User login
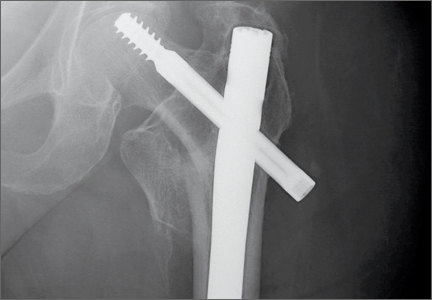
Conversion of Cephalomedullary Nail Fixation to Hip Arthroplasty: Technical Points and Pitfalls
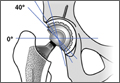
Effect of Acetabular Cup Abduction Angle on Wear of Ultrahigh-Molecular-Weight Polyethylene in Hip Simulator Testing
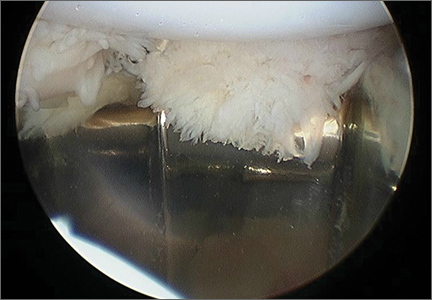
Patellofemoral Crepitation and Clunk Complicating Posterior-Stabilized Total Knee Arthroplasty
Biodegradable Surgical Pin Could Also Promote Bone Growth
Michele Manuel, PhD, Associate Professor of Materials Science and Engineering at the University of Florida in Gainesville, has developed a surgical pin made from magnesium and is working to control the rate at which the pin biodegrades in the body. In laboratory tests, the pin offered several advantages over traditional titanium, plastic, or stainless steel pins.
“The idea with this pin is that it would dissolve over time, and after it’s finished, your body is basically in the same state it was before you had an injury,” stated Dr. Manuel. “Surgical pins don’t have to become permanent fixtures in the body.”
In addition to being biodegradable, the pin also aids in the healing process. Magnesium builds bone, so it can function as a pin and as a nutrient. According to Dr. Manuel, the trick to using magnesium is controlling the rate at which it breaks down to give the body time to absorb the hydrogen that is release as a byproduct of breakdown. Along with controlling the rate at which the magnesium breaks down, Dr. Manuel is seeking to determine how much torque can be applied before the screw is stripped.
In laboratory tests, the magnesium pin has been inserted into the tibia of rats. X-rays show the rate at which the magnesium pins dissolve. At 6 weeks the new bone is indistinguishable from the bone before the break.
“People who have sensitivity to metal or inflammation from a foreign material in the body could benefit from this,” stated Dr. Manuel. “There are a lot of different applications that could be possible.”
Michele Manuel, PhD, Associate Professor of Materials Science and Engineering at the University of Florida in Gainesville, has developed a surgical pin made from magnesium and is working to control the rate at which the pin biodegrades in the body. In laboratory tests, the pin offered several advantages over traditional titanium, plastic, or stainless steel pins.
“The idea with this pin is that it would dissolve over time, and after it’s finished, your body is basically in the same state it was before you had an injury,” stated Dr. Manuel. “Surgical pins don’t have to become permanent fixtures in the body.”
In addition to being biodegradable, the pin also aids in the healing process. Magnesium builds bone, so it can function as a pin and as a nutrient. According to Dr. Manuel, the trick to using magnesium is controlling the rate at which it breaks down to give the body time to absorb the hydrogen that is release as a byproduct of breakdown. Along with controlling the rate at which the magnesium breaks down, Dr. Manuel is seeking to determine how much torque can be applied before the screw is stripped.
In laboratory tests, the magnesium pin has been inserted into the tibia of rats. X-rays show the rate at which the magnesium pins dissolve. At 6 weeks the new bone is indistinguishable from the bone before the break.
“People who have sensitivity to metal or inflammation from a foreign material in the body could benefit from this,” stated Dr. Manuel. “There are a lot of different applications that could be possible.”
Michele Manuel, PhD, Associate Professor of Materials Science and Engineering at the University of Florida in Gainesville, has developed a surgical pin made from magnesium and is working to control the rate at which the pin biodegrades in the body. In laboratory tests, the pin offered several advantages over traditional titanium, plastic, or stainless steel pins.
“The idea with this pin is that it would dissolve over time, and after it’s finished, your body is basically in the same state it was before you had an injury,” stated Dr. Manuel. “Surgical pins don’t have to become permanent fixtures in the body.”
In addition to being biodegradable, the pin also aids in the healing process. Magnesium builds bone, so it can function as a pin and as a nutrient. According to Dr. Manuel, the trick to using magnesium is controlling the rate at which it breaks down to give the body time to absorb the hydrogen that is release as a byproduct of breakdown. Along with controlling the rate at which the magnesium breaks down, Dr. Manuel is seeking to determine how much torque can be applied before the screw is stripped.
In laboratory tests, the magnesium pin has been inserted into the tibia of rats. X-rays show the rate at which the magnesium pins dissolve. At 6 weeks the new bone is indistinguishable from the bone before the break.
“People who have sensitivity to metal or inflammation from a foreign material in the body could benefit from this,” stated Dr. Manuel. “There are a lot of different applications that could be possible.”
Pro Baseball Pitchers’ Missed Days Attributed to Weak Core
Professional baseball pitchers with poor core stability are more likely to miss 30 or more days in a single season because of injury compared with pitchers who have good control of muscles in their pelvis and lower back, according to a study published August 26 online ahead of print in the American Journal of Sports Medicine.
The study shows association, not causation, but does suggest that pitchers might benefit from training to improve their lumbopelvic control. “The nice thing about lumbopelvic control is that there’s not any downside we can think of to trying to improve it,” said Ajit Chaudhari, PhD, Associate Professor of Health and Rehabilitation Sciences and of Orthopedics at The Ohio State University and lead author of the study.
A total of 347 pitchers were assessed for lumbopelvic control during spring training, then followed for the ensuing season. Most participants were between the ages of 18 and 22 years and played on teams at the developmental, minor league, or major league level.
Investigators tested their lumbopelvic control by assessing how much the pelvis tilted forward or backward as pitchers lifted a single foot about 10 cm in a movement similar to stepping up onto a curb or beginning a pitch. Study authors then placed an iPod-based tilt sensor on each participant’s sacrum and a score was assigned to each player based on the magnitude of the tilt.
Medical staff from each baseball organization recorded how many missed days players had throughout the season that followed spring training (a missed day was defined as any day a study participant could not complete his scheduled work because of an injury suffered during baseball-related activity). The majority of injuries recorded were elbow strains, shoulder strains, tears, and fractures. The subjects also were placed into 1 of 3 categories—those whose pelvises tilted less than 4 degrees, between 4 and 7.9 degrees, and more than 8 degrees from the starting position.
Players were categorized by the total numbers of days missed during the season (fewer than 30 days or 30 or more days). The analysis showed that the chances of missing 30 or more days in the season were 3 times higher for the high-tilt group than for pitchers in the lowest-tilt group. It was also 2.2 times higher than for players in the moderate-tilt group.
Further analysis suggested that of the 108 (31.1%) participants who missed at least 1 day because of injury, the average number of days missed was significantly different among the 3 groups. On average, those with poor lumbopelvic control missed 99 days, those with moderate control missed 46 days, and the well-controlled group missed 44 days.
“The core could help prevent injury by spreading out the energy load, allowing pitchers to use their legs more and their throwing arm less,” Dr. Chaudhari said.
Suggested Reading
Chaudhari AM, McKenzie CS, Pan X, Oñate JA. Lumbopelvic control and days missed because of injury in professional baseball pitchers. Am J Sports Med. 2014 Aug 26. pii: 0363546514545861. [Epub ahead of print]
Professional baseball pitchers with poor core stability are more likely to miss 30 or more days in a single season because of injury compared with pitchers who have good control of muscles in their pelvis and lower back, according to a study published August 26 online ahead of print in the American Journal of Sports Medicine.
The study shows association, not causation, but does suggest that pitchers might benefit from training to improve their lumbopelvic control. “The nice thing about lumbopelvic control is that there’s not any downside we can think of to trying to improve it,” said Ajit Chaudhari, PhD, Associate Professor of Health and Rehabilitation Sciences and of Orthopedics at The Ohio State University and lead author of the study.
A total of 347 pitchers were assessed for lumbopelvic control during spring training, then followed for the ensuing season. Most participants were between the ages of 18 and 22 years and played on teams at the developmental, minor league, or major league level.
Investigators tested their lumbopelvic control by assessing how much the pelvis tilted forward or backward as pitchers lifted a single foot about 10 cm in a movement similar to stepping up onto a curb or beginning a pitch. Study authors then placed an iPod-based tilt sensor on each participant’s sacrum and a score was assigned to each player based on the magnitude of the tilt.
Medical staff from each baseball organization recorded how many missed days players had throughout the season that followed spring training (a missed day was defined as any day a study participant could not complete his scheduled work because of an injury suffered during baseball-related activity). The majority of injuries recorded were elbow strains, shoulder strains, tears, and fractures. The subjects also were placed into 1 of 3 categories—those whose pelvises tilted less than 4 degrees, between 4 and 7.9 degrees, and more than 8 degrees from the starting position.
Players were categorized by the total numbers of days missed during the season (fewer than 30 days or 30 or more days). The analysis showed that the chances of missing 30 or more days in the season were 3 times higher for the high-tilt group than for pitchers in the lowest-tilt group. It was also 2.2 times higher than for players in the moderate-tilt group.
Further analysis suggested that of the 108 (31.1%) participants who missed at least 1 day because of injury, the average number of days missed was significantly different among the 3 groups. On average, those with poor lumbopelvic control missed 99 days, those with moderate control missed 46 days, and the well-controlled group missed 44 days.
“The core could help prevent injury by spreading out the energy load, allowing pitchers to use their legs more and their throwing arm less,” Dr. Chaudhari said.
Professional baseball pitchers with poor core stability are more likely to miss 30 or more days in a single season because of injury compared with pitchers who have good control of muscles in their pelvis and lower back, according to a study published August 26 online ahead of print in the American Journal of Sports Medicine.
The study shows association, not causation, but does suggest that pitchers might benefit from training to improve their lumbopelvic control. “The nice thing about lumbopelvic control is that there’s not any downside we can think of to trying to improve it,” said Ajit Chaudhari, PhD, Associate Professor of Health and Rehabilitation Sciences and of Orthopedics at The Ohio State University and lead author of the study.
A total of 347 pitchers were assessed for lumbopelvic control during spring training, then followed for the ensuing season. Most participants were between the ages of 18 and 22 years and played on teams at the developmental, minor league, or major league level.
Investigators tested their lumbopelvic control by assessing how much the pelvis tilted forward or backward as pitchers lifted a single foot about 10 cm in a movement similar to stepping up onto a curb or beginning a pitch. Study authors then placed an iPod-based tilt sensor on each participant’s sacrum and a score was assigned to each player based on the magnitude of the tilt.
Medical staff from each baseball organization recorded how many missed days players had throughout the season that followed spring training (a missed day was defined as any day a study participant could not complete his scheduled work because of an injury suffered during baseball-related activity). The majority of injuries recorded were elbow strains, shoulder strains, tears, and fractures. The subjects also were placed into 1 of 3 categories—those whose pelvises tilted less than 4 degrees, between 4 and 7.9 degrees, and more than 8 degrees from the starting position.
Players were categorized by the total numbers of days missed during the season (fewer than 30 days or 30 or more days). The analysis showed that the chances of missing 30 or more days in the season were 3 times higher for the high-tilt group than for pitchers in the lowest-tilt group. It was also 2.2 times higher than for players in the moderate-tilt group.
Further analysis suggested that of the 108 (31.1%) participants who missed at least 1 day because of injury, the average number of days missed was significantly different among the 3 groups. On average, those with poor lumbopelvic control missed 99 days, those with moderate control missed 46 days, and the well-controlled group missed 44 days.
“The core could help prevent injury by spreading out the energy load, allowing pitchers to use their legs more and their throwing arm less,” Dr. Chaudhari said.
Suggested Reading
Chaudhari AM, McKenzie CS, Pan X, Oñate JA. Lumbopelvic control and days missed because of injury in professional baseball pitchers. Am J Sports Med. 2014 Aug 26. pii: 0363546514545861. [Epub ahead of print]
Suggested Reading
Chaudhari AM, McKenzie CS, Pan X, Oñate JA. Lumbopelvic control and days missed because of injury in professional baseball pitchers. Am J Sports Med. 2014 Aug 26. pii: 0363546514545861. [Epub ahead of print]
Advanced Technology Reveals Tiny Strains in Body Tissue Pre-Injury
Researchers have developed algorithms to pinpoint weak spots in the tendons, bones, and muscles that are prone to breaking or tearing, according to a study published online August 27 in the Journal of the Royal Society Interface.
“Tendons are constantly stretching as muscles pull on them, and bones also bend or compress as we carry out everyday activities,” said senior investigator Stavros Thomopoulos, PhD, Professor of Orthopaedic Surgery at Washington University in St. Louis. “Small cracks or tears can result from these loads and lead to major injuries. Understanding how these tears and cracks develop over time therefore is important for diagnosing and tracking injuries.”
The investigators developed a way to visualize and predict spots where tissues are weakened. This was accomplished by stretching tissues and tracking the results as their shapes changed. Algorithms were then developed that can identify areas of weakening prior to breakage. The algorithm was tested in various materials and in animal models. “The new algorithm allowed us to find the places where the tears were beginning to form and to track them as they extended. Older algorithms are not as good at finding and tracking localized strains,” the researchers reported.
One of the two algorithms is 1,000 times more accurate than older methods at quantifying very large stretches near tiny cracks and tears. A second algorithm has the ability to predict where cracks and failures are likely to form.
Overall, the researchers aim to use these algorithms to prevent additional injuries following surgery to repair shoulders, knees, and other tissue. “It’s vital to understand the ways that physical forces cause structures and tissues to deform so that we can identify the onset of failures and eventually predict them.”
Suggested Reading
Boyle JJ, Kume M, Wyczalkowski MA, et al. Simple and accurate methods for quantifying deformation, disruption, and development in biological tissues. J R Soc Interface. 2014 Nov 6;11(100). pii: 20140685. doi: 10.1098/rsif.2014.0685.
Researchers have developed algorithms to pinpoint weak spots in the tendons, bones, and muscles that are prone to breaking or tearing, according to a study published online August 27 in the Journal of the Royal Society Interface.
“Tendons are constantly stretching as muscles pull on them, and bones also bend or compress as we carry out everyday activities,” said senior investigator Stavros Thomopoulos, PhD, Professor of Orthopaedic Surgery at Washington University in St. Louis. “Small cracks or tears can result from these loads and lead to major injuries. Understanding how these tears and cracks develop over time therefore is important for diagnosing and tracking injuries.”
The investigators developed a way to visualize and predict spots where tissues are weakened. This was accomplished by stretching tissues and tracking the results as their shapes changed. Algorithms were then developed that can identify areas of weakening prior to breakage. The algorithm was tested in various materials and in animal models. “The new algorithm allowed us to find the places where the tears were beginning to form and to track them as they extended. Older algorithms are not as good at finding and tracking localized strains,” the researchers reported.
One of the two algorithms is 1,000 times more accurate than older methods at quantifying very large stretches near tiny cracks and tears. A second algorithm has the ability to predict where cracks and failures are likely to form.
Overall, the researchers aim to use these algorithms to prevent additional injuries following surgery to repair shoulders, knees, and other tissue. “It’s vital to understand the ways that physical forces cause structures and tissues to deform so that we can identify the onset of failures and eventually predict them.”
Researchers have developed algorithms to pinpoint weak spots in the tendons, bones, and muscles that are prone to breaking or tearing, according to a study published online August 27 in the Journal of the Royal Society Interface.
“Tendons are constantly stretching as muscles pull on them, and bones also bend or compress as we carry out everyday activities,” said senior investigator Stavros Thomopoulos, PhD, Professor of Orthopaedic Surgery at Washington University in St. Louis. “Small cracks or tears can result from these loads and lead to major injuries. Understanding how these tears and cracks develop over time therefore is important for diagnosing and tracking injuries.”
The investigators developed a way to visualize and predict spots where tissues are weakened. This was accomplished by stretching tissues and tracking the results as their shapes changed. Algorithms were then developed that can identify areas of weakening prior to breakage. The algorithm was tested in various materials and in animal models. “The new algorithm allowed us to find the places where the tears were beginning to form and to track them as they extended. Older algorithms are not as good at finding and tracking localized strains,” the researchers reported.
One of the two algorithms is 1,000 times more accurate than older methods at quantifying very large stretches near tiny cracks and tears. A second algorithm has the ability to predict where cracks and failures are likely to form.
Overall, the researchers aim to use these algorithms to prevent additional injuries following surgery to repair shoulders, knees, and other tissue. “It’s vital to understand the ways that physical forces cause structures and tissues to deform so that we can identify the onset of failures and eventually predict them.”
Suggested Reading
Boyle JJ, Kume M, Wyczalkowski MA, et al. Simple and accurate methods for quantifying deformation, disruption, and development in biological tissues. J R Soc Interface. 2014 Nov 6;11(100). pii: 20140685. doi: 10.1098/rsif.2014.0685.
Suggested Reading
Boyle JJ, Kume M, Wyczalkowski MA, et al. Simple and accurate methods for quantifying deformation, disruption, and development in biological tissues. J R Soc Interface. 2014 Nov 6;11(100). pii: 20140685. doi: 10.1098/rsif.2014.0685.
Zorvolex® Approved by FDA for Treatment of Osteoarthritis Pain
Iroko Pharmaceuticals (Philadelphia, Pennsylvania) announced that the FDA has approved Zorvolex (diclofenac) capsules, a nonsteroidal anti-inflammatory drug (NSAID) for the management of mild to moderate acute pain and osteoarthritis pain. This marks the second indication for the drug, which was approved by the FDA in October 2013 for treatment of mild to moderate acute pain in adults.
Zorvolex was created to align with recommendations from the FDA and several medical organizations that NSAIDs be used at the lowest effective dose and for the shortest possible duration. This low-dose NSAID was developed using SoluMatrix Fine Particle Technology. Zorvolex contains diclofenac as submicron particles that are approximately 20 times smaller than their original size. The reduction in particle size provides an increased surface area, which leads to faster dissolution.
“NSAIDs continue to be an integral part of the management for osteoarthritis and their use is likely to increase as the US population continues to age and the incidence of osteoarthritis rises,” said Roy Altman, MD, Professor of Medicine in Rheumatology at UCLA.
The approval of Zorvolex is supported by data from a 12-week multicenter, randomized, double-blind, parallel-group, placebo-controlled study. The study included 305 patients aged 41 to 90 years with osteoarthrisis of the knee or hip. Half of the patients were between the ages of 61 and 90 years. They were randomized to 35 mg of Zorvolex three times a day, 35 mg twice daily, or placebo. The Supplemental New Drug Application also included data from a 12-month open-label safety study of 602 patients.
Zorvolex is available in 18 mg or 35 mg capsules. “The approval of Zorvolex is a welcome and meaningful advance and is the first SoluMatrix NSAID option approved by the FDA for osteoarthritis pain,” Dr. Altman stated.
Iroko Pharmaceuticals (Philadelphia, Pennsylvania) announced that the FDA has approved Zorvolex (diclofenac) capsules, a nonsteroidal anti-inflammatory drug (NSAID) for the management of mild to moderate acute pain and osteoarthritis pain. This marks the second indication for the drug, which was approved by the FDA in October 2013 for treatment of mild to moderate acute pain in adults.
Zorvolex was created to align with recommendations from the FDA and several medical organizations that NSAIDs be used at the lowest effective dose and for the shortest possible duration. This low-dose NSAID was developed using SoluMatrix Fine Particle Technology. Zorvolex contains diclofenac as submicron particles that are approximately 20 times smaller than their original size. The reduction in particle size provides an increased surface area, which leads to faster dissolution.
“NSAIDs continue to be an integral part of the management for osteoarthritis and their use is likely to increase as the US population continues to age and the incidence of osteoarthritis rises,” said Roy Altman, MD, Professor of Medicine in Rheumatology at UCLA.
The approval of Zorvolex is supported by data from a 12-week multicenter, randomized, double-blind, parallel-group, placebo-controlled study. The study included 305 patients aged 41 to 90 years with osteoarthrisis of the knee or hip. Half of the patients were between the ages of 61 and 90 years. They were randomized to 35 mg of Zorvolex three times a day, 35 mg twice daily, or placebo. The Supplemental New Drug Application also included data from a 12-month open-label safety study of 602 patients.
Zorvolex is available in 18 mg or 35 mg capsules. “The approval of Zorvolex is a welcome and meaningful advance and is the first SoluMatrix NSAID option approved by the FDA for osteoarthritis pain,” Dr. Altman stated.
Iroko Pharmaceuticals (Philadelphia, Pennsylvania) announced that the FDA has approved Zorvolex (diclofenac) capsules, a nonsteroidal anti-inflammatory drug (NSAID) for the management of mild to moderate acute pain and osteoarthritis pain. This marks the second indication for the drug, which was approved by the FDA in October 2013 for treatment of mild to moderate acute pain in adults.
Zorvolex was created to align with recommendations from the FDA and several medical organizations that NSAIDs be used at the lowest effective dose and for the shortest possible duration. This low-dose NSAID was developed using SoluMatrix Fine Particle Technology. Zorvolex contains diclofenac as submicron particles that are approximately 20 times smaller than their original size. The reduction in particle size provides an increased surface area, which leads to faster dissolution.
“NSAIDs continue to be an integral part of the management for osteoarthritis and their use is likely to increase as the US population continues to age and the incidence of osteoarthritis rises,” said Roy Altman, MD, Professor of Medicine in Rheumatology at UCLA.
The approval of Zorvolex is supported by data from a 12-week multicenter, randomized, double-blind, parallel-group, placebo-controlled study. The study included 305 patients aged 41 to 90 years with osteoarthrisis of the knee or hip. Half of the patients were between the ages of 61 and 90 years. They were randomized to 35 mg of Zorvolex three times a day, 35 mg twice daily, or placebo. The Supplemental New Drug Application also included data from a 12-month open-label safety study of 602 patients.
Zorvolex is available in 18 mg or 35 mg capsules. “The approval of Zorvolex is a welcome and meaningful advance and is the first SoluMatrix NSAID option approved by the FDA for osteoarthritis pain,” Dr. Altman stated.
Knee Surgery Not Necessary for Middle-Aged Patients with Mild Osteoarthritis
New meta-analysis evidence suggests that there is no benefit to having arthroscopic meniscal debridement for degenerative meniscal tears in comparison with nonoperative treatments or sham treatments in middle-aged patients with mild or no concomitant osteoarthritis. The findings were published August 25 online ahead of print in the Canadian Medical Association Journal.
“Doctors need to carefully weigh the costs and benefits when deciding who should undergo such surgery,” said Moin Khan, MD, lead author of the study and research fellow in orthopedic surgery in the Michael G. DeGroote School of Medicine at McMaster University in Hamilton, Ontario.
Dr. Khan and colleagues conducted a meta-analysis of 7 randomized controlled trials published between 1946 and January 20, 2014, on arthroscopic partial meniscectomy in patients with mild to no osteoarthritis compared with nonoperative treatments. Two reviewers independently screened all abstracts and titles for eligibility. In total, there were 811 knees in 805 patients with a mean age of 56 years. The pooled treatment effect of arthroscopic surgery did not show a significant or minimally important difference between treatment arms for long-term functional outcomes. Short-term functional outcomes between groups were significant but did not exceed the threshold for minimally important difference. Arthroscopic surgery did not result in a significant improvement in either short- or long-term pain scores.
“This study shows that surgery should not be the initial option for middle-age or older patients, as there is limited evidence supporting partial meniscectomy surgery for meniscus tears,” Dr. Khan said. “Other treatments should be used first.”
“Arthroscopic debridement or washout of knee osteoarthritis has come under lots of scrutiny based upon trials that suggest patients get no benefit from the procedure. We’re concerned that many surgeons worldwide may still be doing this procedure,” stated the researchers.
Suggested Reading
Khan M, Evaniew N, Bedi A, et al. Arthroscopic surgery for degenerative tears of the meniscus: a systematic review and meta-analysis. CMAJ. 2014 Aug 25. pii: cmaj.140433. [Epub ahead of print]
New meta-analysis evidence suggests that there is no benefit to having arthroscopic meniscal debridement for degenerative meniscal tears in comparison with nonoperative treatments or sham treatments in middle-aged patients with mild or no concomitant osteoarthritis. The findings were published August 25 online ahead of print in the Canadian Medical Association Journal.
“Doctors need to carefully weigh the costs and benefits when deciding who should undergo such surgery,” said Moin Khan, MD, lead author of the study and research fellow in orthopedic surgery in the Michael G. DeGroote School of Medicine at McMaster University in Hamilton, Ontario.
Dr. Khan and colleagues conducted a meta-analysis of 7 randomized controlled trials published between 1946 and January 20, 2014, on arthroscopic partial meniscectomy in patients with mild to no osteoarthritis compared with nonoperative treatments. Two reviewers independently screened all abstracts and titles for eligibility. In total, there were 811 knees in 805 patients with a mean age of 56 years. The pooled treatment effect of arthroscopic surgery did not show a significant or minimally important difference between treatment arms for long-term functional outcomes. Short-term functional outcomes between groups were significant but did not exceed the threshold for minimally important difference. Arthroscopic surgery did not result in a significant improvement in either short- or long-term pain scores.
“This study shows that surgery should not be the initial option for middle-age or older patients, as there is limited evidence supporting partial meniscectomy surgery for meniscus tears,” Dr. Khan said. “Other treatments should be used first.”
“Arthroscopic debridement or washout of knee osteoarthritis has come under lots of scrutiny based upon trials that suggest patients get no benefit from the procedure. We’re concerned that many surgeons worldwide may still be doing this procedure,” stated the researchers.
New meta-analysis evidence suggests that there is no benefit to having arthroscopic meniscal debridement for degenerative meniscal tears in comparison with nonoperative treatments or sham treatments in middle-aged patients with mild or no concomitant osteoarthritis. The findings were published August 25 online ahead of print in the Canadian Medical Association Journal.
“Doctors need to carefully weigh the costs and benefits when deciding who should undergo such surgery,” said Moin Khan, MD, lead author of the study and research fellow in orthopedic surgery in the Michael G. DeGroote School of Medicine at McMaster University in Hamilton, Ontario.
Dr. Khan and colleagues conducted a meta-analysis of 7 randomized controlled trials published between 1946 and January 20, 2014, on arthroscopic partial meniscectomy in patients with mild to no osteoarthritis compared with nonoperative treatments. Two reviewers independently screened all abstracts and titles for eligibility. In total, there were 811 knees in 805 patients with a mean age of 56 years. The pooled treatment effect of arthroscopic surgery did not show a significant or minimally important difference between treatment arms for long-term functional outcomes. Short-term functional outcomes between groups were significant but did not exceed the threshold for minimally important difference. Arthroscopic surgery did not result in a significant improvement in either short- or long-term pain scores.
“This study shows that surgery should not be the initial option for middle-age or older patients, as there is limited evidence supporting partial meniscectomy surgery for meniscus tears,” Dr. Khan said. “Other treatments should be used first.”
“Arthroscopic debridement or washout of knee osteoarthritis has come under lots of scrutiny based upon trials that suggest patients get no benefit from the procedure. We’re concerned that many surgeons worldwide may still be doing this procedure,” stated the researchers.
Suggested Reading
Khan M, Evaniew N, Bedi A, et al. Arthroscopic surgery for degenerative tears of the meniscus: a systematic review and meta-analysis. CMAJ. 2014 Aug 25. pii: cmaj.140433. [Epub ahead of print]
Suggested Reading
Khan M, Evaniew N, Bedi A, et al. Arthroscopic surgery for degenerative tears of the meniscus: a systematic review and meta-analysis. CMAJ. 2014 Aug 25. pii: cmaj.140433. [Epub ahead of print]