User login
Ultrasound after neoadjuvant chemo can guide axillary surgery decisions
After neoadjuvant chemotherapy, axial ultrasound helps identify residual nodal disease – information that can guide the decision to pursue lymph node surgery, according to a report published online Feb. 2 in the Journal of Clinical Oncology.
This strategy of performing axial ultrasound to guide axillary surgery can reduce the number of both false-negative and false-positive results, thus improving both the rate of undertreating residual breast cancer and the rate of overtreating lymph nodes that have been cleared of the disease, said Dr. Judy C. Boughey of the Mayo Clinic, Rochester, Minn., and her associates.
They investigated two secondary end points of the American College of Surgeons Oncology Group Z1071 phase II clinical trial, which addressed sentinel lymph node surgery in women with initially node-positive breast cancer. The two end points were whether a normal appearance on ultrasound of sentinel lymph nodes after neoadjuvant chemotherapy denoted a decreased risk of residual cancer and whether an abnormal appearance of sentinel lymph nodes on ultrasound after neoadjuvant chemotherapy denoted an increased risk of residual cancer.
For this analysis of the ACSOG Z1071 data, Dr. Boughey and her associates assessed 611 study participants who initially had node-positive (stage T0-4, N1-2, M0) breast cancer treated at 136 medical centers, had completed neoadjuvant chemotherapy, had undergone axial ultrasound with archiving of the images, and had undergone sentinel lymph node surgery and axial dissection. A total of 70.4% of these patients had lymph nodes classified as normal on ultrasound and 29.6% had suspicious lymph nodes.
A total of 56.5% of patients with normal-appearing lymph nodes on ultrasound proved to have positive nodes on final pathology. In contrast, 71.8% – significantly more – of patients who had suspicious-looking lymph nodes on ultrasound proved to have positive nodes on final pathology (P less than .001). Women with suspicious nodal status on ultrasound also were more likely to have a higher number of positive nodes (34.5% vs 21.0%) and a larger median size of nodal metastases, representing a greater nodal disease burden, than those with normal appearance on ultrasound.
The investigators recommended a strategy in which patients with normal-appearing lymph nodes following adjuvant chemotherapy could undergo sentinel lymph node surgery. “If any of the sentinel lymph nodes were positive, the patient would undergo an axillary lymph node dissection, and if the sentinel lymph nodes were negative, then no further axillary surgery would be needed,” they wrote.
This approach yielded a false-negative rate of just 9.8% when applied to the Z1071 study population, compared with a 12.6% false-negative rate when axial ultrasound was not used to select patients for surgery. Any false-negative rate under 10% was predetermined to be acceptable when the study was designed, Dr. Boughey and her associates said (J. Clin. Oncol. 2015 [doi:10.1200/JCO.2014.57.8401]).
Among patients who had a normal node appearance on ultrasound but positive findings on sentinel lymph node surgery, 63% proved to have no additional positive nodes in the axillary lymph node dissection. “Therefore, in patients with normal axial ultrasound, sentinel lymph node surgery could be used to identify patients who may be able to avoid axillary lymph node dissection. This is being evaluated in the Alliance A11202 trial, which is currently enrolling patients and comparing axillary radiation to axillary dissection for patients with positive sentinel lymph nodes after neoadjuvant chemotherapy,” they added.
The ACOSOG Z1071 trial was supported by National Cancer Institute grants to the American College of Surgeons Oncology Group, the Alliance for Clinical Trials in Oncology, and the Alliance Statistics and Data Center. Dr. Boughey reported having no financial disclosures; one of her associates reported receiving research funding from Galena Biopharma and Antigen Express.
After neoadjuvant chemotherapy, axial ultrasound helps identify residual nodal disease – information that can guide the decision to pursue lymph node surgery, according to a report published online Feb. 2 in the Journal of Clinical Oncology.
This strategy of performing axial ultrasound to guide axillary surgery can reduce the number of both false-negative and false-positive results, thus improving both the rate of undertreating residual breast cancer and the rate of overtreating lymph nodes that have been cleared of the disease, said Dr. Judy C. Boughey of the Mayo Clinic, Rochester, Minn., and her associates.
They investigated two secondary end points of the American College of Surgeons Oncology Group Z1071 phase II clinical trial, which addressed sentinel lymph node surgery in women with initially node-positive breast cancer. The two end points were whether a normal appearance on ultrasound of sentinel lymph nodes after neoadjuvant chemotherapy denoted a decreased risk of residual cancer and whether an abnormal appearance of sentinel lymph nodes on ultrasound after neoadjuvant chemotherapy denoted an increased risk of residual cancer.
For this analysis of the ACSOG Z1071 data, Dr. Boughey and her associates assessed 611 study participants who initially had node-positive (stage T0-4, N1-2, M0) breast cancer treated at 136 medical centers, had completed neoadjuvant chemotherapy, had undergone axial ultrasound with archiving of the images, and had undergone sentinel lymph node surgery and axial dissection. A total of 70.4% of these patients had lymph nodes classified as normal on ultrasound and 29.6% had suspicious lymph nodes.
A total of 56.5% of patients with normal-appearing lymph nodes on ultrasound proved to have positive nodes on final pathology. In contrast, 71.8% – significantly more – of patients who had suspicious-looking lymph nodes on ultrasound proved to have positive nodes on final pathology (P less than .001). Women with suspicious nodal status on ultrasound also were more likely to have a higher number of positive nodes (34.5% vs 21.0%) and a larger median size of nodal metastases, representing a greater nodal disease burden, than those with normal appearance on ultrasound.
The investigators recommended a strategy in which patients with normal-appearing lymph nodes following adjuvant chemotherapy could undergo sentinel lymph node surgery. “If any of the sentinel lymph nodes were positive, the patient would undergo an axillary lymph node dissection, and if the sentinel lymph nodes were negative, then no further axillary surgery would be needed,” they wrote.
This approach yielded a false-negative rate of just 9.8% when applied to the Z1071 study population, compared with a 12.6% false-negative rate when axial ultrasound was not used to select patients for surgery. Any false-negative rate under 10% was predetermined to be acceptable when the study was designed, Dr. Boughey and her associates said (J. Clin. Oncol. 2015 [doi:10.1200/JCO.2014.57.8401]).
Among patients who had a normal node appearance on ultrasound but positive findings on sentinel lymph node surgery, 63% proved to have no additional positive nodes in the axillary lymph node dissection. “Therefore, in patients with normal axial ultrasound, sentinel lymph node surgery could be used to identify patients who may be able to avoid axillary lymph node dissection. This is being evaluated in the Alliance A11202 trial, which is currently enrolling patients and comparing axillary radiation to axillary dissection for patients with positive sentinel lymph nodes after neoadjuvant chemotherapy,” they added.
The ACOSOG Z1071 trial was supported by National Cancer Institute grants to the American College of Surgeons Oncology Group, the Alliance for Clinical Trials in Oncology, and the Alliance Statistics and Data Center. Dr. Boughey reported having no financial disclosures; one of her associates reported receiving research funding from Galena Biopharma and Antigen Express.
After neoadjuvant chemotherapy, axial ultrasound helps identify residual nodal disease – information that can guide the decision to pursue lymph node surgery, according to a report published online Feb. 2 in the Journal of Clinical Oncology.
This strategy of performing axial ultrasound to guide axillary surgery can reduce the number of both false-negative and false-positive results, thus improving both the rate of undertreating residual breast cancer and the rate of overtreating lymph nodes that have been cleared of the disease, said Dr. Judy C. Boughey of the Mayo Clinic, Rochester, Minn., and her associates.
They investigated two secondary end points of the American College of Surgeons Oncology Group Z1071 phase II clinical trial, which addressed sentinel lymph node surgery in women with initially node-positive breast cancer. The two end points were whether a normal appearance on ultrasound of sentinel lymph nodes after neoadjuvant chemotherapy denoted a decreased risk of residual cancer and whether an abnormal appearance of sentinel lymph nodes on ultrasound after neoadjuvant chemotherapy denoted an increased risk of residual cancer.
For this analysis of the ACSOG Z1071 data, Dr. Boughey and her associates assessed 611 study participants who initially had node-positive (stage T0-4, N1-2, M0) breast cancer treated at 136 medical centers, had completed neoadjuvant chemotherapy, had undergone axial ultrasound with archiving of the images, and had undergone sentinel lymph node surgery and axial dissection. A total of 70.4% of these patients had lymph nodes classified as normal on ultrasound and 29.6% had suspicious lymph nodes.
A total of 56.5% of patients with normal-appearing lymph nodes on ultrasound proved to have positive nodes on final pathology. In contrast, 71.8% – significantly more – of patients who had suspicious-looking lymph nodes on ultrasound proved to have positive nodes on final pathology (P less than .001). Women with suspicious nodal status on ultrasound also were more likely to have a higher number of positive nodes (34.5% vs 21.0%) and a larger median size of nodal metastases, representing a greater nodal disease burden, than those with normal appearance on ultrasound.
The investigators recommended a strategy in which patients with normal-appearing lymph nodes following adjuvant chemotherapy could undergo sentinel lymph node surgery. “If any of the sentinel lymph nodes were positive, the patient would undergo an axillary lymph node dissection, and if the sentinel lymph nodes were negative, then no further axillary surgery would be needed,” they wrote.
This approach yielded a false-negative rate of just 9.8% when applied to the Z1071 study population, compared with a 12.6% false-negative rate when axial ultrasound was not used to select patients for surgery. Any false-negative rate under 10% was predetermined to be acceptable when the study was designed, Dr. Boughey and her associates said (J. Clin. Oncol. 2015 [doi:10.1200/JCO.2014.57.8401]).
Among patients who had a normal node appearance on ultrasound but positive findings on sentinel lymph node surgery, 63% proved to have no additional positive nodes in the axillary lymph node dissection. “Therefore, in patients with normal axial ultrasound, sentinel lymph node surgery could be used to identify patients who may be able to avoid axillary lymph node dissection. This is being evaluated in the Alliance A11202 trial, which is currently enrolling patients and comparing axillary radiation to axillary dissection for patients with positive sentinel lymph nodes after neoadjuvant chemotherapy,” they added.
The ACOSOG Z1071 trial was supported by National Cancer Institute grants to the American College of Surgeons Oncology Group, the Alliance for Clinical Trials in Oncology, and the Alliance Statistics and Data Center. Dr. Boughey reported having no financial disclosures; one of her associates reported receiving research funding from Galena Biopharma and Antigen Express.
FROM THE JOURNAL OF CLINICAL ONCOLOGY
Key clinical point: Axial ultrasound following neoadjuvant chemotherapy can aid decision making on axillary surgery for breast cancer patients.
Major finding: Only 56.5% of patients with normal-appearing lymph nodes on ultrasound proved to have positive nodes on final pathology, compared with 71.8% of patients who had suspicious-looking lymph nodes on ultrasound (P less than .001).
Data source: An analysis of the secondary end points of the American College of Surgeons Oncology Group Z1071 phase II clinical trial, which involved 611 women with node-positive breast cancer planning to undergo sentinel lymph node surgery after completing neoadjuvant chemotherapy.
Disclosures: The ACOSOG Z1071 trial was supported by National Cancer Institute grants to the American College of Surgeons Oncology Group, the Alliance for Clinical Trials in Oncology, and the Alliance Statistics and Data Center. Dr. Boughey reported having no financial disclosures; one of her associates reported receiving research funding from Galena Biopharma and Antigen Express.
Postop NSAIDs may raise anastomotic complications
Postoperative NSAIDs appear to raise the risk for anastomotic complications among patients undergoing nonelective colorectal resection, according to a report in JAMA Surgery.
“Given that other analgesic regimens are effective and well tolerated, these data may be enough from some surgeons to alter practice patterns,” said Dr. Timo W. Hakkarainen of the department of surgery at the University of Washington, Seattle, and his associates.
The recent development of intravenous formulations of NSAIDs has expanded their use in postoperative patients, chiefly because the drugs don’t carry the adverse effects of opioid analgesia, which include impaired GI motility. However, several small and single-institution studies have suggested that NSAIDs used in this setting may impair anastomotic healing and may raise the rates of leakage.
Dr. Hakkarainen and his associates examined this issue using data from a statewide surveillance system for surgical quality. They analyzed 90-day complications among 13,082 adults (mean age, 58 years) who underwent surgery of the GI tract with anastomosis at 47 participating hospitals throughout Washington State during a 5-year period. The investigators tracked the use of ibuprofen, naproxen, ketorolac tromethamine, Caldolor, celecoxib, and diclofenac during the first 24 hours after surgery; they assumed that in most cases, this involved IV NSAIDs because such patients don’t take oral medications within that time period.
Postoperative NSAIDs were given to 24% of the study population. This use was associated with a significantly increased risk for anastomotic leakage during the next 90 days, with an OR of 1.24. Further analysis showed that this association was largely restricted to the subgroup of patients who had nonelective colorectal surgery, in whom the relationship was even stronger, with an OR of 1.70. Among patients who had nonelective colorectal surgery, those who received postoperative NSAIDs had a 12.3% rate of anastomotic leakage, compared with an 8.3% rate among those who did not receive NSAIDs, the investigators said (JAMA Surg. 2015 Jan. 21 [doi:10.1001/jamasurg.2014.2239]).
This study was limited in that the records didn’t specify the dose or duration of NSAID use, didn’t take into account preoperative NSAID use, and didn’t include the timing of anastomotic leakage (immediately following surgery vs. weeks or months later). “We believe that [these] results are sufficient to suggest caution in the use of NSAIDs in the postoperative treatment of patients undergoing nonelective colorectal surgery, and highlight the importance of further evaluation of this association,” the investigators added.
Postoperative NSAIDs appear to raise the risk for anastomotic complications among patients undergoing nonelective colorectal resection, according to a report in JAMA Surgery.
“Given that other analgesic regimens are effective and well tolerated, these data may be enough from some surgeons to alter practice patterns,” said Dr. Timo W. Hakkarainen of the department of surgery at the University of Washington, Seattle, and his associates.
The recent development of intravenous formulations of NSAIDs has expanded their use in postoperative patients, chiefly because the drugs don’t carry the adverse effects of opioid analgesia, which include impaired GI motility. However, several small and single-institution studies have suggested that NSAIDs used in this setting may impair anastomotic healing and may raise the rates of leakage.
Dr. Hakkarainen and his associates examined this issue using data from a statewide surveillance system for surgical quality. They analyzed 90-day complications among 13,082 adults (mean age, 58 years) who underwent surgery of the GI tract with anastomosis at 47 participating hospitals throughout Washington State during a 5-year period. The investigators tracked the use of ibuprofen, naproxen, ketorolac tromethamine, Caldolor, celecoxib, and diclofenac during the first 24 hours after surgery; they assumed that in most cases, this involved IV NSAIDs because such patients don’t take oral medications within that time period.
Postoperative NSAIDs were given to 24% of the study population. This use was associated with a significantly increased risk for anastomotic leakage during the next 90 days, with an OR of 1.24. Further analysis showed that this association was largely restricted to the subgroup of patients who had nonelective colorectal surgery, in whom the relationship was even stronger, with an OR of 1.70. Among patients who had nonelective colorectal surgery, those who received postoperative NSAIDs had a 12.3% rate of anastomotic leakage, compared with an 8.3% rate among those who did not receive NSAIDs, the investigators said (JAMA Surg. 2015 Jan. 21 [doi:10.1001/jamasurg.2014.2239]).
This study was limited in that the records didn’t specify the dose or duration of NSAID use, didn’t take into account preoperative NSAID use, and didn’t include the timing of anastomotic leakage (immediately following surgery vs. weeks or months later). “We believe that [these] results are sufficient to suggest caution in the use of NSAIDs in the postoperative treatment of patients undergoing nonelective colorectal surgery, and highlight the importance of further evaluation of this association,” the investigators added.
Postoperative NSAIDs appear to raise the risk for anastomotic complications among patients undergoing nonelective colorectal resection, according to a report in JAMA Surgery.
“Given that other analgesic regimens are effective and well tolerated, these data may be enough from some surgeons to alter practice patterns,” said Dr. Timo W. Hakkarainen of the department of surgery at the University of Washington, Seattle, and his associates.
The recent development of intravenous formulations of NSAIDs has expanded their use in postoperative patients, chiefly because the drugs don’t carry the adverse effects of opioid analgesia, which include impaired GI motility. However, several small and single-institution studies have suggested that NSAIDs used in this setting may impair anastomotic healing and may raise the rates of leakage.
Dr. Hakkarainen and his associates examined this issue using data from a statewide surveillance system for surgical quality. They analyzed 90-day complications among 13,082 adults (mean age, 58 years) who underwent surgery of the GI tract with anastomosis at 47 participating hospitals throughout Washington State during a 5-year period. The investigators tracked the use of ibuprofen, naproxen, ketorolac tromethamine, Caldolor, celecoxib, and diclofenac during the first 24 hours after surgery; they assumed that in most cases, this involved IV NSAIDs because such patients don’t take oral medications within that time period.
Postoperative NSAIDs were given to 24% of the study population. This use was associated with a significantly increased risk for anastomotic leakage during the next 90 days, with an OR of 1.24. Further analysis showed that this association was largely restricted to the subgroup of patients who had nonelective colorectal surgery, in whom the relationship was even stronger, with an OR of 1.70. Among patients who had nonelective colorectal surgery, those who received postoperative NSAIDs had a 12.3% rate of anastomotic leakage, compared with an 8.3% rate among those who did not receive NSAIDs, the investigators said (JAMA Surg. 2015 Jan. 21 [doi:10.1001/jamasurg.2014.2239]).
This study was limited in that the records didn’t specify the dose or duration of NSAID use, didn’t take into account preoperative NSAID use, and didn’t include the timing of anastomotic leakage (immediately following surgery vs. weeks or months later). “We believe that [these] results are sufficient to suggest caution in the use of NSAIDs in the postoperative treatment of patients undergoing nonelective colorectal surgery, and highlight the importance of further evaluation of this association,” the investigators added.
Key clinical point: Postoperative NSAIDs appear to raise the risk of anastomotic complications in patients undergoing nonelective colorectal resection.
Major finding: Among patients who had nonelective colorectal surgery, those who received postoperative NSAIDs had a 12.3% rate of anastomotic leakage, compared with an 8.3% rate among those who did not receive NSAIDs.
Data source: A secondary analysis of a cohort study involving 13,082 patients who had GI-tract surgery with anastomosis at 47 hospitals in Washington State during a 5-year period.
Disclosures: The Comparative Effective Research Translation Network of the Agency for Healthcare Research and Quality, the Washington State Life Science Discovery Fund, and the National Institutes of Health supported the study. Dr. Hakkarainen and his associates reported having no financial disclosures.
Tight hypertension control in pregnancy not tied to better outcomes
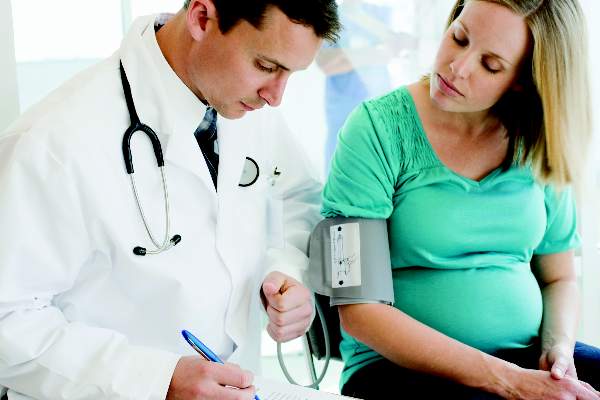
Rates of adverse perinatal outcomes were no different between women who achieved tight control of mild to moderate hypertension during pregnancy and those who achieved less tight control in an international randomized trial.
The findings, published Jan. 29 in the New England Journal of Medicine, showed no significant differences in a composite of pregnancy loss (including miscarriage, ectopic pregnancy, pregnancy termination, stillbirth, or neonatal death) or high-level neonatal care exceeding 48 hours between women with tight control (30.7%) and less tight control (31.4%). There were also no significant differences in serious maternal complications between the two levels of hypertension control.
The results come from the Control of Hypertension in Pregnancy Study (CHIPS), a randomized trial that assessed perinatal outcomes in 986 hypertensive pregnant women treated at 94 sites during a 3-year period.
The appropriate blood pressure targets for women with nonsevere hypertension during pregnancy have been hotly debated, with some research indicating that tight control yields maternal benefits and other studies suggesting it causes problems for the fetus, including poor fetal growth. However, most of the relevant randomized, controlled trials have been small or of moderate or poor quality, according to the CHIPS researchers.
Meanwhile, international guidelines for nonsevere hypertension during pregnancy vary, recommending either less tight control or tight control.
With CHIPS, the researchers are hoping to settle some of the controversy by directly comparing perinatal and maternal outcomes for tight versus less tight control of nonproteinuric, nonsevere hypertension in pregnancy.
“Our trial is substantially larger than previous trials that have examined the effects of lower versus higher blood pressure targets during pregnancy,” Dr. Laura A. Magee of the British Columbia Women’s Hospital and Health Centre in Vancouver and her colleagues wrote (N. Engl. J. Med. 2015;372:407-17).
The study participants, who had nonproteinuric hypertension that was either preexisting or developed during gestation, were randomly assigned to a tight diastolic blood pressure target of 85 mm Hg (489 women) or a less tight target of 100 mm Hg (497 women). Adherence to antihypertensive therapy was similar between the two groups at approximately 74%, and blood pressure was higher throughout pregnancy in the group with less tight control, according to the study.
CHIPS also showed no significant between-group differences in other perinatal outcomes, such as the frequency of newborns who were small for gestational age and respiratory complications and treatment. Further, there were no significant differences in the secondary outcome of serious maternal complications, and no maternal deaths in either group. However, the rate of severe hypertension was higher among women with less tight blood pressure control (40.6% versus 27.5%), though there was no corresponding increase in stroke or transient ischemic attack.
The current study showed that tight control of hypertension conferred no apparent benefits to the fetus and only a moderate benefit (a lower rate of progression to severe hypertension) for the mother.
It does, however, provide valuable reassurance that tight control, as targeted in this study, does not carry major risks for the fetus or newborn.
Dr. Caren G. Solomon and Dr. Michael F. Greene of the department of obstetrics and gynecology at Massachusetts General Hospital, Boston, made these comments in an accompanying editorial (N. Engl. J. Med. 2015;372:475-6). They reported having no relevant financial disclosures.
The current study showed that tight control of hypertension conferred no apparent benefits to the fetus and only a moderate benefit (a lower rate of progression to severe hypertension) for the mother.
It does, however, provide valuable reassurance that tight control, as targeted in this study, does not carry major risks for the fetus or newborn.
Dr. Caren G. Solomon and Dr. Michael F. Greene of the department of obstetrics and gynecology at Massachusetts General Hospital, Boston, made these comments in an accompanying editorial (N. Engl. J. Med. 2015;372:475-6). They reported having no relevant financial disclosures.
The current study showed that tight control of hypertension conferred no apparent benefits to the fetus and only a moderate benefit (a lower rate of progression to severe hypertension) for the mother.
It does, however, provide valuable reassurance that tight control, as targeted in this study, does not carry major risks for the fetus or newborn.
Dr. Caren G. Solomon and Dr. Michael F. Greene of the department of obstetrics and gynecology at Massachusetts General Hospital, Boston, made these comments in an accompanying editorial (N. Engl. J. Med. 2015;372:475-6). They reported having no relevant financial disclosures.
Rates of adverse perinatal outcomes were no different between women who achieved tight control of mild to moderate hypertension during pregnancy and those who achieved less tight control in an international randomized trial.
The findings, published Jan. 29 in the New England Journal of Medicine, showed no significant differences in a composite of pregnancy loss (including miscarriage, ectopic pregnancy, pregnancy termination, stillbirth, or neonatal death) or high-level neonatal care exceeding 48 hours between women with tight control (30.7%) and less tight control (31.4%). There were also no significant differences in serious maternal complications between the two levels of hypertension control.
The results come from the Control of Hypertension in Pregnancy Study (CHIPS), a randomized trial that assessed perinatal outcomes in 986 hypertensive pregnant women treated at 94 sites during a 3-year period.
The appropriate blood pressure targets for women with nonsevere hypertension during pregnancy have been hotly debated, with some research indicating that tight control yields maternal benefits and other studies suggesting it causes problems for the fetus, including poor fetal growth. However, most of the relevant randomized, controlled trials have been small or of moderate or poor quality, according to the CHIPS researchers.
Meanwhile, international guidelines for nonsevere hypertension during pregnancy vary, recommending either less tight control or tight control.
With CHIPS, the researchers are hoping to settle some of the controversy by directly comparing perinatal and maternal outcomes for tight versus less tight control of nonproteinuric, nonsevere hypertension in pregnancy.
“Our trial is substantially larger than previous trials that have examined the effects of lower versus higher blood pressure targets during pregnancy,” Dr. Laura A. Magee of the British Columbia Women’s Hospital and Health Centre in Vancouver and her colleagues wrote (N. Engl. J. Med. 2015;372:407-17).
The study participants, who had nonproteinuric hypertension that was either preexisting or developed during gestation, were randomly assigned to a tight diastolic blood pressure target of 85 mm Hg (489 women) or a less tight target of 100 mm Hg (497 women). Adherence to antihypertensive therapy was similar between the two groups at approximately 74%, and blood pressure was higher throughout pregnancy in the group with less tight control, according to the study.
CHIPS also showed no significant between-group differences in other perinatal outcomes, such as the frequency of newborns who were small for gestational age and respiratory complications and treatment. Further, there were no significant differences in the secondary outcome of serious maternal complications, and no maternal deaths in either group. However, the rate of severe hypertension was higher among women with less tight blood pressure control (40.6% versus 27.5%), though there was no corresponding increase in stroke or transient ischemic attack.
Rates of adverse perinatal outcomes were no different between women who achieved tight control of mild to moderate hypertension during pregnancy and those who achieved less tight control in an international randomized trial.
The findings, published Jan. 29 in the New England Journal of Medicine, showed no significant differences in a composite of pregnancy loss (including miscarriage, ectopic pregnancy, pregnancy termination, stillbirth, or neonatal death) or high-level neonatal care exceeding 48 hours between women with tight control (30.7%) and less tight control (31.4%). There were also no significant differences in serious maternal complications between the two levels of hypertension control.
The results come from the Control of Hypertension in Pregnancy Study (CHIPS), a randomized trial that assessed perinatal outcomes in 986 hypertensive pregnant women treated at 94 sites during a 3-year period.
The appropriate blood pressure targets for women with nonsevere hypertension during pregnancy have been hotly debated, with some research indicating that tight control yields maternal benefits and other studies suggesting it causes problems for the fetus, including poor fetal growth. However, most of the relevant randomized, controlled trials have been small or of moderate or poor quality, according to the CHIPS researchers.
Meanwhile, international guidelines for nonsevere hypertension during pregnancy vary, recommending either less tight control or tight control.
With CHIPS, the researchers are hoping to settle some of the controversy by directly comparing perinatal and maternal outcomes for tight versus less tight control of nonproteinuric, nonsevere hypertension in pregnancy.
“Our trial is substantially larger than previous trials that have examined the effects of lower versus higher blood pressure targets during pregnancy,” Dr. Laura A. Magee of the British Columbia Women’s Hospital and Health Centre in Vancouver and her colleagues wrote (N. Engl. J. Med. 2015;372:407-17).
The study participants, who had nonproteinuric hypertension that was either preexisting or developed during gestation, were randomly assigned to a tight diastolic blood pressure target of 85 mm Hg (489 women) or a less tight target of 100 mm Hg (497 women). Adherence to antihypertensive therapy was similar between the two groups at approximately 74%, and blood pressure was higher throughout pregnancy in the group with less tight control, according to the study.
CHIPS also showed no significant between-group differences in other perinatal outcomes, such as the frequency of newborns who were small for gestational age and respiratory complications and treatment. Further, there were no significant differences in the secondary outcome of serious maternal complications, and no maternal deaths in either group. However, the rate of severe hypertension was higher among women with less tight blood pressure control (40.6% versus 27.5%), though there was no corresponding increase in stroke or transient ischemic attack.
Key clinical point: The rates of pregnancy loss, high-level neonatal care, and maternal complications were no different, regardless of whether mild to moderate hypertension was tightly controlled or less tightly controlled during pregnancy.
Major finding: The rate of the primary outcome – a composite of pregnancy loss or high-level neonatal care exceeding 48 hours – was not significantly different between women with tight control of hypertension (30.7%) and less tight control (31.4%).
Data source: The international randomized, controlled Control of Hypertension in Pregnancy Study involving 986 pregnant women at 94 medical centers who had nonsevere, nonproteinuric hypertension.
Disclosures: CHIPS was supported by the Canadian Institutes of Health Research. Dr. Magee reported having no financial disclosures; one of her associates reported receiving consulting fees and research support from Alere International.
Icatibant rapidly resolved ACE inhibitor–induced angioedema
Angioedema caused by ACE inhibitors resolved 70% more rapidly with icatibant than did standard therapy in a multicenter phase II study in Germany, which was reported online Jan. 29 in the New England Journal of Medicine.
Because of the increasing use of ACE inhibitors, approximately one-third of all cases of angioedema treated in emergency departments now are attributed to these agents. The current standard ED treatment of ACE inhibitor–induced angioedema is glucocorticoids plus antihistamines. However, patients generally don’t respond to this therapy, likely because this form of angioedema isn’t a histamine-mediated reaction. Instead, it is thought by some to be a bradykinin-mediated reaction, said Dr. Murat Bas of the department of otorhinolaryngology, Technische Universität München (Germany), and his associates.
Icatibant injections (Firazyr) are approved by the Food and Drug Administration for the treatment of acute attacks of hereditary angioedema in adults 18 years of age and older. The drug also is being studied in the United States for the treatment of ACE-inhibitor–induced angioedema.
Since ACE inhibitors interfere with the breakdown of bradykinin, and bradykinin-mediated hereditary angioedema is usually treated with bradykinin-receptor antagonists such as icatibant, the investigators performed a double-blind randomized trial comparing subcutaneous icatibant against standard treatment in 27 adults who presented to four German EDs during a 1.5-year period.
The primary endpoint – the time to complete resolution of ACE inhibitor–induced angioedema – was 8 hours with icatibant and 27 hours with standard therapy. Angioedema resolved within 4 hours in five patients (38%) given icatibant; none of the patients given standard therapy responded that quickly. The onset of symptom relief was 2 hours with icatibant and 12 hours with standard glucocorticoids plus antihistamines, a significant difference as judged by the study participants and the researchers. Also, the physician-assessed severity of angioedema began to abate within 1 hour of icatibant administration and within 8 hours for standard treatment (N. Engl. J. Med. 2015 Jan. 29 [doi:10.1056/NEJMoa1312524]).
“Although the sample size in this trial was too small to allow for a robust evaluation of safety, no patient discontinued participation in the study owing to adverse events,” Dr. Bas and his associates added.
Dr. Bas reported receiving grants and personal fees from Shire, the maker of icatibant, as did some of his associates.
Angioedema caused by ACE inhibitors resolved 70% more rapidly with icatibant than did standard therapy in a multicenter phase II study in Germany, which was reported online Jan. 29 in the New England Journal of Medicine.
Because of the increasing use of ACE inhibitors, approximately one-third of all cases of angioedema treated in emergency departments now are attributed to these agents. The current standard ED treatment of ACE inhibitor–induced angioedema is glucocorticoids plus antihistamines. However, patients generally don’t respond to this therapy, likely because this form of angioedema isn’t a histamine-mediated reaction. Instead, it is thought by some to be a bradykinin-mediated reaction, said Dr. Murat Bas of the department of otorhinolaryngology, Technische Universität München (Germany), and his associates.
Icatibant injections (Firazyr) are approved by the Food and Drug Administration for the treatment of acute attacks of hereditary angioedema in adults 18 years of age and older. The drug also is being studied in the United States for the treatment of ACE-inhibitor–induced angioedema.
Since ACE inhibitors interfere with the breakdown of bradykinin, and bradykinin-mediated hereditary angioedema is usually treated with bradykinin-receptor antagonists such as icatibant, the investigators performed a double-blind randomized trial comparing subcutaneous icatibant against standard treatment in 27 adults who presented to four German EDs during a 1.5-year period.
The primary endpoint – the time to complete resolution of ACE inhibitor–induced angioedema – was 8 hours with icatibant and 27 hours with standard therapy. Angioedema resolved within 4 hours in five patients (38%) given icatibant; none of the patients given standard therapy responded that quickly. The onset of symptom relief was 2 hours with icatibant and 12 hours with standard glucocorticoids plus antihistamines, a significant difference as judged by the study participants and the researchers. Also, the physician-assessed severity of angioedema began to abate within 1 hour of icatibant administration and within 8 hours for standard treatment (N. Engl. J. Med. 2015 Jan. 29 [doi:10.1056/NEJMoa1312524]).
“Although the sample size in this trial was too small to allow for a robust evaluation of safety, no patient discontinued participation in the study owing to adverse events,” Dr. Bas and his associates added.
Dr. Bas reported receiving grants and personal fees from Shire, the maker of icatibant, as did some of his associates.
Angioedema caused by ACE inhibitors resolved 70% more rapidly with icatibant than did standard therapy in a multicenter phase II study in Germany, which was reported online Jan. 29 in the New England Journal of Medicine.
Because of the increasing use of ACE inhibitors, approximately one-third of all cases of angioedema treated in emergency departments now are attributed to these agents. The current standard ED treatment of ACE inhibitor–induced angioedema is glucocorticoids plus antihistamines. However, patients generally don’t respond to this therapy, likely because this form of angioedema isn’t a histamine-mediated reaction. Instead, it is thought by some to be a bradykinin-mediated reaction, said Dr. Murat Bas of the department of otorhinolaryngology, Technische Universität München (Germany), and his associates.
Icatibant injections (Firazyr) are approved by the Food and Drug Administration for the treatment of acute attacks of hereditary angioedema in adults 18 years of age and older. The drug also is being studied in the United States for the treatment of ACE-inhibitor–induced angioedema.
Since ACE inhibitors interfere with the breakdown of bradykinin, and bradykinin-mediated hereditary angioedema is usually treated with bradykinin-receptor antagonists such as icatibant, the investigators performed a double-blind randomized trial comparing subcutaneous icatibant against standard treatment in 27 adults who presented to four German EDs during a 1.5-year period.
The primary endpoint – the time to complete resolution of ACE inhibitor–induced angioedema – was 8 hours with icatibant and 27 hours with standard therapy. Angioedema resolved within 4 hours in five patients (38%) given icatibant; none of the patients given standard therapy responded that quickly. The onset of symptom relief was 2 hours with icatibant and 12 hours with standard glucocorticoids plus antihistamines, a significant difference as judged by the study participants and the researchers. Also, the physician-assessed severity of angioedema began to abate within 1 hour of icatibant administration and within 8 hours for standard treatment (N. Engl. J. Med. 2015 Jan. 29 [doi:10.1056/NEJMoa1312524]).
“Although the sample size in this trial was too small to allow for a robust evaluation of safety, no patient discontinued participation in the study owing to adverse events,” Dr. Bas and his associates added.
Dr. Bas reported receiving grants and personal fees from Shire, the maker of icatibant, as did some of his associates.
Key clinical point: Icatibant may prove to be a more effective treatment than glucocorticoids and antihistamines for ACE inhibitor–induced angioedema.
Major finding: The time to complete resolution of ACE inhibitor–induced angioedema was 8 hours with icatibant and 27 hours with standard therapy.
Data source: A multicenter double-blind randomized phase II clinical trial involving 27 adults hospitalized in Germany for ACE inhibitor–induced angioedema during a 1.5-year period.
Disclosures: This study was supported by an educational grant from Shire and by the Federal Ministry of Education and Research of Germany. Dr. Bas reported receiving grants and personal fees from Shire, the maker of icatibant, as did some of his associates.
Targeted fusion biopsy superior for suspected prostate cancer
Targeted biopsy using magnetic resonance/ultrasound fusion imaging increased the detection of high-risk prostate cancer by 30% and decreased the detection of low-risk prostate cancer by 17%, compared with standard biopsy, according to a report published online Jan. 27 in JAMA.
Researchers compared the two approaches in a prospective cohort study involving 1,003 men referred to the National Cancer Institute during a 7-year period for evaluation of suspected prostate cancer. All the study participants had an elevated PSA or abnormal findings on digital rectal exam plus a multiparametric MRI showing at least 1 lesion in the prostate, said Dr. M. Minhaj Siddiqui of the urologic oncology branch, National Cancer Institute, Bethesda, Md., and his associates.
All the patients underwent both standard extended-sextant ultrasound-guided biopsy and targeted magnetic resonance/ultrasound fusion biopsy at the same visit. The latter technique involves electronically superimposing multiparametric MR images in real time onto transrectal ultrasound images, which improves spatial localization and capture of location in three planes. The lesions were separately categorized as low-risk, intermediate-risk, or high-risk by highly experienced genitourinary radiologists.
The two image-guided biopsy techniques agreed on these classifications in 69% of cases and identified a similar number of cancers. However, targeted biopsy detected 173 high-risk tumors, compared with only 122 identified on standard biopsy, and targeted biopsy detected 213 low-risk tumors, compared with 258 identified on standard biopsy. In a subset of 170 cases, these biopsy results could be compared against pathology found at whole-gland prostatectomy. Targeted biopsy proved to be much more accurate than standard biopsy, with sensitivities of 77% and 53%, respectively, the investigators said (JAMA 2015 Jan. 27 [doi:10.1001/jama.2014.17942]).
These findings show that targeted biopsy “could significantly change the distribution of risk in men newly diagnosed with prostate cancer toward diagnosis of more high-risk disease. Although these improvements in risk stratification could translate into substantial clinical benefits, it is important to recognize that this study is preliminary” and didn’t include clinical end points such as cancer recurrence or prostate cancer–specific mortality, Dr. Siddiqui and his associates said.
Despite these promising results, it remains unknown whether improved risk stratification with targeted biopsy will translate into clinically meaningful outcomes such as better functional status or higher survival rates.
Improved classification of tumor grades should lead to more appropriate treatment recommendations – more intense therapy for men with higher-risk disease and active surveillance for those with lower-risk disease. But further study is needed to assess this technique’s impact on quality of life, disease progression, and life expectancy.
Dr. Lawrence H. Schwartz is in the department of radiology at Columbia University, New York, and at New York Presbyterian Hospital. Dr. Ethan Basch is at Lineberger Comprehensive Cancer Center and the University of North Carolina, Chapel Hill, as well as an associate editor at JAMA. Dr. Schwartz reported ties to Pfizer, Celgene, Novartis, Icon, and BioImaging, and Dr. Basch reported having no financial conflicts of interest. They made these remarks in an editorial accompanying Dr. Siddiqui’s report (JAMA 2015 Jan. 27 [doi:10.1001/jama.2014.17943]).
Despite these promising results, it remains unknown whether improved risk stratification with targeted biopsy will translate into clinically meaningful outcomes such as better functional status or higher survival rates.
Improved classification of tumor grades should lead to more appropriate treatment recommendations – more intense therapy for men with higher-risk disease and active surveillance for those with lower-risk disease. But further study is needed to assess this technique’s impact on quality of life, disease progression, and life expectancy.
Dr. Lawrence H. Schwartz is in the department of radiology at Columbia University, New York, and at New York Presbyterian Hospital. Dr. Ethan Basch is at Lineberger Comprehensive Cancer Center and the University of North Carolina, Chapel Hill, as well as an associate editor at JAMA. Dr. Schwartz reported ties to Pfizer, Celgene, Novartis, Icon, and BioImaging, and Dr. Basch reported having no financial conflicts of interest. They made these remarks in an editorial accompanying Dr. Siddiqui’s report (JAMA 2015 Jan. 27 [doi:10.1001/jama.2014.17943]).
Despite these promising results, it remains unknown whether improved risk stratification with targeted biopsy will translate into clinically meaningful outcomes such as better functional status or higher survival rates.
Improved classification of tumor grades should lead to more appropriate treatment recommendations – more intense therapy for men with higher-risk disease and active surveillance for those with lower-risk disease. But further study is needed to assess this technique’s impact on quality of life, disease progression, and life expectancy.
Dr. Lawrence H. Schwartz is in the department of radiology at Columbia University, New York, and at New York Presbyterian Hospital. Dr. Ethan Basch is at Lineberger Comprehensive Cancer Center and the University of North Carolina, Chapel Hill, as well as an associate editor at JAMA. Dr. Schwartz reported ties to Pfizer, Celgene, Novartis, Icon, and BioImaging, and Dr. Basch reported having no financial conflicts of interest. They made these remarks in an editorial accompanying Dr. Siddiqui’s report (JAMA 2015 Jan. 27 [doi:10.1001/jama.2014.17943]).
Targeted biopsy using magnetic resonance/ultrasound fusion imaging increased the detection of high-risk prostate cancer by 30% and decreased the detection of low-risk prostate cancer by 17%, compared with standard biopsy, according to a report published online Jan. 27 in JAMA.
Researchers compared the two approaches in a prospective cohort study involving 1,003 men referred to the National Cancer Institute during a 7-year period for evaluation of suspected prostate cancer. All the study participants had an elevated PSA or abnormal findings on digital rectal exam plus a multiparametric MRI showing at least 1 lesion in the prostate, said Dr. M. Minhaj Siddiqui of the urologic oncology branch, National Cancer Institute, Bethesda, Md., and his associates.
All the patients underwent both standard extended-sextant ultrasound-guided biopsy and targeted magnetic resonance/ultrasound fusion biopsy at the same visit. The latter technique involves electronically superimposing multiparametric MR images in real time onto transrectal ultrasound images, which improves spatial localization and capture of location in three planes. The lesions were separately categorized as low-risk, intermediate-risk, or high-risk by highly experienced genitourinary radiologists.
The two image-guided biopsy techniques agreed on these classifications in 69% of cases and identified a similar number of cancers. However, targeted biopsy detected 173 high-risk tumors, compared with only 122 identified on standard biopsy, and targeted biopsy detected 213 low-risk tumors, compared with 258 identified on standard biopsy. In a subset of 170 cases, these biopsy results could be compared against pathology found at whole-gland prostatectomy. Targeted biopsy proved to be much more accurate than standard biopsy, with sensitivities of 77% and 53%, respectively, the investigators said (JAMA 2015 Jan. 27 [doi:10.1001/jama.2014.17942]).
These findings show that targeted biopsy “could significantly change the distribution of risk in men newly diagnosed with prostate cancer toward diagnosis of more high-risk disease. Although these improvements in risk stratification could translate into substantial clinical benefits, it is important to recognize that this study is preliminary” and didn’t include clinical end points such as cancer recurrence or prostate cancer–specific mortality, Dr. Siddiqui and his associates said.
Targeted biopsy using magnetic resonance/ultrasound fusion imaging increased the detection of high-risk prostate cancer by 30% and decreased the detection of low-risk prostate cancer by 17%, compared with standard biopsy, according to a report published online Jan. 27 in JAMA.
Researchers compared the two approaches in a prospective cohort study involving 1,003 men referred to the National Cancer Institute during a 7-year period for evaluation of suspected prostate cancer. All the study participants had an elevated PSA or abnormal findings on digital rectal exam plus a multiparametric MRI showing at least 1 lesion in the prostate, said Dr. M. Minhaj Siddiqui of the urologic oncology branch, National Cancer Institute, Bethesda, Md., and his associates.
All the patients underwent both standard extended-sextant ultrasound-guided biopsy and targeted magnetic resonance/ultrasound fusion biopsy at the same visit. The latter technique involves electronically superimposing multiparametric MR images in real time onto transrectal ultrasound images, which improves spatial localization and capture of location in three planes. The lesions were separately categorized as low-risk, intermediate-risk, or high-risk by highly experienced genitourinary radiologists.
The two image-guided biopsy techniques agreed on these classifications in 69% of cases and identified a similar number of cancers. However, targeted biopsy detected 173 high-risk tumors, compared with only 122 identified on standard biopsy, and targeted biopsy detected 213 low-risk tumors, compared with 258 identified on standard biopsy. In a subset of 170 cases, these biopsy results could be compared against pathology found at whole-gland prostatectomy. Targeted biopsy proved to be much more accurate than standard biopsy, with sensitivities of 77% and 53%, respectively, the investigators said (JAMA 2015 Jan. 27 [doi:10.1001/jama.2014.17942]).
These findings show that targeted biopsy “could significantly change the distribution of risk in men newly diagnosed with prostate cancer toward diagnosis of more high-risk disease. Although these improvements in risk stratification could translate into substantial clinical benefits, it is important to recognize that this study is preliminary” and didn’t include clinical end points such as cancer recurrence or prostate cancer–specific mortality, Dr. Siddiqui and his associates said.
Key clinical point: Targeted magnetic resonance/ultrasound fusion biopsy detected more high-risk and fewer low-risk prostate cancers than standard ultrasound-guided biopsy.
Major finding: Targeted biopsy detected 173 high-risk tumors, compared with only 122 identified on standard biopsy (30% more), and targeted biopsy detected 213 low-risk tumors, compared with 258 identified on standard biopsy (17% fewer).
Data source: A prospective cohort study involving 1,003 men undergoing both standard ultrasound-guided biopsy and targeted magnetic resonance/ultrasound fusion biopsy of the prostate during a 7-year period at a single medical center.
Disclosures: This study was supported by the National Cancer Institute, the National Institutes of Health, the Center for Cancer Research, and the Center for Interventional Oncology. Dr. Siddiqui reported having no financial disclosures; his associates reported holding multiple patents related to biopsies and imaging,
Sex Addiction, Gambling Disorder Share Similarities
Patients with sexual addiction and patients with gambling disorder share some psychopathologic features and sociodemographic traits that are not found in healthy control subjects, a study showed.
This finding supports the argument that sexual addiction “should be classified more closely to other behavioral addictions such as gambling disorder,” said Dr. Josep M. Farré of Hospital Universitari Quirón-Dexeus, Barcelona, and his associates.
However, patients with sexual addiction are different from those with gambling disorder in their personality traits, particularly with regard to responses to novelty. Both of these disorders “could benefit from ‘transdiagnostic’ treatment programs aimed to improve the character trait ‘self-directedness,’ since it is a factor associated with various personality disorders related to behavioral addictions,” the investigators said (Compr. Psychiatry 2015;56:59-68).
In what they described as the first study to examine the similarities and differences among these two clinical groups and healthy controls, Dr. Farré and his associates assessed during an 8-year period 59 patients seeking treatment for sexual addiction, 2,190 in treatment for gambling disorder, and 93 healthy volunteers who resided in the same geographical area as the clinical participants.
The mean age of the study participants was 42 years. Most (90%) were men, and approximately half were married or living with a partner.
All the study participants underwent a comprehensive battery of evaluations in face-to-face clinical interviews to measure sociodemographic characteristics, general psychopathology, personality traits, and gambling and sex behaviors.
Patients with sexual addiction had scores on all the scales of the Symptom Check List–90 Items–Revised (SCL-90-R) that were very similar to those of patients with gambling disorder, and both groups had significantly different scores from the control subjects. The two patient groups were very similar for somatization, obsession-compulsion, interpersonal sensitivity, depression, anxiety, hostility, phobic anxiety, paranoid ideation, and psychoticism. They also showed similar symptom intensity and similar overall levels of psychological distress.
Continue for more on patient scores >>
In addition, patients with both disorders had similar scores, as well as significantly lower scores than healthy controls, on four of the personality dimensions measured by the Temperament and Character Inventory–Revised (TCI-R): reward dependence, persistence, self-directedness, and cooperativeness.
Both patient groups also showed similar scores for mood and anxiety problems. This is notable, the investigators said, because it has been posited that patients often use gambling to regulate negative emotions associated with stressful life events and frustration; sexual compulsions also are considered to be a mechanism for regulating negative affect.
The only sociodemographic variable that differed between sexual addiction and gambling disorder was socioeconomic status, which was higher in sexual addiction. In fact, high socioeconomic status was a major predictor of sexual addiction. “This could be explained by the fact that many patients with gambling disorder tend to have a low educational level and a low income,” Dr. Farre and his associates wrote.
Yet the two disorders differed from each other to the extent that personality traits could be used to distinguish between them. Patients with gambling disorder had notably higher scores than normal for harm avoidance, novelty seeking, and self-transcendence, while patients with sexual addiction had higher scores for harm avoidance only and had low scores for novelty seeking. Also, patients with sexual addiction had low scores on persistence, compared with those with gambling disorder, indicating poorer perseverance and more difficulty managing frustrations.
Patients with both disorders would benefit from treatment aimed at increasing internal locus of control, learning to take responsibility for one’s own decisions, increasing planning capacity, and improving perception of self-efficacy and satisfaction with one’s abilities. Patients with gambling disorder should aim for improved self-control strategies and emotional regulation, while those with sexual addiction should focus on improving interpersonal relationships and deficiencies in socialization factors such as cooperation, empathy, and tolerance.
Patients with sexual addiction also would benefit from enhancing their ability to identify potentially hazardous conditions and to foresee the negative consequences of certain decisions, the investigators said.
The investigators cited several limitations of the study. One is the cross-sectional design, which they said, did not allow them to make causal inferences. Also, the sample sizes of the three groups were not balanaced.
Nevertheless, they said, their findings expand the understanding of sexual addiction, a condition “that has not been studied in depth,” which in turn opens up new directions for future research.
This study was supported by Fondo de Investigacion Sanitaria of Spain, Ministerio de Economia y Competitividad, and Generalitat de Catalunya. Dr. Farré and his associates did not report their financial disclosures.
Patients with sexual addiction and patients with gambling disorder share some psychopathologic features and sociodemographic traits that are not found in healthy control subjects, a study showed.
This finding supports the argument that sexual addiction “should be classified more closely to other behavioral addictions such as gambling disorder,” said Dr. Josep M. Farré of Hospital Universitari Quirón-Dexeus, Barcelona, and his associates.
However, patients with sexual addiction are different from those with gambling disorder in their personality traits, particularly with regard to responses to novelty. Both of these disorders “could benefit from ‘transdiagnostic’ treatment programs aimed to improve the character trait ‘self-directedness,’ since it is a factor associated with various personality disorders related to behavioral addictions,” the investigators said (Compr. Psychiatry 2015;56:59-68).
In what they described as the first study to examine the similarities and differences among these two clinical groups and healthy controls, Dr. Farré and his associates assessed during an 8-year period 59 patients seeking treatment for sexual addiction, 2,190 in treatment for gambling disorder, and 93 healthy volunteers who resided in the same geographical area as the clinical participants.
The mean age of the study participants was 42 years. Most (90%) were men, and approximately half were married or living with a partner.
All the study participants underwent a comprehensive battery of evaluations in face-to-face clinical interviews to measure sociodemographic characteristics, general psychopathology, personality traits, and gambling and sex behaviors.
Patients with sexual addiction had scores on all the scales of the Symptom Check List–90 Items–Revised (SCL-90-R) that were very similar to those of patients with gambling disorder, and both groups had significantly different scores from the control subjects. The two patient groups were very similar for somatization, obsession-compulsion, interpersonal sensitivity, depression, anxiety, hostility, phobic anxiety, paranoid ideation, and psychoticism. They also showed similar symptom intensity and similar overall levels of psychological distress.
Continue for more on patient scores >>
In addition, patients with both disorders had similar scores, as well as significantly lower scores than healthy controls, on four of the personality dimensions measured by the Temperament and Character Inventory–Revised (TCI-R): reward dependence, persistence, self-directedness, and cooperativeness.
Both patient groups also showed similar scores for mood and anxiety problems. This is notable, the investigators said, because it has been posited that patients often use gambling to regulate negative emotions associated with stressful life events and frustration; sexual compulsions also are considered to be a mechanism for regulating negative affect.
The only sociodemographic variable that differed between sexual addiction and gambling disorder was socioeconomic status, which was higher in sexual addiction. In fact, high socioeconomic status was a major predictor of sexual addiction. “This could be explained by the fact that many patients with gambling disorder tend to have a low educational level and a low income,” Dr. Farre and his associates wrote.
Yet the two disorders differed from each other to the extent that personality traits could be used to distinguish between them. Patients with gambling disorder had notably higher scores than normal for harm avoidance, novelty seeking, and self-transcendence, while patients with sexual addiction had higher scores for harm avoidance only and had low scores for novelty seeking. Also, patients with sexual addiction had low scores on persistence, compared with those with gambling disorder, indicating poorer perseverance and more difficulty managing frustrations.
Patients with both disorders would benefit from treatment aimed at increasing internal locus of control, learning to take responsibility for one’s own decisions, increasing planning capacity, and improving perception of self-efficacy and satisfaction with one’s abilities. Patients with gambling disorder should aim for improved self-control strategies and emotional regulation, while those with sexual addiction should focus on improving interpersonal relationships and deficiencies in socialization factors such as cooperation, empathy, and tolerance.
Patients with sexual addiction also would benefit from enhancing their ability to identify potentially hazardous conditions and to foresee the negative consequences of certain decisions, the investigators said.
The investigators cited several limitations of the study. One is the cross-sectional design, which they said, did not allow them to make causal inferences. Also, the sample sizes of the three groups were not balanaced.
Nevertheless, they said, their findings expand the understanding of sexual addiction, a condition “that has not been studied in depth,” which in turn opens up new directions for future research.
This study was supported by Fondo de Investigacion Sanitaria of Spain, Ministerio de Economia y Competitividad, and Generalitat de Catalunya. Dr. Farré and his associates did not report their financial disclosures.
Patients with sexual addiction and patients with gambling disorder share some psychopathologic features and sociodemographic traits that are not found in healthy control subjects, a study showed.
This finding supports the argument that sexual addiction “should be classified more closely to other behavioral addictions such as gambling disorder,” said Dr. Josep M. Farré of Hospital Universitari Quirón-Dexeus, Barcelona, and his associates.
However, patients with sexual addiction are different from those with gambling disorder in their personality traits, particularly with regard to responses to novelty. Both of these disorders “could benefit from ‘transdiagnostic’ treatment programs aimed to improve the character trait ‘self-directedness,’ since it is a factor associated with various personality disorders related to behavioral addictions,” the investigators said (Compr. Psychiatry 2015;56:59-68).
In what they described as the first study to examine the similarities and differences among these two clinical groups and healthy controls, Dr. Farré and his associates assessed during an 8-year period 59 patients seeking treatment for sexual addiction, 2,190 in treatment for gambling disorder, and 93 healthy volunteers who resided in the same geographical area as the clinical participants.
The mean age of the study participants was 42 years. Most (90%) were men, and approximately half were married or living with a partner.
All the study participants underwent a comprehensive battery of evaluations in face-to-face clinical interviews to measure sociodemographic characteristics, general psychopathology, personality traits, and gambling and sex behaviors.
Patients with sexual addiction had scores on all the scales of the Symptom Check List–90 Items–Revised (SCL-90-R) that were very similar to those of patients with gambling disorder, and both groups had significantly different scores from the control subjects. The two patient groups were very similar for somatization, obsession-compulsion, interpersonal sensitivity, depression, anxiety, hostility, phobic anxiety, paranoid ideation, and psychoticism. They also showed similar symptom intensity and similar overall levels of psychological distress.
Continue for more on patient scores >>
In addition, patients with both disorders had similar scores, as well as significantly lower scores than healthy controls, on four of the personality dimensions measured by the Temperament and Character Inventory–Revised (TCI-R): reward dependence, persistence, self-directedness, and cooperativeness.
Both patient groups also showed similar scores for mood and anxiety problems. This is notable, the investigators said, because it has been posited that patients often use gambling to regulate negative emotions associated with stressful life events and frustration; sexual compulsions also are considered to be a mechanism for regulating negative affect.
The only sociodemographic variable that differed between sexual addiction and gambling disorder was socioeconomic status, which was higher in sexual addiction. In fact, high socioeconomic status was a major predictor of sexual addiction. “This could be explained by the fact that many patients with gambling disorder tend to have a low educational level and a low income,” Dr. Farre and his associates wrote.
Yet the two disorders differed from each other to the extent that personality traits could be used to distinguish between them. Patients with gambling disorder had notably higher scores than normal for harm avoidance, novelty seeking, and self-transcendence, while patients with sexual addiction had higher scores for harm avoidance only and had low scores for novelty seeking. Also, patients with sexual addiction had low scores on persistence, compared with those with gambling disorder, indicating poorer perseverance and more difficulty managing frustrations.
Patients with both disorders would benefit from treatment aimed at increasing internal locus of control, learning to take responsibility for one’s own decisions, increasing planning capacity, and improving perception of self-efficacy and satisfaction with one’s abilities. Patients with gambling disorder should aim for improved self-control strategies and emotional regulation, while those with sexual addiction should focus on improving interpersonal relationships and deficiencies in socialization factors such as cooperation, empathy, and tolerance.
Patients with sexual addiction also would benefit from enhancing their ability to identify potentially hazardous conditions and to foresee the negative consequences of certain decisions, the investigators said.
The investigators cited several limitations of the study. One is the cross-sectional design, which they said, did not allow them to make causal inferences. Also, the sample sizes of the three groups were not balanaced.
Nevertheless, they said, their findings expand the understanding of sexual addiction, a condition “that has not been studied in depth,” which in turn opens up new directions for future research.
This study was supported by Fondo de Investigacion Sanitaria of Spain, Ministerio de Economia y Competitividad, and Generalitat de Catalunya. Dr. Farré and his associates did not report their financial disclosures.
Sex addiction, gambling disorder share similarities
Patients with sexual addiction and patients with gambling disorder share some psychopathologic features and sociodemographic traits that are not found in healthy control subjects, a study showed.
This finding supports the argument that sexual addiction “should be classified more closely to other behavioral addictions such as gambling disorder,” said Dr. Josep M. Farré of Hospital Universitari Quirón-Dexeus, Barcelona, and his associates.
However, patients with sexual addiction are different from those with gambling disorder in their personality traits, particularly with regard to responses to novelty. Both of these disorders “could benefit from ‘transdiagnostic’ treatment programs aimed to improve the character trait ‘self-directedness,’ since it is a factor associated with various personality disorders related to behavioral addictions,” the investigators said (Compr. Psychiatry 2015;56:59-68).
In what they described as the first study to examine the similarities and differences among these two clinical groups and healthy controls, Dr. Farré and his associates assessed during an 8-year period 59 patients seeking treatment for sexual addiction, 2,190 in treatment for gambling disorder, and 93 healthy volunteers who resided in the same geographical area as the clinical participants.
The mean age of the study participants was 42 years. Most (90%) were men, and approximately half were married or living with a partner.
All the study participants underwent a comprehensive battery of evaluations in face-to-face clinical interviews to measure sociodemographic characteristics, general psychopathology, personality traits, and gambling and sex behaviors.
Patients with sexual addiction had scores on all the scales of the Symptom Check List–90 Items–Revised (SCL-90-R) that were very similar to those of patients with gambling disorder, and both groups had significantly different scores from the control subjects. The two patient groups were very similar for somatization, obsession-compulsion, interpersonal sensitivity, depression, anxiety, hostility, phobic anxiety, paranoid ideation, and psychoticism. They also showed similar symptom intensity and similar overall levels of psychological distress.
In addition, patients with both disorders had similar scores, as well as significantly lower scores than healthy controls, on four of the personality dimensions measured by the Temperament and Character Inventory–Revised (TCI-R): reward dependence, persistence, self-directedness, and cooperativeness.
Both patient groups also showed similar scores for mood and anxiety problems. This is notable, the investigators said, because it has been posited that patients often use gambling to regulate negative emotions associated with stressful life events and frustration; sexual compulsions also are considered to be a mechanism for regulating negative affect.
The only sociodemographic variable that differed between sexual addiction and gambling disorder was socioeconomic status, which was higher in sexual addiction. In fact, high socioeconomic status was a major predictor of sexual addiction. “This could be explained by the fact that many patients with gambling disorder tend to have a low educational level and a low income,” Dr. Farre and his associates wrote.
Yet the two disorders differed from each other to the extent that personality traits could be used to distinguish between them. Patients with gambling disorder had notably higher scores than normal for harm avoidance, novelty seeking, and self-transcendence, while patients with sexual addiction had higher scores for harm avoidance only and had low scores for novelty seeking. Also, patients with sexual addiction had low scores on persistence, compared with those with gambling disorder, indicating poorer perseverance and more difficulty managing frustrations.
Patients with both disorders would benefit from treatment aimed at increasing internal locus of control, learning to take responsibility for one’s own decisions, increasing planning capacity, and improving perception of self-efficacy and satisfaction with one’s abilities. Patients with gambling disorder should aim for improved self-control strategies and emotional regulation, while those with sexual addiction should focus on improving interpersonal relationships and deficiencies in socialization factors such as cooperation, empathy, and tolerance.
Patients with sexual addiction also would benefit from enhancing their ability to identify potentially hazardous conditions and to foresee the negative consequences of certain decisions, the investigators said.
The investigators cited several limitations of the study. One is the cross-sectional design, which they said, did not allow them to make causal inferences. Also, the sample sizes of the three groups were not balanaced.
Nevertheless, they said, their findings expand the understanding of sexual addiction, a condition “that has not been studied in depth,” which in turn opens up new directions for future research.
This study was supported by Fondo de Investigacion Sanitaria of Spain, Ministerio de Economia y Competitividad, and Generalitat de Catalunya. Dr. Farré and his associates did not report their financial disclosures.
Patients with sexual addiction and patients with gambling disorder share some psychopathologic features and sociodemographic traits that are not found in healthy control subjects, a study showed.
This finding supports the argument that sexual addiction “should be classified more closely to other behavioral addictions such as gambling disorder,” said Dr. Josep M. Farré of Hospital Universitari Quirón-Dexeus, Barcelona, and his associates.
However, patients with sexual addiction are different from those with gambling disorder in their personality traits, particularly with regard to responses to novelty. Both of these disorders “could benefit from ‘transdiagnostic’ treatment programs aimed to improve the character trait ‘self-directedness,’ since it is a factor associated with various personality disorders related to behavioral addictions,” the investigators said (Compr. Psychiatry 2015;56:59-68).
In what they described as the first study to examine the similarities and differences among these two clinical groups and healthy controls, Dr. Farré and his associates assessed during an 8-year period 59 patients seeking treatment for sexual addiction, 2,190 in treatment for gambling disorder, and 93 healthy volunteers who resided in the same geographical area as the clinical participants.
The mean age of the study participants was 42 years. Most (90%) were men, and approximately half were married or living with a partner.
All the study participants underwent a comprehensive battery of evaluations in face-to-face clinical interviews to measure sociodemographic characteristics, general psychopathology, personality traits, and gambling and sex behaviors.
Patients with sexual addiction had scores on all the scales of the Symptom Check List–90 Items–Revised (SCL-90-R) that were very similar to those of patients with gambling disorder, and both groups had significantly different scores from the control subjects. The two patient groups were very similar for somatization, obsession-compulsion, interpersonal sensitivity, depression, anxiety, hostility, phobic anxiety, paranoid ideation, and psychoticism. They also showed similar symptom intensity and similar overall levels of psychological distress.
In addition, patients with both disorders had similar scores, as well as significantly lower scores than healthy controls, on four of the personality dimensions measured by the Temperament and Character Inventory–Revised (TCI-R): reward dependence, persistence, self-directedness, and cooperativeness.
Both patient groups also showed similar scores for mood and anxiety problems. This is notable, the investigators said, because it has been posited that patients often use gambling to regulate negative emotions associated with stressful life events and frustration; sexual compulsions also are considered to be a mechanism for regulating negative affect.
The only sociodemographic variable that differed between sexual addiction and gambling disorder was socioeconomic status, which was higher in sexual addiction. In fact, high socioeconomic status was a major predictor of sexual addiction. “This could be explained by the fact that many patients with gambling disorder tend to have a low educational level and a low income,” Dr. Farre and his associates wrote.
Yet the two disorders differed from each other to the extent that personality traits could be used to distinguish between them. Patients with gambling disorder had notably higher scores than normal for harm avoidance, novelty seeking, and self-transcendence, while patients with sexual addiction had higher scores for harm avoidance only and had low scores for novelty seeking. Also, patients with sexual addiction had low scores on persistence, compared with those with gambling disorder, indicating poorer perseverance and more difficulty managing frustrations.
Patients with both disorders would benefit from treatment aimed at increasing internal locus of control, learning to take responsibility for one’s own decisions, increasing planning capacity, and improving perception of self-efficacy and satisfaction with one’s abilities. Patients with gambling disorder should aim for improved self-control strategies and emotional regulation, while those with sexual addiction should focus on improving interpersonal relationships and deficiencies in socialization factors such as cooperation, empathy, and tolerance.
Patients with sexual addiction also would benefit from enhancing their ability to identify potentially hazardous conditions and to foresee the negative consequences of certain decisions, the investigators said.
The investigators cited several limitations of the study. One is the cross-sectional design, which they said, did not allow them to make causal inferences. Also, the sample sizes of the three groups were not balanaced.
Nevertheless, they said, their findings expand the understanding of sexual addiction, a condition “that has not been studied in depth,” which in turn opens up new directions for future research.
This study was supported by Fondo de Investigacion Sanitaria of Spain, Ministerio de Economia y Competitividad, and Generalitat de Catalunya. Dr. Farré and his associates did not report their financial disclosures.
Patients with sexual addiction and patients with gambling disorder share some psychopathologic features and sociodemographic traits that are not found in healthy control subjects, a study showed.
This finding supports the argument that sexual addiction “should be classified more closely to other behavioral addictions such as gambling disorder,” said Dr. Josep M. Farré of Hospital Universitari Quirón-Dexeus, Barcelona, and his associates.
However, patients with sexual addiction are different from those with gambling disorder in their personality traits, particularly with regard to responses to novelty. Both of these disorders “could benefit from ‘transdiagnostic’ treatment programs aimed to improve the character trait ‘self-directedness,’ since it is a factor associated with various personality disorders related to behavioral addictions,” the investigators said (Compr. Psychiatry 2015;56:59-68).
In what they described as the first study to examine the similarities and differences among these two clinical groups and healthy controls, Dr. Farré and his associates assessed during an 8-year period 59 patients seeking treatment for sexual addiction, 2,190 in treatment for gambling disorder, and 93 healthy volunteers who resided in the same geographical area as the clinical participants.
The mean age of the study participants was 42 years. Most (90%) were men, and approximately half were married or living with a partner.
All the study participants underwent a comprehensive battery of evaluations in face-to-face clinical interviews to measure sociodemographic characteristics, general psychopathology, personality traits, and gambling and sex behaviors.
Patients with sexual addiction had scores on all the scales of the Symptom Check List–90 Items–Revised (SCL-90-R) that were very similar to those of patients with gambling disorder, and both groups had significantly different scores from the control subjects. The two patient groups were very similar for somatization, obsession-compulsion, interpersonal sensitivity, depression, anxiety, hostility, phobic anxiety, paranoid ideation, and psychoticism. They also showed similar symptom intensity and similar overall levels of psychological distress.
In addition, patients with both disorders had similar scores, as well as significantly lower scores than healthy controls, on four of the personality dimensions measured by the Temperament and Character Inventory–Revised (TCI-R): reward dependence, persistence, self-directedness, and cooperativeness.
Both patient groups also showed similar scores for mood and anxiety problems. This is notable, the investigators said, because it has been posited that patients often use gambling to regulate negative emotions associated with stressful life events and frustration; sexual compulsions also are considered to be a mechanism for regulating negative affect.
The only sociodemographic variable that differed between sexual addiction and gambling disorder was socioeconomic status, which was higher in sexual addiction. In fact, high socioeconomic status was a major predictor of sexual addiction. “This could be explained by the fact that many patients with gambling disorder tend to have a low educational level and a low income,” Dr. Farre and his associates wrote.
Yet the two disorders differed from each other to the extent that personality traits could be used to distinguish between them. Patients with gambling disorder had notably higher scores than normal for harm avoidance, novelty seeking, and self-transcendence, while patients with sexual addiction had higher scores for harm avoidance only and had low scores for novelty seeking. Also, patients with sexual addiction had low scores on persistence, compared with those with gambling disorder, indicating poorer perseverance and more difficulty managing frustrations.
Patients with both disorders would benefit from treatment aimed at increasing internal locus of control, learning to take responsibility for one’s own decisions, increasing planning capacity, and improving perception of self-efficacy and satisfaction with one’s abilities. Patients with gambling disorder should aim for improved self-control strategies and emotional regulation, while those with sexual addiction should focus on improving interpersonal relationships and deficiencies in socialization factors such as cooperation, empathy, and tolerance.
Patients with sexual addiction also would benefit from enhancing their ability to identify potentially hazardous conditions and to foresee the negative consequences of certain decisions, the investigators said.
The investigators cited several limitations of the study. One is the cross-sectional design, which they said, did not allow them to make causal inferences. Also, the sample sizes of the three groups were not balanaced.
Nevertheless, they said, their findings expand the understanding of sexual addiction, a condition “that has not been studied in depth,” which in turn opens up new directions for future research.
This study was supported by Fondo de Investigacion Sanitaria of Spain, Ministerio de Economia y Competitividad, and Generalitat de Catalunya. Dr. Farré and his associates did not report their financial disclosures.
Key clinical point: Sex addiction and gambling disorder “could benefit from ‘transdiagnostic’ treatment programs.”
Major finding: Patients with sexual addiction were very similar to those with gambling disorder on measures of somatization, obsession-compulsion, interpersonal sensitivity, depression, anxiety, hostility, phobic anxiety, paranoid ideation, and psychoticism, and they also showed similar symptom intensity and similar overall levels of psychological distress.
Data source: A cross-sectional cohort study comparing personality and demographic traits among 59 patients seeking help for sexual addiction, 2,190 being treated for gambling disorder, and 93 healthy controls with no psychiatric diagnoses.
Disclosures: This study was supported by Fondo de Investigacion Sanitaria of Spain, Ministerio de Economia y Competitividad, and Generalitat de Catalunya. Dr. Farré and his associates did not report their financial disclosures.
Users of illicit buprenorphine want help, can’t find it
Most participants in a needle-exchange program reported that they abused buprenorphine and wanted treatment to help them quit but didn’t know where to get treatment, according to a report published online in the Journal of Substance Abuse Treatment.
This finding emphasizes the importance of policies to secure access to treatment. Outreach and education efforts also are important “to link marginalized people who use drugs to buprenorphine treatment providers,” said Dr. Aaron D. Fox of Albert Einstein College and Montefiore Medical Center, New York, and his associates.
Buprenorphine maintenance therapy (BMT) is effective against opioid addiction but is underused. Until now, most studies of the barriers to BMT use have focused on the difficulties that physicians or health systems have in providing it. Patients’ inability to access treatment, to pay for treatment, and other potential barriers have not been well investigated, Dr. Fox and his associates said (J. Subst. Abuse Treat. 2015;48:112-6 [doi:10.1016/j.jsat.2014.07.015]).
They performed a cross-sectional study of the barriers to BMT use among people attending a single community-based harm reduction agency that provides syringe exchange and various social services “within an area of New York City that is severely impacted by drug use, HIV/AIDS, and hepatitis C.” The 102 study participants enrolled during a 6-week period, volunteering to complete a 25-minute computer-assisted self-interview in exchange for a small amount of cash as compensation.
Approximately half (57) of the participants said that they used illicit buprenorphine, confirming that the practice is widespread in this population.
Twenty-nine (51%) of those who abused buprenorphine said they were interested in initiating BMT. The most common reason they gave for failing to do so was they “did not know where to go to get treatment.” In New York City, “opioid treatment programs primarily offer methadone maintenance treatment and not BMT, so even experienced participants may not have known how to access BMT,” the investigators noted.
Very few of the respondents said that the cost of treatment, mistrust of doctors, or the stigma of attending a treatment facility presented barriers to access. Medicaid covers BMT in New York state, and almost all the study participants had Medicaid coverage. Thus, “relatively minor interventions addressing the barriers to BMT could dramatically improve treatment access,” Dr. Fox and his associates said.
Many of the study participants said they would readily participate if BMT were offered at a harm-reduction agency such as the one with their needle-exchange program. This offers a promising approach to improving BMT access, the researchers said.
“BMT may be prescribed in office-based settings, so directly initiating BMT onsite at harm reduction agencies may be a better option than referral to address the treatment gap,” they noted.
This study was limited in that the sample was drawn from a single community-based program in a large urban center. The findings may not be generalizable to other settings or geographic locations, Dr. Fox and his associates said.
Most participants in a needle-exchange program reported that they abused buprenorphine and wanted treatment to help them quit but didn’t know where to get treatment, according to a report published online in the Journal of Substance Abuse Treatment.
This finding emphasizes the importance of policies to secure access to treatment. Outreach and education efforts also are important “to link marginalized people who use drugs to buprenorphine treatment providers,” said Dr. Aaron D. Fox of Albert Einstein College and Montefiore Medical Center, New York, and his associates.
Buprenorphine maintenance therapy (BMT) is effective against opioid addiction but is underused. Until now, most studies of the barriers to BMT use have focused on the difficulties that physicians or health systems have in providing it. Patients’ inability to access treatment, to pay for treatment, and other potential barriers have not been well investigated, Dr. Fox and his associates said (J. Subst. Abuse Treat. 2015;48:112-6 [doi:10.1016/j.jsat.2014.07.015]).
They performed a cross-sectional study of the barriers to BMT use among people attending a single community-based harm reduction agency that provides syringe exchange and various social services “within an area of New York City that is severely impacted by drug use, HIV/AIDS, and hepatitis C.” The 102 study participants enrolled during a 6-week period, volunteering to complete a 25-minute computer-assisted self-interview in exchange for a small amount of cash as compensation.
Approximately half (57) of the participants said that they used illicit buprenorphine, confirming that the practice is widespread in this population.
Twenty-nine (51%) of those who abused buprenorphine said they were interested in initiating BMT. The most common reason they gave for failing to do so was they “did not know where to go to get treatment.” In New York City, “opioid treatment programs primarily offer methadone maintenance treatment and not BMT, so even experienced participants may not have known how to access BMT,” the investigators noted.
Very few of the respondents said that the cost of treatment, mistrust of doctors, or the stigma of attending a treatment facility presented barriers to access. Medicaid covers BMT in New York state, and almost all the study participants had Medicaid coverage. Thus, “relatively minor interventions addressing the barriers to BMT could dramatically improve treatment access,” Dr. Fox and his associates said.
Many of the study participants said they would readily participate if BMT were offered at a harm-reduction agency such as the one with their needle-exchange program. This offers a promising approach to improving BMT access, the researchers said.
“BMT may be prescribed in office-based settings, so directly initiating BMT onsite at harm reduction agencies may be a better option than referral to address the treatment gap,” they noted.
This study was limited in that the sample was drawn from a single community-based program in a large urban center. The findings may not be generalizable to other settings or geographic locations, Dr. Fox and his associates said.
Most participants in a needle-exchange program reported that they abused buprenorphine and wanted treatment to help them quit but didn’t know where to get treatment, according to a report published online in the Journal of Substance Abuse Treatment.
This finding emphasizes the importance of policies to secure access to treatment. Outreach and education efforts also are important “to link marginalized people who use drugs to buprenorphine treatment providers,” said Dr. Aaron D. Fox of Albert Einstein College and Montefiore Medical Center, New York, and his associates.
Buprenorphine maintenance therapy (BMT) is effective against opioid addiction but is underused. Until now, most studies of the barriers to BMT use have focused on the difficulties that physicians or health systems have in providing it. Patients’ inability to access treatment, to pay for treatment, and other potential barriers have not been well investigated, Dr. Fox and his associates said (J. Subst. Abuse Treat. 2015;48:112-6 [doi:10.1016/j.jsat.2014.07.015]).
They performed a cross-sectional study of the barriers to BMT use among people attending a single community-based harm reduction agency that provides syringe exchange and various social services “within an area of New York City that is severely impacted by drug use, HIV/AIDS, and hepatitis C.” The 102 study participants enrolled during a 6-week period, volunteering to complete a 25-minute computer-assisted self-interview in exchange for a small amount of cash as compensation.
Approximately half (57) of the participants said that they used illicit buprenorphine, confirming that the practice is widespread in this population.
Twenty-nine (51%) of those who abused buprenorphine said they were interested in initiating BMT. The most common reason they gave for failing to do so was they “did not know where to go to get treatment.” In New York City, “opioid treatment programs primarily offer methadone maintenance treatment and not BMT, so even experienced participants may not have known how to access BMT,” the investigators noted.
Very few of the respondents said that the cost of treatment, mistrust of doctors, or the stigma of attending a treatment facility presented barriers to access. Medicaid covers BMT in New York state, and almost all the study participants had Medicaid coverage. Thus, “relatively minor interventions addressing the barriers to BMT could dramatically improve treatment access,” Dr. Fox and his associates said.
Many of the study participants said they would readily participate if BMT were offered at a harm-reduction agency such as the one with their needle-exchange program. This offers a promising approach to improving BMT access, the researchers said.
“BMT may be prescribed in office-based settings, so directly initiating BMT onsite at harm reduction agencies may be a better option than referral to address the treatment gap,” they noted.
This study was limited in that the sample was drawn from a single community-based program in a large urban center. The findings may not be generalizable to other settings or geographic locations, Dr. Fox and his associates said.
FROM THE JOURNAL OF SUBSTANCE ABUSE TREATMENT
Key clinical point: Most users of illicit buprenorphine at an New York City harm-reduction facility said they wanted treatment but didn’t know where to find it.
Major finding: Of the 57 participants who used illicit buprenorphine, 29 (51%) said they would like to initiate buprenorphine maintenance therapy, but most didn’t know where to get the treatment.
Data source: A cross-sectional survey of 102 people using a needle-exchange program at a single harm-reduction center in New York.
Disclosures: This study was supported by the National Institutes of Health, the Center for AIDS Research at Albert Einstein College of Medicine, Montefiore Medical Center, and the New York Academy of Medicine. Dr. Fox and his associates were not required to provide financial disclosures.
Hospitalization for pneumonia raises CVD risk
Among older adults, hospitalization for pneumonia raises the short-term (1-month) and long-term (10-year) risk of cardiovascular disease events to a degree comparable to those of smoking, diabetes, and hypertension, according to a report published online Jan. 20 in JAMA.
“Our findings suggest that hospitalization for pneumonia should be considered an independent cardiovascular risk factor” and “should prompt clinical trials to test targeted strategies”’ to prevent the disease in this patient population, said Dr. Vicente F. Corrales-Medina of the University of Ottawa and the Ottawa Hospital Research Institute.
The risk of cardiovascular disease (CVD) events within 30 days of severe infections, mainly those involving the respiratory tract, is well established, but the more lasting effects are uncertain. In what the researchers described as “the first study to document the temporal variation in the long-term risk of CVD ... using rigorous methods to adjust for many potential confounders,” they analyzed data from two multicenter population-based cohorts that were followed for 21 years.
The 591 participants in the Cardiovascular Health Study were 65 years of age or older and had been hospitalized for pneumonia. When researchers compared their outcomes to 1,182 matched controls without pneumonia, they found that in the pneumonia group the rate of CVD events was fourfold higher at 30 days, dropped to twofold higher throughout the rest of the first year, and leveled out at 1.5-fold higher for the remainder of the decade.
Researchers then verified this risk pattern in a cohort of 680 pneumonia patients aged 45-64 years and 1,360 matched controls in the Atherosclerosis Risk in Communities study. The increased risk conferred by hospitalization for pneumonia persisted after the data were adjusted to account for demographic traits, preexisting CVD risk factors, and measures of patient frailty; it also was robust to numerous sensitivity analyses, the researchers said (JAMA 2015 Jan. 20 [doi:10.1001/jama.2014.18229]).
Moreover, the magnitude of risk conferred by hospitalization for pneumonia “was similar or higher, compared with the risk of CVD associated with traditional risk factors such as smoking, diabetes, and hypertension,” wrote Dr. Corrales-Medina and his associates.
The Ottawa Hospital, the Ottawa Hospital Research Institute, and the Canadian National Institute of General Medical Sciences funded the study. Dr. Corrales-Medina reported having no financial disclosures; an associate reported ties to Biogen Idec, Bristol-Myers Squibb/Pfizer, Boehringer Ingelheim, CardioNet, Daiichi Sankyo, diaDexus, Janssen, Merck/Organon, and Sanofi.
Among older adults, hospitalization for pneumonia raises the short-term (1-month) and long-term (10-year) risk of cardiovascular disease events to a degree comparable to those of smoking, diabetes, and hypertension, according to a report published online Jan. 20 in JAMA.
“Our findings suggest that hospitalization for pneumonia should be considered an independent cardiovascular risk factor” and “should prompt clinical trials to test targeted strategies”’ to prevent the disease in this patient population, said Dr. Vicente F. Corrales-Medina of the University of Ottawa and the Ottawa Hospital Research Institute.
The risk of cardiovascular disease (CVD) events within 30 days of severe infections, mainly those involving the respiratory tract, is well established, but the more lasting effects are uncertain. In what the researchers described as “the first study to document the temporal variation in the long-term risk of CVD ... using rigorous methods to adjust for many potential confounders,” they analyzed data from two multicenter population-based cohorts that were followed for 21 years.
The 591 participants in the Cardiovascular Health Study were 65 years of age or older and had been hospitalized for pneumonia. When researchers compared their outcomes to 1,182 matched controls without pneumonia, they found that in the pneumonia group the rate of CVD events was fourfold higher at 30 days, dropped to twofold higher throughout the rest of the first year, and leveled out at 1.5-fold higher for the remainder of the decade.
Researchers then verified this risk pattern in a cohort of 680 pneumonia patients aged 45-64 years and 1,360 matched controls in the Atherosclerosis Risk in Communities study. The increased risk conferred by hospitalization for pneumonia persisted after the data were adjusted to account for demographic traits, preexisting CVD risk factors, and measures of patient frailty; it also was robust to numerous sensitivity analyses, the researchers said (JAMA 2015 Jan. 20 [doi:10.1001/jama.2014.18229]).
Moreover, the magnitude of risk conferred by hospitalization for pneumonia “was similar or higher, compared with the risk of CVD associated with traditional risk factors such as smoking, diabetes, and hypertension,” wrote Dr. Corrales-Medina and his associates.
The Ottawa Hospital, the Ottawa Hospital Research Institute, and the Canadian National Institute of General Medical Sciences funded the study. Dr. Corrales-Medina reported having no financial disclosures; an associate reported ties to Biogen Idec, Bristol-Myers Squibb/Pfizer, Boehringer Ingelheim, CardioNet, Daiichi Sankyo, diaDexus, Janssen, Merck/Organon, and Sanofi.
Among older adults, hospitalization for pneumonia raises the short-term (1-month) and long-term (10-year) risk of cardiovascular disease events to a degree comparable to those of smoking, diabetes, and hypertension, according to a report published online Jan. 20 in JAMA.
“Our findings suggest that hospitalization for pneumonia should be considered an independent cardiovascular risk factor” and “should prompt clinical trials to test targeted strategies”’ to prevent the disease in this patient population, said Dr. Vicente F. Corrales-Medina of the University of Ottawa and the Ottawa Hospital Research Institute.
The risk of cardiovascular disease (CVD) events within 30 days of severe infections, mainly those involving the respiratory tract, is well established, but the more lasting effects are uncertain. In what the researchers described as “the first study to document the temporal variation in the long-term risk of CVD ... using rigorous methods to adjust for many potential confounders,” they analyzed data from two multicenter population-based cohorts that were followed for 21 years.
The 591 participants in the Cardiovascular Health Study were 65 years of age or older and had been hospitalized for pneumonia. When researchers compared their outcomes to 1,182 matched controls without pneumonia, they found that in the pneumonia group the rate of CVD events was fourfold higher at 30 days, dropped to twofold higher throughout the rest of the first year, and leveled out at 1.5-fold higher for the remainder of the decade.
Researchers then verified this risk pattern in a cohort of 680 pneumonia patients aged 45-64 years and 1,360 matched controls in the Atherosclerosis Risk in Communities study. The increased risk conferred by hospitalization for pneumonia persisted after the data were adjusted to account for demographic traits, preexisting CVD risk factors, and measures of patient frailty; it also was robust to numerous sensitivity analyses, the researchers said (JAMA 2015 Jan. 20 [doi:10.1001/jama.2014.18229]).
Moreover, the magnitude of risk conferred by hospitalization for pneumonia “was similar or higher, compared with the risk of CVD associated with traditional risk factors such as smoking, diabetes, and hypertension,” wrote Dr. Corrales-Medina and his associates.
The Ottawa Hospital, the Ottawa Hospital Research Institute, and the Canadian National Institute of General Medical Sciences funded the study. Dr. Corrales-Medina reported having no financial disclosures; an associate reported ties to Biogen Idec, Bristol-Myers Squibb/Pfizer, Boehringer Ingelheim, CardioNet, Daiichi Sankyo, diaDexus, Janssen, Merck/Organon, and Sanofi.
FROM JAMA
Key clinical point: Among older adults, hospitalization for pneumonia raises both short-term and long-term risks of a CVD event.
Major finding: The rate of CVD events was fourfold higher at 30 days, dropped to twofold higher throughout the rest of the first year, and leveled out at 1.5-fold higher for the remainder of the decade.
Data source: A secondary analysis of data from two multicenter population-based cohorts, of 5,888 and 15,792 older adults, followed for 21 years.
Disclosures: The Ottawa Hospital, the Ottawa Hospital Research Institute, and the Canadian National Institute of General Medical Sciences funded the study. Dr. Corrales-Medina reported having no financial disclosures; an associate reported ties to Biogen Idec, Bristol-Myers Squibb/Pfizer, Boehringer Ingelheim, CardioNet, Daiichi Sankyo, diaDexus, Janssen, Merck/Organon, and Sanofi.
ICSI use without male factor infertility climbs, but births decline
The use of intracytoplasmic sperm injection in fresh in vitro fertilization cycles has doubled since 1996, increasing chiefly among couples without male factor infertility, but the increase hasn’t been accompanied by any improvement in reproductive outcomes.
ICSI use in cases without male factor infertility is associated with small, but statistically significant declines in implantation, pregnancy, and live birth rates, compared with conventional IVF, Sheree L. Boulet, Dr.P.H., of the Division of Reproductive Health, Centers for Disease Control and Prevention in Atlanta, and her colleagues, reported Jan. 20 in JAMA.
The use of ICSI for men with borderline or even normal semen characteristics has increased over the past 20 years, even though there is no clear evidence of its superiority to conventional IVF. To assess national trends in ICSI use in more detail, the researchers analyzed data from the National Assisted Reproductive Technology Surveillance System for 1,395,634 fresh IVF cycles from 1996 through 2012.
Overall, about 65% of these cycles used ICSI, including 51% of cycles in which there was no male factor infertility.
The percentage of fresh IVF cycles using ICSI increased from 36.4% to 76.2% during the study period. Among couples with no male factor infertility, ICSI use increased from 15.4% to 66.9% of all fresh IVF cycles.
In the entire study population, there were no differences between cycles using ICSI and cycles using conventional IVF in reproductive outcomes. However, in the large subset of couples without male factor infertility, ICSI use was associated with significantly lower implantation rates (23.0% vs 25.2%), pregnancy rates (44.9% vs 47.9%), and live birth rates (36.5% vs 39.2%), according to the study (JAMA. 2015;313:255-63 [doi:10.1001/jama.2014.17985]).
The differences “may be a function of the large sample size and thus not clinically relevant,” the researchers wrote. But the findings suggest that the use of ICSI may improve fertilization rates, but not implementation or pregnancy rates for unexplained infertility, advanced maternal age, and low oocyte yield.
The underlying reasons for these findings are not yet known. ICSI bypasses natural barriers to fertilization, which increases the chance of fertilization, but at the same time increases the possibility of transmitting genetic defects.
It is possible that “by bypassing natural selection, ICSI use could have resulted in poorer-quality embryos, compared with conventional IVF, leading to poorer reproductive outcomes,” the researchers wrote. Another possibility is that ICSI may have been used as a rescue measure after attempts at conventional IVF failed; in such cases, oocyte quality likely was poor, leading to poorer outcomes.
The use of intracytoplasmic sperm injection in fresh in vitro fertilization cycles has doubled since 1996, increasing chiefly among couples without male factor infertility, but the increase hasn’t been accompanied by any improvement in reproductive outcomes.
ICSI use in cases without male factor infertility is associated with small, but statistically significant declines in implantation, pregnancy, and live birth rates, compared with conventional IVF, Sheree L. Boulet, Dr.P.H., of the Division of Reproductive Health, Centers for Disease Control and Prevention in Atlanta, and her colleagues, reported Jan. 20 in JAMA.
The use of ICSI for men with borderline or even normal semen characteristics has increased over the past 20 years, even though there is no clear evidence of its superiority to conventional IVF. To assess national trends in ICSI use in more detail, the researchers analyzed data from the National Assisted Reproductive Technology Surveillance System for 1,395,634 fresh IVF cycles from 1996 through 2012.
Overall, about 65% of these cycles used ICSI, including 51% of cycles in which there was no male factor infertility.
The percentage of fresh IVF cycles using ICSI increased from 36.4% to 76.2% during the study period. Among couples with no male factor infertility, ICSI use increased from 15.4% to 66.9% of all fresh IVF cycles.
In the entire study population, there were no differences between cycles using ICSI and cycles using conventional IVF in reproductive outcomes. However, in the large subset of couples without male factor infertility, ICSI use was associated with significantly lower implantation rates (23.0% vs 25.2%), pregnancy rates (44.9% vs 47.9%), and live birth rates (36.5% vs 39.2%), according to the study (JAMA. 2015;313:255-63 [doi:10.1001/jama.2014.17985]).
The differences “may be a function of the large sample size and thus not clinically relevant,” the researchers wrote. But the findings suggest that the use of ICSI may improve fertilization rates, but not implementation or pregnancy rates for unexplained infertility, advanced maternal age, and low oocyte yield.
The underlying reasons for these findings are not yet known. ICSI bypasses natural barriers to fertilization, which increases the chance of fertilization, but at the same time increases the possibility of transmitting genetic defects.
It is possible that “by bypassing natural selection, ICSI use could have resulted in poorer-quality embryos, compared with conventional IVF, leading to poorer reproductive outcomes,” the researchers wrote. Another possibility is that ICSI may have been used as a rescue measure after attempts at conventional IVF failed; in such cases, oocyte quality likely was poor, leading to poorer outcomes.
The use of intracytoplasmic sperm injection in fresh in vitro fertilization cycles has doubled since 1996, increasing chiefly among couples without male factor infertility, but the increase hasn’t been accompanied by any improvement in reproductive outcomes.
ICSI use in cases without male factor infertility is associated with small, but statistically significant declines in implantation, pregnancy, and live birth rates, compared with conventional IVF, Sheree L. Boulet, Dr.P.H., of the Division of Reproductive Health, Centers for Disease Control and Prevention in Atlanta, and her colleagues, reported Jan. 20 in JAMA.
The use of ICSI for men with borderline or even normal semen characteristics has increased over the past 20 years, even though there is no clear evidence of its superiority to conventional IVF. To assess national trends in ICSI use in more detail, the researchers analyzed data from the National Assisted Reproductive Technology Surveillance System for 1,395,634 fresh IVF cycles from 1996 through 2012.
Overall, about 65% of these cycles used ICSI, including 51% of cycles in which there was no male factor infertility.
The percentage of fresh IVF cycles using ICSI increased from 36.4% to 76.2% during the study period. Among couples with no male factor infertility, ICSI use increased from 15.4% to 66.9% of all fresh IVF cycles.
In the entire study population, there were no differences between cycles using ICSI and cycles using conventional IVF in reproductive outcomes. However, in the large subset of couples without male factor infertility, ICSI use was associated with significantly lower implantation rates (23.0% vs 25.2%), pregnancy rates (44.9% vs 47.9%), and live birth rates (36.5% vs 39.2%), according to the study (JAMA. 2015;313:255-63 [doi:10.1001/jama.2014.17985]).
The differences “may be a function of the large sample size and thus not clinically relevant,” the researchers wrote. But the findings suggest that the use of ICSI may improve fertilization rates, but not implementation or pregnancy rates for unexplained infertility, advanced maternal age, and low oocyte yield.
The underlying reasons for these findings are not yet known. ICSI bypasses natural barriers to fertilization, which increases the chance of fertilization, but at the same time increases the possibility of transmitting genetic defects.
It is possible that “by bypassing natural selection, ICSI use could have resulted in poorer-quality embryos, compared with conventional IVF, leading to poorer reproductive outcomes,” the researchers wrote. Another possibility is that ICSI may have been used as a rescue measure after attempts at conventional IVF failed; in such cases, oocyte quality likely was poor, leading to poorer outcomes.
Key clinical point: The use of ICSI in fresh IVF cycles has doubled since 1996, but reproductive outcomes have worsened slightly.
Major finding: In a large subset of couples without male factor infertility, ICSI use was associated with slightly, but significantly lower implantation rates (23.0% vs 25.2%), pregnancy rates (44.9% vs 47.9%), and live birth rates (36.5% vs 39.2%).
Data source: A retrospective observational cohort study of data from the National Assisted Reproductive Technology Surveillance reporting system regarding 1,395,634 fresh IVF cycles from 1996 through 2012.
Disclosures: This study was supported by the National Center for Advancing Translational Sciences and the National Institutes of Health. The researchers reported having no financial disclosures.