User login
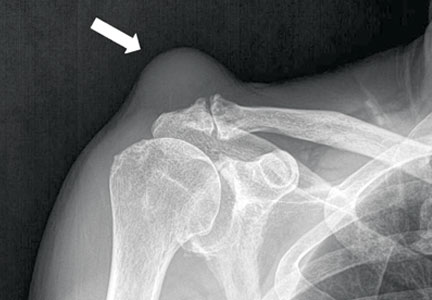
Complicated Acromioclavicular Joint Cyst With Massive Rotator Cuff Tear
A Comparison of Acetate and Digital Templating for Hip Resurfacing
Prediction of Semitendinosus and Gracilis Tendon Lengths and Diameters for Double Bundle ACL Reconstruction
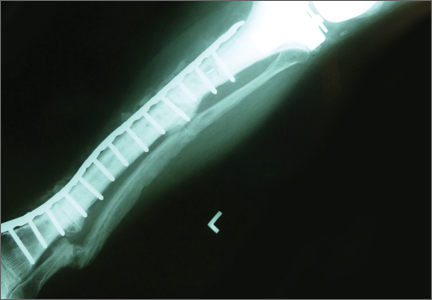
Minimally-Invasive Bone Graft Harvesting Technique Without Sophisticated Instruments
Total Knee Arthroplasty With Concurrent Femoral and Tibial Osteotomies in Osteogenesis Imperfecta
All-Polyethylene Tibial Components in Octogenarians: Survivorship, Performance, and Cost
Symptomatic Carpal Coalition: Scaphotrapezial Joint
Failure of a Constrained Acetabular Liner Without Reinforcement Ring Disruption
International Consensus on Periprosthetic Joint Infection: What Was Discussed and Decided?
Periprosthetic joint infection (PJI), with all its disastrous implications, continues to pose a challenge to the orthopedic community. Practicing orthopedic surgeons have invested great efforts to implement strategies to minimize surgical site infection (SSI). Although high-level evidence supports some of these practices, many have little or no scientific foundation. As a result, there is a remarkable variation in practices across the globe for prevention and management of PJI.
Some of the many questions the orthopedic community faces on a daily basis, include:
◾ Should a laminar flow room be used for elective arthroplasty?
◾ How much, and which antibiotic should be added to cement spacers?
◾ What metric should be used to decide on the optimal timing of reimplantation?
◾ What are the indications and contraindications for irrigation and debridement?
◾ How many irrigation and debridement in a joint should
be attempted before resection arthroplasty needs to be considered?
The medical community understands the importance of high-level evidence and engages in the generation of such whenever possible. The community also recognizes that some aspects of medicine will never lend themselves to the generation of high-level evidence nor should it attempt to do so. It is with the recognition of the latter that The International Consensus Meeting on Periprosthetic Joint Infection was organized. Delegates from various disciplines including orthopedic surgery, infectious disease, musculoskeletal pathology, microbiology, anesthesiology, dermatology, nuclear medicine, rheumatology, musculoskeletal radiology, veterinary surgery, pharmacy, and numerous scientists with interest in orthopedic infections came together to evaluate the available evidence, when present, or reach consensus regarding current practices for management of SSI/PJI. The process of generating the consensus has spanned over 10 months. Every stone has been turned in search of evidence for these questions, with over 3,500 related publications evaluated. The evidence, when available, has been assessed. Otherwise, the cumulative wisdom of 400 delegates from 52 countries and over 100 societies has been amassed to reach consensus about practices that lack higher level of evidence. The members of the Musculoskeletal Infection Society (MSIS) and the European Bone and Joint Infection Society (EBJIS), the 2 societies with a mission is to improve care of patients with musculoskeletal infection, have contributed to this initiative immensely.
The delegates have been engaged every step of the way by communicating through a social website generated for this purpose, with over 25,000 communications exchanged. The consensus document has been developed using the Delphi method under the leadership of Dr. Cats-Baril, a world-renowned expert in consensus development. The design of the consensus process was to include as many stakeholders as possible, allow participation in multiple forums, and provide a comprehensive review of the literature. The topics that were covered included the following: mitigation and education on comorbidities associated with increased SSI/PJI, perioperative skin preparation, perioperative antibiotics, operative environment, blood conservation, prosthesis selection, diagnosis of PJI, wound management, spacers, irrigation and debridement, antibiotic treatment and timing of reimplantation, 1-stage versus 2-stage exchange arthroplasty, management of fungal or atypical PJI, oral antibiotic therapy, and prevention of late PJI. Every consensus statement has undergone extreme scrutiny, especially by those with expertise in a specific area, to ensure that implementation of these practices will indeed lead to improvement of patient care.
After synthesizing the literature and assembling a preliminary draft of the consensus statement, over 300 delegates attended a face-to-face meeting in Philadelphia, were involved in active discussions, and voted on the questions/consensus statements. The delegates first met on July 31, 2013, in smaller workgroups, to discuss and resolve any discrepancies and finalize their statements. Then, they met in the general assembly for further discussion of questions and consensus statements. After revising the consensus statements, the finalized consensus statement was assembled and forwarded to the Audience Response System that evening, with voting occurring on the next day. On August 1, 2013 the delegates came into the general assembly and voted on the 207 questions/consensus statements that were being presented. The voting process was conducted using electronic keypads, where one could agree with the consensus statement, disagree with the consensus statement, or abstain from voting. The strength of the consensus was judged by the following scale: 1) Simple Majority: No Consensus (50.1%-59% agreement), 2) Majority: Weak Consensus (60%-65% agreement), 3) Super Majority: Strong Consensus (66%-99% agreement) and 4) Unanimous: 100% agreement. Of the 207 questions, there was unanimous vote for one question (controlling operating room traffic), 202 questions received super majority (strong consensus), 2 questions had weak consensus, and only 3 questions did not achieve any consensus.
The document generated(REF) is the result of innumerable hours of work by the liaisons, leaders and delegates dedicated to this initiative. We are certain that the “best practice guide” set forth by this initiative will serve many of our patients for years to come.
It is essential to state that the information contained in this document is merely a guide to practicing physicians who treat patients with musculoskeletal infection and should not be considered as a standard of care. Clinicians should exercise their wisdom and clinical acumen in making decisions related to each individual patient. In some circumstances this may require implementation of care that differs from what is stated in this document.
Periprosthetic joint infection (PJI), with all its disastrous implications, continues to pose a challenge to the orthopedic community. Practicing orthopedic surgeons have invested great efforts to implement strategies to minimize surgical site infection (SSI). Although high-level evidence supports some of these practices, many have little or no scientific foundation. As a result, there is a remarkable variation in practices across the globe for prevention and management of PJI.
Some of the many questions the orthopedic community faces on a daily basis, include:
◾ Should a laminar flow room be used for elective arthroplasty?
◾ How much, and which antibiotic should be added to cement spacers?
◾ What metric should be used to decide on the optimal timing of reimplantation?
◾ What are the indications and contraindications for irrigation and debridement?
◾ How many irrigation and debridement in a joint should
be attempted before resection arthroplasty needs to be considered?
The medical community understands the importance of high-level evidence and engages in the generation of such whenever possible. The community also recognizes that some aspects of medicine will never lend themselves to the generation of high-level evidence nor should it attempt to do so. It is with the recognition of the latter that The International Consensus Meeting on Periprosthetic Joint Infection was organized. Delegates from various disciplines including orthopedic surgery, infectious disease, musculoskeletal pathology, microbiology, anesthesiology, dermatology, nuclear medicine, rheumatology, musculoskeletal radiology, veterinary surgery, pharmacy, and numerous scientists with interest in orthopedic infections came together to evaluate the available evidence, when present, or reach consensus regarding current practices for management of SSI/PJI. The process of generating the consensus has spanned over 10 months. Every stone has been turned in search of evidence for these questions, with over 3,500 related publications evaluated. The evidence, when available, has been assessed. Otherwise, the cumulative wisdom of 400 delegates from 52 countries and over 100 societies has been amassed to reach consensus about practices that lack higher level of evidence. The members of the Musculoskeletal Infection Society (MSIS) and the European Bone and Joint Infection Society (EBJIS), the 2 societies with a mission is to improve care of patients with musculoskeletal infection, have contributed to this initiative immensely.
The delegates have been engaged every step of the way by communicating through a social website generated for this purpose, with over 25,000 communications exchanged. The consensus document has been developed using the Delphi method under the leadership of Dr. Cats-Baril, a world-renowned expert in consensus development. The design of the consensus process was to include as many stakeholders as possible, allow participation in multiple forums, and provide a comprehensive review of the literature. The topics that were covered included the following: mitigation and education on comorbidities associated with increased SSI/PJI, perioperative skin preparation, perioperative antibiotics, operative environment, blood conservation, prosthesis selection, diagnosis of PJI, wound management, spacers, irrigation and debridement, antibiotic treatment and timing of reimplantation, 1-stage versus 2-stage exchange arthroplasty, management of fungal or atypical PJI, oral antibiotic therapy, and prevention of late PJI. Every consensus statement has undergone extreme scrutiny, especially by those with expertise in a specific area, to ensure that implementation of these practices will indeed lead to improvement of patient care.
After synthesizing the literature and assembling a preliminary draft of the consensus statement, over 300 delegates attended a face-to-face meeting in Philadelphia, were involved in active discussions, and voted on the questions/consensus statements. The delegates first met on July 31, 2013, in smaller workgroups, to discuss and resolve any discrepancies and finalize their statements. Then, they met in the general assembly for further discussion of questions and consensus statements. After revising the consensus statements, the finalized consensus statement was assembled and forwarded to the Audience Response System that evening, with voting occurring on the next day. On August 1, 2013 the delegates came into the general assembly and voted on the 207 questions/consensus statements that were being presented. The voting process was conducted using electronic keypads, where one could agree with the consensus statement, disagree with the consensus statement, or abstain from voting. The strength of the consensus was judged by the following scale: 1) Simple Majority: No Consensus (50.1%-59% agreement), 2) Majority: Weak Consensus (60%-65% agreement), 3) Super Majority: Strong Consensus (66%-99% agreement) and 4) Unanimous: 100% agreement. Of the 207 questions, there was unanimous vote for one question (controlling operating room traffic), 202 questions received super majority (strong consensus), 2 questions had weak consensus, and only 3 questions did not achieve any consensus.
The document generated(REF) is the result of innumerable hours of work by the liaisons, leaders and delegates dedicated to this initiative. We are certain that the “best practice guide” set forth by this initiative will serve many of our patients for years to come.
It is essential to state that the information contained in this document is merely a guide to practicing physicians who treat patients with musculoskeletal infection and should not be considered as a standard of care. Clinicians should exercise their wisdom and clinical acumen in making decisions related to each individual patient. In some circumstances this may require implementation of care that differs from what is stated in this document.
Periprosthetic joint infection (PJI), with all its disastrous implications, continues to pose a challenge to the orthopedic community. Practicing orthopedic surgeons have invested great efforts to implement strategies to minimize surgical site infection (SSI). Although high-level evidence supports some of these practices, many have little or no scientific foundation. As a result, there is a remarkable variation in practices across the globe for prevention and management of PJI.
Some of the many questions the orthopedic community faces on a daily basis, include:
◾ Should a laminar flow room be used for elective arthroplasty?
◾ How much, and which antibiotic should be added to cement spacers?
◾ What metric should be used to decide on the optimal timing of reimplantation?
◾ What are the indications and contraindications for irrigation and debridement?
◾ How many irrigation and debridement in a joint should
be attempted before resection arthroplasty needs to be considered?
The medical community understands the importance of high-level evidence and engages in the generation of such whenever possible. The community also recognizes that some aspects of medicine will never lend themselves to the generation of high-level evidence nor should it attempt to do so. It is with the recognition of the latter that The International Consensus Meeting on Periprosthetic Joint Infection was organized. Delegates from various disciplines including orthopedic surgery, infectious disease, musculoskeletal pathology, microbiology, anesthesiology, dermatology, nuclear medicine, rheumatology, musculoskeletal radiology, veterinary surgery, pharmacy, and numerous scientists with interest in orthopedic infections came together to evaluate the available evidence, when present, or reach consensus regarding current practices for management of SSI/PJI. The process of generating the consensus has spanned over 10 months. Every stone has been turned in search of evidence for these questions, with over 3,500 related publications evaluated. The evidence, when available, has been assessed. Otherwise, the cumulative wisdom of 400 delegates from 52 countries and over 100 societies has been amassed to reach consensus about practices that lack higher level of evidence. The members of the Musculoskeletal Infection Society (MSIS) and the European Bone and Joint Infection Society (EBJIS), the 2 societies with a mission is to improve care of patients with musculoskeletal infection, have contributed to this initiative immensely.
The delegates have been engaged every step of the way by communicating through a social website generated for this purpose, with over 25,000 communications exchanged. The consensus document has been developed using the Delphi method under the leadership of Dr. Cats-Baril, a world-renowned expert in consensus development. The design of the consensus process was to include as many stakeholders as possible, allow participation in multiple forums, and provide a comprehensive review of the literature. The topics that were covered included the following: mitigation and education on comorbidities associated with increased SSI/PJI, perioperative skin preparation, perioperative antibiotics, operative environment, blood conservation, prosthesis selection, diagnosis of PJI, wound management, spacers, irrigation and debridement, antibiotic treatment and timing of reimplantation, 1-stage versus 2-stage exchange arthroplasty, management of fungal or atypical PJI, oral antibiotic therapy, and prevention of late PJI. Every consensus statement has undergone extreme scrutiny, especially by those with expertise in a specific area, to ensure that implementation of these practices will indeed lead to improvement of patient care.
After synthesizing the literature and assembling a preliminary draft of the consensus statement, over 300 delegates attended a face-to-face meeting in Philadelphia, were involved in active discussions, and voted on the questions/consensus statements. The delegates first met on July 31, 2013, in smaller workgroups, to discuss and resolve any discrepancies and finalize their statements. Then, they met in the general assembly for further discussion of questions and consensus statements. After revising the consensus statements, the finalized consensus statement was assembled and forwarded to the Audience Response System that evening, with voting occurring on the next day. On August 1, 2013 the delegates came into the general assembly and voted on the 207 questions/consensus statements that were being presented. The voting process was conducted using electronic keypads, where one could agree with the consensus statement, disagree with the consensus statement, or abstain from voting. The strength of the consensus was judged by the following scale: 1) Simple Majority: No Consensus (50.1%-59% agreement), 2) Majority: Weak Consensus (60%-65% agreement), 3) Super Majority: Strong Consensus (66%-99% agreement) and 4) Unanimous: 100% agreement. Of the 207 questions, there was unanimous vote for one question (controlling operating room traffic), 202 questions received super majority (strong consensus), 2 questions had weak consensus, and only 3 questions did not achieve any consensus.
The document generated(REF) is the result of innumerable hours of work by the liaisons, leaders and delegates dedicated to this initiative. We are certain that the “best practice guide” set forth by this initiative will serve many of our patients for years to come.
It is essential to state that the information contained in this document is merely a guide to practicing physicians who treat patients with musculoskeletal infection and should not be considered as a standard of care. Clinicians should exercise their wisdom and clinical acumen in making decisions related to each individual patient. In some circumstances this may require implementation of care that differs from what is stated in this document.
Navigation in Total Knee Arthroplasty: Truth, Myths, and Controversies
The overall success of total knee arthroplasty (TKA) depends on proper implant choice, meticulous surgical technique, appropriate patient selection, and
effective postoperative rehabilitation. Inappropriate technique leads to suboptimal placement of implants in coronal, sagittal, or axial planes.1-3 This results in eccentric prosthetic loading, which may contribute to accelerated polyethylene wear, early component loosening, higher rates of revision surgery, and unsatisfactory clinical outcomes. The need to optimize component positioning during TKA stimulated the development of computer-assisted navigation in TKA in the late 1990’s. Proponents of this technology believe that it helps to reduce outliers, improves coronal, sagittal, and rotational alignment, and optimizes flexion and extension gap-balancing. This is believed to result in improved implant survival and better functional outcomes. However, despite these postulated advantages, less than 5% of surgeons in the United States currently use navigation during TKA perhaps due to concerns of costs, increased operating time, learn- ing curve issues, and lack of improvement in functional outcomes at mid-term follow-up.
Navigated TKA, due to its accuracy and low margins of error, has the potential to reduce component malalignment to within 1o to 2o of neutral mechanical axis.4 However, others have reported that alignment of the femoral and tibial components achieved with computer navigation is not different than TKA using conventional techniques.5-12 This lack of improvement reported in these studies may be due to a number of potential sources of errors, which can be either surgeon- or device-related. These errors may pre-dispose to discrepancies between alignments calculated by the computer and the actual position of the implants. Apart from software- and hardware-related calibration issues, the majority of inaccuracies, which are often surgeon-related, result from registration of anatomical landmarks, pin array movements after registration, incorrect bone cuts despite accurate jig placement, and incorrect placement of final components during cementation. Of these surgeon-related factors, variability in the identification of the anatomical landmarks appears to be critical and occurs due to anatomical variations or from inaccurate recognition of intraoperative bony landmarks. A recent study found that registration of the distal femoral epicondyles was more likely to be inaccurate than other anatomical landmarks, as it was found that a small change of 2 mm in the sagittal plane can lead to a 1o change in the femoral component rotation.13
Nevertheless, the general consensus from recent high- level evidence (Level I and II) suggests that navigated TKA leads to improved coronal-alignment outcomes and reduced numbers of outliers.14-18 In a recent systematic review of 27 randomized controlled trials of 2541 patients, Hetaimish and colleagues19 compared the alignment outcomes of navigated with conventional TKA. The authors found that the navigated cohort had a significantly lower risk of producing a mechanical axis deviation of greater than 3o, compared with conventional TKA (relative risk [RR] = 0.37; P<.001). The femoral and tibial, coronal and sagittal malalignment (>3o) were also found to be significantly lower with navigated TKA, compared with conventional techniques. However, no substantial differences were found in the rotation alignment of the femoral component between the 2 comparison cohorts (navigated group, 18.8%; conventional group, 14.5%).
Advocates of navigation believe that improved component alignment would lead to better functional outcomes and lower revision rates.20,21 However, at short- to mid-term follow-up, most studies have failed to show any substantial benefits in terms of functional outcomes, revision rates, patient satisfaction, or patient-perceived quality-of-life, when comparing computer-assisted navigation to conventional techniques.11,22-25 Recent systematic reviews by Zamora et al24 and Burnett et al25 found no significant differences in the functional outcomes between navigated and conventional TKA (P>.05). This lack of the expected improvement in functional outcomes reported in various studies with navigation could be due to variability in registration of anatomical landmarks leading to errors in the rotational axis, or a lack of complete understanding of the interplay of alignment, ligament balance, in vivo joint loading and kinematics. In a report from the Mayo Clinic,26 the authors believed that there may be little practical value in relying on a mechanical alignment of ±3o from neutral as an isolated variable in predicting the longevity of modern TKA. In addition, they suggested that factors apart from mechanical alignment may have a more profound impact on implant durability.
Several studies27-31 that compared the joint line changes or ligament balance between navigated and conventional TKA, report no substantial differences in the maintenance of the joint line, quality of life, and functional outcomes. Despite claims of decreased blood loss, length-of stay, cardiac complications, and lower risks of fat embolism with computer-assisted navigation by some authors, other reports have failed to demonstrate any substantial advantages, therefore, it is controversial if any clear benefit exists.6,32-34 It is postulated that the high initial institutional costs of navigation can even out in the long run if the goals of improved survivorship and functional outcomes are achieved.35 However, as mid-term follow-up studies have failed to show a survival or functional benefit, the purported costs savings from computer navigation may not be accurate. Navigated TKA has been reported to increase operative time by about 15 to 20 minutes, compared with conventional TKA. Although, this increases operative time, it has not been reported to increase the risk of deep prosthetic joint infections.
Navigation provides some benefits in terms of radiological alignment. However, the clinical advantages are yet to be defined. Currently, there are many unanswered ques- tions concerning alignment in TKA, such as having a more individual approach based on the patients’ own anatomic variations including considerations about the presence of constitutional varus in patients. Navigation may have a role when TKA is performed for complex deformities, fractures, or in the presence of retained implants that prevent the use of conventional guides. Nevertheless, one should always keep in mind cost considerations. This has been true with any technological advancement we have had in the past and will be of concern in the future as well, especially with rising healthcare costs. When analyzing costs with naviga- tion, one must take in to account not only the overall costs of technology, but also the added costs of training, increased operating room times, and disposables when performing these procedures. Although we are advocates of change and are excited about this technology, the cost-benefit ratio for computer navigated TKA needs to be reconciled.
The overall success of total knee arthroplasty (TKA) depends on proper implant choice, meticulous surgical technique, appropriate patient selection, and
effective postoperative rehabilitation. Inappropriate technique leads to suboptimal placement of implants in coronal, sagittal, or axial planes.1-3 This results in eccentric prosthetic loading, which may contribute to accelerated polyethylene wear, early component loosening, higher rates of revision surgery, and unsatisfactory clinical outcomes. The need to optimize component positioning during TKA stimulated the development of computer-assisted navigation in TKA in the late 1990’s. Proponents of this technology believe that it helps to reduce outliers, improves coronal, sagittal, and rotational alignment, and optimizes flexion and extension gap-balancing. This is believed to result in improved implant survival and better functional outcomes. However, despite these postulated advantages, less than 5% of surgeons in the United States currently use navigation during TKA perhaps due to concerns of costs, increased operating time, learn- ing curve issues, and lack of improvement in functional outcomes at mid-term follow-up.
Navigated TKA, due to its accuracy and low margins of error, has the potential to reduce component malalignment to within 1o to 2o of neutral mechanical axis.4 However, others have reported that alignment of the femoral and tibial components achieved with computer navigation is not different than TKA using conventional techniques.5-12 This lack of improvement reported in these studies may be due to a number of potential sources of errors, which can be either surgeon- or device-related. These errors may pre-dispose to discrepancies between alignments calculated by the computer and the actual position of the implants. Apart from software- and hardware-related calibration issues, the majority of inaccuracies, which are often surgeon-related, result from registration of anatomical landmarks, pin array movements after registration, incorrect bone cuts despite accurate jig placement, and incorrect placement of final components during cementation. Of these surgeon-related factors, variability in the identification of the anatomical landmarks appears to be critical and occurs due to anatomical variations or from inaccurate recognition of intraoperative bony landmarks. A recent study found that registration of the distal femoral epicondyles was more likely to be inaccurate than other anatomical landmarks, as it was found that a small change of 2 mm in the sagittal plane can lead to a 1o change in the femoral component rotation.13
Nevertheless, the general consensus from recent high- level evidence (Level I and II) suggests that navigated TKA leads to improved coronal-alignment outcomes and reduced numbers of outliers.14-18 In a recent systematic review of 27 randomized controlled trials of 2541 patients, Hetaimish and colleagues19 compared the alignment outcomes of navigated with conventional TKA. The authors found that the navigated cohort had a significantly lower risk of producing a mechanical axis deviation of greater than 3o, compared with conventional TKA (relative risk [RR] = 0.37; P<.001). The femoral and tibial, coronal and sagittal malalignment (>3o) were also found to be significantly lower with navigated TKA, compared with conventional techniques. However, no substantial differences were found in the rotation alignment of the femoral component between the 2 comparison cohorts (navigated group, 18.8%; conventional group, 14.5%).
Advocates of navigation believe that improved component alignment would lead to better functional outcomes and lower revision rates.20,21 However, at short- to mid-term follow-up, most studies have failed to show any substantial benefits in terms of functional outcomes, revision rates, patient satisfaction, or patient-perceived quality-of-life, when comparing computer-assisted navigation to conventional techniques.11,22-25 Recent systematic reviews by Zamora et al24 and Burnett et al25 found no significant differences in the functional outcomes between navigated and conventional TKA (P>.05). This lack of the expected improvement in functional outcomes reported in various studies with navigation could be due to variability in registration of anatomical landmarks leading to errors in the rotational axis, or a lack of complete understanding of the interplay of alignment, ligament balance, in vivo joint loading and kinematics. In a report from the Mayo Clinic,26 the authors believed that there may be little practical value in relying on a mechanical alignment of ±3o from neutral as an isolated variable in predicting the longevity of modern TKA. In addition, they suggested that factors apart from mechanical alignment may have a more profound impact on implant durability.
Several studies27-31 that compared the joint line changes or ligament balance between navigated and conventional TKA, report no substantial differences in the maintenance of the joint line, quality of life, and functional outcomes. Despite claims of decreased blood loss, length-of stay, cardiac complications, and lower risks of fat embolism with computer-assisted navigation by some authors, other reports have failed to demonstrate any substantial advantages, therefore, it is controversial if any clear benefit exists.6,32-34 It is postulated that the high initial institutional costs of navigation can even out in the long run if the goals of improved survivorship and functional outcomes are achieved.35 However, as mid-term follow-up studies have failed to show a survival or functional benefit, the purported costs savings from computer navigation may not be accurate. Navigated TKA has been reported to increase operative time by about 15 to 20 minutes, compared with conventional TKA. Although, this increases operative time, it has not been reported to increase the risk of deep prosthetic joint infections.
Navigation provides some benefits in terms of radiological alignment. However, the clinical advantages are yet to be defined. Currently, there are many unanswered ques- tions concerning alignment in TKA, such as having a more individual approach based on the patients’ own anatomic variations including considerations about the presence of constitutional varus in patients. Navigation may have a role when TKA is performed for complex deformities, fractures, or in the presence of retained implants that prevent the use of conventional guides. Nevertheless, one should always keep in mind cost considerations. This has been true with any technological advancement we have had in the past and will be of concern in the future as well, especially with rising healthcare costs. When analyzing costs with naviga- tion, one must take in to account not only the overall costs of technology, but also the added costs of training, increased operating room times, and disposables when performing these procedures. Although we are advocates of change and are excited about this technology, the cost-benefit ratio for computer navigated TKA needs to be reconciled.
The overall success of total knee arthroplasty (TKA) depends on proper implant choice, meticulous surgical technique, appropriate patient selection, and
effective postoperative rehabilitation. Inappropriate technique leads to suboptimal placement of implants in coronal, sagittal, or axial planes.1-3 This results in eccentric prosthetic loading, which may contribute to accelerated polyethylene wear, early component loosening, higher rates of revision surgery, and unsatisfactory clinical outcomes. The need to optimize component positioning during TKA stimulated the development of computer-assisted navigation in TKA in the late 1990’s. Proponents of this technology believe that it helps to reduce outliers, improves coronal, sagittal, and rotational alignment, and optimizes flexion and extension gap-balancing. This is believed to result in improved implant survival and better functional outcomes. However, despite these postulated advantages, less than 5% of surgeons in the United States currently use navigation during TKA perhaps due to concerns of costs, increased operating time, learn- ing curve issues, and lack of improvement in functional outcomes at mid-term follow-up.
Navigated TKA, due to its accuracy and low margins of error, has the potential to reduce component malalignment to within 1o to 2o of neutral mechanical axis.4 However, others have reported that alignment of the femoral and tibial components achieved with computer navigation is not different than TKA using conventional techniques.5-12 This lack of improvement reported in these studies may be due to a number of potential sources of errors, which can be either surgeon- or device-related. These errors may pre-dispose to discrepancies between alignments calculated by the computer and the actual position of the implants. Apart from software- and hardware-related calibration issues, the majority of inaccuracies, which are often surgeon-related, result from registration of anatomical landmarks, pin array movements after registration, incorrect bone cuts despite accurate jig placement, and incorrect placement of final components during cementation. Of these surgeon-related factors, variability in the identification of the anatomical landmarks appears to be critical and occurs due to anatomical variations or from inaccurate recognition of intraoperative bony landmarks. A recent study found that registration of the distal femoral epicondyles was more likely to be inaccurate than other anatomical landmarks, as it was found that a small change of 2 mm in the sagittal plane can lead to a 1o change in the femoral component rotation.13
Nevertheless, the general consensus from recent high- level evidence (Level I and II) suggests that navigated TKA leads to improved coronal-alignment outcomes and reduced numbers of outliers.14-18 In a recent systematic review of 27 randomized controlled trials of 2541 patients, Hetaimish and colleagues19 compared the alignment outcomes of navigated with conventional TKA. The authors found that the navigated cohort had a significantly lower risk of producing a mechanical axis deviation of greater than 3o, compared with conventional TKA (relative risk [RR] = 0.37; P<.001). The femoral and tibial, coronal and sagittal malalignment (>3o) were also found to be significantly lower with navigated TKA, compared with conventional techniques. However, no substantial differences were found in the rotation alignment of the femoral component between the 2 comparison cohorts (navigated group, 18.8%; conventional group, 14.5%).
Advocates of navigation believe that improved component alignment would lead to better functional outcomes and lower revision rates.20,21 However, at short- to mid-term follow-up, most studies have failed to show any substantial benefits in terms of functional outcomes, revision rates, patient satisfaction, or patient-perceived quality-of-life, when comparing computer-assisted navigation to conventional techniques.11,22-25 Recent systematic reviews by Zamora et al24 and Burnett et al25 found no significant differences in the functional outcomes between navigated and conventional TKA (P>.05). This lack of the expected improvement in functional outcomes reported in various studies with navigation could be due to variability in registration of anatomical landmarks leading to errors in the rotational axis, or a lack of complete understanding of the interplay of alignment, ligament balance, in vivo joint loading and kinematics. In a report from the Mayo Clinic,26 the authors believed that there may be little practical value in relying on a mechanical alignment of ±3o from neutral as an isolated variable in predicting the longevity of modern TKA. In addition, they suggested that factors apart from mechanical alignment may have a more profound impact on implant durability.
Several studies27-31 that compared the joint line changes or ligament balance between navigated and conventional TKA, report no substantial differences in the maintenance of the joint line, quality of life, and functional outcomes. Despite claims of decreased blood loss, length-of stay, cardiac complications, and lower risks of fat embolism with computer-assisted navigation by some authors, other reports have failed to demonstrate any substantial advantages, therefore, it is controversial if any clear benefit exists.6,32-34 It is postulated that the high initial institutional costs of navigation can even out in the long run if the goals of improved survivorship and functional outcomes are achieved.35 However, as mid-term follow-up studies have failed to show a survival or functional benefit, the purported costs savings from computer navigation may not be accurate. Navigated TKA has been reported to increase operative time by about 15 to 20 minutes, compared with conventional TKA. Although, this increases operative time, it has not been reported to increase the risk of deep prosthetic joint infections.
Navigation provides some benefits in terms of radiological alignment. However, the clinical advantages are yet to be defined. Currently, there are many unanswered ques- tions concerning alignment in TKA, such as having a more individual approach based on the patients’ own anatomic variations including considerations about the presence of constitutional varus in patients. Navigation may have a role when TKA is performed for complex deformities, fractures, or in the presence of retained implants that prevent the use of conventional guides. Nevertheless, one should always keep in mind cost considerations. This has been true with any technological advancement we have had in the past and will be of concern in the future as well, especially with rising healthcare costs. When analyzing costs with naviga- tion, one must take in to account not only the overall costs of technology, but also the added costs of training, increased operating room times, and disposables when performing these procedures. Although we are advocates of change and are excited about this technology, the cost-benefit ratio for computer navigated TKA needs to be reconciled.