User login
Patients with needle phobia? Try stress-reducing medical devices
- Adding decorative designs or stickers to medical devices before a procedure significantly reduces aversion, fear, and anxiety, and may be especially useful for needle-phobic patients (A).
Needle phobia—fear of needles, syringes, intravenous therapy, and medical devices—can seriously compromise medical care.1-7 We hypothesized that a novel cognitive therapy consisting of simple designs and decorations on needles and other medical devices would reduce needle phobia. Fear, aversion, and anxiety decreased significantly—as measured by validated visual analogue reaction scales—when patients were exposed to decorated devices.
Materials and methods
Subjects
This was a randomized controlled trial approved by the Institutional Review Board (IRB). Sixty patients were recruited from outpatient clinics: 67% female, 33% male, 100% outpatients, 41% pediatric patients, and 59% adults—representing the typical mix of subjects in a family practice clinic. The mean age of the patients was 32±21 years (range, 3 years to 65 years).
After informed consent, the subjects were randomly exposed to 8 different designs of winged needles and 6 different designs of syringes fitted with a needle. Smaller subsets of subjects were exposed to different designs of intravenous (IV) bags and scalpels.
Stress-reducing needles and syringes
Stress-reducing syringes were created by taking conventional 10-mL syringes (10-mL Luer-Lok BD syringe, ref 309604, Becton Dickinson, Franklin Lakes, NJ) and decorating them so that the markings of the barrel could still be seen (FIGURE 1). Stress-reducing winged catheters (21 G 3/4×12-inch 367281 Vacutainer brand Safety-Lok Blood Collection Set; Becton Dickinson, Franklin Lakes, NJ) were created by decorating the wings in a symmetrical manner (FIGURE 2). Similarly, different designs of IV bag (FIGURE 3) and scalpel were used.
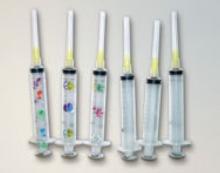
FIGURE 1
Stress-reducing syringes
Stress-reducing syringes (compared with 3 typical conventional syringes at right) yielded a mean 79% decrease in aversion scores, 53% decrease in fear scores, and 51% decrease in anxiety scores. Musical notes were the most favored design (P<.001).
FIGURE 2
Stress-reducing butterfly needles
Stress-reducing butterfly needles (compared with 4 typical designs at bottom) reduced aversion by 68%, fear by 53%, and anxiety by 53% (P<.001).
FIGURE 3
Stress-reducing IV bags
Stress-reducing intravenous bags reduced aversion by 83%, fear by 53%, and anxiety by 73% (P<.001).
Outcome measures
For each group of devices, the presentation of individual devices to each subject was randomized to eliminate the possibility of a consistent bias. Emotional responses to the medical devices were determined with the validated visual analogue reaction scales where 0 is lowest response and 10 is the strongest.8-11 These included the Visual Analogue Anxiety Scale (VAAS), Visual Analogue Fear Scale (VAFS), and Visual Analogue Aversion Scale (VAS). Significant needle phobia was defined as an aversion, fear, or anxiety score of greater than or equal to 5.
Statistical analysis
Primary analyses consisted of comparing the responses to the stress-reducing devices as a class with the conventional devices as a class. These paired data were compared with the paired 2-tailed t-test. To determine whether these responses were class-specific or design-specific, the results for each individual device were then compared with a matched control, design by design, again with the paired 2-tailed t-test. Corrections were made for multiple comparisons.
Results
Patients experienced markedly more aversion to (dislike of) conventional syringes (VAAS score: 5.88±3.61 vs stress-reducing syringes VAAS score: 1.21±1.64; P<.001); they also had greater fear (conventional VAFS score: 4.68±2.8 vs stress-reducing VAFS score: 2.19±2.8, P<.001) and anxiety (conventional VAS score: 4.54±3.68 vs stress-reducing VAS score: 2.21±2.84, P<.001) (TABLE). This corresponds to a mean 79% decrease in aversion scores, 53% reduction in fear scores, and 51% decrease in anxiety scores with the stress-reducing syringes. Ninety-five percent of subjects preferred the stress-reducing syringes to the conventional syringes; 98% of subjects felt that stress-reducing syringes should be available for children; 72% felt that the stress-reducing syringes should also be available for adults.
The syringes most favored were those with musical notes (56%), flowers (18%), and smiley faces (12%). Each of these designs had lower scores in the 3 domains (fear, aversion, and anxiety) compared with the conventional device (P<.01), indicating that the reduction in stress measures was a class effect, rather than a specific effect of the individual design.
Significant needle phobia is defined as aversion, fear, or anxiety scores ≥5. Using this definition, 80% of subjects experienced moderate to severe aversion, 63% suffered moderate to severe fear, and 62% experienced moderate to severe anxiety on exposure to conventional syringes. This corresponded to mean aversion, fear, and anxiety scores of 7.18±1.92, 6.98±2.16, and 6.78±2.44, respectively. In subjects with significant needle phobia, stress-reducing syringes reduced aversion scores by 81% (P<.001), fear scores by 56% (P<.001), and anxiety by 47% (P<.001). Stress-reducing syringes had a positive response rate of 98% for reducing aversion, 87% in reducing fear, and 74% in reducing anxiety.
Stress-reducing butterfly needles reduced aversion by 68%, fear by 53%, and anxiety by 53% (P<.001). The stress-reducing designs most favored were butterfly designs, flowers, fish, and smiley faces. Stress-reducing IV bags significantly reduced aversion by 83%, fear by 53%, and anxiety by 73% (P<.001). Stress-reducing scalpels also significantly reduced aversion by 49%, fear by 36%, and anxiety by 37% (P<.001).
When analyzed separately, both children and adults responded favorably and similarly to the stress-reducing devices in all 3 domains (P<.01), although children had a higher mean stress level in all 3 domains to conventional devices (P<.05).
TABLE
Significant reductions in aversion, fear, and anxiety with stress-reducing syringes
| 60 SUBJECTS’ EXPERIENCES | CONVENTIONAL SYRINGES | STRESS-REDUCING SYRINGES | P VALUE | % DECREASE IN SCORE |
|---|---|---|---|---|
| Aversion | 5.88±3.61 | 1.21±1.64 | P<.001 | 79% |
| Fear | 4.68±2.8 | 2.19±2.8 | P<.001 | 53% |
| Anxiety | 4.54±3.68 | 2.21±2.84 | P<.001 | 51% |
| Most liked | 5% | 95% | P<.001 | |
| Most disliked | 95% | 5% | P<.001 |
Discussion
A fear of needles, syringe procedures, intravenous therapy, and medical devices is given the overall term of needle phobia, and can seriously compromise patient care.1-7 Adults may express needle phobia verbally or even avoid coming to the physician’s office, while children may be more overtly fearful, anxious, or hysterical. Our study focused on the specific psychological components of stress—aversion, fear, and anxiety—induced by exposure to needles and medical devices.
Aversion, fear, and anxiety were each assessed with the relevant VAS, a reproducible and validated method for assessing stress components in clinical populations.8-11 Using a conservative definition for moderate to severe stress (VAS ≥5), 80% of subjects experienced moderate to severe aversion, 63% suffered moderate to severe fear, and 62% experienced moderate to severe anxiety in response to conventional devices. Thus, significant levels of clinically relevant needle phobia are present in typical outpatient populations. Several approaches have been taken to prevent and treat needle phobia, including reassurance, education, avoidance of needles, postural and muscle tension techniques, benzodiazepines, nitrous oxide gas, topical anesthesia, cognitive therapy, participant modeling, distraction, meditation, hypnosis, and coaching—all with variable and inconsistent results.1-7,12-18
We hypothesized that visual modifications to needles, syringes, and other medical devices would result in stress-reducing devices that would lessen patient needle phobia. The stress-reducing needles and medical devices were created by applying simple representative designs on winged needles, syringes, IV bags, and scalpels while maintaining the basic function of these devices (FIGURES 1-3).
Stress-reducing syringes resulted in a 79% decrease in aversion, 53% reduction in fear, and 51% decrease in anxiety in the overall patient population compared to the conventional syringes (P<.001). More importantly, in subjects with significant needle phobia (VAS scores ≥5), stress-reducing syringes reduced aversion by 81%, fear by 56%, and anxiety by 47% (P<.001). This corresponds to favorable responses of 98% for aversion, 87% for fear, and 74% in anxiety in subjects with needle phobia. Similarly, stress-reducing winged needles, IV bags, and scalps in needle-phobic individuals demonstrated significantly positive response rates for reducing aversion, fear, and anxiety. For the stress-reducing devices, each individual design was superior to the corresponding conventional device, indicating a dominant class effect of these stress-reducing medical devices, rather than the specific design.
Damping visual cues of threat
It is likely that decoration of a medical device actually is a neurophysiologic intervention, resulting in stimulation of brain areas not usually associated with the fear, anxiety, and aversion responses caused by viewing medical devices. In this sense, the intervention of decorating a medical device has a close parallel to other cognitive, distraction, and mind-body imagery methods of intervention.1-7,12-18
However, unlike these other interventions, decoration of the medical device actually focuses the patient’s attention and interest on the medical device, yet fear, aversion, and anxiety of needles and syringes are still significantly reduced. This suggests that the decorations interfere with the established link between visual recognition of a perceived threat and the subsequent emotional response to that perceived threat. In the future, neuroimaging of brain activation in response to these decorated devices may provide a more telling explanation of their stress-reducing effects.
This study demonstrates unexpectedly high levels of stress and fear of medical devices in typical clinic patients, and significant reduction of these stress measures by the use of stress-reducing decorated medical devices. The most favorable implementation of this technology would be for these stress-reducing medical devices to be mass-produced and the decorations placed on the device at the factory rather at the site of service. Ultimate implementation of this technology will determined primarily by economic considerations and the acceptance of these aesthetic modifications by nursing, physician, and administrative staff in family practice units.
CORRESPONDENCE
Wilmer L. Sibbitt, Jr, MD, Department of Internal Medicine, 5th floor ACC, University of New Mexico Health Sciences Center, Albuquerque, NM 87131. E-mail: wsibbitt@salud.unm.edu
1. Fassler D. The fear of needles in children. Am J Orthopsychiatry 1985;55:371-377.
2. Hamilton JG. Needle phobia: a neglected diagnosis. J Fam Pract 1995;41:169-175.
3. McSherry J. Perspectives on needle phobia. J Fam Pract 1995;41:437,512.-
4. Daniels AJ. Perspectives on needle phobia. J Fam Pract 1995;41:437.-
5. Stark MM, Brener N. Needle phobia. J Clin Forensic Med 2000;7:35-8.
6. Smalley A. Needle phobia. Paediatr Nurs 1999;11:17-20.
7. Hedstrom M, Haglund K, Skolin I, von Essen L. Distressing events for children and adolescents with cancer: child, parent, and nurse perceptions. J Pediatr Oncol Nurs 2003;20:120-132.
8. Ferguson JM, Taylor CB, Wermuth B. A rapid behavioral treatment for needle phobics. J Nerv Ment Dis 1978;166:294-298.
9. Ferguson JM, Wermuth BM, Taylor CB. Rapid desensitization of a needle phobia by participant modeling. West J Med 1976;124:174-176.
10. Mumford O. Patient tips from industry. Coping with needle phobia Diabetes Educ 2004;30:174.-
11. Koppel SM, Thapar A. Treating blood needle phobia. Hosp Med 1998;59:730-732.
12. Dahlquist LM, Busby SM, Slifer KJ, et al. Distraction for children of different ages who undergo repeated needle sticks. J Pediatr Oncol Nurs 2002;19:22-34.
13. Speirs AF, Taylor KH, Joanes DN, Girdler NM. A randomised, double-blind, placebo-controlled, comparative study of topical skin analgesics and the anxiety and discomfort associated with venous cannulation. Br Dent J 2001;190:444-449.
14. Kleiber C, Craft-Rosenberg M, Harper DC. Parents as distraction coaches during i.v. insertion: a randomized study. J Pain Symptom Manage 2001;22:851-861.
15. Bhachu HS, Kay B, Healy TE, Beatty P. Grading of pain and anxiety. Comparison between a linear analogue and a computerised audiovisual analogue scale. Anaesthesia 1983;38:875-878.
16. Miller MD, Ferris DG. Measurement of subjective phenomena in primary care research: the Visual Analogue Scale. Fam Pract Res J 1993;13:15-24.
17. Salomon JA, Murray CJ. A multi-method approach to measuring health-state valuations. Health Econ 2004;13:281-290.
18. Chapman HR, Kirby-Turner N. Visual/verbal analogue scales: examples of brief assessment methods to aid management of child and adult patients in clinical practice. Br Dent J 2002;193:447-450.
- Adding decorative designs or stickers to medical devices before a procedure significantly reduces aversion, fear, and anxiety, and may be especially useful for needle-phobic patients (A).
Needle phobia—fear of needles, syringes, intravenous therapy, and medical devices—can seriously compromise medical care.1-7 We hypothesized that a novel cognitive therapy consisting of simple designs and decorations on needles and other medical devices would reduce needle phobia. Fear, aversion, and anxiety decreased significantly—as measured by validated visual analogue reaction scales—when patients were exposed to decorated devices.
Materials and methods
Subjects
This was a randomized controlled trial approved by the Institutional Review Board (IRB). Sixty patients were recruited from outpatient clinics: 67% female, 33% male, 100% outpatients, 41% pediatric patients, and 59% adults—representing the typical mix of subjects in a family practice clinic. The mean age of the patients was 32±21 years (range, 3 years to 65 years).
After informed consent, the subjects were randomly exposed to 8 different designs of winged needles and 6 different designs of syringes fitted with a needle. Smaller subsets of subjects were exposed to different designs of intravenous (IV) bags and scalpels.
Stress-reducing needles and syringes
Stress-reducing syringes were created by taking conventional 10-mL syringes (10-mL Luer-Lok BD syringe, ref 309604, Becton Dickinson, Franklin Lakes, NJ) and decorating them so that the markings of the barrel could still be seen (FIGURE 1). Stress-reducing winged catheters (21 G 3/4×12-inch 367281 Vacutainer brand Safety-Lok Blood Collection Set; Becton Dickinson, Franklin Lakes, NJ) were created by decorating the wings in a symmetrical manner (FIGURE 2). Similarly, different designs of IV bag (FIGURE 3) and scalpel were used.
FIGURE 1
Stress-reducing syringes
Stress-reducing syringes (compared with 3 typical conventional syringes at right) yielded a mean 79% decrease in aversion scores, 53% decrease in fear scores, and 51% decrease in anxiety scores. Musical notes were the most favored design (P<.001).
FIGURE 2
Stress-reducing butterfly needles
Stress-reducing butterfly needles (compared with 4 typical designs at bottom) reduced aversion by 68%, fear by 53%, and anxiety by 53% (P<.001).
FIGURE 3
Stress-reducing IV bags
Stress-reducing intravenous bags reduced aversion by 83%, fear by 53%, and anxiety by 73% (P<.001).
Outcome measures
For each group of devices, the presentation of individual devices to each subject was randomized to eliminate the possibility of a consistent bias. Emotional responses to the medical devices were determined with the validated visual analogue reaction scales where 0 is lowest response and 10 is the strongest.8-11 These included the Visual Analogue Anxiety Scale (VAAS), Visual Analogue Fear Scale (VAFS), and Visual Analogue Aversion Scale (VAS). Significant needle phobia was defined as an aversion, fear, or anxiety score of greater than or equal to 5.
Statistical analysis
Primary analyses consisted of comparing the responses to the stress-reducing devices as a class with the conventional devices as a class. These paired data were compared with the paired 2-tailed t-test. To determine whether these responses were class-specific or design-specific, the results for each individual device were then compared with a matched control, design by design, again with the paired 2-tailed t-test. Corrections were made for multiple comparisons.
Results
Patients experienced markedly more aversion to (dislike of) conventional syringes (VAAS score: 5.88±3.61 vs stress-reducing syringes VAAS score: 1.21±1.64; P<.001); they also had greater fear (conventional VAFS score: 4.68±2.8 vs stress-reducing VAFS score: 2.19±2.8, P<.001) and anxiety (conventional VAS score: 4.54±3.68 vs stress-reducing VAS score: 2.21±2.84, P<.001) (TABLE). This corresponds to a mean 79% decrease in aversion scores, 53% reduction in fear scores, and 51% decrease in anxiety scores with the stress-reducing syringes. Ninety-five percent of subjects preferred the stress-reducing syringes to the conventional syringes; 98% of subjects felt that stress-reducing syringes should be available for children; 72% felt that the stress-reducing syringes should also be available for adults.
The syringes most favored were those with musical notes (56%), flowers (18%), and smiley faces (12%). Each of these designs had lower scores in the 3 domains (fear, aversion, and anxiety) compared with the conventional device (P<.01), indicating that the reduction in stress measures was a class effect, rather than a specific effect of the individual design.
Significant needle phobia is defined as aversion, fear, or anxiety scores ≥5. Using this definition, 80% of subjects experienced moderate to severe aversion, 63% suffered moderate to severe fear, and 62% experienced moderate to severe anxiety on exposure to conventional syringes. This corresponded to mean aversion, fear, and anxiety scores of 7.18±1.92, 6.98±2.16, and 6.78±2.44, respectively. In subjects with significant needle phobia, stress-reducing syringes reduced aversion scores by 81% (P<.001), fear scores by 56% (P<.001), and anxiety by 47% (P<.001). Stress-reducing syringes had a positive response rate of 98% for reducing aversion, 87% in reducing fear, and 74% in reducing anxiety.
Stress-reducing butterfly needles reduced aversion by 68%, fear by 53%, and anxiety by 53% (P<.001). The stress-reducing designs most favored were butterfly designs, flowers, fish, and smiley faces. Stress-reducing IV bags significantly reduced aversion by 83%, fear by 53%, and anxiety by 73% (P<.001). Stress-reducing scalpels also significantly reduced aversion by 49%, fear by 36%, and anxiety by 37% (P<.001).
When analyzed separately, both children and adults responded favorably and similarly to the stress-reducing devices in all 3 domains (P<.01), although children had a higher mean stress level in all 3 domains to conventional devices (P<.05).
TABLE
Significant reductions in aversion, fear, and anxiety with stress-reducing syringes
| 60 SUBJECTS’ EXPERIENCES | CONVENTIONAL SYRINGES | STRESS-REDUCING SYRINGES | P VALUE | % DECREASE IN SCORE |
|---|---|---|---|---|
| Aversion | 5.88±3.61 | 1.21±1.64 | P<.001 | 79% |
| Fear | 4.68±2.8 | 2.19±2.8 | P<.001 | 53% |
| Anxiety | 4.54±3.68 | 2.21±2.84 | P<.001 | 51% |
| Most liked | 5% | 95% | P<.001 | |
| Most disliked | 95% | 5% | P<.001 |
Discussion
A fear of needles, syringe procedures, intravenous therapy, and medical devices is given the overall term of needle phobia, and can seriously compromise patient care.1-7 Adults may express needle phobia verbally or even avoid coming to the physician’s office, while children may be more overtly fearful, anxious, or hysterical. Our study focused on the specific psychological components of stress—aversion, fear, and anxiety—induced by exposure to needles and medical devices.
Aversion, fear, and anxiety were each assessed with the relevant VAS, a reproducible and validated method for assessing stress components in clinical populations.8-11 Using a conservative definition for moderate to severe stress (VAS ≥5), 80% of subjects experienced moderate to severe aversion, 63% suffered moderate to severe fear, and 62% experienced moderate to severe anxiety in response to conventional devices. Thus, significant levels of clinically relevant needle phobia are present in typical outpatient populations. Several approaches have been taken to prevent and treat needle phobia, including reassurance, education, avoidance of needles, postural and muscle tension techniques, benzodiazepines, nitrous oxide gas, topical anesthesia, cognitive therapy, participant modeling, distraction, meditation, hypnosis, and coaching—all with variable and inconsistent results.1-7,12-18
We hypothesized that visual modifications to needles, syringes, and other medical devices would result in stress-reducing devices that would lessen patient needle phobia. The stress-reducing needles and medical devices were created by applying simple representative designs on winged needles, syringes, IV bags, and scalpels while maintaining the basic function of these devices (FIGURES 1-3).
Stress-reducing syringes resulted in a 79% decrease in aversion, 53% reduction in fear, and 51% decrease in anxiety in the overall patient population compared to the conventional syringes (P<.001). More importantly, in subjects with significant needle phobia (VAS scores ≥5), stress-reducing syringes reduced aversion by 81%, fear by 56%, and anxiety by 47% (P<.001). This corresponds to favorable responses of 98% for aversion, 87% for fear, and 74% in anxiety in subjects with needle phobia. Similarly, stress-reducing winged needles, IV bags, and scalps in needle-phobic individuals demonstrated significantly positive response rates for reducing aversion, fear, and anxiety. For the stress-reducing devices, each individual design was superior to the corresponding conventional device, indicating a dominant class effect of these stress-reducing medical devices, rather than the specific design.
Damping visual cues of threat
It is likely that decoration of a medical device actually is a neurophysiologic intervention, resulting in stimulation of brain areas not usually associated with the fear, anxiety, and aversion responses caused by viewing medical devices. In this sense, the intervention of decorating a medical device has a close parallel to other cognitive, distraction, and mind-body imagery methods of intervention.1-7,12-18
However, unlike these other interventions, decoration of the medical device actually focuses the patient’s attention and interest on the medical device, yet fear, aversion, and anxiety of needles and syringes are still significantly reduced. This suggests that the decorations interfere with the established link between visual recognition of a perceived threat and the subsequent emotional response to that perceived threat. In the future, neuroimaging of brain activation in response to these decorated devices may provide a more telling explanation of their stress-reducing effects.
This study demonstrates unexpectedly high levels of stress and fear of medical devices in typical clinic patients, and significant reduction of these stress measures by the use of stress-reducing decorated medical devices. The most favorable implementation of this technology would be for these stress-reducing medical devices to be mass-produced and the decorations placed on the device at the factory rather at the site of service. Ultimate implementation of this technology will determined primarily by economic considerations and the acceptance of these aesthetic modifications by nursing, physician, and administrative staff in family practice units.
CORRESPONDENCE
Wilmer L. Sibbitt, Jr, MD, Department of Internal Medicine, 5th floor ACC, University of New Mexico Health Sciences Center, Albuquerque, NM 87131. E-mail: wsibbitt@salud.unm.edu
- Adding decorative designs or stickers to medical devices before a procedure significantly reduces aversion, fear, and anxiety, and may be especially useful for needle-phobic patients (A).
Needle phobia—fear of needles, syringes, intravenous therapy, and medical devices—can seriously compromise medical care.1-7 We hypothesized that a novel cognitive therapy consisting of simple designs and decorations on needles and other medical devices would reduce needle phobia. Fear, aversion, and anxiety decreased significantly—as measured by validated visual analogue reaction scales—when patients were exposed to decorated devices.
Materials and methods
Subjects
This was a randomized controlled trial approved by the Institutional Review Board (IRB). Sixty patients were recruited from outpatient clinics: 67% female, 33% male, 100% outpatients, 41% pediatric patients, and 59% adults—representing the typical mix of subjects in a family practice clinic. The mean age of the patients was 32±21 years (range, 3 years to 65 years).
After informed consent, the subjects were randomly exposed to 8 different designs of winged needles and 6 different designs of syringes fitted with a needle. Smaller subsets of subjects were exposed to different designs of intravenous (IV) bags and scalpels.
Stress-reducing needles and syringes
Stress-reducing syringes were created by taking conventional 10-mL syringes (10-mL Luer-Lok BD syringe, ref 309604, Becton Dickinson, Franklin Lakes, NJ) and decorating them so that the markings of the barrel could still be seen (FIGURE 1). Stress-reducing winged catheters (21 G 3/4×12-inch 367281 Vacutainer brand Safety-Lok Blood Collection Set; Becton Dickinson, Franklin Lakes, NJ) were created by decorating the wings in a symmetrical manner (FIGURE 2). Similarly, different designs of IV bag (FIGURE 3) and scalpel were used.
FIGURE 1
Stress-reducing syringes
Stress-reducing syringes (compared with 3 typical conventional syringes at right) yielded a mean 79% decrease in aversion scores, 53% decrease in fear scores, and 51% decrease in anxiety scores. Musical notes were the most favored design (P<.001).
FIGURE 2
Stress-reducing butterfly needles
Stress-reducing butterfly needles (compared with 4 typical designs at bottom) reduced aversion by 68%, fear by 53%, and anxiety by 53% (P<.001).
FIGURE 3
Stress-reducing IV bags
Stress-reducing intravenous bags reduced aversion by 83%, fear by 53%, and anxiety by 73% (P<.001).
Outcome measures
For each group of devices, the presentation of individual devices to each subject was randomized to eliminate the possibility of a consistent bias. Emotional responses to the medical devices were determined with the validated visual analogue reaction scales where 0 is lowest response and 10 is the strongest.8-11 These included the Visual Analogue Anxiety Scale (VAAS), Visual Analogue Fear Scale (VAFS), and Visual Analogue Aversion Scale (VAS). Significant needle phobia was defined as an aversion, fear, or anxiety score of greater than or equal to 5.
Statistical analysis
Primary analyses consisted of comparing the responses to the stress-reducing devices as a class with the conventional devices as a class. These paired data were compared with the paired 2-tailed t-test. To determine whether these responses were class-specific or design-specific, the results for each individual device were then compared with a matched control, design by design, again with the paired 2-tailed t-test. Corrections were made for multiple comparisons.
Results
Patients experienced markedly more aversion to (dislike of) conventional syringes (VAAS score: 5.88±3.61 vs stress-reducing syringes VAAS score: 1.21±1.64; P<.001); they also had greater fear (conventional VAFS score: 4.68±2.8 vs stress-reducing VAFS score: 2.19±2.8, P<.001) and anxiety (conventional VAS score: 4.54±3.68 vs stress-reducing VAS score: 2.21±2.84, P<.001) (TABLE). This corresponds to a mean 79% decrease in aversion scores, 53% reduction in fear scores, and 51% decrease in anxiety scores with the stress-reducing syringes. Ninety-five percent of subjects preferred the stress-reducing syringes to the conventional syringes; 98% of subjects felt that stress-reducing syringes should be available for children; 72% felt that the stress-reducing syringes should also be available for adults.
The syringes most favored were those with musical notes (56%), flowers (18%), and smiley faces (12%). Each of these designs had lower scores in the 3 domains (fear, aversion, and anxiety) compared with the conventional device (P<.01), indicating that the reduction in stress measures was a class effect, rather than a specific effect of the individual design.
Significant needle phobia is defined as aversion, fear, or anxiety scores ≥5. Using this definition, 80% of subjects experienced moderate to severe aversion, 63% suffered moderate to severe fear, and 62% experienced moderate to severe anxiety on exposure to conventional syringes. This corresponded to mean aversion, fear, and anxiety scores of 7.18±1.92, 6.98±2.16, and 6.78±2.44, respectively. In subjects with significant needle phobia, stress-reducing syringes reduced aversion scores by 81% (P<.001), fear scores by 56% (P<.001), and anxiety by 47% (P<.001). Stress-reducing syringes had a positive response rate of 98% for reducing aversion, 87% in reducing fear, and 74% in reducing anxiety.
Stress-reducing butterfly needles reduced aversion by 68%, fear by 53%, and anxiety by 53% (P<.001). The stress-reducing designs most favored were butterfly designs, flowers, fish, and smiley faces. Stress-reducing IV bags significantly reduced aversion by 83%, fear by 53%, and anxiety by 73% (P<.001). Stress-reducing scalpels also significantly reduced aversion by 49%, fear by 36%, and anxiety by 37% (P<.001).
When analyzed separately, both children and adults responded favorably and similarly to the stress-reducing devices in all 3 domains (P<.01), although children had a higher mean stress level in all 3 domains to conventional devices (P<.05).
TABLE
Significant reductions in aversion, fear, and anxiety with stress-reducing syringes
| 60 SUBJECTS’ EXPERIENCES | CONVENTIONAL SYRINGES | STRESS-REDUCING SYRINGES | P VALUE | % DECREASE IN SCORE |
|---|---|---|---|---|
| Aversion | 5.88±3.61 | 1.21±1.64 | P<.001 | 79% |
| Fear | 4.68±2.8 | 2.19±2.8 | P<.001 | 53% |
| Anxiety | 4.54±3.68 | 2.21±2.84 | P<.001 | 51% |
| Most liked | 5% | 95% | P<.001 | |
| Most disliked | 95% | 5% | P<.001 |
Discussion
A fear of needles, syringe procedures, intravenous therapy, and medical devices is given the overall term of needle phobia, and can seriously compromise patient care.1-7 Adults may express needle phobia verbally or even avoid coming to the physician’s office, while children may be more overtly fearful, anxious, or hysterical. Our study focused on the specific psychological components of stress—aversion, fear, and anxiety—induced by exposure to needles and medical devices.
Aversion, fear, and anxiety were each assessed with the relevant VAS, a reproducible and validated method for assessing stress components in clinical populations.8-11 Using a conservative definition for moderate to severe stress (VAS ≥5), 80% of subjects experienced moderate to severe aversion, 63% suffered moderate to severe fear, and 62% experienced moderate to severe anxiety in response to conventional devices. Thus, significant levels of clinically relevant needle phobia are present in typical outpatient populations. Several approaches have been taken to prevent and treat needle phobia, including reassurance, education, avoidance of needles, postural and muscle tension techniques, benzodiazepines, nitrous oxide gas, topical anesthesia, cognitive therapy, participant modeling, distraction, meditation, hypnosis, and coaching—all with variable and inconsistent results.1-7,12-18
We hypothesized that visual modifications to needles, syringes, and other medical devices would result in stress-reducing devices that would lessen patient needle phobia. The stress-reducing needles and medical devices were created by applying simple representative designs on winged needles, syringes, IV bags, and scalpels while maintaining the basic function of these devices (FIGURES 1-3).
Stress-reducing syringes resulted in a 79% decrease in aversion, 53% reduction in fear, and 51% decrease in anxiety in the overall patient population compared to the conventional syringes (P<.001). More importantly, in subjects with significant needle phobia (VAS scores ≥5), stress-reducing syringes reduced aversion by 81%, fear by 56%, and anxiety by 47% (P<.001). This corresponds to favorable responses of 98% for aversion, 87% for fear, and 74% in anxiety in subjects with needle phobia. Similarly, stress-reducing winged needles, IV bags, and scalps in needle-phobic individuals demonstrated significantly positive response rates for reducing aversion, fear, and anxiety. For the stress-reducing devices, each individual design was superior to the corresponding conventional device, indicating a dominant class effect of these stress-reducing medical devices, rather than the specific design.
Damping visual cues of threat
It is likely that decoration of a medical device actually is a neurophysiologic intervention, resulting in stimulation of brain areas not usually associated with the fear, anxiety, and aversion responses caused by viewing medical devices. In this sense, the intervention of decorating a medical device has a close parallel to other cognitive, distraction, and mind-body imagery methods of intervention.1-7,12-18
However, unlike these other interventions, decoration of the medical device actually focuses the patient’s attention and interest on the medical device, yet fear, aversion, and anxiety of needles and syringes are still significantly reduced. This suggests that the decorations interfere with the established link between visual recognition of a perceived threat and the subsequent emotional response to that perceived threat. In the future, neuroimaging of brain activation in response to these decorated devices may provide a more telling explanation of their stress-reducing effects.
This study demonstrates unexpectedly high levels of stress and fear of medical devices in typical clinic patients, and significant reduction of these stress measures by the use of stress-reducing decorated medical devices. The most favorable implementation of this technology would be for these stress-reducing medical devices to be mass-produced and the decorations placed on the device at the factory rather at the site of service. Ultimate implementation of this technology will determined primarily by economic considerations and the acceptance of these aesthetic modifications by nursing, physician, and administrative staff in family practice units.
CORRESPONDENCE
Wilmer L. Sibbitt, Jr, MD, Department of Internal Medicine, 5th floor ACC, University of New Mexico Health Sciences Center, Albuquerque, NM 87131. E-mail: wsibbitt@salud.unm.edu
1. Fassler D. The fear of needles in children. Am J Orthopsychiatry 1985;55:371-377.
2. Hamilton JG. Needle phobia: a neglected diagnosis. J Fam Pract 1995;41:169-175.
3. McSherry J. Perspectives on needle phobia. J Fam Pract 1995;41:437,512.-
4. Daniels AJ. Perspectives on needle phobia. J Fam Pract 1995;41:437.-
5. Stark MM, Brener N. Needle phobia. J Clin Forensic Med 2000;7:35-8.
6. Smalley A. Needle phobia. Paediatr Nurs 1999;11:17-20.
7. Hedstrom M, Haglund K, Skolin I, von Essen L. Distressing events for children and adolescents with cancer: child, parent, and nurse perceptions. J Pediatr Oncol Nurs 2003;20:120-132.
8. Ferguson JM, Taylor CB, Wermuth B. A rapid behavioral treatment for needle phobics. J Nerv Ment Dis 1978;166:294-298.
9. Ferguson JM, Wermuth BM, Taylor CB. Rapid desensitization of a needle phobia by participant modeling. West J Med 1976;124:174-176.
10. Mumford O. Patient tips from industry. Coping with needle phobia Diabetes Educ 2004;30:174.-
11. Koppel SM, Thapar A. Treating blood needle phobia. Hosp Med 1998;59:730-732.
12. Dahlquist LM, Busby SM, Slifer KJ, et al. Distraction for children of different ages who undergo repeated needle sticks. J Pediatr Oncol Nurs 2002;19:22-34.
13. Speirs AF, Taylor KH, Joanes DN, Girdler NM. A randomised, double-blind, placebo-controlled, comparative study of topical skin analgesics and the anxiety and discomfort associated with venous cannulation. Br Dent J 2001;190:444-449.
14. Kleiber C, Craft-Rosenberg M, Harper DC. Parents as distraction coaches during i.v. insertion: a randomized study. J Pain Symptom Manage 2001;22:851-861.
15. Bhachu HS, Kay B, Healy TE, Beatty P. Grading of pain and anxiety. Comparison between a linear analogue and a computerised audiovisual analogue scale. Anaesthesia 1983;38:875-878.
16. Miller MD, Ferris DG. Measurement of subjective phenomena in primary care research: the Visual Analogue Scale. Fam Pract Res J 1993;13:15-24.
17. Salomon JA, Murray CJ. A multi-method approach to measuring health-state valuations. Health Econ 2004;13:281-290.
18. Chapman HR, Kirby-Turner N. Visual/verbal analogue scales: examples of brief assessment methods to aid management of child and adult patients in clinical practice. Br Dent J 2002;193:447-450.
1. Fassler D. The fear of needles in children. Am J Orthopsychiatry 1985;55:371-377.
2. Hamilton JG. Needle phobia: a neglected diagnosis. J Fam Pract 1995;41:169-175.
3. McSherry J. Perspectives on needle phobia. J Fam Pract 1995;41:437,512.-
4. Daniels AJ. Perspectives on needle phobia. J Fam Pract 1995;41:437.-
5. Stark MM, Brener N. Needle phobia. J Clin Forensic Med 2000;7:35-8.
6. Smalley A. Needle phobia. Paediatr Nurs 1999;11:17-20.
7. Hedstrom M, Haglund K, Skolin I, von Essen L. Distressing events for children and adolescents with cancer: child, parent, and nurse perceptions. J Pediatr Oncol Nurs 2003;20:120-132.
8. Ferguson JM, Taylor CB, Wermuth B. A rapid behavioral treatment for needle phobics. J Nerv Ment Dis 1978;166:294-298.
9. Ferguson JM, Wermuth BM, Taylor CB. Rapid desensitization of a needle phobia by participant modeling. West J Med 1976;124:174-176.
10. Mumford O. Patient tips from industry. Coping with needle phobia Diabetes Educ 2004;30:174.-
11. Koppel SM, Thapar A. Treating blood needle phobia. Hosp Med 1998;59:730-732.
12. Dahlquist LM, Busby SM, Slifer KJ, et al. Distraction for children of different ages who undergo repeated needle sticks. J Pediatr Oncol Nurs 2002;19:22-34.
13. Speirs AF, Taylor KH, Joanes DN, Girdler NM. A randomised, double-blind, placebo-controlled, comparative study of topical skin analgesics and the anxiety and discomfort associated with venous cannulation. Br Dent J 2001;190:444-449.
14. Kleiber C, Craft-Rosenberg M, Harper DC. Parents as distraction coaches during i.v. insertion: a randomized study. J Pain Symptom Manage 2001;22:851-861.
15. Bhachu HS, Kay B, Healy TE, Beatty P. Grading of pain and anxiety. Comparison between a linear analogue and a computerised audiovisual analogue scale. Anaesthesia 1983;38:875-878.
16. Miller MD, Ferris DG. Measurement of subjective phenomena in primary care research: the Visual Analogue Scale. Fam Pract Res J 1993;13:15-24.
17. Salomon JA, Murray CJ. A multi-method approach to measuring health-state valuations. Health Econ 2004;13:281-290.
18. Chapman HR, Kirby-Turner N. Visual/verbal analogue scales: examples of brief assessment methods to aid management of child and adult patients in clinical practice. Br Dent J 2002;193:447-450.