User login
Product Update
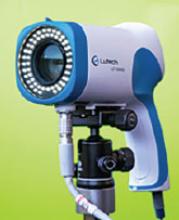
LUTECH LT-300 HD FOR COLPOSCOPY
Background. In March 1924, the colposcope was introduced to evaluate the portio of the cervix by Hans Hinselmann in Germany after years of work with the famous lens manufacturer Leitz.1 Although its adoption as a standard tool for evaluating lower genital tract neoplasia was protracted, today it sits as a cornerstone technology in gynecology, and every ObGyn provider has been trained to perform colposcopic exams that include visualizing the cervix, vagina, and vulva as well as taking biopsies. In December 2000, after 75 years of glass lens technology, Welch-Allyn (Skaneateles Falls, New York) introduced the first video colposcope, shepherding the field into the 21st century with only limited traction. Now, Lutech is entering the fray hoping to further nudge traditionalists into the digital age.
Design/Functionality. The Lutech LT-300 HD works off of a Sony Exmor CMOS (complementary metaloxide semiconductor) camera with 2.13 megapixels to provide high-definition optical magnification of 1-30X illuminated by a circular cool LED array that offers 3000 lx of white light with an adjustable green filter to allow for contrast at working distances between 5.1 and 15.7 inches. The colposcope comes with either a vertical stand or a swing arm stand and has both HDMI and USB 3.0 video output so that the system can be attached to either a stand-alone monitor or a computer (not included). The colposcope also comes in a standard definition configuration (LT-300 SD), but I did not trial that model because the price difference did not seem to justify the potentially lower resolution.
In my experience with its use, the Lutech LT-300 HD was pretty excellent. Being a man and a doctor, I refused the online training session that comes free with the colposcope, assuming I could figure it out on my own. My assumption was mostly true, but there were definitely some tips and tricks that would have made my life easier had I not been so stiff-necked. That said, the biggest adjustment is getting used to looking at a screen and not having to look through eyepieces. The picture output is great and, as a patient (or student) teaching tool, it is phenomenal. Also, because it is digital, the image capture features allow for image importation into notes (although it is clunky and requires work arounds when using Epic).
Innovation. From an innovation point of view, I am not sure that Lutech re-invented fire since, in essence, the LT-300 HD is a modified CMOS video camera. But the company did do a nice job bringing together a lot of existing technologies into a highly functional product. I would love to see better integration with some of the larger electronic medical records (EMRs), but I suspect the barriers lie with the EMR companies rather than with Lutech, so I am giving them a pass on that front.
Summary. At its core, a colposcope is simply a tool with which to obtain a magnified view of the cervix, vagina, and/or vulva. Prior to advent and proliferation of CMOS camera technology, the most readily available means of accomplishing this was to employ glass lenses. But that was then, and this is now; CMOS technology is just better, cheaper, and more versatile. I no longer turn my head to look over my shoulder while backing up my car—I use the back-up camera. My Kodak instamatic has given way to my iPhone. And now, my incredibly heavy, unwieldy Leisegang colposcope has been replaced by a light-weight camera on a stand that I can easily move from room to room. I won’t lie, though,…it still seems weird to not look through eyepieces and work the focus knobs, but I am happy with the change. My patients can now see what I am looking at and better understand their diagnosis (if they want), and my notes are prettier. Onward march of progress.
Reference
1. Fusco E, Padula F, Mancini E, et al. History of colposcopy: a brief biography of Hinselmann. J Prenat Med. 2008;2:19-23.
Continue to: DTR MEDICAL CERVICAL ROTATING BIOPSY PUNCH...
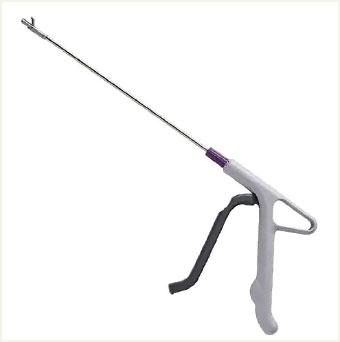
DTR MEDICAL CERVICAL ROTATING BIOPSY PUNCH
The single-use DTR Medical Cervical Rotating Biopsy Punch from Innovia Medical (Swansea, United Kingdom) “works great” and “is reasonably cost-effective to replace reusables.”
Background. Integral to every colposcopic examination is the potential need to biopsy abnormal appearing tissues. To accomplish this latter task, numerous punch-style biopsy devices have been developed in a variety of jaw shapes and styles, crafted from materials ranging from stainless steel to titanium to ceramic, with the ultimate goal the same—get a piece of tissue from the cervix as easily as possible.
Design/Functionality. DTR Medical Cervical Rotating Biopsy Punch is a single-use sterile device that comes packaged as 10 per box. It features Kevorkian-style “stronger than Titanium” jaws that yield a 3.0 mm x 7.5 mm sample attached to a metal shaft that can rotate 360°. The shaft inserts into a lightweight plastic pistol-grip style handle. From tip to handle, the device measures 36.5 cm (14.125 in).
In my experience with its use, the DTR Medical Cervical Rotating Biopsy Punch performed flawlessly. Its relatively low-profile jaws allowed for unobstructed access to biopsy sites and the ability to rotate the jaws was a big plus. The “stronger than Titanium” jaws consistently yielded the exact biopsies I wanted, like a knife going through butter.
Innovation. From an innovation standpoint, the DTR Medical Cervical Rotating Biopsy Punch is more of an engineering “duh” than “wow,” but it works great so who cares that it’s not a fusion reactor. That said, the innovative part from Innovia Medical is their ability to make such a high-quality biopsy device and sell it at a price that makes it reasonably cost-effective to replace reusables.
Summary. Whether it is a Tischler, Kevorkian, or Burke tip, the real question before any gynecologist uses the cervical biopsy device she/he/they has in her/his/ their hand is, will it cut? Because all reusable surgical instruments are in fact reusable, those edges that are designed to cut invariably become dull with reuse. And, unless they are meticulously maintained and routinely sharpened (spoiler alert, they never are), providers are not infrequently chagrinned by the gnawing rather than cutting that these instruments deliver. Thinking back, I could not remember the last time I had made an incision with a surgical scalpel blade that had previously been used then sharpened and re-sterilized. Then I did remember…never. Reflecting on this, I wondered why I was doing this with my cervical biopsy devices. While I really do not like the environmental waste created by single-use devices, reusable instruments that require re-processing do have an environmental impact and a significant cost. Considering this, I do not think that environmental reasons are enough of a barrier to justify using dull biopsy tools if it can be done cost-effectively with a minimal carbon footprint. All-in-all, I like this product, and I plan to use it. ●
LUTECH LT-300 HD FOR COLPOSCOPY
Background. In March 1924, the colposcope was introduced to evaluate the portio of the cervix by Hans Hinselmann in Germany after years of work with the famous lens manufacturer Leitz.1 Although its adoption as a standard tool for evaluating lower genital tract neoplasia was protracted, today it sits as a cornerstone technology in gynecology, and every ObGyn provider has been trained to perform colposcopic exams that include visualizing the cervix, vagina, and vulva as well as taking biopsies. In December 2000, after 75 years of glass lens technology, Welch-Allyn (Skaneateles Falls, New York) introduced the first video colposcope, shepherding the field into the 21st century with only limited traction. Now, Lutech is entering the fray hoping to further nudge traditionalists into the digital age.
Design/Functionality. The Lutech LT-300 HD works off of a Sony Exmor CMOS (complementary metaloxide semiconductor) camera with 2.13 megapixels to provide high-definition optical magnification of 1-30X illuminated by a circular cool LED array that offers 3000 lx of white light with an adjustable green filter to allow for contrast at working distances between 5.1 and 15.7 inches. The colposcope comes with either a vertical stand or a swing arm stand and has both HDMI and USB 3.0 video output so that the system can be attached to either a stand-alone monitor or a computer (not included). The colposcope also comes in a standard definition configuration (LT-300 SD), but I did not trial that model because the price difference did not seem to justify the potentially lower resolution.
In my experience with its use, the Lutech LT-300 HD was pretty excellent. Being a man and a doctor, I refused the online training session that comes free with the colposcope, assuming I could figure it out on my own. My assumption was mostly true, but there were definitely some tips and tricks that would have made my life easier had I not been so stiff-necked. That said, the biggest adjustment is getting used to looking at a screen and not having to look through eyepieces. The picture output is great and, as a patient (or student) teaching tool, it is phenomenal. Also, because it is digital, the image capture features allow for image importation into notes (although it is clunky and requires work arounds when using Epic).
Innovation. From an innovation point of view, I am not sure that Lutech re-invented fire since, in essence, the LT-300 HD is a modified CMOS video camera. But the company did do a nice job bringing together a lot of existing technologies into a highly functional product. I would love to see better integration with some of the larger electronic medical records (EMRs), but I suspect the barriers lie with the EMR companies rather than with Lutech, so I am giving them a pass on that front.
Summary. At its core, a colposcope is simply a tool with which to obtain a magnified view of the cervix, vagina, and/or vulva. Prior to advent and proliferation of CMOS camera technology, the most readily available means of accomplishing this was to employ glass lenses. But that was then, and this is now; CMOS technology is just better, cheaper, and more versatile. I no longer turn my head to look over my shoulder while backing up my car—I use the back-up camera. My Kodak instamatic has given way to my iPhone. And now, my incredibly heavy, unwieldy Leisegang colposcope has been replaced by a light-weight camera on a stand that I can easily move from room to room. I won’t lie, though,…it still seems weird to not look through eyepieces and work the focus knobs, but I am happy with the change. My patients can now see what I am looking at and better understand their diagnosis (if they want), and my notes are prettier. Onward march of progress.
Reference
1. Fusco E, Padula F, Mancini E, et al. History of colposcopy: a brief biography of Hinselmann. J Prenat Med. 2008;2:19-23.
Continue to: DTR MEDICAL CERVICAL ROTATING BIOPSY PUNCH...
DTR MEDICAL CERVICAL ROTATING BIOPSY PUNCH
The single-use DTR Medical Cervical Rotating Biopsy Punch from Innovia Medical (Swansea, United Kingdom) “works great” and “is reasonably cost-effective to replace reusables.”
Background. Integral to every colposcopic examination is the potential need to biopsy abnormal appearing tissues. To accomplish this latter task, numerous punch-style biopsy devices have been developed in a variety of jaw shapes and styles, crafted from materials ranging from stainless steel to titanium to ceramic, with the ultimate goal the same—get a piece of tissue from the cervix as easily as possible.
Design/Functionality. DTR Medical Cervical Rotating Biopsy Punch is a single-use sterile device that comes packaged as 10 per box. It features Kevorkian-style “stronger than Titanium” jaws that yield a 3.0 mm x 7.5 mm sample attached to a metal shaft that can rotate 360°. The shaft inserts into a lightweight plastic pistol-grip style handle. From tip to handle, the device measures 36.5 cm (14.125 in).
In my experience with its use, the DTR Medical Cervical Rotating Biopsy Punch performed flawlessly. Its relatively low-profile jaws allowed for unobstructed access to biopsy sites and the ability to rotate the jaws was a big plus. The “stronger than Titanium” jaws consistently yielded the exact biopsies I wanted, like a knife going through butter.
Innovation. From an innovation standpoint, the DTR Medical Cervical Rotating Biopsy Punch is more of an engineering “duh” than “wow,” but it works great so who cares that it’s not a fusion reactor. That said, the innovative part from Innovia Medical is their ability to make such a high-quality biopsy device and sell it at a price that makes it reasonably cost-effective to replace reusables.
Summary. Whether it is a Tischler, Kevorkian, or Burke tip, the real question before any gynecologist uses the cervical biopsy device she/he/they has in her/his/ their hand is, will it cut? Because all reusable surgical instruments are in fact reusable, those edges that are designed to cut invariably become dull with reuse. And, unless they are meticulously maintained and routinely sharpened (spoiler alert, they never are), providers are not infrequently chagrinned by the gnawing rather than cutting that these instruments deliver. Thinking back, I could not remember the last time I had made an incision with a surgical scalpel blade that had previously been used then sharpened and re-sterilized. Then I did remember…never. Reflecting on this, I wondered why I was doing this with my cervical biopsy devices. While I really do not like the environmental waste created by single-use devices, reusable instruments that require re-processing do have an environmental impact and a significant cost. Considering this, I do not think that environmental reasons are enough of a barrier to justify using dull biopsy tools if it can be done cost-effectively with a minimal carbon footprint. All-in-all, I like this product, and I plan to use it. ●
LUTECH LT-300 HD FOR COLPOSCOPY
Background. In March 1924, the colposcope was introduced to evaluate the portio of the cervix by Hans Hinselmann in Germany after years of work with the famous lens manufacturer Leitz.1 Although its adoption as a standard tool for evaluating lower genital tract neoplasia was protracted, today it sits as a cornerstone technology in gynecology, and every ObGyn provider has been trained to perform colposcopic exams that include visualizing the cervix, vagina, and vulva as well as taking biopsies. In December 2000, after 75 years of glass lens technology, Welch-Allyn (Skaneateles Falls, New York) introduced the first video colposcope, shepherding the field into the 21st century with only limited traction. Now, Lutech is entering the fray hoping to further nudge traditionalists into the digital age.
Design/Functionality. The Lutech LT-300 HD works off of a Sony Exmor CMOS (complementary metaloxide semiconductor) camera with 2.13 megapixels to provide high-definition optical magnification of 1-30X illuminated by a circular cool LED array that offers 3000 lx of white light with an adjustable green filter to allow for contrast at working distances between 5.1 and 15.7 inches. The colposcope comes with either a vertical stand or a swing arm stand and has both HDMI and USB 3.0 video output so that the system can be attached to either a stand-alone monitor or a computer (not included). The colposcope also comes in a standard definition configuration (LT-300 SD), but I did not trial that model because the price difference did not seem to justify the potentially lower resolution.
In my experience with its use, the Lutech LT-300 HD was pretty excellent. Being a man and a doctor, I refused the online training session that comes free with the colposcope, assuming I could figure it out on my own. My assumption was mostly true, but there were definitely some tips and tricks that would have made my life easier had I not been so stiff-necked. That said, the biggest adjustment is getting used to looking at a screen and not having to look through eyepieces. The picture output is great and, as a patient (or student) teaching tool, it is phenomenal. Also, because it is digital, the image capture features allow for image importation into notes (although it is clunky and requires work arounds when using Epic).
Innovation. From an innovation point of view, I am not sure that Lutech re-invented fire since, in essence, the LT-300 HD is a modified CMOS video camera. But the company did do a nice job bringing together a lot of existing technologies into a highly functional product. I would love to see better integration with some of the larger electronic medical records (EMRs), but I suspect the barriers lie with the EMR companies rather than with Lutech, so I am giving them a pass on that front.
Summary. At its core, a colposcope is simply a tool with which to obtain a magnified view of the cervix, vagina, and/or vulva. Prior to advent and proliferation of CMOS camera technology, the most readily available means of accomplishing this was to employ glass lenses. But that was then, and this is now; CMOS technology is just better, cheaper, and more versatile. I no longer turn my head to look over my shoulder while backing up my car—I use the back-up camera. My Kodak instamatic has given way to my iPhone. And now, my incredibly heavy, unwieldy Leisegang colposcope has been replaced by a light-weight camera on a stand that I can easily move from room to room. I won’t lie, though,…it still seems weird to not look through eyepieces and work the focus knobs, but I am happy with the change. My patients can now see what I am looking at and better understand their diagnosis (if they want), and my notes are prettier. Onward march of progress.
Reference
1. Fusco E, Padula F, Mancini E, et al. History of colposcopy: a brief biography of Hinselmann. J Prenat Med. 2008;2:19-23.
Continue to: DTR MEDICAL CERVICAL ROTATING BIOPSY PUNCH...
DTR MEDICAL CERVICAL ROTATING BIOPSY PUNCH
The single-use DTR Medical Cervical Rotating Biopsy Punch from Innovia Medical (Swansea, United Kingdom) “works great” and “is reasonably cost-effective to replace reusables.”
Background. Integral to every colposcopic examination is the potential need to biopsy abnormal appearing tissues. To accomplish this latter task, numerous punch-style biopsy devices have been developed in a variety of jaw shapes and styles, crafted from materials ranging from stainless steel to titanium to ceramic, with the ultimate goal the same—get a piece of tissue from the cervix as easily as possible.
Design/Functionality. DTR Medical Cervical Rotating Biopsy Punch is a single-use sterile device that comes packaged as 10 per box. It features Kevorkian-style “stronger than Titanium” jaws that yield a 3.0 mm x 7.5 mm sample attached to a metal shaft that can rotate 360°. The shaft inserts into a lightweight plastic pistol-grip style handle. From tip to handle, the device measures 36.5 cm (14.125 in).
In my experience with its use, the DTR Medical Cervical Rotating Biopsy Punch performed flawlessly. Its relatively low-profile jaws allowed for unobstructed access to biopsy sites and the ability to rotate the jaws was a big plus. The “stronger than Titanium” jaws consistently yielded the exact biopsies I wanted, like a knife going through butter.
Innovation. From an innovation standpoint, the DTR Medical Cervical Rotating Biopsy Punch is more of an engineering “duh” than “wow,” but it works great so who cares that it’s not a fusion reactor. That said, the innovative part from Innovia Medical is their ability to make such a high-quality biopsy device and sell it at a price that makes it reasonably cost-effective to replace reusables.
Summary. Whether it is a Tischler, Kevorkian, or Burke tip, the real question before any gynecologist uses the cervical biopsy device she/he/they has in her/his/ their hand is, will it cut? Because all reusable surgical instruments are in fact reusable, those edges that are designed to cut invariably become dull with reuse. And, unless they are meticulously maintained and routinely sharpened (spoiler alert, they never are), providers are not infrequently chagrinned by the gnawing rather than cutting that these instruments deliver. Thinking back, I could not remember the last time I had made an incision with a surgical scalpel blade that had previously been used then sharpened and re-sterilized. Then I did remember…never. Reflecting on this, I wondered why I was doing this with my cervical biopsy devices. While I really do not like the environmental waste created by single-use devices, reusable instruments that require re-processing do have an environmental impact and a significant cost. Considering this, I do not think that environmental reasons are enough of a barrier to justify using dull biopsy tools if it can be done cost-effectively with a minimal carbon footprint. All-in-all, I like this product, and I plan to use it. ●
Product updates and reviews
REVIEW
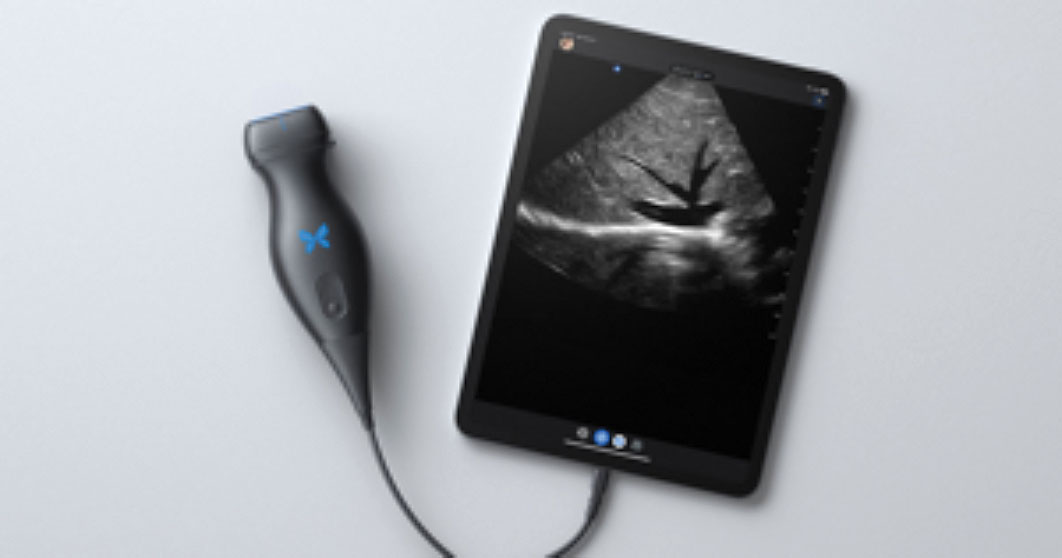
Butterfly iQ+: Offering day-to-day portable ultrasound tech
The Butterfly iQ+ app with an ultrasound probe and cable is available from Butterfly Network, Inc, in Guilford, Connecticut.
Background. It could be reasonably argued that ultrasonography has surpassed the speculum as the single most important tool in ObGyn. From its origins in 1949 with the pioneering work of George Ludwig using A-mode (amplitude-mode) ultrasound and the first publication of its use in pregnancy using B-mode (brightness-mode) ultrasound in Lancet in 1958 by Donald and colleagues, this technology has become so ingrained into ObGyn that it is often frustrating to practice comfortably without it. Thus, today, the biggest question facing most practitioners is not whether or not to have an ultrasound in their practice but which one to have.
Given the wide range of quality, functionality, and price within the ultrasound device space, choosing the right technology can feel as daunting as choosing the perfect restaurant in New York City. That said, when looking for entry-level ultrasound technology to address the day-to-day basic needs of your average ObGyn, the Butterfly iQ+ may be an easy choice.
Design/Functionality. The Butterfly iQ+ app does not come with a screen. Rather, the device is compatible with both iOS and Android systems and readily connects to a vast array of easily purchased devices, with either lightening or USB-C ports. In our office, we use an iPad mini. The probe is lightweight (309 g) and contains a rechargeable 2600 mAh lithium ion battery, so that its power source is independent of the device to which it is attached. The probe is a 2D array with 9000 micro-machined sensors. It allows for imaging using M-mode, B-mode, Color Doppler, Power Doppler, and Pulsed Wave Doppler. (I don’t know what the last two are or what they are used for, but they sound important.) It has a scan depth range of 1 cm to 30 cm. The downloadable Butterfly iQ+ app that has the software that makes the probe functional has more tools, controls, and presets than anyone could ever need. But that’s not all. The App has data encrypted HIPAA/HITECH-compliant Cloud-based connectivity that offers unlimited image storage, access to reports, and embedded CPT codes should billing capabilities be needed.
The true beauty of the Butterfly iQ+ is that the image quality is awesome and it is really easy to use. The software is mostly intuitive and takes only a minimal effort to learn. The device holds its charge more than adequately for a day in the office and the recharging process is fast and easy. When it comes to the device’s design and functionality–as a Capricorn–I am still looking for its flaws.
Innovation. The real innovations of the Butterfly iQ+ are its “ultrasound-on-a-chip”™ technology and its incorporation of a rechargeable battery into the probe. This combination allows for crystal clear imaging in a cordless, portable device. While most other similar technologies waste their time, technology, space, and cost on the screen, the Butterfly iQ+ punted on that challenge and put all their efforts into the probe and the software. It was a great choice.
Summary. In our office, the Butterfly iQ+ has changed the way we practice. Our trusty fetal dopplers are mostly gone, having been replaced by the Butterfly iQ+. At almost every prenatal visit, patients can now see their baby rather than just hear the heartbeat (and they can hear it too if they want by using the M-mode functionality on the device). Patients love it, and so do the doctors. Instead of just hearing heart beats, fetal position and quick fluid checks are now routine, so we think our care is actually a little better than it was. The Butterfly iQ+ is also great for confirming IUD locations after placement or when the strings are not visible. All-in-all, I love this product. Who doesn’t love butterflies?!
For more information, visit https://www.butterflynetwork.com
The views of the author are personal opinions and do not necessarily represent the views of OBG
References
- Kaproth-Joslin KA, Nicola R, Dogra VS. The History of US: from bats and boats to the bedside and beyond: RSNA centennial article. Radiographics. 2015;35:960-970.
- Donald I, MacVicar J, Brown TG. Investigation of abdominal masses by pulsed ultrasound. Lancet. 1958;1:1188-1195.
REVIEW
Butterfly iQ+: Offering day-to-day portable ultrasound tech
The Butterfly iQ+ app with an ultrasound probe and cable is available from Butterfly Network, Inc, in Guilford, Connecticut.
Background. It could be reasonably argued that ultrasonography has surpassed the speculum as the single most important tool in ObGyn. From its origins in 1949 with the pioneering work of George Ludwig using A-mode (amplitude-mode) ultrasound and the first publication of its use in pregnancy using B-mode (brightness-mode) ultrasound in Lancet in 1958 by Donald and colleagues, this technology has become so ingrained into ObGyn that it is often frustrating to practice comfortably without it. Thus, today, the biggest question facing most practitioners is not whether or not to have an ultrasound in their practice but which one to have.
Given the wide range of quality, functionality, and price within the ultrasound device space, choosing the right technology can feel as daunting as choosing the perfect restaurant in New York City. That said, when looking for entry-level ultrasound technology to address the day-to-day basic needs of your average ObGyn, the Butterfly iQ+ may be an easy choice.
Design/Functionality. The Butterfly iQ+ app does not come with a screen. Rather, the device is compatible with both iOS and Android systems and readily connects to a vast array of easily purchased devices, with either lightening or USB-C ports. In our office, we use an iPad mini. The probe is lightweight (309 g) and contains a rechargeable 2600 mAh lithium ion battery, so that its power source is independent of the device to which it is attached. The probe is a 2D array with 9000 micro-machined sensors. It allows for imaging using M-mode, B-mode, Color Doppler, Power Doppler, and Pulsed Wave Doppler. (I don’t know what the last two are or what they are used for, but they sound important.) It has a scan depth range of 1 cm to 30 cm. The downloadable Butterfly iQ+ app that has the software that makes the probe functional has more tools, controls, and presets than anyone could ever need. But that’s not all. The App has data encrypted HIPAA/HITECH-compliant Cloud-based connectivity that offers unlimited image storage, access to reports, and embedded CPT codes should billing capabilities be needed.
The true beauty of the Butterfly iQ+ is that the image quality is awesome and it is really easy to use. The software is mostly intuitive and takes only a minimal effort to learn. The device holds its charge more than adequately for a day in the office and the recharging process is fast and easy. When it comes to the device’s design and functionality–as a Capricorn–I am still looking for its flaws.
Innovation. The real innovations of the Butterfly iQ+ are its “ultrasound-on-a-chip”™ technology and its incorporation of a rechargeable battery into the probe. This combination allows for crystal clear imaging in a cordless, portable device. While most other similar technologies waste their time, technology, space, and cost on the screen, the Butterfly iQ+ punted on that challenge and put all their efforts into the probe and the software. It was a great choice.
Summary. In our office, the Butterfly iQ+ has changed the way we practice. Our trusty fetal dopplers are mostly gone, having been replaced by the Butterfly iQ+. At almost every prenatal visit, patients can now see their baby rather than just hear the heartbeat (and they can hear it too if they want by using the M-mode functionality on the device). Patients love it, and so do the doctors. Instead of just hearing heart beats, fetal position and quick fluid checks are now routine, so we think our care is actually a little better than it was. The Butterfly iQ+ is also great for confirming IUD locations after placement or when the strings are not visible. All-in-all, I love this product. Who doesn’t love butterflies?!
For more information, visit https://www.butterflynetwork.com
The views of the author are personal opinions and do not necessarily represent the views of OBG
References
- Kaproth-Joslin KA, Nicola R, Dogra VS. The History of US: from bats and boats to the bedside and beyond: RSNA centennial article. Radiographics. 2015;35:960-970.
- Donald I, MacVicar J, Brown TG. Investigation of abdominal masses by pulsed ultrasound. Lancet. 1958;1:1188-1195.
REVIEW
Butterfly iQ+: Offering day-to-day portable ultrasound tech
The Butterfly iQ+ app with an ultrasound probe and cable is available from Butterfly Network, Inc, in Guilford, Connecticut.
Background. It could be reasonably argued that ultrasonography has surpassed the speculum as the single most important tool in ObGyn. From its origins in 1949 with the pioneering work of George Ludwig using A-mode (amplitude-mode) ultrasound and the first publication of its use in pregnancy using B-mode (brightness-mode) ultrasound in Lancet in 1958 by Donald and colleagues, this technology has become so ingrained into ObGyn that it is often frustrating to practice comfortably without it. Thus, today, the biggest question facing most practitioners is not whether or not to have an ultrasound in their practice but which one to have.
Given the wide range of quality, functionality, and price within the ultrasound device space, choosing the right technology can feel as daunting as choosing the perfect restaurant in New York City. That said, when looking for entry-level ultrasound technology to address the day-to-day basic needs of your average ObGyn, the Butterfly iQ+ may be an easy choice.
Design/Functionality. The Butterfly iQ+ app does not come with a screen. Rather, the device is compatible with both iOS and Android systems and readily connects to a vast array of easily purchased devices, with either lightening or USB-C ports. In our office, we use an iPad mini. The probe is lightweight (309 g) and contains a rechargeable 2600 mAh lithium ion battery, so that its power source is independent of the device to which it is attached. The probe is a 2D array with 9000 micro-machined sensors. It allows for imaging using M-mode, B-mode, Color Doppler, Power Doppler, and Pulsed Wave Doppler. (I don’t know what the last two are or what they are used for, but they sound important.) It has a scan depth range of 1 cm to 30 cm. The downloadable Butterfly iQ+ app that has the software that makes the probe functional has more tools, controls, and presets than anyone could ever need. But that’s not all. The App has data encrypted HIPAA/HITECH-compliant Cloud-based connectivity that offers unlimited image storage, access to reports, and embedded CPT codes should billing capabilities be needed.
The true beauty of the Butterfly iQ+ is that the image quality is awesome and it is really easy to use. The software is mostly intuitive and takes only a minimal effort to learn. The device holds its charge more than adequately for a day in the office and the recharging process is fast and easy. When it comes to the device’s design and functionality–as a Capricorn–I am still looking for its flaws.
Innovation. The real innovations of the Butterfly iQ+ are its “ultrasound-on-a-chip”™ technology and its incorporation of a rechargeable battery into the probe. This combination allows for crystal clear imaging in a cordless, portable device. While most other similar technologies waste their time, technology, space, and cost on the screen, the Butterfly iQ+ punted on that challenge and put all their efforts into the probe and the software. It was a great choice.
Summary. In our office, the Butterfly iQ+ has changed the way we practice. Our trusty fetal dopplers are mostly gone, having been replaced by the Butterfly iQ+. At almost every prenatal visit, patients can now see their baby rather than just hear the heartbeat (and they can hear it too if they want by using the M-mode functionality on the device). Patients love it, and so do the doctors. Instead of just hearing heart beats, fetal position and quick fluid checks are now routine, so we think our care is actually a little better than it was. The Butterfly iQ+ is also great for confirming IUD locations after placement or when the strings are not visible. All-in-all, I love this product. Who doesn’t love butterflies?!
For more information, visit https://www.butterflynetwork.com
The views of the author are personal opinions and do not necessarily represent the views of OBG
References
- Kaproth-Joslin KA, Nicola R, Dogra VS. The History of US: from bats and boats to the bedside and beyond: RSNA centennial article. Radiographics. 2015;35:960-970.
- Donald I, MacVicar J, Brown TG. Investigation of abdominal masses by pulsed ultrasound. Lancet. 1958;1:1188-1195.
Product updates and reviews
REVIEW
FEMCERV®: Well-designed technology that can minimize patient discomfort
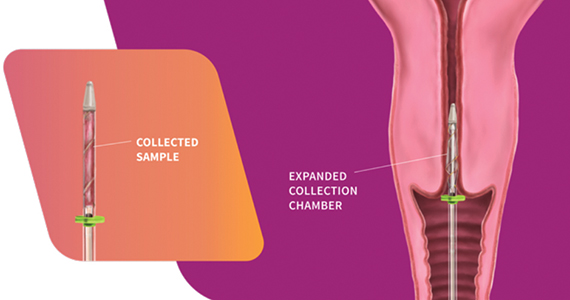
The FemCerv® Endocervical Sampler, developed by Femasys, Inc (Suwanee, Georgia) expands options for colposcopy biopsy.
Background. In the United States, approximately 3 million women per year undergo colposcopic evaluation to work-up abnormal screening cytology. While some controversy exists regarding the exact role of endocervical curettage (ECC) within each age group and clinical situation, it is nonetheless an important component of the colposcopy-biopsy examination in many cases. For over a century, the 3 mm metal endocervical curette has been the primary tool employed to obtain the tissue sample from the endocervical canal. Unfortunately, sharp curettage with a metal curette can have inadequate sampling rates as high as 14%,1 it runs the risk of ectocervical contamination, and it is painful, with almost half the participants in one study rating the procedural pain 3 ̶ 5 out of 8 on a VAS scale.2 So, maybe there is a better way.
Design/Functionality. According to Femasys, the FemCerv® Endocervical Sampler was designed to be the better way of performing an endocervical curettage. FemCerv is a single-use sterile device that comes in a standard 13 F size as well as an 11 F size for the narrower/stenotic os. In truth, at first glance it looks pretty complicated compared with a Kevorkian curette or an endocervical brush. The user end has a handle with a rotatable knob that transitions to a shaft with a flange at the end right before the sampling mechanism. To use the device, the sampling end is inserted into the endocervical canal up to the flange. The knob on the handle is then turned clockwise to open the sheath, thereby exposing sharp rigid plastic edges. The device is then rotated 360° clockwise and then 360° counterclockwise to “curette” the endocervical canal. Finally, the knob on the handle is turned counterclockwise to close the sheath and the device is removed. The specimen is then transferred to a standard vial for processing.
In my experience with its use, it actually exceeded my expectations. The device was easy to use, and the specimens were more than adequate. Truth be told, I came into the trial with a negative mindset having already convinced myself that this device was a waste of money given that doing an ECC with traditional methods is so straightforward. What I had not anticipated was the complete lack of patient discomfort when I used the FemCerv compared with a Kevorkian device.
Innovation. From an innovation standpoint, FemCerv is not super-disruptive technology, but it is well designed and pretty clever in that the opening and closing sheath prevents ectocervical cellular contamination, and the rotational sampling, rather than in-and-out sampling, does dramatically reduce the patient discomfort.
Summary. As I previously noted, before trying it, I did not anticipate liking FemCerv as much as I did. Does it add some non-reimbursable cost to a relatively low-reimbursing procedure? Absolutely. But it is not too expensive and, for me, making a painful procedure relatively painless is good value every time. I think all our patients would agree.
For more information, visit https://femasys.com/.
UPDATE
Hologic, Inc. announces that they received the following 2022 IMV ServiceTrakTM Awards for Mammography: Best Service, Best Customer Satisfaction, and Best System Performance. In addition, Hologic announces that their Affirm Contrast Biopsy software is commercially available in the United States. Tissue samples may be targeted and acquired using the Affirm Contrast Biopsy software from lesions identified using Hologic’s I-View Contrast Enhanced Mammography software. The latter software allows health care facilities an alternative to breast magnetic resonance imaging, which is used as supplemental imaging to mammography and/or ultrasonography.
For more information, visit https://www.hologic.com/
- Damkjaer M, Laursen JB, Petersen LK, et al. Endocervical sampling in women with suspected cervical neoplasia: a systematic review and meta-analysis of diagnostic test accuracy studies. Am J Obstet Gynecol. 2022;227:839-848.e4. doi: 10.1016/j.ajog.2022.07.036.
- Goksedef BP, Api M, Kaya O, et al. Diagnostic accuracy of two endocervical sampling method: randomized controlled trial. Arch Gynecol Obstet. 2013;287:117-22. doi: 10.1007/s00404-012-2542-9.
REVIEW
FEMCERV®: Well-designed technology that can minimize patient discomfort

The FemCerv® Endocervical Sampler, developed by Femasys, Inc (Suwanee, Georgia) expands options for colposcopy biopsy.
Background. In the United States, approximately 3 million women per year undergo colposcopic evaluation to work-up abnormal screening cytology. While some controversy exists regarding the exact role of endocervical curettage (ECC) within each age group and clinical situation, it is nonetheless an important component of the colposcopy-biopsy examination in many cases. For over a century, the 3 mm metal endocervical curette has been the primary tool employed to obtain the tissue sample from the endocervical canal. Unfortunately, sharp curettage with a metal curette can have inadequate sampling rates as high as 14%,1 it runs the risk of ectocervical contamination, and it is painful, with almost half the participants in one study rating the procedural pain 3 ̶ 5 out of 8 on a VAS scale.2 So, maybe there is a better way.
Design/Functionality. According to Femasys, the FemCerv® Endocervical Sampler was designed to be the better way of performing an endocervical curettage. FemCerv is a single-use sterile device that comes in a standard 13 F size as well as an 11 F size for the narrower/stenotic os. In truth, at first glance it looks pretty complicated compared with a Kevorkian curette or an endocervical brush. The user end has a handle with a rotatable knob that transitions to a shaft with a flange at the end right before the sampling mechanism. To use the device, the sampling end is inserted into the endocervical canal up to the flange. The knob on the handle is then turned clockwise to open the sheath, thereby exposing sharp rigid plastic edges. The device is then rotated 360° clockwise and then 360° counterclockwise to “curette” the endocervical canal. Finally, the knob on the handle is turned counterclockwise to close the sheath and the device is removed. The specimen is then transferred to a standard vial for processing.
In my experience with its use, it actually exceeded my expectations. The device was easy to use, and the specimens were more than adequate. Truth be told, I came into the trial with a negative mindset having already convinced myself that this device was a waste of money given that doing an ECC with traditional methods is so straightforward. What I had not anticipated was the complete lack of patient discomfort when I used the FemCerv compared with a Kevorkian device.
Innovation. From an innovation standpoint, FemCerv is not super-disruptive technology, but it is well designed and pretty clever in that the opening and closing sheath prevents ectocervical cellular contamination, and the rotational sampling, rather than in-and-out sampling, does dramatically reduce the patient discomfort.
Summary. As I previously noted, before trying it, I did not anticipate liking FemCerv as much as I did. Does it add some non-reimbursable cost to a relatively low-reimbursing procedure? Absolutely. But it is not too expensive and, for me, making a painful procedure relatively painless is good value every time. I think all our patients would agree.
For more information, visit https://femasys.com/.
UPDATE
Hologic, Inc. announces that they received the following 2022 IMV ServiceTrakTM Awards for Mammography: Best Service, Best Customer Satisfaction, and Best System Performance. In addition, Hologic announces that their Affirm Contrast Biopsy software is commercially available in the United States. Tissue samples may be targeted and acquired using the Affirm Contrast Biopsy software from lesions identified using Hologic’s I-View Contrast Enhanced Mammography software. The latter software allows health care facilities an alternative to breast magnetic resonance imaging, which is used as supplemental imaging to mammography and/or ultrasonography.
For more information, visit https://www.hologic.com/
REVIEW
FEMCERV®: Well-designed technology that can minimize patient discomfort

The FemCerv® Endocervical Sampler, developed by Femasys, Inc (Suwanee, Georgia) expands options for colposcopy biopsy.
Background. In the United States, approximately 3 million women per year undergo colposcopic evaluation to work-up abnormal screening cytology. While some controversy exists regarding the exact role of endocervical curettage (ECC) within each age group and clinical situation, it is nonetheless an important component of the colposcopy-biopsy examination in many cases. For over a century, the 3 mm metal endocervical curette has been the primary tool employed to obtain the tissue sample from the endocervical canal. Unfortunately, sharp curettage with a metal curette can have inadequate sampling rates as high as 14%,1 it runs the risk of ectocervical contamination, and it is painful, with almost half the participants in one study rating the procedural pain 3 ̶ 5 out of 8 on a VAS scale.2 So, maybe there is a better way.
Design/Functionality. According to Femasys, the FemCerv® Endocervical Sampler was designed to be the better way of performing an endocervical curettage. FemCerv is a single-use sterile device that comes in a standard 13 F size as well as an 11 F size for the narrower/stenotic os. In truth, at first glance it looks pretty complicated compared with a Kevorkian curette or an endocervical brush. The user end has a handle with a rotatable knob that transitions to a shaft with a flange at the end right before the sampling mechanism. To use the device, the sampling end is inserted into the endocervical canal up to the flange. The knob on the handle is then turned clockwise to open the sheath, thereby exposing sharp rigid plastic edges. The device is then rotated 360° clockwise and then 360° counterclockwise to “curette” the endocervical canal. Finally, the knob on the handle is turned counterclockwise to close the sheath and the device is removed. The specimen is then transferred to a standard vial for processing.
In my experience with its use, it actually exceeded my expectations. The device was easy to use, and the specimens were more than adequate. Truth be told, I came into the trial with a negative mindset having already convinced myself that this device was a waste of money given that doing an ECC with traditional methods is so straightforward. What I had not anticipated was the complete lack of patient discomfort when I used the FemCerv compared with a Kevorkian device.
Innovation. From an innovation standpoint, FemCerv is not super-disruptive technology, but it is well designed and pretty clever in that the opening and closing sheath prevents ectocervical cellular contamination, and the rotational sampling, rather than in-and-out sampling, does dramatically reduce the patient discomfort.
Summary. As I previously noted, before trying it, I did not anticipate liking FemCerv as much as I did. Does it add some non-reimbursable cost to a relatively low-reimbursing procedure? Absolutely. But it is not too expensive and, for me, making a painful procedure relatively painless is good value every time. I think all our patients would agree.
For more information, visit https://femasys.com/.
UPDATE
Hologic, Inc. announces that they received the following 2022 IMV ServiceTrakTM Awards for Mammography: Best Service, Best Customer Satisfaction, and Best System Performance. In addition, Hologic announces that their Affirm Contrast Biopsy software is commercially available in the United States. Tissue samples may be targeted and acquired using the Affirm Contrast Biopsy software from lesions identified using Hologic’s I-View Contrast Enhanced Mammography software. The latter software allows health care facilities an alternative to breast magnetic resonance imaging, which is used as supplemental imaging to mammography and/or ultrasonography.
For more information, visit https://www.hologic.com/
- Damkjaer M, Laursen JB, Petersen LK, et al. Endocervical sampling in women with suspected cervical neoplasia: a systematic review and meta-analysis of diagnostic test accuracy studies. Am J Obstet Gynecol. 2022;227:839-848.e4. doi: 10.1016/j.ajog.2022.07.036.
- Goksedef BP, Api M, Kaya O, et al. Diagnostic accuracy of two endocervical sampling method: randomized controlled trial. Arch Gynecol Obstet. 2013;287:117-22. doi: 10.1007/s00404-012-2542-9.
- Damkjaer M, Laursen JB, Petersen LK, et al. Endocervical sampling in women with suspected cervical neoplasia: a systematic review and meta-analysis of diagnostic test accuracy studies. Am J Obstet Gynecol. 2022;227:839-848.e4. doi: 10.1016/j.ajog.2022.07.036.
- Goksedef BP, Api M, Kaya O, et al. Diagnostic accuracy of two endocervical sampling method: randomized controlled trial. Arch Gynecol Obstet. 2013;287:117-22. doi: 10.1007/s00404-012-2542-9.
Product updates and reviews
HEGENBERGER RETRACTOR: IS IT HELPFUL FOR PERINEAL REPAIR?
The Hegenberger Retractor, manufactured by Hegenberger Medical (Abingdon, United Kingdom) is available for purchase in the United States through Rocket Medical. A video that I find particularly useful for explaining its use is available here: https://www.youtube.com /watch?v=p-jilXgXZLY
Background. About 85% of women having a vaginal birth experience some form of perineal trauma, and 60% to 70% receive stitches for those spontaneous tears or intentional incisions. As such, repairing perineal lacerations is a requisite skill for all obstetricians and midwives, and every provider has developed exposure techniques to perform their suturing with the goals of good tissue re-approximation, efficiency, minimized patient discomfort, reduced blood loss, and safety from needle sticks. For several millennia, the most commonly used tissue retractor for these repairs has been one’s own fingers, or those of a colleague. While cost-effective and readily available, fingers do have drawbacks as a vaginal retractor. First, their use as a retractor precludes their use for other tasks. Second, their frequent need to be inserted and replaced (see drawback #1) can be uncomfortable for patients. Third, their limited surface area is often insufficient to appropriately provide adequate tissue retraction for optimal surgical site visualization. Finally, they get tired and typically do not appreciate being stuck with needles. Given all this, it is surprising that so many centuries have passed with so little innovation for this ubiquitous procedure. Fortunately, Danish midwife Malene Hegenberger thought now was a good time to change the status quo.
Design/Functionality. The Hegenberger Retractor is brilliant in its simplicity. Its unique molded plastic design is smooth, ergonomic, nonconductive, and packaged as a single-use sterile device. Amazingly, it has a near-perfect pliability balance, making it simultaneously easy to compress for insertion while providing enough retraction tension for good visualization once it has been reexpanded. The subtle ridges on the compression points are just enough to allow for a good grip, and the notches on the sides are a convenient addition for holding extra suture if needed. The device has been cleared by the US Food and Drug Administration (FDA) as a Class 1 device and is approved for sale in the United States. In my experience with its use, I thought it was easy to place and provided excellent exposure for the repairs I was doing. In fact, I thought it provided as good if not better exposure than what I would expect from a Gelpi retractor without any of the trauma the Gelpi adds with its pointed ends. Smile emoji!
Innovation. In the early 1800s, French midwifery pioneer Marie Boivin introduced a novel pelvimeter and a revolutionary 2-part speculum to the technology of the day. Why it took more than 200 years for the ideas of another cutting-edge midwife to breach the walls of the obstetric technological establishment remains a mystery, but fortunately it has been done. While seemingly obvious, the Hegenberger Retractor is the culmination of years of work and 88 prototypes. It looks simple, but the secret to its functionality is the precision with which each dimension and every curve was designed. The device has been cleared by the FDA as a Class 1 device and is approved for sale in the United States.
Summary. There are a lot of reasons to like the Hegenberger Retractor. I like it for its simplicity; I like it for its functionality; I like it for its ability to fill a real need. On the downside, I do not like that it is a single-use plastic device, and I am not happy about adding cost to obstetric care. Most of all, I hate that I did not invent it.
Is the Hegenberger Retractor going to be needed to repair every obstetric laceration? No. Will it provide perfect exposure to repair every obstetric laceration? Of course not. But it is an incredibly clever device that will be very helpful in many situations, and I suspect it will soon become a mainstay on most maternity units as it gains recognition.
FOR MORE INFORMATION, VISIT www.rocketmedical.com
- McCandlish R, Bowler U, van Asten H, et al. A randomised controlled trial of care of the perineum during second stage of normal labour. Br J Obstet Gynaecol. 1998;105:1262-1272.
- Ferry G. Marie Boivin: from midwife to gynaecologist. Lancet. 2019;393:2192-2193. doi: 10.1016/S0140-6736(19)31188-2.
HEGENBERGER RETRACTOR: IS IT HELPFUL FOR PERINEAL REPAIR?
The Hegenberger Retractor, manufactured by Hegenberger Medical (Abingdon, United Kingdom) is available for purchase in the United States through Rocket Medical. A video that I find particularly useful for explaining its use is available here: https://www.youtube.com /watch?v=p-jilXgXZLY
Background. About 85% of women having a vaginal birth experience some form of perineal trauma, and 60% to 70% receive stitches for those spontaneous tears or intentional incisions. As such, repairing perineal lacerations is a requisite skill for all obstetricians and midwives, and every provider has developed exposure techniques to perform their suturing with the goals of good tissue re-approximation, efficiency, minimized patient discomfort, reduced blood loss, and safety from needle sticks. For several millennia, the most commonly used tissue retractor for these repairs has been one’s own fingers, or those of a colleague. While cost-effective and readily available, fingers do have drawbacks as a vaginal retractor. First, their use as a retractor precludes their use for other tasks. Second, their frequent need to be inserted and replaced (see drawback #1) can be uncomfortable for patients. Third, their limited surface area is often insufficient to appropriately provide adequate tissue retraction for optimal surgical site visualization. Finally, they get tired and typically do not appreciate being stuck with needles. Given all this, it is surprising that so many centuries have passed with so little innovation for this ubiquitous procedure. Fortunately, Danish midwife Malene Hegenberger thought now was a good time to change the status quo.
Design/Functionality. The Hegenberger Retractor is brilliant in its simplicity. Its unique molded plastic design is smooth, ergonomic, nonconductive, and packaged as a single-use sterile device. Amazingly, it has a near-perfect pliability balance, making it simultaneously easy to compress for insertion while providing enough retraction tension for good visualization once it has been reexpanded. The subtle ridges on the compression points are just enough to allow for a good grip, and the notches on the sides are a convenient addition for holding extra suture if needed. The device has been cleared by the US Food and Drug Administration (FDA) as a Class 1 device and is approved for sale in the United States. In my experience with its use, I thought it was easy to place and provided excellent exposure for the repairs I was doing. In fact, I thought it provided as good if not better exposure than what I would expect from a Gelpi retractor without any of the trauma the Gelpi adds with its pointed ends. Smile emoji!
Innovation. In the early 1800s, French midwifery pioneer Marie Boivin introduced a novel pelvimeter and a revolutionary 2-part speculum to the technology of the day. Why it took more than 200 years for the ideas of another cutting-edge midwife to breach the walls of the obstetric technological establishment remains a mystery, but fortunately it has been done. While seemingly obvious, the Hegenberger Retractor is the culmination of years of work and 88 prototypes. It looks simple, but the secret to its functionality is the precision with which each dimension and every curve was designed. The device has been cleared by the FDA as a Class 1 device and is approved for sale in the United States.
Summary. There are a lot of reasons to like the Hegenberger Retractor. I like it for its simplicity; I like it for its functionality; I like it for its ability to fill a real need. On the downside, I do not like that it is a single-use plastic device, and I am not happy about adding cost to obstetric care. Most of all, I hate that I did not invent it.
Is the Hegenberger Retractor going to be needed to repair every obstetric laceration? No. Will it provide perfect exposure to repair every obstetric laceration? Of course not. But it is an incredibly clever device that will be very helpful in many situations, and I suspect it will soon become a mainstay on most maternity units as it gains recognition.
FOR MORE INFORMATION, VISIT www.rocketmedical.com
HEGENBERGER RETRACTOR: IS IT HELPFUL FOR PERINEAL REPAIR?
The Hegenberger Retractor, manufactured by Hegenberger Medical (Abingdon, United Kingdom) is available for purchase in the United States through Rocket Medical. A video that I find particularly useful for explaining its use is available here: https://www.youtube.com /watch?v=p-jilXgXZLY
Background. About 85% of women having a vaginal birth experience some form of perineal trauma, and 60% to 70% receive stitches for those spontaneous tears or intentional incisions. As such, repairing perineal lacerations is a requisite skill for all obstetricians and midwives, and every provider has developed exposure techniques to perform their suturing with the goals of good tissue re-approximation, efficiency, minimized patient discomfort, reduced blood loss, and safety from needle sticks. For several millennia, the most commonly used tissue retractor for these repairs has been one’s own fingers, or those of a colleague. While cost-effective and readily available, fingers do have drawbacks as a vaginal retractor. First, their use as a retractor precludes their use for other tasks. Second, their frequent need to be inserted and replaced (see drawback #1) can be uncomfortable for patients. Third, their limited surface area is often insufficient to appropriately provide adequate tissue retraction for optimal surgical site visualization. Finally, they get tired and typically do not appreciate being stuck with needles. Given all this, it is surprising that so many centuries have passed with so little innovation for this ubiquitous procedure. Fortunately, Danish midwife Malene Hegenberger thought now was a good time to change the status quo.
Design/Functionality. The Hegenberger Retractor is brilliant in its simplicity. Its unique molded plastic design is smooth, ergonomic, nonconductive, and packaged as a single-use sterile device. Amazingly, it has a near-perfect pliability balance, making it simultaneously easy to compress for insertion while providing enough retraction tension for good visualization once it has been reexpanded. The subtle ridges on the compression points are just enough to allow for a good grip, and the notches on the sides are a convenient addition for holding extra suture if needed. The device has been cleared by the US Food and Drug Administration (FDA) as a Class 1 device and is approved for sale in the United States. In my experience with its use, I thought it was easy to place and provided excellent exposure for the repairs I was doing. In fact, I thought it provided as good if not better exposure than what I would expect from a Gelpi retractor without any of the trauma the Gelpi adds with its pointed ends. Smile emoji!
Innovation. In the early 1800s, French midwifery pioneer Marie Boivin introduced a novel pelvimeter and a revolutionary 2-part speculum to the technology of the day. Why it took more than 200 years for the ideas of another cutting-edge midwife to breach the walls of the obstetric technological establishment remains a mystery, but fortunately it has been done. While seemingly obvious, the Hegenberger Retractor is the culmination of years of work and 88 prototypes. It looks simple, but the secret to its functionality is the precision with which each dimension and every curve was designed. The device has been cleared by the FDA as a Class 1 device and is approved for sale in the United States.
Summary. There are a lot of reasons to like the Hegenberger Retractor. I like it for its simplicity; I like it for its functionality; I like it for its ability to fill a real need. On the downside, I do not like that it is a single-use plastic device, and I am not happy about adding cost to obstetric care. Most of all, I hate that I did not invent it.
Is the Hegenberger Retractor going to be needed to repair every obstetric laceration? No. Will it provide perfect exposure to repair every obstetric laceration? Of course not. But it is an incredibly clever device that will be very helpful in many situations, and I suspect it will soon become a mainstay on most maternity units as it gains recognition.
FOR MORE INFORMATION, VISIT www.rocketmedical.com
- McCandlish R, Bowler U, van Asten H, et al. A randomised controlled trial of care of the perineum during second stage of normal labour. Br J Obstet Gynaecol. 1998;105:1262-1272.
- Ferry G. Marie Boivin: from midwife to gynaecologist. Lancet. 2019;393:2192-2193. doi: 10.1016/S0140-6736(19)31188-2.
- McCandlish R, Bowler U, van Asten H, et al. A randomised controlled trial of care of the perineum during second stage of normal labour. Br J Obstet Gynaecol. 1998;105:1262-1272.
- Ferry G. Marie Boivin: from midwife to gynaecologist. Lancet. 2019;393:2192-2193. doi: 10.1016/S0140-6736(19)31188-2.
Q Is routine episiotomy justified?
Expert Commentary
Consider this observation, now more than 100 years old:
Episiotomy… is practiced in the belief that the vulvar opening, if sufficiently enlarged by the incisions, will not tear farther, or that in any case the laceration will occur in the continuation of the incisions, whose clean-cut edges will heal more readily than the irregular spontaneous tears. Personally, I see no advantage in the procedure, as my experience is that ordinary perineal tears will heal almost uniformly if properly sutured and cared for.
—J. Whitridge Williams1
Since that opinion was published, many would claim, medicine has evolved from an anecdotal discipline to a more evidence-based science. Ironically, it has taken a systematic, evidence-based review of articles from a 54-year period to determine what Williams discerned anecdotally at the turn of the 20th century.
Details of the study
Hartmann et al reviewed 26 trials from 1950 to 2004, each of which included at least 40 participants. For short-term maternal outcomes, they restricted their review to randomized clinical trials. When long-term outcomes were assessed, they included nonrandomized trials and prospective cohorts.
Short-term outcomes included third- and fourth-degree lacerations, pain, wound healing, and blood loss. Long-term outcomes included incontinence, pelvic floor defects, and sexual function.
The findings: Immediate maternal outcomes were not improved with routine episiotomy. Though we lack long-term follow-up into the age range most likely to have pelvic floor sequelae, episiotomy does not appear to prevent fecal and urinary incontinence or pelvic floor relaxation, or to preserve sexual function.
A resounding chorus
These findings exactly mirror those of a Cochrane review by Carroli and Belizan.2 Both reviews make it clear that routine episiotomy is outdated.
While some uses for episiotomy remain—such as hastening delivery in the setting of a nonreassuring fetal tracing or shoulder dystocia—the procedure of incising the perineum prior to delivery of the baby’s head should be limited to indicated instances only and should never be performed routinely.
Expert Commentary
Consider this observation, now more than 100 years old:
Episiotomy… is practiced in the belief that the vulvar opening, if sufficiently enlarged by the incisions, will not tear farther, or that in any case the laceration will occur in the continuation of the incisions, whose clean-cut edges will heal more readily than the irregular spontaneous tears. Personally, I see no advantage in the procedure, as my experience is that ordinary perineal tears will heal almost uniformly if properly sutured and cared for.
—J. Whitridge Williams1
Since that opinion was published, many would claim, medicine has evolved from an anecdotal discipline to a more evidence-based science. Ironically, it has taken a systematic, evidence-based review of articles from a 54-year period to determine what Williams discerned anecdotally at the turn of the 20th century.
Details of the study
Hartmann et al reviewed 26 trials from 1950 to 2004, each of which included at least 40 participants. For short-term maternal outcomes, they restricted their review to randomized clinical trials. When long-term outcomes were assessed, they included nonrandomized trials and prospective cohorts.
Short-term outcomes included third- and fourth-degree lacerations, pain, wound healing, and blood loss. Long-term outcomes included incontinence, pelvic floor defects, and sexual function.
The findings: Immediate maternal outcomes were not improved with routine episiotomy. Though we lack long-term follow-up into the age range most likely to have pelvic floor sequelae, episiotomy does not appear to prevent fecal and urinary incontinence or pelvic floor relaxation, or to preserve sexual function.
A resounding chorus
These findings exactly mirror those of a Cochrane review by Carroli and Belizan.2 Both reviews make it clear that routine episiotomy is outdated.
While some uses for episiotomy remain—such as hastening delivery in the setting of a nonreassuring fetal tracing or shoulder dystocia—the procedure of incising the perineum prior to delivery of the baby’s head should be limited to indicated instances only and should never be performed routinely.
Expert Commentary
Consider this observation, now more than 100 years old:
Episiotomy… is practiced in the belief that the vulvar opening, if sufficiently enlarged by the incisions, will not tear farther, or that in any case the laceration will occur in the continuation of the incisions, whose clean-cut edges will heal more readily than the irregular spontaneous tears. Personally, I see no advantage in the procedure, as my experience is that ordinary perineal tears will heal almost uniformly if properly sutured and cared for.
—J. Whitridge Williams1
Since that opinion was published, many would claim, medicine has evolved from an anecdotal discipline to a more evidence-based science. Ironically, it has taken a systematic, evidence-based review of articles from a 54-year period to determine what Williams discerned anecdotally at the turn of the 20th century.
Details of the study
Hartmann et al reviewed 26 trials from 1950 to 2004, each of which included at least 40 participants. For short-term maternal outcomes, they restricted their review to randomized clinical trials. When long-term outcomes were assessed, they included nonrandomized trials and prospective cohorts.
Short-term outcomes included third- and fourth-degree lacerations, pain, wound healing, and blood loss. Long-term outcomes included incontinence, pelvic floor defects, and sexual function.
The findings: Immediate maternal outcomes were not improved with routine episiotomy. Though we lack long-term follow-up into the age range most likely to have pelvic floor sequelae, episiotomy does not appear to prevent fecal and urinary incontinence or pelvic floor relaxation, or to preserve sexual function.
A resounding chorus
These findings exactly mirror those of a Cochrane review by Carroli and Belizan.2 Both reviews make it clear that routine episiotomy is outdated.
While some uses for episiotomy remain—such as hastening delivery in the setting of a nonreassuring fetal tracing or shoulder dystocia—the procedure of incising the perineum prior to delivery of the baby’s head should be limited to indicated instances only and should never be performed routinely.
Pearls on the best suture for episiotomy
- Plain catgut produces the highest inflammatory response of all suture materials.
- Synthetic sutures have a higher incidence of suture removal than plain or chromic catgut.
- Synthetic materials are associated with less short-term pain, a reduction in the use of analgesia, and less wound dehiscence than natural fibers.
What’s the best suture material? Technological advances mean there are more suture materials available for perineum repair. In the first edition of Williams’ Obstetrics, the authors opined that silkworm gut accompanied by plain catgut was the ideal suture choice.1 A few years later, carbolized catgut was recommended for perineal repairs.2 Today, chromic catgut remains the standard of choice, with polyglycolic acid sutures offered as a possible alternative.3,4
When considering sutures for episiotomies, I focus on 2 characteristics: strength and inflammation-inducing properties. (For the purposes of this article, perineal lacerations are defined as natural tears or episiotomies confined to the perineum and not involving the anal sphincter or rectum.)
Strength. Because of increased blood flow to the perineum during pregnancy, most perineal lacerations heal in 7 to 14 days.5 Therefore, the suture material must maintain adequate tensile strength for that amount of time. Permanent sutures or those with prolonged resorption rates cause pain and should be avoided.
Inflammation-inducing properties. As with any foreign body, the suture material interacts with the immune system and results in an inflammatory response, which involves infiltration of the affected tissues by polymorphonucleocytes, lymphocytes, monocytes, and macrophagocytes. The degree of local inflammation is directly related to the pain response: the greater the inflammation, the greater the pain.
That said, I believe the “perfect” suture material should maintain tensile strength from 7 to 14 days and dissolve quickly thereafter. In addition, it should cause as little inflammation as possible.
Choosing from what’s available. Generally, suture materials are classified as nonabsorbable and absorbable and then subclassified into natural and synthetic fibers. Within these classifications, sutures have different tensile strengths and reabsorption rates. Since nonabsorbable sutures have no place in postpartum perineal laceration repairs, I will focus only on options in absorbable materials.
Natural fibers include plain catgut and chromic catgut, while polyglycolic acid, coated polyglycolic-910, and pretreated coated polyglactin-910 round out synthetic choices.
Natural Fibers
Plain catgut. Produced from the collagen of the submucosal layer of a sheep’s small intestines or the serosal layer of cattle intestines, this material is chemically treated with formaldehyde to resist enzymatic degradation.
- Mechanism by which it is absorbed: proteolytic enzymes and phagocytosis
- Tensile strength (00 size): 7 lb, losing half of its strength in 4 to 6 days
- Degree of inflammatory response: highest of all suture material6
- Absorption rate: 70 days
Chromic catgut. Like plain catgut, this material is produced from sheep or cow intestines but is coated with chromium to delay degradation.
- Mechanism by which it is absorbed: proteolytic enzymes and phagocytosis
- Tensile strength (00 size): 8 lb, losing half of its strength in 10 to 14 days
- Degree of inflammatory response: high
- Absorption rate: 90 days
Synthetic Fibers
Polyglycolic acid and coated polyglactin-910. Produced by polymerization of glycolic acid, these suture materials are extruded, stretched, and braided into various sizes. The sutures are further coated with silicone to improve their handling characteristics.
- Mechanism by which they are absorbed: hydrolysis
- Tensile strength (00 size): 9.6 lb, losing half of their strength in approximately 21 days
- Degree of inflammatory response: low6
- Absorption rate: 60 to 90 days7,8
Pretreated coated polyglactin-910. This suture is pretreated with ionizing beams to accelerate hydrolysis.
- Mechanism by which it is absorbed: hydrolysis
- Tensile strength (00 size): 9.9 lb, losing half of its strength in 5 days
- Degree of inflammatory response: low
- Absorption rate: 42 days8
Quick study of the evidence. The physiologic characteristics of wound healing after vaginal delivery would seem to dictate the use of glycolic acid-derived sutures for perineal repairs. Recently, this conclusion was echoed by Kettle and Johanson in the Cochrane Database of Systematic Reviews. The authors revisited 8 randomized trials that compared absorbable synthetic sutures with plain or chromic catgut. After an in-depth analysis of the methodology and results of each study, they concluded there was significant evidence that synthetic materials are associated with less short-term pain, a reduction in the use of analgesia, and less wound dehiscence than natural fibers. One caveat: Synthetic sutures were associated with increased rates of suture removal in some patients because the materials were too long-lasting.9
The bottom line. To my mind, the ideal suture material is pretreated coated polyglactin-910. Since it is chemically identical to polyglactin-910, it is reasonable to assume that it has a similar favorable pain profile. Furthermore, because it is completely absorbed within 42 days, a patient will not encounter the persistent suture problem present with polyglycolic acid and polyglactin-910. I have been using this suture for 6 years and have found that it is easier to work with than chromic catgut and well tolerated by my patients. While well-designed, randomized clinical trials are needed to prove the suture’s effectiveness, available data suggest it is currently an obstetrician’s best choice.
The author reports no financial relationship with any companies whose products are mentioned in this article.
1. Williams J. Obstetrics. 1st ed. New York, NY: D. Appleton and Company; 1903;295.-
2. Williams J. Obstetrics. 2nd ed. New York, NY: D. Appleton and Company; 1908.
3. Conduct of Normal Labor and Delivery. In: Cunningham FG, MacDonald PC, Gant N, et al, eds. Williams Obstetrics. 21st ed. New York, NY: McGraw-Hill; 2001;328.-
4. Conduct of Normal Labor and Delivery. In: Cunningham FG, MacDonald PC, Gant N, et al, eds. Williams Obstetrics. 19th ed. Norwalk, Conn: Appleton & Lange; 1993;391.-
5. Van Winkle W, Hastings JC. Considerations in the choice of suture material for various tissues. Surgery, Gynecology & Obstetrics. 1972;135:115.-
6. Hardy J. Hardy’s Textbook of Surgery. 2nd ed. Philadelphia, Pa: J.B. Lippincott Company; 1988;119.-
7. U.S. Surgical Web site. Available at: http://www.ussdgsutures.com. Accessed March 7, 2002.
8. Ethicon Products. Johnson & Johnson Web site. Available at: http://www.jnjgateway.com/home/jtml?loc+USENG. Accessed March 7, 2002.
9. Kettle C, Johanson RB. Absorbable synthetic versus catgut suture material for perineal repair. In: The Cochrane Database of Systematic Reviews. 2001;3.
- Plain catgut produces the highest inflammatory response of all suture materials.
- Synthetic sutures have a higher incidence of suture removal than plain or chromic catgut.
- Synthetic materials are associated with less short-term pain, a reduction in the use of analgesia, and less wound dehiscence than natural fibers.
What’s the best suture material? Technological advances mean there are more suture materials available for perineum repair. In the first edition of Williams’ Obstetrics, the authors opined that silkworm gut accompanied by plain catgut was the ideal suture choice.1 A few years later, carbolized catgut was recommended for perineal repairs.2 Today, chromic catgut remains the standard of choice, with polyglycolic acid sutures offered as a possible alternative.3,4
When considering sutures for episiotomies, I focus on 2 characteristics: strength and inflammation-inducing properties. (For the purposes of this article, perineal lacerations are defined as natural tears or episiotomies confined to the perineum and not involving the anal sphincter or rectum.)
Strength. Because of increased blood flow to the perineum during pregnancy, most perineal lacerations heal in 7 to 14 days.5 Therefore, the suture material must maintain adequate tensile strength for that amount of time. Permanent sutures or those with prolonged resorption rates cause pain and should be avoided.
Inflammation-inducing properties. As with any foreign body, the suture material interacts with the immune system and results in an inflammatory response, which involves infiltration of the affected tissues by polymorphonucleocytes, lymphocytes, monocytes, and macrophagocytes. The degree of local inflammation is directly related to the pain response: the greater the inflammation, the greater the pain.
That said, I believe the “perfect” suture material should maintain tensile strength from 7 to 14 days and dissolve quickly thereafter. In addition, it should cause as little inflammation as possible.
Choosing from what’s available. Generally, suture materials are classified as nonabsorbable and absorbable and then subclassified into natural and synthetic fibers. Within these classifications, sutures have different tensile strengths and reabsorption rates. Since nonabsorbable sutures have no place in postpartum perineal laceration repairs, I will focus only on options in absorbable materials.
Natural fibers include plain catgut and chromic catgut, while polyglycolic acid, coated polyglycolic-910, and pretreated coated polyglactin-910 round out synthetic choices.
Natural Fibers
Plain catgut. Produced from the collagen of the submucosal layer of a sheep’s small intestines or the serosal layer of cattle intestines, this material is chemically treated with formaldehyde to resist enzymatic degradation.
- Mechanism by which it is absorbed: proteolytic enzymes and phagocytosis
- Tensile strength (00 size): 7 lb, losing half of its strength in 4 to 6 days
- Degree of inflammatory response: highest of all suture material6
- Absorption rate: 70 days
Chromic catgut. Like plain catgut, this material is produced from sheep or cow intestines but is coated with chromium to delay degradation.
- Mechanism by which it is absorbed: proteolytic enzymes and phagocytosis
- Tensile strength (00 size): 8 lb, losing half of its strength in 10 to 14 days
- Degree of inflammatory response: high
- Absorption rate: 90 days
Synthetic Fibers
Polyglycolic acid and coated polyglactin-910. Produced by polymerization of glycolic acid, these suture materials are extruded, stretched, and braided into various sizes. The sutures are further coated with silicone to improve their handling characteristics.
- Mechanism by which they are absorbed: hydrolysis
- Tensile strength (00 size): 9.6 lb, losing half of their strength in approximately 21 days
- Degree of inflammatory response: low6
- Absorption rate: 60 to 90 days7,8
Pretreated coated polyglactin-910. This suture is pretreated with ionizing beams to accelerate hydrolysis.
- Mechanism by which it is absorbed: hydrolysis
- Tensile strength (00 size): 9.9 lb, losing half of its strength in 5 days
- Degree of inflammatory response: low
- Absorption rate: 42 days8
Quick study of the evidence. The physiologic characteristics of wound healing after vaginal delivery would seem to dictate the use of glycolic acid-derived sutures for perineal repairs. Recently, this conclusion was echoed by Kettle and Johanson in the Cochrane Database of Systematic Reviews. The authors revisited 8 randomized trials that compared absorbable synthetic sutures with plain or chromic catgut. After an in-depth analysis of the methodology and results of each study, they concluded there was significant evidence that synthetic materials are associated with less short-term pain, a reduction in the use of analgesia, and less wound dehiscence than natural fibers. One caveat: Synthetic sutures were associated with increased rates of suture removal in some patients because the materials were too long-lasting.9
The bottom line. To my mind, the ideal suture material is pretreated coated polyglactin-910. Since it is chemically identical to polyglactin-910, it is reasonable to assume that it has a similar favorable pain profile. Furthermore, because it is completely absorbed within 42 days, a patient will not encounter the persistent suture problem present with polyglycolic acid and polyglactin-910. I have been using this suture for 6 years and have found that it is easier to work with than chromic catgut and well tolerated by my patients. While well-designed, randomized clinical trials are needed to prove the suture’s effectiveness, available data suggest it is currently an obstetrician’s best choice.
The author reports no financial relationship with any companies whose products are mentioned in this article.
- Plain catgut produces the highest inflammatory response of all suture materials.
- Synthetic sutures have a higher incidence of suture removal than plain or chromic catgut.
- Synthetic materials are associated with less short-term pain, a reduction in the use of analgesia, and less wound dehiscence than natural fibers.
What’s the best suture material? Technological advances mean there are more suture materials available for perineum repair. In the first edition of Williams’ Obstetrics, the authors opined that silkworm gut accompanied by plain catgut was the ideal suture choice.1 A few years later, carbolized catgut was recommended for perineal repairs.2 Today, chromic catgut remains the standard of choice, with polyglycolic acid sutures offered as a possible alternative.3,4
When considering sutures for episiotomies, I focus on 2 characteristics: strength and inflammation-inducing properties. (For the purposes of this article, perineal lacerations are defined as natural tears or episiotomies confined to the perineum and not involving the anal sphincter or rectum.)
Strength. Because of increased blood flow to the perineum during pregnancy, most perineal lacerations heal in 7 to 14 days.5 Therefore, the suture material must maintain adequate tensile strength for that amount of time. Permanent sutures or those with prolonged resorption rates cause pain and should be avoided.
Inflammation-inducing properties. As with any foreign body, the suture material interacts with the immune system and results in an inflammatory response, which involves infiltration of the affected tissues by polymorphonucleocytes, lymphocytes, monocytes, and macrophagocytes. The degree of local inflammation is directly related to the pain response: the greater the inflammation, the greater the pain.
That said, I believe the “perfect” suture material should maintain tensile strength from 7 to 14 days and dissolve quickly thereafter. In addition, it should cause as little inflammation as possible.
Choosing from what’s available. Generally, suture materials are classified as nonabsorbable and absorbable and then subclassified into natural and synthetic fibers. Within these classifications, sutures have different tensile strengths and reabsorption rates. Since nonabsorbable sutures have no place in postpartum perineal laceration repairs, I will focus only on options in absorbable materials.
Natural fibers include plain catgut and chromic catgut, while polyglycolic acid, coated polyglycolic-910, and pretreated coated polyglactin-910 round out synthetic choices.
Natural Fibers
Plain catgut. Produced from the collagen of the submucosal layer of a sheep’s small intestines or the serosal layer of cattle intestines, this material is chemically treated with formaldehyde to resist enzymatic degradation.
- Mechanism by which it is absorbed: proteolytic enzymes and phagocytosis
- Tensile strength (00 size): 7 lb, losing half of its strength in 4 to 6 days
- Degree of inflammatory response: highest of all suture material6
- Absorption rate: 70 days
Chromic catgut. Like plain catgut, this material is produced from sheep or cow intestines but is coated with chromium to delay degradation.
- Mechanism by which it is absorbed: proteolytic enzymes and phagocytosis
- Tensile strength (00 size): 8 lb, losing half of its strength in 10 to 14 days
- Degree of inflammatory response: high
- Absorption rate: 90 days
Synthetic Fibers
Polyglycolic acid and coated polyglactin-910. Produced by polymerization of glycolic acid, these suture materials are extruded, stretched, and braided into various sizes. The sutures are further coated with silicone to improve their handling characteristics.
- Mechanism by which they are absorbed: hydrolysis
- Tensile strength (00 size): 9.6 lb, losing half of their strength in approximately 21 days
- Degree of inflammatory response: low6
- Absorption rate: 60 to 90 days7,8
Pretreated coated polyglactin-910. This suture is pretreated with ionizing beams to accelerate hydrolysis.
- Mechanism by which it is absorbed: hydrolysis
- Tensile strength (00 size): 9.9 lb, losing half of its strength in 5 days
- Degree of inflammatory response: low
- Absorption rate: 42 days8
Quick study of the evidence. The physiologic characteristics of wound healing after vaginal delivery would seem to dictate the use of glycolic acid-derived sutures for perineal repairs. Recently, this conclusion was echoed by Kettle and Johanson in the Cochrane Database of Systematic Reviews. The authors revisited 8 randomized trials that compared absorbable synthetic sutures with plain or chromic catgut. After an in-depth analysis of the methodology and results of each study, they concluded there was significant evidence that synthetic materials are associated with less short-term pain, a reduction in the use of analgesia, and less wound dehiscence than natural fibers. One caveat: Synthetic sutures were associated with increased rates of suture removal in some patients because the materials were too long-lasting.9
The bottom line. To my mind, the ideal suture material is pretreated coated polyglactin-910. Since it is chemically identical to polyglactin-910, it is reasonable to assume that it has a similar favorable pain profile. Furthermore, because it is completely absorbed within 42 days, a patient will not encounter the persistent suture problem present with polyglycolic acid and polyglactin-910. I have been using this suture for 6 years and have found that it is easier to work with than chromic catgut and well tolerated by my patients. While well-designed, randomized clinical trials are needed to prove the suture’s effectiveness, available data suggest it is currently an obstetrician’s best choice.
The author reports no financial relationship with any companies whose products are mentioned in this article.
1. Williams J. Obstetrics. 1st ed. New York, NY: D. Appleton and Company; 1903;295.-
2. Williams J. Obstetrics. 2nd ed. New York, NY: D. Appleton and Company; 1908.
3. Conduct of Normal Labor and Delivery. In: Cunningham FG, MacDonald PC, Gant N, et al, eds. Williams Obstetrics. 21st ed. New York, NY: McGraw-Hill; 2001;328.-
4. Conduct of Normal Labor and Delivery. In: Cunningham FG, MacDonald PC, Gant N, et al, eds. Williams Obstetrics. 19th ed. Norwalk, Conn: Appleton & Lange; 1993;391.-
5. Van Winkle W, Hastings JC. Considerations in the choice of suture material for various tissues. Surgery, Gynecology & Obstetrics. 1972;135:115.-
6. Hardy J. Hardy’s Textbook of Surgery. 2nd ed. Philadelphia, Pa: J.B. Lippincott Company; 1988;119.-
7. U.S. Surgical Web site. Available at: http://www.ussdgsutures.com. Accessed March 7, 2002.
8. Ethicon Products. Johnson & Johnson Web site. Available at: http://www.jnjgateway.com/home/jtml?loc+USENG. Accessed March 7, 2002.
9. Kettle C, Johanson RB. Absorbable synthetic versus catgut suture material for perineal repair. In: The Cochrane Database of Systematic Reviews. 2001;3.
1. Williams J. Obstetrics. 1st ed. New York, NY: D. Appleton and Company; 1903;295.-
2. Williams J. Obstetrics. 2nd ed. New York, NY: D. Appleton and Company; 1908.
3. Conduct of Normal Labor and Delivery. In: Cunningham FG, MacDonald PC, Gant N, et al, eds. Williams Obstetrics. 21st ed. New York, NY: McGraw-Hill; 2001;328.-
4. Conduct of Normal Labor and Delivery. In: Cunningham FG, MacDonald PC, Gant N, et al, eds. Williams Obstetrics. 19th ed. Norwalk, Conn: Appleton & Lange; 1993;391.-
5. Van Winkle W, Hastings JC. Considerations in the choice of suture material for various tissues. Surgery, Gynecology & Obstetrics. 1972;135:115.-
6. Hardy J. Hardy’s Textbook of Surgery. 2nd ed. Philadelphia, Pa: J.B. Lippincott Company; 1988;119.-
7. U.S. Surgical Web site. Available at: http://www.ussdgsutures.com. Accessed March 7, 2002.
8. Ethicon Products. Johnson & Johnson Web site. Available at: http://www.jnjgateway.com/home/jtml?loc+USENG. Accessed March 7, 2002.
9. Kettle C, Johanson RB. Absorbable synthetic versus catgut suture material for perineal repair. In: The Cochrane Database of Systematic Reviews. 2001;3.