User login
Weekly Exenatide Shows Long-term Efficacy in Type 2 Diabetes
In patents with type 2 diabetes, weekly injections with exenatide controlled hemoglobin A1c levels more effectively than did daily glargine over a 3-year period, investigators reported online in Lancet Diabetes & Endocrinology.
The results from the DURATION-3 trial indicated sustained HbA1c improvement in half of patients who received the glucagonlike peptide-1 (GLP-1) receptor agonist exenatide, compared with just over 40% of patients who received daily treatment with the insulin glargine, said Dr. Michaela Diamant of VU University Medical Centre in Amsterdam and her associates.
Furthermore, the exposure-adjusted rate of overall hypoglycemia was three times higher in the glargine group (0.9 events/patient per year) than in patients who received exenatide (0.3 events/patient per year), independent of HbA1c levels, the researchers said.
"To our knowledge, ours is the longest prospective trial of a long-acting GLP-1 receptor agonist with a comparator group maintained throughout the study duration," said Dr. Diamant. "Our study suggests that GLP-1 receptor agonists could be a viable treatment option in patients for whom insulin is now the treatment of choice."
The open-label, randomized trial enrolled 456 adults with type 2 diabetes who had suboptimal glycemic control (HbA1c 7.1%-11.0%) despite at least 3 months of maximum-tolerated doses of metformin, with or without a sulfonylurea. In addition to their existing oral regimens, patients received either a once-weekly subcutaneous injection of 2 mg exenatide or once-daily glargine titrated to target.
At 3 years, least-squares mean change in HbA1c for patients treated with once-weekly exenatide was –1.01%, compared with –0.81% in patients treated with glargine, for a statistically significant difference of –0.20% (P =.03). Transient gastrointestinal events were more frequent with exenatide, which is typical of GLP-1 receptor agonists, researchers said. Injection-site reactions were also more common in the exenatide group. The rate of serious adverse events was 15% in both groups, the investigators reported (Lancet Diabetes Endocrinol. 2014 [doi:10.1016/S2213-8587(14)70029-4]).
The study was funded by Eli Lilly and by Amylin, a subsidiary of Bristol-Myers Squibb. Dr. Diamant reported having consulted and spoken on behalf of BMS and Eli Lilly without receiving personal compensation. Four authors reported being employed by the companies at the time of the study.
In patents with type 2 diabetes, weekly injections with exenatide controlled hemoglobin A1c levels more effectively than did daily glargine over a 3-year period, investigators reported online in Lancet Diabetes & Endocrinology.
The results from the DURATION-3 trial indicated sustained HbA1c improvement in half of patients who received the glucagonlike peptide-1 (GLP-1) receptor agonist exenatide, compared with just over 40% of patients who received daily treatment with the insulin glargine, said Dr. Michaela Diamant of VU University Medical Centre in Amsterdam and her associates.
Furthermore, the exposure-adjusted rate of overall hypoglycemia was three times higher in the glargine group (0.9 events/patient per year) than in patients who received exenatide (0.3 events/patient per year), independent of HbA1c levels, the researchers said.
"To our knowledge, ours is the longest prospective trial of a long-acting GLP-1 receptor agonist with a comparator group maintained throughout the study duration," said Dr. Diamant. "Our study suggests that GLP-1 receptor agonists could be a viable treatment option in patients for whom insulin is now the treatment of choice."
The open-label, randomized trial enrolled 456 adults with type 2 diabetes who had suboptimal glycemic control (HbA1c 7.1%-11.0%) despite at least 3 months of maximum-tolerated doses of metformin, with or without a sulfonylurea. In addition to their existing oral regimens, patients received either a once-weekly subcutaneous injection of 2 mg exenatide or once-daily glargine titrated to target.
At 3 years, least-squares mean change in HbA1c for patients treated with once-weekly exenatide was –1.01%, compared with –0.81% in patients treated with glargine, for a statistically significant difference of –0.20% (P =.03). Transient gastrointestinal events were more frequent with exenatide, which is typical of GLP-1 receptor agonists, researchers said. Injection-site reactions were also more common in the exenatide group. The rate of serious adverse events was 15% in both groups, the investigators reported (Lancet Diabetes Endocrinol. 2014 [doi:10.1016/S2213-8587(14)70029-4]).
The study was funded by Eli Lilly and by Amylin, a subsidiary of Bristol-Myers Squibb. Dr. Diamant reported having consulted and spoken on behalf of BMS and Eli Lilly without receiving personal compensation. Four authors reported being employed by the companies at the time of the study.
In patents with type 2 diabetes, weekly injections with exenatide controlled hemoglobin A1c levels more effectively than did daily glargine over a 3-year period, investigators reported online in Lancet Diabetes & Endocrinology.
The results from the DURATION-3 trial indicated sustained HbA1c improvement in half of patients who received the glucagonlike peptide-1 (GLP-1) receptor agonist exenatide, compared with just over 40% of patients who received daily treatment with the insulin glargine, said Dr. Michaela Diamant of VU University Medical Centre in Amsterdam and her associates.
Furthermore, the exposure-adjusted rate of overall hypoglycemia was three times higher in the glargine group (0.9 events/patient per year) than in patients who received exenatide (0.3 events/patient per year), independent of HbA1c levels, the researchers said.
"To our knowledge, ours is the longest prospective trial of a long-acting GLP-1 receptor agonist with a comparator group maintained throughout the study duration," said Dr. Diamant. "Our study suggests that GLP-1 receptor agonists could be a viable treatment option in patients for whom insulin is now the treatment of choice."
The open-label, randomized trial enrolled 456 adults with type 2 diabetes who had suboptimal glycemic control (HbA1c 7.1%-11.0%) despite at least 3 months of maximum-tolerated doses of metformin, with or without a sulfonylurea. In addition to their existing oral regimens, patients received either a once-weekly subcutaneous injection of 2 mg exenatide or once-daily glargine titrated to target.
At 3 years, least-squares mean change in HbA1c for patients treated with once-weekly exenatide was –1.01%, compared with –0.81% in patients treated with glargine, for a statistically significant difference of –0.20% (P =.03). Transient gastrointestinal events were more frequent with exenatide, which is typical of GLP-1 receptor agonists, researchers said. Injection-site reactions were also more common in the exenatide group. The rate of serious adverse events was 15% in both groups, the investigators reported (Lancet Diabetes Endocrinol. 2014 [doi:10.1016/S2213-8587(14)70029-4]).
The study was funded by Eli Lilly and by Amylin, a subsidiary of Bristol-Myers Squibb. Dr. Diamant reported having consulted and spoken on behalf of BMS and Eli Lilly without receiving personal compensation. Four authors reported being employed by the companies at the time of the study.
FROM THE LANCET DIABETES & ENDOCRINOLOGY
Weekly exenatide shows long-term efficacy in type 2 diabetes
In patents with type 2 diabetes, weekly injections with exenatide controlled hemoglobin A1c levels more effectively than did daily glargine over a 3-year period, investigators reported online in Lancet Diabetes & Endocrinology.
The results from the DURATION-3 trial indicated sustained HbA1c improvement in half of patients who received the glucagonlike peptide-1 (GLP-1) receptor agonist exenatide, compared with just over 40% of patients who received daily treatment with the insulin glargine, said Dr. Michaela Diamant of VU University Medical Centre in Amsterdam and her associates.
Furthermore, the exposure-adjusted rate of overall hypoglycemia was three times higher in the glargine group (0.9 events/patient per year) than in patients who received exenatide (0.3 events/patient per year), independent of HbA1c levels, the researchers said.
"To our knowledge, ours is the longest prospective trial of a long-acting GLP-1 receptor agonist with a comparator group maintained throughout the study duration," said Dr. Diamant. "Our study suggests that GLP-1 receptor agonists could be a viable treatment option in patients for whom insulin is now the treatment of choice."
The open-label, randomized trial enrolled 456 adults with type 2 diabetes who had suboptimal glycemic control (HbA1c 7.1%-11.0%) despite at least 3 months of maximum-tolerated doses of metformin, with or without a sulfonylurea. In addition to their existing oral regimens, patients received either a once-weekly subcutaneous injection of 2 mg exenatide or once-daily glargine titrated to target.
At 3 years, least-squares mean change in HbA1c for patients treated with once-weekly exenatide was –1.01%, compared with –0.81% in patients treated with glargine, for a statistically significant difference of –0.20% (P =.03). Transient gastrointestinal events were more frequent with exenatide, which is typical of GLP-1 receptor agonists, researchers said. Injection-site reactions were also more common in the exenatide group. The rate of serious adverse events was 15% in both groups, the investigators reported (Lancet Diabetes Endocrinol. 2014 [doi:10.1016/S2213-8587(14)70029-4]).
The study was funded by Eli Lilly and by Amylin, a subsidiary of Bristol-Myers Squibb. Dr. Diamant reported having consulted and spoken on behalf of BMS and Eli Lilly without receiving personal compensation. Four authors reported being employed by the companies at the time of the study.
In patents with type 2 diabetes, weekly injections with exenatide controlled hemoglobin A1c levels more effectively than did daily glargine over a 3-year period, investigators reported online in Lancet Diabetes & Endocrinology.
The results from the DURATION-3 trial indicated sustained HbA1c improvement in half of patients who received the glucagonlike peptide-1 (GLP-1) receptor agonist exenatide, compared with just over 40% of patients who received daily treatment with the insulin glargine, said Dr. Michaela Diamant of VU University Medical Centre in Amsterdam and her associates.
Furthermore, the exposure-adjusted rate of overall hypoglycemia was three times higher in the glargine group (0.9 events/patient per year) than in patients who received exenatide (0.3 events/patient per year), independent of HbA1c levels, the researchers said.
"To our knowledge, ours is the longest prospective trial of a long-acting GLP-1 receptor agonist with a comparator group maintained throughout the study duration," said Dr. Diamant. "Our study suggests that GLP-1 receptor agonists could be a viable treatment option in patients for whom insulin is now the treatment of choice."
The open-label, randomized trial enrolled 456 adults with type 2 diabetes who had suboptimal glycemic control (HbA1c 7.1%-11.0%) despite at least 3 months of maximum-tolerated doses of metformin, with or without a sulfonylurea. In addition to their existing oral regimens, patients received either a once-weekly subcutaneous injection of 2 mg exenatide or once-daily glargine titrated to target.
At 3 years, least-squares mean change in HbA1c for patients treated with once-weekly exenatide was –1.01%, compared with –0.81% in patients treated with glargine, for a statistically significant difference of –0.20% (P =.03). Transient gastrointestinal events were more frequent with exenatide, which is typical of GLP-1 receptor agonists, researchers said. Injection-site reactions were also more common in the exenatide group. The rate of serious adverse events was 15% in both groups, the investigators reported (Lancet Diabetes Endocrinol. 2014 [doi:10.1016/S2213-8587(14)70029-4]).
The study was funded by Eli Lilly and by Amylin, a subsidiary of Bristol-Myers Squibb. Dr. Diamant reported having consulted and spoken on behalf of BMS and Eli Lilly without receiving personal compensation. Four authors reported being employed by the companies at the time of the study.
In patents with type 2 diabetes, weekly injections with exenatide controlled hemoglobin A1c levels more effectively than did daily glargine over a 3-year period, investigators reported online in Lancet Diabetes & Endocrinology.
The results from the DURATION-3 trial indicated sustained HbA1c improvement in half of patients who received the glucagonlike peptide-1 (GLP-1) receptor agonist exenatide, compared with just over 40% of patients who received daily treatment with the insulin glargine, said Dr. Michaela Diamant of VU University Medical Centre in Amsterdam and her associates.
Furthermore, the exposure-adjusted rate of overall hypoglycemia was three times higher in the glargine group (0.9 events/patient per year) than in patients who received exenatide (0.3 events/patient per year), independent of HbA1c levels, the researchers said.
"To our knowledge, ours is the longest prospective trial of a long-acting GLP-1 receptor agonist with a comparator group maintained throughout the study duration," said Dr. Diamant. "Our study suggests that GLP-1 receptor agonists could be a viable treatment option in patients for whom insulin is now the treatment of choice."
The open-label, randomized trial enrolled 456 adults with type 2 diabetes who had suboptimal glycemic control (HbA1c 7.1%-11.0%) despite at least 3 months of maximum-tolerated doses of metformin, with or without a sulfonylurea. In addition to their existing oral regimens, patients received either a once-weekly subcutaneous injection of 2 mg exenatide or once-daily glargine titrated to target.
At 3 years, least-squares mean change in HbA1c for patients treated with once-weekly exenatide was –1.01%, compared with –0.81% in patients treated with glargine, for a statistically significant difference of –0.20% (P =.03). Transient gastrointestinal events were more frequent with exenatide, which is typical of GLP-1 receptor agonists, researchers said. Injection-site reactions were also more common in the exenatide group. The rate of serious adverse events was 15% in both groups, the investigators reported (Lancet Diabetes Endocrinol. 2014 [doi:10.1016/S2213-8587(14)70029-4]).
The study was funded by Eli Lilly and by Amylin, a subsidiary of Bristol-Myers Squibb. Dr. Diamant reported having consulted and spoken on behalf of BMS and Eli Lilly without receiving personal compensation. Four authors reported being employed by the companies at the time of the study.
FROM THE LANCET DIABETES & ENDOCRINOLOGY
Major finding: At 3 years, least-squares mean change in HbA1c for patients treated with once-weekly exenatide was –1.01%, vs. –0.81% in patients treated with glargine (P = .03).
Data source: An open-label, randomized trial of 456 adults with type 2 diabetes and suboptimal glycemic control despite at least 3 months of maximum-tolerated doses of metformin.
Disclosures: The study was funded by Eli Lilly and Amylin, a subsidiary of Bristol-Myers Squibb. Dr. Diamant reported having consulted and spoken on behalf of BMS and Eli Lilly without receiving personal compensation. Four authors reported being employed by the companies at the time of the study.
Federal Government Releases Updated Viral Hepatitis Action Plan
The federal government published a 3-year update of its viral hepatitis action plan that emphasizes the need to expand awareness of infection; improve surveillance, testing, and treatment; eliminate vaccine-preventable hepatitis; and reduce transmission of hepatitis C virus infection.
By 2020, the updated action plan calls for the United States to double the proportion of patients who know they have hepatitis B virus infection (from 33% to 66%); increase the percentage of patients who know they have HCV infection (from 45% to 66%); cut new HCV infections by 25%; and eliminate maternal-child HBV transmission.
Measures of progress include hepatitis B and C mortality and hepatitis B vaccination coverage among health care workers. The plan builds on recent strides in viral hepatitis prevention and treatment – including more widespread availability of safe, effective vaccines for hepatitis A and B and the development of highly effective direct-acting antivirals for chronic hepatitis C infection.
But despite these advances, 3.5-5.3 million Americans still have viral hepatitis, and most do not know they are infected. Sequelae of these infections cause 12,000-18,000 deaths annually – a higher death toll than that from HIV, according to the U.S. Department of Health & Human Services.
The agency authored the plan with input from the Department of Veterans Affairs, the Department of Justice’s Federal Bureau of Prisons, and the Department of Housing and Urban Development.
View on the news: The most important goal is increasing awareness of infection.
Dr. Sean Koppe
"Perhaps the goal with the greatest potential impact relates to increasing awareness of HCV infection," said Dr. Sean Koppe. He noted that less than half of patients with HCV know they are infected, and patients who are unaware of their infections may not learn they have progressive liver disease until they develop symptoms of cirrhosis.
"From the HCV standpoint, I think the action plan is a step, albeit a step that should have been taken several years ago, given that we are currently in the midst of the tremendous burden of HCV cirrhosis and hepatocellular carcinoma," Dr. Koppe said.
With expanded health coverage under the Affordable Care Act, increasing awareness of HCV infection to more than 66% is achievable by 2020, he said. "I think that the CDC [Centers for Disease Control and Prevention] and U.S. Preventive Services Task Force recommendation to screen for HCV in those born between 1945 and 1965 will have a significant impact on increasing awareness of HCV infection. Primary care providers are generally well aware of USPSTF recommendations and are implementing these in their practices. We’ve already experienced an increase of newly diagnosed HCV patients in our hepatology clinics that have been diagnosed because of HCV screening by their primary care provider."
The advent of highly effective and tolerable interferon-free regimens for HCV may have some impact on the goals, said Dr. Koppe. But "in addition to increasing awareness of HCV, governmental agencies also need to ensure access to treatment," he said.
"With the recently approved sofosbuvir and its retail price of $1,000 per pill, we are experiencing some challenges with getting some patients access to this highly effective and expensive medication. Because of budget limitations at the VA [Department of Veteran Affairs], we must be highly selective in how we use this medication, and the Department of Veteran Affairs cannot currently afford to treat all of the hepatitis C patients under their care unless Congress increases its budget."
The hepatitis B goals also are relevant, Dr. Koppe said. "It seems one of the biggest barriers to preventing vertical transmission is identifying pregnant women with hepatitis B early enough in pregnancy to allow for antiviral treatment if they are significantly viremic," he said. "In these patients, the use of hepatitis B immunoglobulin and vaccination of the newborn is typically not adequate to prevent transmission."
Dr. Koppe is a gastroenterologist with the Northwestern University Feinberg School of Medicine and the Jesse Brown VA Medical Center, Chicago. His remarks were excerpted from an interview with Frontline Medical News.
"Perhaps the goal with the greatest potential impact relates to increasing awareness of HCV infection," said Dr. Sean Koppe. He noted that less than half of patients with HCV know they are infected, and patients who are unaware of their infections may not learn they have progressive liver disease until they develop symptoms of cirrhosis.
"From the HCV standpoint, I think the action plan is a step, albeit a step that should have been taken several years ago, given that we are currently in the midst of the tremendous burden of HCV cirrhosis and hepatocellular carcinoma," Dr. Koppe said.

|
|
With expanded health coverage under the Affordable Care Act, increasing awareness of HCV infection to more than 66% is achievable by 2020, he said. "I think that the CDC [Centers for Disease Control and Prevention] and U.S. Preventive Services Task Force recommendation to screen for HCV in those born between 1945 and 1965 will have a significant impact on increasing awareness of HCV infection. Primary care providers are generally well aware of USPSTF recommendations and are implementing these in their practices. We’ve already experienced an increase of newly diagnosed HCV patients in our hepatology clinics that have been diagnosed because of HCV screening by their primary care provider."
The advent of highly effective and tolerable interferon-free regimens for HCV may have some impact on the goals, said Dr. Koppe. But "in addition to increasing awareness of HCV, governmental agencies also need to ensure access to treatment," he said.
"With the recently approved sofosbuvir and its retail price of $1,000 per pill, we are experiencing some challenges with getting some patients access to this highly effective and expensive medication. Because of budget limitations at the VA [Department of Veteran Affairs], we must be highly selective in how we use this medication, and the Department of Veteran Affairs cannot currently afford to treat all of the hepatitis C patients under their care unless Congress increases its budget."
The hepatitis B goals also are relevant, Dr. Koppe said. "It seems one of the biggest barriers to preventing vertical transmission is identifying pregnant women with hepatitis B early enough in pregnancy to allow for antiviral treatment if they are significantly viremic," he said. "In these patients, the use of hepatitis B immunoglobulin and vaccination of the newborn is typically not adequate to prevent transmission."
Dr. Koppe is a gastroenterologist with the Northwestern University Feinberg School of Medicine and the Jesse Brown VA Medical Center, Chicago. His remarks were excerpted from an interview with Frontline Medical News.
"Perhaps the goal with the greatest potential impact relates to increasing awareness of HCV infection," said Dr. Sean Koppe. He noted that less than half of patients with HCV know they are infected, and patients who are unaware of their infections may not learn they have progressive liver disease until they develop symptoms of cirrhosis.
"From the HCV standpoint, I think the action plan is a step, albeit a step that should have been taken several years ago, given that we are currently in the midst of the tremendous burden of HCV cirrhosis and hepatocellular carcinoma," Dr. Koppe said.

|
|
With expanded health coverage under the Affordable Care Act, increasing awareness of HCV infection to more than 66% is achievable by 2020, he said. "I think that the CDC [Centers for Disease Control and Prevention] and U.S. Preventive Services Task Force recommendation to screen for HCV in those born between 1945 and 1965 will have a significant impact on increasing awareness of HCV infection. Primary care providers are generally well aware of USPSTF recommendations and are implementing these in their practices. We’ve already experienced an increase of newly diagnosed HCV patients in our hepatology clinics that have been diagnosed because of HCV screening by their primary care provider."
The advent of highly effective and tolerable interferon-free regimens for HCV may have some impact on the goals, said Dr. Koppe. But "in addition to increasing awareness of HCV, governmental agencies also need to ensure access to treatment," he said.
"With the recently approved sofosbuvir and its retail price of $1,000 per pill, we are experiencing some challenges with getting some patients access to this highly effective and expensive medication. Because of budget limitations at the VA [Department of Veteran Affairs], we must be highly selective in how we use this medication, and the Department of Veteran Affairs cannot currently afford to treat all of the hepatitis C patients under their care unless Congress increases its budget."
The hepatitis B goals also are relevant, Dr. Koppe said. "It seems one of the biggest barriers to preventing vertical transmission is identifying pregnant women with hepatitis B early enough in pregnancy to allow for antiviral treatment if they are significantly viremic," he said. "In these patients, the use of hepatitis B immunoglobulin and vaccination of the newborn is typically not adequate to prevent transmission."
Dr. Koppe is a gastroenterologist with the Northwestern University Feinberg School of Medicine and the Jesse Brown VA Medical Center, Chicago. His remarks were excerpted from an interview with Frontline Medical News.
"Perhaps the goal with the greatest potential impact relates to increasing awareness of HCV infection," said Dr. Sean Koppe. He noted that less than half of patients with HCV know they are infected, and patients who are unaware of their infections may not learn they have progressive liver disease until they develop symptoms of cirrhosis.
"From the HCV standpoint, I think the action plan is a step, albeit a step that should have been taken several years ago, given that we are currently in the midst of the tremendous burden of HCV cirrhosis and hepatocellular carcinoma," Dr. Koppe said.

|
|
With expanded health coverage under the Affordable Care Act, increasing awareness of HCV infection to more than 66% is achievable by 2020, he said. "I think that the CDC [Centers for Disease Control and Prevention] and U.S. Preventive Services Task Force recommendation to screen for HCV in those born between 1945 and 1965 will have a significant impact on increasing awareness of HCV infection. Primary care providers are generally well aware of USPSTF recommendations and are implementing these in their practices. We’ve already experienced an increase of newly diagnosed HCV patients in our hepatology clinics that have been diagnosed because of HCV screening by their primary care provider."
The advent of highly effective and tolerable interferon-free regimens for HCV may have some impact on the goals, said Dr. Koppe. But "in addition to increasing awareness of HCV, governmental agencies also need to ensure access to treatment," he said.
"With the recently approved sofosbuvir and its retail price of $1,000 per pill, we are experiencing some challenges with getting some patients access to this highly effective and expensive medication. Because of budget limitations at the VA [Department of Veteran Affairs], we must be highly selective in how we use this medication, and the Department of Veteran Affairs cannot currently afford to treat all of the hepatitis C patients under their care unless Congress increases its budget."
The hepatitis B goals also are relevant, Dr. Koppe said. "It seems one of the biggest barriers to preventing vertical transmission is identifying pregnant women with hepatitis B early enough in pregnancy to allow for antiviral treatment if they are significantly viremic," he said. "In these patients, the use of hepatitis B immunoglobulin and vaccination of the newborn is typically not adequate to prevent transmission."
Dr. Koppe is a gastroenterologist with the Northwestern University Feinberg School of Medicine and the Jesse Brown VA Medical Center, Chicago. His remarks were excerpted from an interview with Frontline Medical News.
The federal government published a 3-year update of its viral hepatitis action plan that emphasizes the need to expand awareness of infection; improve surveillance, testing, and treatment; eliminate vaccine-preventable hepatitis; and reduce transmission of hepatitis C virus infection.
By 2020, the updated action plan calls for the United States to double the proportion of patients who know they have hepatitis B virus infection (from 33% to 66%); increase the percentage of patients who know they have HCV infection (from 45% to 66%); cut new HCV infections by 25%; and eliminate maternal-child HBV transmission.
Measures of progress include hepatitis B and C mortality and hepatitis B vaccination coverage among health care workers. The plan builds on recent strides in viral hepatitis prevention and treatment – including more widespread availability of safe, effective vaccines for hepatitis A and B and the development of highly effective direct-acting antivirals for chronic hepatitis C infection.
But despite these advances, 3.5-5.3 million Americans still have viral hepatitis, and most do not know they are infected. Sequelae of these infections cause 12,000-18,000 deaths annually – a higher death toll than that from HIV, according to the U.S. Department of Health & Human Services.
The agency authored the plan with input from the Department of Veterans Affairs, the Department of Justice’s Federal Bureau of Prisons, and the Department of Housing and Urban Development.
View on the news: The most important goal is increasing awareness of infection.
Dr. Sean Koppe
"Perhaps the goal with the greatest potential impact relates to increasing awareness of HCV infection," said Dr. Sean Koppe. He noted that less than half of patients with HCV know they are infected, and patients who are unaware of their infections may not learn they have progressive liver disease until they develop symptoms of cirrhosis.
"From the HCV standpoint, I think the action plan is a step, albeit a step that should have been taken several years ago, given that we are currently in the midst of the tremendous burden of HCV cirrhosis and hepatocellular carcinoma," Dr. Koppe said.
With expanded health coverage under the Affordable Care Act, increasing awareness of HCV infection to more than 66% is achievable by 2020, he said. "I think that the CDC [Centers for Disease Control and Prevention] and U.S. Preventive Services Task Force recommendation to screen for HCV in those born between 1945 and 1965 will have a significant impact on increasing awareness of HCV infection. Primary care providers are generally well aware of USPSTF recommendations and are implementing these in their practices. We’ve already experienced an increase of newly diagnosed HCV patients in our hepatology clinics that have been diagnosed because of HCV screening by their primary care provider."
The advent of highly effective and tolerable interferon-free regimens for HCV may have some impact on the goals, said Dr. Koppe. But "in addition to increasing awareness of HCV, governmental agencies also need to ensure access to treatment," he said.
"With the recently approved sofosbuvir and its retail price of $1,000 per pill, we are experiencing some challenges with getting some patients access to this highly effective and expensive medication. Because of budget limitations at the VA [Department of Veteran Affairs], we must be highly selective in how we use this medication, and the Department of Veteran Affairs cannot currently afford to treat all of the hepatitis C patients under their care unless Congress increases its budget."
The hepatitis B goals also are relevant, Dr. Koppe said. "It seems one of the biggest barriers to preventing vertical transmission is identifying pregnant women with hepatitis B early enough in pregnancy to allow for antiviral treatment if they are significantly viremic," he said. "In these patients, the use of hepatitis B immunoglobulin and vaccination of the newborn is typically not adequate to prevent transmission."
Dr. Koppe is a gastroenterologist with the Northwestern University Feinberg School of Medicine and the Jesse Brown VA Medical Center, Chicago. His remarks were excerpted from an interview with Frontline Medical News.
The federal government published a 3-year update of its viral hepatitis action plan that emphasizes the need to expand awareness of infection; improve surveillance, testing, and treatment; eliminate vaccine-preventable hepatitis; and reduce transmission of hepatitis C virus infection.
By 2020, the updated action plan calls for the United States to double the proportion of patients who know they have hepatitis B virus infection (from 33% to 66%); increase the percentage of patients who know they have HCV infection (from 45% to 66%); cut new HCV infections by 25%; and eliminate maternal-child HBV transmission.
Measures of progress include hepatitis B and C mortality and hepatitis B vaccination coverage among health care workers. The plan builds on recent strides in viral hepatitis prevention and treatment – including more widespread availability of safe, effective vaccines for hepatitis A and B and the development of highly effective direct-acting antivirals for chronic hepatitis C infection.
But despite these advances, 3.5-5.3 million Americans still have viral hepatitis, and most do not know they are infected. Sequelae of these infections cause 12,000-18,000 deaths annually – a higher death toll than that from HIV, according to the U.S. Department of Health & Human Services.
The agency authored the plan with input from the Department of Veterans Affairs, the Department of Justice’s Federal Bureau of Prisons, and the Department of Housing and Urban Development.
View on the news: The most important goal is increasing awareness of infection.
Dr. Sean Koppe
"Perhaps the goal with the greatest potential impact relates to increasing awareness of HCV infection," said Dr. Sean Koppe. He noted that less than half of patients with HCV know they are infected, and patients who are unaware of their infections may not learn they have progressive liver disease until they develop symptoms of cirrhosis.
"From the HCV standpoint, I think the action plan is a step, albeit a step that should have been taken several years ago, given that we are currently in the midst of the tremendous burden of HCV cirrhosis and hepatocellular carcinoma," Dr. Koppe said.
With expanded health coverage under the Affordable Care Act, increasing awareness of HCV infection to more than 66% is achievable by 2020, he said. "I think that the CDC [Centers for Disease Control and Prevention] and U.S. Preventive Services Task Force recommendation to screen for HCV in those born between 1945 and 1965 will have a significant impact on increasing awareness of HCV infection. Primary care providers are generally well aware of USPSTF recommendations and are implementing these in their practices. We’ve already experienced an increase of newly diagnosed HCV patients in our hepatology clinics that have been diagnosed because of HCV screening by their primary care provider."
The advent of highly effective and tolerable interferon-free regimens for HCV may have some impact on the goals, said Dr. Koppe. But "in addition to increasing awareness of HCV, governmental agencies also need to ensure access to treatment," he said.
"With the recently approved sofosbuvir and its retail price of $1,000 per pill, we are experiencing some challenges with getting some patients access to this highly effective and expensive medication. Because of budget limitations at the VA [Department of Veteran Affairs], we must be highly selective in how we use this medication, and the Department of Veteran Affairs cannot currently afford to treat all of the hepatitis C patients under their care unless Congress increases its budget."
The hepatitis B goals also are relevant, Dr. Koppe said. "It seems one of the biggest barriers to preventing vertical transmission is identifying pregnant women with hepatitis B early enough in pregnancy to allow for antiviral treatment if they are significantly viremic," he said. "In these patients, the use of hepatitis B immunoglobulin and vaccination of the newborn is typically not adequate to prevent transmission."
Dr. Koppe is a gastroenterologist with the Northwestern University Feinberg School of Medicine and the Jesse Brown VA Medical Center, Chicago. His remarks were excerpted from an interview with Frontline Medical News.
Federal government releases updated viral hepatitis action plan
The federal government on April 4 published a 3-year update of its viral hepatitis action plan that emphasizes the need to expand awareness of infection; improve surveillance, testing, and treatment; eliminate vaccine-preventable hepatitis; and reduce transmission of hepatitis C virus infection.
By 2020, the updated action plan calls for the United States to double the proportion of patients who know they have hepatitis B virus infection (from 33% to 66%); increase the percentage of patients who know they have HCV infection (from 45% to 66%); cut new HCV infections by 25%; and eliminate maternal-child HBV transmission.
Measures of progress include hepatitis B and C mortality and hepatitis B vaccination coverage among health care workers. The plan builds on recent strides in viral hepatitis prevention and treatment – including more widespread availability of safe, effective vaccines for hepatitis A and B and the development of highly effective direct-acting antivirals for chronic hepatitis C infection.
But despite these advances, 3.5-5.3 million Americans still have viral hepatitis, and most do not know they are infected. Sequelae of these infections cause 12,000-18,000 deaths annually – a higher death toll than that from HIV, according to the U.S. Department of Health & Human Services.
The agency authored the plan with input from the Department of Veterans Affairs, the Department of Justice’s Federal Bureau of Prisons, and the Department of Housing and Urban Development.
"Perhaps the goal with the greatest potential impact relates to increasing awareness of HCV infection," said Dr. Sean Koppe. He noted that less than half of patients with HCV know they are infected, and patients who are unaware of their infections may not learn they have progressive liver disease until they develop symptoms of cirrhosis.
"From the HCV standpoint, I think the action plan is a step, albeit a step that should have been taken several years ago, given that we are currently in the midst of the tremendous burden of HCV cirrhosis and hepatocellular carcinoma," Dr. Koppe said.

|
|
With expanded health coverage under the Affordable Care Act, increasing awareness of HCV infection to more than 66% is achievable by 2020, he said. "I think that the CDC [Centers for Disease Control and Prevention] and U.S. Preventive Services Task Force recommendation to screen for HCV in those born between 1945 and 1965 will have a significant impact on increasing awareness of HCV infection. Primary care providers are generally well aware of USPSTF recommendations and are implementing these in their practices. We’ve already experienced an increase of newly diagnosed HCV patients in our hepatology clinics that have been diagnosed because of HCV screening by their primary care provider."
The advent of highly effective and tolerable interferon-free regimens for HCV may have some impact on the goals, said Dr. Koppe. But "in addition to increasing awareness of HCV, governmental agencies also need to ensure access to treatment," he said.
"With the recently approved sofosbuvir and its retail price of $1,000 per pill, we are experiencing some challenges with getting some patients access to this highly effective and expensive medication. Because of budget limitations at the VA [Department of Veteran Affairs], we must be highly selective in how we use this medication, and the Department of Veteran Affairs cannot currently afford to treat all of the hepatitis C patients under their care unless Congress increases its budget."
The hepatitis B goals also are relevant, Dr. Koppe said. "It seems one of the biggest barriers to preventing vertical transmission is identifying pregnant women with hepatitis B early enough in pregnancy to allow for antiviral treatment if they are significantly viremic," he said. "In these patients, the use of hepatitis B immunoglobulin and vaccination of the newborn is typically not adequate to prevent transmission."
Dr. Koppe is a gastroenterologist with the Northwestern University Feinberg School of Medicine and the Jesse Brown VA Medical Center, Chicago. His remarks were excerpted from an interview with Frontline Medical News.
"Perhaps the goal with the greatest potential impact relates to increasing awareness of HCV infection," said Dr. Sean Koppe. He noted that less than half of patients with HCV know they are infected, and patients who are unaware of their infections may not learn they have progressive liver disease until they develop symptoms of cirrhosis.
"From the HCV standpoint, I think the action plan is a step, albeit a step that should have been taken several years ago, given that we are currently in the midst of the tremendous burden of HCV cirrhosis and hepatocellular carcinoma," Dr. Koppe said.

|
|
With expanded health coverage under the Affordable Care Act, increasing awareness of HCV infection to more than 66% is achievable by 2020, he said. "I think that the CDC [Centers for Disease Control and Prevention] and U.S. Preventive Services Task Force recommendation to screen for HCV in those born between 1945 and 1965 will have a significant impact on increasing awareness of HCV infection. Primary care providers are generally well aware of USPSTF recommendations and are implementing these in their practices. We’ve already experienced an increase of newly diagnosed HCV patients in our hepatology clinics that have been diagnosed because of HCV screening by their primary care provider."
The advent of highly effective and tolerable interferon-free regimens for HCV may have some impact on the goals, said Dr. Koppe. But "in addition to increasing awareness of HCV, governmental agencies also need to ensure access to treatment," he said.
"With the recently approved sofosbuvir and its retail price of $1,000 per pill, we are experiencing some challenges with getting some patients access to this highly effective and expensive medication. Because of budget limitations at the VA [Department of Veteran Affairs], we must be highly selective in how we use this medication, and the Department of Veteran Affairs cannot currently afford to treat all of the hepatitis C patients under their care unless Congress increases its budget."
The hepatitis B goals also are relevant, Dr. Koppe said. "It seems one of the biggest barriers to preventing vertical transmission is identifying pregnant women with hepatitis B early enough in pregnancy to allow for antiviral treatment if they are significantly viremic," he said. "In these patients, the use of hepatitis B immunoglobulin and vaccination of the newborn is typically not adequate to prevent transmission."
Dr. Koppe is a gastroenterologist with the Northwestern University Feinberg School of Medicine and the Jesse Brown VA Medical Center, Chicago. His remarks were excerpted from an interview with Frontline Medical News.
"Perhaps the goal with the greatest potential impact relates to increasing awareness of HCV infection," said Dr. Sean Koppe. He noted that less than half of patients with HCV know they are infected, and patients who are unaware of their infections may not learn they have progressive liver disease until they develop symptoms of cirrhosis.
"From the HCV standpoint, I think the action plan is a step, albeit a step that should have been taken several years ago, given that we are currently in the midst of the tremendous burden of HCV cirrhosis and hepatocellular carcinoma," Dr. Koppe said.

|
|
With expanded health coverage under the Affordable Care Act, increasing awareness of HCV infection to more than 66% is achievable by 2020, he said. "I think that the CDC [Centers for Disease Control and Prevention] and U.S. Preventive Services Task Force recommendation to screen for HCV in those born between 1945 and 1965 will have a significant impact on increasing awareness of HCV infection. Primary care providers are generally well aware of USPSTF recommendations and are implementing these in their practices. We’ve already experienced an increase of newly diagnosed HCV patients in our hepatology clinics that have been diagnosed because of HCV screening by their primary care provider."
The advent of highly effective and tolerable interferon-free regimens for HCV may have some impact on the goals, said Dr. Koppe. But "in addition to increasing awareness of HCV, governmental agencies also need to ensure access to treatment," he said.
"With the recently approved sofosbuvir and its retail price of $1,000 per pill, we are experiencing some challenges with getting some patients access to this highly effective and expensive medication. Because of budget limitations at the VA [Department of Veteran Affairs], we must be highly selective in how we use this medication, and the Department of Veteran Affairs cannot currently afford to treat all of the hepatitis C patients under their care unless Congress increases its budget."
The hepatitis B goals also are relevant, Dr. Koppe said. "It seems one of the biggest barriers to preventing vertical transmission is identifying pregnant women with hepatitis B early enough in pregnancy to allow for antiviral treatment if they are significantly viremic," he said. "In these patients, the use of hepatitis B immunoglobulin and vaccination of the newborn is typically not adequate to prevent transmission."
Dr. Koppe is a gastroenterologist with the Northwestern University Feinberg School of Medicine and the Jesse Brown VA Medical Center, Chicago. His remarks were excerpted from an interview with Frontline Medical News.
The federal government on April 4 published a 3-year update of its viral hepatitis action plan that emphasizes the need to expand awareness of infection; improve surveillance, testing, and treatment; eliminate vaccine-preventable hepatitis; and reduce transmission of hepatitis C virus infection.
By 2020, the updated action plan calls for the United States to double the proportion of patients who know they have hepatitis B virus infection (from 33% to 66%); increase the percentage of patients who know they have HCV infection (from 45% to 66%); cut new HCV infections by 25%; and eliminate maternal-child HBV transmission.
Measures of progress include hepatitis B and C mortality and hepatitis B vaccination coverage among health care workers. The plan builds on recent strides in viral hepatitis prevention and treatment – including more widespread availability of safe, effective vaccines for hepatitis A and B and the development of highly effective direct-acting antivirals for chronic hepatitis C infection.
But despite these advances, 3.5-5.3 million Americans still have viral hepatitis, and most do not know they are infected. Sequelae of these infections cause 12,000-18,000 deaths annually – a higher death toll than that from HIV, according to the U.S. Department of Health & Human Services.
The agency authored the plan with input from the Department of Veterans Affairs, the Department of Justice’s Federal Bureau of Prisons, and the Department of Housing and Urban Development.
The federal government on April 4 published a 3-year update of its viral hepatitis action plan that emphasizes the need to expand awareness of infection; improve surveillance, testing, and treatment; eliminate vaccine-preventable hepatitis; and reduce transmission of hepatitis C virus infection.
By 2020, the updated action plan calls for the United States to double the proportion of patients who know they have hepatitis B virus infection (from 33% to 66%); increase the percentage of patients who know they have HCV infection (from 45% to 66%); cut new HCV infections by 25%; and eliminate maternal-child HBV transmission.
Measures of progress include hepatitis B and C mortality and hepatitis B vaccination coverage among health care workers. The plan builds on recent strides in viral hepatitis prevention and treatment – including more widespread availability of safe, effective vaccines for hepatitis A and B and the development of highly effective direct-acting antivirals for chronic hepatitis C infection.
But despite these advances, 3.5-5.3 million Americans still have viral hepatitis, and most do not know they are infected. Sequelae of these infections cause 12,000-18,000 deaths annually – a higher death toll than that from HIV, according to the U.S. Department of Health & Human Services.
The agency authored the plan with input from the Department of Veterans Affairs, the Department of Justice’s Federal Bureau of Prisons, and the Department of Housing and Urban Development.
Suicide at higher altitudes linked to bipolar disorder
Persons who committed suicide and lived at higher altitudes were significantly more likely to have bipolar disorder, compared with depression, schizophrenia, or anxiety disorders, researchers reported in the April issue of Medical Hypotheses.
Past research has found an association between altitude and suicide, even after controlling for gun ownership, rurality, age, and mental health access. The current study indicates that altitude preferentially affects suicide in bipolar disorder, said Rebekah S. Huber, a researcher at the University of Utah Brain Institute, Salt Lake City, and her associates.
The researchers performed random coefficient logistic regression modeling and least squares means on data for 35,725 suicides in 16 states and 809 counties that occurred during 2005-2008 and were reported to the Centers for Disease Control and Prevention’s National Violent Death Reporting System. The investigators assigned every decedent a single major diagnosis of bipolar disorder, major depressive disorder, schizophrenia, or anxiety disorder, and excluded infrequent diagnoses such as posttraumatic stress disorder or eating disorder.
Living at higher altitude was significantly associated with having coefficient (P = .004) and logistic regression (P = .001) models. Persons with bipolar disorder committed suicide at a higher mean altitude (1,205 meters) than did decedents with anxiety disorders (1,181), major depressive disorder (1,116), or schizophrenia (1,057).
The reason for the effect merits further study but might be tied to underlying mitochondrial dysfunction in bipolar disorder, lower levels of environmental lithium at higher altitudes, or diminished efficacy of bipolar disorder treatments at higher elevations, the investigators said (Med. Hypotheses 2014;82:377-81).
"Metabolic stress due to hypoxia may have important considerations for individuals with [bipolar disorder]," they added. "Hypoxia due to reduced oxygen partial pressure at higher altitudes may further decrease mitochondrial function in individuals with BD. For these individuals, metabolic changes associated with hypoxia may lead to depression, instability of mood, and increased risk of suicide."
The researchers cited several limitations. For example, the findings are based on results from far less than half of the 50 states, but "many states in the intermountain West are included," they wrote.
The VISN 19 Mental Illness Research and Education Center, the Utah Science Technology and Research Initiative, and the National Institutes of Health funded the research. The authors reported no conflicts of interest.
Persons who committed suicide and lived at higher altitudes were significantly more likely to have bipolar disorder, compared with depression, schizophrenia, or anxiety disorders, researchers reported in the April issue of Medical Hypotheses.
Past research has found an association between altitude and suicide, even after controlling for gun ownership, rurality, age, and mental health access. The current study indicates that altitude preferentially affects suicide in bipolar disorder, said Rebekah S. Huber, a researcher at the University of Utah Brain Institute, Salt Lake City, and her associates.
The researchers performed random coefficient logistic regression modeling and least squares means on data for 35,725 suicides in 16 states and 809 counties that occurred during 2005-2008 and were reported to the Centers for Disease Control and Prevention’s National Violent Death Reporting System. The investigators assigned every decedent a single major diagnosis of bipolar disorder, major depressive disorder, schizophrenia, or anxiety disorder, and excluded infrequent diagnoses such as posttraumatic stress disorder or eating disorder.
Living at higher altitude was significantly associated with having coefficient (P = .004) and logistic regression (P = .001) models. Persons with bipolar disorder committed suicide at a higher mean altitude (1,205 meters) than did decedents with anxiety disorders (1,181), major depressive disorder (1,116), or schizophrenia (1,057).
The reason for the effect merits further study but might be tied to underlying mitochondrial dysfunction in bipolar disorder, lower levels of environmental lithium at higher altitudes, or diminished efficacy of bipolar disorder treatments at higher elevations, the investigators said (Med. Hypotheses 2014;82:377-81).
"Metabolic stress due to hypoxia may have important considerations for individuals with [bipolar disorder]," they added. "Hypoxia due to reduced oxygen partial pressure at higher altitudes may further decrease mitochondrial function in individuals with BD. For these individuals, metabolic changes associated with hypoxia may lead to depression, instability of mood, and increased risk of suicide."
The researchers cited several limitations. For example, the findings are based on results from far less than half of the 50 states, but "many states in the intermountain West are included," they wrote.
The VISN 19 Mental Illness Research and Education Center, the Utah Science Technology and Research Initiative, and the National Institutes of Health funded the research. The authors reported no conflicts of interest.
Persons who committed suicide and lived at higher altitudes were significantly more likely to have bipolar disorder, compared with depression, schizophrenia, or anxiety disorders, researchers reported in the April issue of Medical Hypotheses.
Past research has found an association between altitude and suicide, even after controlling for gun ownership, rurality, age, and mental health access. The current study indicates that altitude preferentially affects suicide in bipolar disorder, said Rebekah S. Huber, a researcher at the University of Utah Brain Institute, Salt Lake City, and her associates.
The researchers performed random coefficient logistic regression modeling and least squares means on data for 35,725 suicides in 16 states and 809 counties that occurred during 2005-2008 and were reported to the Centers for Disease Control and Prevention’s National Violent Death Reporting System. The investigators assigned every decedent a single major diagnosis of bipolar disorder, major depressive disorder, schizophrenia, or anxiety disorder, and excluded infrequent diagnoses such as posttraumatic stress disorder or eating disorder.
Living at higher altitude was significantly associated with having coefficient (P = .004) and logistic regression (P = .001) models. Persons with bipolar disorder committed suicide at a higher mean altitude (1,205 meters) than did decedents with anxiety disorders (1,181), major depressive disorder (1,116), or schizophrenia (1,057).
The reason for the effect merits further study but might be tied to underlying mitochondrial dysfunction in bipolar disorder, lower levels of environmental lithium at higher altitudes, or diminished efficacy of bipolar disorder treatments at higher elevations, the investigators said (Med. Hypotheses 2014;82:377-81).
"Metabolic stress due to hypoxia may have important considerations for individuals with [bipolar disorder]," they added. "Hypoxia due to reduced oxygen partial pressure at higher altitudes may further decrease mitochondrial function in individuals with BD. For these individuals, metabolic changes associated with hypoxia may lead to depression, instability of mood, and increased risk of suicide."
The researchers cited several limitations. For example, the findings are based on results from far less than half of the 50 states, but "many states in the intermountain West are included," they wrote.
The VISN 19 Mental Illness Research and Education Center, the Utah Science Technology and Research Initiative, and the National Institutes of Health funded the research. The authors reported no conflicts of interest.
FROM MEDICAL HYPOTHESES
Major finding: Among persons who committed suicide, living at higher altitude was significantly associated with having bipolar disorder instead of another mental health diagnosis in both random coefficient (P = .004) and logistic regression (P = .001) models.
Data source: The study looked at 12,861 suicides by persons with mental health diagnoses reported to the National Violent Death Reporting System. Decedents lived in 16 states and committed suicide during 2005-2008.
Disclosures: The VISN 19 Mental Illness Research and Education Center, the Utah Science Technology and Research Initiative, and the National Institutes of Health funded the research. The authors reported no conflicts of interest.
High medication burden persists in bipolar disorder
Almost one-third of patients with bipolar I disorder were taking at least four psychotropic medications when admitted to a psychiatric hospital, researchers reported in the April issue of Psychiatry Research.
The findings "reflect the enormous challenge of symptom management" in bipolar I disorder and the "fine line between help and harm that clinicians face" because monotherapies for [bipolar disorder] often are ineffective, said Dr. Lauren M. Weinstock and her associates at Brown University and Butler Hospital in Providence, R.I.
Using a computer algorithm, the investigators reviewed the charts of 218 adults with bipolar I disorder presenting for admission to a single psychiatric hospital. Patients averaged 42 years in age (range, 18-77), and 58% were female (Psychiatry Res. 2014;216:24-30).
In all, 82 patients (32%) were taking at least four psychotropic medications on admission. Taking this many medications was significantly associated with comorbid anxiety disorder (P less than .001), depression on admission (P = .002), a past suicide attempt (P = .010), and female gender (P = .025). Women were more likely than men to be prescribed benzodiazepines (P = .008), antidepressants (P = .012), and stimulants (P = .052), even after depressed mood was controlled for.
The results highlight concerns about an "increased risk of adverse side effects, drug interactions, medication error, and poor treatment adherence," and the complex polypharmacy’s "high cost burden to both patients and the health care system," said Dr. Weinstock and her associates. They emphasized the need for more research on outpatient prescribing for bipolar disorder patients and "the potential risks, especially for women, of iatrogenic complications without evidence of potential benefits."
The researchers did not use supplementary methods to confirm chart data and could not distinguish between long-standing treatment patterns or recent changes to medications. Because 94% of patients were white and most had health insurance, the findings could not be generalized to other patient populations.
A grant from the National Institute of Mental Health funded manuscript preparation. The authors did not disclose conflicts of interest.
Almost one-third of patients with bipolar I disorder were taking at least four psychotropic medications when admitted to a psychiatric hospital, researchers reported in the April issue of Psychiatry Research.
The findings "reflect the enormous challenge of symptom management" in bipolar I disorder and the "fine line between help and harm that clinicians face" because monotherapies for [bipolar disorder] often are ineffective, said Dr. Lauren M. Weinstock and her associates at Brown University and Butler Hospital in Providence, R.I.
Using a computer algorithm, the investigators reviewed the charts of 218 adults with bipolar I disorder presenting for admission to a single psychiatric hospital. Patients averaged 42 years in age (range, 18-77), and 58% were female (Psychiatry Res. 2014;216:24-30).
In all, 82 patients (32%) were taking at least four psychotropic medications on admission. Taking this many medications was significantly associated with comorbid anxiety disorder (P less than .001), depression on admission (P = .002), a past suicide attempt (P = .010), and female gender (P = .025). Women were more likely than men to be prescribed benzodiazepines (P = .008), antidepressants (P = .012), and stimulants (P = .052), even after depressed mood was controlled for.
The results highlight concerns about an "increased risk of adverse side effects, drug interactions, medication error, and poor treatment adherence," and the complex polypharmacy’s "high cost burden to both patients and the health care system," said Dr. Weinstock and her associates. They emphasized the need for more research on outpatient prescribing for bipolar disorder patients and "the potential risks, especially for women, of iatrogenic complications without evidence of potential benefits."
The researchers did not use supplementary methods to confirm chart data and could not distinguish between long-standing treatment patterns or recent changes to medications. Because 94% of patients were white and most had health insurance, the findings could not be generalized to other patient populations.
A grant from the National Institute of Mental Health funded manuscript preparation. The authors did not disclose conflicts of interest.
Almost one-third of patients with bipolar I disorder were taking at least four psychotropic medications when admitted to a psychiatric hospital, researchers reported in the April issue of Psychiatry Research.
The findings "reflect the enormous challenge of symptom management" in bipolar I disorder and the "fine line between help and harm that clinicians face" because monotherapies for [bipolar disorder] often are ineffective, said Dr. Lauren M. Weinstock and her associates at Brown University and Butler Hospital in Providence, R.I.
Using a computer algorithm, the investigators reviewed the charts of 218 adults with bipolar I disorder presenting for admission to a single psychiatric hospital. Patients averaged 42 years in age (range, 18-77), and 58% were female (Psychiatry Res. 2014;216:24-30).
In all, 82 patients (32%) were taking at least four psychotropic medications on admission. Taking this many medications was significantly associated with comorbid anxiety disorder (P less than .001), depression on admission (P = .002), a past suicide attempt (P = .010), and female gender (P = .025). Women were more likely than men to be prescribed benzodiazepines (P = .008), antidepressants (P = .012), and stimulants (P = .052), even after depressed mood was controlled for.
The results highlight concerns about an "increased risk of adverse side effects, drug interactions, medication error, and poor treatment adherence," and the complex polypharmacy’s "high cost burden to both patients and the health care system," said Dr. Weinstock and her associates. They emphasized the need for more research on outpatient prescribing for bipolar disorder patients and "the potential risks, especially for women, of iatrogenic complications without evidence of potential benefits."
The researchers did not use supplementary methods to confirm chart data and could not distinguish between long-standing treatment patterns or recent changes to medications. Because 94% of patients were white and most had health insurance, the findings could not be generalized to other patient populations.
A grant from the National Institute of Mental Health funded manuscript preparation. The authors did not disclose conflicts of interest.
FROM PSYCHIATRY RESEARCH
Major finding: Eight-two patients (32%) were taking at least four psychotropic medications. Taking this many medications was significantly associated with comorbid anxiety disorder (P less than .001), depression on admission (P = .002), a past suicide attempt (P = .010), and female gender (P = .025).
Data source: A retrospective chart study of 218 patients with bipolar I disorder who were presenting for psychiatric hospital admission.
Disclosures: A grant from the National Institute of Mental Health funded manuscript preparation. The authors did not disclose conflicts of interest.
Depression at least five times more common than PTSD after critical illness
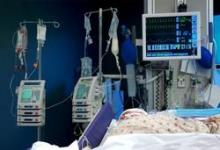
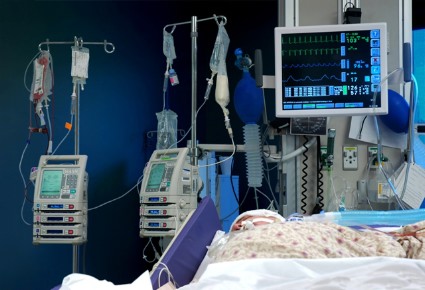
Patients discharged from intensive care units were far more likely to report physical symptoms of depression than posttraumatic distress disorder symptoms, based on research published online April 6 in Lancet Respiratory Medicine.
"Depression and posttraumatic distress disorder are important mental health problems after critical illness, but our findings show that depression is at least five times more common than posttraumatic distress disorder and is largely somatic in nature," said James C. Jackson, Psy.D., at Vanderbilt University in Nashville, Tenn., and his associates. "This finding suggests that physical disability contributes predominantly to this depression, which has implications for the roles of physical rehabilitation vs. antidepressant medications in the prevention and management of depression after ICU admission." Lancet
Respir. Med. 2014 March 6 [doi: 10.1016/S2213-2600(14)70051-7]
The prospective, multicenter longitudinal cohort study enrolled 821 patients (median age, 61 years) treated in medical and surgical ICUs for respiratory failure, cardiogenic shock, or septic shock.
Data were available for 406 patients 3 months after discharge, of which 37% reported at least mild depression symptoms, while only 7% reported posttraumatic stress disorder (PTSD) symptoms. At 12 months after discharge, 33% of patients reported depression, compared with 7% for PTSD. Depression was primarily somatic in nature and was common even among patients with no past history of the disorder (prevalence, 30% and 29% at 3 and 12 months, respectively). Disabilities in activities of daily living affected from 23%-32% of patients.
"Our data further show that monitoring these outcomes is relevant for survivors of all ages, and that non–pharmacological interventions during the ICU stay (previously assumed to improve physical outcomes in ICU survivors) should be tested in terms of their ability to change mental health and functional outcomes," the investigators concluded.
Dr. Jackson receives grant support from the National Institutes of Health. Ten of his associates reported receiving funding, honoraria, and other support from Hospira; Abbott; Orion Pharma; the Veterans Affairs Clinical Science Research and Development Service; the Tennessee Valley Geriatric Research, Education, and Clinical Center; the National Institutes of Health; and the Vanderbilt Clinical and Translational Research Scholars Program.
Just 15 years ago, the long-term sequelae of severe sepsis and acute respiratory distress syndrome were unknown, said Dr. Hallie C. Prescott and Dr. Theodore J. Iwashyna. But as survival rates in intensive care units improved, "it became clear that something was not right. Survivors were not the same after critical illness. Rather, they had new weaknesses, cognitive impairment, depression, and early death."
But the causes and treatment of post–intensive care syndrome have eluded researchers, said Dr. Prescott and Dr. Iwashyna. The current study’s findings help fill that gap. "By differentiation of depression into cognitive and physical components, Jackson and colleagues have provided an important step towards tailoring of future interventions to specific symptoms subsets, and not the generic diagnosis of depression."
Somatic symptoms among survivors might be from functional limitations and medical comorbidities instead of a neurochemical imbalance, they added. "As such, traditional pharmacologic therapies for depression might be less likely to provide significant benefit alone (or at all). Instead, doctors might need to address the many diagnoses that contribute to poor sleep, impaired concentration, weakness, and fatigue. Although largely absent from the history of post–intensive care syndrome to date, consideration is needed of how common chronic medical conditions such as diabetes, heart failure, and chronic pulmonary disease contribute to the morbidity of survivors of critical illness."
Dr. Prescott is a clinical fellow and Dr. Iwashyna is an assistant professor of internal medicine with the University of Michigan, Ann Arbor. They reported receiving grant support from the National Institutes of Health and the Department of Veterans Affairs. These remarks were taken from their editorial accompanying Dr. Jackson’s report (Lancet 2014 [doi:10.1016/S2213-2600(14)70071-2]).
Just 15 years ago, the long-term sequelae of severe sepsis and acute respiratory distress syndrome were unknown, said Dr. Hallie C. Prescott and Dr. Theodore J. Iwashyna. But as survival rates in intensive care units improved, "it became clear that something was not right. Survivors were not the same after critical illness. Rather, they had new weaknesses, cognitive impairment, depression, and early death."
But the causes and treatment of post–intensive care syndrome have eluded researchers, said Dr. Prescott and Dr. Iwashyna. The current study’s findings help fill that gap. "By differentiation of depression into cognitive and physical components, Jackson and colleagues have provided an important step towards tailoring of future interventions to specific symptoms subsets, and not the generic diagnosis of depression."
Somatic symptoms among survivors might be from functional limitations and medical comorbidities instead of a neurochemical imbalance, they added. "As such, traditional pharmacologic therapies for depression might be less likely to provide significant benefit alone (or at all). Instead, doctors might need to address the many diagnoses that contribute to poor sleep, impaired concentration, weakness, and fatigue. Although largely absent from the history of post–intensive care syndrome to date, consideration is needed of how common chronic medical conditions such as diabetes, heart failure, and chronic pulmonary disease contribute to the morbidity of survivors of critical illness."
Dr. Prescott is a clinical fellow and Dr. Iwashyna is an assistant professor of internal medicine with the University of Michigan, Ann Arbor. They reported receiving grant support from the National Institutes of Health and the Department of Veterans Affairs. These remarks were taken from their editorial accompanying Dr. Jackson’s report (Lancet 2014 [doi:10.1016/S2213-2600(14)70071-2]).
Just 15 years ago, the long-term sequelae of severe sepsis and acute respiratory distress syndrome were unknown, said Dr. Hallie C. Prescott and Dr. Theodore J. Iwashyna. But as survival rates in intensive care units improved, "it became clear that something was not right. Survivors were not the same after critical illness. Rather, they had new weaknesses, cognitive impairment, depression, and early death."
But the causes and treatment of post–intensive care syndrome have eluded researchers, said Dr. Prescott and Dr. Iwashyna. The current study’s findings help fill that gap. "By differentiation of depression into cognitive and physical components, Jackson and colleagues have provided an important step towards tailoring of future interventions to specific symptoms subsets, and not the generic diagnosis of depression."
Somatic symptoms among survivors might be from functional limitations and medical comorbidities instead of a neurochemical imbalance, they added. "As such, traditional pharmacologic therapies for depression might be less likely to provide significant benefit alone (or at all). Instead, doctors might need to address the many diagnoses that contribute to poor sleep, impaired concentration, weakness, and fatigue. Although largely absent from the history of post–intensive care syndrome to date, consideration is needed of how common chronic medical conditions such as diabetes, heart failure, and chronic pulmonary disease contribute to the morbidity of survivors of critical illness."
Dr. Prescott is a clinical fellow and Dr. Iwashyna is an assistant professor of internal medicine with the University of Michigan, Ann Arbor. They reported receiving grant support from the National Institutes of Health and the Department of Veterans Affairs. These remarks were taken from their editorial accompanying Dr. Jackson’s report (Lancet 2014 [doi:10.1016/S2213-2600(14)70071-2]).
Patients discharged from intensive care units were far more likely to report physical symptoms of depression than posttraumatic distress disorder symptoms, based on research published online April 6 in Lancet Respiratory Medicine.
"Depression and posttraumatic distress disorder are important mental health problems after critical illness, but our findings show that depression is at least five times more common than posttraumatic distress disorder and is largely somatic in nature," said James C. Jackson, Psy.D., at Vanderbilt University in Nashville, Tenn., and his associates. "This finding suggests that physical disability contributes predominantly to this depression, which has implications for the roles of physical rehabilitation vs. antidepressant medications in the prevention and management of depression after ICU admission." Lancet
Respir. Med. 2014 March 6 [doi: 10.1016/S2213-2600(14)70051-7]
The prospective, multicenter longitudinal cohort study enrolled 821 patients (median age, 61 years) treated in medical and surgical ICUs for respiratory failure, cardiogenic shock, or septic shock.
Data were available for 406 patients 3 months after discharge, of which 37% reported at least mild depression symptoms, while only 7% reported posttraumatic stress disorder (PTSD) symptoms. At 12 months after discharge, 33% of patients reported depression, compared with 7% for PTSD. Depression was primarily somatic in nature and was common even among patients with no past history of the disorder (prevalence, 30% and 29% at 3 and 12 months, respectively). Disabilities in activities of daily living affected from 23%-32% of patients.
"Our data further show that monitoring these outcomes is relevant for survivors of all ages, and that non–pharmacological interventions during the ICU stay (previously assumed to improve physical outcomes in ICU survivors) should be tested in terms of their ability to change mental health and functional outcomes," the investigators concluded.
Dr. Jackson receives grant support from the National Institutes of Health. Ten of his associates reported receiving funding, honoraria, and other support from Hospira; Abbott; Orion Pharma; the Veterans Affairs Clinical Science Research and Development Service; the Tennessee Valley Geriatric Research, Education, and Clinical Center; the National Institutes of Health; and the Vanderbilt Clinical and Translational Research Scholars Program.
Patients discharged from intensive care units were far more likely to report physical symptoms of depression than posttraumatic distress disorder symptoms, based on research published online April 6 in Lancet Respiratory Medicine.
"Depression and posttraumatic distress disorder are important mental health problems after critical illness, but our findings show that depression is at least five times more common than posttraumatic distress disorder and is largely somatic in nature," said James C. Jackson, Psy.D., at Vanderbilt University in Nashville, Tenn., and his associates. "This finding suggests that physical disability contributes predominantly to this depression, which has implications for the roles of physical rehabilitation vs. antidepressant medications in the prevention and management of depression after ICU admission." Lancet
Respir. Med. 2014 March 6 [doi: 10.1016/S2213-2600(14)70051-7]
The prospective, multicenter longitudinal cohort study enrolled 821 patients (median age, 61 years) treated in medical and surgical ICUs for respiratory failure, cardiogenic shock, or septic shock.
Data were available for 406 patients 3 months after discharge, of which 37% reported at least mild depression symptoms, while only 7% reported posttraumatic stress disorder (PTSD) symptoms. At 12 months after discharge, 33% of patients reported depression, compared with 7% for PTSD. Depression was primarily somatic in nature and was common even among patients with no past history of the disorder (prevalence, 30% and 29% at 3 and 12 months, respectively). Disabilities in activities of daily living affected from 23%-32% of patients.
"Our data further show that monitoring these outcomes is relevant for survivors of all ages, and that non–pharmacological interventions during the ICU stay (previously assumed to improve physical outcomes in ICU survivors) should be tested in terms of their ability to change mental health and functional outcomes," the investigators concluded.
Dr. Jackson receives grant support from the National Institutes of Health. Ten of his associates reported receiving funding, honoraria, and other support from Hospira; Abbott; Orion Pharma; the Veterans Affairs Clinical Science Research and Development Service; the Tennessee Valley Geriatric Research, Education, and Clinical Center; the National Institutes of Health; and the Vanderbilt Clinical and Translational Research Scholars Program.
FROM THE LANCET
Major finding: At 3 months and 12 months after discharge, 37% and 33% of patients reported at least mild depression while only 7% reported symptoms of posttraumatic stress disorder.
Data source: Prospective, multicenter longitudinal cohort study of 821 patients with respiratory failure or shock treated in ICUs, with 448 assessed at 3 months and 382 assessed at 12 months.
Disclosures: Dr. Jackson receives grant support from the National Institutes of Health. Ten of his associates reported receiving funding, honoraria, and other support from Hospira; Abbott; Orion Pharma; the Veterans Affairs Clinical Science Research and Development Service; the Tennessee Valley Geriatric Research, Education, and Clinical Center; the National Institutes of Health; and the Vanderbilt Clinical and Translational Research Scholars Program.
One in four patients with hypertension nonadherent to therapy
Urine testing of patients with hypertension revealed that 25% were partially or totally nonadherent to treatment, researchers reported online April 3 in the journal Heart.
Furthermore, nonadherence was linearly related to increased systolic and diastolic blood pressures during clinic visits and 24-hour mean daytime diastolic blood pressure (P < .006 for all), reported Dr. Maciej Tomaszewski of the University of Leicester, England, and his associates.
Using a urine test available to commercial labs, the investigators tested 208 patients for 40 of the most common antihypertensive medications and their metabolites by performing high-performance liquid chromatography–tandem mass spectrometry of spot urine samples. Patients were either newly referred (n = 125), followed up for inadequately controlled blood pressure (66), or referred for renal denervation (17), the investigators reported (Heart 2014 April 3 [doi: 10.1136/heartjnl-2013-305063]).
Nonadherence was particularly common among patients whose hypertension was inadequately controlled (28.8%) or who were referred for renal denervation (23.5%), the investigators said. Without routine urine screening, nonadherent patients might receive or undergo unnecessary tests, procedures, or treatments for perceived nonresponse to treatment, said Dr. Tomaszewski, who is also with the National Institute for Health Research (NIHR) Leicester Biomedical Research Unit in Cardiovascular Disease, and his colleagues.
Larger, multicenter studies should directly estimate biochemical nonadherence in other populations and assess the cost-effectiveness of screening for nonadherence compared with the overall cost of managing resistant hypertension, the investigators said.
Dr. Tomaszewski and five of his associates reported receiving research and other support from the British Heart Foundation and the NIHR.
"A contentious question has been whether resistant hypertension is a pathogenetic subset of hypertension, justifying a search for ‘stratified medicines’; or is it an imaginary condition caused by doctors in white coats and patients who do not take their tablets?" commented Dr. Morris J. Brown.
"On the one hand, there is abundant evidence that primary aldosteronism causes 20%-25% of true treatment resistance," he added. But Tomaszewski et al. show that nonadherent patients "account for an almost identical, high proportion of supposed resistant hypertension. Furthermore, the authors answer not only the question ‘Is my patient taking his/her tablets,’ but also ‘How can I simply and cheaply find out?’ "
The authors "deftly side-stepped" questions related to the ethics of the test and what to do about the findings, said Dr. Brown. "Neither completion nor assent to urine testing could be compulsory," he emphasized. "But then, nor is progression to expensive tests for benign, curable causes of resistant hypertension – without resistance to treatment being first demonstrated."
Dr. Brown is a professor of clinical pharmacology at the University of Cambridge, England. He reported that he had no conflicts of interest. These remarks were taken from his editorial accompanying Dr. Tomaszewski’s report (Heart 2014 April 3 [doi: 10.1136/heartjnl-2013-305063]).
"A contentious question has been whether resistant hypertension is a pathogenetic subset of hypertension, justifying a search for ‘stratified medicines’; or is it an imaginary condition caused by doctors in white coats and patients who do not take their tablets?" commented Dr. Morris J. Brown.
"On the one hand, there is abundant evidence that primary aldosteronism causes 20%-25% of true treatment resistance," he added. But Tomaszewski et al. show that nonadherent patients "account for an almost identical, high proportion of supposed resistant hypertension. Furthermore, the authors answer not only the question ‘Is my patient taking his/her tablets,’ but also ‘How can I simply and cheaply find out?’ "
The authors "deftly side-stepped" questions related to the ethics of the test and what to do about the findings, said Dr. Brown. "Neither completion nor assent to urine testing could be compulsory," he emphasized. "But then, nor is progression to expensive tests for benign, curable causes of resistant hypertension – without resistance to treatment being first demonstrated."
Dr. Brown is a professor of clinical pharmacology at the University of Cambridge, England. He reported that he had no conflicts of interest. These remarks were taken from his editorial accompanying Dr. Tomaszewski’s report (Heart 2014 April 3 [doi: 10.1136/heartjnl-2013-305063]).
"A contentious question has been whether resistant hypertension is a pathogenetic subset of hypertension, justifying a search for ‘stratified medicines’; or is it an imaginary condition caused by doctors in white coats and patients who do not take their tablets?" commented Dr. Morris J. Brown.
"On the one hand, there is abundant evidence that primary aldosteronism causes 20%-25% of true treatment resistance," he added. But Tomaszewski et al. show that nonadherent patients "account for an almost identical, high proportion of supposed resistant hypertension. Furthermore, the authors answer not only the question ‘Is my patient taking his/her tablets,’ but also ‘How can I simply and cheaply find out?’ "
The authors "deftly side-stepped" questions related to the ethics of the test and what to do about the findings, said Dr. Brown. "Neither completion nor assent to urine testing could be compulsory," he emphasized. "But then, nor is progression to expensive tests for benign, curable causes of resistant hypertension – without resistance to treatment being first demonstrated."
Dr. Brown is a professor of clinical pharmacology at the University of Cambridge, England. He reported that he had no conflicts of interest. These remarks were taken from his editorial accompanying Dr. Tomaszewski’s report (Heart 2014 April 3 [doi: 10.1136/heartjnl-2013-305063]).
Urine testing of patients with hypertension revealed that 25% were partially or totally nonadherent to treatment, researchers reported online April 3 in the journal Heart.
Furthermore, nonadherence was linearly related to increased systolic and diastolic blood pressures during clinic visits and 24-hour mean daytime diastolic blood pressure (P < .006 for all), reported Dr. Maciej Tomaszewski of the University of Leicester, England, and his associates.
Using a urine test available to commercial labs, the investigators tested 208 patients for 40 of the most common antihypertensive medications and their metabolites by performing high-performance liquid chromatography–tandem mass spectrometry of spot urine samples. Patients were either newly referred (n = 125), followed up for inadequately controlled blood pressure (66), or referred for renal denervation (17), the investigators reported (Heart 2014 April 3 [doi: 10.1136/heartjnl-2013-305063]).
Nonadherence was particularly common among patients whose hypertension was inadequately controlled (28.8%) or who were referred for renal denervation (23.5%), the investigators said. Without routine urine screening, nonadherent patients might receive or undergo unnecessary tests, procedures, or treatments for perceived nonresponse to treatment, said Dr. Tomaszewski, who is also with the National Institute for Health Research (NIHR) Leicester Biomedical Research Unit in Cardiovascular Disease, and his colleagues.
Larger, multicenter studies should directly estimate biochemical nonadherence in other populations and assess the cost-effectiveness of screening for nonadherence compared with the overall cost of managing resistant hypertension, the investigators said.
Dr. Tomaszewski and five of his associates reported receiving research and other support from the British Heart Foundation and the NIHR.
Urine testing of patients with hypertension revealed that 25% were partially or totally nonadherent to treatment, researchers reported online April 3 in the journal Heart.
Furthermore, nonadherence was linearly related to increased systolic and diastolic blood pressures during clinic visits and 24-hour mean daytime diastolic blood pressure (P < .006 for all), reported Dr. Maciej Tomaszewski of the University of Leicester, England, and his associates.
Using a urine test available to commercial labs, the investigators tested 208 patients for 40 of the most common antihypertensive medications and their metabolites by performing high-performance liquid chromatography–tandem mass spectrometry of spot urine samples. Patients were either newly referred (n = 125), followed up for inadequately controlled blood pressure (66), or referred for renal denervation (17), the investigators reported (Heart 2014 April 3 [doi: 10.1136/heartjnl-2013-305063]).
Nonadherence was particularly common among patients whose hypertension was inadequately controlled (28.8%) or who were referred for renal denervation (23.5%), the investigators said. Without routine urine screening, nonadherent patients might receive or undergo unnecessary tests, procedures, or treatments for perceived nonresponse to treatment, said Dr. Tomaszewski, who is also with the National Institute for Health Research (NIHR) Leicester Biomedical Research Unit in Cardiovascular Disease, and his colleagues.
Larger, multicenter studies should directly estimate biochemical nonadherence in other populations and assess the cost-effectiveness of screening for nonadherence compared with the overall cost of managing resistant hypertension, the investigators said.
Dr. Tomaszewski and five of his associates reported receiving research and other support from the British Heart Foundation and the NIHR.
FROM HEART
Major finding: A urine test available to commercial labs showed that 25% of patients were totally (10.1%) or partially (14.9%) nonadherent to treatment. Nonadherence was linearly associated with increased clinic systolic blood pressure, clinic diastolic blood pressure, and 24-hour mean daytime diastolic blood pressure (P < .006 for all).
Data source: High-performance liquid chromatography–tandem mass spectrometry urine screening and blood pressure measurements in 208 patients with hypertension.
Disclosures: The authors reported receiving research and other support from the British Heart Foundation and the National Institute for Health Research.
Childhood Atopic Dermatitis Persists Into Adolescence and Beyond
Contrary to conventional wisdom, atopic dermatitis persists well into the second decade of life and probably longer, based on data from a prospective longitudinal study published online April 3 in JAMA Dermatology.
At every age studied (2-26 years), more than 80% of patients reported having symptoms of atopic dermatitis (AD) or taking AD medication in the past 6 months, reported Dr. David J. Margolis and his associates at the University of Pennsylvania, Philadelphia.
"Past teaching that nearly 50%-70% of children with AD will achieve a resolution of their AD by age 12 years was not achieved in our study," the researchers said (JAMA Dermatol. 2014 April 3 [doi:10.1001/ jamadermatol.2013.10271]).
The study enrolled 7,157 children aged 2-17 years who had physician-diagnosed mild to moderate AD. In a Kaplan-Meier survival estimate of 2,416 patients followed for at least 5 years, only by age 20 years did 50% of patients report at least 6 months free of AD symptoms or medications.
The findings are consistent with recent data suggesting that AD or eczema affects similar proportions of children and adults in the United States, the researchers said.
The study was funded by the National Institute of Arthritis and Musculoskeletal and Skin Diseases and by Valeant Pharmaceuticals, maker of the atopic dermatitis drug pimecrolimus. The authors reported no individual conflicts of interest.
The findings "challenge the conventional dogma that most childhood AD ‘burns out’ and dissipates by late adolescence and adulthood," said Dr. Jonathan I. Silverberg.
"It seems that children with eczema do not really outgrow their eczema," he said. "Rather, eczema seems to be a lifelong disease with a variable phenotype and/or reduced expression in adulthood."
Adult eczema’s diverse symptoms could have led researchers to underestimate its prevalence, said Dr. Silverberg, adding that many clinical studies of the disease defined cases based on classical criteria, such as flexural eczema. "Thus, the use of self-reported outcomes may be more sensitive and actually better suited for some studies of adult eczema."
The current study’s response rate of 70% is considered very good for mail-based surveys, he said. He noted that participants were geographically diverse, even though the study did not use random, population-based sampling.
Dr. Silverberg is a dermatologist at Northwestern University, Chicago. He reported that he has no financial conflicts of interest. These remarks were taken from his editorial accompanying Dr. Margolis’s report (JAMA Dermatol. 2014 April 3 [doi:10.1001/jamadermatol.2013.10267]).
The findings "challenge the conventional dogma that most childhood AD ‘burns out’ and dissipates by late adolescence and adulthood," said Dr. Jonathan I. Silverberg.
"It seems that children with eczema do not really outgrow their eczema," he said. "Rather, eczema seems to be a lifelong disease with a variable phenotype and/or reduced expression in adulthood."
Adult eczema’s diverse symptoms could have led researchers to underestimate its prevalence, said Dr. Silverberg, adding that many clinical studies of the disease defined cases based on classical criteria, such as flexural eczema. "Thus, the use of self-reported outcomes may be more sensitive and actually better suited for some studies of adult eczema."
The current study’s response rate of 70% is considered very good for mail-based surveys, he said. He noted that participants were geographically diverse, even though the study did not use random, population-based sampling.
Dr. Silverberg is a dermatologist at Northwestern University, Chicago. He reported that he has no financial conflicts of interest. These remarks were taken from his editorial accompanying Dr. Margolis’s report (JAMA Dermatol. 2014 April 3 [doi:10.1001/jamadermatol.2013.10267]).
The findings "challenge the conventional dogma that most childhood AD ‘burns out’ and dissipates by late adolescence and adulthood," said Dr. Jonathan I. Silverberg.
"It seems that children with eczema do not really outgrow their eczema," he said. "Rather, eczema seems to be a lifelong disease with a variable phenotype and/or reduced expression in adulthood."
Adult eczema’s diverse symptoms could have led researchers to underestimate its prevalence, said Dr. Silverberg, adding that many clinical studies of the disease defined cases based on classical criteria, such as flexural eczema. "Thus, the use of self-reported outcomes may be more sensitive and actually better suited for some studies of adult eczema."
The current study’s response rate of 70% is considered very good for mail-based surveys, he said. He noted that participants were geographically diverse, even though the study did not use random, population-based sampling.
Dr. Silverberg is a dermatologist at Northwestern University, Chicago. He reported that he has no financial conflicts of interest. These remarks were taken from his editorial accompanying Dr. Margolis’s report (JAMA Dermatol. 2014 April 3 [doi:10.1001/jamadermatol.2013.10267]).
Contrary to conventional wisdom, atopic dermatitis persists well into the second decade of life and probably longer, based on data from a prospective longitudinal study published online April 3 in JAMA Dermatology.
At every age studied (2-26 years), more than 80% of patients reported having symptoms of atopic dermatitis (AD) or taking AD medication in the past 6 months, reported Dr. David J. Margolis and his associates at the University of Pennsylvania, Philadelphia.
"Past teaching that nearly 50%-70% of children with AD will achieve a resolution of their AD by age 12 years was not achieved in our study," the researchers said (JAMA Dermatol. 2014 April 3 [doi:10.1001/ jamadermatol.2013.10271]).
The study enrolled 7,157 children aged 2-17 years who had physician-diagnosed mild to moderate AD. In a Kaplan-Meier survival estimate of 2,416 patients followed for at least 5 years, only by age 20 years did 50% of patients report at least 6 months free of AD symptoms or medications.
The findings are consistent with recent data suggesting that AD or eczema affects similar proportions of children and adults in the United States, the researchers said.
The study was funded by the National Institute of Arthritis and Musculoskeletal and Skin Diseases and by Valeant Pharmaceuticals, maker of the atopic dermatitis drug pimecrolimus. The authors reported no individual conflicts of interest.
Contrary to conventional wisdom, atopic dermatitis persists well into the second decade of life and probably longer, based on data from a prospective longitudinal study published online April 3 in JAMA Dermatology.
At every age studied (2-26 years), more than 80% of patients reported having symptoms of atopic dermatitis (AD) or taking AD medication in the past 6 months, reported Dr. David J. Margolis and his associates at the University of Pennsylvania, Philadelphia.
"Past teaching that nearly 50%-70% of children with AD will achieve a resolution of their AD by age 12 years was not achieved in our study," the researchers said (JAMA Dermatol. 2014 April 3 [doi:10.1001/ jamadermatol.2013.10271]).
The study enrolled 7,157 children aged 2-17 years who had physician-diagnosed mild to moderate AD. In a Kaplan-Meier survival estimate of 2,416 patients followed for at least 5 years, only by age 20 years did 50% of patients report at least 6 months free of AD symptoms or medications.
The findings are consistent with recent data suggesting that AD or eczema affects similar proportions of children and adults in the United States, the researchers said.
The study was funded by the National Institute of Arthritis and Musculoskeletal and Skin Diseases and by Valeant Pharmaceuticals, maker of the atopic dermatitis drug pimecrolimus. The authors reported no individual conflicts of interest.
FROM JAMA DERMATOLOGY
Childhood atopic dermatitis persists into adolescence and beyond
Contrary to conventional wisdom, atopic dermatitis persists well into the second decade of life and probably longer, based on data from a prospective longitudinal study published online April 3 in JAMA Dermatology.
At every age studied (2-26 years), more than 80% of patients reported having symptoms of atopic dermatitis (AD) or taking AD medication in the past 6 months, reported Dr. David J. Margolis and his associates at the University of Pennsylvania, Philadelphia.
"Past teaching that nearly 50%-70% of children with AD will achieve a resolution of their AD by age 12 years was not achieved in our study," the researchers said (JAMA Dermatol. 2014 April 3 [doi:10.1001/ jamadermatol.2013.10271]).
The study enrolled 7,157 children aged 2-17 years who had physician-diagnosed mild to moderate AD. In a Kaplan-Meier survival estimate of 2,416 patients followed for at least 5 years, only by age 20 years did 50% of patients report at least 6 months free of AD symptoms or medications.
The findings are consistent with recent data suggesting that AD or eczema affects similar proportions of children and adults in the United States, the researchers said.
The study was funded by the National Institute of Arthritis and Musculoskeletal and Skin Diseases and by Valeant Pharmaceuticals, maker of the atopic dermatitis drug pimecrolimus. The authors reported no individual conflicts of interest.
The findings "challenge the conventional dogma that most childhood AD ‘burns out’ and dissipates by late adolescence and adulthood," said Dr. Jonathan I. Silverberg.
"It seems that children with eczema do not really outgrow their eczema," he said. "Rather, eczema seems to be a lifelong disease with a variable phenotype and/or reduced expression in adulthood."
Adult eczema’s diverse symptoms could have led researchers to underestimate its prevalence, said Dr. Silverberg, adding that many clinical studies of the disease defined cases based on classical criteria, such as flexural eczema. "Thus, the use of self-reported outcomes may be more sensitive and actually better suited for some studies of adult eczema."
The current study’s response rate of 70% is considered very good for mail-based surveys, he said. He noted that participants were geographically diverse, even though the study did not use random, population-based sampling.
Dr. Silverberg is a dermatologist at Northwestern University, Chicago. He reported that he has no financial conflicts of interest. These remarks were taken from his editorial accompanying Dr. Margolis’s report (JAMA Dermatol. 2014 April 3 [doi:10.1001/jamadermatol.2013.10267]).
The findings "challenge the conventional dogma that most childhood AD ‘burns out’ and dissipates by late adolescence and adulthood," said Dr. Jonathan I. Silverberg.
"It seems that children with eczema do not really outgrow their eczema," he said. "Rather, eczema seems to be a lifelong disease with a variable phenotype and/or reduced expression in adulthood."
Adult eczema’s diverse symptoms could have led researchers to underestimate its prevalence, said Dr. Silverberg, adding that many clinical studies of the disease defined cases based on classical criteria, such as flexural eczema. "Thus, the use of self-reported outcomes may be more sensitive and actually better suited for some studies of adult eczema."
The current study’s response rate of 70% is considered very good for mail-based surveys, he said. He noted that participants were geographically diverse, even though the study did not use random, population-based sampling.
Dr. Silverberg is a dermatologist at Northwestern University, Chicago. He reported that he has no financial conflicts of interest. These remarks were taken from his editorial accompanying Dr. Margolis’s report (JAMA Dermatol. 2014 April 3 [doi:10.1001/jamadermatol.2013.10267]).
The findings "challenge the conventional dogma that most childhood AD ‘burns out’ and dissipates by late adolescence and adulthood," said Dr. Jonathan I. Silverberg.
"It seems that children with eczema do not really outgrow their eczema," he said. "Rather, eczema seems to be a lifelong disease with a variable phenotype and/or reduced expression in adulthood."
Adult eczema’s diverse symptoms could have led researchers to underestimate its prevalence, said Dr. Silverberg, adding that many clinical studies of the disease defined cases based on classical criteria, such as flexural eczema. "Thus, the use of self-reported outcomes may be more sensitive and actually better suited for some studies of adult eczema."
The current study’s response rate of 70% is considered very good for mail-based surveys, he said. He noted that participants were geographically diverse, even though the study did not use random, population-based sampling.
Dr. Silverberg is a dermatologist at Northwestern University, Chicago. He reported that he has no financial conflicts of interest. These remarks were taken from his editorial accompanying Dr. Margolis’s report (JAMA Dermatol. 2014 April 3 [doi:10.1001/jamadermatol.2013.10267]).
Contrary to conventional wisdom, atopic dermatitis persists well into the second decade of life and probably longer, based on data from a prospective longitudinal study published online April 3 in JAMA Dermatology.
At every age studied (2-26 years), more than 80% of patients reported having symptoms of atopic dermatitis (AD) or taking AD medication in the past 6 months, reported Dr. David J. Margolis and his associates at the University of Pennsylvania, Philadelphia.
"Past teaching that nearly 50%-70% of children with AD will achieve a resolution of their AD by age 12 years was not achieved in our study," the researchers said (JAMA Dermatol. 2014 April 3 [doi:10.1001/ jamadermatol.2013.10271]).
The study enrolled 7,157 children aged 2-17 years who had physician-diagnosed mild to moderate AD. In a Kaplan-Meier survival estimate of 2,416 patients followed for at least 5 years, only by age 20 years did 50% of patients report at least 6 months free of AD symptoms or medications.
The findings are consistent with recent data suggesting that AD or eczema affects similar proportions of children and adults in the United States, the researchers said.
The study was funded by the National Institute of Arthritis and Musculoskeletal and Skin Diseases and by Valeant Pharmaceuticals, maker of the atopic dermatitis drug pimecrolimus. The authors reported no individual conflicts of interest.
Contrary to conventional wisdom, atopic dermatitis persists well into the second decade of life and probably longer, based on data from a prospective longitudinal study published online April 3 in JAMA Dermatology.
At every age studied (2-26 years), more than 80% of patients reported having symptoms of atopic dermatitis (AD) or taking AD medication in the past 6 months, reported Dr. David J. Margolis and his associates at the University of Pennsylvania, Philadelphia.
"Past teaching that nearly 50%-70% of children with AD will achieve a resolution of their AD by age 12 years was not achieved in our study," the researchers said (JAMA Dermatol. 2014 April 3 [doi:10.1001/ jamadermatol.2013.10271]).
The study enrolled 7,157 children aged 2-17 years who had physician-diagnosed mild to moderate AD. In a Kaplan-Meier survival estimate of 2,416 patients followed for at least 5 years, only by age 20 years did 50% of patients report at least 6 months free of AD symptoms or medications.
The findings are consistent with recent data suggesting that AD or eczema affects similar proportions of children and adults in the United States, the researchers said.
The study was funded by the National Institute of Arthritis and Musculoskeletal and Skin Diseases and by Valeant Pharmaceuticals, maker of the atopic dermatitis drug pimecrolimus. The authors reported no individual conflicts of interest.
FROM JAMA DERMATOLOGY
Major finding: At every age studied (2-26 years), more than 80% of participants had experienced symptoms of atopic dermatitis or had used atopic dermatitis medication in the past 6 months.
Data source: A prospective longitudinal cohort study of 7,157 patients with atopic dermatitis who were aged 2-17 years at enrollment.
Disclosures: The study was funded by the National Institute of Arthritis and Musculoskeletal and Skin Diseases and by Valeant Pharmaceuticals, maker of the atopic dermatitis drug pimecrolimus. The authors reported no individual conflicts of interest.