User login
Even low arsenic exposure linked to cardiovascular disease
Even low to moderate levels of exposure to inorganic arsenic in food and water correlate with cardiovascular disease incidence and mortality, according to an analysis of the Strong Heart Study.
The results were published online Sept. 24 in Annals of Internal Medicine.
High environmental arsenic levels have long been recognized as correlating with higher risk of cardiovascular disease, but a secondary analysis of data from a large prospective heart study now shows that even at low levels commonly found in rural communities across the United States, arsenic exposure is strongly related to cardiovascular risk and mortality in a dose-dependent fashion.
"These findings support the importance of low to moderate arsenic exposure as a cardiovascular risk factor with no apparent threshold," said Katherine A. Moon of the department of environmental sciences, Johns Hopkins University Bloomberg School of Public Health, Baltimore, and her associates.
They assessed this correlation using data from the Strong Heart Study, a population-based cohort study of cardiovascular disease in three Native American communities in rural Arizona, Oklahoma, and the Dakotas. For their analysis, Ms. Moon and her colleagues measured arsenic species concentrations in stored urine samples from 3,575 men and women with no cardiovascular disease at enrollment during 1989-1991.
These study subjects, aged 45-75 years at baseline, were followed for cardiovascular outcomes for 17-19 years.
A total of 1,184 subjects developed cardiovascular disease during follow-up, with 846 incident coronary heart disease events and 264 incident strokes. A total of 439 subjects died from cardiovascular disease, including 341 who died from coronary heart disease and 54 who died from stroke.
Urinary arsenic concentrations at baseline correlated with the development of cardiovascular disease. Compared with men and women who had the lowest arsenic levels, those in the highest quartile were more likely to develop cardiovascular disease (hazard ratio 1.32), coronary heart disease (HR 1.30), and stroke (HR 1.47).
Urinary arsenic levels at baseline also correlated with cardiovascular mortality. Compared with men and women who had the lowest levels, those in the highest quartile were more likely to die from cardiovascular disease (hazard ratio, 1.65), coronary heart disease (HR, 1.71), or stroke (HR, 3.03).
These associations persisted after the data were adjusted to account for the effects of sociodemographic factors, smoking status, and lipid levels.
In contrast, urinary levels of arsenobetaine, an organic arsenical that is found chiefly in seafood and is thought to be nontoxic, showed no associations with cardiovascular outcomes.
Overall, these findings provide "important novel data in a Western population with high background cardiovascular risk," Ms. Moon and her associates noted.
The association between arsenic levels and cardiovascular risk was strongest among men and women who had diabetes, a subgroup of the population that has not been evaluated in previous studies of arsenic exposure. This finding "needs to be interpreted cautiously and requires replication in other populations," the researchers said.
The Environmental Protection Agency has estimated that 13 million Americans are chronically exposed to arsenic in drinking water, and many millions more are exposed to arsenic in food. It is possible that mitigating these exposures could reduce the burden of cardiovascular disease in the United States and across the globe, they added.
This study was supported by the National Heart, Lung, and Blood Institute and the National Institute of Environmental Health Sciences. No financial conflicts of interest were reported.
Even low to moderate levels of exposure to inorganic arsenic in food and water correlate with cardiovascular disease incidence and mortality, according to an analysis of the Strong Heart Study.
The results were published online Sept. 24 in Annals of Internal Medicine.
High environmental arsenic levels have long been recognized as correlating with higher risk of cardiovascular disease, but a secondary analysis of data from a large prospective heart study now shows that even at low levels commonly found in rural communities across the United States, arsenic exposure is strongly related to cardiovascular risk and mortality in a dose-dependent fashion.
"These findings support the importance of low to moderate arsenic exposure as a cardiovascular risk factor with no apparent threshold," said Katherine A. Moon of the department of environmental sciences, Johns Hopkins University Bloomberg School of Public Health, Baltimore, and her associates.
They assessed this correlation using data from the Strong Heart Study, a population-based cohort study of cardiovascular disease in three Native American communities in rural Arizona, Oklahoma, and the Dakotas. For their analysis, Ms. Moon and her colleagues measured arsenic species concentrations in stored urine samples from 3,575 men and women with no cardiovascular disease at enrollment during 1989-1991.
These study subjects, aged 45-75 years at baseline, were followed for cardiovascular outcomes for 17-19 years.
A total of 1,184 subjects developed cardiovascular disease during follow-up, with 846 incident coronary heart disease events and 264 incident strokes. A total of 439 subjects died from cardiovascular disease, including 341 who died from coronary heart disease and 54 who died from stroke.
Urinary arsenic concentrations at baseline correlated with the development of cardiovascular disease. Compared with men and women who had the lowest arsenic levels, those in the highest quartile were more likely to develop cardiovascular disease (hazard ratio 1.32), coronary heart disease (HR 1.30), and stroke (HR 1.47).
Urinary arsenic levels at baseline also correlated with cardiovascular mortality. Compared with men and women who had the lowest levels, those in the highest quartile were more likely to die from cardiovascular disease (hazard ratio, 1.65), coronary heart disease (HR, 1.71), or stroke (HR, 3.03).
These associations persisted after the data were adjusted to account for the effects of sociodemographic factors, smoking status, and lipid levels.
In contrast, urinary levels of arsenobetaine, an organic arsenical that is found chiefly in seafood and is thought to be nontoxic, showed no associations with cardiovascular outcomes.
Overall, these findings provide "important novel data in a Western population with high background cardiovascular risk," Ms. Moon and her associates noted.
The association between arsenic levels and cardiovascular risk was strongest among men and women who had diabetes, a subgroup of the population that has not been evaluated in previous studies of arsenic exposure. This finding "needs to be interpreted cautiously and requires replication in other populations," the researchers said.
The Environmental Protection Agency has estimated that 13 million Americans are chronically exposed to arsenic in drinking water, and many millions more are exposed to arsenic in food. It is possible that mitigating these exposures could reduce the burden of cardiovascular disease in the United States and across the globe, they added.
This study was supported by the National Heart, Lung, and Blood Institute and the National Institute of Environmental Health Sciences. No financial conflicts of interest were reported.
Even low to moderate levels of exposure to inorganic arsenic in food and water correlate with cardiovascular disease incidence and mortality, according to an analysis of the Strong Heart Study.
The results were published online Sept. 24 in Annals of Internal Medicine.
High environmental arsenic levels have long been recognized as correlating with higher risk of cardiovascular disease, but a secondary analysis of data from a large prospective heart study now shows that even at low levels commonly found in rural communities across the United States, arsenic exposure is strongly related to cardiovascular risk and mortality in a dose-dependent fashion.
"These findings support the importance of low to moderate arsenic exposure as a cardiovascular risk factor with no apparent threshold," said Katherine A. Moon of the department of environmental sciences, Johns Hopkins University Bloomberg School of Public Health, Baltimore, and her associates.
They assessed this correlation using data from the Strong Heart Study, a population-based cohort study of cardiovascular disease in three Native American communities in rural Arizona, Oklahoma, and the Dakotas. For their analysis, Ms. Moon and her colleagues measured arsenic species concentrations in stored urine samples from 3,575 men and women with no cardiovascular disease at enrollment during 1989-1991.
These study subjects, aged 45-75 years at baseline, were followed for cardiovascular outcomes for 17-19 years.
A total of 1,184 subjects developed cardiovascular disease during follow-up, with 846 incident coronary heart disease events and 264 incident strokes. A total of 439 subjects died from cardiovascular disease, including 341 who died from coronary heart disease and 54 who died from stroke.
Urinary arsenic concentrations at baseline correlated with the development of cardiovascular disease. Compared with men and women who had the lowest arsenic levels, those in the highest quartile were more likely to develop cardiovascular disease (hazard ratio 1.32), coronary heart disease (HR 1.30), and stroke (HR 1.47).
Urinary arsenic levels at baseline also correlated with cardiovascular mortality. Compared with men and women who had the lowest levels, those in the highest quartile were more likely to die from cardiovascular disease (hazard ratio, 1.65), coronary heart disease (HR, 1.71), or stroke (HR, 3.03).
These associations persisted after the data were adjusted to account for the effects of sociodemographic factors, smoking status, and lipid levels.
In contrast, urinary levels of arsenobetaine, an organic arsenical that is found chiefly in seafood and is thought to be nontoxic, showed no associations with cardiovascular outcomes.
Overall, these findings provide "important novel data in a Western population with high background cardiovascular risk," Ms. Moon and her associates noted.
The association between arsenic levels and cardiovascular risk was strongest among men and women who had diabetes, a subgroup of the population that has not been evaluated in previous studies of arsenic exposure. This finding "needs to be interpreted cautiously and requires replication in other populations," the researchers said.
The Environmental Protection Agency has estimated that 13 million Americans are chronically exposed to arsenic in drinking water, and many millions more are exposed to arsenic in food. It is possible that mitigating these exposures could reduce the burden of cardiovascular disease in the United States and across the globe, they added.
This study was supported by the National Heart, Lung, and Blood Institute and the National Institute of Environmental Health Sciences. No financial conflicts of interest were reported.
FROM ANNALS OF INTERNAL MEDICINE
Major Finding: Compared with subjects who had the lowest urinary levels of inorganic arsenic, those with the highest levels were at increased risk for incident CVD (HR 1.32), CVD mortality (HR 1.65 ), incident CHD (HR 1.30), CHD mortality (HR 1.71), incident stroke (HR 1.47), and stroke mortality (HR 3.03).
Data Source: A secondary analysis of data from the Strong Heart Study involving 3,973 Native American men and women aged 45-75 years at baseline who were followed for 17-19 years.
Disclosures: This study was supported by the National Heart, Lung, and Blood Institute and the National Institute of Environmental Health Sciences. No financial conflicts of interest were reported.
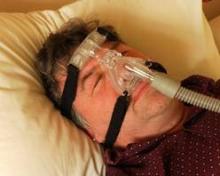
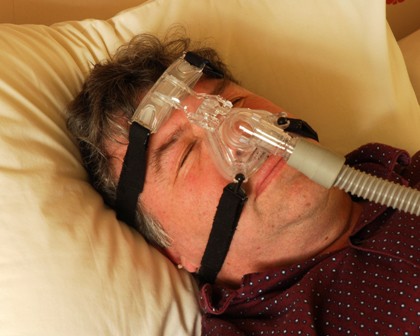
Start sleep apnea therapy with CPAP, not surgery
First-line treatment for adults with obstructive sleep apnea should be continuous positive airway pressure therapy or a mandibular advancement device, according to the American College of Physicians’ clinical practice guideline published online Sept. 24 in Annals of Internal Medicine.
In contrast, no surgical procedures or pharmacologic agents should be considered as first-line treatment, because there is insufficient evidence supporting those approaches, said Dr. Amir Qaseem, director of clinical policy at the ACP, Philadelphia, and his associates on the clinical guidelines committee.
Overweight and obese patients with obstructive sleep apnea (OSA) should be encouraged to lose weight, because that has been shown to improve symptoms and reduce scores on the Apnea-Hypopnea Index. Weight loss also confers many other health benefits, they added, while carrying minimal risk of adverse effects.
Those are the chief recommendations of the clinical practice guideline, which was compiled "to present information on both the benefits and harms of interventions" to all clinicians who treat adults with OSA. The guideline is based on a rigorous review of the evidence regarding OSA published in the literature from 1966 through 2012.
Overall, the evidence concerning hard clinical outcomes for any intervention for OSA was extremely limited.
Continuous positive airway pressure (CPAP) was the most extensively studied intervention for OSA, but the evidence from most studies was considered to be only of moderate quality. Studies assessed only the treatment’s effect on immediate outcomes and did not evaluate longer term outcomes such as cardiovascular illness or mortality. In addition, studies that examined CPAP’s effect on quality of life "were inconsistent and therefore inconclusive."
Nevertheless, the balance of evidence does show that CPAP is more effective than are control conditions or sham CPAP at improving scores on the apnea-hypopnea index, which measures the number of apneic and hypopneic episodes per hour of monitored sleep. CPAP also improved scores on the Epworth Sleepiness Scale, a self-administered questionnaire in which patients rate their likelihood of dozing off during various situations.
CPAP also is effective at improving oxygen saturation and reducing scores on the arousal index, which measures the frequency of arousals per hour of sleep using electroencephalography. However, there were insufficient data to compare the different types of CPAP, such as fixed CPAP, auto-CPAP, flexible bilevel CPAP, or CPAP with humidification.
There also was insufficient evidence to directly compare CPAP against other interventions, Dr. Qaseem and his colleagues said (Ann. Intern. Med. 2013;159:471-83).
The guideline recommends that mandibular or dental advancement devices to position the patient’s jaw while sleeping are a useful alternative for those who prefer this intervention to CPAP or for those who cannot tolerate or adhere to CPAP. Moderate-quality evidence showed that mandibular advancement devices improve scores on the apnea-hypopnea index and the arousal index.
However, that recommendation is considered "weak," because the overall data supporting the use of mandibular advancement devices are of low quality.
The data also were insufficient to recommend the use of any pharmacologic agents as a first-line therapy for OSA, or indeed as any therapy for the condition. Those include mirtazapine, xylometazoline, fluticasone, paroxetine, pantoprazole, steroids, acetazolamide, and protriptyline.
Only seven studies assessed surgical interventions for OSA. They were of varied quality, and their outcomes were inconsistent, so, the evidence is insufficient to support any surgery as first-line treatment. The procedures assessed in the studies included uvulopalatopharyngoplasty (UPPP); laser-assisted uvulopalatoplasty; radiofrequency ablation; and various combinations of pharyngoplasty, tonsillectomy, adenoidectomy, genioglossal advancement septoplasty, ablation of the nasal turbinates, and other nasal surgeries.
However, there was some evidence to suggest that UPPP and tracheostomy reduced mortality in patients with OSA.
The guideline strongly recommends that all OSA patients who are overweight or obese should be encouraged to lose weight. The evidence, albeit of low quality, shows that any intensive weight-loss intervention helps improve OSA symptoms and scores on the apnea-hypopnea index.
Finally, the evidence was insufficient to assess the potential benefits of positional therapy, oropharyngeal exercise, palatal implants, or atrial overdrive pacing for patients who already have dual-chamber pacemakers, Dr. Qaseem and his associates said.
The guideline was supported entirely by the American College of Physicians. The investigators had no relevant conflicts of interest.
Obesity is
epidemic in the United States
and “recommending to patients that they lose weight” is not a particularly
effective intervention. The real take-home message from this study is that
there is poor evidence for all treatments, but that the only studies showing a decreased
mortality were those involving surgery. Noninvasive remedies should generally
be preferred when deemed effective. Many patients find CPAP and oral appliances
uncomfortable and compliance rates with these treatments are poor. Obstructive
sleep apnea presents with a wide spectrum of symptoms, and occasionally, an
emergency tracheotomy may be lifesaving for a moribund patient. Patients with
severe OSA have a three- to sixfold increase in all-cause mortality. Motor
vehicle accidents are a major cause of death in patients with severe OSA. It
should also be emphasized that patients with OSA are best evaluated with a formal
sleep study to quantitate the degree of sleep apnea. OSA is a serious health
problem for which a variety of treatments are available. Although surgery is
rarely the first-line therapy, it plays an important role for patients with
particularly severe OSA, some of whom will require a tracheotomy, and in patients
for whom medical therapy is intolerable, not complied with, or ineffective.
Dr. Mark
Weissler is the J.P. Riddle Distinguished Professor of Otolaryngology – head
and neck surgery, University of North Carolina,
Chapel Hill.
Obesity is
epidemic in the United States
and “recommending to patients that they lose weight” is not a particularly
effective intervention. The real take-home message from this study is that
there is poor evidence for all treatments, but that the only studies showing a decreased
mortality were those involving surgery. Noninvasive remedies should generally
be preferred when deemed effective. Many patients find CPAP and oral appliances
uncomfortable and compliance rates with these treatments are poor. Obstructive
sleep apnea presents with a wide spectrum of symptoms, and occasionally, an
emergency tracheotomy may be lifesaving for a moribund patient. Patients with
severe OSA have a three- to sixfold increase in all-cause mortality. Motor
vehicle accidents are a major cause of death in patients with severe OSA. It
should also be emphasized that patients with OSA are best evaluated with a formal
sleep study to quantitate the degree of sleep apnea. OSA is a serious health
problem for which a variety of treatments are available. Although surgery is
rarely the first-line therapy, it plays an important role for patients with
particularly severe OSA, some of whom will require a tracheotomy, and in patients
for whom medical therapy is intolerable, not complied with, or ineffective.
Dr. Mark
Weissler is the J.P. Riddle Distinguished Professor of Otolaryngology – head
and neck surgery, University of North Carolina,
Chapel Hill.
Obesity is
epidemic in the United States
and “recommending to patients that they lose weight” is not a particularly
effective intervention. The real take-home message from this study is that
there is poor evidence for all treatments, but that the only studies showing a decreased
mortality were those involving surgery. Noninvasive remedies should generally
be preferred when deemed effective. Many patients find CPAP and oral appliances
uncomfortable and compliance rates with these treatments are poor. Obstructive
sleep apnea presents with a wide spectrum of symptoms, and occasionally, an
emergency tracheotomy may be lifesaving for a moribund patient. Patients with
severe OSA have a three- to sixfold increase in all-cause mortality. Motor
vehicle accidents are a major cause of death in patients with severe OSA. It
should also be emphasized that patients with OSA are best evaluated with a formal
sleep study to quantitate the degree of sleep apnea. OSA is a serious health
problem for which a variety of treatments are available. Although surgery is
rarely the first-line therapy, it plays an important role for patients with
particularly severe OSA, some of whom will require a tracheotomy, and in patients
for whom medical therapy is intolerable, not complied with, or ineffective.
Dr. Mark
Weissler is the J.P. Riddle Distinguished Professor of Otolaryngology – head
and neck surgery, University of North Carolina,
Chapel Hill.
First-line treatment for adults with obstructive sleep apnea should be continuous positive airway pressure therapy or a mandibular advancement device, according to the American College of Physicians’ clinical practice guideline published online Sept. 24 in Annals of Internal Medicine.
In contrast, no surgical procedures or pharmacologic agents should be considered as first-line treatment, because there is insufficient evidence supporting those approaches, said Dr. Amir Qaseem, director of clinical policy at the ACP, Philadelphia, and his associates on the clinical guidelines committee.
Overweight and obese patients with obstructive sleep apnea (OSA) should be encouraged to lose weight, because that has been shown to improve symptoms and reduce scores on the Apnea-Hypopnea Index. Weight loss also confers many other health benefits, they added, while carrying minimal risk of adverse effects.
Those are the chief recommendations of the clinical practice guideline, which was compiled "to present information on both the benefits and harms of interventions" to all clinicians who treat adults with OSA. The guideline is based on a rigorous review of the evidence regarding OSA published in the literature from 1966 through 2012.
Overall, the evidence concerning hard clinical outcomes for any intervention for OSA was extremely limited.
Continuous positive airway pressure (CPAP) was the most extensively studied intervention for OSA, but the evidence from most studies was considered to be only of moderate quality. Studies assessed only the treatment’s effect on immediate outcomes and did not evaluate longer term outcomes such as cardiovascular illness or mortality. In addition, studies that examined CPAP’s effect on quality of life "were inconsistent and therefore inconclusive."
Nevertheless, the balance of evidence does show that CPAP is more effective than are control conditions or sham CPAP at improving scores on the apnea-hypopnea index, which measures the number of apneic and hypopneic episodes per hour of monitored sleep. CPAP also improved scores on the Epworth Sleepiness Scale, a self-administered questionnaire in which patients rate their likelihood of dozing off during various situations.
CPAP also is effective at improving oxygen saturation and reducing scores on the arousal index, which measures the frequency of arousals per hour of sleep using electroencephalography. However, there were insufficient data to compare the different types of CPAP, such as fixed CPAP, auto-CPAP, flexible bilevel CPAP, or CPAP with humidification.
There also was insufficient evidence to directly compare CPAP against other interventions, Dr. Qaseem and his colleagues said (Ann. Intern. Med. 2013;159:471-83).
The guideline recommends that mandibular or dental advancement devices to position the patient’s jaw while sleeping are a useful alternative for those who prefer this intervention to CPAP or for those who cannot tolerate or adhere to CPAP. Moderate-quality evidence showed that mandibular advancement devices improve scores on the apnea-hypopnea index and the arousal index.
However, that recommendation is considered "weak," because the overall data supporting the use of mandibular advancement devices are of low quality.
The data also were insufficient to recommend the use of any pharmacologic agents as a first-line therapy for OSA, or indeed as any therapy for the condition. Those include mirtazapine, xylometazoline, fluticasone, paroxetine, pantoprazole, steroids, acetazolamide, and protriptyline.
Only seven studies assessed surgical interventions for OSA. They were of varied quality, and their outcomes were inconsistent, so, the evidence is insufficient to support any surgery as first-line treatment. The procedures assessed in the studies included uvulopalatopharyngoplasty (UPPP); laser-assisted uvulopalatoplasty; radiofrequency ablation; and various combinations of pharyngoplasty, tonsillectomy, adenoidectomy, genioglossal advancement septoplasty, ablation of the nasal turbinates, and other nasal surgeries.
However, there was some evidence to suggest that UPPP and tracheostomy reduced mortality in patients with OSA.
The guideline strongly recommends that all OSA patients who are overweight or obese should be encouraged to lose weight. The evidence, albeit of low quality, shows that any intensive weight-loss intervention helps improve OSA symptoms and scores on the apnea-hypopnea index.
Finally, the evidence was insufficient to assess the potential benefits of positional therapy, oropharyngeal exercise, palatal implants, or atrial overdrive pacing for patients who already have dual-chamber pacemakers, Dr. Qaseem and his associates said.
The guideline was supported entirely by the American College of Physicians. The investigators had no relevant conflicts of interest.
First-line treatment for adults with obstructive sleep apnea should be continuous positive airway pressure therapy or a mandibular advancement device, according to the American College of Physicians’ clinical practice guideline published online Sept. 24 in Annals of Internal Medicine.
In contrast, no surgical procedures or pharmacologic agents should be considered as first-line treatment, because there is insufficient evidence supporting those approaches, said Dr. Amir Qaseem, director of clinical policy at the ACP, Philadelphia, and his associates on the clinical guidelines committee.
Overweight and obese patients with obstructive sleep apnea (OSA) should be encouraged to lose weight, because that has been shown to improve symptoms and reduce scores on the Apnea-Hypopnea Index. Weight loss also confers many other health benefits, they added, while carrying minimal risk of adverse effects.
Those are the chief recommendations of the clinical practice guideline, which was compiled "to present information on both the benefits and harms of interventions" to all clinicians who treat adults with OSA. The guideline is based on a rigorous review of the evidence regarding OSA published in the literature from 1966 through 2012.
Overall, the evidence concerning hard clinical outcomes for any intervention for OSA was extremely limited.
Continuous positive airway pressure (CPAP) was the most extensively studied intervention for OSA, but the evidence from most studies was considered to be only of moderate quality. Studies assessed only the treatment’s effect on immediate outcomes and did not evaluate longer term outcomes such as cardiovascular illness or mortality. In addition, studies that examined CPAP’s effect on quality of life "were inconsistent and therefore inconclusive."
Nevertheless, the balance of evidence does show that CPAP is more effective than are control conditions or sham CPAP at improving scores on the apnea-hypopnea index, which measures the number of apneic and hypopneic episodes per hour of monitored sleep. CPAP also improved scores on the Epworth Sleepiness Scale, a self-administered questionnaire in which patients rate their likelihood of dozing off during various situations.
CPAP also is effective at improving oxygen saturation and reducing scores on the arousal index, which measures the frequency of arousals per hour of sleep using electroencephalography. However, there were insufficient data to compare the different types of CPAP, such as fixed CPAP, auto-CPAP, flexible bilevel CPAP, or CPAP with humidification.
There also was insufficient evidence to directly compare CPAP against other interventions, Dr. Qaseem and his colleagues said (Ann. Intern. Med. 2013;159:471-83).
The guideline recommends that mandibular or dental advancement devices to position the patient’s jaw while sleeping are a useful alternative for those who prefer this intervention to CPAP or for those who cannot tolerate or adhere to CPAP. Moderate-quality evidence showed that mandibular advancement devices improve scores on the apnea-hypopnea index and the arousal index.
However, that recommendation is considered "weak," because the overall data supporting the use of mandibular advancement devices are of low quality.
The data also were insufficient to recommend the use of any pharmacologic agents as a first-line therapy for OSA, or indeed as any therapy for the condition. Those include mirtazapine, xylometazoline, fluticasone, paroxetine, pantoprazole, steroids, acetazolamide, and protriptyline.
Only seven studies assessed surgical interventions for OSA. They were of varied quality, and their outcomes were inconsistent, so, the evidence is insufficient to support any surgery as first-line treatment. The procedures assessed in the studies included uvulopalatopharyngoplasty (UPPP); laser-assisted uvulopalatoplasty; radiofrequency ablation; and various combinations of pharyngoplasty, tonsillectomy, adenoidectomy, genioglossal advancement septoplasty, ablation of the nasal turbinates, and other nasal surgeries.
However, there was some evidence to suggest that UPPP and tracheostomy reduced mortality in patients with OSA.
The guideline strongly recommends that all OSA patients who are overweight or obese should be encouraged to lose weight. The evidence, albeit of low quality, shows that any intensive weight-loss intervention helps improve OSA symptoms and scores on the apnea-hypopnea index.
Finally, the evidence was insufficient to assess the potential benefits of positional therapy, oropharyngeal exercise, palatal implants, or atrial overdrive pacing for patients who already have dual-chamber pacemakers, Dr. Qaseem and his associates said.
The guideline was supported entirely by the American College of Physicians. The investigators had no relevant conflicts of interest.
FROM ANNALS OF INTERNAL MEDICINE
Major finding: First-line therapy for adults with obstructive sleep apnea should be CPAP or a mandibular advancement device; surgery and pharmacotherapy do not appear to be effective, and weight loss is strongly recommended for patients who are overweight or obese.
Data source: The guideline was based on a systematic review of the literature regarding obstructive sleep apnea from 1966 through 2010.
Disclosures: The guideline was supported entirely by the American College of Physicians. The investigators had no relevant conflicts of interest.
Colorectal cancer screening cuts long-term mortality
The long-term incidence of colorectal cancer was lower in patients who underwent screening by either endoscopy or fecal occult-blood testing than in those who did not, even if that screening took place decades earlier, according to two separate reports published online Sept. 19 in the New England Journal of Medicine.
Importantly, colorectal cancer–related mortality also was correspondingly lower in screened patients.
Identifying and removing colorectal polyps yields far-reaching benefits, saving lives for up to 30 years afterward, researchers involved in both studies said.
In the first study, Reiko Nishihara, Ph.D., of the Dana-Farber Cancer Institute and Harvard Medical School, Boston, and her associates assessed lower-GI endoscopy’s effect on the long-term risk of incident colorectal cancer in two large U.S. cohorts that were prospectively followed for 22 years. The Nurses’ Health Study involved 121,700 female nurses aged 30-55 years at baseline in 1976, and the Health Professionals Follow-Up Study involved 51,529 male health professionals aged 40-75 years at baseline in 1986.
For their secondary analysis of data from these cohorts, Dr. Nishihara and her colleagues examined the records of 57,166 female subjects and 31,736 male subjects who developed 1,815 incident colorectal cancers during 22 years of follow-up. "We were able to directly compare actual incidences of cancer among persons after polypectomy with the incidences among persons from the same background population who did not undergo endoscopy, while adjusting for potential confounders."
At their own discretion, 14,287 of the men and 31,423 of the women had undergone no lower endoscopy at all by 1998, the midpoint of follow-up; 3,578 men and 3,957 women had undergone colonoscopy with negative results; 8,091 men and 16,748 women had undergone sigmoidoscopy with negative results; and 1,259 men and 1,481 women had undergone lower endoscopy with polypectomy.
At the end of follow-up, the incidence of colorectal cancer was significantly lower among the men and women who had undergone any of these screening methods than among those who had not had any screening. The multivariate hazard ratios for colorectal cancer were 0.57 after endoscopy plus removal of adenomatous polyps (polypectomy), 0.60 after negative sigmoidoscopy, and 0.44 after negative colonoscopy.
"We estimated that 40% of colorectal cancers (including 61% of distal colorectal cancers and 22% of proximal colon cancers) that developed during follow-up would have been prevented if all the participants in our study had undergone colonoscopy," the investigators said (N. Engl. J. Med. 2013 Sept. 19 [doi:10.1056/NEJMoa1301969]).
This decrease in colorectal cancer occurred in both men and women, across all stages of disease at presentation, and regardless of subject age, body mass index, smoking status, or use of aspirin prophylaxis.
"Negative colonoscopy was associated with a lower incidence of both distal colorectal cancer and proximal colon cancer, whereas negative sigmoidoscopy and colonoscopy with polypectomy were associated primarily with a lower incidence of distal colorectal cancer," they said.
Notably, screening sigmoidoscopy and screening colonoscopy were associated with lower colorectal cancer–specific mortality, compared with no endoscopy.
The association between a negative colonoscopy and a significantly reduced incidence of colorectal cancer persisted for up to 15 years after the procedure. Thus, "our findings support the 10-year examination interval recommended by existing guidelines for persons at average risk who have a negative colonoscopy. Our study suggests that even a single negative colonoscopy is associated with a very low long-term risk of colorectal cancer," Dr. Nishihara and her associates said.
Among study subjects who were found to have adenomas, the reduced incidence of colorectal cancer persisted for up to 5 years after the procedure. Thus, "our data support screening at more frequent intervals for persons with a family history of colorectal cancer, which [also] supports current surveillance guidelines."
The researchers also examined DNA from stored specimens of tumors from 62 patients who developed colorectal cancer within 5 years of "passing" an endoscopy. Compared with other cancers, these interval cancers were much more likely to have CpG island methylator phenotype (CIMP), microsatellite instability, and high levels of LINE-1 methylation – all indicators of increased tumor aggressiveness.
It is possible that such lesions are particularly difficult to detect endoscopically or to remove adequately. "It remains unclear whether any of the challenges posed by these biological differences can be addressed by improvements in colonoscopic technique, including more meticulous inspection or improved bowel cleaning," the researchers said.
In the second study, a different research group found that adults who were screened for colorectal cancer using fecal occult blood testing (FOBT) had a 32% decrease in colorectal cancer–related mortality for up to 30 years afterward.
This association appeared to be stronger for men than for women, said Dr. Aasma Shaukat of the Minneapolis Veterans Affairs Health Care System and the University of Minnesota, Minneapolis, and her associates.
They performed a secondary analysis of data from the Minnesota Colon Cancer Control Study, in which 46,551 healthy men and women aged 50-80 years at baseline in 1975 through 1978 were randomly assigned to undergo annual, biennial, or no FOBT screening until 1993. Dr. Shaukat and her colleagues attempted to identify the mortality status and cause of death for as many of these study subjects as possible in 2011.
They identified 33,020 deaths, which represents 71% of the entire study population. A total of 732 deaths were from colorectal cancer.
Both annual and biennial FOBT screening reduced colorectal-cancer-specific mortality by approximately one-third for up to 30 years. The relative risk of death from colorectal cancer was 0.68 with annual FOBT and 0.78 with biennial FOBT, compared with no FOBT. Overall, the relative risk of death with any FOBT screening was 0.73, compared with no FOBT.
This reduction "is consistent with the effect of removing adenomas that would have progressed to cancer and death," Dr. Shaukat and her associates said (N. Engl. J. Med. 2013 [doi:10.1056/NEJMoa1300720]).
The decline in colorectal cancer-specific mortality was greater for men than for women.
"The high accessibility and acceptability of stool-based tests have major public health implications for improving screening rates, although this approach to screening involves more frequent testing than does screening with flexible sigmoidoscopy or colonoscopy," the investigators noted.
Dr. Nishihara’s study was supported by the National Institutes of Health, the Bennett Family Foundation, and the Entertainment Industry Foundation. Dr. Nishihara reported no ties to industry sources; one of her associates reported ties to Bayer Healthcare, Pfizer, Millenium Pharmaceuticals, and Pozen. Dr. Shaukat’s study was supported by the Veterans Affairs Merit Review Reward Program, the National Institutes of Health, and the National Cancer Institute. Dr. Shaukat and her associates reported no financial conflicts of interest.
These two studies confirm that both colonoscopy and FOBT are effective for colorectal cancer screening, and reaffirm that current screening guidelines are appropriate, said Dr. Theodore R. Levin and Dr. Douglas A. Corley.
However, the two studies are different and have study populations that are not comparable, so it would be a mistake to compare them with each other. "One was a randomized trial, the other an observational study of volunteers, and both [screening] tests have undergone improvements since the studies were performed," they noted.
Randomized trials that are currently underway will clarify remaining questions about the relative value of colonoscopy vs. FOBT, the biologic features of interval cancers, and the overall effectiveness of colorectal-cancer screening programs, Drs. Levin and Corley said.
Dr. Theodore R. Levin and Dr. Douglas A. Corley are at the Kaiser Permanente Medical Centers in Walnut Creek, Antioch, and San Francisco, CA. They reported no relevant financial conflicts of interest. These remarks were taken from their editorial accompanying the reports by Dr. Nishihara and Dr. Shaukat (N. Engl. J. Med. 2013;369:1164-6).
These two studies confirm that both colonoscopy and FOBT are effective for colorectal cancer screening, and reaffirm that current screening guidelines are appropriate, said Dr. Theodore R. Levin and Dr. Douglas A. Corley.
However, the two studies are different and have study populations that are not comparable, so it would be a mistake to compare them with each other. "One was a randomized trial, the other an observational study of volunteers, and both [screening] tests have undergone improvements since the studies were performed," they noted.
Randomized trials that are currently underway will clarify remaining questions about the relative value of colonoscopy vs. FOBT, the biologic features of interval cancers, and the overall effectiveness of colorectal-cancer screening programs, Drs. Levin and Corley said.
Dr. Theodore R. Levin and Dr. Douglas A. Corley are at the Kaiser Permanente Medical Centers in Walnut Creek, Antioch, and San Francisco, CA. They reported no relevant financial conflicts of interest. These remarks were taken from their editorial accompanying the reports by Dr. Nishihara and Dr. Shaukat (N. Engl. J. Med. 2013;369:1164-6).
These two studies confirm that both colonoscopy and FOBT are effective for colorectal cancer screening, and reaffirm that current screening guidelines are appropriate, said Dr. Theodore R. Levin and Dr. Douglas A. Corley.
However, the two studies are different and have study populations that are not comparable, so it would be a mistake to compare them with each other. "One was a randomized trial, the other an observational study of volunteers, and both [screening] tests have undergone improvements since the studies were performed," they noted.
Randomized trials that are currently underway will clarify remaining questions about the relative value of colonoscopy vs. FOBT, the biologic features of interval cancers, and the overall effectiveness of colorectal-cancer screening programs, Drs. Levin and Corley said.
Dr. Theodore R. Levin and Dr. Douglas A. Corley are at the Kaiser Permanente Medical Centers in Walnut Creek, Antioch, and San Francisco, CA. They reported no relevant financial conflicts of interest. These remarks were taken from their editorial accompanying the reports by Dr. Nishihara and Dr. Shaukat (N. Engl. J. Med. 2013;369:1164-6).
The long-term incidence of colorectal cancer was lower in patients who underwent screening by either endoscopy or fecal occult-blood testing than in those who did not, even if that screening took place decades earlier, according to two separate reports published online Sept. 19 in the New England Journal of Medicine.
Importantly, colorectal cancer–related mortality also was correspondingly lower in screened patients.
Identifying and removing colorectal polyps yields far-reaching benefits, saving lives for up to 30 years afterward, researchers involved in both studies said.
In the first study, Reiko Nishihara, Ph.D., of the Dana-Farber Cancer Institute and Harvard Medical School, Boston, and her associates assessed lower-GI endoscopy’s effect on the long-term risk of incident colorectal cancer in two large U.S. cohorts that were prospectively followed for 22 years. The Nurses’ Health Study involved 121,700 female nurses aged 30-55 years at baseline in 1976, and the Health Professionals Follow-Up Study involved 51,529 male health professionals aged 40-75 years at baseline in 1986.
For their secondary analysis of data from these cohorts, Dr. Nishihara and her colleagues examined the records of 57,166 female subjects and 31,736 male subjects who developed 1,815 incident colorectal cancers during 22 years of follow-up. "We were able to directly compare actual incidences of cancer among persons after polypectomy with the incidences among persons from the same background population who did not undergo endoscopy, while adjusting for potential confounders."
At their own discretion, 14,287 of the men and 31,423 of the women had undergone no lower endoscopy at all by 1998, the midpoint of follow-up; 3,578 men and 3,957 women had undergone colonoscopy with negative results; 8,091 men and 16,748 women had undergone sigmoidoscopy with negative results; and 1,259 men and 1,481 women had undergone lower endoscopy with polypectomy.
At the end of follow-up, the incidence of colorectal cancer was significantly lower among the men and women who had undergone any of these screening methods than among those who had not had any screening. The multivariate hazard ratios for colorectal cancer were 0.57 after endoscopy plus removal of adenomatous polyps (polypectomy), 0.60 after negative sigmoidoscopy, and 0.44 after negative colonoscopy.
"We estimated that 40% of colorectal cancers (including 61% of distal colorectal cancers and 22% of proximal colon cancers) that developed during follow-up would have been prevented if all the participants in our study had undergone colonoscopy," the investigators said (N. Engl. J. Med. 2013 Sept. 19 [doi:10.1056/NEJMoa1301969]).
This decrease in colorectal cancer occurred in both men and women, across all stages of disease at presentation, and regardless of subject age, body mass index, smoking status, or use of aspirin prophylaxis.
"Negative colonoscopy was associated with a lower incidence of both distal colorectal cancer and proximal colon cancer, whereas negative sigmoidoscopy and colonoscopy with polypectomy were associated primarily with a lower incidence of distal colorectal cancer," they said.
Notably, screening sigmoidoscopy and screening colonoscopy were associated with lower colorectal cancer–specific mortality, compared with no endoscopy.
The association between a negative colonoscopy and a significantly reduced incidence of colorectal cancer persisted for up to 15 years after the procedure. Thus, "our findings support the 10-year examination interval recommended by existing guidelines for persons at average risk who have a negative colonoscopy. Our study suggests that even a single negative colonoscopy is associated with a very low long-term risk of colorectal cancer," Dr. Nishihara and her associates said.
Among study subjects who were found to have adenomas, the reduced incidence of colorectal cancer persisted for up to 5 years after the procedure. Thus, "our data support screening at more frequent intervals for persons with a family history of colorectal cancer, which [also] supports current surveillance guidelines."
The researchers also examined DNA from stored specimens of tumors from 62 patients who developed colorectal cancer within 5 years of "passing" an endoscopy. Compared with other cancers, these interval cancers were much more likely to have CpG island methylator phenotype (CIMP), microsatellite instability, and high levels of LINE-1 methylation – all indicators of increased tumor aggressiveness.
It is possible that such lesions are particularly difficult to detect endoscopically or to remove adequately. "It remains unclear whether any of the challenges posed by these biological differences can be addressed by improvements in colonoscopic technique, including more meticulous inspection or improved bowel cleaning," the researchers said.
In the second study, a different research group found that adults who were screened for colorectal cancer using fecal occult blood testing (FOBT) had a 32% decrease in colorectal cancer–related mortality for up to 30 years afterward.
This association appeared to be stronger for men than for women, said Dr. Aasma Shaukat of the Minneapolis Veterans Affairs Health Care System and the University of Minnesota, Minneapolis, and her associates.
They performed a secondary analysis of data from the Minnesota Colon Cancer Control Study, in which 46,551 healthy men and women aged 50-80 years at baseline in 1975 through 1978 were randomly assigned to undergo annual, biennial, or no FOBT screening until 1993. Dr. Shaukat and her colleagues attempted to identify the mortality status and cause of death for as many of these study subjects as possible in 2011.
They identified 33,020 deaths, which represents 71% of the entire study population. A total of 732 deaths were from colorectal cancer.
Both annual and biennial FOBT screening reduced colorectal-cancer-specific mortality by approximately one-third for up to 30 years. The relative risk of death from colorectal cancer was 0.68 with annual FOBT and 0.78 with biennial FOBT, compared with no FOBT. Overall, the relative risk of death with any FOBT screening was 0.73, compared with no FOBT.
This reduction "is consistent with the effect of removing adenomas that would have progressed to cancer and death," Dr. Shaukat and her associates said (N. Engl. J. Med. 2013 [doi:10.1056/NEJMoa1300720]).
The decline in colorectal cancer-specific mortality was greater for men than for women.
"The high accessibility and acceptability of stool-based tests have major public health implications for improving screening rates, although this approach to screening involves more frequent testing than does screening with flexible sigmoidoscopy or colonoscopy," the investigators noted.
Dr. Nishihara’s study was supported by the National Institutes of Health, the Bennett Family Foundation, and the Entertainment Industry Foundation. Dr. Nishihara reported no ties to industry sources; one of her associates reported ties to Bayer Healthcare, Pfizer, Millenium Pharmaceuticals, and Pozen. Dr. Shaukat’s study was supported by the Veterans Affairs Merit Review Reward Program, the National Institutes of Health, and the National Cancer Institute. Dr. Shaukat and her associates reported no financial conflicts of interest.
The long-term incidence of colorectal cancer was lower in patients who underwent screening by either endoscopy or fecal occult-blood testing than in those who did not, even if that screening took place decades earlier, according to two separate reports published online Sept. 19 in the New England Journal of Medicine.
Importantly, colorectal cancer–related mortality also was correspondingly lower in screened patients.
Identifying and removing colorectal polyps yields far-reaching benefits, saving lives for up to 30 years afterward, researchers involved in both studies said.
In the first study, Reiko Nishihara, Ph.D., of the Dana-Farber Cancer Institute and Harvard Medical School, Boston, and her associates assessed lower-GI endoscopy’s effect on the long-term risk of incident colorectal cancer in two large U.S. cohorts that were prospectively followed for 22 years. The Nurses’ Health Study involved 121,700 female nurses aged 30-55 years at baseline in 1976, and the Health Professionals Follow-Up Study involved 51,529 male health professionals aged 40-75 years at baseline in 1986.
For their secondary analysis of data from these cohorts, Dr. Nishihara and her colleagues examined the records of 57,166 female subjects and 31,736 male subjects who developed 1,815 incident colorectal cancers during 22 years of follow-up. "We were able to directly compare actual incidences of cancer among persons after polypectomy with the incidences among persons from the same background population who did not undergo endoscopy, while adjusting for potential confounders."
At their own discretion, 14,287 of the men and 31,423 of the women had undergone no lower endoscopy at all by 1998, the midpoint of follow-up; 3,578 men and 3,957 women had undergone colonoscopy with negative results; 8,091 men and 16,748 women had undergone sigmoidoscopy with negative results; and 1,259 men and 1,481 women had undergone lower endoscopy with polypectomy.
At the end of follow-up, the incidence of colorectal cancer was significantly lower among the men and women who had undergone any of these screening methods than among those who had not had any screening. The multivariate hazard ratios for colorectal cancer were 0.57 after endoscopy plus removal of adenomatous polyps (polypectomy), 0.60 after negative sigmoidoscopy, and 0.44 after negative colonoscopy.
"We estimated that 40% of colorectal cancers (including 61% of distal colorectal cancers and 22% of proximal colon cancers) that developed during follow-up would have been prevented if all the participants in our study had undergone colonoscopy," the investigators said (N. Engl. J. Med. 2013 Sept. 19 [doi:10.1056/NEJMoa1301969]).
This decrease in colorectal cancer occurred in both men and women, across all stages of disease at presentation, and regardless of subject age, body mass index, smoking status, or use of aspirin prophylaxis.
"Negative colonoscopy was associated with a lower incidence of both distal colorectal cancer and proximal colon cancer, whereas negative sigmoidoscopy and colonoscopy with polypectomy were associated primarily with a lower incidence of distal colorectal cancer," they said.
Notably, screening sigmoidoscopy and screening colonoscopy were associated with lower colorectal cancer–specific mortality, compared with no endoscopy.
The association between a negative colonoscopy and a significantly reduced incidence of colorectal cancer persisted for up to 15 years after the procedure. Thus, "our findings support the 10-year examination interval recommended by existing guidelines for persons at average risk who have a negative colonoscopy. Our study suggests that even a single negative colonoscopy is associated with a very low long-term risk of colorectal cancer," Dr. Nishihara and her associates said.
Among study subjects who were found to have adenomas, the reduced incidence of colorectal cancer persisted for up to 5 years after the procedure. Thus, "our data support screening at more frequent intervals for persons with a family history of colorectal cancer, which [also] supports current surveillance guidelines."
The researchers also examined DNA from stored specimens of tumors from 62 patients who developed colorectal cancer within 5 years of "passing" an endoscopy. Compared with other cancers, these interval cancers were much more likely to have CpG island methylator phenotype (CIMP), microsatellite instability, and high levels of LINE-1 methylation – all indicators of increased tumor aggressiveness.
It is possible that such lesions are particularly difficult to detect endoscopically or to remove adequately. "It remains unclear whether any of the challenges posed by these biological differences can be addressed by improvements in colonoscopic technique, including more meticulous inspection or improved bowel cleaning," the researchers said.
In the second study, a different research group found that adults who were screened for colorectal cancer using fecal occult blood testing (FOBT) had a 32% decrease in colorectal cancer–related mortality for up to 30 years afterward.
This association appeared to be stronger for men than for women, said Dr. Aasma Shaukat of the Minneapolis Veterans Affairs Health Care System and the University of Minnesota, Minneapolis, and her associates.
They performed a secondary analysis of data from the Minnesota Colon Cancer Control Study, in which 46,551 healthy men and women aged 50-80 years at baseline in 1975 through 1978 were randomly assigned to undergo annual, biennial, or no FOBT screening until 1993. Dr. Shaukat and her colleagues attempted to identify the mortality status and cause of death for as many of these study subjects as possible in 2011.
They identified 33,020 deaths, which represents 71% of the entire study population. A total of 732 deaths were from colorectal cancer.
Both annual and biennial FOBT screening reduced colorectal-cancer-specific mortality by approximately one-third for up to 30 years. The relative risk of death from colorectal cancer was 0.68 with annual FOBT and 0.78 with biennial FOBT, compared with no FOBT. Overall, the relative risk of death with any FOBT screening was 0.73, compared with no FOBT.
This reduction "is consistent with the effect of removing adenomas that would have progressed to cancer and death," Dr. Shaukat and her associates said (N. Engl. J. Med. 2013 [doi:10.1056/NEJMoa1300720]).
The decline in colorectal cancer-specific mortality was greater for men than for women.
"The high accessibility and acceptability of stool-based tests have major public health implications for improving screening rates, although this approach to screening involves more frequent testing than does screening with flexible sigmoidoscopy or colonoscopy," the investigators noted.
Dr. Nishihara’s study was supported by the National Institutes of Health, the Bennett Family Foundation, and the Entertainment Industry Foundation. Dr. Nishihara reported no ties to industry sources; one of her associates reported ties to Bayer Healthcare, Pfizer, Millenium Pharmaceuticals, and Pozen. Dr. Shaukat’s study was supported by the Veterans Affairs Merit Review Reward Program, the National Institutes of Health, and the National Cancer Institute. Dr. Shaukat and her associates reported no financial conflicts of interest.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major finding: The multivariate hazard ratios for colorectal cancer were 0.57 after endoscopy plus removal of adenomatous polyps (polypectomy), 0.60 after negative sigmoidoscopy, and 0.44 after negative colonoscopy.
Data source: A secondary analysis of data from two large cohort studies regarding the 22-year incidence of colorectal cancer among healthy men and women who either had or had not undergone endoscopy, and a secondary analysis of data from a study in which 46,551 healthy volunteers had annual, biennial, or no FOBT screening for colorectal cancer during a 16-year period and were followed up 20-30 years later.
Disclosures: Dr. Nishihara’s study was supported by the National Institutes of Health, the Bennett Family Foundation, and the Entertainment Industry Foundation. Dr. Nishihara reported no ties to industry sources; one of her associates reported ties to Bayer Healthcare, Pfizer, Millenium Pharmaceuticals, and Pozen. Dr. Shaukat’s study was supported by the Veterans Affairs Merit Review Reward Program, the National Institutes of Health, and the National Cancer Institute. Dr. Shaukat and her associates reported no financial conflicts of interest.
Sling surgery bests physiotherapy as initial treatment
Among women who had moderate to severe stress urinary incontinence, those who underwent midurethral-sling surgery as the first line of treatment showed significantly more improvement 1 year later than did women whose initial treatment was physiotherapy, according to a report published online Sept. 18 in the New England Journal of Medicine.
In a randomized Dutch trial involving 460 patients, 49 experienced gynecologists and urologists, and 83 certified pelvic physiotherapists, 1-year rates of both subjective and objective improvement, as well as rates of subjective and objective cure, were markedly higher for women who had immediate surgery than for those who had immediate physiotherapy, reported Dr. Julien Labrie of the University of Utrecht (the Netherlands) Medical Center and his associates.
Improvement in all secondary outcomes also was significantly better with initial surgery than with initial physiotherapy. These included urogenital symptoms, disease-specific quality of life, and the development of new urinary symptoms. However, all 65 adverse events that occurred in the study were related to surgery, including intraoperative bladder perforations, vaginal epithelial perforations, excessive blood loss, and four cases in which reoperation was required.
"Our findings suggest that women with this condition should be counseled regarding both pelvic-floor muscle training and midurethral-sling surgery as initial treatment options. Information on expected outcomes with both interventions, as well as on the potential, albeit infrequent, complications of surgery, will allow for individualized decision making by each woman and her health care provider," the investigators noted.
Dr. Labrie and his colleagues performed this study because standard practice is to recommend physiotherapy as first-line treatment, and to proceed to surgery only if that fails. Yet outcomes from midurethral-sling surgery and physiotherapy have never been directly compared.
Their study involved women aged 35-80 years whose stress urinary incontinence was classified as moderate or severe according to the Sandvik index. These subjects were randomly assigned to receive either initial surgery (230 women) or initial physiotherapy (230 women) at four university medical centers and 19 general hospitals over a 2-year period.
Both retropubic and transobturator midurethral-sling surgical approaches were allowed. Physiotherapy included an average of nine sessions delivered over 18 weeks, and could include biofeedback assistance or functional electrostimulation therapy.
The women were allowed to cross over to the other group if they were not satisfied with their assigned treatment, as "is consistent with usual clinical practice." The data were analyzed on an intention-to-treat basis. However, because approximately half of the physiotherapy group crossed over to surgery after a mean of 31 weeks, the investigators also performed a post hoc per-protocol analysis.
The primary outcome was subjective improvement in symptoms of stress urinary incontinence at 12 months, as measured by the Patient Global Impression of Improvement (PGI-I) scale. In the intention-to-treat analysis, the rate of this outcome was 90.8% with immediate surgery, significantly higher than the 64.4% rate with immediate physiotherapy, Dr. Labrie and his associates reported (New Engl. J. Med. 2013;369:1124-33 [doi: 10.1056/NEJMoa1210627]).
The pattern was the same when outcomes were assessed objectively using a cough stress test.
Both study groups showed improvement over time in urogenital symptoms as measured by the Urogenital Distress Inventory (UDI) and in disease-specific quality of life as measured by the Incontinence Impact Questionnaire (IIQ). The improvements were significantly greater in the immediate-surgery group for incontinence and overactive bladder, "but with only moderate effect sizes," the authors said.
Similarly, improvements were significantly greater in the immediate-surgery group for subscores regarding patients’ mobility and embarrassment, "but again with only moderate effect sizes," the researchers said.
In the post hoc per-protocol analysis, they compared the 103 women who only had physiotherapy, the 99 who had physiotherapy but crossed over to surgery, and the 215 who only had surgery. At 1 year, improvement in the physiotherapy-only group was lower by approximately 62% than in the crossover group and by 59% in the surgery-only group.
Adverse events, which occurred only in women who underwent surgery, included 6 cases of bladder perforation, 10 cases of vaginal epithelial perforation, 6 reoperations for tape exposure, 1 reoperation to loosen a too-tight synthetic sling, 20 hematomas, 18 cases of new-onset urge urinary incontinence, and 3 cases of excessive blood loss.
This study may have been limited by selection bias, because "women with a preference for surgery may have been more likely to participate in the study, because they otherwise would have received initial physiotherapy according to Dutch guidelines," Dr. Labrie and his associates said.
The study was supported by the Netherlands Organization for Health Research and Development (ZonMW) and was performed "without the support or involvement of manufacturers of midurethral slings." Several coauthors reported financial ties to Ethicon, American Medical Systems, and AMS. The remainder of the authors reported no relevant financial conflicts of interest.
Among women who had moderate to severe stress urinary incontinence, those who underwent midurethral-sling surgery as the first line of treatment showed significantly more improvement 1 year later than did women whose initial treatment was physiotherapy, according to a report published online Sept. 18 in the New England Journal of Medicine.
In a randomized Dutch trial involving 460 patients, 49 experienced gynecologists and urologists, and 83 certified pelvic physiotherapists, 1-year rates of both subjective and objective improvement, as well as rates of subjective and objective cure, were markedly higher for women who had immediate surgery than for those who had immediate physiotherapy, reported Dr. Julien Labrie of the University of Utrecht (the Netherlands) Medical Center and his associates.
Improvement in all secondary outcomes also was significantly better with initial surgery than with initial physiotherapy. These included urogenital symptoms, disease-specific quality of life, and the development of new urinary symptoms. However, all 65 adverse events that occurred in the study were related to surgery, including intraoperative bladder perforations, vaginal epithelial perforations, excessive blood loss, and four cases in which reoperation was required.
"Our findings suggest that women with this condition should be counseled regarding both pelvic-floor muscle training and midurethral-sling surgery as initial treatment options. Information on expected outcomes with both interventions, as well as on the potential, albeit infrequent, complications of surgery, will allow for individualized decision making by each woman and her health care provider," the investigators noted.
Dr. Labrie and his colleagues performed this study because standard practice is to recommend physiotherapy as first-line treatment, and to proceed to surgery only if that fails. Yet outcomes from midurethral-sling surgery and physiotherapy have never been directly compared.
Their study involved women aged 35-80 years whose stress urinary incontinence was classified as moderate or severe according to the Sandvik index. These subjects were randomly assigned to receive either initial surgery (230 women) or initial physiotherapy (230 women) at four university medical centers and 19 general hospitals over a 2-year period.
Both retropubic and transobturator midurethral-sling surgical approaches were allowed. Physiotherapy included an average of nine sessions delivered over 18 weeks, and could include biofeedback assistance or functional electrostimulation therapy.
The women were allowed to cross over to the other group if they were not satisfied with their assigned treatment, as "is consistent with usual clinical practice." The data were analyzed on an intention-to-treat basis. However, because approximately half of the physiotherapy group crossed over to surgery after a mean of 31 weeks, the investigators also performed a post hoc per-protocol analysis.
The primary outcome was subjective improvement in symptoms of stress urinary incontinence at 12 months, as measured by the Patient Global Impression of Improvement (PGI-I) scale. In the intention-to-treat analysis, the rate of this outcome was 90.8% with immediate surgery, significantly higher than the 64.4% rate with immediate physiotherapy, Dr. Labrie and his associates reported (New Engl. J. Med. 2013;369:1124-33 [doi: 10.1056/NEJMoa1210627]).
The pattern was the same when outcomes were assessed objectively using a cough stress test.
Both study groups showed improvement over time in urogenital symptoms as measured by the Urogenital Distress Inventory (UDI) and in disease-specific quality of life as measured by the Incontinence Impact Questionnaire (IIQ). The improvements were significantly greater in the immediate-surgery group for incontinence and overactive bladder, "but with only moderate effect sizes," the authors said.
Similarly, improvements were significantly greater in the immediate-surgery group for subscores regarding patients’ mobility and embarrassment, "but again with only moderate effect sizes," the researchers said.
In the post hoc per-protocol analysis, they compared the 103 women who only had physiotherapy, the 99 who had physiotherapy but crossed over to surgery, and the 215 who only had surgery. At 1 year, improvement in the physiotherapy-only group was lower by approximately 62% than in the crossover group and by 59% in the surgery-only group.
Adverse events, which occurred only in women who underwent surgery, included 6 cases of bladder perforation, 10 cases of vaginal epithelial perforation, 6 reoperations for tape exposure, 1 reoperation to loosen a too-tight synthetic sling, 20 hematomas, 18 cases of new-onset urge urinary incontinence, and 3 cases of excessive blood loss.
This study may have been limited by selection bias, because "women with a preference for surgery may have been more likely to participate in the study, because they otherwise would have received initial physiotherapy according to Dutch guidelines," Dr. Labrie and his associates said.
The study was supported by the Netherlands Organization for Health Research and Development (ZonMW) and was performed "without the support or involvement of manufacturers of midurethral slings." Several coauthors reported financial ties to Ethicon, American Medical Systems, and AMS. The remainder of the authors reported no relevant financial conflicts of interest.
Among women who had moderate to severe stress urinary incontinence, those who underwent midurethral-sling surgery as the first line of treatment showed significantly more improvement 1 year later than did women whose initial treatment was physiotherapy, according to a report published online Sept. 18 in the New England Journal of Medicine.
In a randomized Dutch trial involving 460 patients, 49 experienced gynecologists and urologists, and 83 certified pelvic physiotherapists, 1-year rates of both subjective and objective improvement, as well as rates of subjective and objective cure, were markedly higher for women who had immediate surgery than for those who had immediate physiotherapy, reported Dr. Julien Labrie of the University of Utrecht (the Netherlands) Medical Center and his associates.
Improvement in all secondary outcomes also was significantly better with initial surgery than with initial physiotherapy. These included urogenital symptoms, disease-specific quality of life, and the development of new urinary symptoms. However, all 65 adverse events that occurred in the study were related to surgery, including intraoperative bladder perforations, vaginal epithelial perforations, excessive blood loss, and four cases in which reoperation was required.
"Our findings suggest that women with this condition should be counseled regarding both pelvic-floor muscle training and midurethral-sling surgery as initial treatment options. Information on expected outcomes with both interventions, as well as on the potential, albeit infrequent, complications of surgery, will allow for individualized decision making by each woman and her health care provider," the investigators noted.
Dr. Labrie and his colleagues performed this study because standard practice is to recommend physiotherapy as first-line treatment, and to proceed to surgery only if that fails. Yet outcomes from midurethral-sling surgery and physiotherapy have never been directly compared.
Their study involved women aged 35-80 years whose stress urinary incontinence was classified as moderate or severe according to the Sandvik index. These subjects were randomly assigned to receive either initial surgery (230 women) or initial physiotherapy (230 women) at four university medical centers and 19 general hospitals over a 2-year period.
Both retropubic and transobturator midurethral-sling surgical approaches were allowed. Physiotherapy included an average of nine sessions delivered over 18 weeks, and could include biofeedback assistance or functional electrostimulation therapy.
The women were allowed to cross over to the other group if they were not satisfied with their assigned treatment, as "is consistent with usual clinical practice." The data were analyzed on an intention-to-treat basis. However, because approximately half of the physiotherapy group crossed over to surgery after a mean of 31 weeks, the investigators also performed a post hoc per-protocol analysis.
The primary outcome was subjective improvement in symptoms of stress urinary incontinence at 12 months, as measured by the Patient Global Impression of Improvement (PGI-I) scale. In the intention-to-treat analysis, the rate of this outcome was 90.8% with immediate surgery, significantly higher than the 64.4% rate with immediate physiotherapy, Dr. Labrie and his associates reported (New Engl. J. Med. 2013;369:1124-33 [doi: 10.1056/NEJMoa1210627]).
The pattern was the same when outcomes were assessed objectively using a cough stress test.
Both study groups showed improvement over time in urogenital symptoms as measured by the Urogenital Distress Inventory (UDI) and in disease-specific quality of life as measured by the Incontinence Impact Questionnaire (IIQ). The improvements were significantly greater in the immediate-surgery group for incontinence and overactive bladder, "but with only moderate effect sizes," the authors said.
Similarly, improvements were significantly greater in the immediate-surgery group for subscores regarding patients’ mobility and embarrassment, "but again with only moderate effect sizes," the researchers said.
In the post hoc per-protocol analysis, they compared the 103 women who only had physiotherapy, the 99 who had physiotherapy but crossed over to surgery, and the 215 who only had surgery. At 1 year, improvement in the physiotherapy-only group was lower by approximately 62% than in the crossover group and by 59% in the surgery-only group.
Adverse events, which occurred only in women who underwent surgery, included 6 cases of bladder perforation, 10 cases of vaginal epithelial perforation, 6 reoperations for tape exposure, 1 reoperation to loosen a too-tight synthetic sling, 20 hematomas, 18 cases of new-onset urge urinary incontinence, and 3 cases of excessive blood loss.
This study may have been limited by selection bias, because "women with a preference for surgery may have been more likely to participate in the study, because they otherwise would have received initial physiotherapy according to Dutch guidelines," Dr. Labrie and his associates said.
The study was supported by the Netherlands Organization for Health Research and Development (ZonMW) and was performed "without the support or involvement of manufacturers of midurethral slings." Several coauthors reported financial ties to Ethicon, American Medical Systems, and AMS. The remainder of the authors reported no relevant financial conflicts of interest.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major finding: A total of 90.8% of women in the immediate-surgery group reported significant subjective improvement in stress urinary incontinence after 1 year, compared with only 64.4% of women in the immediate-physiotherapy group.
Data source: A national, multicenter, randomized clinical trial involving 460 women with moderate to severe stress urinary incontinence who underwent immediate midurethral-sling surgery or immediate physiotherapy and were followed for 1 year.
Disclosures: The study was supported by the Netherlands Organization for Health Research and Development (ZonMW), and was performed "without the support or involvement of manufacturers of midurethral slings." Several coauthors reported financial ties to Ethicon, American Medical Systems, and AMS. The remainder of the authors reported no relevant financial conflicts of interest.
Adolescents at risk for substance misuse fit three subgroups
Adolescents appear to fall into three distinct subgroups at high risk of misusing drugs and other substances, based on a variety of their previous behaviors, a report published in Addictive Behaviors shows.
If future research confirms this finding, it points the way to tailoring prevention and intervention programs to these three target groups, said James A. Cranford, Ph.D., of the Addiction Research Center, University of Michigan, Ann Arbor, and his associates.
The investigators performed a cross-sectional Web-based survey of adolescents attending five middle schools and high schools in southeastern Michigan to assess whether certain substance-use behaviors could be used to classify them into risk groups. The 2,744 study subjects had a mean age of 14.8 years, and were equally divided between boys and girls. About 64% were white, 31% were black, 4% were Asian, and 2% were Hispanic or other ethnicities (Addict. Behav. 2013;38:2768-71).
These participants first answered questions to classify them into four categories of substance use based on their self-reported behavior during the preceding year: nonuse/low use of prescription agents; nonmedical use of prescription medications such as sleep, antianxiety, stimulant, or pain medications; excessive use of prescription medications such as the aforementioned medicines and antidepressants; or the use of illicit substances such as alcohol, marijuana, tobacco, and others.
In addition, the respondents’ substance use and their parents’ monitoring of it were assessed using several items from the Monitoring the Future instrument, internalizing and externalizing tendencies were assessed using the Youth Self-Report, and parental substance use was measured using the Children of Alcoholics Screening Test.
Nonusers/low users were the largest subgroup of adolescents (76%) and were judged to be at very low risk of substance misuse in the near future
The other three groups were considered to be at high risk of substance misuse in the near future. They included the 12% of study subjects who used tobacco, alcohol, and marijuana at least once during the preceding year; the 8% who reported alcohol, nonmedical prescription drug, and excessive prescription drug use during the preceding year; and the 4% who reported using all substances at least once during the preceding year, Dr. Cranford and his associates said.
Two parental factors – a lack of parental monitoring of the adolescents’ substance use and the parents’ own substance use – predicted membership in all three high-risk groups. This suggests that parent-focused prevention and intervention programs might be beneficial, the researchers said.
Parental factors exerted a more heightened effect on girls than on boys, which further suggests that parent-focused interventions might be particularly helpful to adolescent girls.
Adolescents who had externalizing problems were more likely than were those without such problems to misuse substances, while those who had internalizing problems were the least likely to misuse substances. Similar findings have been reported in previous studies, the investigators said.
Girls were more likely than boys were to report the nonmedical use of prescription drugs and the excessive use of prescription drugs, a trend that also has been reported in previous studies. This finding indicates that parents and teachers should be especially vigilant about possible misuse of prescription drugs among adolescent girls.
Moreover, these risks were particularly high in nonwhite girls, suggesting "a possible unique intervention target for at-risk nonwhite females," they added.
The investigators cited the completion of the survey in school and the possibility that this fact might have led to underestimates of problem behavior as a possible limitation of the study. Furthermore, the results might not be generalizable in the absence of a nationally representative study.
However, the study still "provides important evidence for the existence of distinct subtypes of adolescent substance use based on 12-months use of alcohol, tobacco, marijuana, and illicit drugs, along with excessive medical use and nonmedical use of prescription drugs," they wrote.
This study was supported by the National Institute on Drug Abuse. No financial conflicts of interest were reported.
Adolescents appear to fall into three distinct subgroups at high risk of misusing drugs and other substances, based on a variety of their previous behaviors, a report published in Addictive Behaviors shows.
If future research confirms this finding, it points the way to tailoring prevention and intervention programs to these three target groups, said James A. Cranford, Ph.D., of the Addiction Research Center, University of Michigan, Ann Arbor, and his associates.
The investigators performed a cross-sectional Web-based survey of adolescents attending five middle schools and high schools in southeastern Michigan to assess whether certain substance-use behaviors could be used to classify them into risk groups. The 2,744 study subjects had a mean age of 14.8 years, and were equally divided between boys and girls. About 64% were white, 31% were black, 4% were Asian, and 2% were Hispanic or other ethnicities (Addict. Behav. 2013;38:2768-71).
These participants first answered questions to classify them into four categories of substance use based on their self-reported behavior during the preceding year: nonuse/low use of prescription agents; nonmedical use of prescription medications such as sleep, antianxiety, stimulant, or pain medications; excessive use of prescription medications such as the aforementioned medicines and antidepressants; or the use of illicit substances such as alcohol, marijuana, tobacco, and others.
In addition, the respondents’ substance use and their parents’ monitoring of it were assessed using several items from the Monitoring the Future instrument, internalizing and externalizing tendencies were assessed using the Youth Self-Report, and parental substance use was measured using the Children of Alcoholics Screening Test.
Nonusers/low users were the largest subgroup of adolescents (76%) and were judged to be at very low risk of substance misuse in the near future
The other three groups were considered to be at high risk of substance misuse in the near future. They included the 12% of study subjects who used tobacco, alcohol, and marijuana at least once during the preceding year; the 8% who reported alcohol, nonmedical prescription drug, and excessive prescription drug use during the preceding year; and the 4% who reported using all substances at least once during the preceding year, Dr. Cranford and his associates said.
Two parental factors – a lack of parental monitoring of the adolescents’ substance use and the parents’ own substance use – predicted membership in all three high-risk groups. This suggests that parent-focused prevention and intervention programs might be beneficial, the researchers said.
Parental factors exerted a more heightened effect on girls than on boys, which further suggests that parent-focused interventions might be particularly helpful to adolescent girls.
Adolescents who had externalizing problems were more likely than were those without such problems to misuse substances, while those who had internalizing problems were the least likely to misuse substances. Similar findings have been reported in previous studies, the investigators said.
Girls were more likely than boys were to report the nonmedical use of prescription drugs and the excessive use of prescription drugs, a trend that also has been reported in previous studies. This finding indicates that parents and teachers should be especially vigilant about possible misuse of prescription drugs among adolescent girls.
Moreover, these risks were particularly high in nonwhite girls, suggesting "a possible unique intervention target for at-risk nonwhite females," they added.
The investigators cited the completion of the survey in school and the possibility that this fact might have led to underestimates of problem behavior as a possible limitation of the study. Furthermore, the results might not be generalizable in the absence of a nationally representative study.
However, the study still "provides important evidence for the existence of distinct subtypes of adolescent substance use based on 12-months use of alcohol, tobacco, marijuana, and illicit drugs, along with excessive medical use and nonmedical use of prescription drugs," they wrote.
This study was supported by the National Institute on Drug Abuse. No financial conflicts of interest were reported.
Adolescents appear to fall into three distinct subgroups at high risk of misusing drugs and other substances, based on a variety of their previous behaviors, a report published in Addictive Behaviors shows.
If future research confirms this finding, it points the way to tailoring prevention and intervention programs to these three target groups, said James A. Cranford, Ph.D., of the Addiction Research Center, University of Michigan, Ann Arbor, and his associates.
The investigators performed a cross-sectional Web-based survey of adolescents attending five middle schools and high schools in southeastern Michigan to assess whether certain substance-use behaviors could be used to classify them into risk groups. The 2,744 study subjects had a mean age of 14.8 years, and were equally divided between boys and girls. About 64% were white, 31% were black, 4% were Asian, and 2% were Hispanic or other ethnicities (Addict. Behav. 2013;38:2768-71).
These participants first answered questions to classify them into four categories of substance use based on their self-reported behavior during the preceding year: nonuse/low use of prescription agents; nonmedical use of prescription medications such as sleep, antianxiety, stimulant, or pain medications; excessive use of prescription medications such as the aforementioned medicines and antidepressants; or the use of illicit substances such as alcohol, marijuana, tobacco, and others.
In addition, the respondents’ substance use and their parents’ monitoring of it were assessed using several items from the Monitoring the Future instrument, internalizing and externalizing tendencies were assessed using the Youth Self-Report, and parental substance use was measured using the Children of Alcoholics Screening Test.
Nonusers/low users were the largest subgroup of adolescents (76%) and were judged to be at very low risk of substance misuse in the near future
The other three groups were considered to be at high risk of substance misuse in the near future. They included the 12% of study subjects who used tobacco, alcohol, and marijuana at least once during the preceding year; the 8% who reported alcohol, nonmedical prescription drug, and excessive prescription drug use during the preceding year; and the 4% who reported using all substances at least once during the preceding year, Dr. Cranford and his associates said.
Two parental factors – a lack of parental monitoring of the adolescents’ substance use and the parents’ own substance use – predicted membership in all three high-risk groups. This suggests that parent-focused prevention and intervention programs might be beneficial, the researchers said.
Parental factors exerted a more heightened effect on girls than on boys, which further suggests that parent-focused interventions might be particularly helpful to adolescent girls.
Adolescents who had externalizing problems were more likely than were those without such problems to misuse substances, while those who had internalizing problems were the least likely to misuse substances. Similar findings have been reported in previous studies, the investigators said.
Girls were more likely than boys were to report the nonmedical use of prescription drugs and the excessive use of prescription drugs, a trend that also has been reported in previous studies. This finding indicates that parents and teachers should be especially vigilant about possible misuse of prescription drugs among adolescent girls.
Moreover, these risks were particularly high in nonwhite girls, suggesting "a possible unique intervention target for at-risk nonwhite females," they added.
The investigators cited the completion of the survey in school and the possibility that this fact might have led to underestimates of problem behavior as a possible limitation of the study. Furthermore, the results might not be generalizable in the absence of a nationally representative study.
However, the study still "provides important evidence for the existence of distinct subtypes of adolescent substance use based on 12-months use of alcohol, tobacco, marijuana, and illicit drugs, along with excessive medical use and nonmedical use of prescription drugs," they wrote.
This study was supported by the National Institute on Drug Abuse. No financial conflicts of interest were reported.
FROM ADDICTIVE BEHAVIORS
Major finding: The three distinct subgroups of adolescents at highest risk for misusing substances are the 12% of subjects who used tobacco, alcohol, and marijuana at least once during the preceding year; the 8% who reported alcohol, nonmedical prescription drug, and excessive prescription drug use during the preceding year; and the 4% who reported using all substances at least once during the preceding year.
Data source: A cross-sectional Web-based survey of 2,744 middle- and high-school students in southeastern Michigan regarding their substance use behaviors during the preceding year.
Disclosures: This study was supported by the National Institute on Drug Abuse. No financial conflicts of interest were reported.
Stats show MRSA declining, especially in hospitals
The estimated total of invasive MRSA infections across the United States fell 31% between 2005 and 2011, according to a report published online Sept. 16 in JAMA Internal Medicine.
And for the first time, the estimated number of hospital-onset invasive MRSA infections was lower than that of community-associated infections, said Dr. Raymund Dantes of the Epidemic Intelligence Service of the Centers for Disease Control and Prevention, Atlanta.
The greatest burden of disease continues to fall upon patients in the community who have recent or ongoing exposure to health care services. That includes those recently discharged from acute medical care, long-term–care residents, and patients who require repeated medical visits, such as for diabetes care or dialysis, according to Dr. Dantes and his colleagues.
Those findings, together with other results from their analysis of data in the CDC’s emerging infections surveillance system, indicate that "the U.S. is on track to meet the Department of Health and Human Services 2013 target of reducing health care–associated MRSA invasive infections by 50%," they noted (JAMA Intern. Med. 2013 Sept. 16 [doi:10.1001/jamainternmed.2013.10423]).
To better understand the national burden of invasive MRSA infections, Dr. Dantes and his colleagues analyzed data from nine states participating in the surveillance program: California, Colorado, Connecticut, Georgia, Maryland, Minnesota, New York, Oregon, and Tennessee. They focused on 2011, the most recent year for which complete data are available, and compared the information with that gathered in 2005.
Those nine sites, which represented 16,489,254 people in 2005 and 19,393,677 people in 2011, reported 4,872 cases of invasive MRSA among 4,445 patients in 2011. A total of 18% were classified as hospital-onset infections, 60% as "health-care–associated community onset" infections, and 20% as community-associated infections.
Extrapolating those results to the entire U.S. population, the investigators estimated that 80,461 invasive MRSA infections occurred nationally in 2011, of which 14,156 were hospital-onset, 48,353 were health-care–associated community onset, and 16,560 were community-associated.
"Compared with 6 years earlier, the estimated national rate of invasive MRSA has decreased by 31.2%," Dr. Dantes and his associates said. "Although this rate decrease was most precipitous among hospital-onset infections, at 54.2%, rate decreases were evident among other categories as well: health-care–associated by 27.7%, and community-associated by 5.0%," they wrote.
The 54% decline in hospital-onset cases was particularly encouraging. The exact reason for that reduction is not yet known, but it is likely that implementation of infection prevention measures contributed, especially those targeting intravascular catheter-related infections and health care transmission of multidrug-resistant organisms, they added.
"It is notable that the incidence of community-associated invasive MRSA infections, although relatively stable, has not increased over this time, despite increases in hospitalizations related to MRSA skin and soft-tissue infections documented in discharge data," the investigators said. "Progress in reducing infections among this population is likely to be most challenging due to a lack of clearly effective strategies to control endemic MRSA transmission in the community setting.
Although there is guidance on preventing community-associated MRSA transmission in institutions such as athletic facilities, correctional facilities, and schools, guidance on prevention in other community settings isn’t as well established. Changes in community settings "may be related to transmission in households, prevention of invasive disease from improved early treatment of noninvasive infections, or the natural evolution of this pathogen," they noted.
To substantially reduce the overall burden of invasive MRSA infections, significant progress must be made to prevent postdischarge and dialysis-related cases, the researchers added. In 2011, most cases of health care–associated community-onset invasive MRSA occurred among dialysis patients and patients who had been hospitalized recently.
"Invasive devices that remain placed during the postdischarge period, progression from colonization to clinical infection, and breakdowns in host defense and skin integrity during hospitalization may account for this increased risk," Dr. Dantes and his associates said.
An estimated 11,285 patients with invasive MRSA infections died of all causes during hospitalization in 2011, they added.
The Emerging Infections Program and the National Center for Emerging Zoonotic Infectious Diseases at the Centers for Disease Control and Prevention supported the study. No financial conflicts of interest were reported.
The estimated total of invasive MRSA infections across the United States fell 31% between 2005 and 2011, according to a report published online Sept. 16 in JAMA Internal Medicine.
And for the first time, the estimated number of hospital-onset invasive MRSA infections was lower than that of community-associated infections, said Dr. Raymund Dantes of the Epidemic Intelligence Service of the Centers for Disease Control and Prevention, Atlanta.
The greatest burden of disease continues to fall upon patients in the community who have recent or ongoing exposure to health care services. That includes those recently discharged from acute medical care, long-term–care residents, and patients who require repeated medical visits, such as for diabetes care or dialysis, according to Dr. Dantes and his colleagues.
Those findings, together with other results from their analysis of data in the CDC’s emerging infections surveillance system, indicate that "the U.S. is on track to meet the Department of Health and Human Services 2013 target of reducing health care–associated MRSA invasive infections by 50%," they noted (JAMA Intern. Med. 2013 Sept. 16 [doi:10.1001/jamainternmed.2013.10423]).
To better understand the national burden of invasive MRSA infections, Dr. Dantes and his colleagues analyzed data from nine states participating in the surveillance program: California, Colorado, Connecticut, Georgia, Maryland, Minnesota, New York, Oregon, and Tennessee. They focused on 2011, the most recent year for which complete data are available, and compared the information with that gathered in 2005.
Those nine sites, which represented 16,489,254 people in 2005 and 19,393,677 people in 2011, reported 4,872 cases of invasive MRSA among 4,445 patients in 2011. A total of 18% were classified as hospital-onset infections, 60% as "health-care–associated community onset" infections, and 20% as community-associated infections.
Extrapolating those results to the entire U.S. population, the investigators estimated that 80,461 invasive MRSA infections occurred nationally in 2011, of which 14,156 were hospital-onset, 48,353 were health-care–associated community onset, and 16,560 were community-associated.
"Compared with 6 years earlier, the estimated national rate of invasive MRSA has decreased by 31.2%," Dr. Dantes and his associates said. "Although this rate decrease was most precipitous among hospital-onset infections, at 54.2%, rate decreases were evident among other categories as well: health-care–associated by 27.7%, and community-associated by 5.0%," they wrote.
The 54% decline in hospital-onset cases was particularly encouraging. The exact reason for that reduction is not yet known, but it is likely that implementation of infection prevention measures contributed, especially those targeting intravascular catheter-related infections and health care transmission of multidrug-resistant organisms, they added.
"It is notable that the incidence of community-associated invasive MRSA infections, although relatively stable, has not increased over this time, despite increases in hospitalizations related to MRSA skin and soft-tissue infections documented in discharge data," the investigators said. "Progress in reducing infections among this population is likely to be most challenging due to a lack of clearly effective strategies to control endemic MRSA transmission in the community setting.
Although there is guidance on preventing community-associated MRSA transmission in institutions such as athletic facilities, correctional facilities, and schools, guidance on prevention in other community settings isn’t as well established. Changes in community settings "may be related to transmission in households, prevention of invasive disease from improved early treatment of noninvasive infections, or the natural evolution of this pathogen," they noted.
To substantially reduce the overall burden of invasive MRSA infections, significant progress must be made to prevent postdischarge and dialysis-related cases, the researchers added. In 2011, most cases of health care–associated community-onset invasive MRSA occurred among dialysis patients and patients who had been hospitalized recently.
"Invasive devices that remain placed during the postdischarge period, progression from colonization to clinical infection, and breakdowns in host defense and skin integrity during hospitalization may account for this increased risk," Dr. Dantes and his associates said.
An estimated 11,285 patients with invasive MRSA infections died of all causes during hospitalization in 2011, they added.
The Emerging Infections Program and the National Center for Emerging Zoonotic Infectious Diseases at the Centers for Disease Control and Prevention supported the study. No financial conflicts of interest were reported.
The estimated total of invasive MRSA infections across the United States fell 31% between 2005 and 2011, according to a report published online Sept. 16 in JAMA Internal Medicine.
And for the first time, the estimated number of hospital-onset invasive MRSA infections was lower than that of community-associated infections, said Dr. Raymund Dantes of the Epidemic Intelligence Service of the Centers for Disease Control and Prevention, Atlanta.
The greatest burden of disease continues to fall upon patients in the community who have recent or ongoing exposure to health care services. That includes those recently discharged from acute medical care, long-term–care residents, and patients who require repeated medical visits, such as for diabetes care or dialysis, according to Dr. Dantes and his colleagues.
Those findings, together with other results from their analysis of data in the CDC’s emerging infections surveillance system, indicate that "the U.S. is on track to meet the Department of Health and Human Services 2013 target of reducing health care–associated MRSA invasive infections by 50%," they noted (JAMA Intern. Med. 2013 Sept. 16 [doi:10.1001/jamainternmed.2013.10423]).
To better understand the national burden of invasive MRSA infections, Dr. Dantes and his colleagues analyzed data from nine states participating in the surveillance program: California, Colorado, Connecticut, Georgia, Maryland, Minnesota, New York, Oregon, and Tennessee. They focused on 2011, the most recent year for which complete data are available, and compared the information with that gathered in 2005.
Those nine sites, which represented 16,489,254 people in 2005 and 19,393,677 people in 2011, reported 4,872 cases of invasive MRSA among 4,445 patients in 2011. A total of 18% were classified as hospital-onset infections, 60% as "health-care–associated community onset" infections, and 20% as community-associated infections.
Extrapolating those results to the entire U.S. population, the investigators estimated that 80,461 invasive MRSA infections occurred nationally in 2011, of which 14,156 were hospital-onset, 48,353 were health-care–associated community onset, and 16,560 were community-associated.
"Compared with 6 years earlier, the estimated national rate of invasive MRSA has decreased by 31.2%," Dr. Dantes and his associates said. "Although this rate decrease was most precipitous among hospital-onset infections, at 54.2%, rate decreases were evident among other categories as well: health-care–associated by 27.7%, and community-associated by 5.0%," they wrote.
The 54% decline in hospital-onset cases was particularly encouraging. The exact reason for that reduction is not yet known, but it is likely that implementation of infection prevention measures contributed, especially those targeting intravascular catheter-related infections and health care transmission of multidrug-resistant organisms, they added.
"It is notable that the incidence of community-associated invasive MRSA infections, although relatively stable, has not increased over this time, despite increases in hospitalizations related to MRSA skin and soft-tissue infections documented in discharge data," the investigators said. "Progress in reducing infections among this population is likely to be most challenging due to a lack of clearly effective strategies to control endemic MRSA transmission in the community setting.
Although there is guidance on preventing community-associated MRSA transmission in institutions such as athletic facilities, correctional facilities, and schools, guidance on prevention in other community settings isn’t as well established. Changes in community settings "may be related to transmission in households, prevention of invasive disease from improved early treatment of noninvasive infections, or the natural evolution of this pathogen," they noted.
To substantially reduce the overall burden of invasive MRSA infections, significant progress must be made to prevent postdischarge and dialysis-related cases, the researchers added. In 2011, most cases of health care–associated community-onset invasive MRSA occurred among dialysis patients and patients who had been hospitalized recently.
"Invasive devices that remain placed during the postdischarge period, progression from colonization to clinical infection, and breakdowns in host defense and skin integrity during hospitalization may account for this increased risk," Dr. Dantes and his associates said.
An estimated 11,285 patients with invasive MRSA infections died of all causes during hospitalization in 2011, they added.
The Emerging Infections Program and the National Center for Emerging Zoonotic Infectious Diseases at the Centers for Disease Control and Prevention supported the study. No financial conflicts of interest were reported.
FROM JAMA INTERNAL MEDICINE
Stats show MRSA declining, especially in hospitals
The estimated total of invasive MRSA infections across the United States fell 31% between 2005 and 2011, according to a report published online Sept. 16 in JAMA Internal Medicine.
And for the first time, the estimated number of hospital-onset invasive MRSA infections was lower than that of community-associated infections, said Dr. Raymund Dantes of the Epidemic Intelligence Service of the Centers for Disease Control and Prevention, Atlanta.
The greatest burden of disease continues to fall upon patients in the community who have recent or ongoing exposure to health care services. That includes those recently discharged from acute medical care, long-term–care residents, and patients who require repeated medical visits, such as for diabetes care or dialysis, according to Dr. Dantes and his colleagues.
Those findings, together with other results from their analysis of data in the CDC’s emerging infections surveillance system, indicate that "the U.S. is on track to meet the Department of Health and Human Services 2013 target of reducing health care–associated MRSA invasive infections by 50%," they noted (JAMA Intern. Med. 2013 Sept. 16 [doi:10.1001/jamainternmed.2013.10423]).
To better understand the national burden of invasive MRSA infections, Dr. Dantes and his colleagues analyzed data from nine states participating in the surveillance program: California, Colorado, Connecticut, Georgia, Maryland, Minnesota, New York, Oregon, and Tennessee. They focused on 2011, the most recent year for which complete data are available, and compared the information with that gathered in 2005.
Those nine sites, which represented 16,489,254 people in 2005 and 19,393,677 people in 2011, reported 4,872 cases of invasive MRSA among 4,445 patients in 2011. A total of 18% were classified as hospital-onset infections, 60% as "health-care–associated community onset" infections, and 20% as community-associated infections.
Extrapolating those results to the entire U.S. population, the investigators estimated that 80,461 invasive MRSA infections occurred nationally in 2011, of which 14,156 were hospital-onset, 48,353 were health-care–associated community onset, and 16,560 were community-associated.
"Compared with 6 years earlier, the estimated national rate of invasive MRSA has decreased by 31.2%," Dr. Dantes and his associates said. "Although this rate decrease was most precipitous among hospital-onset infections, at 54.2%, rate decreases were evident among other categories as well: health-care–associated by 27.7%, and community-associated by 5.0%," they wrote.
The 54% decline in hospital-onset cases was particularly encouraging. The exact reason for that reduction is not yet known, but it is likely that implementation of infection prevention measures contributed, especially those targeting intravascular catheter-related infections and health care transmission of multidrug-resistant organisms, they added.
"It is notable that the incidence of community-associated invasive MRSA infections, although relatively stable, has not increased over this time, despite increases in hospitalizations related to MRSA skin and soft-tissue infections documented in discharge data," the investigators said. "Progress in reducing infections among this population is likely to be most challenging due to a lack of clearly effective strategies to control endemic MRSA transmission in the community setting.
Although there is guidance on preventing community-associated MRSA transmission in institutions such as athletic facilities, correctional facilities, and schools, guidance on prevention in other community settings isn’t as well established. Changes in community settings "may be related to transmission in households, prevention of invasive disease from improved early treatment of noninvasive infections, or the natural evolution of this pathogen," they noted.
To substantially reduce the overall burden of invasive MRSA infections, significant progress must be made to prevent postdischarge and dialysis-related cases, the researchers added. In 2011, most cases of health care–associated community-onset invasive MRSA occurred among dialysis patients and patients who had been hospitalized recently.
"Invasive devices that remain placed during the postdischarge period, progression from colonization to clinical infection, and breakdowns in host defense and skin integrity during hospitalization may account for this increased risk," Dr. Dantes and his associates said.
An estimated 11,285 patients with invasive MRSA infections died of all causes during hospitalization in 2011, they added.
The Emerging Infections Program and the National Center for Emerging Zoonotic Infectious Diseases at the Centers for Disease Control and Prevention supported the study. No financial conflicts of interest were reported.
The estimated total of invasive MRSA infections across the United States fell 31% between 2005 and 2011, according to a report published online Sept. 16 in JAMA Internal Medicine.
And for the first time, the estimated number of hospital-onset invasive MRSA infections was lower than that of community-associated infections, said Dr. Raymund Dantes of the Epidemic Intelligence Service of the Centers for Disease Control and Prevention, Atlanta.
The greatest burden of disease continues to fall upon patients in the community who have recent or ongoing exposure to health care services. That includes those recently discharged from acute medical care, long-term–care residents, and patients who require repeated medical visits, such as for diabetes care or dialysis, according to Dr. Dantes and his colleagues.
Those findings, together with other results from their analysis of data in the CDC’s emerging infections surveillance system, indicate that "the U.S. is on track to meet the Department of Health and Human Services 2013 target of reducing health care–associated MRSA invasive infections by 50%," they noted (JAMA Intern. Med. 2013 Sept. 16 [doi:10.1001/jamainternmed.2013.10423]).
To better understand the national burden of invasive MRSA infections, Dr. Dantes and his colleagues analyzed data from nine states participating in the surveillance program: California, Colorado, Connecticut, Georgia, Maryland, Minnesota, New York, Oregon, and Tennessee. They focused on 2011, the most recent year for which complete data are available, and compared the information with that gathered in 2005.
Those nine sites, which represented 16,489,254 people in 2005 and 19,393,677 people in 2011, reported 4,872 cases of invasive MRSA among 4,445 patients in 2011. A total of 18% were classified as hospital-onset infections, 60% as "health-care–associated community onset" infections, and 20% as community-associated infections.
Extrapolating those results to the entire U.S. population, the investigators estimated that 80,461 invasive MRSA infections occurred nationally in 2011, of which 14,156 were hospital-onset, 48,353 were health-care–associated community onset, and 16,560 were community-associated.
"Compared with 6 years earlier, the estimated national rate of invasive MRSA has decreased by 31.2%," Dr. Dantes and his associates said. "Although this rate decrease was most precipitous among hospital-onset infections, at 54.2%, rate decreases were evident among other categories as well: health-care–associated by 27.7%, and community-associated by 5.0%," they wrote.
The 54% decline in hospital-onset cases was particularly encouraging. The exact reason for that reduction is not yet known, but it is likely that implementation of infection prevention measures contributed, especially those targeting intravascular catheter-related infections and health care transmission of multidrug-resistant organisms, they added.
"It is notable that the incidence of community-associated invasive MRSA infections, although relatively stable, has not increased over this time, despite increases in hospitalizations related to MRSA skin and soft-tissue infections documented in discharge data," the investigators said. "Progress in reducing infections among this population is likely to be most challenging due to a lack of clearly effective strategies to control endemic MRSA transmission in the community setting.
Although there is guidance on preventing community-associated MRSA transmission in institutions such as athletic facilities, correctional facilities, and schools, guidance on prevention in other community settings isn’t as well established. Changes in community settings "may be related to transmission in households, prevention of invasive disease from improved early treatment of noninvasive infections, or the natural evolution of this pathogen," they noted.
To substantially reduce the overall burden of invasive MRSA infections, significant progress must be made to prevent postdischarge and dialysis-related cases, the researchers added. In 2011, most cases of health care–associated community-onset invasive MRSA occurred among dialysis patients and patients who had been hospitalized recently.
"Invasive devices that remain placed during the postdischarge period, progression from colonization to clinical infection, and breakdowns in host defense and skin integrity during hospitalization may account for this increased risk," Dr. Dantes and his associates said.
An estimated 11,285 patients with invasive MRSA infections died of all causes during hospitalization in 2011, they added.
The Emerging Infections Program and the National Center for Emerging Zoonotic Infectious Diseases at the Centers for Disease Control and Prevention supported the study. No financial conflicts of interest were reported.
The estimated total of invasive MRSA infections across the United States fell 31% between 2005 and 2011, according to a report published online Sept. 16 in JAMA Internal Medicine.
And for the first time, the estimated number of hospital-onset invasive MRSA infections was lower than that of community-associated infections, said Dr. Raymund Dantes of the Epidemic Intelligence Service of the Centers for Disease Control and Prevention, Atlanta.
The greatest burden of disease continues to fall upon patients in the community who have recent or ongoing exposure to health care services. That includes those recently discharged from acute medical care, long-term–care residents, and patients who require repeated medical visits, such as for diabetes care or dialysis, according to Dr. Dantes and his colleagues.
Those findings, together with other results from their analysis of data in the CDC’s emerging infections surveillance system, indicate that "the U.S. is on track to meet the Department of Health and Human Services 2013 target of reducing health care–associated MRSA invasive infections by 50%," they noted (JAMA Intern. Med. 2013 Sept. 16 [doi:10.1001/jamainternmed.2013.10423]).
To better understand the national burden of invasive MRSA infections, Dr. Dantes and his colleagues analyzed data from nine states participating in the surveillance program: California, Colorado, Connecticut, Georgia, Maryland, Minnesota, New York, Oregon, and Tennessee. They focused on 2011, the most recent year for which complete data are available, and compared the information with that gathered in 2005.
Those nine sites, which represented 16,489,254 people in 2005 and 19,393,677 people in 2011, reported 4,872 cases of invasive MRSA among 4,445 patients in 2011. A total of 18% were classified as hospital-onset infections, 60% as "health-care–associated community onset" infections, and 20% as community-associated infections.
Extrapolating those results to the entire U.S. population, the investigators estimated that 80,461 invasive MRSA infections occurred nationally in 2011, of which 14,156 were hospital-onset, 48,353 were health-care–associated community onset, and 16,560 were community-associated.
"Compared with 6 years earlier, the estimated national rate of invasive MRSA has decreased by 31.2%," Dr. Dantes and his associates said. "Although this rate decrease was most precipitous among hospital-onset infections, at 54.2%, rate decreases were evident among other categories as well: health-care–associated by 27.7%, and community-associated by 5.0%," they wrote.
The 54% decline in hospital-onset cases was particularly encouraging. The exact reason for that reduction is not yet known, but it is likely that implementation of infection prevention measures contributed, especially those targeting intravascular catheter-related infections and health care transmission of multidrug-resistant organisms, they added.
"It is notable that the incidence of community-associated invasive MRSA infections, although relatively stable, has not increased over this time, despite increases in hospitalizations related to MRSA skin and soft-tissue infections documented in discharge data," the investigators said. "Progress in reducing infections among this population is likely to be most challenging due to a lack of clearly effective strategies to control endemic MRSA transmission in the community setting.
Although there is guidance on preventing community-associated MRSA transmission in institutions such as athletic facilities, correctional facilities, and schools, guidance on prevention in other community settings isn’t as well established. Changes in community settings "may be related to transmission in households, prevention of invasive disease from improved early treatment of noninvasive infections, or the natural evolution of this pathogen," they noted.
To substantially reduce the overall burden of invasive MRSA infections, significant progress must be made to prevent postdischarge and dialysis-related cases, the researchers added. In 2011, most cases of health care–associated community-onset invasive MRSA occurred among dialysis patients and patients who had been hospitalized recently.
"Invasive devices that remain placed during the postdischarge period, progression from colonization to clinical infection, and breakdowns in host defense and skin integrity during hospitalization may account for this increased risk," Dr. Dantes and his associates said.
An estimated 11,285 patients with invasive MRSA infections died of all causes during hospitalization in 2011, they added.
The Emerging Infections Program and the National Center for Emerging Zoonotic Infectious Diseases at the Centers for Disease Control and Prevention supported the study. No financial conflicts of interest were reported.
FROM JAMA INTERNAL MEDICINE
Major Finding: The estimated national rate of invasive MRSA infections declined 31% since 2005, with hospital-onset cases dropping 54%, health care–associated cases decreasing 28%, and community-associated cases declining 5%.
Data Source: An analysis of data from a MRSA surveillance program covering more than 16 million residents of nine states in 2005 and more than 19 million residents in those states in 2011.
Disclosures: The Emerging Infections Program and the National Center for Emerging Zoonotic Infectious Diseases at the Centers for Disease Control and Prevention supported the study. No financial conflicts of interest were reported.
‘Catastrophizing’ linked to opioid misuse in chronic pain
For patients with chronic musculoskeletal pain, catastrophizing is associated with an increased risk for prescription opioid misuse, a study has shown.
This finding suggests that "complementary interventions designed to reduce patients’ levels of anxiety and catastrophizing might contribute to decreasing risks for prescription opioid misuse in patients with chronic pain," said Marc O. Martel, Ph.D., of the department of anesthesiology at Harvard Medical School and the pain management center at Brigham and Women’s Hospital, Boston, and his associates.
Patients who catastrophize tend to ruminate about pain, magnify the threat level of pain, and experience helplessness when in pain. Patients with psychiatric disorders are at a greater risk for misusing prescription opioids, Dr. Martel and his colleagues said. In an effort to identify a possible relationship between catastrophizing and risk for the misuse of prescription opioids, the investigators assessed 115 patients treated at their pain center for at least 6 months for spinal musculoskeletal pain with or without radicular symptoms.
These study subjects completed the Screener and Opioid Assessment for Patients With Pain–Revised (SOAPP-R), a self-report questionnaire designed to assess the risk for opioid misuse; the Brief Pain Inventory (BPI), a measure of pain severity and interference with physical and emotional functioning; the Pain Anxiety Symptoms Scale (PASS), a 20-item tool that measures pain-related anxiety; the Beck Depression Inventory (BDI); the Pain Catastrophizing Scale (PCS), a 13-item measure of the thoughts and feelings patients experience when in pain; and quantitative sensory testing (QST), a measure of somatosensory function and pain sensitivity that uses calibrated noxious stimuli to gauge patients’ pain response. The investigators used thermal pain thresholds as an index of pain sensitivity.
Using regression analysis, the investigators found correlations between pain measures (the BPI), pain sensitivity, negative affect (on the PASS and BDI), and catastrophizing. Also, they found a significant negative correlation between thermal pain thresholds and scores on the Pain Catastrophizing Scale (P less than .05). High levels of catastrophizing were associated with high scores on the SOAPP-R, which indicates greater risk for prescription opioid misuse.
Also associated with high scores on the SOAPP-R were a heightened sensitivity to pain, increased pain severity, increased pain-related anxiety, and depressive symptoms. However, the strong association between catastrophizing and high SOAPP-R scores persisted after the data were controlled for those four factors, which is "perhaps the most important finding of our study," Dr. Martel and his associates said (Drug Alcohol Depend. 2013;132:335-41).
It has been suggested that heightened sensitivity to pain, also known as a low pain threshold, could be caused by dysfunction of peripheral or central pain processing, or dysfunction of opioid-mediated endogenous pain inhibitory systems. Such dysfunction might raise the risk of opioid craving and thus of opioid misuse, the investigators said.
In addition, anxiety might alter patients’ beliefs about their medication needs, and thus prompt them to overuse opioids. Pain patients who have high levels of anxiety also might overuse opioids as a way to alleviate or eliminate their psychological distress, they noted.
Previous research has linked catastrophizing to low self-efficacy beliefs, poor pain coping skills, greater impulsivity, and increased sensation seeking. All of those factors in turn raise the risk for prescription opioid misuse, Dr. Martel and his colleagues said.
Their study findings indicate that interventions aimed at decreasing pain patients’ anxiety and catastrophizing also would likely reduce their risk for misusing prescription opioids, they said.
This study was supported by the National Institutes of Health. No financial conflicts of interest were reported.
For patients with chronic musculoskeletal pain, catastrophizing is associated with an increased risk for prescription opioid misuse, a study has shown.
This finding suggests that "complementary interventions designed to reduce patients’ levels of anxiety and catastrophizing might contribute to decreasing risks for prescription opioid misuse in patients with chronic pain," said Marc O. Martel, Ph.D., of the department of anesthesiology at Harvard Medical School and the pain management center at Brigham and Women’s Hospital, Boston, and his associates.
Patients who catastrophize tend to ruminate about pain, magnify the threat level of pain, and experience helplessness when in pain. Patients with psychiatric disorders are at a greater risk for misusing prescription opioids, Dr. Martel and his colleagues said. In an effort to identify a possible relationship between catastrophizing and risk for the misuse of prescription opioids, the investigators assessed 115 patients treated at their pain center for at least 6 months for spinal musculoskeletal pain with or without radicular symptoms.
These study subjects completed the Screener and Opioid Assessment for Patients With Pain–Revised (SOAPP-R), a self-report questionnaire designed to assess the risk for opioid misuse; the Brief Pain Inventory (BPI), a measure of pain severity and interference with physical and emotional functioning; the Pain Anxiety Symptoms Scale (PASS), a 20-item tool that measures pain-related anxiety; the Beck Depression Inventory (BDI); the Pain Catastrophizing Scale (PCS), a 13-item measure of the thoughts and feelings patients experience when in pain; and quantitative sensory testing (QST), a measure of somatosensory function and pain sensitivity that uses calibrated noxious stimuli to gauge patients’ pain response. The investigators used thermal pain thresholds as an index of pain sensitivity.
Using regression analysis, the investigators found correlations between pain measures (the BPI), pain sensitivity, negative affect (on the PASS and BDI), and catastrophizing. Also, they found a significant negative correlation between thermal pain thresholds and scores on the Pain Catastrophizing Scale (P less than .05). High levels of catastrophizing were associated with high scores on the SOAPP-R, which indicates greater risk for prescription opioid misuse.
Also associated with high scores on the SOAPP-R were a heightened sensitivity to pain, increased pain severity, increased pain-related anxiety, and depressive symptoms. However, the strong association between catastrophizing and high SOAPP-R scores persisted after the data were controlled for those four factors, which is "perhaps the most important finding of our study," Dr. Martel and his associates said (Drug Alcohol Depend. 2013;132:335-41).
It has been suggested that heightened sensitivity to pain, also known as a low pain threshold, could be caused by dysfunction of peripheral or central pain processing, or dysfunction of opioid-mediated endogenous pain inhibitory systems. Such dysfunction might raise the risk of opioid craving and thus of opioid misuse, the investigators said.
In addition, anxiety might alter patients’ beliefs about their medication needs, and thus prompt them to overuse opioids. Pain patients who have high levels of anxiety also might overuse opioids as a way to alleviate or eliminate their psychological distress, they noted.
Previous research has linked catastrophizing to low self-efficacy beliefs, poor pain coping skills, greater impulsivity, and increased sensation seeking. All of those factors in turn raise the risk for prescription opioid misuse, Dr. Martel and his colleagues said.
Their study findings indicate that interventions aimed at decreasing pain patients’ anxiety and catastrophizing also would likely reduce their risk for misusing prescription opioids, they said.
This study was supported by the National Institutes of Health. No financial conflicts of interest were reported.
For patients with chronic musculoskeletal pain, catastrophizing is associated with an increased risk for prescription opioid misuse, a study has shown.
This finding suggests that "complementary interventions designed to reduce patients’ levels of anxiety and catastrophizing might contribute to decreasing risks for prescription opioid misuse in patients with chronic pain," said Marc O. Martel, Ph.D., of the department of anesthesiology at Harvard Medical School and the pain management center at Brigham and Women’s Hospital, Boston, and his associates.
Patients who catastrophize tend to ruminate about pain, magnify the threat level of pain, and experience helplessness when in pain. Patients with psychiatric disorders are at a greater risk for misusing prescription opioids, Dr. Martel and his colleagues said. In an effort to identify a possible relationship between catastrophizing and risk for the misuse of prescription opioids, the investigators assessed 115 patients treated at their pain center for at least 6 months for spinal musculoskeletal pain with or without radicular symptoms.
These study subjects completed the Screener and Opioid Assessment for Patients With Pain–Revised (SOAPP-R), a self-report questionnaire designed to assess the risk for opioid misuse; the Brief Pain Inventory (BPI), a measure of pain severity and interference with physical and emotional functioning; the Pain Anxiety Symptoms Scale (PASS), a 20-item tool that measures pain-related anxiety; the Beck Depression Inventory (BDI); the Pain Catastrophizing Scale (PCS), a 13-item measure of the thoughts and feelings patients experience when in pain; and quantitative sensory testing (QST), a measure of somatosensory function and pain sensitivity that uses calibrated noxious stimuli to gauge patients’ pain response. The investigators used thermal pain thresholds as an index of pain sensitivity.
Using regression analysis, the investigators found correlations between pain measures (the BPI), pain sensitivity, negative affect (on the PASS and BDI), and catastrophizing. Also, they found a significant negative correlation between thermal pain thresholds and scores on the Pain Catastrophizing Scale (P less than .05). High levels of catastrophizing were associated with high scores on the SOAPP-R, which indicates greater risk for prescription opioid misuse.
Also associated with high scores on the SOAPP-R were a heightened sensitivity to pain, increased pain severity, increased pain-related anxiety, and depressive symptoms. However, the strong association between catastrophizing and high SOAPP-R scores persisted after the data were controlled for those four factors, which is "perhaps the most important finding of our study," Dr. Martel and his associates said (Drug Alcohol Depend. 2013;132:335-41).
It has been suggested that heightened sensitivity to pain, also known as a low pain threshold, could be caused by dysfunction of peripheral or central pain processing, or dysfunction of opioid-mediated endogenous pain inhibitory systems. Such dysfunction might raise the risk of opioid craving and thus of opioid misuse, the investigators said.
In addition, anxiety might alter patients’ beliefs about their medication needs, and thus prompt them to overuse opioids. Pain patients who have high levels of anxiety also might overuse opioids as a way to alleviate or eliminate their psychological distress, they noted.
Previous research has linked catastrophizing to low self-efficacy beliefs, poor pain coping skills, greater impulsivity, and increased sensation seeking. All of those factors in turn raise the risk for prescription opioid misuse, Dr. Martel and his colleagues said.
Their study findings indicate that interventions aimed at decreasing pain patients’ anxiety and catastrophizing also would likely reduce their risk for misusing prescription opioids, they said.
This study was supported by the National Institutes of Health. No financial conflicts of interest were reported.
FROM DRUG AND ALCOHOL DEPENDENCE
Major finding: A significant negative correlation was found between thermal pain thresholds and scores on the Pain Catastrophizing Scale (P less than .05). Catastrophizing is associated with a high risk of misusing prescription opioids, independently of a patient’s sensitivity to pain, the severity of pain, pain-related anxiety, and depressive symptoms.
Data source: A cross-sectional survey of 115 patients with chronic musculoskeletal pain, correlating their risk of misusing prescription opioids (as measured on the SOAPP-R) with their catastrophizing traits.
Disclosures: This study was supported by the National Institutes of Health. No financial conflicts of interest were reported.
Explanation for erectile dysfunction, sexual disinterest in men
Declines in testosterone regulate decreases in men's muscle mass and strength, declines in estrogen regulate increases in men’s fat mass and abdominal fat, and declines in both hormones regulate decreases in men’s libido and erectile function, according to a report published online Sept. 11 in the New England Journal of Medicine.
These are the key findings from a dose-ranging study designed to tease out the complex roles played by both testosterone and estrogen in so-called androgen deficiency. They indicate that a simple, straightforward decline in testosterone doesn’t account for the myriad changes in body composition, strength, and sexual factors experienced by men with "low T."
This in turn suggests that the current approach to assessing and managing the condition – a one-time measurement of serum testosterone only, an across-the-board designation of a "low" level, and simple replenishment with endogenous testosterone only – should be replaced by more rational, nuanced approaches, said Dr. Joel S. Finkelstein of the endocrine unit and his associates at Massachusetts General Hospital, Boston.
They examined a wide spectrum of testosterone levels, and the adverse effects of different levels, by temporarily suppressing the normal endogenous gonadal steroids of healthy men aged 20-50 years using subcutaneous goserelin. In one cohort, 198 men then were randomly assigned to receive placebo, 1.25 g, 2.5 g, 5 g, or 10 g of a topical testosterone gel daily for 16 weeks. In another cohort, 202 men were randomly assigned to receive these same doses of topical testosterone plus 1 mg daily of anastrozole to block the aromatization of testosterone to estrogen.
All the study subjects, who were blinded to their medication assignments, were assessed every 4 weeks for the duration of the study for gonadal steroid levels, physical function, health status, vitality, and sexual function. Dual-energy x-ray absorptiometry (DXA) was used to measure body fat and lean mass, and CT was used to measure the areas of subcutaneous fat, intra-abdominal fat, and thigh muscle. Thigh-muscle strength was assessed using leg presses.
"By administering a variety of testosterone doses, with and without concomitant aromatase inhibition, we found that changes in lean mass, thigh-muscle area, and leg-press strength were attributable to changes in testosterone levels, whereas changes in fat measures were primarily related to changes in estradiol levels. Both androgens and estrogens contributed to the maintenance of normal libido and erectile function," Dr. Finkelstein and his associates said (N. Engl. J. Med. 2013 Sept. 11 [doi:10.1056/NEJMoa1206168]).
As important, the level of testosterone needed to maintain lean mass, fat mass, strength, and sexual function was found to vary considerably among these study subjects.
Most men showed reduced lean mass, muscle area, and erectile function at a mean serum testosterone level of 200 ng/dL, so testosterone supplementation appears to be justified at this level. However, many men showed impairment in these outcomes at lower or higher testosterone levels. In addition, the testosterone levels at which body fat increased and sexual desire decreased varied widely.
"Thus, each person’s specific clinical scenario should be considered when interpreting the clinical significance of the circulating testosterone level," Dr. Finkelstein and his colleagues said.
Also important was the finding that deficiency of estrogen, not testosterone, "is largely responsible for some of the key consequences of male hypogonadism." This indicates that measuring men’s estradiol levels may help in assessing their risk for sexual dysfunction, bone loss, or fat accumulation, the researchers added.
This study was limited in that the duration was restricted to 16 weeks, so as to avoid inducing clinically significant changes in the healthy men who participated. "Because changes in body composition may progress over time, greater changes might have been seen at higher testosterone and estradiol levels if gonadal steroids had been suppressed over a longer period," the investigators noted.
This study was supported by the National Institutes of Health and Abbott Laboratories. Abbott also supplied the testosterone gel at no cost, and Astra Zeneca provided goserelin and anastrozole at no cost, but neither company played a role in study design, data analysis, data interpretation, or manuscript preparation.
The study by Dr. Finkelstein and his colleagues answers important questions but raises new questions as well, said Dr. David J. Handelsman.
The findings are unequivocal, and "this excellent study contributes to our expanding appreciation of the complex mechanisms of action of testosterone." However, longer studies are necessary to elucidate the hormone’s effects on important clinical end points such as bone density, fractures, prostate growth and diseases, metabolism, cardiovascular function, and cerebral function (including mood, behavior, and cognition), he said.
Dr. Handelsman is at the Australia and New Zealand Army Corps (ANZAC) Research Institute, Concord Hospital, University of Sydney. He reported having received research support from Organon, Schering, Ascend/Besins, Lilly, Pharmacia, Serono, and Lawley. These remarks were taken from his editorial accompanying Dr. Finkelstein’s report (N. Engl. J. Med. 2013 Sept. 11 [doi:10.1056/NEJMe1305307]).
The study by Dr. Finkelstein and his colleagues answers important questions but raises new questions as well, said Dr. David J. Handelsman.
The findings are unequivocal, and "this excellent study contributes to our expanding appreciation of the complex mechanisms of action of testosterone." However, longer studies are necessary to elucidate the hormone’s effects on important clinical end points such as bone density, fractures, prostate growth and diseases, metabolism, cardiovascular function, and cerebral function (including mood, behavior, and cognition), he said.
Dr. Handelsman is at the Australia and New Zealand Army Corps (ANZAC) Research Institute, Concord Hospital, University of Sydney. He reported having received research support from Organon, Schering, Ascend/Besins, Lilly, Pharmacia, Serono, and Lawley. These remarks were taken from his editorial accompanying Dr. Finkelstein’s report (N. Engl. J. Med. 2013 Sept. 11 [doi:10.1056/NEJMe1305307]).
The study by Dr. Finkelstein and his colleagues answers important questions but raises new questions as well, said Dr. David J. Handelsman.
The findings are unequivocal, and "this excellent study contributes to our expanding appreciation of the complex mechanisms of action of testosterone." However, longer studies are necessary to elucidate the hormone’s effects on important clinical end points such as bone density, fractures, prostate growth and diseases, metabolism, cardiovascular function, and cerebral function (including mood, behavior, and cognition), he said.
Dr. Handelsman is at the Australia and New Zealand Army Corps (ANZAC) Research Institute, Concord Hospital, University of Sydney. He reported having received research support from Organon, Schering, Ascend/Besins, Lilly, Pharmacia, Serono, and Lawley. These remarks were taken from his editorial accompanying Dr. Finkelstein’s report (N. Engl. J. Med. 2013 Sept. 11 [doi:10.1056/NEJMe1305307]).
Declines in testosterone regulate decreases in men's muscle mass and strength, declines in estrogen regulate increases in men’s fat mass and abdominal fat, and declines in both hormones regulate decreases in men’s libido and erectile function, according to a report published online Sept. 11 in the New England Journal of Medicine.
These are the key findings from a dose-ranging study designed to tease out the complex roles played by both testosterone and estrogen in so-called androgen deficiency. They indicate that a simple, straightforward decline in testosterone doesn’t account for the myriad changes in body composition, strength, and sexual factors experienced by men with "low T."
This in turn suggests that the current approach to assessing and managing the condition – a one-time measurement of serum testosterone only, an across-the-board designation of a "low" level, and simple replenishment with endogenous testosterone only – should be replaced by more rational, nuanced approaches, said Dr. Joel S. Finkelstein of the endocrine unit and his associates at Massachusetts General Hospital, Boston.
They examined a wide spectrum of testosterone levels, and the adverse effects of different levels, by temporarily suppressing the normal endogenous gonadal steroids of healthy men aged 20-50 years using subcutaneous goserelin. In one cohort, 198 men then were randomly assigned to receive placebo, 1.25 g, 2.5 g, 5 g, or 10 g of a topical testosterone gel daily for 16 weeks. In another cohort, 202 men were randomly assigned to receive these same doses of topical testosterone plus 1 mg daily of anastrozole to block the aromatization of testosterone to estrogen.
All the study subjects, who were blinded to their medication assignments, were assessed every 4 weeks for the duration of the study for gonadal steroid levels, physical function, health status, vitality, and sexual function. Dual-energy x-ray absorptiometry (DXA) was used to measure body fat and lean mass, and CT was used to measure the areas of subcutaneous fat, intra-abdominal fat, and thigh muscle. Thigh-muscle strength was assessed using leg presses.
"By administering a variety of testosterone doses, with and without concomitant aromatase inhibition, we found that changes in lean mass, thigh-muscle area, and leg-press strength were attributable to changes in testosterone levels, whereas changes in fat measures were primarily related to changes in estradiol levels. Both androgens and estrogens contributed to the maintenance of normal libido and erectile function," Dr. Finkelstein and his associates said (N. Engl. J. Med. 2013 Sept. 11 [doi:10.1056/NEJMoa1206168]).
As important, the level of testosterone needed to maintain lean mass, fat mass, strength, and sexual function was found to vary considerably among these study subjects.
Most men showed reduced lean mass, muscle area, and erectile function at a mean serum testosterone level of 200 ng/dL, so testosterone supplementation appears to be justified at this level. However, many men showed impairment in these outcomes at lower or higher testosterone levels. In addition, the testosterone levels at which body fat increased and sexual desire decreased varied widely.
"Thus, each person’s specific clinical scenario should be considered when interpreting the clinical significance of the circulating testosterone level," Dr. Finkelstein and his colleagues said.
Also important was the finding that deficiency of estrogen, not testosterone, "is largely responsible for some of the key consequences of male hypogonadism." This indicates that measuring men’s estradiol levels may help in assessing their risk for sexual dysfunction, bone loss, or fat accumulation, the researchers added.
This study was limited in that the duration was restricted to 16 weeks, so as to avoid inducing clinically significant changes in the healthy men who participated. "Because changes in body composition may progress over time, greater changes might have been seen at higher testosterone and estradiol levels if gonadal steroids had been suppressed over a longer period," the investigators noted.
This study was supported by the National Institutes of Health and Abbott Laboratories. Abbott also supplied the testosterone gel at no cost, and Astra Zeneca provided goserelin and anastrozole at no cost, but neither company played a role in study design, data analysis, data interpretation, or manuscript preparation.
Declines in testosterone regulate decreases in men's muscle mass and strength, declines in estrogen regulate increases in men’s fat mass and abdominal fat, and declines in both hormones regulate decreases in men’s libido and erectile function, according to a report published online Sept. 11 in the New England Journal of Medicine.
These are the key findings from a dose-ranging study designed to tease out the complex roles played by both testosterone and estrogen in so-called androgen deficiency. They indicate that a simple, straightforward decline in testosterone doesn’t account for the myriad changes in body composition, strength, and sexual factors experienced by men with "low T."
This in turn suggests that the current approach to assessing and managing the condition – a one-time measurement of serum testosterone only, an across-the-board designation of a "low" level, and simple replenishment with endogenous testosterone only – should be replaced by more rational, nuanced approaches, said Dr. Joel S. Finkelstein of the endocrine unit and his associates at Massachusetts General Hospital, Boston.
They examined a wide spectrum of testosterone levels, and the adverse effects of different levels, by temporarily suppressing the normal endogenous gonadal steroids of healthy men aged 20-50 years using subcutaneous goserelin. In one cohort, 198 men then were randomly assigned to receive placebo, 1.25 g, 2.5 g, 5 g, or 10 g of a topical testosterone gel daily for 16 weeks. In another cohort, 202 men were randomly assigned to receive these same doses of topical testosterone plus 1 mg daily of anastrozole to block the aromatization of testosterone to estrogen.
All the study subjects, who were blinded to their medication assignments, were assessed every 4 weeks for the duration of the study for gonadal steroid levels, physical function, health status, vitality, and sexual function. Dual-energy x-ray absorptiometry (DXA) was used to measure body fat and lean mass, and CT was used to measure the areas of subcutaneous fat, intra-abdominal fat, and thigh muscle. Thigh-muscle strength was assessed using leg presses.
"By administering a variety of testosterone doses, with and without concomitant aromatase inhibition, we found that changes in lean mass, thigh-muscle area, and leg-press strength were attributable to changes in testosterone levels, whereas changes in fat measures were primarily related to changes in estradiol levels. Both androgens and estrogens contributed to the maintenance of normal libido and erectile function," Dr. Finkelstein and his associates said (N. Engl. J. Med. 2013 Sept. 11 [doi:10.1056/NEJMoa1206168]).
As important, the level of testosterone needed to maintain lean mass, fat mass, strength, and sexual function was found to vary considerably among these study subjects.
Most men showed reduced lean mass, muscle area, and erectile function at a mean serum testosterone level of 200 ng/dL, so testosterone supplementation appears to be justified at this level. However, many men showed impairment in these outcomes at lower or higher testosterone levels. In addition, the testosterone levels at which body fat increased and sexual desire decreased varied widely.
"Thus, each person’s specific clinical scenario should be considered when interpreting the clinical significance of the circulating testosterone level," Dr. Finkelstein and his colleagues said.
Also important was the finding that deficiency of estrogen, not testosterone, "is largely responsible for some of the key consequences of male hypogonadism." This indicates that measuring men’s estradiol levels may help in assessing their risk for sexual dysfunction, bone loss, or fat accumulation, the researchers added.
This study was limited in that the duration was restricted to 16 weeks, so as to avoid inducing clinically significant changes in the healthy men who participated. "Because changes in body composition may progress over time, greater changes might have been seen at higher testosterone and estradiol levels if gonadal steroids had been suppressed over a longer period," the investigators noted.
This study was supported by the National Institutes of Health and Abbott Laboratories. Abbott also supplied the testosterone gel at no cost, and Astra Zeneca provided goserelin and anastrozole at no cost, but neither company played a role in study design, data analysis, data interpretation, or manuscript preparation.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Gene study sheds light on response to panitumumab-FOLFOX4 therapy
In addition to KRAS exon 2 mutations, other RAS mutations in tumor samples predict a poor response to antiepidermal growth factor receptor agents such as panitumumab among patients with metastatic colon cancer, according to a report published online Sept. 12 in the New England Journal of Medicine.
In a secondary and exploratory analysis of data from a phase-III randomized clinical trial, patients whose tumors carried any activating RAS mutations did not benefit from, and may have been harmed by, combined panitumumab plus FOLFOX4 (oxaliplatin, fluorouracil, and leucovorin) chemotherapy, said Dr. Jean-Yves Douillard of the Institut de Cancerologie de l’Ouest Rene Gauducheau, Nantes (France), and his associates.
In contrast, patients whose tumors did not carry any activating RAS mutations had clear improvements in progression-free and overall survival when they received the combination panitumumab plus FOLFOX4 treatment.
If these findings are confirmed in other studies, they indicate that "further refinement of tumor-specific genetic markers will allow more accurate selection of patients who are likely to have a response to a particular treatment and prevent toxic effects in those who are unlikely to benefit," the researchers said.
At present, oncologists only test for KRAS exon 2 mutations to identify patients least likely to respond to antiepidermal growth factor receptor (anti-EGFR) therapy. However, even with this effort at patient selection, there remains "a substantial fraction" of patients who have no KRAS exon 2 mutations but still do not benefit from the treatment.
Dr. Douillard and his colleagues reasoned that perhaps the presence of activating mutations in KRAS or NRAS genes might further rule out patients who won’t respond to anti-EGFR agents. So they studied activating mutations of the RAS oncogene family using data from the PRIME (Panitumumab Randomized Trial in Combination with Chemotherapy for Metastatic Colorectal Cancer to Determine Efficacy) study, which compared the efficacy and safety of FOLFOX4 alone against that of FOLFOX4 plus panitumumab in metastatic colon cancer.
Their industry-sponsored secondary analysis involved 1,060 study subjects in whom RAS status could be ascertained: 512 patients whose banked tumor specimens had no RAS mutations and 548 whose tumors had any RAS mutations in exons 2, 3, or 4.
In the patients with no RAS mutations, progression-free survival was longer with the combination therapy (10.1 months) than with FOLFOX alone (7.9 months), as was overall survival (26.0 vs 20.2 months, respectively).
In contrast, among patients who didn’t have KRAS mutations in exon 2 but did have activating mutations in other RAS genes, progression-free survival was significantly shorter with the combined panitumumab-FOLFOX4 therapy (7.3 months) than with FOLFOX4 alone (8.8 months). Overall survival also was shorter.
These trends were observed across all subgroups of patients and for all meaningful endpoints, the investigators said (N. Engl. J. Med. 2013 Sept. 12;369:1023-34 [doi:10.1056/NEJMoa1305272]).
"The observed incidence, types, and severity of adverse events associated with panitumumab-FOLFOX4 in the nonmutated RAS and mutated RAS subgroups were similar to the previously reported safety findings in PRIME, and no new safety signals were identified," Dr. Douillard and his associates said.
These findings must be confirmed in further studies such as pooled trials or meta-analyses of anti-EGFR therapy, they added.
This study was supported by the Royal Marsden Hospital, the Institute of Cancer Research, the National Institute for Health Research, and the Biomedical Research Centre, all in the United Kingdom; Amgen; and Oncologia Ca Granda Onlus Foundazione in Milan. Amgen supervised the gene sequencing analysis, performed all statistical analyses, and assisted with manuscript preparation. Dr. Douillard and his associates reported ties to numerous industry sources.
Medical oncologists now face a challenge: When should they begin screening patients with metastatic colon cancer for a range of RAS mutations?
The retrospective findings from Dr. Douillard et al. "are not definitive enough to require a change from the limited KRAS exon 2 testing currently performed to a broader assessment of RAS status." However, clinicians cannot wait too long for these results to be confirmed or refuted, because many patients with RAS mutations will not be helped, and may indeed be harmed, by treatment with anti-EGFR agents.
Dr. Jordan Berlin is at Vanderbilt-Ingram Cancer Center, Nashville, Tenn. He reported ties to numerous industry sources, including Amgen. These remarks were taken from his editorial accompanying Dr. Douillard’s report (New Engl. J. Med. 2013 [doi:10.1056.NEJMe1307992]).
Medical oncologists now face a challenge: When should they begin screening patients with metastatic colon cancer for a range of RAS mutations?
The retrospective findings from Dr. Douillard et al. "are not definitive enough to require a change from the limited KRAS exon 2 testing currently performed to a broader assessment of RAS status." However, clinicians cannot wait too long for these results to be confirmed or refuted, because many patients with RAS mutations will not be helped, and may indeed be harmed, by treatment with anti-EGFR agents.
Dr. Jordan Berlin is at Vanderbilt-Ingram Cancer Center, Nashville, Tenn. He reported ties to numerous industry sources, including Amgen. These remarks were taken from his editorial accompanying Dr. Douillard’s report (New Engl. J. Med. 2013 [doi:10.1056.NEJMe1307992]).
Medical oncologists now face a challenge: When should they begin screening patients with metastatic colon cancer for a range of RAS mutations?
The retrospective findings from Dr. Douillard et al. "are not definitive enough to require a change from the limited KRAS exon 2 testing currently performed to a broader assessment of RAS status." However, clinicians cannot wait too long for these results to be confirmed or refuted, because many patients with RAS mutations will not be helped, and may indeed be harmed, by treatment with anti-EGFR agents.
Dr. Jordan Berlin is at Vanderbilt-Ingram Cancer Center, Nashville, Tenn. He reported ties to numerous industry sources, including Amgen. These remarks were taken from his editorial accompanying Dr. Douillard’s report (New Engl. J. Med. 2013 [doi:10.1056.NEJMe1307992]).
In addition to KRAS exon 2 mutations, other RAS mutations in tumor samples predict a poor response to antiepidermal growth factor receptor agents such as panitumumab among patients with metastatic colon cancer, according to a report published online Sept. 12 in the New England Journal of Medicine.
In a secondary and exploratory analysis of data from a phase-III randomized clinical trial, patients whose tumors carried any activating RAS mutations did not benefit from, and may have been harmed by, combined panitumumab plus FOLFOX4 (oxaliplatin, fluorouracil, and leucovorin) chemotherapy, said Dr. Jean-Yves Douillard of the Institut de Cancerologie de l’Ouest Rene Gauducheau, Nantes (France), and his associates.
In contrast, patients whose tumors did not carry any activating RAS mutations had clear improvements in progression-free and overall survival when they received the combination panitumumab plus FOLFOX4 treatment.
If these findings are confirmed in other studies, they indicate that "further refinement of tumor-specific genetic markers will allow more accurate selection of patients who are likely to have a response to a particular treatment and prevent toxic effects in those who are unlikely to benefit," the researchers said.
At present, oncologists only test for KRAS exon 2 mutations to identify patients least likely to respond to antiepidermal growth factor receptor (anti-EGFR) therapy. However, even with this effort at patient selection, there remains "a substantial fraction" of patients who have no KRAS exon 2 mutations but still do not benefit from the treatment.
Dr. Douillard and his colleagues reasoned that perhaps the presence of activating mutations in KRAS or NRAS genes might further rule out patients who won’t respond to anti-EGFR agents. So they studied activating mutations of the RAS oncogene family using data from the PRIME (Panitumumab Randomized Trial in Combination with Chemotherapy for Metastatic Colorectal Cancer to Determine Efficacy) study, which compared the efficacy and safety of FOLFOX4 alone against that of FOLFOX4 plus panitumumab in metastatic colon cancer.
Their industry-sponsored secondary analysis involved 1,060 study subjects in whom RAS status could be ascertained: 512 patients whose banked tumor specimens had no RAS mutations and 548 whose tumors had any RAS mutations in exons 2, 3, or 4.
In the patients with no RAS mutations, progression-free survival was longer with the combination therapy (10.1 months) than with FOLFOX alone (7.9 months), as was overall survival (26.0 vs 20.2 months, respectively).
In contrast, among patients who didn’t have KRAS mutations in exon 2 but did have activating mutations in other RAS genes, progression-free survival was significantly shorter with the combined panitumumab-FOLFOX4 therapy (7.3 months) than with FOLFOX4 alone (8.8 months). Overall survival also was shorter.
These trends were observed across all subgroups of patients and for all meaningful endpoints, the investigators said (N. Engl. J. Med. 2013 Sept. 12;369:1023-34 [doi:10.1056/NEJMoa1305272]).
"The observed incidence, types, and severity of adverse events associated with panitumumab-FOLFOX4 in the nonmutated RAS and mutated RAS subgroups were similar to the previously reported safety findings in PRIME, and no new safety signals were identified," Dr. Douillard and his associates said.
These findings must be confirmed in further studies such as pooled trials or meta-analyses of anti-EGFR therapy, they added.
This study was supported by the Royal Marsden Hospital, the Institute of Cancer Research, the National Institute for Health Research, and the Biomedical Research Centre, all in the United Kingdom; Amgen; and Oncologia Ca Granda Onlus Foundazione in Milan. Amgen supervised the gene sequencing analysis, performed all statistical analyses, and assisted with manuscript preparation. Dr. Douillard and his associates reported ties to numerous industry sources.
In addition to KRAS exon 2 mutations, other RAS mutations in tumor samples predict a poor response to antiepidermal growth factor receptor agents such as panitumumab among patients with metastatic colon cancer, according to a report published online Sept. 12 in the New England Journal of Medicine.
In a secondary and exploratory analysis of data from a phase-III randomized clinical trial, patients whose tumors carried any activating RAS mutations did not benefit from, and may have been harmed by, combined panitumumab plus FOLFOX4 (oxaliplatin, fluorouracil, and leucovorin) chemotherapy, said Dr. Jean-Yves Douillard of the Institut de Cancerologie de l’Ouest Rene Gauducheau, Nantes (France), and his associates.
In contrast, patients whose tumors did not carry any activating RAS mutations had clear improvements in progression-free and overall survival when they received the combination panitumumab plus FOLFOX4 treatment.
If these findings are confirmed in other studies, they indicate that "further refinement of tumor-specific genetic markers will allow more accurate selection of patients who are likely to have a response to a particular treatment and prevent toxic effects in those who are unlikely to benefit," the researchers said.
At present, oncologists only test for KRAS exon 2 mutations to identify patients least likely to respond to antiepidermal growth factor receptor (anti-EGFR) therapy. However, even with this effort at patient selection, there remains "a substantial fraction" of patients who have no KRAS exon 2 mutations but still do not benefit from the treatment.
Dr. Douillard and his colleagues reasoned that perhaps the presence of activating mutations in KRAS or NRAS genes might further rule out patients who won’t respond to anti-EGFR agents. So they studied activating mutations of the RAS oncogene family using data from the PRIME (Panitumumab Randomized Trial in Combination with Chemotherapy for Metastatic Colorectal Cancer to Determine Efficacy) study, which compared the efficacy and safety of FOLFOX4 alone against that of FOLFOX4 plus panitumumab in metastatic colon cancer.
Their industry-sponsored secondary analysis involved 1,060 study subjects in whom RAS status could be ascertained: 512 patients whose banked tumor specimens had no RAS mutations and 548 whose tumors had any RAS mutations in exons 2, 3, or 4.
In the patients with no RAS mutations, progression-free survival was longer with the combination therapy (10.1 months) than with FOLFOX alone (7.9 months), as was overall survival (26.0 vs 20.2 months, respectively).
In contrast, among patients who didn’t have KRAS mutations in exon 2 but did have activating mutations in other RAS genes, progression-free survival was significantly shorter with the combined panitumumab-FOLFOX4 therapy (7.3 months) than with FOLFOX4 alone (8.8 months). Overall survival also was shorter.
These trends were observed across all subgroups of patients and for all meaningful endpoints, the investigators said (N. Engl. J. Med. 2013 Sept. 12;369:1023-34 [doi:10.1056/NEJMoa1305272]).
"The observed incidence, types, and severity of adverse events associated with panitumumab-FOLFOX4 in the nonmutated RAS and mutated RAS subgroups were similar to the previously reported safety findings in PRIME, and no new safety signals were identified," Dr. Douillard and his associates said.
These findings must be confirmed in further studies such as pooled trials or meta-analyses of anti-EGFR therapy, they added.
This study was supported by the Royal Marsden Hospital, the Institute of Cancer Research, the National Institute for Health Research, and the Biomedical Research Centre, all in the United Kingdom; Amgen; and Oncologia Ca Granda Onlus Foundazione in Milan. Amgen supervised the gene sequencing analysis, performed all statistical analyses, and assisted with manuscript preparation. Dr. Douillard and his associates reported ties to numerous industry sources.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major finding: Among patients who didn’t have KRAS mutations in exon 2 but did have activating mutations in other RAS genes, progression-free survival was significantly shorter with panitumumab-FOLFOX4 therapy (7.3 months) than with FOLFOX4 alone (8.8 months).
Data source: A secondary analysis of data on 1,060 patients with metastatic colon cancer who participated in a phase-III randomized clinical trial comparing combination panitumumab + FOLFOX4 therapy with FOLFOX4 therapy alone.
Disclosures: This study was supported by the Royal Marsden Hospital, the Institute of Cancer Research, the National Institute for Health Research, and the Biomedical Research Centre, all in the United Kingdom; Amgen; and Oncologia Ca Granda Onlus Foundazione in Milan. Amgen supervised the gene sequencing analysis, performed all statistical analyses, and assisted with manuscript preparation. Dr. Douillard and his associates reported ties to numerous industry sources.