric banding. Follow-up rates after 6 years were approximately 92% in both groups. The same team performed the operations at the same two hospitals.
Maximal weight loss was achieved at a mean of 18 months after Roux-en-Y gastric bypass, compared with 36 months after gastric banding. The percentage of excess weight lost was significantly higher after Roux-en-Y (78.5%) than after gastric banding (64.8%), and the mean nadir in BMI was significantly lower (26.7 vs. 29.4, respectively). After 6 years, only 5 patients (2.4%) in the Roux-en-Y group had a BMI greater than 40, compared with 21 patients (13.8%) in the gastric banding group.
As a result, significantly more patients who had Roux-en-Y surgery were rated as having excellent or acceptable results at all time points during follow-up, Dr. Romy and his associates said (Arch. Surg. 2012 Jan. 16 [doi:10.1001/archsurg.2011.1708]).
Treatment failures were defined as a weight loss of less than 25% of baseline weight or the need to reverse the surgery or convert to a different bariatric procedure. At the 3-year mark, there were no treatment failures among Roux-en-Y patients, compared with 39 treatment failures (18.2%) among gastric banding patients. After 6 years, failure rates were 2.5% and 38.9%, respectively, in Roux-en-Y and gastric banding patients.
Improvement in lipid profiles was significantly greater after Roux-en-Y than after gastric banding. Total cholesterol, LDL cholesterol, and triglyceride levels decreased after Roux-en-Y but not after gastric banding. Fasting glucose levels also were lower after Roux-en-Y (89.55 mg/dL vs. 92.79 mg/dL).
Quality of life improved in both groups, but the improvement was significantly faster and persisted for a longer time after Roux-en-Y surgery. In particular, Roux-en-Y patients had much better food tolerance, with no worsening after surgery, whereas food tolerance tended to worsen over time after gastric banding.
There were significantly more early complications after Roux-en-Y (17.2%) than after gastric banding (5.4%), which is not surprising given that Roux-en-Y is a more complex operation and requires a longer operative time and longer hospitalization. However, most of these early complications required only conservative treatment, and there was no significant difference between the two groups in early major complications, the researchers said.
In contrast, gastric banding was associated with significantly more long-term complications than was Roux-en-Y (41.6% vs. 19%) and required more than twice as many reoperations (26.7% vs. 12.7%).
"After gastric banding, functional problems like esophageal dilatation (10.4%), impairing reflux requiring (or resistant to) daily high-dose proton-pump inhibitor therapy (6.8%), or severe food intolerance (6.3%) accounted for the majority of long-term complications, together with band erosions (7.7%). Overall, band removal was necessary in 47 patients (21.3%)," they said.
"Long-term complications after Roux-en-Y gastric bypass are essentially limited to anastomotic strictures and bowel obstructions and symptomatic internal hernia." Most strictures were not considered major complications, requiring only endoscopic dilatation. Although bowel obstruction is potentially life threatening, in most cases it doesn’t jeopardize the bypass or require reversal, Dr. Romy and his colleagues said.
No financial conflicts of interest were reported by the researchers.
Roux-en-Y gastric bypass surgery resulted in greater, more rapid, and more sustained weight loss compared with gastric banding, but also a higher number of complications in a matched-pair study published online Jan. 16 in Archives of Surgery.
The weight loss advantage achieved with Roux-en-Y leads to better correction of the comorbidities that accompany obesity, such as adverse lipid profiles and high fasting glucose levels, said Dr. Sébastein Romy of the department of visceral surgery, Centre Hospitalier Universitaire Vaudois, Lausanne, Switzerland, and his associates.
Although there are more early complications with the Roux-en-Y procedure, they are outweighed by "the much higher long-term major morbidity seen after gastric bypass, leading to a large number of major reoperations and their risks," the investigators noted.
The sharp rise in bariatric surgeries performed in recent years in the United States has occurred predominantly in gastric banding procedures. "This is probably because gastric banding is perceived both by doctors and patients as a simple, safe, and reversible operation but also because of a huge industry-driven marketing campaign," they said.
Which surgery is "better" has been contested. To date, among the 17 published studies comparing the two procedures, many have had important methodologic flaws such as small numbers of patients and very limited follow-up.
Dr. Romy and his colleagues performed a matched-pair analysis of patients who underwent the two procedures in 1998-2005. The study subjects, who had failed to lose weight with more conservative approaches, all had a body mass index of 40 or more, or a BMI of 35 plus at least one severe comorbidity. A total of 221 patients who underwent Roux-en-Y gastric bypass were matched for age, sex, and BMI with 221 who underwent gastric banding. Follow-up rates after 6 years were approximately 92% in both groups. The same team performed the operations at the same two hospitals.
Maximal weight loss was achieved at a mean of 18 months after Roux-en-Y gastric bypass, compared with 36 months after gastric banding. The percentage of excess weight lost was significantly higher after Roux-en-Y (78.5%) than after gastric banding (64.8%), and the mean nadir in BMI was significantly lower (26.7 vs. 29.4, respectively). After 6 years, only 5 patients (2.4%) in the Roux-en-Y group had a BMI greater than 40, compared with 21 patients (13.8%) in the gastric banding group.
As a result, significantly more patients who had Roux-en-Y surgery were rated as having excellent or acceptable results at all time points during follow-up, Dr. Romy and his associates said (Arch. Surg. 2012 Jan. 16 [doi:10.1001/archsurg.2011.1708]).
Treatment failures were defined as a weight loss of less than 25% of baseline weight or the need to reverse the surgery or convert to a different bariatric procedure. At the 3-year mark, there were no treatment failures among Roux-en-Y patients, compared with 39 treatment failures (18.2%) among gastric banding patients. After 6 years, failure rates were 2.5% and 38.9%, respectively, in Roux-en-Y and gastric banding patients.
Improvement in lipid profiles was significantly greater after Roux-en-Y than after gastric banding. Total cholesterol, LDL cholesterol, and triglyceride levels decreased after Roux-en-Y but not after gastric banding. Fasting glucose levels also were lower after Roux-en-Y (89.55 mg/dL vs. 92.79 mg/dL).
Quality of life improved in both groups, but the improvement was significantly faster and persisted for a longer time after Roux-en-Y surgery. In particular, Roux-en-Y patients had much better food tolerance, with no worsening after surgery, whereas food tolerance tended to worsen over time after gastric banding.
There were significantly more early complications after Roux-en-Y (17.2%) than after gastric banding (5.4%), which is not surprising given that Roux-en-Y is a more complex operation and requires a longer operative time and longer hospitalization. However, most of these early complications required only conservative treatment, and there was no significant difference between the two groups in early major complications, the researchers said.
In contrast, gastric banding was associated with significantly more long-term complications than was Roux-en-Y (41.6% vs. 19%) and required more than twice as many reoperations (26.7% vs. 12.7%).
"After gastric banding, functional problems like esophageal dilatation (10.4%), impairing reflux requiring (or resistant to) daily high-dose proton-pump inhibitor therapy (6.8%), or severe food intolerance (6.3%) accounted for the majority of long-term complications, together with band erosions (7.7%). Overall, band removal was necessary in 47 patients (21.3%)," they said.
"Long-term complications after Roux-en-Y gastric bypass are essentially limited to anastomotic strictures and bowel obstructions and symptomatic internal hernia." Most strictures were not considered major complications, requiring only endoscopic dilatation. Although bowel obstruction is potentially life threatening, in most cases it doesn’t jeopardize the bypass or require reversal, Dr. Romy and his colleagues said.
No financial conflicts of interest were reported by the researchers.
FROM ARCHIVES OF SURGERY
Major Finding: Patients lost 78.5% of excess weight after Roux-en-Y gastric bypass vs. 64.8% after gastric banding, and the treatment failure rate after 6 years was 2.5% vs. 38.9%, respectively.
Data Source: A retrospective matched-pair study of 221 Roux-en-Y gastric bypass patients and 221 gastric banding patients at a single center who were followed for at least 6 years.
Disclosures: No financial conflicts of interest were reported.
Marathon Runners Are at Low Risk of Cardiac Arrest
Marathon runners’ risk of cardiac arrest is relatively low – equivalent to or lower than that of other athletes engaged in vigorous activity, according to a report in the Jan. 12 issue of the New England Journal of Medicine.
The number of cardiac arrests related to marathon (26.2-mile) and half-marathon (13.1-mile) races has increased in recent years, but that is largely explained by the increase in the number of people who have taken up the sport, said Dr. Jonathan H. Kim of the division of cardiology, Massachusetts General Hospital, Boston, and his associates.
"The growth of long-distance running has been accompanied by studies documenting post-race cardiac dysfunction and numerous reports of race-related cardiac arrest. These unexpected tragedies attract considerable media attention and have led to concerns regarding the health risks of this activity," the researchers wrote.
Until now, no large studies have examined the incidence, clinical profiles, and outcomes of cardiac arrests that occur during or immediately after long-distances races. The Race Associated Cardiac Arrest Event Registry (RACER) collected data to facilitate such studies. It included information on all marathon or half-marathon races held in the United States between 2000 and May 2010.
Dr. Kim and his associates in the RACER study group identified 59 marathon-related cardiac arrests (out of 10.9 million registered marathon runners) during this period and contacted survivors, as well as the next of kin of nonsurvivors, to ascertain demographic data, exercise history, personal and family medical histories, and pertinent medical records.
The overall incidence of cardiac arrest was 1 per 184,000 participants, and that of sudden death was 1 per 259,000 participants. This translates to 0.2 cardiac arrests and 0.14 sudden deaths per 100,000 runner-hours at risk, assuming an average running time of 4 hours for marathons and 2 hours for half-marathons.
"Thus, event rates among marathon and half-marathon runners are relatively low, as compared with other athletic populations, including collegiate athletes (1 death per 43,770 participants per year), triathlon participants (1 death per 52,630 participants), and previously healthy middle-aged joggers (1 death per 7,620 participants)," the researchers wrote (N. Engl. J. Med. 2012;366:130-40).
The absolute number of marathon-related cardiac arrests rose each year during the study period, but the incidence remained stable because of an annual increase in runners from fewer than 1 million in 2000 to approximately 2 million in 2010, according to the investigators.
Men were more likely than were women runners to have a cardiac arrest or sudden death (0.90 per 100,000 vs. 0.16 per 100,000), which the authors noted is "consistent with reports on other populations and reaffirms a male predisposition to exertional cardiac arrest."
The distance of a race was a key determinant of the risk of cardiac arrest, since rates were three to five times higher during marathons (1.01 per 100,000 runners) than during half-marathons (0.27 per 100,000). "A possible explanation is that longer races involve more physiological stress and thus a higher likelihood of precipitating an adverse event in a predisposed participant," the researchers wrote.
The overall case fatality rate was 71%. Sufficient information was available to determine the cause of cardiac arrest in only 31 of the 59 cases.
The most frequent cause of death was hypertrophic cardiomyopathy (8 cases) or possible hypertrophic cardiomyopathy (7 cases). This is also the primary cause of death in young competitive athletes, they pointed out.
"Notably, 9 of the 15 nonsurvivors who had cardiac hypertrophy had an additional clinical factor or postmortem finding: obstructive coronary artery disease (in 3), myocarditis (in 2), bicuspid aortic valve or coronary anomaly (in 2), accessory atrioventricular nodal bypass tract (in 1), or hyperthermia (in 1)," the researchers wrote. The race-related disorders of hyperthermia and hyponatremia, which led to the death of one runner without cardiac hypertrophy, thus are not common causes of cardiac arrest and sudden death, they added.
Among the eight survivors of cardiac arrest, ischemic heart disease was the most frequent cause of the arrest. The strongest predictor of survival of cardiac arrest was bystander-administered CPR, underscoring the importance of onsite medical services.
It was "surprising" that none of the runners with serious coronary atherosclerosis had angiographic evidence of acute plaque rupture or thrombus, because previous studies as well as expert consensus statements have suggest that exercise-induced coronary syndromes result from disruption of atherosclerotic plaque and coronary thrombosis. "In contrast, our findings suggest that demand ischemia (i.e., ischemia due to an imbalance between oxygen supply and demand) may be operative in exercise-related acute coronary events during long-distance running races," they wrote.
This finding also suggests that the practice of taking aspirin before a race to prevent cardiac arrest is likely ineffective, since acute coronary artery thrombosis is not an important cause of marathon-related cardiac arrest, they added.
Physicians called on to evaluate potential marathon participants "should be aware of the risks of hypertrophic cardiomyopathy and atherosclerotic disease in this patient population." Prerace exercise testing may detect physiologically significant coronary artery stenosis or may identify patients with exertion-induced myocardial ischemia, the investigators said.
This study was limited in that the researchers were unable to obtain complete clinical information on 45% of the nonsurvivors or on 53% of the survivors.
Dr. Kim reported no financial conflicts of interest, but two of his coauthors reported ties to industry sources.
Marathon runners’ risk of cardiac arrest is relatively low – equivalent to or lower than that of other athletes engaged in vigorous activity, according to a report in the Jan. 12 issue of the New England Journal of Medicine.
The number of cardiac arrests related to marathon (26.2-mile) and half-marathon (13.1-mile) races has increased in recent years, but that is largely explained by the increase in the number of people who have taken up the sport, said Dr. Jonathan H. Kim of the division of cardiology, Massachusetts General Hospital, Boston, and his associates.
"The growth of long-distance running has been accompanied by studies documenting post-race cardiac dysfunction and numerous reports of race-related cardiac arrest. These unexpected tragedies attract considerable media attention and have led to concerns regarding the health risks of this activity," the researchers wrote.
Until now, no large studies have examined the incidence, clinical profiles, and outcomes of cardiac arrests that occur during or immediately after long-distances races. The Race Associated Cardiac Arrest Event Registry (RACER) collected data to facilitate such studies. It included information on all marathon or half-marathon races held in the United States between 2000 and May 2010.
Dr. Kim and his associates in the RACER study group identified 59 marathon-related cardiac arrests (out of 10.9 million registered marathon runners) during this period and contacted survivors, as well as the next of kin of nonsurvivors, to ascertain demographic data, exercise history, personal and family medical histories, and pertinent medical records.
The overall incidence of cardiac arrest was 1 per 184,000 participants, and that of sudden death was 1 per 259,000 participants. This translates to 0.2 cardiac arrests and 0.14 sudden deaths per 100,000 runner-hours at risk, assuming an average running time of 4 hours for marathons and 2 hours for half-marathons.
"Thus, event rates among marathon and half-marathon runners are relatively low, as compared with other athletic populations, including collegiate athletes (1 death per 43,770 participants per year), triathlon participants (1 death per 52,630 participants), and previously healthy middle-aged joggers (1 death per 7,620 participants)," the researchers wrote (N. Engl. J. Med. 2012;366:130-40).
The absolute number of marathon-related cardiac arrests rose each year during the study period, but the incidence remained stable because of an annual increase in runners from fewer than 1 million in 2000 to approximately 2 million in 2010, according to the investigators.
Men were more likely than were women runners to have a cardiac arrest or sudden death (0.90 per 100,000 vs. 0.16 per 100,000), which the authors noted is "consistent with reports on other populations and reaffirms a male predisposition to exertional cardiac arrest."
The distance of a race was a key determinant of the risk of cardiac arrest, since rates were three to five times higher during marathons (1.01 per 100,000 runners) than during half-marathons (0.27 per 100,000). "A possible explanation is that longer races involve more physiological stress and thus a higher likelihood of precipitating an adverse event in a predisposed participant," the researchers wrote.
The overall case fatality rate was 71%. Sufficient information was available to determine the cause of cardiac arrest in only 31 of the 59 cases.
The most frequent cause of death was hypertrophic cardiomyopathy (8 cases) or possible hypertrophic cardiomyopathy (7 cases). This is also the primary cause of death in young competitive athletes, they pointed out.
"Notably, 9 of the 15 nonsurvivors who had cardiac hypertrophy had an additional clinical factor or postmortem finding: obstructive coronary artery disease (in 3), myocarditis (in 2), bicuspid aortic valve or coronary anomaly (in 2), accessory atrioventricular nodal bypass tract (in 1), or hyperthermia (in 1)," the researchers wrote. The race-related disorders of hyperthermia and hyponatremia, which led to the death of one runner without cardiac hypertrophy, thus are not common causes of cardiac arrest and sudden death, they added.
Among the eight survivors of cardiac arrest, ischemic heart disease was the most frequent cause of the arrest. The strongest predictor of survival of cardiac arrest was bystander-administered CPR, underscoring the importance of onsite medical services.
It was "surprising" that none of the runners with serious coronary atherosclerosis had angiographic evidence of acute plaque rupture or thrombus, because previous studies as well as expert consensus statements have suggest that exercise-induced coronary syndromes result from disruption of atherosclerotic plaque and coronary thrombosis. "In contrast, our findings suggest that demand ischemia (i.e., ischemia due to an imbalance between oxygen supply and demand) may be operative in exercise-related acute coronary events during long-distance running races," they wrote.
This finding also suggests that the practice of taking aspirin before a race to prevent cardiac arrest is likely ineffective, since acute coronary artery thrombosis is not an important cause of marathon-related cardiac arrest, they added.
Physicians called on to evaluate potential marathon participants "should be aware of the risks of hypertrophic cardiomyopathy and atherosclerotic disease in this patient population." Prerace exercise testing may detect physiologically significant coronary artery stenosis or may identify patients with exertion-induced myocardial ischemia, the investigators said.
This study was limited in that the researchers were unable to obtain complete clinical information on 45% of the nonsurvivors or on 53% of the survivors.
Dr. Kim reported no financial conflicts of interest, but two of his coauthors reported ties to industry sources.
Marathon runners’ risk of cardiac arrest is relatively low – equivalent to or lower than that of other athletes engaged in vigorous activity, according to a report in the Jan. 12 issue of the New England Journal of Medicine.
The number of cardiac arrests related to marathon (26.2-mile) and half-marathon (13.1-mile) races has increased in recent years, but that is largely explained by the increase in the number of people who have taken up the sport, said Dr. Jonathan H. Kim of the division of cardiology, Massachusetts General Hospital, Boston, and his associates.
"The growth of long-distance running has been accompanied by studies documenting post-race cardiac dysfunction and numerous reports of race-related cardiac arrest. These unexpected tragedies attract considerable media attention and have led to concerns regarding the health risks of this activity," the researchers wrote.
Until now, no large studies have examined the incidence, clinical profiles, and outcomes of cardiac arrests that occur during or immediately after long-distances races. The Race Associated Cardiac Arrest Event Registry (RACER) collected data to facilitate such studies. It included information on all marathon or half-marathon races held in the United States between 2000 and May 2010.
Dr. Kim and his associates in the RACER study group identified 59 marathon-related cardiac arrests (out of 10.9 million registered marathon runners) during this period and contacted survivors, as well as the next of kin of nonsurvivors, to ascertain demographic data, exercise history, personal and family medical histories, and pertinent medical records.
The overall incidence of cardiac arrest was 1 per 184,000 participants, and that of sudden death was 1 per 259,000 participants. This translates to 0.2 cardiac arrests and 0.14 sudden deaths per 100,000 runner-hours at risk, assuming an average running time of 4 hours for marathons and 2 hours for half-marathons.
"Thus, event rates among marathon and half-marathon runners are relatively low, as compared with other athletic populations, including collegiate athletes (1 death per 43,770 participants per year), triathlon participants (1 death per 52,630 participants), and previously healthy middle-aged joggers (1 death per 7,620 participants)," the researchers wrote (N. Engl. J. Med. 2012;366:130-40).
The absolute number of marathon-related cardiac arrests rose each year during the study period, but the incidence remained stable because of an annual increase in runners from fewer than 1 million in 2000 to approximately 2 million in 2010, according to the investigators.
Men were more likely than were women runners to have a cardiac arrest or sudden death (0.90 per 100,000 vs. 0.16 per 100,000), which the authors noted is "consistent with reports on other populations and reaffirms a male predisposition to exertional cardiac arrest."
The distance of a race was a key determinant of the risk of cardiac arrest, since rates were three to five times higher during marathons (1.01 per 100,000 runners) than during half-marathons (0.27 per 100,000). "A possible explanation is that longer races involve more physiological stress and thus a higher likelihood of precipitating an adverse event in a predisposed participant," the researchers wrote.
The overall case fatality rate was 71%. Sufficient information was available to determine the cause of cardiac arrest in only 31 of the 59 cases.
The most frequent cause of death was hypertrophic cardiomyopathy (8 cases) or possible hypertrophic cardiomyopathy (7 cases). This is also the primary cause of death in young competitive athletes, they pointed out.
"Notably, 9 of the 15 nonsurvivors who had cardiac hypertrophy had an additional clinical factor or postmortem finding: obstructive coronary artery disease (in 3), myocarditis (in 2), bicuspid aortic valve or coronary anomaly (in 2), accessory atrioventricular nodal bypass tract (in 1), or hyperthermia (in 1)," the researchers wrote. The race-related disorders of hyperthermia and hyponatremia, which led to the death of one runner without cardiac hypertrophy, thus are not common causes of cardiac arrest and sudden death, they added.
Among the eight survivors of cardiac arrest, ischemic heart disease was the most frequent cause of the arrest. The strongest predictor of survival of cardiac arrest was bystander-administered CPR, underscoring the importance of onsite medical services.
It was "surprising" that none of the runners with serious coronary atherosclerosis had angiographic evidence of acute plaque rupture or thrombus, because previous studies as well as expert consensus statements have suggest that exercise-induced coronary syndromes result from disruption of atherosclerotic plaque and coronary thrombosis. "In contrast, our findings suggest that demand ischemia (i.e., ischemia due to an imbalance between oxygen supply and demand) may be operative in exercise-related acute coronary events during long-distance running races," they wrote.
This finding also suggests that the practice of taking aspirin before a race to prevent cardiac arrest is likely ineffective, since acute coronary artery thrombosis is not an important cause of marathon-related cardiac arrest, they added.
Physicians called on to evaluate potential marathon participants "should be aware of the risks of hypertrophic cardiomyopathy and atherosclerotic disease in this patient population." Prerace exercise testing may detect physiologically significant coronary artery stenosis or may identify patients with exertion-induced myocardial ischemia, the investigators said.
This study was limited in that the researchers were unable to obtain complete clinical information on 45% of the nonsurvivors or on 53% of the survivors.
Dr. Kim reported no financial conflicts of interest, but two of his coauthors reported ties to industry sources.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major Finding: The overall rate of sudden death during or immediately after marathon and half-marathon races is 1 per 259,000 runners, which compares favorably with rates for collegiate athletics (1 death per 43,770 participants), triathlon participants (1 death per 52,630 participants), and previously healthy middle-aged joggers (1 death per 7,620 participants).
Data Source: Analysis of data in the Race Associated Cardiac Arrest Event Registry (RACER) on 59 cardiac arrests that occurred in marathon and half-marathon runners during 2000-2010.
Disclosures: Dr. Kim reported no financial conflicts of interest, but two of his coauthors reported ties to industry sources.
Potassium Targets for Acute MI Too High, Outdated
Current guidelines for correcting serum potassium levels in patients who present with acute MI are out of date and aim for targets that are too high, raising the risk of in-hospital mortality, according to a report in the Jan. 11 issue of JAMA.
In a retrospective study of 38,689 cases of MI in a nationally representative database, there was a U-shaped relationship between serum potassium level at admission an in-hospital mortality. The lowest mortality occurred in patients with potassium levels of 3.5-4.5 mEq/L, with higher mortality in those with potassium levels of 4.5 mEq/L or higher as well as those with levels less than 3.5 mEq/L.
Current practice guidelines recommend raising "low" potassium to 4.0-5.0 mEq/L, "and some experts even advise a higher range of 4.5-5.5 mEq/L," said Dr. Abhinav Goyal of the schools of medicine and public health at Emory University, Atlanta, and his associates.
"These guidelines are based on small, older studies that focused only on [preventing] ventricular arrhythmias (and not mortality) and were conducted before the routine use of beta-blockers, reperfusion therapy, and early invasive management in acute MI patients. Our data suggest that ... potassium levels of greater than 4.5 mEq/L are associated with increased mortality and probably should be avoided," they noted.
Dr. Goyal and his colleagues performed their study because measuring and repleting potassium to prevent arrhythmia in patients who present with acute MI is an entrenched practice, despite "the lack of current, adequately powered studies that define the optimal range of serum potassium levels with respect to mortality and other important clinical outcomes." They used information from the Cerner Corporation’s Health Facts database, which covers nearly 400,000 consecutive MI patients who presented to 67 U.S. hospitals representing all geographic regions of the country in 2000-2008.
A total of 2,679 of these study subjects (6.9%) died during hospitalization.
Compared with the reference group (potassium level of 3.5-4.0 mEq/L), in which in-hospital mortality was 4.8%, patients with levels of 4.0-4.5 had comparable mortality (5.0%).
In contrast, mortality was twice as great (10.0%) for patients with potassium levels of 4.5-5.0 mEq/L, and was even greater at higher levels, the investigators said (JAMA 2012;307:157-64).
"Our findings suggest that overly aggressive repletion of potassium levels (which is often automated through the implementation of hospital order sets) may not be advisable in patients with acute MI ... as potassium levels of at least 4.5 mEq/L are associated with harm," they noted.
As expected, mortality also was greater for patients with low potassium levels below 3.5 mEq/L.
These associations persisted in further analyses that adjusted for potentially confounding factors such as patient age, sex, and glomerular filtration rate at admission. They also remained robust regardless of whether patients did or did not receive potassium supplementation during hospitalization, and remained robust when the analysis was restricted only to patients who survived past the first 24 hours.
The investigators cautioned that their findings apply only to patients with acute MI and should not be extrapolated to those with other cardiac conditions, including heart failure.
This study was supported in part by Saint Luke’s Mid America Heart Institute, Kansas City, Mo. No conflicts of interest were reported.
Potassium repletion to levels higher than 4.5 mEq/L no longer appear to be justified in acute MI, said Dr. Benjamin M. Scirica and Dr. David A. Morrow.
Even potassium levels of 4.0-4.5 mEq/L were associated with increased mortality, compared with levels of 3.5-4.0 mEq/L, and 43% of all the patients in this study fell into that category.
However, it is reasonable to avoid significant hypokalemia (less than 3.5 mEq/L), especially for patients who have significant, sustained, ventricular ectopy or other high-risk features.
Dr. Scirica and Dr. Morrow are at the Levine Cardiac Unit at Brigham and Women’s Hospital and Harvard Medical School, both in Boston. They reported numerous ties to pharmaceutical companies. These remarks were adapted from their editorial comment accompanying Dr. Goyal’s report (JAMA 2012;307:195-6).
Potassium repletion to levels higher than 4.5 mEq/L no longer appear to be justified in acute MI, said Dr. Benjamin M. Scirica and Dr. David A. Morrow.
Even potassium levels of 4.0-4.5 mEq/L were associated with increased mortality, compared with levels of 3.5-4.0 mEq/L, and 43% of all the patients in this study fell into that category.
However, it is reasonable to avoid significant hypokalemia (less than 3.5 mEq/L), especially for patients who have significant, sustained, ventricular ectopy or other high-risk features.
Dr. Scirica and Dr. Morrow are at the Levine Cardiac Unit at Brigham and Women’s Hospital and Harvard Medical School, both in Boston. They reported numerous ties to pharmaceutical companies. These remarks were adapted from their editorial comment accompanying Dr. Goyal’s report (JAMA 2012;307:195-6).
Potassium repletion to levels higher than 4.5 mEq/L no longer appear to be justified in acute MI, said Dr. Benjamin M. Scirica and Dr. David A. Morrow.
Even potassium levels of 4.0-4.5 mEq/L were associated with increased mortality, compared with levels of 3.5-4.0 mEq/L, and 43% of all the patients in this study fell into that category.
However, it is reasonable to avoid significant hypokalemia (less than 3.5 mEq/L), especially for patients who have significant, sustained, ventricular ectopy or other high-risk features.
Dr. Scirica and Dr. Morrow are at the Levine Cardiac Unit at Brigham and Women’s Hospital and Harvard Medical School, both in Boston. They reported numerous ties to pharmaceutical companies. These remarks were adapted from their editorial comment accompanying Dr. Goyal’s report (JAMA 2012;307:195-6).
Current guidelines for correcting serum potassium levels in patients who present with acute MI are out of date and aim for targets that are too high, raising the risk of in-hospital mortality, according to a report in the Jan. 11 issue of JAMA.
In a retrospective study of 38,689 cases of MI in a nationally representative database, there was a U-shaped relationship between serum potassium level at admission an in-hospital mortality. The lowest mortality occurred in patients with potassium levels of 3.5-4.5 mEq/L, with higher mortality in those with potassium levels of 4.5 mEq/L or higher as well as those with levels less than 3.5 mEq/L.
Current practice guidelines recommend raising "low" potassium to 4.0-5.0 mEq/L, "and some experts even advise a higher range of 4.5-5.5 mEq/L," said Dr. Abhinav Goyal of the schools of medicine and public health at Emory University, Atlanta, and his associates.
"These guidelines are based on small, older studies that focused only on [preventing] ventricular arrhythmias (and not mortality) and were conducted before the routine use of beta-blockers, reperfusion therapy, and early invasive management in acute MI patients. Our data suggest that ... potassium levels of greater than 4.5 mEq/L are associated with increased mortality and probably should be avoided," they noted.
Dr. Goyal and his colleagues performed their study because measuring and repleting potassium to prevent arrhythmia in patients who present with acute MI is an entrenched practice, despite "the lack of current, adequately powered studies that define the optimal range of serum potassium levels with respect to mortality and other important clinical outcomes." They used information from the Cerner Corporation’s Health Facts database, which covers nearly 400,000 consecutive MI patients who presented to 67 U.S. hospitals representing all geographic regions of the country in 2000-2008.
A total of 2,679 of these study subjects (6.9%) died during hospitalization.
Compared with the reference group (potassium level of 3.5-4.0 mEq/L), in which in-hospital mortality was 4.8%, patients with levels of 4.0-4.5 had comparable mortality (5.0%).
In contrast, mortality was twice as great (10.0%) for patients with potassium levels of 4.5-5.0 mEq/L, and was even greater at higher levels, the investigators said (JAMA 2012;307:157-64).
"Our findings suggest that overly aggressive repletion of potassium levels (which is often automated through the implementation of hospital order sets) may not be advisable in patients with acute MI ... as potassium levels of at least 4.5 mEq/L are associated with harm," they noted.
As expected, mortality also was greater for patients with low potassium levels below 3.5 mEq/L.
These associations persisted in further analyses that adjusted for potentially confounding factors such as patient age, sex, and glomerular filtration rate at admission. They also remained robust regardless of whether patients did or did not receive potassium supplementation during hospitalization, and remained robust when the analysis was restricted only to patients who survived past the first 24 hours.
The investigators cautioned that their findings apply only to patients with acute MI and should not be extrapolated to those with other cardiac conditions, including heart failure.
This study was supported in part by Saint Luke’s Mid America Heart Institute, Kansas City, Mo. No conflicts of interest were reported.
Current guidelines for correcting serum potassium levels in patients who present with acute MI are out of date and aim for targets that are too high, raising the risk of in-hospital mortality, according to a report in the Jan. 11 issue of JAMA.
In a retrospective study of 38,689 cases of MI in a nationally representative database, there was a U-shaped relationship between serum potassium level at admission an in-hospital mortality. The lowest mortality occurred in patients with potassium levels of 3.5-4.5 mEq/L, with higher mortality in those with potassium levels of 4.5 mEq/L or higher as well as those with levels less than 3.5 mEq/L.
Current practice guidelines recommend raising "low" potassium to 4.0-5.0 mEq/L, "and some experts even advise a higher range of 4.5-5.5 mEq/L," said Dr. Abhinav Goyal of the schools of medicine and public health at Emory University, Atlanta, and his associates.
"These guidelines are based on small, older studies that focused only on [preventing] ventricular arrhythmias (and not mortality) and were conducted before the routine use of beta-blockers, reperfusion therapy, and early invasive management in acute MI patients. Our data suggest that ... potassium levels of greater than 4.5 mEq/L are associated with increased mortality and probably should be avoided," they noted.
Dr. Goyal and his colleagues performed their study because measuring and repleting potassium to prevent arrhythmia in patients who present with acute MI is an entrenched practice, despite "the lack of current, adequately powered studies that define the optimal range of serum potassium levels with respect to mortality and other important clinical outcomes." They used information from the Cerner Corporation’s Health Facts database, which covers nearly 400,000 consecutive MI patients who presented to 67 U.S. hospitals representing all geographic regions of the country in 2000-2008.
A total of 2,679 of these study subjects (6.9%) died during hospitalization.
Compared with the reference group (potassium level of 3.5-4.0 mEq/L), in which in-hospital mortality was 4.8%, patients with levels of 4.0-4.5 had comparable mortality (5.0%).
In contrast, mortality was twice as great (10.0%) for patients with potassium levels of 4.5-5.0 mEq/L, and was even greater at higher levels, the investigators said (JAMA 2012;307:157-64).
"Our findings suggest that overly aggressive repletion of potassium levels (which is often automated through the implementation of hospital order sets) may not be advisable in patients with acute MI ... as potassium levels of at least 4.5 mEq/L are associated with harm," they noted.
As expected, mortality also was greater for patients with low potassium levels below 3.5 mEq/L.
These associations persisted in further analyses that adjusted for potentially confounding factors such as patient age, sex, and glomerular filtration rate at admission. They also remained robust regardless of whether patients did or did not receive potassium supplementation during hospitalization, and remained robust when the analysis was restricted only to patients who survived past the first 24 hours.
The investigators cautioned that their findings apply only to patients with acute MI and should not be extrapolated to those with other cardiac conditions, including heart failure.
This study was supported in part by Saint Luke’s Mid America Heart Institute, Kansas City, Mo. No conflicts of interest were reported.
FROM JAMA
Major Finding: In-hospital mortality was lowest (less than 5%) in patients with potassium levels of 3.5-4.5 mEq/L at admission; it was twice as high (10%) in those with levels of 4.5 mEq/L or higher, which is recommended in "outdated" practice guidelines.
Data Source: A retrospective cohort study involving 38,689 cases of acute MI treated at 67 U.S. hospitals in 2000-2008.
Disclosures: This study was supported in part by Saint Luke’s Mid America Heart Institute, Kansas City, Mo. No conflicts of interest were reported.
No Lung Damage Seen in Typical Marijuana Smokers
Unlike cigarette smoking, 20 years of typical marijuana smoking doesn’t appear to impair lung function, according to a report in the Jan. 11 issue of JAMA.
"With up to 7 joint-years of lifetime exposure (e.g., one joint per day for 7 years or one joint per week for 49 years), we found no evidence that increasing exposure to marijuana adversely affects pulmonary function," said Dr. Mark J. Pletcher of the department of epidemiology and biostatistics and the department of medicine, University of California, San Francisco, and his associates.
While heavier use may impair lung function, the number of such users was too small in this study cohort to allow reliable estimates. The data suggested a detrimental effect with heavier marijuana smoking, the investigators noted.
Previous studies of the pulmonary effects of long-term marijuana use have yielded inconsistent results. On the one hand, they have demonstrated "consistent evidence of airway mucosal injury and inflammation, as well as increased respiratory symptoms such as cough, phlegm production, and wheeze, similar to that seen in tobacco smokers." On the other hand, these appear to be short-term effects, and there has been no clear evidence of long-term damage to lung function.
Dr. Pletcher and his colleagues studied the issue using data from a large longitudinal study of coronary risk that closely followed the cigarette and marijuana smoking habits of 5,016 young adults in four U.S. communities from 1985 through 2006. As part of that study, the subjects (aged 18-30 years at baseline) underwent pulmonary function testing at baseline, 2 years, 5 years, 10 years, and 20 years.
Using that data, "we estimated both current intensity and lifetime cumulative exposure to tobacco and marijuana smoking and analyzed their associations with spirometric measures of pulmonary function over the 20 years of follow-up," the researchers said.
One joint-year of exposure was defined as the equivalent of 365 joints or filled pipe bowls smoked. Secondhand smoke exposure also was taken into account.
As expected, both current and lifetime tobacco smoking were associated with lower forced expiratory volume in 1 second (FEV1) and lower forced vital capacity (FVC). But unexpectedly, both current and lifetime marijuana smoking were associated with higher FEV1 and higher FVC, the authors wrote (JAMA 2012;307:173-81).
"For example, compared with zero exposure, FVC increased with greater lifetime exposure in joint-years, and FEV1 increased with greater lifetime exposure of up to 10 joint-years and then declined to ... greater than zero-exposure level," the investigators said.
Why marijuana smoking would increase lung capacity is unknown, but other studies have also found this effect. "Some investigators have proposed that the deep inspiratory maneuvers practiced by marijuana smokers could stretch the lungs, resulting in larger lung volumes. Another speculative possibility is strengthening of chest wall musculature or another ‘training’ effect that allows marijuana users to inspire more fully (closer to lung capacity) on spirometry testing," Dr. Pletcher and his associates said.
In a separate analysis of the data using different statistical methods, "we again found strong, dose-related associations between increasing exposure to tobacco and lower FEV1 and FVC," but no such associations for marijuana smoking. Only at very high levels of marijuana smoking was a detrimental effect on pulmonary function suggested.
"Hypothetically speaking, a positive effect from marijuana in the short term (the stretch/training effect) and a negative effect in the long term (damage from smoke exposure) should result in a nonlinear association such as the one we observed. According to this explanation, the predominant effect for FEV1 at very high exposure (more than 40 joint-years) reflects cumulative damage; the predominant effect for FVC at all levels of exposure is from the stretch/training mechanism," they noted.
"Marijuana may have beneficial effects on pain control, appetite, mood, and management of other chronic symptoms. Our findings suggest that occasional use of marijuana for these or other purposes may not be associated with adverse consequences on pulmonary function," the investigators said.
This study was supported by the National Institute on Drug Abuse and the National Heart, Lung, and Blood Institute. Dr. Pletcher reported no conflicts of interest.
Unlike cigarette smoking, 20 years of typical marijuana smoking doesn’t appear to impair lung function, according to a report in the Jan. 11 issue of JAMA.
"With up to 7 joint-years of lifetime exposure (e.g., one joint per day for 7 years or one joint per week for 49 years), we found no evidence that increasing exposure to marijuana adversely affects pulmonary function," said Dr. Mark J. Pletcher of the department of epidemiology and biostatistics and the department of medicine, University of California, San Francisco, and his associates.
While heavier use may impair lung function, the number of such users was too small in this study cohort to allow reliable estimates. The data suggested a detrimental effect with heavier marijuana smoking, the investigators noted.
Previous studies of the pulmonary effects of long-term marijuana use have yielded inconsistent results. On the one hand, they have demonstrated "consistent evidence of airway mucosal injury and inflammation, as well as increased respiratory symptoms such as cough, phlegm production, and wheeze, similar to that seen in tobacco smokers." On the other hand, these appear to be short-term effects, and there has been no clear evidence of long-term damage to lung function.
Dr. Pletcher and his colleagues studied the issue using data from a large longitudinal study of coronary risk that closely followed the cigarette and marijuana smoking habits of 5,016 young adults in four U.S. communities from 1985 through 2006. As part of that study, the subjects (aged 18-30 years at baseline) underwent pulmonary function testing at baseline, 2 years, 5 years, 10 years, and 20 years.
Using that data, "we estimated both current intensity and lifetime cumulative exposure to tobacco and marijuana smoking and analyzed their associations with spirometric measures of pulmonary function over the 20 years of follow-up," the researchers said.
One joint-year of exposure was defined as the equivalent of 365 joints or filled pipe bowls smoked. Secondhand smoke exposure also was taken into account.
As expected, both current and lifetime tobacco smoking were associated with lower forced expiratory volume in 1 second (FEV1) and lower forced vital capacity (FVC). But unexpectedly, both current and lifetime marijuana smoking were associated with higher FEV1 and higher FVC, the authors wrote (JAMA 2012;307:173-81).
"For example, compared with zero exposure, FVC increased with greater lifetime exposure in joint-years, and FEV1 increased with greater lifetime exposure of up to 10 joint-years and then declined to ... greater than zero-exposure level," the investigators said.
Why marijuana smoking would increase lung capacity is unknown, but other studies have also found this effect. "Some investigators have proposed that the deep inspiratory maneuvers practiced by marijuana smokers could stretch the lungs, resulting in larger lung volumes. Another speculative possibility is strengthening of chest wall musculature or another ‘training’ effect that allows marijuana users to inspire more fully (closer to lung capacity) on spirometry testing," Dr. Pletcher and his associates said.
In a separate analysis of the data using different statistical methods, "we again found strong, dose-related associations between increasing exposure to tobacco and lower FEV1 and FVC," but no such associations for marijuana smoking. Only at very high levels of marijuana smoking was a detrimental effect on pulmonary function suggested.
"Hypothetically speaking, a positive effect from marijuana in the short term (the stretch/training effect) and a negative effect in the long term (damage from smoke exposure) should result in a nonlinear association such as the one we observed. According to this explanation, the predominant effect for FEV1 at very high exposure (more than 40 joint-years) reflects cumulative damage; the predominant effect for FVC at all levels of exposure is from the stretch/training mechanism," they noted.
"Marijuana may have beneficial effects on pain control, appetite, mood, and management of other chronic symptoms. Our findings suggest that occasional use of marijuana for these or other purposes may not be associated with adverse consequences on pulmonary function," the investigators said.
This study was supported by the National Institute on Drug Abuse and the National Heart, Lung, and Blood Institute. Dr. Pletcher reported no conflicts of interest.
Unlike cigarette smoking, 20 years of typical marijuana smoking doesn’t appear to impair lung function, according to a report in the Jan. 11 issue of JAMA.
"With up to 7 joint-years of lifetime exposure (e.g., one joint per day for 7 years or one joint per week for 49 years), we found no evidence that increasing exposure to marijuana adversely affects pulmonary function," said Dr. Mark J. Pletcher of the department of epidemiology and biostatistics and the department of medicine, University of California, San Francisco, and his associates.
While heavier use may impair lung function, the number of such users was too small in this study cohort to allow reliable estimates. The data suggested a detrimental effect with heavier marijuana smoking, the investigators noted.
Previous studies of the pulmonary effects of long-term marijuana use have yielded inconsistent results. On the one hand, they have demonstrated "consistent evidence of airway mucosal injury and inflammation, as well as increased respiratory symptoms such as cough, phlegm production, and wheeze, similar to that seen in tobacco smokers." On the other hand, these appear to be short-term effects, and there has been no clear evidence of long-term damage to lung function.
Dr. Pletcher and his colleagues studied the issue using data from a large longitudinal study of coronary risk that closely followed the cigarette and marijuana smoking habits of 5,016 young adults in four U.S. communities from 1985 through 2006. As part of that study, the subjects (aged 18-30 years at baseline) underwent pulmonary function testing at baseline, 2 years, 5 years, 10 years, and 20 years.
Using that data, "we estimated both current intensity and lifetime cumulative exposure to tobacco and marijuana smoking and analyzed their associations with spirometric measures of pulmonary function over the 20 years of follow-up," the researchers said.
One joint-year of exposure was defined as the equivalent of 365 joints or filled pipe bowls smoked. Secondhand smoke exposure also was taken into account.
As expected, both current and lifetime tobacco smoking were associated with lower forced expiratory volume in 1 second (FEV1) and lower forced vital capacity (FVC). But unexpectedly, both current and lifetime marijuana smoking were associated with higher FEV1 and higher FVC, the authors wrote (JAMA 2012;307:173-81).
"For example, compared with zero exposure, FVC increased with greater lifetime exposure in joint-years, and FEV1 increased with greater lifetime exposure of up to 10 joint-years and then declined to ... greater than zero-exposure level," the investigators said.
Why marijuana smoking would increase lung capacity is unknown, but other studies have also found this effect. "Some investigators have proposed that the deep inspiratory maneuvers practiced by marijuana smokers could stretch the lungs, resulting in larger lung volumes. Another speculative possibility is strengthening of chest wall musculature or another ‘training’ effect that allows marijuana users to inspire more fully (closer to lung capacity) on spirometry testing," Dr. Pletcher and his associates said.
In a separate analysis of the data using different statistical methods, "we again found strong, dose-related associations between increasing exposure to tobacco and lower FEV1 and FVC," but no such associations for marijuana smoking. Only at very high levels of marijuana smoking was a detrimental effect on pulmonary function suggested.
"Hypothetically speaking, a positive effect from marijuana in the short term (the stretch/training effect) and a negative effect in the long term (damage from smoke exposure) should result in a nonlinear association such as the one we observed. According to this explanation, the predominant effect for FEV1 at very high exposure (more than 40 joint-years) reflects cumulative damage; the predominant effect for FVC at all levels of exposure is from the stretch/training mechanism," they noted.
"Marijuana may have beneficial effects on pain control, appetite, mood, and management of other chronic symptoms. Our findings suggest that occasional use of marijuana for these or other purposes may not be associated with adverse consequences on pulmonary function," the investigators said.
This study was supported by the National Institute on Drug Abuse and the National Heart, Lung, and Blood Institute. Dr. Pletcher reported no conflicts of interest.
FROM JAMA
Major Finding: Typical current and lifetime levels of marijuana smoking (up to 7 joint-years of exposure) were associated with high FEV1 and FVC values, indicating no impairment of pulmonary function.
Data Source: A secondary analysis of data from a longitudinal study of coronary risk in which smoking habits and pulmonary function were closely followed for 20 years in 5,016 men and women aged 18-30 years at baseline in 1985.
Disclosures: This study was supported by the National Institute on Drug Abuse and the National Heart, Lung, and Blood Institute. Dr. Pletcher reported no conflicts of interest.
Dabigatran Tied to Increase in Heart Attack Risk
The direct thrombin inhibitor dabigatran appears to raise the risk of myocardial infarction or acute coronary syndromes, according to a meta-analysis of seven randomized clinical trials published online Jan. 9 in the Archives of Internal Medicine.
The meta-analysis included randomized clinical trials assessing the noninferiority of dabigatran against various control treatments including adjusted-dose warfarin, enoxaparin, and placebo, in a broad spectrum of patients using the drug for a variety of indications.
"We used several meta-analytic methods and several association measures, and the results were consistent. Although the relative risk increase was 33%, the absolute risk increase was very small, at 0.27%," said Dr. Ken Uchino and Dr. Adrian V. Hernandez, both of the Cleveland Clinic.
The mechanism by which dabigatran increases the risk of MI or acute coronary syndrome (ACS) is not yet known. It is possible that the drug doesn’t actively raise this risk, but instead lacks some protective effect that the control treatments possess, the investigators noted.
The meta-analysis covered 30,514 study subjects, including patients with atrial fibrillation who used dabigatran to prevent stroke, patients with atrial fibrillation who used it to prevent acute venous thromboembolism, patients with ACS who used it to prevent recurrent ACS, and patients undergoing joint replacement who used it to prevent deep vein thrombosis.
Overall, patients who received dabigatran were at significantly higher risk of MI or ACS than were control patients. The incidence of these events was 1.19% in those taking dabigatran, compared with 0.79% in control subjects, Dr. Uchino and Dr. Hernandez said (Arch. Intern. Med. 2012 [doi:10.1001/archinternmed.2011.1666]).
Since it is possible that dabigatran’s negative effects may increase with longer duration of use, the investigators performed a separate analysis excluding three of the seven studies that had exceptionally short (less than 1 month) exposure times. The risk of MI or ACS remained high and significant in this analysis of the data, they noted.
An important limitation of the meta-analysis is that a single large trial, with a study population of 18,113 patients, overshadowed the findings from the other 6 trials, which had populations of 515 to 2,451 patients. In addition, the large trial followed patients for a median of 2 years, while the smaller trials did so for 6 months or less.
Because of this imbalance, the large trial accounted for 59% of the meta-analysis cohort and 74% of the cardiovascular events, they said.
Overall, the findings indicate that dabigatran’s cardiovascular risks should be investigated further, "especially if [the drug] is used in populations at high risk of MI or ACS," they added.
All seven studies included in the meta-analysis were sponsored by the drug manufacturer, Boehringer Ingelheim. No financial conflicts of interest were reported among the investigators for this current study.
Dr. Jacobs and Dr. Stessman reported having no financial conflicts of interest.
The "robust" finding by Dr. Uchino and Dr. Hernandez that dabigatran is associated with increased MI "is alarming and emphasizes the need for continued critical appraisal of new drugs after phase III trials," said Dr. Jeremy M. Jacobs and Dr. Jochanan Stessman.
The researchers’ results "suggest that physicians [should] step back for a moment, take their own pulse, and retain a critical view as a powerful new drug enters clinical use on a potentially massive scale," Dr. Jacobs and Dr. Stessman said.
The findings also highlight another deeply concerning issue: "the enthusiasm – nearly to the level of euphoria – to embrace the new," they added.
Dr. Jacobs is at the Jerusalem Institute of Aging Research at Hadassah-Hebrew University Medical Center, and Dr. Stessman is at Hebrew University–Hadassah Medical School, Jerusalem. They reported having no financial conflicts of interest. These remarks were taken from their invited commentary, which accompanied the meta-analysis (Arch. Intern. Med. 2012 [doi:10.1001/archinternmed.2011.1721]).
The "robust" finding by Dr. Uchino and Dr. Hernandez that dabigatran is associated with increased MI "is alarming and emphasizes the need for continued critical appraisal of new drugs after phase III trials," said Dr. Jeremy M. Jacobs and Dr. Jochanan Stessman.
The researchers’ results "suggest that physicians [should] step back for a moment, take their own pulse, and retain a critical view as a powerful new drug enters clinical use on a potentially massive scale," Dr. Jacobs and Dr. Stessman said.
The findings also highlight another deeply concerning issue: "the enthusiasm – nearly to the level of euphoria – to embrace the new," they added.
Dr. Jacobs is at the Jerusalem Institute of Aging Research at Hadassah-Hebrew University Medical Center, and Dr. Stessman is at Hebrew University–Hadassah Medical School, Jerusalem. They reported having no financial conflicts of interest. These remarks were taken from their invited commentary, which accompanied the meta-analysis (Arch. Intern. Med. 2012 [doi:10.1001/archinternmed.2011.1721]).
The "robust" finding by Dr. Uchino and Dr. Hernandez that dabigatran is associated with increased MI "is alarming and emphasizes the need for continued critical appraisal of new drugs after phase III trials," said Dr. Jeremy M. Jacobs and Dr. Jochanan Stessman.
The researchers’ results "suggest that physicians [should] step back for a moment, take their own pulse, and retain a critical view as a powerful new drug enters clinical use on a potentially massive scale," Dr. Jacobs and Dr. Stessman said.
The findings also highlight another deeply concerning issue: "the enthusiasm – nearly to the level of euphoria – to embrace the new," they added.
Dr. Jacobs is at the Jerusalem Institute of Aging Research at Hadassah-Hebrew University Medical Center, and Dr. Stessman is at Hebrew University–Hadassah Medical School, Jerusalem. They reported having no financial conflicts of interest. These remarks were taken from their invited commentary, which accompanied the meta-analysis (Arch. Intern. Med. 2012 [doi:10.1001/archinternmed.2011.1721]).
The direct thrombin inhibitor dabigatran appears to raise the risk of myocardial infarction or acute coronary syndromes, according to a meta-analysis of seven randomized clinical trials published online Jan. 9 in the Archives of Internal Medicine.
The meta-analysis included randomized clinical trials assessing the noninferiority of dabigatran against various control treatments including adjusted-dose warfarin, enoxaparin, and placebo, in a broad spectrum of patients using the drug for a variety of indications.
"We used several meta-analytic methods and several association measures, and the results were consistent. Although the relative risk increase was 33%, the absolute risk increase was very small, at 0.27%," said Dr. Ken Uchino and Dr. Adrian V. Hernandez, both of the Cleveland Clinic.
The mechanism by which dabigatran increases the risk of MI or acute coronary syndrome (ACS) is not yet known. It is possible that the drug doesn’t actively raise this risk, but instead lacks some protective effect that the control treatments possess, the investigators noted.
The meta-analysis covered 30,514 study subjects, including patients with atrial fibrillation who used dabigatran to prevent stroke, patients with atrial fibrillation who used it to prevent acute venous thromboembolism, patients with ACS who used it to prevent recurrent ACS, and patients undergoing joint replacement who used it to prevent deep vein thrombosis.
Overall, patients who received dabigatran were at significantly higher risk of MI or ACS than were control patients. The incidence of these events was 1.19% in those taking dabigatran, compared with 0.79% in control subjects, Dr. Uchino and Dr. Hernandez said (Arch. Intern. Med. 2012 [doi:10.1001/archinternmed.2011.1666]).
Since it is possible that dabigatran’s negative effects may increase with longer duration of use, the investigators performed a separate analysis excluding three of the seven studies that had exceptionally short (less than 1 month) exposure times. The risk of MI or ACS remained high and significant in this analysis of the data, they noted.
An important limitation of the meta-analysis is that a single large trial, with a study population of 18,113 patients, overshadowed the findings from the other 6 trials, which had populations of 515 to 2,451 patients. In addition, the large trial followed patients for a median of 2 years, while the smaller trials did so for 6 months or less.
Because of this imbalance, the large trial accounted for 59% of the meta-analysis cohort and 74% of the cardiovascular events, they said.
Overall, the findings indicate that dabigatran’s cardiovascular risks should be investigated further, "especially if [the drug] is used in populations at high risk of MI or ACS," they added.
All seven studies included in the meta-analysis were sponsored by the drug manufacturer, Boehringer Ingelheim. No financial conflicts of interest were reported among the investigators for this current study.
Dr. Jacobs and Dr. Stessman reported having no financial conflicts of interest.
The direct thrombin inhibitor dabigatran appears to raise the risk of myocardial infarction or acute coronary syndromes, according to a meta-analysis of seven randomized clinical trials published online Jan. 9 in the Archives of Internal Medicine.
The meta-analysis included randomized clinical trials assessing the noninferiority of dabigatran against various control treatments including adjusted-dose warfarin, enoxaparin, and placebo, in a broad spectrum of patients using the drug for a variety of indications.
"We used several meta-analytic methods and several association measures, and the results were consistent. Although the relative risk increase was 33%, the absolute risk increase was very small, at 0.27%," said Dr. Ken Uchino and Dr. Adrian V. Hernandez, both of the Cleveland Clinic.
The mechanism by which dabigatran increases the risk of MI or acute coronary syndrome (ACS) is not yet known. It is possible that the drug doesn’t actively raise this risk, but instead lacks some protective effect that the control treatments possess, the investigators noted.
The meta-analysis covered 30,514 study subjects, including patients with atrial fibrillation who used dabigatran to prevent stroke, patients with atrial fibrillation who used it to prevent acute venous thromboembolism, patients with ACS who used it to prevent recurrent ACS, and patients undergoing joint replacement who used it to prevent deep vein thrombosis.
Overall, patients who received dabigatran were at significantly higher risk of MI or ACS than were control patients. The incidence of these events was 1.19% in those taking dabigatran, compared with 0.79% in control subjects, Dr. Uchino and Dr. Hernandez said (Arch. Intern. Med. 2012 [doi:10.1001/archinternmed.2011.1666]).
Since it is possible that dabigatran’s negative effects may increase with longer duration of use, the investigators performed a separate analysis excluding three of the seven studies that had exceptionally short (less than 1 month) exposure times. The risk of MI or ACS remained high and significant in this analysis of the data, they noted.
An important limitation of the meta-analysis is that a single large trial, with a study population of 18,113 patients, overshadowed the findings from the other 6 trials, which had populations of 515 to 2,451 patients. In addition, the large trial followed patients for a median of 2 years, while the smaller trials did so for 6 months or less.
Because of this imbalance, the large trial accounted for 59% of the meta-analysis cohort and 74% of the cardiovascular events, they said.
Overall, the findings indicate that dabigatran’s cardiovascular risks should be investigated further, "especially if [the drug] is used in populations at high risk of MI or ACS," they added.
All seven studies included in the meta-analysis were sponsored by the drug manufacturer, Boehringer Ingelheim. No financial conflicts of interest were reported among the investigators for this current study.
Dr. Jacobs and Dr. Stessman reported having no financial conflicts of interest.
FROM THE ARCHIVES OF INTERNAL MEDICINE
Major Finding: The incidence of MI or ACS was significantly higher in patients taking the thrombin inhibitor dabigatran (1.19%) than in those taking various control treatments including warfarin, enoxaparin, and placebo (0.79%), representing a 33% increase in relative risk.
Data Source: A meta-analysis of seven randomized controlled trials (30,514 subjects) assessing dabigatran’s adverse CV effects when used for a variety of indications.
Disclosures: No financial conflicts of interest were reported.
Diabetes Prevention Models Deliver Modest Weight Loss
The U.S. Diabetes Prevention Program conducted a clinical trial in 2002 showing that modest weight loss through caloric restriction and increased physical activity reduced the incidence of diabetes in high-risk patients by 58%.
Structured lifestyle interventions based on the U.S. Diabetes Prevention Program’s curriculum were effective at promoting clinically significant weight loss of approximately 4% when applied in real-world settings, according to a meta-analysis in the January issue of Health Affairs.
The U.S. Diabetes Prevention Program conducted a clinical trial in 2002 showing that modest weight loss through caloric restriction and increased physical activity reduced the incidence of diabetes in high-risk patients by 58%. Weight loss was found to be the single most important factor in preventing diabetes from developing over the course of 3 years among patients who were at high risk for the disease. For every kilogram of weight lost, the incidence of diabetes decreased by 16%.
"Yet these results have not been ‘translated’ into routine clinical practice and public health policy," said Dr. Mohammed K. Ali of Emory University, Atlanta, and his associates.
They performed what they described as the first meta-analysis of U.S. studies in which the structured intervention recommended by they Diabetes Prevention Program was applied to high-risk patients in real-world settings. The meta-analysis included 28 studies published in 2003-2011. In all, 4 were randomized, controlled trials (RCTs), 2 were cluster RCTs, 20 were single-group studies comparing pre-intervention and post-intervention weight, and 2 were nonrandomized, controlled studies.
Most of the studies were conducted in urban areas. In all, 12 were based in community centers, recreation centers, and church organizations, and 11 were based in health care facilities. The total number of patients was 2,916, and the median study duration was 1 year.
Across all the reviewed studies, the mean weight loss was 3.99%, which is considered clinically meaningful, Dr. Ali and his colleagues said (Health Aff. 2012 [doi:10.1377/hlthaff.2011.1009]).
Weight loss was comparable among programs that used medical and allied health professionals to implement the intervention (average 4.27% weight loss), programs that used lay community educators (3.15% weight loss), and programs that used electronic media-assisted interventions (4.20% weight loss).
Moreover, sensitivity analyses showed that programs with lay community educators achieved greater weight loss than those with medical and allied health professionals as educators. That finding "has enormous importance for the scalability and economic sustainability of diabetes interventions," Dr. Ali and his colleagues noted, because lay educators required lower salaries and their training was neither costly nor time-consuming.
Programs that included more "core sessions" in which patients received counseling maintained the highest attendance rates. And higher attendance rates correlated positively with greater weight loss.
The rate of attrition varied greatly among the studies, ranging from 0% to 49%. In some studies that analyzed patient feedback, it appeared that attrition was more strongly related to patients’ perceptions of their risk and to their readiness to change than it was to specific features of the intervention, such as the number of counseling sessions.
No disclosure information was provided.
The U.S. Diabetes Prevention Program conducted a clinical trial in 2002 showing that modest weight loss through caloric restriction and increased physical activity reduced the incidence of diabetes in high-risk patients by 58%.
Structured lifestyle interventions based on the U.S. Diabetes Prevention Program’s curriculum were effective at promoting clinically significant weight loss of approximately 4% when applied in real-world settings, according to a meta-analysis in the January issue of Health Affairs.
The U.S. Diabetes Prevention Program conducted a clinical trial in 2002 showing that modest weight loss through caloric restriction and increased physical activity reduced the incidence of diabetes in high-risk patients by 58%. Weight loss was found to be the single most important factor in preventing diabetes from developing over the course of 3 years among patients who were at high risk for the disease. For every kilogram of weight lost, the incidence of diabetes decreased by 16%.
"Yet these results have not been ‘translated’ into routine clinical practice and public health policy," said Dr. Mohammed K. Ali of Emory University, Atlanta, and his associates.
They performed what they described as the first meta-analysis of U.S. studies in which the structured intervention recommended by they Diabetes Prevention Program was applied to high-risk patients in real-world settings. The meta-analysis included 28 studies published in 2003-2011. In all, 4 were randomized, controlled trials (RCTs), 2 were cluster RCTs, 20 were single-group studies comparing pre-intervention and post-intervention weight, and 2 were nonrandomized, controlled studies.
Most of the studies were conducted in urban areas. In all, 12 were based in community centers, recreation centers, and church organizations, and 11 were based in health care facilities. The total number of patients was 2,916, and the median study duration was 1 year.
Across all the reviewed studies, the mean weight loss was 3.99%, which is considered clinically meaningful, Dr. Ali and his colleagues said (Health Aff. 2012 [doi:10.1377/hlthaff.2011.1009]).
Weight loss was comparable among programs that used medical and allied health professionals to implement the intervention (average 4.27% weight loss), programs that used lay community educators (3.15% weight loss), and programs that used electronic media-assisted interventions (4.20% weight loss).
Moreover, sensitivity analyses showed that programs with lay community educators achieved greater weight loss than those with medical and allied health professionals as educators. That finding "has enormous importance for the scalability and economic sustainability of diabetes interventions," Dr. Ali and his colleagues noted, because lay educators required lower salaries and their training was neither costly nor time-consuming.
Programs that included more "core sessions" in which patients received counseling maintained the highest attendance rates. And higher attendance rates correlated positively with greater weight loss.
The rate of attrition varied greatly among the studies, ranging from 0% to 49%. In some studies that analyzed patient feedback, it appeared that attrition was more strongly related to patients’ perceptions of their risk and to their readiness to change than it was to specific features of the intervention, such as the number of counseling sessions.
No disclosure information was provided.
The U.S. Diabetes Prevention Program conducted a clinical trial in 2002 showing that modest weight loss through caloric restriction and increased physical activity reduced the incidence of diabetes in high-risk patients by 58%.
Structured lifestyle interventions based on the U.S. Diabetes Prevention Program’s curriculum were effective at promoting clinically significant weight loss of approximately 4% when applied in real-world settings, according to a meta-analysis in the January issue of Health Affairs.
The U.S. Diabetes Prevention Program conducted a clinical trial in 2002 showing that modest weight loss through caloric restriction and increased physical activity reduced the incidence of diabetes in high-risk patients by 58%. Weight loss was found to be the single most important factor in preventing diabetes from developing over the course of 3 years among patients who were at high risk for the disease. For every kilogram of weight lost, the incidence of diabetes decreased by 16%.
"Yet these results have not been ‘translated’ into routine clinical practice and public health policy," said Dr. Mohammed K. Ali of Emory University, Atlanta, and his associates.
They performed what they described as the first meta-analysis of U.S. studies in which the structured intervention recommended by they Diabetes Prevention Program was applied to high-risk patients in real-world settings. The meta-analysis included 28 studies published in 2003-2011. In all, 4 were randomized, controlled trials (RCTs), 2 were cluster RCTs, 20 were single-group studies comparing pre-intervention and post-intervention weight, and 2 were nonrandomized, controlled studies.
Most of the studies were conducted in urban areas. In all, 12 were based in community centers, recreation centers, and church organizations, and 11 were based in health care facilities. The total number of patients was 2,916, and the median study duration was 1 year.
Across all the reviewed studies, the mean weight loss was 3.99%, which is considered clinically meaningful, Dr. Ali and his colleagues said (Health Aff. 2012 [doi:10.1377/hlthaff.2011.1009]).
Weight loss was comparable among programs that used medical and allied health professionals to implement the intervention (average 4.27% weight loss), programs that used lay community educators (3.15% weight loss), and programs that used electronic media-assisted interventions (4.20% weight loss).
Moreover, sensitivity analyses showed that programs with lay community educators achieved greater weight loss than those with medical and allied health professionals as educators. That finding "has enormous importance for the scalability and economic sustainability of diabetes interventions," Dr. Ali and his colleagues noted, because lay educators required lower salaries and their training was neither costly nor time-consuming.
Programs that included more "core sessions" in which patients received counseling maintained the highest attendance rates. And higher attendance rates correlated positively with greater weight loss.
The rate of attrition varied greatly among the studies, ranging from 0% to 49%. In some studies that analyzed patient feedback, it appeared that attrition was more strongly related to patients’ perceptions of their risk and to their readiness to change than it was to specific features of the intervention, such as the number of counseling sessions.
No disclosure information was provided.
FROM HEALTH AFFAIRS
Major Finding: The mean weight loss across all 28 studies of lifestyle intervention programs was approximately 4%, which is considered clinically meaningful.
Data Source: A meta-analysis of 28 published U.S. studies (including 2,916 subjects) of lifestyle intervention programs incorporating the findings of the U.S. Diabetes Prevention Program to prevent diabetes by promoting weight loss.
Disclosures: No disclosure information was provided.