User login
Idelalisib approved to treat CLL, FL in EU

The European Commission has granted marketing authorization for the PI3K delta inhibitor idelalisib (Zydelig) to treat chronic lymphocytic leukemia (CLL) and follicular lymphoma (FL) in the European Union.
The drug is now approved for use in combination with rituximab for CLL patients who have received at least 1 prior therapy or as first-line treatment in CLL patients who have 17p deletion or TP53 mutation and are not eligible for chemo-immunotherapy.
Idelalisib is also approved as monotherapy for FL patients who were refractory to 2 prior lines of treatment.
These approvals are based on data from 2 clinical trials—Study 116 and Study 101-09.
Study 116: Idelalisib in CLL
This phase 3 trial was stopped early because idelalisib had a significant impact on progression-free survival.
The study included 220 CLL patients who could not receive chemotherapy. Half were randomized to receive idelalisib plus rituximab, and the other half were randomized to rituximab plus placebo.
Patients in the rituximab-idelalisib arm had a much higher overall response rate than patients in the rituximab-placebo arm—81% and 13%, respectively (P<0.001). There were no complete responses.
At 24 weeks, the rate of progression-free survival was 93% in the rituximab-idelalisib arm and 46% in the rituximab-placebo arm (P<0.001). The median progression-free survival was 5.5 months in the rituximab-placebo arm and not reached in the rituximab-idelalisib arm (P<0.001).
At 12 months, the overall survival rate was 92% in the rituximab-idelalisib arm and 80% in the rituximab-placebo arm (P=0.02).
Most adverse events, in either treatment arm, were grade 2 or lower. The most common events in the rituximab-idelalisib arm were pyrexia, fatigue, nausea, chills, and diarrhea. In the rituximab-placebo arm, the most common events were infusion-related reactions, fatigue, cough, nausea, and dyspnea.
There were more serious adverse events in the rituximab-idelalisib arm than in the rituximab-placebo arm—40% and 35%, respectively. The most frequent serious events were pneumonia, pyrexia, and febrile neutropenia (in both treatment arms).
Study 101-09: Idelalisib in FL
This phase 2 trial enrolled 125 patients with indolent non-Hodgkin lymphoma who were refractory to rituximab and chemotherapy containing an alkylating agent. Patients received idelalisib monotherapy.
Of the 72 subjects with FL, 54% achieved a response, and 8% had a complete response. The median duration of response was not reached (range, 0-14.8 months).
Improvements in survival or disease-related symptoms have not been established.
In all patients, the most common grade 3 or higher adverse events were neutropenia (27%), elevations in aminotransferase levels (13%), diarrhea (13%), and pneumonia (7%).
Idelalisib is under development by Gilead Sciences. The drug is already approved in the US for the aforementioned indications, as well as to treat small lymphocytic lymphoma. ![]()

The European Commission has granted marketing authorization for the PI3K delta inhibitor idelalisib (Zydelig) to treat chronic lymphocytic leukemia (CLL) and follicular lymphoma (FL) in the European Union.
The drug is now approved for use in combination with rituximab for CLL patients who have received at least 1 prior therapy or as first-line treatment in CLL patients who have 17p deletion or TP53 mutation and are not eligible for chemo-immunotherapy.
Idelalisib is also approved as monotherapy for FL patients who were refractory to 2 prior lines of treatment.
These approvals are based on data from 2 clinical trials—Study 116 and Study 101-09.
Study 116: Idelalisib in CLL
This phase 3 trial was stopped early because idelalisib had a significant impact on progression-free survival.
The study included 220 CLL patients who could not receive chemotherapy. Half were randomized to receive idelalisib plus rituximab, and the other half were randomized to rituximab plus placebo.
Patients in the rituximab-idelalisib arm had a much higher overall response rate than patients in the rituximab-placebo arm—81% and 13%, respectively (P<0.001). There were no complete responses.
At 24 weeks, the rate of progression-free survival was 93% in the rituximab-idelalisib arm and 46% in the rituximab-placebo arm (P<0.001). The median progression-free survival was 5.5 months in the rituximab-placebo arm and not reached in the rituximab-idelalisib arm (P<0.001).
At 12 months, the overall survival rate was 92% in the rituximab-idelalisib arm and 80% in the rituximab-placebo arm (P=0.02).
Most adverse events, in either treatment arm, were grade 2 or lower. The most common events in the rituximab-idelalisib arm were pyrexia, fatigue, nausea, chills, and diarrhea. In the rituximab-placebo arm, the most common events were infusion-related reactions, fatigue, cough, nausea, and dyspnea.
There were more serious adverse events in the rituximab-idelalisib arm than in the rituximab-placebo arm—40% and 35%, respectively. The most frequent serious events were pneumonia, pyrexia, and febrile neutropenia (in both treatment arms).
Study 101-09: Idelalisib in FL
This phase 2 trial enrolled 125 patients with indolent non-Hodgkin lymphoma who were refractory to rituximab and chemotherapy containing an alkylating agent. Patients received idelalisib monotherapy.
Of the 72 subjects with FL, 54% achieved a response, and 8% had a complete response. The median duration of response was not reached (range, 0-14.8 months).
Improvements in survival or disease-related symptoms have not been established.
In all patients, the most common grade 3 or higher adverse events were neutropenia (27%), elevations in aminotransferase levels (13%), diarrhea (13%), and pneumonia (7%).
Idelalisib is under development by Gilead Sciences. The drug is already approved in the US for the aforementioned indications, as well as to treat small lymphocytic lymphoma. ![]()

The European Commission has granted marketing authorization for the PI3K delta inhibitor idelalisib (Zydelig) to treat chronic lymphocytic leukemia (CLL) and follicular lymphoma (FL) in the European Union.
The drug is now approved for use in combination with rituximab for CLL patients who have received at least 1 prior therapy or as first-line treatment in CLL patients who have 17p deletion or TP53 mutation and are not eligible for chemo-immunotherapy.
Idelalisib is also approved as monotherapy for FL patients who were refractory to 2 prior lines of treatment.
These approvals are based on data from 2 clinical trials—Study 116 and Study 101-09.
Study 116: Idelalisib in CLL
This phase 3 trial was stopped early because idelalisib had a significant impact on progression-free survival.
The study included 220 CLL patients who could not receive chemotherapy. Half were randomized to receive idelalisib plus rituximab, and the other half were randomized to rituximab plus placebo.
Patients in the rituximab-idelalisib arm had a much higher overall response rate than patients in the rituximab-placebo arm—81% and 13%, respectively (P<0.001). There were no complete responses.
At 24 weeks, the rate of progression-free survival was 93% in the rituximab-idelalisib arm and 46% in the rituximab-placebo arm (P<0.001). The median progression-free survival was 5.5 months in the rituximab-placebo arm and not reached in the rituximab-idelalisib arm (P<0.001).
At 12 months, the overall survival rate was 92% in the rituximab-idelalisib arm and 80% in the rituximab-placebo arm (P=0.02).
Most adverse events, in either treatment arm, were grade 2 or lower. The most common events in the rituximab-idelalisib arm were pyrexia, fatigue, nausea, chills, and diarrhea. In the rituximab-placebo arm, the most common events were infusion-related reactions, fatigue, cough, nausea, and dyspnea.
There were more serious adverse events in the rituximab-idelalisib arm than in the rituximab-placebo arm—40% and 35%, respectively. The most frequent serious events were pneumonia, pyrexia, and febrile neutropenia (in both treatment arms).
Study 101-09: Idelalisib in FL
This phase 2 trial enrolled 125 patients with indolent non-Hodgkin lymphoma who were refractory to rituximab and chemotherapy containing an alkylating agent. Patients received idelalisib monotherapy.
Of the 72 subjects with FL, 54% achieved a response, and 8% had a complete response. The median duration of response was not reached (range, 0-14.8 months).
Improvements in survival or disease-related symptoms have not been established.
In all patients, the most common grade 3 or higher adverse events were neutropenia (27%), elevations in aminotransferase levels (13%), diarrhea (13%), and pneumonia (7%).
Idelalisib is under development by Gilead Sciences. The drug is already approved in the US for the aforementioned indications, as well as to treat small lymphocytic lymphoma. ![]()
Predicting chemo drugs’ effects on male fertility

Credit: Rhoda Baer
A mathematical formula may help physicians predict which cancer survivors are likely to have normal sperm production following chemotherapy with alkylating agents.
Researchers developed the formula to calculate survivors’ cumulative treatment exposure to alkylating agents as a cyclophosphamide-equivalent dose (CED).
The team used this formula to evaluate a cohort of cancer survivors and found that CEDs of 4 g/m2 or less were associated with normal sperm concentrations.
An account of this research was published in The Lancet Oncology.
“Based on these results, we would recommend pretreatment fertility preservation be offered, whenever clinically possible, to any male whose projected treatment is expected to include a cyclophosphamide-equivalent dose greater than 4 g/m2,” said study author Daniel Green, MD, of St Jude Children’s Research Hospital in Memphis, Tennessee.
Dr Green and his colleagues had studied 214 male survivors of childhood cancer who had a median age of 29. Subjects had received cyclophosphamide and other alkylating agents, but their treatment did not include radiation.
The researchers performed semen analysis in the survivors a median of 21 years from their diagnosis. The analysis showed that 47.6% of survivors had normal sperm concentrations (at least 15 million per milliliter), 27.6% had low sperm counts, and 24.8% produced no sperm.
To determine the impact of alkylating agents on the survivors’ sperm production, the researchers calculated each survivor’s cumulative treatment exposure as a CED.
They did this using the following formula: CED (mg/m2)= 1.0 (cumulative cyclophosphamide dose [mg/m2]) + 0.244 (cumulative ifosfamide dose [mg/m2]) + 0.857 (cumulative procarbazine dose [mg/m2]) + 14.286 (cumulative chlorambucil dose [mg/m2]) + 15.0 (cumulative carmustine dose [mg/m2]) + 16.0 (cumulative lomustine dose [mg/m2]) + 40 (cumulative melphalan dose [mg/m2]) + 50 (cumulative thiotepa dose [mg/m2]) + 100 cumulative chlormethine dose [mg/m2]) + 8.823 (cumulative busulfan dose [mg/m2]).
The researchers could not identify a uniformly safe or toxic dose of these drugs, but they found that survivor sperm concentrations generally decreased as cumulative exposure to alkylating agents increased.
And CEDs of 4 g/m2 or less were associated with normal sperm concentrations. Almost 89% of survivors whose CED was 4 g/m2 or less had a normal sperm count. Their sperm were also more likely than sperm from other survivors to look and behave normally.
Dr Green did note that, although a lower cumulative dose of alkylating agents was associated with normal sperm production, outcomes for individual patients were unpredictable and varied. ![]()

Credit: Rhoda Baer
A mathematical formula may help physicians predict which cancer survivors are likely to have normal sperm production following chemotherapy with alkylating agents.
Researchers developed the formula to calculate survivors’ cumulative treatment exposure to alkylating agents as a cyclophosphamide-equivalent dose (CED).
The team used this formula to evaluate a cohort of cancer survivors and found that CEDs of 4 g/m2 or less were associated with normal sperm concentrations.
An account of this research was published in The Lancet Oncology.
“Based on these results, we would recommend pretreatment fertility preservation be offered, whenever clinically possible, to any male whose projected treatment is expected to include a cyclophosphamide-equivalent dose greater than 4 g/m2,” said study author Daniel Green, MD, of St Jude Children’s Research Hospital in Memphis, Tennessee.
Dr Green and his colleagues had studied 214 male survivors of childhood cancer who had a median age of 29. Subjects had received cyclophosphamide and other alkylating agents, but their treatment did not include radiation.
The researchers performed semen analysis in the survivors a median of 21 years from their diagnosis. The analysis showed that 47.6% of survivors had normal sperm concentrations (at least 15 million per milliliter), 27.6% had low sperm counts, and 24.8% produced no sperm.
To determine the impact of alkylating agents on the survivors’ sperm production, the researchers calculated each survivor’s cumulative treatment exposure as a CED.
They did this using the following formula: CED (mg/m2)= 1.0 (cumulative cyclophosphamide dose [mg/m2]) + 0.244 (cumulative ifosfamide dose [mg/m2]) + 0.857 (cumulative procarbazine dose [mg/m2]) + 14.286 (cumulative chlorambucil dose [mg/m2]) + 15.0 (cumulative carmustine dose [mg/m2]) + 16.0 (cumulative lomustine dose [mg/m2]) + 40 (cumulative melphalan dose [mg/m2]) + 50 (cumulative thiotepa dose [mg/m2]) + 100 cumulative chlormethine dose [mg/m2]) + 8.823 (cumulative busulfan dose [mg/m2]).
The researchers could not identify a uniformly safe or toxic dose of these drugs, but they found that survivor sperm concentrations generally decreased as cumulative exposure to alkylating agents increased.
And CEDs of 4 g/m2 or less were associated with normal sperm concentrations. Almost 89% of survivors whose CED was 4 g/m2 or less had a normal sperm count. Their sperm were also more likely than sperm from other survivors to look and behave normally.
Dr Green did note that, although a lower cumulative dose of alkylating agents was associated with normal sperm production, outcomes for individual patients were unpredictable and varied. ![]()

Credit: Rhoda Baer
A mathematical formula may help physicians predict which cancer survivors are likely to have normal sperm production following chemotherapy with alkylating agents.
Researchers developed the formula to calculate survivors’ cumulative treatment exposure to alkylating agents as a cyclophosphamide-equivalent dose (CED).
The team used this formula to evaluate a cohort of cancer survivors and found that CEDs of 4 g/m2 or less were associated with normal sperm concentrations.
An account of this research was published in The Lancet Oncology.
“Based on these results, we would recommend pretreatment fertility preservation be offered, whenever clinically possible, to any male whose projected treatment is expected to include a cyclophosphamide-equivalent dose greater than 4 g/m2,” said study author Daniel Green, MD, of St Jude Children’s Research Hospital in Memphis, Tennessee.
Dr Green and his colleagues had studied 214 male survivors of childhood cancer who had a median age of 29. Subjects had received cyclophosphamide and other alkylating agents, but their treatment did not include radiation.
The researchers performed semen analysis in the survivors a median of 21 years from their diagnosis. The analysis showed that 47.6% of survivors had normal sperm concentrations (at least 15 million per milliliter), 27.6% had low sperm counts, and 24.8% produced no sperm.
To determine the impact of alkylating agents on the survivors’ sperm production, the researchers calculated each survivor’s cumulative treatment exposure as a CED.
They did this using the following formula: CED (mg/m2)= 1.0 (cumulative cyclophosphamide dose [mg/m2]) + 0.244 (cumulative ifosfamide dose [mg/m2]) + 0.857 (cumulative procarbazine dose [mg/m2]) + 14.286 (cumulative chlorambucil dose [mg/m2]) + 15.0 (cumulative carmustine dose [mg/m2]) + 16.0 (cumulative lomustine dose [mg/m2]) + 40 (cumulative melphalan dose [mg/m2]) + 50 (cumulative thiotepa dose [mg/m2]) + 100 cumulative chlormethine dose [mg/m2]) + 8.823 (cumulative busulfan dose [mg/m2]).
The researchers could not identify a uniformly safe or toxic dose of these drugs, but they found that survivor sperm concentrations generally decreased as cumulative exposure to alkylating agents increased.
And CEDs of 4 g/m2 or less were associated with normal sperm concentrations. Almost 89% of survivors whose CED was 4 g/m2 or less had a normal sperm count. Their sperm were also more likely than sperm from other survivors to look and behave normally.
Dr Green did note that, although a lower cumulative dose of alkylating agents was associated with normal sperm production, outcomes for individual patients were unpredictable and varied. ![]()
Study supports new gold standard for FL
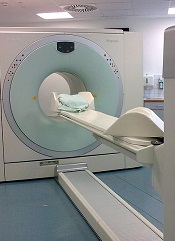
PET-CT should be the new standard for response assessment in patients with follicular lymphoma (FL), according to researchers.
The group found evidence suggesting that PET-CT is more accurate than conventional CT in measuring treatment response and predicting survival in patients with FL.
“Our findings have important implications for patients with follicular lymphoma,” said study author Judith Trotman, MBChB, of the University of Sydney in Australia.
“Compared to conventional CT scanning, PET-CT is more accurate in mapping out the lymphoma and better identifies the majority of patients who have a prolonged remission after treatment.”
Dr Trotman and her colleagues reported these findings in The Lancet Haematology. The results will also be discussed at the International Workshop on PET in Lymphoma in Menton, France, which is taking place September 19-20.
By assessing imaging performed in 3 clinical trials, the researchers examined the link between PET-CT status and survival following first-line immunochemotherapy for advanced FL.
Independent, masked reviewers evaluated scans of 246 patients who underwent both PET-CT and traditional CT imaging within 3 months of their last dose of therapy. Patients were followed for a median of 54.8 months.
Seventeen percent of patients had a positive post-induction PET scan, according to a cutoff of 4 or higher on the 5PS.
When the researchers compared patients with a positive PET scan to those with a negative scan, the hazard ratio (HR) for progression-free survival (PFS) was 3.9 (P<0.0001). For overall survival, the HR was 6.7 (P=0.0002).
The 4-year PFS was 23.2% in patients with a positive PET scan and 63.4% in those who had a negative PET scan (P<0.0001). The 4-year overall survival was 87.2% and 97.1%, respectively (P<0.0001).
The researchers also discovered that conventional CT-based response—complete response or unconfirmed complete response compared to partial response—was weakly predictive of PFS. The HR was 1.7 (P=0.017).
“Our study shows that PET-CT is much better in evaluating treatment response and is an early predictor of survival,” Dr Trotman said. “This greater accuracy will assist physicians to more effectively monitor their patients.”
“We expect this research will result in PET-CT imaging replacing CT, becoming the new gold standard to evaluate patients with follicular lymphoma after treatment. Importantly, it will be a platform for future studies of response-adapted therapies aimed to improve the poor outcomes for those patients who remain PET-positive.”
This study may also pave the way for several new research opportunities, according to Bruce Cheson, MD, of Georgetown University in Washington DC, who wrote a comment article related to this study.
“One such possibility would be to assess if an early reaction to the PET scan result improves patient outcome,” he wrote. “Thus, patients with a positive PET scan after induction therapy could be randomly assigned to either deferred treatment until disease progression or immediate intervention.”
“A preferable alternative would be to introduce a unique agent at that time, such as the newly developed small molecules (eg, idelalisib, ibrutinib, or ABT-199) in a novel combination.” ![]()

PET-CT should be the new standard for response assessment in patients with follicular lymphoma (FL), according to researchers.
The group found evidence suggesting that PET-CT is more accurate than conventional CT in measuring treatment response and predicting survival in patients with FL.
“Our findings have important implications for patients with follicular lymphoma,” said study author Judith Trotman, MBChB, of the University of Sydney in Australia.
“Compared to conventional CT scanning, PET-CT is more accurate in mapping out the lymphoma and better identifies the majority of patients who have a prolonged remission after treatment.”
Dr Trotman and her colleagues reported these findings in The Lancet Haematology. The results will also be discussed at the International Workshop on PET in Lymphoma in Menton, France, which is taking place September 19-20.
By assessing imaging performed in 3 clinical trials, the researchers examined the link between PET-CT status and survival following first-line immunochemotherapy for advanced FL.
Independent, masked reviewers evaluated scans of 246 patients who underwent both PET-CT and traditional CT imaging within 3 months of their last dose of therapy. Patients were followed for a median of 54.8 months.
Seventeen percent of patients had a positive post-induction PET scan, according to a cutoff of 4 or higher on the 5PS.
When the researchers compared patients with a positive PET scan to those with a negative scan, the hazard ratio (HR) for progression-free survival (PFS) was 3.9 (P<0.0001). For overall survival, the HR was 6.7 (P=0.0002).
The 4-year PFS was 23.2% in patients with a positive PET scan and 63.4% in those who had a negative PET scan (P<0.0001). The 4-year overall survival was 87.2% and 97.1%, respectively (P<0.0001).
The researchers also discovered that conventional CT-based response—complete response or unconfirmed complete response compared to partial response—was weakly predictive of PFS. The HR was 1.7 (P=0.017).
“Our study shows that PET-CT is much better in evaluating treatment response and is an early predictor of survival,” Dr Trotman said. “This greater accuracy will assist physicians to more effectively monitor their patients.”
“We expect this research will result in PET-CT imaging replacing CT, becoming the new gold standard to evaluate patients with follicular lymphoma after treatment. Importantly, it will be a platform for future studies of response-adapted therapies aimed to improve the poor outcomes for those patients who remain PET-positive.”
This study may also pave the way for several new research opportunities, according to Bruce Cheson, MD, of Georgetown University in Washington DC, who wrote a comment article related to this study.
“One such possibility would be to assess if an early reaction to the PET scan result improves patient outcome,” he wrote. “Thus, patients with a positive PET scan after induction therapy could be randomly assigned to either deferred treatment until disease progression or immediate intervention.”
“A preferable alternative would be to introduce a unique agent at that time, such as the newly developed small molecules (eg, idelalisib, ibrutinib, or ABT-199) in a novel combination.” ![]()

PET-CT should be the new standard for response assessment in patients with follicular lymphoma (FL), according to researchers.
The group found evidence suggesting that PET-CT is more accurate than conventional CT in measuring treatment response and predicting survival in patients with FL.
“Our findings have important implications for patients with follicular lymphoma,” said study author Judith Trotman, MBChB, of the University of Sydney in Australia.
“Compared to conventional CT scanning, PET-CT is more accurate in mapping out the lymphoma and better identifies the majority of patients who have a prolonged remission after treatment.”
Dr Trotman and her colleagues reported these findings in The Lancet Haematology. The results will also be discussed at the International Workshop on PET in Lymphoma in Menton, France, which is taking place September 19-20.
By assessing imaging performed in 3 clinical trials, the researchers examined the link between PET-CT status and survival following first-line immunochemotherapy for advanced FL.
Independent, masked reviewers evaluated scans of 246 patients who underwent both PET-CT and traditional CT imaging within 3 months of their last dose of therapy. Patients were followed for a median of 54.8 months.
Seventeen percent of patients had a positive post-induction PET scan, according to a cutoff of 4 or higher on the 5PS.
When the researchers compared patients with a positive PET scan to those with a negative scan, the hazard ratio (HR) for progression-free survival (PFS) was 3.9 (P<0.0001). For overall survival, the HR was 6.7 (P=0.0002).
The 4-year PFS was 23.2% in patients with a positive PET scan and 63.4% in those who had a negative PET scan (P<0.0001). The 4-year overall survival was 87.2% and 97.1%, respectively (P<0.0001).
The researchers also discovered that conventional CT-based response—complete response or unconfirmed complete response compared to partial response—was weakly predictive of PFS. The HR was 1.7 (P=0.017).
“Our study shows that PET-CT is much better in evaluating treatment response and is an early predictor of survival,” Dr Trotman said. “This greater accuracy will assist physicians to more effectively monitor their patients.”
“We expect this research will result in PET-CT imaging replacing CT, becoming the new gold standard to evaluate patients with follicular lymphoma after treatment. Importantly, it will be a platform for future studies of response-adapted therapies aimed to improve the poor outcomes for those patients who remain PET-positive.”
This study may also pave the way for several new research opportunities, according to Bruce Cheson, MD, of Georgetown University in Washington DC, who wrote a comment article related to this study.
“One such possibility would be to assess if an early reaction to the PET scan result improves patient outcome,” he wrote. “Thus, patients with a positive PET scan after induction therapy could be randomly assigned to either deferred treatment until disease progression or immediate intervention.”
“A preferable alternative would be to introduce a unique agent at that time, such as the newly developed small molecules (eg, idelalisib, ibrutinib, or ABT-199) in a novel combination.” ![]()
Group investigates link between implants and ALCL
![]()
Credit: FDA
A newly published review provides insight into anaplastic large-cell lymphoma (ALCL) associated with breast implants.
Previous reports have demonstrated a link between breast implants and ALCL, but the reasons why implants may contribute to this type of lymphoma have remained unclear.
So Suzanne Turner, PhD, of the University of Cambridge in the UK, and her colleagues evaluated the 71 recorded cases of implant-associated ALCL (iALCL).
The researchers recounted their findings in Mutation Research/Reviews in Mutations Research.
The team calculated that the absolute risk of developing iALCL is low, ranging from 1:500,000 to 1:3,000,000 patients with breast implants per year.
Among the 71 cases of iALCL, the average patient was 50 years of age. The average time from breast augmentation/reconstruction to iALCL diagnosis was 10 years.
Most of the cases presented in the capsule surrounding the implant, as part of the periprosthetic fluid or the capsule itself.
The majority of cases were ALK-negative but had a good prognosis. Of the 49 cases where information on the patients’ progress was available, there were 5 deaths.
Some patients received chemotherapy and radiotherapy, but many achieved remission once the implant and surrounding tissue were removed. This suggests it is the body’s abnormal immune response to the implant that is causing iALCL, the researchers said.
There is some evidence to suggest that having any type of prosthetic implant can increase the risk of lymphoma. And some researchers have suggested that lifestyle differences between patients with and without breast implants may be at the root of iALCL.
But Dr Turner and her colleagues said the biological features of lymphomas in the presence of implants, such as the lack of ALK and the proximity to the implant, suggest a real link.
“It’s becoming clear that implant-related ALCL is a distinct clinical entity in itself,” Dr Turner said. “There are still unanswered questions, and only by getting to the bottom of this very rare disease will we be able to find alternative ways to treat it.” ![]()
![]()
Credit: FDA
A newly published review provides insight into anaplastic large-cell lymphoma (ALCL) associated with breast implants.
Previous reports have demonstrated a link between breast implants and ALCL, but the reasons why implants may contribute to this type of lymphoma have remained unclear.
So Suzanne Turner, PhD, of the University of Cambridge in the UK, and her colleagues evaluated the 71 recorded cases of implant-associated ALCL (iALCL).
The researchers recounted their findings in Mutation Research/Reviews in Mutations Research.
The team calculated that the absolute risk of developing iALCL is low, ranging from 1:500,000 to 1:3,000,000 patients with breast implants per year.
Among the 71 cases of iALCL, the average patient was 50 years of age. The average time from breast augmentation/reconstruction to iALCL diagnosis was 10 years.
Most of the cases presented in the capsule surrounding the implant, as part of the periprosthetic fluid or the capsule itself.
The majority of cases were ALK-negative but had a good prognosis. Of the 49 cases where information on the patients’ progress was available, there were 5 deaths.
Some patients received chemotherapy and radiotherapy, but many achieved remission once the implant and surrounding tissue were removed. This suggests it is the body’s abnormal immune response to the implant that is causing iALCL, the researchers said.
There is some evidence to suggest that having any type of prosthetic implant can increase the risk of lymphoma. And some researchers have suggested that lifestyle differences between patients with and without breast implants may be at the root of iALCL.
But Dr Turner and her colleagues said the biological features of lymphomas in the presence of implants, such as the lack of ALK and the proximity to the implant, suggest a real link.
“It’s becoming clear that implant-related ALCL is a distinct clinical entity in itself,” Dr Turner said. “There are still unanswered questions, and only by getting to the bottom of this very rare disease will we be able to find alternative ways to treat it.” ![]()
![]()
Credit: FDA
A newly published review provides insight into anaplastic large-cell lymphoma (ALCL) associated with breast implants.
Previous reports have demonstrated a link between breast implants and ALCL, but the reasons why implants may contribute to this type of lymphoma have remained unclear.
So Suzanne Turner, PhD, of the University of Cambridge in the UK, and her colleagues evaluated the 71 recorded cases of implant-associated ALCL (iALCL).
The researchers recounted their findings in Mutation Research/Reviews in Mutations Research.
The team calculated that the absolute risk of developing iALCL is low, ranging from 1:500,000 to 1:3,000,000 patients with breast implants per year.
Among the 71 cases of iALCL, the average patient was 50 years of age. The average time from breast augmentation/reconstruction to iALCL diagnosis was 10 years.
Most of the cases presented in the capsule surrounding the implant, as part of the periprosthetic fluid or the capsule itself.
The majority of cases were ALK-negative but had a good prognosis. Of the 49 cases where information on the patients’ progress was available, there were 5 deaths.
Some patients received chemotherapy and radiotherapy, but many achieved remission once the implant and surrounding tissue were removed. This suggests it is the body’s abnormal immune response to the implant that is causing iALCL, the researchers said.
There is some evidence to suggest that having any type of prosthetic implant can increase the risk of lymphoma. And some researchers have suggested that lifestyle differences between patients with and without breast implants may be at the root of iALCL.
But Dr Turner and her colleagues said the biological features of lymphomas in the presence of implants, such as the lack of ALK and the proximity to the implant, suggest a real link.
“It’s becoming clear that implant-related ALCL is a distinct clinical entity in itself,” Dr Turner said. “There are still unanswered questions, and only by getting to the bottom of this very rare disease will we be able to find alternative ways to treat it.” ![]()
RT use on decline in early HL despite survival benefit
Credit: Rhoda Baer
SAN FRANCISCO—Results of a large study suggest that consolidation radiation therapy (RT) can improve survival in patients with stage I and II Hodgkin lymphoma (HL), but the use of RT in these patients may be on the decline.
In this study of more than 40,000 patients, the 10-year survival rate was 84% among those who received RT and 76% among those who did not.
Despite this benefit, the use of RT declined during the period studied, from 56% in 1998 to 41% in 2011.
These data were presented at the American Society for Radiation Oncology’s 56th Annual Meeting (abstract 1042).
“Multiple prospective, randomized trials have shown a significant improvement in disease control with the addition of RT,” said lead study author Rahul R. Parikh, MD, of the Mount Sinai Health System in New York.
“However, previous trials were limited by low patient numbers and limited follow-up and, thus, were unable to demonstrate an overall survival benefit. This is the largest dataset in this patient population to demonstrate a survival benefit with the addition of RT.”
Dr Parikh and his colleagues studied 41,502 patients who were diagnosed with stage I and II HL from 1998 to 2011. They were included in the National Cancer Data Base, which consists of cases from 1500 sites and represents more than 75% of all cancers diagnosed in the US.
The average patient age was 37 years (range, 18 to 90). The median follow-up was 7.5 years. Ninety-six percent of patients (n=39,842) received multi-agent chemotherapy, and 49% (n=20,441) received a median RT dose of 30.6 Gy.
The 10-year overall survival of the entire group was 80.8%. Patients receiving RT had significantly better overall survival than those who did not (84.4% vs 76.4%; P<0.00001).
When adjusting for age, stage, comorbidity, transplant, chemotherapy use, and socioeconomic status, RT use was still associated with significantly improved overall survival (hazard ratio=0.51; P<0.00001).
The study also showed that omitting RT was related to higher rates of salvage transplant procedures, a surrogate for persistent/relapsed disease (P=0.04).
Nevertheless, RT use decreased at the study sites from 56% to 41% between 1998 and 2011.
In 88.4% of patients who did not receive RT, the physician-reported reason was that RT was not part of the planned initial treatment strategy.
The research also indicated that RT use was more likely among younger patients (40 years or younger), those in a higher socioeconomic status, those who had access to health insurance, and those who received treatment at comprehensive cancer centers (all P<0.0001).
“[W]e have highlighted ongoing disparities in Hodgkin’s disease treatment, and it is important that we recognize these findings as potential barriers to care,” Dr Parikh said.
“Given the survival benefit demonstrated in this study, radiotherapy should be included in the combined modality approach of multi-agent chemotherapy followed by consolidation RT in order to maintain high overall survival rates for this curable disease.” ![]()

Credit: Rhoda Baer
SAN FRANCISCO—Results of a large study suggest that consolidation radiation therapy (RT) can improve survival in patients with stage I and II Hodgkin lymphoma (HL), but the use of RT in these patients may be on the decline.
In this study of more than 40,000 patients, the 10-year survival rate was 84% among those who received RT and 76% among those who did not.
Despite this benefit, the use of RT declined during the period studied, from 56% in 1998 to 41% in 2011.
These data were presented at the American Society for Radiation Oncology’s 56th Annual Meeting (abstract 1042).
“Multiple prospective, randomized trials have shown a significant improvement in disease control with the addition of RT,” said lead study author Rahul R. Parikh, MD, of the Mount Sinai Health System in New York.
“However, previous trials were limited by low patient numbers and limited follow-up and, thus, were unable to demonstrate an overall survival benefit. This is the largest dataset in this patient population to demonstrate a survival benefit with the addition of RT.”
Dr Parikh and his colleagues studied 41,502 patients who were diagnosed with stage I and II HL from 1998 to 2011. They were included in the National Cancer Data Base, which consists of cases from 1500 sites and represents more than 75% of all cancers diagnosed in the US.
The average patient age was 37 years (range, 18 to 90). The median follow-up was 7.5 years. Ninety-six percent of patients (n=39,842) received multi-agent chemotherapy, and 49% (n=20,441) received a median RT dose of 30.6 Gy.
The 10-year overall survival of the entire group was 80.8%. Patients receiving RT had significantly better overall survival than those who did not (84.4% vs 76.4%; P<0.00001).
When adjusting for age, stage, comorbidity, transplant, chemotherapy use, and socioeconomic status, RT use was still associated with significantly improved overall survival (hazard ratio=0.51; P<0.00001).
The study also showed that omitting RT was related to higher rates of salvage transplant procedures, a surrogate for persistent/relapsed disease (P=0.04).
Nevertheless, RT use decreased at the study sites from 56% to 41% between 1998 and 2011.
In 88.4% of patients who did not receive RT, the physician-reported reason was that RT was not part of the planned initial treatment strategy.
The research also indicated that RT use was more likely among younger patients (40 years or younger), those in a higher socioeconomic status, those who had access to health insurance, and those who received treatment at comprehensive cancer centers (all P<0.0001).
“[W]e have highlighted ongoing disparities in Hodgkin’s disease treatment, and it is important that we recognize these findings as potential barriers to care,” Dr Parikh said.
“Given the survival benefit demonstrated in this study, radiotherapy should be included in the combined modality approach of multi-agent chemotherapy followed by consolidation RT in order to maintain high overall survival rates for this curable disease.” ![]()

Credit: Rhoda Baer
SAN FRANCISCO—Results of a large study suggest that consolidation radiation therapy (RT) can improve survival in patients with stage I and II Hodgkin lymphoma (HL), but the use of RT in these patients may be on the decline.
In this study of more than 40,000 patients, the 10-year survival rate was 84% among those who received RT and 76% among those who did not.
Despite this benefit, the use of RT declined during the period studied, from 56% in 1998 to 41% in 2011.
These data were presented at the American Society for Radiation Oncology’s 56th Annual Meeting (abstract 1042).
“Multiple prospective, randomized trials have shown a significant improvement in disease control with the addition of RT,” said lead study author Rahul R. Parikh, MD, of the Mount Sinai Health System in New York.
“However, previous trials were limited by low patient numbers and limited follow-up and, thus, were unable to demonstrate an overall survival benefit. This is the largest dataset in this patient population to demonstrate a survival benefit with the addition of RT.”
Dr Parikh and his colleagues studied 41,502 patients who were diagnosed with stage I and II HL from 1998 to 2011. They were included in the National Cancer Data Base, which consists of cases from 1500 sites and represents more than 75% of all cancers diagnosed in the US.
The average patient age was 37 years (range, 18 to 90). The median follow-up was 7.5 years. Ninety-six percent of patients (n=39,842) received multi-agent chemotherapy, and 49% (n=20,441) received a median RT dose of 30.6 Gy.
The 10-year overall survival of the entire group was 80.8%. Patients receiving RT had significantly better overall survival than those who did not (84.4% vs 76.4%; P<0.00001).
When adjusting for age, stage, comorbidity, transplant, chemotherapy use, and socioeconomic status, RT use was still associated with significantly improved overall survival (hazard ratio=0.51; P<0.00001).
The study also showed that omitting RT was related to higher rates of salvage transplant procedures, a surrogate for persistent/relapsed disease (P=0.04).
Nevertheless, RT use decreased at the study sites from 56% to 41% between 1998 and 2011.
In 88.4% of patients who did not receive RT, the physician-reported reason was that RT was not part of the planned initial treatment strategy.
The research also indicated that RT use was more likely among younger patients (40 years or younger), those in a higher socioeconomic status, those who had access to health insurance, and those who received treatment at comprehensive cancer centers (all P<0.0001).
“[W]e have highlighted ongoing disparities in Hodgkin’s disease treatment, and it is important that we recognize these findings as potential barriers to care,” Dr Parikh said.
“Given the survival benefit demonstrated in this study, radiotherapy should be included in the combined modality approach of multi-agent chemotherapy followed by consolidation RT in order to maintain high overall survival rates for this curable disease.” ![]()
Antifungal shows promise in hematologic conditions

WASHINGTON, DC—A new antifungal agent is as effective as an existing drug against invasive mold infection in patients with hematologic disorders, results of a phase 3 trial suggest.
Overall response and all-cause mortality rates were comparable with the newer drug, isavuconazole (ISA), and the existing drug, voriconazole (VRC).
The overall rates of treatment-emergent adverse events were comparable as well, but ISA was associated with a significantly lower incidence of several events.
Kieren Marr, MD, of Johns Hopkins University in Baltimore, Maryland, and her colleagues presented these results in a subset of patients from the SECURE trial at the 54th Interscience Conference on Antimicrobial Agents and Chemotherapy (poster M-1757).
Patient characteristics and safety outcomes
Of the 433 patients with a hematologic disorder enrolled in the trial, 217 had proven or probable invasive mold infection. The researchers divided patients into 2 groups according to disease: those with acute myeloid leukemia (AML) and those with acute lymphoblastic leukemia (ALL) or other conditions.
In all, 102 patients had AML, and 115 had ALL (n=28) or other conditions, including non-Hodgkin lymphoma (n=19), chronic lymphocytic leukemia (n=15), refractory anemia with excess blasts (n=9), myelodysplastic syndrome (n=8), chronic myeloid leukemia (n=6), and “other” underlying conditions (n=30).
Patients were randomized to receive VRC (n=105) or ISA (N=112). Thirty patients in the ISA arm and 26 in the VRC arm had undergone allogeneic transplant prior to therapy.
The primary outcome was all-cause mortality at day 42. Overall response and safety were secondary endpoints.
The overall rates of treatment-emergent adverse events were similar between ISA and VRC arms. Ninety-seven percent of patients in the ISA arm and 98% of patients in the VRC arm reported at least 1 treatment-emergent adverse event.
However, patients in the ISA arm had significantly fewer (P<0.05) events for the cardiac disorders, eye, psychiatric disorders, renal and urinary, and vascular system organ classes.
Response and mortality
All-cause mortality rates were comparable between the ISA and VRC arms—22% and 24%, respectively—as were overall response rates—39% and 34%, respectively—and complete response rates—13% and 10%, respectively.
All-cause mortality rates among patients with AML were 18% in the ISA arm and 15% in the VRC arm. Overall response rates were 36% and 48%, respectively.
For patients with ALL or other hematologic conditions, all-cause mortality rates were 26% in the ISA arm and 32% in the VRC arm. Overall response rates were 42% and 21%, respectively.
In transplant patients, the all-cause mortality rate was 27% for both the ISA and VRC arms. The overall response rate was 27% for both arms as well.
“These results show the potential of isavuconazole as a potent antifungal in the fight against invasive mold disease,” Dr Marr said.
ISA is an investigational antifungal under development by Astellas and Basilea Pharmaceutica International Ltd. The SECURE trial was funded by Astellas.
The US Food and Drug Administration recently accepted a new drug application seeking approval for ISA for the treatment of invasive aspergillosis and invasive mucormycosis. ![]()

WASHINGTON, DC—A new antifungal agent is as effective as an existing drug against invasive mold infection in patients with hematologic disorders, results of a phase 3 trial suggest.
Overall response and all-cause mortality rates were comparable with the newer drug, isavuconazole (ISA), and the existing drug, voriconazole (VRC).
The overall rates of treatment-emergent adverse events were comparable as well, but ISA was associated with a significantly lower incidence of several events.
Kieren Marr, MD, of Johns Hopkins University in Baltimore, Maryland, and her colleagues presented these results in a subset of patients from the SECURE trial at the 54th Interscience Conference on Antimicrobial Agents and Chemotherapy (poster M-1757).
Patient characteristics and safety outcomes
Of the 433 patients with a hematologic disorder enrolled in the trial, 217 had proven or probable invasive mold infection. The researchers divided patients into 2 groups according to disease: those with acute myeloid leukemia (AML) and those with acute lymphoblastic leukemia (ALL) or other conditions.
In all, 102 patients had AML, and 115 had ALL (n=28) or other conditions, including non-Hodgkin lymphoma (n=19), chronic lymphocytic leukemia (n=15), refractory anemia with excess blasts (n=9), myelodysplastic syndrome (n=8), chronic myeloid leukemia (n=6), and “other” underlying conditions (n=30).
Patients were randomized to receive VRC (n=105) or ISA (N=112). Thirty patients in the ISA arm and 26 in the VRC arm had undergone allogeneic transplant prior to therapy.
The primary outcome was all-cause mortality at day 42. Overall response and safety were secondary endpoints.
The overall rates of treatment-emergent adverse events were similar between ISA and VRC arms. Ninety-seven percent of patients in the ISA arm and 98% of patients in the VRC arm reported at least 1 treatment-emergent adverse event.
However, patients in the ISA arm had significantly fewer (P<0.05) events for the cardiac disorders, eye, psychiatric disorders, renal and urinary, and vascular system organ classes.
Response and mortality
All-cause mortality rates were comparable between the ISA and VRC arms—22% and 24%, respectively—as were overall response rates—39% and 34%, respectively—and complete response rates—13% and 10%, respectively.
All-cause mortality rates among patients with AML were 18% in the ISA arm and 15% in the VRC arm. Overall response rates were 36% and 48%, respectively.
For patients with ALL or other hematologic conditions, all-cause mortality rates were 26% in the ISA arm and 32% in the VRC arm. Overall response rates were 42% and 21%, respectively.
In transplant patients, the all-cause mortality rate was 27% for both the ISA and VRC arms. The overall response rate was 27% for both arms as well.
“These results show the potential of isavuconazole as a potent antifungal in the fight against invasive mold disease,” Dr Marr said.
ISA is an investigational antifungal under development by Astellas and Basilea Pharmaceutica International Ltd. The SECURE trial was funded by Astellas.
The US Food and Drug Administration recently accepted a new drug application seeking approval for ISA for the treatment of invasive aspergillosis and invasive mucormycosis. ![]()

WASHINGTON, DC—A new antifungal agent is as effective as an existing drug against invasive mold infection in patients with hematologic disorders, results of a phase 3 trial suggest.
Overall response and all-cause mortality rates were comparable with the newer drug, isavuconazole (ISA), and the existing drug, voriconazole (VRC).
The overall rates of treatment-emergent adverse events were comparable as well, but ISA was associated with a significantly lower incidence of several events.
Kieren Marr, MD, of Johns Hopkins University in Baltimore, Maryland, and her colleagues presented these results in a subset of patients from the SECURE trial at the 54th Interscience Conference on Antimicrobial Agents and Chemotherapy (poster M-1757).
Patient characteristics and safety outcomes
Of the 433 patients with a hematologic disorder enrolled in the trial, 217 had proven or probable invasive mold infection. The researchers divided patients into 2 groups according to disease: those with acute myeloid leukemia (AML) and those with acute lymphoblastic leukemia (ALL) or other conditions.
In all, 102 patients had AML, and 115 had ALL (n=28) or other conditions, including non-Hodgkin lymphoma (n=19), chronic lymphocytic leukemia (n=15), refractory anemia with excess blasts (n=9), myelodysplastic syndrome (n=8), chronic myeloid leukemia (n=6), and “other” underlying conditions (n=30).
Patients were randomized to receive VRC (n=105) or ISA (N=112). Thirty patients in the ISA arm and 26 in the VRC arm had undergone allogeneic transplant prior to therapy.
The primary outcome was all-cause mortality at day 42. Overall response and safety were secondary endpoints.
The overall rates of treatment-emergent adverse events were similar between ISA and VRC arms. Ninety-seven percent of patients in the ISA arm and 98% of patients in the VRC arm reported at least 1 treatment-emergent adverse event.
However, patients in the ISA arm had significantly fewer (P<0.05) events for the cardiac disorders, eye, psychiatric disorders, renal and urinary, and vascular system organ classes.
Response and mortality
All-cause mortality rates were comparable between the ISA and VRC arms—22% and 24%, respectively—as were overall response rates—39% and 34%, respectively—and complete response rates—13% and 10%, respectively.
All-cause mortality rates among patients with AML were 18% in the ISA arm and 15% in the VRC arm. Overall response rates were 36% and 48%, respectively.
For patients with ALL or other hematologic conditions, all-cause mortality rates were 26% in the ISA arm and 32% in the VRC arm. Overall response rates were 42% and 21%, respectively.
In transplant patients, the all-cause mortality rate was 27% for both the ISA and VRC arms. The overall response rate was 27% for both arms as well.
“These results show the potential of isavuconazole as a potent antifungal in the fight against invasive mold disease,” Dr Marr said.
ISA is an investigational antifungal under development by Astellas and Basilea Pharmaceutica International Ltd. The SECURE trial was funded by Astellas.
The US Food and Drug Administration recently accepted a new drug application seeking approval for ISA for the treatment of invasive aspergillosis and invasive mucormycosis. ![]()
Mutations linked to population disparities in cancers

Credit: NIGMS
Researchers have identified mutations in microRNAs (miRNAs) that are closely associated with certain global populations and have been implicated in cancers.
The group discovered 31 miRNAs containing variants that occur with different frequencies in African and non-African populations.
Seven of these miRNAs have been linked to the onset, progression, and spread of cancers with known health disparities between patients of European and African descent.
And a variant in one of these miRNAs is associated with a significantly increased risk of non-Hodgkin lymphoma (NHL).
These findings appear in BMC Medical Genomics.
To better understand miRNA diversity across the world, the researchers searched for miRNA variants in the genome sequences of 69 individuals from 14 populations in Europe, Asia, the Americas, and Africa. The samples included genetic material from diverse African populations, including 3 hunter-gatherer populations.
“We wanted to try to see if there was variability in miRNA that hadn’t been identified before,” said study author Renata A. Rawlings-Goss, PhD, of the University of Pennsylvania’s Perelman School of Medicine in Philadelphia.
Overall, the researchers found that miRNA sequences were similar across the populations they sampled. But they did identify 33 novel variants and found that variants in 31 miRNAs were population-differentiated.
The team searched available databases to see which genes these miRNAs were known to inhibit. Their query turned up a large proportion of genes involved in glucose and insulin metabolism, indicating a possible connection between diabetes risk and possessing one of these variants. The search also pointed to effects on genes implicated in cancers.
Specifically, 7 of the population-differentiated miRNAs are currently implicated as cancer biomarkers: hsa-mir-202, hsa-mir-423, hsa-mir-196a-2, hsa-mir-520h, hsa-mir-647, hsa-mir-943, and hsa-mir-1908.
Of particular interest was hsa-mir-202, which contained one of the most highly population-differentiated variants in the dataset and is under investigation as a marker for NHL and early stage breast cancer.
Recent research suggested that a T allele at SNP rs12355840 in hsa-mir-202 helps protect against death from breast cancer by increasing mature hsa-mir-202 expression levels, which leads to downregulation of its gene targets.
On the other hand, diminished expression of mature hsa-mir-202 in subjects harboring at least 1 non-T allele resulted in a significantly elevated risk of NHL (odds ratio=1.83, P=0.008).
Dr Rawlings-Goss and her colleagues found that African/African-American populations had a lower frequency of the T allele compared to European/Asian populations—26% vs 65%, on average. And this suggests decreased baseline expression levels of mature hsa-mir-202 in African populations.
“It’s becoming more and more apparent that miRNAs can have a broad-reaching and global effect on our health and adaptation to disease,” Dr Rawlings-Goss said. “Learning more about differences across populations could be helpful to doing early diagnostics and treating disease across diverse populations.” ![]()

Credit: NIGMS
Researchers have identified mutations in microRNAs (miRNAs) that are closely associated with certain global populations and have been implicated in cancers.
The group discovered 31 miRNAs containing variants that occur with different frequencies in African and non-African populations.
Seven of these miRNAs have been linked to the onset, progression, and spread of cancers with known health disparities between patients of European and African descent.
And a variant in one of these miRNAs is associated with a significantly increased risk of non-Hodgkin lymphoma (NHL).
These findings appear in BMC Medical Genomics.
To better understand miRNA diversity across the world, the researchers searched for miRNA variants in the genome sequences of 69 individuals from 14 populations in Europe, Asia, the Americas, and Africa. The samples included genetic material from diverse African populations, including 3 hunter-gatherer populations.
“We wanted to try to see if there was variability in miRNA that hadn’t been identified before,” said study author Renata A. Rawlings-Goss, PhD, of the University of Pennsylvania’s Perelman School of Medicine in Philadelphia.
Overall, the researchers found that miRNA sequences were similar across the populations they sampled. But they did identify 33 novel variants and found that variants in 31 miRNAs were population-differentiated.
The team searched available databases to see which genes these miRNAs were known to inhibit. Their query turned up a large proportion of genes involved in glucose and insulin metabolism, indicating a possible connection between diabetes risk and possessing one of these variants. The search also pointed to effects on genes implicated in cancers.
Specifically, 7 of the population-differentiated miRNAs are currently implicated as cancer biomarkers: hsa-mir-202, hsa-mir-423, hsa-mir-196a-2, hsa-mir-520h, hsa-mir-647, hsa-mir-943, and hsa-mir-1908.
Of particular interest was hsa-mir-202, which contained one of the most highly population-differentiated variants in the dataset and is under investigation as a marker for NHL and early stage breast cancer.
Recent research suggested that a T allele at SNP rs12355840 in hsa-mir-202 helps protect against death from breast cancer by increasing mature hsa-mir-202 expression levels, which leads to downregulation of its gene targets.
On the other hand, diminished expression of mature hsa-mir-202 in subjects harboring at least 1 non-T allele resulted in a significantly elevated risk of NHL (odds ratio=1.83, P=0.008).
Dr Rawlings-Goss and her colleagues found that African/African-American populations had a lower frequency of the T allele compared to European/Asian populations—26% vs 65%, on average. And this suggests decreased baseline expression levels of mature hsa-mir-202 in African populations.
“It’s becoming more and more apparent that miRNAs can have a broad-reaching and global effect on our health and adaptation to disease,” Dr Rawlings-Goss said. “Learning more about differences across populations could be helpful to doing early diagnostics and treating disease across diverse populations.” ![]()

Credit: NIGMS
Researchers have identified mutations in microRNAs (miRNAs) that are closely associated with certain global populations and have been implicated in cancers.
The group discovered 31 miRNAs containing variants that occur with different frequencies in African and non-African populations.
Seven of these miRNAs have been linked to the onset, progression, and spread of cancers with known health disparities between patients of European and African descent.
And a variant in one of these miRNAs is associated with a significantly increased risk of non-Hodgkin lymphoma (NHL).
These findings appear in BMC Medical Genomics.
To better understand miRNA diversity across the world, the researchers searched for miRNA variants in the genome sequences of 69 individuals from 14 populations in Europe, Asia, the Americas, and Africa. The samples included genetic material from diverse African populations, including 3 hunter-gatherer populations.
“We wanted to try to see if there was variability in miRNA that hadn’t been identified before,” said study author Renata A. Rawlings-Goss, PhD, of the University of Pennsylvania’s Perelman School of Medicine in Philadelphia.
Overall, the researchers found that miRNA sequences were similar across the populations they sampled. But they did identify 33 novel variants and found that variants in 31 miRNAs were population-differentiated.
The team searched available databases to see which genes these miRNAs were known to inhibit. Their query turned up a large proportion of genes involved in glucose and insulin metabolism, indicating a possible connection between diabetes risk and possessing one of these variants. The search also pointed to effects on genes implicated in cancers.
Specifically, 7 of the population-differentiated miRNAs are currently implicated as cancer biomarkers: hsa-mir-202, hsa-mir-423, hsa-mir-196a-2, hsa-mir-520h, hsa-mir-647, hsa-mir-943, and hsa-mir-1908.
Of particular interest was hsa-mir-202, which contained one of the most highly population-differentiated variants in the dataset and is under investigation as a marker for NHL and early stage breast cancer.
Recent research suggested that a T allele at SNP rs12355840 in hsa-mir-202 helps protect against death from breast cancer by increasing mature hsa-mir-202 expression levels, which leads to downregulation of its gene targets.
On the other hand, diminished expression of mature hsa-mir-202 in subjects harboring at least 1 non-T allele resulted in a significantly elevated risk of NHL (odds ratio=1.83, P=0.008).
Dr Rawlings-Goss and her colleagues found that African/African-American populations had a lower frequency of the T allele compared to European/Asian populations—26% vs 65%, on average. And this suggests decreased baseline expression levels of mature hsa-mir-202 in African populations.
“It’s becoming more and more apparent that miRNAs can have a broad-reaching and global effect on our health and adaptation to disease,” Dr Rawlings-Goss said. “Learning more about differences across populations could be helpful to doing early diagnostics and treating disease across diverse populations.”
Discovery could lead to better proteasome inhibitors

showing multiple myeloma
A newly discovered mechanism has paved the way for the next generation of proteasome inhibitors, according to a paper published in Chemistry & Biology.
Investigators developed a series of molecules that employ this mechanism, inhibiting the proteasome in 2 ways.
They are now planning to synthesize related compounds that may offer improved proteasome inhibition, target cancer cells more selectivity, and eliminate the resistance problems that occur with current drugs.
The group’s research began with epoxyketone, a molecule isolated from a cyanobacterium called carmaphycin, whose reactive group is the same as that of the proteasome inhibitor carfilzomib.
“Epoxyketones are very potent, selective inhibitors of the proteasome because they interact with this enzyme in 2 stages—the first reversible, and the second irreversible,” noted study author Daniela Trivella, PhD, of the Brazilian Biosciences National Laboratory at the Brazilian Center for Research in Energy and Materials in Campinas.
To optimize epoxyketone’s effects and find new reactive groups, the investigators developed and tested a series of synthetic analogs with slight structural modifications.
One of the molecules had an enone as a reactive group and had characteristics of carmaphycin and another natural molecule called syringolin, which was isolated from plant pathogens.
By investigating the reaction mechanisms of the new molecule, called carmaphycin-syringolin enone, the team verified that the enone interacts with the proteasome in 2 stages, with the second stage being irreversible.
The investigators also observed that, in the case of the enone, the second reaction occurs more slowly, increasing the duration of the reversible phase of carmaphycin-syringolin enone inhibition.
“Because the irreversible inactivation of the proteasome has toxic effects, the best window of reversibility observed for the carmaphycin-syringolin enone will potentially reduce the toxicity of this new class of proteasome inhibitors,” Dr Trivella said. “The compound would therefore present a balance between selectivity and potency.”
Toxicity tests are still underway. But the investigators have already conducted studies to determine exactly how the interaction between the enzyme target and the carmaphycin-syringolin enone target occurs.
“We discovered that a chemical reaction called hydroamination occurs, which had never before [been] seen under physiological conditions,” Dr Trivella said.
“This type of reaction is frequently used by synthetic chemists in preparing substances, but, normally, it requires very specific temperature and pH conditions and the use of catalysts to occur. It has never been reported as a mechanism of enzyme inhibition.”
Inspired by this new mechanism for proteasome inhibition, the investigators plan to synthesize and test a new series of carmaphycin-syringolin enone analogs to determine their effects on the therapeutic window and assess whether they are also capable of reacting with proteasomes that are resistant to traditional inhibitors.

showing multiple myeloma
A newly discovered mechanism has paved the way for the next generation of proteasome inhibitors, according to a paper published in Chemistry & Biology.
Investigators developed a series of molecules that employ this mechanism, inhibiting the proteasome in 2 ways.
They are now planning to synthesize related compounds that may offer improved proteasome inhibition, target cancer cells more selectivity, and eliminate the resistance problems that occur with current drugs.
The group’s research began with epoxyketone, a molecule isolated from a cyanobacterium called carmaphycin, whose reactive group is the same as that of the proteasome inhibitor carfilzomib.
“Epoxyketones are very potent, selective inhibitors of the proteasome because they interact with this enzyme in 2 stages—the first reversible, and the second irreversible,” noted study author Daniela Trivella, PhD, of the Brazilian Biosciences National Laboratory at the Brazilian Center for Research in Energy and Materials in Campinas.
To optimize epoxyketone’s effects and find new reactive groups, the investigators developed and tested a series of synthetic analogs with slight structural modifications.
One of the molecules had an enone as a reactive group and had characteristics of carmaphycin and another natural molecule called syringolin, which was isolated from plant pathogens.
By investigating the reaction mechanisms of the new molecule, called carmaphycin-syringolin enone, the team verified that the enone interacts with the proteasome in 2 stages, with the second stage being irreversible.
The investigators also observed that, in the case of the enone, the second reaction occurs more slowly, increasing the duration of the reversible phase of carmaphycin-syringolin enone inhibition.
“Because the irreversible inactivation of the proteasome has toxic effects, the best window of reversibility observed for the carmaphycin-syringolin enone will potentially reduce the toxicity of this new class of proteasome inhibitors,” Dr Trivella said. “The compound would therefore present a balance between selectivity and potency.”
Toxicity tests are still underway. But the investigators have already conducted studies to determine exactly how the interaction between the enzyme target and the carmaphycin-syringolin enone target occurs.
“We discovered that a chemical reaction called hydroamination occurs, which had never before [been] seen under physiological conditions,” Dr Trivella said.
“This type of reaction is frequently used by synthetic chemists in preparing substances, but, normally, it requires very specific temperature and pH conditions and the use of catalysts to occur. It has never been reported as a mechanism of enzyme inhibition.”
Inspired by this new mechanism for proteasome inhibition, the investigators plan to synthesize and test a new series of carmaphycin-syringolin enone analogs to determine their effects on the therapeutic window and assess whether they are also capable of reacting with proteasomes that are resistant to traditional inhibitors.

showing multiple myeloma
A newly discovered mechanism has paved the way for the next generation of proteasome inhibitors, according to a paper published in Chemistry & Biology.
Investigators developed a series of molecules that employ this mechanism, inhibiting the proteasome in 2 ways.
They are now planning to synthesize related compounds that may offer improved proteasome inhibition, target cancer cells more selectivity, and eliminate the resistance problems that occur with current drugs.
The group’s research began with epoxyketone, a molecule isolated from a cyanobacterium called carmaphycin, whose reactive group is the same as that of the proteasome inhibitor carfilzomib.
“Epoxyketones are very potent, selective inhibitors of the proteasome because they interact with this enzyme in 2 stages—the first reversible, and the second irreversible,” noted study author Daniela Trivella, PhD, of the Brazilian Biosciences National Laboratory at the Brazilian Center for Research in Energy and Materials in Campinas.
To optimize epoxyketone’s effects and find new reactive groups, the investigators developed and tested a series of synthetic analogs with slight structural modifications.
One of the molecules had an enone as a reactive group and had characteristics of carmaphycin and another natural molecule called syringolin, which was isolated from plant pathogens.
By investigating the reaction mechanisms of the new molecule, called carmaphycin-syringolin enone, the team verified that the enone interacts with the proteasome in 2 stages, with the second stage being irreversible.
The investigators also observed that, in the case of the enone, the second reaction occurs more slowly, increasing the duration of the reversible phase of carmaphycin-syringolin enone inhibition.
“Because the irreversible inactivation of the proteasome has toxic effects, the best window of reversibility observed for the carmaphycin-syringolin enone will potentially reduce the toxicity of this new class of proteasome inhibitors,” Dr Trivella said. “The compound would therefore present a balance between selectivity and potency.”
Toxicity tests are still underway. But the investigators have already conducted studies to determine exactly how the interaction between the enzyme target and the carmaphycin-syringolin enone target occurs.
“We discovered that a chemical reaction called hydroamination occurs, which had never before [been] seen under physiological conditions,” Dr Trivella said.
“This type of reaction is frequently used by synthetic chemists in preparing substances, but, normally, it requires very specific temperature and pH conditions and the use of catalysts to occur. It has never been reported as a mechanism of enzyme inhibition.”
Inspired by this new mechanism for proteasome inhibition, the investigators plan to synthesize and test a new series of carmaphycin-syringolin enone analogs to determine their effects on the therapeutic window and assess whether they are also capable of reacting with proteasomes that are resistant to traditional inhibitors.
AVAHO 2014 Meeting: Lymphoma Mini-Symposium Preview
Federal Practitioner recently talked with Dr. Adrian Weistner and Dr. Mark Roschewski of the National Institutes of Health. Both doctors will be presenting during the September 12, 2014 Lymphoma Mini-Symposium and panel discussion that kicks off this weekend’s 2014 AVAHO Meeting in Portland, Oregon.
Federal Practitioner recently talked with Dr. Adrian Weistner and Dr. Mark Roschewski of the National Institutes of Health. Both doctors will be presenting during the September 12, 2014 Lymphoma Mini-Symposium and panel discussion that kicks off this weekend’s 2014 AVAHO Meeting in Portland, Oregon.
Federal Practitioner recently talked with Dr. Adrian Weistner and Dr. Mark Roschewski of the National Institutes of Health. Both doctors will be presenting during the September 12, 2014 Lymphoma Mini-Symposium and panel discussion that kicks off this weekend’s 2014 AVAHO Meeting in Portland, Oregon.
Cancer centers may not allow for dignified deaths
Credit: NCI and
Mathews Media Group
A new study suggests many patients in cancer centers do not experience a dignified death.
Study investigators surveyed physicians and nurses in 16 hospitals belonging to 10 cancer centers in Baden-Württemberg, Germany.
The results revealed a need for cancer centers to invest more in palliative care services, adequate rooms for dying patients, staff training in end-of-life care, and advance-care-planning standards.
Karin Jors, of the University Medical Center Freiburg, and her colleagues reported these findings in Cancer.
Previous research has shown that hospitals are often ill-prepared to provide care for dying patients.
To investigate whether the circumstances for dying on cancer center wards allow for a dignified death, Jors and her colleagues surveyed physicians and nurses in German cancer centers.
Among 1131 survey respondents, 57% believed that patients could die with dignity on their ward.
Half of the surveyed staff members indicated that they rarely have enough time to care for dying patients, and 55% found the rooms available for dying patients unsatisfactory.
Only 19% of respondents felt they had been well-prepared to care for dying patients, and only 6% of physicians felt that way.
On the other hand, physicians perceived the circumstances for dying patients much more positively than nurses, especially regarding communication and life-prolonging measures.
While 72% of physicians reported that patients can usually die a dignified death on their ward, only 52% of nurses shared this opinion.
Palliative care staff reported much better conditions for dying patients than staff from other wards, with 95% of palliative care staff indicating that patients die with dignity on their wards.
“In our aging society, it is predicted that the number of hospital deaths will continue to rise in the coming years, and many of these deaths will be attributable to cancer,” Jors said.
“For this reason, it is particularly important that cancer centers strive to create a comfortable, dignified experience for dying patients and their families. Above all, this requires that staff members are provided with the adequate resources to care for these patients.”
The investigators therefore encourage the integration of palliative care into standard oncology care, beginning as early as diagnosis. They also believe physicians and nurses would benefit from increased education and training in end-of-life care.

Credit: NCI and
Mathews Media Group
A new study suggests many patients in cancer centers do not experience a dignified death.
Study investigators surveyed physicians and nurses in 16 hospitals belonging to 10 cancer centers in Baden-Württemberg, Germany.
The results revealed a need for cancer centers to invest more in palliative care services, adequate rooms for dying patients, staff training in end-of-life care, and advance-care-planning standards.
Karin Jors, of the University Medical Center Freiburg, and her colleagues reported these findings in Cancer.
Previous research has shown that hospitals are often ill-prepared to provide care for dying patients.
To investigate whether the circumstances for dying on cancer center wards allow for a dignified death, Jors and her colleagues surveyed physicians and nurses in German cancer centers.
Among 1131 survey respondents, 57% believed that patients could die with dignity on their ward.
Half of the surveyed staff members indicated that they rarely have enough time to care for dying patients, and 55% found the rooms available for dying patients unsatisfactory.
Only 19% of respondents felt they had been well-prepared to care for dying patients, and only 6% of physicians felt that way.
On the other hand, physicians perceived the circumstances for dying patients much more positively than nurses, especially regarding communication and life-prolonging measures.
While 72% of physicians reported that patients can usually die a dignified death on their ward, only 52% of nurses shared this opinion.
Palliative care staff reported much better conditions for dying patients than staff from other wards, with 95% of palliative care staff indicating that patients die with dignity on their wards.
“In our aging society, it is predicted that the number of hospital deaths will continue to rise in the coming years, and many of these deaths will be attributable to cancer,” Jors said.
“For this reason, it is particularly important that cancer centers strive to create a comfortable, dignified experience for dying patients and their families. Above all, this requires that staff members are provided with the adequate resources to care for these patients.”
The investigators therefore encourage the integration of palliative care into standard oncology care, beginning as early as diagnosis. They also believe physicians and nurses would benefit from increased education and training in end-of-life care.

Credit: NCI and
Mathews Media Group
A new study suggests many patients in cancer centers do not experience a dignified death.
Study investigators surveyed physicians and nurses in 16 hospitals belonging to 10 cancer centers in Baden-Württemberg, Germany.
The results revealed a need for cancer centers to invest more in palliative care services, adequate rooms for dying patients, staff training in end-of-life care, and advance-care-planning standards.
Karin Jors, of the University Medical Center Freiburg, and her colleagues reported these findings in Cancer.
Previous research has shown that hospitals are often ill-prepared to provide care for dying patients.
To investigate whether the circumstances for dying on cancer center wards allow for a dignified death, Jors and her colleagues surveyed physicians and nurses in German cancer centers.
Among 1131 survey respondents, 57% believed that patients could die with dignity on their ward.
Half of the surveyed staff members indicated that they rarely have enough time to care for dying patients, and 55% found the rooms available for dying patients unsatisfactory.
Only 19% of respondents felt they had been well-prepared to care for dying patients, and only 6% of physicians felt that way.
On the other hand, physicians perceived the circumstances for dying patients much more positively than nurses, especially regarding communication and life-prolonging measures.
While 72% of physicians reported that patients can usually die a dignified death on their ward, only 52% of nurses shared this opinion.
Palliative care staff reported much better conditions for dying patients than staff from other wards, with 95% of palliative care staff indicating that patients die with dignity on their wards.
“In our aging society, it is predicted that the number of hospital deaths will continue to rise in the coming years, and many of these deaths will be attributable to cancer,” Jors said.
“For this reason, it is particularly important that cancer centers strive to create a comfortable, dignified experience for dying patients and their families. Above all, this requires that staff members are provided with the adequate resources to care for these patients.”
The investigators therefore encourage the integration of palliative care into standard oncology care, beginning as early as diagnosis. They also believe physicians and nurses would benefit from increased education and training in end-of-life care.
